Remdesivir may exacerbate ischemic acute kidney injury through molecular alterations in PGC-1α and apoptosis pathways: An in vivo study
et al., PLOS One, doi:10.1371/journal.pone.0336221, Feb 2026
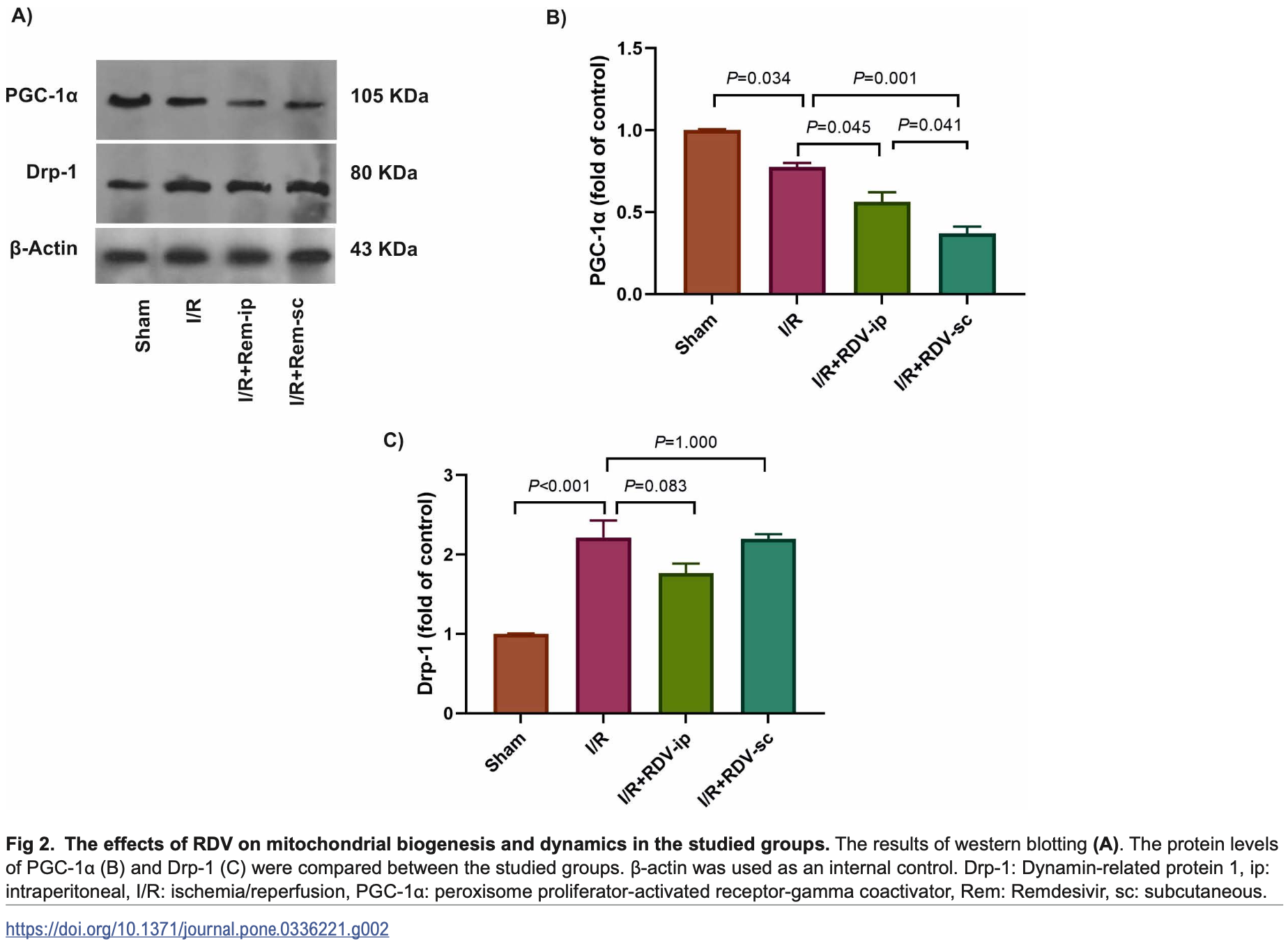
Animal study (rat model) showing potential harm of remdesivir in ischemia/reperfusion-induced acute kidney injury. Authors found that subcutaneous RDV significantly decreased PGC-1α expression - a master regulator of mitochondrial biogenesis - and significantly increased caspase-3, suggesting enhanced apoptosis.
Gérard, Zhou, Wu, Kamo, Choi, Kim show increased risk of acute kidney injury, Leo, Briciu, Muntean, Petrov, Arch show increased risk of liver injury, Negru, Cheng, Mohammed, Kwok, Zhu show increased risk of cardiac disorders, and Kwok, Merches, Akinci, Tang, Bagheri show increased risk of mitochondrial toxicity with remdesivir.
1.
Gérard et al., Remdesivir and Acute Renal Failure: A Potential Safety Signal From Disproportionality Analysis of the WHO Safety Database, Clinical Pharmacology & Therapeutics, doi:10.1002/cpt.2145.
2.
Zhou et al., Acute Kidney Injury and Drugs Prescribed for COVID-19 in Diabetes Patients: A Real-World Disproportionality Analysis, Frontiers in Pharmacology, doi:10.3389/fphar.2022.833679.
3.
Wu et al., Acute Kidney Injury Associated With Remdesivir: A Comprehensive Pharmacovigilance Analysis of COVID-19 Reports in FAERS, Frontiers in Pharmacology, doi:10.3389/fphar.2022.692828.
4.
Kamo et al., Association of Antiviral Drugs for the Treatment of COVID-19 With Acute Renal Failure, In Vivo, doi:10.21873/invivo.13637.
5.
Choi et al., Comparative effectiveness of combination therapy with nirmatrelvir–ritonavir and remdesivir versus monotherapy with remdesivir or nirmatrelvir–ritonavir in patients hospitalised with COVID-19: a target trial emulation study, The Lancet Infectious Diseases, doi:10.1016/S1473-3099(24)00353-0.
6.
Kim et al., Investigating the Safety Profile of Fast‐Track COVID‐19 Drugs Using the FDA Adverse Event Reporting System Database: A Comparative Observational Study, Pharmacoepidemiology and Drug Safety, doi:10.1002/pds.70043.
7.
Leo et al., Hepatocellular liver injury in hospitalized patients affected by COVID-19: Presence of different risk factors at different time points, Digestive and Liver Disease, doi:10.1016/j.dld.2021.12.014.
8.
Briciu et al., Evolving Clinical Manifestations and Outcomes in COVID-19 Patients: A Comparative Analysis of SARS-CoV-2 Variant Waves in a Romanian Hospital Setting, Pathogens, doi:10.3390/pathogens12121453.
9.
Muntean et al., Effects of COVID-19 on the Liver and Mortality in Patients with SARS-CoV-2 Pneumonia Caused by Delta and Non-Delta Variants: An Analysis in a Single Centre, Pharmaceuticals, doi:10.3390/ph17010003.
10.
Petrov et al., The Effect of Potentially Hepatotoxic Medicinal Products on Alanine Transaminase Levels in COVID-19 Patients: A Case–Control Study, Safety and Risk of Pharmacotherapy, doi:10.30895/2312-7821-2025-458.
11.
Arch et al., Evaluation of the effectiveness of remdesivir in treating severe COVID-19 using data from the ISARIC WHO Clinical Characterisation Protocol UK: a prospective, national cohort study, medRxiv, doi:10.1101/2021.06.18.21259072.
12.
Negru et al., Comparative Pharmacovigilance Analysis of Approved and Repurposed Antivirals for COVID-19: Insights from EudraVigilance Data, Biomedicines, doi:10.3390/biomedicines13061387.
13.
Cheng et al., Cardiovascular Safety of COVID-19 Treatments: A Disproportionality Analysis of Adverse Event Reports from the WHO VigiBase, Infectious Diseases and Therapy, doi:10.1007/s40121-025-01225-z.
14.
Mohammed et al., Bradycardia associated with remdesivir treatment in coronavirus disease 2019 patients: A propensity score-matched analysis, Medicine, doi:10.1097/MD.0000000000044501.
15.
Kwok et al., Remdesivir induces persistent mitochondrial and structural damage in human induced pluripotent stem cell-derived cardiomyocytes, Cardiovascular Research, doi:10.1093/cvr/cvab311.
16.
Zhu et al., Cardiovascular Risks of COVID-19 Therapeutics: Integrated Analysis of FAERS, Electronic Health Records, and Transcriptomics, Pharmaceuticals, doi:10.3390/ph19040574.
17.
Merches et al., The potential of remdesivir to affect function, metabolism and proliferation of cardiac and kidney cells in vitro, Archives of Toxicology, doi:10.1007/s00204-022-03306-1.
18.
Akinci et al., Elucidation of remdesivir cytotoxicity pathways through genome-wide CRISPR-Cas9 screening and transcriptomics, bioRxiv, doi:10.1101/2020.08.27.270819.
Bagheri et al., 12 Feb 2026, peer-reviewed, 9 authors.
Contact: sepide.zununi@gmail.com, zununivahed@tbzmed.ac.ir.
Abstract:
Citation: Bagheri Y, Malekinejad Z, Hejazian SM, Abdollahpour A, Khajepour F , Farahbod M, et al. (2026) Remdesivir may exacerbate ischemic acute kidney injury through molecular alterations in PGC-1 α and apoptosis pathways: An in vivo study. PLoS One 21(2): e0336221.
[https://doi.org/10.1371/journal.pone.0336221](https://doi.org/10.1371/journal.pone.0336221)
Editor: Otávio Augusto Chaves, University of Coimbra: Universidade de Coimbra, PORTUGAL
Received:
July 22, 2025
Accepted:
October 22, 2025
Published:
February 12, 2026
Copyright: © 2026 Bagheri et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Data availability statement : All relevant data are within the manuscript and its Supporting Information files.
Funding: This work was financially supported by Tabriz University of Medical Sciences, Tabriz, Iran (Grant No. 71236).
RESEARCH ARTICLE
Remdesivir may exacerbate ischemic acute kidney injury through molecular alterations in PGC-1 α and apoptosis pathways: An in vivo study
Yasin Bagheri 1 , Zahra Malekinejad 2 , Seyyedeh Mina Hejazian 1 , Abdollah Abdollahpour 2 , Fatemeh Khajepour 3 , Mohaddeseh Farahbod 4 , Sama Ahmadi 3 , Samira Matin 5 , Sepideh Zununi Vahed 1 *
- 1 Kidney Research Center, Tabriz University of Medical Sciences, Tabriz, Iran, 2 Department of
Pathobiology, Faculty of Veterinary Medicine, Tabriz Branch, Islamic Azad University, Tabriz, Iran, 3 Faculty of Veterinary Medicine, Tabriz Branch, Islamic Azad University, Tabriz, Iran, 4 Department of Clinical Science, Faculty of Veterinary Medicine, Tabriz Branch, Islamic Azad University, Tabriz, Iran, 5 Faculty of Medicine, Tabriz University of Medical Sciences, Tabriz, Iran
* Sepide.zununi@gmail.com, zununivahed@tbzmed.ac.ir
Abstract
Acute kidney injury (AKI) represents a significant complication in patients with COVID-19. Although Remdesivir (RDV) has been shown to reduce viral loads and improve clinical outcomes, concerns persist regarding its safety in individuals with pre-existing kidney impairment. This study investigated the effects of RDV on a rat model of ischemia/reperfusion (I/R)-induced kidney damage. A total of 24 rats were divided randomly into four groups: (1) control, (2) I/R, (3) I/R + RDV by intraperitoneal (ip) injections, and (4) I/R + RDV by subcutaneous (sc) injection groups. Rats in groups 3 and 4 received a single dosage of RDV (25 mg/kg) one hour before I/R induction. The effect of RDV on master genes involved in the mitochondrial biogenesis [Peroxisome proliferator-activated receptor gamma coactivator (PGC-1 α )] and dynamics [Dynamin-related protein 1 (Drp-1)], cellular stress [Activating transcription factor 3 (ATF3)], inflammation [Nuclear factor kappa B (NFκ B)], cell death [p53, p21 (a cyclin-dependent kinase inhibitor), and caspase-3], as well as oxidant malondialdehyde (MDA) and antioxidant factors were evaluated. Moreover, renal function, along with histology assessments were studied. Significant reductions in mitochondrial biogenesis marker PGC-1 α ( P ≤ 0.04) and increases in caspase-3 ( P = 0.003) expression levels were observed in the I/R + RDV + sc group compared to the I/R group. Oxidative stress marker was elevated ( P = 0.016), while glutathione peroxidase (GPX) activity and total antioxidant capacity..
DOI record:
{
"DOI": "10.1371/journal.pone.0336221",
"ISSN": [
"1932-6203"
],
"URL": "http://dx.doi.org/10.1371/journal.pone.0336221",
"abstract": "<jats:p>\n Acute kidney injury (AKI) represents a significant complication in patients with COVID-19. Although Remdesivir (RDV) has been shown to reduce viral loads and improve clinical outcomes, concerns persist regarding its safety in individuals with pre-existing kidney impairment. This study investigated the effects of RDV on a rat model of ischemia/reperfusion (I/R)-induced kidney damage. A total of 24 rats were divided randomly into four groups: (1) control, (2) I/R, (3) I/R + RDV by intraperitoneal (ip) injections, and (4) I/R + RDV by subcutaneous (sc) injection groups. Rats in groups 3 and 4 received a single dosage of RDV (25 mg/kg) one hour before I/R induction. The effect of RDV on master genes involved in the mitochondrial biogenesis [Peroxisome proliferator-activated receptor gamma coactivator (PGC-1α)] and dynamics [Dynamin-related protein 1 (Drp-1)], cellular stress [Activating transcription factor 3 (ATF3)], inflammation [Nuclear factor kappa B (NF-κB)], cell death [p53, p21 (a cyclin-dependent kinase inhibitor), and caspase-3], as well as oxidant malondialdehyde (MDA) and antioxidant factors were evaluated. Moreover, renal function, along with histology assessments were studied. Significant reductions in mitochondrial biogenesis marker PGC-1α (\n <jats:italic>P</jats:italic>\n ≤ 0.04) and increases in caspase-3 (\n <jats:italic>P</jats:italic>\n = 0.003) expression levels were observed in the I/R + RDV + sc group compared to the I/R group. Oxidative stress marker was elevated (\n <jats:italic>P</jats:italic>\n = 0.016), while glutathione peroxidase (GPX) activity and total antioxidant capacity (TAC) were significantly decreased in the I/R + RDV + sc group (0.003 and 0.045, respectively). However, no significant changes were observed in p-p53, p-p21, NF-κB, or Drp-1 levels. Subcutaneous injection of RDV could induce more injury to the kidney compared to the intraperitoneal injection. These findings suggest that RDV may exacerbate AKI by hindering mitochondrial biogenesis and promoting renal cell apoptosis, without significantly affecting overall kidney function or histopathology. Clinically, these results highlight the need for caution when using RDV in patients with impaired renal function, especially during COVID-19 treatment.\n </jats:p>",
"author": [
{
"affiliation": [],
"family": "Bagheri",
"given": "Yasin",
"sequence": "first"
},
{
"affiliation": [],
"family": "Malekinejad",
"given": "Zahra",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Hejazian",
"given": "Seyyedeh Mina",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Abdollahpour",
"given": "Abdollah",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Khajepour",
"given": "Fatemeh",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Farahbod",
"given": "Mohaddeseh",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ahmadi",
"given": "Sama",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Matin",
"given": "Samira",
"sequence": "additional"
},
{
"ORCID": "https://orcid.org/0000-0003-0179-4562",
"affiliation": [],
"authenticated-orcid": true,
"family": "Zununi Vahed",
"given": "Sepideh",
"sequence": "additional"
}
],
"container-title": "PLOS One",
"container-title-short": "PLoS One",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"www.plosone.org"
]
},
"created": {
"date-parts": [
[
2026,
2,
12
]
],
"date-time": "2026-02-12T18:28:48Z",
"timestamp": 1770920928000
},
"deposited": {
"date-parts": [
[
2026,
2,
12
]
],
"date-time": "2026-02-12T18:28:56Z",
"timestamp": 1770920936000
},
"editor": [
{
"affiliation": [],
"family": "Chaves",
"given": "Otávio Augusto",
"sequence": "first"
}
],
"funder": [
{
"DOI": "10.13039/501100004366",
"award": [
"71236"
],
"award-info": [
{
"award-number": [
"71236"
]
}
],
"doi-asserted-by": "publisher",
"id": [
{
"asserted-by": "publisher",
"id": "10.13039/501100004366",
"id-type": "DOI"
}
],
"name": "Tabriz University of Medical Sciences"
}
],
"indexed": {
"date-parts": [
[
2026,
2,
12
]
],
"date-time": "2026-02-12T19:18:40Z",
"timestamp": 1770923920937,
"version": "3.50.1"
},
"is-referenced-by-count": 0,
"issue": "2",
"issued": {
"date-parts": [
[
2026,
2,
12
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2026,
2,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "http://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2026,
2,
12
]
],
"date-time": "2026-02-12T00:00:00Z",
"timestamp": 1770854400000
}
}
],
"link": [
{
"URL": "https://dx.plos.org/10.1371/journal.pone.0336221",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "340",
"original-title": [],
"page": "e0336221",
"prefix": "10.1371",
"published": {
"date-parts": [
[
2026,
2,
12
]
]
},
"published-online": {
"date-parts": [
[
2026,
2,
12
]
]
},
"publisher": "Public Library of Science (PLoS)",
"reference": [
{
"article-title": "Macrophages in kidney injury, inflammation, and fibrosis",
"author": "Q Cao",
"first-page": "183",
"issue": "3",
"journal-title": "Physiology (Bethesda)",
"key": "pone.0336221.ref001",
"volume": "30",
"year": "2015"
},
{
"DOI": "10.1159/000142934",
"article-title": "Inflammation in acute kidney injury",
"author": "GR Kinsey",
"doi-asserted-by": "crossref",
"issue": "4",
"journal-title": "Nephron Exp Nephrol",
"key": "pone.0336221.ref002",
"volume": "109",
"year": "2008"
},
{
"DOI": "10.1172/JCI112112",
"article-title": "Macrophage-induced glomerular fibrin deposition in experimental glomerulonephritis in the rabbit",
"author": "SR Holdsworth",
"doi-asserted-by": "crossref",
"first-page": "1367",
"issue": "4",
"journal-title": "J Clin Invest",
"key": "pone.0336221.ref003",
"volume": "76",
"year": "1985"
},
{
"DOI": "10.1016/j.transproceed.2008.10.004",
"article-title": "Ischemia/reperfusion injury in kidney transplantation: mechanisms and prevention",
"author": "M Kosieradzki",
"doi-asserted-by": "crossref",
"first-page": "3279",
"issue": "10",
"journal-title": "Transplant Proc",
"key": "pone.0336221.ref004",
"volume": "40",
"year": "2008"
},
{
"DOI": "10.1002/1097-0347(200010)22:7<700::AID-HED10>3.0.CO;2-H",
"article-title": "Ischemia/reperfusion injury in microvascular surgery",
"author": "WR Carroll",
"doi-asserted-by": "crossref",
"first-page": "700",
"issue": "7",
"journal-title": "Head Neck",
"key": "pone.0336221.ref005",
"volume": "22",
"year": "2000"
},
{
"DOI": "10.1016/j.kint.2019.05.026",
"article-title": "Acute kidney injury from sepsis: current concepts, epidemiology, pathophysiology, prevention and treatment",
"author": "S Peerapornratana",
"doi-asserted-by": "crossref",
"first-page": "1083",
"issue": "5",
"journal-title": "Kidney Int",
"key": "pone.0336221.ref006",
"volume": "96",
"year": "2019"
},
{
"article-title": "NLRP3 inflammasome and its inhibitors: a review",
"author": "B-Z Shao",
"first-page": "262",
"journal-title": "Front Pharmacol",
"key": "pone.0336221.ref007",
"volume": "6",
"year": "2015"
},
{
"DOI": "10.1016/j.bbrc.2020.03.034",
"article-title": "Remdesivir attenuates high fat diet (HFD)-induced NAFLD by regulating hepatocyte dyslipidemia and inflammation via the suppression of STING",
"author": "Y-N Li",
"doi-asserted-by": "crossref",
"first-page": "381",
"issue": "2",
"journal-title": "Biochem Biophys Res Commun",
"key": "pone.0336221.ref008",
"volume": "526",
"year": "2020"
},
{
"DOI": "10.1186/s12882-020-01921-7",
"article-title": "Macrophage polarization in innate immune responses contributing to pathogenesis of chronic kidney disease",
"author": "H Lee",
"doi-asserted-by": "crossref",
"first-page": "270",
"issue": "1",
"journal-title": "BMC Nephrol",
"key": "pone.0336221.ref009",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.3389/fimmu.2021.652446",
"article-title": "Remdesivir alleviates acute kidney injury by inhibiting the activation of NLRP3 inflammasome",
"author": "L Yin",
"doi-asserted-by": "crossref",
"first-page": "652446",
"journal-title": "Front Immunol",
"key": "pone.0336221.ref010",
"volume": "12",
"year": "2021"
},
{
"article-title": "Long-term kidney function recovery and mortality after COVID-19-associated acute kidney injury: an international multi-centre observational cohort study",
"author": "BWL Tan",
"first-page": "101724",
"journal-title": "EClinicalMedicine",
"key": "pone.0336221.ref011",
"volume": "55",
"year": "2022"
},
{
"DOI": "10.1002/cpt.2145",
"article-title": "Remdesivir and acute renal failure: a potential safety signal from disproportionality analysis of the WHO Safety Database",
"author": "AO Gérard",
"doi-asserted-by": "crossref",
"first-page": "1021",
"issue": "4",
"journal-title": "Clin Pharmacol Ther",
"key": "pone.0336221.ref012",
"volume": "109",
"year": "2021"
},
{
"DOI": "10.1016/j.kint.2021.02.015",
"article-title": "Kidney disorders as serious adverse drug reactions of remdesivir in coronavirus disease 2019: a retrospective case-noncase study",
"author": "L Chouchana",
"doi-asserted-by": "crossref",
"first-page": "1235",
"issue": "5",
"journal-title": "Kidney Int",
"key": "pone.0336221.ref013",
"volume": "99",
"year": "2021"
},
{
"DOI": "10.3389/fphar.2022.692828",
"article-title": "Acute kidney injury associated with remdesivir: a comprehensive pharmacovigilance analysis of COVID-19 reports in FAERS",
"author": "B Wu",
"doi-asserted-by": "crossref",
"first-page": "692828",
"journal-title": "Front Pharmacol",
"key": "pone.0336221.ref014",
"volume": "13",
"year": "2022"
},
{
"DOI": "10.1093/cid/ciaa1851",
"article-title": "Remdesivir use in the setting of severe renal impairment: a theoretical concern or real risk?",
"author": "NN Pettit",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "Clin Infect Dis",
"key": "pone.0336221.ref015",
"volume": "73",
"year": "2021"
},
{
"DOI": "10.1128/AAC.02290-20",
"article-title": "A valid warning or clinical lore: an evaluation of safety outcomes of remdesivir in patients with impaired renal function from a multicenter matched cohort",
"author": "TW Ackley",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "Antimicrob Agents Chemother",
"key": "pone.0336221.ref016",
"volume": "65",
"year": "2021"
},
{
"DOI": "10.1007/s15010-022-01850-7",
"article-title": "Is remdesivir safe in patients with renal impairment? Experience at a large tertiary urban medical center",
"author": "S Sunny",
"doi-asserted-by": "crossref",
"first-page": "247",
"issue": "1",
"journal-title": "Infection",
"key": "pone.0336221.ref017",
"volume": "51",
"year": "2023"
},
{
"DOI": "10.1371/journal.pone.0279765",
"article-title": "Effect of remdesivir on adverse kidney outcomes in hospitalized patients with COVID-19 and impaired kidney function",
"author": "R Seethapathy",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "PLoS One",
"key": "pone.0336221.ref018",
"volume": "18",
"year": "2023"
},
{
"DOI": "10.1016/j.ekir.2020.10.005",
"article-title": "Safety of remdesivir in patients with acute kidney injury or CKD",
"author": "S Thakare",
"doi-asserted-by": "crossref",
"first-page": "206",
"issue": "1",
"journal-title": "Kidney Int Rep",
"key": "pone.0336221.ref019",
"volume": "6",
"year": "2021"
},
{
"DOI": "10.1001/jamanetworkopen.2022.29236",
"article-title": "Remdesivir in patients with severe kidney dysfunction: a secondary analysis of the CATCO randomized trial",
"author": "M Cheng",
"doi-asserted-by": "crossref",
"issue": "8",
"journal-title": "JAMA Netw Open",
"key": "pone.0336221.ref020",
"volume": "5",
"year": "2022"
},
{
"DOI": "10.1097/MJT.0000000000001543",
"article-title": "Remdesivir administration in COVID-19 patients with renal impairment: a systematic review",
"author": "E Davoudi-Monfared",
"doi-asserted-by": "crossref",
"issue": "5",
"journal-title": "Am J Ther",
"key": "pone.0336221.ref021",
"volume": "29",
"year": "2022"
},
{
"DOI": "10.1007/s00204-022-03306-1",
"article-title": "The potential of remdesivir to affect function, metabolism and proliferation of cardiac and kidney cells in vitro",
"author": "K Merches",
"doi-asserted-by": "crossref",
"first-page": "2341",
"issue": "8",
"journal-title": "Arch Toxicol",
"key": "pone.0336221.ref022",
"volume": "96",
"year": "2022"
},
{
"DOI": "10.21315/mjms2017.24.5.11",
"article-title": "Sample size calculation in animal studies using resource equation approach",
"author": "WN Arifin",
"doi-asserted-by": "crossref",
"first-page": "101",
"issue": "5",
"journal-title": "Malays J Med Sci",
"key": "pone.0336221.ref023",
"volume": "24",
"year": "2017"
},
{
"DOI": "10.1016/j.celrep.2020.107940",
"article-title": "Remdesivir inhibits SARS-CoV-2 in human lung cells and chimeric SARS-CoV expressing the SARS-CoV-2 RNA polymerase in mice",
"author": "AJ Pruijssers",
"doi-asserted-by": "crossref",
"first-page": "107940",
"issue": "3",
"journal-title": "Cell Rep",
"key": "pone.0336221.ref024",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1038/s41467-019-13940-6",
"article-title": "Comparative therapeutic efficacy of remdesivir and combination lopinavir, ritonavir, and interferon beta against MERS-CoV",
"author": "TP Sheahan",
"doi-asserted-by": "crossref",
"first-page": "222",
"issue": "1",
"journal-title": "Nat Commun",
"key": "pone.0336221.ref025",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1093/jpp/rgac054",
"article-title": "Eplerenone reduces renal ischaemia/reperfusion injury by modulating Klotho, NF-κB and SIRT1/SIRT3/PGC-1α signalling pathways",
"author": "A Barati",
"doi-asserted-by": "crossref",
"first-page": "819",
"issue": "6",
"journal-title": "J Pharm Pharmacol",
"key": "pone.0336221.ref026",
"volume": "75",
"year": "2023"
},
{
"DOI": "10.1177/0960327120979014",
"article-title": "Protective effects of Gamma Oryzanol on distant organs after kidney ischemia-reperfusion in rats: A focus on liver protection",
"author": "Y Bagheri",
"doi-asserted-by": "crossref",
"first-page": "1022",
"issue": "6",
"journal-title": "Hum Exp Toxicol",
"key": "pone.0336221.ref027",
"volume": "40",
"year": "2021"
},
{
"article-title": "The effect of fingolimod on renal ischemia/reperfusion injury in a rat model",
"author": "Y Bagheri",
"journal-title": "Curr Mol Pharmacol",
"key": "pone.0336221.ref028",
"volume": "17",
"year": "2024"
},
{
"DOI": "10.1172/JCI0215623",
"article-title": "Neutrophil-independent mechanisms of caspase-1- and IL-18-mediated ischemic acute tubular necrosis in mice",
"author": "VY Melnikov",
"doi-asserted-by": "crossref",
"first-page": "1083",
"issue": "8",
"journal-title": "J Clin Invest",
"key": "pone.0336221.ref029",
"volume": "110",
"year": "2002"
},
{
"DOI": "10.1006/jmcc.2002.2091",
"article-title": "ATF3 inhibits doxorubicin-induced apoptosis in cardiac myocytes: a novel cardioprotective role of ATF3",
"author": "K Nobori",
"doi-asserted-by": "crossref",
"first-page": "1387",
"issue": "10",
"journal-title": "J Mol Cell Cardiol",
"key": "pone.0336221.ref030",
"volume": "34",
"year": "2002"
},
{
"DOI": "10.1681/ASN.2005111155",
"article-title": "ATF3 protects against renal ischemia-reperfusion injury",
"author": "T Yoshida",
"doi-asserted-by": "crossref",
"first-page": "217",
"issue": "2",
"journal-title": "J Am Soc Nephrol",
"key": "pone.0336221.ref031",
"volume": "19",
"year": "2008"
},
{
"DOI": "10.1681/ASN.2020050589",
"article-title": "Remdesivir in patients with acute or chronic kidney disease and COVID-19",
"author": "ML Adamsick",
"doi-asserted-by": "crossref",
"first-page": "1384",
"issue": "7",
"journal-title": "J Am Soc Nephrol",
"key": "pone.0336221.ref032",
"volume": "31",
"year": "2020"
},
{
"DOI": "10.1002/jcph.1077",
"article-title": "Clinical pharmacokinetics of sulfobutylether-β-Cyclodextrin in patients with varying degrees of renal impairment",
"author": "RK Hoover",
"doi-asserted-by": "crossref",
"first-page": "814",
"issue": "6",
"journal-title": "J Clin Pharmacol",
"key": "pone.0336221.ref033",
"volume": "58",
"year": "2018"
},
{
"DOI": "10.1007/s12010-023-04529-3",
"article-title": "The Effects of Remdesivir and Dexamethasone on Renal Sirtuin-1 Expression and Renal Function in Male Rats",
"author": "S Danaiyan",
"doi-asserted-by": "crossref",
"first-page": "632",
"issue": "2",
"journal-title": "Appl Biochem Biotechnol",
"key": "pone.0336221.ref034",
"volume": "196",
"year": "2024"
},
{
"DOI": "10.3390/v11040326",
"article-title": "Mechanism of inhibition of ebola virus RNA-dependent RNA polymerase by remdesivir",
"author": "EP Tchesnokov",
"doi-asserted-by": "crossref",
"first-page": "326",
"issue": "4",
"journal-title": "Viruses",
"key": "pone.0336221.ref035",
"volume": "11",
"year": "2019"
},
{
"DOI": "10.1016/j.taap.2021.115783",
"article-title": "Remdesivir; molecular and functional measures of mitochondrial safety",
"author": "JA Bjork",
"doi-asserted-by": "crossref",
"first-page": "115783",
"journal-title": "Toxicol Appl Pharmacol",
"key": "pone.0336221.ref036",
"volume": "433",
"year": "2021"
},
{
"article-title": "Off-target in vitro profiling demonstrates that remdesivir is a highly selective antiviral agent",
"author": "Y Xu",
"issue": "2",
"journal-title": "Antimicrob Agents Chemother",
"key": "pone.0336221.ref037",
"volume": "65",
"year": "2021"
},
{
"DOI": "10.1016/j.toxlet.2021.07.015",
"article-title": "Little in vitro effect of remdesivir on mitochondrial respiration and monoamine oxidase activity in isolated mitochondria",
"author": "Z Fišar",
"doi-asserted-by": "crossref",
"first-page": "143",
"journal-title": "Toxicol Lett",
"key": "pone.0336221.ref038",
"volume": "350",
"year": "2021"
},
{
"article-title": "Elucidation of remdesivir cytotoxicity pathways through genome-wide CRISPR-Cas9 screening and transcriptomics",
"author": "E Akinci",
"journal-title": "bioRxiv",
"key": "pone.0336221.ref039",
"year": "2020"
},
{
"DOI": "10.1093/cvr/cvab311",
"article-title": "Remdesivir induces persistent mitochondrial and structural damage in human induced pluripotent stem cell-derived cardiomyocytes",
"author": "M Kwok",
"doi-asserted-by": "crossref",
"first-page": "2652",
"issue": "12",
"journal-title": "Cardiovasc Res",
"key": "pone.0336221.ref040",
"volume": "118",
"year": "2022"
},
{
"article-title": "The roles of ATF3 in glucose homeostasis. a transgenic mouse model with liver dysfunction and defects in endocrine pancreas",
"author": "AE Allen-Jennings",
"first-page": "29507",
"issue": "31",
"journal-title": "J Biol Chem",
"key": "pone.0336221.ref041",
"volume": "276",
"year": "2001"
},
{
"DOI": "10.1083/jcb.201702058",
"article-title": "Multi-omics analysis identifies ATF4 as a key regulator of the mitochondrial stress response in mammals",
"author": "PM Quirós",
"doi-asserted-by": "crossref",
"first-page": "2027",
"issue": "7",
"journal-title": "J Cell Biol",
"key": "pone.0336221.ref042",
"volume": "216",
"year": "2017"
},
{
"DOI": "10.1038/nature04768",
"article-title": "Systems biology approaches identify ATF3 as a negative regulator of Toll-like receptor 4",
"author": "M Gilchrist",
"doi-asserted-by": "crossref",
"first-page": "173",
"issue": "7090",
"journal-title": "Nature",
"key": "pone.0336221.ref043",
"volume": "441",
"year": "2006"
},
{
"DOI": "10.1038/srep14470",
"article-title": "Activating transcription factor 3 represses inflammatory responses by binding to the p65 subunit of NF-κB",
"author": "J-W Kwon",
"doi-asserted-by": "crossref",
"first-page": "14470",
"journal-title": "Sci Rep",
"key": "pone.0336221.ref044",
"volume": "5",
"year": "2015"
},
{
"DOI": "10.1093/nar/gkp865",
"article-title": "Expression of stress-response ATF3 is mediated by Nrf2 in astrocytes",
"author": "K-H Kim",
"doi-asserted-by": "crossref",
"first-page": "48",
"issue": "1",
"journal-title": "Nucleic Acids Res",
"key": "pone.0336221.ref045",
"volume": "38",
"year": "2010"
},
{
"DOI": "10.1038/s41392-023-01688-x",
"article-title": "Ischemia-reperfusion injury: molecular mechanisms and therapeutic targets",
"author": "M Zhang",
"doi-asserted-by": "crossref",
"first-page": "12",
"issue": "1",
"journal-title": "Signal Transduct Target Ther",
"key": "pone.0336221.ref046",
"volume": "9",
"year": "2024"
},
{
"DOI": "10.1097/01.ASN.0000040596.23073.01",
"article-title": "P53 mediates the apoptotic response to GTP depletion after renal ischemia-reperfusion: protective role of a p53 inhibitor",
"author": "KJ Kelly",
"doi-asserted-by": "crossref",
"first-page": "128",
"issue": "1",
"journal-title": "J Am Soc Nephrol",
"key": "pone.0336221.ref047",
"volume": "14",
"year": "2003"
},
{
"DOI": "10.1152/ajprenal.00328.2018",
"article-title": "Plasma and urinary p21: potential biomarkers of AKI and renal aging",
"author": "AC Johnson",
"doi-asserted-by": "crossref",
"issue": "5",
"journal-title": "Am J Physiol Renal Physiol",
"key": "pone.0336221.ref048",
"volume": "315",
"year": "2018"
},
{
"DOI": "10.1152/ajprenal.00084.2006",
"article-title": "p21 and mTERT are novel markers for determining different ischemic time periods in renal ischemia-reperfusion injury",
"author": "K Hochegger",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "Am J Physiol Renal Physiol",
"key": "pone.0336221.ref049",
"volume": "292",
"year": "2007"
},
{
"DOI": "10.1038/ki.2013.496",
"article-title": "The cyclin-dependent kinase inhibitor p21 is essential for the beneficial effects of renal ischemic preconditioning on renal ischemia/reperfusion injury in mice",
"author": "S Nishioka",
"doi-asserted-by": "crossref",
"first-page": "871",
"issue": "4",
"journal-title": "Kidney Int",
"key": "pone.0336221.ref050",
"volume": "85",
"year": "2014"
},
{
"DOI": "10.1074/jbc.M202974200",
"article-title": "Transcriptional repressor activating transcription factor 3 protects human umbilical vein endothelial cells from tumor necrosis factor-alpha-induced apoptosis through down-regulation of p53 transcription",
"author": "J Kawauchi",
"doi-asserted-by": "crossref",
"first-page": "39025",
"issue": "41",
"journal-title": "J Biol Chem",
"key": "pone.0336221.ref051",
"volume": "277",
"year": "2002"
},
{
"DOI": "10.1038/s41581-023-00694-0",
"article-title": "Regulated cell death pathways in kidney disease",
"author": "AB Sanz",
"doi-asserted-by": "crossref",
"first-page": "281",
"issue": "5",
"journal-title": "Nat Rev Nephrol",
"key": "pone.0336221.ref052",
"volume": "19",
"year": "2023"
},
{
"DOI": "10.1371/journal.pone.0026848",
"article-title": "Systems analysis of ATF3 in stress response and cancer reveals opposing effects on pro-apoptotic genes in p53 pathway",
"author": "Y Tanaka",
"doi-asserted-by": "crossref",
"issue": "10",
"journal-title": "PLoS One",
"key": "pone.0336221.ref053",
"volume": "6",
"year": "2011"
},
{
"DOI": "10.1038/s41392-024-01757-9",
"article-title": "NF-κB in biology and targeted therapy: new insights and translational implications",
"author": "Q Guo",
"doi-asserted-by": "crossref",
"first-page": "53",
"issue": "1",
"journal-title": "Signal Transduct Target Ther",
"key": "pone.0336221.ref054",
"volume": "9",
"year": "2024"
},
{
"DOI": "10.1016/j.clinsp.2023.100200",
"article-title": "Acute kidney injury in COVID-19 patients receiving remdesivir: A systematic review and meta-analysis of randomized clinical trials",
"author": "G Shams",
"doi-asserted-by": "crossref",
"first-page": "100200",
"journal-title": "Clinics (Sao Paulo)",
"key": "pone.0336221.ref055",
"volume": "78",
"year": "2023"
},
{
"DOI": "10.1371/journal.pone.0152153",
"article-title": "Unilateral renal ischemia-reperfusion as a robust model for acute to chronic kidney injury in mice",
"author": "N Le Clef",
"doi-asserted-by": "crossref",
"issue": "3",
"journal-title": "PLoS One",
"key": "pone.0336221.ref056",
"volume": "11",
"year": "2016"
}
],
"reference-count": 56,
"references-count": 56,
"relation": {},
"resource": {
"primary": {
"URL": "https://dx.plos.org/10.1371/journal.pone.0336221"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Remdesivir may exacerbate ischemic acute kidney injury through molecular alterations in PGC-1α and apoptosis pathways: An in vivo study",
"type": "journal-article",
"update-policy": "https://doi.org/10.1371/journal.pone.corrections_policy",
"volume": "21"
}