Relationship between antidepressants and severity of SARS-CoV-2 Omicron infection: a retrospective cohort study using real-world data
et al., The Lancet Regional Health - Western Pacific, doi:10.1016/j.lanwpc.2023.100716, Feb 2023
30th treatment shown to reduce risk in
November 2021, now with p = 0.00014 from 21 studies, recognized in 2 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
PSM retrospective 60,903 hospitalized COVID-19 patients in Hong Kong, showing antidepressants associated with lower mortality, including for SSRIs, and for FIASMA antidepressants.
9 meta-analyses show significant improvements with fluvoxamine for mortality1-3,
hospitalization1,4-8 ,
progression2,8, and
severity9.
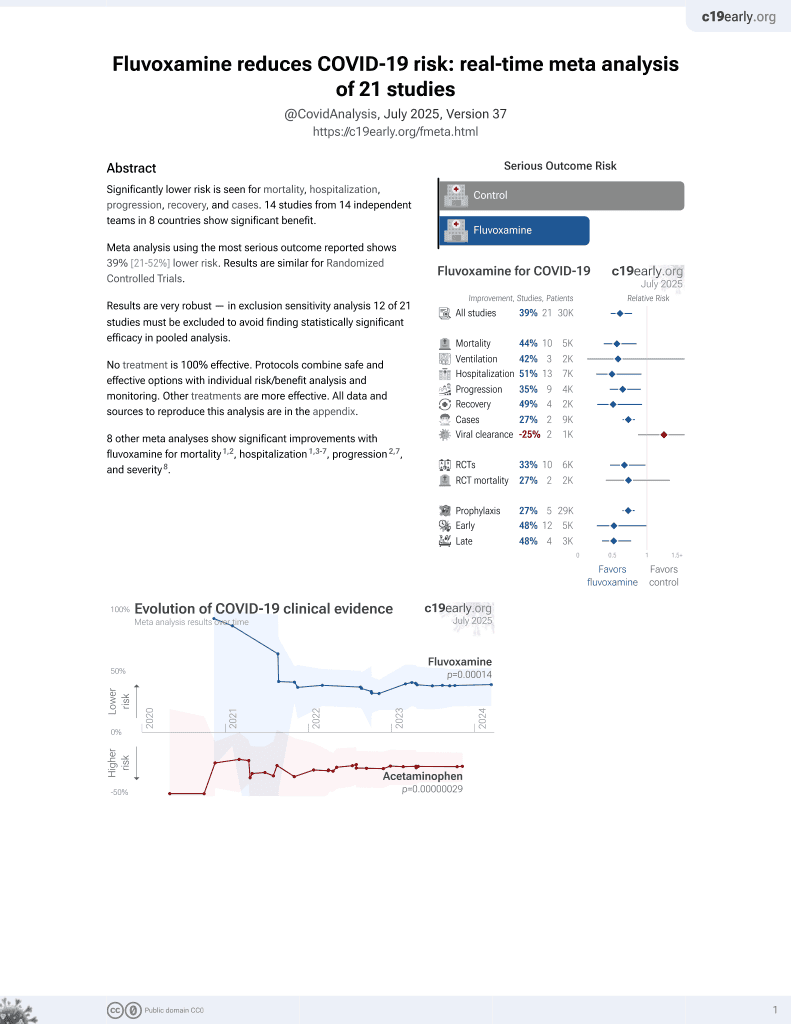
Currently there are 21 fluvoxamine for COVID-19 studies, showing 44% lower mortality [15‑63%], 42% lower ventilation [-151‑86%], 10% higher ICU admission [-72‑326%], 51% lower hospitalization [14‑72%], and 27% fewer cases [18‑35%].
1.
Deng et al., Efficacy and safety of selective serotonin reuptake inhibitors in COVID-19 management: A systematic review and meta-analysis, Clinical Microbiology and Infection, doi:10.1016/j.cmi.2023.01.010.
2.
Prasanth et al., A systematic review and meta-analysis, investigating dose and time of fluvoxamine treatment efficacy for COVID-19 clinical deterioration, death, and Long-COVID complications, Scientific Reports, doi:10.1038/s41598-024-64260-9.
3.
Fico et al., Psychotropic drug repurposing for COVID-19: A Systematic Review and Meta-Analysis, European Neuropsychopharmacology, doi:10.1016/j.euroneuro.2022.10.004.
4.
Lee et al., Fluvoxamine for Outpatient Management of COVID-19 to Prevent Hospitalization: A Systematic Review and Meta-analysis, JAMA Network Open, doi:10.1001/jamanetworkopen.2022.6269.
5.
Lu et al., Effect of fluvoxamine on outcomes of nonhospitalized patients with COVID-19: A systematic review and meta-analysis, Journal of Infection and Public Health, doi:10.1016/j.jiph.2022.10.010.
6.
Marcec et al., A meta-analysis regarding fluvoxamine and hospitalization risk of COVID-19 patients: TOGETHER making a difference, Journal of Infection, doi:10.1016/j.jinf.2022.11.011.
7.
Deng (B) et al., Evaluating fluvoxamine for the outpatient treatment of COVID‐19: A systematic review and meta‐analysis, Reviews in Medical Virology, doi:10.1002/rmv.2501.
Wang et al., 27 Feb 2023, retrospective, China, peer-reviewed, 15 authors.
Relationship between antidepressants and severity of SARS-CoV-2 Omicron infection: a retrospective cohort study using real-world data
The Lancet Regional Health - Western Pacific, doi:10.1016/j.lanwpc.2023.100716
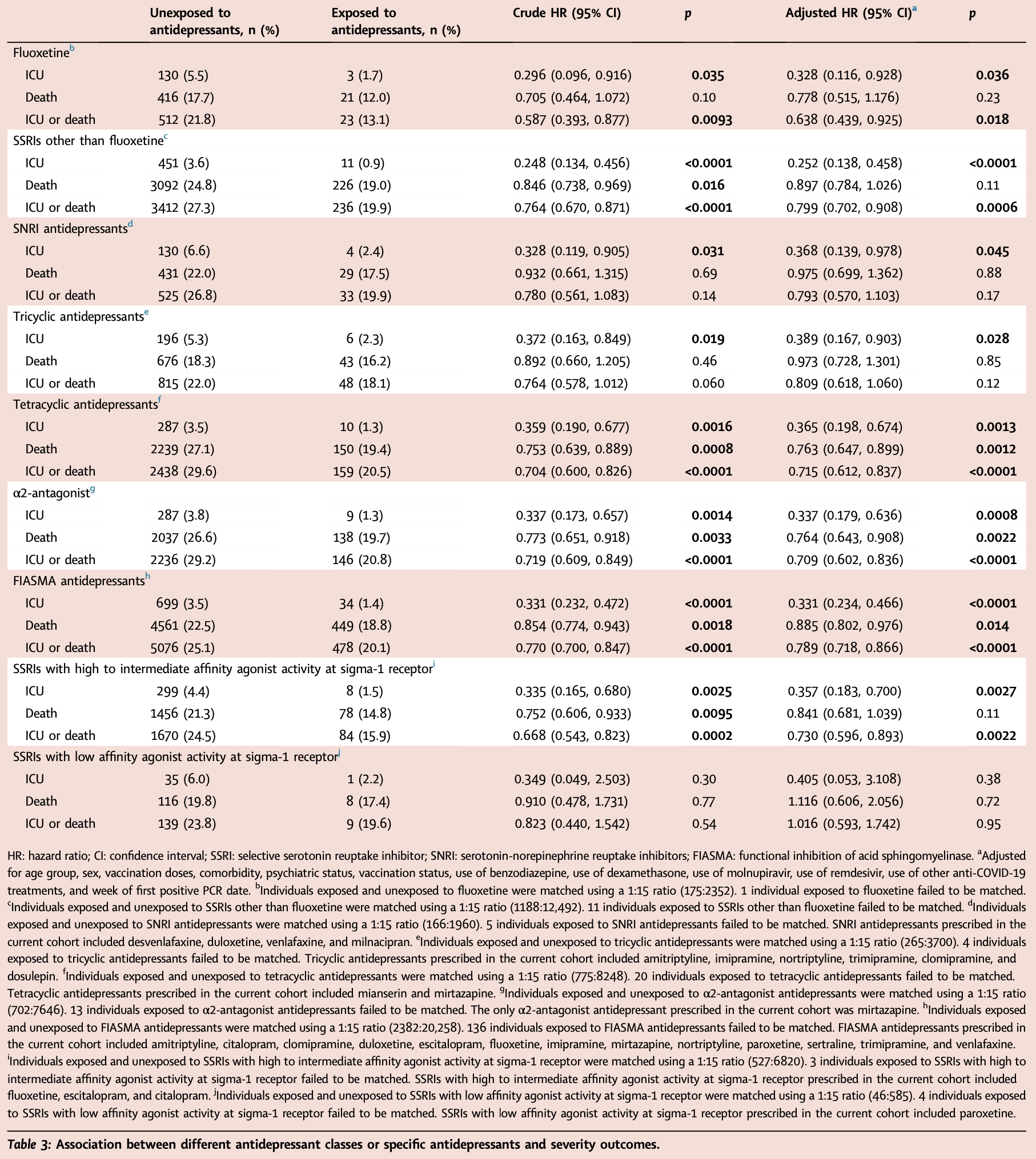
Background Few studies have used real-world data to evaluate the impact of antidepressant use on the risk of developing severe outcomes after SARS-CoV-2 Omicron infection. Methods This is a retrospective cohort study using propensity-score matching to examine the relationship between antidepressant use and COVID-19 severity. Inpatient and medication records of all adult COVID-19 patients in Hong Kong during the Omicron-predominated period were obtained. Severe clinical outcomes including intensive care unit admission and inpatient death after the first positive results of reverse transcription polymerase chain reaction as well as a composite outcome of both were studied. Cox proportional hazard models were applied to estimate the crude and adjusted hazard ratios (HR). Findings Of 60,903 hospitalised COVID-19 patients admitted, 40,459 were included for matching, among which 3821 (9.4%) were prescribed antidepressants. The rates of intensive care unit admission, inpatient death, and the composite event were 3.9%, 25.5%, and 28.3% respectively in the unexposed group, 1.3%, 20.0%, and 21.1% respectively in the exposed group, with adjusted HR equal to 0.332 (95% CI, 0.245-0.449), 0.868 (95% CI, 0.800-0.942), and 0.786 (95% CI, 0.727-0.850) respectively. The result was generally consistent when stratified by selective serotonin reuptake inhibitors (SSRIs) and non-SSRIs. Antidepressants with functional inhibition of acid sphingomyelinase activity, specifically fluoxetine, were also negatively associated with the outcomes. The effect of antidepressants was more apparent in female and fully vaccinated COVID-19 patients. Interpretation Antidepressant use was associated with a lower risk of severe COVID-19. The findings support the continuation of antidepressants in patients with COVID-19, and provide evidence for the treatment potential of antidepressants for severe COVID-19.
Ethics approval and consent to participate This was an observational study based on identity-masked datasets provided by the Department of Health, The Government of the Hong Kong Special Administrative Region. Ethics approval was obtained from the Joint CUHK-NTEC Clinical Research Ethics Committee, The Chinese University of Hong Kong. As this study was a retrospective analysis using secondary data without any personal information, the requirement for obtaining informed consent was waived.
Declaration of interests All authors declare no competing interests. Appendix A. Supplementary data Supplementary data related to this article can be found at https://doi. org/10.1016/j.lanwpc.2023.100716.
References
Anderson, Fluvoxamine, melatonin and COVID-19, Psychopharmacology
Anttila, Leinonen, A review of the pharmacological and clinical profile of mirtazapine, CNS Drug Rev
Austin, Optimal caliper widths for propensity-score matching when estimating differences in means and differences in proportions in observational studies, Pharm Stat
Austin, Some methods of propensity-score matching had superior performance to others: results of an empirical investigation and Monte Carlo simulations, Biom J
Austin, Statistical criteria for selecting the optimal number of untreated subjects matched to each treated subject when using many-to-one matching on the propensity score, Am J Epidemiol
Austin, Using the standardized difference to Compare the prevalence of a binary variable between two groups in observational research, Commun Stat Simulat Comput
Bramante, Huling, Tignanelli, Randomized trial of metformin, ivermectin, and fluvoxamine for Covid-19, N Engl J Med
Brody, Gu, Antidepressant use among adults: United States, 2015-2018, NCHS Data Brief
Bryce, Mathias, Harrison, Watanabe, Geha et al., The H1 histamine receptor regulates allergic lung responses, J Clin Invest
Bushnell, Stürmer, Gaynes, Pate, Miller, Simultaneous antidepressant and benzodiazepine new use and subsequent long-term benzodiazepine use in adults with depression, United States, 2001-2014, JAMA Psychiatr
Fritz, Hoertel, Lenze, Jalali, Reiersen, Association between antidepressant use and ED or hospital visits in outpatients with SARS-CoV-2, Transl Psychiatry
Gulbins, Palmada, Reichel, Acid sphingomyelinaseceramide system mediates effects of antidepressant drugs, Nat Med
Hammond, Leister-Tebbe, Gardner, Oral nirmatrelvir for high-risk, nonhospitalized adults with Covid-19, N Engl J Med
Hannestad, Dellagioia, Bloch, The effect of antidepressant medication treatment on serum levels of inflammatory cytokines: a meta-analysis, Neuropsychopharmacology
Hashimoto, Repurposing of CNS drugs to treat COVID-19 infection: targeting the sigma-1 receptor, Eur Arch Psychiatr Clin Neurosci
Hoertel, Boulware, Sánchez-Rico, Burgun, Limosin, Prevalence of contraindications to nirmatrelvir-ritonavir among hospitalized patients with COVID-19 at risk for progression to severe disease, JAMA Netw Open
Hoertel, Do the selective serotonin reuptake inhibitor antidepressants fluoxetine and fluvoxamine reduce mortality among patients with COVID-19?, JAMA Netw Open
Hoertel, Sánchez-Rico, Gulbins, Association between FIASMA psychotropic medications and reduced risk of intubation or death in individuals with psychiatric disorders hospitalized for severe COVID-19: an observational multicenter study, Transl Psychiatry
Hoertel, Sánchez-Rico, Gulbins, Association between FIASMAs and reduced risk of intubation or death in individuals hospitalized for severe COVID-19: an observational multicenter study, Clin Pharmacol Ther
Hoertel, Sánchez-Rico, Gulbins, Association between benzodiazepine receptor agonist use and mortality in patients hospitalised for COVID-19: a multicentre observational study, Epidemiol Psychiatr Sci
Hoertel, Sánchez-Rico, Kornhuber, Antidepressant use and its association with 28-day mortality in inpatients with SARS-CoV-2: support for the FIASMA model against COVID-19, J Clin Med
Hoertel, Sánchez-Rico, Vernet, Association between antidepressant use and reduced risk of intubation or death in hospitalized patients with COVID-19: results from an observational study, Mol Psychiatr
Jilani, Gibbons, Faizy, Saadabadi, Mirtazapine. Stat-Pearls. Treasure Island
Jutel, Watanabe, Klunker, Histamine regulates T-cell and antibody responses by differential expression of H1 and H2 receptors, Nature
Khan, Brodhead, Schwartz, Kolts, Brown, Sex differences in antidepressant response in recent antidepressant clinical trials, J Clin Psychopharmacol
Kornhuber, Hoertel, Gulbins, The acid sphingomyelinase/ ceramide system in COVID-19, Mol Psychiatr
Kuehn, Persistent disparities in COVID-19 antiviral dispensing, JAMA
Köseler, Sabirli, Gören, Türkçüer, Kurt, Endoplasmic reticulum stress markers in SARS-COV-2 infection and pneumonia: case-control study, Vivo
Lenze, Mattar, Zorumski, Fluvoxamine vs placebo and clinical deterioration in outpatients with symptomatic COVID-19: a randomized clinical trial, JAMA
Lewer, Reilly, Mojtabai, Evans-Lacko, Antidepressant use in 27 European countries: associations with sociodemographic, cultural and economic factors, Br J Psychiatry
Li, Li, Fortunati, Krystal, Association of a prior psychiatric diagnosis with mortality among hospitalized patients with coronavirus disease 2019 (COVID-19) infection, JAMA Netw Open
Lim, Tignanelli, Hoertel, Boulware, Usher, Prevalence of medical contraindications to nirmatrelvir/ritonavir in a cohort of hospitalized and nonhospitalized patients with COVID-19, Open Forum Infect Dis
Lu, Chao, Chang, Lan, Lai, Effect of fluvoxamine on outcomes of nonhospitalized patients with COVID-19: a systematic review and meta-analysis, J Infect Public Health
Marcec, Dodig, Likic, A meta-analysis regarding fluvoxamine and hospitalization risk of COVID-19 patients: TOGETHER making a difference, J Infect
Moiseev, Brovko, Tao, Bulanov, Akulkina et al., Sex differences in mortality in the intensive care unit patients with severe COVID-19, J Infect
Montazersaheb, Khatibi, Hejazi, COVID-19 infection: an overview on cytokine storm and related interventions, Virol J
Niitsu, Fujisaki, Shiina, A randomized, double-blind, placebo-controlled trial of fluvoxamine in patients with schizophrenia: a preliminary study, J Clin Psychopharmacol
Oskotsky, Marić, Tang, Mortality risk among patients with COVID-19 prescribed selective serotonin reuptake inhibitor antidepressants, JAMA Netw Open
Péricat, Sa, Rico, Antiviral and antiinflammatory activities of fluoxetine in a SARS-CoV-2 infection mouse model, Int J Mol Sci
Reis, Santos Moreira-Silva, Silva, Effect of early treatment with fluvoxamine on risk of emergency care and hospitalisation among patients with COVID-19: the TOGETHER randomised, platform clinical trial, Lancet Global Health
Rybaczyk, Bashaw, Pathak, Moody, Gilders et al., An overlooked connection: serotonergic mediation of estrogen-related physiology and pathology, BMC Wom Health
Sramek, Murphy, Cutler, Sex differences in the psychopharmacological treatment of depression, Dialogues Clin Neurosci
Zhang, Hu, Cai, Lu, Nie et al., Antidepressants utilization in mainland China: based on the national health insurance database, Aust N Z J Psychiatry