Plasma 25(OH)D Level is Associated with the Nucleic Acid Negative Conversion Time of COVID-19 Patients: An Exploratory Study
et al., Infection and Drug Resistance, doi:10.2147/idr.s400561, Feb 2023
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 158 COVID+ patients in China, showing low vitamin D levels associated with slower viral clearance.
This is the 159th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
Standard of Care (SOC) for COVID-19 in the study country,
China, is poor with low average efficacy for approved treatments1.
|
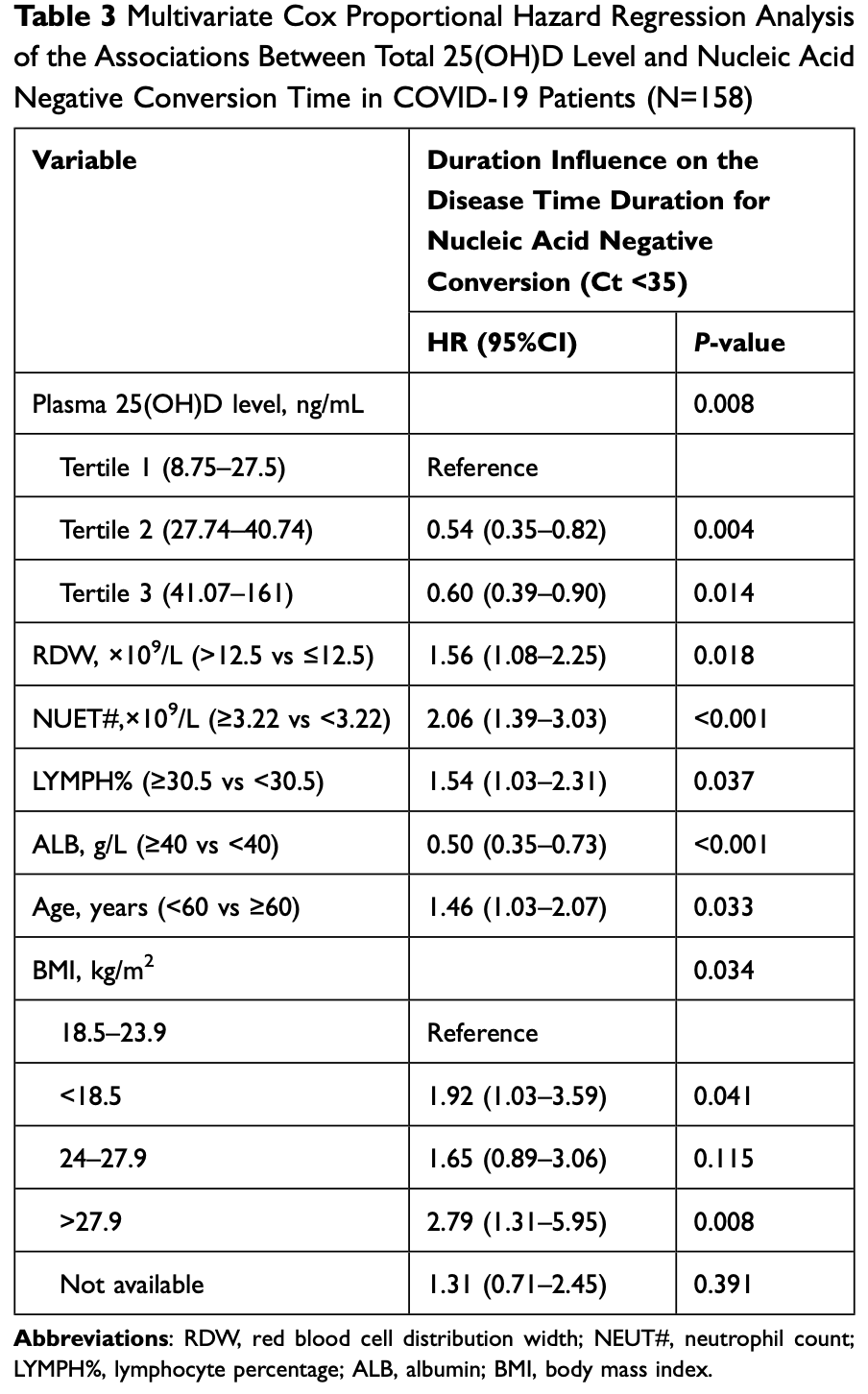
viral clearance, 40.0% improved, HR 0.60, p = 0.01, high D levels (≥41.07ng/mL) 52, low D levels (<27.5ng/mL) 53, adjusted per study, tertile 3 vs. tertile 1, multivariable, Cox proportional hazards.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Chen et al., 28 Feb 2023, retrospective, China, peer-reviewed, 9 authors, study period 1 June, 2022 - 5 July, 2022.
Contact: pzchen@me.com, guzhidongruijin@163.com.
Plasma 25(OH)D Level is Associated with the Nucleic Acid Negative Conversion Time of COVID-19 Patients: An Exploratory Study
Infection and Drug Resistance, doi:10.2147/idr.s400561
Vitamin D, an essential nutrient and a pleiotropic steroid hormone, has been reported to be associated with the risk and severity in patients infected with Coronavirus Disease-2019 (COVID-19). The role of vitamin D in predicting clinical outcome for COVID-19 patients is unknown. Here, we aimed to determine the prognostic value of plasma 25(OH)D level in COVID-19 patients. Patients and Methods: A total of 158 patients infected with novel COVID-19 Omicron variants in Shanghai were recruited in this study and were categorized into three groups by the tertile levels of plasma 25(OH)D. Plasma 25(OH)D level was determined along with routine blood tests related to liver and renal functions in newly diagnosed COVID-19 patients at admission. The nucleic acid negative conversion time of throat swab samples was evaluated as the primary clinical outcome. The prognostic value of clinical characteristics and plasma 25(OH)D level was assessed using the Kaplan-Meier plot and Cox proportional hazards regression tests. Results: Higher level of plasma 25(OH)D level in COVID-19 patients was independently associated with shorter nucleic acid negative conversion time from COVID-19 infection (multivariate adjusted HR: 0.54, 95%CI: 0.35-0.82, P=0.004, tertile 2 vs 1; multivariate adjusted HR: 0.60, 95%CI: 0.39-0.90, P=0.014, tertile 3 vs 1). Conclusion: Plasma 25(OH)D level may serve as an independent prognostic factor in COVID-19 patient. Our findings indicate the protective roles of vitamin D supplementation in the regiment of patients with COVID-19.
Abbreviations vitD, plasma 25(OH)D level; WBC#, white blood cell count; RDW, red blood cell distribution width; RBC#, red blood cell count; PLT#, platelet count; NEUT%, neutrophil percentage; MPV, mean platelet volume; NEUT#, neutrophil count; MONO%, monocyte percentage; MONO#, monocyte count; MCHC, mean corpuscular hemoglobin concentration; MCV, mean corpuscular volume; LYMPH%, lymphocyte percentage; MCH, mean corpuscular hemoglobin; HGB, hemoglobin; LYMPH#, lymphocyte count; HCT, hematocrit; EO#, eosinophil count; EO%, eosinophil percentage; BASO%, basophil percentage; BASO#, basophil count; A/G, albumin-globulin ratio; ALB, albumin; ALP, alkaline phosphatase; ALT, alanine aminotransferase; AST, aspartate aminotransferase; UREA, urea; CREA, creatinine; DBIL, direct bilirubin; GGT, γ-glutamyl transpeptidase; TBIL, total bilirubin; TP, total protein; TBA, total biliary acid; UA, uric acid; PA, prealbumin; ADA, adenosine deaminase; eGFR, estimated glomerular filtration rate; CG, cholyglycine.
Author Contributions All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure The authors..
References
Abdollahi, Sarvestani, Rafat, The association between the level of serum 25(OH) vitamin D, obesity, and underlying diseases with the risk of developing COVID-19 infection: a case-control study of hospitalized patients in Tehran, Iran, J Med Virol, doi:10.1002/jmv.26726
Arora, Patel, Nicol, Vitamin D and the ability to produce 1,25(OH)2D are critical for protection from viral infection of the lungs, Nutrients, doi:10.3390/nu14153061
Baktash, Hosack, Patel, Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad Med J, doi:10.1136/postgradmedj-2020-138712
Bergman, Lindh, Björkhem-Bergman, Lindh, Vitamin D and respiratory tract infections: a systematic review and meta-analysis of randomized controlled trials, PLoS One, doi:10.1371/journal.pone.0065835
Biesalski, Obesity, vitamin D deficiency and old age a serious combination with respect to coronavirus disease-2019 severity and outcome, Curr Opin Clin Nutr Metab Care, doi:10.1097/MCO.0000000000000700
Castillo, Costa, Barrios, Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: a pilot randomized clinical study, J Steroid Biochem Mol Biol, doi:10.1016/j.jsbmb.2020.105751
Charan, Goyal, Saxena, Yadav, Vitamin D for prevention of respiratory tract infections: a systematic review and meta-analysis, J Pharmacol Pharmacother, doi:10.4103/0976-500X.103685
Cheung, Chan, Jin, Lessons learned from the fifth wave of COVID-19 in Hong Kong in early 2022, Emerg Microbes Infect, doi:10.1080/22221751.2022.2060137
D'avolio, Avataneo, Manca, 25-hydroxyvitamin D concentrations are lower in patients with positive PCR for SARS-CoV-2, Nutrients, doi:10.3390/nu12051359
Daneshkhah, Agrawal, Eshein, Subramanian, Roy et al., Evidence for possible association of vitamin D status with cytokine storm and unregulated inflammation in COVID-19 patients, Aging Clin Exp Res, doi:10.1007/s40520-020-01677-y
De, Puente-Yagüe, Cuadrado-Cenzual, Hernández-Cabria, Collado-Yurrita, Vitamin D: and its role in breast cancer, Kaohsiung J Med Sci, doi:10.1016/j.kjms.2018.03.004
Filippo, Allora, Doga, Vitamin D levels are associated with blood glucose and BMI in COVID-19 patients, predicting disease severity, J Clin Endocrinol Metab, doi:10.1210/clinem/dgab599
Foy, Carlson, Reinertsen, Association of red blood cell distribution width with mortality risk in hospitalized adults with SARS-CoV-2 infection, JAMA Netw Open, doi:10.1001/jamanetworkopen.2020.22058
Fu, Han, Zhu, Risk factors for viral RNA shedding in COVID-19 patients, Eur Respir J, doi:10.1183/13993003.01190-2020
Hayashi, Okamatsu, Ogasawara, Oral supplementation of the vitamin D metabolite 25(OH)D3 against influenza virus infection in mice, Nutrients, doi:10.3390/nu12072000
Henry, Benoit, Benoit, Red Blood Cell Distribution Width (RDW) predicts COVID-19 severity: a prospective, observational study from the Cincinnati SARS-CoV-2 emergency department cohort, Diagnostics, doi:10.3390/diagnostics10090618
Huang, Sun, Xing, Wang, Functional impairment and serum albumin predict in-hospital mortality in nonagenarians with acute infection: a retrospective cohort study, BMC Geriatr, doi:10.1186/s12877-019-1301-1
Huang, Wang, Li, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet
Im, Je, Baek, Chung, Kwon et al., Nutritional status of patients with COVID-19, Int J Infect Dis, doi:10.1016/j.ijid.2020.08.018
Jagannath, Filippini, Pietrantonj, Vitamin D for the management of multiple sclerosis, Cochrane Database Syst Rev, doi:10.1002/14651858.CD008422.pub3
Jeon, Shin, Exploring vitamin D metabolism and function in cancer, Exp Mol Med, doi:10.1038/s12276-018-0038-9
Jolliffe, Griffiths, Martineau, Vitamin D in the prevention of acute respiratory infection: systematic review of clinical studies, J Steroid Biochem Mol Biol, doi:10.1016/j.jsbmb.2012.11.017
Kaufman, Niles, Kroll, Bi, Holick, SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels, PLoS One, doi:10.1371/journal.pone.0239252
Lau, Majumder, Torabi, Vitamin D insufficiency is prevalent in severe COVID-19, medRxiv, doi:10.1101/2020.04.24.20075838
Li, Chen, Duan, Bioavailable 25(OH)D but not total 25(OH)D is an independent determinant for bone mineral density in Chinese postmenopausal women, doi:10.1016/j.ebiom.2016.11.029
Liu, Sun, Wang, Zhang, Zhao et al., Low vitamin D status is associated with coronavirus disease 2019 outcomes: a systematic review and meta-analysis, Int J Infect Dis, doi:10.1016/j.ijid.2020.12.077
Luo, Ye, Shao, Vitamin D status presents different relationships with severity in metabolic-associated fatty liver disease patients with or without hepatitis B infection, Nutrients, doi:10.3390/nu14102114
Ma, Zhou, Heianza, Qi, Habitual use of vitamin D supplements and risk of coronavirus disease 2019 (COVID-19) infection: a prospective study in UK Biobank, Am J Clin Nutr, doi:10.1093/ajcn/nqaa381
Martineau, Jolliffe, Hooper, Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data, BMJ, doi:10.1136/bmj.i6583
Merzon, Tworowski, Gorohovski, Low plasma 25(OH) vitamin D level is associated with increased risk of COVID-19 infection: an Israeli population-based study, FEBS J, doi:10.1111/febs.15495
Murai, Fernandes, Sales, Effect of a single high dose of vitamin D3 on hospital length of stay in patients with moderate to severe COVID-19: a randomized clinical trial, JAMA, doi:10.1001/jama.2020.26848
Rhodes, Dunstan, Laird, Subramanian, Kenny, COVID-19 mortality increases with northerly latitude after adjustment for age suggesting a link with ultraviolet and vitamin D, BMJ Nutr Prev Health, doi:10.1136/bmjnph-2020-000110
Smet, Smet, Herroelen, Gryspeerdt, Martens, Serum 25(OH)D level on hospital admission associated with COVID-19 stage and mortality, Am J Clin Pathol, doi:10.1093/ajcp/aqaa252
Tentolouris, Samakidou, Eleftheriadou, Tentolouris, Jude, The effect of vitamin D supplementation on mortality and intensive care unit admission of COVID-19 patients. A systematic review, meta-analysis and meta-regression, Diabetes Metab Res Rev, doi:10.1002/dmrr.3517
Wang, Deng, Gou, Preliminary study to identify severe from moderate cases of COVID-19 using combined hematology parameters, Ann Transl Med, doi:10.21037/atm-20-3391
Xu, Yang, Chen, Luo, Zhang et al., Vitamin D alleviates lipopolysaccharide-induced acute lung injury via regulation of the renin-angiotensin system, Mol Med Rep, doi:10.3892/mmr.2017.7546
Ye, Wang, Mao, Epidemiological analysis of COVID-19 and practical experience from China, J Med Virol, doi:10.1002/jmv.25813
Zhang, Zhang, Chen, Shanghai's life-saving efforts against the current omicron wave of the COVID-19 pandemic, Lancet
Zhu, Zhu, Gu, Zhan, Chen et al., Association between vitamin D and influenza: meta-analysis and systematic review of randomized controlled trials, Front Nutr, doi:10.3389/fnut.2021.799709
DOI record:
{
"DOI": "10.2147/idr.s400561",
"ISSN": [
"1178-6973"
],
"URL": "http://dx.doi.org/10.2147/idr.s400561",
"author": [
{
"affiliation": [],
"family": "Chen",
"given": "Changqiang",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0001-6888-0305",
"affiliation": [],
"authenticated-orcid": true,
"family": "Li",
"given": "Pu",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Chen",
"given": "Jiuming",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Liu",
"given": "Chunxiao",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wang",
"given": "Xiaodan",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Cai",
"given": "Jialin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Xiang",
"given": "Enfei",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Gu",
"given": "Zhidong",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Chen",
"given": "Peizhan",
"sequence": "additional"
}
],
"container-title": "Infection and Drug Resistance",
"container-title-short": "IDR",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
2,
15
]
],
"date-time": "2023-02-15T04:05:06Z",
"timestamp": 1676433906000
},
"deposited": {
"date-parts": [
[
2023,
2,
15
]
],
"date-time": "2023-02-15T04:05:38Z",
"timestamp": 1676433938000
},
"indexed": {
"date-parts": [
[
2023,
2,
16
]
],
"date-time": "2023-02-16T05:53:36Z",
"timestamp": 1676526816590
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2023,
2
]
]
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by-nc/3.0/",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
2,
1
]
],
"date-time": "2023-02-01T00:00:00Z",
"timestamp": 1675209600000
}
}
],
"link": [
{
"URL": "https://www.dovepress.com/getfile.php?fileID=87516",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://www.dovepress.com/getfile.php?fileID=87516",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "301",
"original-title": [],
"page": "937-947",
"prefix": "10.2147",
"published": {
"date-parts": [
[
2023,
2
]
]
},
"published-online": {
"date-parts": [
[
2023,
2
]
]
},
"publisher": "Informa UK Limited",
"reference": [
{
"DOI": "10.1002/jmv.25813",
"author": "Ye",
"doi-asserted-by": "publisher",
"first-page": "755",
"journal-title": "J Med Virol",
"key": "ref1",
"volume": "92",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(22)00838-8",
"author": "Zhang",
"doi-asserted-by": "publisher",
"first-page": "2011",
"journal-title": "Lancet",
"key": "ref2",
"volume": "399",
"year": "2022"
},
{
"DOI": "10.1080/22221751.2022.2060137",
"author": "Cheung",
"doi-asserted-by": "publisher",
"first-page": "1072",
"journal-title": "Emerg Microbes Infect",
"key": "ref3",
"volume": "11",
"year": "2022"
},
{
"key": "ref4",
"unstructured": "Diagnosis and treatment protocol for novel coronavirus pneumonia (Trial Version 9); 2022. Available from: http://www.gov.cn/zhengce/zhengceku/2022-03/15/content_5679257.htm. Accessed February 11, 2023."
},
{
"DOI": "10.3390/nu14102114",
"author": "Luo",
"doi-asserted-by": "publisher",
"first-page": "2114",
"journal-title": "Nutrients",
"key": "ref5",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1038/s12276-018-0038-9",
"author": "Jeon",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Exp Mol Med",
"key": "ref6",
"volume": "50",
"year": "2018"
},
{
"DOI": "10.1016/j.kjms.2018.03.004",
"author": "de La Puente-Yagüe",
"doi-asserted-by": "publisher",
"first-page": "423",
"journal-title": "Kaohsiung J Med Sci",
"key": "ref7",
"volume": "34",
"year": "2018"
},
{
"DOI": "10.1002/14651858.CD008422.pub3",
"author": "Jagannath",
"doi-asserted-by": "publisher",
"first-page": "CD008422",
"journal-title": "Cochrane Database Syst Rev",
"key": "ref8",
"volume": "9",
"year": "2018"
},
{
"DOI": "10.1136/bmj.i6583",
"author": "Martineau",
"doi-asserted-by": "publisher",
"first-page": "i6583",
"journal-title": "BMJ",
"key": "ref9",
"volume": "356",
"year": "2017"
},
{
"DOI": "10.1371/journal.pone.0239252",
"author": "Kaufman",
"doi-asserted-by": "publisher",
"first-page": "e0239252",
"journal-title": "PLoS One",
"key": "ref10",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1111/febs.15495",
"author": "Merzon",
"doi-asserted-by": "publisher",
"first-page": "3693",
"journal-title": "FEBS J",
"key": "ref11",
"volume": "287",
"year": "2020"
},
{
"DOI": "10.3390/nu12051359",
"author": "D’Avolio",
"doi-asserted-by": "publisher",
"first-page": "1359",
"journal-title": "Nutrients",
"key": "ref12",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/j.ijid.2020.08.018",
"author": "Im",
"doi-asserted-by": "publisher",
"first-page": "390",
"journal-title": "Int J Infect Dis",
"key": "ref13",
"volume": "100",
"year": "2020"
},
{
"DOI": "10.1002/jmv.26726",
"author": "Abdollahi",
"doi-asserted-by": "publisher",
"first-page": "2359",
"journal-title": "J Med Virol",
"key": "ref14",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.1016/j.ijid.2020.12.077",
"author": "Liu",
"doi-asserted-by": "publisher",
"first-page": "58",
"journal-title": "Int J Infect Dis",
"key": "ref15",
"volume": "104",
"year": "2021"
},
{
"DOI": "10.1093/ajcp/aqaa252",
"author": "De Smet",
"doi-asserted-by": "publisher",
"first-page": "381",
"journal-title": "Am J Clin Pathol",
"key": "ref16",
"volume": "155",
"year": "2021"
},
{
"DOI": "10.1136/postgradmedj-2020-138712",
"author": "Baktash",
"doi-asserted-by": "publisher",
"first-page": "442",
"journal-title": "Postgrad Med J",
"key": "ref17",
"volume": "97",
"year": "2021"
},
{
"DOI": "10.1016/j.jsbmb.2020.105751",
"author": "Entrenas Castillo",
"doi-asserted-by": "publisher",
"first-page": "105751",
"journal-title": "J Steroid Biochem Mol Biol",
"key": "ref18",
"volume": "203",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.26848",
"author": "Murai",
"doi-asserted-by": "publisher",
"first-page": "1053",
"journal-title": "JAMA",
"key": "ref19",
"volume": "325",
"year": "2021"
},
{
"DOI": "10.3390/nu14153061",
"author": "Arora",
"doi-asserted-by": "publisher",
"first-page": "3061",
"journal-title": "Nutrients",
"key": "ref20",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1016/j.jsbmb.2012.11.017",
"author": "Jolliffe",
"doi-asserted-by": "publisher",
"first-page": "321",
"journal-title": "J Steroid Biochem Mol Biol",
"key": "ref21",
"volume": "136",
"year": "2013"
},
{
"DOI": "10.3389/fnut.2021.799709",
"author": "Zhu",
"doi-asserted-by": "publisher",
"first-page": "799709",
"journal-title": "Front Nutr",
"key": "ref22",
"volume": "8",
"year": "2022"
},
{
"DOI": "10.1101/2020.04.24.20075838",
"author": "Lau",
"doi-asserted-by": "publisher",
"journal-title": "medRxiv",
"key": "ref23",
"year": "2020"
},
{
"DOI": "10.1007/s40520-020-01677-y",
"author": "Daneshkhah",
"doi-asserted-by": "publisher",
"first-page": "2141",
"journal-title": "Aging Clin Exp Res",
"key": "ref24",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1136/bmjnph-2020-000110",
"author": "Rhodes",
"doi-asserted-by": "publisher",
"first-page": "118",
"journal-title": "BMJ Nutr Prev Health",
"key": "ref25",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.4103/0976-500X.103685",
"author": "Charan",
"doi-asserted-by": "publisher",
"first-page": "300",
"journal-title": "J Pharmacol Pharmacother",
"key": "ref26",
"volume": "3",
"year": "2012"
},
{
"DOI": "10.1371/journal.pone.0065835",
"author": "Bergman",
"doi-asserted-by": "publisher",
"first-page": "e65835",
"journal-title": "PLoS One",
"key": "ref27",
"volume": "8",
"year": "2013"
},
{
"DOI": "10.1093/ajcn/nqaa381",
"author": "Ma",
"doi-asserted-by": "publisher",
"first-page": "1275",
"journal-title": "Am J Clin Nutr",
"key": "ref28",
"volume": "113",
"year": "2021"
},
{
"DOI": "10.3390/nu12072000",
"author": "Hayashi",
"doi-asserted-by": "publisher",
"first-page": "2000",
"journal-title": "Nutrients",
"key": "ref29",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3892/mmr.2017.7546",
"author": "Xu",
"doi-asserted-by": "publisher",
"first-page": "7432",
"journal-title": "Mol Med Rep",
"key": "ref30",
"volume": "16",
"year": "2017"
},
{
"DOI": "10.1002/dmrr.3517",
"author": "Tentolouris",
"doi-asserted-by": "publisher",
"first-page": "e3517",
"journal-title": "Diabetes Metab Res Rev",
"key": "ref31",
"volume": "38",
"year": "2022"
},
{
"DOI": "10.1183/13993003.01190-2020",
"author": "Fu",
"doi-asserted-by": "publisher",
"first-page": "2001190",
"journal-title": "Eur Respir J",
"key": "ref32",
"volume": "56",
"year": "2020"
},
{
"DOI": "10.1186/s12877-019-1301-1",
"author": "Huang",
"doi-asserted-by": "publisher",
"first-page": "269",
"journal-title": "BMC Geriatr",
"key": "ref33",
"volume": "19",
"year": "2019"
},
{
"DOI": "10.3390/diagnostics10090618",
"author": "Henry",
"doi-asserted-by": "publisher",
"first-page": "618",
"journal-title": "Diagnostics",
"key": "ref34",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2020.22058",
"author": "Foy",
"doi-asserted-by": "publisher",
"first-page": "e2022058",
"journal-title": "JAMA Netw Open",
"key": "ref35",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.21037/atm-20-3391",
"author": "Wang",
"doi-asserted-by": "publisher",
"first-page": "593",
"journal-title": "Ann Transl Med",
"key": "ref36",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"author": "Huang",
"doi-asserted-by": "publisher",
"first-page": "497",
"journal-title": "Lancet",
"key": "ref37",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1210/clinem/dgab599",
"author": "Di Filippo",
"doi-asserted-by": "publisher",
"first-page": "e348",
"journal-title": "J Clin Endocrinol Metab",
"key": "ref38",
"volume": "107",
"year": "2022"
},
{
"DOI": "10.1097/MCO.0000000000000700",
"author": "Biesalski",
"doi-asserted-by": "publisher",
"first-page": "18",
"journal-title": "Curr Opin Clin Nutr Metab Care",
"key": "ref39",
"volume": "24",
"year": "2021"
},
{
"DOI": "10.1016/j.ebiom.2016.11.029",
"author": "Li",
"doi-asserted-by": "publisher",
"first-page": "184",
"journal-title": "EBioMedicine",
"key": "ref40",
"volume": "15",
"year": "2017"
}
],
"reference-count": 40,
"references-count": 40,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.dovepress.com/plasma-25ohd-level-is-associated-with-the-nucleic-acid-negative-conver-peer-reviewed-fulltext-article-IDR"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Pharmacology (medical)",
"Infectious Diseases",
"Pharmacology"
],
"subtitle": [],
"title": "Plasma 25(OH)D Level is Associated with the Nucleic Acid Negative Conversion Time of COVID-19 Patients: An Exploratory Study",
"type": "journal-article",
"volume": "Volume 16"
}
