Vitamin B12 status and outcomes in patients admitted to intensive care unit with COVID-19: a three-group comparative analysis
et al., Journal of Health Sciences and Medicine, doi:10.32322/jhsm.1854699, Mar 2026
38th treatment shown to reduce risk in
February 2022, now with p = 0.023 from 4 studies.
Lower risk for recovery.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
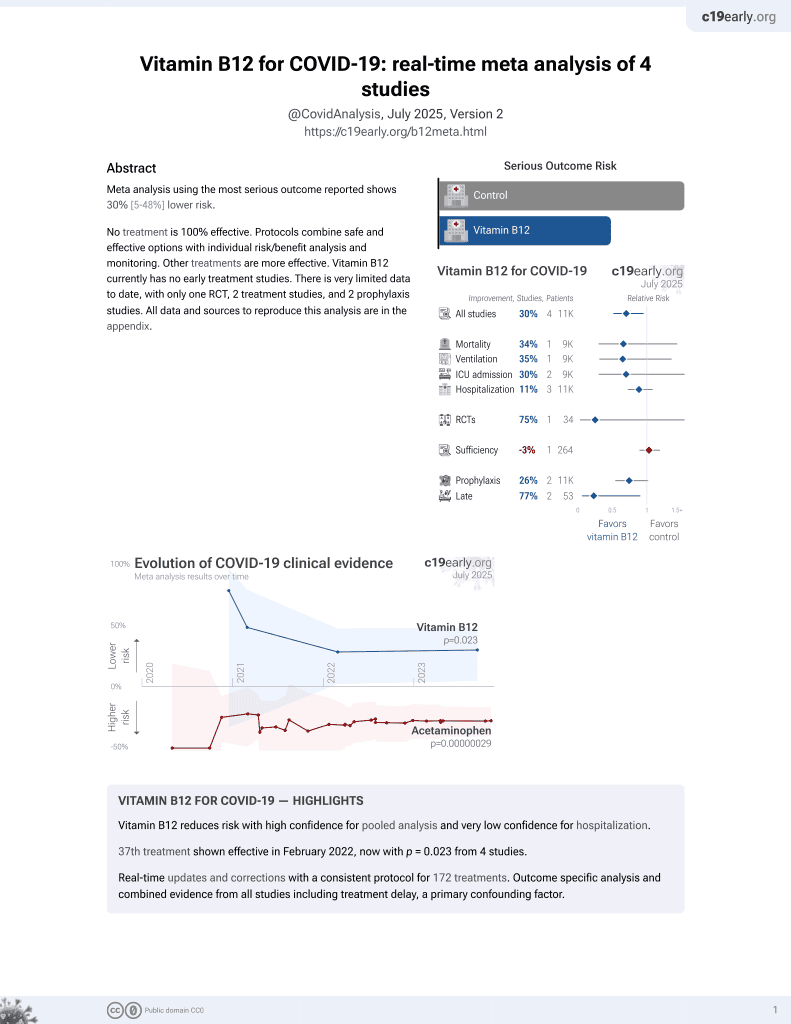
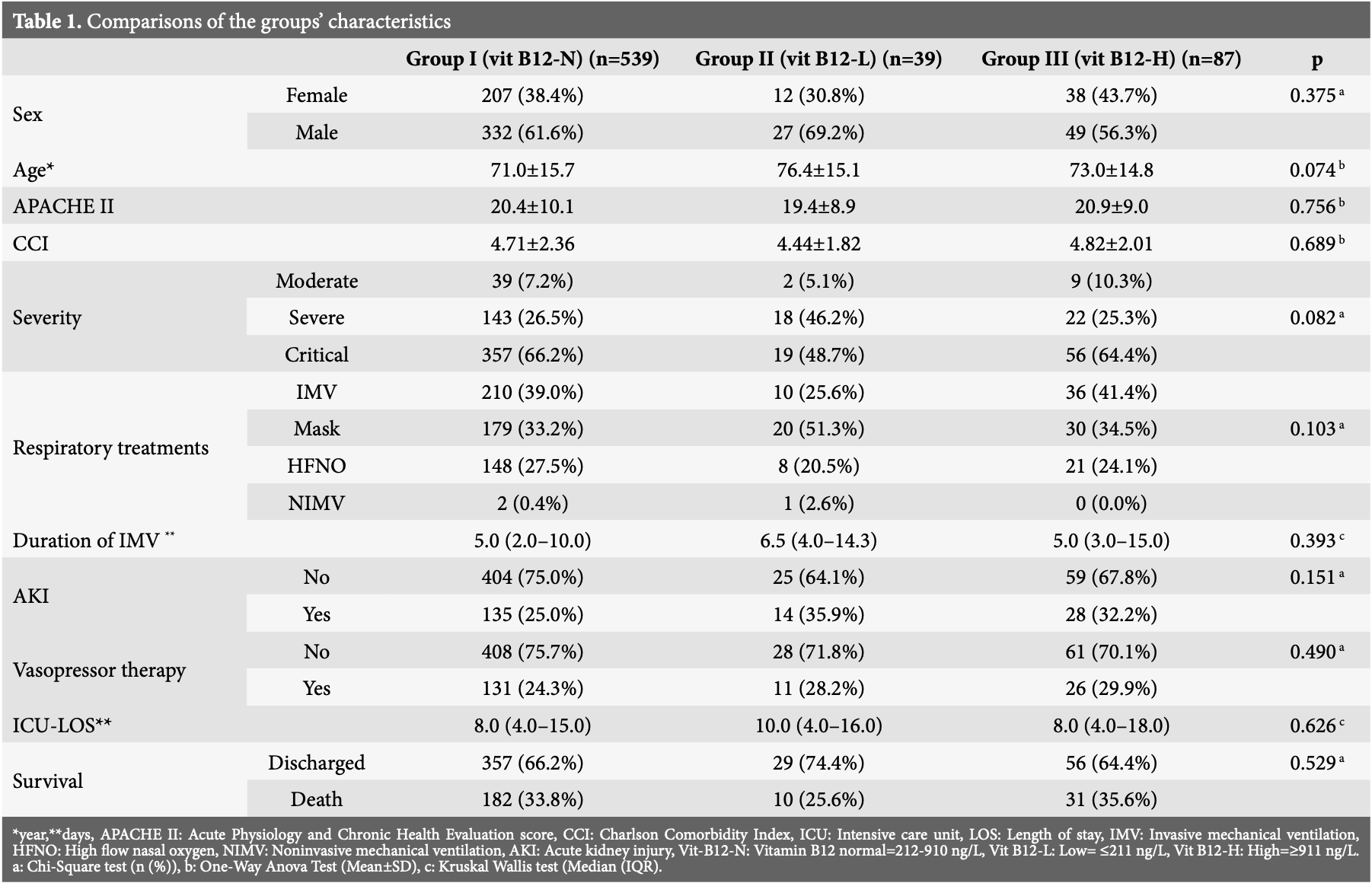
Retrospective 665 COVID-19 ICU patients in Turkey showing no significant association between vitamin B12 levels at ICU admission and disease severity, ICU length of stay, or mortality.
Authors rely exclusively on total serum vitamin B12 rather than the biologically active form, potentially causing exposure misclassification. The study omits data and statistical adjustment for COVID-19 therapeutics (e.g., corticosteroids, antivirals).
The logistic regression shows vitamin B12 OR = 1.00 (95% CI 1.00-1.00), however with vitamin B12 on a continuous ng/L scale, a one-unit increase in B12 would have a negligible effect. The OR should ideally be reported per clinically meaningful increment (e.g., per 100 ng/L).
|
risk of death, 31.7% higher, RR 1.32, p = 0.38, treatment 182 of 539 (33.8%), control 10 of 39 (25.6%), normal vs. deficient levels.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Kayar Çalılı et al., 12 Mar 2026, retrospective, Belgium, peer-reviewed, 7 authors, study period March 2020 - June 2021.
Contact: duygukayar@gmail.com.
Vitamin B12 status and outcomes in patients admitted to intensive care unit with COVID-19: a three-group comparative analysis
Journal of Health Sciences and Medicine, doi:10.32322/jhsm.1854699
Aims: Vitamin B12 (Vit B12) plays important role in immune modulation. We aimed to compare clinical outcomes, laboratory findings, and survival rates among coronavirus disease 2019 (COVID-19) patients admitted to the intensive care unit (ICU) based on their vit B12 levels and to identify factors associated with mortality. Methods: This retrospective study examined ICU patients with COVID-19. Patients were categorized into three groups according to their vit B12 levels at ICU admission: normal (Vit B12-N), low (Vit B12-L) and high (Vit B12). The groups were compared in terms of patient characteristics, laboratory parameters, and survival outcomes. Additionally, the characteristics and laboratory values of the entire cohort were analyzed based on survival status. Results: A total of 665 patients were included (Vit B12-N: 539; Vit B12-L: 39; Vit B12-H: 87). There were no differences in disease severity, clinical characteristics, length of stay, and mortality between the groups (p>0.05). The high vit B12 group showed higher RDW and lower albumin levels compared with the normal vit B12 group (p<0.05). A higher Acute Physiology and Chronic Health Evaluation (APACHE) II score was found to be independently associated with increased mortality (p=0.000). Conclusion: Serum vit B12 levels at ICU admission were not associated with disease severity, clinical outcomes, or survival in critically ill patients with COVID-19. APACHE II score was the only variable independently associated with mortality. However, the observed relationships between vit B12 levels and RDW and albumin suggest the presence of complex metabolic interactions that require further investigation in prospective, multicenter studies.
Conflict of Interest The authors declare no conflicts of interest related to this study.
Financial Disclosure The authors received no financial support for the conduct or publication of this research.
Author Contributions
Concept
References
Akbar, Pranata, Wibowo, Lim, Sihite et al., The association between serum prealbumin and poor outcome in COVID-19-systematic review and meta-analysis, Eur Rev Med Pharmacol Sci, doi:10.26355/eurrev_202105_25955
Andrès, Serraj, Zhu, Vermorken, The pathophysiology of elevated vitamin B12 in clinical practice, QJM, doi:10.1093/qjmed/hct051
Batista, Cintra, Lucena, The role of vitamin B12 in viral infections: a comprehensive review of its relationship with the muscle-gut-brain axis and implications for SARS-CoV-2 infection, Nutr Rev, doi:10.1093/nutrit/nuab092
Battaglini, Lopes-Pacheco, Castro-Faria-Neto, Pelosi, Rocco, Laboratory biomarkers for diagnosis and prognosis in COVID-19, Front Immunol, doi:10.3389/fimmu.2022.857573
Choi, Shin, Hyper-inflammatory responses in COVID-19 and anti-inflammatory therapeutic approaches, BMB Rep, doi:10.5483/BMBRep.2022.55.1.152
Damayanthi, Prabani, Nutritional determinants and COVID-19 outcomes of older patients with COVID-19: a systematic review, Arch Gerontol Geriatr, doi:10.1016/j.archger.2021.104411
Djordjevic, Milenkovic, Stojanovic, Vitamins, microelements and the immune system: current standpoint in the fight against coronavirus disease 2019, Br J Nutr, doi:10.1017/S0007114522000083
Domínguez-López, Kovatcheva, Casas, Higher circulating vitamin B12 is associated with lower levels of inflammatory markers in individuals at high cardiovascular risk and in naturally aged mice, J Sci Food Agric, doi:10.1002/jsfa.12976
Ersöz, Yılmaz, The association between micronutrient and hemogram values and prognostic factors in COVID-19 patients: a singlecenter experience from Turkey, Int J Clin Pract, doi:10.1111/ijcp.14078
Gamarra-Morales, Molina-López, Herrera-Quintana, Vázquez-Lorente, Planells, Folic acid and vitamin B12 as biomarkers of morbidity and mortality in patients with septic shock, Nutr Hosp, doi:10.20960/nh.03505
Gonçalves, Gonçalves, COVID-19: a multiorgan perspective, Front Cell Infect Microbiol, doi:10.3389/fcimb.2024.1425547
Guaní-Guerra, Torres-Murillo, Muñoz-Corona, Diagnostic accuracy of the RDW for predicting death in COVID-19, Medicina, doi:10.3390/medicina58050613
Gupta, The lactate and the lactate dehydrogenase in inflammatory diseases and major risk factors in COVID-19 patients, Inflammation, doi:10.1007/s10753-022-01680-7
Harb, Deckert, Bressenot, The deficit in folate and vitamin B12 triggers liver macrovesicular steatosis and inflammation in rats with dextran sodium sulfate-induced colitis, J Nutr Biochem, doi:10.1016/j.jnutbio.2020.108415
Itelman, Wasserstrum, Segev, Clinical characterization of 162 COVID-19 patients in Israel: preliminary report from a large tertiary center, Isr Med Assoc J
Kellum, Norbert, Aspelin, KDIGO clinical practice guideline for acute kidney injury, Kidney Int Suppl, doi:10.1038/kisup.2012
Lymperaki, Kazeli, Variti, Potential role of certain biomarkers such as vitamin B12, ROS, albumin, as early predictors for prognosis of COVID-19 outcomes, Medicines, doi:10.3390/medicines9060036
Moatasim, Kutkat, Osman, Potent antiviral activity of vitamin B12 against severe acute respiratory syndrome coronavirus 2, middle east respiratory syndrome coronavirus, and human coronavirus 229E, Microorganisms, doi:10.3390/microorganisms11112777
Oztas, Erdogan, Benzil, Nadar, Erel, A new inflammatory marker: vitamin B12, J Immunol Clin Microbiol
Palladino, Complete blood count alterations in COVID-19 patients: a narrative review, Biochem Med, doi:10.11613/BM.2021.030501
Richardson, Lovegrove, Nutritional status of micronutrients as a possible and modifiable risk factor for COVID-19: a UK perspective, Br J Nutr, doi:10.1017/S000711452000330X
Romain, Sviri, Linton, Stav, Van Heerden, The role of vitamin B12 in the critically ill-a review, Anaesth Intensive Care, doi:10.1177/0310057X1604400410
Seyedalinaghi, Shahidi, Mojdeganlou, The effect of macronutrient and micronutrient supplements on COVID-19: an umbrella review, J Health Popul Nutr, doi:10.1186/s41043-024-00504-8
Sezgin, Evaluation of serum vitamin B12 levels in patients with COVID-19 infection: a case-control study, J Med Biochem, doi:10.5937/jomb0-42357
Soohoo, Ahmadi, Qader, Association of serum vitamin B12 and folate with mortality in incident hemodialysis patients, Nephrol Dial Transplant, doi:10.1093/ndt/gfw090
Stabler, Vitamin B12
Taylor, Marson, Elhadi, Factors associated with mortality in patients with COVID-19 admitted to intensive care: a systematic review and meta-analysis, Anaesthesia, doi:10.1111/anae.15532
Tripathi, Singh, Zhou, Vitamin B12 and folate decrease inflammation and fibrosis in NASH by preventing syntaxin 17 homocysteinylation, J Hepatol, doi:10.1016/j.jhep.2022.06.033
Tuuminen, Sorsa, Tornudd, Poussa, Antila et al., The association between high sensitivity C-reactive protein and micronutrient levels: a cross-sectional analysis based on a laboratory database, Clin Nutr ESPEN, doi:10.1016/j.clnesp.2019.06.011
Ulloque-Badaracco, Alarcon-Braga, Association of vitamin B12, folate, and homocysteine with COVID-19 severity and mortality: a systematic review and meta-analysis, SAGE Open Med, doi:10.1177/20503121241253957
Valdez-Martínez, Márquez-González, Ramírez-Aldana, Bedolla, The controversial issue of hypervitaminosis B12 as prognostic factor of mortality: global lessons from a systematic review and meta-analysis, Nutrients, doi:10.3390/nu17132184
Wee, COVID-19's toll on the elderly and those with diabetes mellitus-is vitamin B12 deficiency an accomplice?, Med Hypotheses, doi:10.1016/j.mehy.2020.110374
DOI record:
{
"DOI": "10.32322/jhsm.1854699",
"ISSN": [
"2636-8579"
],
"URL": "http://dx.doi.org/10.32322/jhsm.1854699",
"abstract": "<jats:p xml:lang=\"en\">Aims: Vitamin B12 (Vit B12) plays important role in immune modulation. We aimed to compare clinical outcomes, laboratory findings, and survival rates among coronavirus disease 2019 (COVID-19) patients admitted to the intensive care unit (ICU) based on their vit B12 levels and to identify factors associated with mortality. Methods: This retrospective study examined ICU patients with COVID-19. Patients were categorized into three groups according to their vit B12 levels at ICU admission: normal (Vit B12-N), low (Vit B12-L) and high (Vit B12). The groups were compared in terms of patient characteristics, laboratory parameters, and survival outcomes. Additionally, the characteristics and laboratory values of the entire cohort were analyzed based on survival status.Results: A total of 665 patients were included (Vit B12-N: 539; Vit B12-L: 39; Vit B12-H: 87). There were no differences in disease severity, clinical characteristics, length of stay, and mortality between the groups (p&gt;0.05). The high vit B12 group showed higher RDW and lower albumin levels compared with the normal vit B12 group (p</jats:p>",
"accepted": {
"date-parts": [
[
2026,
2,
14
]
]
},
"author": [
{
"ORCID": "https://orcid.org/0000-0001-9251-3708",
"affiliation": [
{
"name": "ANKARA YILDIRIM BEYAZIT ÜNİVERSİTESİ, TIP FAKÜLTESİ"
}
],
"authenticated-orcid": false,
"family": "Kayar Çalılı",
"given": "Duygu",
"sequence": "first"
},
{
"ORCID": "https://orcid.org/0009-0005-2512-0556",
"affiliation": [
{
"name": "Adıyaman Training and Research Hospital"
}
],
"authenticated-orcid": false,
"family": "Yüzbaşıoğlu",
"given": "Nihal",
"sequence": "additional"
},
{
"ORCID": "https://orcid.org/0000-0003-2193-7655",
"affiliation": [
{
"name": "Ankara Bilkent City Hospital"
}
],
"authenticated-orcid": false,
"family": "Bölükbaşı",
"given": "Demet",
"sequence": "additional"
},
{
"ORCID": "https://orcid.org/0000-0002-9255-9084",
"affiliation": [
{
"name": "Ankara Bilkent City Hospital"
}
],
"authenticated-orcid": false,
"family": "Seğmen",
"given": "Fatih",
"sequence": "additional"
},
{
"ORCID": "https://orcid.org/0000-0002-9329-7485",
"affiliation": [
{
"name": "University of Health Sciences Ankara Bilkent City Hospital"
}
],
"authenticated-orcid": false,
"family": "Erdem",
"given": "Deniz",
"sequence": "additional"
},
{
"ORCID": "https://orcid.org/0000-0002-0405-0107",
"affiliation": [
{
"name": "University of Health Sciences Ankara Bilkent City Hospital"
}
],
"authenticated-orcid": false,
"family": "Özkoçak Turan",
"given": "Işıl",
"sequence": "additional"
},
{
"ORCID": "https://orcid.org/0000-0001-9856-2391",
"affiliation": [
{
"name": "ANKARA YILDIRIM BEYAZIT ÜNİVERSİTESİ, TIP FAKÜLTESİ"
}
],
"authenticated-orcid": false,
"family": "İzdeş",
"given": "Seval",
"sequence": "additional"
}
],
"container-title": "Journal of Health Sciences and Medicine",
"container-title-short": "J Health Sci Med / JHSM",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2026,
3,
19
]
],
"date-time": "2026-03-19T11:59:19Z",
"timestamp": 1773921559000
},
"deposited": {
"date-parts": [
[
2026,
3,
19
]
],
"date-time": "2026-03-19T11:59:23Z",
"timestamp": 1773921563000
},
"indexed": {
"date-parts": [
[
2026,
3,
19
]
],
"date-time": "2026-03-19T14:41:35Z",
"timestamp": 1773931295595,
"version": "3.50.1"
},
"is-referenced-by-count": 0,
"issue": "2",
"issued": {
"date-parts": [
[
2026,
3,
12
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2026,
3,
12
]
]
}
},
"language": "en",
"member": "17352",
"original-title": [],
"page": "462-468",
"prefix": "10.32322",
"published": {
"date-parts": [
[
2026,
3,
12
]
]
},
"published-online": {
"date-parts": [
[
2026,
3,
12
]
]
},
"publisher": "Journal of Health Sciences and Medicine",
"reference": [
{
"DOI": "10.3389/fcimb.2024.1425547",
"doi-asserted-by": "crossref",
"key": "ref1",
"unstructured": "Guarienti FA, Gonçalves JIB, Gonçalves JB, et al. COVID-19: a multi-organ perspective. Front Cell Infect Microbiol. 2024;14:1425547. doi:10. 3389/fcimb.2024.1425547"
},
{
"DOI": "10.5483/BMBRep.2022.55.1.152",
"doi-asserted-by": "crossref",
"key": "ref2",
"unstructured": "Choi H, Shin EC. Hyper-inflammatory responses in COVID-19 and anti- inflammatory therapeutic approaches. BMB Rep. 2022;55(1):11-19. doi:10.5483/BMBRep.2022.55.1.152"
},
{
"DOI": "10.1186/s41043-024-00504-8",
"doi-asserted-by": "crossref",
"key": "ref3",
"unstructured": "SeyedAlinaghi S, Shahidi R, Mojdeganlou H, et al. The effect of macronutrient and micronutrient supplements on COVID-19: an umbrella review. J Health Popul Nutr. 2024;43(1):16. doi:10.1186/s41043-024-00504-8"
},
{
"DOI": "10.3390/microorganisms11112777",
"doi-asserted-by": "crossref",
"key": "ref4",
"unstructured": "Moatasim Y, Kutkat O, Osman AM, et al. Potent antiviral activity of vitamin B12 against severe acute respiratory syndrome coronavirus 2, middle east respiratory syndrome coronavirus, and human coronavirus 229E. Microorganisms. 2023;11(11):2777. doi:10.3390/microorganisms 11112777"
},
{
"DOI": "10.1177/20503121241253957",
"doi-asserted-by": "crossref",
"key": "ref5",
"unstructured": "Ulloque-Badaracco JR, Al-Kassab-Córdova A, Alarcon-Braga EA, et al. Association of vitamin B12, folate, and homocysteine with COVID-19 severity and mortality: a systematic review and meta-analysis. SAGE Open Med. 2024;12:20503121241253957. doi:10.1177/20503121241253957"
},
{
"DOI": "10.1016/B978-0-323-66162-1.00015-9",
"doi-asserted-by": "crossref",
"key": "ref6",
"unstructured": "Stabler SP. Vitamin B12. In: Marriott BP, Birt DF, Stallings VA, Yates AA, eds. Present knowledge in nutrition. 11th ed. Washington, DC: Elsevier. 2020."
},
{
"DOI": "10.1017/S0007114522000083",
"doi-asserted-by": "crossref",
"key": "ref7",
"unstructured": "Djordjevic B, Milenkovic J, Stojanovic D, et al. Vitamins, microelements and the immune system: current standpoint in the fight against coronavirus disease 2019. Br J Nutr. 2022;128(11):2131-2146. doi:10.1017/S0007114522000083"
},
{
"DOI": "10.1093/nutrit/nuab092",
"doi-asserted-by": "crossref",
"key": "ref8",
"unstructured": "Batista KS, Cintra VM, Lucena PAF, et al. The role of vitamin B12 in viral infections: a comprehensive review of its relationship with the muscle-gut-brain axis and implications for SARS-CoV-2 infection. Nutr Rev. 2022;80(3):561-578. doi:10.1093/nutrit/nuab092"
},
{
"DOI": "10.1016/j.mehy.2020.110374",
"doi-asserted-by": "crossref",
"key": "ref9",
"unstructured": "Wee AKH. COVID-19's toll on the elderly and those with diabetes mellitus–is vitamin B12 deficiency an accomplice? Med Hypotheses. 2021;146:110374. doi:10.1016/j.mehy.2020.110374"
},
{
"DOI": "10.5937/jomb0-42357",
"doi-asserted-by": "crossref",
"key": "ref10",
"unstructured": "Sezgin Y. Evaluation of serum vitamin B12 levels in patients with COVID-19 infection: a case-control study. J Med Biochem. 2023;42(3): 524-529. doi:10.5937/jomb0-42357"
},
{
"key": "ref11",
"unstructured": "Oztas D, Erdogan S, Benzil A, Nadar O, Erel O. A new inflammatory marker: vitamin B12. J Immunol Clin Microbiol. 2019;4(1):1-12."
},
{
"DOI": "10.15557/PiMR.2020.0004",
"doi-asserted-by": "crossref",
"key": "ref12",
"unstructured": "World Health Organization. Clinical management of COVID-19: interim guidance, 27 May 2020. World Health Organization. License: CC BY-NC-SA 3.0 IGO. 2020. Available from: https://iris.who.int/handle/10665/332196"
},
{
"DOI": "10.1038/kisup.2012.1",
"doi-asserted-by": "crossref",
"key": "ref13",
"unstructured": "Kellum JAL, Norbert L, Aspelin P, et al. KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl. 2012;2(1):1 138. doi: 10.1038/kisup.2012.1"
},
{
"DOI": "10.1177/0310057X1604400410",
"doi-asserted-by": "crossref",
"key": "ref14",
"unstructured": "Romain M, Sviri S, Linton DM, Stav I, Van Heerden PV. The role of vitamin B12 in the critically ill-a review. Anaesth Intensive Care. 2016; 44(4):447-452. doi:10.1177/0310057X1604400410"
},
{
"DOI": "10.1016/j.jnutbio.2020.108415",
"doi-asserted-by": "crossref",
"key": "ref15",
"unstructured": "Harb Z, Deckert V, Bressenot AM, et al. The deficit in folate and vitamin B12 triggers liver macrovesicular steatosis and inflammation in rats with dextran sodium sulfate-induced colitis. J Nutr Biochem. 2020;84: 108415. doi:10.1016/j.jnutbio.2020.108415"
},
{
"DOI": "10.1017/S000711452000330X",
"doi-asserted-by": "crossref",
"key": "ref16",
"unstructured": "Richardson DP, Lovegrove JA. Nutritional status of micronutrients as a possible and modifiable risk factor for COVID-19: a UK perspective. Br J Nutr. 2021;125(6):678-684. doi:10.1017/S000711452000330X"
},
{
"DOI": "10.1016/j.archger.2021.104411",
"doi-asserted-by": "crossref",
"key": "ref17",
"unstructured": "Damayanthi HDWT, Prabani KIP. Nutritional determinants and COVID-19 outcomes of older patients with COVID-19: a systematic review. Arch Gerontol Geriatr. 2021;95:104411. doi:10.1016/j.archger. 2021.104411"
},
{
"DOI": "10.1016/j.jhep.2022.06.033",
"doi-asserted-by": "crossref",
"key": "ref18",
"unstructured": "Tripathi M, Singh BK, Zhou J, et al. Vitamin B12 and folate decrease inflammation and fibrosis in NASH by preventing syntaxin 17 homocysteinylation. J Hepatol. 2022;77(5):1246-1255. doi:10.1016/j.jhep. 2022.06.033"
},
{
"DOI": "10.1002/jsfa.12976",
"doi-asserted-by": "crossref",
"key": "ref19",
"unstructured": "Domínguez-López I, Kovatcheva M, Casas R, et al. Higher circulating vitamin B12 is associated with lower levels of inflammatory markers in individuals at high cardiovascular risk and in naturally aged mice. J Sci Food Agric. 2024;104(2):875-882. doi:10.1002/jsfa.12976"
},
{
"DOI": "10.1093/qjmed/hct051",
"doi-asserted-by": "crossref",
"key": "ref20",
"unstructured": "Andrès E, Serraj K, Zhu J, Vermorken AJ. The pathophysiology of elevated vitamin B12 in clinical practice. QJM. 2013;106(6):505-515. doi: 10.1093/qjmed/hct051"
},
{
"DOI": "10.1093/ndt/gfw090",
"doi-asserted-by": "crossref",
"key": "ref21",
"unstructured": "Soohoo M, Ahmadi SF, Qader H, et al. Association of serum vitamin B12 and folate with mortality in incident hemodialysis patients. Nephrol Dial Transplant. 2017;32(6):1024-1032. doi:10.1093/ndt/gfw090"
},
{
"DOI": "10.20960/nh.03505",
"doi-asserted-by": "crossref",
"key": "ref22",
"unstructured": "Gamarra-Morales Y, Molina-López J, Herrera-Quintana L, Vázquez-Lorente H, Planells E. Folic acid and vitamin B12 as biomarkers of morbidity and mortality in patients with septic shock. Nutr Hosp. 2022; 39(2):247-255. doi:10.20960/nh.03505"
},
{
"DOI": "10.3390/medicines9060036",
"doi-asserted-by": "crossref",
"key": "ref23",
"unstructured": "Lymperaki E, Kazeli K, Variti G, et al. Potential role of certain biomarkers such as vitamin B12, ROS, albumin, as early predictors for prognosis of COVID-19 outcomes. Medicines (Basel). 2022;9(6):36. doi: 10.3390/medicines9060036"
},
{
"DOI": "10.1111/ijcp.14078",
"doi-asserted-by": "crossref",
"key": "ref24",
"unstructured": "Ersöz A, Yılmaz TE. The association between micronutrient and hemogram values and prognostic factors in COVID-19 patients: a single-center experience from Turkey. Int J Clin Pract. 2021;75(6):e14078. doi: 10.1111/ijcp.14078"
},
{
"key": "ref25",
"unstructured": "Itelman E, Wasserstrum Y, Segev A, et al. Clinical characterization of 162 COVID-19 patients in Israel: preliminary report from a large tertiary center. Isr Med Assoc J. 2020;22(5):271-274."
},
{
"DOI": "10.1111/anae.15532",
"doi-asserted-by": "crossref",
"key": "ref26",
"unstructured": "Taylor EH, Marson EJ, Elhadi M, et al. Factors associated with mortality in patients with COVID-19 admitted to intensive care: a systematic review and meta-analysis. Anaesthesia. 2021;76(9):1224-1232. doi:10. 1111/anae.15532"
},
{
"DOI": "10.1016/j.clnesp.2019.06.011",
"doi-asserted-by": "crossref",
"key": "ref27",
"unstructured": "Tuuminen T, Sorsa M, Tornudd M, Poussa T, Antila E, Jaakkola K. The association between high sensitivity C-reactive protein and micronutrient levels: a cross-sectional analysis based on a laboratory database. Clin Nutr ESPEN. 2019;33:283-289. doi:10.1016/j.clnesp.2019. 06.011"
},
{
"DOI": "10.3390/nu17132184",
"doi-asserted-by": "crossref",
"key": "ref28",
"unstructured": "Valdez-Martínez E, Márquez-González H, Ramírez-Aldana R, Bedolla M. The controversial issue of hypervitaminosis B12 as prognostic factor of mortality: global lessons from a systematic review and meta-analysis. Nutrients. 2025;17(13):2184. doi:10.3390/nu17132184"
},
{
"DOI": "10.11613/BM.2021.030501",
"doi-asserted-by": "crossref",
"key": "ref29",
"unstructured": "Palladino M. Complete blood count alterations in COVID-19 patients: a narrative review. Biochem Med (Zagreb). 2021;31(3):030501. doi:10. 11613/BM.2021.030501"
},
{
"DOI": "10.3389/fimmu.2022.857573",
"doi-asserted-by": "crossref",
"key": "ref30",
"unstructured": "Battaglini D, Lopes-Pacheco M, Castro-Faria-Neto HC, Pelosi P, Rocco PRM. Laboratory biomarkers for diagnosis and prognosis in COVID-19. Front Immunol. 2022;13:857573. doi:10.3389/fimmu.2022.857573"
},
{
"DOI": "10.1007/s10753-022-01680-7",
"doi-asserted-by": "crossref",
"key": "ref31",
"unstructured": "Gupta GS. The lactate and the lactate dehydrogenase in inflammatory diseases and major risk factors in COVID-19 patients. Inflammation. 2022;45(6):2091-2123. doi:10.1007/s10753-022-01680-7"
},
{
"DOI": "10.3390/medicina58050613",
"doi-asserted-by": "crossref",
"key": "ref32",
"unstructured": "Guaní-Guerra E, Torres-Murillo B, Muñoz-Corona C, et al. Diagnostic accuracy of the RDW for predicting death in COVID-19. Medicina (Kaunas). 2022;58(5):613. doi:10.3390/medicina58050613"
},
{
"key": "ref33",
"unstructured": "Akbar MR, Pranata R, Wibowo A, Lim MA, Sihite TA, Martha JW. The association between serum prealbumin and poor outcome in COVID-19-systematic review and meta-analysis. Eur Rev Med Pharmacol Sci. 2021;25(10):3879-3885. doi:10.26355/eurrev_202105_25955"
}
],
"reference-count": 33,
"references-count": 33,
"relation": {},
"resource": {
"primary": {
"URL": "https://dergipark.org.tr/en/doi/10.32322/jhsm.1854699"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Vitamin B12 status and outcomes in patients admitted to intensive care unit with COVID-19: a three-group comparative analysis",
"type": "journal-article",
"volume": "9"
}
