Melatonin: highlighting its use as a potential treatment for SARS-CoV-2 infection
et al., Cellular and Molecular Life Sciences, doi:10.1007/s00018-021-04102-3, Feb 2022
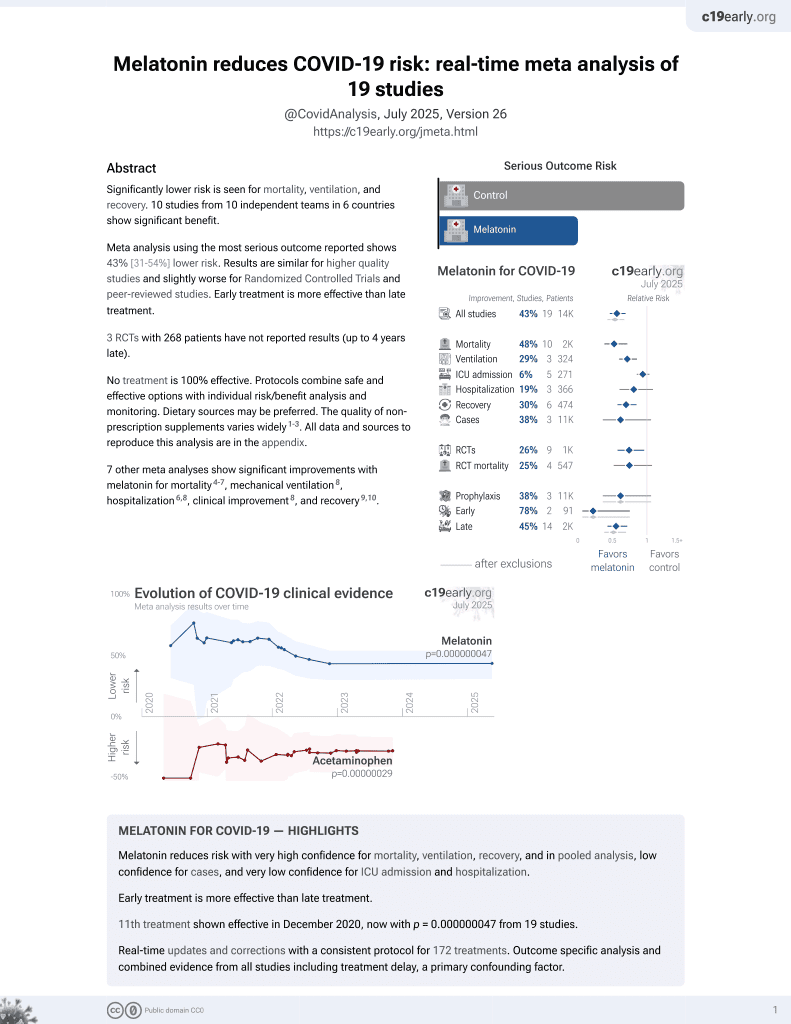
Melatonin for COVID-19
25th treatment shown to reduce risk in
May 2021, now with p = 0.000000015 from 18 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Review of the clinical evidence and mechanisms of action supporting the use of melatonin for COVID-19.
1.
Chen et al., Viral mitochondriopathy in COVID-19, Redox Biology, doi:10.1016/j.redox.2025.103766.
2.
Sanduzzi Zamparelli et al., Immune-Boosting and Antiviral Effects of Antioxidants in COVID-19 Pneumonia: A Therapeutic Perspective, Life, doi:10.3390/life15010113.
3.
Xie et al., The role of reactive oxygen species in severe acute respiratory syndrome coronavirus 2 (SARS-COV-2) infection-induced cell death, Cellular & Molecular Biology Letters, doi:10.1186/s11658-024-00659-6.
4.
Zhao et al., Melatonin Potentially Acts as a Widely-Acting Protective Tool in COVID-19, Medicine Research, doi:10.21127/yaoyimr20240006.
5.
Yehia et al., Melatonin: a ferroptosis inhibitor with potential therapeutic efficacy for the post-COVID-19 trajectory of accelerated brain aging and neurodegeneration, Molecular Neurodegeneration, doi:10.1186/s13024-024-00728-6.
6.
Chacin-Bonilla et al., Melatonin and viral infections: A review focusing on therapeutic effects and SARS-CoV-2, Melatonin Research, doi:10.32794/mr112500168.
7.
Lempesis et al., A mid‑pandemic night's dream: Melatonin, from harbinger of anti‑inflammation to mitochondrial savior in acute and long COVID‑19 (Review), International Journal of Molecular Medicine, doi:10.3892/ijmm.2024.5352.
8.
Alomari et al., Assessing the antiviral potential of melatonin: A comprehensive systematic review, Reviews in Medical Virology, doi:10.1002/rmv.2499.
9.
Donzelli, A., Neglected Effective Early Therapies against COVID-19: Focus on Functional Foods and Related Active Substances. A Review, MDPI AG, doi:10.20944/preprints202312.1178.v1.
10.
Langen, M., Melatonin - the Hormone of Both Sun and Darkness - Protects Your Health and Can Save Your Life, Rounding The Earth, roundingtheearth.substack.com/p/melatonin-the-hormone-of-both-sun.
11.
Hosseinzadeh et al., Melatonin effect on platelets and coagulation: Implications for a prophylactic indication in COVID-19, Life Sciences, doi:10.1016/j.lfs.2022.120866.
12.
Loh et al., Melatonin: Regulation of Viral Phase Separation and Epitranscriptomics in Post-Acute Sequelae of COVID-19, International Journal of Molecular Sciences, doi:10.3390/ijms23158122.
13.
Reiter et al., Melatonin: highlighting its use as a potential treatment for SARS-CoV-2 infection, Cellular and Molecular Life Sciences, doi:10.1007/s00018-021-04102-3.
14.
Tan et al., Mechanisms and clinical evidence to support melatonin's use in severe COVID-19 patients to lower mortality, Life Sciences, doi:10.1016/j.lfs.2022.120368.
15.
Behl et al., CD147-spike protein interaction in COVID-19: Get the ball rolling with a novel receptor and therapeutic target, Science of The Total Environment, doi:10.1016/j.scitotenv.2021.152072.
16.
Castle et al., Implications for Systemic Approaches to COVID-19: Effect Sizes of Remdesivir, Tocilizumab, Melatonin, Vitamin D3, and Meditation, Journal of Inflammation Research, doi:10.2147/JIR.S323356.
17.
Ramos et al., The Coronavirus Disease 2019 (COVID-19): Key Emphasis on Melatonin Safety and Therapeutic Efficacy, Antioxidants, doi:10.3390/antiox10071152.
18.
Camp et al., Melatonin interferes with COVID-19 at several distinct ROS-related steps, Journal of Inorganic Biochemistry, doi:10.1016/j.jinorgbio.2021.111546.
19.
Cross et al., Melatonin for the Early Treatment of COVID-19: A Narrative Review of Current Evidence and Possible Efficacy, Endocrine Practice, doi:10.1016/j.eprac.2021.06.001.
20.
DiNicolantonio et al., Melatonin may decrease risk for and aid treatment of COVID-19 and other RNA viral infections, Open Heart, doi:10.1136/openhrt-2020-001568.
21.
Reiter (B) et al., Therapeutic Algorithm for Use of Melatonin in Patients With COVID-19, Frontiers in Medicine, doi:10.3389/fmed.2020.00226.
22.
Charaa et al., Prophylactic Treatment Protocol against the Severity of COVID-19 Using Melatonin, SSRN, doi:10.2139/ssrn.3601861.
Reiter et al., 20 Feb 2022, peer-reviewed, 11 authors.
Melatonin: highlighting its use as a potential treatment for SARS-CoV-2 infection
Cellular and Molecular Life Sciences, doi:10.1007/s00018-021-04102-3
Numerous pharmaceutical drugs have been repurposed for use as treatments for COVID-19 disease. These drugs have not consistently demonstrated high efficacy in preventing or treating this serious condition and all have side effects to differing degrees. We encourage the continued consideration of the use of the antioxidant and anti-inflammatory agent, melatonin, as a countermeasure to a SARS-CoV-2 infection. More than 140 scientific publications have identified melatonin as a likely useful agent to treat this disease. Moreover, the publications cited provide the rationale for the use of melatonin as a prophylactic agent against this condition. Melatonin has pan-antiviral effects and it diminishes the severity of viral infections and reduces the death of animals infected with numerous different viruses, including three different coronaviruses. Network analyses, which compared drugs used to treat SARS-CoV-2 in humans, also predicted that melatonin would be the most effective agent for preventing/treating COVID-19. Finally, when seriously infected COVID-19 patients were treated with melatonin, either alone or in combination with other medications, these treatments reduced the severity of infection, lowered the death rate, and shortened the duration of hospitalization. Melatonin's ability to arrest SARS-CoV-2 infections may reduce health care exhaustion by limiting the need for hospitalization. Importantly, melatonin has a high safety profile over a wide range of doses and lacks significant toxicity. Some molecular processes by which melatonin resists a SARS-CoV-2 infection are summarized. The authors believe that all available, potentially beneficial drugs, including melatonin, that lack toxicity should be used in pandemics such as that caused by SARS-CoV-2.
Author contributions Before writing began, all co-authors discussed the publications related to this report. The final selection of papers to be covered in the report was done by RJR and RS. The initial draft of the paper was written by RJR and then reviewed by all co-authors. The suggestions of all co-authors were incorporated into the final version of the review by RJR. All co-authors read and approved the final version of the manuscript.
Declarations Conflict of interest The authors declare no conflicts of interest. Ethical approval Not applicable.
Consent to participate Not applicable. Consent for publication Not applicable.
Ethical approval Not applicable. Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http:// creat..
References
Al-Gburi, Beissert, Gunther, Molecular mechanisms of vaculopathy and coagulopathy in COVID-19, Biol Chem, doi:10.1515/hsz-2021=0245
Al-Zyoud, Haddad, Dynamics prediction of emerging notable spike protein mutations in SARS-CoV-2 implies a need for updated vaccines, Biochimie, doi:10.1016/j.biochi.2021.08.011
Alizadeh, Keyhanian, Ghaderkhani, Dashti-Khavidaki, Shoormasti et al., A Pilot Study on Controlling Coronavirus Disease 2019 (COVID-19) Inflammation Using Melatonin Supplement, Iran J Allergy Asthma Immunol
Alonazi, Farghaly, Mostafa, Al-Watban, Zindani et al., Brain MRI in SARS-CoV-2 pneumonia patients with newly developed neurological manifestations suggestive of brain involvement, Sci Rep, doi:10.1038/s41598-021-00064-5
Ambrus, Bakos, Sarkadi, Ozvegy-Laczka, Telbisz, Interactions of anti-COVID-19 drug candidates with hepatic transporters may cause liver toxicity and affect pharmacokinetics, Sci Rep, doi:10.1038/s41598-021-97160-3
Anderson, Carbone, Mazzoccoli, Aryl Hydrocarbon Receptor Role in Co-Ordinating SARS-CoV-2 Entry and Symptomatology: Linking Cytotoxicity Changes in COVID-19 and Cancers; Modulation by Racial Discrimination Stress, Biology, doi:10.3390/biology9090249
Anderson, Good, Gellad, Prevalence and compensation of academic leaders, professors, and trustees on publicly traded US healthcare company boards of directors: cross sectional study, BMJ, doi:10.1136/bmj.h4826
Angelo, Impellizzeri, Marseglia, Montalto, Russo et al., Current status of laboratory and imaging diagnosis of neonatal necrotizing enterocolitis, Ital J Pediatr, doi:10.1186/s13052-018-0528-3
Angelo, Marseglia, Reiter, Buonocore, Gitto, Melatonin and neonatal sepsis: a promising antioxidant adjuvant agent, Am J Perinatol, doi:10.1055/s-0037-1604244
Appiah, Park, Akama, Nakamori, Kawamoto et al., Cellular and exosomal regulations of sepsis-induced metabolic alterations, Int J Mol Sci, doi:10.3390/ijms22158295
Artigas, Coma, Matos-Filipe, Aguirre-Plans, Farres et al., In-silico drug repurposing study predicts the combination of pirfenidone and melatonin as a promising candidate therapy to reduce SARS-CoV-2 infection progression and respiratory distress caused by cytokine storm, PLoS ONE, doi:10.1371/journal.pone.0240149
Baj, Novazzi, Genoni, Ferrante, Taborelli et al., Symptomatic SARS-CoV-2 infections after full schedule BNT162b2 vaccination in seropositive healthcare workers: a case series from a single institution, Emerg Microbes Infect, doi:10.1080/22221751.2021.1942230
Baltatu, Amaral, Campos, Cipolla-Neto, Melatonin, mitochondria and hypertension, Cell Mol Life Sci, doi:10.1007/s00018-017-2613-y
Bar-Or, Carrick, Tanner A 2nd, Lieser, Rael et al., Overcoming the Warburg Effect: Is it the key to survival in sepsis?, J Crit Care, doi:10.1016/j.jcrc.2017.09.012
Bardenheier, Gravenstein, Blackman, Gutman, Sarkar et al., Adverse Events Following One Dose of mRNA COVID-19 Vaccination Among US Nursing Home Residents With and Without a Previous SARS-CoV-2 Infection, J Am Med Dir Assoc, doi:10.1016/j.jamda.2021.08.024
Becker, Relationships between academic medicine leaders and industry-time for another look, JAMA, doi:10.1001/jama.2020.21021
Bickler, Amplification of Snake Venom Toxicity by Endogenous Signaling Pathways, Toxins, doi:10.3390/toxins12020068
Boga, Coto-Montes, Rosales-Corral, Tan, Reiter, Beneficial actions of melatonin in the management of viral infections: a new use for this "molecular handyman, Rev Med Virol, doi:10.1002/rmv.1714
Camp, Bai, Gonullu, Nayak, Hm, Melatonin interferes with COVID-19 at several distinct ROSrelated steps, J Inorg Biochem, doi:10.1016/j.jinorgbio.2021.111546
Cardinali, Brown, Sr, An urgent proposal for the immediate use of melatonin as an adjuvant to anti-SARS-CoV-2 vaccination, Melatonin Res, doi:10.32794/mr11250091
Cardinali, Brown, Sr, Can Melatonin Be a Potential "Silver Bullet, doi:10.3390/diseases8040044
Cardinali, High doses of melatonin as a potential therapeutic tool for the neurologic sequels of covid-19 infection, Melatonin Res, doi:10.32794/mr11250064
Castillo, Quizon, Juco, Roman, De Leon et al., Melatonin as adjuvant treatment for coronavirus disease 2019 pneumonia patients requiring hospitalization (MAC-19 PRO): a case series, Melatonin Res, doi:10.32794/mr11250063
Castle, Williams, Bushell, Rindfleisch, Peterson et al., Implications for systemic approaches to COVID-19: effect sizes of remdesivir, tocilizumab, melatonin, vitamin D3, and meditation, J Inflamm Res, doi:10.2147/JIR.S323356
Chavarria, Vazquez, Cherit, Bello, Suastegui et al., Antioxidants and pentoxifylline as coadjuvant measures to standard therapy to improve prognosis of patients with pneumonia by COVID-19, Comput Struct Biotechnol J, doi:10.1016/j.csbj.2021.02.009
Chen, Hao, Li, Reiter, Bai et al., Melatonin inhibits lung cancer development by reversing the Warburg effect via stimulating the SIRT3/PDH axis, J Pineal Res, doi:10.1111/jpi.12755
Chen, Yang, Wang, Huang, Yu et al., Melatonin ameliorates cognitive deficits through improving mitophagy in a mouse model of Alzheimer's disease, J Pineal Res, doi:10.1111/jpi.12774
Codo, Davanzo, Monteiro, De Souza, Muraro et al., Elevated Glucose Levels Favor SARS-CoV-2 Infection and Monocyte Response through a HIF-1alpha/Glycolysis-Dependent Axis, Cell Metab, doi:10.1016/j.cmet.2020.07.007
Costa, Mohanapriya, Bharadwaj, Noceda, Thiers et al., ROS/RNS Balancing, Aerobic Fermentation Regulation and Cell Cycle Control-a Complex Early Trait ('CoV-MAC-TED') for Combating SARS-CoV-2-Induced Cell Reprogramming, Front Immunol, doi:10.3389/fimmu.2021.673692
Cross, Landis, Sehgal, Payne, Melatonin for the early treatment of COVID-19: a narrative review of current evidence and possible efficacy, Endocr Pract, doi:10.1016/j.eprac.2021.06.001
De Araujo, De Almeida, Bretones, Cirillo, Curi et al., Crotoxin promotes macrophage reprogramming towards an antiangiogenic phenotype, Sci Rep, doi:10.1038/s41598-019-40903-0
De Jong, Guryev, Moshkin, Estimates of gene ensemble noise highlight critical pathways and predict disease severity in H1N1, COVID-19 and mortality in sepsis patients, Sci Rep, doi:10.1038/s41598-021-90192-9
Dyer, Shkreli Awards" go to pandemic's top profiteers, BMJ, doi:10.1136/bmj.n16
Ellis, Melatonin reduces mortality from Aleutian disease in mink (Mustela vison), J Pineal Res, doi:10.1111/j.1600-079x.1996.tb00288.x
Elrashdy, Tambuwala, Hassan, Adadi, Seyran et al., Autoimmunity roots of the thrombotic events after COVID-19 vaccination, Autoimmun Rev, doi:10.1016/j.autrev.2021.102941
Estaras, Gonzalez-Portillo, Fernandez-Bermejo, Mateos, Vara et al., Melatonin Induces Apoptosis and Modulates Cyclin Expression and MAPK Phosphorylation in Pancreatic Stellate Cells Subjected to Hypoxia, Int J Mol Sci, doi:10.3390/ijms22115555
Farnoosh, Akbariqomi, Badri, Bagheri, Izadi et al., Efficacy of a Low Dose of Melatonin as an Adjunctive Therapy in Hospitalized Patients with COVID-19: A Randomized, Double-blind Clinical Trial, Arch Med Res, doi:10.1016/j.arcmed.2021.06.006
Feitosa, Neto, Matos, Moura, Rosales et al., COVID-19: Rational discovery of the therapeutic potential of Melatonin as a SARS-CoV-2 main Protease Inhibitor, Int J Med Sci, doi:10.7150/ijms.48053
Gimenez, De Las, Ferder, Lahera, Reiter et al., Potential Effects of Melatonin and Micronutrients on Mitochondrial Dysfunction during a Cytokine Storm Typical of Oxidative/Inflammatory Diseases, Diseases, doi:10.3390/diseases9020030
Gimenez, Prado, Diez, Manucha, Reiter, New proposal involving nanoformulated melatonin targeted to the mitochondria as a potential COVID-19 treatment, Nanomedicine (Lond), doi:10.2217/nnm-2020-0371
Gitto, Karbownik, Reiter, Tan, Cuzzocrea et al., Effects of melatonin treatment in septic newborns, Pediatr Res, doi:10.1203/00006450-200112000-00021
Gouvarchin Ghaleh, Hosseini, Aghamollaei, Fasihi-Ramandi, Alishiri et al., NLRP3 inflammasome activation and oxidative stress status in the mild and moderate SARS-CoV-2 infected patients: impact of melatonin as a medicinal supplement, Z Naturforsch C J Biosci, doi:10.1515/znc-2021-0101
Gurunathan, Kang, Choi, Reiter, Kim, Melatonin: a potential therapeutic agent against COVID-19, Melatonin Res, doi:10.32794/mr11250081
Hardeland, Aging, Melatonin, and the Pro-and Anti-Inflammatory Networks, Int J Mol Sci, doi:10.3390/ijms20051223
Hardeland, Melatonin and Microglia, Int J Mol Sci, doi:10.3390/ijms22158296
Hasan, Atrakji, Mehuaiden, The Effect of Melatonin on Thrombosis, Sepsis and Mortality Rate in COVID-19, doi:10.1016/j.ijid.2021.10.012
Hasnie, Hasnie, Patel, Aziz, Xie et al., Perimyocarditis following first dose of the mRNA-1273 SARS-CoV-2 (Moderna) vaccine in a healthy young male: a case report, BMC Cardiovasc Disord, doi:10.1186/s12872-021-02183-3
He, Wu, Zhang, Li, Ye et al., Bacteriostatic potential of melatonin: therapeutic standing and mechanistic insights, Front Immunol, doi:10.3389/fimmu.2021.683879
He, Zhou, Lu, Mao, Xi et al., Melatonin antagonizes nickel-induced aerobic glycolysis by blocking ROS-mediated HIF-1alpha/miR210/ISCU axis activation, Oxid Med Cell Longev, doi:10.1155/2020/5406284
Hosseini, Gouvarchin Ghaleh, Aghamollaei, Ramandi, Alishiri et al., Evaluation of Th1 and Th2 mediated cellular and humoral immunity in patients with COVID-19 following the use of melatonin as an adjunctive treatment, Eur J Pharmacol, doi:10.1016/j.ejphar.2021.174193
Jaworek, Szepietowski, Halubiec, Wojas-Pelc, Jaworek, Melatonin as an antioxidant and immunomodulator in atopic dermatitis-a new look on an old story: a review, Antioxidants, doi:10.3390/antiox10081179
Juybari, Pourhanifeh, Hosseinzadeh, Hemati, Mehrzadi, Melatonin potentials against viral infections including COVID-19: Current evidence and new findings, Virus Res, doi:10.1016/j.virusres.2020.198108
Katkar, Sundaram, Hemshekhar, Sharma, Santhosh et al., Melatonin alleviates Echis carinatus venom-induced toxicities by modulating inflammatory mediators and oxidative stress, J Pineal Res, doi:10.1111/jpi.12123
Khan, Gupta, Singh, Kaur, Mechanistic insight on the role of leukotriene receptors in ischemic-reperfusion injury, Pharmacol Rep, doi:10.1007/s43440-021-00258-8
Kleszczynski, Slominski, Steinbrink, Reiter, Clinical Trials for Use of Melatonin to Fight against COVID-19, doi:10.3390/nu12092561
Kulkarni, Nadler, Mirmira, Casimiuro, Regulation of tissue inflammation by 12-lipoxygenase, Biomolcules, doi:10.3390/biom11050717
Lee, Glickman, Sleep, Circadian Health and Melatonin for Mitigating COVID-19 and Optimizing Vaccine Efficacy, Front Neurosci, doi:10.3389/fnins.2021.711605
Lee, Tan, Tan, Snake venom proteomics and antivenomics of two Sundaic lance-headed pit vipers: Trimeresurus wiroti (Malaysia) and Trimeresurus puniceus
Letsiou, Htwe, Dudek, Secretory Phospholipase A2 Enzymes in Acute Lung Injury, Cell Biochem Biophys, doi:10.1007/s12013-021-01003-x
Li, Hao, Zhang, Reiter, Lin et al., Melatonin enhances radiofrequency-induced NK antitumor immunity, causing cancer metabolism reprogramming and inhibition of multiple pulmonary tumor development, Signal Transduct Target Ther, doi:10.1038/s41392-021-00745-7
Li, Lv, Yao, Wu, Wang et al., Overexpression of ASMT likely enhances the resistance of transgenic sheep to brucellosis by influencing immune-related signaling pathways and gut microbiota, FASEB J, doi:10.1096/fj.202100651R
Lien, Lee, Weng, Lin, Liu et al., Repurposing colchicine in treating patients with COVID-19: a systematic review and meta-analysis, doi:10.3390/life11080864
Lu, Lu, Lu, Tang, Su et al., The potential remedy of melatonin on osteoarthritis, J Pineal Res, doi:10.1111/jpi.12762
Luo, Li, Chen, Gou, Yan et al., Effects of lactate in immunosuppression and inflammation: progress and prospects, Int Rev Immunol, doi:10.1080/08830185.2021.1974856
Maestroni, Therapeutic potential of melatonin in immunodeficiency states, viral diseases, and cancer, Adv Exp Med Biol, doi:10.1007/978-1-4615-4709-9_28
Malani, Salunke, Kulkarni, Jain, Sheikh et al., Repurposing pharmaceutical excipients as an antiviral agent against SARS-CoV-2, J Biomater Sci Polym Ed
Mansouri, Kee, Garcia, Bradley, Role of systems science in preventing and controlling emerging infectious diseases: protocol for a scoping review, BMJ Open, doi:10.1136/bmjopen-2020-046057
Marino, Paola, Crisafulli, Mazzon, Morabito et al., Protective effect of melatonin against the inflammatory response elicited by crude venom from isolated nematocysts of Pelagia noctiluca (Cnidaria, Scyphozoa), J Pineal Res, doi:10.1111/j.1600-079X.2009.00688.x
Maroufi, Amiri, Dizaji, Vahedian, Akbarzadeh et al., Inhibitory effect of melatonin on hypoxia-induced vasculogenic mimicry via suppressing epithelial-mesenchymal transition (EMT) in breast cancer stem cells, Eur J Pharmacol, doi:10.1016/j.ejphar.2020.173282
Martorina, Tavares, Possible role of exogenous melatonin in preventing more serious COVID-19 infection in patients with type 2 diabetes mellitus, Rev Assoc Med Bras, doi:10.1590/1806-9282.67.Suppl1.20200968
Merad, Martin, Pathological inflammation in patients with COVID-19: a key role for monocytes and macrophages, Nat Rev Immunol, doi:10.1038/s41577-020-0331-4
Moneim, Ortiz, Mendonca, Vergano-Villodres, Guerrero-Martinez et al., Protective effects of melatonin against oxidative damage induced by Egyptian cobra (Naja haje) crude venom in rats, Acta Trop, doi:10.1016/j.actatropica.2014.12.007
Montiel, Bonilla, Valero, Mosquera, Espina et al., Melatonin decreases brain apoptosis, oxidative stress, and CD200 expression and increased survival rate in mice infected by Venezuelan equine encephalitis virus, Antivir Chem Chemother, doi:10.3390/v13040659
Mouffak, Shubbar, Saleh, El-Awady, Recent advances in management of COVID-19: a review, Biomed Pharmacother, doi:10.1016/j.biopha.2021.112107
Mousavi, Heydari, Mehravaran, Saeedi, Alizadeh-Navaei et al., Melatonin effects on sleep quality and outcomes of COVID-19 patients: An open-label, randomized, controlled trial, J Med Virol, doi:10.1002/jmv.27312
Natesan, Adrenergic blockade inhibits bacterial quorum sensing and reverses Warburg effect in septic shock, Br J Anaesth, doi:10.1016/j.bja.2017.12.010
Nordlund, Lerner, The effects of oral melatonin on skin color and on the release of pituitary hormones, J Clin Endocrinol Metab, doi:10.1210/jcem-45-4-768
Noroozneezhad, Mansouri, Endothelial cell dysfunction, coagulation, and angiogenesis in coronavirus disease 2019 (COVID-19), Microvasc Res, doi:10.1016/j.mvr.2021.104188
Oba, Altinay, Salkaya, Turk, Evaluation of the effect of clinical characteristics and intensive care treatment methods on the mortality of covid-19 patients aged 80 years and older, BMC Anesthesiol, doi:10.1186/s12871-021-01511-6
Pandi-Perumal, Cardinali, Reiter, Brown, Low melatonin as a contributor to SARS-CoV-2 disease, Melatonin Res, doi:10.32794/mr11250079
Patel, Louis, Atalay, Agarwal, Shah, Cardiovascular magnetic resonance findings in young adult patients with acute myocarditis following mRNA COVID-19 vaccination: a case series, J Cardiovasc Magn Reson, doi:10.1186/s12968-021-00795-4
Peng, Du, Diamond, HIF-1alpha is a negative regulator of interferon regulatory factors: implications for interferon production by hypoxic monocytes, Proc Natl Acad Sci, doi:10.1073/pnas.2106017118
Perez-Gonzalez, Castaneda-Arriaga, Alvarez-Idaboy, Reiter, Galano, Melatonin and its metabolites as chemical agents capable of directly repairing oxidized DNA, J Pineal Res, doi:10.1111/jpi.12539
Peschechera, Veronesi, Injectable melatonin: an anticancer and anti-viral treatment option, Melatonin Res, doi:10.32794/mr11250049
Prauchner, Oxidative stress in sepsis: pathophysiological implications justifying antioxidant co-therapy, Burns, doi:10.1016/j.burns.2016.09.023
Ramlall, Zucker, Tatonetti, Melatonin is significantly associated with survival of intubated COVID-19 patients, doi:10.1101/2020.10.15.20213546
Ramos, Lopez-Munoz, Gil-Martin, Egea, Alvarez-Merz et al., The coronavirus disease 2019 (COVID-19): key emphasis on melatonin safety and therapeutic efficacy, Antioxidants, doi:10.3390/antiox10071152
Reiter, Ma, Sharma, Melatonin in mitochondria: mitigating clear and present dangers, Physiology (Bethesda), doi:10.1152/physiol.00034.2019
Reiter, Ma, Sharma, Treatment of ebola and other infectious diseases: melatonin "goes viral, Melatonin Res, doi:10.32794/mr11250047
Reiter, Mayo, Tan, Sainz, Jimenez et al., Melatonin as an antioxidant: under promises but over delivers, J Pineal Res, doi:10.1111/jpi.12360
Reiter, Sharma, Ma, Rorsales-Corral, De et al., Melatonin inhibits Warburg-dependent cancer by redirecting glucose oxidation to the mitochondria: a mechanistic hypothesis, Cell Mol Life Sci, doi:10.1007/s00018-019-03438-1
Reiter, Sharma, Ma, Rosales-Corral, Acuna-Castroviejo et al., Inhibition of mitochondrial pyruvate dehydrogenase kinase: a proposed mechanism by which melatonin causes cancer cells to overcome cytosolic glycolysis, reduce tumor biomass and reverse insensitivity to chemotherapy, Melatonin Res, doi:10.32794/mr11250033
Reiter, Sharma, Rosales-Corral, Anti-warburg effect of melatonin: a proposed mechanism to explain its inhibition of multiple diseases, Int J Mol Sci, doi:10.3390/ijms22020764
Ristic-Medic, Petrovic, Arsic, Vucic, Liver disease and COVID-19: the link with oxidative stress, antioxidants and nutrition, World J Gastroenterol, doi:10.3748/wjg.v27.i34.5682
Rochette, Ghibu, Mechanics insights of alpha-lipoic acid against cardiovascular diseases during COVID-19 infection, Int J Mol Sci, doi:10.3390/ijms22157979
Root-Bernstein, Innate Receptor Activation Patterns Involving TLR and NLR Synergisms in COVID-19, ALI/ARDS and Sepsis Cytokine Storms: A Review and Model Making Novel Predictions and Therapeutic Suggestions, Int J Mol Sci, doi:10.3390/ijms22042108
Sack, Lewy, Erb, Vollmer, Singer, Human melatonin production decreases with age, J Pineal Res, doi:10.1111/j.1600-079x.1986.tb00760.x
Schmoch, Uhle, Siegler, Fleming, Morgenstern et al., The glyoxalase system and methylglyoxal-derived carbonyl stress in sepsis: glycotoxic aspects of sepsis pathophysiology, Int J Mol Sci, doi:10.3390/ijms18030657
Scholtens, Van Munster, Van Kempen, De Rooij, Physiological melatonin levels in healthy older people: a systematic review, J Psychosom Res, doi:10.1016/j.jpsychores.2016.05.005
Science, Bolotin, Silverman, Nadarajah, Maguire et al., SARS-CoV-2 antibodies in Ontario health care workers during and after the first wave of the pandemic: a cohort study, CMAJ Open, doi:10.9778/cmajo.20210044
Shavit, Maoz-Segal, Iancovici-Kidon, Offengenden, Yahia et al., Prevalence of Allergic Reactions After Pfizer-BioNTech COVID-19 Vaccination Among Adults With High Allergy Risk, JAMA Netw Open, doi:10.1001/jamanetworkopen.2021.22255
Simko, Reiter, Is melatonin deficiency a unifying pathomechanism of high risk patients with COVID-19?, Life Sci, doi:10.1016/j.lfs.2020.117902
Snider, You, Wang, Snider, Hallmark et al., Group IIA secreted phospholipase A2 is associated with the pathobiology leading to COVID-19 mortality, J Clin Invest, doi:10.1172/JCI149236
Srinivasan, Mohamed, Kato, Melatonin in bacterial and viral infections with focus on sepsis: a review, Recent Pat Endocr Metab Immune Drug Discov, doi:10.2174/187221412799015317
Srivastava, Singh, Drug repurposing in COVID-19: a review with past, present and future, Metabol Open, doi:10.1016/j.metop.2021.100121
Suofu, Li, Fg, Jia, Khattar et al., Dual role of mitochondria in producing melatonin and driving GPCR signaling to block cytochrome c release, Proc Natl Acad Sci, doi:10.1073/pnas.1705768114
Swain, Romano, Miryala, Tsai, Parikh et al., SARS-CoV-2 neuronal invasion and complications: potential mechanisms and therapeutic approaches, J Neurosci, doi:10.1523/JNEUROSCI.3188-20.2021
Takahashi, Luzum, Nicol, Jacobson, Pharmacogenomics of COVID-19 therapies, NPJ Genom Med, doi:10.1038/s41525-020-00143-y
Tan, Goh, The role of group IIA secretory phospholipase A2 (sPLA2-IIA) as a biomarker for the diagnosis of sepsis and bacterial infection in adults-A systematic review, PLoS ONE, doi:10.1371/journal.pone.0180554
Tan, Hardeland, Estimated doses of melatonin for treating deadly virus infections: focus on COVID-19, Melatonin Res, doi:10.32794/mr11250062
Tan, Hardeland, Targeting Host Defense System and Rescuing Compromised Mitochondria to Increase Tolerance against Pathogens by Melatonin May Impact Outcome of Deadly Virus Infection Pertinent to COVID-19, Molecules, doi:10.3390/molecules25194410
Tan, Korkmaz, Reiter, Manchester, Ebola virus disease: potential use of melatonin as a treatment, J Pineal Res, doi:10.1111/jpi.12186
Targhetta, Amaral, Camara, Through DNA sensors and hidden mitochondrial effects of SARS-CoV-2, J Venom Anim Toxins Incl Trop Dis, doi:10.1590/1678-9199-JVATITD-2020-0183
Tekbas, Ogur, Korkmaz, Kilic, Reiter, Melatonin as an antibiotic: new insights into the actions of this ubiquitous molecule, J Pineal Res, doi:10.1111/j.1600-079X.2007.00516.x
Tesarik, Melatonin attenuates growth factor receptor signaling required for SARS-CoV-2 replication, Melatonin Res, doi:10.32794/mr11250077
Tian, Liu, Li, Zhao, Shereen et al., HIF-1alpha promotes SARS-CoV-2 infection and aggravates inflammatory responses to COVID-19, Signal Transduct Target Ther, doi:10.1038/s41392-021-00726-w
Tiwari, Kumar, Tiwari, Sahoo, Singh et al., Current trends in diagnosis and treatment strategies of COVID-19 infection, Environ Sci Pollut Res Int, doi:10.1007/s11356-021-16715-z
Trostchansky, Wood, Rubbo, Regulation of arachidonic acid oxidation and metabolism by lipid electrophiles, Prostaglandins Other Lipid Mediat, doi:10.1016/j.prostaglandins.2020.106482
Vaamonde-Garcia, Lopez-Armada, Role of mitochondrial dysfunction on rheumatic diseases, Biochem Pharmacol, doi:10.1016/j.bcp.2019.03.008
Van Hensbergen, Wu, Van Sorge, Touqui, Type IIA Secreted Phospholipase A2 in Host Defense against Bacterial Infections, Trends Immunol, doi:10.1016/j.it.2020.02.003
Vaughan, Human melatonin in physiologic and diseased states: neural control of the rhythm, J Neural Transm Suppl
Vielma, Bonilla, Chacin-Bonilla, Mora, Medina-Leendertz et al., Effects of melatonin on oxidative stress, and resistance to bacterial, parasitic, and viral infections: a review, Acta Trop, doi:10.1016/j.actatropica.2014.04.021
Vriend, Reiter, Melatonin and the von Hippel-Lindau/ HIF-1 oxygen sensing mechanism: a review, Biochim Biophys Acta, doi:10.1016/j.bbcan.2016.02.004
Wang, Wang, Cao, Wu, Yuan et al., Regulatory T cells in COVID-19, Aging Dis, doi:10.14336/AD.2021.0709
Ward, Gortz, Ernst, Andersen, Kjaer et al., The effect of immunosuppressants on the prognosis of SARS-CoV-2 infection, Eur Respir J, doi:10.1183/13993003.00769-2021
Warren, Snow, Lee, Shah, Heider et al., Assessment of Allergic and Anaphylactic Reactions to mRNA COVID-19 Vaccines With Confirmatory Testing in a US Regional Health System, JAMA Netw Open, doi:10.1001/jamanetworkopen.2021.25524
Wichniak, Kania, Sieminski, Cubala, Melatonin as a potential adjuvant treatment for COVID-19 beyond sleep disorders, Int J Mol Sci, doi:10.3390/ijms22168623
Wongchitrat, Shukla, Sharma, Govitrapong, Reiter, Role of Melatonin on Virus-Induced Neuropathogenesis-A Concomitant Therapeutic Strategy to Understand SARS-CoV-2 Infection, Antioxidants, doi:10.3390/antiox10010047
Xia, Chen, Zeng, Zhao, Zhu et al., Melatonin in macrophage biology: current understanding and future perspectives, J Pineal Res, doi:10.1111/jpi.12547
Xia, Liang, Wang, Chen, Huang et al., Melatonin modulates TLR4-mediated inflammatory genes through MyD88-and TRIF-dependent signaling pathways in lipopolysaccharidestimulated RAW2647 cells, J Pineal Res, doi:10.1111/j.1600-079X.2012.01002.x
Xu, Lin, Bais, Reynolds, Tan et al., Mitochondrial respiration defects in single-ventricle congenital heart disease, Front Cardiovasc Med, doi:10.3389/fcvm.2021.734388
Yang, Wang, Liu, Cao, Pan et al., Targeting the complex I and III of mitochondrial electron transport chain as a potentially viable option in liver cancer management, Cell Death Discovery, doi:10.1038/s41420-021-00675-x
Yang, Wei, Chang, Chang, Tsai et al., Remdesivir use in the coronavirus disease 2019 pandemic: a mini-review, J Microbiol Immunol Infect, doi:10.1016/j.jmii.2020.09.002
Yavuz, Kaya, Behcet, Ozturk, Yavuz, Effects of melatonin on Candida sepsis in an experimental rat model, Adv Ther, doi:10.1007/BF02849996
Yin, Liu, Liu, Ma, Sun et al., Metformin inhibits epithelial-mesenchymal transition of oral squamous cell carcinoma via the mTOR/HIF-1alpha/PKM2/STAT3 pathway, Oncol Lett, doi:10.3892/ol.2020.12292
Younis, Zareef, Fakhri, Bitar, Eid et al., COVID-19: potential therapeutics for pediatric patients, Pharmacol Rep, doi:10.1007/s43440-021-00316-1
Zhai, Wang, Jiao, Zhang, Li et al., Melatonin and other indoles show antiviral activities against swine coronaviruses in vitro at pharmacological concentrations, J Pineal Res, doi:10.1111/jpi.12754
Zhang, Tang, Huang, Zhou, Cui et al., Metabolic regulation of gene expression by histone lactylation, Nature, doi:10.1038/s41586-019-1678-1
Zhang, Wang, Ni, Di, Ma et al., COVID-19: Melatonin as a potential adjuvant treatment, Life Sci, doi:10.1016/j.lfs.2020.117583
Zhao, Sun, Du, Li, Lv et al., Venom of the annulated sea snake Hydrophis cyanocinctus: a biochemically simple but genetically complex weapon, Toxins, doi:10.3390/toxins13080548
Zhou, Hou, Shen, Mehra, Kallianpur et al., A network medicine approach to investigation and populationbased validation of disease manifestations and drug repurposing for COVID-19, PLoS Biol, doi:10.1371/journal.pbio.3000970
Zhu, Wu, Huang, Zhang, Son et al., Uncoupling of macrophage inflammation from self-renewal modulates host recovery from respiratory viral infection, Immunity, doi:10.1016/j.immuni.2021.04.001
Zonta, Martinez, Camargo, Domeniconi, Junior et al., Melatonin Reduces Angiogenesis in Serous Papillary Ovarian Carcinoma of Ethanol-Preferring Rats, Int J Mol Sci, doi:10.3390/ijms18040763
DOI record:
{
"DOI": "10.1007/s00018-021-04102-3",
"ISSN": [
"1420-682X",
"1420-9071"
],
"URL": "http://dx.doi.org/10.1007/s00018-021-04102-3",
"abstract": "<jats:title>Abstract</jats:title><jats:p>Numerous pharmaceutical drugs have been repurposed for use as treatments for COVID-19 disease. These drugs have not consistently demonstrated high efficacy in preventing or treating this serious condition and all have side effects to differing degrees. We encourage the continued consideration of the use of the antioxidant and anti-inflammatory agent, melatonin, as a countermeasure to a SARS-CoV-2 infection. More than 140 scientific publications have identified melatonin as a likely useful agent to treat this disease. Moreover, the publications cited provide the rationale for the use of melatonin as a prophylactic agent against this condition. Melatonin has pan-antiviral effects and it diminishes the severity of viral infections and reduces the death of animals infected with numerous different viruses, including three different coronaviruses. Network analyses, which compared drugs used to treat SARS-CoV-2 in humans, also predicted that melatonin would be the most effective agent for preventing/treating COVID-19. Finally, when seriously infected COVID-19 patients were treated with melatonin, either alone or in combination with other medications, these treatments reduced the severity of infection, lowered the death rate, and shortened the duration of hospitalization. Melatonin’s ability to arrest SARS-CoV-2 infections may reduce health care exhaustion by limiting the need for hospitalization. Importantly, melatonin has a high safety profile over a wide range of doses and lacks significant toxicity. Some molecular processes by which melatonin resists a SARS-CoV-2 infection are summarized. The authors believe that all available, potentially beneficial drugs, including melatonin, that lack toxicity should be used in pandemics such as that caused by SARS-CoV-2.</jats:p>",
"alternative-id": [
"4102"
],
"article-number": "143",
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "19 October 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Revised",
"name": "revised",
"order": 2,
"value": "29 November 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 3,
"value": "16 December 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 4,
"value": "20 February 2022"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Conflict of interest",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "The authors declare no conflicts of interest."
},
{
"group": {
"label": "Ethical approval",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "Not applicable."
},
{
"group": {
"label": "Consent to participate",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 4,
"value": "Not applicable."
},
{
"group": {
"label": "Consent for publication",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 5,
"value": "Not applicable."
},
{
"group": {
"label": "Ethical approval",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 6,
"value": "Not applicable."
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0001-6763-4225",
"affiliation": [],
"authenticated-orcid": false,
"family": "Reiter",
"given": "Russel J.",
"sequence": "first"
},
{
"affiliation": [],
"family": "Sharma",
"given": "Ramaswamy",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Simko",
"given": "Fedor",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Dominguez-Rodriguez",
"given": "Alberto",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Tesarik",
"given": "Jan",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Neel",
"given": "Richard L.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Slominski",
"given": "Andrzej T.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kleszczynski",
"given": "Konrad",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Martin-Gimenez",
"given": "Verna M.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Manucha",
"given": "Walter",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Cardinali",
"given": "Daniel P.",
"sequence": "additional"
}
],
"container-title": [
"Cellular and Molecular Life Sciences"
],
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2022,
2,
20
]
],
"date-time": "2022-02-20T19:02:23Z",
"timestamp": 1645383743000
},
"deposited": {
"date-parts": [
[
2022,
2,
20
]
],
"date-time": "2022-02-20T19:11:14Z",
"timestamp": 1645384274000
},
"indexed": {
"date-parts": [
[
2022,
4,
13
]
],
"date-time": "2022-04-13T06:14:39Z",
"timestamp": 1649830479452
},
"is-referenced-by-count": 2,
"issn-type": [
{
"type": "print",
"value": "1420-682X"
},
{
"type": "electronic",
"value": "1420-9071"
}
],
"issue": "3",
"issued": {
"date-parts": [
[
2022,
2,
20
]
]
},
"journal-issue": {
"issue": "3",
"published-print": {
"date-parts": [
[
2022,
3
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
2,
20
]
],
"date-time": "2022-02-20T00:00:00Z",
"timestamp": 1645315200000
}
},
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
2,
20
]
],
"date-time": "2022-02-20T00:00:00Z",
"timestamp": 1645315200000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1007/s00018-021-04102-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1007/s00018-021-04102-3/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1007/s00018-021-04102-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1007",
"published": {
"date-parts": [
[
2022,
2,
20
]
]
},
"published-online": {
"date-parts": [
[
2022,
2,
20
]
]
},
"published-print": {
"date-parts": [
[
2022,
3
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.32794/mr11250064",
"author": "DP Cardinali",
"doi-asserted-by": "publisher",
"first-page": "311",
"issue": "3",
"journal-title": "Melatonin Res",
"key": "4102_CR1",
"unstructured": "Cardinali DP (2020) High doses of melatonin as a potential therapeutic tool for the neurologic sequels of covid-19 infection. Melatonin Res 3(3):311–317. https://doi.org/10.32794/mr11250064",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.3390/diseases8040044",
"author": "DP Cardinali",
"doi-asserted-by": "publisher",
"journal-title": "Diseases",
"key": "4102_CR2",
"unstructured": "Cardinali DP, Brown GM, Pandi-Perumal SR (2020) Can Melatonin Be a Potential “Silver Bullet” in Treating COVID-19 Patients? Diseases. https://doi.org/10.3390/diseases8040044",
"year": "2020"
},
{
"DOI": "10.2217/nnm-2020-0371",
"author": "VM Martin Gimenez",
"doi-asserted-by": "publisher",
"first-page": "2819",
"issue": "29",
"journal-title": "Nanomedicine (Lond)",
"key": "4102_CR3",
"unstructured": "Martin Gimenez VM, Prado N, Diez E, Manucha W, Reiter RJ (2020) New proposal involving nanoformulated melatonin targeted to the mitochondria as a potential COVID-19 treatment. Nanomedicine (Lond) 15(29):2819–2821. https://doi.org/10.2217/nnm-2020-0371",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1101/2020.10.15.20213546",
"author": "V Ramlall",
"doi-asserted-by": "publisher",
"journal-title": "medRxiv",
"key": "4102_CR4",
"unstructured": "Ramlall V, Zucker J, Tatonetti N (2020) Melatonin is significantly associated with survival of intubated COVID-19 patients. medRxiv. https://doi.org/10.1101/2020.10.15.20213546",
"year": "2020"
},
{
"DOI": "10.32794/mr11250077",
"author": "J Tesarik",
"doi-asserted-by": "publisher",
"first-page": "534",
"issue": "4",
"journal-title": "Melatonin Res",
"key": "4102_CR5",
"unstructured": "Tesarik J (2020) Melatonin attenuates growth factor receptor signaling required for SARS-CoV-2 replication. Melatonin Res 3(4):534–537. https://doi.org/10.32794/mr11250077",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.32794/mr11250062",
"author": "D-X Tan",
"doi-asserted-by": "publisher",
"first-page": "276",
"issue": "3",
"journal-title": "Melatonin Res",
"key": "4102_CR6",
"unstructured": "Tan D-X, Hardeland R (2020) Estimated doses of melatonin for treating deadly virus infections: focus on COVID-19. Melatonin Res 3(3):276–296. https://doi.org/10.32794/mr11250062",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1016/j.lfs.2020.117583",
"author": "R Zhang",
"doi-asserted-by": "publisher",
"first-page": "117583",
"journal-title": "Life Sci",
"key": "4102_CR7",
"unstructured": "Zhang R, Wang X, Ni L, Di X, Ma B, Niu S, Liu C, Reiter RJ (2020) COVID-19: Melatonin as a potential adjuvant treatment. Life Sci 250:117583. https://doi.org/10.1016/j.lfs.2020.117583",
"volume": "250",
"year": "2020"
},
{
"DOI": "10.1016/j.jinorgbio.2021.111546",
"author": "OG Camp",
"doi-asserted-by": "publisher",
"first-page": "111546",
"journal-title": "J Inorg Biochem",
"key": "4102_CR8",
"unstructured": "Camp OG, Bai D, Gonullu DC, Nayak N, Abu-Soud HM (2021) Melatonin interferes with COVID-19 at several distinct ROS-related steps. J Inorg Biochem 223:111546. https://doi.org/10.1016/j.jinorgbio.2021.111546",
"volume": "223",
"year": "2021"
},
{
"DOI": "10.1016/j.eprac.2021.06.001",
"author": "KM Cross",
"doi-asserted-by": "publisher",
"first-page": "850",
"issue": "8",
"journal-title": "Endocr Pract",
"key": "4102_CR9",
"unstructured": "Cross KM, Landis DM, Sehgal L, Payne JD (2021) Melatonin for the early treatment of COVID-19: a narrative review of current evidence and possible efficacy. Endocr Pract 27(8):850–855. https://doi.org/10.1016/j.eprac.2021.06.001",
"volume": "27",
"year": "2021"
},
{
"DOI": "10.1515/znc-2021-0101",
"author": "H Esmaeili Gouvarchin Ghaleh",
"doi-asserted-by": "publisher",
"journal-title": "Z Naturforsch C J Biosci",
"key": "4102_CR10",
"unstructured": "Esmaeili Gouvarchin Ghaleh H, Hosseini A, Aghamollaei H, Fasihi-Ramandi M, Alishiri G, Saeedi-Boroujeni A, Hassanpour K, Mahmoudian-Sani MR, Farnoosh G (2021) NLRP3 inflammasome activation and oxidative stress status in the mild and moderate SARS-CoV-2 infected patients: impact of melatonin as a medicinal supplement. Z Naturforsch C J Biosci. https://doi.org/10.1515/znc-2021-0101",
"year": "2021"
},
{
"DOI": "10.1371/journal.pbio.3000970",
"author": "Y Zhou",
"doi-asserted-by": "publisher",
"first-page": "e3000970",
"issue": "11",
"journal-title": "PLoS Biol",
"key": "4102_CR11",
"unstructured": "Zhou Y, Hou Y, Shen J, Mehra R, Kallianpur A, Culver DA, Gack MU, Farha S, Zein J, Comhair S, Fiocchi C, Stappenbeck T, Chan T, Eng C, Jung JU, Jehi L, Erzurum S, Cheng F (2020) A network medicine approach to investigation and population-based validation of disease manifestations and drug repurposing for COVID-19. PLoS Biol 18(11):e3000970. https://doi.org/10.1371/journal.pbio.3000970",
"volume": "18",
"year": "2020"
},
{
"DOI": "10.3390/ijms22042108",
"doi-asserted-by": "publisher",
"key": "4102_CR12",
"unstructured": "Root-Bernstein R (2021) Innate Receptor Activation Patterns Involving TLR and NLR Synergisms in COVID-19, ALI/ARDS and Sepsis Cytokine Storms: A Review and Model Making Novel Predictions and Therapeutic Suggestions. Int J Mol Sci https://doi.org/10.3390/ijms22042108"
},
{
"DOI": "10.1016/j.lfs.2020.117902",
"author": "F Simko",
"doi-asserted-by": "publisher",
"first-page": "117902",
"journal-title": "Life Sci",
"key": "4102_CR13",
"unstructured": "Simko F, Reiter RJ (2020) Is melatonin deficiency a unifying pathomechanism of high risk patients with COVID-19? Life Sci 256:117902. https://doi.org/10.1016/j.lfs.2020.117902",
"volume": "256",
"year": "2020"
},
{
"DOI": "10.1016/j.biopha.2021.112107",
"author": "S Mouffak",
"doi-asserted-by": "publisher",
"first-page": "112107",
"journal-title": "Biomed Pharmacother",
"key": "4102_CR14",
"unstructured": "Mouffak S, Shubbar Q, Saleh E, El-Awady R (2021) Recent advances in management of COVID-19: a review. Biomed Pharmacother 143:112107. https://doi.org/10.1016/j.biopha.2021.112107",
"volume": "143",
"year": "2021"
},
{
"DOI": "10.3390/ijms22168623",
"author": "A Wichniak",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR15",
"unstructured": "Wichniak A, Kania A, Sieminski M, Cubala WJ (2021) Melatonin as a potential adjuvant treatment for COVID-19 beyond sleep disorders. Int J Mol Sci. https://doi.org/10.3390/ijms22168623",
"year": "2021"
},
{
"DOI": "10.3390/antiox10071152",
"author": "E Ramos",
"doi-asserted-by": "publisher",
"journal-title": "Antioxidants (Basel)",
"key": "4102_CR16",
"unstructured": "Ramos E, Lopez-Munoz F, Gil-Martin E, Egea J, Alvarez-Merz I, Painuli S, Semwal P, Martins N, Hernandez-Guijo JM, Romero A (2021) The coronavirus disease 2019 (COVID-19): key emphasis on melatonin safety and therapeutic efficacy. Antioxidants (Basel). https://doi.org/10.3390/antiox10071152",
"year": "2021"
},
{
"DOI": "10.1002/rmv.1714",
"author": "JA Boga",
"doi-asserted-by": "publisher",
"first-page": "323",
"issue": "5",
"journal-title": "Rev Med Virol",
"key": "4102_CR17",
"unstructured": "Boga JA, Coto-Montes A, Rosales-Corral SA, Tan DX, Reiter RJ (2012) Beneficial actions of melatonin in the management of viral infections: a new use for this “molecular handyman”? Rev Med Virol 22(5):323–338. https://doi.org/10.1002/rmv.1714",
"volume": "22",
"year": "2012"
},
{
"DOI": "10.1016/j.virusres.2020.198108",
"author": "K Bahrampour Juybari",
"doi-asserted-by": "publisher",
"first-page": "198108",
"journal-title": "Virus Res",
"key": "4102_CR18",
"unstructured": "Bahrampour Juybari K, Pourhanifeh MH, Hosseinzadeh A, Hemati K, Mehrzadi S (2020) Melatonin potentials against viral infections including COVID-19: Current evidence and new findings. Virus Res 287:198108. https://doi.org/10.1016/j.virusres.2020.198108",
"volume": "287",
"year": "2020"
},
{
"DOI": "10.3390/life11080864",
"author": "CH Lien",
"doi-asserted-by": "publisher",
"journal-title": "Life (Basel)",
"key": "4102_CR19",
"unstructured": "Lien CH, Lee MD, Weng SL, Lin CH, Liu LY, Tai YL, Lei WT, Liu JM, Huang YN, Chi H, Chiu NC, Lin CY (2021) Repurposing colchicine in treating patients with COVID-19: a systematic review and meta-analysis. Life (Basel). https://doi.org/10.3390/life11080864",
"year": "2021"
},
{
"DOI": "10.1183/13993003.00769-2021",
"author": "D Ward",
"doi-asserted-by": "publisher",
"journal-title": "Eur Respir J",
"key": "4102_CR20",
"unstructured": "Ward D, Gortz S, Ernst MT, Andersen NN, Kjaer SK, Hallas J, Christensen S, Christiansen CF, Israelsen SB, Benfield T, Pottegard A, Jess T (2021) The effect of immunosuppressants on the prognosis of SARS-CoV-2 infection. Eur Respir J. https://doi.org/10.1183/13993003.00769-2021",
"year": "2021"
},
{
"DOI": "10.1007/s43440-021-00316-1",
"author": "NK Younis",
"doi-asserted-by": "publisher",
"journal-title": "Pharmacol Rep",
"key": "4102_CR21",
"unstructured": "Younis NK, Zareef RO, Fakhri G, Bitar F, Eid AH, Arabi M (2021) COVID-19: potential therapeutics for pediatric patients. Pharmacol Rep. https://doi.org/10.1007/s43440-021-00316-1",
"year": "2021"
},
{
"DOI": "10.1038/s41598-021-97160-3",
"author": "C Ambrus",
"doi-asserted-by": "publisher",
"first-page": "17810",
"issue": "1",
"journal-title": "Sci Rep",
"key": "4102_CR22",
"unstructured": "Ambrus C, Bakos E, Sarkadi B, Ozvegy-Laczka C, Telbisz A (2021) Interactions of anti-COVID-19 drug candidates with hepatic transporters may cause liver toxicity and affect pharmacokinetics. Sci Rep 11(1):17810. https://doi.org/10.1038/s41598-021-97160-3",
"volume": "11",
"year": "2021"
},
{
"author": "M Malani",
"first-page": "1975020",
"issue": "1080/09205063",
"journal-title": "J Biomater Sci Polym Ed",
"key": "4102_CR23",
"unstructured": "Malani M, Salunke P, Kulkarni S, Jain GK, Sheikh A, Kesharwani P (2021) Nirmal J (2021) Repurposing pharmaceutical excipients as an antiviral agent against SARS-CoV-2. J Biomater Sci Polym Ed 10(1080/09205063):1975020",
"volume": "10",
"year": "2021"
},
{
"DOI": "10.1007/s11356-021-16715-z",
"author": "V Tiwari",
"doi-asserted-by": "publisher",
"journal-title": "Environ Sci Pollut Res Int",
"key": "4102_CR24",
"unstructured": "Tiwari V, Kumar M, Tiwari A, Sahoo BM, Singh S, Kumar S, Saharan R (2021) Current trends in diagnosis and treatment strategies of COVID-19 infection. Environ Sci Pollut Res Int. https://doi.org/10.1007/s11356-021-16715-z",
"year": "2021"
},
{
"DOI": "10.1016/j.metop.2021.100121",
"author": "K Srivastava",
"doi-asserted-by": "publisher",
"journal-title": "Metabol Open",
"key": "4102_CR25",
"unstructured": "Srivastava K, Singh MK (2021) Drug repurposing in COVID-19: a review with past, present and future. Metabol Open. https://doi.org/10.1016/j.metop.2021.100121",
"year": "2021"
},
{
"DOI": "10.1016/j.autrev.2021.102941",
"author": "F Elrashdy",
"doi-asserted-by": "publisher",
"journal-title": "Autoimmun Rev",
"key": "4102_CR26",
"unstructured": "Elrashdy F, Tambuwala MM, Hassan SS, Adadi P, Seyran M, Abd El-Aziz TM, Rezaei N, Lal A, Aljabali AAA, Kandimalla R, Bazan NG, Azad GK, Sherchan SP, Choudhury PP, Serrano-Aroca A, Takayama K, Chauhan G, Pizzol D, Barh D, Panda PK, Mishra YK, Palu G, Lundstrom K, Redwan EM, Uversky VN (2021) Autoimmunity roots of the thrombotic events after COVID-19 vaccination. Autoimmun Rev. https://doi.org/10.1016/j.autrev.2021.102941",
"year": "2021"
},
{
"DOI": "10.1186/s12872-021-02183-3",
"author": "AA Hasnie",
"doi-asserted-by": "publisher",
"first-page": "375",
"issue": "1",
"journal-title": "BMC Cardiovasc Disord",
"key": "4102_CR27",
"unstructured": "Hasnie AA, Hasnie UA, Patel N, Aziz MU, Xie M, Lloyd SG, Prabhu SD (2021) Perimyocarditis following first dose of the mRNA-1273 SARS-CoV-2 (Moderna) vaccine in a healthy young male: a case report. BMC Cardiovasc Disord 21(1):375. https://doi.org/10.1186/s12872-021-02183-3",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1186/s12968-021-00795-4",
"author": "YR Patel",
"doi-asserted-by": "publisher",
"first-page": "101",
"issue": "1",
"journal-title": "J Cardiovasc Magn Reson",
"key": "4102_CR28",
"unstructured": "Patel YR, Louis DW, Atalay M, Agarwal S, Shah NR (2021) Cardiovascular magnetic resonance findings in young adult patients with acute myocarditis following mRNA COVID-19 vaccination: a case series. J Cardiovasc Magn Reson 23(1):101. https://doi.org/10.1186/s12968-021-00795-4",
"volume": "23",
"year": "2021"
},
{
"DOI": "10.1016/j.biochi.2021.08.011",
"author": "W Al-Zyoud",
"doi-asserted-by": "publisher",
"first-page": "91",
"journal-title": "Biochimie",
"key": "4102_CR29",
"unstructured": "Al-Zyoud W, Haddad H (2021) Dynamics prediction of emerging notable spike protein mutations in SARS-CoV-2 implies a need for updated vaccines. Biochimie 191:91–103. https://doi.org/10.1016/j.biochi.2021.08.011",
"volume": "191",
"year": "2021"
},
{
"DOI": "10.1080/22221751.2021.1942230",
"author": "A Baj",
"doi-asserted-by": "publisher",
"first-page": "1254",
"issue": "1",
"journal-title": "Emerg Microbes Infect",
"key": "4102_CR30",
"unstructured": "Baj A, Novazzi F, Genoni A, Ferrante FD, Taborelli S, Pini B, Partenope M, Valli M, Gasperina DD, Capuano R, Prestia M, Spezia PG, Azzi L, Focosi D, Maggi F (2021) Symptomatic SARS-CoV-2 infections after full schedule BNT162b2 vaccination in seropositive healthcare workers: a case series from a single institution. Emerg Microbes Infect 10(1):1254–1256. https://doi.org/10.1080/22221751.2021.1942230",
"volume": "10",
"year": "2021"
},
{
"DOI": "10.2174/187221412799015317",
"author": "V Srinivasan",
"doi-asserted-by": "publisher",
"first-page": "30",
"issue": "1",
"journal-title": "Recent Pat Endocr Metab Immune Drug Discov",
"key": "4102_CR31",
"unstructured": "Srinivasan V, Mohamed M, Kato H (2012) Melatonin in bacterial and viral infections with focus on sepsis: a review. Recent Pat Endocr Metab Immune Drug Discov 6(1):30–39. https://doi.org/10.2174/187221412799015317",
"volume": "6",
"year": "2012"
},
{
"DOI": "10.3390/diseases9020030",
"author": "VM Martin Gimenez",
"doi-asserted-by": "publisher",
"journal-title": "Diseases",
"key": "4102_CR32",
"unstructured": "Martin Gimenez VM, de Las HN, Ferder L, Lahera V, Reiter RJ, Manucha W (2021) Potential Effects of Melatonin and Micronutrients on Mitochondrial Dysfunction during a Cytokine Storm Typical of Oxidative/Inflammatory Diseases. Diseases. https://doi.org/10.3390/diseases9020030",
"year": "2021"
},
{
"DOI": "10.32794/mr11250049",
"author": "E Peschechera",
"doi-asserted-by": "publisher",
"first-page": "77",
"issue": "1",
"journal-title": "Melatonin Res",
"key": "4102_CR33",
"unstructured": "Peschechera E, Veronesi PA (2020) Injectable melatonin: an anti-cancer and anti-viral treatment option. Melatonin Res 3(1):77–80. https://doi.org/10.32794/mr11250049",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1111/jpi.12186",
"author": "DX Tan",
"doi-asserted-by": "publisher",
"first-page": "381",
"issue": "4",
"journal-title": "J Pineal Res",
"key": "4102_CR34",
"unstructured": "Tan DX, Korkmaz A, Reiter RJ, Manchester LC (2014) Ebola virus disease: potential use of melatonin as a treatment. J Pineal Res 57(4):381–384. https://doi.org/10.1111/jpi.12186",
"volume": "57",
"year": "2014"
},
{
"DOI": "10.32794/mr11250047",
"author": "RJ Reiter",
"doi-asserted-by": "publisher",
"first-page": "43",
"issue": "1",
"journal-title": "Melatonin Res",
"key": "4102_CR35",
"unstructured": "Reiter RJ, Ma Q, Sharma R (2020) Treatment of ebola and other infectious diseases: melatonin “goes viral.” Melatonin Res 3(1):43–57. https://doi.org/10.32794/mr11250047",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0240149",
"author": "L Artigas",
"doi-asserted-by": "publisher",
"first-page": "e0240149",
"issue": "10",
"journal-title": "PLoS ONE",
"key": "4102_CR36",
"unstructured": "Artigas L, Coma M, Matos-Filipe P, Aguirre-Plans J, Farres J, Valls R, Fernandez-Fuentes N, de la Haba-Rodriguez J, Olvera A, Barbera J, Morales R, Oliva B, Mas JM (2020) In-silico drug repurposing study predicts the combination of pirfenidone and melatonin as a promising candidate therapy to reduce SARS-CoV-2 infection progression and respiratory distress caused by cytokine storm. PLoS ONE 15(10):e0240149. https://doi.org/10.1371/journal.pone.0240149",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.7150/ijms.48053",
"author": "EL Feitosa",
"doi-asserted-by": "publisher",
"first-page": "2133",
"issue": "14",
"journal-title": "Int J Med Sci",
"key": "4102_CR37",
"unstructured": "Feitosa EL, Junior F, Nery Neto JAO, Matos LFL, Moura MHS, Rosales TO, De Freitas GBL (2020) COVID-19: Rational discovery of the therapeutic potential of Melatonin as a SARS-CoV-2 main Protease Inhibitor. Int J Med Sci 17(14):2133–2146. https://doi.org/10.7150/ijms.48053",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1016/j.csbj.2021.02.009",
"author": "AP Chavarria",
"doi-asserted-by": "publisher",
"first-page": "1379",
"journal-title": "Comput Struct Biotechnol J",
"key": "4102_CR38",
"unstructured": "Chavarria AP, Vazquez RRV, Cherit JGD, Bello HH, Suastegui HC, Moreno-Castaneda L, Alanis Estrada G, Hernandez F, Gonzalez-Marcos O, Saucedo-Orozco H, Manzano-Pech L, Marquez-Velasco R, Guarner-Lans V, Perez-Torres I, Soto ME (2021) Antioxidants and pentoxifylline as coadjuvant measures to standard therapy to improve prognosis of patients with pneumonia by COVID-19. Comput Struct Biotechnol J 19:1379–1390. https://doi.org/10.1016/j.csbj.2021.02.009",
"volume": "19",
"year": "2021"
},
{
"DOI": "10.1111/j.1600-079X.2007.00516.x",
"author": "OF Tekbas",
"doi-asserted-by": "publisher",
"first-page": "222",
"issue": "2",
"journal-title": "J Pineal Res",
"key": "4102_CR39",
"unstructured": "Tekbas OF, Ogur R, Korkmaz A, Kilic A, Reiter RJ (2008) Melatonin as an antibiotic: new insights into the actions of this ubiquitous molecule. J Pineal Res 44(2):222–226. https://doi.org/10.1111/j.1600-079X.2007.00516.x",
"volume": "44",
"year": "2008"
},
{
"DOI": "10.3389/fimmu.2021.683879",
"author": "F He",
"doi-asserted-by": "publisher",
"first-page": "683879",
"journal-title": "Front Immunol",
"key": "4102_CR40",
"unstructured": "He F, Wu X, Zhang Q, Li Y, Ye Y, Li P, Chen S, Peng Y, Hardeland R, Xia Y (2021) Bacteriostatic potential of melatonin: therapeutic standing and mechanistic insights. Front Immunol 12:683879. https://doi.org/10.3389/fimmu.2021.683879",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1203/00006450-200112000-00021",
"author": "E Gitto",
"doi-asserted-by": "publisher",
"first-page": "756",
"issue": "6",
"journal-title": "Pediatr Res",
"key": "4102_CR41",
"unstructured": "Gitto E, Karbownik M, Reiter RJ, Tan DX, Cuzzocrea S, Chiurazzi P, Cordaro S, Corona G, Trimarchi G, Barberi I (2001) Effects of melatonin treatment in septic newborns. Pediatr Res 50(6):756–760. https://doi.org/10.1203/00006450-200112000-00021",
"volume": "50",
"year": "2001"
},
{
"DOI": "10.1055/s-0037-1604244",
"author": "G D'Angelo",
"doi-asserted-by": "publisher",
"first-page": "1382",
"issue": "14",
"journal-title": "Am J Perinatol",
"key": "4102_CR42",
"unstructured": "D’Angelo G, Marseglia L, Reiter RJ, Buonocore G, Gitto E (2017) Melatonin and neonatal sepsis: a promising antioxidant adjuvant agent. Am J Perinatol 34(14):1382–1388. https://doi.org/10.1055/s-0037-1604244",
"volume": "34",
"year": "2017"
},
{
"DOI": "10.1186/s13052-018-0528-3",
"author": "G D'Angelo",
"doi-asserted-by": "publisher",
"first-page": "84",
"issue": "1",
"journal-title": "Ital J Pediatr",
"key": "4102_CR43",
"unstructured": "D’Angelo G, Impellizzeri P, Marseglia L, Montalto AS, Russo T, Salamone I, Falsaperla R, Corsello G, Romeo C, Gitto E (2018) Current status of laboratory and imaging diagnosis of neonatal necrotizing enterocolitis. Ital J Pediatr 44(1):84. https://doi.org/10.1186/s13052-018-0528-3",
"volume": "44",
"year": "2018"
},
{
"DOI": "10.1096/fj.202100651R",
"author": "G Li",
"doi-asserted-by": "publisher",
"first-page": "e21783",
"issue": "9",
"journal-title": "FASEB J",
"key": "4102_CR44",
"unstructured": "Li G, Lv D, Yao Y, Wu H, Wang J, Deng S, Song Y, Guan S, Wang L, Ma W, Yang H, Yan L, Zhang J, Ji P, Zhang L, Lian Z, Liu G (2021) Overexpression of ASMT likely enhances the resistance of transgenic sheep to brucellosis by influencing immune-related signaling pathways and gut microbiota. FASEB J 35(9):e21783. https://doi.org/10.1096/fj.202100651R",
"volume": "35",
"year": "2021"
},
{
"DOI": "10.1172/JCI149236",
"author": "JM Snider",
"doi-asserted-by": "publisher",
"journal-title": "J Clin Invest",
"key": "4102_CR45",
"unstructured": "Snider JM, You JK, Wang X, Snider AJ, Hallmark B, Zec MM, Seeds MC, Sergeant S, Johnstone L, Wang Q, Sprissler R, Carr TF, Lutrick K, Parthasarathy S, Bime C, Zhang HH, Luberto C, Kew RR, Hannun YA, Guerra S, McCall CE, Yao G, Del Poeta M, Chilton FH (2021) Group IIA secreted phospholipase A2 is associated with the pathobiology leading to COVID-19 mortality. J Clin Invest. https://doi.org/10.1172/JCI149236",
"year": "2021"
},
{
"DOI": "10.1016/j.it.2020.02.003",
"author": "VP van Hensbergen",
"doi-asserted-by": "publisher",
"first-page": "313",
"issue": "4",
"journal-title": "Trends Immunol",
"key": "4102_CR46",
"unstructured": "van Hensbergen VP, Wu Y, van Sorge NM, Touqui L (2020) Type IIA Secreted Phospholipase A2 in Host Defense against Bacterial Infections. Trends Immunol 41(4):313–326. https://doi.org/10.1016/j.it.2020.02.003",
"volume": "41",
"year": "2020"
},
{
"DOI": "10.1007/BF02849996",
"author": "T Yavuz",
"doi-asserted-by": "publisher",
"first-page": "91",
"issue": "1",
"journal-title": "Adv Ther",
"key": "4102_CR47",
"unstructured": "Yavuz T, Kaya D, Behcet M, Ozturk E, Yavuz O (2007) Effects of melatonin on Candida sepsis in an experimental rat model. Adv Ther 24(1):91–100. https://doi.org/10.1007/BF02849996",
"volume": "24",
"year": "2007"
},
{
"DOI": "10.1016/j.burns.2016.09.023",
"author": "CA Prauchner",
"doi-asserted-by": "publisher",
"first-page": "471",
"issue": "3",
"journal-title": "Burns",
"key": "4102_CR48",
"unstructured": "Prauchner CA (2017) Oxidative stress in sepsis: pathophysiological implications justifying antioxidant co-therapy. Burns 43(3):471–485. https://doi.org/10.1016/j.burns.2016.09.023",
"volume": "43",
"year": "2017"
},
{
"DOI": "10.1016/j.bja.2017.12.010",
"author": "V Natesan",
"doi-asserted-by": "publisher",
"first-page": "412",
"issue": "2",
"journal-title": "Br J Anaesth",
"key": "4102_CR49",
"unstructured": "Natesan V (2018) Adrenergic blockade inhibits bacterial quorum sensing and reverses Warburg effect in septic shock. Br J Anaesth 120(2):412–413. https://doi.org/10.1016/j.bja.2017.12.010",
"volume": "120",
"year": "2018"
},
{
"DOI": "10.1038/s41586-019-1678-1",
"author": "D Zhang",
"doi-asserted-by": "publisher",
"first-page": "575",
"issue": "7779",
"journal-title": "Nature",
"key": "4102_CR50",
"unstructured": "Zhang D, Tang Z, Huang H, Zhou G, Cui C, Weng Y, Liu W, Kim S, Lee S, Perez-Neut M, Ding J, Czyz D, Hu R, Ye Z, He M, Zheng YG, Shuman HA, Dai L, Ren B, Roeder RG, Becker L, Zhao Y (2019) Metabolic regulation of gene expression by histone lactylation. Nature 574(7779):575–580. https://doi.org/10.1038/s41586-019-1678-1",
"volume": "574",
"year": "2019"
},
{
"DOI": "10.1038/s41598-021-90192-9",
"author": "TV de Jong",
"doi-asserted-by": "publisher",
"first-page": "10793",
"issue": "1",
"journal-title": "Sci Rep",
"key": "4102_CR51",
"unstructured": "de Jong TV, Guryev V, Moshkin YM (2021) Estimates of gene ensemble noise highlight critical pathways and predict disease severity in H1N1, COVID-19 and mortality in sepsis patients. Sci Rep 11(1):10793. https://doi.org/10.1038/s41598-021-90192-9",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1080/08830185.2021.1974856",
"author": "Y Luo",
"doi-asserted-by": "publisher",
"journal-title": "Int Rev Immunol",
"key": "4102_CR52",
"unstructured": "Luo Y, Li L, Chen X, Gou H, Yan K, Xu Y (2021) Effects of lactate in immunosuppression and inflammation: progress and prospects. Int Rev Immunol. https://doi.org/10.1080/08830185.2021.1974856",
"year": "2021"
},
{
"DOI": "10.1111/jpi.12547",
"author": "Y Xia",
"doi-asserted-by": "publisher",
"first-page": "e12547",
"issue": "2",
"journal-title": "J Pineal Res",
"key": "4102_CR53",
"unstructured": "Xia Y, Chen S, Zeng S, Zhao Y, Zhu C, Deng B, Zhu G, Yin Y, Wang W, Hardeland R, Ren W (2019) Melatonin in macrophage biology: current understanding and future perspectives. J Pineal Res 66(2):e12547. https://doi.org/10.1111/jpi.12547",
"volume": "66",
"year": "2019"
},
{
"DOI": "10.3390/ijms18030657",
"author": "T Schmoch",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR54",
"unstructured": "Schmoch T, Uhle F, Siegler BH, Fleming T, Morgenstern J, Nawroth PP, Weigand MA, Brenner T (2017) The glyoxalase system and methylglyoxal-derived carbonyl stress in sepsis: glycotoxic aspects of sepsis pathophysiology. Int J Mol Sci. https://doi.org/10.3390/ijms18030657",
"year": "2017"
},
{
"DOI": "10.1038/s41392-021-00726-w",
"author": "M Tian",
"doi-asserted-by": "publisher",
"first-page": "308",
"issue": "1",
"journal-title": "Signal Transduct Target Ther",
"key": "4102_CR55",
"unstructured": "Tian M, Liu W, Li X, Zhao P, Shereen MA, Zhu C, Huang S, Liu S, Yu X, Yue M, Pan P, Wang W, Li Y, Chen X, Wu K, Luo Z, Zhang Q, Wu J (2021) HIF-1alpha promotes SARS-CoV-2 infection and aggravates inflammatory responses to COVID-19. Signal Transduct Target Ther 6(1):308. https://doi.org/10.1038/s41392-021-00726-w",
"volume": "6",
"year": "2021"
},
{
"DOI": "10.1038/s41577-020-0331-4",
"author": "M Merad",
"doi-asserted-by": "publisher",
"first-page": "355",
"issue": "6",
"journal-title": "Nat Rev Immunol",
"key": "4102_CR56",
"unstructured": "Merad M, Martin JC (2020) Pathological inflammation in patients with COVID-19: a key role for monocytes and macrophages. Nat Rev Immunol 20(6):355–362. https://doi.org/10.1038/s41577-020-0331-4",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.32794/mr11250033",
"author": "RJ Reiter",
"doi-asserted-by": "publisher",
"first-page": "105",
"issue": "3",
"journal-title": "Melatonin Res",
"key": "4102_CR57",
"unstructured": "Reiter RJ, Sharma R, Ma Q, Rosales-Corral S, Acuna-Castroviejo D, Escames G (2019) Inhibition of mitochondrial pyruvate dehydrogenase kinase: a proposed mechanism by which melatonin causes cancer cells to overcome cytosolic glycolysis, reduce tumor biomass and reverse insensitivity to chemotherapy. Melatonin Res 2(3):105–119. https://doi.org/10.32794/mr11250033",
"volume": "2",
"year": "2019"
},
{
"DOI": "10.3390/ijms22020764",
"author": "RJ Reiter",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR58",
"unstructured": "Reiter RJ, Sharma R, Rosales-Corral S (2021) Anti-warburg effect of melatonin: a proposed mechanism to explain its inhibition of multiple diseases. Int J Mol Sci. https://doi.org/10.3390/ijms22020764",
"year": "2021"
},
{
"DOI": "10.1073/pnas.2106017118",
"author": "T Peng",
"doi-asserted-by": "publisher",
"journal-title": "Proc Natl Acad Sci USA",
"key": "4102_CR59",
"unstructured": "Peng T, Du SY, Son M, Diamond B (2021) HIF-1alpha is a negative regulator of interferon regulatory factors: implications for interferon production by hypoxic monocytes. Proc Natl Acad Sci USA. https://doi.org/10.1073/pnas.2106017118",
"year": "2021"
},
{
"DOI": "10.1515/hsz-2021=0245",
"author": "S Al-Gburi",
"doi-asserted-by": "publisher",
"journal-title": "Biol Chem",
"key": "4102_CR60",
"unstructured": "Al-Gburi S, Beissert S, Gunther C (2021) Molecular mechanisms of vaculopathy and coagulopathy in COVID-19. Biol Chem. https://doi.org/10.1515/hsz-2021=0245",
"year": "2021"
},
{
"DOI": "10.1136/bmjopen-2020-046057",
"author": "MA Mansouri",
"doi-asserted-by": "publisher",
"first-page": "e046057",
"issue": "6",
"journal-title": "BMJ Open",
"key": "4102_CR61",
"unstructured": "Mansouri MA, Kee F, Garcia L, Bradley DT (2021) Role of systems science in preventing and controlling emerging infectious diseases: protocol for a scoping review. BMJ Open 11(6):e046057. https://doi.org/10.1136/bmjopen-2020-046057",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1016/j.immuni.2021.04.001",
"author": "B Zhu",
"doi-asserted-by": "publisher",
"first-page": "1200",
"issue": "6",
"journal-title": "Immunity",
"key": "4102_CR62",
"unstructured": "Zhu B, Wu Y, Huang S, Zhang R, Son YM, Li C, Cheon IS, Gao X, Wang M, Chen Y, Zhou X, Nguyen Q, Phan AT, Behl S, Taketo MM, Mack M, Shapiro VS, Zeng H, Ebihara H, Mullon JJ, Edell ES, Reisenauer JS, Demirel N, Kern RM, Chakraborty R, Cui W, Kaplan MH, Zhou X, Goldrath AW, Sun J (2021) Uncoupling of macrophage inflammation from self-renewal modulates host recovery from respiratory viral infection. Immunity 54(6):1200-1218e1209. https://doi.org/10.1016/j.immuni.2021.04.001",
"volume": "54",
"year": "2021"
},
{
"DOI": "10.1016/j.mvr.2021.104188",
"author": "AH Noroozneezhad",
"doi-asserted-by": "publisher",
"first-page": "104188",
"journal-title": "Microvasc Res",
"key": "4102_CR63",
"unstructured": "Noroozneezhad AH, Mansouri K (2021) Endothelial cell dysfunction, coagulation, and angiogenesis in coronavirus disease 2019 (COVID-19). Microvasc Res 137:104188. https://doi.org/10.1016/j.mvr.2021.104188",
"volume": "137",
"year": "2021"
},
{
"DOI": "10.1016/j.cmet.2020.07.007",
"author": "AC Codo",
"doi-asserted-by": "publisher",
"first-page": "437",
"issue": "3",
"journal-title": "Cell Metab",
"key": "4102_CR64",
"unstructured": "Codo AC, Davanzo GG, Monteiro LB, de Souza GF, Muraro SP, Virgilio-da-Silva JV, Prodonoff JS, Carregari VC, de Biagi Junior CAO, Crunfli F, Jimenez Restrepo JL, Vendramini PH, Reis-de-Oliveira G, Bispo Dos Santos K, Toledo-Teixeira DA, Parise PL, Martini MC, Marques RE, Carmo HR, Borin A, Coimbra LD, Boldrini VO, Brunetti NS, Vieira AS, Mansour E, Ulaf RG, Bernardes AF, Nunes TA, Ribeiro LC, Palma AC, Agrela MV, Moretti ML, Sposito AC, Pereira FB, Velloso LA, Vinolo MAR, Damasio A, Proenca-Modena JL, Carvalho RF, Mori MA, Martins-de-Souza D, Nakaya HI, Farias AS, Moraes-Vieira PM (2020) Elevated Glucose Levels Favor SARS-CoV-2 Infection and Monocyte Response through a HIF-1alpha/Glycolysis-Dependent Axis. Cell Metab 32(3):437-446e435. https://doi.org/10.1016/j.cmet.2020.07.007",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.3390/ijms18040763",
"author": "YR Zonta",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR65",
"unstructured": "Zonta YR, Martinez M, Camargo IC, Domeniconi RF, Lupi Junior LA, Pinheiro PF, Reiter RJ, Martinez FE, Chuffa LG (2017) Melatonin Reduces Angiogenesis in Serous Papillary Ovarian Carcinoma of Ethanol-Preferring Rats. Int J Mol Sci. https://doi.org/10.3390/ijms18040763",
"year": "2017"
},
{
"DOI": "10.1016/j.ejphar.2020.173282",
"author": "NF Maroufi",
"doi-asserted-by": "publisher",
"first-page": "173282",
"journal-title": "Eur J Pharmacol",
"key": "4102_CR66",
"unstructured": "Maroufi NF, Amiri M, Dizaji BF, Vahedian V, Akbarzadeh M, Roshanravan N, Haiaty S, Nouri M, Rashidi MR (2020) Inhibitory effect of melatonin on hypoxia-induced vasculogenic mimicry via suppressing epithelial-mesenchymal transition (EMT) in breast cancer stem cells. Eur J Pharmacol 881:173282. https://doi.org/10.1016/j.ejphar.2020.173282",
"volume": "881",
"year": "2020"
},
{
"DOI": "10.3892/ol.2020.12292",
"author": "W Yin",
"doi-asserted-by": "publisher",
"first-page": "31",
"issue": "1",
"journal-title": "Oncol Lett",
"key": "4102_CR67",
"unstructured": "Yin W, Liu Y, Liu X, Ma X, Sun B, Yu Z (2021) Metformin inhibits epithelial-mesenchymal transition of oral squamous cell carcinoma via the mTOR/HIF-1alpha/PKM2/STAT3 pathway. Oncol Lett 21(1):31. https://doi.org/10.3892/ol.2020.12292",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1016/j.bbcan.2016.02.004",
"author": "J Vriend",
"doi-asserted-by": "publisher",
"first-page": "176",
"journal-title": "Biochim Biophys Acta 1865",
"key": "4102_CR68",
"unstructured": "Vriend J, Reiter RJ (2016) Melatonin and the von Hippel-Lindau/HIF-1 oxygen sensing mechanism: a review. Biochim Biophys Acta 1865 2:176–183. https://doi.org/10.1016/j.bbcan.2016.02.004",
"volume": "2",
"year": "2016"
},
{
"DOI": "10.1155/2020/5406284",
"author": "M He",
"doi-asserted-by": "publisher",
"first-page": "5406284",
"journal-title": "Oxid Med Cell Longev",
"key": "4102_CR69",
"unstructured": "He M, Zhou C, Lu Y, Mao L, Xi Y, Mei X, Wang X, Zhang L, Yu Z, Zhou Z (2020) Melatonin antagonizes nickel-induced aerobic glycolysis by blocking ROS-mediated HIF-1alpha/miR210/ISCU axis activation. Oxid Med Cell Longev 2020:5406284. https://doi.org/10.1155/2020/5406284",
"volume": "2020",
"year": "2020"
},
{
"DOI": "10.3389/fimmu.2021.673692",
"author": "JH Costa",
"doi-asserted-by": "publisher",
"first-page": "673692",
"journal-title": "Front Immunol",
"key": "4102_CR70",
"unstructured": "Costa JH, Mohanapriya G, Bharadwaj R, Noceda C, Thiers KLL, Aziz S, Srivastava S, Oliveira M, Gupta KJ, Kumari A, Sircar D, Kumar SR, Achra A, Sathishkumar R, Adholeya A, Arnholdt-Schmitt B (2021) ROS/RNS Balancing, Aerobic Fermentation Regulation and Cell Cycle Control—a Complex Early Trait ('CoV-MAC-TED’) for Combating SARS-CoV-2-Induced Cell Reprogramming. Front Immunol 12:673692. https://doi.org/10.3389/fimmu.2021.673692",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1590/1806-9282.67.Suppl1.20200968",
"author": "WJ Martorina",
"doi-asserted-by": "publisher",
"first-page": "18",
"issue": "Suppl 1",
"journal-title": "Rev Assoc Med Bras (1992)",
"key": "4102_CR71",
"unstructured": "Martorina WJ, Tavares A (2021) Possible role of exogenous melatonin in preventing more serious COVID-19 infection in patients with type 2 diabetes mellitus. Rev Assoc Med Bras (1992) 67(Suppl 1):18–21. https://doi.org/10.1590/1806-9282.67.Suppl1.20200968",
"volume": "67",
"year": "2021"
},
{
"DOI": "10.1016/j.ejphar.2021.174193",
"author": "A Hosseini",
"doi-asserted-by": "publisher",
"first-page": "174193",
"journal-title": "Eur J Pharmacol",
"key": "4102_CR72",
"unstructured": "Hosseini A, Esmaeili Gouvarchin Ghaleh H, Aghamollaei H, Fasihi Ramandi M, Alishiri G, Shahriary A, Hassanpour K, Tat M, Farnoosh G (2021) Evaluation of Th1 and Th2 mediated cellular and humoral immunity in patients with COVID-19 following the use of melatonin as an adjunctive treatment. Eur J Pharmacol 904:174193. https://doi.org/10.1016/j.ejphar.2021.174193",
"volume": "904",
"year": "2021"
},
{
"DOI": "10.1007/s12013-021-01003-x",
"author": "E Letsiou",
"doi-asserted-by": "publisher",
"journal-title": "Cell Biochem Biophys",
"key": "4102_CR73",
"unstructured": "Letsiou E, Htwe YM, Dudek SM (2021) Secretory Phospholipase A2 Enzymes in Acute Lung Injury. Cell Biochem Biophys. https://doi.org/10.1007/s12013-021-01003-x",
"year": "2021"
},
{
"DOI": "10.1016/j.cbd.2021.100875",
"author": "LP Lee",
"doi-asserted-by": "publisher",
"first-page": "100875",
"journal-title": "Comp Biochem Physiol Part D Genomics Proteomics",
"key": "4102_CR74",
"unstructured": "Lee LP, Tan KY, Tan CH (2021) Snake venom proteomics and antivenomics of two Sundaic lance-headed pit vipers: Trimeresurus wiroti (Malaysia) and Trimeresurus puniceus (Indonesia). Comp Biochem Physiol Part D Genomics Proteomics 40:100875. https://doi.org/10.1016/j.cbd.2021.100875",
"volume": "40",
"year": "2021"
},
{
"DOI": "10.3390/toxins13080548",
"author": "HY Zhao",
"doi-asserted-by": "publisher",
"journal-title": "Toxins (Basel)",
"key": "4102_CR75",
"unstructured": "Zhao HY, Sun Y, Du Y, Li JQ, Lv JG, Qu YF, Lin LH, Lin CX, Ji X, Gao JF (2021) Venom of the annulated sea snake Hydrophis cyanocinctus: a biochemically simple but genetically complex weapon. Toxins (Basel). https://doi.org/10.3390/toxins13080548",
"year": "2021"
},
{
"DOI": "10.1007/s43440-021-00258-8",
"author": "H Khan",
"doi-asserted-by": "publisher",
"first-page": "1240",
"issue": "5",
"journal-title": "Pharmacol Rep",
"key": "4102_CR76",
"unstructured": "Khan H, Gupta A, Singh TG, Kaur A (2021) Mechanistic insight on the role of leukotriene receptors in ischemic-reperfusion injury. Pharmacol Rep 73(5):1240–1254. https://doi.org/10.1007/s43440-021-00258-8",
"volume": "73",
"year": "2021"
},
{
"DOI": "10.3390/biom11050717",
"author": "A Kulkarni",
"doi-asserted-by": "publisher",
"first-page": "717",
"issue": "5",
"journal-title": "Biomolcules",
"key": "4102_CR77",
"unstructured": "Kulkarni A, Nadler JL, Mirmira R, Casimiuro I (2021) Regulation of tissue inflammation by 12-lipoxygenase. Biomolcules 11(5):717. https://doi.org/10.3390/biom11050717",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1016/j.prostaglandins.2020.106482",
"author": "A Trostchansky",
"doi-asserted-by": "publisher",
"first-page": "106482",
"journal-title": "Prostaglandins Other Lipid Mediat",
"key": "4102_CR78",
"unstructured": "Trostchansky A, Wood I, Rubbo H (2021) Regulation of arachidonic acid oxidation and metabolism by lipid electrophiles. Prostaglandins Other Lipid Mediat 152:106482. https://doi.org/10.1016/j.prostaglandins.2020.106482",
"volume": "152",
"year": "2021"
},
{
"DOI": "10.3390/ijms22158295",
"author": "MG Appiah",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR79",
"unstructured": "Appiah MG, Park EJ, Akama Y, Nakamori Y, Kawamoto E, Gaowa A, Shimaoka M (2021) Cellular and exosomal regulations of sepsis-induced metabolic alterations. Int J Mol Sci. https://doi.org/10.3390/ijms22158295",
"year": "2021"
},
{
"DOI": "10.3390/biology9090249",
"author": "G Anderson",
"doi-asserted-by": "publisher",
"journal-title": "Biology (Basel)",
"key": "4102_CR80",
"unstructured": "Anderson G, Carbone A, Mazzoccoli G (2020) Aryl Hydrocarbon Receptor Role in Co-Ordinating SARS-CoV-2 Entry and Symptomatology: Linking Cytotoxicity Changes in COVID-19 and Cancers; Modulation by Racial Discrimination Stress. Biology (Basel). https://doi.org/10.3390/biology9090249",
"year": "2020"
},
{
"DOI": "10.1016/j.jcrc.2017.09.012",
"author": "D Bar-Or",
"doi-asserted-by": "publisher",
"first-page": "197",
"journal-title": "J Crit Care",
"key": "4102_CR81",
"unstructured": "Bar-Or D, Carrick M, Tanner A 2nd, Lieser MJ, Rael LT, Brody E (2018) Overcoming the Warburg Effect: Is it the key to survival in sepsis? J Crit Care 43:197–201. https://doi.org/10.1016/j.jcrc.2017.09.012",
"volume": "43",
"year": "2018"
},
{
"DOI": "10.1111/jpi.12755",
"author": "X Chen",
"doi-asserted-by": "publisher",
"journal-title": "J Pineal Res",
"key": "4102_CR82",
"unstructured": "Chen X, Hao B, Li D, Reiter RJ, Bai Y, Abay B, Chen G, Lin S, Zheng T, Ren Y, Xu X, Li M, Fan L (2021) Melatonin inhibits lung cancer development by reversing the Warburg effect via stimulating the SIRT3/PDH axis. J Pineal Res. https://doi.org/10.1111/jpi.12755",
"year": "2021"
},
{
"DOI": "10.1038/s41392-021-00745-7",
"author": "M Li",
"doi-asserted-by": "publisher",
"first-page": "330",
"issue": "1",
"journal-title": "Signal Transduct Target Ther",
"key": "4102_CR83",
"unstructured": "Li M, Hao B, Zhang M, Reiter RJ, Lin S, Zheng T, Chen X, Ren Y, Yue L, Abay B, Chen G, Xu X, Shi Y, Fan L (2021) Melatonin enhances radiofrequency-induced NK antitumor immunity, causing cancer metabolism reprogramming and inhibition of multiple pulmonary tumor development. Signal Transduct Target Ther 6(1):330. https://doi.org/10.1038/s41392-021-00745-7",
"volume": "6",
"year": "2021"
},
{
"DOI": "10.1371/journal.pone.0180554",
"author": "TL Tan",
"doi-asserted-by": "publisher",
"first-page": "e0180554",
"issue": "7",
"journal-title": "PLoS ONE",
"key": "4102_CR84",
"unstructured": "Tan TL, Goh YY (2017) The role of group IIA secretory phospholipase A2 (sPLA2- IIA) as a biomarker for the diagnosis of sepsis and bacterial infection in adults-A systematic review. PLoS ONE 12(7):e0180554. https://doi.org/10.1371/journal.pone.0180554",
"volume": "12",
"year": "2017"
},
{
"DOI": "10.3390/toxins12020068",
"author": "PE Bickler",
"doi-asserted-by": "publisher",
"journal-title": "Toxins (Basel)",
"key": "4102_CR85",
"unstructured": "Bickler PE (2020) Amplification of Snake Venom Toxicity by Endogenous Signaling Pathways. Toxins (Basel). https://doi.org/10.3390/toxins12020068",
"year": "2020"
},
{
"DOI": "10.1038/s41598-019-40903-0",
"author": "PL de Araujo",
"doi-asserted-by": "publisher",
"first-page": "4281",
"issue": "1",
"journal-title": "Sci Rep",
"key": "4102_CR86",
"unstructured": "de Araujo PL, de Almeida MES, Bretones ML, Cirillo MC, Curi R, Sampaio SC (2019) Crotoxin promotes macrophage reprogramming towards an antiangiogenic phenotype. Sci Rep 9(1):4281. https://doi.org/10.1038/s41598-019-40903-0",
"volume": "9",
"year": "2019"
},
{
"DOI": "10.1111/jpi.12123",
"author": "GD Katkar",
"doi-asserted-by": "publisher",
"first-page": "295",
"issue": "3",
"journal-title": "J Pineal Res",
"key": "4102_CR87",
"unstructured": "Katkar GD, Sundaram MS, Hemshekhar M, Sharma DR, Santhosh MS, Sunitha K, Rangappa KS, Girish KS, Kemparaju K (2014) Melatonin alleviates Echis carinatus venom-induced toxicities by modulating inflammatory mediators and oxidative stress. J Pineal Res 56(3):295–312. https://doi.org/10.1111/jpi.12123",
"volume": "56",
"year": "2014"
},
{
"DOI": "10.1016/j.actatropica.2014.12.007",
"author": "AE Abdel Moneim",
"doi-asserted-by": "publisher",
"first-page": "58",
"journal-title": "Acta Trop",
"key": "4102_CR88",
"unstructured": "Abdel Moneim AE, Ortiz F, Leonardo-Mendonca RC, Vergano-Villodres R, Guerrero-Martinez JA, Lopez LC, Acuna-Castroviejo D, Escames G (2015) Protective effects of melatonin against oxidative damage induced by Egyptian cobra (Naja haje) crude venom in rats. Acta Trop 143:58–65. https://doi.org/10.1016/j.actatropica.2014.12.007",
"volume": "143",
"year": "2015"
},
{
"DOI": "10.3390/ijms22115555",
"author": "M Estaras",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR89",
"unstructured": "Estaras M, Gonzalez-Portillo MR, Fernandez-Bermejo M, Mateos JM, Vara D, Blanco-Fernandez G, Lopez-Guerra D, Roncero V, Salido GM, Gonzalez A (2021) Melatonin Induces Apoptosis and Modulates Cyclin Expression and MAPK Phosphorylation in Pancreatic Stellate Cells Subjected to Hypoxia. Int J Mol Sci. https://doi.org/10.3390/ijms22115555",
"year": "2021"
},
{
"DOI": "10.1111/j.1600-079X.2009.00688.x",
"author": "A Marino",
"doi-asserted-by": "publisher",
"first-page": "56",
"issue": "1",
"journal-title": "J Pineal Res",
"key": "4102_CR90",
"unstructured": "Marino A, Di Paola R, Crisafulli C, Mazzon E, Morabito R, Paterniti I, Galuppo M, Genovese T, La Spada G, Cuzzocrea S (2009) Protective effect of melatonin against the inflammatory response elicited by crude venom from isolated nematocysts of Pelagia noctiluca (Cnidaria, Scyphozoa). J Pineal Res 47(1):56–69. https://doi.org/10.1111/j.1600-079X.2009.00688.x",
"volume": "47",
"year": "2009"
},
{
"DOI": "10.1111/jpi.12360",
"author": "RJ Reiter",
"doi-asserted-by": "publisher",
"first-page": "253",
"issue": "3",
"journal-title": "J Pineal Res",
"key": "4102_CR91",
"unstructured": "Reiter RJ, Mayo JC, Tan DX, Sainz RM, Alatorre-Jimenez M, Qin L (2016) Melatonin as an antioxidant: under promises but over delivers. J Pineal Res 61(3):253–278. https://doi.org/10.1111/jpi.12360",
"volume": "61",
"year": "2016"
},
{
"DOI": "10.3390/ijms20051223",
"author": "R Hardeland",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR92",
"unstructured": "Hardeland R (2019) Aging, Melatonin, and the Pro- and Anti-Inflammatory Networks. Int J Mol Sci. https://doi.org/10.3390/ijms20051223",
"year": "2019"
},
{
"DOI": "10.1111/jpi.12539",
"author": "A Perez-Gonzalez",
"doi-asserted-by": "publisher",
"first-page": "e12539",
"issue": "2",
"journal-title": "J Pineal Res",
"key": "4102_CR93",
"unstructured": "Perez-Gonzalez A, Castaneda-Arriaga R, Alvarez-Idaboy JR, Reiter RJ, Galano A (2019) Melatonin and its metabolites as chemical agents capable of directly repairing oxidized DNA. J Pineal Res 66(2):e12539. https://doi.org/10.1111/jpi.12539",
"volume": "66",
"year": "2019"
},
{
"DOI": "10.3390/molecules25194410",
"author": "DX Tan",
"doi-asserted-by": "publisher",
"journal-title": "Molecules",
"key": "4102_CR94",
"unstructured": "Tan DX, Hardeland R (2020) Targeting Host Defense System and Rescuing Compromised Mitochondria to Increase Tolerance against Pathogens by Melatonin May Impact Outcome of Deadly Virus Infection Pertinent to COVID-19. Molecules. https://doi.org/10.3390/molecules25194410",
"year": "2020"
},
{
"DOI": "10.32794/mr11250063",
"doi-asserted-by": "publisher",
"key": "4102_CR95",
"unstructured": "Castillo RR, Quizon GRA, Juco MJM, Roman ADE, de Leon DG, Punzalan FER, R.B.L. G, Morales DD, Tan D-X, Reiter RJ (2020) Melatonin as adjuvant treatment for coronavirus disease 2019 pneumonia patients requiring hospitalization (MAC-19 PRO): a case series. Melatonin Res 3 (3):297-310. https://doi.org/10.32794/mr11250063"
},
{
"DOI": "10.1016/j.arcmed.2021.06.006",
"doi-asserted-by": "publisher",
"key": "4102_CR96",
"unstructured": "Farnoosh G, Akbariqomi M, Badri T, Bagheri M, Izadi M, Saeedi-Boroujeni A, Rezaie E, Ghaleh HEG, Aghamollaei H, Fasihi-Ramandi M, Hassanpour K, Alishiri G (2021) Efficacy of a Low Dose of Melatonin as an Adjunctive Therapy in Hospitalized Patients with COVID-19: A Randomized, Double-blind Clinical Trial. Arch Med Res. https://doi.org/10.1016/j.arcmed.2021.06.006"
},
{
"DOI": "10.1111/j.1600-079x.1996.tb00288.x",
"author": "LC Ellis",
"doi-asserted-by": "publisher",
"first-page": "214",
"issue": "4",
"journal-title": "J Pineal Res",
"key": "4102_CR97",
"unstructured": "Ellis LC (1996) Melatonin reduces mortality from Aleutian disease in mink (Mustela vison). J Pineal Res 21(4):214–217. https://doi.org/10.1111/j.1600-079x.1996.tb00288.x",
"volume": "21",
"year": "1996"
},
{
"DOI": "10.1007/978-1-4615-4709-9_28",
"author": "GJ Maestroni",
"doi-asserted-by": "publisher",
"first-page": "217",
"journal-title": "Adv Exp Med Biol",
"key": "4102_CR98",
"unstructured": "Maestroni GJ (1999) Therapeutic potential of melatonin in immunodeficiency states, viral diseases, and cancer. Adv Exp Med Biol 467:217–226. https://doi.org/10.1007/978-1-4615-4709-9_28",
"volume": "467",
"year": "1999"
},
{
"DOI": "10.1016/j.actatropica.2014.04.021",
"author": "JR Vielma",
"doi-asserted-by": "publisher",
"first-page": "31",
"journal-title": "Acta Trop",
"key": "4102_CR99",
"unstructured": "Vielma JR, Bonilla E, Chacin-Bonilla L, Mora M, Medina-Leendertz S, Bravo Y (2014) Effects of melatonin on oxidative stress, and resistance to bacterial, parasitic, and viral infections: a review. Acta Trop 137:31–38. https://doi.org/10.1016/j.actatropica.2014.04.021",
"volume": "137",
"year": "2014"
},
{
"DOI": "10.1177/2040206616660851",
"author": "M Montiel",
"doi-asserted-by": "publisher",
"first-page": "99",
"issue": "3–4",
"journal-title": "Antivir Chem Chemother",
"key": "4102_CR100",
"unstructured": "Montiel M, Bonilla E, Valero N, Mosquera J, Espina LM, Quiroz Y, Alvarez-Mon M (2015) Melatonin decreases brain apoptosis, oxidative stress, and CD200 expression and increased survival rate in mice infected by Venezuelan equine encephalitis virus. Antivir Chem Chemother 24(3–4):99–108. https://doi.org/10.1177/2040206616660851",
"volume": "24",
"year": "2015"
},
{
"DOI": "10.3390/v13040659",
"author": "A Morchang",
"doi-asserted-by": "publisher",
"journal-title": "Viruses",
"key": "4102_CR101",
"unstructured": "Morchang A, Malakar S, Poonudom K, Noisakran S, Yenchitsomanus PT, Limjindaporn T (2021) Melatonin Inhibits Dengue Virus Infection via the Sirtuin 1-Mediated Interferon Pathway. Viruses. https://doi.org/10.3390/v13040659",
"year": "2021"
},
{
"DOI": "10.1111/jpi.12754",
"author": "X Zhai",
"doi-asserted-by": "publisher",
"journal-title": "J Pineal Res",
"key": "4102_CR102",
"unstructured": "Zhai X, Wang N, Jiao H, Zhang J, Li C, Ren W, Reiter RJ, Su S (2021) Melatonin and other indoles show antiviral activities against swine coronaviruses in vitro at pharmacological concentrations. J Pineal Res. https://doi.org/10.1111/jpi.12754",
"year": "2021"
},
{
"DOI": "10.1016/j.ijid.2021.10.012",
"author": "ZT Hasan",
"doi-asserted-by": "publisher",
"journal-title": "Int J Infect Dis",
"key": "4102_CR103",
"unstructured": "Hasan ZT, Atrakji D, Mehuaiden DAK (2021) The Effect of Melatonin on Thrombosis, Sepsis and Mortality Rate in COVID-19 Patients. Int J Infect Dis. https://doi.org/10.1016/j.ijid.2021.10.012",
"year": "2021"
},
{
"DOI": "10.1002/jmv.27312",
"author": "SA Mousavi",
"doi-asserted-by": "publisher",
"first-page": "263",
"issue": "1",
"journal-title": "J Med Virol",
"key": "4102_CR104",
"unstructured": "Mousavi SA, Heydari K, Mehravaran H, Saeedi M, Alizadeh-Navaei R, Hedayatizadeh-Omran A, Shamshirian A (2022) Melatonin effects on sleep quality and outcomes of COVID-19 patients: An open-label, randomized, controlled trial. J Med Virol 94(1):263–271. https://doi.org/10.1002/jmv.27312",
"volume": "94",
"year": "2022"
},
{
"author": "Z Alizadeh",
"first-page": "494",
"issue": "4",
"journal-title": "Iran J Allergy Asthma Immunol",
"key": "4102_CR105",
"unstructured": "Alizadeh Z, Keyhanian N, Ghaderkhani S, Dashti-Khavidaki S, Shokouhi Shoormasti R, Pourpak Z (2021) A Pilot Study on Controlling Coronavirus Disease 2019 (COVID-19) Inflammation Using Melatonin Supplement. Iran J Allergy Asthma Immunol 20(4):494–499",
"volume": "20",
"year": "2021"
},
{
"DOI": "10.1111/j.1600-079x.1986.tb00760.x",
"author": "RL Sack",
"doi-asserted-by": "publisher",
"first-page": "379",
"issue": "4",
"journal-title": "J Pineal Res",
"key": "4102_CR106",
"unstructured": "Sack RL, Lewy AJ, Erb DL, Vollmer WM, Singer CM (1986) Human melatonin production decreases with age. J Pineal Res 3(4):379–388. https://doi.org/10.1111/j.1600-079x.1986.tb00760.x",
"volume": "3",
"year": "1986"
},
{
"DOI": "10.1016/j.jpsychores.2016.05.005",
"author": "RM Scholtens",
"doi-asserted-by": "publisher",
"first-page": "20",
"journal-title": "J Psychosom Res",
"key": "4102_CR107",
"unstructured": "Scholtens RM, van Munster BC, van Kempen MF, de Rooij SE (2016) Physiological melatonin levels in healthy older people: a systematic review. J Psychosom Res 86:20–27. https://doi.org/10.1016/j.jpsychores.2016.05.005",
"volume": "86",
"year": "2016"
},
{
"DOI": "10.1186/s12871-021-01511-6",
"author": "S Oba",
"doi-asserted-by": "publisher",
"first-page": "291",
"issue": "1",
"journal-title": "BMC Anesthesiol",
"key": "4102_CR108",
"unstructured": "Oba S, Altinay M, Salkaya A, Turk HS (2021) Evaluation of the effect of clinical characteristics and intensive care treatment methods on the mortality of covid-19 patients aged 80 years and older. BMC Anesthesiol 21(1):291. https://doi.org/10.1186/s12871-021-01511-6",
"volume": "21",
"year": "2021"
},
{
"author": "GM Vaughan",
"first-page": "199",
"journal-title": "J Neural Transm Suppl",
"key": "4102_CR109",
"unstructured": "Vaughan GM (1986) Human melatonin in physiologic and diseased states: neural control of the rhythm. J Neural Transm Suppl 21:199–215",
"volume": "21",
"year": "1986"
},
{
"DOI": "10.32794/mr11250079",
"author": "S Pandi-Perumal",
"doi-asserted-by": "publisher",
"first-page": "558",
"issue": "4",
"journal-title": "Melatonin Res",
"key": "4102_CR110",
"unstructured": "Pandi-Perumal S, Cardinali D, Reiter RJ, Brown G (2020) Low melatonin as a contributor to SARS-CoV-2 disease. Melatonin Res 3(4):558–576. https://doi.org/10.32794/mr11250079",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1210/jcem-45-4-768",
"author": "JJ Nordlund",
"doi-asserted-by": "publisher",
"first-page": "768",
"issue": "4",
"journal-title": "J Clin Endocrinol Metab",
"key": "4102_CR111",
"unstructured": "Nordlund JJ, Lerner AB (1977) The effects of oral melatonin on skin color and on the release of pituitary hormones. J Clin Endocrinol Metab 45(4):768–774. https://doi.org/10.1210/jcem-45-4-768",
"volume": "45",
"year": "1977"
},
{
"DOI": "10.1111/jpi.12762",
"author": "KH Lu",
"doi-asserted-by": "publisher",
"issue": "3",
"journal-title": "J Pineal Res",
"key": "4102_CR112",
"unstructured": "Lu KH, Lu PW, Lu EW, Tang CH, Su SC, Lin CW, Yang SF (2021) The potential remedy of melatonin on osteoarthritis. J Pineal Res 71(3):e12762. https://doi.org/10.1111/jpi.12762",
"volume": "71",
"year": "2021"
},
{
"DOI": "10.3390/antiox10081179",
"author": "AK Jaworek",
"doi-asserted-by": "publisher",
"journal-title": "Antioxidants",
"key": "4102_CR113",
"unstructured": "Jaworek AK, Szepietowski JC, Halubiec P, Wojas-Pelc A, Jaworek J (2021) Melatonin as an antioxidant and immunomodulator in atopic dermatitis-a new look on an old story: a review. Antioxidants. https://doi.org/10.3390/antiox10081179",
"year": "2021"
},
{
"DOI": "10.3390/ijms22158296",
"author": "R Hardeland",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR114",
"unstructured": "Hardeland R (2021) Melatonin and Microglia. Int J Mol Sci. https://doi.org/10.3390/ijms22158296",
"year": "2021"
},
{
"DOI": "10.3390/antiox10010047",
"author": "P Wongchitrat",
"doi-asserted-by": "publisher",
"journal-title": "Antioxidants (Basel)",
"key": "4102_CR115",
"unstructured": "Wongchitrat P, Shukla M, Sharma R, Govitrapong P, Reiter RJ (2021) Role of Melatonin on Virus-Induced Neuropathogenesis-A Concomitant Therapeutic Strategy to Understand SARS-CoV-2 Infection. Antioxidants (Basel). https://doi.org/10.3390/antiox10010047",
"year": "2021"
},
{
"DOI": "10.1007/s00018-017-2613-y",
"author": "OC Baltatu",
"doi-asserted-by": "publisher",
"first-page": "3955",
"issue": "21",
"journal-title": "Cell Mol Life Sci",
"key": "4102_CR116",
"unstructured": "Baltatu OC, Amaral FG, Campos LA, Cipolla-Neto J (2017) Melatonin, mitochondria and hypertension. Cell Mol Life Sci 74(21):3955–3964. https://doi.org/10.1007/s00018-017-2613-y",
"volume": "74",
"year": "2017"
},
{
"DOI": "10.1590/1678-9199-JVATITD-2020-0183",
"author": "VP Targhetta",
"doi-asserted-by": "publisher",
"first-page": "e20200183",
"journal-title": "J Venom Anim Toxins Incl Trop Dis",
"key": "4102_CR117",
"unstructured": "Targhetta VP, Amaral MA, Camara NOS (2021) Through DNA sensors and hidden mitochondrial effects of SARS-CoV-2. J Venom Anim Toxins Incl Trop Dis 27:e20200183. https://doi.org/10.1590/1678-9199-JVATITD-2020-0183",
"volume": "27",
"year": "2021"
},
{
"DOI": "10.1038/s41598-021-00064-5",
"author": "B Alonazi",
"doi-asserted-by": "publisher",
"first-page": "20476",
"issue": "1",
"journal-title": "Sci Rep",
"key": "4102_CR118",
"unstructured": "Alonazi B, Farghaly AM, Mostafa MA, Al-Watban JA, Zindani SA, Altaimi F, Fagiry MA, Mahmoud MZ (2021) Brain MRI in SARS-CoV-2 pneumonia patients with newly developed neurological manifestations suggestive of brain involvement. Sci Rep 11(1):20476. https://doi.org/10.1038/s41598-021-00064-5",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.3748/wjg.v27.i34.5682",
"author": "D Ristic-Medic",
"doi-asserted-by": "publisher",
"first-page": "5682",
"issue": "34",
"journal-title": "World J Gastroenterol",
"key": "4102_CR119",
"unstructured": "Ristic-Medic D, Petrovic S, Arsic A, Vucic V (2021) Liver disease and COVID-19: the link with oxidative stress, antioxidants and nutrition. World J Gastroenterol 27(34):5682–5699. https://doi.org/10.3748/wjg.v27.i34.5682",
"volume": "27",
"year": "2021"
},
{
"DOI": "10.14336/AD.2021.0709",
"author": "H Wang",
"doi-asserted-by": "publisher",
"first-page": "1545",
"issue": "7",
"journal-title": "Aging Dis",
"key": "4102_CR120",
"unstructured": "Wang H, Wang Z, Cao W, Wu Q, Yuan Y, Zhang X (2021) Regulatory T cells in COVID-19. Aging Dis 12(7):1545–1553. https://doi.org/10.14336/AD.2021.0709",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1016/j.bcp.2019.03.008",
"author": "C Vaamonde-Garcia",
"doi-asserted-by": "publisher",
"first-page": "181",
"journal-title": "Biochem Pharmacol",
"key": "4102_CR121",
"unstructured": "Vaamonde-Garcia C, Lopez-Armada MJ (2019) Role of mitochondrial dysfunction on rheumatic diseases. Biochem Pharmacol 165:181–195. https://doi.org/10.1016/j.bcp.2019.03.008",
"volume": "165",
"year": "2019"
},
{
"DOI": "10.3389/fcvm.2021.734388",
"author": "X Xu",
"doi-asserted-by": "publisher",
"first-page": "734388",
"journal-title": "Front Cardiovasc Med",
"key": "4102_CR122",
"unstructured": "Xu X, Lin JI, Bais AS, Reynolds MJ, Tan T, Gabriel GC, Kondos Z, Liu X, Shiva SS, Lo CW (2021) Mitochondrial respiration defects in single-ventricle congenital heart disease. Front Cardiovasc Med 8:734388. https://doi.org/10.3389/fcvm.2021.734388",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.1038/s41420-021-00675-x",
"author": "Q Yang",
"doi-asserted-by": "publisher",
"first-page": "293",
"issue": "1",
"journal-title": "Cell Death Discovery",
"key": "4102_CR123",
"unstructured": "Yang Q, Wang L, Liu J, Cao W, Pan Q, Li M (2021) Targeting the complex I and III of mitochondrial electron transport chain as a potentially viable option in liver cancer management. Cell Death Discovery 7(1):293. https://doi.org/10.1038/s41420-021-00675-x",
"volume": "7",
"year": "2021"
},
{
"DOI": "10.1111/jpi.12774",
"author": "C Chen",
"doi-asserted-by": "publisher",
"journal-title": "J Pineal Res",
"key": "4102_CR124",
"unstructured": "Chen C, Yang C, Wang J, Huang X, Yu H, Li S, Li S, Zhang Z, Liu J, Yang X, Liu GP (2021) Melatonin ameliorates cognitive deficits through improving mitophagy in a mouse model of Alzheimer’s disease. J Pineal Res. https://doi.org/10.1111/jpi.12774",
"year": "2021"
},
{
"DOI": "10.3390/ijms22157979",
"author": "L Rochette",
"doi-asserted-by": "publisher",
"journal-title": "Int J Mol Sci",
"key": "4102_CR125",
"unstructured": "Rochette L, Ghibu S (2021) Mechanics insights of alpha-lipoic acid against cardiovascular diseases during COVID-19 infection. Int J Mol Sci. https://doi.org/10.3390/ijms22157979",
"year": "2021"
},
{
"DOI": "10.1523/JNEUROSCI.3188-20.2021",
"author": "O Swain",
"doi-asserted-by": "publisher",
"first-page": "5338",
"issue": "25",
"journal-title": "J Neurosci",
"key": "4102_CR126",
"unstructured": "Swain O, Romano SK, Miryala R, Tsai J, Parikh V, Umanah GKE (2021) SARS-CoV-2 neuronal invasion and complications: potential mechanisms and therapeutic approaches. J Neurosci 41(25):5338–5349. https://doi.org/10.1523/JNEUROSCI.3188-20.2021",
"volume": "41",
"year": "2021"
},
{
"DOI": "10.9778/cmajo.20210044",
"author": "M Science",
"doi-asserted-by": "publisher",
"first-page": "E929",
"issue": "4",
"journal-title": "CMAJ Open",
"key": "4102_CR127",
"unstructured": "Science M, Bolotin S, Silverman M, Nadarajah J, Maguire B, Parekh RS, McGeer A, Schwartz KL, Alexander L, Allen U, Ariyarajah A, Castellani L, Cohn RD, Downing M, Katz K, Kazmi K, Leis JA, Liu D, Pernica JM, Schneiderman JE, Sumaida M, Campigotto A (2021) SARS-CoV-2 antibodies in Ontario health care workers during and after the first wave of the pandemic: a cohort study. CMAJ Open 9(4):E929–E939. https://doi.org/10.9778/cmajo.20210044",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1111/j.1600-079X.2012.01002.x",
"author": "MZ Xia",
"doi-asserted-by": "publisher",
"first-page": "325",
"issue": "4",
"journal-title": "J Pineal Res",
"key": "4102_CR128",
"unstructured": "Xia MZ, Liang YL, Wang H, Chen X, Huang YY, Zhang ZH, Chen YH, Zhang C, Zhao M, Xu DX, Song LH (2012) Melatonin modulates TLR4-mediated inflammatory genes through MyD88- and TRIF-dependent signaling pathways in lipopolysaccharide-stimulated RAW2647 cells. J Pineal Res 53(4):325–334. https://doi.org/10.1111/j.1600-079X.2012.01002.x",
"volume": "53",
"year": "2012"
},
{
"DOI": "10.1007/s00018-019-03438-1",
"author": "RJ Reiter",
"doi-asserted-by": "publisher",
"first-page": "2527",
"issue": "13",
"journal-title": "Cell Mol Life Sci",
"key": "4102_CR129",
"unstructured": "Reiter RJ, Sharma R, Ma Q, Rorsales-Corral S, de Almeida Chuffa LG (2020) Melatonin inhibits Warburg-dependent cancer by redirecting glucose oxidation to the mitochondria: a mechanistic hypothesis. Cell Mol Life Sci 77(13):2527–2542. https://doi.org/10.1007/s00018-019-03438-1",
"volume": "77",
"year": "2020"
},
{
"DOI": "10.1152/physiol.00034.2019",
"author": "RJ Reiter",
"doi-asserted-by": "publisher",
"first-page": "86",
"issue": "2",
"journal-title": "Physiology (Bethesda)",
"key": "4102_CR130",
"unstructured": "Reiter RJ, Ma Q, Sharma R (2020) Melatonin in mitochondria: mitigating clear and present dangers. Physiology (Bethesda) 35(2):86–95. https://doi.org/10.1152/physiol.00034.2019",
"volume": "35",
"year": "2020"
},
{
"DOI": "10.1073/pnas.1705768114",
"author": "Y Suofu",
"doi-asserted-by": "publisher",
"first-page": "E7997",
"issue": "38",
"journal-title": "Proc Natl Acad Sci USA",
"key": "4102_CR131",
"unstructured": "Suofu Y, Li W, Jean-Alphonse FG, Jia J, Khattar NK, Li J, Baranov SV, Leronni D, Mihalik AC, He Y, Cecon E, Wehbi VL, Kim J, Heath BE, Baranova OV, Wang X, Gable MJ, Kretz ES, Di Benedetto G, Lezon TR, Ferrando LM, Larkin TM, Sullivan M, Yablonska S, Wang J, Minnigh MB, Guillaumet G, Suzenet F, Richardson RM, Poloyac SM, Stolz DB, Jockers R, Witt-Enderby PA, Carlisle DL, Vilardaga JP, Friedlander RM (2017) Dual role of mitochondria in producing melatonin and driving GPCR signaling to block cytochrome c release. Proc Natl Acad Sci USA 114(38):E7997–E8006. https://doi.org/10.1073/pnas.1705768114",
"volume": "114",
"year": "2017"
},
{
"DOI": "10.2147/JIR.S323356",
"author": "RD Castle",
"doi-asserted-by": "publisher",
"first-page": "4859",
"journal-title": "J Inflamm Res",
"key": "4102_CR132",
"unstructured": "Castle RD, Williams MA, Bushell WC, Rindfleisch JA, Peterson CT, Marzolf J, Brouwer K, Mills PJ (2021) Implications for systemic approaches to COVID-19: effect sizes of remdesivir, tocilizumab, melatonin, vitamin D3, and meditation. J Inflamm Res 14:4859–4876. https://doi.org/10.2147/JIR.S323356",
"volume": "14",
"year": "2021"
},
{
"DOI": "10.1038/s41525-020-00143-y",
"author": "T Takahashi",
"doi-asserted-by": "publisher",
"first-page": "35",
"journal-title": "NPJ Genom Med",
"key": "4102_CR133",
"unstructured": "Takahashi T, Luzum JA, Nicol MR, Jacobson PA (2020) Pharmacogenomics of COVID-19 therapies. NPJ Genom Med 5:35. https://doi.org/10.1038/s41525-020-00143-y",
"volume": "5",
"year": "2020"
},
{
"DOI": "10.1016/j.jmii.2020.09.002",
"author": "CJ Yang",
"doi-asserted-by": "publisher",
"first-page": "27",
"issue": "1",
"journal-title": "J Microbiol Immunol Infect",
"key": "4102_CR134",
"unstructured": "Yang CJ, Wei YJ, Chang HL, Chang PY, Tsai CC, Chen YH, Hsueh PR (2021) Remdesivir use in the coronavirus disease 2019 pandemic: a mini-review. J Microbiol Immunol Infect 54(1):27–36. https://doi.org/10.1016/j.jmii.2020.09.002",
"volume": "54",
"year": "2021"
},
{
"DOI": "10.1136/bmj.h4826",
"author": "TS Anderson",
"doi-asserted-by": "publisher",
"first-page": "h4826",
"journal-title": "BMJ",
"key": "4102_CR135",
"unstructured": "Anderson TS, Good CB, Gellad WF (2015) Prevalence and compensation of academic leaders, professors, and trustees on publicly traded US healthcare company boards of directors: cross sectional study. BMJ 351:h4826. https://doi.org/10.1136/bmj.h4826",
"volume": "351",
"year": "2015"
},
{
"DOI": "10.1001/jama.2020.21021",
"author": "C Becker",
"doi-asserted-by": "publisher",
"first-page": "1833",
"issue": "18",
"journal-title": "JAMA",
"key": "4102_CR136",
"unstructured": "Becker C (2020) Relationships between academic medicine leaders and industry-time for another look? JAMA 324(18):1833–1834. https://doi.org/10.1001/jama.2020.21021",
"volume": "324",
"year": "2020"
},
{
"DOI": "10.1136/bmj.n16",
"author": "O Dyer",
"doi-asserted-by": "publisher",
"first-page": "n16",
"journal-title": "BMJ",
"key": "4102_CR137",
"unstructured": "Dyer O (2021) Covid-19: “Shkreli Awards” go to pandemic’s top profiteers. BMJ 372:n16. https://doi.org/10.1136/bmj.n16",
"volume": "372",
"year": "2021"
},
{
"DOI": "10.3390/nu12092561",
"author": "K Kleszczynski",
"doi-asserted-by": "publisher",
"journal-title": "Nutrients",
"key": "4102_CR138",
"unstructured": "Kleszczynski K, Slominski AT, Steinbrink K, Reiter RJ (2020) Clinical Trials for Use of Melatonin to Fight against COVID-19 Are Urgently Needed. Nutrients. https://doi.org/10.3390/nu12092561",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2021.22255",
"author": "R Shavit",
"doi-asserted-by": "publisher",
"first-page": "e2122255",
"issue": "8",
"journal-title": "JAMA Netw Open",
"key": "4102_CR139",
"unstructured": "Shavit R, Maoz-Segal R, Iancovici-Kidon M, Offengenden I, Haj Yahia S, Machnes Maayan D, Lifshitz-Tunitsky Y, Niznik S, Frizinsky S, Deutch M, Elbaz E, Genaim H, Rahav G, Levy I, Belkin A, Regev-Yochay G, Afek A, Agmon-Levin N (2021) Prevalence of Allergic Reactions After Pfizer-BioNTech COVID-19 Vaccination Among Adults With High Allergy Risk. JAMA Netw Open 4(8):e2122255. https://doi.org/10.1001/jamanetworkopen.2021.22255",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.1001/jamanetworkopen.2021.25524",
"author": "CM Warren",
"doi-asserted-by": "publisher",
"first-page": "e2125524",
"issue": "9",
"journal-title": "JAMA Netw Open",
"key": "4102_CR140",
"unstructured": "Warren CM, Snow TT, Lee AS, Shah MM, Heider A, Blomkalns A, Betts B, Buzzanco AS, Gonzalez J, Chinthrajah RS, Do E, Chang I, Dunham D, Lee G, O’Hara R, Park H, Shamji MH, Schilling L, Sindher SB, Sisodiya D, Smith E, Tsai M, Galli SJ, Akdis C, Nadeau KC (2021) Assessment of Allergic and Anaphylactic Reactions to mRNA COVID-19 Vaccines With Confirmatory Testing in a US Regional Health System. JAMA Netw Open 4(9):e2125524. https://doi.org/10.1001/jamanetworkopen.2021.25524",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.1016/j.jamda.2021.08.024",
"author": "BH Bardenheier",
"doi-asserted-by": "publisher",
"journal-title": "J Am Med Dir Assoc",
"key": "4102_CR141",
"unstructured": "Bardenheier BH, Gravenstein S, Blackman C, Gutman R, Sarkar IN, Feifer RA, White EM, McConeghy K, Nanda A, Bosco E, Mor V (2021) Adverse Events Following One Dose of mRNA COVID-19 Vaccination Among US Nursing Home Residents With and Without a Previous SARS-CoV-2 Infection. J Am Med Dir Assoc. https://doi.org/10.1016/j.jamda.2021.08.024",
"year": "2021"
},
{
"DOI": "10.3389/fnins.2021.711605",
"author": "RU Lee",
"doi-asserted-by": "publisher",
"first-page": "711605",
"journal-title": "Front Neurosci",
"key": "4102_CR142",
"unstructured": "Lee RU, Glickman GL (2021) Sleep, Circadian Health and Melatonin for Mitigating COVID-19 and Optimizing Vaccine Efficacy. Front Neurosci 15:711605. https://doi.org/10.3389/fnins.2021.711605",
"volume": "15",
"year": "2021"
},
{
"DOI": "10.32794/mr11250081",
"author": "S Gurunathan",
"doi-asserted-by": "publisher",
"first-page": "30",
"issue": "1",
"journal-title": "Melatonin Res",
"key": "4102_CR143",
"unstructured": "Gurunathan S, Kang M-H, Choi Y, Reiter RJ, Kim J-H (2021) Melatonin: a potential therapeutic agent against COVID-19. Melatonin Res 4(1):30–69. https://doi.org/10.32794/mr11250081",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.32794/mr11250091",
"doi-asserted-by": "publisher",
"key": "4102_CR144",
"unstructured": "Cardinali DP, Brown GM, Pandi-Perumal SR An urgent proposal for the immediate use of melatonin as an adjuvant to anti- SARS-CoV-2 vaccination. Melatonin Res 4 (1):206–212. doi:https://doi.org/10.32794/mr11250091."
}
],
"reference-count": 144,
"references-count": 144,
"relation": {},
"resource": {
"primary": {
"URL": "https://link.springer.com/10.1007/s00018-021-04102-3"
}
},
"score": 1,
"short-container-title": [
"Cell. Mol. Life Sci."
],
"short-title": [],
"source": "Crossref",
"subject": [
"Cell Biology",
"Cellular and Molecular Neuroscience",
"Pharmacology",
"Molecular Biology",
"Molecular Medicine"
],
"subtitle": [],
"title": [
"Melatonin: highlighting its use as a potential treatment for SARS-CoV-2 infection"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "79"
}
