Influence of vitamin D status on hospital length of stay and prognosis in hospitalized patients with moderate to severe COVID-19: a multicenter prospective cohort study
et al., The American Journal of Clinical Nutrition, doi:10.1093/ajcn/nqab151, May 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 220 hospitalized patients in Brazil, showing no significant differences based on vitamin D levels. There was a trend (p=0.057) towards longer hospital stay for patients with levels <10ng/mL.
This is the 67th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
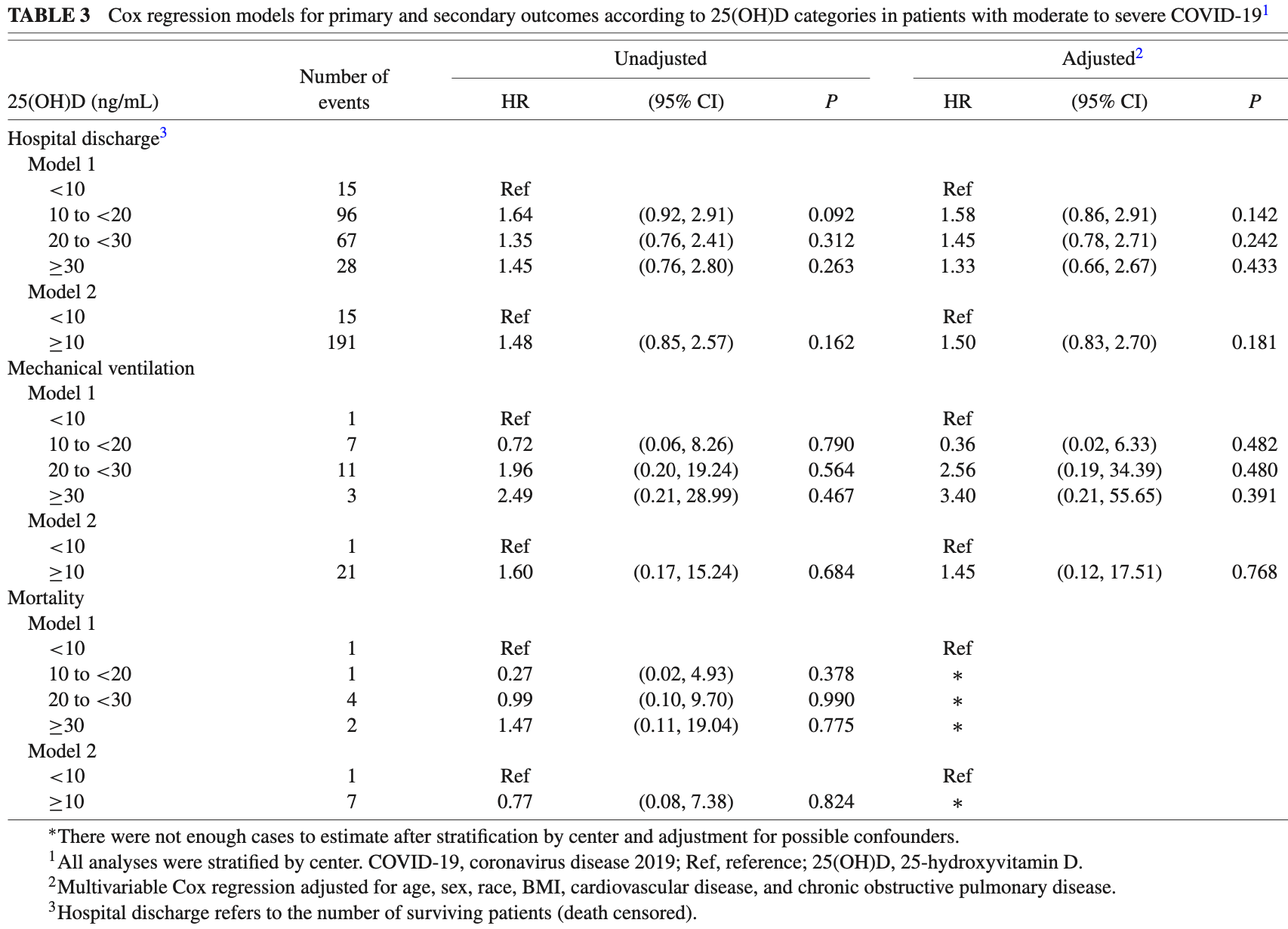
risk of death, 23.0% lower, HR 0.77, p = 0.82, high D levels (≥10ng/mL) 198, low D levels (<10ng/mL) 16, model 2, Cox proportional hazards.
|
|
risk of mechanical ventilation, 45.0% higher, HR 1.45, p = 0.77, high D levels (≥10ng/mL) 198, low D levels (<10ng/mL) 16, adjusted per study, model 2, multivariable, Cox proportional hazards.
|
|
risk of no hospital discharge, 33.3% lower, HR 0.67, p = 0.18, high D levels (≥10ng/mL) 198, low D levels (<10ng/mL) 16, adjusted per study, inverted to make HR<1 favor high D levels (≥10ng/mL), model 2, multivariable, Cox proportional hazards.
|
|
hospitalization time, 22.2% lower, relative time 0.78, p = 0.06, high D levels (≥10ng/mL) 191, low D levels (<10ng/mL) 15, model 2.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Reis et al., 21 May 2021, prospective, Brazil, peer-reviewed, 19 authors.
Influence of vitamin D status on hospital length of stay and prognosis in hospitalized patients with moderate to severe COVID-19: a multicenter prospective cohort study
doi:10.1093/ajcn/
Background: Vitamin D acts as a mediator in the immune system regulating antiviral mechanisms and inflammatory processes. Vitamin D insufficiency has been suggested as a potential risk factor for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection, although its impact on the prognosis of hospitalized patients with coronavirus disease 2019 (COVID-19) remains unclear. Objective: This multicenter prospective cohort study was designed to investigate whether serum 25-hydroxyvitamin D [25(OH)D] concentration is associated with hospital length of stay and prognosis in hospitalized patients with COVID-19. Methods: Patients with moderate to severe COVID-19 (n = 220) were recruited from 2 hospitals in Sao Paulo, Brazil. Serum 25(OH)D concentrations were categorized as follows: <10 ng/mL, 10 to <20 ng/mL, 20 to <30 ng/mL, and ≥30 ng/mL, and <10 ng/mL and ≥10 ng/mL. The primary outcome was hospital length of stay and the secondary outcomes were the rate of patients who required invasive mechanical ventilation and mortality. Results: There were no significant differences in hospital length of stay when the 4 25(OH)D categories were compared (P = 0.120). Patients exhibiting 25(OH)D <10 ng/mL showed a trend (P = 0.057) for longer hospital length of stay compared with those with 25(OH)D ≥10 ng/mL [9.0 d (95% CI: 6.4, 11.6 d) vs. 7.0 d (95% CI: 6.6, 7.4 d)]. The multivariable Cox proportional hazard models showed no significant associations between 25(OH)D and primary or secondary outcomes. Conclusions: Among hospitalized patients with moderate to severe COVID-19, those with severe 25(OH)D deficiency (<10 ng/mL) exhibited a trend for longer hospital length of stay compared with patients with higher 25(OH)D concentrations. This association was not significant in the multivariable Cox regression model. Prospective studies should test whether correcting severe 25(OH)D deficiency could improve the prognosis of patients with COVID-19.
References
Abrishami, Dalili, Torbati, Asgari, Arab-Ahmadi et al., Possible association of vitamin D status with lung involvement and outcome in patients with COVID-19: a retrospective study, Eur J Nutr, doi:10.1007/s00394-020-02411-0
Aibana, Huang, Aboud, Arnedo-Pena, Becerra et al., systematic review, and individual-participant data meta-analysis
Alexander, Tinkov, Strand, Alehagen, Skalny et al., Early nutritional interventions with zinc, selenium and vitamin D for raising anti-viral resistance against progressive COVID-19, Nutrients
Autier, Boniol, Pizot, Mullie, Vitamin D status and ill health: a systematic review, Lancet Diabetes Endocrinol
Baktash, Hosack, Patel, Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad Med J, doi:10.1136/postgradmedj-2020-138712
Bilezikian, Bikle, Hewison, Lazaretti-Castro, Formenti et al., Mechanisms in endocrinology: vitamin D and COVID-19, Eur J Endocrinol
Brenner, Holleczek, Schöttker, Vitamin D insufficiency and deficiency and mortality from respiratory diseases in a cohort of older adults: potential for limiting the death toll during and beyond the COVID-19 pandemic?, Nutrients
Cereda, Bogliolo, Klersy, Lobascio, Masi et al., Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital, Clin Nutr
Daneshkhah, Agrawal, Eshein, Subramanian, Roy et al., Evidence for possible association of vitamin D status with cytokine storm and unregulated inflammation in COVID-19 patients, Aging Clin Exp Res
Hars, Mendes, Serratrice, Herrmann, Gold et al., Sex-specific association between vitamin D deficiency and COVID-19 mortality in older patients, Osteoporos Int
Hernández, Nan, Fernandez-Ayala, García-Unzueta, Hernández-Hernández et al., Vitamin D status in hospitalized patients with SARS-CoV-2 infection, J Clin Endocrinol Metab, doi:10.1210/clinem/dgaa733
Kaufman, Niles, Kroll, Bi, Holick, SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels, PLoS One
Laird, Rhodes, Kenny, Vitamin D and inflammation: potential implications for severity of Covid-19, Ir Med J
Lips, Cashman, Lamberg-Allardt, Bischoff-Ferrari, Obermayer-Pietsch et al., Management of endocrine disease: current vitamin D status in European and Middle East countries and strategies to prevent vitamin D deficiency; a position statement of the European Calcified Tissue Society, Eur J Endocrinol
Luo, Liao, Shen, Li, Cheng, Vitamin D deficiency is inversely associated with COVID-19 incidence and disease severity in Chinese people, J Nutr
Macaya, Espejo, Valls, Fernández-Ortiz, Del Castillo et al., Interacción entre la edad y el déficit de vitamina D en la COVID-19 grave, Nutr Hosp
Maghbooli, Sahraian, Ebrahimi, Pazoki, Kafan et al., Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection, PLoS One
Martineau, Forouhi, Vitamin D for COVID-19: a case to answer?, Lancet Diabetes Endocrinol
Meltzer, Best, Zhang, Vokes, Arora et al., Association of vitamin D status and other clinical characteristics with COVID-19 test results, JAMA Netw Open
Mitchell, Vitamin-D and COVID-19: do deficient risk a poorer outcome?, Lancet Diabetes Endocrinol
Murai, Fernandes, Sales, Pinto, Goessler et al., Effect of a single high dose of vitamin D3 on hospital length of stay in patients with moderate to severe COVID-19: a randomized clinical trial, JAMA
Pecora, Persico, Argentiero, Neglia, Esposito, The role of micronutrients in support of the immune response against viral infections, Nutrients
Pizzini, Aichner, Sahanic, Bohm, Egger et al., Impact of vitamin D deficiency on COVID-19-a prospective analysis from the CovILD Registry, Nutrients
Quesada-Gomez, Castillo, Bouillon, Vitamin D receptor stimulation to reduce acute respiratory distress syndrome (ARDS) in patients with coronavirus SARS-CoV-2 infections, J Steroid Biochem Mol Biol
Rosa, Malaguarnera, Nicoletti, Malaguarnera, Vitamin D3: a helpful immuno-modulator, Immunology
Sabetta, Depetrillo, Cipriani, Smardin, Burns et al., Serum 25-hydroxyvitamin D and the incidence of acute viral respiratory tract infections in healthy adults, PLoS One
Silva, Furlanetto, Does serum 25-hydroxyvitamin D decrease during acute-phase response? A systematic review, Nutr Res
Szeto, Zucker, Lasota, Rubin, Walker et al., Vitamin D status and COVID-19 clinical outcomes in hospitalized patients, Endocr Res
Who, Obesity: preventing and managing the global epidemic
Who, WHO coronavirus disease (COVID-19) dashboard
Ye, Tang, Liao, Shaw, Deng et al., Does serum vitamin D level affect COVID-19 infection and its severity? A case-control study, J Am Coll Nutr, doi:10.1080/07315724.2020.1826005
Zhang, Leung, Richers, Liu, Remigio et al., Vitamin D inhibits monocyte/macrophage proinflammatory cytokine production by targeting MAPK phosphatase-1, J Immunol
DOI record:
{
"DOI": "10.1093/ajcn/nqab151",
"ISSN": [
"0002-9165",
"1938-3207"
],
"URL": "http://dx.doi.org/10.1093/ajcn/nqab151",
"abstract": "<jats:title>ABSTRACT</jats:title>\n <jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>Vitamin D acts as a mediator in the immune system regulating antiviral mechanisms and inflammatory processes. Vitamin D insufficiency has been suggested as a potential risk factor for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection, although its impact on the prognosis of hospitalized patients with coronavirus disease 2019 (COVID-19) remains unclear.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>Objective</jats:title>\n <jats:p>This multicenter prospective cohort study was designed to investigate whether serum 25-hydroxyvitamin D [25(OH)D] concentration is associated with hospital length of stay and prognosis in hospitalized patients with COVID-19.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>Methods</jats:title>\n <jats:p>Patients with moderate to severe COVID-19 (n = 220) were recruited from 2 hospitals in Sao Paulo, Brazil. Serum 25(OH)D concentrations were categorized as follows: &lt;10 ng/mL, 10 to &lt;20 ng/mL, 20 to &lt;30 ng/mL, and ≥30 ng/mL, and &lt;10 ng/mL and ≥10 ng/mL. The primary outcome was hospital length of stay and the secondary outcomes were the rate of patients who required invasive mechanical ventilation and mortality.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>There were no significant differences in hospital length of stay when the 4 25(OH)D categories were compared (P = 0.120). Patients exhibiting 25(OH)D &lt;10 ng/mL showed a trend (P = 0.057) for longer hospital length of stay compared with those with 25(OH)D ≥10 ng/mL [9.0 d (95% CI: 6.4, 11.6 d) vs. 7.0 d (95% CI: 6.6, 7.4 d)]. The multivariable Cox proportional hazard models showed no significant associations between 25(OH)D and primary or secondary outcomes.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>Conclusions</jats:title>\n <jats:p>Among hospitalized patients with moderate to severe COVID-19, those with severe 25(OH)D deficiency (&lt;10 ng/mL) exhibited a trend for longer hospital length of stay compared with patients with higher 25(OH)D concentrations. This association was not significant in the multivariable Cox regression model. Prospective studies should test whether correcting severe 25(OH)D deficiency could improve the prognosis of patients with COVID-19.</jats:p>\n </jats:sec>",
"author": [
{
"ORCID": "http://orcid.org/0000-0001-8726-8699",
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"authenticated-orcid": false,
"family": "Reis",
"given": "Bruna Z",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-6786-3922",
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"authenticated-orcid": false,
"family": "Fernandes",
"given": "Alan L",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Sales",
"given": "Lucas P",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Santos",
"given": "Mayara D",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "dos Santos",
"given": "Caroline C",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Applied Physiology and Nutrition Research Group, Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Pinto",
"given": "Ana J",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Applied Physiology and Nutrition Research Group, Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Goessler",
"given": "Karla F",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Franco",
"given": "Andre S",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Duran",
"given": "Camila S C",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Silva",
"given": "Carla B R",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Macêdo",
"given": "Marina B",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Dalmolin",
"given": "Henrique H H",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Baggio",
"given": "Janaína",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Balbi",
"given": "Guilherme G M",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Clinical Pathology Division, Hospital das Clinicas HCFMUSP, Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Antonangelo",
"given": "Leila",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"family": "Caparbo",
"given": "Valeria F",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-7100-8681",
"affiliation": [
{
"name": "Applied Physiology and Nutrition Research Group, Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
},
{
"name": "Food Research Center, Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"authenticated-orcid": false,
"family": "Gualano",
"given": "Bruno",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-0077-5004",
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"authenticated-orcid": false,
"family": "Murai",
"given": "Igor H",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-3723-5028",
"affiliation": [
{
"name": "Rheumatology Division, Hospital das Clinicas da Faculdade de Medicina da Universidade de Sao Paulo (HCFMUSP), Faculdade de Medicina da Universidade de Sao Paulo, Sao Paulo, Brazil"
}
],
"authenticated-orcid": false,
"family": "Pereira",
"given": "Rosa M R",
"sequence": "additional"
}
],
"container-title": [
"The American Journal of Clinical Nutrition"
],
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2021,
4,
11
]
],
"date-time": "2021-04-11T11:07:07Z",
"timestamp": 1618139227000
},
"deposited": {
"date-parts": [
[
2021,
8,
2
]
],
"date-time": "2021-08-02T00:03:53Z",
"timestamp": 1627862633000
},
"funder": [
{
"DOI": "10.13039/501100001807",
"award": [
"20/05752-4",
"19/24782-4",
"20/11102-2",
"16/00006-7",
"17/13552-2",
"15/26937-4",
"19/18039-7"
],
"doi-asserted-by": "publisher",
"name": "FAPESP"
},
{
"DOI": "10.13039/501100003593",
"award": [
"305556/2017-7"
],
"doi-asserted-by": "publisher",
"name": "Conselho Nacional de Desenvolvimento Científico e Tecnológico"
},
{
"DOI": "10.13039/501100002322",
"award": [
"88887.507119/2020-00"
],
"doi-asserted-by": "publisher",
"name": "CAPES"
}
],
"indexed": {
"date-parts": [
[
2021,
12,
11
]
],
"date-time": "2021-12-11T11:56:19Z",
"timestamp": 1639223779337
},
"is-referenced-by-count": 4,
"issn-type": [
{
"type": "print",
"value": "0002-9165"
},
{
"type": "electronic",
"value": "1938-3207"
}
],
"issue": "2",
"issued": {
"date-parts": [
[
2021,
5,
21
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2021,
5,
21
]
]
},
"published-print": {
"date-parts": [
[
2021,
8,
2
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://academic.oup.com/journals/pages/open_access/funder_policies/chorus/standard_publication_model",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
21
]
],
"date-time": "2021-05-21T00:00:00Z",
"timestamp": 1621555200000
}
}
],
"link": [
{
"URL": "http://academic.oup.com/ajcn/article-pdf/114/2/598/39510655/nqab151.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "syndication"
},
{
"URL": "http://academic.oup.com/ajcn/article-pdf/114/2/598/39510655/nqab151.pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "286",
"original-title": [],
"page": "598-604",
"prefix": "10.1093",
"published": {
"date-parts": [
[
2021,
5,
21
]
]
},
"published-online": {
"date-parts": [
[
2021,
5,
21
]
]
},
"published-other": {
"date-parts": [
[
2021,
8
]
]
},
"published-print": {
"date-parts": [
[
2021,
8,
2
]
]
},
"publisher": "Oxford University Press (OUP)",
"reference": [
{
"author": "WHO",
"journal-title": "WHO coronavirus disease (COVID-19) dashboard",
"key": "2021080200013914300_bib1",
"year": "2020"
},
{
"DOI": "10.3390/nu12082488",
"article-title": "Vitamin D insufficiency and deficiency and mortality from respiratory diseases in a cohort of older adults: potential for limiting the death toll during and beyond the COVID-19 pandemic?",
"author": "Brenner",
"doi-asserted-by": "crossref",
"first-page": "2488",
"issue": "8",
"journal-title": "Nutrients",
"key": "2021080200013914300_bib2",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3390/nu12082358",
"article-title": "Early nutritional interventions with zinc, selenium and vitamin D for raising anti-viral resistance against progressive COVID-19",
"author": "Alexander",
"doi-asserted-by": "crossref",
"first-page": "2358",
"issue": "8",
"journal-title": "Nutrients",
"key": "2021080200013914300_bib3",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.3390/nu12103198",
"article-title": "The role of micronutrients in support of the immune response against viral infections",
"author": "Pecora",
"doi-asserted-by": "crossref",
"first-page": "3198",
"issue": "10",
"journal-title": "Nutrients",
"key": "2021080200013914300_bib4",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1530/EJE-20-0665",
"article-title": "Mechanisms in endocrinology: vitamin D and COVID-19",
"author": "Bilezikian",
"doi-asserted-by": "crossref",
"first-page": "R133",
"issue": "5",
"journal-title": "Eur J Endocrinol",
"key": "2021080200013914300_bib5",
"volume": "183",
"year": "2020"
},
{
"DOI": "10.1111/j.1365-2567.2011.03482.x",
"article-title": "Vitamin D3: a helpful immuno-modulator",
"author": "Di Rosa",
"doi-asserted-by": "crossref",
"first-page": "123",
"issue": "2",
"journal-title": "Immunology",
"key": "2021080200013914300_bib6",
"volume": "134",
"year": "2011"
},
{
"DOI": "10.4049/jimmunol.1102412",
"article-title": "Vitamin D inhibits monocyte/macrophage proinflammatory cytokine production by targeting MAPK phosphatase-1",
"author": "Zhang",
"doi-asserted-by": "crossref",
"first-page": "2127",
"issue": "5",
"journal-title": "J Immunol",
"key": "2021080200013914300_bib7",
"volume": "188",
"year": "2012"
},
{
"DOI": "10.1016/S2213-8587(13)70165-7",
"article-title": "Vitamin D status and ill health: a systematic review",
"author": "Autier",
"doi-asserted-by": "crossref",
"first-page": "76",
"issue": "1",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "2021080200013914300_bib8",
"volume": "2",
"year": "2014"
},
{
"DOI": "10.1371/journal.pmed.1002907",
"article-title": "Vitamin D status and risk of incident tuberculosis disease: a nested case-control study, systematic review, and individual-participant data meta-analysis",
"author": "Aibana",
"doi-asserted-by": "crossref",
"first-page": "e1002907",
"issue": "9",
"journal-title": "PLoS Med",
"key": "2021080200013914300_bib9",
"volume": "16",
"year": "2019"
},
{
"DOI": "10.1371/journal.pone.0011088",
"article-title": "Serum 25-hydroxyvitamin D and the incidence of acute viral respiratory tract infections in healthy adults",
"author": "Sabetta",
"doi-asserted-by": "crossref",
"first-page": "e11088",
"issue": "6",
"journal-title": "PLoS One",
"key": "2021080200013914300_bib10",
"volume": "5",
"year": "2010"
},
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"article-title": "Association of vitamin D status and other clinical characteristics with COVID-19 test results",
"author": "Meltzer",
"doi-asserted-by": "crossref",
"first-page": "e2019722",
"issue": "9",
"journal-title": "JAMA Netw Open",
"key": "2021080200013914300_bib11",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0239252",
"article-title": "SARS-CoV-2 positivity rates associated with circulating 25-hydroxyvitamin D levels",
"author": "Kaufman",
"doi-asserted-by": "crossref",
"first-page": "e0239252",
"issue": "9",
"journal-title": "PLoS One",
"key": "2021080200013914300_bib12",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1080/07315724.2020.1826005",
"article-title": "Does serum vitamin D level affect COVID-19 infection and its severity? A case-control study",
"author": "Ye",
"doi-asserted-by": "crossref",
"journal-title": "J Am Coll Nutr",
"key": "2021080200013914300_bib13",
"year": "2020"
},
{
"DOI": "10.1007/s40520-020-01677-y",
"article-title": "Evidence for possible association of vitamin D status with cytokine storm and unregulated inflammation in COVID-19 patients",
"author": "Daneshkhah",
"doi-asserted-by": "crossref",
"first-page": "2141",
"issue": "10",
"journal-title": "Aging Clin Exp Res",
"key": "2021080200013914300_bib14",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1007/s00198-020-05677-6",
"article-title": "Sex-specific association between vitamin D deficiency and COVID-19 mortality in older patients",
"author": "Hars",
"doi-asserted-by": "crossref",
"first-page": "2495",
"journal-title": "Osteoporos Int",
"key": "2021080200013914300_bib15",
"volume": "31",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0239799",
"article-title": "Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection",
"author": "Maghbooli",
"doi-asserted-by": "crossref",
"first-page": "e0239799",
"issue": "9",
"journal-title": "PLoS One",
"key": "2021080200013914300_bib16",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1136/postgradmedj-2020-138712",
"article-title": "Vitamin D status and outcomes for hospitalised older patients with COVID-19",
"author": "Baktash",
"doi-asserted-by": "crossref",
"journal-title": "Postgrad Med J",
"key": "2021080200013914300_bib17",
"year": "2020"
},
{
"article-title": "Vitamin D status in hospitalized patients with SARS-CoV-2 infection",
"author": "Hernández",
"journal-title": "J Clin Endocrinol Metab",
"key": "2021080200013914300_bib18",
"year": "2020"
},
{
"DOI": "10.3390/nu12092775",
"article-title": "Impact of vitamin D deficiency on COVID-19—a prospective analysis from the CovILD Registry",
"author": "Pizzini",
"doi-asserted-by": "crossref",
"first-page": "2775",
"issue": "9",
"journal-title": "Nutrients",
"key": "2021080200013914300_bib19",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/j.clnu.2020.10.055",
"article-title": "Vitamin D 25OH deficiency in COVID-19 patients admitted to a tertiary referral hospital",
"author": "Cereda",
"doi-asserted-by": "crossref",
"first-page": "2469",
"issue": "4",
"journal-title": "Clin Nutr",
"key": "2021080200013914300_bib20",
"volume": "40",
"year": "2021"
},
{
"author": "NIH",
"key": "2021080200013914300_bib21",
"volume-title": "Coronavirus disease 2019 (COVID-19) treatment guidelines",
"year": "2020"
},
{
"article-title": "Obesity: preventing and managing the global epidemic",
"author": "WHO",
"key": "2021080200013914300_bib22",
"year": "2000"
},
{
"DOI": "10.1530/EJE-18-0736",
"article-title": "Management of endocrine disease: current vitamin D status in European and Middle East countries and strategies to prevent vitamin D deficiency; a position statement of the European Calcified Tissue Society",
"author": "Lips",
"doi-asserted-by": "crossref",
"first-page": "P23",
"issue": "4",
"journal-title": "Eur J Endocrinol",
"key": "2021080200013914300_bib23",
"volume": "180",
"year": "2019"
},
{
"DOI": "10.1016/j.jsbmb.2020.105719",
"article-title": "Vitamin D receptor stimulation to reduce acute respiratory distress syndrome (ARDS) in patients with coronavirus SARS-CoV-2 infections",
"author": "Quesada-Gomez",
"doi-asserted-by": "crossref",
"first-page": "105719",
"journal-title": "J Steroid Biochem Mol Biol",
"key": "2021080200013914300_bib24",
"volume": "202",
"year": "2020"
},
{
"article-title": "Vitamin D and inflammation: potential implications for severity of Covid-19",
"author": "Laird",
"first-page": "81",
"issue": "5",
"journal-title": "Ir Med J",
"key": "2021080200013914300_bib25",
"volume": "113",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30183-2",
"article-title": "Vitamin-D and COVID-19: do deficient risk a poorer outcome?",
"author": "Mitchell",
"doi-asserted-by": "crossref",
"first-page": "570",
"issue": "7",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "2021080200013914300_bib26",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30268-0",
"article-title": "Vitamin D for COVID-19: a case to answer?",
"author": "Martineau",
"doi-asserted-by": "crossref",
"first-page": "735",
"issue": "9",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "2021080200013914300_bib27",
"volume": "8",
"year": "2020"
},
{
"article-title": "Possible association of vitamin D status with lung involvement and outcome in patients with COVID-19: a retrospective study",
"author": "Abrishami",
"first-page": "1",
"journal-title": "Eur J Nutr",
"key": "2021080200013914300_bib28",
"year": "2020"
},
{
"DOI": "10.1093/jn/nxaa332",
"article-title": "Vitamin D deficiency is inversely associated with COVID-19 incidence and disease severity in Chinese people",
"author": "Luo",
"doi-asserted-by": "crossref",
"first-page": "98",
"issue": "1",
"journal-title": "J Nutr",
"key": "2021080200013914300_bib29",
"volume": "151",
"year": "2021"
},
{
"article-title": "Interacción entre la edad y el déficit de vitamina D en la COVID-19 grave",
"author": "Macaya",
"first-page": "1039",
"issue": "5",
"journal-title": "Nutr Hosp",
"key": "2021080200013914300_bib30",
"volume": "37",
"year": "2020"
},
{
"DOI": "10.1016/j.nutres.2014.12.008",
"article-title": "Does serum 25-hydroxyvitamin D decrease during acute-phase response? A systematic review",
"author": "Silva",
"doi-asserted-by": "crossref",
"first-page": "91",
"issue": "2",
"journal-title": "Nutr Res",
"key": "2021080200013914300_bib31",
"volume": "35",
"year": "2015"
},
{
"DOI": "10.1080/07435800.2020.1867162",
"article-title": "Vitamin D status and COVID-19 clinical outcomes in hospitalized patients",
"author": "Szeto",
"doi-asserted-by": "crossref",
"first-page": "66",
"issue": "2",
"journal-title": "Endocr Res",
"key": "2021080200013914300_bib32",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.26848",
"article-title": "Effect of a single high dose of vitamin D3 on hospital length of stay in patients with moderate to severe COVID-19: a randomized clinical trial",
"author": "Murai",
"doi-asserted-by": "crossref",
"first-page": "1053",
"issue": "11",
"journal-title": "JAMA",
"key": "2021080200013914300_bib33",
"volume": "325",
"year": "2021"
}
],
"reference-count": 33,
"references-count": 33,
"relation": {},
"score": 1,
"short-container-title": [],
"short-title": [],
"source": "Crossref",
"subject": [
"Nutrition and Dietetics",
"Medicine (miscellaneous)"
],
"subtitle": [],
"title": [
"Influence of vitamin D status on hospital length of stay and prognosis in hospitalized patients with moderate to severe COVID-19: a multicenter prospective cohort study"
],
"type": "journal-article",
"volume": "114"
}
