Lack of association of baseline 25-hydroxyvitamin D levels with disease severity and mortality in Indian patients hospitalized for COVID-19
et al., Scientific Reports, doi:10.1038/s41598-021-85809-y, Dec 2020 (preprint)
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
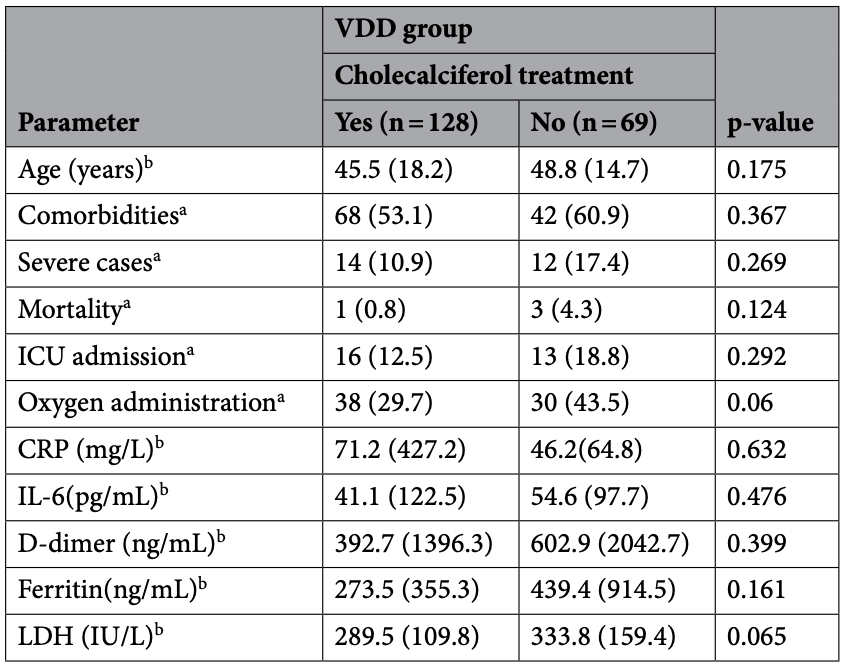
Prospective study of 410 hospitalized patients in India showing lower mortality and ICU admission with cholecalciferol treatment, although not statistically significant with the small number of cases. The median total dose was 60,000IU.
No significant difference was found for outcomes based on baseline vitamin D deficiency, however this analysis does not appear to account for the deficient patients that were treated with vitamin D.
Cholecalciferol was used in this study.
Meta-analysis shows that late stage treatment with calcitriol / calcifediol (or
paricalcitol, alfacalcidol, etc.) is more effective than cholecalciferol: 66% [47‑78%] lower risk vs. 43% [32‑52%] lower risk.
Cholecalciferol requires two hydroxylation steps to become activated - first
in the liver to calcifediol, then in the kidney to calcitriol. Calcitriol,
paricalcitol, and alfacalcidol are active vitamin D analogs that do not
require conversion. This allows them to have more rapid onset of action
compared to cholecalciferol. The time delay for cholecalciferol to increase
serum calcifediol levels can be 2-3 days, and the delay for converting
calcifediol to active calcitriol can be up to 7 days.
Bolus treatment is less effective.
Pharmacokinetics and the potential side effects of high bolus doses suggest
that ongoing treatment spread over time is more appropriate.
Research has confirmed that lower dose regular treatment with vitamin D is more
effective than intermittent high-dose bolus treatment for various conditions,
including rickets and acute respiratory infections1,2. The biological mechanisms supporting these
findings involve the induction of enzymes such as 24-hydroxylase and
fibroblast growth factor 23 (FGF23) by high-dose bolus treatments. These
enzymes play roles in inactivating vitamin D, which can paradoxically reduce
levels of activated vitamin D and suppress its activation for extended periods
post-dosage. Evidence indicates that 24-hydroxylase activity may remain
elevated for several weeks following a bolus dose, leading to reduced levels
of the activated form of vitamin D. Additionally, FGF23 levels can increase
for at least three months after a large bolus dose, which also contributes to
the suppression of vitamin D activation1.
This is the 16th of 137 COVID-19 controlled studies for vitamin D, which collectively show efficacy with p<0.0000000001.
41 studies are RCTs, which show efficacy with p=0.00000049.
|
risk of death, 82.0% lower, RR 0.18, p = 0.12, treatment 1 of 128 (0.8%), control 3 of 69 (4.3%), NNT 28.
|
|
risk of ICU admission, 33.7% lower, RR 0.66, p = 0.29, treatment 16 of 128 (12.5%), control 13 of 69 (18.8%), NNT 16.
|
|
risk of oxygen therapy, 31.7% lower, RR 0.68, p = 0.06, treatment 38 of 128 (29.7%), control 30 of 69 (43.5%), NNT 7.3.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Jevalikar et al., 28 Dec 2020, prospective, India, peer-reviewed, 8 authors, dosage 60,000IU single dose, median total dose.
Lack of association of baseline 25-hydroxyvitamin D levels with disease severity and mortality in Indian patients hospitalized for COVID-19
Scientific Reports, doi:10.1038/s41598-021-85809-y
Vitamin D deficiency (VDD) owing to its immunomodulatory effects is believed to influence outcomes in COVID-19. We conducted a prospective, observational study of patients, hospitalized with COVID-19. Serum 25-OHD level < 20 ng/mL was considered VDD. Patients were classified as having mild and severe disease on basis of the WHO ordinal scale for clinical improvement (OSCI). Of the 410 patients recruited, patients with VDD (197,48.2%) were significantly younger and had lesser comorbidities. The levels of PTH were significantly higher in the VDD group (63.5 ± 54.4 vs. 47.5 ± 42.9 pg/mL). The proportion of severe cases (13.2% vs.14.6%), mortality (2% vs. 5.2%), oxygen requirement (34.5% vs.43.4%), ICU admission (14.7% vs.19.8%) was not significantly different between patients with or without VDD. There was no significant correlation between serum 25-OHD levels and inflammatory markers studied. Serum parathormone levels correlated with D-dimer (r 0.117, p-0.019), ferritin (r 0.132, p-0.010), and LDH (r 0.124, p-0.018). Amongst VDD patients, 128(64.9%) were treated with oral cholecalciferol (median dose of 60,000 IU). The proportion of severe cases, oxygen, or ICU admission was not significantly different in the treated vs. untreated group. In conclusion, serum 25-OHD levels at admission did not correlate with inflammatory markers, clinical outcomes, or mortality in hospitalized COVID-19 patients. Treatment of VDD with cholecalciferol did not make any difference to the outcomes.
Author contributions G.J. drafted the study protocol, supervised patient enrollment, analyzed data, wrote the first draft of the manuscript, and will be the corresponding author for the manuscript. A.M. conceptualized the study, guided the study protocol, and critically reviewed the manuscript. A.S. supervised collection and reporting of laboratory investigations and contributed to the data collection. R.S., K.J.F., S.M. contributed to the data collection and analysis. K.J.F. reviewed the study protocol. A.D., S.B. critically reviewed the manuscript along with A.M.
Competing interests The authors declare no competing interests.
References
Adams, Hewison, Unexpected actions of vitamin D: New perspectives on the regulation of innate and adaptive immunity, Nat. Clin. Pract. Endocrinol. Metab
Ali, Role of vitamin D in preventing of COVID-19 infection, progression and severity, J. Infect. Public Health
Baktash, Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad. Med. J, doi:10.1136/postgradmedj-2020-138712
Cannell, Epidemic influenza and vitamin D, Epidemiol. Infect
Carpagnano, Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19, J. Endocrinol. Invest, doi:10.1007/s40618-020-01370-x
Cereda, Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital, Clin. Nutr, doi:10.1016/j.clnu.2020.10.055
Guan, Clinical characteristics of Coronavirus disease 2019 in China, N. Engl. J. Med
Hansdottir, Vitamin D decreases respiratory syncytial virus induction of NF-kappaB-linked chemokines and cytokines in airway epithelium while maintaining the antiviral state, J. Immunol
Hernández, Vitamin D status in hospitalized patients with SARS-CoV-2 infection, J. Clin. Endocrinol. Metab, doi:10.1210/clinem/dgaa733
Holick, Evaluation, treatment, and prevention of vitamin D deficiency: An Endocrine Society clinical practice guideline, J. Clin. Endocrinol. Metab
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin. Exp. Res, doi:10.1007/s40520-020-01570-8
Jain, Analysis of vitamin D level among asymptomatic and critically ill COVID-19 patients and its correlation with inflammatory markers, Sci. Rep
Karahan, Katkat, Impact of serum 25(OH) vitamin D level on mortality in patients with COVID-19 in Turkey, J. Nutr. Health Aging
Liu, Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response, Science
Maghbooli, Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection, PLoS ONE, doi:10.1371/journal.pone.0239799
Martineau, Forouhi, Vitamin D for COVID-19: A case to answer?, Lancet Diabetes Endocrinol
Martineau, Vitamin D supplementation to prevent acute respiratory tract infections: Systematic review and meta-analysis of individual participant data, BMJ
Mithal, Global vitamin D status and determinants of hypovitaminosis D, Osteoporos. Int
Murai, Effect of a Single High Dose of Vitamin D3 on Hospital Length of Stay in Patients With Moderate to Severe COVID-19: A Randomized Clinical Trial, JAMA, doi:10.1001/jama.2020.26848
Ohaegbulam, Swalih, Patel, Smith, Perrin, Vitamin D supplementation in COVID-19 patients: A clinical case series, Am J Ther, doi:10.1097/MJT.0000000000001222
Padhi, Suvankar, Panda, Pati, Panda, Lower levels of vitamin D are associated with SARS-CoV-2 infection and mortality in the Indian population: An observational study, Int. Immunopharmacol
Panagiotou, Low serum 25-hydroxyvitamin D (25[OH]D) levels in patients hospitalised with COVID-19 are associated with greater disease severity, Clin. Endocrinol, doi:10.1111/cen.14276
Pham, Rahman, Majidi, Waterhouse, Neale, Acute respiratory tract infection and 25-hydroxyvitamin D concentration: A systematic review and meta-analysis, Int. J. Environ. Res. Public Health, doi:10.3390/ijerph16173020
Pizzini, Impact of vitamin D deficiency on COVID-19: A prospective analysis from the CovILD registry, Nutrients, doi:10.3390/nu12092775
Radujkovic, Vitamin D deficiency and outcome of COVID-19 patients, Nutrients, doi:10.3390/nu12092757
Rastogi, Short term, high-dose vitamin D supplementation for COVID-19 disease: A randomised, placebo-controlled, study (SHADE study), Postgraduate Med. J, doi:10.1136/postgradmedj-2020-139065
Rhodes, Subramanian, Laird, Kenny, low population mortality from COVID-19 in countries south of latitude 35 degrees North supports vitamin D as a factor determining severity, Aliment. Pharmacol. Ther, doi:10.1111/apt.15777
Samaddar, Gadepalli, Nag, Misra, The enigma of low COVID-19 fatality rate in India, Front. Genet
Wu, Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan China, JAMA Intern. Med, doi:10.1001/jamainternmed.2020.0994
Xiao, Vitamin D supplementation for the prevention of childhood acute respiratory infections: A systematic review of randomised controlled trials, Br. J. Nutr
DOI record:
{
"DOI": "10.1038/s41598-021-85809-y",
"ISSN": [
"2045-2322"
],
"URL": "http://dx.doi.org/10.1038/s41598-021-85809-y",
"abstract": "<jats:title>Abstract</jats:title><jats:p>Vitamin D deficiency (VDD) owing to its immunomodulatory effects is believed to influence outcomes in COVID-19. We conducted a prospective, observational study of patients, hospitalized with COVID-19. Serum 25-OHD level < 20 ng/mL was considered VDD. Patients were classified as having mild and severe disease on basis of the WHO ordinal scale for clinical improvement (OSCI). Of the 410 patients recruited, patients with VDD (197,48.2%) were significantly younger and had lesser comorbidities. The levels of PTH were significantly higher in the VDD group (63.5 ± 54.4 vs. 47.5 ± 42.9 pg/mL). The proportion of severe cases (13.2% vs.14.6%), mortality (2% vs. 5.2%), oxygen requirement (34.5% vs.43.4%), ICU admission (14.7% vs.19.8%) was not significantly different between patients with or without VDD. There was no significant correlation between serum 25-OHD levels and inflammatory markers studied. Serum parathormone levels correlated with D-dimer (r 0.117, p- 0.019), ferritin (r 0.132, p-0.010), and LDH (r 0.124, p-0.018). Amongst VDD patients, 128(64.9%) were treated with oral cholecalciferol (median dose of 60,000 IU). The proportion of severe cases, oxygen, or ICU admission was not significantly different in the treated vs. untreated group. In conclusion, serum 25-OHD levels at admission did not correlate with inflammatory markers, clinical outcomes, or mortality in hospitalized COVID-19 patients. Treatment of VDD with cholecalciferol did not make any difference to the outcomes.</jats:p>",
"alternative-id": [
"85809"
],
"article-number": "6258",
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "15 December 2020"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "3 March 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "18 March 2021"
},
{
"group": {
"label": "Competing interests",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1,
"value": "The authors declare no competing interests."
}
],
"author": [
{
"affiliation": [],
"family": "Jevalikar",
"given": "Ganesh",
"sequence": "first"
},
{
"affiliation": [],
"family": "Mithal",
"given": "Ambrish",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Singh",
"given": "Anshu",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sharma",
"given": "Rutuja",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Farooqui",
"given": "Khalid J.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mahendru",
"given": "Shama",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Dewan",
"given": "Arun",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Budhiraja",
"given": "Sandeep",
"sequence": "additional"
}
],
"container-title": "Scientific Reports",
"container-title-short": "Sci Rep",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2021,
3,
18
]
],
"date-time": "2021-03-18T16:47:41Z",
"timestamp": 1616086061000
},
"deposited": {
"date-parts": [
[
2022,
12,
3
]
],
"date-time": "2022-12-03T05:23:36Z",
"timestamp": 1670045016000
},
"indexed": {
"date-parts": [
[
2024,
3,
1
]
],
"date-time": "2024-03-01T17:29:54Z",
"timestamp": 1709314194645
},
"is-referenced-by-count": 42,
"issue": "1",
"issued": {
"date-parts": [
[
2021,
3,
18
]
]
},
"journal-issue": {
"issue": "1",
"published-online": {
"date-parts": [
[
2021,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
3,
18
]
],
"date-time": "2021-03-18T00:00:00Z",
"timestamp": 1616025600000
}
},
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
3,
18
]
],
"date-time": "2021-03-18T00:00:00Z",
"timestamp": 1616025600000
}
}
],
"link": [
{
"URL": "https://www.nature.com/articles/s41598-021-85809-y.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://www.nature.com/articles/s41598-021-85809-y",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://www.nature.com/articles/s41598-021-85809-y.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1038",
"published": {
"date-parts": [
[
2021,
3,
18
]
]
},
"published-online": {
"date-parts": [
[
2021,
3,
18
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"key": "85809_CR1",
"unstructured": "Coronavirus Update (Live): 63,198,955 Cases and 1,467,506 Deaths from COVID-19 Virus Pandemic—Worldometer. https://www.worldometers.info/coronavirus/. Accessed 30 Nov 2020."
},
{
"DOI": "10.1017/S0950268806007175",
"author": "JJ Cannell",
"doi-asserted-by": "publisher",
"first-page": "1129",
"journal-title": "Epidemiol. Infect.",
"key": "85809_CR2",
"unstructured": "Cannell, J. J. et al. Epidemic influenza and vitamin D. Epidemiol. Infect. 134, 1129–1140 (2006).",
"volume": "134",
"year": "2006"
},
{
"DOI": "10.1136/bmj.i6583",
"author": "AR Martineau",
"doi-asserted-by": "publisher",
"first-page": "i6583",
"journal-title": "BMJ",
"key": "85809_CR3",
"unstructured": "Martineau, A. R. et al. Vitamin D supplementation to prevent acute respiratory tract infections: Systematic review and meta-analysis of individual participant data. BMJ 356, i6583 (2017).",
"volume": "356",
"year": "2017"
},
{
"DOI": "10.3390/ijerph16173020",
"author": "H Pham",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Int. J. Environ. Res. Public Health",
"key": "85809_CR4",
"unstructured": "Pham, H., Rahman, A., Majidi, A., Waterhouse, M. & Neale, R. E. Acute respiratory tract infection and 25-hydroxyvitamin D concentration: A systematic review and meta-analysis. Int. J. Environ. Res. Public Health 16, 1. https://doi.org/10.3390/ijerph16173020 (2019).",
"volume": "16",
"year": "2019"
},
{
"DOI": "10.1017/S000711451500207X",
"author": "L Xiao",
"doi-asserted-by": "publisher",
"first-page": "1026",
"journal-title": "Br. J. Nutr.",
"key": "85809_CR5",
"unstructured": "Xiao, L. et al. Vitamin D supplementation for the prevention of childhood acute respiratory infections: A systematic review of randomised controlled trials. Br. J. Nutr. 114, 1026–1034 (2015).",
"volume": "114",
"year": "2015"
},
{
"DOI": "10.1126/science.1123933",
"author": "PT Liu",
"doi-asserted-by": "publisher",
"first-page": "1770",
"journal-title": "Science",
"key": "85809_CR6",
"unstructured": "Liu, P. T. et al. Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response. Science 311, 1770–1773 (2006).",
"volume": "311",
"year": "2006"
},
{
"DOI": "10.1038/ncpendmet0716",
"author": "JS Adams",
"doi-asserted-by": "publisher",
"first-page": "80",
"journal-title": "Nat. Clin. Pract. Endocrinol. Metab.",
"key": "85809_CR7",
"unstructured": "Adams, J. S. & Hewison, M. Unexpected actions of vitamin D: New perspectives on the regulation of innate and adaptive immunity. Nat. Clin. Pract. Endocrinol. Metab. 4, 80–90 (2008).",
"volume": "4",
"year": "2008"
},
{
"DOI": "10.4049/jimmunol.0902840",
"author": "S Hansdottir",
"doi-asserted-by": "publisher",
"first-page": "965",
"journal-title": "J. Immunol.",
"key": "85809_CR8",
"unstructured": "Hansdottir, S. et al. Vitamin D decreases respiratory syncytial virus induction of NF-kappaB-linked chemokines and cytokines in airway epithelium while maintaining the antiviral state. J. Immunol. 184, 965–974 (2010).",
"volume": "184",
"year": "2010"
},
{
"DOI": "10.1056/NEJMoa2002032",
"author": "W-J Guan",
"doi-asserted-by": "publisher",
"first-page": "1708",
"journal-title": "N. Engl. J. Med.",
"key": "85809_CR9",
"unstructured": "Guan, W.-J. et al. Clinical characteristics of Coronavirus disease 2019 in China. N. Engl. J. Med. 382, 1708–1720 (2020).",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1001/jamainternmed.2020.0994",
"author": "C Wu",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "JAMA Intern. Med.",
"key": "85809_CR10",
"unstructured": "Wu, C. et al. Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan China. JAMA Intern. Med. 1, 1. https://doi.org/10.1001/jamainternmed.2020.0994 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1111/apt.15777",
"author": "JM Rhodes",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Aliment. Pharmacol. Ther.",
"key": "85809_CR11",
"unstructured": "Rhodes, J. M., Subramanian, S., Laird, E. & Kenny, R. A. low population mortality from COVID-19 in countries south of latitude 35 degrees North supports vitamin D as a factor determining severity. Aliment. Pharmacol. Ther. 1, 1. https://doi.org/10.1111/apt.15777 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1007/s40520-020-01570-8",
"author": "PC Ilie",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Aging Clin. Exp. Res.",
"key": "85809_CR12",
"unstructured": "Ilie, P. C., Stefanescu, S. & Smith, L. The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality. Aging Clin. Exp. Res. 1, 1. https://doi.org/10.1007/s40520-020-01570-8 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1111/cen.14276",
"author": "G Panagiotou",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Clin. Endocrinol.",
"key": "85809_CR13",
"unstructured": "Panagiotou, G. et al. Low serum 25-hydroxyvitamin D (25[OH]D) levels in patients hospitalised with COVID-19 are associated with greater disease severity. Clin. Endocrinol. 1, 1. https://doi.org/10.1111/cen.14276 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.3390/nu12092757",
"author": "A Radujkovic",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Nutrients",
"key": "85809_CR14",
"unstructured": "Radujkovic, A. et al. Vitamin D deficiency and outcome of COVID-19 patients. Nutrients 12, 1. https://doi.org/10.3390/nu12092757 (2020).",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1038/s41598-020-77093-z",
"author": "A Jain",
"doi-asserted-by": "publisher",
"first-page": "20191",
"journal-title": "Sci. Rep.",
"key": "85809_CR15",
"unstructured": "Jain, A. et al. Analysis of vitamin D level among asymptomatic and critically ill COVID-19 patients and its correlation with inflammatory markers. Sci. Rep. 10, 20191 (2020).",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30268-0",
"author": "AR Martineau",
"doi-asserted-by": "publisher",
"first-page": "735",
"journal-title": "Lancet Diabetes Endocrinol.",
"key": "85809_CR16",
"unstructured": "Martineau, A. R. & Forouhi, N. G. Vitamin D for COVID-19: A case to answer?. Lancet Diabetes Endocrinol. 8, 735–736 (2020).",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1007/s00198-009-0954-6",
"author": "A Mithal",
"doi-asserted-by": "publisher",
"first-page": "1807",
"journal-title": "Osteoporos. Int.",
"key": "85809_CR17",
"unstructured": "Mithal, A. et al. Global vitamin D status and determinants of hypovitaminosis D. Osteoporos. Int. 20, 1807–1820 (2009).",
"volume": "20",
"year": "2009"
},
{
"DOI": "10.3389/fgene.2020.00854",
"author": "A Samaddar",
"doi-asserted-by": "publisher",
"first-page": "854",
"journal-title": "Front. Genet.",
"key": "85809_CR18",
"unstructured": "Samaddar, A., Gadepalli, R., Nag, V. L. & Misra, S. The enigma of low COVID-19 fatality rate in India. Front. Genet. 11, 854 (2020).",
"volume": "11",
"year": "2020"
},
{
"key": "85809_CR19",
"unstructured": "COVID-19_Treatment_Trial_Design_Master_Protocol_synopsis_Final_18022020.pdf. https://www.who.int/blueprint/priority-diseases/key-action/COVID-19_Treatment_Trial_Design_Master_Protocol_synopsis_Final_18022020.pdf. Accessed Nov 6 2020."
},
{
"DOI": "10.1016/j.jiph.2020.06.021",
"author": "N Ali",
"doi-asserted-by": "publisher",
"first-page": "1373",
"journal-title": "J. Infect. Public Health",
"key": "85809_CR20",
"unstructured": "Ali, N. Role of vitamin D in preventing of COVID-19 infection, progression and severity. J. Infect. Public Health 13, 1373–1380 (2020).",
"volume": "13",
"year": "2020"
},
{
"DOI": "10.1210/jc.2011-0385",
"author": "MF Holick",
"doi-asserted-by": "publisher",
"first-page": "1911",
"journal-title": "J. Clin. Endocrinol. Metab.",
"key": "85809_CR21",
"unstructured": "Holick, M. F. et al. Evaluation, treatment, and prevention of vitamin D deficiency: An Endocrine Society clinical practice guideline. J. Clin. Endocrinol. Metab. 96, 1911–1930 (2011).",
"volume": "96",
"year": "2011"
},
{
"DOI": "10.1016/j.intimp.2020.107001",
"author": "S Padhi",
"doi-asserted-by": "publisher",
"first-page": "107001",
"journal-title": "Int. Immunopharmacol.",
"key": "85809_CR22",
"unstructured": "Padhi, S., Suvankar, S., Panda, V. K., Pati, A. & Panda, A. K. Lower levels of vitamin D are associated with SARS-CoV-2 infection and mortality in the Indian population: An observational study. Int. Immunopharmacol. 88, 107001 (2020).",
"volume": "88",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0239799",
"author": "Z Maghbooli",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "PLoS ONE",
"key": "85809_CR23",
"unstructured": "Maghbooli, Z. et al. Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection. PLoS ONE 15, 1. https://doi.org/10.1371/journal.pone.0239799 (2020).",
"volume": "15",
"year": "2020"
},
{
"author": "S Karahan",
"first-page": "1",
"journal-title": "J. Nutr. Health Aging",
"key": "85809_CR24",
"unstructured": "Karahan, S. & Katkat, F. Impact of serum 25(OH) vitamin D level on mortality in patients with COVID-19 in Turkey. J. Nutr. Health Aging 1, 1–8 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1136/postgradmedj-2020-138712",
"author": "V Baktash",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Postgrad. Med. J.",
"key": "85809_CR25",
"unstructured": "Baktash, V. et al. Vitamin D status and outcomes for hospitalised older patients with COVID-19. Postgrad. Med. J. 1, 1. https://doi.org/10.1136/postgradmedj-2020-138712 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1007/s40618-020-01370-x",
"author": "GE Carpagnano",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "J. Endocrinol. Invest.",
"key": "85809_CR26",
"unstructured": "Carpagnano, G. E. et al. Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19. J. Endocrinol. Invest. 1, 1. https://doi.org/10.1007/s40618-020-01370-x (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1016/j.clnu.2020.10.055",
"author": "E Cereda",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Clin. Nutr.",
"key": "85809_CR27",
"unstructured": "Cereda, E. et al. Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital. Clin. Nutr. 1, 1. https://doi.org/10.1016/j.clnu.2020.10.055 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1210/clinem/dgaa733",
"author": "JL Hernández",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "J. Clin. Endocrinol. Metab.",
"key": "85809_CR28",
"unstructured": "Hernández, J. L. et al. Vitamin D status in hospitalized patients with SARS-CoV-2 infection. J. Clin. Endocrinol. Metab. 1, 1. https://doi.org/10.1210/clinem/dgaa733 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.3390/nu12092775",
"author": "A Pizzini",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Nutrients",
"key": "85809_CR29",
"unstructured": "Pizzini, A. et al. Impact of vitamin D deficiency on COVID-19: A prospective analysis from the CovILD registry. Nutrients 12, 1. https://doi.org/10.3390/nu12092775 (2020).",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1136/postgradmedj-2020-139065",
"author": "A Rastogi",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Postgraduate Med. J.",
"key": "85809_CR30",
"unstructured": "Rastogi, A. et al. Short term, high-dose vitamin D supplementation for COVID-19 disease: A randomised, placebo-controlled, study (SHADE study). Postgraduate Med. J. 1, 1. https://doi.org/10.1136/postgradmedj-2020-139065 (2020).",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1097/MJT.0000000000001222",
"author": "KC Ohaegbulam",
"doi-asserted-by": "publisher",
"first-page": "e485",
"issue": "5",
"journal-title": "Am J Ther.",
"key": "85809_CR31",
"unstructured": "Ohaegbulam, K. C., Swalih, M., Patel, P., Smith, M. A. & Perrin, R. Vitamin D supplementation in COVID-19 patients: A clinical case series. Am J Ther. 27(5), e485–e490. https://doi.org/10.1097/MJT.0000000000001222 (2020).",
"volume": "27",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.26848",
"doi-asserted-by": "publisher",
"key": "85809_CR32",
"unstructured": "Murai, IH. et al. Effect of a Single High Dose of Vitamin D3 on Hospital Length of Stay in Patients With Moderate to Severe COVID-19: A Randomized Clinical Trial. JAMA. 2021 Feb 17:e2026848. https://doi.org/10.1001/jama.2020.26848 (2020). "
}
],
"reference-count": 32,
"references-count": 32,
"relation": {
"has-preprint": [
{
"asserted-by": "object",
"id": "10.21203/rs.3.rs-129238/v1",
"id-type": "doi"
}
]
},
"resource": {
"primary": {
"URL": "https://www.nature.com/articles/s41598-021-85809-y"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Multidisciplinary"
],
"subtitle": [],
"title": "Lack of association of baseline 25-hydroxyvitamin D levels with disease severity and mortality in Indian patients hospitalized for COVID-19",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "11"
}
