A mid‑pandemic night's dream: Melatonin, from harbinger of anti‑inflammation to mitochondrial savior in acute and long COVID‑19 (Review)
et al., International Journal of Molecular Medicine, doi:10.3892/ijmm.2024.5352, Jan 2024
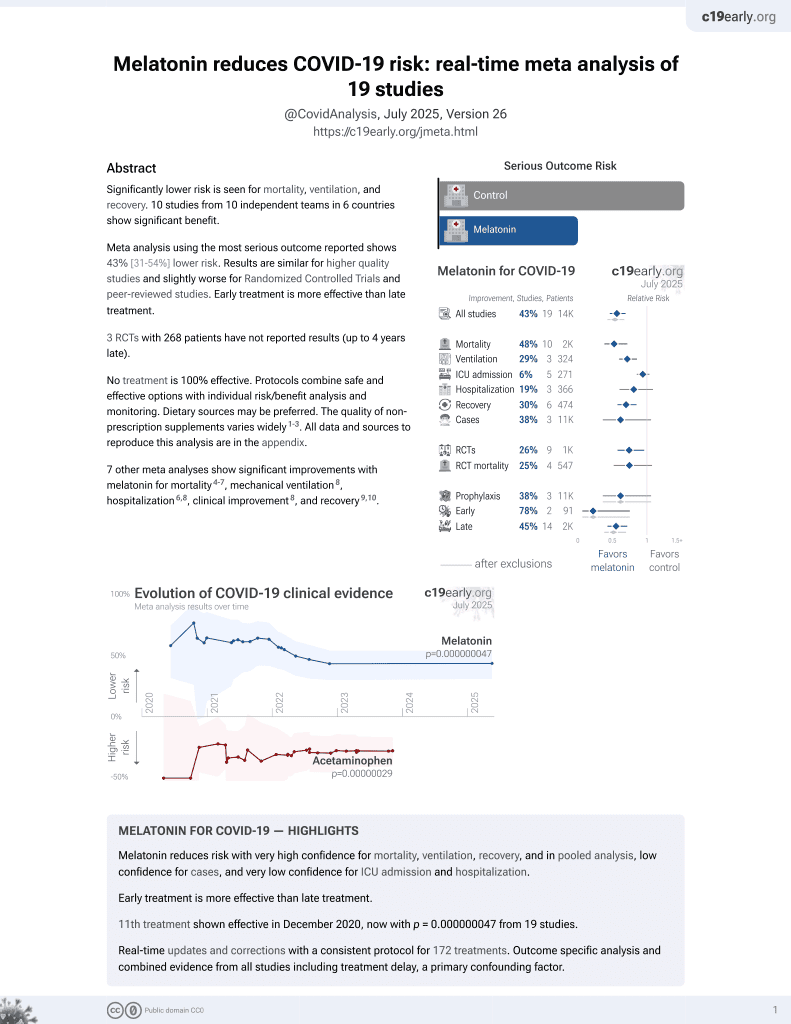
Melatonin for COVID-19
25th treatment shown to reduce risk in
May 2021, now with p = 0.000000015 from 18 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
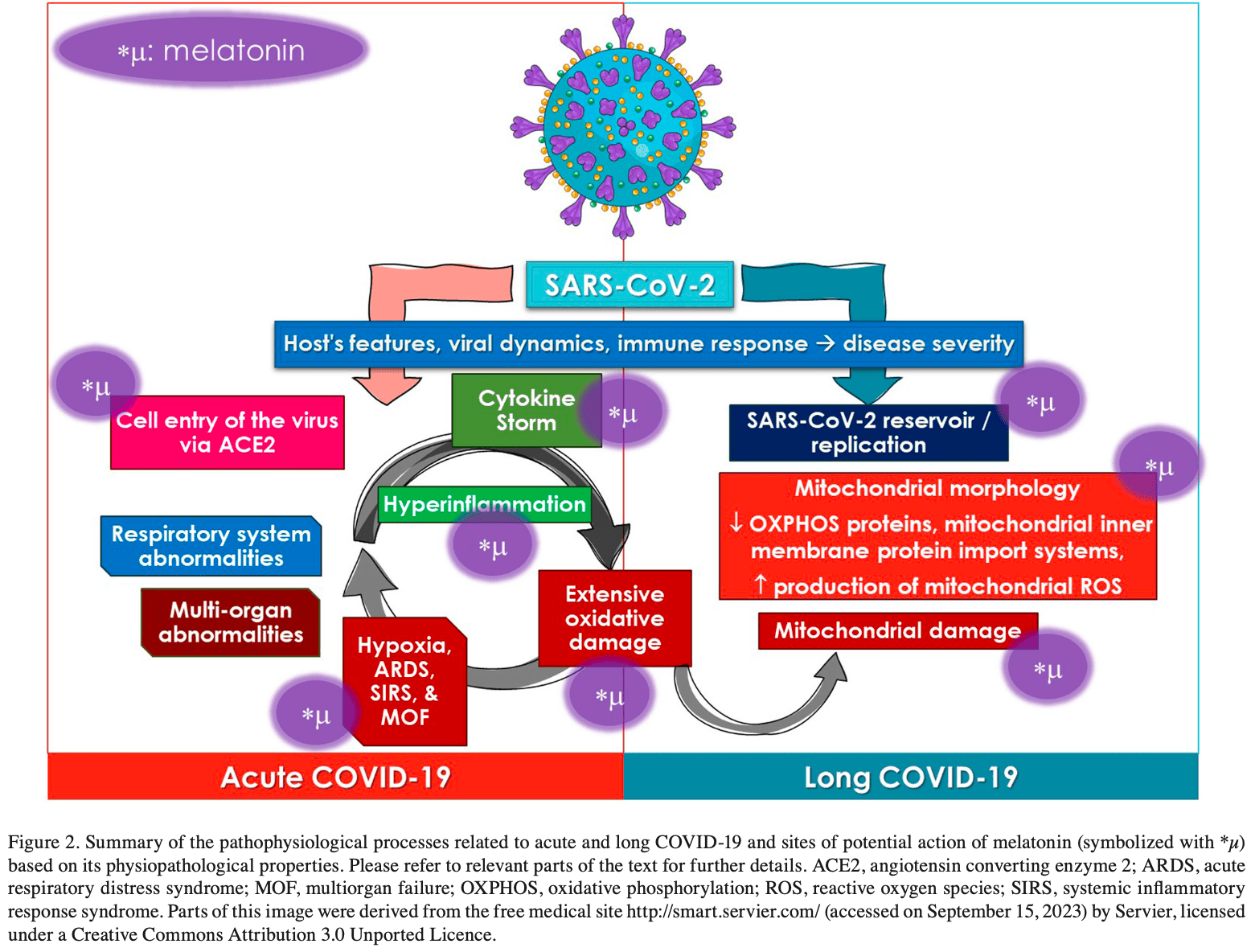
Review of the therapeutic potential of melatonin for COVID-19 and long COVID. Authors provide an extensive review of melatonin's role in health and disease, covering antioxidant, anti-inflammatory, antiviral, and mitochondria-protective properties. Authors detail the pathophysiology of acute COVID-19 and the potential long-term effects like mitochondrial dysfunction. Multiple mechanisms are proposed for how melatonin could alleviate acute symptoms and long-term organ damage from COVID-19 through targeting oxidative stress, inflammation, immune system regulation, viral entry, and supporting mitochondrial health.
1.
Chen et al., Viral mitochondriopathy in COVID-19, Redox Biology, doi:10.1016/j.redox.2025.103766.
2.
Sanduzzi Zamparelli et al., Immune-Boosting and Antiviral Effects of Antioxidants in COVID-19 Pneumonia: A Therapeutic Perspective, Life, doi:10.3390/life15010113.
3.
Xie et al., The role of reactive oxygen species in severe acute respiratory syndrome coronavirus 2 (SARS-COV-2) infection-induced cell death, Cellular & Molecular Biology Letters, doi:10.1186/s11658-024-00659-6.
4.
Zhao et al., Melatonin Potentially Acts as a Widely-Acting Protective Tool in COVID-19, Medicine Research, doi:10.21127/yaoyimr20240006.
5.
Yehia et al., Melatonin: a ferroptosis inhibitor with potential therapeutic efficacy for the post-COVID-19 trajectory of accelerated brain aging and neurodegeneration, Molecular Neurodegeneration, doi:10.1186/s13024-024-00728-6.
6.
Chacin-Bonilla et al., Melatonin and viral infections: A review focusing on therapeutic effects and SARS-CoV-2, Melatonin Research, doi:10.32794/mr112500168.
7.
Lempesis et al., A mid‑pandemic night's dream: Melatonin, from harbinger of anti‑inflammation to mitochondrial savior in acute and long COVID‑19 (Review), International Journal of Molecular Medicine, doi:10.3892/ijmm.2024.5352.
8.
Alomari et al., Assessing the antiviral potential of melatonin: A comprehensive systematic review, Reviews in Medical Virology, doi:10.1002/rmv.2499.
9.
Donzelli, A., Neglected Effective Early Therapies against COVID-19: Focus on Functional Foods and Related Active Substances. A Review, MDPI AG, doi:10.20944/preprints202312.1178.v1.
10.
Langen, M., Melatonin - the Hormone of Both Sun and Darkness - Protects Your Health and Can Save Your Life, Rounding The Earth, roundingtheearth.substack.com/p/melatonin-the-hormone-of-both-sun.
11.
Hosseinzadeh et al., Melatonin effect on platelets and coagulation: Implications for a prophylactic indication in COVID-19, Life Sciences, doi:10.1016/j.lfs.2022.120866.
12.
Loh et al., Melatonin: Regulation of Viral Phase Separation and Epitranscriptomics in Post-Acute Sequelae of COVID-19, International Journal of Molecular Sciences, doi:10.3390/ijms23158122.
13.
Reiter et al., Melatonin: highlighting its use as a potential treatment for SARS-CoV-2 infection, Cellular and Molecular Life Sciences, doi:10.1007/s00018-021-04102-3.
14.
Tan et al., Mechanisms and clinical evidence to support melatonin's use in severe COVID-19 patients to lower mortality, Life Sciences, doi:10.1016/j.lfs.2022.120368.
15.
Behl et al., CD147-spike protein interaction in COVID-19: Get the ball rolling with a novel receptor and therapeutic target, Science of The Total Environment, doi:10.1016/j.scitotenv.2021.152072.
16.
Castle et al., Implications for Systemic Approaches to COVID-19: Effect Sizes of Remdesivir, Tocilizumab, Melatonin, Vitamin D3, and Meditation, Journal of Inflammation Research, doi:10.2147/JIR.S323356.
17.
Ramos et al., The Coronavirus Disease 2019 (COVID-19): Key Emphasis on Melatonin Safety and Therapeutic Efficacy, Antioxidants, doi:10.3390/antiox10071152.
18.
Camp et al., Melatonin interferes with COVID-19 at several distinct ROS-related steps, Journal of Inorganic Biochemistry, doi:10.1016/j.jinorgbio.2021.111546.
19.
Cross et al., Melatonin for the Early Treatment of COVID-19: A Narrative Review of Current Evidence and Possible Efficacy, Endocrine Practice, doi:10.1016/j.eprac.2021.06.001.
20.
DiNicolantonio et al., Melatonin may decrease risk for and aid treatment of COVID-19 and other RNA viral infections, Open Heart, doi:10.1136/openhrt-2020-001568.
21.
Reiter (B) et al., Therapeutic Algorithm for Use of Melatonin in Patients With COVID-19, Frontiers in Medicine, doi:10.3389/fmed.2020.00226.
22.
Charaa et al., Prophylactic Treatment Protocol against the Severity of COVID-19 Using Melatonin, SSRN, doi:10.2139/ssrn.3601861.
Lempesis et al., 26 Jan 2024, multiple countries, peer-reviewed, 4 authors.
Contact: vaso_georgakopoulou@hotmail.com.
A mid‑pandemic night's dream: Melatonin, from harbinger of anti‑inflammation to mitochondrial savior in acute and long COVID‑19 (Review)
International Journal of Molecular Medicine, doi:10.3892/ijmm.2024.5352
Coronavirus disease 2019 (COVID-19) , a systemic illness caused by severe acute respiratory distress syndrome 2 (SARS-CoV-2), has triggered a worldwide pandemic with symptoms ranging from asymptomatic to chronic, affecting practically every organ. Melatonin, an ancient antioxidant found in all living organisms, has been suggested as a safe and effective therapeutic option for the treatment of SARS-CoV-2 infection due to its good safety characteristics and broad-spectrum antiviral medication properties. Melatonin is essential in various metabolic pathways and governs physiological processes, such as the sleep-wake cycle and circadian rhythms. It exhibits oncostatic, anti-inflammatory, antioxidant and anti-aging properties, exhibiting promise for use in the treatment of numerous disorders, including COVID-19. The preventive and therapeutic effects of melatonin have been widely explored in a number of conditions and have been well-established in experimental ischemia/reperfusion investigations, particularly in coronary heart disease and stroke. Clinical research evaluating the use of melatonin in COVID-19 has shown various improved outcomes, including reduced hospitalization durations; however, the trials are small. Melatonin can alleviate mitochondrial dysfunction in COVID-19, improve immune cell function and provide antioxidant properties. However, its therapeutic potential remains underexplored due to funding limitations and thus further investigations are required.
Authors' contributions DAS and VEG conceptualized the study. IGL, VEG, RJR and DAS made a substantial contribution to the interpretation and analysis of data from the literature to be included in the review, and wrote and prepared the draft of the manuscript. DAS and RJR analyzed the data and provided critical revisions. All authors contributed to manuscript revision, and have read and approved the final version of the manuscript. Data authentication is not applicable.
Ethics approval and consent to participate Not applicable.
Patient consent for publication Not applicable.
Competing interests DAS is the Editor-in-Chief for the journal, but had no personal involvement in the reviewing process, or any influence in terms of adjudicating on the final decision, for this article. The other authors declare that they have no competing interests.
References
Ahmad, Ali, Bilal, Rashid, Wani et al., Melatonin and health: Insights of melatonin action, biological functions, and associated disorders, Cell Mol Neurobiol
Ali, Rahman, Hao, Li, Liu et al., Melatonin prevents neuroinflammation and relieves depression by attenuating autophagy impairment through FOXO3a regulation, J Pineal Res
Alizadeh, Keyhanian, Ghaderkhani, Dashti-Khavidaki, Shoormasti et al., A Pilot study on controlling coronavirus disease 2019 (COVID-19) inflammation using melatonin supplement, Iran J Allergy Asthma Immunol
Andersen, Gögenur, Rosenberg, Reiter, Pharmacokinetics of melatonin: The missing link in clinical efficacy?, Clin Pharmacokinet
Antonelli, Pujol, Spector, Ourselin, Steves, Risk of long COVID associated with delta versus omicron variants of SARS-CoV-2, Lancet
Bali, Georgakopoulou, Kamiliou, Vergos, Adamantou et al., Abnormal liver function tests and coronavirus disease 2019: A close relationship, J Viral Hepat
Basoulis, Tsakanikas, Gkoufa, Bitsani, Karamanakos et al., Effectiveness of oral nirmatrelvir/ritonavir vs intravenous three-day remdesivir in preventing progression to severe COVID-19: A single-center, prospective, comparative, real-life study, Viruses
Beaupre, Brown, Vf, Kennedy, Melatonin's neuroprotective role in mitochondria and its potential as a biomarker in aging, cognition and psychiatric disorders, Transl Psychiatry
Behl, Kaur, Aleya, Sehgal, Singh et al., CD147-spike protein interaction in COVID-19: Get the ball rolling with a novel receptor and therapeutic target, Sci Total Environ
Beyer, Steketee, Saphier, Antioxidant properties of melatonin-an emerging mystery, Biochem Pharmacol
Boga, Coto-Montes, Rosales-Corral, Dx, Reiter, Beneficial actions of melatonin in the management of viral infections: A new use for this 'molecular handyman, Rev Med Virol
Bojkova, Klann, Koch, Widera, Krause et al., Proteomics of SARS-CoV-2-infected host cells reveals therapy targets, Nature
Bologna, Pone, Efficacy of prolonged-release melatonin 2 mg (PRM 2 mg) prescribed for insomnia in hospitalized patients for COVID-19: A retrospective observational study, J Clin Med
Bougea, Georga Kopoulou V E, Efthymiopoulou, Angelopoulou, Da et al., New-onset non-motor symptoms in patients with Parkinson's disease and post-COVID-19 syndrome: A prospective cross-sectional study, J Clin Neurosci
Cao, Shrestha, Li, Yu, Chen et al., Melatonin-mediated mitophagy protects against early brain injury after subarachnoid hemorrhage through inhibition of NLRP3 inflammasome activation, Sci Rep
Cardinali, Brown, Sr, An urgent proposal for the immediate use of melatonin as an adjuvant to anti-SARS-CoV-2 vaccination, Melatonin Res
Cecon, Fernandois, Renault, Coelho, Wenzel et al., The potential of melatonin in the prevention and attenuation of oxidative hemolysis and myocardial injury from cd147 SARS-CoV-2 spike protein receptor binding, Cell Mol Life Sci
Cecon, Izabelle, Poder, Real, Zhu et al., Therapeutic potential of melatonin and melatonergic drugs on K18-hACE2 mice infected with SARS-CoV-2, J Pineal Res
Chavarría, Vázquez, Cherit, Bello, Suastegui et al., Antioxidants and pentoxifylline as coadjuvant measures to standard therapy to improve prognosis of patients with pneumonia by COVID-19, Comput Struct Biotechnol J
Cholongitas, Bali, Georgakopoulou, Giannakodimos, Gyftopoulos et al., Prevalence of abnormal liver biochemistry and its impact on COVID-19 patients' outcomes: A single-center Greek study, Ann Gastroenterol
Cholongitas, Bali, Georgakopoulou, Kamiliou, Vergos et al., Comparison of liver function test-and inflammation-based prognostic scores for coronavirus disease 2019: A single center study, Eur J Gastroenterol Hepatol
Chumboatong, Thummayot, Govitrapong, Tocharus, Jittiwat et al., Neuroprotection of agomelatine against cerebral ischemia/reperfusion injury through an antiapoptotic pathway in rat, Neurochem Int
Cipolla-Neto, Amaral, Afeche, Tan, Reiter, Melatonin, energy metabolism, and obesity: A review, J Pineal Res
Cipolla-Neto, Amaral, Melatonin as a hormone: New physiological and clinical insights, Endocr Rev
Codo, Davanzo, Monteiro, De Souza, Muraro et al., Elevated glucose levels favor SARS-CoV-2 infection and monocyte response through a HIF-1α/glycolysis-dependent axis, Cell Metab
Cortese, Lee, Cerikan, Neufeldt, Oorschot et al., Integrative imaging reveals SARS-CoV-2-induced reshaping of subcellular morphologies, Cell Host Microbe
Costantino, Cuzzocrea, Mazzon, Caputi, Protective effects of melatonin in zymosan-activated plasma-induced paw inflammation, Eur J Pharmacol
Cuzzocrea, Zingarelli, Costantino, Caputi, Protective effect of melatonin in a non-septic shock model induced by zymosan in the rat, J Pineal Res
Cuzzocrea, Zingarelli, Gilad, Hake, Salzman et al., Protective effect of melatonin in carrageenan-induced models of local inflammation: Relationship to its inhibitory effect on nitric oxide production and its peroxynitrite scavenging activity, J Pineal Res
Darban, Malek, Memarian, Gohari, Kiani et al., Efficacy of high dose vitamin C, melatonin and zinc in iranian patients with acute respiratory syndrome due to coronavirus infection: A pilot randomized trial, J Cell Mol Anesth
Daugherty, Guo, Heath, Dasmariñas, Jubilo et al., Risk of clinical sequelae after the acute phase of SARS-CoV-2 infection: Retrospective cohort study, BMJ
Davies, Albensi, The effect of COVID-19 on NF-κB and neurological manifestations of disease, Mol Neurobiol
Davis, Assaf, Mccorkell, Wei, Low et al., Characterizing long COVID in an international cohort: 7 Months of symptoms and their impact, EClinicalMedicine
Davis, Mccorkell, Vogel, Topol, Long COVID: Major findings, mechanisms and recommendations, Nat Rev Microbiol
De Vries, Witte, Hondius, Rozemuller, Drukarch et al., Nrf2-induced antioxidant protection: A promising target to counteract ROS-mediated damage in neurodegenerative disease?, Free Radic Biol Med
Dominguez-Rodriguez, Abreu-Gonzalez, Marik, Reiter, Melatonin, cardiovascular disease and COVID-19: A potential therapeutic strategy?, Melatonin Res
Efstathiou, Stefanou, Demetriou, Siafakas, Katsantoni et al., New-onset neuropsychiatric sequelae and 'long-COVID'syndrome (Review), Exp Ther Med
Efstathiou, Stefanou, Demetriou, Siafakas, Makris et al., Long COVID and neuropsychiatric manifestations (Review), Exp Ther Med
El-Sokkary, Omar, Hassanein, Cuzzocrea, Reiter, Melatonin reduces oxidative damage and increases survival of mice infected with Schistosoma mansoni, Free Radic Biol Med
Elrashdy, Tambuwala, Hassan, Adadi, Seyran et al., Autoimmunity roots of the thrombotic events after COVID-19 vaccination, Autoimmun Rev
Erren, Reiter, Melatonin: A universal time messenger, Neuro Endocrinol Lett
Esposito, Cuzzocrea, Antiinflammatory activity of melatonin in central nervous system, Curr Neuropharmacol
Fara, Mitrev, Assas, Cytokine storm and COVID-19: A chronicle of pro-inflammatory cytokines, Open Biol
Farez, Mascanfroni, Méndez-Huergo, Yeste, Murugaiyan et al., Melatonin contributes to the seasonality of multiple sclerosis relapses, Cell
Farnoosh, Akbariqomi, Badri, Bagheri, Izadi et al., Efficacy of a low dose of melatonin as an adjunctive therapy in hospitalized patients with COVID-19: A randomized, double-blind clinical trial, Arch Med Res
Feng, Adeniran, Huang, Li, Ma et al., The ameliorative effect of melatonin on LPS-induced Sertoli cells inflammatory and tight junctions damage via suppression of the TLR4/MyD88/NF-κB signaling pathway in newborn calf, Theriogenology
Gaebler, Wang, Lorenzi, Muecksch, Finkin et al., Evolution of antibody immunity to SARS-CoV-2, Nature
Galano, Tan, Reiter, Melatonin: A versatile protector against oxidative DNA damage, Molecules
García, López-Pingarrón, Almeida-Souza, Tres, Escudero et al., Protective effects of melatonin in reducing oxidative stress and in preserving the fluidity of biological membranes: A review, J Pineal Res
Georgakopoulou, Bali, Adamantou, Asimakopoulou, Makrodimitri et al., Acute hepatitis and liver injury in hospitalized patients with COVID-19 infection, Exp Ther Med
Georgakopoulou, Basoulis, Voutsinas, Makrodimitri, Samara et al., Factors predicting poor outcomes of patients treated with tocilizumab for COVID-19-associated pneumonia: A retrospective study, Exp Ther Med
Georgakopoulou, Gkoufa, Damaskos, Papalexis, Pierrakou et al., COVID-19-associated acute appendicitis in adults. A report of five cases and a review of the literature, Exp Ther Med
Georgakopoulou, Gkoufa, Garmpis, Makrodimitri, Papageorgiou et al., COVID-19 and acute pancreatitis: A systematic review of case reports and case series, Ann Saudi Med
Georgakopoulou, Gkoufa, Makrodimitri, Basoulis, Tsakanikas et al., Early 3-day course of remdesivir for the prevention of the progression to severe COVID-19 in the elderly: A single-centre, real-life cohort study, Exp Ther Med
Georgakopoulou, Gkoufa, Tsakanikas, Makrodimitri, Karamanakos et al., Predictors of COVID-19-associated mortality among hospitalized elderly patients with dementia, Exp Ther Med
Georgakopoulou, Lembessis, Skarlis, Gkoufa, Sipsas et al., Hematological abnormalities in COVID-19 disease: Association with type I interferon pathway activation and disease outcomes, Front Med
Georgakopoulou, Makrodimitri, Triantafyllou, Samara, Voutsinas et al., Immature granulocytes: Innovative biomarker for SARS-CoV-2 infection, Mol Med Rep
Gheban, Rosca, Crisan, The morphological and functional characteristics of the pineal gland, Med Pharm Rep
Giménez, De Las Heras, Ferder, Lahera, Reiter et al., Potential Effects of melatonin and micronutrients on mitochondrial dysfunction during a cytokine storm typical of oxidative/inflammatory diseases, Diseases
Gkoufa, Maneta, Ntoumas, Georgakopoulou, Mantelou et al., Elderly adults with COVID-19 admitted to intensive care unit: A narrative review, World J Crit Care Med
Gkoufa, Saridaki, Georgakopoulou, Da, Cholongitas, COVID-19 vaccination in liver transplant recipients (Review), Exp Ther Med
Goeser, Ruble, Chandler, Melatonin: Historical and clinical perspectives, J Pharmaceut Care Pain Symptom Contr
Gordon, Hiatt, Bouhaddou, Rezelj, Ulferts et al., Comparative host-coronavirus protein interaction networks reveal pan-viral disease mechanisms, Science
Gouvarchin Ghaleh, Hosseini, Aghamollaei, Fasihi-Ramandi, Alishiri et al., NLRP3 inflammasome activation and oxidative stress status in the mild and moderate SARS-CoV-2 infected patients: Impact of melatonin as a medicinal supplement, Z Naturforsch C J Biosci
Guan, Ni, Hu, Liang, Ou et al., Clinical characteristics of coronavirus disease 2019 in China, N Engl J Med
Guarnieri, Dybas, Fazelinia, Kim, Frere et al., Core mitochondrial genes are down-regulated during SARS-CoV-2 infection of rodent and human hosts, Sci Transl Med
Gurunathan, Kang, Choi, Reiter, Kim, Melatonin: A potential therapeutic agent against COVID-19, Melatonin Res
Gurunathan, Qasim, Kang, Kim, Role and therapeutic potential of melatonin in various type of cancers, Onco Targets Ther
Han, Wang, Li, Li, Ge et al., Melatonin protects against maternal obesity-associated oxidative stress and meiotic defects in oocytes via the SIRT3-SOD2-dependent pathway, J Pineal Res
Hardeland, Balzer, Poeggeler, Fuhrberg, Uría et al., On the primary functions of melatonin in evolution: Mediation of photoperiodic signals in a unicell, photooxidation, and scavenging of free radicals, J Pineal Res
Hardeland, Cardinali, Brown, Sr, Melatonin and brain inflammaging, Prog Neurobiol
Hardeland, Reiter, Poeggeler, Tan, The significance of the metabolism of the neurohormone melatonin: Antioxidative protection and formation of bioactive substances, Neurosci Biobehav Rev
Hasan, Islam, Matsumoto, Kawai, Meta-analysis of single-cell RNA-seq data reveals phenotypic switching of immune cells in severe COVID-19 patients, Comput Biol Med
Hayes, Sculthorpe, More than 100 persistent symptoms of SARS-CoV-2 (long COVID): A scoping review, Front Med
Hazra, Chaudhuri, Tiwary, Chakrabarti, Matrix metallopeptidase 9 as a host protein target of chloroquine and melatonin for immunoregulation in COVID-19: A network-based meta-analysis, Life Sci
He, Wang, Zhang, Yang, Li et al., Mitochondria synthesize melatonin to ameliorate its function and improve mice oocyte's quality under in vitro conditions, Int J Mol Sci
Hosseini, Gouvarchin Ghaleh, Aghamollaei, Ramandi, Alishiri et al., Evaluation of Th1 and Th2 mediated cellular and humoral immunity in patients with COVID-19 following the use of melatonin as an adjunctive treatment, Eur J Pharmacol
Hosseinzadeh, Bagherifard, Koosha, Amiri, Karimi-Behnagh et al., Melatonin effect on platelets and coagulation: Implications for a prophylactic indication in COVID-19, Life Sci
Huang, Huang, Wang, Li, Ren et al., 6-Month consequences of COVID-19 in patients discharged from hospital: A cohort study, Lancet
Huang, Li, Gu, Zhang, Ren et al., Health outcomes in people 2 years after surviving hospitalisation with COVID-19: A longitudinal cohort study, Lancet Respir Med
Huang, Wu, Liu, Tsai, Chen et al., The clinical efficacy of melatonin in the treatment of patients with COVID-19: A systematic review and meta-analysis of randomized controlled trials, Front Med
Hui, Azhar, Madani, Ntoumi, Kock et al., The continuing 2019-nCoV epidemic threat of novel coronaviruses to global health-the latest 2019 novel coronavirus outbreak in Wuhan, China, Int J Infect Dis
Juybari, Pourhanifeh, Hosseinzadeh, Hemati, Mehrzadi, Melatonin potentials against viral infections including COVID-19: Current evidence and new findings, Virus Res
Kaivola, Nyman, Matikainen, Inflammasomes and SARS-CoV-2 infection, Viruses
Kalkeri, Goebel, Sharma, SARS-CoV-2 shedding from asymptomatic patients: Contribution of potential extrapulmonary tissue reservoirs, Am J Trop Med Hyg
Karlafti, Paramythiotis, Pantazi, Georgakopoulou, Kaiafa et al., Drug-induced liver injury in hospitalized patients during SARS-CoV-2 infection, Medicina
Klann, Bojkova, Tascher, Ciesek, Münch et al., Growth factor receptor signaling inhibition prevents SARS-CoV-2 replication, Mol Cell
Kong, Zhang, Liu, Li, Liu et al., Melatonin attenuates angiotensin II-induced abdominal aortic aneurysm through the down-regulation of matrix metalloproteinases, Oncotarget
Kucia, Ratajczak, Bujko, Adamiak, Ciechanowicz et al., An evidence that SARS-Cov-2/COVID-19 spike protein (SP) damages hematopoietic stem/progenitor cells in the mechanism of pyroptosis in Nlrp3 inflammasome-dependent manner, Leukemia
Legrand, Bell, Forni, Joannidis, Koyner et al., Pathophysiology of COVID-19-associated acute kidney injury, Nat Rev Nephrol
Lempesis, Apple, Duarte, Palaiodimos, Kalaitzopoulos et al., Cardiometabolic effects of SGLT2 inhibitors on polycystic ovary syndrome, Diabetes Metab Res Rev
Lempesis, Georgakopoulou, Papalexis, Chrousos, Da ; Gordijn et al., Characteristics and outcomes of elderly patients with Parkinson's disease hospitalized due to COVID-19-associated pneumonia, Med Int (Lond)
Lempesis, Hoebers, Essers, Jocken, Dineen et al., Distinct inflammatory signatures of upper and lower body adipose tissue and adipocytes in women with normal weight or obesity, Front Endocrinol
Lempesis, Karlafti, Papalexis, Fotakopoulos, Tarantinos et al., COVID-19 and liver injury in individuals with obesity, World J Gastroenterol
Lempesis, Tsilingiris, Liu, Dalamaga, Of mice and men: Considerations on adipose tissue physiology in animal models of obesity and human studies, Metabol Open
Lempesis, Varrias, Sagris, Attaran, Altin et al., Obesity and peripheral artery disease: Current evidence and controversies, Curr Obes Rep
Lempesis, Ve, Implications of obesity and adiposopathy on respiratory infections; focus on emerging challenges, World J Clin Cases
Lempesis, Ve, Physiopathological mechanisms related to inflammation in obesity and type 2 diabetes mellitus, World J Exp Med
Li, Ma, Yokota, Garcia, Jr et al., Metabolic reprogramming and epigenetic changes of vital organs in SARS-CoV-2-induced systemic toxicity, JCI insight
Li, Ying, Cai, Yang, Wu, Exogenous melatonin alleviates hemorrhagic shock-induced hepatic ischemic injury in rats by inhibiting the NF-κB/IκBα signaling pathway, Mol Med Rep
Lipsitch, Krammer, Regev-Yochay, Lustig, Balicer, SARS-CoV-2 breakthrough infections in vaccinated individuals: Measurement, causes and impact, Nat Rev Immunol
Loh, Reiter, Melatonin: Regulation of viral phase separation and epitranscriptomics in post-acute sequelae of COVID-19, Int J Mol Sci
Long, Brady, Koyfman, Gottlieb, Cardiovascular complications in COVID-19, Am J Emerg Med
Luo, Song, Zhang, Zhang, Liu et al., Melatonin mediated Foxp3-downregulation decreases cytokines production via the TLR2 and TLR4 pathways in H. pylori infected mice, Int Immunopharmacol
Ma R T Í N M, Macía S M, Esca Mes G, L E Ón J A Nd Acuña-Castroviejo, Melatonin but not vitamins C and E maintains glutathione homeostasis in t-butyl hydroperoxide-induced mitochondrial oxidative stress, FASEB J
Madjid, Safavi-Naeini, Sd, Vardeny, Potential effects of coronaviruses on the cardiovascular system: A review, JAMA Cardiol
Maldonado, García-Moreno, Yanes, Calvo, Possible involvement of the inhibition of NF-κB factor in anti-inflammatory actions that melatonin exerts on mast cells, J Cell Biochem
Maldonado, Mora-Santos, Naji, Carrascosa-Salmoral, Naranjo et al., Evidence of melatonin synthesis and release by mast cells. Possible modulatory role on inflammation, Pharmacol Res
Manchester, Coto-Montes, Boga, Andersen, Zhou et al., Melatonin: An ancient molecule that makes oxygen metabolically tolerable, J Pineal Res
Manik, Singh, Role of toll-like receptors in modulation of cytokine storm signaling in SARS-CoV-2-induced COVID-19, J Med Virol
Marchi, Guilbaud, Tait, Yamazaki, Galluzzi, West AP and Shadel GS: Mitochondrial DNA in innate immune responses and inflammatory pathology, Nat Rev Immunol
Martin, Macias, Escames, Reiter, Agapito et al., Melatonin-induced increased activity of the respiratory chain complexes I and IV can prevent mitochondrial damage induced by ruthenium red in vivo, J Pineal Res
Mathioudakis, Zachiotis, Papadakos, Triantafyllou, Karapanou et al., Onodera's prognostic nutritional index: Comparison of its role in the severity and outcomes of patients with COVID-19 during the periods of alpha, delta and omicron variant predominance, Exp Ther Med
Mauriz, Collado, Veneroso, Reiter, A review of the molecular aspects of melatonin's anti-inflammatory actions: Recent insights and new perspectives, J Pineal Res
Mayo, Sainz, Menéndez, Cepas, Tan et al., Melatonin and sirtuins: A 'not-so unexpected' relationship, J Pineal Res
Medini, Zirman, Mishmar, Immune system cells from COVID-19 patients display compromised mitochondrial-nuclear expression co-regulation and rewiring toward glycolysis, iScience
Mehandru, Merad, Pathological sequelae of long-haul COVID, Nat Immunol
Mehrzadi, Karimi, Fatemi, Reiter, Hosseinzadeh, SARS-CoV-2 and other coronaviruses negatively influence mitochondrial quality control: Beneficial effects of melatonin, Pharmacol Ther
Miller, Silverstein, Flores, Cao, Kumagai et al., Host mitochondrial transcriptome response to SARS-CoV-2 in multiple cell models and clinical samples, Sci Rep
Mirza-Aghazadeh-Attari, Reiter, Rikhtegar, Jalili, Hajalioghli et al., Melatonin: An atypical hormone with major functions in the regulation of angiogenesis, IUBMB Life
Morchang, Malakar, Poonudom, Noisakran, Yenchitsomanus et al., Melatonin inhibits dengue virus infection via the sirtuin 1-mediated interferon pathway, Viruses
Mouffak, Shubbar, Saleh, El-Awady, Recent advances in management of COVID-19: A review, Biomed Pharmacother
Mousavi, Heydari, Mehravaran, Saeedi, Alizadeh-Navaei et al., Melatonin effects on sleep quality and outcomes of COVID-19 patients: An open-label, randomized, controlled trial, J Med Virol
Muxel, Pires-Lapa, Monteiro, Cecon, Tamura et al., NF-κB drives the synthesis of melatonin in RAW 264.7 macrophages by inducing the transcription of the arylalkylamine-N-acetyltransferase (AA-NAT) gene, PLoS One
Naskar, Prabhakar, Singh, Dutta, Mohanakumar, Melatonin enhances L-DOPA therapeutic effects, helps to reduce its dose, and protects dopaminergic neurons in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-induced Parkinsonism in mice, J Pineal Res
Ozdemir, Ergün, Bakariş, Kılınç, Durdu et al., Melatonin prevents retinal oxidative stress and vascular changes in diabetic rats, Eye (Lond)
Ozkurt, Tanrıverdi, COVID-19: Gastrointestinal manifestations, liver injury and recommendations, World J Clin Cases
Papadopoulou, Karavalakis, Papadopoulou, Xochelli, Bousiou et al., SARS-CoV-2-specific T cell therapy for severe COVID-19: a randomized phase 1/2 trial, Nat Med
Peluso, Deeks, Mustapic, Kapogiannis, Henrich et al., Marginal BH4 deficiencies, iNOS, and self-perpetuating oxidative stress in post-acute sequelae of Covid-19, Med Hypotheses
Pourhanifeh, Mehrzadi, Kamali, Hosseinzadeh, Melatonin and gastrointestinal cancers: Current evidence based on underlying signaling pathways, Eur J Pharmacol
Proal, Vanelzakker, Long COVID or post-acute sequelae of COVID-19 (PASC): An overview of biological factors that may contribute to persistent symptoms, Front Microbiol
Qin, Liu, Sun, Li, Xu et al., Protective effects of melatonin on the white matter damage of neonatal rats by regulating NLRP3 inflammasome activity, Neuroreport
Quaglia, Salladini, Carraro, Minervini, Tosatto et al., SARS-CoV-2 variants preferentially emerge at intrinsically disordered protein sites helping immune evasion, FEBS J
Quintana, Contreras-Omana, Auron, Liver dysfunction and SARS-CoV-2 infection, World J Gastroenterol
Ramos, López-Muñoz, Gil-Martín, Egea, Álvarez-Merz et al., The coronavirus disease 2019 (COVID-19): key emphasis on melatonin safety and therapeutic efficacy, Antioxidants
Ramos, Patiño, Reiter, Gil-Martín, Marco-Contelles et al., Ischemic brain injury: New insights on the protective role of melatonin, Free Radic Biol Med
Reiter, Abreu-Gonzalez, Marik, Dominguez-Rodriguez, Therapeutic algorithm for use of melatonin in patients with COVID-19, Front Med
Reiter, Cardinali, Neel, Rodriguez, Brown et al., Rationale for the continued use of melatonin to combat the delta variant of SARS-CoV-2, Melatonin Res
Reiter, Ma, Sharma, Melatonin in mitochondria: Mitigating clear and present dangers, Physiology (Bethesda)
Reiter, Ma, Sharma, Treatment of Ebola and other infectious diseases: Melatonin 'goes viral, Melatonin Res
Reiter, Mayo, Tan, Sainz, Jimenez et al., Melatonin as an antioxidant: Under promises but over delivers, J Pineal Res
Reiter, Pineal melatonin: Cell biology of its synthesis and of its physiological interactions, Endocr Rev
Reiter, Rosales-Corral, Tan, Acuna-Castroviejo, Qin et al., Melatonin, a full service anti-cancer agent: inhibition of initiation, progression and metastasis, Int J Mol Sci
Reiter, Rosales-Corral, Tan, Jou, Galano et al., Melatonin as a mitochondria-targeted antioxidant: One of evolution's best ideas, Cell Mol Life Sci
Reiter, Sharma, Ma, Dominquez-Rodriguez, Marik et al., Melatonin inhibits COVID-19-induced cytokine storm by reversing aerobic glycolysis in immune cells: A mechanistic analysis, Med Drug Discov
Reiter, Sharma, Ma, Liu, Manucha et al., Metabolic plasticity of activated immune cells: Advantages for suppression of COVID-19 disease by melatonin, Melatonin Res
Reiter, Sharma, Rosales-Corral, Zuccari, De Almeida Chuffa, Melatonin: A mitochondrial resident with a diverse skill set, Life Sci
Reiter, Sharma, Simko, Dominguez-Rodriguez, Tesarik et al., Melatonin: Highlighting its use as a potential treatment for SARS-CoV-2 infection, Cell Mol Life Sci
Reiter, Sharma, Tan, Neel, Simko et al., Melatonin use for SARS-CoV-2 infection: Time to diversify the treatment portfolio, J Med Virol
Reiter, Tan, Galano, Melatonin: Exceeding expectations, Physiology (Bethesda)
Reiter, Tan, Kim, Qi, Melatonin as a pharmacological agent against oxidative damage to lipids and DNA, Proc West Pharmacol Soc
Reiter, Tan, Korkmaz, The circadian melatonin rhythm and its modulation: Possible impact on hypertension, J Hypertens Suppl
Reiter, Tan, Paredes, Fuentes-Broto, Beneficial effects of melatonin in cardiovascular disease, Ann Med
Reiter, Tan, Rosales-Corral, Galano, Jou et al., Melatonin mitigates mitochondrial meltdown: Interactions with SIRT3, Int J Mol Sci
Reiter, Tan, Rosales-Corral, Manchester, The universal nature, unequal distribution and antioxidant functions of melatonin and its derivatives, Mini Rev Med Chem
Ren, Sun, Li, Chen, Ge et al., Exogenous melatonin inhibits neutrophil migration through suppression of ERK activation, J Endocrinol
Rodriguez, Mayo, Sainz, Antolín, Herrera et al., Regulation of antioxidant enzymes: A significant role for melatonin, J Pineal Res
Romero, Ramos, López-Muñoz, Gil-Martín, Escames et al., Coronavirus disease 2019 (COVID-19) and its neuroinvasive capacity: Is it time for melatonin?, Cell Mol Neurobiol
Saleh, Peyssonnaux, Singh, Edeas, Mitochondria and microbiota dysfunction in COVID-19 pathogenesis, Mitochondrion
Sanchez-Barcelo, Rueda, Mediavilla, Martinez-Cue, Reiter, Clinical uses of melatonin in neurological diseases and mental and behavioural disorders, Curr Med Chem
Sarkar, Chattopadhyay, Bandyopadhyay, Multiple strategies of melatonin protecting against cardiovascular injury related to inflammation: A comprehensive overview, Melatonin Res
Schreiner, Harrer, Scheibenbogen, Lamer, Schlosser et al., Human herpesvirus-6 reactivation, mitochondrial fragmentation, and the coordination of antiviral and metabolic phenotypes in myalgic encephalomyelitis/chronic fatigue syndrome, Immunohorizons
Sheleme, Bekele, Ayela, Clinical presentation of patients infected with coronavirus disease 19: A systematic review, Infect Dis (Auckl)
Shukla, Htoo, Wintachai, Hernandez, Dubois et al., Melatonin stimulates the nonamyloidogenic processing of βAPP through the positive transcriptional regulation of ADAM10 and ADAM17, J Pineal Res
Simko, Baka, Paulis, Reiter, Elevated heart rate and nondipping heart rate as potential targets for melatonin: A review, J Pineal Res
Simko, Hrenak, Dominguez-Rodriguez, Reiter, Melatonin as a putative protection against myocardial injury in COVID-19 infection, Expert Rev Clin Pharmacol
Singh, Chaubey, Chen, Suravajhala, Decoding SARS-CoV-2 hijacking of host mitochondria in COVID-19 pathogenesis, Am J Physiol Cell Physiol
Slominski, Reiter, Schlabritz-Loutsevitch, Ostrom, Slominski, Melatonin membrane receptors in peripheral tissues: Distribution and functions, Mol Cell Endocrinol
Stukalov, Girault, Grass, Karayel, Bergant et al., Multilevel proteomics reveals host perturbations by SARS-CoV-2 and SARS-CoV, Nature
Su, Yuan, Chen, Ng, Wang et al., Multiple early factors anticipate post-acute COVID-19 sequelae, Cell
Suofu, Li, Fg, Jia, Khattar et al., Dual role of mitochondria in producing melatonin and driving GPCR signaling to block cytochrome c release, Proc Natl Acad Sci
Taha, Saed, Moawad, El-Tawab Moawad, Al-Hejazi et al., Safety and efficacy of melatonin as an adjuvant therapy in COVID-19 patients: Systematic review and meta-analysis, Adv Med Sci
Tan, Hardeland, Manchester, Paredes, Korkmaz et al., The changing biological roles of melatonin during evolution: From an antioxidant to signals of darkness, sexual selection and fitness, Biol Rev Camb Philos Soc
Tan, Hardeland, Manchester, Poeggeler, Lopez-Burillo et al., Mechanistic and comparative studies of melatonin and classic antioxidants in terms of their interactions with the ABTS cation radical, J Pineal Res
Tan, Hardeland, Targeting host defense system and rescuing compromised mitochondria to increase tolerance against pathogens by melatonin may impact outcome of deadly virus infection pertinent to COVID-19, Braz J Infect Dis
Tan, Korkmaz, Reiter, Manchester, Ebola virus disease: Potential use of melatonin as a treatment, J Pineal Res
Tan, Manchester, Terron, Flores, Reiter, One molecule, many derivatives: A never-ending interaction of melatonin with reactive oxygen and nitrogen species?, J Pineal Res
Tan, Reiter, Mechanisms and clinical evidence to support melatonin's use in severe COVID-19 patients to lower mortality, Life Sci
Tan, Reiter, Melatonin reduces the mortality of severely-infected COVID-19 patients, Melatonin Res
Taskou, Sarantaki, Beloukas, Georgakopoulou, Daskalakis et al., Knowledge and attitudes of healthcare professionals regarding perinatal influenza vaccination during the COVID-19 pandemic, Vaccines
Thakur, Ratho, Kumar, Bhatia, Bora et al., Multi-organ involvement in COVID-19: Beyond pulmonary manifestations, J Clin Med
Thaweethai, Jolley, Karlson, Levitan, Levy et al., Development of a definition of postacute sequelae of SARS-CoV-2 infection, JAMA
Tian, Liu, Li, Zhao, Shereen et al., HIF-1α promotes SARS-CoV-2 infection and aggravates inflammatory responses to COVID-19, Signal Transduct Target Ther
Vehar, Boushra, Ntiamoah, Biehl, Post-acute sequelae of SARS-CoV-2 infection: Caring for the 'long-haulers, Cleve Clin J Med
Venegas, García, Escames, Ortiz, López et al., Extrapineal melatonin: Analysis of its subcellular distribution and daily fluctuations, J Pineal Res
Vriend, Reiter, Melatonin as a proteasome inhibitor. Is there any clinical evidence?, Life Sci
Vriend, Reiter, Melatonin feedback on clock genes: A theory involving the proteasome, J Pineal Res
Wakatsuki, Okatani, Shinohara, Ikenoue, Kaneda et al., Melatonin protects fetal rat brain against oxidative mitochondrial damage, J Pineal Res
Wang, Chen, Zhang, Deng, Lian et al., CD147-spike protein is a novel route for SARS-CoV-2 infection to host cells, Signal Transduct Target Ther
Wang, Hu, Hu, Zhu, Liu et al., Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China, JAMA
Wang, Luo, Zhang, Wang, Song et al., A cross-talk between epithelium and endothelium mediates human alveolar-capillary injury during SARS-CoV-2 infection, Cell Death Dis
Wichniak, Kania, Siemiński, Cubała, Melatonin as a potential adjuvant treatment for COVID-19 beyond sleep disorders, Int J Mol Sci
Xu, Wang, Ai, Shi, Zhang et al., Melatonin suppresses TLR9-triggered proinflammatory cytokine production in macrophages by inhibiting ERK1/2 and AKT activation, Sci Rep
Zhai, Wang, Jiao, Zhang, Li et al., Melatonin and other indoles show antiviral activities against swine coronaviruses in vitro at pharmacological concentrations, Melatonin Res
Zhang, Li, Grailer, Wang, Wang et al., Melatonin alleviates acute lung injury through inhibiting the NLRP3 inflammasome, J Pineal Res
Zhang, Xiang, Huo, Zhou, Jiang et al., Molecular mechanism of interaction between SARS-CoV-2 and host cells and interventional therapy, Signal Transduct Target Ther
Zipeto, Palmeira, Argañaraz, Argañaraz, ACE2/ADAM17/TMPRSS2 interplay may be the main risk factor for COVID-19, Front Immunol
Zlacká, Stebelová, Zeman, Herichová, Interactions of renin-angiotensin system and COVID-19: The importance of daily rhythms in ACE2, ADAM17 and TMPRSS2 expression, Physiol Res
Zubchenko, Kril, Nadizhko, Matsyura, Chopyak, Herpesvirus infections and post-COVID-19 manifestations: A pilot observational study, Rheumatol Int
Öi, Im, Impaired diffusing capacity for carbon monoxide is common in critically ill Covid-19 patients at four months post-discharge, Respir Med
DOI record:
{
"DOI": "10.3892/ijmm.2024.5352",
"ISSN": [
"1107-3756",
"1791-244X"
],
"URL": "http://dx.doi.org/10.3892/ijmm.2024.5352",
"article-number": "28",
"author": [
{
"affiliation": [
{
"name": "Department of Pathophysiology, Laiko General Hospital, National and Kapodistrian University of Athens, 11527 Athens, Greece"
}
],
"family": "Lempesis",
"given": "Ioannis",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Department of Pathophysiology, Laiko General Hospital, National and Kapodistrian University of Athens, 11527 Athens, Greece"
}
],
"family": "Georgakopoulou",
"given": "Vasiliki",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Cellular and Structural Biology, UT Health Science Center, San Antonio, TX 78229, USA"
}
],
"family": "Reiter",
"given": "Russel",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Laboratory of Clinical Virology, School of Medicine, University of Crete, 71003 Heraklion, Greece"
}
],
"family": "Spandidos",
"given": "Demetrios",
"sequence": "additional"
}
],
"container-title": "International Journal of Molecular Medicine",
"container-title-short": "Int J Mol Med",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2024,
1,
26
]
],
"date-time": "2024-01-26T10:15:43Z",
"timestamp": 1706264143000
},
"deposited": {
"date-parts": [
[
2024,
1,
26
]
],
"date-time": "2024-01-26T10:15:44Z",
"timestamp": 1706264144000
},
"indexed": {
"date-parts": [
[
2024,
1,
27
]
],
"date-time": "2024-01-27T00:08:27Z",
"timestamp": 1706314107630
},
"is-referenced-by-count": 0,
"issue": "3",
"issued": {
"date-parts": [
[
2024,
1,
26
]
]
},
"journal-issue": {
"issue": "3",
"published-online": {
"date-parts": [
[
2024,
1,
26
]
]
}
},
"member": "2249",
"original-title": [],
"prefix": "10.3892",
"published": {
"date-parts": [
[
2024,
1,
26
]
]
},
"published-online": {
"date-parts": [
[
2024,
1,
26
]
]
},
"publisher": "Spandidos Publications",
"reference-count": 0,
"references-count": 0,
"relation": {},
"resource": {
"primary": {
"URL": "http://www.spandidos-publications.com/10.3892/ijmm.2024.5352"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Genetics",
"General Medicine"
],
"subtitle": [],
"title": "A mid‑pandemic night's dream: Melatonin, from harbinger of anti‑inflammation to mitochondrial savior in acute and long COVID‑19 (Review)",
"type": "journal-article",
"volume": "53"
}
