Previous vitamin D status and total cholesterol are associated with SARS-CoV-2 infection
et al., Clinica Chimica Acta, doi:10.1016/j.cca.2021.08.003, Aug 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 1,634 patients tested for SARS-CoV-2 in Brazil, showing vitamin D levels <30ng/mL associated with greater odds of a positive SARS-CoV-2 test in patients older than 49 years.
This is the 84th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
risk of case, 50.5% lower, OR 0.50, p = 0.01, inverted to make OR<1 favor high D levels, >30ng/mL, multivariate, RR approximated with OR.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Ribeiro et al., 5 Aug 2021, retrospective, Brazil, peer-reviewed, 8 authors.
Previous vitamin D status and total cholesterol are associated with SARS-CoV-2 infection
Clinica Chimica Acta, doi:10.1016/j.cca.2021.08.003
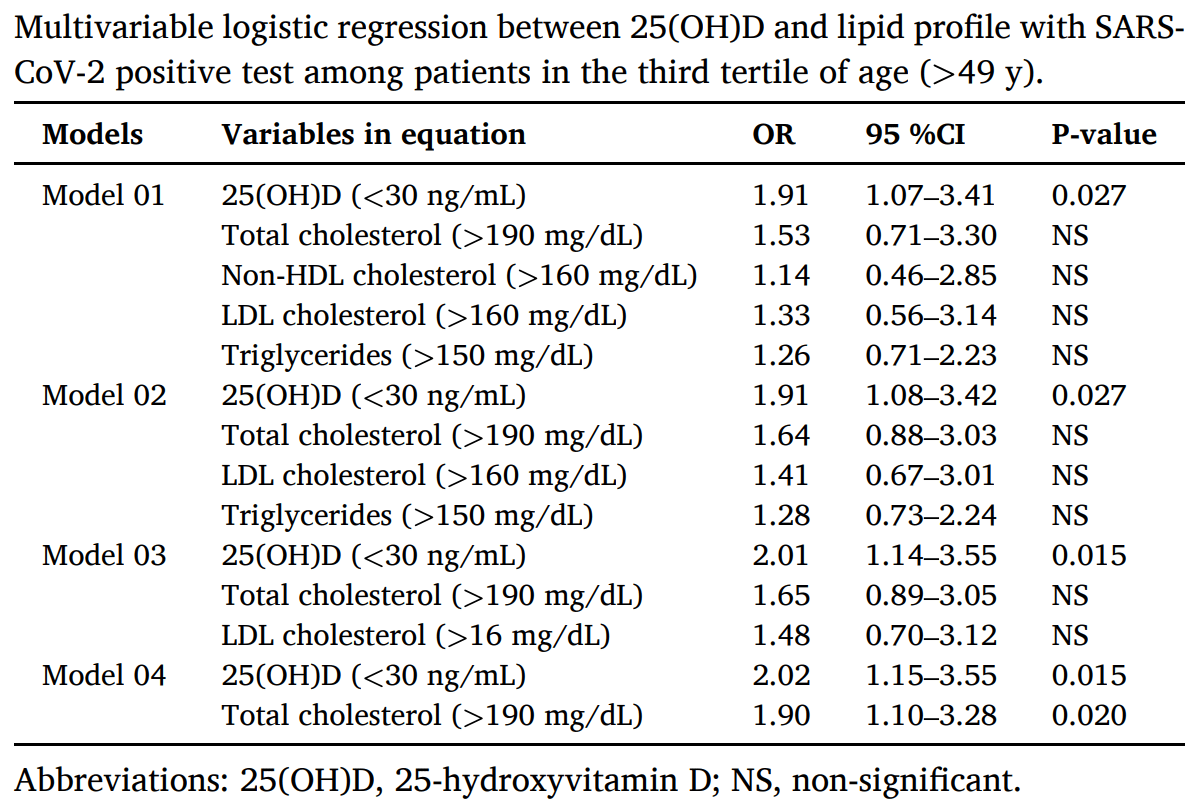
Background: The relationship of vitamin D status and other biochemical parameters with the risk of SARS-CoV-2 infection remains inconclusive, especially in regions with high solar incidence. Therefore, we aimed to associate the 25-hydroxyvitamin D (25(OH)D) concentrations and lipid profile prior to the SARS-CoV-2 tests in a population from a sunny region in Brazil (5 degrees S, 35 degrees W). Methods: This retrospective cohort study enrolled 1634 patients tested for SARS-CoV-2 of a private medical laboratory with 25(OH)D concentration and lipid profile measured ≥ 7 days before the date of the first SARS-CoV-2 RT-PCR test and were categorized according to 25(OH)D sufficiency (≥30 ng/mL) or insufficiency (<30 ng/mL). Multiple logistic regression analyses were performed to assess risk factors associated with positive tests for SARS-CoV-2. Results: Average serum 25(OH)D was 33.6 ng/mL. Vitamin D deficiency (<20 ng/mL) was only found in 2.6% of the participants. Multivariate analysis demonstrated that patients > 49 y with insufficient 25(OH)D (<30 ng/mL) presented increased odds to test positive for SARS-CoV-2 (OR: 2.02, 95 %CI: 1.15 to 3.55, P = 0.015). The same is observed among those with total cholesterol > 190 mg/dL (OR: 1.90, 95 %CI: 1.10 to 3.28, P = 0.020). Conclusions: Previous insufficient 25(OH)D (<30 ng/mL) concentration and high total cholesterol were associated with SARS-CoV-2 infection among adults > 48 y in the study population. Further studies should be conducted to confirm whether measurement of 25(OH)D and lipid profile could be useful to identify patients who are more susceptible to COVID-19.
Author contributions VNS and HGR designed and executed the study; HGR, RCSDK, JFPM, MCCC, and BZR wrote the paper; ADL performed statistical analysis of the data; VLS contributed to the execution of the study; VNS, ADL, and BZR revised the final draft of the manuscript. All authors read and approved the final manuscript.
Declaration of Competing Interest The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Appendix A. Supplementary data Supplementary data to this article can be found online at https://doi. org/10.1016/j.cca.2021.08.003.
References
Abrishami, Dalili, Torbati, Asgari, Arab-Ahmadi et al., Possible association of vitamin D status with lung involvement and outcome in patients with COVID-19: a retrospective study, Eur. J. Nutr, doi:10.1007/s00394-020-02411-0
Ahmed, Siman-Tov, Hall, Bhalla, Narayanan, Human antimicrobial peptides as therapeutics for viral infections, Viruses, doi:10.3390/v11080704
Barlow, Svoboda, Mackellar, Nash, York et al., Antiviral activity and increased host defense against influenza infection elicited by the human cathelicidin LL-37, PLoS ONE, doi:10.1371/journal.pone.0025333
Bilezikian, Bikle, Hewison, Lazaretti-Castro, Formenti et al., Mechanisms in endocrinology: vitamin D and COVID-19, Eur. J. Endocrinol, doi:10.1530/EJE-20-0665
Cereda, Bogliolo, Klersy, Lobascio, Masi et al., Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital, Clin. Nutr, doi:10.1016/j.clnu.2020.10.055
Daneshkhah, Agrawal, Eshein, Subramanian, Roy et al., The possible role of vitamin D in suppressing cytokine storm and associated mortality in COVID-19 patients, doi:10.1007/s40520-020-01677-y
Faludi, Update of the Brazilian Dyslipidemia and Atherosclerosis Prevention Directive, Arq. Bras. Cardiol, doi:10.5935/abc.20170121
Greiller, Martineau, Modulation of the immune response to respiratory viruses by vitamin D, Nutrients, doi:10.3390/nu7064240
Hars, Mendes, Serratrice, Herrmann, Gold et al., Sex-specific association between vitamin D deficiency and COVID-19 mortality in older patients, Osteoporos. Int, doi:10.1007/s00198-020-05677-6
Hastie, Mackay, Ho, Celis-Morales, Katikireddi et al., Vitamin D concentrations and COVID-19 infection UK Biobank, Diabet. Metab. Syndr. Clin. Res. Rev, doi:10.1016/j.dsx.2020.07.021
Heaney, Evaluation, treatment, and prevention of vitamin D 513 deficiency: An endocrine society clinical practice guideline, J. Clin. Endocrinol, doi:10.1210/jc.2011-0385
Hernández, Nan, Fernandez-Ayala, García-Unzueta, Hernández-Hernández et al., Vitamin D status in hospitalized patients with SARS-CoV-2 infection, J. Clin. Endocrinol. Metab, doi:10.1210/clinem/dgaa733
Holick, Binkley, Bischoff-Ferrari, Gordon, Hanley, None
Holick, The vitamin D deficiency pandemic: Approaches for diagnosis, treatment and prevention, Rev. Endocrine Metab. Disord, doi:10.1007/s11154-017-9424-1
Hu, Chen, Wu, He, Ye, Declined serum high density lipoprotein cholesterol is associated with the severity of COVID-19 infection, Clin. Chim. Acta, doi:10.1016/j.cca.2020.07.015
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin. Exp. Res, doi:10.1007/s40520-020-01570-8
Jassil, Sharma, Bikle, Wang, Vitamin d binding protein and 25-hydroxyvitamin d concentrations: emerging clinical applications, Endocr. Pract, doi:10.4158/EP161604.RA
Jose, Manuel, COVID-19 cytokine storm: the interplay between inflammation and coagulation, Lancet Respir. Med, doi:10.1016/S2213-2600(20)30216-2
Kaufman, Niles, Kroll, Bi, Holick, SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D concentrations, PLoS ONE, doi:10.1371/journal.pone.0239252
Kočar, Režen, Rozman, Cholesterol, lipoproteins, and COVID-19: Basic concepts and clinical applications, Biochim. Biophys. Acta -Mol. Cell Biol. Lipids, doi:10.1016/j.bbalip.2020.158849
Kucirka, Lauer, Laeyendecker, Boon, Lessler, Variation in falsenegative rate of reverse transcriptase polymerase chain reaction-based SARS-CoV-2 tests by time since exposure, Ann. Intern. Med, doi:10.7326/M20-1495
Lau, Majumder, Torabi, Saeg, Hoffman et al., Vitamin D insufficiency is prevalent in severe COVID-19, Infect. Dis, doi:10.1101/2020.04.24.20075838
Lips, Current vitamin D status in European and Middle East countries and strategies to prevent vitamin D deficiency: a position statement of the European Calcified Tissue Society, Eur. J. Endocrinol, doi:10.1530/EJE-18-0736
Liu, Chen, Liu, Nie, Lu, Comorbid Chronic Diseases are Strongly Correlated with Disease Severity among COVID-19 Patients: A Systematic Review and Meta-Analysis, Aging Dis, doi:10.14336/AD.2020.0502
Liu, Stenger, Li, Wenzel, Tan et al., Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response, Science, doi:10.1126/science.1123933
Luo, Liao, Shen, Li, Cheng, Vitamin D deficiency is inversely associated with covid-19 incidence and disease severity in Chinese people, J. Nutr, doi:10.1093/jn/nxaa332
Martin, Comparison of a novel method vs the Friedewald equation for estimating low-density lipoprotein cholesterol concentrations from the standard lipid profile, JAMA, doi:10.1001/jama.2013.280532
Masana, Correig, Ibarretxe, Anoro, Arroyo et al., Low HDL and high triglycerides predict COVID-19 severity, Sci. Rep, doi:10.1038/s41598-021-86747-5
Mehta, Mcauley, Brown, Sanchez, Tattersall et al., HLH Across Speciality Collaboration, UK. COVID-19: consider cytokine storm syndromes and immunosuppression, Lancet, doi:10.1016/S0140-6736(20)30628-0
Meltzer, Association of vitamin D status and other clinical characteristics with COVID-19 test results, JAMA Netw Open, doi:10.1001/jamanetworkopen.2020.19722
Meltzer, Best, Zhang, Vokes, Arora et al., Association of Vitamin D Concentrations, Race/Ethnicity, and Clinical Characteristics With COVID-19 Test Results, JAMA Netw. Open, doi:10.1001/jamanetworkopen.2021.4117
Mohan, Cherian, Sharma, Exploring links between vitamin D deficiency and COVID-19, PLoS Pathog, doi:10.1371/journal.ppat.1008874
Moreira, Ferreira, Madeira, Silva, Maeda et al., Reference values of 25-hydroxyvitamin D revisited: a position statement from the Brazilian Society of Endocrinology and Metabolism (SBEM) and the Brazilian Society of Clinical Pathology/Laboratory Medicine (SBPC), Arch. Endocrinol. Metab, doi:10.20945/2359-3997000000258
Panarese, Shahini, Letter: Covid-19, and vitamin D, Aliment. Pharmacol. Ther, doi:10.1111/apt.15752
Pizzini, Aichner, Sahanic, Böhm, Egger et al., Impact of vitamin d deficiency on COVID-19-A prospective analysis from the CovILD registry, Nutrients, doi:10.3390/nu12092775
Raisi-Estabragh, Mccracken, Bethell, Cooper, Cooper et al., Greater risk of severe COVID-19 in Black, Asian and Minority Ethnic populations is not explained by cardiometabolic, socioeconomic or behavioural factors, or by 25 (OH)-vitamin D status: study of 1326 cases from the UK Biobank, J. Public Health, doi:10.1093/pubmed/fdaa095
Raisi-Estabragh, Mccracken, Bethell, Cooper, Cooper et al., Greater risk of severe COVID-19 in Black, Asian and Minority Ethnic populations is not explained by cardiometabolic, socioeconomic or behavioural factors, or by 25(OH)-vitamin D status: study of 1326 cases from the UK Biobank, J Public Health (Oxf), doi:10.1093/pubmed/fdaa095
Schaan, Costa, Santos, Modesto, Amador et al., MtDNA structure: The women who formed the Brazilian Northeast, BMC Evol. Biol, doi:10.1186/s12862-017-1027-7
Schaan, Gusmaõ, Jannuzzi, Modesto, Amador et al., New insights on intercontinental origins of paternal lineages in Northeast Brazil, BMC Evol. Biol, doi:10.1186/s12862-020-1579-9
Silva, Furlanetto, Does serum 25-hydroxyvitamin D decrease during acute-phase response? A systematic review, Nutr. Res, doi:10.1016/j.nutres.2014.12.008
Sly, Lopez, Nauseef, Reiner, 1alpha,25-dihydroxyvitamin D3-induced monocyte antimycobacterial activity is regulated by phosphatidylinositol 3-kinase and mediated by the NADPH-dependent phagocyte oxidase, J. Biol. Chem, doi:10.1074/jbc.M102876200
Stefan, Birkenfeld, Schulze, Ludwig, Obesity and impaired metabolic health in patients with COVID-19, Nat. Rev. Endocrinol, doi:10.1038/s41574-020-0364-6
Szeto, Zucker, Lasota, Rubin, Walker et al., Vitamin D Status and COVID-19 Clinical Outcomes in Hospitalized Patients, Endocr. Res, doi:10.1080/07435800.2020.1867162
Vazquez, Huerta-Delgado, Castillo, Correlation of vitamin D with inflammatory cytokines, atherosclerotic parameters, and lifestyle factors in the setting of heart failure: a 12-month follow-up study, Int J Mol Sci, doi:10.3390/ijms20225811
Virani, Non-HDL cholesterol as a metric of good quality of care: opportunities and challenges, Tex. Heart Inst. J
Wang, Yuan, Pavel, Hobson, Hansen, The role of high cholesterol in age-related COVID19 lethality, BioRxiv, doi:10.1101/2020.05.09.086249
Wickham, Ggplot2: Elegant Graphics for Data Analysis
Yin, Vitamin D and inflammatory diseases, J. Inflamm. Res, doi:10.2147/JIR.S63898
Zdrenghea, Makrinioti, Bagacean, Bush, Johnston et al., Vitamin D modulation of innate immune responses to respiratory viral infections, Rev. Med. Virol, doi:10.1002/rmv.1909
Zhou, Luo, Qin, The association between vitamin D deficiency and community-acquired pneumonia: a meta-analysis of observational studies, Medicine, doi:10.1097/MD.0000000000017252
DOI record:
{
"DOI": "10.1016/j.cca.2021.08.003",
"ISSN": [
"0009-8981"
],
"URL": "http://dx.doi.org/10.1016/j.cca.2021.08.003",
"alternative-id": [
"S0009898121002709"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Previous vitamin D status and total cholesterol are associated with SARS-CoV-2 infection"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Clinica Chimica Acta"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.cca.2021.08.003"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2021 Elsevier B.V."
}
],
"author": [
{
"affiliation": [],
"family": "Ribeiro",
"given": "Heriks Gomes",
"sequence": "first"
},
{
"affiliation": [],
"family": "Dantas-Komatsu",
"given": "Raquel Costa Silva",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Medeiros",
"given": "Jeane Franco Pires",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Carvalho",
"given": "Maria Clara da Cruz",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Soares",
"given": "Victor de Lima",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Reis",
"given": "Bruna Zavarize",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Luchessi",
"given": "André Ducati",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Silbiger",
"given": "Vivian Nogueira",
"sequence": "additional"
}
],
"container-title": "Clinica Chimica Acta",
"container-title-short": "Clinica Chimica Acta",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2021,
8,
5
]
],
"date-time": "2021-08-05T14:55:09Z",
"timestamp": 1628175309000
},
"deposited": {
"date-parts": [
[
2022,
12,
22
]
],
"date-time": "2022-12-22T14:06:21Z",
"timestamp": 1671717981000
},
"funder": [
{
"DOI": "10.13039/501100002322",
"doi-asserted-by": "publisher",
"name": "Coordenação de Aperfeiçoamento de Pessoal de Nível Superior"
},
{
"DOI": "10.13039/501100003593",
"doi-asserted-by": "publisher",
"name": "Conselho Nacional de Desenvolvimento Científico e Tecnológico"
}
],
"indexed": {
"date-parts": [
[
2023,
5,
1
]
],
"date-time": "2023-05-01T23:27:33Z",
"timestamp": 1682983653123
},
"is-referenced-by-count": 6,
"issued": {
"date-parts": [
[
2021,
11
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
11,
1
]
],
"date-time": "2021-11-01T00:00:00Z",
"timestamp": 1635724800000
}
},
{
"URL": "http://www.elsevier.com/open-access/userlicense/1.0/",
"content-version": "vor",
"delay-in-days": 283,
"start": {
"date-parts": [
[
2022,
8,
11
]
],
"date-time": "2022-08-11T00:00:00Z",
"timestamp": 1660176000000
}
},
{
"URL": "https://doi.org/10.15223/policy-017",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
11,
1
]
],
"date-time": "2021-11-01T00:00:00Z",
"timestamp": 1635724800000
}
},
{
"URL": "https://doi.org/10.15223/policy-037",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
11,
1
]
],
"date-time": "2021-11-01T00:00:00Z",
"timestamp": 1635724800000
}
},
{
"URL": "https://doi.org/10.15223/policy-012",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
11,
1
]
],
"date-time": "2021-11-01T00:00:00Z",
"timestamp": 1635724800000
}
},
{
"URL": "https://doi.org/10.15223/policy-029",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
11,
1
]
],
"date-time": "2021-11-01T00:00:00Z",
"timestamp": 1635724800000
}
},
{
"URL": "https://doi.org/10.15223/policy-004",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
11,
1
]
],
"date-time": "2021-11-01T00:00:00Z",
"timestamp": 1635724800000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S0009898121002709?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S0009898121002709?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "8-13",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
11
]
]
},
"published-print": {
"date-parts": [
[
2021,
11
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1371/journal.ppat.1008874",
"article-title": "Exploring links between vitamin D deficiency and COVID-19",
"author": "Mohan",
"doi-asserted-by": "crossref",
"issue": "9",
"journal-title": "PLoS Pathog.",
"key": "10.1016/j.cca.2021.08.003_b0005",
"volume": "16",
"year": "2020"
},
{
"DOI": "10.1002/rmv.1909",
"article-title": "Vitamin D modulation of innate immune responses to respiratory viral infections",
"author": "Zdrenghea",
"doi-asserted-by": "crossref",
"journal-title": "Rev. Med. Virol.",
"key": "10.1016/j.cca.2021.08.003_b0010",
"volume": "27",
"year": "2017"
},
{
"DOI": "10.3390/nu7064240",
"article-title": "Modulation of the immune response to respiratory viruses by vitamin D",
"author": "Greiller",
"doi-asserted-by": "crossref",
"first-page": "4240",
"journal-title": "Nutrients",
"key": "10.1016/j.cca.2021.08.003_b0015",
"volume": "7",
"year": "2015"
},
{
"DOI": "10.1530/EJE-20-0665",
"article-title": "Mechanisms in endocrinology: vitamin D and COVID-19",
"author": "Bilezikian",
"doi-asserted-by": "crossref",
"first-page": "R133",
"issue": "5",
"journal-title": "Eur. J. Endocrinol.",
"key": "10.1016/j.cca.2021.08.003_b0020",
"volume": "183",
"year": "2020"
},
{
"article-title": "The association between vitamin D deficiency and community-acquired pneumonia: a meta-analysis of observational studies",
"author": "Zhou",
"journal-title": "Medicine",
"key": "10.1016/j.cca.2021.08.003_b0025",
"volume": "98",
"year": "2019"
},
{
"DOI": "10.1016/j.dsx.2020.04.050",
"article-title": "Vitamin D concentrations and COVID-19 infection UK Biobank",
"author": "Hastie",
"doi-asserted-by": "crossref",
"first-page": "561",
"journal-title": "Diabet. Metab. Syndr. Clin. Res. Rev.",
"key": "10.1016/j.cca.2021.08.003_b0030",
"volume": "14",
"year": "2020"
},
{
"article-title": "The possible role of vitamin D in suppressing cytokine storm and associated mortality in COVID-19 patients",
"author": "Daneshkhah",
"journal-title": "Infect. Dis. (except HIV/AIDS)",
"key": "10.1016/j.cca.2021.08.003_b0035",
"year": "2020"
},
{
"article-title": "Vitamin D insufficiency is prevalent in severe COVID-19",
"author": "Lau",
"journal-title": "Infect. Dis. (exceptHIV/AIDS)",
"key": "10.1016/j.cca.2021.08.003_b0040",
"year": "2020"
},
{
"DOI": "10.1016/S2213-2600(20)30216-2",
"article-title": "COVID-19 cytokine storm: the interplay between inflammation and coagulation",
"author": "Jose",
"doi-asserted-by": "crossref",
"journal-title": "Lancet Respir. Med.",
"key": "10.1016/j.cca.2021.08.003_b0045",
"year": "2020"
},
{
"DOI": "10.1074/jbc.M102876200",
"article-title": "1alpha,25-dihydroxyvitamin D3-induced monocyte antimycobacterial activity is regulated by phosphatidylinositol 3-kinase and mediated by the NADPH-dependent phagocyte oxidase",
"author": "Sly",
"doi-asserted-by": "crossref",
"first-page": "35482",
"issue": "38",
"journal-title": "J. Biol. Chem.",
"key": "10.1016/j.cca.2021.08.003_b0050",
"volume": "276",
"year": "2001"
},
{
"DOI": "10.1126/science.1123933",
"article-title": "Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response",
"author": "Liu",
"doi-asserted-by": "crossref",
"first-page": "1770",
"issue": "5768",
"journal-title": "Science",
"key": "10.1016/j.cca.2021.08.003_b0055",
"volume": "311",
"year": "2006"
},
{
"DOI": "10.1111/apt.15752",
"article-title": "Letter: Covid-19, and vitamin D",
"author": "Panarese",
"doi-asserted-by": "crossref",
"first-page": "993",
"journal-title": "Aliment. Pharmacol. Ther.",
"key": "10.1016/j.cca.2021.08.003_b0060",
"volume": "51",
"year": "2020"
},
{
"DOI": "10.21203/rs.3.rs-21211/v1",
"doi-asserted-by": "crossref",
"key": "10.1016/j.cca.2021.08.003_b0065",
"unstructured": "Ilie PC, Stefanescu S, Smith L. The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality. Aging Clin. Exp. Res. 2020. http://doi.org/10.1007/s40520-020-01570-8."
},
{
"DOI": "10.1371/journal.pone.0025333",
"article-title": "Antiviral activity and increased host defense against influenza infection elicited by the human cathelicidin LL-37",
"author": "Barlow",
"doi-asserted-by": "crossref",
"journal-title": "PLoS ONE",
"key": "10.1016/j.cca.2021.08.003_b0070",
"volume": "6",
"year": "2011"
},
{
"DOI": "10.3390/v11080704",
"article-title": "Human antimicrobial peptides as therapeutics for viral infections",
"author": "Ahmed",
"doi-asserted-by": "crossref",
"first-page": "704",
"journal-title": "Viruses",
"key": "10.1016/j.cca.2021.08.003_b0075",
"volume": "11",
"year": "2019"
},
{
"DOI": "10.1210/clinem/dgaa733",
"article-title": "Vitamin D status in hospitalized patients with SARS-CoV-2 infection",
"author": "Hernández",
"doi-asserted-by": "crossref",
"first-page": "e1343",
"issue": "3",
"journal-title": "J. Clin. Endocrinol. Metab.",
"key": "10.1016/j.cca.2021.08.003_b0080",
"volume": "106",
"year": "2021"
},
{
"DOI": "10.3390/nu12092775",
"article-title": "Impact of vitamin d deficiency on COVID-19—A prospective analysis from the CovILD registry",
"author": "Pizzini",
"doi-asserted-by": "crossref",
"first-page": "2775",
"issue": "9",
"journal-title": "Nutrients",
"key": "10.1016/j.cca.2021.08.003_b0085",
"volume": "12",
"year": "2020"
},
{
"article-title": "Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital",
"author": "Cereda",
"journal-title": "Clin. Nutr",
"key": "10.1016/j.cca.2021.08.003_b0090",
"year": "2020"
},
{
"DOI": "10.1093/jn/nxaa332",
"article-title": "Vitamin D deficiency is inversely associated with covid-19 incidence and disease severity in Chinese people",
"author": "Luo",
"doi-asserted-by": "crossref",
"first-page": "98",
"issue": "1",
"journal-title": "J. Nutr.",
"key": "10.1016/j.cca.2021.08.003_b0095",
"volume": "151",
"year": "2021"
},
{
"article-title": "Possible association of vitamin D status with lung involvement and outcome in patients with COVID-19: a retrospective study",
"author": "Abrishami",
"first-page": "1",
"journal-title": "Eur. J. Nutr.",
"key": "10.1016/j.cca.2021.08.003_b0100",
"year": "2020"
},
{
"DOI": "10.1007/s00198-020-05677-6",
"article-title": "Sex-specific association between vitamin D deficiency and COVID-19 mortality in older patients",
"author": "Hars",
"doi-asserted-by": "crossref",
"first-page": "2495",
"issue": "12",
"journal-title": "Osteoporos. Int.",
"key": "10.1016/j.cca.2021.08.003_b0105",
"volume": "31",
"year": "2020"
},
{
"DOI": "10.14336/AD.2020.0502",
"article-title": "Comorbid Chronic Diseases are Strongly Correlated with Disease Severity among COVID-19 Patients: A Systematic Review and Meta-Analysis",
"author": "Liu",
"doi-asserted-by": "crossref",
"first-page": "668",
"journal-title": "Aging Dis.",
"key": "10.1016/j.cca.2021.08.003_b0110",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1038/s41574-020-0364-6",
"article-title": "Obesity and impaired metabolic health in patients with COVID-19",
"author": "Stefan",
"doi-asserted-by": "crossref",
"first-page": "341",
"journal-title": "Nat. Rev. Endocrinol.",
"key": "10.1016/j.cca.2021.08.003_b0115",
"volume": "16",
"year": "2020"
},
{
"article-title": "Vitamin D Status and COVID-19 Clinical Outcomes in Hospitalized Patients",
"author": "Szeto",
"first-page": "1",
"journal-title": "Endocr. Res.",
"key": "10.1016/j.cca.2021.08.003_b0120",
"volume": "30",
"year": "2020"
},
{
"DOI": "10.1016/j.nutres.2014.12.008",
"article-title": "Does serum 25-hydroxyvitamin D decrease during acute-phase response? A systematic review",
"author": "Silva",
"doi-asserted-by": "crossref",
"first-page": "91",
"issue": "2",
"journal-title": "Nutr. Res.",
"key": "10.1016/j.cca.2021.08.003_b0125",
"volume": "35",
"year": "2015"
},
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"doi-asserted-by": "crossref",
"key": "10.1016/j.cca.2021.08.003_b0130",
"unstructured": "Meltzer DO, et al. Association of vitamin D status and other clinical characteristics with COVID-19 test results. JAMA Netw Open 2020;3(9):e2019722-e2019722. http://doi.org/10.1001/jamanetworkopen.2020.19722."
},
{
"DOI": "10.1093/pubmed/fdaa095",
"article-title": "Greater risk of severe COVID-19 in Black, Asian and Minority Ethnic populations is not explained by cardiometabolic, socioeconomic or behavioural factors, or by 25 (OH)-vitamin D status: study of 1326 cases from the UK Biobank",
"author": "Raisi-Estabragh",
"doi-asserted-by": "crossref",
"first-page": "451",
"issue": "3",
"journal-title": "J. Public Health",
"key": "10.1016/j.cca.2021.08.003_b0135",
"volume": "42",
"year": "2020"
},
{
"key": "10.1016/j.cca.2021.08.003_b0140",
"unstructured": "National Institute for Space Research (NISR). Natal UV radiation. Natal (RN/Brazil): Laboratory of tropical environmental variables, Ministry of Science, Technology and Innovation 2012."
},
{
"DOI": "10.1210/jc.2011-0385",
"doi-asserted-by": "crossref",
"key": "10.1016/j.cca.2021.08.003_b0145",
"unstructured": "Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, 512 Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D 513 deficiency: An endocrine society clinical practice guideline. J. Clin. Endocrinol. 514 Metab 2011;96:1911–30. http://doi.org/10.1210/jc.2011-0385."
},
{
"DOI": "10.1001/jama.2013.280532",
"article-title": "Comparison of a novel method vs the Friedewald equation for estimating low-density lipoprotein cholesterol concentrations from the standard lipid profile",
"author": "Martin",
"doi-asserted-by": "crossref",
"first-page": "2061",
"issue": "19",
"journal-title": "JAMA",
"key": "10.1016/j.cca.2021.08.003_b0150",
"volume": "310",
"year": "2013"
},
{
"article-title": "Non-HDL cholesterol as a metric of good quality of care: opportunities and challenges",
"author": "Virani",
"first-page": "160",
"issue": "2",
"journal-title": "Tex. Heart Inst. J.",
"key": "10.1016/j.cca.2021.08.003_b0155",
"volume": "38",
"year": "2011"
},
{
"DOI": "10.5935/abc.20170121",
"doi-asserted-by": "crossref",
"key": "10.1016/j.cca.2021.08.003_b0160",
"unstructured": "Faludi AA, et al. Update of the Brazilian Dyslipidemia and Atherosclerosis Prevention Directive. Arq. Bras. Cardiol. 2017;109(2 Supl 1):1-76. http://doi.org/10.5935/abc.20170121."
},
{
"author": "Wickham",
"key": "10.1016/j.cca.2021.08.003_b0165",
"series-title": "Ggplot2: Elegant Graphics for Data Analysis",
"year": "2016"
},
{
"DOI": "10.4158/EP161604.RA",
"article-title": "Vitamin d binding protein and 25-hydroxyvitamin d concentrations: emerging clinical applications",
"author": "Jassil",
"doi-asserted-by": "crossref",
"first-page": "605",
"issue": "5",
"journal-title": "Endocr. Pract.",
"key": "10.1016/j.cca.2021.08.003_b0170",
"volume": "23",
"year": "2017"
},
{
"DOI": "10.1371/journal.pone.0239252",
"article-title": "SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D concentrations",
"author": "Kaufman",
"doi-asserted-by": "crossref",
"issue": "9",
"journal-title": "PLoS ONE",
"key": "10.1016/j.cca.2021.08.003_b0175",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2021.4117",
"article-title": "Association of Vitamin D Concentrations, Race/Ethnicity, and Clinical Characteristics With COVID-19 Test Results",
"author": "Meltzer",
"doi-asserted-by": "crossref",
"issue": "3",
"journal-title": "JAMA Netw. Open",
"key": "10.1016/j.cca.2021.08.003_b0180",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.1186/s12862-020-1579-9",
"article-title": "New insights on intercontinental origins of paternal lineages in Northeast Brazil",
"author": "Schaan",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "BMC Evol. Biol.",
"key": "10.1016/j.cca.2021.08.003_b0185",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1186/s12862-017-1027-7",
"article-title": "MtDNA structure: The women who formed the Brazilian Northeast",
"author": "Schaan",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "BMC Evol. Biol.",
"key": "10.1016/j.cca.2021.08.003_b0190",
"volume": "17",
"year": "2017"
},
{
"DOI": "10.1093/pubmed/fdaa095",
"doi-asserted-by": "crossref",
"key": "10.1016/j.cca.2021.08.003_b0195",
"unstructured": "Raisi-Estabragh Z, McCracken C, Bethell MS, Cooper J, Cooper C, Caulfield MJ, Munroe PB, Harvey NC, Petersen SE. Greater risk of severe COVID-19 in Black, Asian and Minority Ethnic populations is not explained by cardiometabolic, socioeconomic or behavioural factors, or by 25(OH)-vitamin D status: study of 1326 cases from the UK Biobank. J Public Health (Oxf) 2020;18;42(3):451-460. http://doi.org/10.1093/pubmed/fdaa095."
},
{
"article-title": "Vitamin D and inflammatory diseases",
"author": "Yin",
"first-page": "69",
"journal-title": "J. Inflamm. Res.",
"key": "10.1016/j.cca.2021.08.003_b0200",
"volume": "7",
"year": "2014"
},
{
"DOI": "10.3390/ijms20225811",
"doi-asserted-by": "crossref",
"key": "10.1016/j.cca.2021.08.003_b0205",
"unstructured": "Roffe-Vazquez DN, Huerta-Delgado AS, Castillo EC, et al. Correlation of vitamin D with inflammatory cytokines, atherosclerotic parameters, and lifestyle factors in the setting of heart failure: a 12-month follow-up study. Int J Mol Sci. 2019;20(22):5811. http://doi.org/10.3390/ijms20225811."
},
{
"DOI": "10.1016/S0140-6736(20)30628-0",
"article-title": "HLH Across Speciality Collaboration, UK. COVID-19: consider cytokine storm syndromes and immunosuppression",
"author": "Mehta",
"doi-asserted-by": "crossref",
"first-page": "1033",
"issue": "10229",
"journal-title": "Lancet",
"key": "10.1016/j.cca.2021.08.003_b0210",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1530/EJE-18-0736",
"article-title": "Current vitamin D status in European and Middle East countries and strategies to prevent vitamin D deficiency: a position statement of the European Calcified Tissue Society",
"author": "Lips",
"doi-asserted-by": "crossref",
"first-page": "23",
"issue": "4",
"journal-title": "Eur. J. Endocrinol.",
"key": "10.1016/j.cca.2021.08.003_b0215",
"volume": "180",
"year": "2019"
},
{
"article-title": "Reference values of 25-hydroxyvitamin D revisited: a position statement from the Brazilian Society of Endocrinology and Metabolism (SBEM) and the Brazilian Society of Clinical Pathology/Laboratory Medicine (SBPC)",
"author": "Moreira",
"first-page": "462",
"issue": "4",
"journal-title": "Arch. Endocrinol. Metab",
"key": "10.1016/j.cca.2021.08.003_b0220",
"volume": "64",
"year": "2020"
},
{
"DOI": "10.1007/s11154-017-9424-1",
"article-title": "The vitamin D deficiency pandemic: Approaches for diagnosis, treatment and prevention",
"author": "Holick",
"doi-asserted-by": "crossref",
"first-page": "153",
"journal-title": "Rev. Endocrine Metab. Disord.",
"key": "10.1016/j.cca.2021.08.003_b0225",
"volume": "18",
"year": "2017"
},
{
"article-title": "Cholesterol, lipoproteins, and COVID-19: Basic concepts and clinical applications",
"author": "Kočar",
"issue": "2",
"journal-title": "Biochim. Biophys. Acta – Mol. Cell Biol. Lipids",
"key": "10.1016/j.cca.2021.08.003_b0230",
"volume": "1866",
"year": "2021"
},
{
"article-title": "The role of high cholesterol in age-related COVID19 lethality",
"author": "Wang",
"first-page": "1",
"journal-title": "BioRxiv",
"key": "10.1016/j.cca.2021.08.003_b0235",
"year": "2020"
},
{
"DOI": "10.1016/j.cca.2020.07.015",
"article-title": "Declined serum high density lipoprotein cholesterol is associated with the severity of COVID-19 infection",
"author": "Hu",
"doi-asserted-by": "crossref",
"first-page": "105",
"journal-title": "Clin. Chim. Acta",
"key": "10.1016/j.cca.2021.08.003_b0240",
"volume": "510",
"year": "2020"
},
{
"DOI": "10.1038/s41598-021-86747-5",
"article-title": "Low HDL and high triglycerides predict COVID-19 severity",
"author": "Masana",
"doi-asserted-by": "crossref",
"first-page": "7217",
"issue": "1",
"journal-title": "Sci. Rep.",
"key": "10.1016/j.cca.2021.08.003_b0245",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.7326/M20-1495",
"article-title": "Variation in false-negative rate of reverse transcriptase polymerase chain reaction–based SARS-CoV-2 tests by time since exposure",
"author": "Kucirka",
"doi-asserted-by": "crossref",
"first-page": "262",
"issue": "4",
"journal-title": "Ann. Intern. Med.",
"key": "10.1016/j.cca.2021.08.003_b0250",
"volume": "173",
"year": "2020"
}
],
"reference-count": 50,
"references-count": 50,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S0009898121002709"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Biochemistry (medical)",
"Clinical Biochemistry",
"Biochemistry",
"General Medicine"
],
"subtitle": [],
"title": "Previous vitamin D status and total cholesterol are associated with SARS-CoV-2 infection",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "522"
}
