Predictors of Mortality among Patients Hospitalized with COVID-19 during the First Wave in India: A Multisite Case-Control Study
et al., The American Journal of Tropical Medicine and Hygiene, doi:10.4269/ajtmh.22-0705, Apr 2023
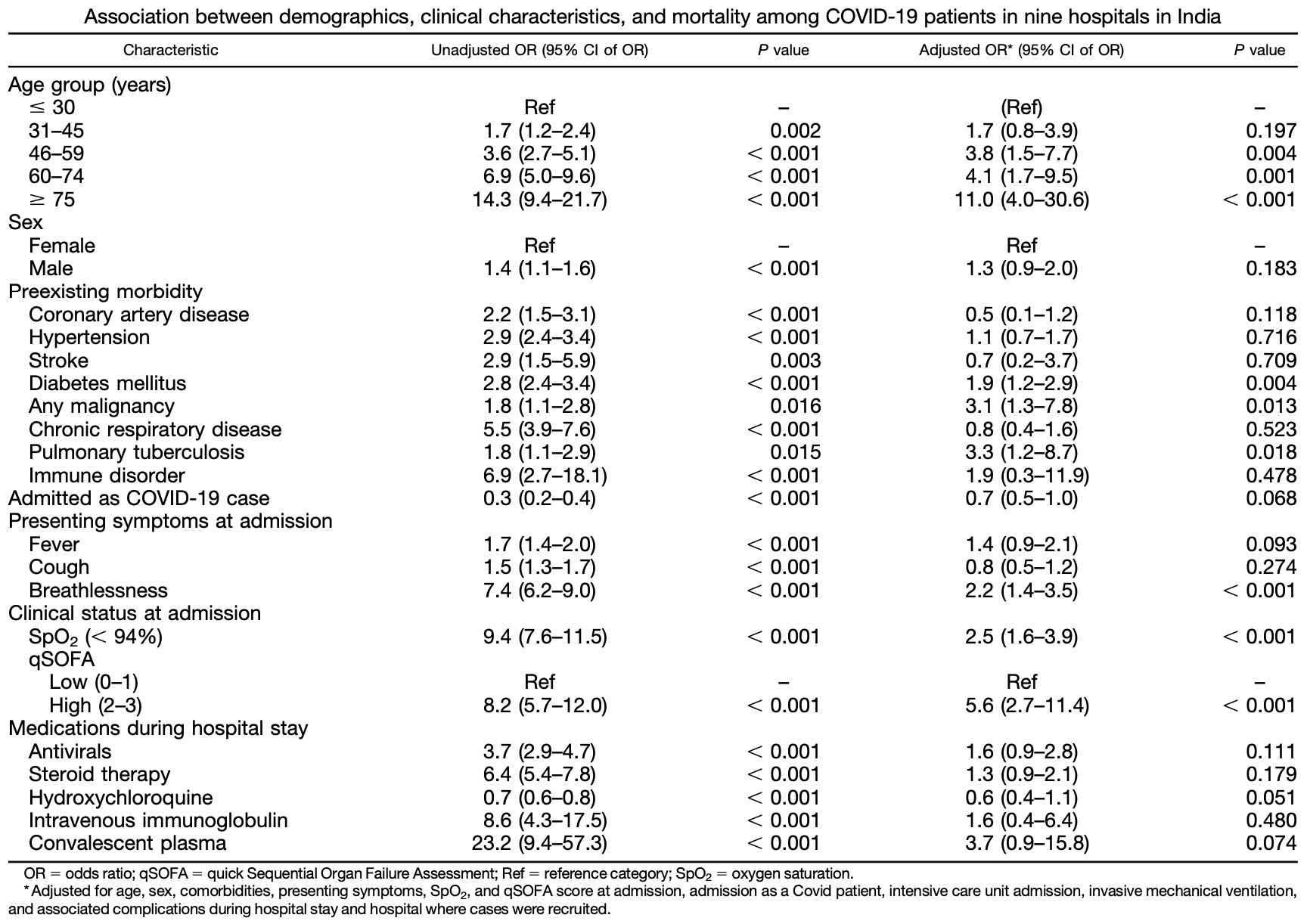
Case control study with 2,431 hospitalized COVID-19 patients in India, showing higher mortality with convalescent plasma treatment, without statistical significance.
Study covers convalescent plasma and HCQ.
|
risk of death, 270.0% higher, OR 3.70, p = 0.07, adjusted per study, case control OR, multivariable.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Krishnan et al., 5 Apr 2023, retrospective, India, peer-reviewed, mean age 52.8, 48 authors, study period March 2020 - March 2021.
Predictors of Mortality among Patients Hospitalized with COVID-19 during the First Wave in India: A Multisite Case-Control Study
The American Journal of Tropical Medicine and Hygiene, doi:10.4269/ajtmh.22-0705
Severe acute respiratory syndrome coronavirus 2 disease (COVID-19) has caused more than 6 million deaths globally. Understanding predictors of mortality will help in prioritizing patient care and preventive approaches. This was a multicentric, unmatched, hospital-based case-control study conducted in nine teaching hospitals in India. Cases were microbiologically confirmed COVID-19 patients who died in the hospital during the period of study and controls were microbiologically confirmed COVID-19 patients who were discharged from the same hospital after recovery. Cases were recruited sequentially from March 2020 until December-March 2021. All information regarding cases and controls was extracted retrospectively from the medical records of patients by trained physicians. Univariable and multivariable logistic regression was done to assess the association between various predictor variables and deaths due to COVID-19. A total of 2,431 patients (1,137 cases and 1,294 controls) were included in the study. The mean age of patients was 52.8 years (SD: 16.5 years), and 32.1% were females. Breathlessness was the most common symptom at the time of admission (53.2%). Increasing age (adjusted odds ratio [aOR]: 46-59 years, 3.4 [95% CI: 1.5-7.7]; 60-74 years, 4.1 [95% CI: 1.7-9.5]; and $ 75 years, 11.0 [95% CI: 4.0-30.6]); preexisting diabetes mellitus (aOR: 1.9 [95% CI: 1.2-2.9]); malignancy (aOR: 3.1 [95% CI: 1.3-7.8]); pulmonary tuberculosis (aOR: 3.3 [95% CI: 1.2-8.8]); breathlessness at the time of admission (aOR: 2.2 [95% CI: 1.4-3.5]); high quick Sequential Organ Failure Assessment score at the time of admission (aOR: 5.6 [95% CI: 2.7-11.4]); and oxygen saturation , 94% at the time of admission (aOR: 2.5 [95% CI: 1.6-3.9]) were associated with mortality due to COVID-19. These results can be used to prioritize patients who are at increased risk of death and to rationalize therapy to reduce mortality due to COVID-19.
References
Agarwal, Biswas, Lohani, Epidemiological determinants of COVID-19 infection and mortality: a study among patients presenting with severe acute respiratory illness during the pandemic in Bihar, India. Niger Postgrad Med J
Agarwal, Mukherjee, Kumar, Chatterjee, Bhatnagar et al., Convalescent plasma in the management of moderate Covid-19 in adults in India: open label phase II multicentre randomized controlled trial (PLACID Trial), BMJ
Arshad, Treatment with hydroxychloroquine, azithromycin, and combination in patients hospitalized with COVID-19, Int J Infect Dis
Bairwa, Kumar, Ajmal, Bahurupi, Kant, Predictors of critical illness and mortality based on symptoms and initial physical examination for patients with SARS-CoV-2: a retrospective cohort study, J Infect Public Health
Bellan, Patti, Hayden, Azzolina, Pirisi et al., Fatality rate and predictors of mortality in an Italian cohort of hospitalized COVID-19 patients, Sci Rep
Bepouka, Predictors of mortality in COVID-19 patients at Kinshasa University Hospital, Democratic Republic of the Congo, from March to, Pan Afr Med J
Berenguer, Characteristics and predictors of death among 4035 consecutively hospitalized patients with COVID-19 in Spain, Clin Microbiol Infect
Bhargava, Sharma, Akagi, Szpunar, Saravolatz, Predictors for in-hospital mortality from coronavirus disease 2019 (COVID-19) infection among adults aged 18-65 years, Infect Control Hosp Epidemiol
Cao, Hiyoshi, Montgomery, Covid-19 case-fatality rate and demographic and socioeconomic influencers: worldwide spatial regression analysis based on country-level data, BMJ Open
Castelnuovo, Common cardiovascular risk factors and in-hospital mortality in 3,894 patients with COVID-19: survival analysis and machine learning-based findings from the multicentre Italian CORIST Study, Nutr Metab Cardiovasc Dis
Chidambaram, Factors associated with disease severity and mortality among patients with COVID-19: a systematic review and meta-analysis, PLoS One
Corona, Pizzocaro, Vena, Rastrelli, Semeraro et al., Diabetes is most important cause for mortality in COVID-19 hospitalized patients: systematic review and meta-analysis, Rev Endocr Metab Disord
Dorjee, Kim, Bonomo, Dolma, Prevalence and predictors of death and severe disease in patients hospitalized due to COVID-19: a comprehensive systematic review and meta-analysis of 77 studies and 38,000 patients, PLoS One
Gopalan, Predictors of mortality among hospitalized COVID-19 patients and risk score formulation for prioritizing tertiary care-an experience from south India, PLOS One
Gupta, Ish, Kumar, Dev, Yadav et al., Evaluation of the clinical profile, laboratory parameters and outcome of two hundred COVID-19 patients from a tertiary centre in India, Monaldi Arch Chest Dis
Imam, Odish, Gill, Connor, Armstrong et al., Older age and comorbidity are independent mortality predictors in a large cohort of 1305 COVID-19 patients in Michigan, United States, J Intern Med
Jain, Iyengar, Vaish, Vaishya, Differential mortality in COVID-19 patients from India and western countries, Diabetes Metab Syndr
Jaspard, Clinical presentation, outcomes and factors associated with mortality: a prospective study from three COVID-19 referral care centres in West Africa, Int J Infect Dis
Mesas, Cavero-Redondo, Alvarez-Bueno, Cabrera, Deandrade et al., Predictors of in-hospital COVID-19 mortality: a comprehensive systematic review and meta-analysis exploring differences by age, sex and health conditions, PLoS One
Recovery, Group, Horby, Dexamethasone in hospitalized patients with Covid-19, N Engl J Med
Recovery, Group, Horby, Effect of hydroxychloroquine in hospitalized patients with Covid-19, N Engl J Med
Tian, Jiang, Yao, Nicholson, Li et al., Predictors of mortality in hospitalized COVID-19 patients: a systematic review and meta-analysis, J Med Virol
Who Solidarity, Consortium, Pan, Repurposed antiviral drugs for Covid-19: interim WHO Solidarity Trial results, N Engl J Med
DOI record:
{
"DOI": "10.4269/ajtmh.22-0705",
"ISSN": [
"0002-9637",
"1476-1645"
],
"URL": "http://dx.doi.org/10.4269/ajtmh.22-0705",
"abstract": "<jats:title>ABSTRACT.</jats:title>\n<jats:p>Severe acute respiratory syndrome coronavirus 2 disease (COVID-19) has caused more than 6 million deaths globally. Understanding predictors of mortality will help in prioritizing patient care and preventive approaches. This was a multicentric, unmatched, hospital-based case-control study conducted in nine teaching hospitals in India. <jats:italic>Cases were microbiologically confirmed COVID-19 patients who died in the hospital during the period of study and controls were microbiologically confirmed COVID-19 patients who were discharged from the same hospital after recovery</jats:italic>. Cases were recruited sequentially from March 2020 until December–March 2021. All information regarding cases and controls was extracted retrospectively from the medical records of patients by trained physicians. Univariable and multivariable logistic regression was done to assess the association between various predictor variables and deaths due to COVID-19. A total of 2,431 patients (1,137 cases and 1,294 controls) were included in the study. The mean age of patients was 52.8 years (SD: 16.5 years), and 32.1% were females. Breathlessness was the most common symptom at the time of admission (53.2%). Increasing age (adjusted odds ratio [aOR]: 46–59 years, 3.4 [95% CI: 1.5–7.7]; 60–74 years, 4.1 [95% CI: 1.7–9.5]; and ≥ 75 years, 11.0 [95% CI: 4.0–30.6]); preexisting diabetes mellitus (aOR: 1.9 [95% CI: 1.2–2.9]); malignancy (aOR: 3.1 [95% CI: 1.3–7.8]); pulmonary tuberculosis (aOR: 3.3 [95% CI: 1.2–8.8]); breathlessness at the time of admission (aOR: 2.2 [95% CI: 1.4–3.5]); high quick Sequential Organ Failure Assessment score at the time of admission (aOR: 5.6 [95% CI: 2.7–11.4]); and oxygen saturation < 94% at the time of admission (aOR: 2.5 [95% CI: 1.6–3.9]) were associated with mortality due to COVID-19. These results can be used to prioritize patients who are at increased risk of death and to rationalize therapy to reduce mortality due to COVID-19.</jats:p>",
"author": [
{
"affiliation": [
{
"name": "Centre for Community Medicine, All India Institute of Medical Sciences (AIIMS), New Delhi, India;"
}
],
"family": "Krishnan",
"given": "Anand",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Centre for Community Medicine, All India Institute of Medical Sciences (AIIMS), New Delhi, India;"
}
],
"family": "Kumar",
"given": "Rakesh",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Centre for Community Medicine, All India Institute of Medical Sciences (AIIMS), New Delhi, India;"
}
],
"family": "Amarchand",
"given": "Ritvik",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Pulmonary, Critical Care and Sleep Medicine, AIIMS, New Delhi, India;"
}
],
"family": "Mohan",
"given": "Anant",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "AIIMS, Rishikesh, India;"
}
],
"family": "Kant",
"given": "Ravi",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Anaesthesia, AIIMS, Rishikesh, India;"
}
],
"family": "Agarwal",
"given": "Ankit",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Physiology, AIIMS, Rishikesh, India;"
}
],
"family": "Kulshreshtha",
"given": "Poorvi",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, AIIMS, Rishikesh, India;"
}
],
"family": "Panda",
"given": "Prasan Kumar",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Rishikesh, India;"
}
],
"family": "Bhadoria",
"given": "Ajeet Singh",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Patna, India;"
}
],
"family": "Agarwal",
"given": "Neeraj",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Patna, India;"
}
],
"family": "Biswas",
"given": "Bijit",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "College of Nursing, AIIMS, Patna, India;"
}
],
"family": "Nair",
"given": "Rathish",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, AIIMS, New Delhi, India;"
}
],
"family": "Wig",
"given": "Naveet",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Jai Prakash Narayan Apex Trauma Center, AIIMS, New Delhi, India;"
}
],
"family": "Malhotra",
"given": "Rajesh",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Onco-Anaesthesia, BRAIRCH, AIIMS, New Delhi, India;"
}
],
"family": "Bhatnagar",
"given": "Sushma",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Anaesthesia and Critical Care, Jai Prakash Narayan Apex Trauma Center, AIIMS, New Delhi, India;"
}
],
"family": "Aggarwal",
"given": "Richa",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Anaesthesia and Critical Care, Jai Prakash Narayan Apex Trauma Center, AIIMS, New Delhi, India;"
}
],
"family": "Soni",
"given": "Kapil Dev",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Hospital Administration, AIIMS, New Delhi, India;"
}
],
"family": "Madan",
"given": "Nirupam",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Anaesthesiology, Pain Medicine and Critical Care, AIIMS, New Delhi, India;"
}
],
"family": "Trikha",
"given": "Anjan",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Pulmonary, Critical Care and Sleep Medicine, AIIMS, New Delhi, India;"
}
],
"family": "Tiwari",
"given": "Pawan",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Hospital Administration, AIIMS, New Delhi, India;"
}
],
"family": "Singh",
"given": "Angel Rajan",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, Jawaharlal Institute of Postgraduate Medical Education & Research (JIPMER), India;"
}
],
"family": "Wyawahare",
"given": "Mukta",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Geriatric Medicine, JIPMER, India;"
}
],
"family": "Gunasekaran",
"given": "Venugopalan",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, Jawaharlal Institute of Postgraduate Medical Education & Research (JIPMER), India;"
}
],
"family": "Sekar",
"given": "Dineshbabu",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "AIIMS, Jodhpur, India;"
}
],
"family": "Misra",
"given": "Sanjeev",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Jodhpur, India;"
}
],
"family": "Bhardwaj",
"given": "Pankaj",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Jodhpur, India;"
}
],
"family": "Goel",
"given": "Akhil Dhanesh",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Pulmonary Medicine, AIIMS, Jodhpur, India;"
}
],
"family": "Dutt",
"given": "Naveen",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, AIIMS, Jodhpur, India;"
}
],
"family": "Kumar",
"given": "Deepak",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "AIIMS, Raipur, India;"
}
],
"family": "Nagarkar",
"given": "Nitin M.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Raipur, India;"
}
],
"family": "Galhotra",
"given": "Abhiruchi",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Paediatrics, AIIMS, Raipur, India;"
}
],
"family": "Jindal",
"given": "Atul",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "National Tuberculosis Elimination Program, AIIMS, Raipur, India;"
}
],
"family": "Raj",
"given": "Utsav",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Pulmonary Medicine, AIIMS, Raipur, India;"
}
],
"family": "Behera",
"given": "Ajoy",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, AIIMS, Raipur, India;"
}
],
"family": "Siddiqui",
"given": "Sabbah",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Bhopal, India;"
}
],
"family": "Kokane",
"given": "Arun",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, AIIMS, Bhopal, India;"
}
],
"family": "Joshi",
"given": "Rajnish",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Bhopal, India;"
}
],
"family": "Pakhare",
"given": "Abhijit",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Bhopal, India;"
}
],
"family": "Farooque",
"given": "Farhan",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, AIIMS, Bhopal, India;"
}
],
"family": "Pawan",
"given": "Sai",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Nagpur, India;"
}
],
"family": "Deshmukh",
"given": "Pradeep",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Community & Family Medicine, AIIMS, Nagpur, India;"
}
],
"family": "Solanki",
"given": "Ranjan",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Medicine, AIIMS, Nagpur, India;"
}
],
"family": "Rathod",
"given": "Bharatsing",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "AIIMS, Nagpur, India;"
}
],
"family": "Dutta",
"given": "Vibha",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Pulmonary Medicine & Critical Care, AIIMS, Bhubaneswar, India;"
}
],
"family": "Mohapatra",
"given": "Prasanta Raghab",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Pulmonary Medicine & Critical Care, AIIMS, Bhubaneswar, India;"
}
],
"family": "Panigrahi",
"given": "Manoj Kumar",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Trauma & Emergency Medicine, AIIMS, Bhubaneswar, India;"
}
],
"family": "Barik",
"given": "Sadananda",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "AIIMS, New Delhi, India"
}
],
"family": "Guleria",
"given": "Randeep",
"sequence": "additional"
}
],
"container-title": "The American Journal of Tropical Medicine and Hygiene",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
3,
13
]
],
"date-time": "2023-03-13T12:36:43Z",
"timestamp": 1678711003000
},
"deposited": {
"date-parts": [
[
2023,
4,
5
]
],
"date-time": "2023-04-05T14:33:35Z",
"timestamp": 1680705215000
},
"indexed": {
"date-parts": [
[
2023,
4,
6
]
],
"date-time": "2023-04-06T04:49:11Z",
"timestamp": 1680756551524
},
"is-referenced-by-count": 0,
"issue": "4",
"issued": {
"date-parts": [
[
2023,
4,
5
]
]
},
"journal-issue": {
"issue": "4"
},
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
4,
5
]
],
"date-time": "2023-04-05T00:00:00Z",
"timestamp": 1680652800000
}
}
],
"link": [
{
"URL": "https://www.ajtmh.org/view/journals/tpmd/108/4/article-p727.xml",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://www.ajtmh.org/downloadpdf/journals/tpmd/108/4/article-p727.xml",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "syndication"
},
{
"URL": "https://www.ajtmh.org/downloadpdf/journals/tpmd/108/4/article-p727.xml",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "2795",
"original-title": [],
"page": "727-733",
"prefix": "10.4269",
"published": {
"date-parts": [
[
2023,
4,
5
]
]
},
"published-print": {
"date-parts": [
[
2023,
4,
5
]
]
},
"publisher": "American Society of Tropical Medicine and Hygiene",
"reference": [
{
"key": "b1",
"year": "2023"
},
{
"key": "b2"
},
{
"article-title": "Covid-19 case-fatality rate and demographic and socioeconomic influencers: worldwide spatial regression analysis based on country-level data",
"first-page": "e043560",
"key": "b3",
"series-title": "BMJ Open",
"volume": "10",
"year": "2010"
},
{
"article-title": "Differential mortality in COVID-19 patients from India and western countries",
"first-page": "1037",
"key": "b4",
"series-title": "Diabetes Metab Syndr",
"volume": "14",
"year": "2020"
},
{
"article-title": "Factors associated with disease severity and mortality among patients with COVID-19: a systematic review and meta-analysis",
"first-page": "e0241541",
"key": "b5",
"series-title": "PLoS One",
"volume": "15",
"year": "2020"
},
{
"article-title": "Prevalence and predictors of death and severe disease in patients hospitalized due to COVID-19: a comprehensive systematic review and meta-analysis of 77 studies and 38,000 patients",
"author": "Dorjee",
"first-page": "e0243191",
"key": "b6",
"series-title": "PLoS One",
"volume": "15",
"year": "2020"
},
{
"article-title": "Predictors of mortality in hospitalized COVID‐19 patients: a systematic review and meta‐analysis",
"first-page": "1875",
"key": "b7",
"series-title": "J Med Virol",
"volume": "92",
"year": "2020"
},
{
"article-title": "Predictors of in-hospital COVID-19 mortality: a comprehensive systematic review and meta-analysis exploring differences by age, sex and health conditions",
"first-page": "e0241742",
"key": "b8",
"series-title": "PLoS One",
"volume": "15",
"year": "2020"
},
{
"article-title": "Treatment with hydroxychloroquine, azithromycin, and combination in patients hospitalized with COVID-19",
"first-page": "396",
"key": "b9",
"series-title": "Int J Infect Dis",
"volume": "97",
"year": "2020"
},
{
"article-title": "Effect of hydroxychloroquine in hospitalized patients with Covid-19",
"first-page": "2030",
"key": "b10",
"series-title": "N Engl J Med",
"volume": "383",
"year": "2020"
},
{
"article-title": "Remdisivir and three other drugs for hospitalized patients with COVID-19: final results of the WHO solidarity randomized trial and updated meta-analyses",
"first-page": "1941",
"key": "b11",
"series-title": "Lancet",
"volume": "399"
},
{
"article-title": "Epidemiological determinants of COVID-19 infection and mortality: a study among patients presenting with severe acute respiratory illness during the pandemic in Bihar, India",
"first-page": "293",
"key": "b12",
"series-title": "Niger Postgrad Med J",
"volume": "27",
"year": "2020"
},
{
"article-title": "Evaluation of the clinical profile, laboratory parameters and outcome of two hundred COVID-19 patients from a tertiary centre in India",
"author": "Gupta",
"first-page": "33169598",
"key": "b13",
"series-title": "Monaldi Arch Chest Dis",
"volume": "9",
"year": "2020"
},
{
"article-title": "Patient care and clinical outcomes for patients with COVID-19 infection admitted to African high-care or intensive care units (ACCCOS): a multicentre, prospective, observational cohort study",
"first-page": "1885",
"key": "b14",
"series-title": "Lancet",
"volume": "397",
"year": "2021"
},
{
"article-title": "Fatality rate and predictors of mortality in an Italian cohort of hospitalized COVID‐19 patients",
"first-page": "20731",
"key": "b15",
"series-title": "Sci Rep",
"volume": "10",
"year": "2020"
},
{
"article-title": "Predictors of mortality in COVID-19 patients at Kinshasa University Hospital, Democratic Republic of the Congo, from March to June 2020",
"first-page": "105",
"key": "b16",
"series-title": "Pan Afr Med J",
"volume": "37",
"year": "2020"
},
{
"article-title": "Characteristics and predictors of death among 4035 consecutively hospitalized patients with COVID-19 in Spain",
"first-page": "1525",
"key": "b17",
"series-title": "Clin Microbiol Infect",
"volume": "26",
"year": "2020"
},
{
"article-title": "Common cardiovascular risk factors and in-hospital mortality in 3,894 patients with COVID-19: survival analysis and machine learning-based findings from the multicentre Italian CORIST Study",
"first-page": "1899",
"key": "b18",
"series-title": "Nutr Metab Cardiovasc Dis",
"volume": "30",
"year": "2020"
},
{
"article-title": "Clinical presentation, outcomes and factors associated with mortality: a prospective study from three COVID-19 referral care centres in West Africa",
"first-page": "45",
"key": "b19",
"series-title": "Int J Infect Dis",
"volume": "108",
"year": "2021"
},
{
"article-title": "Predictors for in-hospital mortality from coronavirus disease 2019 (COVID-19) infection among adults aged 18–65 years",
"first-page": "775",
"key": "b20",
"series-title": "Infect Control Hosp Epidemiol",
"volume": "42",
"year": "2021"
},
{
"article-title": "Predictors of critical illness and mortality based on symptoms and initial physical examination for patients with SARS-CoV-2: a retrospective cohort study",
"first-page": "1028",
"key": "b21",
"series-title": "J Infect Public Health",
"volume": "14",
"year": "2021"
},
{
"article-title": "Older age and comorbidity are independent mortality predictors in a large cohort of 1305 COVID-19 patients in Michigan, United States",
"first-page": "469",
"key": "b22",
"series-title": "J Intern Med",
"volume": "288",
"year": "2020"
},
{
"article-title": "Diabetes is most important cause for mortality in COVID-19 hospitalized patients: systematic review and meta-analysis",
"first-page": "275",
"key": "b23",
"series-title": "Rev Endocr Metab Disord",
"volume": "22",
"year": "2021"
},
{
"article-title": "Repurposed antiviral drugs for Covid-19: interim WHO Solidarity Trial results",
"first-page": "497",
"key": "b24",
"series-title": "N Engl J Med",
"volume": "384",
"year": "2021"
},
{
"article-title": "Dexamethasone in hospitalized patients with Covid-19",
"first-page": "693",
"key": "b25",
"series-title": "N Engl J Med",
"volume": "384",
"year": "2021"
},
{
"article-title": "Convalescent plasma in patients admitted to hospital with Covid-19 (RECOVERY): a randomized controlled, open-label, platform trial",
"first-page": "2049",
"key": "b26",
"series-title": "Lancet",
"volume": "397",
"year": "2021"
},
{
"article-title": "Convalescent plasma in the management of moderate Covid-19 in adults in India: open label phase II multicentre randomized controlled trial (PLACID Trial)",
"first-page": "m3939",
"key": "b27",
"series-title": "BMJ",
"volume": "371",
"year": "2020"
},
{
"article-title": "Predictors of mortality among hospitalized COVID-19 patients and risk score formulation for prioritizing tertiary care—an experience from south India",
"author": "Gopalan",
"first-page": "e0263471",
"key": "b28",
"series-title": "PLOS One",
"volume": "17",
"year": "2022"
}
],
"reference-count": 28,
"references-count": 28,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.ajtmh.org/view/journals/tpmd/108/4/article-p727.xml"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Virology",
"Infectious Diseases",
"Parasitology"
],
"subtitle": [],
"title": "Predictors of Mortality among Patients Hospitalized with COVID-19 during the First Wave in India: A Multisite Case-Control Study",
"type": "journal-article",
"volume": "108"
}
krishnan2