Association of Vitamin D Status and Other Clinical Characteristics With COVID-19 Test Results
et al., JAMA network open, 3:9, doi:10.1001/jamanetworkopen.2020.19722, Sep 2020
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 489 patients showing 44% lower risk for COVID-19 with vitamin D sufficiency, relative risk RR = 0.56, p = 0.02.
This is the 13th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
Standard of Care (SOC) for COVID-19 in the study country,
the USA, is very poor with very low average efficacy for approved treatments1.
Only expensive, high-profit treatments were approved for early treatment. Low-cost treatments were excluded, reducing the probability of early treatment due to access and cost barriers, and eliminating complementary and synergistic benefits seen with many low-cost treatments.
|
risk of case, 43.5% lower, RR 0.56, p = 0.02, high D levels 39 of 317 (12.3%), low D levels 32 of 172 (18.6%), NNT 16, adjusted per study, inverted to make RR<1 favor high D levels, >20ng/mL.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Meltzer et al., 3 Sep 2020, retrospective, USA, peer-reviewed, 6 authors.
Association of Vitamin D Status and Other Clinical Characteristics With COVID-19 Test Results
JAMA Network Open, doi:10.1001/jamanetworkopen.2020.19722
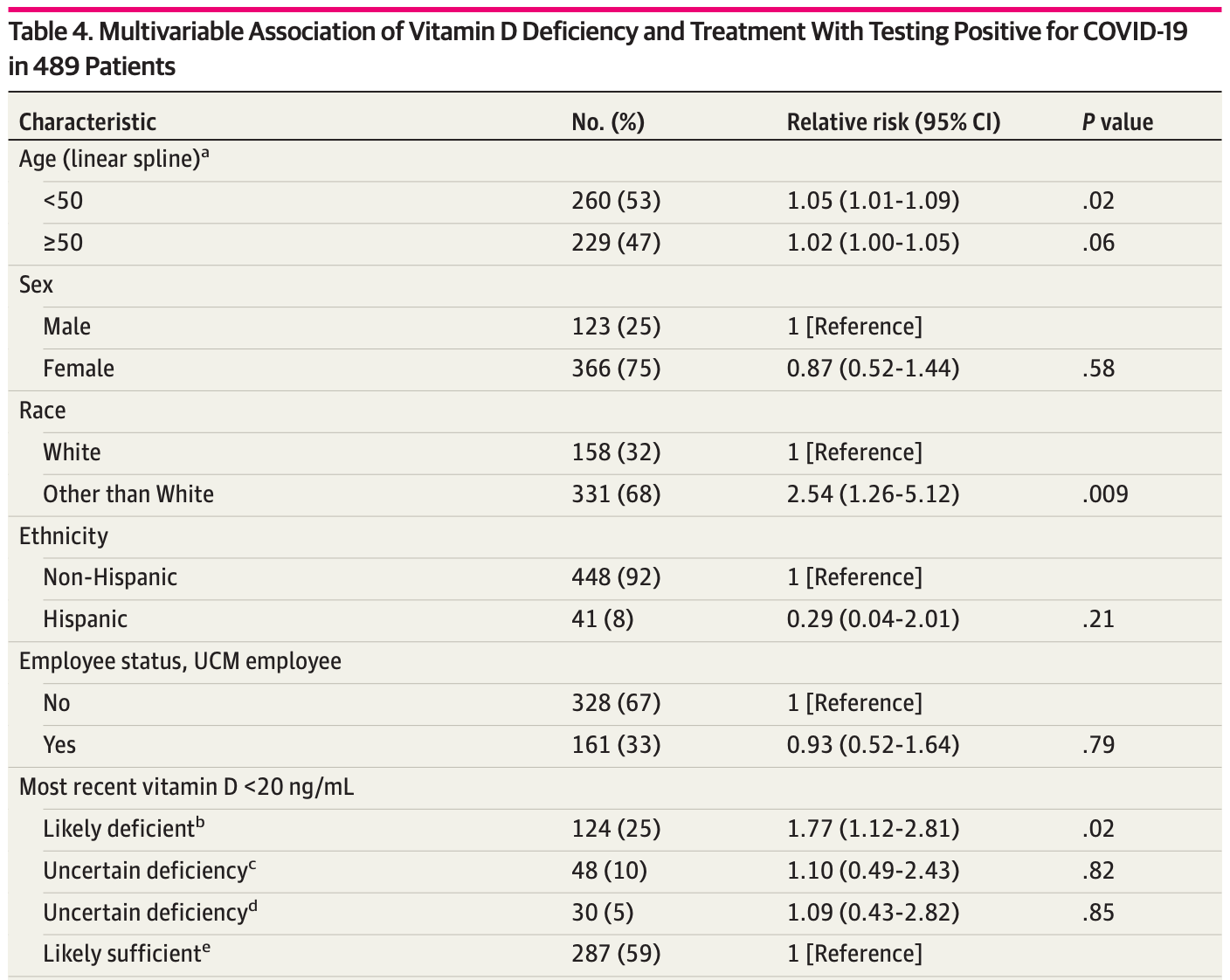
IMPORTANCE Vitamin D treatment has been found to decrease the incidence of viral respiratory tract infection, especially in patients with vitamin D deficiency. Whether vitamin D is associated with coronavirus disease 2019 (COVID-19) incidence is unknown. OBJECTIVE To examine whether the last vitamin D status before COVID-19 testing is associated with COVID-19 test results. DESIGN, SETTING, AND PARTICIPANTS This retrospective cohort study at an urban academic medical center included patients with a 25-hydroxycholecalciferol or 1,25-dihydroxycholecalciferol level measured within 1 year before being tested for COVID-19 from March 3 to April 10, 2020. EXPOSURES Vitamin D deficiency was defined by the last measurement of 25-hydroxycholecalciferol less than 20 ng/mL or 1,25-dihydroxycholecalciferol less than 18 pg/mL before COVID-19 testing. Treatment changes were defined by changes in vitamin D type and dose between the date of the last vitamin D level measurement and the date of COVID-19 testing. Vitamin D deficiency and treatment changes were combined to categorize the most recent vitamin D status before COVID-19 testing as likely deficient (last level deficient and treatment not increased), likely sufficient (last level not deficient and treatment not decreased), and 2 groups with uncertain deficiency (last level deficient and treatment increased, and last level not deficient and treatment decreased). MAIN OUTCOMES AND MEASURES The outcome was a positive COVID-19 polymerase chain reaction test result. Multivariable analysis tested whether vitamin D status before COVID-19 testing was associated with testing positive for COVID-19, controlling for demographic and comorbidity indicators. RESULTS A total of 489 patients (mean [SD] age, 49.2 [18.4] years; 366 [75%] women; and 331 [68%] race other than White) had a vitamin D level measured in the year before COVID-19 testing. Vitamin D status before COVID-19 testing was categorized as likely deficient for 124 participants (25%), likely sufficient for 287 (59%), and uncertain for 78 (16%). Overall, 71 participants (15%) tested positive for COVID-19. In multivariate analysis, testing positive for COVID-19 was associated with increasing age up to age 50 years (relative risk, 1.06; 95% CI, 1.01-1.09; P = .02); non-White race (relative risk, 2.54; 95% CI, 1.26-5.12; P = .009), and likely deficient vitamin D status (relative risk, 1.77; 95% CI, 1.12-2.81; P = .02) compared with likely sufficient vitamin D status. Predicted COVID-19 rates in the deficient group were 21.6% (95% CI, 14.0%-29.2%) vs 12.2%(95% CI, 8.9%-15.4%) in the sufficient group. (continued) Key Points Question Is vitamin D status, reflecting vitamin D levels and treatment, associated with test results for coronavirus disease 2019 (COVID-19)? Findings In this cohort study of 489 patients who had a vitamin D level measured in the year before COVID-19 testing, the relative risk of testing positive for COVID-19 was 1.77 times greater for patients..
References
Blizzard, Hosmer, Parameter estimation and goodness-of-fit in log binomial regression, Biom J, doi:10.1002/bimj.200410165
Cdc Covid-, Characteristics of health care personnel with COVID-19 -United States, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm6915e6
Diagnostics, cobas Elecsys Vitamin D total II assay
Diagnostics, cobas SARS-CoV-2 test (for the COVID-19 coronavirus)
Elliott, Binkley, Carnes, Fracture risks for women in long-term care: high prevalence of calcaneal osteoporosis and hypovitaminosis D, Pharmacotherapy, doi:10.1592/phco.23.6.702.32182
Forrest, Stuhldreher, Prevalence and correlates of vitamin D deficiency in US adults, Nutr Res, doi:10.1016/j.nutres.2010.12.001
Frieden, Former, Chief Dr, Tom Frieden: coronavirus infection risk may be reduced by vitamin D. Fox News, Opinion
Garg, Kim, Whitaker, Hospitalization rates and characteristics of patients hospitalized with laboratory-confirmed coronavirus disease 2019: COVID-NET, 14 States, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm6915e3
Ginde, Sullivan, Mansbach, Camargo, Vitamin D insufficiency in pregnant and nonpregnant women of childbearing age in the United States, Am J Obstet Gynecol, doi:10.1016/j.ajog.2009.11.036
Gold, Wong, Szablewski, Characteristics and clinical outcomes of adult patients hospitalized with COVID-19 -Georgia, March 2020, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm6918e1
Grant, Lahore, Mcdonnell, Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths, Nutrients, doi:10.3390/nu12040988
Greger, Effect of Variations in Dietary Protein, Phosphorus, Electrolytes and Vitamin D on Calcium and Zinc Metabolism: Nutrient Interactions, Marcel Dekker
Hastie, Mackay, Ho, Vitamin D concentrations and COVID-19 infection in UK Biobank, Diabetes Metab Syndr, doi:10.1016/j.dsx.2020.04.050
Holick, Binkley, Bischoff-Ferrari, Endocrine Society. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline, J Clin Endocrinol Metab, doi:10.1210/jc.2011-0385
Hunt, Britons urged to take vitamin D while sheltering inside during the pandemic, Published
Huotari, Herzig, Vitamin D and living in northern latitudes-an endemic risk area for vitamin D deficiency, Int J Circumpolar Health, doi:10.3402/ijch.v67i2-3.18258
Li, Guan, Wu, Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia, N Engl J Med, doi:10.1056/NEJMoa2001316
Martineau, Jolliffe, Hooper, Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data, BMJ, doi:10.1136/bmj.i6583
Mcnutt, Wu, Xue, Hafner, Estimating the relative risk in cohort studies and clinical trials of common outcomes, Am J Epidemiol, doi:10.1093/aje/kwg074
Misra, Pacaud, Petryk, Collett-Solberg, Kappy, Drug and Therapeutics Committee of the Lawson Wilkins Pediatric Endocrine Society. Vitamin D deficiency in children and its management: review of current knowledge and recommendations, Pediatrics, doi:10.1542/peds.2007-1894
Nakamura, Vitamin D insufficiency in Japanese populations: from the viewpoint of the prevention of osteoporosis, J Bone Miner Metab, doi:10.1007/s00774-005-0637-0
Pregibon, Data Analytic Methods for Generalized Linear Models
Ross, Dietary Reference Intakes for Calcium and Vitamin D
Sassi, Tamone, Amelio, Vitamin D: nutrient, hormone, and immunomodulator, Nutrients, doi:10.3390/nu10111656
Sowah, Fan, Dennett, Hagtvedt, Straube, Vitamin D levels and deficiency with different occupations: a systematic review, BMC Public Health, doi:10.1186/s12889-017-4436-z
Stokes, Zambrano, Anderson, Coronavirus disease 2019 case surveillance -United States, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm6924e2
Umhau, Casting sunlight on an epidemic: is vitamin D a critical host factor to prevent COVID-19? MedPage Today
Velthuis, Van Den Worm, Sims, Baric, Snijder et al., Zn(2+) inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture, PLoS Pathog, doi:10.1371/journal.ppat.1001176
Viracor, Coronavirus (COVID-19) SARS-CoV-2 PCR
Yin, Agrawal, Vitamin D and inflammatory diseases, J Inflamm Res, doi:10.2147/JIR.S63898
Zhang, Iwashyna, Christakis, The performance of different lookback periods and sources of information for Charlson comorbidity adjustment in Medicare claims, Med Care, doi:10.1097/00005650-199911000-00005
DOI record:
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"ISSN": [
"2574-3805"
],
"URL": "http://dx.doi.org/10.1001/jamanetworkopen.2020.19722",
"author": [
{
"affiliation": [
{
"name": "Department of Medicine, University of Chicago, Chicago, Illinois"
}
],
"family": "Meltzer",
"given": "David O.",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Center for Health and the Social Sciences, University of Chicago, Chicago, Illinois"
}
],
"family": "Best",
"given": "Thomas J.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Center for Health and the Social Sciences, University of Chicago, Chicago, Illinois"
}
],
"family": "Zhang",
"given": "Hui",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, University of Chicago, Chicago, Illinois"
}
],
"family": "Vokes",
"given": "Tamara",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, University of Chicago, Chicago, Illinois"
}
],
"family": "Arora",
"given": "Vineet",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, University of Chicago, Chicago, Illinois"
}
],
"family": "Solway",
"given": "Julian",
"sequence": "additional"
}
],
"container-title": "JAMA Network Open",
"container-title-short": "JAMA Netw Open",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2020,
9,
3
]
],
"date-time": "2020-09-03T15:35:58Z",
"timestamp": 1599147358000
},
"deposited": {
"date-parts": [
[
2020,
10,
14
]
],
"date-time": "2020-10-14T21:31:23Z",
"timestamp": 1602711083000
},
"indexed": {
"date-parts": [
[
2024,
4,
8
]
],
"date-time": "2024-04-08T12:41:22Z",
"timestamp": 1712580082301
},
"is-referenced-by-count": 357,
"issue": "9",
"issued": {
"date-parts": [
[
2020,
9,
3
]
]
},
"journal-issue": {
"issue": "9",
"published-print": {
"date-parts": [
[
2020,
9,
1
]
]
}
},
"language": "en",
"link": [
{
"URL": "https://jamanetwork.com/journals/jamanetworkopen/articlepdf/2770157/meltzer_2020_oi_200688_1602709420.0976.pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "10",
"original-title": [],
"page": "e2019722",
"prefix": "10.1001",
"published": {
"date-parts": [
[
2020,
9,
3
]
]
},
"published-online": {
"date-parts": [
[
2020,
9,
3
]
]
},
"publisher": "American Medical Association (AMA)",
"reference": [
{
"DOI": "10.3390/nu12040988",
"article-title": "Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths.",
"author": "Grant",
"doi-asserted-by": "publisher",
"first-page": "988",
"issue": "4",
"journal-title": "Nutrients",
"key": "zoi200688r2",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1136/bmj.i6583",
"article-title": "Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data.",
"author": "Martineau",
"doi-asserted-by": "publisher",
"first-page": "i6583",
"journal-title": "BMJ",
"key": "zoi200688r3",
"volume": "356",
"year": "2017"
},
{
"DOI": "10.1016/j.nutres.2010.12.001",
"article-title": "Prevalence and correlates of vitamin D deficiency in US adults.",
"author": "Forrest",
"doi-asserted-by": "publisher",
"first-page": "48",
"issue": "1",
"journal-title": "Nutr Res",
"key": "zoi200688r4",
"volume": "31",
"year": "2011"
},
{
"DOI": "10.15585/mmwr.mm6915e3",
"article-title": "Hospitalization rates and characteristics of patients hospitalized with laboratory-confirmed coronavirus disease 2019: COVID-NET, 14 States, March 1–30, 2020.",
"author": "Garg",
"doi-asserted-by": "publisher",
"first-page": "458",
"issue": "15",
"journal-title": "MMWR Morb Mortal Wkly Rep",
"key": "zoi200688r5",
"volume": "69",
"year": "2020"
},
{
"DOI": "10.15585/mmwr.mm6915e6",
"article-title": "Characteristics of health care personnel with COVID-19 - United States, February 12-April 9, 2020.",
"author": "CDC COVID-19 Response Team",
"doi-asserted-by": "publisher",
"first-page": "477",
"issue": "15",
"journal-title": "MMWR Morb Mortal Wkly Rep",
"key": "zoi200688r9",
"volume": "69",
"year": "2020"
},
{
"DOI": "10.3402/ijch.v67i2-3.18258",
"article-title": "Vitamin D and living in northern latitudes—an endemic risk area for vitamin D deficiency.",
"author": "Huotari",
"doi-asserted-by": "publisher",
"first-page": "164",
"issue": "2-3",
"journal-title": "Int J Circumpolar Health",
"key": "zoi200688r10",
"volume": "67",
"year": "2008"
},
{
"DOI": "10.1592/phco.23.6.702.32182",
"article-title": "Fracture risks for women in long-term care: high prevalence of calcaneal osteoporosis and hypovitaminosis D.",
"author": "Elliott",
"doi-asserted-by": "publisher",
"first-page": "702",
"issue": "6",
"journal-title": "Pharmacotherapy",
"key": "zoi200688r11",
"volume": "23",
"year": "2003"
},
{
"DOI": "10.1186/s12889-017-4436-z",
"article-title": "Vitamin D levels and deficiency with different occupations: a systematic review.",
"author": "Sowah",
"doi-asserted-by": "publisher",
"first-page": "519",
"issue": "1",
"journal-title": "BMC Public Health",
"key": "zoi200688r12",
"volume": "17",
"year": "2017"
},
{
"DOI": "10.1056/NEJMoa2001316",
"article-title": "Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia.",
"author": "Li",
"doi-asserted-by": "publisher",
"first-page": "1199",
"issue": "13",
"journal-title": "N Engl J Med",
"key": "zoi200688r13",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1016/j.ajog.2009.11.036",
"article-title": "Vitamin D insufficiency in pregnant and nonpregnant women of childbearing age in the United States.",
"author": "Ginde",
"doi-asserted-by": "publisher",
"first-page": "436.e1",
"issue": "5",
"journal-title": "Am J Obstet Gynecol",
"key": "zoi200688r15",
"volume": "202",
"year": "2010"
},
{
"DOI": "10.1542/peds.2007-1894",
"article-title": "Vitamin D deficiency in children and its management: review of current knowledge and recommendations.",
"author": "Misra",
"doi-asserted-by": "publisher",
"first-page": "398",
"issue": "2",
"journal-title": "Pediatrics",
"key": "zoi200688r16",
"volume": "122",
"year": "2008"
},
{
"DOI": "10.1007/s00774-005-0637-0",
"article-title": "Vitamin D insufficiency in Japanese populations: from the viewpoint of the prevention of osteoporosis.",
"author": "Nakamura",
"doi-asserted-by": "publisher",
"first-page": "1",
"issue": "1",
"journal-title": "J Bone Miner Metab",
"key": "zoi200688r17",
"volume": "24",
"year": "2006"
},
{
"DOI": "10.1210/jc.2011-0385",
"article-title": "Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline.",
"author": "Holick",
"doi-asserted-by": "publisher",
"first-page": "1911",
"issue": "7",
"journal-title": "J Clin Endocrinol Metab",
"key": "zoi200688r27",
"volume": "96",
"year": "2011"
},
{
"DOI": "10.1097/00005650-199911000-00005",
"article-title": "The performance of different lookback periods and sources of information for Charlson comorbidity adjustment in Medicare claims.",
"author": "Zhang",
"doi-asserted-by": "publisher",
"first-page": "1128",
"issue": "11",
"journal-title": "Med Care",
"key": "zoi200688r29",
"volume": "37",
"year": "1999"
},
{
"DOI": "10.1093/aje/kwg074",
"article-title": "Estimating the relative risk in cohort studies and clinical trials of common outcomes.",
"author": "McNutt",
"doi-asserted-by": "publisher",
"first-page": "940",
"issue": "10",
"journal-title": "Am J Epidemiol",
"key": "zoi200688r30",
"volume": "157",
"year": "2003"
},
{
"DOI": "10.1002/(ISSN)1521-4036",
"article-title": "Parameter estimation and goodness-of-fit in log binomial regression.",
"author": "Blizzard",
"doi-asserted-by": "publisher",
"first-page": "5",
"issue": "1",
"journal-title": "Biom J",
"key": "zoi200688r32",
"volume": "48",
"year": "2006"
},
{
"DOI": "10.1016/j.dsx.2020.04.050",
"article-title": "Vitamin D concentrations and COVID-19 infection in UK Biobank.",
"author": "Hastie",
"doi-asserted-by": "publisher",
"first-page": "561",
"issue": "4",
"journal-title": "Diabetes Metab Syndr",
"key": "zoi200688r33",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.15585/mmwr.mm6924e2",
"article-title": "Coronavirus disease 2019 case surveillance - United States, January 22-May 30, 2020.",
"author": "Stokes",
"doi-asserted-by": "publisher",
"first-page": "759",
"issue": "24",
"journal-title": "MMWR Morb Mortal Wkly Rep",
"key": "zoi200688r35",
"volume": "69",
"year": "2020"
},
{
"DOI": "10.15585/mmwr.mm6918e1",
"article-title": "Characteristics and clinical outcomes of adult patients hospitalized with COVID-19 - Georgia, March 2020.",
"author": "Gold",
"doi-asserted-by": "publisher",
"first-page": "545",
"issue": "18",
"journal-title": "MMWR Morb Mortal Wkly Rep",
"key": "zoi200688r36",
"volume": "69",
"year": "2020"
},
{
"DOI": "10.3390/nu10111656",
"article-title": "Vitamin D: nutrient, hormone, and immunomodulator.",
"author": "Sassi",
"doi-asserted-by": "publisher",
"first-page": "1656",
"issue": "11",
"journal-title": "Nutrients",
"key": "zoi200688r37",
"volume": "10",
"year": "2018"
},
{
"DOI": "10.1371/journal.ppat.1001176",
"article-title": "Zn(2+) inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture.",
"author": "te Velthuis",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "PLoS Pathog",
"key": "zoi200688r39",
"volume": "6",
"year": "2010"
},
{
"article-title": "Vitamin D and inflammatory diseases.",
"author": "Yin",
"first-page": "69",
"journal-title": "J Inflamm Res",
"key": "zoi200688r40",
"volume": "7",
"year": "2014"
},
{
"DOI": "10.3390/ijms20225811",
"article-title": "Correlation of vitamin D with inflammatory cytokines, atherosclerotic parameters, and lifestyle factors in the setting of heart failure: a 12-month follow-up study.",
"author": "Roffe-Vazquez",
"doi-asserted-by": "publisher",
"first-page": "5811",
"issue": "22",
"journal-title": "Int J Mol Sci",
"key": "zoi200688r41",
"volume": "20",
"year": "2019"
},
{
"DOI": "10.1016/S0140-6736(20)30628-0",
"article-title": "COVID-19: consider cytokine storm syndromes and immunosuppression.",
"author": "Mehta",
"doi-asserted-by": "publisher",
"first-page": "1033",
"issue": "10229",
"journal-title": "Lancet",
"key": "zoi200688r42",
"volume": "395",
"year": "2020"
},
{
"author": "Del Valle",
"key": "zoi200688r26",
"volume-title": "Dietary Reference Intakes for Calcium and Vitamin D",
"year": "2011"
},
{
"author": "Institute of Medicine",
"key": "zoi200688r34",
"volume-title": "Dietary Reference Intakes for Calcium and Vitamin D",
"year": "2011"
},
{
"author": "Greger",
"first-page": "205",
"key": "zoi200688r38",
"volume-title": "Effect of Variations in Dietary Protein, Phosphorus, Electrolytes and Vitamin D on Calcium and Zinc Metabolism: Nutrient Interactions",
"year": "1988"
},
{
"key": "zoi200688r1",
"unstructured": "COVID-19 corona virus pandemic. Worldometer. Updated August 12, 2020. Accessed August 12, 2020. https://www.worldometers.info/coronavirus"
},
{
"key": "zoi200688r6",
"unstructured": "Umhau? JC. Casting sunlight on an epidemic: is vitamin D a critical host factor to prevent COVID-19? MedPage Today. Published March 25, 2020. Accessed April 13, 2020. https://www.medpagetoday.com/infectiousdisease/covid19/85596?"
},
{
"key": "zoi200688r7",
"unstructured": "NCHS, National Vital Statistics System. Provisional death counts for coronavirus disease (COVID-19). Centers for Disease Control and Prevention. Updated August 12, 2020. Accessed August 12, 2020. https://www.cdc.gov/nchs/nvss/vsrr/COVID19/index.htm"
},
{
"key": "zoi200688r8",
"unstructured": "National Center for Immunization and Respiratory Diseases (NCIRD), Division of Viral Diseases. Preparing for COVID-19 in nursing homes. Updated August 12, 2020. Accessed August 12, 2020. https://www.cdc.gov/coronavirus/2019-ncov/hcp/long-term-care.html"
},
{
"key": "zoi200688r14",
"unstructured": "Cumulative number of patients diagnosed with coronavirus disease (COVID-19) in Japan as of August 7, 2020. Statista. Accessed August 12, 2020. https://www.statista.com/statistics/1096478/japan-confirmed-cases-of-coronavirus-by-state-of-health"
},
{
"key": "zoi200688r18",
"unstructured": "Hunt? K. Britons urged to take vitamin D while sheltering inside during the pandemic. Published April 23, 2020. Accessed April 27, 2020. https://www.cnn.com/2020/04/23/health/vitamin-d-uk-coronavirus-wellness/index.html"
},
{
"key": "zoi200688r19",
"unstructured": "Frieden? T. Former CDC Chief Dr. Tom Frieden: coronavirus infection risk may be reduced by vitamin D. Fox News, Opinion. Published March 23, 2020. Accessed April 13, 2020. https://www.foxnews.com/opinion/former-cdc-chief-tom-frieden-coronavirus-risk-may-be-reduced-with-vitamin-d"
},
{
"key": "zoi200688r20",
"unstructured": "Medical societies advise on vitamin D in midst of COVID-19. Medscape. Published July 10, 2020. Accessed July 10, 2020. https://www.medscape.com/viewarticle/933715"
},
{
"key": "zoi200688r21",
"unstructured": "National Center for Immunization and Respiratory Diseases (NCIRD), Division of Viral Diseases. CDC diagnostic tests for COVID-19. Centers for Disease Control and Prevention. Updated August 5, 2020. Accessed August 12, 2020. https://www.cdc.gov/coronavirus/2019-ncov/lab/testing.html"
},
{
"DOI": "10.22627/2072-8107-2020-19-1-5-6",
"doi-asserted-by": "crossref",
"key": "zoi200688r22",
"unstructured": "Viracor. Coronavirus (COVID-19) SARS-CoV-2 PCR. Accessed July 13, 2020. https://www.viracor-eurofins.com/test-menu/8300-coronavirus-covid-19-sars-cov-2-rt-pcr/"
},
{
"key": "zoi200688r23",
"unstructured": "Roche Diagnostics. cobas SARS-CoV-2 test (for the COVID-19 coronavirus). Accessed July 13, 2020. https://diagnostics.roche.com/us/en/products/params/cobas-sars-cov-2-test.html"
},
{
"key": "zoi200688r24",
"unstructured": "Roche Diagnostics. cobas Elecsys Vitamin D total II assay. Accessed July 15, 2020. https://diagnostics.roche.com/se/sv/products/params/elecsys-vitamin-d-total-ii.html"
},
{
"key": "zoi200688r25",
"unstructured": "Mayo Clinic Laboratories. Test ID: DHVD: 1,25-dihydroxyvitamin D, serum. Accessed July 15, 2020. https://www.mayocliniclabs.com/test-catalog/Performance/8822"
},
{
"key": "zoi200688r28",
"unstructured": "Healthcare Cost and Utilization Project (HCUP). Elixhauser Comorbidity Software for ICD-10-CM (beta version).Version 2020 v1. Accessed April 8, 2020. https://www.hcup-us.ahrq.gov/toolssoftware/comorbidityicd10/comorbidity_icd10.jsp"
},
{
"key": "zoi200688r31",
"unstructured": "Pregibon? D. Data Analytic Methods for Generalized Linear Models. Dissertation. University of Toronto; 1979; 43."
}
],
"reference-count": 42,
"references-count": 42,
"relation": {},
"resource": {
"primary": {
"URL": "https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2770157"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Association of Vitamin D Status and Other Clinical Characteristics With COVID-19 Test Results",
"type": "journal-article",
"volume": "3"
}
