Vitamin D supplementation and clinical outcomes in COVID-19: a systematic review and meta-analysis
et al., Journal of Endocrinological Investigation, doi:10.1007/s40618-021-01614-4, Jun 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
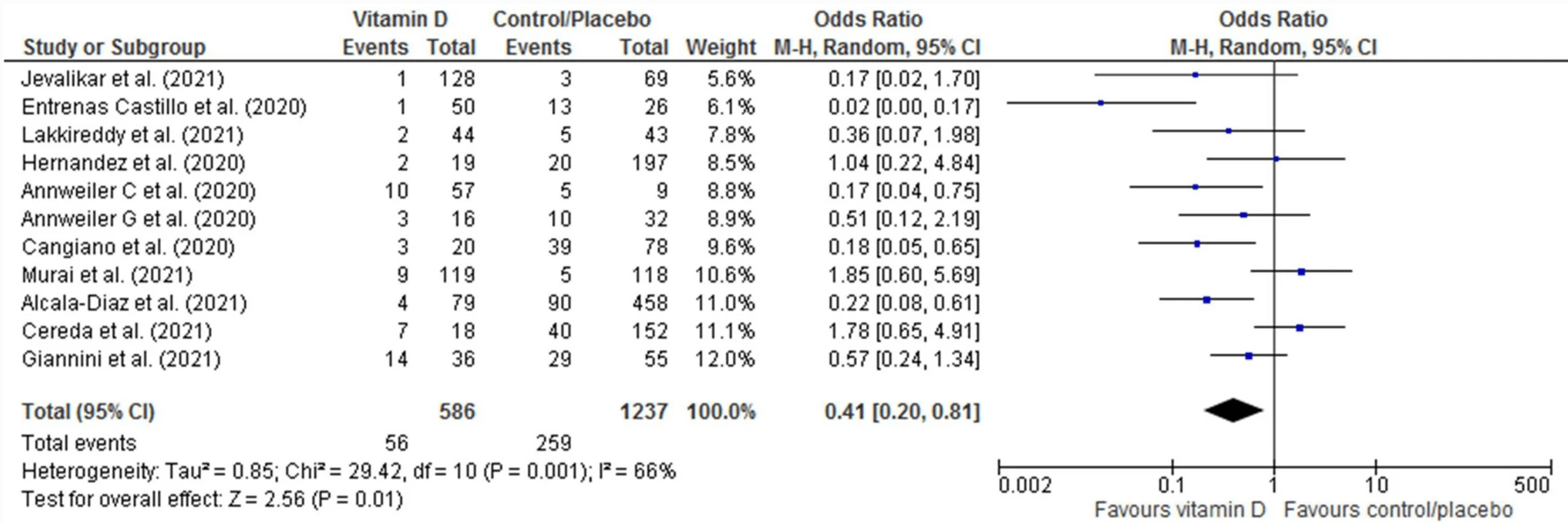
Meta analysis of 13 vitamin D treatment studies, showing significantly lower ICU admission/mortality with treatment.
22 meta-analyses show significant improvements with vitamin D treatment for mortality1-15,
mechanical ventilation1,5,6,11,16-18 ,
ICU admission1,3,5,6,9,11,13,15-21 ,
hospitalization11,
severity2,4,5,10,22 , and
cases7,20,22 .
Currently there are 137 vitamin D treatment for COVID-19 studies, showing 39% lower mortality [32‑45%], 17% lower ventilation [-5‑35%], 45% lower ICU admission [28‑57%], 22% lower hospitalization [13‑30%], and 17% fewer cases [9‑25%].
1.
Shah et al., Does vitamin D supplementation reduce COVID-19 severity? - a systematic review, QJM: An International Journal of Medicine, doi:10.1093/qjmed/hcac040.
2.
Nikniaz et al., The impact of vitamin D supplementation on mortality rate and clinical outcomes of COVID-19 patients: A systematic review and meta-analysis, Pharmaceutical Sciences, doi:10.34172/PS.2021.13.
3.
Hosseini et al., Effects of Vitamin D Supplementation on COVID-19 Related Outcomes: A Systematic Review and Meta-Analysis, Nutrients, doi:10.3390/nu14102134.
4.
D’Ecclesiis et al., Vitamin D and SARS-CoV2 infection, severity and mortality: A systematic review and meta-analysis, PLOS ONE, doi:10.1371/journal.pone.0268396.
5.
Xie et al., Micronutrient perspective on COVID-19: Umbrella review and reanalysis of meta-analyses, Critical Reviews in Food Science and Nutrition, doi:10.1080/10408398.2023.2174948.
6.
Hariyanto et al., Vitamin D supplementation and Covid‐19 outcomes: A systematic review, meta‐analysis and meta‐regression, Reviews in Medical Virology, doi:10.1002/rmv.2269.
7.
Begum et al., The Role of Vitamin D in COVID-19 Survival and Prevention: A Meta-analysis, Sudan Journal of Medical Sciences, doi:10.18502/sjms.v19i1.15776.
8.
Jamilian et al., The role of vitamin D in outcomes of critical care in COVID-19 patients: Evidence from an umbrella meta-analysis of interventional and observational studies, Public Health Nutrition, doi:10.1017/S1368980024000934.
9.
Sobczak et al., Effect of Vitamin D3 Supplementation on Severe COVID-19: A Meta-Analysis of Randomized Clinical Trials, Nutrients, doi:10.3390/nu16101402.
10.
Petrelli et al., Therapeutic and prognostic role of vitamin D for COVID-19 infection: A systematic review and meta-analysis of 43 observational studies, The Journal of Steroid Biochemistry and Molecular Biology, doi:10.1016/j.jsbmb.2021.105883.
11.
Asla et al., Vitamin D on COVID-19 Patients During the Pandemic, 2022. A Systematic Review and Meta-Analysis, Current Research in Nutrition and Food Science Journal, doi:10.12944/CRNFSJ.11.1.3.
12.
Kow et al., The impact of vitamin D administration on mortality in COVID-19 patients: a systematic review and meta-analysis of randomized controlled trials, Inflammopharmacology, doi:10.1007/s10787-024-01564-2.
13.
Zhang et al., The impact of supplementing vitamin D through different methods on the prognosis of COVID-19 patients: a systematic review and meta-analysis, Frontiers in Nutrition, doi:10.3389/fnut.2024.1441847.
14.
Doustmohammadian et al., Impact of vitamin D supplementation on COVID-19 mortality: A systematic review and meta-analysis, Nutrition Clinique et Métabolisme, doi:10.1016/j.nupar.2025.12.001.
15.
Yang et al., Vitamin D supplementation benefits COVID-19: A systematic review and meta-analysis, Heliyon, doi:10.1016/j.heliyon.2026.e44988.
16.
Meng et al., The role of vitamin D in the prevention and treatment of SARS-CoV-2 infection: A meta-analysis of randomized controlled trials, Clinical Nutrition, doi:10.1016/j.clnu.2023.09.008.
17.
Yang (B) et al., Therapeutic effects of vitamin D supplementation on COVID-19 aggravation: a systematic review and meta-analysis of randomized controlled trials, Frontiers in Pharmacology, doi:10.3389/fphar.2024.1367686.
18.
Szarpak et al., Vitamin D supplementation to treat SARS-CoV-2 positive patients. Evidence from meta-analysis, Cardiology Journal, doi:10.5603/CJ.a2021.0122.
19.
Tentolouris et al., The effect of vitamin D supplementation on mortality and intensive care unit admission of COVID-19 patients. A systematic review, meta-analysis and meta-regression, Diabetes/Metabolism Research and Reviews, doi:10.1002/dmrr.3517.
20.
Sartini et al., Preventive Vitamin D Supplementation and Risk for COVID-19 Infection: A Systematic Review and Meta-Analysis, Nutrients, doi:10.3390/nu16050679.
Pal et al., 24 Jun 2021, peer-reviewed, 6 authors.
Vitamin D supplementation and clinical outcomes in COVID-19: a systematic review and meta-analysis
Journal of Endocrinological Investigation, doi:10.1007/s40618-021-01614-4
Purpose To provide a precise summary and collate the hitherto available clinical evidence on the effect of vitamin D supplementation on clinical outcomes in COVID-19 patients. Methods PubMed/MEDLINE, Scopus, and Web of Science databases were systematically searched using appropriate keywords till June 8, 2021, to identify observational studies and randomized controlled trials (RCTs) reporting adverse clinical outcomes (ICU admission and/or mortality) in COVID-19 patients receiving vitamin D supplementation vs. those not receiving the same. Both prior use and use of vitamin D after COVID-19 diagnosis were considered. Unadjusted/adjusted pooled odds ratio (OR) with 95% confidence intervals (CI) were calculated (PROSPERO registration number CRD42021248488).
Results We identified 13 studies (10 observational, 3 RCTs) pooling data retrieved from 2933 COVID-19 patients. Pooled analysis of unadjusted data showed that vitamin D use in COVID-19 was significantly associated with reduced ICU admission/mortality (OR 0.41, 95% CI: 0.20, 0.81, p = 0.01, I 2 = 66%, random-effects model). Similarly, on pooling adjusted risk estimates, vitamin D was also found to reduce the risk of adverse outcomes (pooled OR 0.27, 95% CI: 0.08, 0.91, p = 0.03, I 2 = 80%, random-effects model). Subgroup analysis showed that vitamin D supplementation was associated with improved clinical outcomes only in patients receiving the drug post-COVID-19 diagnosis and not in those who had received vitamin D before diagnosis. Conclusions Vitamin D supplementation might be associated with improved clinical outcomes, especially when administered after the diagnosis of COVID-19. However, issues regarding the appropriate dose, duration, and mode of administration of vitamin D remain unanswered and need further research.
Supplementary Information The online version contains supplementary material available at https:// doi. org/ 10. 1007/ s40618-021-01614-4. Author contributions RP and MB are the co-primary authors, had performed literature search, data extraction and statistical analysis. SKB is the corresponding author, had conceptualized, supervised and edited the manuscript. AJS had helped in risk of bias assessment. BS and AV had helped in statistical analysis and had edited the manuscript. All the authors approved the final version of the manuscript.
Declarations
Conflicts of interest None to declare. Ethical approval This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent No informed consent. Publisher's Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Akbar, Wibowo, Pranata, Setiabudiawan, Low Serum 25-hydroxyvitamin D (Vitamin D) level is associated with susceptibility to COVID-19, severity, and mortality: a systematic review and meta-analysis, Front Nutr, doi:10.3389/fnut.2021.660420
Alcala-Diaz, Limia-Perez, Gomez-Huelgas, Calcifediol treatment and hospital mortality due to COVID-19: a cohort study, Nutrients, doi:10.3390/nu13061760
Annweiler, Corvaisier, Gautier, Vitamin D supplementation associated to better survival in hospitalized frail elderly COVID-19 patients: the GERIA-COVID quasiexperimental study, Nutrients, doi:10.3390/nu12113377
Annweiler, Hanotte, Eprevier, Vitamin D and survival in COVID-19 patients: a quasi-experimental study, J Steroid Biochem Mol Biol, doi:10.1016/j.jsbmb.2020.105771
Annweiler, Mercat, Souberbielle, Learning from previous methodological pitfalls to propose well-designed trials on vitamin D in COVID-19, J Steroid Biochem Mol Biol, doi:10.1016/j.jsbmb.2021.105901
Baktash, Hosack, Patel, Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad Med J, doi:10.1136/postgradmedj-2020-138712
Barker, May, Doty, Vitamin D supplementation protects against reductions in plasma 25-hydroxyvitamin D induced by open-heart surgery: Assess-d trial, Physiol Rep, doi:10.14814/phy2.14747
Bassatne, Basbous, Chakhtoura, The link between COVID-19 and VItamin D (VIVID): a systematic review and meta-analysis, Metabolism, doi:10.1016/j.metabol.2021.154753
Bilezikian, Bikle, Hewison, Mechanisms in endocrinology: vitamin D and COVID-19, Eur J Endocrinol, doi:10.1530/EJE-20-0665
Brice, Diamond, Antiviral activities of human host defense peptides, Curr Med Chem, doi:10.2174/0929867326666190805151654
Cangiano, Fatti, Danesi, Mortality in an Italian nursing home during COVID-19 pandemic: correlation with gender, age, ADL, vitamin D supplementation, and limitations of the diagnostic tests, Aging, doi:10.18632/aging.202307
Castillo, Costa, Barrios, Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: a pilot randomized clinical study, J Steroid Biochem Mol Biol, doi:10.1016/j.jsbmb.2020.105751
Cereda, Bogliolo, Lobascio, Vitamin D supplementation and outcomes in coronavirus disease 2019 (COVID-19) patients from the outbreak area of Lombardy, Italy Nutrition, doi:10.1016/j.nut.2020.111055
Charoenngam, Shirvani, Reddy, Association of vitamin D status with hospital morbidity and mortality in adult hospitalized patients with COVID-19, Endocr Pract, doi:10.1016/j.eprac.2021.02.013
Giannini, Passeri, Tripepi, Effectiveness of in-hospital cholecalciferol use on clinical outcomes in comorbid COVID-19 patients: a hypothesis-generating study, Nutrients, doi:10.3390/nu13010219
Grant, Lahore, Mcdonnell, Evidence that vitamin D Supplementation could reduce risk of influenza and COVID-19 infections and deaths, Nutrients, doi:10.3390/nu12040988
Grant, Lahore, Rockwell, The benefits of vitamin D supplementation for athletes: better performance and reduced risk of COVID-19, Nutrients, doi:10.3390/nu12123741
Griffin, Hewison, Hopkin, Perspective: Vitamin D supplementation prevents rickets and acute respiratory infections when given as daily maintenance but not as intermittent bolus: implications for COVID-19, Clin Med, doi:10.7861/clinmed.2021-0035
Heaney, Guidelines for optimizing design and analysis of clinical studies of nutrient effects, Nutr Rev, doi:10.1111/nure.12090
Hernández, Nan, Fernandez-Ayala, Vitamin D status in hospitalized patients with SARS-CoV-2 infection, J Clin Endocrinol Metab, doi:10.1210/clinem/dgaa733
Hernández, Nan, Fernandez-Ayala, Vitamin D status in hospitalized patients with SARS-CoV-2 infection, J Clin Endocrinol Metab, doi:10.1210/clinem/dgaa733
Higgins, Measuring inconsistency in meta-analyses, BMJ, doi:10.1136/bmj.327.7414.557
Higgins, Sterne, Savovic, A revised tool for assessing risk of bias in randomized trials, Cochrane Database Syst Rev
Jevalikar, Mithal, Singh, Lack of association of baseline 25-hydroxyvitamin D levels with disease severity and mortality in Indian patients hospitalized for COVID-19, Sci Rep, doi:10.1038/s41598-021-85809-y
Kaufman, Niles, Kroll, SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels, PLoS ONE, doi:10.1371/journal.pone.0239252
Kearns, Binongo, Watson, The effect of a single, large bolus of vitamin D in healthy adults over the winter and following year: a randomized, double-blind, placebocontrolled trial, Eur J Clin Nutr, doi:10.1038/ejcn.2014.209
Ketha, Thacher, Oberhelman, Comparison of the effect of daily versus bolus dose maternal vitamin D3 supplementation on the 24,25-dihydroxyvitamin D3 to 25-hydroxyvitamin D3 ratio, Bone, doi:10.1016/j.bone.2018.02.024
Lakkireddy, Gadiga, Malathi, Impact of daily high dose oral vitamin D therapy on the inflammatory markers in patients with COVID 19 disease, Sci Rep, doi:10.1038/s41598-021-90189-4
Liberati, Altman, Tetzlaff, The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration, BMJ, doi:10.1136/bmj.b2700
Ling, Broad, Murphy, High-dose cholecalciferol booster therapy is associated with a reduced risk of mortality in patients with COVID-19: a cross-sectional multi-centre observational study, Nutrients, doi:10.3390/nu12123799
Lohia, Nguyen, Patel, Kapur, Exploring the link between vitamin D and clinical outcomes in COVID-19, Am J Physiol-Endocrinol Metab, doi:10.1152/ajpendo.00517.2020
Luchini, Stubbs, Solmi, Veronese, Assessing the quality of studies in meta-analyses: advantages and limitations of the Newcastle Ottawa Scale, World J Meta-Anal, doi:10.13105/wjma.v5.i4.80
Maghbooli, Sahraian, Ebrahimi, Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/ mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection, PLoS ONE, doi:10.1371/journal.pone.0239799
Mahdavi, A brief review of interplay between vitamin D and angiotensin-converting enzyme 2: implications for a potential treatment for COVID-19, Rev Med Virol, doi:10.1002/rmv.2119
Mariani, Giménez, Bergam, Association between vitamin D deficiency and COVID-19 incidence, complications, and mortality in 46 countries: an ecological study, doi:10.1089/hs.2020.0137
Meltzer, Best, Zhang, Association of vitamin D status and other clinical characteristics with COVID-19 test results, JAMA Netw Open, doi:10.1001/jamanetworkopen.2020.19722
Mercola, Grant, Wagner, Evidence regarding vitamin D and Risk of COVID-19 and its severity, Nutrients, doi:10.3390/nu12113361
Munshi, Hussein, Toraih, Vitamin D insufficiency as a potential culprit in critical COVID-19 patients, J Med Virol, doi:10.1002/jmv.26360
Murai, Fernandes, Sales, Effect of a single high dose of vitamin D 3 on hospital length of stay in patients with moderate to severe COVID-19: a randomized clinical trial, JAMA, doi:10.1001/jama.2020.26848
Pacha, Sallman, Evans, COVID-19: a case for inhibiting IL-17?, Nat Rev Immunol, doi:10.1038/s41577-020-0328-z
Pal, Bhadada, Vitamin D supplementation and adverse clinical outcomes in COVID-19: a systematic review and meta-analysis
Pal, Bhansali, COVID-19, diabetes mellitus and ACE2: the conundrum, Diabetes Res Clin Pract, doi:10.1016/j.diabres.2020.108132
Pal, Ram, Zohmangaihi, High prevalence of hypocalcemia in non-severe COVID-19 patients: a retrospective case-control study, Front Med, doi:10.3389/fmed.2020.590805
Pereira, Damascena, Azevedo, Vitamin D deficiency aggravates COVID-19: systematic review and meta-analysis, Crit Rev Food Sci Nutr, doi:10.1080/10408398.2020.1841090
Radujkovic, Hippchen, Tiwari-Heckler, Vitamin D deficiency and outcome of COVID-19 patients, doi:10.3390/nu12092757
Rastogi, Bhansali, Khare, Short term, high-dose vitamin D supplementation for COVID-19 disease: a randomised, placebo-controlled, study (SHADE study), Postgrad Med J postgrad, doi:10.1136/postgradmedj-2020-139065
Raucci, Mansour, Casillo, Interleukin-17A (IL-17A), a key molecule of innate and adaptive immunity, and its potential involvement in COVID-19-related thrombotic and vascular mechanisms, Autoimmun Rev, doi:10.1016/j.autrev.2020.102572
Shah Alam, Czajkowsky, Islam Md, Rahman Md, The role of vitamin D in reducing SARS-CoV-2 infection: an update, Int Immunopharmacol, doi:10.1016/j.intimp.2021.107686
Shah, Saxena, Mavalankar, Vitamin D supplementation, COVID-19 and disease severity: a meta-analysis, QJM Int J Med, doi:10.1093/qjmed/hcab009
Sánchez-Zuno, González-Estevez, Mg, Vitamin D levels in COVID-19 outpatients from Western Mexico: clinical correlation and effect of its supplementation, J Clin Med, doi:10.3390/jcm10112378
Tan, Ho, Kalimuddin, Cohort study to evaluate the effect of vitamin D, magnesium, and vitamin B12 in combination on progression to severe outcomes in older patients with coronavirus (COVID-19), Nutrition, doi:10.1016/j.nut.2020.111017
Teshome, Adane, Girma, Mekonnen, The impact of vitamin D level on COVID-19 infection: systematic review and meta-analysis, Front Public Health, doi:10.3389/fpubh.2021.624559
Wells, Shea, Connell, The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses
Zou, Yan, Shu, Angiotensin-converting enzyme 2 protects from lethal avian influenza A H5N1 infections, Nat Commun, doi:10.1038/ncomms4594
DOI record:
{
"DOI": "10.1007/s40618-021-01614-4",
"ISSN": [
"1720-8386"
],
"URL": "http://dx.doi.org/10.1007/s40618-021-01614-4",
"alternative-id": [
"1614"
],
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "18 April 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "12 June 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "24 June 2021"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Conflicts of interest",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "None to declare."
},
{
"group": {
"label": "Ethical approval",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "This article does not contain any studies with human participants or animals performed by any of the authors."
},
{
"group": {
"label": "Informed consent",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 4,
"value": "No informed consent."
},
{
"label": "Free to read",
"name": "free",
"value": "This content has been made available to all."
}
],
"author": [
{
"affiliation": [],
"family": "Pal",
"given": "R.",
"sequence": "first"
},
{
"affiliation": [],
"family": "Banerjee",
"given": "M.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-0410-8778",
"affiliation": [],
"authenticated-orcid": false,
"family": "Bhadada",
"given": "S. K.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Shetty",
"given": "A. J.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Singh",
"given": "B.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Vyas",
"given": "A.",
"sequence": "additional"
}
],
"container-title": "Journal of Endocrinological Investigation",
"container-title-short": "J Endocrinol Invest",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2021,
6,
24
]
],
"date-time": "2021-06-24T11:03:51Z",
"timestamp": 1624532631000
},
"deposited": {
"date-parts": [
[
2022,
1,
7
]
],
"date-time": "2022-01-07T19:16:00Z",
"timestamp": 1641582960000
},
"indexed": {
"date-parts": [
[
2024,
5,
7
]
],
"date-time": "2024-05-07T12:42:15Z",
"timestamp": 1715085735163
},
"is-referenced-by-count": 77,
"issue": "1",
"issued": {
"date-parts": [
[
2021,
6,
24
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2022,
1
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.springer.com/tdm",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
24
]
],
"date-time": "2021-06-24T00:00:00Z",
"timestamp": 1624492800000
}
},
{
"URL": "https://www.springer.com/tdm",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
24
]
],
"date-time": "2021-06-24T00:00:00Z",
"timestamp": 1624492800000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1007/s40618-021-01614-4.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1007/s40618-021-01614-4/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1007/s40618-021-01614-4.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"page": "53-68",
"prefix": "10.1007",
"published": {
"date-parts": [
[
2021,
6,
24
]
]
},
"published-online": {
"date-parts": [
[
2021,
6,
24
]
]
},
"published-print": {
"date-parts": [
[
2022,
1
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"author": "DO Meltzer",
"doi-asserted-by": "publisher",
"journal-title": "JAMA Netw Open",
"key": "1614_CR1",
"unstructured": "Meltzer DO, Best TJ, Zhang H et al (2020) Association of vitamin D status and other clinical characteristics with COVID-19 test results. JAMA Netw Open 3:e2019722. https://doi.org/10.1001/jamanetworkopen.2020.19722",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.3389/fmed.2020.590805",
"author": "R Pal",
"doi-asserted-by": "publisher",
"journal-title": "Front Med",
"key": "1614_CR2",
"unstructured": "Pal R, Ram S, Zohmangaihi D et al (2020) High prevalence of hypocalcemia in non-severe COVID-19 patients: a retrospective case-control study. Front Med 7:590805. https://doi.org/10.3389/fmed.2020.590805",
"volume": "7",
"year": "2020"
},
{
"DOI": "10.1002/jmv.26360",
"author": "R Munshi",
"doi-asserted-by": "publisher",
"first-page": "733",
"journal-title": "J Med Virol",
"key": "1614_CR3",
"unstructured": "Munshi R, Hussein MH, Toraih EA et al (2021) Vitamin D insufficiency as a potential culprit in critical COVID-19 patients. J Med Virol 93:733–740. https://doi.org/10.1002/jmv.26360",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.1089/hs.2020.0137",
"author": "J Mariani",
"doi-asserted-by": "publisher",
"journal-title": "Health Secur",
"key": "1614_CR4",
"unstructured": "Mariani J, Giménez VMM, Bergam I et al (2020) Association between vitamin D deficiency and COVID-19 incidence, complications, and mortality in 46 countries: an ecological study. Health Secur. https://doi.org/10.1089/hs.2020.0137",
"year": "2020"
},
{
"DOI": "10.3390/nu12092757",
"author": "A Radujkovic",
"doi-asserted-by": "publisher",
"journal-title": "Nutrients",
"key": "1614_CR5",
"unstructured": "Radujkovic A, Hippchen T, Tiwari-Heckler S et al (2020) Vitamin D deficiency and outcome of COVID-19 patients. Nutrients. https://doi.org/10.3390/nu12092757",
"year": "2020"
},
{
"DOI": "10.1136/postgradmedj-2020-138712",
"author": "V Baktash",
"doi-asserted-by": "publisher",
"journal-title": "Postgrad Med J",
"key": "1614_CR6",
"unstructured": "Baktash V, Hosack T, Patel N et al (2020) Vitamin D status and outcomes for hospitalised older patients with COVID-19. Postgrad Med J. https://doi.org/10.1136/postgradmedj-2020-138712",
"year": "2020"
},
{
"DOI": "10.3390/nu12113377",
"author": "G Annweiler",
"doi-asserted-by": "publisher",
"first-page": "3377",
"journal-title": "Nutrients",
"key": "1614_CR7",
"unstructured": "Annweiler G, Corvaisier M, Gautier J et al (2020) Vitamin D supplementation associated to better survival in hospitalized frail elderly COVID-19 patients: the GERIA-COVID quasi-experimental study. Nutrients 12:3377. https://doi.org/10.3390/nu12113377",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/j.jsbmb.2020.105771",
"author": "C Annweiler",
"doi-asserted-by": "publisher",
"journal-title": "J Steroid Biochem Mol Biol",
"key": "1614_CR8",
"unstructured": "Annweiler C, Hanotte B, Grandin de l’Eprevier C et al (2020) Vitamin D and survival in COVID-19 patients: a quasi-experimental study. J Steroid Biochem Mol Biol 204:105771. https://doi.org/10.1016/j.jsbmb.2020.105771",
"volume": "204",
"year": "2020"
},
{
"DOI": "10.3390/nu12123799",
"author": "SF Ling",
"doi-asserted-by": "publisher",
"first-page": "3799",
"journal-title": "Nutrients",
"key": "1614_CR9",
"unstructured": "Ling SF, Broad E, Murphy R et al (2020) High-dose cholecalciferol booster therapy is associated with a reduced risk of mortality in patients with COVID-19: a cross-sectional multi-centre observational study. Nutrients 12:3799. https://doi.org/10.3390/nu12123799",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3390/nu13010219",
"author": "S Giannini",
"doi-asserted-by": "publisher",
"first-page": "219",
"journal-title": "Nutrients",
"key": "1614_CR10",
"unstructured": "Giannini S, Passeri G, Tripepi G et al (2021) Effectiveness of in-hospital cholecalciferol use on clinical outcomes in comorbid COVID-19 patients: a hypothesis-generating study. Nutrients 13:219. https://doi.org/10.3390/nu13010219",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1016/j.jsbmb.2020.105751",
"author": "M Entrenas Castillo",
"doi-asserted-by": "publisher",
"journal-title": "J Steroid Biochem Mol Biol",
"key": "1614_CR11",
"unstructured": "Entrenas Castillo M, Entrenas Costa LM, Vaquero Barrios JM et al (2020) Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: a pilot randomized clinical study. J Steroid Biochem Mol Biol 203:105751. https://doi.org/10.1016/j.jsbmb.2020.105751",
"volume": "203",
"year": "2020"
},
{
"DOI": "10.1210/clinem/dgaa733",
"author": "JL Hernández",
"doi-asserted-by": "publisher",
"journal-title": "J Clin Endocrinol Metab",
"key": "1614_CR12",
"unstructured": "Hernández JL, Nan D, Fernandez-Ayala M et al (2020) Vitamin D status in hospitalized patients with SARS-CoV-2 infection. J Clin Endocrinol Metab. https://doi.org/10.1210/clinem/dgaa733",
"year": "2020"
},
{
"DOI": "10.1038/s41598-021-85809-y",
"author": "G Jevalikar",
"doi-asserted-by": "publisher",
"first-page": "6258",
"journal-title": "Sci Rep",
"key": "1614_CR13",
"unstructured": "Jevalikar G, Mithal A, Singh A et al (2021) Lack of association of baseline 25-hydroxyvitamin D levels with disease severity and mortality in Indian patients hospitalized for COVID-19. Sci Rep 11:6258. https://doi.org/10.1038/s41598-021-85809-y",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1016/j.nut.2020.111055",
"author": "E Cereda",
"doi-asserted-by": "publisher",
"journal-title": "Italy Nutrition",
"key": "1614_CR14",
"unstructured": "Cereda E, Bogliolo L, Lobascio F et al (2021) Vitamin D supplementation and outcomes in coronavirus disease 2019 (COVID-19) patients from the outbreak area of Lombardy. Italy Nutrition 82:111055. https://doi.org/10.1016/j.nut.2020.111055",
"volume": "82",
"year": "2021"
},
{
"DOI": "10.1001/jama.2020.26848",
"author": "IH Murai",
"doi-asserted-by": "publisher",
"first-page": "1053",
"journal-title": "JAMA",
"key": "1614_CR15",
"unstructured": "Murai IH, Fernandes AL, Sales LP et al (2021) Effect of a single high dose of vitamin D3 on hospital length of stay in patients with moderate to severe COVID-19: a randomized clinical trial. JAMA 325:1053. https://doi.org/10.1001/jama.2020.26848",
"volume": "325",
"year": "2021"
},
{
"DOI": "10.1136/bmj.b2700",
"author": "A Liberati",
"doi-asserted-by": "publisher",
"first-page": "b2700",
"journal-title": "BMJ",
"key": "1614_CR16",
"unstructured": "Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700–b2700. https://doi.org/10.1136/bmj.b2700",
"volume": "339",
"year": "2009"
},
{
"DOI": "10.1007/s40618-021-01614-4",
"doi-asserted-by": "crossref",
"key": "1614_CR17",
"unstructured": "Pal R, Bhadada SK (2021) Vitamin D supplementation and adverse clinical outcomes in COVID-19: a systematic review and meta-analysis. PROSPERO 2021 CRD42021248488. https://www.crd.york.ac.uk/PROSPERO/display_record.php?RecordID=248488"
},
{
"key": "1614_CR18",
"unstructured": "Wells G, Shea B, O’Connell D et al (2013) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp"
},
{
"DOI": "10.13105/wjma.v5.i4.80",
"author": "C Luchini",
"doi-asserted-by": "publisher",
"first-page": "80",
"journal-title": "World J Meta-Anal",
"key": "1614_CR19",
"unstructured": "Luchini C, Stubbs B, Solmi M, Veronese N (2017) Assessing the quality of studies in meta-analyses: advantages and limitations of the Newcastle Ottawa Scale. World J Meta-Anal 5:80. https://doi.org/10.13105/wjma.v5.i4.80",
"volume": "5",
"year": "2017"
},
{
"author": "J Higgins",
"first-page": "29",
"journal-title": "Cochrane Database Syst Rev",
"key": "1614_CR20",
"unstructured": "Higgins J, Sterne J, Savovic J et al (2016) A revised tool for assessing risk of bias in randomized trials. Cochrane Database Syst Rev 10:29–31",
"volume": "10",
"year": "2016"
},
{
"DOI": "10.1136/bmj.327.7414.557",
"author": "JPT Higgins",
"doi-asserted-by": "publisher",
"first-page": "557",
"journal-title": "BMJ",
"key": "1614_CR21",
"unstructured": "Higgins JPT (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557",
"volume": "327",
"year": "2003"
},
{
"DOI": "10.3390/nu13061760",
"author": "JF Alcala-Diaz",
"doi-asserted-by": "publisher",
"first-page": "1760",
"journal-title": "Nutrients",
"key": "1614_CR22",
"unstructured": "Alcala-Diaz JF, Limia-Perez L, Gomez-Huelgas R et al (2021) Calcifediol treatment and hospital mortality due to COVID-19: a cohort study. Nutrients 13:1760. https://doi.org/10.3390/nu13061760",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1152/ajpendo.00517.2020",
"author": "P Lohia",
"doi-asserted-by": "publisher",
"first-page": "E520",
"journal-title": "Am J Physiol-Endocrinol Metab",
"key": "1614_CR23",
"unstructured": "Lohia P, Nguyen P, Patel N, Kapur S (2021) Exploring the link between vitamin D and clinical outcomes in COVID-19. Am J Physiol-Endocrinol Metab 320:E520–E526. https://doi.org/10.1152/ajpendo.00517.2020",
"volume": "320",
"year": "2021"
},
{
"DOI": "10.18632/aging.202307",
"author": "B Cangiano",
"doi-asserted-by": "publisher",
"first-page": "24522",
"journal-title": "Aging",
"key": "1614_CR24",
"unstructured": "Cangiano B, Fatti LM, Danesi L et al (2020) Mortality in an Italian nursing home during COVID-19 pandemic: correlation with gender, age, ADL, vitamin D supplementation, and limitations of the diagnostic tests. Aging 12:24522–24534. https://doi.org/10.18632/aging.202307",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1038/s41598-021-90189-4",
"author": "M Lakkireddy",
"doi-asserted-by": "publisher",
"first-page": "10641",
"journal-title": "Sci Rep",
"key": "1614_CR25",
"unstructured": "Lakkireddy M, Gadiga SG, Malathi RD et al (2021) Impact of daily high dose oral vitamin D therapy on the inflammatory markers in patients with COVID 19 disease. Sci Rep 11:10641. https://doi.org/10.1038/s41598-021-90189-4",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1136/postgradmedj-2020-139065",
"author": "A Rastogi",
"doi-asserted-by": "publisher",
"journal-title": "Postgrad Med J postgrad",
"key": "1614_CR26",
"unstructured": "Rastogi A, Bhansali A, Khare N et al (2020) Short term, high-dose vitamin D supplementation for COVID-19 disease: a randomised, placebo-controlled, study (SHADE study). Postgrad Med J postgrad. https://doi.org/10.1136/postgradmedj-2020-139065",
"year": "2020"
},
{
"DOI": "10.3390/jcm10112378",
"author": "GA Sánchez-Zuno",
"doi-asserted-by": "publisher",
"first-page": "2378",
"journal-title": "J Clin Med",
"key": "1614_CR27",
"unstructured": "Sánchez-Zuno GA, González-Estevez G, Matuz-Flores MG et al (2021) Vitamin D levels in COVID-19 outpatients from Western Mexico: clinical correlation and effect of its supplementation. J Clin Med 10:2378. https://doi.org/10.3390/jcm10112378",
"volume": "10",
"year": "2021"
},
{
"DOI": "10.1016/j.nut.2020.111017",
"author": "CW Tan",
"doi-asserted-by": "publisher",
"journal-title": "Nutrition",
"key": "1614_CR28",
"unstructured": "Tan CW, Ho LP, Kalimuddin S et al (2020) Cohort study to evaluate the effect of vitamin D, magnesium, and vitamin B12 in combination on progression to severe outcomes in older patients with coronavirus (COVID-19). Nutrition 79–80:111017. https://doi.org/10.1016/j.nut.2020.111017",
"volume": "79–80",
"year": "2020"
},
{
"DOI": "10.1210/clinem/dgaa733",
"author": "JL Hernández",
"doi-asserted-by": "publisher",
"first-page": "e1343",
"journal-title": "J Clin Endocrinol Metab",
"key": "1614_CR29",
"unstructured": "Hernández JL, Nan D, Fernandez-Ayala M et al (2021) Vitamin D status in hospitalized patients with SARS-CoV-2 infection. J Clin Endocrinol Metab 106:e1343–e1353. https://doi.org/10.1210/clinem/dgaa733",
"volume": "106",
"year": "2021"
},
{
"DOI": "10.1111/nure.12090",
"author": "RP Heaney",
"doi-asserted-by": "publisher",
"first-page": "48",
"journal-title": "Nutr Rev",
"key": "1614_CR30",
"unstructured": "Heaney RP (2014) Guidelines for optimizing design and analysis of clinical studies of nutrient effects. Nutr Rev 72:48–54. https://doi.org/10.1111/nure.12090",
"volume": "72",
"year": "2014"
},
{
"DOI": "10.1371/journal.pone.0239252",
"author": "HW Kaufman",
"doi-asserted-by": "publisher",
"journal-title": "PLoS ONE",
"key": "1614_CR31",
"unstructured": "Kaufman HW, Niles JK, Kroll MH et al (2020) SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels. PLoS ONE 15:e0239252. https://doi.org/10.1371/journal.pone.0239252",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1016/j.intimp.2021.107686",
"author": "M Shah Alam",
"doi-asserted-by": "publisher",
"journal-title": "Int Immunopharmacol",
"key": "1614_CR32",
"unstructured": "Shah Alam M, Czajkowsky DM, Aminul Islam Md, Ataur Rahman Md (2021) The role of vitamin D in reducing SARS-CoV-2 infection: an update. Int Immunopharmacol 97:107686. https://doi.org/10.1016/j.intimp.2021.107686",
"volume": "97",
"year": "2021"
},
{
"DOI": "10.1016/j.eprac.2021.02.013",
"author": "N Charoenngam",
"doi-asserted-by": "publisher",
"first-page": "271",
"journal-title": "Endocr Pract",
"key": "1614_CR33",
"unstructured": "Charoenngam N, Shirvani A, Reddy N et al (2021) Association of vitamin D status with hospital morbidity and mortality in adult hospitalized patients with COVID-19. Endocr Pract 27:271–278. https://doi.org/10.1016/j.eprac.2021.02.013",
"volume": "27",
"year": "2021"
},
{
"DOI": "10.3389/fnut.2021.660420",
"author": "MR Akbar",
"doi-asserted-by": "publisher",
"journal-title": "Front Nutr",
"key": "1614_CR34",
"unstructured": "Akbar MR, Wibowo A, Pranata R, Setiabudiawan B (2021) Low Serum 25-hydroxyvitamin D (Vitamin D) level is associated with susceptibility to COVID-19, severity, and mortality: a systematic review and meta-analysis. Front Nutr 8:660420. https://doi.org/10.3389/fnut.2021.660420",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.3389/fpubh.2021.624559",
"author": "A Teshome",
"doi-asserted-by": "publisher",
"journal-title": "Front Public Health",
"key": "1614_CR35",
"unstructured": "Teshome A, Adane A, Girma B, Mekonnen ZA (2021) The impact of vitamin D level on COVID-19 infection: systematic review and meta-analysis. Front Public Health 9:624559. https://doi.org/10.3389/fpubh.2021.624559",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1080/10408398.2020.1841090",
"author": "M Pereira",
"doi-asserted-by": "publisher",
"journal-title": "Crit Rev Food Sci Nutr",
"key": "1614_CR36",
"unstructured": "Pereira M, Dantas Damascena A, Galvão Azevedo LM et al (2020) Vitamin D deficiency aggravates COVID-19: systematic review and meta-analysis. Crit Rev Food Sci Nutr. https://doi.org/10.1080/10408398.2020.1841090",
"year": "2020"
},
{
"DOI": "10.1016/j.metabol.2021.154753",
"author": "A Bassatne",
"doi-asserted-by": "publisher",
"journal-title": "Metabolism",
"key": "1614_CR37",
"unstructured": "Bassatne A, Basbous M, Chakhtoura M et al (2021) The link between COVID-19 and VItamin D (VIVID): a systematic review and meta-analysis. Metabolism. https://doi.org/10.1016/j.metabol.2021.154753",
"year": "2021"
},
{
"DOI": "10.3390/nu12113361",
"author": "J Mercola",
"doi-asserted-by": "publisher",
"first-page": "3361",
"journal-title": "Nutrients",
"key": "1614_CR38",
"unstructured": "Mercola J, Grant WB, Wagner CL (2020) Evidence regarding vitamin D and Risk of COVID-19 and its severity. Nutrients 12:3361. https://doi.org/10.3390/nu12113361",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3390/nu12040988",
"author": "WB Grant",
"doi-asserted-by": "publisher",
"first-page": "988",
"journal-title": "Nutrients",
"key": "1614_CR39",
"unstructured": "Grant WB, Lahore H, McDonnell SL et al (2020) Evidence that vitamin D Supplementation could reduce risk of influenza and COVID-19 infections and deaths. Nutrients 12:988. https://doi.org/10.3390/nu12040988",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3390/nu12123741",
"author": "WB Grant",
"doi-asserted-by": "publisher",
"first-page": "3741",
"journal-title": "Nutrients",
"key": "1614_CR40",
"unstructured": "Grant WB, Lahore H, Rockwell MS (2020) The benefits of vitamin D supplementation for athletes: better performance and reduced risk of COVID-19. Nutrients 12:3741. https://doi.org/10.3390/nu12123741",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.2174/0929867326666190805151654",
"author": "DC Brice",
"doi-asserted-by": "publisher",
"first-page": "1420",
"journal-title": "Curr Med Chem",
"key": "1614_CR41",
"unstructured": "Brice DC, Diamond G (2020) Antiviral activities of human host defense peptides. Curr Med Chem 27:1420–1443. https://doi.org/10.2174/0929867326666190805151654",
"volume": "27",
"year": "2020"
},
{
"DOI": "10.1016/j.autrev.2020.102572",
"author": "F Raucci",
"doi-asserted-by": "publisher",
"journal-title": "Autoimmun Rev",
"key": "1614_CR42",
"unstructured": "Raucci F, Mansour AA, Casillo GM et al (2020) Interleukin-17A (IL-17A), a key molecule of innate and adaptive immunity, and its potential involvement in COVID-19-related thrombotic and vascular mechanisms. Autoimmun Rev 19:102572. https://doi.org/10.1016/j.autrev.2020.102572",
"volume": "19",
"year": "2020"
},
{
"DOI": "10.1038/s41577-020-0328-z",
"author": "O Pacha",
"doi-asserted-by": "publisher",
"first-page": "345",
"journal-title": "Nat Rev Immunol",
"key": "1614_CR43",
"unstructured": "Pacha O, Sallman MA, Evans SE (2020) COVID-19: a case for inhibiting IL-17? Nat Rev Immunol 20:345–346. https://doi.org/10.1038/s41577-020-0328-z",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1530/EJE-20-0665",
"author": "JP Bilezikian",
"doi-asserted-by": "publisher",
"first-page": "R133",
"journal-title": "Eur J Endocrinol",
"key": "1614_CR44",
"unstructured": "Bilezikian JP, Bikle D, Hewison M et al (2020) Mechanisms in endocrinology: vitamin D and COVID-19. Eur J Endocrinol 183:R133–R147. https://doi.org/10.1530/EJE-20-0665",
"volume": "183",
"year": "2020"
},
{
"DOI": "10.1038/ncomms4594",
"author": "Z Zou",
"doi-asserted-by": "publisher",
"journal-title": "Nat Commun",
"key": "1614_CR45",
"unstructured": "Zou Z, Yan Y, Shu Y et al (2014) Angiotensin-converting enzyme 2 protects from lethal avian influenza A H5N1 infections. Nat Commun. https://doi.org/10.1038/ncomms4594",
"year": "2014"
},
{
"DOI": "10.1016/j.diabres.2020.108132",
"author": "R Pal",
"doi-asserted-by": "publisher",
"journal-title": "Diabetes Res Clin Pract",
"key": "1614_CR46",
"unstructured": "Pal R, Bhansali A (2020) COVID-19, diabetes mellitus and ACE2: the conundrum. Diabetes Res Clin Pract 162:108132. https://doi.org/10.1016/j.diabres.2020.108132",
"volume": "162",
"year": "2020"
},
{
"DOI": "10.1002/rmv.2119",
"author": "A Malek Mahdavi",
"doi-asserted-by": "publisher",
"journal-title": "Rev Med Virol",
"key": "1614_CR47",
"unstructured": "Malek Mahdavi A (2020) A brief review of interplay between vitamin D and angiotensin-converting enzyme 2: implications for a potential treatment for COVID-19. Rev Med Virol. https://doi.org/10.1002/rmv.2119",
"year": "2020"
},
{
"DOI": "10.1093/qjmed/hcab009",
"author": "K Shah",
"doi-asserted-by": "publisher",
"journal-title": "QJM Int J Med",
"key": "1614_CR48",
"unstructured": "Shah K, Saxena D, Mavalankar D (2021) Vitamin D supplementation, COVID-19 and disease severity: a meta-analysis. QJM Int J Med. https://doi.org/10.1093/qjmed/hcab009",
"year": "2021"
},
{
"DOI": "10.1016/j.jsbmb.2021.105901",
"author": "C Annweiler",
"doi-asserted-by": "publisher",
"journal-title": "J Steroid Biochem Mol Biol",
"key": "1614_CR49",
"unstructured": "Annweiler C, Mercat A, Souberbielle J-C (2021) Learning from previous methodological pitfalls to propose well-designed trials on vitamin D in COVID-19. J Steroid Biochem Mol Biol 211:105901. https://doi.org/10.1016/j.jsbmb.2021.105901",
"volume": "211",
"year": "2021"
},
{
"DOI": "10.1371/journal.pone.0239799",
"author": "Z Maghbooli",
"doi-asserted-by": "publisher",
"journal-title": "PLoS ONE",
"key": "1614_CR50",
"unstructured": "Maghbooli Z, Sahraian MA, Ebrahimi M et al (2020) Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection. PLoS ONE 15:e0239799. https://doi.org/10.1371/journal.pone.0239799",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1038/ejcn.2014.209",
"author": "MD Kearns",
"doi-asserted-by": "publisher",
"first-page": "193",
"journal-title": "Eur J Clin Nutr",
"key": "1614_CR51",
"unstructured": "Kearns MD, Binongo JNG, Watson D et al (2015) The effect of a single, large bolus of vitamin D in healthy adults over the winter and following year: a randomized, double-blind, placebo-controlled trial. Eur J Clin Nutr 69:193–197. https://doi.org/10.1038/ejcn.2014.209",
"volume": "69",
"year": "2015"
},
{
"DOI": "10.14814/phy2.14747",
"author": "T Barker",
"doi-asserted-by": "publisher",
"journal-title": "Physiol Rep",
"key": "1614_CR52",
"unstructured": "Barker T, May HT, Doty JR et al (2021) Vitamin D supplementation protects against reductions in plasma 25-hydroxyvitamin D induced by open-heart surgery: Assess-d trial. Physiol Rep. https://doi.org/10.14814/phy2.14747",
"year": "2021"
},
{
"DOI": "10.7861/clinmed.2021-0035",
"author": "G Griffin",
"doi-asserted-by": "publisher",
"first-page": "e144",
"journal-title": "Clin Med",
"key": "1614_CR53",
"unstructured": "Griffin G, Hewison M, Hopkin J et al (2021) Perspective: Vitamin D supplementation prevents rickets and acute respiratory infections when given as daily maintenance but not as intermittent bolus: implications for COVID-19. Clin Med 21:e144–e149. https://doi.org/10.7861/clinmed.2021-0035",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1016/j.bone.2018.02.024",
"author": "H Ketha",
"doi-asserted-by": "publisher",
"first-page": "321",
"journal-title": "Bone",
"key": "1614_CR54",
"unstructured": "Ketha H, Thacher TD, Oberhelman SS et al (2018) Comparison of the effect of daily versus bolus dose maternal vitamin D3 supplementation on the 24,25-dihydroxyvitamin D3 to 25-hydroxyvitamin D3 ratio. Bone 110:321–325. https://doi.org/10.1016/j.bone.2018.02.024",
"volume": "110",
"year": "2018"
}
],
"reference-count": 54,
"references-count": 54,
"relation": {},
"resource": {
"primary": {
"URL": "https://link.springer.com/10.1007/s40618-021-01614-4"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Vitamin D supplementation and clinical outcomes in COVID-19: a systematic review and meta-analysis",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "45"
}
