Duration of SARS-CoV-2 RNA Shedding Is Significantly Influenced by Disease Severity, Bilateral Pulmonary Infiltrates, Antibiotic Treatment, and Diabetic Status: Consideration for Isolation Period
et al., Pathophysiology, doi:10.3390/pathophysiology30020016, May 2023
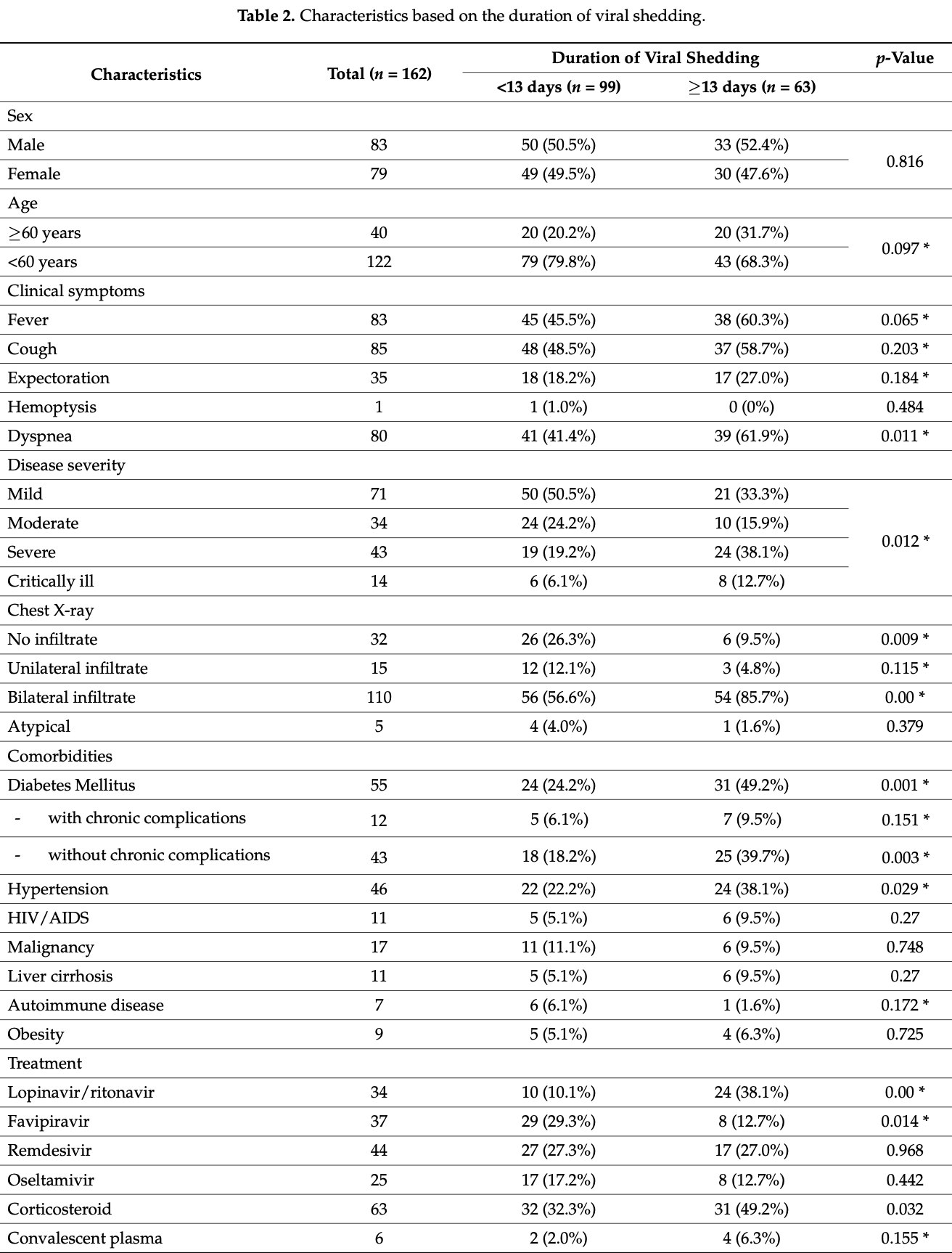
Retrospective 162 hospitalized COVID-19 patients in Indonesia, showing lower incidence of delayed viral clearance with favipiravir treatment in unadjusted results.
Potential risks of favipiravir include kidney injury1-3, liver injury2-5, cardiovascular events5,6, pulmonary toxicity6,7, and mutagenicity, carcinogenicity, teratogenicity, embryotoxicity, and the creation of dangerous variants8-14.
This study is excluded in the after exclusion results of meta-analysis:
unadjusted results with no group details.
Study covers remdesivir and favipiravir.
|
delayed viral clearance, 50.9% lower, RR 0.49, p = 0.02, treatment 8 of 37 (21.6%), control 55 of 125 (44.0%), NNT 4.5.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
1.
Abdulaziz et al., Clinical Features and Prognosis of Acute Kidney Injury in Hospital-Admitted Patients with COVID-19 in Egypt: A Single-Center Experience, Mansoura Medical Journal, doi:10.58775/2735-3990.1433.
2.
Ülger et al., Experimental evaluation of favipiravir (T-705)-induced liver and kidney toxicity in rats, Food and Chemical Toxicology, doi:10.1016/j.fct.2025.115472.
3.
El-Fetouh et al., Experimental Studies on Some Drugs Used in Covid-19 Treatment (Favipiravir and Dexamethasone) in Albino Rats, Journal of Advanced Veterinary Research, 13:10, www.advetresearch.com/index.php/AVR/article/view/1635.
4.
Almutairi et al., Liver Injury in Favipiravir-Treated COVID-19 Patients: Retrospective Single-Center Cohort Study, Tropical Medicine and Infectious Disease, doi:10.3390/tropicalmed8020129.
5.
Siby et al., Temporal Trends in Serious Adverse Events Associated with Oral Antivirals During the COVID-19 Pandemic: Insights from the FAERS Database (2020–2023), Open Forum Infectious Diseases, doi:10.1093/ofid/ofaf695.1825.
6.
Ozhan et al., Evaluation of the cardiopulmonary effects of repurposed COVID-19 therapeutics in healthy rats, Scientific Reports, doi:10.1038/s41598-025-31048-4.
7.
Ülger (B) et al., Evaluation of the effects of favipiravir (T-705) on the lung tissue of healty rats: An experimental study, Food and Chemical Toxicology, doi:10.1016/j.fct.2025.115235.
8.
Zhirnov et al., Favipiravir: the hidden threat of mutagenic action, Journal of microbiology, epidemiology and immunobiology, doi:10.36233/0372-9311-114.
9.
Waters et al., Human genetic risk of treatment with antiviral nucleoside analog drugs that induce lethal mutagenesis: the special case of molnupiravir, Environmental and Molecular Mutagenesis, doi:10.1002/em.22471.
10.
Hadj Hassine et al., Lethal Mutagenesis of RNA Viruses and Approved Drugs with Antiviral Mutagenic Activity, Viruses, doi:10.3390/v14040841.
11.
Shum, C., An investigational study into the drug-associated mutational signature in SARS-CoV-2 viruses, The University of Hong Kong, PhD Thesis, hub.hku.hk/handle/10722/344396.
12.
Shiraki et al., Convenient screening of the reproductive toxicity of favipiravir and antiviral drugs in Caenorhabditis elegans, Heliyon, doi:10.1016/j.heliyon.2024.e35331.
Arfijanto et al., 4 May 2023, retrospective, Indonesia, peer-reviewed, 8 authors, study period June 2021 - December 2021.
Contact: tpasmarawati@fk.unair.ac.id (corresponding author).
Duration of SARS-CoV-2 RNA Shedding Is Significantly Influenced by Disease Severity, Bilateral Pulmonary Infiltrates, Antibiotic Treatment, and Diabetic Status: Consideration for Isolation Period
Pathophysiology, doi:10.3390/pathophysiology30020016
Severe acute respiratory syndrome coronavirus type 2 (SARS-CoV-2) ribonucleic acid (RNA) shedding is an important parameter for determining the optimal length of isolation period required for coronavirus disease 2019 (COVID-19) patients. However, the clinical (i.e., patient and disease) characteristics that could influence this parameter have yet to be determined. In this study, we aim to explore the potential associations between several clinical features and the duration of SARS-CoV-2 RNA shedding in patients hospitalized with COVID-19. A retrospective cohort study involving 162 patients hospitalized for COVID-19 in a tertiary referral teaching hospital in Indonesia was performed from June to December 2021. Patients were grouped based on the mean duration of viral shedding and were compared based on several clinical characteristics (e.g., age, sex, comorbidities, COVID-19 symptoms, severity, and therapies). Subsequently, clinical factors potentially associated with the duration of SARS-CoV-2 RNA shedding were further assessed using multivariate logistic regression analysis. As a result, the mean duration of SARS-CoV-2 RNA shedding was found to be 13 ± 8.44 days. In patients with diabetes mellitus (without chronic complications) or hypertension, the duration of viral shedding was significantly prolonged (≥13 days; p = 0.001 and p = 0.029, respectively). Furthermore, patients with dyspnea displayed viral shedding for longer durations (p = 0.011). The multivariate logistic regression analysis reveals that independent risk factors associated with the duration of SARS-CoV-2 RNA shedding include disease severity (adjusted odds ratio [aOR] = 2.94; 95% CI = 1.36-6.44), bilateral lung infiltrates (aOR = 2.79; 95% CI = 1.14-6.84), diabetes mellitus (aOR = 2.17; 95% CI = 1.02-4.63), and antibiotic treatment (aOR = 3.66; 95% CI = 1.74-7.71). In summary, several clinical factors are linked with the duration of SARS-CoV-2 RNA shedding. Disease severity is positively associated with the duration of viral shedding, while bilateral lung infiltrates, diabetes mellitus, and antibiotic treatment are negatively linked with the duration of viral shedding. Overall, our findings suggest the need to consider different isolation period estimations for specific clinical characteristics of patients with COVID-19 that affect the duration of SARS-CoV-2 RNA shedding.
Conflicts of Interest: The authors declare no conflict of interest.
References
Aghili, Ebrahimpur, Arjmand, Shadman, Pejman Sani et al., Obesity in COVID-19 era, implications for mechanisms, comorbidities, and prognosis: A review and meta-analysis, Int. J. Obes, doi:10.1038/s41366-021-00776-8
Aly, Rahman, Ahmed, Alghamedi, Al Shehri et al., Indicators of Critical Illness and Predictors of Mortality in COVID-19 Patients, Infect. Drug Resist, doi:10.2147/IDR.S261159
Askanase, Khalili, Buyon, Thoughts on COVID-19 and autoimmune diseases, Lupus Sci. Med, doi:10.1136/lupus-2020-000396
Asmarawati, Rosyid, Suryantoro, Mahdi, Windradi et al., The clinical impact of bacterial co-infection among moderate, severe and critically ill COVID-19 patients in the second referral hospital in Surabaya, doi:10.12688/f1000research.31645.1
Asmarawati, Suryantoro, Rosyid, Marfiani, Windradi et al., Predictive Value of Sequential Organ Failure Assessment, Quick Sequential Organ Failure Assessment, Acute Physiology and Chronic Health Evaluation II, and New Early Warning Signs Scores Estimate Mortality of COVID-19 Patients Requiring Intensive Care Unit, Indian J. Crit. Care Med, doi:10.5005/jp-journals-10071-24170
Bitker, Dhelft, Chauvelot, Frobert, Folliet et al., Protracted viral shedding and viral load are associated with ICU mortality in Covid-19 patients with acute respiratory failure, Ann. Intensiv. Care, doi:10.1186/s13613-020-00783-4
Buetti, Trimboli, Mazzuchelli, Priore, Balmelli et al., Diabetes mellitus is a risk factor for prolonged SARS-CoV-2 viral shedding in lower respiratory tract samples of critically ill patients, Endocrine, doi:10.1007/s12020-020-02465-4
Burhan, Susanto, Isbaniah, Sally, Eka et al., Pedoman Tatalaksana COVID-19
Chen, Tsai, Yu, Cheng, Yeh, Prolonged viral shedding and new mutations of COVID-19 could complicate the control of the pandemic, doi:10.1099/acmi.0.000133
Codo, Davanzo, De Brito Monteiro, De Souza, Muraro et al., Elevated Glucose Levels Favor SARS-CoV-2 Infection and Monocyte Response through a HIF-1α/Glycolysis-Dependent Axis, Cell Metab, doi:10.1016/j.cmet.2020.07.007
Cunha, Vilela, Molina, Acuna, Muxel et al., Atypical Prolonged Viral Shedding With Intra-Host SARS-CoV-2 Evolution in a Mildly Affected Symptomatic Patient, Front. Med, doi:10.3389/fmed.2021.760170
De Leeuw, Oude Luttikhuis, Wellen, Müller, Calkhoven, Obesity and its impact on COVID-19, J. Mol. Med, doi:10.1007/s00109-021-02072-4
Feng, Li, Yao, Yu, Zhou et al., Clinical Factors Associated with Progression and Prolonged Viral Shedding in COVID-19 Patients: A Multicenter Study, Aging Dis, doi:10.14336/AD.2020.0630
Fu, Han, Zhu, Bai, Yi et al., Risk factors for viral RNA shedding in COVID-19 patients, Eur. Respir. J, doi:10.1183/13993003.01190-2020
Karia, Nagraj, A Review of Viral Shedding in Resolved and Convalescent COVID-19 Patients. SN Compr, Clin. Med, doi:10.1007/s42399-020-00499-3
Langford, So, Raybardhan, Leung, Westwood et al., Bacterial co-infection and secondary infection in patients with COVID-19: A living rapid review and meta-analysis, Clin. Microbiol. Infect, doi:10.1016/j.cmi.2020.07.016
Leung, Chorlton, Tyson, Al-Rawahi, Jassem et al., COVID-19 in an immunocompromised host: Persistent shedding of viable SARS-CoV-2 and emergence of multiple mutations: A case report, Int. J. Infect. Dis, doi:10.1016/j.ijid.2021.10.045
Li, Cao, Chen, Cai, Zhang et al., Duration of SARS-CoV-2 RNA shedding and factors associated with prolonged viral shedding in patients with COVID-19, J. Med. Virol
Menghua, Xin, Jianwei, Yu, Qinwei, Case report: One case of coronavirus disease 2019 (COVID-19) in a patient co-infected by HIV with a normal CD4+ T cell count, AIDS Res. Ther, doi:10.1186/s12981-020-00301-3
Muhamad, Ugusman, Kumar, Skiba, Hamid et al., COVID-19 and Hypertension: The What, the Why, and the How, Front. Physiol, doi:10.3389/fphys.2021.665064
Nugroho, Suryantoro, Yuliasih, Rosyid, Asmarawati et al., Optimal use of tocilizumab for severe and critical COVID-19: A systematic review and meta-analysis, doi:10.12688/f1000research.45046.1
Pradhan, Olsson, Sex differences in severity and mortality from COVID-19: Are males more vulnerable?, Biol. Sex Differ, doi:10.1186/s13293-020-00330-7
Qi, Yang, Jiang, Tu, Wan et al., Factors associated with the duration of viral shedding in adults with COVID-19 outside of Wuhan, China: A retrospective cohort study, Int. J. Infect. Dis, doi:10.1016/j.ijid.2020.05.045
Ryoo, Kim, Sohn, Seo, Oh et al., Factors promoting the prolonged shedding of the pandemic (H1N1) 2009 influenza virus in patients treated with oseltamivir for 5 days, Influenza Other Respir. Viruses, doi:10.1111/irv.12065
Soegiarto, Wulandari, Purnomosari, Dhia Fahmita, Ikhwan Gautama et al., Hypertension is asso-ciated with antibody response and breakthrough infection in health care workers following vaccination with inactivated SARS-CoV-2, Vaccine, doi:10.1016/j.vaccine.2022.05.059
Wang, Zhang, Sang, Ye, Ruan et al., Kinetics of viral load and antibody response in relation to COVID-19 severity, J. Clin. Investig, doi:10.1172/JCI138759
Wibisono, Hadi, Bramantono Arfijanto, Rusli, Rahman et al., National early warning score (NEWS) 2 predicts hospital mortality from COVID-19 patients, Ann. Med. Surg, doi:10.1016/j.amsu.2022.103462
Xu, Chen, Yuan, Yi, Ding et al., Factors Associated With Prolonged Viral RNA Shedding in Patients with Coronavirus Disease 2019 (COVID-19), Clin. Infect. Dis, doi:10.1093/cid/ciaa351
Yousaf, Hameed, Alsoub, Khatib, Jamal et al., COVID-19: Prolonged viral shedding in an HIV patient with literature review of risk factors for prolonged viral shedding and its implications for isolation strategies, Clin. Case Rep, doi:10.1002/ccr3.3786
Zhang, Hu, Luo, Fang, Chen et al., Clinical features and short-term outcomes of 221 patients with COVID-19 in Wuhan, China. J. Clin. Virol, doi:10.1016/j.jcv.2020.104364
Zhang, Zhu, Ye, Hu, Zheng et al., Risk factors for prolonged virus shedding of respiratory tract and fecal in adults with severe acute respiratory syndrome coronavirus-2 infection, J. Clin. Lab. Anal, doi:10.1002/jcla.23923
Zhou, She, Wang, Ma, Duration of Viral Shedding of Discharged Patients With Severe COVID-19, Clin. Infect. Dis, doi:10.1093/cid/ciaa451
Zhou, Yu, Du, Fan, Liu et al., Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan
Zhou, Zhang, Ren, Sun, Yu et al., Impact of age on duration of viral RNA shedding in patients with COVID-19, Aging, doi:10.18632/aging.104114
DOI record:
{
"DOI": "10.3390/pathophysiology30020016",
"ISSN": [
"1873-149X"
],
"URL": "http://dx.doi.org/10.3390/pathophysiology30020016",
"abstract": "<jats:p>Severe acute respiratory syndrome coronavirus type 2 (SARS-CoV-2) ribonucleic acid (RNA) shedding is an important parameter for determining the optimal length of isolation period required for coronavirus disease 2019 (COVID-19) patients. However, the clinical (i.e., patient and disease) characteristics that could influence this parameter have yet to be determined. In this study, we aim to explore the potential associations between several clinical features and the duration of SARS-CoV-2 RNA shedding in patients hospitalized with COVID-19. A retrospective cohort study involving 162 patients hospitalized for COVID-19 in a tertiary referral teaching hospital in Indonesia was performed from June to December 2021. Patients were grouped based on the mean duration of viral shedding and were compared based on several clinical characteristics (e.g., age, sex, comorbidities, COVID-19 symptoms, severity, and therapies). Subsequently, clinical factors potentially associated with the duration of SARS-CoV-2 RNA shedding were further assessed using multivariate logistic regression analysis. As a result, the mean duration of SARS-CoV-2 RNA shedding was found to be 13 ± 8.44 days. In patients with diabetes mellitus (without chronic complications) or hypertension, the duration of viral shedding was significantly prolonged (≥13 days; p = 0.001 and p = 0.029, respectively). Furthermore, patients with dyspnea displayed viral shedding for longer durations (p = 0.011). The multivariate logistic regression analysis reveals that independent risk factors associated with the duration of SARS-CoV-2 RNA shedding include disease severity (adjusted odds ratio [aOR] = 2.94; 95% CI = 1.36–6.44), bilateral lung infiltrates (aOR = 2.79; 95% CI = 1.14–6.84), diabetes mellitus (aOR = 2.17; 95% CI = 1.02–4.63), and antibiotic treatment (aOR = 3.66; 95% CI = 1.74–7.71). In summary, several clinical factors are linked with the duration of SARS-CoV-2 RNA shedding. Disease severity is positively associated with the duration of viral shedding, while bilateral lung infiltrates, diabetes mellitus, and antibiotic treatment are negatively linked with the duration of viral shedding. Overall, our findings suggest the need to consider different isolation period estimations for specific clinical characteristics of patients with COVID-19 that affect the duration of SARS-CoV-2 RNA shedding.</jats:p>",
"alternative-id": [
"pathophysiology30020016"
],
"author": [
{
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
}
],
"family": "Arfijanto",
"given": "Muhammad Vitanata",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0001-9869-5098",
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
},
{
"name": "Universitas Airlangga Hospital, Airlangga University, Surabaya 60115, Indonesia"
}
],
"authenticated-orcid": false,
"family": "Asmarawati",
"given": "Tri Pudy",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
}
],
"family": "Bramantono",
"given": "Bramantono",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-4834-2259",
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
}
],
"authenticated-orcid": false,
"family": "Rusli",
"given": "Musofa",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
},
{
"name": "Universitas Airlangga Hospital, Airlangga University, Surabaya 60115, Indonesia"
}
],
"family": "Rachman",
"given": "Brian Eka",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-6634-6088",
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
}
],
"authenticated-orcid": false,
"family": "Mahdi",
"given": "Bagus Aulia",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
},
{
"name": "Universitas Airlangga Hospital, Airlangga University, Surabaya 60115, Indonesia"
}
],
"family": "Nasronudin",
"given": "Nasronudin",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine, Faculty of Medicine, Airlangga University, Surabaya 60132, Indonesia"
}
],
"family": "Hadi",
"given": "Usman",
"sequence": "additional"
}
],
"container-title": "Pathophysiology",
"container-title-short": "Pathophysiology",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
5,
5
]
],
"date-time": "2023-05-05T08:55:50Z",
"timestamp": 1683276950000
},
"deposited": {
"date-parts": [
[
2023,
5,
5
]
],
"date-time": "2023-05-05T09:45:35Z",
"timestamp": 1683279935000
},
"indexed": {
"date-parts": [
[
2023,
5,
6
]
],
"date-time": "2023-05-06T04:26:27Z",
"timestamp": 1683347187963
},
"is-referenced-by-count": 0,
"issue": "2",
"issued": {
"date-parts": [
[
2023,
5,
4
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2023,
6
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
5,
4
]
],
"date-time": "2023-05-04T00:00:00Z",
"timestamp": 1683158400000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/1873-149X/30/2/16/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "186-198",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2023,
5,
4
]
]
},
"published-online": {
"date-parts": [
[
2023,
5,
4
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"key": "ref_1",
"unstructured": "(2023, March 01). Weekly Epidemiological Update on COVID-19—1 March 2023. Available online: https://www.who.int/publications/m/item/weekly-epidemiological-update-on-covid-19---1-march-2023."
},
{
"key": "ref_2",
"unstructured": "(2023, March 12). Infeksi Emerging Kementerian Kesehatan RI. Available online: https://infeksiemerging.kemkes.go.id/dashboard/covid-19."
},
{
"DOI": "10.1002/jmv.26280",
"article-title": "Duration of SARS-CoV-2 RNA shedding and factors associated with prolonged viral shedding in patients with COVID-19",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "506",
"journal-title": "J. Med. Virol.",
"key": "ref_3",
"volume": "93",
"year": "2020"
},
{
"DOI": "10.1093/cid/ciaa451",
"article-title": "Duration of Viral Shedding of Discharged Patients With Severe COVID-19",
"author": "Zhou",
"doi-asserted-by": "crossref",
"first-page": "2240",
"journal-title": "Clin. Infect. Dis.",
"key": "ref_4",
"volume": "71",
"year": "2020"
},
{
"DOI": "10.1172/JCI138759",
"article-title": "Kinetics of viral load and antibody response in relation to COVID-19 severity",
"author": "Wang",
"doi-asserted-by": "crossref",
"first-page": "5235",
"journal-title": "J. Clin. Investig.",
"key": "ref_5",
"volume": "130",
"year": "2020"
},
{
"DOI": "10.1183/13993003.01190-2020",
"article-title": "Risk factors for viral RNA shedding in COVID-19 patients",
"author": "Fu",
"doi-asserted-by": "crossref",
"first-page": "2001190",
"journal-title": "Eur. Respir. J.",
"key": "ref_6",
"volume": "56",
"year": "2020"
},
{
"DOI": "10.1007/s42399-020-00499-3",
"article-title": "A Review of Viral Shedding in Resolved and Convalescent COVID-19 Patients",
"author": "Karia",
"doi-asserted-by": "crossref",
"first-page": "2086",
"journal-title": "SN Compr. Clin. Med.",
"key": "ref_7",
"volume": "2",
"year": "2020"
},
{
"DOI": "10.1016/j.ijid.2021.10.045",
"article-title": "COVID-19 in an immunocompromised host: Persistent shedding of viable SARS-CoV-2 and emergence of multiple mutations: A case report",
"author": "Leung",
"doi-asserted-by": "crossref",
"first-page": "178",
"journal-title": "Int. J. Infect. Dis.",
"key": "ref_8",
"volume": "114",
"year": "2021"
},
{
"DOI": "10.1099/acmi.0.000133",
"article-title": "Prolonged viral shedding and new mutations of COVID-19 could complicate the control of the pandemic",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "acmi000133",
"journal-title": "Access Microbiol.",
"key": "ref_9",
"volume": "2",
"year": "2020"
},
{
"DOI": "10.1016/j.amsu.2022.103462",
"article-title": "National early warning score (NEWS) 2 predicts hospital mortality from COVID-19 patients",
"author": "Wibisono",
"doi-asserted-by": "crossref",
"first-page": "103462",
"journal-title": "Ann. Med. Surg.",
"key": "ref_10",
"volume": "76",
"year": "2022"
},
{
"DOI": "10.12688/f1000research.45046.1",
"article-title": "Optimal use of tocilizumab for severe and critical COVID-19: A systematic review and meta-analysis",
"author": "Nugroho",
"doi-asserted-by": "crossref",
"first-page": "73",
"journal-title": "F1000Research",
"key": "ref_11",
"volume": "10",
"year": "2021"
},
{
"DOI": "10.1016/j.vaccine.2022.05.059",
"article-title": "Hypertension is asso-ciated with antibody response and breakthrough infection in health care workers following vaccination with inactivated SARS-CoV-2",
"author": "Soegiarto",
"doi-asserted-by": "crossref",
"first-page": "4046",
"journal-title": "Vaccine",
"key": "ref_12",
"volume": "40",
"year": "2022"
},
{
"DOI": "10.5005/jp-journals-10071-24170",
"article-title": "Predictive Value of Sequential Organ Failure Assessment, Quick Sequential Organ Failure Assessment, Acute Physiology and Chronic Health Evaluation II, and New Early Warning Signs Scores Estimate Mortality of COVID-19 Patients Requiring Intensive Care Unit",
"author": "Asmarawati",
"doi-asserted-by": "crossref",
"first-page": "466",
"journal-title": "Indian J. Crit. Care Med.",
"key": "ref_13",
"volume": "26",
"year": "2022"
},
{
"DOI": "10.12688/f1000research.31645.1",
"article-title": "The clinical impact of bacterial co-infection among moderate, severe and critically ill COVID-19 patients in the second referral hospital in Surabaya",
"author": "Asmarawati",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "F1000Research",
"key": "ref_14",
"volume": "10",
"year": "2021"
},
{
"key": "ref_15",
"unstructured": "Burhan, E., Susanto, A.D., Isbaniah, F., Sally, A.N., Eka, G., Ceva, W.P., Susilo, A., Firdaus, I., Santoso, A., and Juzar, D.A. (2020). Pedoman Tatalaksana COVID-19, IDAI. [3rd ed.]."
},
{
"DOI": "10.1016/j.ijid.2020.05.045",
"article-title": "Factors associated with the duration of viral shedding in adults with COVID-19 outside of Wuhan, China: A retrospective cohort study",
"author": "Qi",
"doi-asserted-by": "crossref",
"first-page": "531",
"journal-title": "Int. J. Infect. Dis.",
"key": "ref_16",
"volume": "96",
"year": "2020"
},
{
"DOI": "10.1093/cid/ciaa351",
"article-title": "Factors Associated With Prolonged Viral RNA Shedding in Patients with Coronavirus Disease 2019 (COVID-19)",
"author": "Xu",
"doi-asserted-by": "crossref",
"first-page": "799",
"journal-title": "Clin. Infect. Dis.",
"key": "ref_17",
"volume": "71",
"year": "2020"
},
{
"DOI": "10.14336/AD.2020.0630",
"article-title": "Clinical Factors Associated with Progression and Prolonged Viral Shedding in COVID-19 Patients: A Multicenter Study",
"author": "Feng",
"doi-asserted-by": "crossref",
"first-page": "1069",
"journal-title": "Aging Dis.",
"key": "ref_18",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30566-3",
"article-title": "Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study",
"author": "Zhou",
"doi-asserted-by": "crossref",
"first-page": "1054",
"journal-title": "Lancet",
"key": "ref_19",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.2147/IDR.S261159",
"article-title": "Indicators of Critical Illness and Predictors of Mortality in COVID-19 Patients",
"author": "Aly",
"doi-asserted-by": "crossref",
"first-page": "1995",
"journal-title": "Infect. Drug Resist.",
"key": "ref_20",
"volume": "13",
"year": "2020"
},
{
"DOI": "10.1016/j.jcv.2020.104364",
"article-title": "Clinical features and short-term outcomes of 221 patients with COVID-19 in Wuhan, China",
"author": "Zhang",
"doi-asserted-by": "crossref",
"first-page": "104364",
"journal-title": "J. Clin. Virol.",
"key": "ref_21",
"volume": "127",
"year": "2020"
},
{
"article-title": "Impact of age on duration of viral RNA shedding in patients with COVID-19",
"author": "Zhou",
"first-page": "22399",
"journal-title": "Aging",
"key": "ref_22",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1186/s13293-020-00330-7",
"article-title": "Sex differences in severity and mortality from COVID-19: Are males more vulnerable?",
"author": "Pradhan",
"doi-asserted-by": "crossref",
"first-page": "53",
"journal-title": "Biol. Sex Differ.",
"key": "ref_23",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.3389/fphys.2021.665064",
"article-title": "COVID-19 and Hypertension: The What, the Why, and the How",
"author": "Muhamad",
"doi-asserted-by": "crossref",
"first-page": "665064",
"journal-title": "Front. Physiol.",
"key": "ref_24",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1007/s12020-020-02465-4",
"article-title": "Diabetes mellitus is a risk factor for prolonged SARS-CoV-2 viral shedding in lower respiratory tract samples of critically ill patients",
"author": "Buetti",
"doi-asserted-by": "crossref",
"first-page": "454",
"journal-title": "Endocrine",
"key": "ref_25",
"volume": "70",
"year": "2020"
},
{
"DOI": "10.1016/j.cmet.2020.07.007",
"article-title": "Elevated Glucose Levels Favor SARS-CoV-2 Infection and Monocyte Response through a HIF-1α/Glycolysis-Dependent Axis",
"author": "Codo",
"doi-asserted-by": "crossref",
"first-page": "437",
"journal-title": "Cell Metab.",
"key": "ref_26",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1002/jcla.23923",
"article-title": "Risk factors for prolonged virus shedding of respiratory tract and fecal in adults with severe acute respiratory syndrome coronavirus-2 infection",
"author": "Zhang",
"doi-asserted-by": "crossref",
"first-page": "e23923",
"journal-title": "J. Clin. Lab. Anal.",
"key": "ref_27",
"volume": "35",
"year": "2021"
},
{
"DOI": "10.3389/fmed.2021.760170",
"article-title": "Atypical Prolonged Viral Shedding With Intra-Host SARS-CoV-2 Evolution in a Mildly Affected Symptomatic Patient",
"author": "Cunha",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Front. Med.",
"key": "ref_28",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.1186/s12981-020-00301-3",
"article-title": "Case report: One case of coronavirus disease 2019 (COVID-19) in a patient co-infected by HIV with a normal CD4+ T cell count",
"author": "Menghua",
"doi-asserted-by": "crossref",
"first-page": "46",
"journal-title": "AIDS Res. Ther.",
"key": "ref_29",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1002/ccr3.3786",
"article-title": "COVID-19: Prolonged viral shedding in an HIV patient with literature review of risk factors for prolonged viral shedding and its implications for isolation strategies",
"author": "Yousaf",
"doi-asserted-by": "crossref",
"first-page": "1397",
"journal-title": "Clin. Case Rep.",
"key": "ref_30",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1136/lupus-2020-000396",
"article-title": "Thoughts on COVID-19 and autoimmune diseases",
"author": "Askanase",
"doi-asserted-by": "crossref",
"first-page": "e000396",
"journal-title": "Lupus Sci. Med.",
"key": "ref_31",
"volume": "7",
"year": "2020"
},
{
"DOI": "10.1038/s41366-021-00776-8",
"article-title": "Obesity in COVID-19 era, implications for mechanisms, comorbidities, and prognosis: A review and meta-analysis",
"author": "Aghili",
"doi-asserted-by": "crossref",
"first-page": "998",
"journal-title": "Int. J. Obes.",
"key": "ref_32",
"volume": "45",
"year": "2021"
},
{
"DOI": "10.1007/s00109-021-02072-4",
"article-title": "Obesity and its impact on COVID-19",
"author": "Wellen",
"doi-asserted-by": "crossref",
"first-page": "899",
"journal-title": "J. Mol. Med.",
"key": "ref_33",
"volume": "99",
"year": "2021"
},
{
"DOI": "10.1186/s13613-020-00783-4",
"article-title": "Protracted viral shedding and viral load are associated with ICU mortality in Covid-19 patients with acute respiratory failure",
"author": "Bitker",
"doi-asserted-by": "crossref",
"first-page": "167",
"journal-title": "Ann. Intensiv. Care",
"key": "ref_34",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1111/irv.12065",
"article-title": "Factors promoting the prolonged shedding of the pandemic (H1N1) 2009 influenza virus in patients treated with oseltamivir for 5 days",
"author": "Ryoo",
"doi-asserted-by": "crossref",
"first-page": "833",
"journal-title": "Influenza Other Respir. Viruses",
"key": "ref_35",
"volume": "7",
"year": "2012"
},
{
"DOI": "10.1016/j.cmi.2020.07.016",
"article-title": "Bacterial co-infection and secondary infection in patients with COVID-19: A living rapid review and meta-analysis",
"author": "Langford",
"doi-asserted-by": "crossref",
"first-page": "1622",
"journal-title": "Clin. Microbiol. Infect.",
"key": "ref_36",
"volume": "26",
"year": "2020"
}
],
"reference-count": 36,
"references-count": 36,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/1873-149X/30/2/16"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Duration of SARS-CoV-2 RNA Shedding Is Significantly Influenced by Disease Severity, Bilateral Pulmonary Infiltrates, Antibiotic Treatment, and Diabetic Status: Consideration for Isolation Period",
"type": "journal-article",
"volume": "30"
}