COVID-19 Disease Severity and Death in Relation to Vitamin D Status among SARS-CoV-2-Positive UAE Residents
et al., Nutrients, doi:10.3390/nu13051714, May 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 464 patients in United Arab Emirates showing low D levels at first hospital visit associated with higher COVID-19 severity and mortality.
This is the 66th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
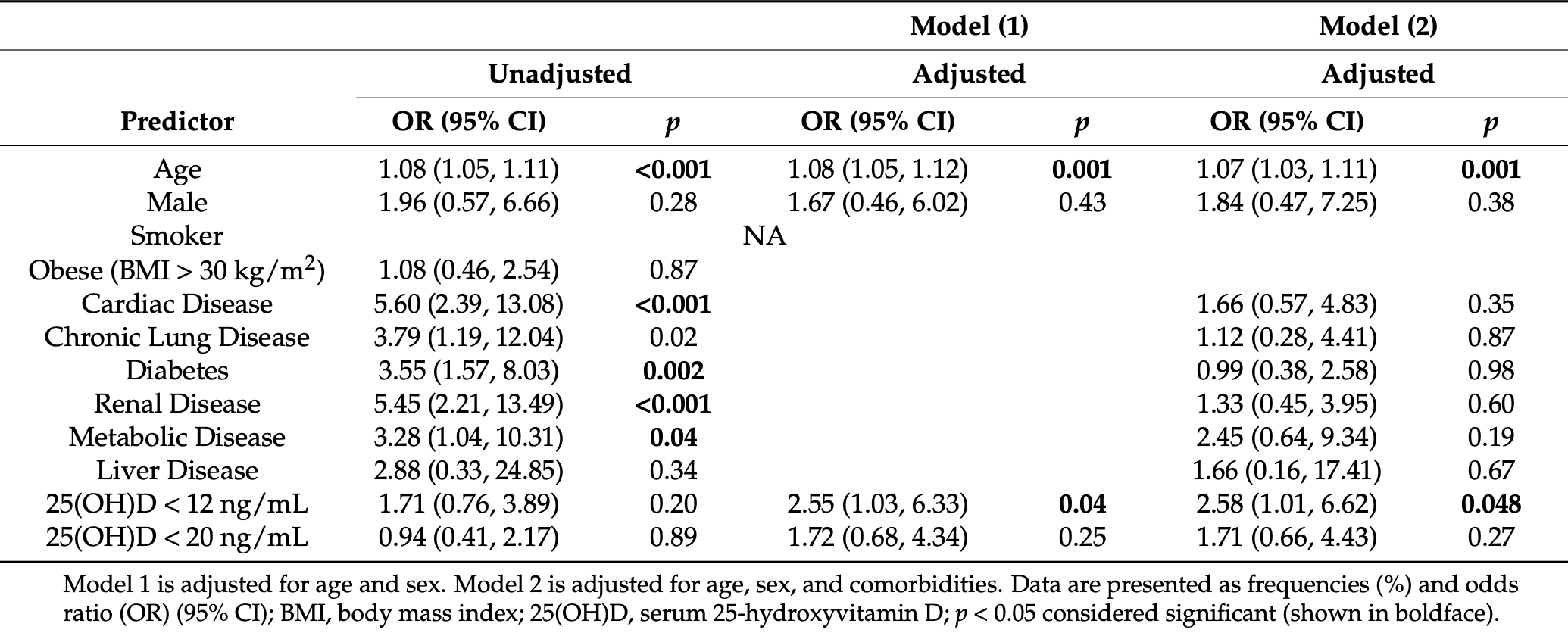
risk of death, 59.3% lower, RR 0.41, p = 0.048, high D levels 16 of 337 (4.7%), low D levels 10 of 127 (7.9%), adjusted per study, inverted to make RR<1 favor high D levels, odds ratio converted to relative risk, ≥12ng/mL.
|
|
risk of severe case, 33.2% lower, RR 0.67, p = 0.005, high D levels 337, low D levels 127, adjusted per study, inverted to make RR<1 favor high D levels, odds ratio converted to relative risk, ≥12ng/mL.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
AlSafar et al., 19 May 2021, retrospective, United Arab Emirates, peer-reviewed, 8 authors.
COVID-19 Disease Severity and Death in Relation to Vitamin D Status among SARS-CoV-2-Positive UAE Residents
Nutrients, doi:10.3390/nu13051714
Insufficient blood levels of the neurohormone vitamin D are associated with increased risk of COVID-19 severity and mortality. Despite the global rollout of vaccinations and promising preliminary results, the focus remains on additional preventive measures to manage COVID-19. Results conflict on vitamin D's plausible role in preventing and treating COVID-19. We examined the relation between vitamin D status and COVID-19 severity and mortality among the multiethnic population of the United Arab Emirates. Our observational study used data for 522 participants who tested positive for SARS-CoV-2 at one of the main hospitals in Abu Dhabi and Dubai. Only 464 of those patients were included for data analysis. Demographic and clinical data were retrospectively analyzed. Serum samples immediately drawn at the first hospital visit were used to measure serum 25-hydroxyvitamin D [25(OH)D] concentrations through automated electrochemiluminescence. Levels < 12 ng/mL were significantly associated with higher risk of severe COVID-19 infection and of death. Age was the only other independent risk factor, whereas comorbidities and smoking did not contribute to the outcomes upon adjustment. Sex of patients was not an important predictor for severity or death. Our study is the first conducted in the UAE to measure 25(OH)D levels in SARS-CoV-2-positive patients and confirm the association of levels < 12 ng/mL with COVID-19 severity and mortality.
References
Abdul-Cader, Amarasinghe, Abdul-Careem, Activation of toll-like receptor signaling pathways leading to nitric oxide-mediated antiviral responses, Arch. Virol, doi:10.1007/s00705-016-2904-x
Abrishami, Dalili, Torbati, Asgari, Arab-Ahmadi et al., Possible association of vitamin D status with lung involvement and outcome in patients with COVID-19: A retrospective study, Eur. J. Nutr, doi:10.1007/s00394-020-02411-0
Al-Daghri, Amer, Alotaibi, Aldisi, Enani et al., Vitamin D status of Arab Gulf residents screened for SARS-CoV-2 and its association with COVID-19 infection: A multi-centre case-control study, J. Transl. Med, doi:10.1186/s12967-021-02838-x
Alanouti, Thomas, Abdel-Wareth, Rajah, Grant et al., Vitamin D deficiency and sun avoidance among university students at Abu Dhabi, United Arab Emirates, Dermato-Endocrinol, doi:10.4161/derm.3.4.16881
Alguwaihes, Sabico, Hasanato, Al-Sofiani, Megdad et al., Severe vitamin D deficiency is not related to SARS-CoV-2 infection but may increase mortality risk in hospitalized adults: A retrospective case-control study in an Arab Gulf country, Aging Clin. Exp. Res, doi:10.1007/s40520-021-01831-0
Andrukhova, Slavic, Zeitz, Riesen, Heppelmann et al., Vitamin D Is a Regulator of Endothelial Nitric Oxide Synthase and Arterial Stiffness in Mice, Mol. Endocrinol, doi:10.1210/me.2013-1252
Bayramo Glu, Akkoç, Gbaş, Akgün, Yurdakul et al., The association between vitamin D levels and the clinical severity and inflammation markers in pediatric COVID-19 patients: Single-center experience from a pandemic hospital, Eur. J. Nucl. Med. Mol. Imaging, doi:10.1007/s00431-021-04030-1
Beard, Bearden, Striker, Vitamin D and the anti-viral state, J. Clin. Virol, doi:10.1016/j.jcv.2010.12.006
Biesalski, Vitamin D deficiency and co-morbidities in COVID-19 patients-A fatal relationship?, NFS J, doi:10.1016/j.nfs.2020.06.001
Bordelon, Ghetu, Langan, Recognition and management of vitamin D deficiency, Am. Fam. Physician
Braun, Chang, Mahadevappa, Gibbons, Liu et al., Association of low serum 25-hydroxyvitamin D levels and mortality in the critically ill, Crit. Care Med, doi:10.1097/CCM.0b013e318206ccdf
Butt, Kurdowska, Allen, Acute Lung Injury: A Clinical and Molecular Review, Arch. Pathol. Lab. Med, doi:10.5858/arpa.2015-0519-RA
Castillo, Costa, Barrios, Díaz, Miranda et al., Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study, J. Steroid Biochem. Mol. Biol, doi:10.1016/j.jsbmb.2020.105751
Charoenngam, Shirvani, Reddy, Vodopivec, Apovian et al., Association of Vitamin D Status With Hospital Morbidity and Mortality in Adult Hospitalized Patients With COVID-19, Endocr. Pr, doi:10.1016/j.eprac.2021.02.013
Cohen, Complex systems dynamics in aging: New evidence, continuing questions, Biogerontology, doi:10.1007/s10522-015-9584-x
Dalamaga, Christodoulatos, Karampela, Vallianou, Apovian, Understanding the Co-Epidemic of Obesity and COVID-19: Current Evidence, Comparison with Previous Epidemics, Mechanisms, and Preventive and Therapeutic Perspectives, Curr. Obes. Rep, doi:10.1007/s13679-021-00436-y
Dastoli, Bennardo, Patruno, Nisticò, Are erythema multiforme and urticaria related to a better outcome of COVID-19?, Dermatol. Ther, doi:10.1111/dth.13681
Dattola, Silvestri, Bennardo, Passante, Scali et al., Role of Vitamins in Skin Health: A Systematic Review, Curr. Nutr. Rep, doi:10.1007/s13668-020-00322-4
De Haan, Groeneveld, De Geus, Egal, Struijs, Vitamin D deficiency as a risk factor for infection, sepsis and mortality in the critically ill: Systematic review and meta-analysis, Crit. Care, doi:10.1186/s13054-014-0660-4
Drincic, Armas, Van Diest, Heaney, Volumetric Dilution, Rather Than Sequestration Best Explains the Low Vitamin D Status of Obesity, Obesity, doi:10.1038/oby.2011.404
Ekiz, Pazarlı, Relationship between COVID-19 and obesity, Diabetes Metab. Syndr. Clin. Res. Rev, doi:10.1016/j.dsx.2020.05.047
Franceschi, Salvioli, Garagnani, De Eguileor, Monti et al., Immunobiography and the Heterogeneity of Immune Responses in the Elderly: A Focus on Inflammaging and Trained Immunity, Front. Immunol, doi:10.3389/fimmu.2017.00982
Fulop, Mcelhaney, Pawelec, Cohen, Morais et al., Inflammation and Immunosenescence, Frailty Aging
Fülöp, Dupuis, Witkowski, Larbi, The Role of Immunosenescence in the Development of Age-Related Diseases, Rev. Investig. Clin
Fülöp, Jr, Foris, Worum, Leövey, Age-dependent alterations of Fc gamma receptor-mediated effector functions of human polymorphonuclear leucocytes, Clin. Exp. Immunol
Glinsky, Tripartite combination of candidate pandemic mitigation agents: Vitamin D, quercetin, and estradiol manifest properties of medicinal agents for targeted mitigation of the COVID-19 pandemic defined by genomics-guided tracing of SARS-CoV-2 targets in human cells, Biomedicines
Gois, Ferreira, Olenski, Seguro, Vitamin D and Infectious Diseases: Simple Bystander or Contributing Factor?, Nutrients, doi:10.3390/nu9070651
Gombart, Pierre, Maggini, A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection, Nutrients, doi:10.3390/nu12010236
Goronzy, Fang, Cavanagh, Fengqin, Weyand, Naive T Cell Maintenance and Function in Human Aging, J. Immunol, doi:10.4049/jimmunol.1500046
Graham, Rapid COVID-19 vaccine development, Science, doi:10.1126/science.abb8923
Grant, Lahore, Mcdonnell, Baggerly, French et al., Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths, Nutrients, doi:10.3390/nu12040988
Gröber, Holick, The coronavirus disease (COVID-19)-A supportive approach with selected micronutrients, Int. J. Vitam. Nutr. Res, doi:10.1024/0300-9831/a000693
Guan, Seet, Kennedy, Does eNOS derived nitric oxide protect the young from severe COVID-19 complications?, Ageing Res. Rev, doi:10.1016/j.arr.2020.101201
Gunville, Mourani, Ginde, The role of vitamin D in prevention and treatment of infection, Inflamm. Allergy-Drug Targets, doi:10.2174/18715281113129990046
Hamer, Gale, Kivimäki, Batty, Overweight, obesity, and risk of hospitalization for COVID-19: A communitybased cohort study of adults in the United Kingdom, doi:10.1073/pnas.2011086117
Haq, Svobodová, Imran, Stanford, Razzaque, Vitamin D deficiency: A single centre analysis of patients from 136 countries, J. Steroid Biochem. Mol. Biol, doi:10.1016/j.jsbmb.2016.02.007
Hooper, Nápoles, Pérez-Stable, COVID-19 and Racial/Ethnic Disparities, JAMA, doi:10.1001/jama.2020.8598
Hossein-Nezhad, Holick, Vitamin D for Health: A Global Perspective
Hughes, Beasley, Pulmonary Manifestations of Acute Lung Injury: More Than Just Diffuse Alveolar Damage, Arch. Pathol. Lab. Med, doi:10.5858/arpa.2016-0342-RA
Hussein, Löndahl, Thuresson, Alsved, Al-Hunaiti et al., Indoor Model Simulation for COVID-19 Transport and Exposure, Int. J. Environ. Res. Public Health, doi:10.3390/ijerph18062927
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin. Exp. Res, doi:10.1007/s40520-020-01570-8
Jazwinski, Yashin, Aging and health-A systems biology perspective, Introduction. Interdiscip. Top. Gerontol
Kaufman, Niles, Kroll, Bi, Holick, SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels, PLoS ONE, doi:10.1371/journal.pone.0239252
Kazemi, Mohammadi, Aghababaee, Golzarand, Clark et al., Association of Vitamin D status with SARS-CoV-2 infection or COVID-19 severity: A systematic review and meta-analysis, Adv. Nutr, doi:10.1093/advances/nmab012
Kleinnijenhuis, Quintin, Preijers, Joosten, Ifrim et al., Bacille Calmette-Guerin induces NOD2-dependent nonspecific protection from reinfection via epigenetic reprogramming of monocytes, Proc. Natl. Acad. Sci, doi:10.1073/pnas.1202870109
Kuba, Imai, Penninger, Angiotensin-converting enzyme 2 in lung diseases, Curr. Opin. Pharmacol, doi:10.1016/j.coph.2006.03.001
Martineau, Jolliffe, Hooper, Greenberg, Aloia et al., Vitamin D supplementation to prevent acute respiratory tract infections: Systematic review and meta-analysis of individual participant data, BMJ, doi:10.1136/bmj.i6583
Mcdonnell, Baggerly, French, Baggerly, Garland et al., Breast cancer risk markedly lower with serum 25-hydroxyvitamin D concentrations ≥60 vs <20 ng/mL (150 vs 50 nmol/L): Pooled analysis of two randomized trials and a prospective cohort, PLoS ONE, doi:10.1371/journal.pone.0199265
Mercola, Grant, Wagner, Evidence Regarding Vitamin D and Risk of COVID-19 and Its Severity, Nutrients, doi:10.3390/nu12113361
Merzon, Tworowski, Gorohovski, Vinker, Cohen et al., Low plasma 25(OH) vitamin D level is associated with increased risk of COVID-19 infection: An Israeli population-based study, FEBS J, doi:10.1111/febs.15495
Mirhosseini, Vatanparast, Kimball, The Association between Serum 25(OH)D Status and Blood Pressure in Participants of a Community-Based Program Taking Vitamin D Supplements, Nutrients, doi:10.3390/nu9111244
Netea, Van Der Meer, Trained immunity: An ancient way of remembering, Cell Host Microbe, doi:10.1016/j.chom.2017.02.003
Palacios, Gonzalez, Is vitamin D deficiency a major global public health problem?, J. Steroid Biochem. Mol. Biol, doi:10.1016/j.jsbmb.2013.11.003
Pawelec, Does the human immune system ever really become "senescent, doi:10.12688/f1000research.11297.1
Pludowski, Holick, Grant, Konstantynowicz, Mascarenhas et al., Vitamin D supplementation guidelines, J. Steroid Biochem. Mol. Biol, doi:10.1016/j.jsbmb.2017.01.021
Rhodes, Subramanian, Laird, Kenny, Editorial: Low population mortality from COVID-19 in countries south of latitude 35 degrees North supports vitamin D as a factor determining severity, Aliment. Pharmacol. Ther, doi:10.1111/apt.15777
Rodríguez-Puertas, ACE2 activators for the treatment of COVID 19 patients, J. Med. Virol, doi:10.1002/jmv.25992
Rossetti, Martucci, Starchl, Amrein, Micronutrients in Sepsis and COVID-19: A Narrative Review on What We Have Learned and What We Want to Know in Future Trials, Medicina, doi:10.3390/medicina57050419
Saleh, Beshyah, Hussein, Almadani, Hassoun et al., Diagnosis and management of vitamin D deficiency in the Gulf Cooperative Council (GCC) countries: An expert consensus summary statement from the GCC vitamin D advisory board, Arch. Osteoporos, doi:10.1007/s11657-020-0709-8
Sasabe, Suzuki, Imanishi, Aiso, Activity of D-amino acid oxidase is widespread in the human central nervous system, Front. Synaptic Neurosci, doi:10.3389/fnsyn.2014.00014
Sattar, Mcinnes, Mcmurray, Obesity is a risk factor for severe COVID-19 infection: Multiple potential mechanisms, Circulation, doi:10.1161/CIRCULATIONAHA.120.047659
Science, Maguire, Russell, Smieja, Walter et al., Low serum 25-hydroxyvitamin D level and risk of upper respiratory tract infection in children and adolescents, Clin. Infect. Dis, doi:10.1093/cid/cit289
Simonnet, Chetboun, Poissy, Raverdy, Noulette et al., High prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation, Obesity, doi:10.1002/oby.22831
Smolders, Ouweland, Geven, Pickkers, Kox, Letter to the Editor: Vitamin D deficiency in COVID-19: Mixing up cause and consequence, Metab. Clin. Exp, doi:10.1016/j.metabol.2020.154434
Teymoori-Rad, Shokri, Salimi, Marashi, The interplay between vitamin D and viral infections, Rev. Med. Virol, doi:10.1002/rmv.2032
Thompson, Pandemic potential of 2019-nCoV, Lancet Infect. Dis, doi:10.1016/S1473-3099(20)30068-2
Van Der Weele, Principles of confounder selection, Eur. J. Epidemiol, doi:10.1007/s10654-019-00494-6
Watkins, Lemonovich, Salata, An update on the association of vitamin D deficiency with common infectious diseases, Can. J. Physiol. Pharmacol, doi:10.1139/cjpp-2014-0352
Weiss, Murdoch, Clinical course and mortality risk of severe COVID-19, Lancet, doi:10.1016/S0140-6736(20)30633-4
Weller, Wang, He, Maddux, Usvyat et al., Does Incident Solar Ultraviolet Radiation Lower Blood Pressure?, J. Am. Hear. Assoc, doi:10.1161/JAHA.119.013837
Wimalawansa, Global epidemic of coronavirus-Covid-19: What can we do to minimize risks, Eur. J. Biomed. Pharm. Sci
Xu, Larbi, Markers of T Cell Senescence in Humans, Int. J. Mol. Sci, doi:10.3390/ijms18081742
Xudong, Junzhu, Xingxiang, Furong, Yanrong, Age-and gender-related difference of ACE2 expression in rat lung, Life Sci, doi:10.1016/j.lfs.2005.09.038
Yanes, Gustafson, Weyand, Goronzy, Lymphocyte generation and population homeostasis throughout life, Semin. Hematol, doi:10.1053/j.seminhematol.2016.10.003
Zierer, Menni, Kastenmüller, Spector, Integration of 'omics' data in aging research: From biomarkers to systems biology, Aging Cell, doi:10.1111/acel.12386
Åkerström, Mousavi-Jazi, Klingström, Leijon, Lundkvist et al., Nitric Oxide Inhibits the Replication Cycle of Severe Acute Respiratory Syndrome Coronavirus, J. Virol, doi:10.1128/JVI.79.3.1966-1969.2005
DOI record:
{
"DOI": "10.3390/nu13051714",
"ISSN": [
"2072-6643"
],
"URL": "http://dx.doi.org/10.3390/nu13051714",
"abstract": "<jats:p>Insufficient blood levels of the neurohormone vitamin D are associated with increased risk of COVID-19 severity and mortality. Despite the global rollout of vaccinations and promising preliminary results, the focus remains on additional preventive measures to manage COVID-19. Results conflict on vitamin D’s plausible role in preventing and treating COVID-19. We examined the relation between vitamin D status and COVID-19 severity and mortality among the multiethnic population of the United Arab Emirates. Our observational study used data for 522 participants who tested positive for SARS-CoV-2 at one of the main hospitals in Abu Dhabi and Dubai. Only 464 of those patients were included for data analysis. Demographic and clinical data were retrospectively analyzed. Serum samples immediately drawn at the first hospital visit were used to measure serum 25-hydroxyvitamin D [25(OH)D] concentrations through automated electrochemiluminescence. Levels < 12 ng/mL were significantly associated with higher risk of severe COVID-19 infection and of death. Age was the only other independent risk factor, whereas comorbidities and smoking did not contribute to the outcomes upon adjustment. Sex of patients was not an important predictor for severity or death. Our study is the first conducted in the UAE to measure 25(OH)D levels in SARS-CoV-2-positive patients and confirm the association of levels < 12 ng/mL with COVID-19 severity and mortality.</jats:p>",
"alternative-id": [
"nu13051714"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0001-7141-1438",
"affiliation": [],
"authenticated-orcid": false,
"family": "AlSafar",
"given": "Habiba",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-1439-3285",
"affiliation": [],
"authenticated-orcid": false,
"family": "Grant",
"given": "William B.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-6895-9280",
"affiliation": [],
"authenticated-orcid": false,
"family": "Hijazi",
"given": "Rafiq",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-1175-4145",
"affiliation": [],
"authenticated-orcid": false,
"family": "Uddin",
"given": "Maimunah",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Alkaabi",
"given": "Nawal",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-6639-3298",
"affiliation": [],
"authenticated-orcid": false,
"family": "Tay",
"given": "Guan",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-4665-6024",
"affiliation": [],
"authenticated-orcid": false,
"family": "Mahboub",
"given": "Bassam",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-1993-6656",
"affiliation": [],
"authenticated-orcid": false,
"family": "Al Anouti",
"given": "Fatme",
"sequence": "additional"
}
],
"container-title": "Nutrients",
"container-title-short": "Nutrients",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2021,
5,
20
]
],
"date-time": "2021-05-20T01:49:21Z",
"timestamp": 1621475361000
},
"deposited": {
"date-parts": [
[
2021,
5,
20
]
],
"date-time": "2021-05-20T02:00:16Z",
"timestamp": 1621476016000
},
"funder": [
{
"award": [
"R20104"
],
"name": "Zayed Univerity"
},
{
"DOI": "10.13039/501100004070",
"award": [
"Internal grant"
],
"doi-asserted-by": "publisher",
"name": "Khalifa University"
}
],
"indexed": {
"date-parts": [
[
2024,
3,
20
]
],
"date-time": "2024-03-20T05:57:36Z",
"timestamp": 1710914256077
},
"is-referenced-by-count": 58,
"issue": "5",
"issued": {
"date-parts": [
[
2021,
5,
19
]
]
},
"journal-issue": {
"issue": "5",
"published-online": {
"date-parts": [
[
2021,
5
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
19
]
],
"date-time": "2021-05-19T00:00:00Z",
"timestamp": 1621382400000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/2072-6643/13/5/1714/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "1714",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2021,
5,
19
]
]
},
"published-online": {
"date-parts": [
[
2021,
5,
19
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"DOI": "10.3390/ijerph18062927",
"doi-asserted-by": "publisher",
"key": "ref1"
},
{
"article-title": "Global epidemic of coronavirus—Covid-19: What can we do to minimize risks",
"author": "Wimalawansa",
"first-page": "432",
"journal-title": "Eur. J. Biomed. Pharm. Sci.",
"key": "ref2",
"volume": "7",
"year": "2020"
},
{
"DOI": "10.1016/S1473-3099(20)30068-2",
"doi-asserted-by": "publisher",
"key": "ref3"
},
{
"DOI": "10.5858/arpa.2015-0519-RA",
"doi-asserted-by": "publisher",
"key": "ref4"
},
{
"DOI": "10.5858/arpa.2016-0342-RA",
"doi-asserted-by": "publisher",
"key": "ref5"
},
{
"DOI": "10.1007/s13668-020-00322-4",
"doi-asserted-by": "publisher",
"key": "ref6"
},
{
"DOI": "10.3390/nu12113361",
"doi-asserted-by": "publisher",
"key": "ref7"
},
{
"DOI": "10.1002/rmv.2032",
"doi-asserted-by": "publisher",
"key": "ref8"
},
{
"DOI": "10.1001/jama.2020.8598",
"doi-asserted-by": "publisher",
"key": "ref9"
},
{
"DOI": "10.1016/S0140-6736(20)30633-4",
"doi-asserted-by": "publisher",
"key": "ref10"
},
{
"DOI": "10.1111/dth.13681",
"doi-asserted-by": "publisher",
"key": "ref11"
},
{
"DOI": "10.3390/nu12040988",
"doi-asserted-by": "publisher",
"key": "ref12"
},
{
"DOI": "10.1111/apt.15777",
"doi-asserted-by": "publisher",
"key": "ref13"
},
{
"article-title": "Recognition and management of vitamin D deficiency",
"author": "Bordelon",
"first-page": "841",
"journal-title": "Am. Fam. Physician",
"key": "ref14",
"volume": "80",
"year": "2009"
},
{
"DOI": "10.1139/cjpp-2014-0352",
"doi-asserted-by": "publisher",
"key": "ref15"
},
{
"DOI": "10.1093/cid/cit289",
"doi-asserted-by": "publisher",
"key": "ref16"
},
{
"DOI": "10.1136/bmj.i6583",
"doi-asserted-by": "publisher",
"key": "ref17"
},
{
"DOI": "10.3390/biomedicines8050129",
"article-title": "Tripartite combination of candidate pandemic mitigation agents: Vitamin D, quercetin, and estradiol manifest properties of medicinal agents for targeted mitigation of the COVID-19 pandemic defined by genomics-guided tracing of SARS-CoV-2 targets in human cells",
"author": "Glinsky",
"doi-asserted-by": "crossref",
"first-page": "129",
"journal-title": "Biomedicines",
"key": "ref18",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.3390/nu9070651",
"doi-asserted-by": "publisher",
"key": "ref19"
},
{
"article-title": "Vitamin D for Health: A Global Perspective",
"author": "Hossein-Nezhad",
"first-page": "720",
"key": "ref20",
"series-title": "Proceedings of the Mayo Clinic Proceedings",
"volume": "Volume 88",
"year": "2013"
},
{
"DOI": "10.1016/j.coph.2006.03.001",
"doi-asserted-by": "publisher",
"key": "ref21"
},
{
"DOI": "10.1002/jmv.25992",
"doi-asserted-by": "publisher",
"key": "ref22"
},
{
"DOI": "10.1016/j.lfs.2005.09.038",
"doi-asserted-by": "publisher",
"key": "ref23"
},
{
"DOI": "10.1007/s40520-020-01570-8",
"doi-asserted-by": "publisher",
"key": "ref24"
},
{
"DOI": "10.3389/fnsyn.2014.00014",
"doi-asserted-by": "publisher",
"key": "ref25"
},
{
"DOI": "10.1016/j.jsbmb.2020.105751",
"doi-asserted-by": "publisher",
"key": "ref26"
},
{
"DOI": "10.1016/j.eprac.2021.02.013",
"doi-asserted-by": "publisher",
"key": "ref27"
},
{
"DOI": "10.1097/CCM.0b013e318206ccdf",
"doi-asserted-by": "publisher",
"key": "ref28"
},
{
"DOI": "10.1186/s13054-014-0660-4",
"doi-asserted-by": "publisher",
"key": "ref29"
},
{
"DOI": "10.1016/j.jcv.2010.12.006",
"doi-asserted-by": "publisher",
"key": "ref30"
},
{
"DOI": "10.2174/18715281113129990046",
"doi-asserted-by": "publisher",
"key": "ref31"
},
{
"DOI": "10.1126/science.abb8923",
"doi-asserted-by": "publisher",
"key": "ref32"
},
{
"DOI": "10.4161/derm.3.4.16881",
"doi-asserted-by": "publisher",
"key": "ref33"
},
{
"DOI": "10.1016/j.jsbmb.2016.02.007",
"doi-asserted-by": "publisher",
"key": "ref34"
},
{
"DOI": "10.1016/j.jsbmb.2013.11.003",
"doi-asserted-by": "publisher",
"key": "ref35"
},
{
"DOI": "10.1038/oby.2011.404",
"doi-asserted-by": "publisher",
"key": "ref36"
},
{
"DOI": "10.1007/s10654-019-00494-6",
"doi-asserted-by": "publisher",
"key": "ref37"
},
{
"DOI": "10.3390/nu12010236",
"doi-asserted-by": "publisher",
"key": "ref38"
},
{
"DOI": "10.1024/0300-9831/a000693",
"doi-asserted-by": "publisher",
"key": "ref39"
},
{
"DOI": "10.3390/medicina57050419",
"doi-asserted-by": "publisher",
"key": "ref40"
},
{
"DOI": "10.1016/j.nfs.2020.06.001",
"doi-asserted-by": "publisher",
"key": "ref41"
},
{
"DOI": "10.1111/acel.12386",
"doi-asserted-by": "publisher",
"key": "ref42"
},
{
"article-title": "Aging and health—A systems biology perspective. Introduction",
"author": "Jazwinski",
"first-page": "VII",
"journal-title": "Interdiscip. Top. Gerontol.",
"key": "ref43",
"volume": "40",
"year": "2015"
},
{
"DOI": "10.1007/s10522-015-9584-x",
"doi-asserted-by": "publisher",
"key": "ref44"
},
{
"DOI": "10.1159/000381134",
"article-title": "Frailty, Inflammation and Immunosenescence",
"author": "Fulop",
"doi-asserted-by": "crossref",
"first-page": "26",
"journal-title": "Frailty Aging",
"key": "ref45",
"volume": "41",
"year": "2015"
},
{
"DOI": "10.12688/f1000research.11297.1",
"doi-asserted-by": "publisher",
"key": "ref46"
},
{
"DOI": "10.3389/fimmu.2017.00982",
"doi-asserted-by": "publisher",
"key": "ref47"
},
{
"DOI": "10.3390/ijms18081742",
"doi-asserted-by": "publisher",
"key": "ref48"
},
{
"DOI": "10.4049/jimmunol.1500046",
"doi-asserted-by": "publisher",
"key": "ref49"
},
{
"DOI": "10.1053/j.seminhematol.2016.10.003",
"doi-asserted-by": "publisher",
"key": "ref50"
},
{
"DOI": "10.1073/pnas.1202870109",
"doi-asserted-by": "publisher",
"key": "ref51"
},
{
"DOI": "10.1016/j.chom.2017.02.003",
"doi-asserted-by": "publisher",
"key": "ref52"
},
{
"article-title": "Age-dependent alterations of Fc gamma receptor-mediated effector functions of human polymorphonuclear leucocytes",
"author": "Fülöp",
"first-page": "425",
"journal-title": "Clin. Exp. Immunol.",
"key": "ref53",
"volume": "61",
"year": "1985"
},
{
"article-title": "The Role of Immunosenescence in the Development of Age-Related Diseases",
"author": "Fülöp",
"first-page": "84",
"journal-title": "Rev. Investig. Clin.",
"key": "ref54",
"volume": "68",
"year": "2016"
},
{
"DOI": "10.1007/s00431-021-04030-1",
"doi-asserted-by": "publisher",
"key": "ref55"
},
{
"DOI": "10.1016/j.metabol.2020.154434",
"doi-asserted-by": "publisher",
"key": "ref56"
},
{
"DOI": "10.1007/s13679-021-00436-y",
"doi-asserted-by": "publisher",
"key": "ref57"
},
{
"DOI": "10.1016/j.dsx.2020.05.047",
"doi-asserted-by": "publisher",
"key": "ref58"
},
{
"DOI": "10.1073/pnas.2011086117",
"doi-asserted-by": "publisher",
"key": "ref59"
},
{
"DOI": "10.1161/CIRCULATIONAHA.120.047659",
"doi-asserted-by": "publisher",
"key": "ref60"
},
{
"DOI": "10.1007/s11657-020-0709-8",
"doi-asserted-by": "publisher",
"key": "ref61"
},
{
"DOI": "10.1002/oby.22831",
"doi-asserted-by": "publisher",
"key": "ref62"
},
{
"DOI": "10.1093/advances/nmab012",
"doi-asserted-by": "publisher",
"key": "ref63"
},
{
"DOI": "10.1371/journal.pone.0239252",
"doi-asserted-by": "publisher",
"key": "ref64"
},
{
"DOI": "10.1016/j.arr.2020.101201",
"doi-asserted-by": "publisher",
"key": "ref65"
},
{
"DOI": "10.1128/JVI.79.3.1966-1969.2005",
"doi-asserted-by": "publisher",
"key": "ref66"
},
{
"DOI": "10.1007/s00705-016-2904-x",
"doi-asserted-by": "publisher",
"key": "ref67"
},
{
"DOI": "10.1210/me.2013-1252",
"doi-asserted-by": "publisher",
"key": "ref68"
},
{
"DOI": "10.1161/JAHA.119.013837",
"doi-asserted-by": "publisher",
"key": "ref69"
},
{
"DOI": "10.1111/febs.15495",
"doi-asserted-by": "publisher",
"key": "ref70"
},
{
"DOI": "10.1007/s00394-020-02411-0",
"doi-asserted-by": "publisher",
"key": "ref71"
},
{
"DOI": "10.1007/s40520-021-01831-0",
"doi-asserted-by": "publisher",
"key": "ref72"
},
{
"DOI": "10.1186/s12967-021-02838-x",
"doi-asserted-by": "publisher",
"key": "ref73"
},
{
"DOI": "10.1016/j.jsbmb.2017.01.021",
"doi-asserted-by": "publisher",
"key": "ref74"
},
{
"DOI": "10.1371/journal.pone.0199265",
"doi-asserted-by": "publisher",
"key": "ref75"
},
{
"DOI": "10.3390/nu9111244",
"doi-asserted-by": "publisher",
"key": "ref76"
}
],
"reference-count": 76,
"references-count": 76,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/2072-6643/13/5/1714"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Food Science",
"Nutrition and Dietetics"
],
"subtitle": [],
"title": "COVID-19 Disease Severity and Death in Relation to Vitamin D Status among SARS-CoV-2-Positive UAE Residents",
"type": "journal-article",
"volume": "13"
}
