Effect of colchicine on mortality in patients with COVID-19 – A systematic review and meta-analysis
et al., Diabetes & Metabolic Syndrome: Clinical Research & Reviews, doi:10.1016/j.dsx.2022.102395, Jan 2022
Colchicine for COVID-19
5th treatment shown to reduce risk in
September 2020, now with p = 0.0000049 from 54 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
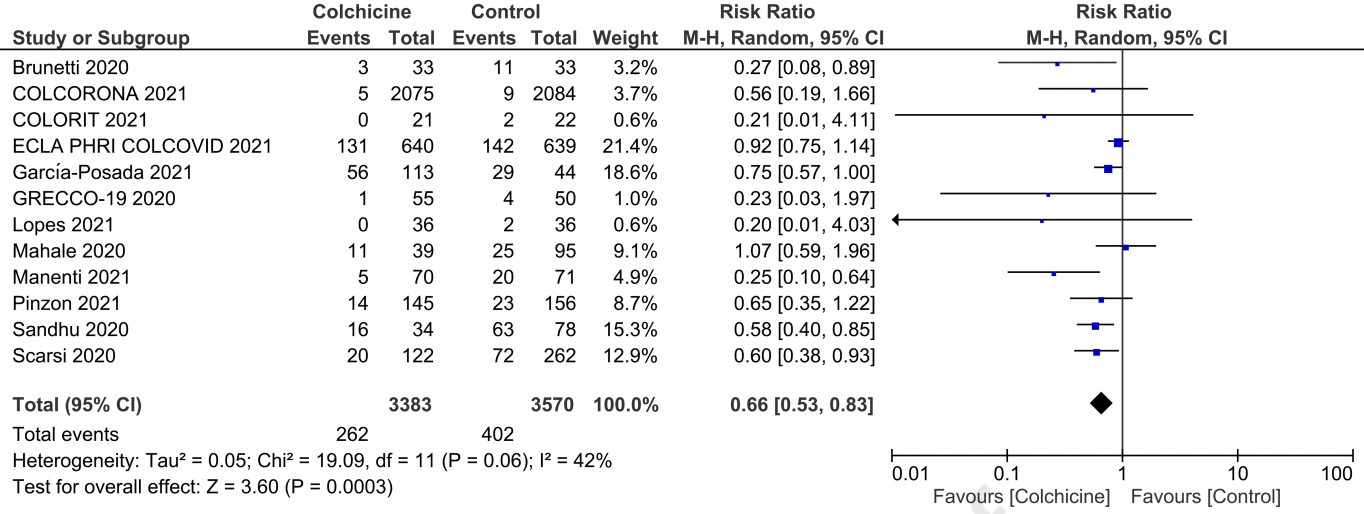
Systematic review and meta analysis showing that colchicine was associated with lower mortality in COVID-19 patients:
All studies: RR 0.66 [95%CI 0.53, 0.83], p < 0.001; I2: 42%
RCTs: RR 0.81 [95%CI 0.54, 1.20], p = 0.29; I2: 10%
RCTs: RR 0.81 [95%CI 0.54, 1.20], p = 0.29; I2: 10%
The RCT result is non-significant, but is highly affected by the very late stage RECOVERY trial, which is not generalizable to earlier usage.
10 meta-analyses show significant improvements with colchicine for mortality1-8,
oxygen therapy8,
hospitalization9, and
severity10.
Currently there are 54 colchicine for COVID-19 studies, showing 22% lower mortality [12‑31%], 29% lower ventilation [-15‑56%], 34% lower ICU admission [8‑52%], 17% lower hospitalization [9‑25%], and 9% more cases [-8‑29%].
1.
Zein et al., Effect of colchicine on mortality in patients with COVID-19 – A systematic review and meta-analysis, Diabetes & Metabolic Syndrome: Clinical Research & Reviews, doi:10.1016/j.dsx.2022.102395.
2.
Rai et al., The Potential Role of Colchicine in Reducing Mortality and Mechanical Ventilation Rates in COVID-19 Infection: A Meta-analysis, Journal of Advances in Medicine and Medical Research, doi:10.9734/jammr/2022/v34i2031503.
3.
Elshafei et al., Colchicine use might be associated with lower mortality in COVID‐19 patients: A meta‐analysis, European Journal of Clinical Investigation, doi:10.1111/eci.13645.
4.
Lien et al., Repurposing Colchicine in Treating Patients with COVID-19: A Systematic Review and Meta-Analysis, Life, doi:10.3390/life11080864.
5.
Danjuma et al., Does Colchicine Reduce Mortality in Patients with Covid-19 Clinical Syndrome? An Umbrella Review of Published Meta-Analyses, Elsevier BV, doi:10.2139/ssrn.4447127.
6.
Salah et al., Meta-analysis of the Effect of Colchicine on Mortality and Mechanical Ventilation in COVID-19, The American Journal of Cardiology, doi:10.1016/j.amjcard.2021.02.005.
7.
Golpour et al., The effectiveness of Colchicine as an anti-inflammatory drug in the treatment of coronavirus disease 2019: Meta-analysis, International Journal of Immunopathology and Pharmacology, doi:10.1177/20587384211031763.
8.
Elshiwy et al., The role of colchicine in the management of COVID-19: a meta-analysis, BMC Pulmonary Medicine, doi:10.1186/s12890-024-03001-0.
Zein et al., 12 Jan 2022, peer-reviewed, 2 authors.
Effect of colchicine on mortality in patients with COVID-19 – A systematic review and meta-analysis
Diabetes & Metabolic Syndrome: Clinical Research & Reviews, doi:10.1016/j.dsx.2022.102395
This is a PDF file of an article that has undergone enhancements after acceptance, such as the addition of a cover page and metadata, and formatting for readability, but it is not yet the definitive version of record. This version will undergo additional copyediting, typesetting and review before it is published in its final form, but we are providing this version to give early visibility of the article. Please note that, during the production process, errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
References
Akbar, Pranata, Wibowo, Lim, Sihite et al., The prognostic value of elevated creatine kinase to predict poor outcome in patients with COVID-19 -A systematic review and meta-analysis: Creatinine Kinase in COVID-19, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2021.02.012
Akbar, Wibowo, Pranata, Setiabudiawan, Low Serum 25-hydroxyvitamin D (Vitamin D) Level Is Associated With Susceptibility to COVID-19, Severity, and Mortality: A Systematic Review and Meta-Analysis, Front Nutr, doi:10.3389/fnut.2021.660420
Ben-Chetrit, Levy, Does the lack of the P-glycoprotein efflux pump in neutrophils explain the efficacy of colchicine in familial Mediterranean fever and other inflammatory diseases?, Med Hypotheses, doi:10.1016/S0306-9877(98)90031-7J
Bhattacharyya, Panda, Gupta, Banerjee, Anti-mitotic activity of colchicine and the structural basis for its interaction with tubulin, Med Res Rev, doi:10.1002/med.20097
Brunetti, Diawara, Tsai, Colchicine to Weather the Cytokine Storm in Hospitalized Patients with COVID-19, J Clin Med, doi:10.3390/jcm9092961
Dalal, Hui, Bidaut, Relationships Among Body Mass Index, Longitudinal Body Composition Alterations, and Survival in Patients With Locally Advanced Pancreatic Cancer Receiving Chemoradiation: A Pilot Study, J Pain Symptom Manage, doi:10.1016/j.jpainsymman.2011.09.010
Deftereos, Giannopoulos, Vrachatis, Effect of Colchicine vs Standard Care on Cardiac and Inflammatory Biomarkers and Clinical Outcomes in Patients Hospitalized With Coronavirus Disease 2019: The GRECCO-19 Randomized Clinical Trial, JAMA Netw open, doi:10.1001/jamanetworkopen.2020.13136
Diaz, Orlandini, Castellana, Effect of Colchicine vs Usual Care Alone on Intubation and 28-Day Mortality in Patients Hospitalized With COVID-19: A Randomized Clinical Trial, JAMA Netw open, doi:10.1001/jamanetworkopen.2021.41328
García-Posada, Vesga, Mestra, Clinical outcomes of patients hospitalized for COVID-19 and evidence-based on the pharmacological management reduce mortality in a region of the Colombian Caribbean, J Infect Public Health, doi:10.1016/j.jiph.2021.02.013
Higgins, Altman, Gøtzsche, The Cochrane Collaboration's tool for assessing risk of bias in randomised trials, BMJ, doi:10.1136/bmj.d5928
Huang, Lim, Pranata, Diabetes mellitus is associated with increased mortality and severity of disease in COVID-19 pneumonia -A systematic review, meta-analysis, and meta-regression: Diabetes and COVID-19, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2020.04.018
Huang, Pranata, Lymphopenia in severe coronavirus disease-2019 (COVID-19): Systematic review and meta-analysis, J Intensive Care, doi:10.1186/s40560-020-00453-4
J O U R N A L P R E, -p r o o f
J O U R N A L P R E, -p r o o f
J O U R N A L P R E, -p r o o f
J O U R N A L P R E, -p r o o f
J O U R N A L P R E, -p r o o f
Jn, Cason, Currey, Prolonged reduction in polymorphonuclear adhesion following oral colchicine, Ann Rheum Dis, doi:10.1136/ard.40.6.605
July, Pranata, Impact of the Coronavirus Disease Pandemic on the Number of Strokes and Mechanical Thrombectomies: A Systematic Review and Meta-Analysis, J Stroke Cerebrovasc Dis, doi:10.1016/j.jstrokecerebrovasdis.2020.105185
July, Pranata, Prevalence of dementia and its impact on mortality in patients with coronavirus disease 2019: A systematic review and meta-analysis, Geriatr Gerontol Int, doi:10.1111/ggi.14107
Kuswardhani, Henrina, Pranata, Lim, Lawrensia et al., Charlson comorbidity index and a composite of poor outcomes in COVID-19 patients: A systematic review and meta-analysis, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2020.10.022
Leung, Hui, Kraus, Colchicine--Update on mechanisms of action and therapeutic uses, Semin Arthritis Rheum, doi:10.1016/J.SEMARTHRIT.2015.06.013
Lim, Pranata, Huang, Yonas, Soeroto et al., Multiorgan Failure With Emphasis on Acute Kidney Injury and Severity of COVID-19: Systematic Review and Meta-Analysis, Can J Kidney Heal Dis, doi:10.1177/2054358120938573
Lopes, Bonjorno, Giannini, Beneficial effects of colchicine for moderate to severe COVID-19: A randomised, double-blinded, placebo-controlled clinical trial, RMD Open, doi:10.1136/rmdopen-2020-001455
Lukito, Pranata, Henrina, Lim, Lawrensia et al., The Effect of Metformin Consumption on Mortality in Hospitalized COVID-19 patients: a systematic review and meta-analysis, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2020.11.006
Manenti, Maggiore, Fiaccadori, Reduced mortality in COVID-19 patients treated with colchicine: Results from a retrospective, observational study, PLoS One, doi:10.1371/journal.pone.0248276
Mareev, Orlova, Plisyk, Proactive anti-inflammatory therapy with J o u r n a l P r e -p r o o f colchicine in the treatment of advanced stages of new coronavirus infection. The first results of the COLORIT study, Kardiologiya, doi:10.18087/CARDIO.2021.2.N1560
Martha, Pranata, Lim, Wibowo, Akbar, Active prescription of low-dose aspirin during or prior to hospitalization and mortality in COVID-19: A systematic review and meta-analysis of adjusted effect estimates, Int J Infect Dis, doi:10.1016/j.ijid.2021.05.016
Martha, Pranata, Wibowo, Lim, Tricuspid annular plane systolic excursion (TAPSE) measured by echocardiography and mortality in COVID-19: A systematic review and meta-analysis, Int J Infect Dis, doi:10.1016/j.ijid.2021.02.029
Martha, Wibowo, Pranata, Prognostic value of elevated lactate dehydrogenase in patients with COVID-19: A systematic review and meta-analysis, Postgrad Med J. Published online, doi:10.1136/postgradmedj-2020-139542
Martínez, Celermajer, Patel, The NLRP3 inflammasome and the emerging role of colchicine to inhibit atherosclerosis-associated inflammation, Atherosclerosis, doi:10.1016/j.atherosclerosis.2017.12.027
Milewska, Nowak, Owczarek, Entry of Human Coronavirus NL63 into the Cell, J Virol, doi:10.1128/JVI.01933-17
Pinzón, Doris Cardona Arango, Betancur, Arias, Muñoz et al., Clinical Outcome of Patients with COVID-19 Pneumonia Treated with Corticosteroids and Colchicine in Colombia, Res Sq. Published online, doi:10.21203/rs.3.rs-94922/v1
Pranata, Henrina, Lim, Clinical frailty scale and mortality in COVID-19: A systematic review and dose-response meta-analysis: Clinical Frailty Scale in COVID-19, Arch Gerontol Geriatr, doi:10.1016/j.archger.2020.104324
Pranata, Henrina, Raffaello, Lawrensia, Huang, Diabetes and COVID-19: The past, the present, and the future, Metabolism, doi:10.1016/j.metabol.2021.154814
Pranata, Huang, Lawrensia, Proton pump inhibitor on susceptibility to COVID-19 and its severity: a systematic review and meta-analysis, Pharmacol Reports, doi:10.1007/s43440-021-00263-x
Pranata, Huang, Lim, Elevated De Ritis Ratio Is Associated With Poor Prognosis in COVID-19: A Systematic Review and Meta-Analysis, Front Med, doi:10.3389/fmed.2021.676581
Pranata, Huang, Lim, Wahjoepramono, July, Impact of cerebrovascular and cardiovascular diseases on mortality and severity of COVID-19-systematic review, metaanalysis, and meta-regression, J Stroke Cerebrovasc Dis, doi:10.1016/j.jstrokecerebrovasdis.2020.104949
Pranata, Huang, Lim, Yonas, Vania et al., Delirium and Mortality in Coronavirus Disease 2019 (COVID-19) -A Systematic Review and Meta-analysis, Arch Gerontol Geriatr, doi:10.1016/j.archger.2021.104388
Pranata, Huang, Lukito, Raharjo, Elevated N-Terminal pro-brain natriuretic peptide is associated with increased mortality in patients with COVID-19: Systematic review and meta-Analysis, Postgrad Med J, doi:10.1136/postgradmedj-2020-137884
Pranata, Huang, Raharjo, Incidence and impact of cardiac arrhythmias in coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis, Indian Pacing Electrophysiol J, doi:10.1016/j.ipej.2020.08.001
Pranata, Lim, Huang, Raharjo, Lukito, Hypertension is associated with increased mortality and severity of disease in COVID-19 pneumonia: A systematic review, meta-analysis and meta-regression. JRAAS -J Renin-Angiotensin, -Aldosterone Syst, doi:10.1177/1470320320926899
Pranata, Lim, Huang, Visceral adiposity, subcutaneous adiposity, and severe coronavirus disease-2019 (COVID-19): Systematic review and meta-analysis, Clin Nutr ESPEN, doi:10.1016/j.clnesp.2021.04.001
Pranata, Lim, Yonas, Body Mass Index and Outcome in Patients with COVID-19: A Dose-Response Meta-Analysis, Diabetes Metab, doi:10.1016/j.diabet.2020.07.005
Pranata, Lim, Yonas, Siswanto, Meyer, Out-of-hospital cardiac arrest prognosis during the COVID-19 pandemic, Intern Emerg Med, doi:10.1007/s11739-020-02428-7
Pranata, Lim, Yonas, Thrombocytopenia as a prognostic marker in COVID-19 patients: Diagnostic test accuracy meta-analysis, Epidemiol Infect, doi:10.1017/S0950268821000236
Pranata, Permana, Huang, The use of renin angiotensin system inhibitor on mortality in patients with coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2020.06.047
Pranata, Soeroto, Huang, Effect of chronic obstructive pulmonary disease and smoking on the outcome of COVID-19, Int J Tuberc Lung Dis, doi:10.5588/ijtld.20.0278
Pranata, Yonas, Huang, Lim, Nasution et al., Fibrosis-4 index and mortality in coronavirus disease 2019: a meta-analysis, Eur J Gastroenterol Hepatol
Purandare, Rajhans, Jog, A Retrospective Observational Study of Hypoxic COVID-19 Patients Treated with Immunomodulatory Drugs in a Tertiary Care Hospital, Indian J Crit Care Med, doi:10.5005/jp-journals-10071-23599
Raffaello, Huang, Siswanto, Pranata, In-depth review of cardiopulmonary support in COVID-19 patients with heart failure, World J Cardiol, doi:10.4330/wjc.v13.i8.298
Rakhmat, Kusmala, Handayani, Dipeptidyl peptidase-4 (DPP-4) inhibitor and mortality in coronavirus disease 2019 (COVID-19) -A systematic review, meta-analysis, and meta-regression, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2021.03.027
Reyes, Hu, Teperman, Anti-inflammatory therapy for COVID-19 infection: The case for colchicine, Ann Rheum Dis, doi:10.1136/annrheumdis-2020-219174
Richter, Boldescu, Graf, Synthesis, Biological Evaluation, and Molecular Docking of Combretastatin and Colchicine Derivatives and their hCE1-Activated Prodrugs as Antiviral Agents, ChemMedChem, doi:10.1002/CMDC.201800641
Sandhu, Tieng, Chilimuri, Franchin, A case control study to evaluate the impact of J o u r n a l P r e -p r o o f colchicine on patients admitted to the hospital with moderate to severe covid-19 infection, Can J Infect Dis Med Microbiol, doi:10.1155/2020/8865954
Sawicki, Sawicki, Siddell, A contemporary view of coronavirus transcription, J Virol, doi:10.1128/JVI.01358-06
Scarsi, Piantoni, Colombo, Association between treatment with colchicine and improved survival in a single-centre cohort of adult hospitalised patients with COVID-19 pneumonia and acute respiratory distress syndrome, Ann Rheum Dis, doi:10.1136/annrheumdis-2020-217712
Schlesinger, Firestein, Brunetti, Colchicine in COVID-19: an Old Drug, New Use, Curr Pharmacol Reports, doi:10.1007/s40495-020-00225-6
Siemieniuk, Bartoszko, Ge, Drug treatments for covid-19: Living systematic review and network meta-Analysis, BMJ, doi:10.1136/bmj.m2980
Sutandyo, Kurniawati, Jayusman, Syafiyah, Pranata et al., Repurposing FIB-4 index as a predictor of mortality in patients with hematological malignancies and COVID-19, PLoS One, doi:10.1371/journal.pone.0257775
Tardif, Bouabdallaoui, Allier, Efficacy of Colchicine in Non-Hospitalized Patients with COVID-19
Wells, Shea, Connell, Peterson, The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses
Wibowo, Pranata, Akbar, Purnomowati, Martha, Prognostic performance of troponin in COVID-19: A diagnostic meta-analysis and meta-regression, Int J Infect Dis, doi:10.1016/j.ijid.2021.02.113
Wibowo, Pranata, Astuti, Left and right ventricular longitudinal strains are associated with poor outcome in COVID-19: a systematic review and meta-analysis, J Intensive Care, doi:10.1186/s40560-020-00519-3
Yonas, Alwi, Pranata, Effect of heart failure on the outcome of COVID-19 -A meta analysis and systematic review, Am J Emerg Med. Published, doi:10.1016/j.ajem.2020.07.009
Yonas, Alwi, Pranata, Effect of heart failure on the outcome of COVID-19 -A meta analysis and systematic review, Am J Emerg Med. Published, doi:10.1016/j.ajem.2020.07.009
Yonas, Alwi, Pranata, Elevated interleukin levels are associated with higher severity and mortality in COVID 19 -A systematic review, meta-analysis, and metaregression, Diabetes Metab Syndr Clin Res Rev, doi:10.1016/j.dsx.2020.11.011
Zein, Sulistiyana, Khasanah, Wibowo, Lim et al., Statin and mortality in COVID-19: a systematic review and meta-analysis of pooled adjusted effect estimates from propensity-matched cohorts, Postgrad Med J. Published online, doi:10.1136/postgradmedj-2021-140409
DOI record:
{
"DOI": "10.1016/j.dsx.2022.102395",
"ISSN": [
"1871-4021"
],
"URL": "http://dx.doi.org/10.1016/j.dsx.2022.102395",
"alternative-id": [
"S1871402122000091"
],
"article-number": "102395",
"author": [
{
"ORCID": "http://orcid.org/0000-0001-7821-3813",
"affiliation": [],
"authenticated-orcid": false,
"family": "Zein",
"given": "Ahmad Fariz Malvi Zamzam",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-4086-1492",
"affiliation": [],
"authenticated-orcid": false,
"family": "Raffaello",
"given": "Wilson Matthew",
"sequence": "additional"
}
],
"container-title": [
"Diabetes & Metabolic Syndrome: Clinical Research & Reviews"
],
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2022,
1,
12
]
],
"date-time": "2022-01-12T02:47:05Z",
"timestamp": 1641955625000
},
"deposited": {
"date-parts": [
[
2022,
1,
12
]
],
"date-time": "2022-01-12T02:47:42Z",
"timestamp": 1641955662000
},
"indexed": {
"date-parts": [
[
2022,
1,
12
]
],
"date-time": "2022-01-12T03:15:18Z",
"timestamp": 1641957318414
},
"is-referenced-by-count": 0,
"issn-type": [
{
"type": "print",
"value": "1871-4021"
}
],
"issued": {
"date-parts": [
[
2022,
1
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
1,
1
]
],
"date-time": "2022-01-01T00:00:00Z",
"timestamp": 1640995200000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S1871402122000091?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S1871402122000091?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "102395",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2022,
1
]
]
},
"published-print": {
"date-parts": [
[
2022,
1
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1007/s11739-020-02428-7",
"article-title": "Out-of-hospital cardiac arrest prognosis during the COVID-19 pandemic",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "875",
"issue": "5",
"journal-title": "Intern Emerg Med",
"key": "10.1016/j.dsx.2022.102395_bib1",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1016/j.jstrokecerebrovasdis.2020.105185",
"article-title": "Impact of the coronavirus disease pandemic on the number of strokes and mechanical thrombectomies: a systematic review and meta-analysis",
"author": "July",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "J Stroke Cerebrovasc Dis",
"key": "10.1016/j.dsx.2022.102395_bib2",
"volume": "29",
"year": "2020"
},
{
"article-title": "Drug treatments for covid-19: living systematic review and network meta-Analysis",
"author": "Siemieniuk",
"journal-title": "BMJ",
"key": "10.1016/j.dsx.2022.102395_bib3",
"volume": "370",
"year": "2020"
},
{
"DOI": "10.1016/j.ijid.2021.05.016",
"article-title": "Active prescription of low-dose aspirin during or prior to hospitalization and mortality in COVID-19: a systematic review and meta-analysis of adjusted effect estimates",
"author": "Martha",
"doi-asserted-by": "crossref",
"first-page": "6",
"journal-title": "Int J Infect Dis",
"key": "10.1016/j.dsx.2022.102395_bib4",
"volume": "108",
"year": "2021"
},
{
"DOI": "10.1136/postgradmedj-2021-140409",
"article-title": "Statin and mortality in COVID-19: a systematic review and meta-analysis of pooled adjusted effect estimates from propensity-matched cohorts",
"author": "Zein",
"doi-asserted-by": "crossref",
"journal-title": "Postgrad Med J",
"key": "10.1016/j.dsx.2022.102395_bib5",
"year": "2021"
},
{
"DOI": "10.1016/j.dsx.2021.03.027",
"article-title": "Dipeptidyl peptidase-4 (DPP-4) inhibitor and mortality in coronavirus disease 2019 (COVID-19) – a systematic review, meta-analysis, and meta-regression",
"author": "Rakhmat",
"doi-asserted-by": "crossref",
"first-page": "777",
"issue": "3",
"journal-title": "Diabetes Metab Syndr Clin Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib6",
"volume": "15",
"year": "2021"
},
{
"key": "10.1016/j.dsx.2022.102395_bib7",
"unstructured": "Colchicine (marketed as colcrys) information | FDA."
},
{
"DOI": "10.1007/s40495-020-00225-6",
"article-title": "Colchicine in COVID-19: an old drug, new use",
"author": "Schlesinger",
"doi-asserted-by": "crossref",
"first-page": "137",
"issue": "4",
"journal-title": "Curr Pharmacol Reports",
"key": "10.1016/j.dsx.2022.102395_bib8",
"volume": "6",
"year": "2020"
},
{
"DOI": "10.1016/j.semarthrit.2015.06.013",
"article-title": "Colchicine--Update on mechanisms of action and therapeutic uses",
"author": "Leung",
"doi-asserted-by": "crossref",
"first-page": "341",
"issue": "3",
"journal-title": "Semin Arthritis Rheum",
"key": "10.1016/j.dsx.2022.102395_bib9",
"volume": "45",
"year": "2015"
},
{
"DOI": "10.1016/j.jiph.2021.02.013",
"article-title": "Clinical outcomes of patients hospitalized for COVID-19 and evidence-based on the pharmacological management reduce mortality in a region of the Colombian Caribbean",
"author": "García-Posada",
"doi-asserted-by": "crossref",
"first-page": "696",
"issue": "6",
"journal-title": "J Infect Publ Health",
"key": "10.1016/j.dsx.2022.102395_bib10",
"volume": "14",
"year": "2021"
},
{
"article-title": "Reduced mortality in COVID-19 patients treated with colchicine: results from a retrospective, observational study",
"author": "Manenti",
"first-page": "1",
"issue": "3 March",
"journal-title": "PLoS One",
"key": "10.1016/j.dsx.2022.102395_bib11",
"volume": "16",
"year": "2021"
},
{
"author": "Wells",
"key": "10.1016/j.dsx.2022.102395_bib12",
"series-title": "The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses",
"year": "2000"
},
{
"article-title": "The Cochrane Collaboration's tool for assessing risk of bias in randomised trials",
"author": "Higgins",
"issue": "7829",
"journal-title": "BMJ",
"key": "10.1016/j.dsx.2022.102395_bib13",
"volume": "343",
"year": "2011"
},
{
"DOI": "10.18087/cardio.2021.2.n1560",
"article-title": "Proactive anti-inflammatory therapy with colchicine in the treatment of advanced stages of new coronavirus infection. The first results of the COLORIT study",
"author": "Mareev",
"doi-asserted-by": "crossref",
"first-page": "15",
"issue": "2",
"journal-title": "Kardiologiya",
"key": "10.1016/j.dsx.2022.102395_bib14",
"volume": "61",
"year": "2021"
},
{
"DOI": "10.1001/jamanetworkopen.2021.41328",
"article-title": "Effect of colchicine vs usual care alone on intubation and 28-day mortality in patients hospitalized with COVID-19: a randomized clinical trial",
"author": "Diaz",
"doi-asserted-by": "crossref",
"issue": "12",
"journal-title": "JAMA Netw Open",
"key": "10.1016/j.dsx.2022.102395_bib15",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.1136/rmdopen-2020-001455",
"article-title": "Beneficial effects of colchicine for moderate to severe COVID-19: a randomised, double-blinded, placebo-controlled clinical trial",
"author": "Lopes",
"doi-asserted-by": "crossref",
"issue": "1",
"journal-title": "RMD Open",
"key": "10.1016/j.dsx.2022.102395_bib16",
"volume": "7",
"year": "2021"
},
{
"DOI": "10.5005/jp-journals-10071-23599",
"article-title": "A retrospective observational study of hypoxic COVID-19 patients treated with immunomodulatory drugs in a tertiary care hospital",
"author": "Purandare",
"doi-asserted-by": "crossref",
"first-page": "1020",
"issue": "11",
"journal-title": "Indian J Crit Care Med",
"key": "10.1016/j.dsx.2022.102395_bib17",
"volume": "24",
"year": "2020"
},
{
"article-title": "Clinical outcome of patients with COVID-19 pneumonia treated with corticosteroids and colchicine in Colombia",
"author": "Alejandro Pinzón",
"first-page": "1",
"journal-title": "Res Sq",
"key": "10.1016/j.dsx.2022.102395_bib18",
"year": "2020"
},
{
"author": "Tardif",
"key": "10.1016/j.dsx.2022.102395_bib19",
"series-title": "Efficacy of colchicine in non-hospitalized patients with COVID-19. MedRxiv",
"year": "2021"
},
{
"DOI": "10.1155/2020/8865954",
"article-title": "A case control study to evaluate the impact of colchicine on patients admitted to the hospital with moderate to severe covid-19 infection",
"author": "Sandhu",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Can J Infect Dis Med Microbiol",
"key": "10.1016/j.dsx.2022.102395_bib20",
"volume": "2020",
"year": "2020"
},
{
"DOI": "10.3390/jcm9092961",
"article-title": "Colchicine to weather the cytokine storm in hospitalized patients with COVID-19",
"author": "Brunetti",
"doi-asserted-by": "crossref",
"first-page": "2961",
"issue": "9",
"journal-title": "J Clin Med",
"key": "10.1016/j.dsx.2022.102395_bib21",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1136/annrheumdis-2020-217712",
"article-title": "Association between treatment with colchicine and improved survival in a single-centre cohort of adult hospitalised patients with COVID-19 pneumonia and acute respiratory distress syndrome",
"author": "Scarsi",
"doi-asserted-by": "crossref",
"first-page": "1286",
"issue": "10",
"journal-title": "Ann Rheum Dis",
"key": "10.1016/j.dsx.2022.102395_bib22",
"volume": "79",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2020.13136",
"article-title": "Effect of colchicine vs standard care on cardiac and inflammatory biomarkers and clinical outcomes in patients hospitalized with coronavirus disease 2019: the GRECCO-19 randomized clinical trial",
"author": "Deftereos",
"doi-asserted-by": "crossref",
"issue": "6",
"journal-title": "JAMA Netw Open",
"key": "10.1016/j.dsx.2022.102395_bib23",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1016/j.jstrokecerebrovasdis.2020.104949",
"article-title": "Impact of cerebrovascular and cardiovascular diseases on mortality and severity of COVID-19–systematic review, meta-analysis, and meta-regression",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "104949",
"issue": "8",
"journal-title": "J Stroke Cerebrovasc Dis",
"key": "10.1016/j.dsx.2022.102395_bib24",
"volume": "29",
"year": "2020"
},
{
"article-title": "Effect of heart failure on the outcome of COVID-19 — a meta analysis and systematic review",
"author": "Yonas",
"journal-title": "Am J Emerg Med",
"key": "10.1016/j.dsx.2022.102395_bib25",
"year": "2020"
},
{
"DOI": "10.1111/ggi.14107",
"article-title": "Prevalence of dementia and its impact on mortality in patients with coronavirus disease 2019: a systematic review and meta-analysis",
"author": "July",
"doi-asserted-by": "crossref",
"first-page": "172",
"issue": "2",
"journal-title": "Geriatr Gerontol Int",
"key": "10.1016/j.dsx.2022.102395_bib26",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1016/j.dsx.2020.10.022",
"article-title": "Charlson comorbidity index and a composite of poor outcomes in COVID-19 patients: a systematic review and meta-analysis",
"author": "Tuty Kuswardhani",
"doi-asserted-by": "crossref",
"first-page": "2103",
"issue": "6",
"journal-title": "Diabetes Metab Syndr Clin Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib27",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/j.clnesp.2021.04.001",
"article-title": "Visceral adiposity, subcutaneous adiposity, and severe coronavirus disease-2019 (COVID-19): systematic review and meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "163",
"journal-title": "Clin Nutr ESPEN",
"key": "10.1016/j.dsx.2022.102395_bib28",
"volume": "43",
"year": "2021"
},
{
"article-title": "Body Mass index and outcome in patients with COVID-19: a dose-response meta-analysis",
"author": "Pranata",
"journal-title": "Diabetes Metab",
"key": "10.1016/j.dsx.2022.102395_bib29",
"year": "2020"
},
{
"DOI": "10.5588/ijtld.20.0278",
"article-title": "Effect of chronic obstructive pulmonary disease and smoking on the outcome of COVID-19",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "838",
"issue": "8",
"journal-title": "Int J Tubercul Lung Dis",
"key": "10.1016/j.dsx.2022.102395_bib30",
"volume": "24",
"year": "2020"
},
{
"article-title": "Low serum 25-hydroxyvitamin D (vitamin D) level is associated with susceptibility to COVID-19, severity, and mortality: a systematic review and meta-analysis",
"author": "Akbar",
"journal-title": "Front Nutr",
"key": "10.1016/j.dsx.2022.102395_bib31",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.1016/j.archger.2020.104324",
"article-title": "Clinical frailty scale and mortality in COVID-19: a systematic review and dose-response meta-analysis: clinical Frailty Scale in COVID-19",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "104324",
"journal-title": "Arch Gerontol Geriatr",
"key": "10.1016/j.dsx.2022.102395_bib32",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.1016/j.dsx.2020.06.047",
"article-title": "The use of renin angiotensin system inhibitor on mortality in patients with coronavirus disease 2019 (COVID-19): a systematic review and meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "983",
"issue": "5",
"journal-title": "Diabetes Metab Syndr Clin Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib33",
"volume": "14",
"year": "2020"
},
{
"article-title": "Hypertension is associated with increased mortality and severity of disease in COVID-19 pneumonia: a systematic review, meta-analysis and meta-regression",
"author": "Pranata",
"issue": "2",
"journal-title": "JRAAS - J Renin-Angiotensin-Aldosterone Syst.",
"key": "10.1016/j.dsx.2022.102395_bib34",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1016/j.metabol.2021.154814",
"article-title": "Diabetes and COVID-19: the past, the present, and the future",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "154814",
"journal-title": "Metabolism",
"key": "10.1016/j.dsx.2022.102395_bib35",
"volume": "121",
"year": "2021"
},
{
"DOI": "10.1016/j.dsx.2020.04.018",
"article-title": "Diabetes mellitus is associated with increased mortality and severity of disease in COVID-19 pneumonia – a systematic review, meta-analysis, and meta-regression: diabetes and COVID-19",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "395",
"issue": "4",
"journal-title": "Diabetes Metab Syndr Clin Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib36",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.11.006",
"article-title": "The effect of metformin consumption on mortality in hospitalized COVID-19 patients: a systematic review and meta-analysis",
"author": "Lukito",
"doi-asserted-by": "crossref",
"first-page": "2177",
"issue": "6",
"journal-title": "Diabetes Metab Syndr Clin Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib37",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1007/s43440-021-00263-x",
"article-title": "Proton pump inhibitor on susceptibility to COVID-19 and its severity: a systematic review and meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "1642",
"issue": "6",
"journal-title": "Pharmacol Rep",
"key": "10.1016/j.dsx.2022.102395_bib38",
"volume": "73",
"year": "2021"
},
{
"DOI": "10.1136/annrheumdis-2020-219174",
"article-title": "Anti-inflammatory therapy for COVID-19 infection: the case for colchicine",
"author": "Reyes",
"doi-asserted-by": "crossref",
"first-page": "550",
"issue": "5",
"journal-title": "Ann Rheum Dis",
"key": "10.1016/j.dsx.2022.102395_bib39",
"volume": "80",
"year": "2021"
},
{
"DOI": "10.1002/med.20097",
"article-title": "Anti-mitotic activity of colchicine and the structural basis for its interaction with tubulin",
"author": "Bhattacharyya",
"doi-asserted-by": "crossref",
"first-page": "155",
"issue": "1",
"journal-title": "Med Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib40",
"volume": "28",
"year": "2008"
},
{
"DOI": "10.1002/cmdc.201800641",
"article-title": "Synthesis, biological evaluation, and molecular docking of combretastatin and colchicine derivatives and their hCE1-activated prodrugs as antiviral agents",
"author": "Richter",
"doi-asserted-by": "crossref",
"first-page": "469",
"issue": "4",
"journal-title": "ChemMedChem",
"key": "10.1016/j.dsx.2022.102395_bib41",
"volume": "14",
"year": "2019"
},
{
"DOI": "10.1128/JVI.01358-06",
"article-title": "A contemporary view of coronavirus transcription",
"author": "Sawicki",
"doi-asserted-by": "crossref",
"first-page": "20",
"issue": "1",
"journal-title": "J Virol",
"key": "10.1016/j.dsx.2022.102395_bib42",
"volume": "81",
"year": "2007"
},
{
"DOI": "10.1128/JVI.01933-17",
"article-title": "Entry of human coronavirus NL63 into the cell",
"author": "Milewska",
"doi-asserted-by": "crossref",
"issue": "3",
"journal-title": "J Virol",
"key": "10.1016/j.dsx.2022.102395_bib43",
"volume": "92",
"year": "2018"
},
{
"DOI": "10.1016/S0306-9877(98)90031-7",
"article-title": "Does the lack of the P-glycoprotein efflux pump in neutrophils explain the efficacy of colchicine in familial Mediterranean fever and other inflammatory diseases?",
"author": "Ben-Chetrit",
"doi-asserted-by": "crossref",
"first-page": "377",
"issue": "5",
"journal-title": "Med Hypotheses",
"key": "10.1016/j.dsx.2022.102395_bib44",
"volume": "51",
"year": "1998"
},
{
"DOI": "10.1016/j.jpainsymman.2011.09.010",
"article-title": "Relationships among Body Mass index, longitudinal Body composition alterations, and survival in patients with locally advanced pancreatic cancer receiving chemoradiation: a pilot study",
"author": "Dalal",
"doi-asserted-by": "crossref",
"first-page": "181",
"issue": "2",
"journal-title": "J Pain Symptom Manag",
"key": "10.1016/j.dsx.2022.102395_bib45",
"volume": "44",
"year": "2012"
},
{
"DOI": "10.1016/j.atherosclerosis.2017.12.027",
"article-title": "The NLRP3 inflammasome and the emerging role of colchicine to inhibit atherosclerosis-associated inflammation",
"author": "Martínez",
"doi-asserted-by": "crossref",
"first-page": "262",
"journal-title": "Atherosclerosis",
"key": "10.1016/j.dsx.2022.102395_bib46",
"volume": "269",
"year": "2018"
},
{
"DOI": "10.1136/ard.40.6.605",
"article-title": "Prolonged reduction in polymorphonuclear adhesion following oral colchicine",
"author": "Fordham",
"doi-asserted-by": "crossref",
"first-page": "605",
"issue": "6",
"journal-title": "Ann Rheum Dis",
"key": "10.1016/j.dsx.2022.102395_bib47",
"volume": "40",
"year": "1981"
},
{
"article-title": "Multiorgan failure with emphasis on acute kidney injury and severity of COVID-19: systematic review and meta-analysis",
"author": "Lim",
"journal-title": "Can J Kidney Heal Dis",
"key": "10.1016/j.dsx.2022.102395_bib48",
"volume": "7",
"year": "2020"
},
{
"article-title": "Effect of heart failure on the outcome of COVID-19 — a meta analysis and systematic review",
"author": "Yonas",
"journal-title": "Am J Emerg Med",
"key": "10.1016/j.dsx.2022.102395_bib49",
"year": "2020"
},
{
"DOI": "10.1017/S0950268821000236",
"article-title": "Thrombocytopenia as a prognostic marker in COVID-19 patients: diagnostic test accuracy meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"journal-title": "Epidemiol Infect",
"key": "10.1016/j.dsx.2022.102395_bib50",
"year": "2021"
},
{
"DOI": "10.1016/j.archger.2021.104388",
"article-title": "Delirium and mortality in coronavirus disease 2019 (COVID-19) – a systematic review and meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"journal-title": "Arch Gerontol Geriatr",
"key": "10.1016/j.dsx.2022.102395_bib51",
"volume": "95",
"year": "2021"
},
{
"DOI": "10.1016/j.ijid.2021.02.029",
"article-title": "Tricuspid annular plane systolic excursion (TAPSE) measured by echocardiography and mortality in COVID-19: a systematic review and meta-analysis",
"author": "Martha",
"doi-asserted-by": "crossref",
"first-page": "351",
"issue": "1",
"journal-title": "Int J Infect Dis",
"key": "10.1016/j.dsx.2022.102395_bib52",
"volume": "105",
"year": "2021"
},
{
"DOI": "10.1016/j.ipej.2020.08.001",
"article-title": "Incidence and impact of cardiac arrhythmias in coronavirus disease 2019 (COVID-19): a systematic review and meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "193",
"issue": "5",
"journal-title": "Indian Pacing Electrophysiol J",
"key": "10.1016/j.dsx.2022.102395_bib53",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1136/postgradmedj-2020-137884",
"article-title": "Elevated N-Terminal pro-brain natriuretic peptide is associated with increased mortality in patients with COVID-19: systematic review and meta-Analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"first-page": "387",
"issue": "1137",
"journal-title": "Postgrad Med",
"key": "10.1016/j.dsx.2022.102395_bib54",
"volume": "96",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.11.011",
"article-title": "Elevated interleukin levels are associated with higher severity and mortality in COVID 19 – a systematic review, meta-analysis, and meta-regression",
"author": "Yonas",
"doi-asserted-by": "crossref",
"first-page": "2219",
"issue": "6",
"journal-title": "Diabetes Metab Syndr Clin Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib55",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1136/postgradmedj-2020-139542",
"article-title": "Prognostic value of elevated lactate dehydrogenase in patients with COVID-19: a systematic review and meta-analysis",
"author": "Martha",
"doi-asserted-by": "crossref",
"journal-title": "Postgrad Med",
"key": "10.1016/j.dsx.2022.102395_bib56",
"year": "2021"
},
{
"DOI": "10.1186/s40560-020-00453-4",
"article-title": "Lymphopenia in severe coronavirus disease-2019 (COVID-19): systematic review and meta-analysis",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "36",
"issue": "1",
"journal-title": "J Intens Care",
"key": "10.1016/j.dsx.2022.102395_bib57",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1097/MEG.0000000000002091",
"article-title": "Fibrosis-4 index and mortality in coronavirus disease 2019: a meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"journal-title": "Eur J Gastroenterol Hepatol",
"key": "10.1016/j.dsx.2022.102395_bib58",
"year": "2021"
},
{
"article-title": "Repurposing FIB-4 index as a predictor of mortality in patients with hematological malignancies and COVID-19",
"author": "Sutandyo",
"issue": "9 September",
"journal-title": "PLoS One",
"key": "10.1016/j.dsx.2022.102395_bib59",
"volume": "16",
"year": "2021"
},
{
"DOI": "10.3389/fmed.2021.676581",
"article-title": "Elevated de ritis ratio is associated with poor prognosis in COVID-19: a systematic review and meta-analysis",
"author": "Pranata",
"doi-asserted-by": "crossref",
"journal-title": "Front Med",
"key": "10.1016/j.dsx.2022.102395_bib60",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.1016/j.dsx.2021.02.012",
"article-title": "The prognostic value of elevated creatine kinase to predict poor outcome in patients with COVID-19 - a systematic review and meta-analysis: creatinine Kinase in COVID-19",
"author": "Akbar",
"doi-asserted-by": "crossref",
"first-page": "529",
"issue": "2",
"journal-title": "Diabetes Metab Syndr Clin Res Rev",
"key": "10.1016/j.dsx.2022.102395_bib61",
"volume": "15",
"year": "2021"
},
{
"DOI": "10.4330/wjc.v13.i8.298",
"article-title": "In-depth review of cardiopulmonary support in COVID-19 patients with heart failure",
"author": "Raffaello",
"doi-asserted-by": "crossref",
"first-page": "298",
"issue": "8",
"journal-title": "World J Cardiol",
"key": "10.1016/j.dsx.2022.102395_bib62",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1016/j.ijid.2021.02.113",
"article-title": "Prognostic performance of troponin in COVID-19: a diagnostic meta-analysis and meta-regression",
"author": "Wibowo",
"doi-asserted-by": "crossref",
"first-page": "312",
"journal-title": "Int J Infect Dis",
"key": "10.1016/j.dsx.2022.102395_bib63",
"volume": "105",
"year": "2021"
},
{
"DOI": "10.1186/s40560-020-00519-3",
"article-title": "Left and right ventricular longitudinal strains are associated with poor outcome in COVID-19: a systematic review and meta-analysis",
"author": "Wibowo",
"doi-asserted-by": "crossref",
"first-page": "9",
"issue": "1",
"journal-title": "J Intens Care",
"key": "10.1016/j.dsx.2022.102395_bib64",
"volume": "9",
"year": "2021"
}
],
"reference-count": 64,
"references-count": 64,
"relation": {},
"score": 1,
"short-container-title": [
"Diabetes & Metabolic Syndrome: Clinical Research & Reviews"
],
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine",
"Endocrinology, Diabetes and Metabolism",
"Internal Medicine"
],
"subtitle": [],
"title": [
"Effect of colchicine on mortality in patients with COVID-19 – A systematic review and meta-analysis"
],
"type": "journal-article"
}
