Vitamin D status and COVID-19 severity
et al., Southern African Journal of Infectious Diseases, doi:10.4102/sajid.v37i1.359, Apr 2022
Sunlight for COVID-19
35th treatment shown to reduce risk in
December 2021, now with p = 0.0000011 from 6 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 100 COVID-19 patients in South Africa, 50 with COVID-19 pneumonia and 50 asymptomatic, showing higher risk of symptomatic COVID-19 with lower exposure to sunlight, and with vitamin D deficiency. Sunlight exposure may be correlated with physical activity and may have additional benefits independent of vitamin D1.
Study covers sunlight and vitamin D.
|
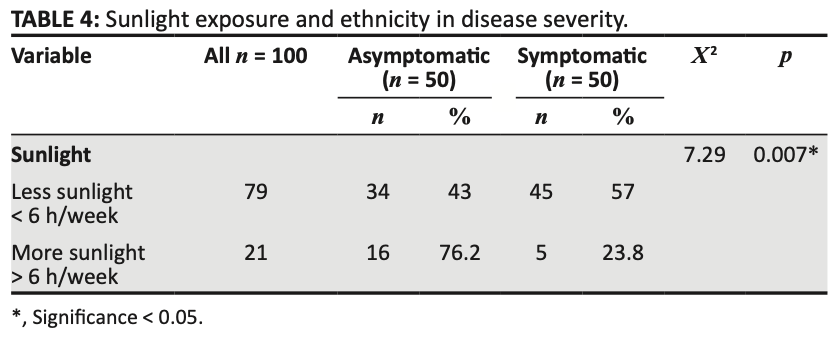
risk of symptomatic case, 58.2% lower, RR 0.42, p = 0.004, higher sunlight exposure 21, lower sunlight exposure 79, inverted to make RR<1 favor higher sunlight exposure, higher sunlight exposure vs. lower sunlight exposure.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Kalichuran et al., 26 Apr 2022, prospective, South Africa, peer-reviewed, survey, 4 authors, study period September 2020 - February 2021.
Vitamin D status and COVID-19 severity
Southern African Journal of Infectious Diseases, doi:10.4102/sajid.v37i1.359
Background: Age, body mass index (BMI) and pre-existing comorbidities are known risk factors of severe coronavirus disease 2019 (COVID-19). In this study we explore the relationship between vitamin D status and COVID-19 severity.
Methods: We conducted a prospective, cross-sectional descriptive study. We enrolled 100 COVID-19 positive patients admitted to a tertiary level hospital in Johannesburg, South Africa. Fifty had symptomatic disease (COVID-19 pneumonia) and 50 who were asymptomatic (incidental diagnosis). Following written informed consent, patients were interviewed regarding age, gender and sunlight exposure during the past week, disease severity, BMI, calcium, albumin, magnesium and alkaline phosphatase levels. Finally, blood was collected for vitamin D measurement.
Results: We found an 82% prevalence rate of vitamin D deficiency or insufficiency among COVID-19 patients. Vitamin D levels were lower in the symptomatic group (18.1 ng/mL ± 8.1 ng/mL) than the asymptomatic group (25.9 ng/mL ± 7.1 ng/mL) with a p-value of 0.000. The relative risk of symptomatic COVID-19 was 2.5-fold higher among vitamin D deficient patients than vitamin D non-deficient patients (confidence interval [CI]: 1.14-3.26). Additional predictors of symptomatic disease were older age, hypocalcaemia and hypoalbuminaemia. Using multiple regression, the only independent predictors of COVID-19 severity were age and vitamin D levels. The patients exposed to less sunlight had a 2.39-fold increased risk for symptomatic disease compared to those with more sunlight exposure (CI: 1.32-4.33).
Conclusion: We found a high prevalence of vitamin D deficiency and insufficiency among patients admitted to hospital with COVID-19 and an increased risk for symptomatic disease in vitamin D deficient patients.
Authors' contributions S.K. wrote the proposal, obtained ethics approval, collected data and wrote the original article. S.A.v.B. contributed to the conceptualisation of the article, data collection as well as supervising and reviewing of protocol and article writing. M.V. assisted with reviewing of the protocol and manuscript. S.O. contributed to statistical analysis and reviewing of article writing.
Disclaimer The views and opinions expressed in this article are those of the authors only.
References
Alamdari, Afaghi, Rahimi, Mortality risk factors among hospitalized COVID-19 patients in a major referral center in Iran, Tohoku J Exp Med, doi:10.1620/tjem.252.73
Avci, Demir, Aslan, Nar, Şenol, Assessment of Abbott Architect 25-OH vitamin D assay in different levels of vitamin D, J Med Biochem, doi:10.2478/jomb-2019-0039
Bennouar, Cherif, Kessira, Bennouar, Abdi, Vitamin D deficiency and low serum calcium as predictors of poor prognosis in patients with severe COVID-19, J Am Coll Nutr, doi:10.1080/07315724.2020.1856013
Bergman, Lindh, Bjorkhem-Bergman, Lindh, Vitamin D and respiratory tract infections: A systematic review and meta-analysis of randomized controlled trials, PLoS One, doi:10.1371/journal.pone.0065835
Campi, Gennari, Merlotti, Vitamin D and COVID-19 severity and related mortality: A prospective study in Italy, BMC Infect Dis, doi:10.1186/s12879-021-06281-7
Cannell, Vieth, Umhau, Epidemic influenza and vitamin D, Epidemiol Infect, doi:10.1017/S0950268806007175
Chen, Zheng, Zhang, Clinical characteristics of 145 patients with corona virus disease 2019 (COVID-19) in Taizhou, Zhejiang, China, Infection, doi:10.1007/s15010-020-01432-5
Coussens, Naude, Goliath, Chaplin, Wilkinson et al., Highdose vitamin D3 reduces deficiency caused by low UVB exposure and limits HIV-1 replication in urban Southern Africans, Proc Natl Acad Sci U S A, doi:10.1073/pnas.1500909112
Filippo, Formenti, Rovere-Querini, Hypocalcemia is highly prevalent and predicts hospitalization in patients with COVID-19, Endocrine, doi:10.1007/s12020-020-02383-5
Garg, Kim, Whitaker, Hospitalization rates and characteristics of patients hospitalized with laboratory-confirmed coronavirus disease 2019 -COVID-NET, 14 states, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm6915e3
George, Norris, Van Deventer, Pettifor, Crowther, Effect of adiposity, season, diet and calcium or vitamin D supplementation on the vitamin D status of healthy urban African and Asian-Indian adults, Br J Nutr, doi:10.1017/S0007114514001202
Guasp, Laredo, Urra, Higher solar irradiance is associated with a lower incidence of coronavirus disease 2019, Clin Infect Dis, doi:10.1093/cid/ciaa575
Gulhar, Ashraf, Jialal, Physiology, acute phase reactants
Holick, Binkley, Bischoff-Ferrari, Evaluation, treatment, and prevention of vitamin D deficiency: An endocrine society clinical practice guideline, J Clin Endocrinol Metabolism, doi:10.1210/jc.2011-0385
Mohan, Cherian, Sharma, Exploring links between vitamin D deficiency and COVID-19, PLoS Pathog, doi:10.1371/journal.ppat.1008874
Norval, Coussens, Wilkinson, Bornman, Lucas et al., Vitamin D status and its consequences for health in South Africa, Int J Environ Res Public Health, doi:10.3390/ijerph13101019
Panagiotou, Tee, Ihsan, Low serum 25-hydroxyvitamin D (25[OH]D) levels in patients hospitalized with COVID-19 are associated with greater disease severity, Clin Endocrinol, doi:10.1111/cen.14276
Prietl, Treiber, Pieber, Amrein, Vitamin D and immune function, Nutrients, doi:10.3390/nu5072502
Radujkovic, Hippchen, Tiwari-Heckler, Dreher, Boxberger, Vitamin D deficiency and outcome of COVID-19 patients, Nutrients, doi:10.3390/nu12092757
Rhodes, Dunstan, Laird, Subramanian, Kenny, COVID-19 mortality increases with northerly latitude after adjustment for age suggesting a link with ultraviolet and vitamin D, BMJ Nutr Prev Health, doi:10.1136/bmjnph-2020-000110
Roth, Abrams, Aloia, Global prevalence and disease burden of vitamin D deficiency: A roadmap for action in low-and middle-income countries, Ann N Y Acad Sci, doi:10.1111/nyas.13968
Rothan, Byrareddy, The epidemiology and pathogenesis of coronavirus disease (COVID-19) outbreak, J Autoimmun, doi:10.1016/j.jaut.2020.102433
Salman, Khouzami, Harb, Prevalence and predictors of vitamin D inadequacy: A sample of 2,547 patients in a Mediterranean country, Cureus, doi:10.7759/cureus.14881
Sharun, Tiwari, Dhama, COVID-19 and sunlight: Impact on SARS-CoV-2 transmissibility, morbidity, and mortality, Ann Med Surg, doi:10.1016/j.amsu.2021.102419
Simonnet, Chetboun, Poissy, High prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation, Obesity, doi:10.1002/oby.22831
Singh, Kang, Luo, COVID-19: Current knowledge in clinical features, immunological responses, and vaccine development, FASEB J, doi:10.1096/fj.202002662R
Singh, Nimavat, Singh, Ahmad, Sinha, Prevalence of low level of vitamin D among COVID-19 patients and associated risk factors in India -A hospital-based study, Int J Gen Med, doi:10.2147/IJGM.S309003
Smet, Smet, Herroelen, Gryspeerdt, Martens, Vitamin D deficiency as risk factor for severe COVID-19: A convergence of two pandemics, medRxiv, doi:10.1101/2020.05.01.20079376
Sowah, Fan, Dennett, Hagtvedt, Straube, Vitamin D levels and deficiency with different occupations: A systematic review, BMC Public Health, doi:10.1186/s12889-017-4436-z
Tian, Hu, Lou, Characteristics of COVID-19 infection in Beijing, J Infect, doi:10.1016/j.jinf.2020.02.018
Wacker, Holick, Sunlight and Vitamin D, Dermato-Endocrinology, doi:10.4161/derm.24494
Whittemore, COVID-19 fatalities, latitude, sunlight, and vitamin D, Am J Infect Control, doi:10.1016/j.ajic.2020.06.193
DOI record:
{
"DOI": "10.4102/sajid.v37i1.359",
"ISSN": [
"2313-1810",
"2312-0053"
],
"URL": "http://dx.doi.org/10.4102/sajid.v37i1.359",
"author": [
{
"affiliation": [],
"family": "Kalichuran",
"given": "Senrina",
"sequence": "first"
},
{
"affiliation": [],
"family": "van Blydenstein",
"given": "Sarah A.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Venter",
"given": "Michelle",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Omar",
"given": "Shahed",
"sequence": "additional"
}
],
"container-title": "Southern African Journal of Infectious Diseases",
"container-title-short": "Southern African Journal of Infectious Diseases",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2022,
5,
9
]
],
"date-time": "2022-05-09T09:32:22Z",
"timestamp": 1652088742000
},
"deposited": {
"date-parts": [
[
2022,
6,
14
]
],
"date-time": "2022-06-14T12:59:54Z",
"timestamp": 1655211594000
},
"indexed": {
"date-parts": [
[
2022,
6,
14
]
],
"date-time": "2022-06-14T13:41:37Z",
"timestamp": 1655214097587
},
"is-referenced-by-count": 0,
"issue": "1",
"issued": {
"date-parts": [
[
2022,
4,
26
]
]
},
"journal-issue": {
"issue": "1",
"published-online": {
"date-parts": [
[
2022,
4,
26
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
4,
26
]
],
"date-time": "2022-04-26T00:00:00Z",
"timestamp": 1650931200000
}
}
],
"link": [
{
"URL": "https://sajid.co.za/index.php/sajid/article/viewFile/359/946",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://sajid.co.za/index.php/sajid/article/viewFile/359/947",
"content-type": "application/epub+zip",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://sajid.co.za/index.php/sajid/article/viewFile/359/948",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://sajid.co.za/index.php/sajid/article/viewFile/359/949",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://sajid.co.za/index.php/sajid/article/viewFile/359/949",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "2580",
"original-title": [],
"prefix": "10.4102",
"published": {
"date-parts": [
[
2022,
4,
26
]
]
},
"published-online": {
"date-parts": [
[
2022,
4,
26
]
]
},
"publisher": "AOSIS",
"reference": [
{
"DOI": "10.1016/j.jaut.2020.102433",
"author": "Rothan",
"doi-asserted-by": "publisher",
"first-page": "102433",
"journal-title": "J Autoimmun",
"key": "CIT0001",
"volume": "109",
"year": "2020"
},
{
"DOI": "10.1096/fj.202002662R",
"author": "Singh",
"doi-asserted-by": "publisher",
"first-page": "e21409",
"journal-title": "FASEB J",
"key": "CIT0002",
"volume": "35",
"year": "2021"
},
{
"DOI": "10.1371/journal.ppat.1008874",
"author": "Mohan",
"doi-asserted-by": "publisher",
"first-page": "e1008874",
"journal-title": "PLoS Pathog",
"key": "CIT0003",
"volume": "16",
"year": "2020"
},
{
"DOI": "10.4161/derm.24494",
"author": "Wacker",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Dermato-Endocrinology",
"key": "CIT0004",
"volume": "5",
"year": "2013"
},
{
"DOI": "10.3390/ijerph13101019",
"author": "Norval",
"doi-asserted-by": "publisher",
"first-page": "1019",
"journal-title": "Int J Environ Res Public Health",
"key": "CIT0005",
"volume": "13",
"year": "2016"
},
{
"DOI": "10.3390/nu5072502",
"author": "Prietl",
"doi-asserted-by": "publisher",
"first-page": "2502",
"journal-title": "Nutrients",
"key": "CIT0006",
"volume": "5",
"year": "2013"
},
{
"DOI": "10.1111/nyas.13968",
"author": "Roth",
"doi-asserted-by": "publisher",
"first-page": "44",
"journal-title": "Ann N Y Acad Sci",
"key": "CIT0007",
"volume": "1430",
"year": "2018"
},
{
"DOI": "10.1017/S0007114514001202",
"author": "George",
"doi-asserted-by": "publisher",
"first-page": "590",
"journal-title": "Br J Nutr",
"key": "CIT0008",
"volume": "112",
"year": "2014"
},
{
"DOI": "10.7759/cureus.14881",
"author": "Salman",
"doi-asserted-by": "publisher",
"first-page": "e14881",
"journal-title": "Cureus",
"key": "CIT0009",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1073/pnas.1500909112",
"author": "Coussens",
"doi-asserted-by": "publisher",
"first-page": "8052",
"journal-title": "Proc Natl Acad Sci U S A",
"key": "CIT0010",
"volume": "112",
"year": "2015"
},
{
"DOI": "10.1186/s12889-017-4436-z",
"author": "Sowah",
"doi-asserted-by": "publisher",
"first-page": "519",
"journal-title": "BMC Public Health",
"key": "CIT0011",
"volume": "17",
"year": "2017"
},
{
"DOI": "10.1371/journal.pone.0065835",
"author": "Bergman",
"doi-asserted-by": "publisher",
"first-page": "e65835",
"journal-title": "PLoS One",
"key": "CIT0012",
"volume": "8",
"year": "2013"
},
{
"DOI": "10.1017/S0950268806007175",
"author": "Cannell",
"doi-asserted-by": "publisher",
"first-page": "1129",
"journal-title": "Epidemiol Infect",
"key": "CIT0013",
"volume": "134",
"year": "2006"
},
{
"DOI": "10.2478/jomb-2019-0039",
"author": "Avci",
"doi-asserted-by": "publisher",
"first-page": "100",
"journal-title": "J Med Biochem",
"key": "CIT0014",
"volume": "39",
"year": "2020"
},
{
"DOI": "10.1210/jc.2011-0385",
"author": "Holick",
"doi-asserted-by": "publisher",
"first-page": "1911",
"journal-title": "J Clin Endocrinol Metabolism",
"key": "CIT0015",
"volume": "96",
"year": "2011"
},
{
"DOI": "10.2147/IJGM.S309003",
"author": "Singh",
"doi-asserted-by": "publisher",
"first-page": "2523",
"journal-title": "Int J Gen Med",
"key": "CIT0016",
"volume": "14",
"year": "2021"
},
{
"DOI": "10.1080/07315724.2020.1856013",
"author": "Bennouar",
"doi-asserted-by": "publisher",
"first-page": "104",
"journal-title": "J Am Coll Nutr",
"key": "CIT0017",
"volume": "40",
"year": "2021"
},
{
"DOI": "10.3390/nu12092757",
"author": "Radujkovic",
"doi-asserted-by": "publisher",
"first-page": "2757",
"journal-title": "Nutrients",
"key": "CIT0018",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1111/cen.14276",
"author": "Panagiotou",
"doi-asserted-by": "publisher",
"first-page": "508",
"journal-title": "Clin Endocrinol",
"key": "CIT0019",
"volume": "93",
"year": "2020"
},
{
"DOI": "10.1186/s12879-021-06281-7",
"author": "Campi",
"doi-asserted-by": "publisher",
"first-page": "566",
"journal-title": "BMC Infect Dis",
"key": "CIT0020",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1101/2020.05.01.20079376",
"author": "De Smet",
"doi-asserted-by": "publisher",
"journal-title": "medRxiv",
"key": "CIT0021",
"year": "2020"
},
{
"DOI": "10.1007/s15010-020-01432-5",
"author": "Chen",
"doi-asserted-by": "publisher",
"first-page": "543",
"journal-title": "Infection",
"key": "CIT0022",
"volume": "48",
"year": "2020"
},
{
"DOI": "10.1016/j.jinf.2020.02.018",
"author": "Tian",
"doi-asserted-by": "publisher",
"first-page": "401",
"journal-title": "J Infect",
"key": "CIT0023",
"volume": "80",
"year": "2020"
},
{
"DOI": "10.15585/mmwr.mm6915e3",
"author": "Garg",
"doi-asserted-by": "publisher",
"first-page": "458",
"journal-title": "MMWR Morb Mortal Wkly Rep",
"key": "CIT0024",
"volume": "69",
"year": "2020"
},
{
"DOI": "10.1002/oby.22831",
"author": "Simonnet",
"doi-asserted-by": "publisher",
"first-page": "1195",
"journal-title": "Obesity",
"key": "CIT0025",
"volume": "28",
"year": "2020"
},
{
"DOI": "10.1620/tjem.252.73",
"author": "Alamdari",
"doi-asserted-by": "publisher",
"first-page": "73",
"journal-title": "Tohoku J Exp Med",
"key": "CIT0026",
"volume": "252",
"year": "2020"
},
{
"DOI": "10.1007/s12020-020-02383-5",
"author": "Di Filippo",
"doi-asserted-by": "publisher",
"first-page": "475",
"journal-title": "Endocrine",
"key": "CIT0027",
"volume": "68",
"year": "2020"
},
{
"author": "Gulhar",
"journal-title": "Physiology, acute phase reactants",
"key": "CIT0028",
"year": "2021"
},
{
"DOI": "10.1016/j.ajic.2020.06.193",
"author": "Whittemore",
"doi-asserted-by": "publisher",
"first-page": "1042",
"journal-title": "Am J Infect Control",
"key": "CIT0029",
"volume": "48",
"year": "2020"
},
{
"DOI": "10.1136/bmjnph-2020-000110",
"author": "Rhodes",
"doi-asserted-by": "publisher",
"first-page": "118",
"journal-title": "BMJ Nutr Prev Health",
"key": "CIT0030",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1093/cid/ciaa575",
"author": "Guasp",
"doi-asserted-by": "publisher",
"first-page": "2269",
"journal-title": "Clin Infect Dis",
"key": "CIT0031",
"volume": "71",
"year": "2020"
},
{
"DOI": "10.1016/j.amsu.2021.102419",
"author": "Sharun",
"doi-asserted-by": "publisher",
"first-page": "102419",
"journal-title": "Ann Med Surg",
"key": "CIT0032",
"volume": "66",
"year": "2021"
}
],
"reference-count": 32,
"references-count": 32,
"relation": {},
"resource": {
"primary": {
"URL": "https://sajid.co.za/index.php/sajid/article/view/359"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subtitle": [],
"title": "Vitamin D status and COVID-19 severity",
"type": "journal-article",
"volume": "37"
}
kalichuran
