Association between antidepressant use and reduced risk of intubation or death in hospitalized patients with COVID-19: results from an observational study
et al., Molecular Psychiatry, doi:10.1038/s41380-021-01021-4, Aug 2020
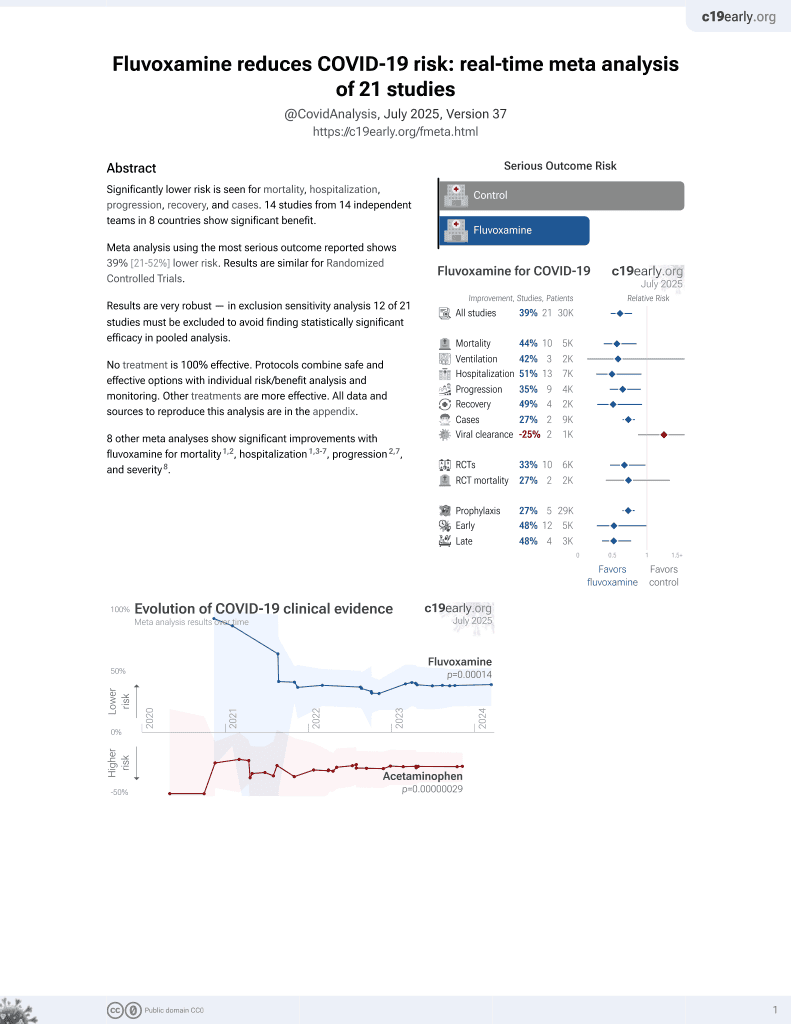
30th treatment shown to reduce risk in
November 2021, now with p = 0.00014 from 21 studies, recognized in 2 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
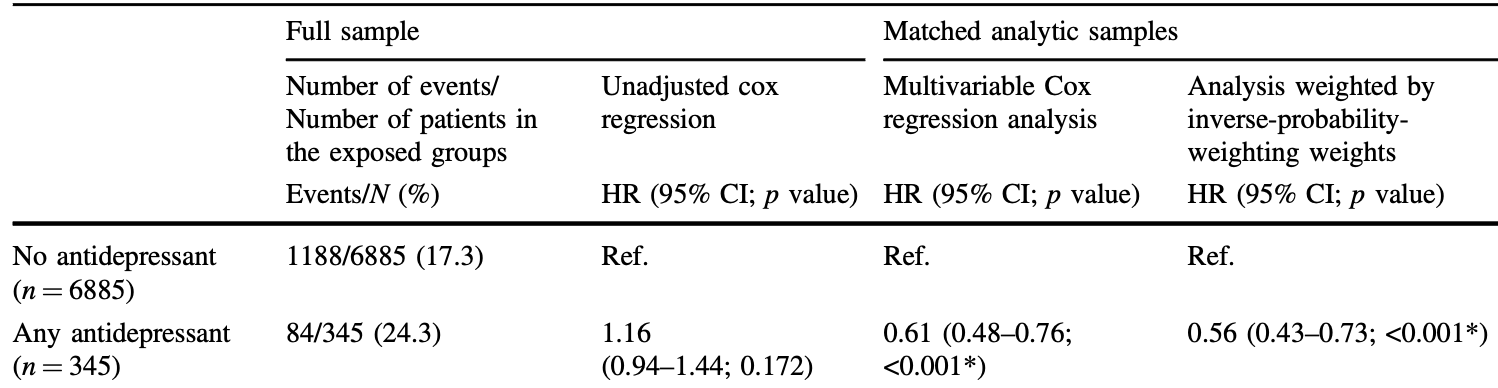
Retrospective 7,230 hospitalized COVID-19 patients in France, 345 receiving an antidepressant medication within 48 hours of admission. There was a significant association between antidepressant use and reduced risk of intubation or death. There was only one patient for fluvoxamine.
|
risk of death/intubation, 44.0% lower, RR 0.56, p < 0.001, treatment 84 of 345 (24.3%), control 1,188 of 6,885 (17.3%), adjusted per study, IPW multivariable Cox regression.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Hoertel et al., 17 Aug 2020, retrospective, France, peer-reviewed, 17 authors.
Association between antidepressant use and reduced risk of intubation or death in hospitalized patients with COVID-19: results from an observational study
Molecular Psychiatry, doi:10.1038/s41380-021-01021-4
A prior meta-analysis showed that antidepressant use in major depressive disorder was associated with reduced plasma levels of several pro-inflammatory mediators, which have been associated with severe COVID-19. Recent studies also suggest that several antidepressants may inhibit acid sphingomyelinase activity, which may prevent the infection of epithelial cells with SARS-CoV-2, and that the SSRI fluoxetine may exert in-vitro antiviral effects on SARS-CoV-2. We examined the potential usefulness of antidepressant use in patients hospitalized for COVID-19 in an observational multicenter retrospective cohort study conducted at AP-HP Greater Paris University hospitals. Of 7230 adults hospitalized for COVID-19, 345 patients (4.8%) received an antidepressant within 48 h of hospital admission. The primary endpoint was a composite of intubation or death. We compared this endpoint between patients who received antidepressants and those who did not in time-to-event analyses adjusted for patient characteristics, clinical and biological markers of disease severity, and other psychotropic medications. The primary analysis was a multivariable Cox model with inverse probability weighting. This analysis showed a significant association between antidepressant use and reduced risk of intubation or death (HR, 0.56; 95% CI, 0.43-0.73, p < 0.001). This association remained significant in multiple sensitivity analyses. Exploratory analyses suggest that this association was also significant for SSRI and non-SSRI antidepressants, and for fluoxetine, paroxetine, escitalopram, venlafaxine, and mirtazapine (all p < 0.05). These results suggest that antidepressant use could be associated with lower risk of death or intubation in patients hospitalized for COVID-19. Double-blind controlled randomized clinical trials of antidepressant medications for COVID-19 are needed.
Conflict of interest All authors have completed the Unified Competing Interest form (available on request from the corresponding author) and declare: no support from any organization for the submitted work; NH has received personal fees and non-financial support from Lundbeck, outside the submitted work. FL has received speaker and consulting fees from Janssen-Cilag, Euthérapie-Servier, and Lundbeck, outside the submitted work. CL reports personal fees and non-financial support from Janssen-Cilag, Lundbeck, Otsuka Pharmaceutical, and Boehringer Ingelheim, outside the submitted work. GA reports personal fees from Pfizer, Pierre Fabre and Lundbeck, outside the submitted work; other authors declare no financial relationships with any organization that might have an interest in the submitted work in the previous three years; no other relationships or activities that could appear to have influenced the submitted work. Ethical approval This observational study using routinely collected data received approval from the Institutional Review Board of the AP-HP clinical data warehouse (decision CSE-20-20_COVID19, IRB00011591, April 8th, 2020). AP-HP clinical Data Warehouse initiative ensures patients' information and informed consent regarding the different approved studies through a transparency portal in accordance with European Regulation on data protection and authorization n°1980120 from National Commission for Information Technology and Civil Liberties (CNIL). All procedures..
References
Biorxiv, None, doi:10.1101/2020.06.14.150490v2
Carpinteiro, Edwards, Hoffmann, Kochs, Gripp et al., Pharmacological inhibition of acid sphingomyelinase prevents uptake of SARS-CoV-2 by epithelial cells, Cell Reports Med
Chevance, Gourion, Hoertel, Llorca, Thomas et al., Ensuring mental health care during the SARS-CoV-2 epidemic in France: a narrative review, L'Encephale
Cipriani, Furukawa, Salanti, Chaimani, Atkinson et al., Comparative efficacy and acceptability of 21 antidepressant drugs for the acute treatment of adults with major depressive disorder: a systematic review and network metaanalysis, Focus
Devlin, Chang, Lee, Toutanova, Bert: Pre-training of deep bidirectional transformers for language understanding
Efron, Nonparametric standard errors and confidence intervals, Can J Stat
Elm, Altman, Egger, Pocock, Gøtzsche et al., The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies, Ann Intern Med
Fa, Neutrophil-to-lymphocyte ratio and lymphocyte-to-C-reactive protein ratio in patients with severe coronavirus disease 2019 (COVID-19): a meta-analysis, J Med Virol
Geleris, Sun, Platt, Zucker, Baldwin et al., Observational study of hydroxychloroquine in hospitalized patients with Covid-19, N. Engl J Med
Gordon, Jang, Bouhaddou, Xu, Obernier et al., A SARS-CoV-2 protein interaction map reveals targets for drug repurposing, Nature
Gulbins, Palmada, Reichel, Lüth, Böhmer et al., Acid sphingomyelinase-ceramide system mediates effects of antidepressant drugs, Nat Med
Hayasaka, Purgato, Magni, Ogawa, Takeshima et al., Dose equivalents of antidepressants: evidencebased recommendations from randomized controlled trials, J Affect Disord
Hoertel, Blachier, Blanco, Olfson, Massetti et al., A stochastic agent-based model of the SARS-CoV-2 epidemic in France, Nat Med
Hoertel, Blachier, Blanco, Olfson, Massetti et al., Facing the COVID-19 epidemic in NYC: a stochastic agent-based model of various intervention strategies, doi:10.1101/2020.04.23.20076885
Hoertel, Sánchez-Rico, Vernet, Beeker, Neuraz et al., Dexamethasone use and Mortality in Hospitalized Patients with Coronavirus Disease, MedRxiv, doi:10.1101/2020.10.23.20218172
Hoertel, Sánchez-Rico, Vernet, Jannot, Neuraz et al., Observational study of chlorpromazine in hospitalized patients with Covid-19, doi:10.1101/2020.07.15.20154310
Hoertel, Sánchez-Rico, Vernet, Jannot, Neuraz et al., Observational study of haloperidol in hospitalized patients with Covid-19, MedRxiv, doi:10.1101/2020.07.15.20150490
Hojyo, Uchida, Tanaka, Hasebe, Tanaka et al., How COVID-19 induces cytokine storm with high mortality, Inflamm Regen
Hur, Price, Gray, Gulati, Maksimoski et al., Factors associated with intubation and prolonged intubation in hospitalized patients with COVID-19, Otolaryngol Head Neck Surg
Kaplan, Meier, Nonparametric estimation from incomplete observations, J Am Stat Assoc
Krause, Gutsmiedl, Bighelli, Schneider-Thoma, Chaimani et al., Efficacy and tolerability of pharmacological and nonpharmacological interventions in older patients with major depressive disorder: A systematic review, pairwise and network meta-analysis, Eur Neuropsychopharmacol
Köhler, Freitas, Stubbs, Maes, Solmi et al., Peripheral alterations in cytokine and chemokine levels after antidepressant drug treatment for major depressive disorder: systematic review and meta-analysis, Mol Neurobiol
Lenze, Mattar, Zorumski, Stevens, Schweiger et al., Fluvoxamine vs placebo and clinical deterioration in outpatients with symptomatic COVID-19: a randomized clinical trial, JAMA
Li, Li, Fortunati, Krystal, Association of a prior psychiatric diagnosis with mortality among hospitalized patients with coronavirus disease 2019 (COVID-19) Infection, JAMA Netw Open
Liu, Yan, Xiang, Liu, Viral dynamics in mild and severe cases of COVID-19, The Lancet Infectious Diseases
Robins, Hernán, Brumback, Marginal structural models and causal inference in epidemiology, Epidemiology
Ruan, Yang, Wang, Jiang, Song, Clinical predictors of mortality due to COVID-19 based on an analysis of data of 150 patients from Wuhan, China, Intensive Care Med
Stebbing, Phelan, Griffin, Tucker, Oechsle et al., COVID-19: combining antiviral and anti-inflammatory treatments, Lancet Infect Dis
Strat, Hoertel, Correlation is no causation: gymnasium proliferation and the risk of obesity, Addiction
Tham, Jonsson, Andersson, Söderlund, Allard et al., Efficacy and tolerability of antidepressants in people aged 65 years or older with major depressive disorder-a systematic review and a meta-analysis, J Affect Disord
Wang, Kaelber, Xu, Volkow, COVID-19 risk and outcomes in patients with substance use disorders: analyses from electronic health records in the United States, Mol Psychiatry
Williamson, Walker, Bhaskaran, Bacon, Bates et al., OpenSAFELY: factors associated with COVID-19-related hospital death in the linked electronic health records of 17 million adult NHS patients, MedRxiv, doi:10.1101/2020.05.06.20092999
Ye, Wang, Mao, The pathogenesis and treatment of the-Cytokine Storm'in COVID-19, J Infect
Zhou, Yu, Du, Fan, Liu et al., Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study, Lancet
Zimniak, Kirschner, Hilpert, Seibel, Bodem, The serotonin reuptake inhibitor Fluoxetine inhibits SARS-CoV-2
DOI record:
{
"DOI": "10.1038/s41380-021-01021-4",
"ISSN": [
"1359-4184",
"1476-5578"
],
"URL": "http://dx.doi.org/10.1038/s41380-021-01021-4",
"alternative-id": [
"1021"
],
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "19 September 2020"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Revised",
"name": "revised",
"order": 2,
"value": "18 December 2020"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 3,
"value": "7 January 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 4,
"value": "4 February 2021"
},
{
"group": {
"label": "Compliance with ethical standards",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Conflict of interest",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "All authors have completed the Unified Competing Interest form (available on request from the corresponding author) and declare: no support from any organization for the submitted work; NH has received personal fees and non-financial support from Lundbeck, outside the submitted work. FL has received speaker and consulting fees from Janssen-Cilag, Euthérapie-Servier, and Lundbeck, outside the submitted work. CL reports personal fees and non-financial support from Janssen-Cilag, Lundbeck, Otsuka Pharmaceutical, and Boehringer Ingelheim, outside the submitted work. GA reports personal fees from Pfizer, Pierre Fabre and Lundbeck, outside the submitted work; other authors declare no financial relationships with any organization that might have an interest in the submitted work in the previous three years; no other relationships or activities that could appear to have influenced the submitted work."
},
{
"group": {
"label": "Ethical approval",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "This observational study using routinely collected data received approval from the Institutional Review Board of the AP-HP clinical data warehouse (decision CSE-20-20_COVID19, IRB00011591, April 8th, 2020). AP-HP clinical Data Warehouse initiative ensures patients’ information and informed consent regarding the different approved studies through a transparency portal in accordance with European Regulation on data protection and authorization n°1980120 from National Commission for Information Technology and Civil Liberties (CNIL). All procedures related to this work adhered to the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008."
},
{
"label": "Free to read",
"name": "free",
"value": "This content has been made available to all."
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-7890-1349",
"affiliation": [],
"authenticated-orcid": false,
"family": "Hoertel",
"given": "Nicolas",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-1121-8641",
"affiliation": [],
"authenticated-orcid": false,
"family": "Sánchez-Rico",
"given": "Marina",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-3358-9005",
"affiliation": [],
"authenticated-orcid": false,
"family": "Vernet",
"given": "Raphaël",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Beeker",
"given": "Nathanaël",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jannot",
"given": "Anne-Sophie",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Neuraz",
"given": "Antoine",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Salamanca",
"given": "Elisa",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Paris",
"given": "Nicolas",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Daniel",
"given": "Christel",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Gramfort",
"given": "Alexandre",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lemaitre",
"given": "Guillaume",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bernaux",
"given": "Mélodie",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bellamine",
"given": "Ali",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-3487-4721",
"affiliation": [],
"authenticated-orcid": false,
"family": "Lemogne",
"given": "Cédric",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Airagnes",
"given": "Guillaume",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Burgun",
"given": "Anita",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Limosin",
"given": "Frédéric",
"sequence": "additional"
},
{
"affiliation": [],
"name": "On behalf of AP-HP / Universities / INSERM COVID-19 Research Collaboration and AP-HP COVID CDR Initiative",
"sequence": "additional"
}
],
"container-title": "Molecular Psychiatry",
"container-title-short": "Mol Psychiatry",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2021,
2,
4
]
],
"date-time": "2021-02-04T02:03:24Z",
"timestamp": 1612404204000
},
"deposited": {
"date-parts": [
[
2021,
11,
12
]
],
"date-time": "2021-11-12T19:40:04Z",
"timestamp": 1636746004000
},
"indexed": {
"date-parts": [
[
2024,
5,
13
]
],
"date-time": "2024-05-13T15:59:54Z",
"timestamp": 1715615994816
},
"is-referenced-by-count": 170,
"issue": "9",
"issued": {
"date-parts": [
[
2021,
2,
4
]
]
},
"journal-issue": {
"issue": "9",
"published-print": {
"date-parts": [
[
2021,
9
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.springer.com/tdm",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
2,
4
]
],
"date-time": "2021-02-04T00:00:00Z",
"timestamp": 1612396800000
}
},
{
"URL": "https://www.springer.com/tdm",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
2,
4
]
],
"date-time": "2021-02-04T00:00:00Z",
"timestamp": 1612396800000
}
}
],
"link": [
{
"URL": "https://www.nature.com/articles/s41380-021-01021-4.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://www.nature.com/articles/s41380-021-01021-4",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://www.nature.com/articles/s41380-021-01021-4.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"page": "5199-5212",
"prefix": "10.1038",
"published": {
"date-parts": [
[
2021,
2,
4
]
]
},
"published-online": {
"date-parts": [
[
2021,
2,
4
]
]
},
"published-print": {
"date-parts": [
[
2021,
9
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.1038/s41591-020-1001-6",
"author": "N Hoertel",
"doi-asserted-by": "publisher",
"first-page": "1417",
"journal-title": "Nat Med.",
"key": "1021_CR1",
"unstructured": "Hoertel N, Blachier M, Blanco C, Olfson M, Massetti M, Sánchez-Rico M, et al. A stochastic agent-based model of the SARS-CoV-2 epidemic in France. Nat Med. 2020;26:1417–21.",
"volume": "26",
"year": "2020"
},
{
"DOI": "10.1101/2020.04.23.20076885",
"doi-asserted-by": "publisher",
"key": "1021_CR2",
"unstructured": "Hoertel N, Blachier M, Blanco C, Olfson M, Massetti M, Limosin F, et al. Facing the COVID-19 epidemic in NYC: a stochastic agent-based model of various intervention strategies. MedRxiv. 2020. 2020. https://doi.org/10.1101/2020.04.23.20076885."
},
{
"DOI": "10.1038/s41586-020-2286-9",
"author": "DE Gordon",
"doi-asserted-by": "publisher",
"first-page": "459",
"journal-title": "Nature.",
"key": "1021_CR3",
"unstructured": "Gordon DE, Jang GM, Bouhaddou M, Xu J, Obernier K, White KM, et al. A SARS-CoV-2 protein interaction map reveals targets for drug repurposing. Nature. 2020;583:459–68.",
"volume": "583",
"year": "2020"
},
{
"DOI": "10.1016/j.encep.2020.03.001",
"author": "A Chevance",
"doi-asserted-by": "publisher",
"first-page": "S3",
"journal-title": "L’Encephale",
"key": "1021_CR4",
"unstructured": "Chevance A, Gourion D, Hoertel N, Llorca P-M, Thomas P, Bocher R, et al. Ensuring mental health care during the SARS-CoV-2 epidemic in France: a narrative review. L’Encephale. 2020;46:S3–S13.",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.1016/S1473-3099(20)30132-8",
"author": "J Stebbing",
"doi-asserted-by": "publisher",
"first-page": "400",
"journal-title": "Lancet Infect Dis",
"key": "1021_CR5",
"unstructured": "Stebbing J, Phelan A, Griffin I, Tucker C, Oechsle O, Smith D, et al. COVID-19: combining antiviral and anti-inflammatory treatments. Lancet Infect Dis. 2020;20:400–2.",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1016/S1473-3099(20)30232-2",
"author": "Y Liu",
"doi-asserted-by": "publisher",
"first-page": "656",
"journal-title": "The Lancet Infectious Diseases.",
"key": "1021_CR6",
"unstructured": "Liu Y, Yan L-M, Wan L, Xiang T-X, Le A, Liu J-M, et al. Viral dynamics in mild and severe cases of COVID-19. The Lancet Infectious Diseases. 2020;20:656–7.",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1186/s41232-020-00146-3",
"author": "S Hojyo",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Inflamm Regen",
"key": "1021_CR7",
"unstructured": "Hojyo S, Uchida M, Tanaka K, Hasebe R, Tanaka Y, Murakami M, et al. How COVID-19 induces cytokine storm with high mortality. Inflamm Regen. 2020;40:1–7.",
"volume": "40",
"year": "2020"
},
{
"author": "CA Köhler",
"first-page": "4195",
"journal-title": "Mol Neurobiol",
"key": "1021_CR8",
"unstructured": "Köhler CA, Freitas TH, Stubbs B, Maes M, Solmi M, Veronese N, et al. Peripheral alterations in cytokine and chemokine levels after antidepressant drug treatment for major depressive disorder: systematic review and meta-analysis. Mol Neurobiol. 2018;55:4195–206.",
"volume": "55",
"year": "2018"
},
{
"DOI": "10.1016/j.jinf.2020.03.037",
"author": "Q Ye",
"doi-asserted-by": "publisher",
"first-page": "607",
"journal-title": "J Infect",
"key": "1021_CR9",
"unstructured": "Ye Q, Wang B, Mao J. The pathogenesis and treatment of theCytokine Storm’in COVID-19. J Infect. 2020;80:607–13.",
"volume": "80",
"year": "2020"
},
{
"DOI": "10.1038/nm.3214",
"author": "E Gulbins",
"doi-asserted-by": "publisher",
"first-page": "934",
"journal-title": "Nat Med",
"key": "1021_CR10",
"unstructured": "Gulbins E, Palmada M, Reichel M, Lüth A, Böhmer C, Amato D, et al. Acid sphingomyelinase–ceramide system mediates effects of antidepressant drugs. Nat Med. 2013;19:934–8.",
"volume": "19",
"year": "2013"
},
{
"DOI": "10.1016/j.xcrm.2020.100142",
"author": "A Carpinteiro",
"doi-asserted-by": "publisher",
"first-page": "100142",
"journal-title": "Cell Reports Med",
"key": "1021_CR11",
"unstructured": "Carpinteiro A, Edwards MJ, Hoffmann M, Kochs G, Gripp B, Weigang S, et al. Pharmacological inhibition of acid sphingomyelinase prevents uptake of SARS-CoV-2 by epithelial cells. Cell Reports Med. 2020;1:100142.",
"volume": "1",
"year": "2020"
},
{
"DOI": "10.1101/2020.06.14.150490",
"doi-asserted-by": "crossref",
"key": "1021_CR12",
"unstructured": "Zimniak M, Kirschner L, Hilpert H, Seibel J, Bodem J. The serotonin reuptake inhibitor Fluoxetine inhibits SARS-CoV-2. BioRxiv. 2020. https://www.biorxiv.org/content/10.1101/2020.06.14.150490v2."
},
{
"DOI": "10.1001/jama.2020.22760",
"author": "EJ Lenze",
"doi-asserted-by": "publisher",
"first-page": "2292",
"journal-title": "JAMA.",
"key": "1021_CR13",
"unstructured": "Lenze EJ, Mattar C, Zorumski CF, Stevens A, Schweiger J, Nicol GE, et al. Fluvoxamine vs placebo and clinical deterioration in outpatients with symptomatic COVID-19: a randomized clinical trial. JAMA. 2020;324:2292–2300.",
"volume": "324",
"year": "2020"
},
{
"DOI": "10.1176/appi.focus.16407",
"author": "A Cipriani",
"doi-asserted-by": "publisher",
"first-page": "420",
"journal-title": "Focus.",
"key": "1021_CR14",
"unstructured": "Cipriani A, Furukawa TA, Salanti G, Chaimani A, Atkinson LZ, Ogawa Y, et al. Comparative efficacy and acceptability of 21 antidepressant drugs for the acute treatment of adults with major depressive disorder: a systematic review and network meta-analysis. Focus. 2018;16:420–9.",
"volume": "16",
"year": "2018"
},
{
"DOI": "10.1016/j.jad.2016.06.013",
"author": "A Tham",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "J Affect Disord",
"key": "1021_CR15",
"unstructured": "Tham A, Jonsson U, Andersson G, Söderlund A, Allard P, Bertilsson G. Efficacy and tolerability of antidepressants in people aged 65 years or older with major depressive disorder–a systematic review and a meta-analysis. J Affect Disord. 2016;205:1–12.",
"volume": "205",
"year": "2016"
},
{
"DOI": "10.1016/j.euroneuro.2019.07.130",
"author": "M Krause",
"doi-asserted-by": "publisher",
"first-page": "1003",
"journal-title": "Eur Neuropsychopharmacol",
"key": "1021_CR16",
"unstructured": "Krause M, Gutsmiedl K, Bighelli I, Schneider-Thoma J, Chaimani A, Leucht S. Efficacy and tolerability of pharmacological and non-pharmacological interventions in older patients with major depressive disorder: A systematic review, pairwise and network meta-analysis. Eur Neuropsychopharmacol. 2019;29:1003–22.",
"volume": "29",
"year": "2019"
},
{
"DOI": "10.1101/2020.05.06.20092999",
"doi-asserted-by": "publisher",
"key": "1021_CR17",
"unstructured": "Williamson E, Walker AJ, Bhaskaran KJ, Bacon S, Bates C, Morton CE, et al. OpenSAFELY: factors associated with COVID-19-related hospital death in the linked electronic health records of 17 million adult NHS patients. MedRxiv. 2020. https://doi.org/10.1101/2020.05.06.20092999."
},
{
"key": "1021_CR18",
"unstructured": "Devlin J, Chang M-W, Lee K, Toutanova K. Bert: Pre-training of deep bidirectional transformers for language understanding. ArXiv. 2018. https://arxiv.org/abs/1810.04805."
},
{
"DOI": "10.1016/S0140-6736(20)30566-3",
"author": "F Zhou",
"doi-asserted-by": "publisher",
"first-page": "1054",
"journal-title": "Lancet.",
"key": "1021_CR19",
"unstructured": "Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395:1054–62.",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1007/s00134-020-05991-x",
"author": "Q Ruan",
"doi-asserted-by": "publisher",
"first-page": "846",
"journal-title": "Intensive Care Med",
"key": "1021_CR20",
"unstructured": "Ruan Q, Yang K, Wang W, Jiang L, Song J. Clinical predictors of mortality due to COVID-19 based on an analysis of data of 150 patients from Wuhan, China. Intensive Care Med. 2020;46:846–8.",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.1177/0194599820929640",
"author": "K Hur",
"doi-asserted-by": "publisher",
"first-page": "170",
"journal-title": "Otolaryngol Head Neck Surg.",
"key": "1021_CR21",
"unstructured": "Hur K, Price CP, Gray EL, Gulati RK, Maksimoski M, Racette SD, et al. Factors associated with intubation and prolonged intubation in hospitalized patients with COVID-19. Otolaryngol Head Neck Surg. 2020;163:170–8.",
"volume": "163",
"year": "2020"
},
{
"DOI": "10.1101/2020.10.23.20218172",
"doi-asserted-by": "publisher",
"key": "1021_CR22",
"unstructured": "Hoertel N, Sánchez-Rico M, Vernet R, Beeker N, Neuraz A, Alvarado JM, et al. Dexamethasone use and Mortality in Hospitalized Patients with Coronavirus Disease 2019: a Multicenter Retrospective Observational Study. MedRxiv. 2020. https://doi.org/10.1101/2020.10.23.20218172."
},
{
"key": "1021_CR23",
"unstructured": "Haut Conseil de la Santé Publique. Statement on the management at home or in a care facility of suspected or confirmed Covid-19 patients. April 8, 2020. Statement on the management at home or in a care facility of suspected or confirmed Covid-19 patients. https://www.hcsp.fr\\textgreater."
},
{
"DOI": "10.1002/jmv.25819",
"author": "FA Lagunas‐Rangel",
"doi-asserted-by": "publisher",
"first-page": "1733",
"journal-title": "J Med Virol.",
"key": "1021_CR24",
"unstructured": "Lagunas‐Rangel FA. Neutrophil‐to‐lymphocyte ratio and lymphocyte‐to‐C‐reactive protein ratio in patients with severe coronavirus disease 2019 (COVID‐19): a meta‐analysis. J Med Virol. 2020;92:1733–4.",
"volume": "92",
"year": "2020"
},
{
"DOI": "10.1101/2020.07.15.20154310",
"doi-asserted-by": "publisher",
"key": "1021_CR25",
"unstructured": "Hoertel N, Sánchez-Rico M, Vernet R, Jannot A-S, Neuraz A, Blanco C, et al. Observational study of chlorpromazine in hospitalized patients with Covid-19. MedRxiv. 2020. 2020. https://doi.org/10.1101/2020.07.15.20154310."
},
{
"DOI": "10.1101/2020.07.15.20150490",
"doi-asserted-by": "publisher",
"key": "1021_CR26",
"unstructured": "Hoertel N, Sánchez-Rico M, Vernet R, Jannot A-S, Neuraz A, Blanco C, et al. Observational study of haloperidol in hospitalized patients with Covid-19. MedRxiv. 2020. https://doi.org/10.1101/2020.07.15.20150490."
},
{
"DOI": "10.1097/00001648-200009000-00011",
"author": "JM Robins",
"doi-asserted-by": "publisher",
"first-page": "550",
"journal-title": "Epidemiology.",
"key": "1021_CR27",
"unstructured": "Robins JM, Hernán MÁ, Brumback B. Marginal structural models and causal inference in epidemiology. Epidemiology. 2000;11:550–60.",
"volume": "11",
"year": "2000"
},
{
"DOI": "10.1056/NEJMoa2012410",
"author": "J Geleris",
"doi-asserted-by": "publisher",
"first-page": "2411",
"journal-title": "N. Engl J Med",
"key": "1021_CR28",
"unstructured": "Geleris J, Sun Y, Platt J, Zucker J, Baldwin M, Hripcsak G, et al. Observational study of hydroxychloroquine in hospitalized patients with Covid-19. N. Engl J Med. 2020;382:2411–8.",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1080/01621459.1958.10501452",
"author": "EL Kaplan",
"doi-asserted-by": "publisher",
"first-page": "457",
"journal-title": "J Am Stat Assoc",
"key": "1021_CR29",
"unstructured": "Kaplan EL, Meier P. Nonparametric estimation from incomplete observations. J Am Stat Assoc. 1958;53:457–81.",
"volume": "53",
"year": "1958"
},
{
"DOI": "10.2307/3314608",
"author": "B Efron",
"doi-asserted-by": "publisher",
"first-page": "139",
"journal-title": "Can J Stat",
"key": "1021_CR30",
"unstructured": "Efron B. Nonparametric standard errors and confidence intervals. Can J Stat. 1981;9:139–58.",
"volume": "9",
"year": "1981"
},
{
"DOI": "10.1016/j.jad.2015.03.021",
"author": "Y Hayasaka",
"doi-asserted-by": "publisher",
"first-page": "179",
"journal-title": "J Affect Disord",
"key": "1021_CR31",
"unstructured": "Hayasaka Y, Purgato M, Magni LR, Ogawa Y, Takeshima N, Cipriani A, et al. Dose equivalents of antidepressants: evidence-based recommendations from randomized controlled trials. J Affect Disord. 2015;180:179–84.",
"volume": "180",
"year": "2015"
},
{
"DOI": "10.7326/0003-4819-147-8-200710160-00010",
"author": "E Von Elm",
"doi-asserted-by": "publisher",
"first-page": "573",
"journal-title": "Ann Intern Med",
"key": "1021_CR32",
"unstructured": "Von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Ann Intern Med. 2007;147:573–7.",
"volume": "147",
"year": "2007"
},
{
"DOI": "10.1038/s41380-020-00880-7",
"author": "QQ Wang",
"doi-asserted-by": "publisher",
"first-page": "30",
"journal-title": "Mol Psychiatry.",
"key": "1021_CR33",
"unstructured": "Wang QQ, Kaelber DC, Xu R, Volkow ND. COVID-19 risk and outcomes in patients with substance use disorders: analyses from electronic health records in the United States. Mol Psychiatry. 2021;26:30–9.",
"volume": "26",
"year": "2021"
},
{
"DOI": "10.1001/jamanetworkopen.2020.23282",
"author": "L Li",
"doi-asserted-by": "publisher",
"first-page": "e2023282",
"journal-title": "JAMA Netw Open",
"key": "1021_CR34",
"unstructured": "Li L, Li F, Fortunati F, Krystal JH. Association of a prior psychiatric diagnosis with mortality among hospitalized patients with coronavirus disease 2019 (COVID-19) Infection. JAMA Netw Open. 2020;3:e2023282–e2023282.",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1111/j.1360-0443.2011.03547.x",
"author": "Y Le Strat",
"doi-asserted-by": "publisher",
"first-page": "1871",
"journal-title": "Addiction.",
"key": "1021_CR35",
"unstructured": "Le Strat Y, Hoertel N. Correlation is no causation: gymnasium proliferation and the risk of obesity. Addiction. 2011;106:1871–2.",
"volume": "106",
"year": "2011"
}
],
"reference-count": 35,
"references-count": 35,
"relation": {
"has-preprint": [
{
"asserted-by": "object",
"id": "10.1101/2020.07.09.20143339",
"id-type": "doi"
}
]
},
"resource": {
"primary": {
"URL": "https://www.nature.com/articles/s41380-021-01021-4"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Association between antidepressant use and reduced risk of intubation or death in hospitalized patients with COVID-19: results from an observational study",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "26"
}