Lack of association between vitamin D insufficiency and clinical outcomes of patients with COVID-19 infection
et al., BMC Infectious Diseases, doi:10.1186/s12879-021-06168-7, May 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 153 hospitalized patients in Iran, showing no significant difference in outcomes based on vitamin D levels. Adjusted results are only provided for vitamin D as a continuous variable.
This is the 64th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
This study is excluded in the after exclusion results of meta-analysis:
excessive unadjusted differences between groups.
|
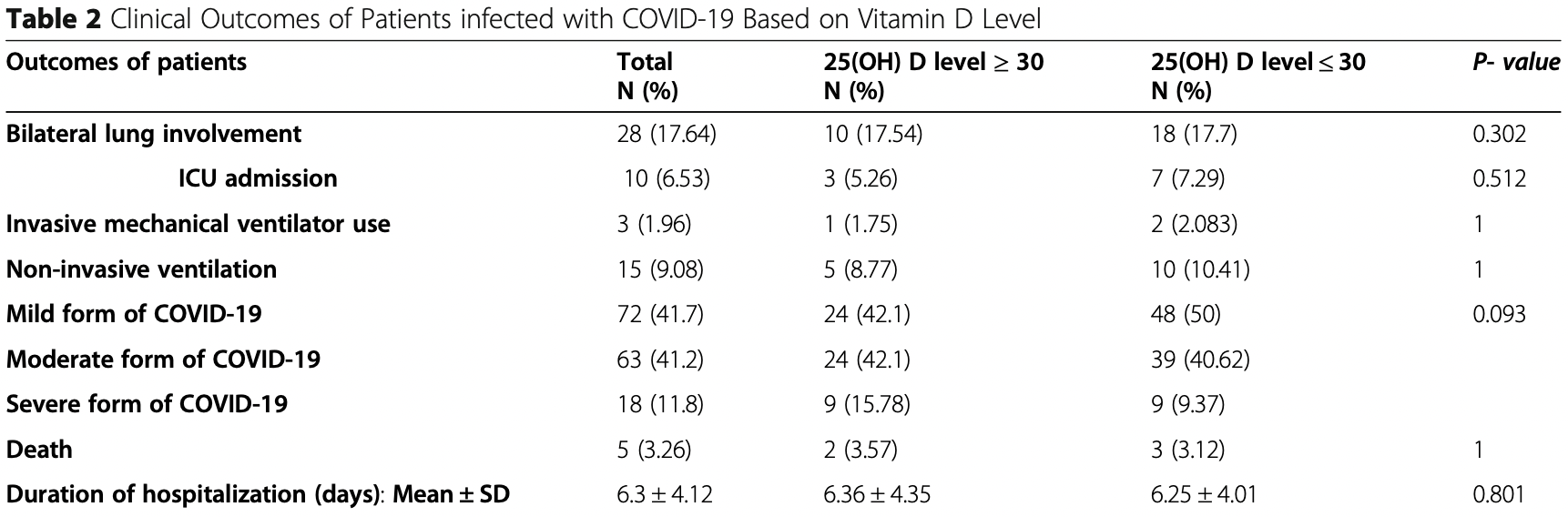
risk of death, 12.3% higher, RR 1.12, p = 1.00, high D levels (≥30ng/mL) 2 of 57 (3.5%), low D levels (<30ng/mL) 3 of 96 (3.1%).
|
|
risk of mechanical ventilation, 15.8% lower, RR 0.84, p = 1.00, high D levels (≥30ng/mL) 1 of 57 (1.8%), low D levels (<30ng/mL) 2 of 96 (2.1%), NNT 304.
|
|
risk of ICU admission, 27.8% lower, RR 0.72, p = 0.74, high D levels (≥30ng/mL) 3 of 57 (5.3%), low D levels (<30ng/mL) 7 of 96 (7.3%), NNT 49.
|
|
risk of severe case, 68.4% higher, RR 1.68, p = 0.30, high D levels (≥30ng/mL) 9 of 57 (15.8%), low D levels (<30ng/mL) 9 of 96 (9.4%).
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Davoudi et al., 18 May 2021, retrospective, Iran, peer-reviewed, 11 authors, study period February 2020 - March 2020.
Contact: fkani63@gmail.com (corresponding author).
Lack of association between vitamin D insufficiency and clinical outcomes of patients with COVID-19 infection
BMC Infectious Diseases, doi:10.1186/s12879-021-06168-7
Background: A protective effect of vitamin D against COVID-19 infection is under investigation. We aimed to analyze the effect of vitamin D sufficiency on the clinical outcomes of patients infected with COVID-19. Methods: In this cross-sectional study we analyzed the vitamin D levels of COVID-19 patients who were admitted to Razi Hospital (an infectious disease referral center in Mazandaran province in northern Iran) from February to March 2020. Overall, a cutoff point of 30 ng/mL was used for the definition of vitamin D sufficiency. Results: One hundred fifty-three patients were analyzed in this study who had laboratory documentation of a 25(OH) D level at the time of hospitalization. The vitamin D levels of the patients were 27.19 ± 20.17 ng/mL. In total, 62.7% (n = 96) of the patients had a 25(OH) D level of less than 30 ng/mL and 37.25% (n = 57) had a 25(OH) D level of more than 30 ng/mL. In total, 49% (n = 75) of the patients suffered from at least one underlying disease. The univariate and multivariable regression showed that vitamin D sufficiency was not associated with a statistically significant lower risk of adverse clinical outcomes of COVID-19 such as duration of hospitalization and severity of infection (P > 0.05). Conclusions: Sufficient vitamin D levels were not found to be protective against adverse clinical outcomes in patients infected with COVID-19. Chronic disorders in COVID-19 patients were found to have greater relevance than vitamin D levels in determining the adverse outcomes of the infection. Further studies are needed to determine the role of vitamin D level in predicting the outcomes of COVID-19 infection.
Authors' contributions AD, NN and FA designed the project, collected data, wrote and performed the critical review of the manuscript. MA, AT, HI, ZS, LD, RN, NV and ZD contributed to clinical data collection. MA and RN carried out statistical interpretation. All authors read and approved the final manuscript.
Declarations
Ethics approval and consent to participate This study was approved by the Ethics Committee of Ramsar international branch of Mazandaran University of Medical Sciences with code: IR.MAZUMS.RIB.REC.1399.019. In addition, written informed consent was obtained from all subjects or, for subjects under the age of 18, from a parent and/or legal guardian. In this study all applied methods were carried out in accordance with relevant guidelines and regulations.
Consent for publication Not applicable.
Competing interests The authors declare that they have no competing interests.
Publisher's Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Arabi, Fowler, Hayden, Critical care management of adults with community-acquired severe respiratory viral infection, Intensive Care Med, doi:10.1007/s00134-020-05943-5
Azadeh, Hedayatizadeh-Omran, Saeedi, Vahedi-Larijani, Mehravaran et al., Serum vitamin D concentrations in CoVID19 patients, J Mazandaran Univ Med Sci
Baktash, Hosack, Patel, Shah, Kandiah et al., Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad Med J, doi:10.1136/postgradmedj-2020-138712
Banerjee, Ganguly, Saha, Chakrabarti, Saini et al., Vitamin D and immuno-pathology of COVID-19: many interactions but uncertain therapeutic benefits, Expert Rev Anti-Infect Ther, doi:10.1080/14787210.2021.1905519
Beard, Bearden, Striker, Vitamin D and the anti-viral state, J Clin Virol, doi:10.1016/j.jcv.2010.12.006
Biesalski, Vitamin D deficiency and co-morbidities in COVID-19 patientsa relationship?, NFS J, doi:10.1016/j.nfs.2020.06.001
Brandão, Chiamolera, Biscolla, Lima, De et al., No association between vitamin D status and COVID-19 infection in São Paulo, Brazil, Arch Endocrinol Metab, doi:10.20945/2359-3997000000343
Ch, Gu, Hou, Zhang, Bai et al., with COVID-19: a systematic review and meta-analysis, doi:10.1101/2020.03.17.20037572
D'avolio, Avataneo, Manca, Cusato, Nicolò et al., 25-Hydroxyvitamin D Concentrations Are Lower in Patients with Positive PCR for SARS-CoV-2, Nutrients, doi:10.3390/nu12051359
Ghasemian, Shamshirian, Heydari, Malekan, Alizadeh-Navaei et al., The Role of Vitamin D in The Age of COVID-19: A Systematic Review and Meta-Analysis Along with an Ecological Approach, doi:10.1101/2020.06.05.20123554
Grant, Lahore, Mcdonnell, Baggerly, French et al., Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths, Nutrients, doi:10.3390/nu12040988
Guan, Ni, Hu, Liang, Ou et al., Clinical characteristics of coronavirus disease 2019 in China, N Engl J Med, doi:10.1056/NEJMoa2002032
Hastie, Mackay, Ho, Celis-Morales, Katikireddi et al., Vitamin D concentrations and COVID-19 infection in UK biobank, Diab Metab Syndrome, doi:10.1016/j.dsx.2020.04.050
Holick, Binkley, Bischoff-Ferrari, Gordon, Hanley et al., Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline, J Clin Endocrinol Metab, doi:10.1210/jc.2011-0385
Huang, Wang, Li, Ren, Zhao et al., Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin Exp Res, doi:10.1007/s40520-020-01570-8
Jevalikar, Mithal, Singh, Sharma, Farooqui et al., Lack of association of baseline 25-hydroxyvitamin D levels with disease severity and mortality in Indian patients hospitalized for COVID-19, Sci Rep, doi:10.1038/s41598-021-85809-y
Jolliffe, Camargo, Sluyter, Aglipay, Aloia et al., Vitamin D supplementation to prevent acute respiratory infections: systematic review and meta-analysis of aggregate data from randomised controlled trials, Lancet Diab Endocrinol, doi:10.1016/S2213-8587(21)00051-6
Laird, Rhodes, Kenny, Vitamin D and inflammation: potential implications for severity of Covid-19, Ir Med J
Larijani, Hossein-Nezhad, Feizabad, Maghbooli, Adibi et al., Vitamin D deficiency, bone turnover markers and causative factors among adolescents: a cross-sectional study, J Diab Metab Disord, doi:10.1186/s40200-016-0266-2
Li, Diagnosis and clinical management of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection: an operational recommendation of Peking union medical college hospital
Maghbooli, Sahraian, Ebrahimi, Pazoki, Kafan et al., Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection, PLoS One, doi:10.1371/journal.pone.0239799
Martineau, Forouhi, Vitamin D for COVID-19: a case to answer?, Lancet Diab Endocrinol, doi:10.1016/S2213-8587(20)30268-0
Mathyssen, Aelbrecht, Serré, Everaerts, Maes et al., Local expression profiles of vitamin D-related genes in airways of COPD patients, Respir Res
Panagiotou, Tee, Ihsan, Athar, Marchitelli et al., Low serum 25-hydroxyvitamin D (25[OH]D) levels in patients hospitalized with COVID-19 are associated with greater disease severity, Clin Endocrinol, doi:10.1111/cen.14276
Patel, Penkert, Jones, Sealy, Surman et al., Baseline Serum Vitamin A and D Levels Determine Benefit of Oral Vitamin A&D Supplements to Humoral Immune Responses Following Pediatric Influenza Vaccination, Viruses, doi:10.3390/v11100907
Perez-Saez, Lauer, Kaiser, Regard, Delaporte et al., Serology-informed estimates of SARS-CoV-2 infection fatality risk in Geneva, Switzerland, Lancet Infect Dis, doi:10.1016/S1473-3099(20)30584-3
Petrilli, Jones, Yang, Rajagopalan, Donnell et al., Factors associated with hospital admission and critical illness among 5279 people with coronavirus disease 2019 in New York City: prospective cohort study, Bmj, doi:10.1136/bmj.m1966
Pham, Rahman, Majidi, Waterhouse, Neale, Acute Respiratory Tract Infection and 25-Hydroxyvitamin D Concentration: A Systematic Review and Meta-Analysis, Int J Environ Res Public Health, doi:10.3390/ijerph16173020
Rhodes, Subramanian, Laird, Kenny, Editorial: low population mortality from COVID-19 in countries south of latitude 35 degrees north supports vitamin D as a factor determining severity, Aliment Pharmacol Ther, doi:10.1111/apt.15777
Richardson, Hirsch, Narasimhan, Crawford, Mcginn et al., Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area, Jama, doi:10.1001/jama.2020.6775
Tabrizi, Moosazadeh, Akbari, Dabbaghmanesh, Mohamadkhani et al., High prevalence of vitamin D deficiency among Iranian population: a systematic review and meta-analysis, Iran J Med Sci
Wintergerst, Maggini, Hornig, Contribution of selected vitamins and trace elements to immune function, Ann Nutr Metab, doi:10.1159/000107673
Xu, Yang, Chen, Luo, Zhang et al., Vitamin D alleviates lipopolysaccharide-induced acute lung injury via regulation of the reninangiotensin system, Mol Med Rep, doi:10.3892/mmr.2017.7546
Zheng, Peng, Xu, Zhao, Liu et al., Risk factors of critical & mortal COVID-19 cases: a systematic literature review and meta-analysis, J Inf Secur
Zhou, Yu, Du, Fan, Liu et al., Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study, Lancet
DOI record:
{
"DOI": "10.1186/s12879-021-06168-7",
"ISSN": [
"1471-2334"
],
"URL": "http://dx.doi.org/10.1186/s12879-021-06168-7",
"abstract": "<jats:title>Abstract</jats:title><jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>A protective effect of vitamin D against COVID-19 infection is under investigation. We aimed to analyze the effect of vitamin D sufficiency on the clinical outcomes of patients infected with COVID-19.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Methods</jats:title>\n <jats:p>In this cross-sectional study we analyzed the vitamin D levels of COVID-19 patients who were admitted to Razi Hospital (an infectious disease referral center in Mazandaran province in northern Iran) from February to March 2020. Overall, a cutoff point of 30 ng/mL was used for the definition of vitamin D sufficiency.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>One hundred fifty-three patients were analyzed in this study who had laboratory documentation of a 25(OH) D level at the time of hospitalization. The vitamin D levels of the patients were 27.19 ± 20.17 ng/mL. In total, 62.7% (<jats:italic>n</jats:italic> = 96) of the patients had a 25(OH) D level of less than 30 ng/mL and 37.25% (<jats:italic>n</jats:italic> = 57) had a 25(OH) D level of more than 30 ng/mL. In total, 49% (<jats:italic>n</jats:italic> = 75) of the patients suffered from at least one underlying disease. The univariate and multivariable regression showed that vitamin D sufficiency was not associated with a statistically significant lower risk of adverse clinical outcomes of COVID-19 such as duration of hospitalization and severity of infection (<jats:italic>P</jats:italic> > 0.05).</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Conclusions</jats:title>\n <jats:p>Sufficient vitamin D levels were not found to be protective against adverse clinical outcomes in patients infected with COVID-19. Chronic disorders in COVID-19 patients were found to have greater relevance than vitamin D levels in determining the adverse outcomes of the infection. Further studies are needed to determine the role of vitamin D level in predicting the outcomes of COVID-19 infection.</jats:p>\n </jats:sec>",
"alternative-id": [
"6168"
],
"article-number": "450",
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "4 December 2020"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "11 May 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "18 May 2021"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Ethics approval and consent to participate",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "This study was approved by the Ethics Committee of Ramsar international branch of Mazandaran University of Medical Sciences with code: IR.MAZUMS.RIB.REC.1399.019. In addition, written informed consent was obtained from all subjects or, for subjects under the age of 18, from a parent and/or legal guardian. In this study all applied methods were carried out in accordance with relevant guidelines and regulations."
},
{
"group": {
"label": "Consent for publication",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "Not applicable."
},
{
"group": {
"label": "Competing interests",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 4,
"value": "The authors declare that they have no competing interests."
}
],
"author": [
{
"affiliation": [],
"family": "Davoudi",
"given": "Alireza",
"sequence": "first"
},
{
"affiliation": [],
"family": "Najafi",
"given": "Narges",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Aarabi",
"given": "Mohsen",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Tayebi",
"given": "Atefeh",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Nikaeen",
"given": "Roja",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Izadyar",
"given": "Hamideh",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Salar",
"given": "Zahra",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Delavarian",
"given": "Leila",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Vaseghi",
"given": "Narges",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Daftarian",
"given": "Zahra",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ahangarkani",
"given": "Fatemeh",
"sequence": "additional"
}
],
"container-title": [
"BMC Infectious Diseases"
],
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2021,
6,
4
]
],
"date-time": "2021-06-04T09:21:56Z",
"timestamp": 1622798516000
},
"deposited": {
"date-parts": [
[
2021,
6,
4
]
],
"date-time": "2021-06-04T09:22:24Z",
"timestamp": 1622798544000
},
"indexed": {
"date-parts": [
[
2022,
4,
22
]
],
"date-time": "2022-04-22T12:51:19Z",
"timestamp": 1650631879410
},
"is-referenced-by-count": 4,
"issn-type": [
{
"type": "electronic",
"value": "1471-2334"
}
],
"issue": "1",
"issued": {
"date-parts": [
[
2021,
5,
18
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2021,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
18
]
],
"date-time": "2021-05-18T00:00:00Z",
"timestamp": 1621296000000
}
},
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
5,
18
]
],
"date-time": "2021-05-18T00:00:00Z",
"timestamp": 1621296000000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1186/s12879-021-06168-7.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1186/s12879-021-06168-7/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1186/s12879-021-06168-7.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1186",
"published": {
"date-parts": [
[
2021,
5,
18
]
]
},
"published-online": {
"date-parts": [
[
2021,
5,
18
]
]
},
"published-print": {
"date-parts": [
[
2021,
12
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.3390/nu12040988",
"doi-asserted-by": "publisher",
"key": "6168_CR1",
"unstructured": "Grant WB, Lahore H, McDonnell SL, Baggerly CA, French CB, Aliano JL, Bhattoa HP: Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths. Nutrients. 2020;12(4):988. https://doi.org/10.3390/nu12040988."
},
{
"DOI": "10.1056/NEJMoa2002032",
"author": "WJ Guan",
"doi-asserted-by": "publisher",
"first-page": "1708",
"issue": "18",
"journal-title": "N Engl J Med",
"key": "6168_CR2",
"unstructured": "Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020;382(18):1708–20. https://doi.org/10.1056/NEJMoa2002032.",
"volume": "382",
"year": "2020"
},
{
"author": "E Laird",
"first-page": "81",
"issue": "5",
"journal-title": "Ir Med J",
"key": "6168_CR3",
"unstructured": "Laird E, Rhodes J, Kenny RA. Vitamin D and inflammation: potential implications for severity of Covid-19. Ir Med J. 2020;113(5):81.",
"volume": "113",
"year": "2020"
},
{
"DOI": "10.1007/s00134-020-05943-5",
"author": "YM Arabi",
"doi-asserted-by": "publisher",
"first-page": "315",
"issue": "2",
"journal-title": "Intensive Care Med",
"key": "6168_CR4",
"unstructured": "Arabi YM, Fowler R, Hayden FG. Critical care management of adults with community-acquired severe respiratory viral infection. Intensive Care Med. 2020;46(2):315–28. https://doi.org/10.1007/s00134-020-05943-5.",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.1080/22221751.2020.1735265",
"author": "T Li",
"doi-asserted-by": "publisher",
"first-page": "582",
"issue": "1",
"journal-title": "Emerg Microbes Infect",
"key": "6168_CR5",
"unstructured": "Li T. Diagnosis and clinical management of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection: an operational recommendation of Peking union medical college hospital (V2.0). Emerg Microbes Infect. 2020;9(1):582–5. https://doi.org/10.1080/22221751.2020.1735265.",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1111/apt.15777",
"author": "JM Rhodes",
"doi-asserted-by": "publisher",
"first-page": "1434",
"issue": "12",
"journal-title": "Aliment Pharmacol Ther",
"key": "6168_CR6",
"unstructured": "Rhodes JM, Subramanian S, Laird E, Kenny RA. Editorial: low population mortality from COVID-19 in countries south of latitude 35 degrees north supports vitamin D as a factor determining severity. Aliment Pharmacol Ther. 2020;51(12):1434–7. https://doi.org/10.1111/apt.15777.",
"volume": "51",
"year": "2020"
},
{
"author": "Z Zheng",
"first-page": "e16",
"issue": "2",
"journal-title": "J Inf Secur",
"key": "6168_CR7",
"unstructured": "Zheng Z, Peng F, Xu B, Zhao J, Liu H, Peng J, et al. Risk factors of critical & mortal COVID-19 cases: a systematic literature review and meta-analysis. J Inf Secur. 2020;81(2):e16–25.",
"volume": "81",
"year": "2020"
},
{
"DOI": "10.1159/000107673",
"author": "ES Wintergerst",
"doi-asserted-by": "publisher",
"first-page": "301",
"issue": "4",
"journal-title": "Ann Nutr Metab",
"key": "6168_CR8",
"unstructured": "Wintergerst ES, Maggini S, Hornig DH. Contribution of selected vitamins and trace elements to immune function. Ann Nutr Metab. 2007;51(4):301–23. https://doi.org/10.1159/000107673.",
"volume": "51",
"year": "2007"
},
{
"DOI": "10.3390/v11100907",
"doi-asserted-by": "publisher",
"key": "6168_CR9",
"unstructured": "Patel N, Penkert RR, Jones BG, Sealy RE, Surman SL, Sun Y, Tang L, DeBeauchamp J, Webb A, Richardson J, et al. Baseline Serum Vitamin A and D Levels Determine Benefit of Oral Vitamin A&D Supplements to Humoral Immune Responses Following Pediatric Influenza Vaccination. Viruses. 2019;11(10):907. https://doi.org/10.3390/v11100907."
},
{
"DOI": "10.1080/14787210.2021.1905519",
"doi-asserted-by": "publisher",
"key": "6168_CR10",
"unstructured": "Banerjee A, Ganguly U, Saha S, Chakrabarti S, Saini RV, Rawal RK, et al. Vitamin D and immuno-pathology of COVID-19: many interactions but uncertain therapeutic benefits. Expert Rev Anti-Infect Ther. 2021:1–14. https://doi.org/10.1080/14787210.2021.1905519."
},
{
"DOI": "10.1016/j.jcv.2010.12.006",
"author": "JA Beard",
"doi-asserted-by": "publisher",
"first-page": "194",
"issue": "3",
"journal-title": "J Clin Virol",
"key": "6168_CR11",
"unstructured": "Beard JA, Bearden A, Striker R. Vitamin D and the anti-viral state. J Clin Virol. 2011;50(3):194–200. https://doi.org/10.1016/j.jcv.2010.12.006.",
"volume": "50",
"year": "2011"
},
{
"DOI": "10.1186/s12931-020-01405-0",
"author": "C Mathyssen",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Respir Res",
"key": "6168_CR12",
"unstructured": "Mathyssen C, Aelbrecht C, Serré J, Everaerts S, Maes K, Gayan-Ramirez G, et al. Local expression profiles of vitamin D-related genes in airways of COPD patients. Respir Res. 2020;21:1–10.",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0239799",
"author": "Z Maghbooli",
"doi-asserted-by": "publisher",
"issue": "9",
"journal-title": "PLoS One",
"key": "6168_CR13",
"unstructured": "Maghbooli Z, Sahraian MA, Ebrahimi M, Pazoki M, Kafan S, Tabriz HM, et al. Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection. PLoS One. 2020;15(9):e0239799. https://doi.org/10.1371/journal.pone.0239799.",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1111/cen.14276",
"doi-asserted-by": "publisher",
"key": "6168_CR14",
"unstructured": "Panagiotou G, Tee SA, Ihsan Y, Athar W, Marchitelli G, Kelly D, et al. Low serum 25-hydroxyvitamin D (25[OH]D) levels in patients hospitalized with COVID-19 are associated with greater disease severity. Clin Endocrinol. 2020;93(4):508–11. https://doi.org/10.1111/cen.14276."
},
{
"DOI": "10.1038/s41598-021-85809-y",
"author": "G Jevalikar",
"doi-asserted-by": "publisher",
"first-page": "6258",
"issue": "1",
"journal-title": "Sci Rep",
"key": "6168_CR15",
"unstructured": "Jevalikar G, Mithal A, Singh A, Sharma R, Farooqui KJ, Mahendru S, et al. Lack of association of baseline 25-hydroxyvitamin D levels with disease severity and mortality in Indian patients hospitalized for COVID-19. Sci Rep. 2021;11(1):6258. https://doi.org/10.1038/s41598-021-85809-y.",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.3390/ijerph16173020",
"doi-asserted-by": "publisher",
"key": "6168_CR16",
"unstructured": "Pham H, Rahman A, Majidi A, Waterhouse M, Neale RE. Acute Respiratory Tract Infection and 25-Hydroxyvitamin D Concentration: A Systematic Review and Meta-Analysis. Int J Environ Res Public Health. 2019;16(17):3020. https://doi.org/10.3390/ijerph16173020."
},
{
"DOI": "10.3390/nu12051359",
"doi-asserted-by": "publisher",
"key": "6168_CR17",
"unstructured": "D'Avolio A, Avataneo V, Manca A, Cusato J, De Nicolò A, Lucchini R, Keller F, Cantù M. 25-Hydroxyvitamin D Concentrations Are Lower in Patients with Positive PCR for SARS-CoV-2. Nutrients. 2020;12(5):1359. https://doi.org/10.3390/nu12051359."
},
{
"DOI": "10.1186/s40200-016-0266-2",
"author": "B Larijani",
"doi-asserted-by": "publisher",
"first-page": "46",
"issue": "1",
"journal-title": "J Diab Metab Disord",
"key": "6168_CR18",
"unstructured": "Larijani B, Hossein-Nezhad A, Feizabad E, Maghbooli Z, Adibi H, Ramezani M, et al. Vitamin D deficiency, bone turnover markers and causative factors among adolescents: a cross-sectional study. J Diab Metab Disord. 2016;15(1):46. https://doi.org/10.1186/s40200-016-0266-2.",
"volume": "15",
"year": "2016"
},
{
"author": "R Tabrizi",
"first-page": "125",
"issue": "2",
"journal-title": "Iran J Med Sci",
"key": "6168_CR19",
"unstructured": "Tabrizi R, Moosazadeh M, Akbari M, Dabbaghmanesh MH, Mohamadkhani M, Asemi Z, et al. High prevalence of vitamin D deficiency among Iranian population: a systematic review and meta-analysis. Iran J Med Sci. 2018;43(2):125–39.",
"volume": "43",
"year": "2018"
},
{
"DOI": "10.1210/jc.2011-0385",
"author": "MF Holick",
"doi-asserted-by": "publisher",
"first-page": "1911",
"issue": "7",
"journal-title": "J Clin Endocrinol Metab",
"key": "6168_CR20",
"unstructured": "Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96(7):1911–30. https://doi.org/10.1210/jc.2011-0385.",
"volume": "96",
"year": "2011"
},
{
"author": "O World Health",
"key": "6168_CR21",
"unstructured": "World Health O. COVID-19 clinical management: living guidance, 25 January 2021. Geneva: World Health Organization; 2021.",
"volume-title": "COVID-19 clinical management: living guidance, 25 January 2021",
"year": "2021"
},
{
"DOI": "10.1016/S1473-3099(20)30584-3",
"author": "J Perez-Saez",
"doi-asserted-by": "publisher",
"first-page": "e69",
"issue": "4",
"journal-title": "Lancet Infect Dis",
"key": "6168_CR22",
"unstructured": "Perez-Saez J, Lauer SA, Kaiser L, Regard S, Delaporte E, Guessous I, et al. Serology-informed estimates of SARS-CoV-2 infection fatality risk in Geneva, Switzerland. Lancet Infect Dis. 2020;21(4):e69–70. https://doi.org/10.1016/S1473-3099(20)30584-3.",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(21)00051-6",
"doi-asserted-by": "publisher",
"key": "6168_CR23",
"unstructured": "Jolliffe D, Camargo CA, Sluyter J, Aglipay M, Aloia J, Bergman P, et al. Vitamin D supplementation to prevent acute respiratory infections: systematic review and meta-analysis of aggregate data from randomised controlled trials. Lancet Diab Endocrinol. 2021;9(5):276–92. https://doi.org/10.1016/S2213-8587(21)00051-6."
},
{
"DOI": "10.3892/mmr.2017.7546",
"author": "J Xu",
"doi-asserted-by": "publisher",
"first-page": "7432",
"issue": "5",
"journal-title": "Mol Med Rep",
"key": "6168_CR24",
"unstructured": "Xu J, Yang J, Chen J, Luo Q, Zhang Q, Zhang H. Vitamin D alleviates lipopolysaccharide-induced acute lung injury via regulation of the renin-angiotensin system. Mol Med Rep. 2017;16(5):7432–8. https://doi.org/10.3892/mmr.2017.7546.",
"volume": "16",
"year": "2017"
},
{
"DOI": "10.1016/j.dsx.2020.04.050",
"author": "CE Hastie",
"doi-asserted-by": "publisher",
"first-page": "561",
"issue": "4",
"journal-title": "Diab Metab Syndrome",
"key": "6168_CR25",
"unstructured": "Hastie CE, Mackay DF, Ho F, Celis-Morales CA, Katikireddi SV, Niedzwiedz CL, et al. Vitamin D concentrations and COVID-19 infection in UK biobank. Diab Metab Syndrome. 2020;14(4):561–5. https://doi.org/10.1016/j.dsx.2020.04.050.",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30268-0",
"author": "AR Martineau",
"doi-asserted-by": "publisher",
"first-page": "735",
"issue": "9",
"journal-title": "Lancet Diab Endocrinol",
"key": "6168_CR26",
"unstructured": "Martineau AR, Forouhi NG. Vitamin D for COVID-19: a case to answer? Lancet Diab Endocrinol. 2020;8(9):735–6. https://doi.org/10.1016/S2213-8587(20)30268-0.",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/j.nfs.2020.06.001",
"doi-asserted-by": "publisher",
"key": "6168_CR27",
"unstructured": "Biesalski HK: Vitamin D deficiency and co-morbidities in COVID-19 patients–a fatal relationship? NFS J. 2020;20:10–21. https://doi.org/10.1016/j.nfs.2020.06.001."
},
{
"author": "H Azadeh",
"first-page": "30",
"issue": "195",
"journal-title": "J Mazandaran Univ Med Sci",
"key": "6168_CR28",
"unstructured": "Azadeh H, Hedayatizadeh-Omran A, Saeedi M, Vahedi-Larijani L, Mehravaran H, Heydari K. Serum vitamin D concentrations in CoVID19 patients. J Mazandaran Univ Med Sci. 2021;31(195):30–6.",
"volume": "31",
"year": "2021"
},
{
"DOI": "10.20945/2359-3997000000343",
"doi-asserted-by": "publisher",
"key": "6168_CR29",
"unstructured": "Brandão C, Chiamolera MI, Biscolla RPM, Lima JVJ, De Francischi Ferrer CM, Prieto WH, de Sá Tavares Russo P, de Sá J, Dos Santos Lazari C, Granato CFH et al. No association between vitamin D status and COVID-19 infection in São Paulo, Brazil. Arch Endocrinol Metab 2021, DOI: https://doi.org/10.20945/2359-3997000000343."
},
{
"DOI": "10.1136/postgradmedj-2020-138712",
"doi-asserted-by": "publisher",
"key": "6168_CR30",
"unstructured": "Baktash V, Hosack T, Patel N, Shah S, Kandiah P, Van Den Abbeele K, et al. Vitamin D status and outcomes for hospitalised older patients with COVID-19. Postgrad Med J. 2020:postgradmedj-2020-138712. https://doi.org/10.1136/postgradmedj-2020-138712."
},
{
"DOI": "10.1101/2020.06.05.20123554",
"doi-asserted-by": "publisher",
"key": "6168_CR31",
"unstructured": "Ghasemian R, Shamshirian A, Heydari K, Malekan M, Alizadeh-Navaei R, Ebrahimzadeh MA, Jafarpour H, Shahmirzadi AR, Khodabandeh M, Seyfari B: The Role of Vitamin D in The Age of COVID-19: A Systematic Review and Meta-Analysis Along with an Ecological Approach. medRxiv. 2020. https://doi.org/10.1101/2020.06.05.20123554."
},
{
"DOI": "10.1101/2020.03.17.20037572",
"doi-asserted-by": "publisher",
"key": "6168_CR32",
"unstructured": "Ma Ch, Gu J, Hou P, Zhang L, Bai Y, Guo Zh, et al. Incidence, clinical characteristics and prognostic factor of patients with COVID-19: a systematic review and meta-analysis. medRxiv. 2020. https://doi.org/10.1101/2020.03.17.20037572."
},
{
"DOI": "10.1136/bmj.m1966",
"doi-asserted-by": "publisher",
"key": "6168_CR33",
"unstructured": "Petrilli CM, Jones SA, Yang J, Rajagopalan H, O’Donnell L, Chernyak Y, et al. Factors associated with hospital admission and critical illness among 5279 people with coronavirus disease 2019 in New York City: prospective cohort study. Bmj. 2020;22;369. https://doi.org/10.1136/bmj.m1966."
},
{
"DOI": "10.1001/jama.2020.6775",
"author": "S Richardson",
"doi-asserted-by": "publisher",
"first-page": "2052",
"issue": "20",
"journal-title": "Jama",
"key": "6168_CR34",
"unstructured": "Richardson S, Hirsch JS, Narasimhan M, Crawford JM, McGinn T, Davidson KW, et al. Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area. Jama. 2020;323(20):2052–9. https://doi.org/10.1001/jama.2020.6775.",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30566-3",
"author": "F Zhou",
"doi-asserted-by": "publisher",
"first-page": "1054",
"issue": "10229",
"journal-title": "Lancet (London, England)",
"key": "6168_CR35",
"unstructured": "Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet (London, England). 2020;395(10229):1054–62.",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"author": "C Huang",
"doi-asserted-by": "publisher",
"first-page": "497",
"issue": "10223",
"journal-title": "Lancet (London, England)",
"key": "6168_CR36",
"unstructured": "Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet (London, England). 2020;395(10223):497–506.",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1007/s40520-020-01570-8",
"doi-asserted-by": "publisher",
"key": "6168_CR37",
"unstructured": "Ilie PC, Stefanescu S, Smith L. The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality. Aging Clin Exp Res. 2020;32(7):1195–8. https://doi.org/10.1007/s40520-020-01570-8."
}
],
"reference-count": 37,
"references-count": 37,
"relation": {},
"resource": {
"primary": {
"URL": "https://bmcinfectdis.biomedcentral.com/articles/10.1186/s12879-021-06168-7"
}
},
"score": 1,
"short-container-title": [
"BMC Infect Dis"
],
"short-title": [],
"source": "Crossref",
"subject": [
"Infectious Diseases"
],
"subtitle": [],
"title": [
"Lack of association between vitamin D insufficiency and clinical outcomes of patients with COVID-19 infection"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "21"
}
