Association Between FIASMAs and Reduced Risk of Intubation or Death in Individuals Hospitalized for Severe COVID-19: An Observational Multicenter Study
et al., Clinical Pharmacology & Therapeutics, doi:10.1002/cpt.2317, May 2021
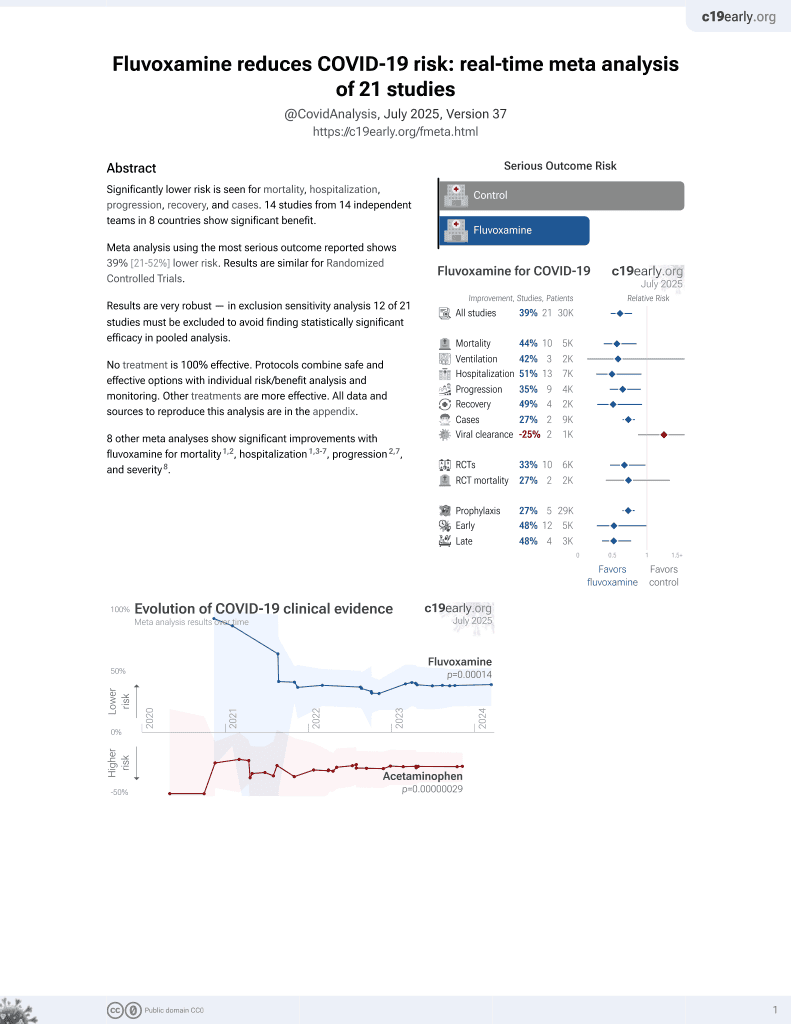
30th treatment shown to reduce risk in
November 2021, now with p = 0.00014 from 21 studies, recognized in 2 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
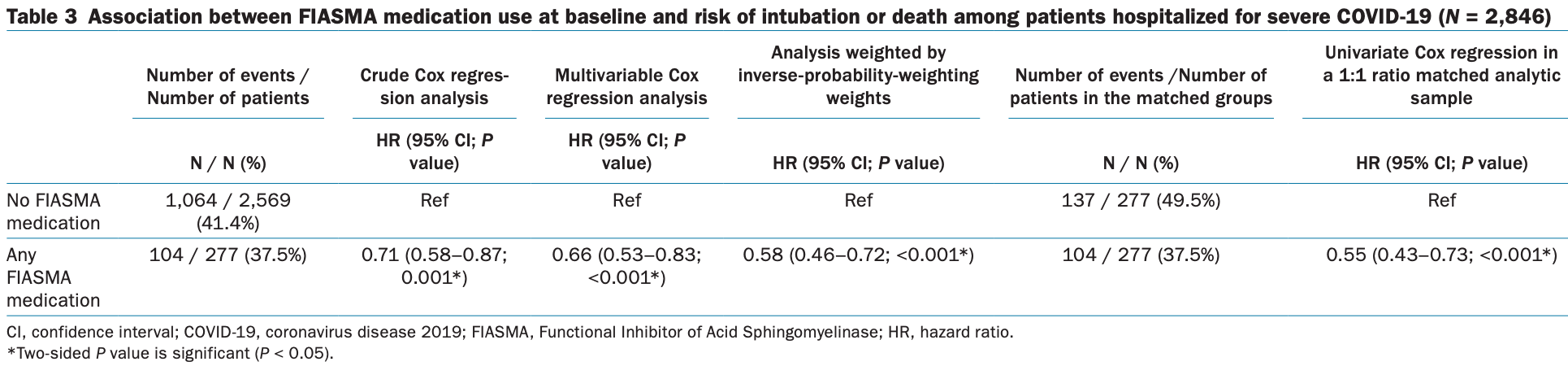
Retrospective 2,846 severe COVID-19 patients in France, 277 taking a FIASMA medication, showing lower risk of intubation of death with FIASMA use.
|
risk of death/intubation, 42.0% lower, RR 0.58, p < 0.001, treatment 104 of 277 (37.5%), control 1,064 of 2,569 (41.4%), adjusted per study, IPW multivariable Cox regression.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Hoertel et al., 29 May 2021, retrospective, France, peer-reviewed, 78 authors.
Association Between FIASMAs and Reduced Risk of Intubation or Death in Individuals Hospitalized for Severe COVID‐19: An Observational Multicenter Study
Clinical Pharmacology & Therapeutics, doi:10.1002/cpt.2317
Several medications commonly used for a number of medical conditions share a property of functional inhibition of acid sphingomyelinase (ASM), or FIASMA. Preclinical and clinical evidence suggest that the ASM/ceramide system may be central to severe acute respiratory syndrome-coronavirus 2 (SARS-CoV-2) infection. We examined the potential usefulness of FIASMA use among patients hospitalized for severe coronavirus disease 2019 (COVID-19) in an observational multicenter study conducted at Greater Paris University hospitals. Of 2,846 adult patients hospitalized for severe COVID-19, 277 (9.7%) were taking an FIASMA medication at the time of their hospital admission. The primary end point was a composite of intubation and/or death. We compared this end point between patients taking vs. not taking an FIASMA medication in time-to-event analyses adjusted for sociodemographic characteristics and medical comorbidities. The primary analysis was a Cox regression model with inverse probability weighting (IPW). Over a mean follow-up of 9.2 days (SD = 12.5), the primary end point occurred in 104 patients (37.5%) receiving an FIASMA medication, and 1,060 patients (41.4%) who did not. Despite being significantly and substantially associated with older age and greater medical severity, FIASMA medication use was significantly associated with reduced likelihood of intubation or death in both crude (hazard ratio (HR) = 0.71, 95% confidence interval (CI) = 0.58-0.87, P < 0.001) and primary IPW (HR = 0.58, 95%CI = 0.46-0.72, P < 0.001) analyses. This association remained significant in multiple sensitivity analyses and was not specific to one particular FIASMA class or medication. These results show the potential importance of the ASM/ceramide system in COVID-19 and support the continuation of FIASMA medications in these patients. Double-blind controlled randomized clinical trials of these medications for COVID-19 are needed.
SUPPORTING INFORMATION Supplementary information accompanies this paper on the Clinical Pharmacology & Therapeutics website (www.cpt-journal.com).
ACKNOWLEDGMENTS The authors warmly thank the EDS APHP COVID consortium integrating the APHP Health Data Warehouse team as well as all the APHP staff and volunteers who contributed to the implementation of the EDS-COVID database and operating solutions for this database.
FUNDING No funding was received for this work.
CONFLICT OF INTEREST
DISCLAIMER The information contained in this study is provided for research purpose and should not be used as a substitute or replacement for diagnosis or treatment recommendations or other clinical decisions or judgment. The views presented in this manuscript are those of the authors and should not be construed to represent the views of any of the sponsoring organizations, agencies, or the National Institute on Drug Abuse or any US Government Agency.
APPENDIX 1 EDS APHP Covid consortium
References
Austin, Using the standardized difference to compare the prevalence of a binary variable between two groups in observational research, Commun. Stat.-Simul. Comput, doi:10.1080/03610910902859574
Carpinteiro, Inhibition of acid sphingomyelinase by ambroxol prevents SARS-CoV-2 entry into epithelial cells, J. Biol. Chem, doi:10.1016/j.jbc.2021.100701
Carpinteiro, Pharmacological inhibition of acid sphingomyelinase prevents uptake of SARS-CoV-2 by epithelial cells, Cell Rep. Med, doi:10.1016/j.xcrm.2020.100142
Chevance, Ensuring mental health care during the SARS-CoV-2 epidemic in France: A narrative review, L'Encephale
Chouchana, Association of antihypertensive agents with the risk of in-hospital death in patients with COVID-19, Cardiovasc. Drugs Ther, doi:10.1007/s10557-021-07155-5
Dragioti, Association of antidepressant use with adverse health outcomes: a systematic umbrella review, JAMA Psychiatry, doi:10.1001/jamapsychiatry.2019.2859
Efron, Nonparametric standard errors and confidence intervals, Can. J. Stat, doi:10.2307/3314608
Gordon, Comparative host-coronavirus protein interaction networks reveal pan-viral disease mechanisms, Science, doi:10.1126/science.abe9403
Gulbins, Acid sphingomyelinase-ceramide system mediates effects of antidepressant drugs, Nat. Med, doi:10.1038/nm.3214
Hashimoto, Activation of sigma-1 receptor chaperone in the treatment of neuropsychiatric diseases and its clinical implication, J. Pharmacol. Sci, doi:10.1016/j.jphs.2014.11.010
Hoertel, A stochastic agent-based model of the SARS-CoV-2 epidemic in France, Nat. Med, doi:10.1038/s41591-020-1001-6
Hoertel, Association between antidepressant use and reduced risk of intubation or death in hospitalized patients with COVID-19: results from an observational study, Mol. Psychiatry, doi:10.1038/s41380-021-01021-4
Hoertel, Association between hydroxyzine use and reduced mortality in patients hospitalized for coronavirus disease 2019: results from a multicenter observational study, doi:10.1101/2020.10.23.20154302
Hoertel, Blachier, Sánchez-Rico, Limosin, Leleu, Impact of the timing and adherence to face mask use on the course of the COVID-19 epidemic in France, J. Travel Med, doi:10.1093/jtm/taab016
Hoertel, Dexamethasone use and mortality in hospitalized patients with coronavirus disease 2019: a multicenter retrospective observational study, Br. J. Clin. Pharmacol, doi:10.1111/bcp.14784
Hoertel, Facing the COVID-19 epidemic in NYC: a stochastic agent-based model of various intervention strategies, doi:10.1101/2020.04.23.20076885
Hoertel, Observational study of chlorpromazine in hospitalized patients with COVID-19, Clin. Drug Investig, doi:10.1007/s40261-021-01001-0
Hoertel, Observational study of haloperidol in hospitalized patients with COVID-19, PLoS One, doi:10.1371/journal.pone.0247122
Hojyo, How COVID-19 induces cytokine storm with high mortality, Inflamm. Regen
Ishikawa, High occupancy of sigma-1 receptors in the human brain after single oral administration of fluvoxamine: a positron emission tomography study using [11C] SA4503, Biol. Psychiatry, doi:10.1016/j.biopsych.2007.04.001
Ishima, Fujita, Hashimoto, Interaction of new antidepressants with sigma-1 receptor chaperones and their potentiation of neurite outgrowth in PC12 cells, Eur. J. Pharmacol, doi:10.1016/j.ejphar.2014.01.064
Kornhuber, Functional Inhibitors of Acid Sphingomyelinase (FIASMAs): a novel pharmacological group of drugs with broad clinical applications, Cell. Physiol. Biochem, doi:10.1159/000315101
Kornhuber, Identification of new functional inhibitors of acid sphingomyelinase using a structure-property-activity relation model, J. Med. Chem, doi:10.1021/jm070524a
Kornhuber, Identification of novel functional inhibitors of acid sphingomyelinase, PLoS One, doi:10.1371/journal.pone.0023852
Krutetskaya, Melnitskaya, Antonov, Nozdrachev, Sigma-1 receptor antagonists haloperidol and chlorpromazine modulate the effect of glutoxim on Na+ transport in frog skin, Doklady Biochem. Biophys, doi:10.1134/S1607672919010186
Köhler, Peripheral alterations in cytokine and chemokine levels after antidepressant drug treatment for major depressive disorder: systematic review and meta-analysis, Mol. Neurobiol
Lenze, Fluvoxamine vs placebo and clinical deterioration in outpatients with symptomatic COVID-19: A randomized clinical trial, JAMA, doi:10.1001/jama.2020.22760
Mengozzi, Chlorpromazine specifically inhibits peripheral and brain TNF production, and up-regulates IL-10 production, in mice, Immunology
Neuraz, Natural language processing for rapid response to emergent diseases: Case study of calcium channel blockers and hypertension in the COVID-19 pandemic, J. Med. Internet Res, doi:10.2196/20773
Obuchowicz, Bielecka-Wajdman, Paul-Samojedny, Nowacka, Different influence of antipsychotics on the balance between pro-and anti-inflammatory cytokines depends on glia activation: an in vitro study, Cytokine, doi:10.1016/j.cyto.2017.04.004
Plaze, Inhibition of the replication of SARS-CoV-2 in human cells by the FDA-approved drug chlorpromazine, Int. J. Antimicrob. Agents, doi:10.1016/j.ijantimicag.2020.106274
Robins, Hernán, Brumback, Marginal structural models and causal inference in epidemiology, Epidemiology
Schloer, Targeting the endolysosomal host-SARS-CoV-2 interface by clinically licensed functional inhibitors of acid sphingomyelinase (FIASMA) including the antidepressant fluoxetine, Emerg. Microbes Infect, doi:10.1080/22221751.2020.1829082
Seftel, Boulware, Prospective cohort of fluvoxamine for early treatment of coronavirus disease 19, Open Forum Infect. Dis, doi:10.1093/ofid/ofab050
Solaimanzadeh, Nifedipine and amlodipine are associated with improved mortality and decreased risk for intubation and mechanical ventilation in elderly patients hospitalized for COVID-19, Cureus, doi:10.7759/cureus.8069
Stuart, Lee, Leacy, Prognostic score-based balance measures can be a useful diagnostic for propensity score methods in comparative effectiveness research, J. Clin. Epidemiol, doi:10.1016/j.jclinepi.2013.01.013
Sugino, Futamura, Mitsumoto, Maeda, Marunaka, Atypical antipsychotics suppress production of proinflammatory cytokines and up-regulate interleukin-10 in lipopolysaccharide-treated mice, Prog. Neuropsychopharmacol. Biol. Psychiatry, doi:10.1016/j.pnpbp.2008.12.006
Sukhatme, Reiersen, Vayttaden, Sukhatme, Fluvoxamine: A review of its mechanism of action and its role in COVID-19, Front. Pharmacol
Therneau, Patricia, Grambsch Modeling Survival Data: Extending the Cox Model
Vela, Repurposing sigma-1 receptor ligands for Covid-19 therapy?, Front. Pharmacol
Williamson, Factors associated with COVID-19-related death using OpenSAFELY, Nature, doi:10.1038/s41586-020-2521-4
Ye, Wang, Mao, The pathogenesis and treatment of the Cytokine Storm' in COVID-19, J. Infect, doi:10.1016/j.jinf.2020.03.037
Zhang, Calcium channel blocker amlodipine besylate therapy is associated with reduced case fatality rate of COVID-19 patients with hypertension, Cell Discov, doi:10.1038/s41421-020-00235-0
Zhang, Kim, Lonjon, Zhu, Written on behalf of AME Big-Data Clinical Trial Collaborative Group, Ann. Transl. Med, doi:10.21037/atm.2018.12.10
Zhou, Network-based drug repurposing for novel coronavirus 2019-nCoV/SARS-CoV-2, Cell Discov, doi:10.1038/s41421-020-0153-3
Zimniak, The serotonin reuptake inhibitor Fluoxetine inhibits SARS-CoV-2 in human lung tissue, Sci. Rep
DOI record:
{
"DOI": "10.1002/cpt.2317",
"ISSN": [
"0009-9236",
"1532-6535"
],
"URL": "http://dx.doi.org/10.1002/cpt.2317",
"alternative-id": [
"10.1002/cpt.2317"
],
"archive": [
"Portico"
],
"assertion": [
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Received",
"name": "received",
"order": 0,
"value": "2021-03-02"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Accepted",
"name": "accepted",
"order": 1,
"value": "2021-05-20"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Published",
"name": "published",
"order": 2,
"value": "2021-07-02"
}
],
"author": [
{
"affiliation": [
{
"name": "Assistance Publique‐Hopitaux de Paris DMU Psychiatrie et Addictologie Hôpital Corentin‐Celton Institut de Psychiatrie et Neurosciences de Paris (IPNP) INSERM UMR_S1266 Université de Paris Paris France"
}
],
"family": "Hoertel",
"given": "Nicolas",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Assistance Publique‐Hopitaux de Paris DMU Psychiatrie et Addictologie Hôpital Corentin‐Celton Institut de Psychiatrie et Neurosciences de Paris (IPNP) INSERM UMR_S1266 Université de Paris Paris France"
},
{
"name": "Department of Psychobiology and Behavioural Sciences Methods Faculty of Psychology Universidad Complutense de Madrid Pozuelo de Alarcón, Madrid Spain"
}
],
"family": "Sánchez‐Rico",
"given": "Marina",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Institute for Molecular Biology University Medicine Essen University of Duisburg‐Essen Essen Germany"
}
],
"family": "Gulbins",
"given": "Erich",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Psychiatry and Psychotherapy University Hospital Friedrich‐Alexander‐University of Erlangen‐Nuremberg Erlangen Germany"
}
],
"family": "Kornhuber",
"given": "Johannes",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Institute for Molecular Biology University Medicine Essen University of Duisburg‐Essen Essen Germany"
},
{
"name": "Department of Hematology and Stem Cell Transplantation University Hospital Essen University of Duisburg‐Essen Essen Germany"
}
],
"family": "Carpinteiro",
"given": "Alexander",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Psychiatry Washington University in St. Louis School of Medicine St. Louis Missouri USA"
}
],
"family": "Lenze",
"given": "Eric J.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Psychiatry Washington University in St. Louis School of Medicine St. Louis Missouri USA"
}
],
"family": "Reiersen",
"given": "Angela M.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Assistance Publique‐Hopitaux de Paris DMU Psychiatrie et Addictologie Hôpital Corentin‐Celton Institut de Psychiatrie et Neurosciences de Paris (IPNP) INSERM UMR_S1266 Université de Paris Paris France"
}
],
"family": "Abellán",
"given": "Miriam",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Assistance Publique‐Hopitaux de Paris DMU Psychiatrie et Addictologie Hôpital Corentin‐Celton Institut de Psychiatrie et Neurosciences de Paris (IPNP) INSERM UMR_S1266 Université de Paris Paris France"
},
{
"name": "Department of Psychobiology and Behavioural Sciences Methods Faculty of Psychology Universidad Complutense de Madrid Pozuelo de Alarcón, Madrid Spain"
}
],
"family": "Muela",
"given": "Pedro",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Medical Informatics, Biostatistics and Public Health Department Assistance Publique‐Hopitaux de Paris, Centre‐Université de Paris Hôpital Européen Georges Pompidou Paris France"
}
],
"family": "Vernet",
"given": "Raphaël",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Division of Epidemiology, Services, and Prevention Research National Institute on Drug Abuse North Bethesda Maryland USA"
}
],
"family": "Blanco",
"given": "Carlos",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Institut de Pharmacologie et de Biologie Structurale IPBS Université de Toulouse Toulouse France"
}
],
"family": "Cougoule",
"given": "Céline",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Unité de Recherche clinique, Hopital Cochin Assistance Publique‐Hopitaux de Paris Paris France"
}
],
"family": "Beeker",
"given": "Nathanaël",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "INSERM UMR_S 1138 Cordeliers Research Center Université de Paris Paris France"
},
{
"name": "Department of Medical Informatics Necker‐Enfants Malades Hospital Assistance Publique‐Hopitaux de Paris Centre‐Université de Paris Paris France"
}
],
"family": "Neuraz",
"given": "Antoine",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "INSERM U1266 (Institute of Psychiatry and Neuroscience of Paris) Université de Paris Paris France"
}
],
"family": "Gorwood",
"given": "Philip",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Psychobiology and Behavioural Sciences Methods Faculty of Psychology Universidad Complutense de Madrid Pozuelo de Alarcón, Madrid Spain"
}
],
"family": "Alvarado",
"given": "Jesús M.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "INSERM U1142 LIMICS UMRS 1142 Sorbonne Universities UPMC University of Paris 06 University of Paris 13 Paris France"
}
],
"family": "Meneton",
"given": "Pierre",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Assistance Publique‐Hopitaux de Paris DMU Psychiatrie et Addictologie Hôpital Corentin‐Celton Institut de Psychiatrie et Neurosciences de Paris (IPNP) INSERM UMR_S1266 Université de Paris Paris France"
}
],
"family": "Limosin",
"given": "Frédéric",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ancel",
"given": "Pierre‐Yves",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bauchet",
"given": "Alain",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Beeker",
"given": "Nathanaël",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Benoit",
"given": "Vincent",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bernaux",
"given": "Mélodie",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bellamine",
"given": "Ali",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bey",
"given": "Romain",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bourmaud",
"given": "Aurélie",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Breant",
"given": "Stéphane",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Burgun",
"given": "Anita",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Carrat",
"given": "Fabrice",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Caucheteux",
"given": "Charlotte",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Champ",
"given": "Julien",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Cormont",
"given": "Sylvie",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Daniel",
"given": "Christel",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Dubiel",
"given": "Julien",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ducloas",
"given": "Catherine",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Esteve",
"given": "Loic",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Frank",
"given": "Marie",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Garcelon",
"given": "Nicolas",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Gramfort",
"given": "Alexandre",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Griffon",
"given": "Nicolas",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Grisel",
"given": "Olivier",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Guilbaud",
"given": "Martin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Hassen‐Khodja",
"given": "Claire",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Hemery",
"given": "François",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Hilka",
"given": "Martin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sophie Jannot",
"given": "Anne",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lambert",
"given": "Jerome",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Layese",
"given": "Richard",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Leblanc",
"given": "Judith",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lebouter",
"given": "Léo",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lemaitre",
"given": "Guillaume",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Leprovost",
"given": "Damien",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lerner",
"given": "Ivan",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Levi Sallah",
"given": "Kankoe",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Maire",
"given": "Aurélien",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mamzer",
"given": "Marie‐France",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Martel",
"given": "Patricia",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mensch",
"given": "Arthur",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Moreau",
"given": "Thomas",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Neuraz",
"given": "Antoine",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Orlova",
"given": "Nina",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Paris",
"given": "Nicolas",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Rance",
"given": "Bastien",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ravera",
"given": "Hélène",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Rozes",
"given": "Antoine",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Salamanca",
"given": "Elisa",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sandrin",
"given": "Arnaud",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Serre",
"given": "Patricia",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Tannier",
"given": "Xavier",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Treluyer",
"given": "Jean‐Marc",
"sequence": "additional"
},
{
"affiliation": [],
"family": "van Gysel",
"given": "Damien",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Varoquaux",
"given": "Gaël",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Vie",
"given": "Jill Jen",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wack",
"given": "Maxime",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wajsburt",
"given": "Perceval",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wassermann",
"given": "Demian",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Zapletal",
"given": "Eric",
"sequence": "additional"
},
{
"affiliation": [],
"name": "AP‐HP / Université de Paris / INSERM COVID‐19 research collaboration, AP‐HP COVID CDR Initiative, “Entrepôt de Données de Santé” AP‐HP Consortium",
"sequence": "additional"
}
],
"container-title": [
"Clinical Pharmacology & Therapeutics"
],
"content-domain": {
"crossmark-restriction": true,
"domain": [
"onlinelibrary.wiley.com"
]
},
"created": {
"date-parts": [
[
2021,
6,
4
]
],
"date-time": "2021-06-04T10:53:36Z",
"timestamp": 1622804016000
},
"deposited": {
"date-parts": [
[
2021,
11,
13
]
],
"date-time": "2021-11-13T18:33:33Z",
"timestamp": 1636828413000
},
"indexed": {
"date-parts": [
[
2021,
11,
15
]
],
"date-time": "2021-11-15T16:54:57Z",
"timestamp": 1636995297627
},
"is-referenced-by-count": 7,
"issn-type": [
{
"type": "print",
"value": "0009-9236"
},
{
"type": "electronic",
"value": "1532-6535"
}
],
"issue": "6",
"issued": {
"date-parts": [
[
2021,
7,
2
]
]
},
"journal-issue": {
"issue": "6",
"published-print": {
"date-parts": [
[
2021,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "http://creativecommons.org/licenses/by-nc-nd/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
7,
2
]
],
"date-time": "2021-07-02T00:00:00Z",
"timestamp": 1625184000000
}
},
{
"URL": "http://doi.wiley.com/10.1002/tdm_license_1.1",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
7,
2
]
],
"date-time": "2021-07-02T00:00:00Z",
"timestamp": 1625184000000
}
}
],
"link": [
{
"URL": "https://onlinelibrary.wiley.com/doi/pdf/10.1002/cpt.2317",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://onlinelibrary.wiley.com/doi/full-xml/10.1002/cpt.2317",
"content-type": "application/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://onlinelibrary.wiley.com/doi/pdf/10.1002/cpt.2317",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "311",
"original-title": [],
"page": "1498-1511",
"prefix": "10.1002",
"published": {
"date-parts": [
[
2021,
7,
2
]
]
},
"published-online": {
"date-parts": [
[
2021,
7,
2
]
]
},
"published-print": {
"date-parts": [
[
2021,
12
]
]
},
"publisher": "Wiley",
"reference": [
{
"DOI": "10.1038/s41591-020-1001-6",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_1_1"
},
{
"article-title": "Facing the COVID‐19 epidemic in NYC: a stochastic agent‐based model of various intervention strategies",
"author": "Hoertel N.",
"journal-title": "medRxiv",
"key": "e_1_2_12_2_1"
},
{
"DOI": "10.1016/j.encep.2020.04.005",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_3_1"
},
{
"DOI": "10.1093/jtm/taab016",
"article-title": "Impact of the timing and adherence to face mask use on the course of the COVID‐19 epidemic in France",
"author": "Hoertel N.",
"doi-asserted-by": "crossref",
"journal-title": "J. Travel Med.",
"key": "e_1_2_12_4_1",
"volume": "28",
"year": "2021"
},
{
"DOI": "10.1016/j.xcrm.2020.100142",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_5_1"
},
{
"DOI": "10.1159/000315101",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_6_1"
},
{
"DOI": "10.1038/nm.3214",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_7_1"
},
{
"DOI": "10.1371/journal.pone.0023852",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_8_1"
},
{
"DOI": "10.1021/jm070524a",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_9_1"
},
{
"DOI": "10.1016/j.jbc.2021.100701",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_10_1"
},
{
"DOI": "10.1080/22221751.2020.1829082",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_11_1"
},
{
"DOI": "10.1001/jama.2020.22760",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_12_1"
},
{
"DOI": "10.1093/ofid/ofab050",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_13_1"
},
{
"article-title": "Association between antidepressant use and reduced risk of intubation or death in hospitalized patients with COVID‐19: results from an observational study",
"author": "Hoertel N.",
"journal-title": "Mol. Psychiatry",
"key": "e_1_2_12_14_1"
},
{
"article-title": "Association between hydroxyzine use and reduced mortality in patients hospitalized for coronavirus disease 2019: results from a multicenter observational study",
"author": "Hoertel N.",
"journal-title": "medRxiv",
"key": "e_1_2_12_15_1"
},
{
"article-title": "Nifedipine and amlodipine are associated with improved mortality and decreased risk for intubation and mechanical ventilation in elderly patients hospitalized for COVID‐19",
"author": "Solaimanzadeh I",
"first-page": "e8069",
"issue": "5",
"journal-title": "Cureus",
"key": "e_1_2_12_16_1",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1038/s41421-020-00235-0",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_17_1"
},
{
"article-title": "Association of antihypertensive agents with the risk of in‐hospital death in patients with COVID‐19",
"author": "Chouchana L.",
"journal-title": "Cardiovasc. Drugs Ther.",
"key": "e_1_2_12_18_1"
},
{
"DOI": "10.1371/journal.pone.0247122",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_19_1"
},
{
"DOI": "10.1007/s40261-021-01001-0",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_20_1"
},
{
"article-title": "Dexamethasone use and mortality in hospitalized patients with coronavirus disease 2019: a multicenter retrospective observational study",
"author": "Hoertel N.",
"journal-title": "Br. J. Clin. Pharmacol.",
"key": "e_1_2_12_21_1"
},
{
"key": "e_1_2_12_22_1",
"unstructured": "Haut Conseil de la Santé Publique.Statement on the management at home or in a care facility of suspected or confirmed Covid‐19 patients. (2020). <https://www.hcsp.fr>."
},
{
"DOI": "10.1038/s41586-020-2521-4",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_23_1"
},
{
"DOI": "10.2196/20773",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_24_1"
},
{
"key": "e_1_2_12_25_1",
"unstructured": "WHO Collaborating Centre for Drug Statistics Methodology ATC/DDD Index. 2021. (2020). <https://www.whocc.no/atc_ddd_index/>."
},
{
"DOI": "10.21037/atm.2018.12.10",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_26_1"
},
{
"DOI": "10.1080/03610910902859574",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_27_1"
},
{
"DOI": "10.1016/j.jclinepi.2013.01.013",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_28_1"
},
{
"DOI": "10.1007/978-1-4757-3294-8",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_29_1"
},
{
"DOI": "10.1097/00001648-200009000-00011",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_30_1"
},
{
"DOI": "10.2307/3314608",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_31_1"
},
{
"key": "e_1_2_12_32_1",
"unstructured": "U.S. National Library of Medicine ClinicalTrials.gov.(2021). <https://clinicaltrials.gov/ct2/results?cond=Covid19&term=paracetamol&cntry=&state=&city=&dist=>."
},
{
"DOI": "10.3389/fphar.2021.652688",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_33_1"
},
{
"DOI": "10.1016/j.ijantimicag.2020.106274",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_34_1"
},
{
"DOI": "10.1038/s41598-021-85049-0",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_35_1"
},
{
"DOI": "10.1016/j.ejphar.2014.01.064",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_36_1"
},
{
"DOI": "10.1016/j.biopsych.2007.04.001",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_37_1"
},
{
"DOI": "10.1038/s41421-020-0153-3",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_38_1"
},
{
"DOI": "10.1016/j.jphs.2014.11.010",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_39_1"
},
{
"DOI": "10.1134/S1607672919010186",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_40_1"
},
{
"DOI": "10.3389/fphar.2020.582310",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_41_1"
},
{
"DOI": "10.1126/science.abe9403",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_42_1"
},
{
"article-title": "Peripheral alterations in cytokine and chemokine levels after antidepressant drug treatment for major depressive disorder: systematic review and meta‐analysis",
"author": "Köhler C.A.",
"first-page": "4195",
"journal-title": "Mol. Neurobiol.",
"key": "e_1_2_12_43_1",
"volume": "55",
"year": "2018"
},
{
"DOI": "10.1186/s41232-020-00146-3",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_44_1"
},
{
"DOI": "10.1016/j.jinf.2020.03.037",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_45_1"
},
{
"DOI": "10.1016/j.cyto.2017.04.004",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_46_1"
},
{
"DOI": "10.1016/j.pnpbp.2008.12.006",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_47_1"
},
{
"article-title": "Chlorpromazine specifically inhibits peripheral and brain TNF production, and up‐regulates IL‐10 production, in mice",
"author": "Mengozzi M.",
"first-page": "207",
"journal-title": "Immunology",
"key": "e_1_2_12_48_1",
"volume": "82",
"year": "1994"
},
{
"DOI": "10.1001/jamapsychiatry.2019.2859",
"doi-asserted-by": "publisher",
"key": "e_1_2_12_49_1"
}
],
"reference-count": 49,
"references-count": 49,
"relation": {},
"score": 1,
"short-container-title": [
"Clin. Pharmacol. Ther."
],
"short-title": [],
"source": "Crossref",
"subject": [
"Pharmacology (medical)",
"Pharmacology"
],
"subtitle": [],
"title": [
"Association Between FIASMAs and Reduced Risk of Intubation or Death in Individuals Hospitalized for Severe COVID‐19: An Observational Multicenter Study"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1002/crossmark_policy",
"volume": "110"
}