Redox Homeostasis Alteration Is Restored through Melatonin Treatment in COVID-19 Patients: A Preliminary Study
et al., International Journal of Molecular Sciences, doi:10.3390/ijms25084543, Jan 2024 (preprint)
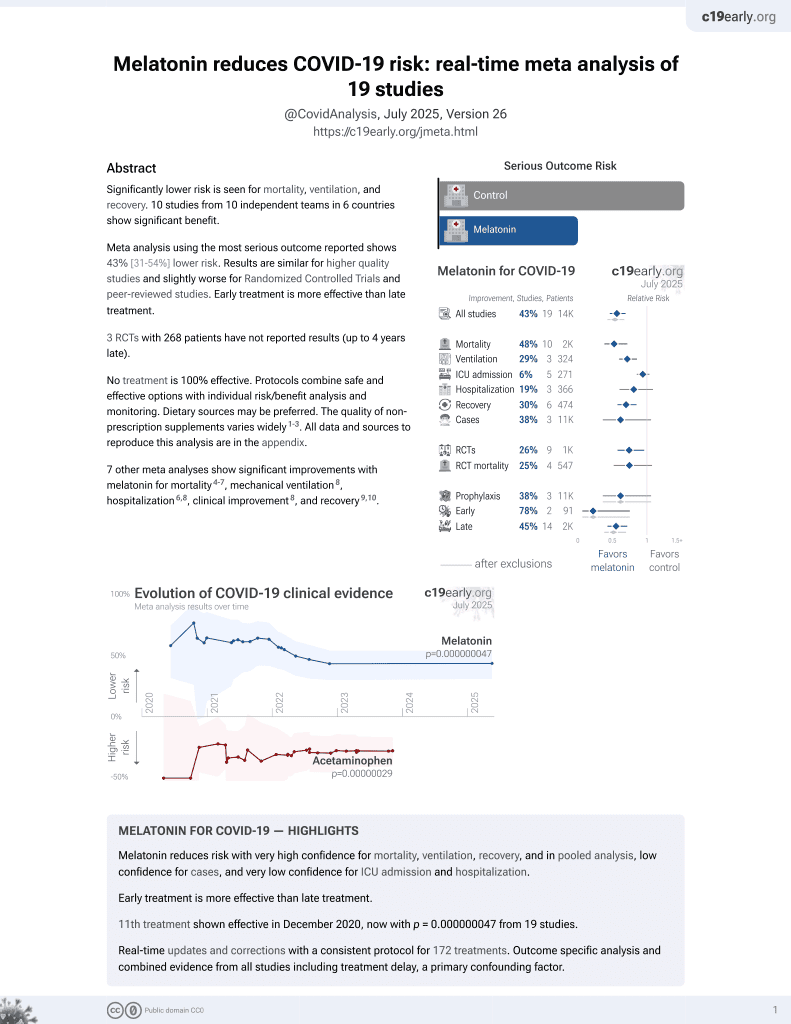
Melatonin for COVID-19
25th treatment shown to reduce risk in
May 2021, now with p = 0.000000015 from 18 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 17 hospitalized COVID-19 patients showing restored redox homeostasis, decreased oxidative stress, improved antioxidant enzyme activity, modulated glucose homeostasis, and inhibited Warburg effect with melatonin treatment. Melatonin capsules (5mg) were administered every 12 hours for 5 days. The results suggest that melatonin may restore altered redox homeostasis in COVID-19 through antioxidant and anti-inflammatory effects, and could be used as an adjuvant therapy.
Soto et al., 31 Jan 2024, prospective, Mexico, peer-reviewed, median age 62.0, 9 authors, study period August 2020 - September 2020.
Contact: vicente.castrejon@cardiologia.org.mx (corresponding author), vicente.castrejon@cardiologia.org.mx (corresponding author), elena.soto@cardiologia.org.mx, israel.perez@cardiologia.org.mx, loe_mana@hotmail.com, elizabeth.soria@cardiologia.org.mx, a2novi@hotmail.com, rrvaldezvazquez@gmail.com, veronica.guarner@cardiologia.org.mx, eulses.diazd@incmnsz.mx.
Redox Homeostasis Alteration Is Restored through Melatonin Treatment in COVID-19 Patients: A Preliminary Study
International Journal of Molecular Sciences, doi:10.3390/ijms25084543
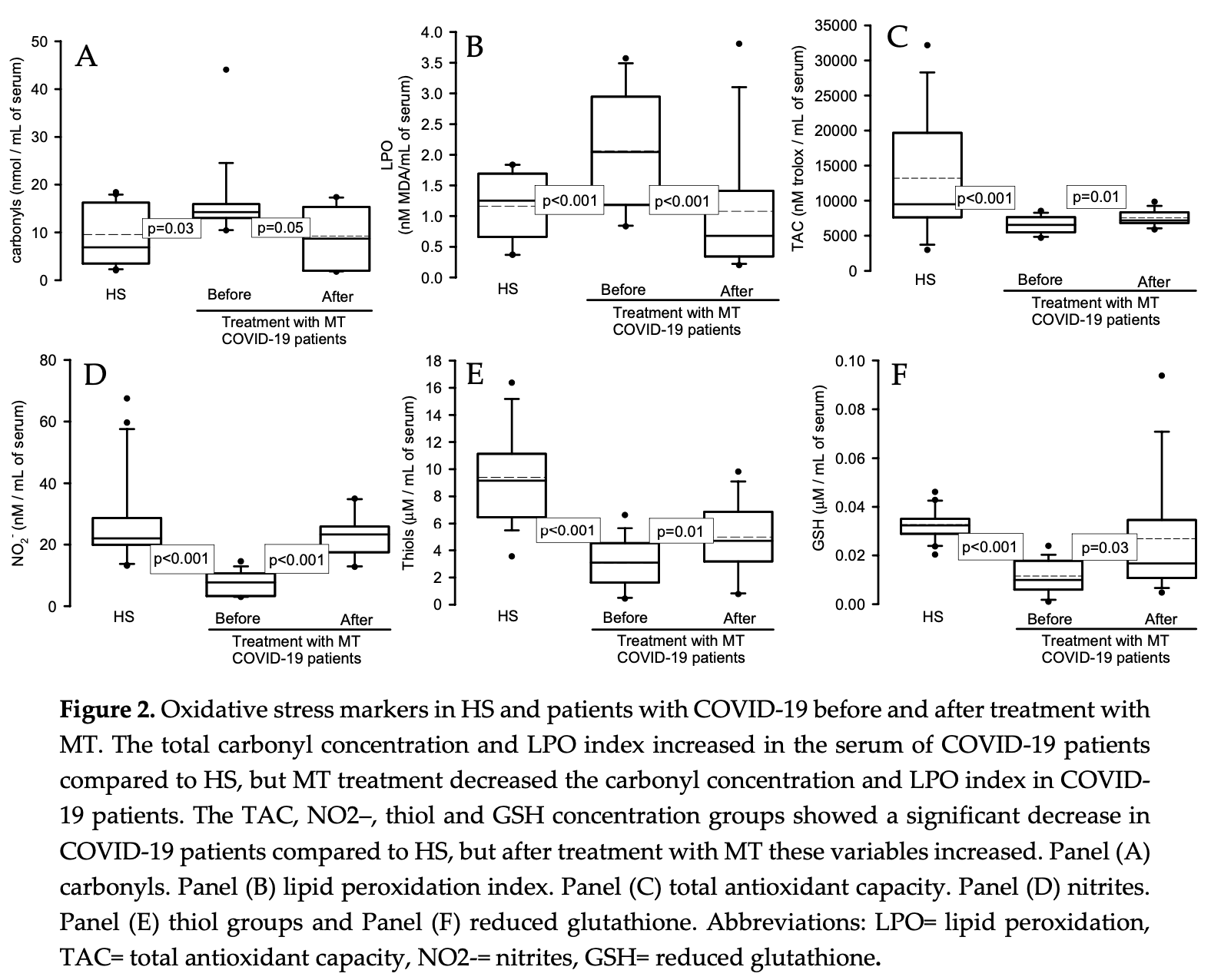
Type II pneumocytes are the target of the SARS-CoV-2 virus, which alters their redox homeostasis to increase reactive oxygen species (ROS). Melatonin (MT) has antioxidant proprieties and protects mitochondrial function. In this study, we evaluated whether treatment with MT compensated for the redox homeostasis alteration in serum from COVID-19 patients. We determined oxidative stress (OS) markers such as carbonyls, glutathione (GSH), total antioxidant capacity (TAC), thiols, nitrites (NO 2 -), lipid peroxidation (LPO), and thiol groups in serum. We also studied the enzymatic activities of glutathione peroxidase (GPx), glutathione-S-transferase (GST), reductase (GR), thioredoxin reductase (TrxR), extracellular superoxide dismutase (ecSOD) and peroxidases. There were significant increases in LPO and carbonyl quantities (p ≤ 0.03) and decreases in TAC and the quantities of NO 2 -, thiols, and GSH (p < 0.001) in COVID-19 patients. The activities of the antioxidant enzymes such as ecSOD, TrxR, GPx, GST, GR, and peroxidases were decreased (p ≤ 0.04) after the MT treatment. The treatment with MT favored the activity of the antioxidant enzymes that contributed to an increase in TAC and restored the lost redox homeostasis. MT also modulated glucose homeostasis, functioning as a glycolytic agent, and inhibited the Warburg effect. Thus, MT restores the redox homeostasis that is altered in COVID-19 patients and can be used as adjuvant therapy in SARS-CoV-2 infection.
Institutional Review Board Statement: The studies involving human participants were reviewed and approved with ethical approval from the local ethics committee on 19 August 2020 (Control-9867/2020, register REG. CONBIOETICA-09 CEI-011-20160627). A written informed consent form for enrollment or consent to use patient data was obtained from each patient or their legal surrogate.
Conflicts of Interest: The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
Abbas-Mousavi, Heydari, Mehravaran, Saeedi, Alizadeh-Navaei et al., Melatonin effects on sleep quality and outcomes of COVID-19 patients: An open-label, randomized, controlled trial, J. Med. Virol, doi:10.1002/jmv.27312
Abu-Soud, Hazen, Nitric oxide is a physiological substrate for mammalian peroxidases, J. Biol. Chem, doi:10.1074/jbc.275.48.37524
Alizadeh, Dianatkhah, Alimohamadi, Moradi, Akbarpour et al., High dose melatonin as an adjuvant therapy in intubated patients with COVID-19: A randomized clinical trial, J. Taibah Univ. Med. Sci, doi:10.1016/j.jtumed.2022.04.012
Alizadeh, Keyhanian, Ghaderkhani, Dashti-Khavidaki, Shoormasti et al., A pilot study on controlling coronavirus disease 2019 (COVID-19) inflammation using melatonin supplement, Iran. J. Allergy. Asthma. Immunol, doi:10.18502/ijaai.v20i4.6959
Ameri, Asadi, Ziaei, Vatankhah, Safa et al., Efficacy and safety of oral melatonin in patients with severe COVID-19: A randomized controlled trial, Inflammopharmacology, doi:10.1007/s10787-022-01096-7
Anderson, Reiter, Melatonin: Roles in influenza, COVID-19, and other viral infections, Rev. Med. Virol, doi:10.1002/rmv.2109
Bahrampour, Pourhanifeh, Hosseinzadeh, Hemati, Mehrzadi, Melatonin potentials against viral infections including COVID-19: Current evidence and new findings, Virus. Res, doi:10.1016/j.virusres.2020.198108
Boga, Coto-Montes, Rosales-Corral, Tan, Reiter, Beneficial actions of melatonin in the management of viral infections: A new use for this molecular handyman, Rev. Med. Virol, doi:10.1002/rmv.1714
Bologna, Madonna, Pone, Efficacy of prolonged-release melatonin 2 mg (PRM 2 mg) prescribed for insomnia in hospitalized patients for COVID-19: A retrospective observational study, J. Clin. Med, doi:10.3390/jcm10245857
Boutin, Liberelle, Yous, Ferry, Nepveu, Melatonin facts: Lack of evidence that melatonin is a radical scavenger in living systems, J. Pineal. Res, doi:10.1111/jpi.12926
Brower, Lanken, Macintyre, Matthay, Morris et al., National heart, lung, and blood institute ARDS clinical trials network higher versus lower positive end-expiratory pressures in patients with the acute respiratory distress syndrome, N. Engl. J. Med
Budkowska, Cecerska-Heryć, Marcinowska, Siennicka, Dołęgowska, The influence of circadian rhythm on the activity of oxidative stress enzymes, Int. J. Mol. Sci, doi:10.3390/ijms232214275
Camp, Bai, Gonullu, Nayak, Abu-Soud, Melatonin interferes with COVID-19 at several distinct ROS-related steps, J. Inorg. Biochem, doi:10.1016/j.jinorgbio.2021.111546
Cao, Cheng, Recombinant myeloperoxidase as a New class of antimicrobial agents, Microbiol. Spectr, doi:10.1128/spectrum.00522-21
Cardinali, Brown, Pandi-Perumal, Can Melatonin be a potential "Silver Bullet" in treating COVID-19 patients?, Diseases, doi:10.3390/diseases8040044
Chavarría, Vázquez, Cherit, Bello, Suastegui et al., Antioxidants and pentoxifylline as coadjuvant measures to standard therapy to improve prognosis of patients with pneumonia by COVID-19, Comput. Struct. Biotechnol. J, doi:10.1016/j.csbj.2021.02.009
Corrao, Bocchio, Monaco, Natoli, Cavezzi et al., Does evidence exist to blunt inflammatory response by nutraceutical supplementation during COVID-19 pandemic? An overview of systematic reviews of vitamin D, vitamin C, melatonin, and Zinc, Nutrients, doi:10.3390/nu13041261
Crespo, Miguel, Laliena, Alvarez, Culebras et al., Melatonin prevents the decreased activity of antioxidant enzymes and activates nuclear erythroid 2-related factor 2 signaling in an animal model of fulminant hepatic failure of viral origin, J. Pineal. Res, doi:10.1111/j.1600-079X.2010.00787.x
Erel, Neşelio Glu, Tunçay, Eren, Akkuş et al., A sensitive indicator for the severity of COVID-19: Thiol, Turk. J. Med. Sci
Farnoosh, Akbariqomi, Badri, Bagheri, Izadi et al., Efficacy of a low dose of melatonin as an adjunctive therapy in hospitalized patients with COVID-19: A randomized, double-blind clinical Trial, Arch. Med. Res, doi:10.1016/j.arcmed.2021.06.006
Feitosa, Júnior, Neryneto, Matos, Moura et al., Rational discovery of the therapeutic potential of melatonin as a SARS-CoV-2 main protease inhibitor, Int. J. Med. Sci, doi:10.7150/ijms.48053
Fogleman, Cohen, Mercier, Farrell, Rutz et al., A pilot of a randomized control trial of melatonin and vitamin C for mild-to-moderate COVID-19, J. Am. Board. Fam. Med, doi:10.3122/jabfm.2022.04.210529
Galano, Tan, Reiter, Melatonin and related compounds: Chemical insights into their protective effects against oxidative stress, Curr. Org. Chem, doi:10.2174/1385272820666161024124058
Ghaleh, Hosseini, Aghamollaei, Fasihi-Ramandi, Alishiri et al., NLRP3 inflammasome activation and oxidative stress status in the mild and moderate SARS-CoV-2 infected patients: Impact of melatonin as a medicinal supplement, Z. Naturforsch. C J. Biosci, doi:10.1515/znc-2021-0101
Gomez-Pastora, Weigand, Kim, Wu, Strayer et al., Hyperferritinemia in critically ill COVID-19 patients-Is ferritin the product of inflammation or a pathogenic mediator?, Clin. Chim. Acta, doi:10.1016/j.cca.2020.06.033
Goud, Bai, Abu-Soud, A Multiple-hit hypothesis involving reactive oxygen species and myeloperoxidase explains clinical deterioration and fatality in COVID-19, Int. J. Biol. Sci, doi:10.7150/ijbs.51811
Guimarães, Timerman, Rodrigues, Corrêa, Schubert et al., Position statement: Cardiopulmonary resuscitation of patients with confirmed or suspected COVID-19-2020, Arq. Bras. Cardiol, doi:10.36660/abc.20200548
Gulcin, Buyukokuroglu, Kufrevioglu, Metal chelating and hydrogen peroxide scavenging effects of melatonin, J. Pineal. Res, doi:10.1034/j.1600-079X.2003.00042.x
Hardeland, Antioxidant protection by melatonin: Multiplicity of mechanisms from radical detoxification to radical avoidance, Endocrine, doi:10.1385/ENDO:27:2:119
Hasan, Al-Atrakji, Alsaaty, Abdulnafa, Mehuaiden, The effect of melatonin on C-reactive protein, serum ferritin and D-dimer in COVID-19 patients, Int. J. Drug. Delivery. Technol, doi:10.25258/ijddt.12.1.21
Hasan, Atrakji, Mehuaiden, The effect of melatonin on thrombosis, sepsis and mortality rate in COVID-19 patients, Int. J. Infect. Dis, doi:10.1016/j.ijid.2021.10.012
Hosseini, Ghaleh, Aghamollaei, Ramandi, Alishiri et al., Evaluation of Th1 and Th2 mediated cellular and humoral immunity in patients with COVID-19 following the use of melatonin as an adjunctive treatment, Eur. J. Pharmacol, doi:10.1016/j.ejphar.2021.174193
Kim, Kim, Ryu, Kim, Park et al., Reactive oxygen species induce antiviral innate immune response through IFN-lambda regulation in human nasal epithelial cells, Am. J. Respir. Cell. Mol. Biol, doi:10.1165/rcmb.2013-0003OC
Kouhpayeh, Shariati, Boshtam, Rahimmanesh, Mirian et al., The molecular basis of COVID-19 pathogenesis, conventional and nanomedicine therapy, Int. J. Mol. Sci, doi:10.3390/ijms22115438
Lambden, Laterre, Levy, Francois, The SOFA score-development, utility, and challenges of accurate assessment in clinical trials, Crit. Care, doi:10.1186/s13054-019-2663-7
Mahjoub, Youssef, Yaakoubi, Salah, Jaballah et al., Melatonin, vitamins and minerals supplements for the treatment of COVID-19 and Covid-like illness: A prospective, randomized, double-blind multicenter study, Explore, doi:10.1016/j.explore.2023.06.009
Markus, Fernandes, Kinker, Da Silveira, Marçola, Immune-pineal axis-Acute inflammatory responses coordinate melatonin synthesis by pinealocytes and phagocytes, Br. J. Pharmacol, doi:10.1111/bph.14083
Mehrzadi, Karimi, Fatemi, Reiter, Hosseinzadeh, SARS-CoV-2 and other coronaviruses negatively influence mitochondrial quality control: Beneficial effects of melatonin, Pharmacol. Ther, doi:10.1016/j.pharmthera.2021.107825
Molina-Carballo, Palacios-López, Jerez-Calero, Augustín-Morales, Agil et al., Protective effect of melatonin administration against SARS-CoV-2 infection: A systematic review, Curr. Issues. Mol. Biol, doi:10.3390/cimb44010003
Muhammad, Kani, Iliya, Muhammad, Binji et al., Deficiency of antioxidants and increased oxidative stress in COVID-19 patients: A cross-sectional comparative study in Jigawa, Northwestern Nigeria, SAGE. Open. Med, doi:10.1177/2050312121991246
Nakao, Morita, Maemura, Amiya, Inajima et al., Melatonin ameliorates Angiotensin II-induced vascular endothelial damage via its antioxidative properties, J. Pineal. Res, doi:10.1111/jpi.12071
Negru, Radu, Vesa, Behl, Abdel-Daim et al., Therapeutic dilemmas in addressing SARS-CoV-2 infection: Favipiravir versus Remdesivir, Biomed. Pharmacother, doi:10.1016/j.biopha.2022.112700
Olson, Andrew, Diagnosis and treatment of adults with community-acquired pneumonia, JAMA, doi:10.1001/jama.2019.21118
Owino, Buonfiglio, Tchio, Tosini, Melatonin signaling a key regulator of glucose homeostasis and energy metabolism, Front. Endocrinol, doi:10.3389/fendo.2019.00488
Pablos, Guerrero, Ortiz, Agapito, Reiter, Both melatonin and a putative nuclear melatonin receptor agonist CGP 52608 stimulate glutathione peroxidase and glutathione reductase activities in mouse brain in vivo, Neuroendocrinol. Lett
Pontes, Cardoso, Carneiro-Sampaio, Markus, Pineal melatonin and the innate immune response: The TNF-alpha increase after cesarean section suppresses nocturnal melatonin production, J. Pineal. Res, doi:10.1111/j.1600-079X.2007.00487.x
Pérez-Torres, Guarner-Lans, Soria-Castro, Manzano-Pech, Palacios-Chavarría et al., Alteration in the lipid profile and the desaturases activity in patients with severe pneumonia by SARS-CoV-2, Front. Physiol, doi:10.3389/fphys.2021.667024
Ramos, López-Muñoz, Gil-Martín, Egea, Álvarez-Merz et al., The coronavirus disease 2019 (COVID-19): Key emphasis on melatonin safety and therapeutic efficacy, Antioxidants, doi:10.3390/antiox10071152
Ranieri, Rubenfeld, Thompson, Ferguson, Caldwell et al., Acute respiratory distress syndrome: The Berlin Definition, JAMA
Reiter, Sharma, Rosales-Corral, Anti-Warburg effect of melatonin: A proposed mechanism to explain its inhibition of multiple diseases, Int. J. Mol. Sci, doi:10.3390/ijms22020764
Reppert, Melatonin receptors: Molecular biology of a new family of G protein-coupled receptors, J. Biol. Rhythm, doi:10.1177/074873049701200606
Rodriguez, Mayo, Sainz, Antolín, Herrera, Regulation of antioxidant enzymes: A significant role for melatonin, J. Pineal. Res, doi:10.1046/j.1600-079X.2003.00092.x
Sayed, Fernández-Ortiz, Diaz-Casado, Rusanova, Rahim et al., The protective effect of melatonin against age-associated, sarcopenia-dependent tubular aggregate formation, lactate depletion, and mitochondrial changes, J. Gerontol. A Biol. Sci. Med. Sci, doi:10.1093/gerona/gly059
Serdengeçti, Tarakçıo Glu, COVID-19-related brief insomnia in a 13-year-old adolescent girl, Sleep. Sci, doi:10.1055/s-0043-1777780
Sezgin, Özturk, Güney, Sinano Glu, Tunçdemir, Protective effect of melatonin and 1,25-dihydroxyvitamin D3 on renal ischemia-reperfusion injury in rats, Ren. Fail, doi:10.3109/0886022X.2012.760409
Soria-Castro, Soto, Guarner-Lans, Rojas, Perezpeña-Diazconti et al., The kidnapping of mitochondrial function associated with the SARS-CoV-2 infection, Histol. Histopathol
Soto, Guarner-Lans, Díaz-Díaz, Manzano-Pech, Palacios-Chavarría et al., Hyperglycemia and loss of redox homeostasis in COVID-19 Patients, Cells, doi:10.3390/cells11060932
Soto, Guarner-Lans, Soria-Castro, Manzano-Pech, Pérez-Torres, Is antioxidant therapy a useful complementary measure for COVID-19 treatment? An algorithm for its application, Medicina, doi:10.3390/medicina56080386
Soto, Manzano-Pech, Palacios-Chavarría, Valdez-Vázquez, Guarner-Lans et al., N-acetyl cysteine restores the diminished activity of the antioxidant enzymatic system caused by SARS-CoV-2 infection: Preliminary findings, Pharmaceuticals, doi:10.3390/ph16040591
Soto, Pérez-Torres, Manzano-Pech, Soria-Castro, Morales-Marín et al., Reduced levels of selenium and thioredoxin reductase in the thoracic aorta could contribute to aneurysm formation in patients with Marfan syndrome, Int. J. Mol. Sci, doi:10.3390/ijms241310429
Sánchez-Rico, De La Muela, Herrera-Morueco, Geoffroy, Limosin et al., Melatonin does not reduce mortality in adult hospitalized patients with COVID-19: A multicenter retrospective observational study, J. Travel. Med, doi:10.1093/jtm/taab195
Taha, Abdelkader, Hossam-Eldin, El-Tawab, Al-Hejazi et al., Safety and efficacy of melatonin as an adjuvant therapy in COVID-19 patients: Systematic review and meta-analysis, Adv. Med. Sci, doi:10.1016/j.advms.2023.09.007
Tan, Manchester, Esteban-Zubero, Zhou, Reiter, Melatonin as a potent and inducible endogenous antioxidant: Synthesis and metabolism, Molecules, doi:10.3390/molecules201018886
Tang, Comish, Kang, The hallmarks of COVID-19 disease, PLoS. Pathog, doi:10.1371/journal.ppat.1008536
Tarocco, Caroccia, Morciano, Wieckowski, Ancora et al., Melatonin as a master regulator of cell death and inflammation: Molecular mechanisms and clinical implications for newborn care, Cell Death. Dis, doi:10.1038/s41419-019-1556-7
Terron, Flores, Czarnocki, Melatonin and its metabolites: New findings regarding their production and their radical scavenging actions, Acta. Biochim. Pol
Thachil, Tang, Gando, Falanga, Cattaneo et al., ISTH interim guidance on recognition and management of coagulopathy in COVID-19, J. Thromb. Haemost, doi:10.1111/jth.14810
Vlasova, Peroxidase activity of human hemoproteins: Keeping the fire under control, Molecules, doi:10.3390/molecules23102561
Wang, Mei, Bai, Zhou, Liu et al., Serum nitrite and nitrate: A potential biomarker for post-COVID-19 complications? Free Radic, Biol. Med, doi:10.1016/j.freeradbiomed.2021.08.237
Wu, Zhao, Xie, Xu, Fei, TLR2-melatonin feedback loop regulates the activation of NLRP3 inflammasome in murine allergic airway inflammation, Front. Immunol, doi:10.3389/fimmu.2020.00172
Yamasaki, Blood nitrate and nitrite modulating nitric oxide bioavailability: Potential therapeutic functions in COVID-19, Nitric. Oxide, doi:10.1016/j.niox.2020.07.005
Yao, Zhu, Han, Shi, Xu, New insights into how melatonin ameliorates bisphenol A-induced colon damage: Inhibition of NADPH oxidase, J. Agric. Food. Chem, doi:10.1021/acs.jafc.2c07236
Zarezadeh, Khorshidi, Emami, Janmohammadi, Kord-Varkaneh et al., Melatonin supplementation and pro-inflammatory mediators: A systematic review and meta-analysis of clinical trials, Eur. J. Nutr, doi:10.1007/s00394-019-02123-0
Zhang, Kukkar, Kim, Bhatt, A comprehensive review on immunogen and immune-response proteins of SARS-CoV-2 and their applications in prevention, diagnosis, and treatment of COVID-19, Int. J. Biol. Macromol, doi:10.1016/j.ijbiomac.2024.129284
Zhang, Zhang, Melatonin: A well-documented antioxidant with conditional pro-oxidant actions, J. Pineal. Res, doi:10.1111/jpi.12162
Öztürk, Akbulut, Güney, Acuna-Castroviejo, Age-related changes in the rat brain mitochondrial antioxidative enzyme ratios: Modulation by melatonin, Exp. Gerontol, doi:10.1016/j.exger.2012.06.011
DOI record:
{
"DOI": "10.3390/ijms25084543",
"ISSN": [
"1422-0067"
],
"URL": "http://dx.doi.org/10.3390/ijms25084543",
"abstract": "<jats:p>Type II pneumocytes are the target of the SARS-CoV-2 virus, which alters their redox homeostasis to increase reactive oxygen species (ROS). Melatonin (MT) has antioxidant proprieties and protects mitochondrial function. In this study, we evaluated whether treatment with MT compensated for the redox homeostasis alteration in serum from COVID-19 patients. We determined oxidative stress (OS) markers such as carbonyls, glutathione (GSH), total antioxidant capacity (TAC), thiols, nitrites (NO2−), lipid peroxidation (LPO), and thiol groups in serum. We also studied the enzymatic activities of glutathione peroxidase (GPx), glutathione-S-transferase (GST), reductase (GR), thioredoxin reductase (TrxR), extracellular superoxide dismutase (ecSOD) and peroxidases. There were significant increases in LPO and carbonyl quantities (p ≤ 0.03) and decreases in TAC and the quantities of NO2−, thiols, and GSH (p < 0.001) in COVID-19 patients. The activities of the antioxidant enzymes such as ecSOD, TrxR, GPx, GST, GR, and peroxidases were decreased (p ≤ 0.04) after the MT treatment. The treatment with MT favored the activity of the antioxidant enzymes that contributed to an increase in TAC and restored the lost redox homeostasis. MT also modulated glucose homeostasis, functioning as a glycolytic agent, and inhibited the Warburg effect. Thus, MT restores the redox homeostasis that is altered in COVID-19 patients and can be used as adjuvant therapy in SARS-CoV-2 infection.</jats:p>",
"alternative-id": [
"ijms25084543"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0003-1332-2888",
"affiliation": [
{
"name": "Research Direction, Instituto Nacional de Cardiología Ignacio Chávez, Juan Badiano 1, Sección XVI, Tlalpan, Mexico City 14080, Mexico"
}
],
"authenticated-orcid": false,
"family": "Soto",
"given": "María Elena",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0001-6510-2954",
"affiliation": [
{
"name": "Department of Cardiovascular Biomedicine, Instituto Nacional de Cardiología Ignacio Chávez, Mexico City 14080, Mexico"
}
],
"authenticated-orcid": false,
"family": "Pérez-Torres",
"given": "Israel",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Cardiovascular Biomedicine, Instituto Nacional de Cardiología Ignacio Chávez, Mexico City 14080, Mexico"
}
],
"family": "Manzano-Pech",
"given": "Linaloe",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Critical Care Units, Temporal COVID-19 Unit, Citibanamex Center, Mexico City 11200, Mexico"
}
],
"family": "Palacios-Chavarría",
"given": "Adrían",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Critical Care Units, Temporal COVID-19 Unit, Citibanamex Center, Mexico City 11200, Mexico"
}
],
"family": "Valdez-Vázquez",
"given": "Rafael Ricardo",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-2655-7590",
"affiliation": [
{
"name": "Department of Physiology, Instituto Nacional de Cardiología Ignacio Chávez, Juan Badiano 1, Sección XVI, Tlalpan, Mexico City 14080, Mexico"
}
],
"authenticated-orcid": false,
"family": "Guarner-Lans",
"given": "Verónica",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Cardiovascular Biomedicine, Instituto Nacional de Cardiología Ignacio Chávez, Mexico City 14080, Mexico"
}
],
"family": "Soria-Castro",
"given": "Elizabeth",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Reproductive Biology, Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán, Vasco de Quiroga 15, Sección XVI, Tlalpan, Mexico City 14000, Mexico"
}
],
"family": "Díaz-Díaz",
"given": "Eulises",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-8518-6961",
"affiliation": [
{
"name": "Department of Physiology, Instituto Nacional de Cardiología Ignacio Chávez, Juan Badiano 1, Sección XVI, Tlalpan, Mexico City 14080, Mexico"
}
],
"authenticated-orcid": false,
"family": "Castrejón-Tellez",
"given": "Vicente",
"sequence": "additional"
}
],
"container-title": "International Journal of Molecular Sciences",
"container-title-short": "IJMS",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2024,
4,
22
]
],
"date-time": "2024-04-22T11:44:09Z",
"timestamp": 1713786249000
},
"deposited": {
"date-parts": [
[
2024,
4,
22
]
],
"date-time": "2024-04-22T12:02:32Z",
"timestamp": 1713787352000
},
"funder": [
{
"award": [
"312167"
],
"name": "Consejo Nacional de Humanidades Ciencias y Tecnologías (CONACHYT) México"
}
],
"indexed": {
"date-parts": [
[
2024,
4,
23
]
],
"date-time": "2024-04-23T00:34:20Z",
"timestamp": 1713832460897
},
"is-referenced-by-count": 0,
"issue": "8",
"issued": {
"date-parts": [
[
2024,
4,
21
]
]
},
"journal-issue": {
"issue": "8",
"published-online": {
"date-parts": [
[
2024,
4
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2024,
4,
21
]
],
"date-time": "2024-04-21T00:00:00Z",
"timestamp": 1713657600000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/1422-0067/25/8/4543/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "4543",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2024,
4,
21
]
]
},
"published-online": {
"date-parts": [
[
2024,
4,
21
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"DOI": "10.3390/medicina56080386",
"article-title": "Is antioxidant therapy a useful complementary measure for COVID-19 treatment? An algorithm for its application",
"author": "Soto",
"doi-asserted-by": "crossref",
"first-page": "386",
"journal-title": "Medicina",
"key": "ref_1",
"volume": "56",
"year": "2020"
},
{
"article-title": "The kidnapping of mitochondrial function associated with the SARS-CoV-2 infection",
"author": "Soto",
"first-page": "947",
"journal-title": "Histol. Histopathol.",
"key": "ref_2",
"volume": "36",
"year": "2021"
},
{
"DOI": "10.1016/j.ijbiomac.2024.129284",
"doi-asserted-by": "crossref",
"key": "ref_3",
"unstructured": "Zhang, D., Kukkar, D., Kim, K.H., and Bhatt, P. (2024). A comprehensive review on immunogen and immune-response proteins of SARS-CoV-2 and their applications in prevention, diagnosis, and treatment of COVID-19. Int. J. Biol. Macromol., 259."
},
{
"DOI": "10.3389/fphys.2021.667024",
"article-title": "Alteration in the lipid profile and the desaturases activity in patients with severe pneumonia by SARS-CoV-2",
"doi-asserted-by": "crossref",
"first-page": "667024",
"journal-title": "Front. Physiol.",
"key": "ref_4",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1016/j.biopha.2022.112700",
"doi-asserted-by": "crossref",
"key": "ref_5",
"unstructured": "Negru, P.A., Radu, A.F., Vesa, C.M., Behl, T., Abdel-Daim, M.M., Nechifor, A.C., Endres, L., Stoicescu, M., Pasca, B., and Tit, D.M. (2022). Therapeutic dilemmas in addressing SARS-CoV-2 infection: Favipiravir versus Remdesivir. Biomed. Pharmacother., 147."
},
{
"article-title": "Protective effect of melatonin administration against SARS-CoV-2 infection: A systematic review",
"author": "Agil",
"first-page": "31",
"journal-title": "Curr. Issues. Mol. Biol.",
"key": "ref_6",
"volume": "44",
"year": "2022"
},
{
"DOI": "10.1111/jpi.12926",
"article-title": "Melatonin facts: Lack of evidence that melatonin is a radical scavenger in living systems",
"author": "Boutin",
"doi-asserted-by": "crossref",
"first-page": "e12926",
"journal-title": "J. Pineal. Res.",
"key": "ref_7",
"volume": "76",
"year": "2023"
},
{
"DOI": "10.1177/074873049701200606",
"article-title": "Melatonin receptors: Molecular biology of a new family of G protein-coupled receptors",
"author": "Reppert",
"doi-asserted-by": "crossref",
"first-page": "528",
"journal-title": "J. Biol. Rhythm.",
"key": "ref_8",
"volume": "12",
"year": "1997"
},
{
"DOI": "10.1016/j.pharmthera.2021.107825",
"article-title": "SARS-CoV-2 and other coronaviruses negatively influence mitochondrial quality control: Beneficial effects of melatonin",
"author": "Mehrzadi",
"doi-asserted-by": "crossref",
"first-page": "107825",
"journal-title": "Pharmacol. Ther.",
"key": "ref_9",
"volume": "224",
"year": "2021"
},
{
"DOI": "10.1111/j.1600-079X.2007.00487.x",
"article-title": "Pineal melatonin and the innate immune response: The TNF-alpha increase after cesarean section suppresses nocturnal melatonin production",
"author": "Pontes",
"doi-asserted-by": "crossref",
"first-page": "365",
"journal-title": "J. Pineal. Res.",
"key": "ref_10",
"volume": "43",
"year": "2007"
},
{
"DOI": "10.1111/bph.14083",
"article-title": "Immune-pineal axis—Acute inflammatory responses coordinate melatonin synthesis by pinealocytes and phagocytes",
"author": "Markus",
"doi-asserted-by": "crossref",
"first-page": "3239",
"journal-title": "Br. J. Pharmacol.",
"key": "ref_11",
"volume": "175",
"year": "2018"
},
{
"article-title": "Both melatonin and a putative nuclear melatonin receptor agonist CGP 52608 stimulate glutathione peroxidase and glutathione reductase activities in mouse brain in vivo",
"author": "Pablos",
"first-page": "49",
"journal-title": "Neuroendocrinol. Lett.",
"key": "ref_12",
"volume": "18",
"year": "1997"
},
{
"DOI": "10.18388/abp.2007_3264",
"article-title": "Melatonin and its metabolites: New findings regarding their production and their radical scavenging actions",
"author": "Terron",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Acta. Biochim. Pol.",
"key": "ref_13",
"volume": "54",
"year": "2007"
},
{
"DOI": "10.1034/j.1600-079X.2003.00042.x",
"article-title": "Metal chelating and hydrogen peroxide scavenging effects of melatonin",
"author": "Gulcin",
"doi-asserted-by": "crossref",
"first-page": "278",
"journal-title": "J. Pineal. Res.",
"key": "ref_14",
"volume": "34",
"year": "2003"
},
{
"DOI": "10.2174/1385272820666161024124058",
"article-title": "Melatonin and related compounds: Chemical insights into their protective effects against oxidative stress",
"author": "Galano",
"doi-asserted-by": "crossref",
"first-page": "2077",
"journal-title": "Curr. Org. Chem.",
"key": "ref_15",
"volume": "21",
"year": "2017"
},
{
"DOI": "10.1021/acs.jafc.2c07236",
"article-title": "New insights into how melatonin ameliorates bisphenol A-induced colon damage: Inhibition of NADPH oxidase",
"author": "Yao",
"doi-asserted-by": "crossref",
"first-page": "2566",
"journal-title": "J. Agric. Food. Chem.",
"key": "ref_16",
"volume": "71",
"year": "2023"
},
{
"DOI": "10.1385/ENDO:27:2:119",
"article-title": "Antioxidant protection by melatonin: Multiplicity of mechanisms from radical detoxification to radical avoidance",
"author": "Hardeland",
"doi-asserted-by": "crossref",
"first-page": "119",
"journal-title": "Endocrine.",
"key": "ref_17",
"volume": "27",
"year": "2005"
},
{
"DOI": "10.1111/jpi.12162",
"article-title": "Melatonin: A well-documented antioxidant with conditional pro-oxidant actions",
"author": "Zhang",
"doi-asserted-by": "crossref",
"first-page": "131",
"journal-title": "J. Pineal. Res.",
"key": "ref_18",
"volume": "57",
"year": "2014"
},
{
"DOI": "10.3390/ijms232214275",
"doi-asserted-by": "crossref",
"key": "ref_19",
"unstructured": "Budkowska, M., Cecerska-Heryć, E., Marcinowska, Z., Siennicka, A., and Dołęgowska, B. (2022). The influence of circadian rhythm on the activity of oxidative stress enzymes. Int. J. Mol. Sci., 23."
},
{
"DOI": "10.3390/cells11060932",
"doi-asserted-by": "crossref",
"key": "ref_20",
"unstructured": "Soto, M.E., Guarner-Lans, V., Díaz-Díaz, E., Manzano-Pech, L., Palacios-Chavarría, A., Valdez-Vázquez, R.R., Aisa-Álvarez, A., Saucedo-Orozco, H., and Pérez-Torres, I. (2022). Hyperglycemia and loss of redox homeostasis in COVID-19 Patients. Cells., 11."
},
{
"DOI": "10.1111/jpi.12071",
"article-title": "Melatonin ameliorates Angiotensin II-induced vascular endothelial damage via its antioxidative properties",
"author": "Nakao",
"doi-asserted-by": "crossref",
"first-page": "287",
"journal-title": "J. Pineal. Res.",
"key": "ref_21",
"volume": "55",
"year": "2013"
},
{
"DOI": "10.7150/ijms.48053",
"article-title": "COVID-19: Rational discovery of the therapeutic potential of melatonin as a SARS-CoV-2 main protease inhibitor",
"author": "Feitosa",
"doi-asserted-by": "crossref",
"first-page": "2133",
"journal-title": "Int. J. Med. Sci.",
"key": "ref_22",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1002/rmv.1714",
"article-title": "Beneficial actions of melatonin in the management of viral infections: A new use for this molecular handyman",
"author": "Boga",
"doi-asserted-by": "crossref",
"first-page": "323",
"journal-title": "Rev. Med. Virol.",
"key": "ref_23",
"volume": "22",
"year": "2012"
},
{
"DOI": "10.1002/rmv.2109",
"article-title": "Melatonin: Roles in influenza, COVID-19, and other viral infections",
"author": "Anderson",
"doi-asserted-by": "crossref",
"first-page": "e2109",
"journal-title": "Rev. Med. Virol.",
"key": "ref_24",
"volume": "30",
"year": "2020"
},
{
"DOI": "10.1016/j.virusres.2020.198108",
"article-title": "Melatonin potentials against viral infections including COVID-19: Current evidence and new findings",
"author": "Bahrampour",
"doi-asserted-by": "crossref",
"first-page": "198108",
"journal-title": "Virus. Res.",
"key": "ref_25",
"volume": "287",
"year": "2020"
},
{
"DOI": "10.3390/ph16040591",
"doi-asserted-by": "crossref",
"key": "ref_26",
"unstructured": "Soto, M.E., Manzano-Pech, L., Palacios-Chavarría, A., Valdez-Vázquez, R.R., Guarner-Lans, V., and Pérez-Torres, I. (2023). N-acetyl cysteine restores the diminished activity of the antioxidant enzymatic system caused by SARS-CoV-2 infection: Preliminary findings. Pharmaceuticals, 16."
},
{
"DOI": "10.1046/j.1600-079X.2003.00092.x",
"article-title": "Regulation of antioxidant enzymes: A significant role for melatonin",
"author": "Rodriguez",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "J. Pineal. Res.",
"key": "ref_27",
"volume": "36",
"year": "2004"
},
{
"DOI": "10.1016/j.exger.2012.06.011",
"article-title": "Age-related changes in the rat brain mitochondrial antioxidative enzyme ratios: Modulation by melatonin",
"author": "Akbulut",
"doi-asserted-by": "crossref",
"first-page": "706",
"journal-title": "Exp. Gerontol.",
"key": "ref_28",
"volume": "47",
"year": "2012"
},
{
"DOI": "10.3109/0886022X.2012.760409",
"article-title": "Protective effect of melatonin and 1,25-dihydroxyvitamin D3 on renal ischemia-reperfusion injury in rats",
"author": "Sezgin",
"doi-asserted-by": "crossref",
"first-page": "374",
"journal-title": "Ren. Fail.",
"key": "ref_29",
"volume": "35",
"year": "2013"
},
{
"article-title": "Melatonin prevents the decreased activity of antioxidant enzymes and activates nuclear erythroid 2-related factor 2 signaling in an animal model of fulminant hepatic failure of viral origin",
"author": "Crespo",
"first-page": "193",
"journal-title": "J. Pineal. Res.",
"key": "ref_30",
"volume": "49",
"year": "2010"
},
{
"DOI": "10.1177/2050312121991246",
"article-title": "Deficiency of antioxidants and increased oxidative stress in COVID-19 patients: A cross-sectional comparative study in Jigawa, Northwestern Nigeria",
"author": "Muhammad",
"doi-asserted-by": "crossref",
"first-page": "2050312121991246",
"journal-title": "SAGE. Open. Med.",
"key": "ref_31",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1371/journal.ppat.1008536",
"doi-asserted-by": "crossref",
"key": "ref_32",
"unstructured": "Tang, D., Comish, P., and Kang, R. (2020). The hallmarks of COVID-19 disease. PLoS. Pathog., 16."
},
{
"DOI": "10.1165/rcmb.2013-0003OC",
"article-title": "Reactive oxygen species induce antiviral innate immune response through IFN-lambda regulation in human nasal epithelial cells",
"author": "Kim",
"doi-asserted-by": "crossref",
"first-page": "855",
"journal-title": "Am. J. Respir. Cell. Mol. Biol.",
"key": "ref_33",
"volume": "49",
"year": "2013"
},
{
"DOI": "10.3390/molecules23102561",
"doi-asserted-by": "crossref",
"key": "ref_34",
"unstructured": "Vlasova, I.I. (2018). Peroxidase activity of human hemoproteins: Keeping the fire under control. Molecules., 23."
},
{
"DOI": "10.1128/spectrum.00522-21",
"doi-asserted-by": "crossref",
"key": "ref_35",
"unstructured": "Cao, Z., and Cheng, G. (2022). Recombinant myeloperoxidase as a New class of antimicrobial agents. Microbiol. Spectr., 10."
},
{
"DOI": "10.1016/j.jinorgbio.2021.111546",
"doi-asserted-by": "crossref",
"key": "ref_36",
"unstructured": "Camp, O.G., Bai, D., Gonullu, D.C., Nayak, N., and Abu-Soud, H.M. (2021). Melatonin interferes with COVID-19 at several distinct ROS-related steps. J. Inorg. Biochem., 223."
},
{
"DOI": "10.7150/ijbs.51811",
"article-title": "A Multiple-hit hypothesis involving reactive oxygen species and myeloperoxidase explains clinical deterioration and fatality in COVID-19",
"author": "Goud",
"doi-asserted-by": "crossref",
"first-page": "62",
"journal-title": "Int. J. Biol. Sci.",
"key": "ref_37",
"volume": "17",
"year": "2021"
},
{
"DOI": "10.1074/jbc.275.48.37524",
"article-title": "Nitric oxide is a physiological substrate for mammalian peroxidases",
"author": "Hazen",
"doi-asserted-by": "crossref",
"first-page": "37524",
"journal-title": "J. Biol. Chem.",
"key": "ref_38",
"volume": "275",
"year": "2000"
},
{
"DOI": "10.1016/j.niox.2020.07.005",
"article-title": "Blood nitrate and nitrite modulating nitric oxide bioavailability: Potential therapeutic functions in COVID-19",
"author": "Yamasaki",
"doi-asserted-by": "crossref",
"first-page": "29",
"journal-title": "Nitric. Oxide.",
"key": "ref_39",
"volume": "103",
"year": "2020"
},
{
"DOI": "10.3390/ijms22115438",
"doi-asserted-by": "crossref",
"key": "ref_40",
"unstructured": "Kouhpayeh, S., Shariati, L., Boshtam, M., Rahimmanesh, I., Mirian, M., Esmaeili, Y., Najaflu, M., Khanahmad, N., Zeinalian, M., and Trovato, M. (2021). The molecular basis of COVID-19 pathogenesis, conventional and nanomedicine therapy. Int. J. Mol. Sci., 22."
},
{
"DOI": "10.1016/j.freeradbiomed.2021.08.237",
"article-title": "Serum nitrite and nitrate: A potential biomarker for post-COVID-19 complications?",
"author": "Wang",
"doi-asserted-by": "crossref",
"first-page": "216",
"journal-title": "Free Radic. Biol. Med.",
"key": "ref_41",
"volume": "175",
"year": "2021"
},
{
"DOI": "10.3390/nu13041261",
"doi-asserted-by": "crossref",
"key": "ref_42",
"unstructured": "Corrao, S., Bocchio, M.R., Monaco, M.L., Natoli, G., Cavezzi, A., Troiani, E., and Argano, C. (2021). Does evidence exist to blunt inflammatory response by nutraceutical supplementation during COVID-19 pandemic? An overview of systematic reviews of vitamin D, vitamin C, melatonin, and Zinc. Nutrients, 13."
},
{
"DOI": "10.1515/znc-2021-0101",
"article-title": "NLRP3 inflammasome activation and oxidative stress status in the mild and moderate SARS-CoV-2 infected patients: Impact of melatonin as a medicinal supplement",
"author": "Ghaleh",
"doi-asserted-by": "crossref",
"first-page": "37",
"journal-title": "Z. Naturforsch. C J. Biosci.",
"key": "ref_43",
"volume": "77",
"year": "2022"
},
{
"DOI": "10.1007/s00394-019-02123-0",
"article-title": "Melatonin supplementation and pro-inflammatory mediators: A systematic review and meta-analysis of clinical trials",
"author": "Zarezadeh",
"doi-asserted-by": "crossref",
"first-page": "1803",
"journal-title": "Eur. J. Nutr.",
"key": "ref_44",
"volume": "59",
"year": "2020"
},
{
"DOI": "10.1016/j.arcmed.2021.06.006",
"article-title": "Efficacy of a low dose of melatonin as an adjunctive therapy in hospitalized patients with COVID-19: A randomized, double-blind clinical Trial",
"author": "Farnoosh",
"doi-asserted-by": "crossref",
"first-page": "79",
"journal-title": "Arch. Med. Res.",
"key": "ref_45",
"volume": "53",
"year": "2021"
},
{
"article-title": "High dose melatonin as an adjuvant therapy in intubated patients with COVID-19: A randomized clinical trial",
"author": "Alizadeh",
"first-page": "454",
"journal-title": "J. Taibah Univ. Med. Sci.",
"key": "ref_46",
"volume": "17",
"year": "2022"
},
{
"DOI": "10.3390/diseases8040044",
"doi-asserted-by": "crossref",
"key": "ref_47",
"unstructured": "Cardinali, D.P., Brown, G.M., and Pandi-Perumal, S.R. (2020). Can Melatonin be a potential “Silver Bullet” in treating COVID-19 patients?. Diseases, 8."
},
{
"DOI": "10.3389/fimmu.2020.00172",
"article-title": "TLR2-melatonin feedback loop regulates the activation of NLRP3 inflammasome in murine allergic airway inflammation",
"author": "Wu",
"doi-asserted-by": "crossref",
"first-page": "172",
"journal-title": "Front. Immunol.",
"key": "ref_48",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1055/s-0043-1777780",
"article-title": "COVID-19-related brief insomnia in a 13-year-old adolescent girl",
"doi-asserted-by": "crossref",
"first-page": "e112",
"journal-title": "Sleep. Sci.",
"key": "ref_49",
"volume": "17",
"year": "2024"
},
{
"DOI": "10.1016/j.advms.2023.09.007",
"article-title": "Safety and efficacy of melatonin as an adjuvant therapy in COVID-19 patients: Systematic review and meta-analysis",
"author": "Taha",
"doi-asserted-by": "crossref",
"first-page": "341",
"journal-title": "Adv. Med. Sci.",
"key": "ref_50",
"volume": "68",
"year": "2023"
},
{
"DOI": "10.1016/j.explore.2023.06.009",
"article-title": "Melatonin, vitamins and minerals supplements for the treatment of COVID-19 and Covid-like illness: A prospective, randomized, double-blind multicenter study",
"author": "Mahjoub",
"doi-asserted-by": "crossref",
"first-page": "95",
"journal-title": "Explore",
"key": "ref_51",
"volume": "20",
"year": "2024"
},
{
"DOI": "10.1002/jmv.27312",
"article-title": "Melatonin effects on sleep quality and outcomes of COVID-19 patients: An open-label, randomized, controlled trial",
"author": "Heydari",
"doi-asserted-by": "crossref",
"first-page": "263",
"journal-title": "J. Med. Virol.",
"key": "ref_52",
"volume": "94",
"year": "2022"
},
{
"DOI": "10.1016/j.ijid.2021.10.012",
"article-title": "The effect of melatonin on thrombosis, sepsis and mortality rate in COVID-19 patients",
"author": "Hasan",
"doi-asserted-by": "crossref",
"first-page": "79",
"journal-title": "Int. J. Infect. Dis.",
"key": "ref_53",
"volume": "114",
"year": "2022"
},
{
"article-title": "A pilot study on controlling coronavirus disease 2019 (COVID-19) inflammation using melatonin supplement",
"author": "Alizadeh",
"first-page": "494",
"journal-title": "Iran. J. Allergy. Asthma. Immunol.",
"key": "ref_54",
"volume": "20",
"year": "2021"
},
{
"DOI": "10.25258/ijddt.12.1.21",
"article-title": "The effect of melatonin on C-reactive protein, serum ferritin and D-dimer in COVID-19 patients",
"author": "Hasan",
"doi-asserted-by": "crossref",
"first-page": "108",
"journal-title": "Int. J. Drug. Delivery. Technol.",
"key": "ref_55",
"volume": "12",
"year": "2022"
},
{
"DOI": "10.1007/s10787-022-01096-7",
"article-title": "Efficacy and safety of oral melatonin in patients with severe COVID-19: A randomized controlled trial",
"author": "Ameri",
"doi-asserted-by": "crossref",
"first-page": "265",
"journal-title": "Inflammopharmacology",
"key": "ref_56",
"volume": "1",
"year": "2023"
},
{
"DOI": "10.3122/jabfm.2022.04.210529",
"article-title": "A pilot of a randomized control trial of melatonin and vitamin C for mild-to-moderate COVID-19",
"author": "Fogleman",
"doi-asserted-by": "crossref",
"first-page": "695",
"journal-title": "J. Am. Board. Fam. Med.",
"key": "ref_57",
"volume": "35",
"year": "2022"
},
{
"DOI": "10.1093/jtm/taab195",
"article-title": "Melatonin does not reduce mortality in adult hospitalized patients with COVID-19: A multicenter retrospective observational study",
"author": "Geoffroy",
"doi-asserted-by": "crossref",
"first-page": "taab195",
"journal-title": "J. Travel. Med.",
"key": "ref_58",
"volume": "29",
"year": "2022"
},
{
"DOI": "10.3390/jcm10245857",
"doi-asserted-by": "crossref",
"key": "ref_59",
"unstructured": "Bologna, C., Madonna, P., and Pone, E. (2021). Efficacy of prolonged-release melatonin 2 mg (PRM 2 mg) prescribed for insomnia in hospitalized patients for COVID-19: A retrospective observational study. J. Clin. Med., 10."
},
{
"DOI": "10.1016/j.ejphar.2021.174193",
"article-title": "Evaluation of Th1 and Th2 mediated cellular and humoral immunity in patients with COVID-19 following the use of melatonin as an adjunctive treatment",
"author": "Hosseini",
"doi-asserted-by": "crossref",
"first-page": "174193",
"journal-title": "Eur. J. Pharmacol.",
"key": "ref_60",
"volume": "904",
"year": "2021"
},
{
"DOI": "10.3389/fendo.2019.00488",
"article-title": "Melatonin signaling a key regulator of glucose homeostasis and energy metabolism",
"author": "Owino",
"doi-asserted-by": "crossref",
"first-page": "488",
"journal-title": "Front. Endocrinol.",
"key": "ref_61",
"volume": "10",
"year": "2019"
},
{
"DOI": "10.3390/ijms22020764",
"doi-asserted-by": "crossref",
"key": "ref_62",
"unstructured": "Reiter, R.J., Sharma, R., and Rosales-Corral, S. (2021). Anti-Warburg effect of melatonin: A proposed mechanism to explain its inhibition of multiple diseases. Int. J. Mol. Sci., 22."
},
{
"DOI": "10.1016/j.cca.2020.06.033",
"article-title": "Hyperferritinemia in critically ill COVID-19 patients—Is ferritin the product of inflammation or a pathogenic mediator?",
"author": "Weigand",
"doi-asserted-by": "crossref",
"first-page": "249",
"journal-title": "Clin. Chim. Acta.",
"key": "ref_63",
"volume": "509",
"year": "2020"
},
{
"DOI": "10.1093/gerona/gly059",
"article-title": "The protective effect of melatonin against age-associated, sarcopenia-dependent tubular aggregate formation, lactate depletion, and mitochondrial changes",
"author": "Sayed",
"doi-asserted-by": "crossref",
"first-page": "1330",
"journal-title": "J. Gerontol. A Biol. Sci. Med. Sci.",
"key": "ref_64",
"volume": "73",
"year": "2018"
},
{
"DOI": "10.3390/molecules201018886",
"article-title": "Melatonin as a potent and inducible endogenous antioxidant: Synthesis and metabolism",
"author": "Tan",
"doi-asserted-by": "crossref",
"first-page": "18886",
"journal-title": "Molecules",
"key": "ref_65",
"volume": "20",
"year": "2015"
},
{
"DOI": "10.1038/s41419-019-1556-7",
"article-title": "Melatonin as a master regulator of cell death and inflammation: Molecular mechanisms and clinical implications for newborn care",
"author": "Tarocco",
"doi-asserted-by": "crossref",
"first-page": "317",
"journal-title": "Cell Death. Dis.",
"key": "ref_66",
"volume": "10",
"year": "2019"
},
{
"DOI": "10.3390/antiox10071152",
"doi-asserted-by": "crossref",
"key": "ref_67",
"unstructured": "Ramos, E., López-Muñoz, F., Gil-Martín, E., Egea, J., Álvarez-Merz, I., Painuli, S., Semwal, P., Martins, N., Hernández-Guijo, J.M., and Romero, A. (2021). The coronavirus disease 2019 (COVID-19): Key emphasis on melatonin safety and therapeutic efficacy. Antioxidants, 10."
},
{
"DOI": "10.1001/jama.2019.21118",
"article-title": "Diagnosis and treatment of adults with community-acquired pneumonia",
"author": "Olson",
"doi-asserted-by": "crossref",
"first-page": "885",
"journal-title": "JAMA",
"key": "ref_68",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1186/s13054-019-2663-7",
"article-title": "The SOFA score-development, utility, and challenges of accurate assessment in clinical trials",
"author": "Lambden",
"doi-asserted-by": "crossref",
"first-page": "374",
"journal-title": "Crit. Care",
"key": "ref_69",
"volume": "23",
"year": "2019"
},
{
"article-title": "Acute respiratory distress syndrome: The Berlin Definition",
"author": "Ranieri",
"first-page": "2526",
"journal-title": "JAMA",
"key": "ref_70",
"volume": "307",
"year": "2012"
},
{
"DOI": "10.1016/j.csbj.2021.02.009",
"article-title": "Antioxidants and pentoxifylline as coadjuvant measures to standard therapy to improve prognosis of patients with pneumonia by COVID-19",
"author": "Cherit",
"doi-asserted-by": "crossref",
"first-page": "1379",
"journal-title": "Comput. Struct. Biotechnol. J.",
"key": "ref_71",
"volume": "19",
"year": "2021"
},
{
"DOI": "10.1056/NEJMoa032193",
"article-title": "National heart, lung, and blood institute ARDS clinical trials network higher versus lower positive end-expiratory pressures in patients with the acute respiratory distress syndrome",
"author": "Brower",
"doi-asserted-by": "crossref",
"first-page": "327",
"journal-title": "N. Engl. J. Med.",
"key": "ref_72",
"volume": "351",
"year": "2004"
},
{
"DOI": "10.1111/jth.14810",
"article-title": "ISTH interim guidance on recognition and management of coagulopathy in COVID-19",
"author": "Thachil",
"doi-asserted-by": "crossref",
"first-page": "1023",
"journal-title": "J. Thromb. Haemost.",
"key": "ref_73",
"volume": "18",
"year": "2020"
},
{
"article-title": "Position statement: Cardiopulmonary resuscitation of patients with confirmed or suspected COVID-19-2020",
"author": "Timerman",
"first-page": "1078",
"journal-title": "Arq. Bras. Cardiol.",
"key": "ref_74",
"volume": "114",
"year": "2020"
},
{
"DOI": "10.3390/ijms241310429",
"doi-asserted-by": "crossref",
"key": "ref_75",
"unstructured": "Soto, M.E., Pérez-Torres, I., Manzano-Pech, L., Soria-Castro, E., Morales-Marín, A., Ramírez-Marroquín, E.S., Martínez-Hernández, H., Herrera-Alarcón, V., and Guarner-Lans, V. (2023). Reduced levels of selenium and thioredoxin reductase in the thoracic aorta could contribute to aneurysm formation in patients with Marfan syndrome. Int. J. Mol. Sci., 24."
},
{
"DOI": "10.3906/sag-2011-139",
"article-title": "A sensitive indicator for the severity of COVID-19: Thiol",
"author": "Erel",
"doi-asserted-by": "crossref",
"first-page": "921",
"journal-title": "Turk. J. Med. Sci.",
"key": "ref_76",
"volume": "51",
"year": "2021"
}
],
"reference-count": 76,
"references-count": 76,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/1422-0067/25/8/4543"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Redox Homeostasis Alteration Is Restored through Melatonin Treatment in COVID-19 Patients: A Preliminary Study",
"type": "journal-article",
"volume": "25"
}
