Characteristics and outcomes of COVID-19 patients with IPF: A multi-center retrospective study
et al., Respiratory Medicine and Research, doi:10.1016/j.resmer.2022.100900, Mar 2022
Retrospective 46 idiopathic pulmonary fibrosis patients with COVID-19 in Turkey, showing lower mortality with favipiravir in unadjusted results, without statistical significance.
Potential risks of favipiravir include kidney injury1-3, liver injury2-5, cardiovascular events5,6, pulmonary toxicity6,7, and mutagenicity, carcinogenicity, teratogenicity, embryotoxicity, and the creation of dangerous variants8-14.
This study is excluded in the after exclusion results of meta-analysis:
unadjusted results with no group details.
|
risk of death, 37.5% lower, RR 0.62, p = 0.51, treatment 5 of 23 (21.7%), control 8 of 23 (34.8%), NNT 7.7, day 30.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
1.
Abdulaziz et al., Clinical Features and Prognosis of Acute Kidney Injury in Hospital-Admitted Patients with COVID-19 in Egypt: A Single-Center Experience, Mansoura Medical Journal, doi:10.58775/2735-3990.1433.
2.
Ülger et al., Experimental evaluation of favipiravir (T-705)-induced liver and kidney toxicity in rats, Food and Chemical Toxicology, doi:10.1016/j.fct.2025.115472.
3.
El-Fetouh et al., Experimental Studies on Some Drugs Used in Covid-19 Treatment (Favipiravir and Dexamethasone) in Albino Rats, Journal of Advanced Veterinary Research, 13:10, www.advetresearch.com/index.php/AVR/article/view/1635.
4.
Almutairi et al., Liver Injury in Favipiravir-Treated COVID-19 Patients: Retrospective Single-Center Cohort Study, Tropical Medicine and Infectious Disease, doi:10.3390/tropicalmed8020129.
5.
Siby et al., Temporal Trends in Serious Adverse Events Associated with Oral Antivirals During the COVID-19 Pandemic: Insights from the FAERS Database (2020–2023), Open Forum Infectious Diseases, doi:10.1093/ofid/ofaf695.1825.
6.
Ozhan et al., Evaluation of the cardiopulmonary effects of repurposed COVID-19 therapeutics in healthy rats, Scientific Reports, doi:10.1038/s41598-025-31048-4.
7.
Ülger (B) et al., Evaluation of the effects of favipiravir (T-705) on the lung tissue of healty rats: An experimental study, Food and Chemical Toxicology, doi:10.1016/j.fct.2025.115235.
8.
Zhirnov et al., Favipiravir: the hidden threat of mutagenic action, Journal of microbiology, epidemiology and immunobiology, doi:10.36233/0372-9311-114.
9.
Waters et al., Human genetic risk of treatment with antiviral nucleoside analog drugs that induce lethal mutagenesis: the special case of molnupiravir, Environmental and Molecular Mutagenesis, doi:10.1002/em.22471.
10.
Hadj Hassine et al., Lethal Mutagenesis of RNA Viruses and Approved Drugs with Antiviral Mutagenic Activity, Viruses, doi:10.3390/v14040841.
11.
Shum, C., An investigational study into the drug-associated mutational signature in SARS-CoV-2 viruses, The University of Hong Kong, PhD Thesis, hub.hku.hk/handle/10722/344396.
12.
Shiraki et al., Convenient screening of the reproductive toxicity of favipiravir and antiviral drugs in Caenorhabditis elegans, Heliyon, doi:10.1016/j.heliyon.2024.e35331.
Cilli et al., 3 Mar 2022, retrospective, Turkey, peer-reviewed, 10 authors.
Characteristics and outcomes of COVID-19 patients with IPF: A multi-center retrospective study
Respiratory Medicine and Research, doi:10.1016/j.resmer.2022.100900
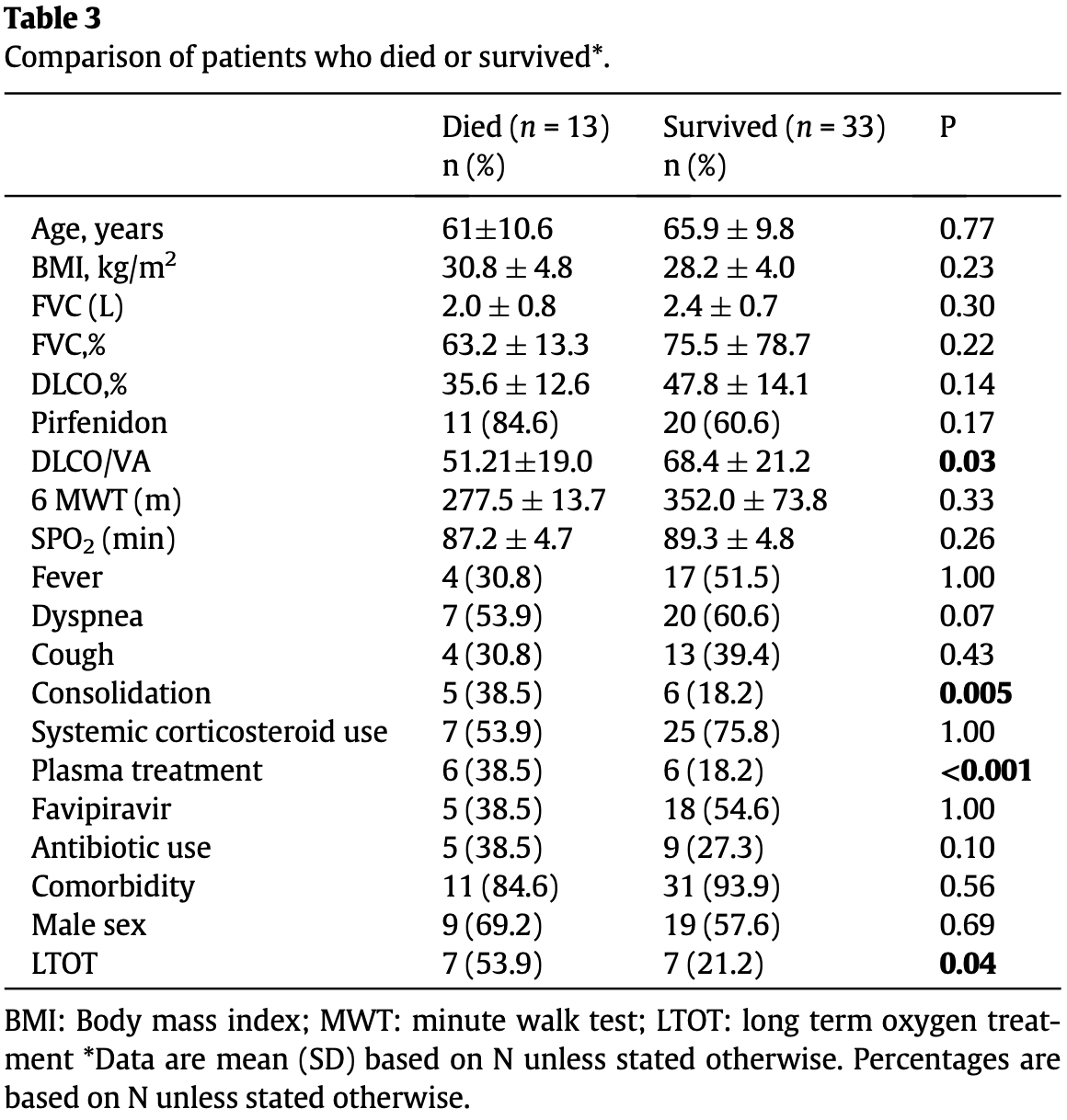
Background: There are few data on severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) (COVID-19) infection in patients with idiopathic pulmonary fibrosis (IPF). The objective of this study is to describe the characteristics and outcomes of IPF patients confirmed COVID-19 infection. Methods: In this retrospective, multi-center, cohort study, patients from 4 hospital medical records with known IPF and a COVID-19 diagnosis were identified. Demographic and clinical outcome data were abstracted through a review of electronic medical records. Results: Records for 46 patients with IPF and COVID-19 were abstracted. The mean age was 65 § 10 years. The most common symptom was dyspnea, followed by fever and cough. Ground-glass opacities (n = 35, 83.3%) and consolidations (n = 11, 26.1%) were the main imaging features of the disease in thorax computed tomography (CT). Twenty-four patients (52.1%) required hospitalization. Among the hospitalized patients, 16 (66.6%) were admitted to the intensive care unit (ICU), and 10 (41.6%) underwent invasive mechanical ventilation. Thirteen patients (28.2%) died of COVID-19 complications. Mortality rate was significantly associated with lower DLCO/VA, long term oxygen therapy and consolidation finding on CT of thorax (p<0.05). On multivariable analysis, neither factor was associated with hospitalization or mortality. Conclusions: IPF patients represent a vulnerable population for COVID-19, according to the high rate of hospitalization, ICU requirement, and mortality rate. Measures to minimize the risk of COVID-19 infection remain key to protect IPF patients.
Conflict of Interest None.
References
Aloufi, Traboulsi, Ding, Fonseca, Nair et al., Angiotensin-converting enzyme 2 expression in COPD and IPF fibroblasts: the forgotten cell in COVID-19, Am J Physiol Lung Cell Mol Physiol, doi:10.1152/ajplung.00455.2020
Drake, Docherty, Harrison, Quint, Adamali et al., Outcome of hospitalization for COVID-19 in patients with interstitial lung disease. An international multicenter study, Am J Respir Crit Care Med, doi:10.1164/rccm.202007-2794OC
Esposito, Menon, Ghosh, Putman, Fredenburgh et al., Increased odds of death for patients with interstitial lung disease and COVID-19: a case-control study, Am J Respir Crit Care Med, doi:10.1164/rccm.202006-2441LE
Gallay, Uzunhan, Borie, Lazor, Rigaud et al., Risk factors for mortality after COVID-19 in patients with preexisting interstitial lung disease, Am J Respir Crit Care Med, doi:10.1164/rccm.202007-2638LE
George, Wells, Jenkins, Pulmonary fibrosis and COVID-19: the potential role for antifibrotic therapy, Lancet Respirat Med, doi:10.1016/S2213-2600(20)30225-3
Huang, Zhang, Chen, Zhang, Wei et al., Clinical characteristics of COVID-19 in patients with pre-existing ILD: a retrospective study in a single center in Wuhan, China, J Med Virol, doi:10.1002/jmv.26174
Lee, Choi, Yang, Lee, Park et al., Interstitial lung disease increases susceptibility to and severity of COVID-19, Eur Respir J, doi:10.1183/13993003.04125-2020
Li, Liu, Hsu, Lin, Hsu et al., Upregulation of ACE2 and TMPRSS2 by particulate matter and idiopathic pulmonary fibrosis: a potential role in severe COVID-19, Part Fibre Toxicol, doi:10.1186/s12989-021-00404-3
Li, Wu, Wu, Guo, Chen et al., The clinical and chest CT features associated with severe and critical COVID-19 pneumonia, Invest Radiol, doi:10.1097/RLI.0000000000000672
Naqvi, Lakhani, Sohail, Maurer, Sofka et al., Patients with idiopathic pulmonary fibrosis have poor clinical outcomes with COVID-19 disease: a propensity matched multicentre research network analysis, BMJ Open Respir Res, doi:10.1136/bmjresp-2021-000969
Pascarella, Strumia, Piliego, Bruno, Buono et al., COVID-19 diagnosis and management: a comprehensive review, J Intern Med, doi:10.1111/joim.13091
Podolanczuk, Richeldi, COVID-19 and interstitial lung disease: keep them separate, Am J Respir Crit Care Med, doi:10.1164/rccm.202010-3918ED
Raghu, Collard, Egan, Martinez, Behr et al., An Official ATS/ ERS/JRS/ALAT statement: idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management, Am J Respir Crit Care Med, doi:10.1164/rccm.2009-040GL
Rajasurya, Gunasekaran, Damarla, Kolluru, A Fatal case of coronavirus disease 2019 (COVID-19) in a patient with idiopathic pulmonary fibrosis, Cureus n, doi:10.7759/cureus.8432
Tuite, Fisman, Odutayo, Bobos, Allen et al., COVID-19 hospitalizations, ICU admissions and deaths associated with the new variants of concern, Ontario COVID-19 Science Advisory Table, doi:10.47326/ocsat.2021.02.18.1.0
Wong, Fidler, Marcoux, Johannson, Assayag et al., Practical considerations for the diagnosis and treatment of fibrotic interstitial lung disease during the coronavirus disease 2019 pandemic, Chest, doi:10.1016/j.chest.2020.04.019
Ye, Zhang, Wang, Huang, Song, Chest CT manifestations of new coronavirus disease 2019 (COVID-19): a pictorial review, Eur Radiol, doi:10.1007/s00330-020-06801-0
Yuan, Yin, Tao, Tan, Hu, Association of radiologic findings with mortality of patients infected with 2019 novel coronavirus in Wuhan, China, PLoS ONE, doi:10.1371/journal.pone.0230548
DOI record:
{
"DOI": "10.1016/j.resmer.2022.100900",
"ISSN": [
"2590-0412"
],
"URL": "http://dx.doi.org/10.1016/j.resmer.2022.100900",
"alternative-id": [
"S2590041222000174"
],
"article-number": "100900",
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Characteristics and outcomes of COVID-19 patients with IPF: A multi-center retrospective study"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Respiratory Medicine and Research"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.resmer.2022.100900"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2022 SPLF and Elsevier Masson SAS. All rights reserved."
}
],
"author": [
{
"affiliation": [],
"family": "Cilli",
"given": "Aykut",
"sequence": "first"
},
{
"affiliation": [],
"family": "Hanta",
"given": "Ismail",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Uzer",
"given": "Fatih",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Coskun",
"given": "Funda",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sevinc",
"given": "Can",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Deniz",
"given": "Pelin Pınar",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Parlak",
"given": "Mehmet",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Altunok",
"given": "Ersoy",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Tertemiz",
"given": "Kemal Can",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ursavas",
"given": "Ahmet",
"sequence": "additional"
}
],
"container-title": [
"Respiratory Medicine and Research"
],
"content-domain": {
"crossmark-restriction": true,
"domain": [
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2022,
3,
3
]
],
"date-time": "2022-03-03T01:30:28Z",
"timestamp": 1646271028000
},
"deposited": {
"date-parts": [
[
2022,
3,
23
]
],
"date-time": "2022-03-23T17:37:46Z",
"timestamp": 1648057066000
},
"indexed": {
"date-parts": [
[
2022,
4,
2
]
],
"date-time": "2022-04-02T15:18:05Z",
"timestamp": 1648912685541
},
"is-referenced-by-count": 0,
"issn-type": [
{
"type": "print",
"value": "2590-0412"
}
],
"issued": {
"date-parts": [
[
2022,
5
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
5,
1
]
],
"date-time": "2022-05-01T00:00:00Z",
"timestamp": 1651363200000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S2590041222000174?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S2590041222000174?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "100900",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2022,
5
]
]
},
"published-print": {
"date-parts": [
[
2022,
5
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"key": "10.1016/j.resmer.2022.100900_bib0001",
"unstructured": "WHO Coronavirus (COVID-19) Dashboard n.d. https://covid19.who.int (accessed October 27, 2021)."
},
{
"DOI": "10.1016/j.chest.2020.04.019",
"article-title": "Practical considerations for the diagnosis and treatment of fibrotic interstitial lung disease during the coronavirus disease 2019 pandemic",
"author": "Wong",
"doi-asserted-by": "crossref",
"first-page": "1069",
"journal-title": "Chest",
"key": "10.1016/j.resmer.2022.100900_bib0002",
"volume": "158",
"year": "2020"
},
{
"DOI": "10.1016/S2213-2600(20)30225-3",
"article-title": "Pulmonary fibrosis and COVID-19: the potential role for antifibrotic therapy",
"author": "George",
"doi-asserted-by": "crossref",
"first-page": "807",
"journal-title": "Lancet Respirat Med",
"key": "10.1016/j.resmer.2022.100900_bib0003",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1164/rccm.202007-2794OC",
"article-title": "Outcome of hospitalization for COVID-19 in patients with interstitial lung disease. An international multicenter study",
"author": "Drake",
"doi-asserted-by": "crossref",
"first-page": "1656",
"journal-title": "Am J Respir Crit Care Med",
"key": "10.1016/j.resmer.2022.100900_bib0004",
"volume": "202",
"year": "2020"
},
{
"DOI": "10.1164/rccm.202006-2441LE",
"article-title": "Increased odds of death for patients with interstitial lung disease and COVID-19: a case-control study",
"author": "Esposito",
"doi-asserted-by": "crossref",
"first-page": "1710",
"journal-title": "Am J Respir Crit Care Med",
"key": "10.1016/j.resmer.2022.100900_bib0005",
"volume": "202",
"year": "2020"
},
{
"DOI": "10.1183/13993003.04125-2020",
"article-title": "Interstitial lung disease increases susceptibility to and severity of COVID-19",
"author": "Lee",
"doi-asserted-by": "crossref",
"journal-title": "Eur Respir J",
"key": "10.1016/j.resmer.2022.100900_bib0006",
"year": "2021"
},
{
"DOI": "10.1164/rccm.202007-2638LE",
"article-title": "Risk factors for mortality after COVID-19 in patients with preexisting interstitial lung disease",
"author": "Gallay",
"doi-asserted-by": "crossref",
"first-page": "245",
"journal-title": "Am J Respir Crit Care Med",
"key": "10.1016/j.resmer.2022.100900_bib0007",
"volume": "203",
"year": "2021"
},
{
"DOI": "10.1164/rccm.2009-040GL",
"article-title": "An Official ATS/ERS/JRS/ALAT statement: idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management",
"author": "Raghu",
"doi-asserted-by": "crossref",
"first-page": "788",
"journal-title": "Am J Respir Crit Care Med",
"key": "10.1016/j.resmer.2022.100900_bib0008",
"volume": "183",
"year": "2011"
},
{
"article-title": "COVID-19 hospitalizations, ICU admissions and deaths associated with the new variants of concern",
"author": "Tuite",
"key": "10.1016/j.resmer.2022.100900_bib0009",
"series-title": "Ontario COVID-19 Science Advisory Table",
"year": "2021"
},
{
"DOI": "10.1111/joim.13091",
"article-title": "COVID-19 diagnosis and management: a comprehensive review",
"author": "Pascarella",
"doi-asserted-by": "crossref",
"first-page": "192",
"journal-title": "J Intern Med",
"key": "10.1016/j.resmer.2022.100900_bib0010",
"volume": "288",
"year": "2020"
},
{
"DOI": "10.1002/jmv.26174",
"article-title": "Clinical characteristics of COVID-19 in patients with pre-existing ILD: a retrospective study in a single center in Wuhan, China",
"author": "Huang",
"doi-asserted-by": "crossref",
"journal-title": "J Med Virol",
"key": "10.1016/j.resmer.2022.100900_bib0011",
"year": "2020"
},
{
"DOI": "10.1136/bmjresp-2021-000969",
"article-title": "Patients with idiopathic pulmonary fibrosis have poor clinical outcomes with COVID-19 disease: a propensity matched multicentre research network analysis",
"author": "Naqvi",
"doi-asserted-by": "crossref",
"journal-title": "BMJ Open Respir Res",
"key": "10.1016/j.resmer.2022.100900_bib0012",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.7759/cureus.8432",
"doi-asserted-by": "crossref",
"key": "10.1016/j.resmer.2022.100900_bib0013",
"unstructured": "Rajasurya V., Gunasekaran K., Damarla V., Kolluru A. A Fatal case of coronavirus disease 2019 (COVID-19) in a patient with idiopathic pulmonary fibrosis. Cureus n.d. ;12:e8432. https://doi.org/10.7759/cureus.8432."
},
{
"DOI": "10.1186/s12989-021-00404-3",
"article-title": "Upregulation of ACE2 and TMPRSS2 by particulate matter and idiopathic pulmonary fibrosis: a potential role in severe COVID-19",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "11",
"journal-title": "Part Fibre Toxicol",
"key": "10.1016/j.resmer.2022.100900_bib0014",
"volume": "18",
"year": "2021"
},
{
"DOI": "10.1152/ajplung.00455.2020",
"article-title": "Angiotensin-converting enzyme 2 expression in COPD and IPF fibroblasts: the forgotten cell in COVID-19",
"author": "Aloufi",
"doi-asserted-by": "crossref",
"first-page": "L152",
"journal-title": "Am J Physiol Lung Cell Mol Physiol",
"key": "10.1016/j.resmer.2022.100900_bib0015",
"volume": "320",
"year": "2021"
},
{
"DOI": "10.1164/rccm.202010-3918ED",
"article-title": "COVID-19 and interstitial lung disease: keep them separate",
"author": "Podolanczuk",
"doi-asserted-by": "crossref",
"first-page": "1614",
"journal-title": "Am J Respir Crit Care Med",
"key": "10.1016/j.resmer.2022.100900_bib0016",
"volume": "202",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0230548",
"article-title": "Association of radiologic findings with mortality of patients infected with 2019 novel coronavirus in Wuhan, China",
"author": "Yuan",
"doi-asserted-by": "crossref",
"journal-title": "PLoS ONE",
"key": "10.1016/j.resmer.2022.100900_bib0017",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1097/RLI.0000000000000672",
"article-title": "The clinical and chest CT features associated with severe and critical COVID-19 pneumonia",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "327",
"journal-title": "Invest Radiol",
"key": "10.1016/j.resmer.2022.100900_bib0018",
"volume": "55",
"year": "2020"
},
{
"DOI": "10.1007/s00330-020-06801-0",
"article-title": "Chest CT manifestations of new coronavirus disease 2019 (COVID-19): a pictorial review",
"author": "Ye",
"doi-asserted-by": "crossref",
"first-page": "4381",
"journal-title": "Eur Radiol",
"key": "10.1016/j.resmer.2022.100900_bib0019",
"volume": "30",
"year": "2020"
}
],
"reference-count": 19,
"references-count": 19,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S2590041222000174"
}
},
"score": 1,
"short-container-title": [
"Respiratory Medicine and Research"
],
"short-title": [],
"source": "Crossref",
"subject": [
"Pulmonary and Respiratory Medicine"
],
"subtitle": [],
"title": [
"Characteristics and outcomes of COVID-19 patients with IPF: A multi-center retrospective study"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "81"
}