Low Serum 25-hydroxyvitamin D (Vitamin D) Level Is Associated With Susceptibility to COVID-19, Severity, and Mortality: A Systematic Review and Meta-Analysis
et al., Front. Nutr. 8:660420, doi:10.3389/fnut.2021.660420, Mar 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Systematic review and meta analysis showing that low vitamin D levels was associated with COVID-19 cases, severity, and mortality.
22 meta-analyses show significant improvements with vitamin D treatment for mortality1-15,
mechanical ventilation1,5,6,11,16-18 ,
ICU admission1,3,5,6,9,11,13,15-21 ,
hospitalization11,
severity2,4,5,10,22 , and
cases7,20,22 .
Currently there are 137 vitamin D treatment for COVID-19 studies, showing 39% lower mortality [32‑45%], 17% lower ventilation [-5‑35%], 45% lower ICU admission [28‑57%], 22% lower hospitalization [13‑30%], and 17% fewer cases [9‑25%].
1.
Shah et al., Does vitamin D supplementation reduce COVID-19 severity? - a systematic review, QJM: An International Journal of Medicine, doi:10.1093/qjmed/hcac040.
2.
Nikniaz et al., The impact of vitamin D supplementation on mortality rate and clinical outcomes of COVID-19 patients: A systematic review and meta-analysis, Pharmaceutical Sciences, doi:10.34172/PS.2021.13.
3.
Hosseini et al., Effects of Vitamin D Supplementation on COVID-19 Related Outcomes: A Systematic Review and Meta-Analysis, Nutrients, doi:10.3390/nu14102134.
4.
D’Ecclesiis et al., Vitamin D and SARS-CoV2 infection, severity and mortality: A systematic review and meta-analysis, PLOS ONE, doi:10.1371/journal.pone.0268396.
5.
Xie et al., Micronutrient perspective on COVID-19: Umbrella review and reanalysis of meta-analyses, Critical Reviews in Food Science and Nutrition, doi:10.1080/10408398.2023.2174948.
6.
Hariyanto et al., Vitamin D supplementation and Covid‐19 outcomes: A systematic review, meta‐analysis and meta‐regression, Reviews in Medical Virology, doi:10.1002/rmv.2269.
7.
Begum et al., The Role of Vitamin D in COVID-19 Survival and Prevention: A Meta-analysis, Sudan Journal of Medical Sciences, doi:10.18502/sjms.v19i1.15776.
8.
Jamilian et al., The role of vitamin D in outcomes of critical care in COVID-19 patients: Evidence from an umbrella meta-analysis of interventional and observational studies, Public Health Nutrition, doi:10.1017/S1368980024000934.
9.
Sobczak et al., Effect of Vitamin D3 Supplementation on Severe COVID-19: A Meta-Analysis of Randomized Clinical Trials, Nutrients, doi:10.3390/nu16101402.
10.
Petrelli et al., Therapeutic and prognostic role of vitamin D for COVID-19 infection: A systematic review and meta-analysis of 43 observational studies, The Journal of Steroid Biochemistry and Molecular Biology, doi:10.1016/j.jsbmb.2021.105883.
11.
Asla et al., Vitamin D on COVID-19 Patients During the Pandemic, 2022. A Systematic Review and Meta-Analysis, Current Research in Nutrition and Food Science Journal, doi:10.12944/CRNFSJ.11.1.3.
12.
Kow et al., The impact of vitamin D administration on mortality in COVID-19 patients: a systematic review and meta-analysis of randomized controlled trials, Inflammopharmacology, doi:10.1007/s10787-024-01564-2.
13.
Zhang et al., The impact of supplementing vitamin D through different methods on the prognosis of COVID-19 patients: a systematic review and meta-analysis, Frontiers in Nutrition, doi:10.3389/fnut.2024.1441847.
14.
Doustmohammadian et al., Impact of vitamin D supplementation on COVID-19 mortality: A systematic review and meta-analysis, Nutrition Clinique et Métabolisme, doi:10.1016/j.nupar.2025.12.001.
15.
Yang et al., Vitamin D supplementation benefits COVID-19: A systematic review and meta-analysis, Heliyon, doi:10.1016/j.heliyon.2026.e44988.
16.
Meng et al., The role of vitamin D in the prevention and treatment of SARS-CoV-2 infection: A meta-analysis of randomized controlled trials, Clinical Nutrition, doi:10.1016/j.clnu.2023.09.008.
17.
Yang (B) et al., Therapeutic effects of vitamin D supplementation on COVID-19 aggravation: a systematic review and meta-analysis of randomized controlled trials, Frontiers in Pharmacology, doi:10.3389/fphar.2024.1367686.
18.
Szarpak et al., Vitamin D supplementation to treat SARS-CoV-2 positive patients. Evidence from meta-analysis, Cardiology Journal, doi:10.5603/CJ.a2021.0122.
19.
Tentolouris et al., The effect of vitamin D supplementation on mortality and intensive care unit admission of COVID-19 patients. A systematic review, meta-analysis and meta-regression, Diabetes/Metabolism Research and Reviews, doi:10.1002/dmrr.3517.
20.
Sartini et al., Preventive Vitamin D Supplementation and Risk for COVID-19 Infection: A Systematic Review and Meta-Analysis, Nutrients, doi:10.3390/nu16050679.
Akbar et al., 29 Mar 2021, peer-reviewed, 4 authors.
Low Serum 25-hydroxyvitamin D (Vitamin D) Level Is Associated With Susceptibility to COVID-19, Severity, and Mortality: A Systematic Review and Meta-Analysis
Frontiers in Nutrition, doi:10.3389/fnut.2021.660420
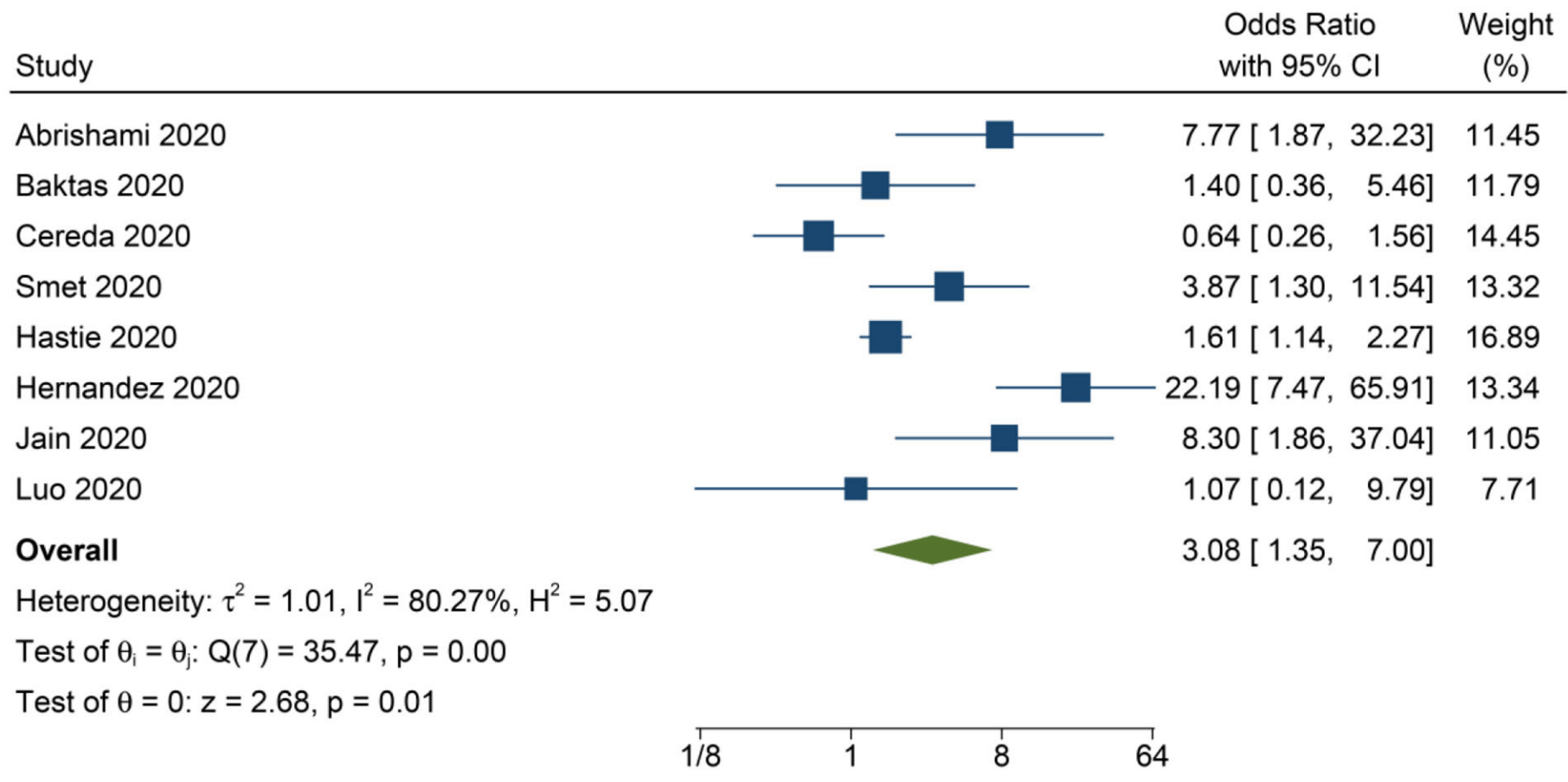
Background: This systematic review and meta-analysis aimed to assess whether low serum 25-hydroxyvitamin D (25-OHD) level is associated with susceptibility to COVID-19, severity, and mortality related to COVID-19. Methods: Systematic literature searches of PubMed, Scopus, and Embase database up until 9 December 2020. We include published observational prospective and retrospective studies with information on 25-OHD that reported main/secondary outcome. Low serum 25-OHD refers to participants with serum 25-OHD level below a cut-off point ranging from 20 to 30 ng/mL. Other cut-off values were excluded to reduce heterogeneity. The main outcome was mortality defined as non-survivor/death. The secondary outcome was susceptibility and severe COVID-19. Results: There were 14 studies comprising of 999,179 participants. Low serum 25-OHD was associated with higher rate of COVID-19 infection compared to the control group (OR = 2.71 [1.72, 4.29], p < 0.001; I 2 : 92.6%). Higher rate of severe COVID-19 was observed in patients with low serum 25-OHD (OR = 1.90 [1.24, 2.93], p = 0.003; I 2 : 55.3%), with a sensitivity of 83%, specificity of 39%, PLR of 1.4, NLR of 0.43, and DOR of 3. Low serum 25-OHD was associated with higher mortality (OR = 3.08 [1.35, 7 .00], p = 0.011; I 2 : 80.3%), with a sensitivity of 85%, specificity of 35%, PLR of 1.3, NLR of 0.44, and DOR of 3. Meta-regression analysis showed that the association between low serum 25-OHD and mortality was affected by male gender (OR = 1.22 [1.08, 1.39], p = 0.002), diabetes (OR = 0.88 [0.79, 0.98], p = 0.019).
Conclusion: Low serum 25-OHD level was associated with COVID-19 infection, severe presentation, and mortality.
AUTHOR CONTRIBUTIONS MA: conceptualization, investigation, writing -original draft, writing -review and editing, and supervision. AW: data curation, investigation, and writing -original draft. RP: conceptualization, methodology, software, data curation, formal analysis, statistical analysis, investigation, validation, and writing -original draft. BS: investigation, and writing -review and editing. All authors contributed to the article and approved the submitted version.
Conflict of Interest: The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. Copyright © 2021 Akbar, Wibowo, Pranata and Setiabudiawan. This is an openaccess article distributed under the terms of the Creative Commons Attribution License (CC BY). The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
References
Abrishami, Dalili, Torbati, Asgari, Arab-Ahmadi et al., Possible association of vitamin D status with lung involvement and outcome in patients with COVID-19: a retrospective study, Eur J Nutr, doi:10.1007/s00394-020-02411-0
Almerighi, Sinistro, Cavazza, Ciaprini, Rocchi et al., 1α,25-Dihydroxyvitamin D3 inhibits CD40L-induced pro-inflammatory and immunomodulatory activity in Human Monocytes, Cytokine, doi:10.1016/j.cyto.2008.12.009
Annweiler, Hanotte, De L'eprevier, Sabatier, Lafaie et al., Vitamin D and survival in COVID-19 patients: a quasi-experimental study, J Steroid Biochem Mol Biol, doi:10.1016/j.jsbmb.2020.105771
Baktash, Hosack, Patel, Shah, Kandiah et al., Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad Med J, doi:10.1136/postgradmedj-2020-138712
Carpagnano, Lecce, Quaranta, Zito, Buonamico et al., Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19, J Endocrinol Invest, doi:10.1007/s40618-020-01370-x
Cereda, Bogliolo, Klersy, Lobascio, Masi et al., Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital, Clin Nutr, doi:10.1016/j.clnu.2020.10.055
Egsmose, Lund, Mcnair, Lund, Storm et al., Low serum levels of 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D in institutionalized old people: influence of solar exposure and vitamin D supplementation, Age Ageing, doi:10.1093/ageing/16.1.35
Fahmi, #Covid19 Coronavirus Disease
Hastie, Pell, Sattar, Vitamin D and COVID-19 infection and mortality in UK Biobank, Eur J Nutr, doi:10.1101/2020.06.26.20140921
Henrina, Lim, Pranata, COVID-19 and misinformation: how an infodemic fueled the prominence of vitamin D, Br J Nutr, doi:10.1017/S0007114520002950
Hernández, Nan, Fernandez-Ayala, García-Unzueta, Hernández-Hernández et al., Vitamin D status in hospitalized patients with SARS-CoV-2 infection, J Clin Endocrinol Metab, doi:10.1210/clinem/dgaa733
Hofer, Münzker, Schwetz, Ulbing, Hutz et al., Testicular synthesis and vitamin D action, J Clin Endocrinol Metab, doi:10.1210/jc.2014-1690
Huang, Lim, Pranata, Diabetes mellitus is associated with increased mortality and severity of disease in COVID-19 pneumonia -a systematic review, meta-analysis, and meta-regression: diabetes and COVID-19, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2020.04.018
Huang, Pranata, Lymphopenia in severe coronavirus disease-2019 (COVID-19): systematic review and meta-analysis, J Intensive Care, doi:10.1186/s40560-020-00453-4
Im, Je, Baek, Chung, Kwon et al., Nutritional status of patients with COVID-19, Int J Infect Dis, doi:10.1016/j.ijid.2020.08.018
Jain, Chaurasia, Sengar, Singh, Mahor et al., Analysis of vitamin D level among asymptomatic and critically ill COVID-19 patients and its correlation with inflammatory markers, Sci Rep, doi:10.1038/s41598-020-77093-z
July, Pranata, Prevalence of dementia and its impact on mortality in patients with coronavirus disease 2019: a systematic review and meta-analysis, Geriatr Gerontol Int, doi:10.1111/ggi.14107
Katz, Yue, Xue, Increased risk for COVID-19 in patients with vitamin D deficiency, Nutrition, doi:10.1016/j.nut.2020.111106
Kennel, Drake, Hurley, Vitamin D deficiency in adults: when to test and how to treat, Mayo Clin Proc, doi:10.4065/mcp.2010.0138
Lim, Pranata, Huang, Yonas, Soeroto et al., Multiorgan failure with emphasis on acute kidney injury and severity of COVID-19: systematic review and meta-Analysis, Can J Kidney Heal Dis, doi:10.1177/2054358120938573
Luo, Liao, Shen, Li, Cheng, Vitamin D deficiency is inversely associated with COVID-19 incidence and disease severity in Chinese people, J Nutr, doi:10.1093/jn/nxaa332
Maghbooli, Sahraian, Ebrahimi, Pazoki, Kafan et al., Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection, PLoS One, doi:10.1371/journal.pone.0239799
Martineau, Jolliffe, Hooper, Greenberg, Aloia et al., Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data, BMJ, doi:10.1136/bmj.i6583
Meltzer, Best, Zhang, Vokes, Arora et al., Association of vitamin D status and other clinical characteristics with COVID-19 test results, JAMA Netw open, doi:10.1001/jamanetworkopen.2020.19722
Merzon, Tworowski, Gorohovski, Vinker, Cohen et al., Low plasma 25(OH) vitamin D level is associated with increased risk of COVID-19 infection: an Israeli population-based study, FEBS J, doi:10.1111/febs.15495
Metlay, Waterer, Long, Anzueto, Brozek et al., Diagnosis and treatment of adults with communityacquired pneumonia, Am J Respir Crit Care Med, doi:10.1164/rccm.201908-1581ST
Park, Lee, Hong, Lim, Koh et al., Effect of vitamin D deficiency in korean patients with acute respiratory distress syndrome, Korean J Intern Med, doi:10.3904/kjim.2017.380
Pizzini, Aichner, Sahanic, Böhm, Egger et al., Impact of vitamin d deficiency on covid-19-a prospective analysis from the covild registry, Nutrients, doi:10.3390/nu12092775
Pranata, Henrina, Lim, Lawrensia, Yonas et al., Clinical frailty scale and mortality in COVID-19: a systematic review and doseresponse meta-analysis: Clinical Frailty Scale in COVID-19, Arch Gerontol Geriatr, doi:10.1016/j.archger.2020.104324
Pranata, Huang, Lim, Wahjoepramono, July, Impact of cerebrovascular and cardiovascular diseases on mortality and severity of COVID-19-systematic review, metaanalysis, and meta-regression, J Stroke Cerebrovasc Dis, doi:10.1016/j.jstrokecerebrovasdis.2020.104949
Pranata, Lim, Huang, Raharjo, Lukito, Hypertension is associated with increased mortality and severity of disease in COVID-19 pneumonia: A systematic review, meta-analysis and meta-regression, J Renin Angiotensin Aldosterone Syst, doi:10.1177/1470320320926899
Pranata, Lim, Yonas, Vania, Lukito et al., Body mass index and outcome in patients with COVID-19: a dose-response metaanalysis, Diabetes Metab, doi:10.1016/j.diabet.2020.07.005
Pranata, Supriyadi, Huang, Permana, Lim et al., The association between chronic kidney disease and new onset renal replacement therapy on the outcome of COVID-19 patients: a meta-analysis, Clin Med Insights Circ Respir Pulm Med, doi:10.1177/1179548420959165
Radujkovic, Hippchen, Tiwari-Heckler, Dreher, Boxberger, Vitamin D deficiency and outcome of COVID-19 patients, Nutrients, doi:10.3390/nu12092757
Rastogi, Bhansali, Khare, Suri, Yaddanapudi et al., Short term, high-dose vitamin D supplementation for COVID-19 disease: a randomised, placebo-controlled
Sanghera, Sapkota, Aston, Blackett, Vitamin D status, gender differences, and cardiometabolic health disparities, Ann Nutr Metab, doi:10.1159/000458765
Santoso, Pranata, Wibowo, Al-Farabi, Huang et al., Cardiac injury is associated with mortality and critically ill pneumonia in COVID-19: a meta-analysis, Am J Emerg Med, doi:10.1016/j.ajem.2020.04.052
Shea, Griffin T S. P, Brennan, Mulkerrin, COVID-19: the older adult and the importance of vitamin D sufficiency, J Nutr Sci, doi:10.1017/jns.2020.36
Smet, Smet, Herroelen, Gryspeerdt, Martens, Serum 25(OH)D level on hospital admission associated with COVID-19 stage and mortality, Am J Clin Pathol, doi:10.1093/ajcp/aqaa252
Tan, Ho, Kalimuddin, Cherng, Teh et al., Cohort study to evaluate effect of vitamin D, magnesium, and vitamin B12 in combination on severe outcome progression in older patients with coronavirus (COVID-19), Nutrition, doi:10.1016/j.nut.2020.111017
Yonas, Alwi, Pranata, Huang, Lim et al., Effect of heart failure on the outcome of COVID-19 -a meta analysis and systematic review, Am J Emerg Med, doi:10.1016/j.ajem.2020.07.009
Zhang, Xu, Ni, Small studies may overestimate the effect sizes in critical care meta-analyses: a meta-epidemiological study, Crit Care, doi:10.1186/cc11919
DOI record:
{
"DOI": "10.3389/fnut.2021.660420",
"ISSN": [
"2296-861X"
],
"URL": "http://dx.doi.org/10.3389/fnut.2021.660420",
"abstract": "<jats:p><jats:bold>Background:</jats:bold> This systematic review and meta-analysis aimed to assess whether low serum 25-hydroxyvitamin D (25-OHD) level is associated with susceptibility to COVID-19, severity, and mortality related to COVID-19.</jats:p><jats:p><jats:bold>Methods:</jats:bold> Systematic literature searches of PubMed, Scopus, and Embase database up until 9 December 2020. We include published observational prospective and retrospective studies with information on 25-OHD that reported main/secondary outcome. Low serum 25-OHD refers to participants with serum 25-OHD level below a cut-off point ranging from 20 to 30 ng/mL. Other cut-off values were excluded to reduce heterogeneity. The main outcome was mortality defined as non-survivor/death. The secondary outcome was susceptibility and severe COVID-19.</jats:p><jats:p><jats:bold>Results:</jats:bold> There were 14 studies comprising of 999,179 participants. Low serum 25-OHD was associated with higher rate of COVID-19 infection compared to the control group (OR = 2.71 [1.72, 4.29], <jats:italic>p</jats:italic> &lt; 0.001; <jats:italic>I</jats:italic><jats:sup>2</jats:sup>: 92.6%). Higher rate of severe COVID-19 was observed in patients with low serum 25-OHD (OR = 1.90 [1.24, 2.93], <jats:italic>p</jats:italic> = 0.003; <jats:italic>I</jats:italic><jats:sup>2</jats:sup>: 55.3%), with a sensitivity of 83%, specificity of 39%, PLR of 1.4, NLR of 0.43, and DOR of 3. Low serum 25-OHD was associated with higher mortality (OR = 3.08 [1.35, 7.00], <jats:italic>p</jats:italic> = 0.011; <jats:italic>I</jats:italic><jats:sup>2</jats:sup>: 80.3%), with a sensitivity of 85%, specificity of 35%, PLR of 1.3, NLR of 0.44, and DOR of 3. Meta-regression analysis showed that the association between low serum 25-OHD and mortality was affected by male gender (OR = 1.22 [1.08, 1.39], <jats:italic>p</jats:italic> = 0.002), diabetes (OR = 0.88 [0.79, 0.98], <jats:italic>p</jats:italic> = 0.019).</jats:p><jats:p><jats:bold>Conclusion:</jats:bold> Low serum 25-OHD level was associated with COVID-19 infection, severe presentation, and mortality.</jats:p>",
"alternative-id": [
"10.3389/fnut.2021.660420"
],
"author": [
{
"affiliation": [],
"family": "Akbar",
"given": "Mohammad Rizki",
"sequence": "first"
},
{
"affiliation": [],
"family": "Wibowo",
"given": "Arief",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Pranata",
"given": "Raymond",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Setiabudiawan",
"given": "Budi",
"sequence": "additional"
}
],
"container-title": "Frontiers in Nutrition",
"container-title-short": "Front. Nutr.",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"frontiersin.org"
]
},
"created": {
"date-parts": [
[
2021,
3,
29
]
],
"date-time": "2021-03-29T05:09:07Z",
"timestamp": 1616994547000
},
"deposited": {
"date-parts": [
[
2021,
9,
27
]
],
"date-time": "2021-09-27T18:29:18Z",
"timestamp": 1632767358000
},
"indexed": {
"date-parts": [
[
2024,
5,
10
]
],
"date-time": "2024-05-10T12:47:35Z",
"timestamp": 1715345255512
},
"is-referenced-by-count": 60,
"issued": {
"date-parts": [
[
2021,
3,
29
]
]
},
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
3,
29
]
],
"date-time": "2021-03-29T00:00:00Z",
"timestamp": 1616976000000
}
}
],
"link": [
{
"URL": "https://www.frontiersin.org/articles/10.3389/fnut.2021.660420/full",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1965",
"original-title": [],
"prefix": "10.3389",
"published": {
"date-parts": [
[
2021,
3,
29
]
]
},
"published-online": {
"date-parts": [
[
2021,
3,
29
]
]
},
"publisher": "Frontiers Media SA",
"reference": [
{
"key": "B1",
"unstructured": "FahmiI\n #Covid19 Coronavirus Disease 2019 Situation Report - 312020"
},
{
"DOI": "10.1177/2054358120938573",
"article-title": "Multiorgan failure with emphasis on acute kidney injury and severity of COVID-19: systematic review and meta-Analysis",
"author": "Lim",
"doi-asserted-by": "publisher",
"first-page": "205435812093857",
"journal-title": "Can J Kidney Heal Dis.",
"key": "B2",
"volume": "7",
"year": "2020"
},
{
"DOI": "10.1016/j.ajem.2020.04.052",
"article-title": "Cardiac injury is associated with mortality and critically ill pneumonia in COVID-19: a meta-analysis",
"author": "Santoso",
"doi-asserted-by": "publisher",
"journal-title": "Am J Emerg Med",
"key": "B3",
"year": "2020"
},
{
"DOI": "10.1016/j.cyto.2008.12.009",
"article-title": "1α,25-Dihydroxyvitamin D3 inhibits CD40L-induced pro-inflammatory and immunomodulatory activity in Human Monocytes",
"author": "Almerighi",
"doi-asserted-by": "publisher",
"first-page": "190",
"journal-title": "Cytokine.",
"key": "B4",
"volume": "45",
"year": "2009"
},
{
"DOI": "10.3904/kjim.2017.380",
"article-title": "Effect of vitamin D deficiency in korean patients with acute respiratory distress syndrome",
"author": "Park",
"doi-asserted-by": "publisher",
"first-page": "1129",
"journal-title": "Korean J Intern Med.",
"key": "B5",
"volume": "33",
"year": "2018"
},
{
"DOI": "10.1136/bmj.i6583",
"article-title": "Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data",
"author": "Martineau",
"doi-asserted-by": "publisher",
"first-page": "i6583",
"journal-title": "BMJ.",
"key": "B6",
"volume": "356",
"year": "2017"
},
{
"DOI": "10.1017/S0007114520002950",
"article-title": "COVID-19 and misinformation: how an infodemic fueled the prominence of vitamin D",
"author": "Henrina",
"doi-asserted-by": "publisher",
"first-page": "359",
"journal-title": "Br J Nutr.",
"key": "B7",
"volume": "125",
"year": "2020"
},
{
"DOI": "10.1164/rccm.201908-1581ST",
"article-title": "Diagnosis and treatment of adults with community-acquired pneumonia",
"author": "Metlay",
"doi-asserted-by": "publisher",
"first-page": "E45",
"journal-title": "Am J Respir Crit Care Med.",
"key": "B8",
"volume": "200",
"year": "2019"
},
{
"DOI": "10.1136/postgradmedj-2020-138712",
"article-title": "Vitamin D status and outcomes for hospitalised older patients with COVID-19",
"author": "Baktash",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Postgrad Med J.",
"key": "B9",
"volume": "2",
"year": "2020"
},
{
"DOI": "10.1007/s00394-020-02411-0",
"article-title": "Possible association of vitamin D status with lung involvement and outcome in patients with COVID-19: a retrospective study",
"author": "Abrishami",
"doi-asserted-by": "publisher",
"journal-title": "Eur J Nutr",
"key": "B10",
"year": "2020"
},
{
"DOI": "10.1016/j.nut.2020.111106",
"article-title": "Increased risk for COVID-19 in patients with vitamin D deficiency",
"author": "Katz",
"doi-asserted-by": "publisher",
"first-page": "111106",
"journal-title": "Nutrition.",
"key": "B11",
"volume": "84",
"year": "2021"
},
{
"DOI": "10.1038/s41598-020-77093-z",
"article-title": "Analysis of vitamin D level among asymptomatic and critically ill COVID-19 patients and its correlation with inflammatory markers",
"author": "Jain",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Sci Rep.",
"key": "B12",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1093/ajcp/aqaa252",
"article-title": "Serum 25(OH)D level on hospital admission associated with COVID-19 stage and mortality",
"author": "De Smet",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Am J Clin Pathol.",
"key": "B13",
"volume": "25",
"year": "2020"
},
{
"DOI": "10.1093/jn/nxaa332",
"article-title": "Vitamin D deficiency is inversely associated with COVID-19 incidence and disease severity in Chinese people",
"author": "Luo",
"doi-asserted-by": "publisher",
"first-page": "98",
"journal-title": "J Nutr.",
"key": "B14",
"volume": "151",
"year": "2021"
},
{
"DOI": "10.3390/nu12092757",
"article-title": "Vitamin D deficiency and outcome of COVID-19 patients",
"author": "Radujkovic",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Nutrients.",
"key": "B15",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1111/febs.15495",
"article-title": "Low plasma 25(OH) vitamin D level is associated with increased risk of COVID-19 infection: an Israeli population-based study",
"author": "Merzon",
"doi-asserted-by": "publisher",
"first-page": "3693",
"journal-title": "FEBS J.",
"key": "B16",
"volume": "287",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"article-title": "Association of vitamin D status and other clinical characteristics with COVID-19 test results",
"author": "Meltzer",
"doi-asserted-by": "publisher",
"first-page": "e2019722",
"journal-title": "JAMA Netw open.",
"key": "B17",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1016/j.ijid.2020.08.018",
"article-title": "Nutritional status of patients with COVID-19",
"author": "Im",
"doi-asserted-by": "publisher",
"first-page": "390",
"journal-title": "Int J Infect Dis.",
"key": "B18",
"volume": "100",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0239799",
"article-title": "Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection",
"author": "Maghbooli",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "PLoS One.",
"key": "B19",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1210/clinem/dgaa733",
"article-title": "Vitamin D status in hospitalized patients with SARS-CoV-2 infection",
"author": "Hernández",
"doi-asserted-by": "publisher",
"first-page": "1343",
"journal-title": "J Clin Endocrinol Metab.",
"key": "B20",
"volume": "106",
"year": "2020"
},
{
"DOI": "10.1101/2020.06.26.20140921",
"article-title": "Vitamin D and COVID-19 infection and mortality in UK Biobank",
"author": "Hastie",
"doi-asserted-by": "publisher",
"first-page": "545",
"journal-title": "Eur J Nutr.",
"key": "B21",
"volume": "60",
"year": "2020"
},
{
"DOI": "10.1016/j.clnu.2020.10.055",
"article-title": "Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital",
"author": "Cereda",
"doi-asserted-by": "publisher",
"journal-title": "Clin Nutr",
"key": "B22",
"year": "2020"
},
{
"DOI": "10.1017/jns.2020.36",
"article-title": "COVID-19: the older adult and the importance of vitamin D sufficiency",
"author": "Shea",
"doi-asserted-by": "publisher",
"first-page": "e40",
"journal-title": "J Nutr Sci.",
"key": "B23",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1186/s40560-020-00453-4",
"article-title": "Lymphopenia in severe coronavirus disease-2019 (COVID-19): systematic review and meta-analysis",
"author": "Huang",
"doi-asserted-by": "publisher",
"first-page": "36",
"journal-title": "J Intensive Care.",
"key": "B24",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.4065/mcp.2010.0138",
"article-title": "Vitamin D deficiency in adults: when to test and how to treat",
"author": "Kennel",
"doi-asserted-by": "publisher",
"first-page": "752",
"journal-title": "Mayo Clin Proc.",
"key": "B25",
"volume": "85",
"year": "2010"
},
{
"DOI": "10.1210/jc.2014-1690",
"article-title": "Testicular synthesis and vitamin D action",
"author": "Hofer",
"doi-asserted-by": "publisher",
"first-page": "3766",
"journal-title": "J Clin Endocrinol Metab.",
"key": "B26",
"volume": "99",
"year": "2014"
},
{
"DOI": "10.1159/000458765",
"article-title": "Vitamin D status, gender differences, and cardiometabolic health disparities",
"author": "Sanghera",
"doi-asserted-by": "publisher",
"first-page": "79",
"journal-title": "Ann Nutr Metab.",
"key": "B27",
"volume": "70",
"year": "2017"
},
{
"DOI": "10.3390/nu12092775",
"article-title": "Impact of vitamin d deficiency on covid-19-a prospective analysis from the covild registry",
"author": "Pizzini",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Nutrients.",
"key": "B28",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1007/s40618-020-01370-x",
"article-title": "Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19",
"author": "Carpagnano",
"doi-asserted-by": "publisher",
"first-page": "765",
"journal-title": "J Endocrinol Invest",
"key": "B29",
"volume": "44",
"year": "2020"
},
{
"DOI": "10.1093/ageing/16.1.35",
"article-title": "Low serum levels of 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D in institutionalized old people: influence of solar exposure and vitamin D supplementation",
"author": "Egsmose",
"doi-asserted-by": "publisher",
"first-page": "35",
"journal-title": "Age Ageing.",
"key": "B30",
"volume": "16",
"year": "1987"
},
{
"DOI": "10.1016/j.jstrokecerebrovasdis.2020.104949",
"article-title": "Impact of cerebrovascular and cardiovascular diseases on mortality and severity of COVID-19-systematic review, meta-analysis, and meta-regression",
"author": "Pranata",
"doi-asserted-by": "publisher",
"first-page": "104949",
"journal-title": "J Stroke Cerebrovasc Dis.",
"key": "B31",
"volume": "29",
"year": "2020"
},
{
"DOI": "10.1016/j.diabet.2020.07.005",
"article-title": "Body mass index and outcome in patients with COVID-19: a dose-response meta-analysis",
"author": "Pranata",
"doi-asserted-by": "publisher",
"first-page": "101178",
"journal-title": "Diabetes Metab",
"key": "B32",
"volume": "47",
"year": "2020"
},
{
"DOI": "10.1177/1179548420959165",
"article-title": "The association between chronic kidney disease and new onset renal replacement therapy on the outcome of COVID-19 patients: a meta-analysis",
"author": "Pranata",
"doi-asserted-by": "publisher",
"first-page": "1179548420959165",
"journal-title": "Clin Med Insights Circ Respir Pulm Med.",
"key": "B33",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1177/1470320320926899",
"article-title": "Hypertension is associated with increased mortality and severity of disease in COVID-19 pneumonia: A systematic review, meta-analysis and meta-regression",
"author": "Pranata",
"doi-asserted-by": "publisher",
"first-page": "147032032092689",
"journal-title": "J Renin Angiotensin Aldosterone Syst.",
"key": "B34",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.04.018",
"article-title": "Diabetes mellitus is associated with increased mortality and severity of disease in COVID-19 pneumonia - a systematic review, meta-analysis, and meta-regression: diabetes and COVID-19",
"author": "Huang",
"doi-asserted-by": "publisher",
"first-page": "395",
"journal-title": "Diabetes Metab Syndr Clin Res Rev.",
"key": "B35",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/j.ajem.2020.07.009",
"article-title": "Effect of heart failure on the outcome of COVID-19 - a meta analysis and systematic review",
"author": "Yonas",
"doi-asserted-by": "publisher",
"journal-title": "Am J Emerg Med",
"key": "B36",
"year": "2020"
},
{
"DOI": "10.1016/j.archger.2020.104324",
"article-title": "Clinical frailty scale and mortality in COVID-19: a systematic review and dose-response meta-analysis: Clinical Frailty Scale in COVID-19",
"author": "Pranata",
"doi-asserted-by": "publisher",
"first-page": "104324",
"journal-title": "Arch Gerontol Geriatr.",
"key": "B37",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.1111/ggi.14107",
"article-title": "Prevalence of dementia and its impact on mortality in patients with coronavirus disease 2019: a systematic review and meta-analysis",
"author": "July",
"doi-asserted-by": "publisher",
"first-page": "172",
"journal-title": "Geriatr Gerontol Int",
"key": "B38",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1136/postgradmedj-2020-139065",
"article-title": "Short term, high-dose vitamin D supplementation for COVID-19 disease: a randomised, placebo-controlled, study (SHADE study)",
"author": "Rastogi",
"doi-asserted-by": "publisher",
"journal-title": "Postgrad Med J",
"key": "B39",
"year": "2020"
},
{
"DOI": "10.1016/j.nut.2020.111017",
"article-title": "Cohort study to evaluate effect of vitamin D, magnesium, and vitamin B12 in combination on severe outcome progression in older patients with coronavirus (COVID-19)",
"author": "Tan",
"doi-asserted-by": "publisher",
"first-page": "79",
"journal-title": "Nutrition.",
"key": "B40",
"year": "2020"
},
{
"DOI": "10.1016/j.jsbmb.2020.105771",
"article-title": "Vitamin D and survival in COVID-19 patients: a quasi-experimental study",
"author": "Annweiler",
"doi-asserted-by": "publisher",
"first-page": "105771",
"journal-title": "J Steroid Biochem Mol Biol.",
"key": "B41",
"volume": "204",
"year": "2020"
},
{
"DOI": "10.1186/cc11919",
"article-title": "Small studies may overestimate the effect sizes in critical care meta-analyses: a meta-epidemiological study",
"author": "Zhang",
"doi-asserted-by": "publisher",
"first-page": "R2",
"journal-title": "Crit Care.",
"key": "B42",
"volume": "17",
"year": "2013"
}
],
"reference-count": 42,
"references-count": 42,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.frontiersin.org/articles/10.3389/fnut.2021.660420/full"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Low Serum 25-hydroxyvitamin D (Vitamin D) Level Is Associated With Susceptibility to COVID-19, Severity, and Mortality: A Systematic Review and Meta-Analysis",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.3389/crossmark-policy",
"volume": "8"
}
