Vitamin D as a predictor of negative outcomes in hospitalized COVID-19 patients: An observational study
et al., Canadian Journal of Respiratory Therapy, doi:10.29390/001c.87408, Aug 2023
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 70 hospitalized COVID-19 patients in Iran, showing higher mortality, ventilation, and need for respiratory support with low vitamin D levels, all without statistical significance. Adjusted results are provided only for respiratory support.
This is the 187th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
risk of death, 70.0% lower, RR 0.30, p = 0.24, high D levels (≥30ng/ml) 1 of 28 (3.6%), low D levels (<30ng/ml) 5 of 42 (11.9%), NNT 12, inverted to make RR<1 favor high D levels (≥30ng/ml), odds ratio converted to relative risk.
|
|
risk of mechanical ventilation, 75.0% lower, RR 0.25, p = 0.23, high D levels (≥30ng/ml) 1 of 28 (3.6%), low D levels (<30ng/ml) 6 of 42 (14.3%), NNT 9.3.
|
|
risk of progression, 62.5% lower, RR 0.38, p = 0.30, high D levels (≥30ng/ml) 2 of 28 (7.1%), low D levels (<30ng/ml) 8 of 42 (19.0%), NNT 8.4, critical case.
|
|
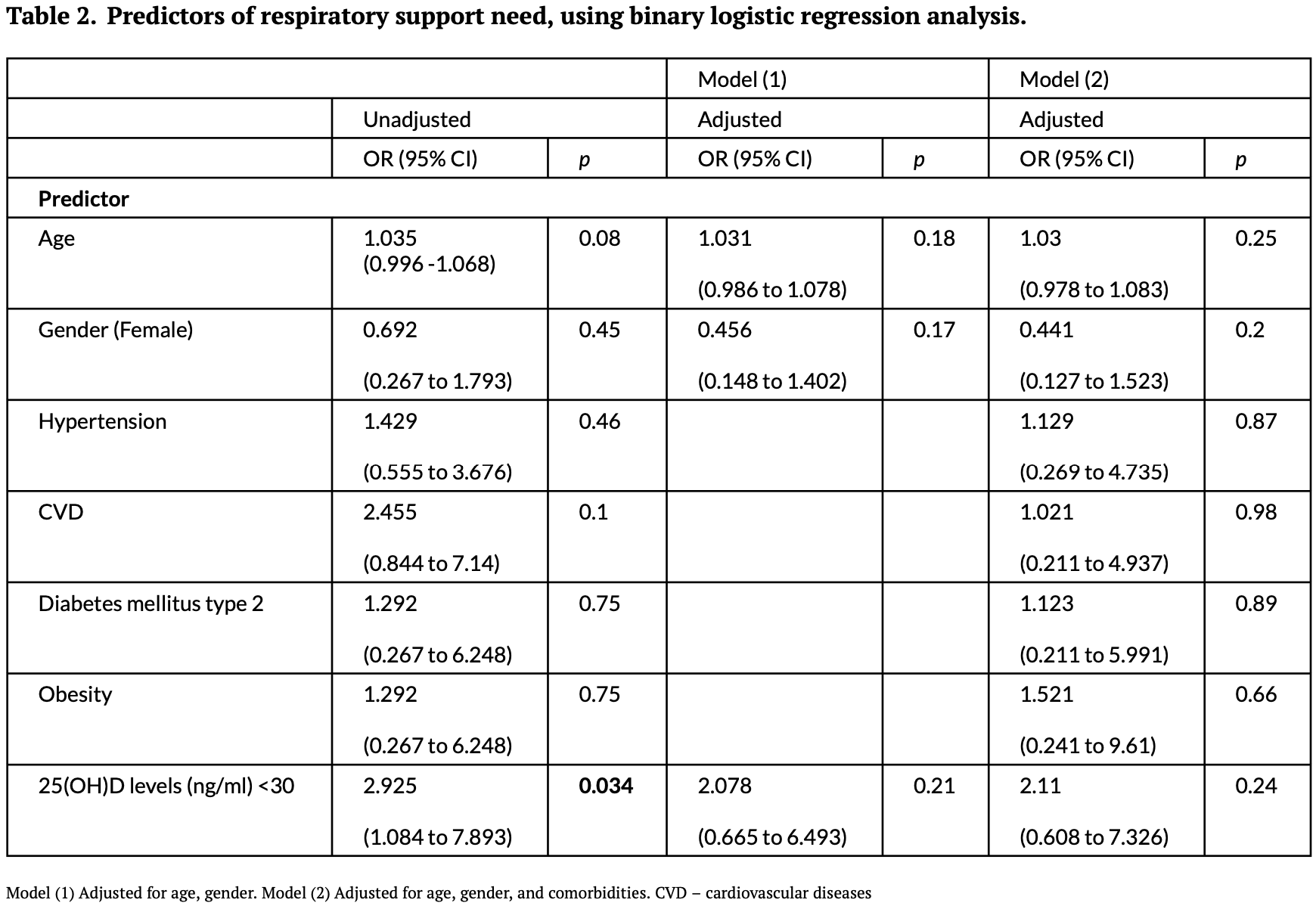
risk of oxygen therapy, 27.0% lower, RR 0.73, p = 0.24, high D levels (≥30ng/ml) 10 of 28 (35.7%), low D levels (<30ng/ml) 28 of 42 (66.7%), NNT 3.2, adjusted per study, inverted to make RR<1 favor high D levels (≥30ng/ml), odds ratio converted to relative risk, multivariable.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Bogomaz et al., 24 Aug 2023, retrospective, Ukraine, peer-reviewed, median age 62.0, 2 authors.
Vitamin D as a predictor of negative outcomes in hospitalized COVID-19 patients: An observational study
Canadian Journal of Respiratory Therapy, doi:10.29390/001c.87408
Introduction Serum vitamin D deficiency is thought to be associated with worse clinical outcomes in COVID-19 patients.
Methods This single-centre observational study evaluated the association between serum vitamin D levels and negative outcomes in hospitalized COVID-19 patients in Ukraine. We included hospitalized patients with COVID-19 confirmed by PCR and serum vitamin D measurement on admission. Patients were divided into two groups based on their serum vitamin D level: with adequate vitamin D (≥ 30 ng/ml) and with low vitamin D (<30 ng/ ml). Outcomes such as death and the need for respiratory support were recorded.
Results A total of 70 patients were included. The gender; severity of COVID-19; comorbidities such as hypertension, diabetes mellitus type 2, obesity; type of respiratory support, and the length of hospital stay did not differ in both groups. Patients with low serum vitamin D levels have higher C-reactive protein levels 26.14 mg/L [Q1, Q3: 16.61, 57.79] compared to another group 13.43 mg/L [Q1, Q3: 8.84, 27.58]. Low vitamin D level was associated with an increased risk of respiratory support need OR [Odds ratio] 2.925 [95% CI, 1.0839 to 7.8931]. However, after adjustment for age, gender, and common comorbidities, it did not remain significant. Vitamin D serum levels did not significantly differ in patients who died during hospitalization compared to those who survived.
Conclusion The role of vitamin D as a sole predictor of mortality and respiratory support appears to be overestimated. Low vitamin D levels may have a greater impact on COVID-19 outcomes in hospitalized elderly patients with comorbidities.
COMPETING INTERESTS The authors have no conflicts of interest to declare. FUNDING This study did not receive any specific grant from public, commercial or not-for-profit funding agencies.
CONTRIBUTORS The authors confirm their contribution to the paper: study conception and design: All patients and/or their representatives gave informed consent. For analysis, we used datasets which were properly anonymized.
AI STATEMENT The authors confirm no generative AI or AI-assisted technology was used to generate content.
References
Adami, Giollo, Fassio, Vitamin D and disease severity in coronavirus disease 19 (COVID-19), Reumatismo, doi:10.4081/reumatismo.2020.1333
Alsafar, Grant, Hijazi, COVID-19 Disease Severity and Death in Relation to Vitamin D Status among SARS-CoV-2-Positive UAE Residents, Nutrients, doi:10.3390/nu13051714
Bouayed, Laaribi, Chatar, C-Reactive Protein (CRP): A poor prognostic biomarker in COVID-19, Front Immunol, doi:10.3389/fimmu.2022.1040024
Chen, Mei, Xie, Low vitamin D levels do not aggravate COVID-19 risk or death, and vitamin D supplementation does not improve outcomes in hospitalized patients with COVID-19: a metaanalysis and GRADE assessment of cohort studies and RCTs, Nutr J, doi:10.1186/s12937-021-00744-y
Demir, Demir, Aygun, Vitamin D deficiency is associated with COVID-19 positivity and severity of the disease, J Med Virol, doi:10.1002/jmv.26832
Dubrov, Надання медичної допомоги для лікування коронавірусної хвороби (COVID-19)» 2020-2023
Holick, Binkley, Bischoff-Ferrari, Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline [published correction appears, J Clin Endocrinol Metab, doi:10.1210/jc.2011-0385
Hossein-Nezhad, Holick, Vitamin D for health: a global perspective, Mayo Clin Proc, doi:10.1016/j.mayocp.2013.05.011
Kupisz-Urbańska, Łukaszkiewicz, Marcinowska-Suchowierska, Vitamin D in Elderly, Vitamin D, doi:10.5772/intechopen.97324
Kweder, Eidi, Vitamin D deficiency in elderly: Risk factors and drugs impact on vitamin D status, Avicenna J Med, doi:10.4103/ajm.ajm_20_18
Mendy, Apewokin, Wells, Morrow, Factors Associated with Hospitalization and Disease Severity in a Racially and Ethnically Diverse Population of COVID-19 Patients. medRxiv, doi:10.1101/2020.06.25.20137323
Pludowski, Takacs, Boyanov, Clinical Practice in the Prevention, Diagnosis and Treatment of Vitamin D Deficiency: A Central and Eastern European Expert Consensus Statement, Nutrients, doi:10.3390/nu14071483
Radujkovic, Hippchen, Tiwari-Heckler, Dreher, Boxberger, Vitamin D Deficiency and Outcome of COVID-19 Patients, Nutrients, doi:10.3390/nu12092757
Reis, Fernandes, Sales, Influence of vitamin D status on hospital length of stay and prognosis in hospitalized patients with moderate to severe COVID-19: a multicenter prospective cohort study [published correction appears, Am J Clin Nutr, doi:10.1093/ajcn/nqab151
Saponaro, Franzini, Okoye, Is There a Crucial Link Between Vitamin D Status and Inflammatory Response in Patients With COVID-19?, Front Immunol, doi:10.3389/fimmu.2021.745713
Sulli, Gotelli, Casabella, Vitamin D and Lung Outcomes in Elderly COVID-19 Patients, Nutrients, doi:10.3390/nu13030717
Wang, Zhu, Deluca, Where is the vitamin D receptor?, Arch Biochem Biophys, doi:10.1016/j.abb.2012.04.001
DOI record:
{
"DOI": "10.29390/001c.87408",
"ISSN": [
"2368-6820"
],
"URL": "http://dx.doi.org/10.29390/001c.87408",
"abstract": "<jats:sec id=\"introduction\"> <jats:title>Introduction</jats:title> <jats:p>Serum vitamin D deficiency is thought to be associated with worse clinical outcomes in COVID-19 patients.</jats:p> </jats:sec> <jats:sec id=\"methods\"> <jats:title>Methods</jats:title> <jats:p>This single-centre observational study evaluated the association between serum vitamin D levels and negative outcomes in hospitalized COVID-19 patients in Ukraine. We included hospitalized patients with COVID-19 confirmed by PCR and serum vitamin D measurement on admission. Patients were divided into two groups based on their serum vitamin D level: with adequate vitamin D (≥ 30 ng/ml) and with low vitamin D (<30 ng/ml). Outcomes such as death and the need for respiratory support were recorded.</jats:p> </jats:sec> <jats:sec id=\"results\"> <jats:title>Results</jats:title> <jats:p>A total of 70 patients were included. The gender; severity of COVID-19; comorbidities such as hypertension, diabetes mellitus type 2, obesity; type of respiratory support, and the length of hospital stay did not differ in both groups. Patients with low serum vitamin D levels have higher C-reactive protein levels 26.14 mg/L [Q1, Q3: 16.61, 57.79] compared to another group 13.43 mg/L [Q1, Q3: 8.84, 27.58]. Low vitamin D level was associated with an increased risk of respiratory support need OR [Odds ratio] 2.925 [95% CI, 1.0839 to 7.8931]. However, after adjustment for age, gender, and common comorbidities, it did not remain significant. Vitamin D serum levels did not significantly differ in patients who died during hospitalization compared to those who survived.</jats:p> </jats:sec> <jats:sec id=\"conclusion\"> <jats:title>Conclusion</jats:title> <jats:p>The role of vitamin D as a sole predictor of mortality and respiratory support appears to be overestimated. Low vitamin D levels may have a greater impact on COVID-19 outcomes in hospitalized elderly patients with comorbidities.</jats:p> </jats:sec>",
"author": [
{
"ORCID": "http://orcid.org/0000-0003-1493-6558",
"affiliation": [
{
"department": [
"Department of Internal Medicine, Faculty of Dentistry"
],
"id": [
{
"asserted-by": "publisher",
"id": "https://ror.org/03edafd86",
"id-type": "ROR"
}
],
"name": "Bogomolets National Medical University"
}
],
"authenticated-orcid": false,
"family": "Bogomaz",
"given": "Volodymyr",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0001-6201-3710",
"affiliation": [
{
"department": [
"Department of Internal Medicine, Faculty of Dentistry"
],
"id": [
{
"asserted-by": "publisher",
"id": "https://ror.org/03edafd86",
"id-type": "ROR"
}
],
"name": "Bogomolets National Medical University"
}
],
"authenticated-orcid": false,
"family": "Shatylo",
"given": "Sofiia",
"sequence": "additional"
}
],
"container-title": "Canadian Journal of Respiratory Therapy",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
8,
29
]
],
"date-time": "2023-08-29T14:54:40Z",
"timestamp": 1693320880000
},
"deposited": {
"date-parts": [
[
2023,
9,
6
]
],
"date-time": "2023-09-06T17:26:01Z",
"timestamp": 1694021161000
},
"indexed": {
"date-parts": [
[
2023,
9,
7
]
],
"date-time": "2023-09-07T21:10:01Z",
"timestamp": 1694121001671
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2023,
8,
24
]
]
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by-nc/4.0",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
8,
24
]
],
"date-time": "2023-08-24T00:00:00Z",
"timestamp": 1692835200000
}
}
],
"link": [
{
"URL": "https://cjrt.ca/article/87408-vitamin-d-as-a-predictor-of-negative-outcomes-in-hospitalized-covid-19-patients-an-observational-study",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "11956",
"original-title": [],
"prefix": "10.29390",
"published": {
"date-parts": [
[
2023,
8,
24
]
]
},
"published-online": {
"date-parts": [
[
2023,
8,
24
]
]
},
"publisher": "Canadian Society of Respiratory Therapists",
"reference": [
{
"article-title": "MedCalc® Statistical Software version 20.215",
"key": "ref1",
"year": "2023"
},
{
"DOI": "10.4103/ajm.ajm_20_18",
"article-title": "Vitamin D deficiency in elderly: Risk factors and drugs impact on vitamin D status",
"author": "Hasan Kweder",
"doi-asserted-by": "publisher",
"first-page": "139",
"issue": "4",
"journal-title": "Avicenna Journal of Medicine",
"key": "ref2",
"volume": "8",
"year": "2018"
},
{
"DOI": "10.5772/intechopen.97324",
"article-title": "Vitamin D in Elderly",
"author": "Malgorzata Kupisz-Urbańska",
"doi-asserted-by": "publisher",
"journal-title": "Vitamin D",
"key": "ref3",
"year": "2021"
},
{
"DOI": "10.3389/fimmu.2022.1040024",
"article-title": "C-Reactive Protein (CRP): A poor prognostic biomarker in COVID-19",
"author": "Mohamed Zakaria Bouayed",
"doi-asserted-by": "publisher",
"first-page": "1040024",
"journal-title": "Frontiers in Immunology",
"key": "ref4",
"volume": "13",
"year": "2022"
},
{
"DOI": "10.3389/fimmu.2021.745713",
"article-title": "Is There a Crucial Link Between Vitamin D Status and Inflammatory Response in Patients With COVID-19?",
"author": "Federica Saponaro",
"doi-asserted-by": "publisher",
"first-page": "745713",
"journal-title": "Frontiers in Immunology",
"key": "ref5",
"volume": "12",
"year": "2022"
},
{
"DOI": "10.1002/jmv.26832",
"article-title": "Vitamin D deficiency is associated with COVID-19 positivity and severity of the disease",
"author": "Mustafa Demir",
"doi-asserted-by": "publisher",
"first-page": "2992",
"issue": "5",
"journal-title": "Journal of Medical Virology",
"key": "ref6",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.4081/reumatismo.2020.1333",
"article-title": "Vitamin D and disease severity in coronavirus disease 19 (COVID-19)",
"author": "G. Adami",
"doi-asserted-by": "publisher",
"first-page": "189",
"issue": "4",
"journal-title": "Reumatismo",
"key": "ref7",
"volume": "72",
"year": "2021"
},
{
"DOI": "10.1093/ajcn/nqab151",
"article-title": "Influence of vitamin D status on hospital length of stay and prognosis in hospitalized patients with moderate to severe COVID-19: a multicenter prospective cohort study [published correction appears in Am J Clin Nutr. 2021 Aug 2;114(2):827]",
"author": "Bruna Z Reis",
"doi-asserted-by": "publisher",
"first-page": "598",
"issue": "2",
"journal-title": "The American Journal of Clinical Nutrition",
"key": "ref8",
"volume": "114",
"year": "2021"
},
{
"DOI": "10.3390/nu13051714",
"article-title": "COVID-19 Disease Severity and Death in Relation to Vitamin D Status among SARS-CoV-2-Positive UAE Residents",
"author": "Habiba AlSafar",
"doi-asserted-by": "publisher",
"first-page": "1714",
"issue": "5",
"journal-title": "Nutrients",
"key": "ref9",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.3390/nu13030717",
"article-title": "Vitamin D and Lung Outcomes in Elderly COVID-19 Patients",
"author": "Alberto Sulli",
"doi-asserted-by": "publisher",
"first-page": "717",
"issue": "3",
"journal-title": "Nutrients",
"key": "ref10",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.3390/nu14071483",
"article-title": "Clinical Practice in the Prevention, Diagnosis and Treatment of Vitamin D Deficiency: A Central and Eastern European Expert Consensus Statement",
"author": "Pawel Pludowski",
"doi-asserted-by": "publisher",
"first-page": "1483",
"issue": "7",
"journal-title": "Nutrients",
"key": "ref11",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1016/j.abb.2012.04.001",
"article-title": "Where is the vitamin D receptor?",
"author": "Yongji Wang",
"doi-asserted-by": "publisher",
"first-page": "123",
"issue": "1",
"journal-title": "Archives of Biochemistry and Biophysics",
"key": "ref12",
"volume": "523",
"year": "2012"
},
{
"DOI": "10.1016/j.mayocp.2013.05.011",
"article-title": "Vitamin D for health: a global perspective",
"author": "Arash Hossein-nezhad",
"doi-asserted-by": "publisher",
"first-page": "720",
"issue": "7",
"journal-title": "Mayo Clinic Proceedings",
"key": "ref13",
"volume": "88",
"year": "2013"
},
{
"DOI": "10.1101/2020.06.25.20137323",
"article-title": "Factors Associated with Hospitalization and Disease Severity in a Racially and Ethnically Diverse Population of COVID-19 Patients",
"author": "Angelico Mendy",
"doi-asserted-by": "publisher",
"journal-title": "medRxiv",
"key": "ref14",
"year": "2020"
},
{
"DOI": "10.3390/nu12092757",
"article-title": "Vitamin D Deficiency and Outcome of COVID-19 Patients",
"author": "Aleksandar Radujkovic",
"doi-asserted-by": "publisher",
"first-page": "2757",
"issue": "9",
"journal-title": "Nutrients",
"key": "ref15",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1186/s12937-021-00744-y",
"article-title": "Low vitamin D levels do not aggravate COVID-19 risk or death, and vitamin D supplementation does not improve outcomes in hospitalized patients with COVID-19: a meta-analysis and GRADE assessment of cohort studies and RCTs",
"author": "Jie Chen",
"doi-asserted-by": "publisher",
"first-page": "89",
"issue": "1",
"journal-title": "Nutrition Journal",
"key": "ref16",
"volume": "20",
"year": "2021"
},
{
"article-title": "Living guidance for clinical management of COVID-19: Living guidance",
"journal-title": "World Health Organization (WHO)",
"key": "ref17",
"year": "2021"
},
{
"article-title": "Протокол «Надання медичної допомоги для лікування коронавірусної хвороби (COVID-19)» 2020-2023 [Protocol \"Providing medical assistance for the treatment of coronavirus disease\"]",
"author": "S.O. Dubrov",
"key": "ref18"
},
{
"DOI": "10.1210/jc.2011-0385",
"article-title": "Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline [published correction appears in J Clin Endocrinol Metab. 2011 Dec;96(12):3908]",
"author": "Michael F. Holick",
"doi-asserted-by": "publisher",
"first-page": "1911",
"issue": "7",
"journal-title": "The Journal of Clinical Endocrinology & Metabolism",
"key": "ref19",
"volume": "96",
"year": "2011"
}
],
"reference-count": 19,
"references-count": 19,
"relation": {},
"resource": {
"primary": {
"URL": "https://cjrt.ca/article/87408-vitamin-d-as-a-predictor-of-negative-outcomes-in-hospitalized-covid-19-patients-an-observational-study"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Pulmonary and Respiratory Medicine",
"Health Professions (miscellaneous)"
],
"subtitle": [],
"title": "Vitamin D as a predictor of negative outcomes in hospitalized COVID-19 patients: An observational study",
"type": "journal-article",
"volume": "59"
}
