Survival and Mortality in Hospitalized Children with COVID-19: A Referral Center Experience in Yazd, Iran
et al., Canadian Journal of Infectious Diseases and Medical Microbiology, doi:10.1155/2023/5205188, Jul 2023
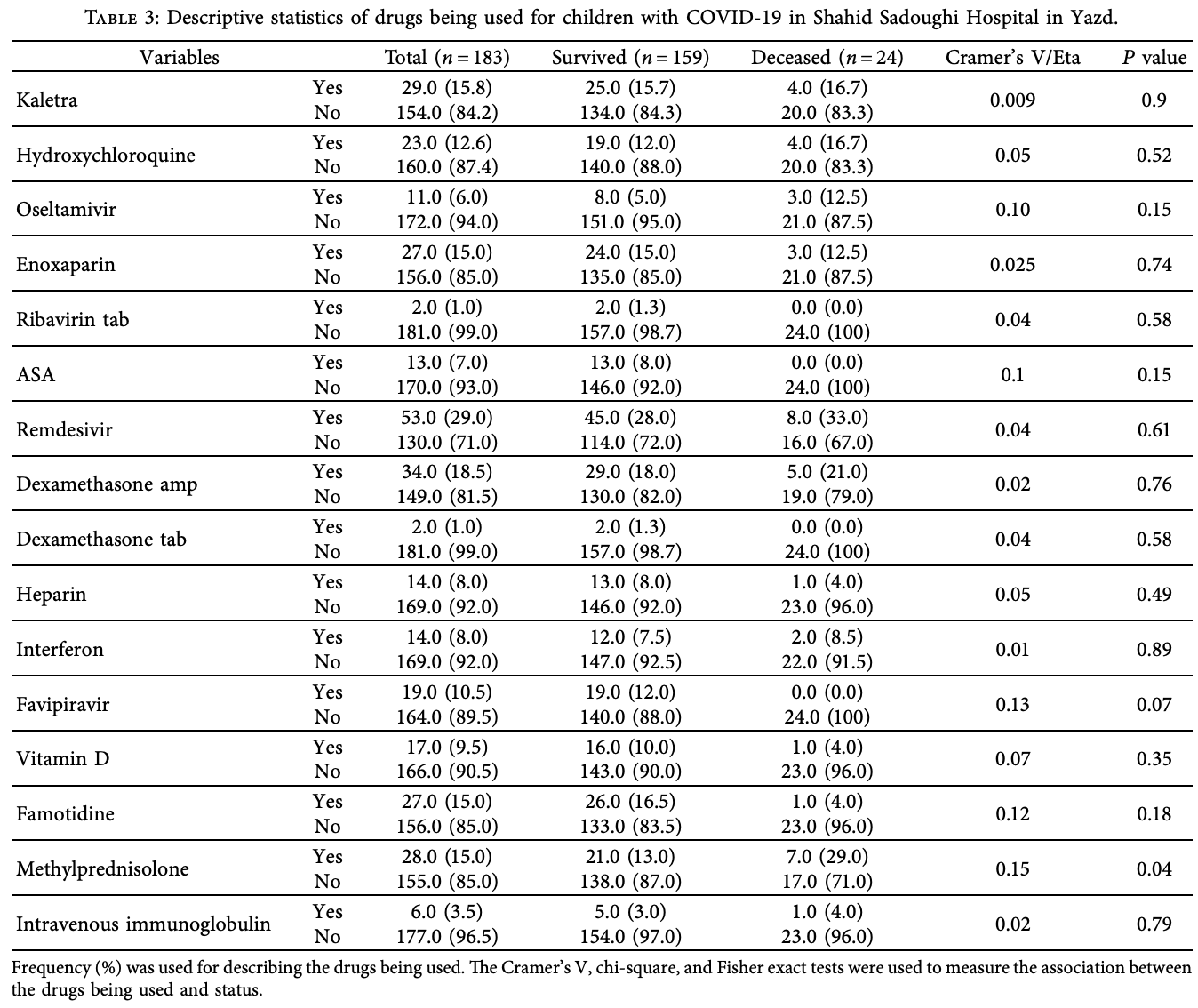
Retrospective 183 hospitalized pediatric COVID-19 patients in Iran, showing no significant difference in mortality with remdesivir in unadjusted results.
Gérard, Zhou, Wu, Kamo, Choi, Kim show increased risk of acute kidney injury, Leo, Briciu, Muntean, Petrov, Arch show increased risk of liver injury, Negru, Cheng, Mohammed, Kwok, Zhu show increased risk of cardiac disorders, and Kwok, Merches, Akinci, Tang, Bagheri show increased risk of mitochondrial toxicity with remdesivir.
This study is excluded in the after exclusion results of meta-analysis:
unadjusted results with no group details.
|
risk of death, 22.6% higher, RR 1.23, p = 0.63, treatment 8 of 53 (15.1%), control 16 of 130 (12.3%).
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
1.
Gérard et al., Remdesivir and Acute Renal Failure: A Potential Safety Signal From Disproportionality Analysis of the WHO Safety Database, Clinical Pharmacology & Therapeutics, doi:10.1002/cpt.2145.
2.
Zhou et al., Acute Kidney Injury and Drugs Prescribed for COVID-19 in Diabetes Patients: A Real-World Disproportionality Analysis, Frontiers in Pharmacology, doi:10.3389/fphar.2022.833679.
3.
Wu et al., Acute Kidney Injury Associated With Remdesivir: A Comprehensive Pharmacovigilance Analysis of COVID-19 Reports in FAERS, Frontiers in Pharmacology, doi:10.3389/fphar.2022.692828.
4.
Kamo et al., Association of Antiviral Drugs for the Treatment of COVID-19 With Acute Renal Failure, In Vivo, doi:10.21873/invivo.13637.
5.
Choi et al., Comparative effectiveness of combination therapy with nirmatrelvir–ritonavir and remdesivir versus monotherapy with remdesivir or nirmatrelvir–ritonavir in patients hospitalised with COVID-19: a target trial emulation study, The Lancet Infectious Diseases, doi:10.1016/S1473-3099(24)00353-0.
6.
Kim et al., Investigating the Safety Profile of Fast‐Track COVID‐19 Drugs Using the FDA Adverse Event Reporting System Database: A Comparative Observational Study, Pharmacoepidemiology and Drug Safety, doi:10.1002/pds.70043.
7.
Leo et al., Hepatocellular liver injury in hospitalized patients affected by COVID-19: Presence of different risk factors at different time points, Digestive and Liver Disease, doi:10.1016/j.dld.2021.12.014.
8.
Briciu et al., Evolving Clinical Manifestations and Outcomes in COVID-19 Patients: A Comparative Analysis of SARS-CoV-2 Variant Waves in a Romanian Hospital Setting, Pathogens, doi:10.3390/pathogens12121453.
9.
Muntean et al., Effects of COVID-19 on the Liver and Mortality in Patients with SARS-CoV-2 Pneumonia Caused by Delta and Non-Delta Variants: An Analysis in a Single Centre, Pharmaceuticals, doi:10.3390/ph17010003.
10.
Petrov et al., The Effect of Potentially Hepatotoxic Medicinal Products on Alanine Transaminase Levels in COVID-19 Patients: A Case–Control Study, Safety and Risk of Pharmacotherapy, doi:10.30895/2312-7821-2025-458.
11.
Arch et al., Evaluation of the effectiveness of remdesivir in treating severe COVID-19 using data from the ISARIC WHO Clinical Characterisation Protocol UK: a prospective, national cohort study, medRxiv, doi:10.1101/2021.06.18.21259072.
12.
Negru et al., Comparative Pharmacovigilance Analysis of Approved and Repurposed Antivirals for COVID-19: Insights from EudraVigilance Data, Biomedicines, doi:10.3390/biomedicines13061387.
13.
Cheng et al., Cardiovascular Safety of COVID-19 Treatments: A Disproportionality Analysis of Adverse Event Reports from the WHO VigiBase, Infectious Diseases and Therapy, doi:10.1007/s40121-025-01225-z.
14.
Mohammed et al., Bradycardia associated with remdesivir treatment in coronavirus disease 2019 patients: A propensity score-matched analysis, Medicine, doi:10.1097/MD.0000000000044501.
15.
Kwok et al., Remdesivir induces persistent mitochondrial and structural damage in human induced pluripotent stem cell-derived cardiomyocytes, Cardiovascular Research, doi:10.1093/cvr/cvab311.
16.
Zhu et al., Cardiovascular Risks of COVID-19 Therapeutics: Integrated Analysis of FAERS, Electronic Health Records, and Transcriptomics, Pharmaceuticals, doi:10.3390/ph19040574.
17.
Merches et al., The potential of remdesivir to affect function, metabolism and proliferation of cardiac and kidney cells in vitro, Archives of Toxicology, doi:10.1007/s00204-022-03306-1.
18.
Akinci et al., Elucidation of remdesivir cytotoxicity pathways through genome-wide CRISPR-Cas9 screening and transcriptomics, bioRxiv, doi:10.1101/2020.08.27.270819.
Shamsi et al., 17 Jul 2023, retrospective, Iran, peer-reviewed, 4 authors, study period 1 March, 2020 - 1 August, 2021.
Contact: farimahshamssi@gmail.com.
Survival and Mortality in Hospitalized Children with COVID-19: A Referral Center Experience in Yazd, Iran
Canadian Journal of Infectious Diseases and Medical Microbiology, doi:10.1155/2023/5205188
Introduction. COVID-19 prognostic risk factors, therapeutic protocols, and clinical outcomes in pediatric cases are still under investigation. Materials and Methods. Tis historical cohort study evaluated the survival time of hospitalized children (1 month-18 years old) with COVID-19 admitted from March 2020 to August 2021 to an educational hospital in Yazd, Iran. Te follow-up of patients was performed at least one month after discharge. Results. From 183 hospitalized cases, 24 children were deceased. Te median age of patients was 5.41, and 54.2% were male. Te survival rate after one-month follow-up was 0.88, and the most signifcant predictors associated with survival time were the male sex, positive history of hospitalization, lymphopenia, hypoxia, and length of stay more than two weeks using Bayesian Cox regression analysis. Conclusion. Accurate estimation of the impact of predictors on poor outcomes may help healthcare providers use therapeutic protocols based on risk factors and healthcare requirements of each patient to improve their survival.
Conflicts of Interest Te authors declare that they have no conficts of interest.
References
Armin, Fahimzad, Tabatabaei, COVID-19 mortality in children: a referral center experience from Iran (mofd children's hospital, tehran, Iran), Te Canadian Journal of Infectious Diseases and Medical Microbiology
Baumgart, Danese, Peyrin-Biroulet, Diarrhea during COVID-19 infection: pathogenesis, epidemiology, prevention, and management, Clinical Gastroenterology and Hepatology
Bialek, Coronavirus disease
Buonsenso, Di Giuda, Sigfrid, Evidence of lung perfusion defects and ongoing infammation in an adolescent with post-acute sequelae of SARS-CoV-2 infection, Te Lancet Child & Adolescent Health
Buonsenso, Munblit, Rose, Preliminary evidence on long COVID in children, Acta Paediatrica
Burke, Killerby, Newton, Symptom profles of a convenience sample of patients with COVID-19-United States, MMWR. Morbidity and Mortality Weekly Report
Chang, Wu, Chang, Clinical characteristics and diagnostic challenges of pediatric COVID-19: a systematic review and meta-analysis, Journal of the Formosan Medical Association
Dong, Mo, Hu, Epidemiology of COVID-19 among children in China, Pediatrics
Gallo Marin, Aghagoli, Lavine, Predictors of COVID-19 severity: a literature review, Reviews in Medical Virology
Garg, Kim, Whitaker, Hospitalization rates and characteristics of patients hospitalized with laboratory-10 Canadian Journal of Infectious Diseases and Medical Microbiology confrmed coronavirus disease
Götzinger, Santiago-García, Noguera-Julián, COVID-19 in children and adolescents in Europe: a multinational, multicentre cohort study, Te Lancet Child & Adolescent Health
Jutzeler, Bourguignon, Weis, Comorbidities, clinical signs and symptoms, laboratory fndings, imaging features, treatment strategies, and outcomes in adult and pediatric patients with COVID-19: a systematic review and meta-analysis, Travel Medicine and Infectious Disease
Kim, Whitaker, O'halloran, Hospitalization rates and characteristics of children aged< 18 years hospitalized with laboratory-confrmed COVID-19-COVID-NET, 14 states, MMWR. Morbidity and Mortality Weekly Report
Kirby, New variant of SARS-CoV-2 in UK causes surge of COVID-19, Te Lancet Respiratory Medicine
Kompaniyets, Agathis, Nelson, Underlying medical conditions associated with severe COVID-19 illness among children, JAMA Network Open
Lee, Park, Kim, Lee, Kim, Lymphopenia as a biological predictor of outcomes in COVID-19 patients: a nationwide cohort study, Cancers
Li, Xu, Yu, Risk factors for severity and mortality in adult COVID-19 inpatients in Wuhan, Journal of Allergy and Clinical Immunology
Liu, Lei, Xiao, Epidemiological and clinical characteristics of patients with coronavirus disease-2019 in Shiyan City, China, Frontiers in Cellular and Infection Microbiology
Ludvigsson, Systematic review of COVID-19 in children shows milder cases and a better prognosis than adults, Acta Paediatrica
Madani, Shahin, Yoosef, Red fags of poor prognosis in pediatric cases of COVID-19: the frst 6610 hospitalized children in Iran, BMC Pediatrics
Mahase, Covid-19: What New Variants Are Emerging and How Are Tey Being Investigated? 2021, British Medical Journal Publishing Group
Mahmoudi, Mehdizadeh, Badv, Te coronavirus disease 2019 (COVID-19) in children: a study in an Iranian children's referral hospital, Infection and Drug Resistance
Mamishi, Movahedi, Mohammadi, Multisystem infammatory syndrome associated with SARS-CoV-2 infection in 45 children: a frst report from Iran, Epidemiology and Infection
Mansourian, Ghandi, Habibi, Mehrabi, COVID-19 infection in children: a systematic review and meta-analysis of clinical features and laboratory fndings, Archives de Pediatrie
Martin, Dewitt, Russell, Characteristics, outcomes, and severity risk factors associated with SARS-CoV-2 infection among children in the US national COVID cohort collaborative, JAMA Network Open
Nguyen, Tuc, Hung, Risk factors for disease severity and mortality of children with Covid-19: a study at a Vietnamese Children's hospital, Journal of Infection and Chemotherapy
Oliveira, Colosimo, Simões E Silva, Clinical characteristics and risk factors for death among hospitalised children and adolescents with COVID-19 in Brazil: an analysis of a nationwide database, Te Lancet Child and Adolescent Health
Saeed, Gaba, Shah, Correlation between chest CT severity scores and the clinical parameters of adult patients with COVID-19 pneumonia, Radiology research and practice
States, MMWR, Morbidity and Mortality Weekly Report
Swann, Clinical Characteristics of Children and Young People Admitted to Hospital with Covid-19 in United Kingdom: Prospective Multicentre Observational Cohort Study, British Medical Journal Publishing Group
Von Elm, Altman, Egger, Pocock, Gøtzsche et al., Te Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies, Preventive Medicine
Wang, Zheng, Zheng, Sun, Attaching clinical signifcance to COVID-19-associated diarrhea, Life Sciences
Woodruf, Risk factors for severe COVID-19 in children, Pediatrics
Worldometers, Iran COVID-Coronavirus Statistics-Worldometer
Zachariah, Johnson, Halabi, Epidemiology, clinical features, and disease severity in patients with coronavirus disease 2019 (COVID-19) in a children's hospital in New York City, JAMA Pediatrics
Zhou, Yu, Du, Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study, Lancet
DOI record:
{
"DOI": "10.1155/2023/5205188",
"ISSN": [
"1918-1493",
"1712-9532"
],
"URL": "http://dx.doi.org/10.1155/2023/5205188",
"abstract": "<jats:p>Introduction. COVID-19 prognostic risk factors, therapeutic protocols, and clinical outcomes in pediatric cases are still under investigation. Materials and Methods. This historical cohort study evaluated the survival time of hospitalized children (1 month–18 years old) with COVID-19 admitted from March 2020 to August 2021 to an educational hospital in Yazd, Iran. The follow-up of patients was performed at least one month after discharge. Results. From 183 hospitalized cases, 24 children were deceased. The median age of patients was 5.41, and 54.2% were male. The survival rate after one-month follow-up was 0.88, and the most significant predictors associated with survival time were the male sex, positive history of hospitalization, lymphopenia, hypoxia, and length of stay more than two weeks using Bayesian Cox regression analysis. Conclusion. Accurate estimation of the impact of predictors on poor outcomes may help healthcare providers use therapeutic protocols based on risk factors and healthcare requirements of each patient to improve their survival.</jats:p>",
"alternative-id": [
"5205188",
"5205188"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-8812-0765",
"affiliation": [
{
"name": "Center for Healthcare Data Modeling, Department of Biostatistics and Epidemiology, School of Public Health, Shahid Sadoughi University of Medical Sciences, Yazd, Iran"
}
],
"authenticated-orcid": true,
"family": "Shamsi",
"given": "Farimah",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0001-7987-6694",
"affiliation": [
{
"name": "Children Growth Disorder Research Center, Shahid Sadoughi University of Medical Sciences, Yazd, Iran"
}
],
"authenticated-orcid": true,
"family": "Karimi",
"given": "Mehran",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-8714-2201",
"affiliation": [
{
"name": "Children Growth Disorder Research Center, Shahid Sadoughi University of Medical Sciences, Yazd, Iran"
}
],
"authenticated-orcid": true,
"family": "Nafei",
"given": "Zahra",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-7485-0567",
"affiliation": [
{
"name": "Children Growth Disorder Research Center, Shahid Sadoughi University of Medical Sciences, Yazd, Iran"
}
],
"authenticated-orcid": true,
"family": "Akbarian",
"given": "Elahe",
"sequence": "additional"
}
],
"container-title": "Canadian Journal of Infectious Diseases and Medical Microbiology",
"container-title-short": "Canadian Journal of Infectious Diseases and Medical Microbiology",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
7,
17
]
],
"date-time": "2023-07-17T23:35:10Z",
"timestamp": 1689636910000
},
"deposited": {
"date-parts": [
[
2023,
7,
17
]
],
"date-time": "2023-07-17T23:35:15Z",
"timestamp": 1689636915000
},
"editor": [
{
"affiliation": [],
"family": "Messina",
"given": "Gabriele",
"sequence": "additional"
}
],
"funder": [
{
"DOI": "10.13039/501100015034",
"doi-asserted-by": "publisher",
"name": "Shahid Sadoughi University of Medical Sciences"
}
],
"indexed": {
"date-parts": [
[
2023,
7,
18
]
],
"date-time": "2023-07-18T04:23:20Z",
"timestamp": 1689654200620
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2023,
7,
17
]
]
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
7,
17
]
],
"date-time": "2023-07-17T00:00:00Z",
"timestamp": 1689552000000
}
}
],
"link": [
{
"URL": "http://downloads.hindawi.com/journals/cjidmm/2023/5205188.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://downloads.hindawi.com/journals/cjidmm/2023/5205188.xml",
"content-type": "application/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://downloads.hindawi.com/journals/cjidmm/2023/5205188.pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "98",
"original-title": [],
"page": "1-12",
"prefix": "10.1155",
"published": {
"date-parts": [
[
2023,
7,
17
]
]
},
"published-print": {
"date-parts": [
[
2023,
7,
17
]
]
},
"publisher": "Hindawi Limited",
"reference": [
{
"article-title": "Iran COVID-Coronavirus Statistics-Worldometer",
"author": "Worldometers",
"key": "1",
"year": "2021"
},
{
"DOI": "10.1016/s0140-6736(20)30566-3",
"doi-asserted-by": "publisher",
"key": "2"
},
{
"DOI": "10.15585/mmwr.mm6928a2",
"doi-asserted-by": "publisher",
"key": "3"
},
{
"DOI": "10.15585/mmwr.mm6915e3",
"doi-asserted-by": "publisher",
"key": "4"
},
{
"DOI": "10.1016/j.jaci.2020.04.006",
"doi-asserted-by": "publisher",
"key": "5"
},
{
"DOI": "10.3389/fcimb.2020.00284",
"doi-asserted-by": "publisher",
"key": "6"
},
{
"DOI": "10.1016/j.jfma.2020.04.007",
"doi-asserted-by": "publisher",
"key": "7"
},
{
"DOI": "10.1016/s2352-4642(20)30177-2",
"doi-asserted-by": "publisher",
"key": "8"
},
{
"author": "E. Mahase",
"key": "9",
"volume-title": "Covid-19: What New Variants Are Emerging and How Are They Being Investigated? 2021",
"year": "2021"
},
{
"DOI": "10.1016/s2213-2600(21)00005-9",
"doi-asserted-by": "publisher",
"key": "10"
},
{
"DOI": "10.1111/apa.15870",
"doi-asserted-by": "publisher",
"key": "11"
},
{
"DOI": "10.1016/s2352-4642(21)00196-6",
"doi-asserted-by": "publisher",
"key": "12"
},
{
"DOI": "10.1016/j.ypmed.2007.08.012",
"doi-asserted-by": "publisher",
"key": "13"
},
{
"DOI": "10.1155/2021/6697677",
"doi-asserted-by": "publisher",
"key": "14"
},
{
"author": "World Health Organization",
"key": "15",
"volume-title": "Clinical Management of COVID-19: Interim Guidance",
"year": "2020"
},
{
"DOI": "10.1186/s12887-021-03030-2",
"doi-asserted-by": "publisher",
"key": "16"
},
{
"DOI": "10.1111/apa.15270",
"doi-asserted-by": "publisher",
"key": "17"
},
{
"DOI": "10.1016/s2352-4642(21)00134-6",
"doi-asserted-by": "publisher",
"key": "18"
},
{
"DOI": "10.1542/peds.2020-0702",
"doi-asserted-by": "publisher",
"key": "19"
},
{
"author": "S. Bialek",
"key": "20",
"volume-title": "Coronavirus disease 2019 In Children—United States",
"year": "2020"
},
{
"DOI": "10.2147/idr.s259064",
"doi-asserted-by": "publisher",
"key": "21"
},
{
"author": "O. V. Swann",
"key": "22",
"volume-title": "Clinical Characteristics of Children and Young People Admitted to Hospital with Covid-19 in United Kingdom: Prospective Multicentre Observational Cohort Study",
"year": "2020"
},
{
"DOI": "10.1155/2022/2737719",
"doi-asserted-by": "publisher",
"key": "23"
},
{
"DOI": "10.1001/jamanetworkopen.2021.43151",
"doi-asserted-by": "publisher",
"key": "24"
},
{
"DOI": "10.1002/rmv.2146",
"doi-asserted-by": "publisher",
"key": "25"
},
{
"DOI": "10.15585/mmwr.mm6932e3",
"doi-asserted-by": "publisher",
"key": "26"
},
{
"DOI": "10.1001/jamanetworkopen.2021.11182",
"doi-asserted-by": "publisher",
"key": "27"
},
{
"DOI": "10.1542/peds.2021-053418",
"doi-asserted-by": "publisher",
"key": "28"
},
{
"DOI": "10.1017/s095026882000196x",
"doi-asserted-by": "publisher",
"key": "29"
},
{
"DOI": "10.1001/jamapediatrics.2020.2430",
"doi-asserted-by": "publisher",
"key": "30"
},
{
"DOI": "10.1016/j.jiac.2022.06.010",
"doi-asserted-by": "publisher",
"key": "31"
},
{
"DOI": "10.1016/j.lfs.2020.118312",
"doi-asserted-by": "publisher",
"key": "32"
},
{
"DOI": "10.1016/j.cgh.2020.04.001",
"doi-asserted-by": "publisher",
"key": "33"
},
{
"DOI": "10.1016/j.arcped.2020.12.008",
"doi-asserted-by": "publisher",
"key": "34"
},
{
"DOI": "10.1016/j.tmaid.2020.101825",
"doi-asserted-by": "publisher",
"key": "35"
},
{
"DOI": "10.3390/cancers13030471",
"doi-asserted-by": "publisher",
"key": "36"
}
],
"reference-count": 36,
"references-count": 36,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.hindawi.com/journals/cjidmm/2023/5205188/"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Infectious Diseases",
"Microbiology (medical)"
],
"subtitle": [],
"title": "Survival and Mortality in Hospitalized Children with COVID-19: A Referral Center Experience in Yazd, Iran",
"type": "journal-article",
"volume": "2023"
}
shamsi