Vitamin D Deficiency and Low Serum Calcium as Predictors of Poor Prognosis in Patients with Severe COVID-19
et al., Journal of the American College of Nutrition, doi:10.1080/07315724.2020.1856013, Jan 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 120 severe cases of COVID-19 in Algeria finding low vitamin D and low calcium both associated with increased mortality.
This is the 40th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
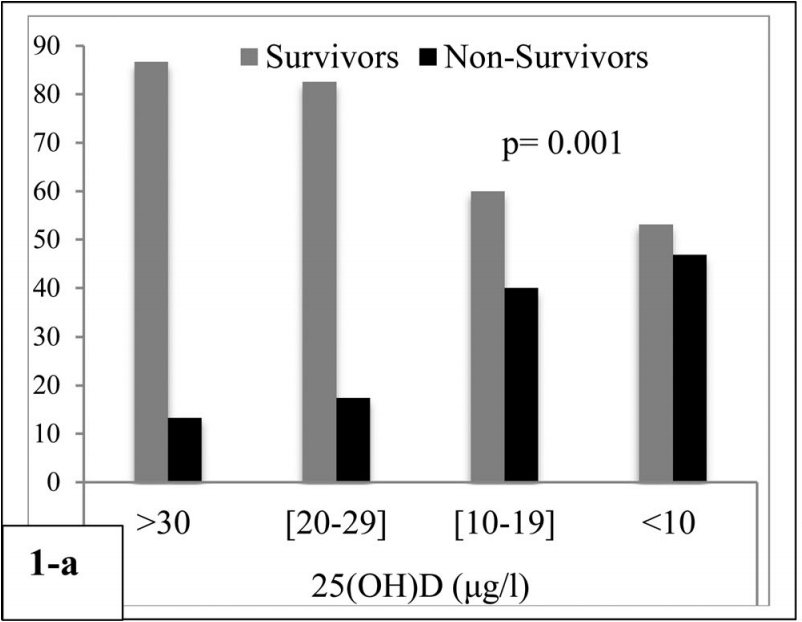
risk of death, 85.5% lower, RR 0.14, p = 0.002, high D levels 4 of 30 (13.3%), low D levels 15 of 32 (46.9%), NNT 3.0, adjusted per study, inverted to make RR<1 favor high D levels, >30μg/l vs. <10μg/l, proportional Cox regression.
|
|
risk of death, 63.0% lower, RR 0.37, p = 0.10, high D levels 4 of 30 (13.3%), low D levels 14 of 35 (40.0%), NNT 3.7, adjusted per study, inverted to make RR<1 favor high D levels, >30μg/l vs. 10-19μg/l, proportional Cox regression.
|
|
risk of death, 23.1% lower, RR 0.77, p = 0.73, high D levels 4 of 30 (13.3%), low D levels 4 of 23 (17.4%), NNT 25, adjusted per study, inverted to make RR<1 favor high D levels, >30μg/l vs. 20-29μg/l, proportional Cox regression.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Bennouar et al., 12 Jan 2021, prospective, Algeria, peer-reviewed, 5 authors.
Vitamin D Deficiency and Low Serum Calcium as Predictors of Poor Prognosis in Patients with Severe COVID-19
Journal of the American College of Nutrition, doi:10.1080/07315724.2020.1856013
Background: The severity of Coronavirus Disease 2019 (COVID-19) is a multifactorial condition. An increasing body of evidence argues for a direct implication of vitamin D deficiency, low serum calcium on poor outcomes in COVID-19 patients. This study was designed to investigate the relationship between these two factors and COVID-19 in-hospital mortality. Materials: This is a prospective study, including 120 severe cases of COVID-19, admitted at the department of Reanimation-Anesthesia. Vitamin D was assessed by an immuno-fluoroassay method. Total serum calcium by a colorimetric method, then, corrected for serum albumin levels. The association with in-hospital mortality was assessed using the Kaplan-Meier survival curve, proportional Cox regression analyses and the receiver operating characteristic curve. Results: Hypovitaminosis D and hypocalcemia were very common, occurring in 75% and 35.8% of patients. When analyzing survival, both were significantly associated with in-hospital mortality in a dose-effect manner (p Log-Rank ¼ 0.009 and 0.001 respectively). A cutoff value of 39 nmol/l for vitamin D and 2.05 mmol/l for corrected calcemia could predict poor prognosis with a sensitivity of 76% and 84%, and a specificity of 69% and 60% respectively. Hazard ratios were (HR ¼ 6.9, 95% CI [2.0-24.1], p ¼ 0.002 and HR ¼ 6.2, 95% CI [2.1-18.3], p ¼ 0.001) respectively. Conclusion: This study demonstrates the high frequency of hypocalcemia and hypovitaminosis D in severe COVID-19 patients and provides further evidence of their potential link to poor shortterm prognosis. It is, therefore, possible that the correction of hypocalcemia, as well as supplementation with vitamin D, may improve the vital prognosis.
Disclosure statement The authors have no conflicts of interest to declare.
ORCID
Salam Bennouar http://orcid.org/0000-0001-7414-6721
References
Ali, Role of vitamin D in preventing of COVID-19 infection, progression and severity, J Infect Public Health, doi:10.1016/j.jiph.2020.06.021
Bennouar, Cherif, Kessira, Hamel, Boudahdir et al., Usefulness of biological markers in the early prediction of corona virus disease-2019 severity, Scand J Clin Lab Invest
Biesalski, Vitamin D deficiency and co-morbidities in COVID-19 patients -a fatal relationship?, NFS J, doi:10.1016/j.nfs.2020.06.001
Cappellini, Brivio, Casati, Cavallero, Contro et al., Low levels of total and ionized calcium in blood of COVID-19 patients, Clin Chem Lab Med, doi:10.1515/cclm-2020-0611
Carpagnano, Lecce, Quaranta, Zito, Buonamico et al., Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19, J Endocrinol Invest
Chakhtoura, Napoli, Hajj Fuleihan, Commentary: myths and facts on vitamin D amidst the COVID-19 pandemic, Metabolism, doi:10.1016/j.metabol.2020.154276
Chandran, Maung, Mithal, Parameswaran, Vitamin D in COVID -19: dousing the fire or averting the storm? -a perspective from the Asia-Pacific, Osteoporos Sarcopenia, doi:10.1016/j.afos.2020.07.003
D'avolio, Avataneo, Manca, Cusato, Nicol O et al., 25-Hydroxyvitamin D concentrations are lower in patients with positive PCR for SARS-CoV-2, Nutrients, doi:10.3390/nu12051359
Grant, Lahore, Mcdonnell, Baggerly, French et al., Evidence that Vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths, Nutrients, doi:10.3390/nu12040988
Holick, Binkley, Bischoff-Ferrari, Gordon, Hanley et al., Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline, J Clin Endocrinol Metab, doi:10.1210/jc.2011-0385
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin Exp Res, doi:10.1007/s40520-020-01570-8
Kellum, Lameire, Aspelin, Kellum, Lameire et al., Kidney disease: improving global outcomes (KDIGO) acute kidney injury work group. KDIGO clinical practice guideline for acute kidney injury, Kidney Int suppl
Lippi, South, Henry, Electrolyte imbalances in patients with severe coronavirus disease 2019 (COVID-19), Ann Clin Biochem, doi:10.1177/0004563220922255
Mahdavi, A brief review of interplay between vitamin D and angiotensin-converting enzyme 2: implications for a potential treatment for COVID-19, Rev Med Virol, doi:10.1002/rmv.2119
Marik, Kory, Varon, Does vitamin D status impact mortality from SARS-CoV-2 infection?, Med Drug Discov, doi:10.1016/j.medidd.2020.100041
Merzon, Tworowski, Gorohovski, Vinker, Cohen et al., Low plasma 25(OH) vitamin D level is associated with increased risk of COVID-19 infection: an Israeli population-based study, FEBS J, doi:10.1111/febs.15495
Munshi, Hussein, Toraih, Elshazli, Jardak et al., Vitamin D insufficiency as a potential culprit in critical COVID-19 patients, J Med Virol, doi:10.1002/jmv.26360
Razdan, Singh, Singh, Vitamin D levels and COVID-19 susceptibility: is there any correlation?, Med Drug Discov, doi:10.1016/j.medidd.2020.100051
Rhodes, Subramanian, Laird, Kenny, Editorial: low population mortality from COVID-19 in countries south of latitude 35 degrees North supports vitamin D as a factor determining severity, Aliment Pharmacol Ther, doi:10.1111/apt.15777
Slominski, Stefan, Athar, Holick, Jetten et al., COVID-19 and Vitamin D: a lesson from the skin, Exp Dermatol, doi:10.1111/exd.14170
Sun, Zhang, Zou, Liu, Li et al., Serum calcium as a biomarker of clinical severity and prognosis in patients with coronavirus disease 2019, Aging, doi:10.18632/aging.103526
Whittemore, COVID-19 fatalities, latitude, sunlight, and vitamin D, Am J Infect Control, doi:10.1016/j.ajic.2020.06.193
Xu, Baylink, Chen, Reeves, Xiao et al., The importance of vitamin d metabolism as a potential prophylactic, immunoregulatory and neuroprotective treatment for COVID-19, J Transl Med, doi:10.1186/s12967-020-02488-5
DOI record:
{
"DOI": "10.1080/07315724.2020.1856013",
"ISSN": [
"0731-5724",
"1541-1087"
],
"URL": "http://dx.doi.org/10.1080/07315724.2020.1856013",
"alternative-id": [
"10.1080/07315724.2020.1856013"
],
"assertion": [
{
"label": "Peer Review Statement",
"name": "peerreview_statement",
"order": 1,
"value": "The publishing and review policy for this title is described in its Aims & Scope."
},
{
"URL": "http://www.tandfonline.com/action/journalInformation?show=aimsScope&journalCode=uacn20",
"label": "Aim & Scope",
"name": "aims_and_scope_url",
"order": 2,
"value": "http://www.tandfonline.com/action/journalInformation?show=aimsScope&journalCode=uacn20"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Received",
"name": "received",
"order": 0,
"value": "2020-11-06"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Revised",
"name": "revised",
"order": 1,
"value": "2020-11-19"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "2020-11-22"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Published",
"name": "published",
"order": 3,
"value": "2021-01-12"
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0001-7414-6721",
"affiliation": [
{
"name": "Central Laboratory of Clinical Biology, University Hospital Center of Blida, Blida, Algeria"
}
],
"authenticated-orcid": false,
"family": "Bennouar",
"given": "Salam",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Department of Internal Medicine and Cardiology, University Hospital Center of Blida, Blida, Algeria"
}
],
"family": "Cherif",
"given": "Abdelghani Bachir",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Hemobiology and Blood Transfusion, University Hospital Center of Annaba, Annaba, Algeria"
}
],
"family": "Kessira",
"given": "Amel",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Hemobiology and Blood Transfusion, University Hospital Center of Annaba, Annaba, Algeria"
}
],
"family": "Bennouar",
"given": "Djamel-Eddine",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Central Laboratory of Clinical Biology, University Hospital Center of Blida, Blida, Algeria"
}
],
"family": "Abdi",
"given": "Samia",
"sequence": "additional"
}
],
"container-title": "Journal of the American College of Nutrition",
"container-title-short": "Journal of the American College of Nutrition",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"www.tandfonline.com"
]
},
"created": {
"date-parts": [
[
2021,
1,
15
]
],
"date-time": "2021-01-15T00:12:34Z",
"timestamp": 1610669554000
},
"deposited": {
"date-parts": [
[
2021,
2,
19
]
],
"date-time": "2021-02-19T12:55:42Z",
"timestamp": 1613739342000
},
"indexed": {
"date-parts": [
[
2024,
3,
5
]
],
"date-time": "2024-03-05T05:19:44Z",
"timestamp": 1709615984877
},
"is-referenced-by-count": 66,
"issue": "2",
"issued": {
"date-parts": [
[
2021,
1,
12
]
]
},
"journal-issue": {
"issue": "2",
"published-print": {
"date-parts": [
[
2021,
2,
17
]
]
}
},
"language": "en",
"link": [
{
"URL": "https://www.tandfonline.com/doi/pdf/10.1080/07315724.2020.1856013",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "301",
"original-title": [],
"page": "104-110",
"prefix": "10.1080",
"published": {
"date-parts": [
[
2021,
1,
12
]
]
},
"published-online": {
"date-parts": [
[
2021,
1,
12
]
]
},
"published-print": {
"date-parts": [
[
2021,
2,
17
]
]
},
"publisher": "Informa UK Limited",
"reference": [
{
"DOI": "10.1002/rmv.2119",
"doi-asserted-by": "publisher",
"key": "CIT0001"
},
{
"DOI": "10.3390/nu12040988",
"doi-asserted-by": "publisher",
"key": "CIT0002"
},
{
"DOI": "10.1016/j.jiph.2020.06.021",
"doi-asserted-by": "publisher",
"key": "CIT0003"
},
{
"DOI": "10.1186/s12967-020-02488-5",
"doi-asserted-by": "publisher",
"key": "CIT0004"
},
{
"DOI": "10.1016/j.metabol.2020.154276",
"doi-asserted-by": "publisher",
"key": "CIT0005"
},
{
"DOI": "10.1016/j.medidd.2020.100051",
"doi-asserted-by": "publisher",
"key": "CIT0006"
},
{
"DOI": "10.1016/j.nfs.2020.06.001",
"doi-asserted-by": "publisher",
"key": "CIT0007"
},
{
"DOI": "10.1016/j.medidd.2020.100041",
"doi-asserted-by": "publisher",
"key": "CIT0008"
},
{
"DOI": "10.1016/j.afos.2020.07.003",
"doi-asserted-by": "publisher",
"key": "CIT0009"
},
{
"DOI": "10.1007/s40520-020-01570-8",
"doi-asserted-by": "publisher",
"key": "CIT0010"
},
{
"DOI": "10.18632/aging.103526",
"doi-asserted-by": "publisher",
"key": "CIT0011"
},
{
"DOI": "10.1515/cclm-2020-0611",
"doi-asserted-by": "publisher",
"key": "CIT0012"
},
{
"key": "CIT0013",
"unstructured": "Laboratory testing for coronavirus disease 2019 (COVID-19) in suspected human cases: interim guidance; 2020 Mar 2. Available from: https://apps.who.int/iris/handle/10665/331329."
},
{
"author": "Bennouar S",
"first-page": "1",
"journal-title": "Scand J Clin Lab Invest",
"key": "CIT0014",
"volume": "18",
"year": "2020"
},
{
"DOI": "10.1210/jc.2011-0385",
"doi-asserted-by": "publisher",
"key": "CIT0015"
},
{
"DOI": "10.1038/kisup.2012.1",
"author": "Kellum A",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Kidney Int suppl",
"key": "CIT0016",
"volume": "2",
"year": "2012"
},
{
"DOI": "10.3390/nu12051359",
"doi-asserted-by": "publisher",
"key": "CIT0017"
},
{
"DOI": "10.1111/febs.15495",
"doi-asserted-by": "publisher",
"key": "CIT0018"
},
{
"author": "Carpagnano GE",
"first-page": "1",
"journal-title": "J Endocrinol Invest.",
"key": "CIT0019",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1002/jmv.26360",
"doi-asserted-by": "publisher",
"key": "CIT0020"
},
{
"DOI": "10.1016/j.ajic.2020.06.193",
"doi-asserted-by": "publisher",
"key": "CIT0021"
},
{
"DOI": "10.1111/apt.15777",
"doi-asserted-by": "publisher",
"key": "CIT0022"
},
{
"DOI": "10.1111/exd.14170",
"doi-asserted-by": "publisher",
"key": "CIT0023"
},
{
"DOI": "10.1177/0004563220922255",
"doi-asserted-by": "publisher",
"key": "CIT0024"
}
],
"reference-count": 24,
"references-count": 24,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.tandfonline.com/doi/full/10.1080/07315724.2020.1856013"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Nutrition and Dietetics",
"Medicine (miscellaneous)"
],
"subtitle": [],
"title": "Vitamin D Deficiency and Low Serum Calcium as Predictors of Poor Prognosis in Patients with Severe COVID-19",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1080/tandf_crossmark_01",
"volume": "40"
}
