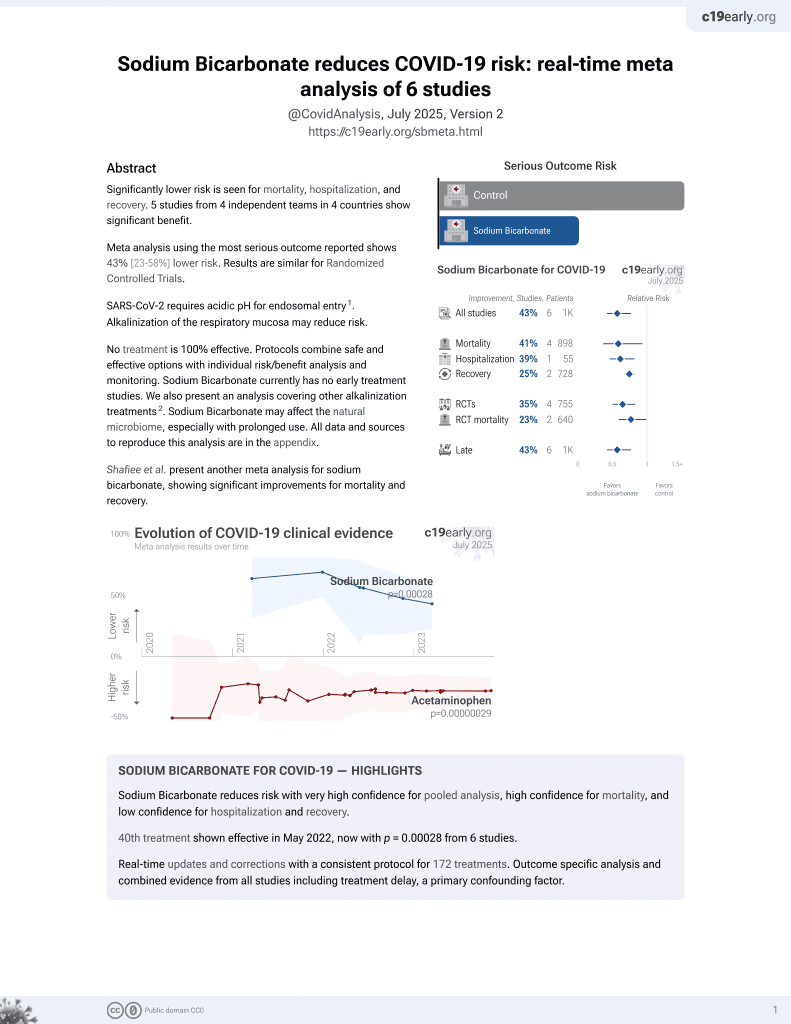
Effects of Different Inhalation Therapy on Ventilator-Associated Pneumonia in Ventilated COVID-19 Patients: A Randomized Controlled Trial
et al., Microorganisms, doi:10.3390/microorganisms10061118, NCT04755972, May 2022
41st treatment shown to reduce risk in
May 2022, now with p = 0.00028 from 6 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
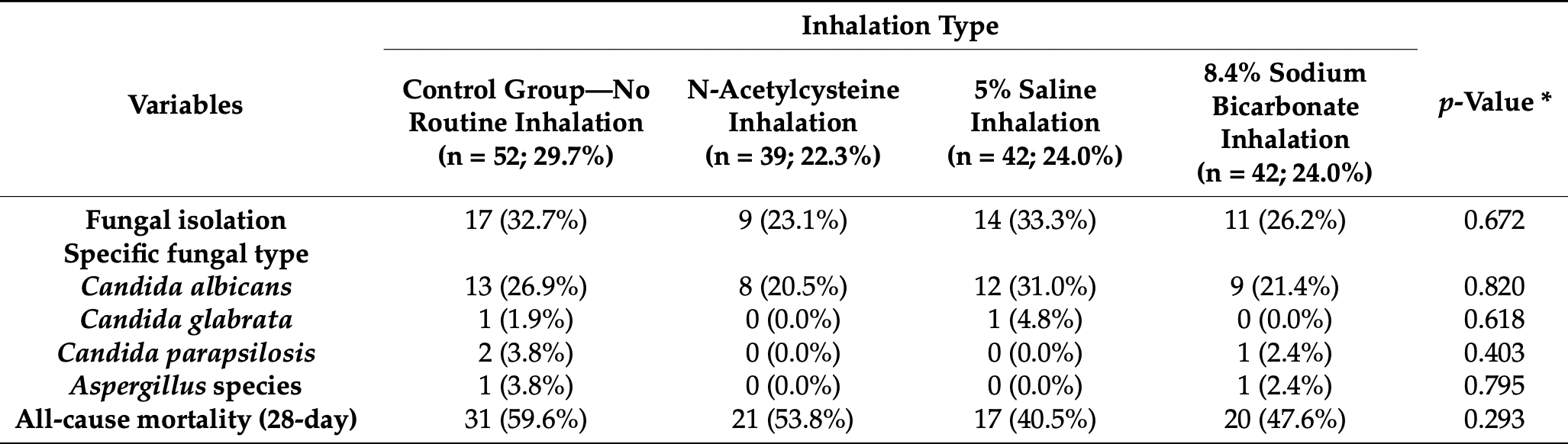
RCT mechanically ventilated patients in Croatia, 42 treated with sodium bicarbonate inhalation, and 52 control patients, showing no significant difference in mortality with treatment. Treated patients showed a lower incidence of gram-positive or MRSA-caused ventilator-associated pneumonia. ICU mortality results are from1.
Targeted administration to the respiratory tract provides treatment directly
to the typical source of initial SARS-CoV-2 infection and replication, and
allows for rapid onset of action, higher local drug concentration, and reduced systemic side effects (early treatment may be more beneficial).
Study covers sodium bicarbonate, NaCl, and N-acetylcysteine.
|
risk of death, 23.0% lower, RR 0.77, p = 0.13, treatment 23 of 42 (54.8%), control 37 of 52 (71.2%), NNT 6.1, ICU mortality.
|
|
risk of death, 20.1% lower, RR 0.80, p = 0.30, treatment 20 of 42 (47.6%), control 31 of 52 (59.6%), NNT 8.3, 28 day mortality.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
2.
Wang et al., Efficacy of nasal irrigation and oral rinse with sodium bicarbonate solution on virus clearance for COVID-19 patients, Frontiers in Public Health, doi:10.3389/fpubh.2023.1145669.
3.
El-Badrawy et al., Efficacy and safety of nebulized Sodium Bicarbonate in adults with COVID-19 (SODIC): a randomized, single center, double-blinded, controlled trial, Current Therapeutic Research, doi:10.1016/j.curtheres.2025.100801.
4.
Baxter et al., Rapid initiation of nasal saline irrigation to reduce severity in high-risk COVID+ outpatients, Ear, Nose & Throat Journal, doi:10.1177/01455613221123737.
5.
El-Badrawy (B) et al., Role of Sodium Bicarbonate as Adjuvant Treatment of Nonsevere Computed Tomography-identified COVID-19 Pneumonia: A Preliminary Report, Indian Journal of Respiratory Care, doi:10.4103/ijrc.ijrc_48_21.
Delić et al., 28 May 2022, Randomized Controlled Trial, Croatia, peer-reviewed, 12 authors, study period October 2020 - June 2021, trial NCT04755972 (history).
Contact: ndelic@kbsplit.hr (corresponding author), tkljakgas@kbsplit.hr, lsaric@kbsplit.hr, dilic@kbsplit.hr, sdosenovic@kbsplit.hr, jdomazet@kbsplit.hr, rkovac@kbsplit.hr, sastojanovic@kbsplit.hr, bduplanc@kbsplit.hr, andrija.matetic@gmail.com, frane.runjic@gmail.com, josipa.domjanovic@gmail.com.
DOI record:
{
"DOI": "10.3390/microorganisms10061118",
"ISSN": [
"2076-2607"
],
"URL": "http://dx.doi.org/10.3390/microorganisms10061118",
"abstract": "<jats:p>The effect of routine inhalation therapy on ventilator-associated pneumonia (VAP) in mechanically ventilated patients with the coronavirus disease (COVID-19) has not been well-defined. This randomized controlled trial included 175 eligible adult patients with COVID-19 who were treated with mechanical ventilation at the University Hospital of Split between October 2020 and June 2021. Patients were randomized and allocated to a control group (no routine inhalation) or one of the treatment arms (inhalation of N-acetylcysteine; 5% saline solution; or 8.4% sodium bicarbonate). The primary outcome was the incidence of VAP, while secondary outcomes included all-cause mortality. Routine inhalation therapy had no effect on the incidence of bacterial or fungal VAP nor on all-cause mortality (p > 0.05). Secondary analyses revealed a significant reduction of Gram-positive and methicillin-resistant Staphylococcus aureus (MRSA) VAP in the treatment groups. Specifically, the bicarbonate group had a statistically significantly lower incidence of Gram-positive bacterial VAP (4.8%), followed by the N-acetylcysteine group (10.3%), 5% saline group (19.0%), and control group (34.6%; p = 0.001). This difference was driven by a lower incidence of MRSA VAP in the bicarbonate group (2.4%), followed by the N-acetylcysteine group (7.7%), 5% saline group (14.3%), and control group (34.6%; p < 0.001). Longer duration of ventilator therapy was the only significant, independent predictor of any bacterial or fungal VAP in the multivariate analysis (aOR 1.14, 95% CI 1.01–1.29, p = 0.038 and aOR 1.05, 95% CI 1.01–1.10, p = 0.028, respectively). In conclusion, inhalation therapy had no effect on the overall VAP incidence or all-cause mortality. Further studies should explore the secondary findings of this study such as the reduction of Gram-positive or MRSA-caused VAP in treated patients.</jats:p>",
"alternative-id": [
"microorganisms10061118"
],
"author": [
{
"affiliation": [],
"family": "Delić",
"given": "Nikola",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0001-9272-6906",
"affiliation": [],
"authenticated-orcid": false,
"family": "Matetic",
"given": "Andrija",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-7003-8192",
"affiliation": [],
"authenticated-orcid": false,
"family": "Domjanović",
"given": "Josipa",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kljaković-Gašpić",
"given": "Toni",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-5621-580X",
"affiliation": [],
"authenticated-orcid": false,
"family": "Šarić",
"given": "Lenko",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ilić",
"given": "Darko",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Došenović",
"given": "Svjetlana",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Domazet",
"given": "Josipa",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kovač",
"given": "Ruben",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Runjić",
"given": "Frane",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Stipić",
"given": "Sanda Stojanović",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Duplančić",
"given": "Božidar",
"sequence": "additional"
}
],
"container-title": "Microorganisms",
"container-title-short": "Microorganisms",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2022,
5,
30
]
],
"date-time": "2022-05-30T03:43:03Z",
"timestamp": 1653882183000
},
"deposited": {
"date-parts": [
[
2022,
5,
30
]
],
"date-time": "2022-05-30T04:00:51Z",
"timestamp": 1653883251000
},
"indexed": {
"date-parts": [
[
2022,
5,
30
]
],
"date-time": "2022-05-30T04:42:53Z",
"timestamp": 1653885773518
},
"is-referenced-by-count": 0,
"issue": "6",
"issued": {
"date-parts": [
[
2022,
5,
28
]
]
},
"journal-issue": {
"issue": "6",
"published-online": {
"date-parts": [
[
2022,
6
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
5,
28
]
],
"date-time": "2022-05-28T00:00:00Z",
"timestamp": 1653696000000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/2076-2607/10/6/1118/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "1118",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2022,
5,
28
]
]
},
"published-online": {
"date-parts": [
[
2022,
5,
28
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"DOI": "10.1001/jama.2020.2648",
"doi-asserted-by": "publisher",
"key": "ref1"
},
{
"key": "ref2"
},
{
"DOI": "10.3390/antibiotics10050545",
"doi-asserted-by": "publisher",
"key": "ref3"
},
{
"DOI": "10.1097/CCM.0b013e3182281f33",
"doi-asserted-by": "publisher",
"key": "ref4"
},
{
"DOI": "10.1097/MCC.0000000000000908",
"doi-asserted-by": "publisher",
"key": "ref5"
},
{
"DOI": "10.1080/17476348.2017.1359090",
"doi-asserted-by": "publisher",
"key": "ref6"
},
{
"DOI": "10.1007/s40261-019-00861-x",
"doi-asserted-by": "publisher",
"key": "ref7"
},
{
"article-title": "Evaluation of the Effect of Nebulized N-Acetylcysteine on Respiratory Secretions in Mechanically Ventilated Patients: Randomized Clinical Trial",
"author": "Masoompour",
"first-page": "309",
"journal-title": "Iran. J. Med. Sci.",
"key": "ref8",
"volume": "40",
"year": "2015"
},
{
"DOI": "10.1002/14651858.CD001506.pub4",
"doi-asserted-by": "publisher",
"key": "ref9"
},
{
"article-title": "Acute Respiratory Distress Syndrome: The Berlin Definition",
"author": "Ranieri",
"first-page": "2526",
"journal-title": "JAMA",
"key": "ref10",
"volume": "307",
"year": "2012"
},
{
"DOI": "10.1186/s13054-021-03460-5",
"doi-asserted-by": "publisher",
"key": "ref11"
},
{
"article-title": "Hydrator Therapies for Chronic Bronchitis. Lessons from Cystic Fibrosis",
"author": "Bennett",
"first-page": "S186",
"journal-title": "Ann. Am. Thorac. Soc.",
"key": "ref12",
"volume": "13",
"year": "2016"
},
{
"DOI": "10.1056/NEJMoa043891",
"doi-asserted-by": "publisher",
"key": "ref13"
},
{
"DOI": "10.1136/thx.52.10.900",
"doi-asserted-by": "publisher",
"key": "ref14"
},
{
"DOI": "10.1164/ajrccm.156.1.9512074",
"doi-asserted-by": "publisher",
"key": "ref15"
},
{
"DOI": "10.1172/JCI119138",
"doi-asserted-by": "publisher",
"key": "ref16"
},
{
"DOI": "10.4049/jimmunol.0803959",
"doi-asserted-by": "publisher",
"key": "ref17"
},
{
"DOI": "10.1371/journal.pone.0090164",
"doi-asserted-by": "publisher",
"key": "ref18"
},
{
"DOI": "10.1177/1753466619866102",
"doi-asserted-by": "publisher",
"key": "ref19"
},
{
"DOI": "10.1136/thoraxjnl-2014-205953",
"doi-asserted-by": "publisher",
"key": "ref20"
},
{
"article-title": "Mucoactive agents for airway mucus hypersecretory diseases",
"author": "Rogers",
"first-page": "1176",
"journal-title": "Respir. Care",
"key": "ref21",
"volume": "52",
"year": "2007"
},
{
"DOI": "10.1152/ajplung.00180.2010",
"doi-asserted-by": "publisher",
"key": "ref22"
},
{
"DOI": "10.29328/journal.jcicm.1001029",
"doi-asserted-by": "publisher",
"key": "ref23"
},
{
"DOI": "10.1186/s13054-021-03517-5",
"doi-asserted-by": "publisher",
"key": "ref24"
},
{
"DOI": "10.1186/s13613-020-00775-4",
"doi-asserted-by": "publisher",
"key": "ref25"
},
{
"DOI": "10.1007/s00134-020-06323-9",
"doi-asserted-by": "publisher",
"key": "ref26"
},
{
"DOI": "10.1371/journal.pone.0246318",
"doi-asserted-by": "publisher",
"key": "ref27"
},
{
"DOI": "10.1186/s13054-021-03571-z",
"doi-asserted-by": "publisher",
"key": "ref28"
},
{
"DOI": "10.1007/s00134-020-06062-x",
"doi-asserted-by": "publisher",
"key": "ref29"
},
{
"DOI": "10.1016/j.jiac.2021.01.011",
"doi-asserted-by": "publisher",
"key": "ref30"
},
{
"DOI": "10.3390/jcm10040555",
"doi-asserted-by": "publisher",
"key": "ref31"
},
{
"DOI": "10.3390/v9030058",
"doi-asserted-by": "publisher",
"key": "ref32"
},
{
"DOI": "10.1038/nrmicro3231",
"doi-asserted-by": "publisher",
"key": "ref33"
},
{
"DOI": "10.1016/j.mib.2016.11.003",
"doi-asserted-by": "publisher",
"key": "ref34"
},
{
"DOI": "10.1016/S2666-5247(20)30009-4",
"doi-asserted-by": "publisher",
"key": "ref35"
},
{
"DOI": "10.1093/cid/ciaa530",
"doi-asserted-by": "publisher",
"key": "ref36"
},
{
"DOI": "10.1002/14651858.CD006458.pub3",
"doi-asserted-by": "publisher",
"key": "ref37"
},
{
"article-title": "ffect of N-acetylcysteine inhalation on ventilator-associated pneumonia caused by biofilm in endotracheal tubes",
"author": "Qu",
"first-page": "278",
"journal-title": "Zhonghua Er Ke Za Zhi",
"key": "ref38",
"volume": "54",
"year": "2016"
},
{
"DOI": "10.1001/jama.2018.0949",
"doi-asserted-by": "publisher",
"key": "ref39"
},
{
"DOI": "10.1152/ajplung.00143.2012",
"doi-asserted-by": "publisher",
"key": "ref40"
},
{
"DOI": "10.1089/jamp.2015.1228",
"doi-asserted-by": "publisher",
"key": "ref41"
},
{
"DOI": "10.1186/s13054-021-03493-w",
"doi-asserted-by": "publisher",
"key": "ref42"
},
{
"DOI": "10.3390/antibiotics10080988",
"doi-asserted-by": "publisher",
"key": "ref43"
},
{
"DOI": "10.1164/rccm.202106-1354OC",
"doi-asserted-by": "publisher",
"key": "ref44"
}
],
"reference-count": 44,
"references-count": 44,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/2076-2607/10/6/1118"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Virology",
"Microbiology (medical)",
"Microbiology"
],
"subtitle": [],
"title": "Effects of Different Inhalation Therapy on Ventilator-Associated Pneumonia in Ventilated COVID-19 Patients: A Randomized Controlled Trial",
"type": "journal-article",
"volume": "10"
}
delicph
