The effect of Vitamin D levels on the course of COVID-19 in hospitalized patients – a 1-year prospective cohort study
et al., F1000Research, doi:10.12688/f1000research.131730.1, Mar 2023
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 301 hospitalized patients in Slovenia, showing higher mortality with vitamin D deficiency, without statistical significance. Fewer patients with severe cases were deficient, which authors hypothesize was due to their recommendations for supplementation - many patients reported initiating supplementation after symptoms started but before hospitalization (while asymptomatic patients did not initiate supplementation).
This is the 163rd of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
risk of death, 55.9% lower, RR 0.44, p = 0.24, high D levels (≥30nmol/L) 10 of 255 (3.9%), low D levels (<30nmol/L) 4 of 45 (8.9%), NNT 20.
|
|
risk of ICU admission, 58.8% higher, RR 1.59, p = 0.59, high D levels (≥30nmol/L) 27 of 255 (10.6%), low D levels (<30nmol/L) 3 of 45 (6.7%).
|
|
risk of severe case, 61.0% higher, RR 1.61, p = 0.009, high D levels (≥30nmol/L) 146 of 255 (57.3%), low D levels (<30nmol/L) 16 of 45 (35.6%).
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Siuka et al., 9 Mar 2023, prospective, Slovenia, peer-reviewed, 7 authors, study period December 2020 - December 2021.
Contact: josko.osredkar@kclj.si.
The effect of Vitamin D levels on the course of COVID-19 in hospitalized patients – a 1-year prospective cohort study
F1000Research, doi:10.12688/f1000research.131730.1
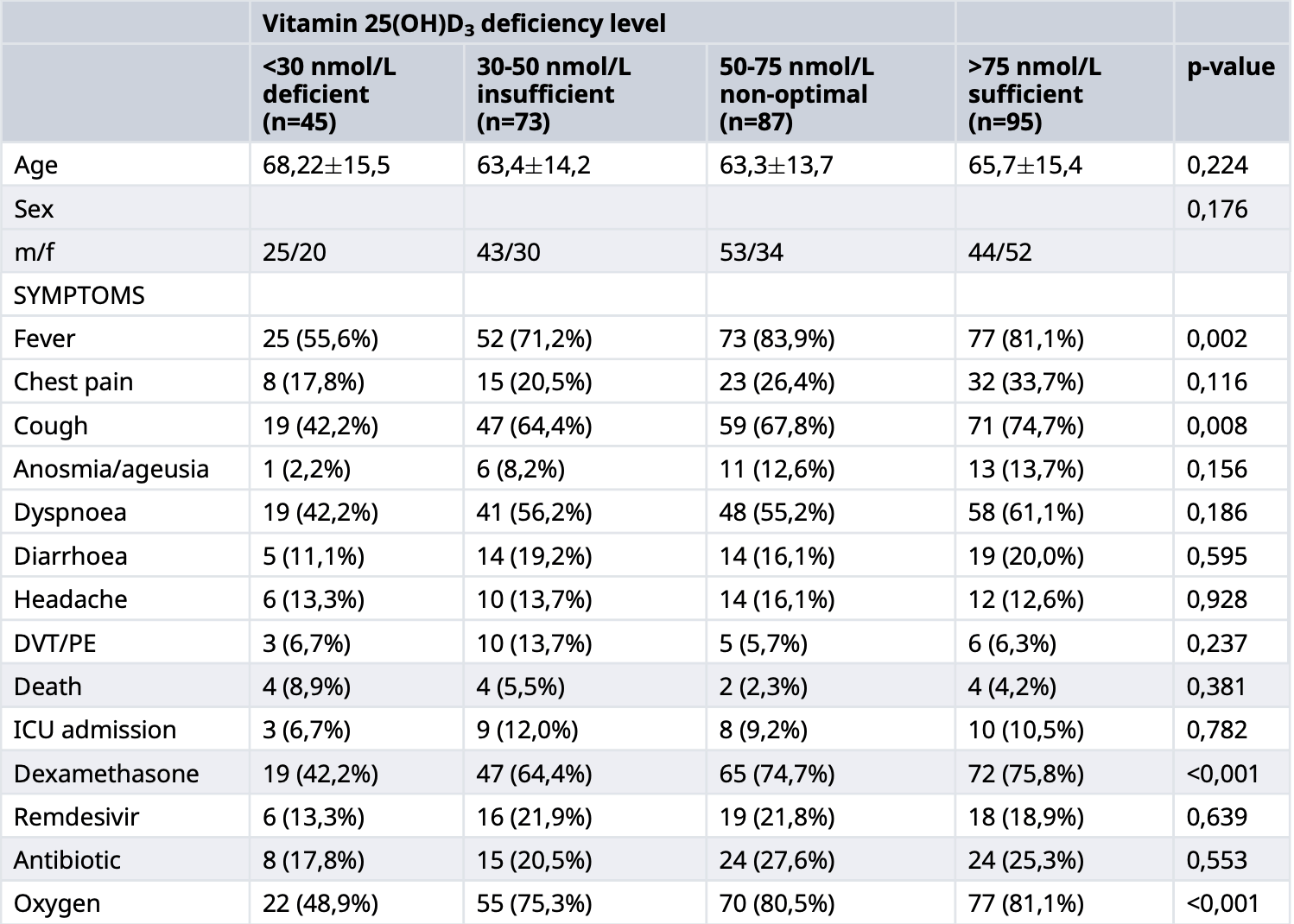
Background: The aim of the current study was to assess the patients with COVID-19 and the impact of vitamin D supplementation on the course of COVID-19. Methods: This prospective cohort study included patients hospitalized due to COVID-19 between December 2020 and December 2021. Patients' demographic, clinical, and laboratory parameters were analysed. Results: 301 participants were enrolled in the study. 46 (15,3%) had moderate, and 162 (53,8%) had severe COVID-19. 14 (4,7%) patients died, and 30 (10,0%) were admitted to the ICU due to disease worsening. The majority needed oxygen therapy (n=224; 74,4%). Average vitamin 25(OH)D3 levels were below optimal at the admittance, and vitamin D deficiency was detected in 205 individuals. More male patients were suffering from vitamin D deficiency. Patients with the more severe disease showed lower levels of vitamin 25(OH)D3 in their blood. The most severe group of patients had more symptoms that lasted significantly longer with progressing disease severity. This group of patients also suffered from more deaths, ICU admissions, and treatments with dexamethasone, remdesivir, and oxygen. Conclusion: Patients with the severe course of COVID-19 were shown to have increased inflammatory parameters, increased mortality, and higher incidence of vitamin D deficiency. The results suggest that the vitamin D deficiency might represent a significant risk factor for a severe course of COVID-19.
Author contribution D.Si. and J.O. conceived of the idea for the project; D.Si. and J.O. wrote the draft version of the manuscript, R.S. supervised the patients invited to participate in the study; J.U. and K.J. compiled the clinical data on the patients involved; O.J. and D. St were responsible for completing laboratory data, and D.St. and R.J. performed the statistical calculations. All authors reviewed and agreed with the manuscript, and final approval was given by D.Si. and J.O. All authors have read and agreed to the published version of the manuscript.
References
Alguwaihes, Sabico, Hasanato, Severe vitamin D deficiency is not related to SARS-CoV-2 infection but may increase mortality risk in hospitalized adults: a retrospective casecontrol study in an Arab Gulf country, Aging Clin. Exp. Res, doi:10.1007/s40520-021-01831-0
Ali, Role of vitamin D in preventing COVID-19 infection, progression and severity, J. Infect. Public Health, doi:10.1016/j.jiph.2020.06.021
Amer, Alotaibi, Vitamin D status of Arab Gulf residents screened for SARS-CoV-2 and its association with COVID-19 infection: a multi-centre case-control study, J. Transl. Med, doi:10.1186/s12967-021-02838-x
Amrein, Schnedl, Holl, Effect of high-dose vitamin D3 on hospital length of stay in critically ill patients with vitamin D deficiency: The VITdAL-ICU randomized clinical trial, JAMA, doi:10.1001/jama.2014.13204
Barnett, Zhao, Koyama, Vitamin D deficiency and risk of acute lung injury in severe sepsis and severe trauma: A casecontrol study, Ann. Intensive Care, doi:10.1186/2110-5820-4-5
Beard, Bearden, Striker, Vitamin D and the anti-viral state, J. Clin. Virol
Braun, Gibbons, Litonjua, Low serum 25-hydroxyvitamin D at critical care initiation is associated with increased mortality, Crit. Care Med, doi:10.1097/CCM.0b013e31822d74f3
Campi, Gennari, Merlotti, Vitamin D and COVID-19 severity and related mortality: a prospective study in Italy, BMC Infect. Dis, doi:10.1186/s12879-021-06281-7
Carpagnano, Lecce, Quaranta, Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19, J. Endocrinol. Investig
Castillo, Costa, Barrios, Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study, J. Steroid Biochem. Mol. Biol, doi:10.1016/j.jsbmb.2020.105751
Chiodini, Gatti, Soranna, Vitamin D Status and SARS-CoV-2 Infection and COVID-19 Clinical Outcomes, Front. Public Health, doi:10.3389/fpubh.2021.736665
Coussens, The role of UV radiation and vitamin D in the seasonality and outcomes of infectious disease, Photochem. Photobiol. Sci
D'avolio, Avataneo, Manca, 25-Hydroxyvitamin D concentrations are lower in patients with positive PCR for SARS-CoV-2, Nutrients, doi:10.3390/nu12051359
Fabbri, Infante, Ricordi, Editorial-Vitamin D status: A key modulator of innate immunity and natural defense from acute viral respiratory infections, Eur. Rev. Med. Pharmacol. Sci
Fares, Factors influencing the seasonal patterns of infectious diseases, Int. J. Prev. Med
Ghasemian, Shamshirian, Heydari, The role of vitamin D in the age of COVID-19: A systematic review and meta-analysis, Int. J. Clin. Pract, doi:10.1111/ijcp.14675
Golpour, Bereswill, Heimesaat, Antimicrobial and Immune-Modulatory Effects of Vitamin D Provide Promising Antibiotics-Independent Approaches to Tackle Bacterial Infections-Lessons Learnt from a Literature Survey, Eur. J. Microbiol. Immunol
Gombart, Pierre, Maggini, A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection, Nutrients, doi:10.3390/nu12010236
Greiller, Martineau, Modulation of the immune response to respiratory viruses by vitamin D, Nutrients, doi:10.3390/nu7064240
Gruber-Bzura, Vitamin D and Influenza-Prevention or Therapy?, Int. J. Mol. Sci, doi:10.3390/ijms19082419
Hansdottir, Monick, Hinde, Respiratory epithelial cells convert inactive vitamin D to its active form: Potential effects on host defense, J Immunol Baltim Md, doi:10.4049/jimmunol.181.10.7090
Hewison, Vitamin D and immune function: An overview, Proc. Nutr. Soc, doi:10.1017/S0029665111001650
Higgins, Wischmeyer, Queensland, Relationship of vitamin D deficiency to clinical outcomes in critically ill patients, JPEN J Parenter Enter Nutr, doi:10.1177/0148607112444449
Hribar, Hristov, Gregorič, Socio-Demographic and Knowledge-Related Determinants of Vitamin D Supplementation in the Context of the COVID-19 Pandemic: Assessment of an Educational Intervention, Front. Nutr, doi:10.3389/fnut.2021.648450
Jolliffe, Camargo, Jr, Sluyter, Vitamin D supplementation to prevent acute respiratory infections: A systematic review and meta-analysis of aggregate data from randomised controlled trials, Lancet Diabetes Endocrinol
Jolliffe, Griffiths, Martineau, Vitamin D in the prevention of acute respiratory infection: Systematic review of clinical studies, J. Steroid Biochem. Mol. Biol
Jolliffe, Griffiths, Martineau, Vitamin D in the prevention of acute respiratory infection: Systematic review of clinical studies, J. Steroid Biochem. Mol. Biol, doi:10.1016/j.jsbmb.2012.11.017
Jordan, Siuka, Rotovnik, COVID-19 and Vitamin D-a Systematic Review, Zdr. Varst, doi:10.2478/sjph-2022-0017
Kaufman, Niles, Kroll, SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels, PLoS One
Kempker, West, Kempker, Vitamin D status and the risk for hospital-acquired infections in critically ill adults: A prospective cohort study, PLoS One, doi:10.1371/journal.pone.0122136
Laird, Vitamin D and Inflammation: Potential Implications for Severity of Covid-19, Ir. Med. J
Lang, Aspinall, Vitamin D Status and the Host Resistance to Infections: What It Is Currently (Not) Understood, Clin. Ther
Liu, Sun, Wang, Low vitamin D status is associated with coronavirus disease 2019 outcomes: a systematic review and meta-analysis, Int. J. Infect. Dis
Martineau, Vitamin D supplementation to prevent acute respiratory infections: individual participant data metaanalysis, Health Technol. Assess, doi:10.3310/hta23020
Mcnally, Menon, Chakraborty, The association of vitamin D status with pediatric critical illness, Pediatrics, doi:10.1542/peds.2011-3059
Meltzer, Best, Zhang, Association of Vitamin D Status and Other Clinical Characteristics With COVID-19 Test Results, JAMA Netw. Open, doi:10.1001/jamanetworkopen.2020.19722
Merzon, Tworowski, Gorohovski, Low plasma 25(OH) vitamin D level is associated with increased risk of COVID-19 infection: an Israeli population-based study
Monlezun, Bittner, Christopher, Vitamin D status and acute respiratory infection: cross sectional results from the United States National\Health and Nutrition Examination Survey, 2001-2006, Nutrients, doi:10.3390/nu7031933
Moromizato, Litonjua, Braun, Association of low serum 25-hydroxyvitamin D levels and sepsis in the critically ill, Crit. Care Med
Murai, Fernandes, Sales, Effect of a single high dose of vitamin D3 on hospital length of stay in patients with moderate to severe COVID-19: A randomized clinical trial, JAMA
Nair, Lee, Reynolds, Significant perturbation of vitamin Dparathyroid-calcium axis and adverse clinical outcomes in critically ill patients, Intensive Care Med, doi:10.1007/s00134-012-2713-y
Niet, Trémège, Coffiner, Positive Effects of Vitamin D Supplementation in Patients Hospitalized for COVID-19: A Randomized, Double-Blind, Placebo-Controlled Trial, Nutrients, doi:10.3390/nu14153048
Olliver, Spelmink, Hiew, Immunomodulatory effects of vitamin D on innate and adaptive immune responses to Streptococcus pneumoniae, J. Infect. Dis, doi:10.1093/infdis/jit355
Petrelli, Luciani, Perego, Therapeutic and prognostic role of vitamin D for COVID-19 infection: A systematic review and meta-analysis of 43 observational studies, J. Steroid Biochem. Mol. Biol, doi:10.1016/j.jsbmb.2021.105883
Pfeifer, Siuka, Pravst, Recommendations for replacing cholecalciferol (vitamin D3) during periods respiratory infections and to replace cholecalciferol in individuals with COVID-19
Quraishi, Litonjua, Moromizato, Association between prehospital vitamin D status and hospital-acquired Clostridium difficile infections, JPEN J. Parenter. Enter. Nutr, doi:10.1177/0148607113511991
Radujkovic, Hippchen, Tiwari-Heckler, Vitamin D Deficiency and Outcome of COVID-19 Patients, Nutrients, doi:10.3390/nu12092757
Rondanelli, Miccono, Lamburghini, Self-Care for Common Colds: The Pivotal Role of Vitamin D, Vitamin C, Zinc, and Echinacea in Three Main Immune Interactive Clusters (Physical Barriers, Innate and Adaptive Immunity) Involved during an Episode of Common Colds-Practical Advice on Dosages and on the Time to Take These Nutrients/Botanicals in order to Prevent or Treat Common Colds. Evid.-Based Complement, Altern Med ECAM
Sabetta, Depetrillo, Cipriani, Serum 25-Hydroxyvitamin D and the Incidence of Acute Viral Respiratory Tract Infections in Healthy Adults, PLoS One, doi:10.1371/journal.pone.0011088
Siuka, Fabjan, Osredkar, The COVID-19 Pandemic, Seasons and the Vitamin D Laboratory Strategy, International Journal of Sciences: Basic and Applied Research (IJSBAR)
Siuka, Saletinger, Uršič, The effect of Vitamin D levels on the course of COVID, doi:10.5281/zenodo.7679129
Thickett, Moromizato, Litonjua, Association between prehospital vitamin D status and incident acute respiratory failure in critically ill patients: A retrospective cohort study, BMJ Open Respir. Res, doi:10.1136/bmjresp-2014-000074
Vanherwegen, Gysemans, Mathieu, Regulation of immune function by vitamin D and its use in diseases of immunity, Endocrinol. Metab. Clin. N. Am, doi:10.1016/j.ecl.2017.07.010
Wei, Christakos, Mechanisms Underlying the Regulation of Innate and Adaptive Immunity by Vitamin D, Nutrients, doi:10.3390/nu7105392
Zheng, Peng, Xu, Risk factors of critical & mortal COVID-19 cases: a systematic literature review and metaanalysis, J. Infect, doi:10.1016/j.jinf.2020.04.021
DOI record:
{
"DOI": "10.12688/f1000research.131730.1",
"ISSN": [
"2046-1402"
],
"URL": "http://dx.doi.org/10.12688/f1000research.131730.1",
"abstract": "<ns4:p>Background: The aim of the current study was to assess the patients with COVID-19 and the impact of vitamin D supplementation on the course of COVID-19. </ns4:p><ns4:p> Methods: This prospective cohort study included patients hospitalized due to COVID-19 between December 2020 and December 2021. Patients' demographic, clinical, and laboratory parameters were analysed. </ns4:p><ns4:p> Results: 301 participants were enrolled in the study. 46 (15,3%) had moderate, and 162 (53,8%) had severe COVID-19. 14 (4,7%) patients died, and 30 (10,0%) were admitted to the ICU due to disease worsening. The majority needed oxygen therapy (n=224; 74,4%). Average vitamin 25(OH)D3 levels were below optimal at the admittance, and vitamin D deficiency was detected in 205 individuals. More male patients were suffering from vitamin D deficiency. Patients with the more severe disease showed lower levels of vitamin 25(OH)D3 in their blood. The most severe group of patients had more symptoms that lasted significantly longer with progressing disease severity. This group of patients also suffered from more deaths, ICU admissions, and treatments with dexamethasone, remdesivir, and oxygen. </ns4:p><ns4:p> Conclusion: Patients with the severe course of COVID-19 were shown to have increased inflammatory parameters, increased mortality, and higher incidence of vitamin D deficiency. The results suggest that the vitamin D deficiency might represent a significant risk factor for a severe course of COVID-19.</ns4:p>",
"assertion": [
{
"URL": "https://f1000research.com/articles/12-254/v1#article-reports",
"group": {
"label": "Current Referee Status",
"name": "current-referee-status"
},
"label": "Referee status",
"name": "referee-status",
"order": 0,
"value": "Awaiting Peer Review"
},
{
"label": "Grant Information",
"name": "grant-information",
"order": 0,
"value": "The author(s) declared that no grants were involved in supporting this work"
},
{
"label": "Copyright",
"name": "copyright-info",
"order": 0,
"value": "This is an open access article distributed under the terms of the Creative Commons Attribution Licence, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited."
}
],
"author": [
{
"affiliation": [],
"family": "Siuka",
"given": "Darko",
"sequence": "first"
},
{
"affiliation": [],
"family": "Saletinger",
"given": "Rajko",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Uršič",
"given": "Jure",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jevnikar",
"given": "Kristina",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Janša",
"given": "Rado",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-9653-9830",
"affiliation": [],
"authenticated-orcid": false,
"family": "Štubljar",
"given": "David",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-1839-2415",
"affiliation": [],
"authenticated-orcid": false,
"family": "Osredkar",
"given": "Joško",
"sequence": "additional"
}
],
"container-title": "F1000Research",
"container-title-short": "F1000Res",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"f1000research.com"
]
},
"created": {
"date-parts": [
[
2023,
3,
9
]
],
"date-time": "2023-03-09T14:26:41Z",
"timestamp": 1678372001000
},
"deposited": {
"date-parts": [
[
2023,
3,
9
]
],
"date-time": "2023-03-09T14:26:49Z",
"timestamp": 1678372009000
},
"indexed": {
"date-parts": [
[
2023,
3,
10
]
],
"date-time": "2023-03-10T05:46:39Z",
"timestamp": 1678427199389
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2023,
3,
9
]
]
},
"language": "en",
"license": [
{
"URL": "http://creativecommons.org/licenses/by/4.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
3,
9
]
],
"date-time": "2023-03-09T00:00:00Z",
"timestamp": 1678320000000
}
}
],
"link": [
{
"URL": "https://f1000research.com/articles/12-254/v1/xml",
"content-type": "application/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://f1000research.com/articles/12-254/v1/pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://f1000research.com/articles/12-254/v1/iparadigms",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "2560",
"original-title": [],
"page": "254",
"prefix": "10.12688",
"published": {
"date-parts": [
[
2023,
3,
9
]
]
},
"published-online": {
"date-parts": [
[
2023,
3,
9
]
]
},
"publisher": "F1000 Research Ltd",
"reference": [
{
"article-title": "The COVID-19 Pandemic, Seasons and the Vitamin D Laboratory Strategy.",
"author": "D Siuka",
"first-page": "182-189",
"journal-title": "International Journal of Sciences: Basic and Applied Research (IJSBAR).",
"key": "ref1",
"volume": "56",
"year": "2021"
},
{
"article-title": "Factors influencing the seasonal patterns of infectious diseases.",
"author": "A Fares",
"first-page": "128-132",
"journal-title": "Int. J. Prev. Med.",
"key": "ref2",
"volume": "4",
"year": "2013"
},
{
"DOI": "10.2478/sjph-2022-0017",
"article-title": "COVID-19 and Vitamin D- a Systematic Review.",
"author": "T Jordan",
"doi-asserted-by": "publisher",
"first-page": "124-132",
"journal-title": "Zdr. Varst.",
"key": "ref3",
"volume": "61",
"year": "2022"
},
{
"DOI": "10.1016/j.jsbmb.2012.11.017",
"article-title": "Vitamin D in the prevention of acute respiratory infection: Systematic review of clinical studies.",
"author": "D Jolliffe",
"doi-asserted-by": "publisher",
"first-page": "321-329",
"journal-title": "J. Steroid Biochem. Mol. Biol.",
"key": "ref4",
"volume": "136",
"year": "2013"
},
{
"DOI": "10.3390/nu14153048",
"article-title": "Positive Effects of Vitamin D Supplementation in Patients Hospitalized for COVID-19: A Randomized, Double-Blind, Placebo-Controlled Trial.",
"author": "S De Niet",
"doi-asserted-by": "publisher",
"first-page": "3048",
"journal-title": "Nutrients.",
"key": "ref5",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1016/j.ecl.2017.07.010",
"article-title": "Regulation of immune function by vitamin D and its use in diseases of immunity.",
"author": "A Vanherwegen",
"doi-asserted-by": "publisher",
"first-page": "1061-1094",
"journal-title": "Endocrinol. Metab. Clin. N. Am.",
"key": "ref6",
"volume": "46",
"year": "2017"
},
{
"DOI": "10.1016/j.jcv.2010.12.006",
"article-title": "Vitamin D and the anti-viral state.",
"author": "J Beard",
"doi-asserted-by": "publisher",
"first-page": "194-200",
"journal-title": "J. Clin. Virol.",
"key": "ref7",
"volume": "50",
"year": "2011"
},
{
"DOI": "10.3390/nu7064240",
"article-title": "Modulation of the immune response to respiratory viruses by vitamin D.",
"author": "C Greiller",
"doi-asserted-by": "publisher",
"first-page": "4240-4270",
"journal-title": "Nutrients.",
"key": "ref8",
"volume": "7",
"year": "2015"
},
{
"article-title": "The role of UV radiation and vitamin D in the seasonality and outcomes of infectious disease.",
"author": "A Coussens",
"first-page": "314-338",
"journal-title": "Photochem. Photobiol. Sci.",
"key": "ref9",
"volume": "16",
"year": "2017"
},
{
"DOI": "10.1016/j.clinthera.2017.04.004",
"article-title": "Vitamin D Status and the Host Resistance to Infections: What It Is Currently (Not) Understood.",
"author": "P Lang",
"doi-asserted-by": "publisher",
"first-page": "930-945",
"journal-title": "Clin. Ther.",
"key": "ref10",
"volume": "39",
"year": "2017"
},
{
"DOI": "10.3390/ijms19082419",
"article-title": "Vitamin D and Influenza-Prevention or Therapy?",
"author": "B Gruber-Bzura",
"doi-asserted-by": "publisher",
"first-page": "2419",
"journal-title": "Int. J. Mol. Sci.",
"key": "ref11",
"volume": "19",
"year": "2018"
},
{
"article-title": "Self-Care for Common Colds: The Pivotal Role of Vitamin D, Vitamin C, Zinc, and Echinacea in Three Main Immune Interactive Clusters (Physical Barriers, Innate and Adaptive Immunity) Involved during an Episode of Common Colds-Practical Advice on Dosages and on the Time to Take These Nutrients/Botanicals in order to Prevent or Treat Common Colds.",
"author": "M Rondanelli",
"first-page": "5813095",
"journal-title": "Evid.-Based Complement. Altern Med ECAM.",
"key": "ref12",
"volume": "2018",
"year": "2018"
},
{
"DOI": "10.3390/nu12010236",
"article-title": "A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection.",
"author": "A Gombart",
"doi-asserted-by": "publisher",
"first-page": "236",
"journal-title": "Nutrients.",
"key": "ref13",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(21)00051-6",
"article-title": "Vitamin D supplementation to prevent acute respiratory infections: A systematic review and meta-analysis of aggregate data from randomised controlled trials.",
"author": "D Jolliffe",
"doi-asserted-by": "publisher",
"first-page": "276-292",
"journal-title": "Lancet Diabetes Endocrinol.",
"key": "ref14",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1017/S0029665111001650",
"article-title": "Vitamin D and immune function: An overview.",
"author": "M Hewison",
"doi-asserted-by": "publisher",
"first-page": "50-61",
"journal-title": "Proc. Nutr. Soc.",
"key": "ref15",
"volume": "71",
"year": "2012"
},
{
"DOI": "10.3390/nu7105392",
"article-title": "Mechanisms Underlying the Regulation of Innate and Adaptive Immunity by Vitamin D.",
"author": "R Wei",
"doi-asserted-by": "publisher",
"first-page": "8251-8260",
"journal-title": "Nutrients.",
"key": "ref16",
"volume": "7",
"year": "2015"
},
{
"DOI": "10.26355/eurrev_202004_20876",
"article-title": "Editorial—Vitamin D status: A key modulator of innate immunity and natural defense from acute viral respiratory infections.",
"author": "A Fabbri",
"doi-asserted-by": "publisher",
"first-page": "4048-4052",
"journal-title": "Eur. Rev. Med. Pharmacol. Sci.",
"key": "ref17",
"volume": "24",
"year": "2020"
},
{
"DOI": "10.1016/j.jsbmb.2012.11.017",
"article-title": "Vitamin D in the prevention of acute respiratory infection: Systematic review of clinical studies.",
"author": "D Jolliffe",
"doi-asserted-by": "publisher",
"first-page": "321-329",
"journal-title": "J. Steroid Biochem. Mol. Biol.",
"key": "ref18",
"volume": "136",
"year": "2013"
},
{
"DOI": "10.4049/jimmunol.181.10.7090",
"article-title": "Respiratory epithelial cells convert inactive vitamin D to its active form: Potential effects on host defense.",
"author": "S Hansdottir",
"doi-asserted-by": "publisher",
"first-page": "7090-7099",
"journal-title": "J Immunol Baltim Md.",
"key": "ref19",
"volume": "181",
"year": "1950"
},
{
"DOI": "10.1093/infdis/jit355",
"article-title": "Immunomodulatory effects of vitamin D on innate and adaptive immune responses to Streptococcus pneumoniae.",
"author": "M Olliver",
"doi-asserted-by": "publisher",
"first-page": "1474-1481",
"journal-title": "J. Infect. Dis.",
"key": "ref20",
"volume": "208",
"year": "2013"
},
{
"DOI": "10.1556/1886.2019.00014",
"article-title": "Antimicrobial and Immune-Modulatory Effects of Vitamin D Provide Promising Antibiotics-Independent Approaches to Tackle Bacterial Infections—Lessons Learnt from a Literature Survey.",
"author": "A Golpour",
"doi-asserted-by": "publisher",
"first-page": "80-87",
"journal-title": "Eur. J. Microbiol. Immunol.",
"key": "ref21",
"volume": "9",
"year": "2019"
},
{
"DOI": "10.1097/CCM.0b013e31829eb7af",
"article-title": "Association of low serum 25-hydroxyvitamin D levels and sepsis in the critically ill.",
"author": "T Moromizato",
"doi-asserted-by": "publisher",
"first-page": "97-107",
"journal-title": "Crit. Care Med.",
"key": "ref22",
"volume": "42",
"year": "2014"
},
{
"DOI": "10.1136/bmjresp-2014-000074",
"article-title": "Association between prehospital vitamin D status and incident acute respiratory failure in critically ill patients: A retrospective cohort study.",
"author": "D Thickett",
"doi-asserted-by": "publisher",
"first-page": "e000074",
"journal-title": "BMJ Open Respir. Res.",
"key": "ref23",
"volume": "2",
"year": "2015"
},
{
"DOI": "10.1177/0148607112444449",
"article-title": "Relationship of vitamin D deficiency to clinical outcomes in critically ill patients.",
"author": "D Higgins",
"doi-asserted-by": "publisher",
"first-page": "713-720",
"journal-title": "JPEN J Parenter Enter Nutr.",
"key": "ref24",
"volume": "36",
"year": "2012"
},
{
"DOI": "10.1007/s00134-012-2713-y",
"article-title": "Significant perturbation of vitamin Dparathyroid-calcium axis and adverse clinical outcomes in critically ill patients.",
"author": "P Nair",
"doi-asserted-by": "publisher",
"first-page": "267-274",
"journal-title": "Intensive Care Med.",
"key": "ref25",
"volume": "39",
"year": "2013"
},
{
"DOI": "10.1097/CCM.0b013e31822d74f3",
"article-title": "Low serum 25-hydroxyvitamin D at critical care initiation is associated with increased mortality.",
"author": "A Braun",
"doi-asserted-by": "publisher",
"first-page": "63-72",
"journal-title": "Crit. Care Med.",
"key": "ref26",
"volume": "40",
"year": "2012"
},
{
"DOI": "10.1177/0148607113511991",
"article-title": "Association between prehospital vitamin D status and hospital-acquired Clostridium difficile infections.",
"author": "S Quraishi",
"doi-asserted-by": "publisher",
"first-page": "47-55",
"journal-title": "JPEN J. Parenter. Enter. Nutr.",
"key": "ref27",
"volume": "39",
"year": "2015"
},
{
"DOI": "10.1186/2110-5820-4-5",
"article-title": "Vitamin D deficiency and risk of acute lung injury in severe sepsis and severe trauma: A case-control study.",
"author": "N Barnett",
"doi-asserted-by": "publisher",
"first-page": "5",
"journal-title": "Ann. Intensive Care.",
"key": "ref28",
"volume": "4",
"year": "2014"
},
{
"DOI": "10.1001/jama.2014.13204",
"article-title": "Effect of high-dose vitamin D3 on hospital length of stay in critically ill patients with vitamin D deficiency: The VITdAL-ICU randomized clinical trial.",
"author": "K Amrein",
"doi-asserted-by": "publisher",
"first-page": "1520-1530",
"journal-title": "JAMA.",
"key": "ref29",
"volume": "312",
"year": "2014"
},
{
"DOI": "10.1542/peds.2011-3059",
"article-title": "The association of vitamin D status with pediatric critical illness.",
"author": "J McNally",
"doi-asserted-by": "publisher",
"first-page": "429-436",
"journal-title": "Pediatrics.",
"key": "ref30",
"volume": "130",
"year": "2012"
},
{
"DOI": "10.1371/journal.pone.0122136",
"article-title": "Vitamin D status and the risk for hospital-acquired infections in critically ill adults: A prospective cohort study.",
"author": "J Kempker",
"doi-asserted-by": "publisher",
"first-page": "e0122136",
"journal-title": "PLoS One.",
"key": "ref31",
"volume": "10",
"year": "2015"
},
{
"DOI": "10.1371/journal.pone.0239252",
"article-title": "SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels.",
"author": "H Kaufman",
"doi-asserted-by": "publisher",
"first-page": "e0239252",
"journal-title": "PLoS One.",
"key": "ref32",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1016/j.jiph.2020.06.021",
"article-title": "Role of vitamin D in preventing COVID-19 infection, pro- gression and severity.",
"author": "N Ali",
"doi-asserted-by": "publisher",
"first-page": "1373-1380",
"journal-title": "J. Infect. Public Health.",
"key": "ref33",
"volume": "13",
"year": "2020"
},
{
"DOI": "10.1007/s40520-021-01831-0",
"article-title": "Severe vitamin D de- ficiency is not related to SARS-CoV-2 infection but may increase mortality risk in hospitalized adults: a retrospective case-control study in an Arab Gulf country.",
"author": "A Alguwaihes",
"doi-asserted-by": "publisher",
"first-page": "1415-1422",
"journal-title": "Aging Clin. Exp. Res.",
"key": "ref34",
"volume": "33",
"year": "2021"
},
{
"DOI": "10.1186/s12967-021-02838-x",
"article-title": "Vitamin D status of Arab Gulf residents screened for SARS-CoV-2 and its association with COVID-19 infection: a multi-centre case-control study.",
"author": "N Al-Daghri",
"doi-asserted-by": "publisher",
"first-page": "166",
"journal-title": "J. Transl. Med.",
"key": "ref35",
"volume": "19",
"year": "2021"
},
{
"DOI": "10.1186/s12879-021-06281-7",
"article-title": "Vitamin D and COVID-19 severity and related mortality: a prospective study in Italy.",
"author": "I Campi",
"doi-asserted-by": "publisher",
"first-page": "566",
"journal-title": "BMC Infect. Dis.",
"key": "ref36",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.3389/fpubh.2021.736665",
"article-title": "Vitamin D Status and SARS- CoV-2 Infection and COVID-19 Clinical Outcomes.",
"author": "I Chiodini",
"doi-asserted-by": "publisher",
"first-page": "736665",
"journal-title": "Front. Public Health.",
"key": "ref37",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1016/j.jsbmb.2021.105883",
"article-title": "Therapeutic and prognostic role of vitamin D for COVID-19 infection: A systematic review and meta-analysis of 43 observational studies.",
"author": "F Petrelli",
"doi-asserted-by": "publisher",
"first-page": "105883",
"journal-title": "J. Steroid Biochem. Mol. Biol.",
"key": "ref38",
"volume": "211",
"year": "2021"
},
{
"DOI": "10.1016/j.ijid.2020.12.077",
"article-title": "Low vitamin D status is associated with coronavirus disease 2019 outcomes: a systematic review and meta-analysis.",
"author": "N Liu",
"doi-asserted-by": "publisher",
"first-page": "58-64",
"journal-title": "Int. J. Infect. Dis.",
"key": "ref39",
"volume": "104",
"year": "2021"
},
{
"DOI": "10.1111/ijcp.14675",
"article-title": "The role of vitamin D in the age of COVID-19: A systematic review and meta-analysis.",
"author": "R Ghasemian",
"doi-asserted-by": "publisher",
"first-page": "e14675",
"journal-title": "Int. J. Clin. Pract.",
"key": "ref40",
"volume": "75",
"year": "2021"
},
{
"article-title": "Recommendations for replacing cholecalciferol (vitamin D3) during periods respiratory infections and to replace cholecalciferol in individuals with COVID-19.",
"author": "M Pfeifer",
"key": "ref41"
},
{
"DOI": "10.1016/j.jinf.2020.04.021",
"article-title": "Risk factors of critical & mortal COVID-19 cases: a systematic literature review and metaanalysis.",
"author": "Z Zheng",
"doi-asserted-by": "publisher",
"first-page": "e16-e25",
"journal-title": "J. Infect.",
"key": "ref42",
"volume": "81",
"year": "2020"
},
{
"DOI": "10.3390/nu12061838",
"article-title": "Nutrihealth Study: Seasonal Variation in Vitamin D Status Among the Slovenian Adult and Elderly Population.",
"author": "M Hribar",
"doi-asserted-by": "publisher",
"first-page": "1838",
"journal-title": "Nutrients.",
"key": "ref43",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3389/fnut.2021.648450",
"article-title": "Socio-Demographic and Knowledge-Related Determinants of Vitamin D Supplementation in the Context of the COVID-19 Pandemic: Assessment of an Educational Intervention.",
"author": "K Žmitek",
"doi-asserted-by": "publisher",
"first-page": "648450",
"journal-title": "Front. Nutr.",
"key": "ref44",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.2903/j.efsa.2016.4547",
"article-title": "Scientific opinion on dietary reference values for vitamin D.",
"doi-asserted-by": "publisher",
"first-page": "4547",
"journal-title": "EFSA J.",
"key": "ref46",
"volume": "14",
"year": "2016"
},
{
"DOI": "10.1159/000337547",
"article-title": "German Nutrition Society, New Reference Values for Vitamin D (D-A-CH).",
"doi-asserted-by": "publisher",
"first-page": "241-246",
"journal-title": "Ann. Nutr. Metab.",
"key": "ref47",
"volume": "60",
"year": "2012"
},
{
"DOI": "10.3310/hta23020",
"article-title": "Vitamin D supplementation to prevent acute respiratory infections: individual participant data meta-analysis.",
"author": "A Martineau",
"doi-asserted-by": "publisher",
"first-page": "1-44",
"journal-title": "Health Technol. Assess.",
"key": "ref48",
"volume": "23",
"year": "2019"
},
{
"DOI": "10.1371/journal.pone.0011088",
"article-title": "Serum 25-Hydroxyvitamin D and the Incidence of Acute Viral Respiratory Tract Infections in Healthy Adults.",
"author": "J Sabetta",
"doi-asserted-by": "publisher",
"first-page": "e11088",
"journal-title": "PLoS One.",
"key": "ref49",
"volume": "5",
"year": "2010"
},
{
"DOI": "10.3390/nu7031933",
"article-title": "Vitamin D status and acute respiratory infection: cross sectional results from the United States National\\Health and Nutrition Examination Survey, 2001-2006.",
"author": "D Monlezun",
"doi-asserted-by": "publisher",
"first-page": "1933-1944",
"journal-title": "Nutrients.",
"key": "ref50",
"volume": "7",
"year": "2015"
},
{
"article-title": "Vitamin D and Inflammation: Potential Implications for Severity of Covid-19.",
"author": "E Laird",
"first-page": "81",
"journal-title": "Ir. Med. J.",
"key": "ref51",
"volume": "113",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"article-title": "Association of Vitamin D Status and Other Clinical Characteristics With COVID-19 Test Results.",
"author": "D Meltzer",
"doi-asserted-by": "publisher",
"first-page": "e2019722",
"journal-title": "JAMA Netw. Open.",
"key": "ref52",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.3390/nu12051359",
"article-title": "25-Hydroxyvitamin D concentrations are lower in patients with positive PCR for SARS-CoV-2.",
"author": "A D’Avolio",
"doi-asserted-by": "publisher",
"first-page": "1359",
"journal-title": "Nutrients.",
"key": "ref53",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1111/febs.15495",
"article-title": "Low plasma 25(OH) vitamin D level is associated with increased risk of COVID-19 infection: an Israeli population-based study.",
"author": "E Merzon",
"doi-asserted-by": "crossref",
"key": "ref54"
},
{
"article-title": "Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19.",
"author": "G Carpagnano",
"journal-title": "J. Endocrinol. Investig.",
"key": "ref55",
"year": "2020"
},
{
"DOI": "10.3390/nu12092757",
"article-title": "Vitamin D Deficiency and Outcome of COVID-19 Patients.",
"author": "A Radujkovic",
"doi-asserted-by": "publisher",
"first-page": "2757",
"journal-title": "Nutrients.",
"key": "ref56",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/j.jsbmb.2020.105751",
"article-title": "Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study.",
"author": "M Entrenas Castillo",
"doi-asserted-by": "publisher",
"first-page": "105751",
"journal-title": "J. Steroid Biochem. Mol. Biol.",
"key": "ref57",
"volume": "203",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.26848",
"article-title": "Effect of a single high dose of vitamin D3 on hospital length of stay in patients with moderate to severe COVID-19: A randomized clinical trial.",
"author": "I Murai",
"doi-asserted-by": "publisher",
"first-page": "1053-1060",
"journal-title": "JAMA.",
"key": "ref58",
"volume": "325",
"year": "2021"
},
{
"DOI": "10.5281/zenodo.7679129",
"author": "D Siuka",
"doi-asserted-by": "publisher",
"journal-title": "Zenodo.",
"key": "ref59",
"year": "2023"
}
],
"reference-count": 58,
"references-count": 58,
"relation": {},
"resource": {
"primary": {
"URL": "https://f1000research.com/articles/12-254/v1"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Pharmacology, Toxicology and Pharmaceutics",
"General Immunology and Microbiology",
"General Biochemistry, Genetics and Molecular Biology",
"General Medicine"
],
"subtitle": [],
"title": "The effect of Vitamin D levels on the course of COVID-19 in hospitalized patients – a 1-year prospective cohort study",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.12688/f1000research.crossmark-policy",
"volume": "12"
}
