Reduction of SARS-CoV-2 viral load in saliva after rinsing with mouthwashes containing cetylpyridinium chloride: a randomized clinical study
et al., PeerJ, doi:10.7717/peerj.15080, NCT04902976, Dec 2023
58th treatment shown to reduce risk in
September 2025, now with p = 0.0035 from 4 studies.
Lower risk for recovery and viral clearance.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
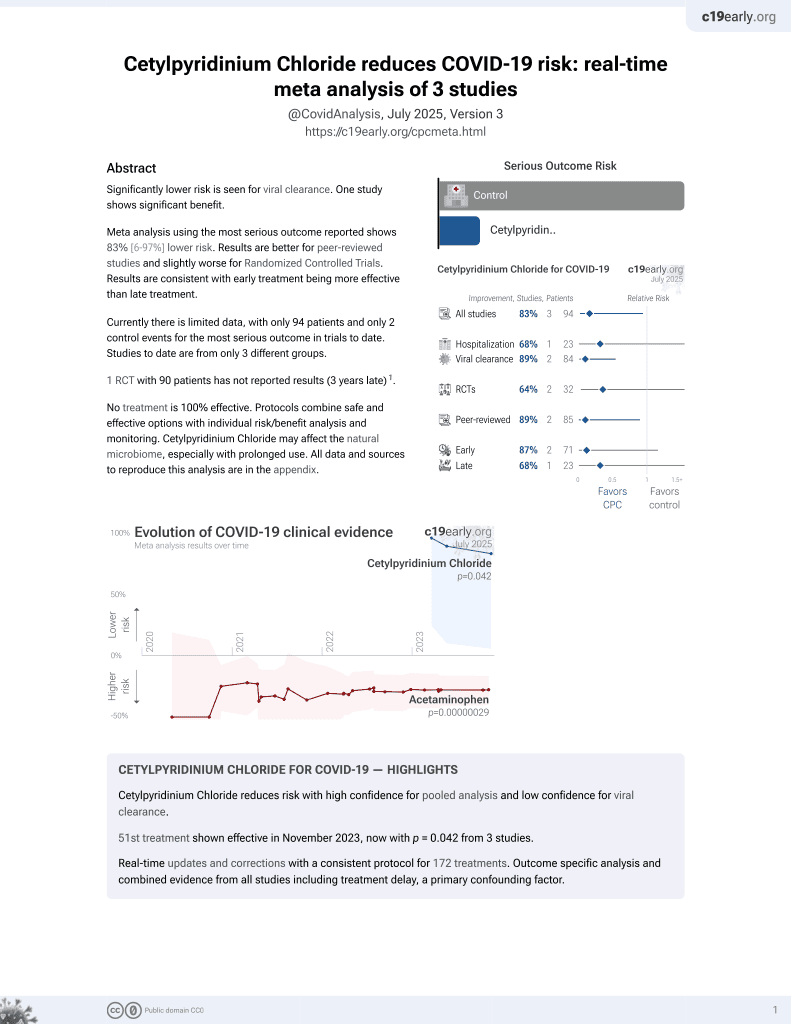
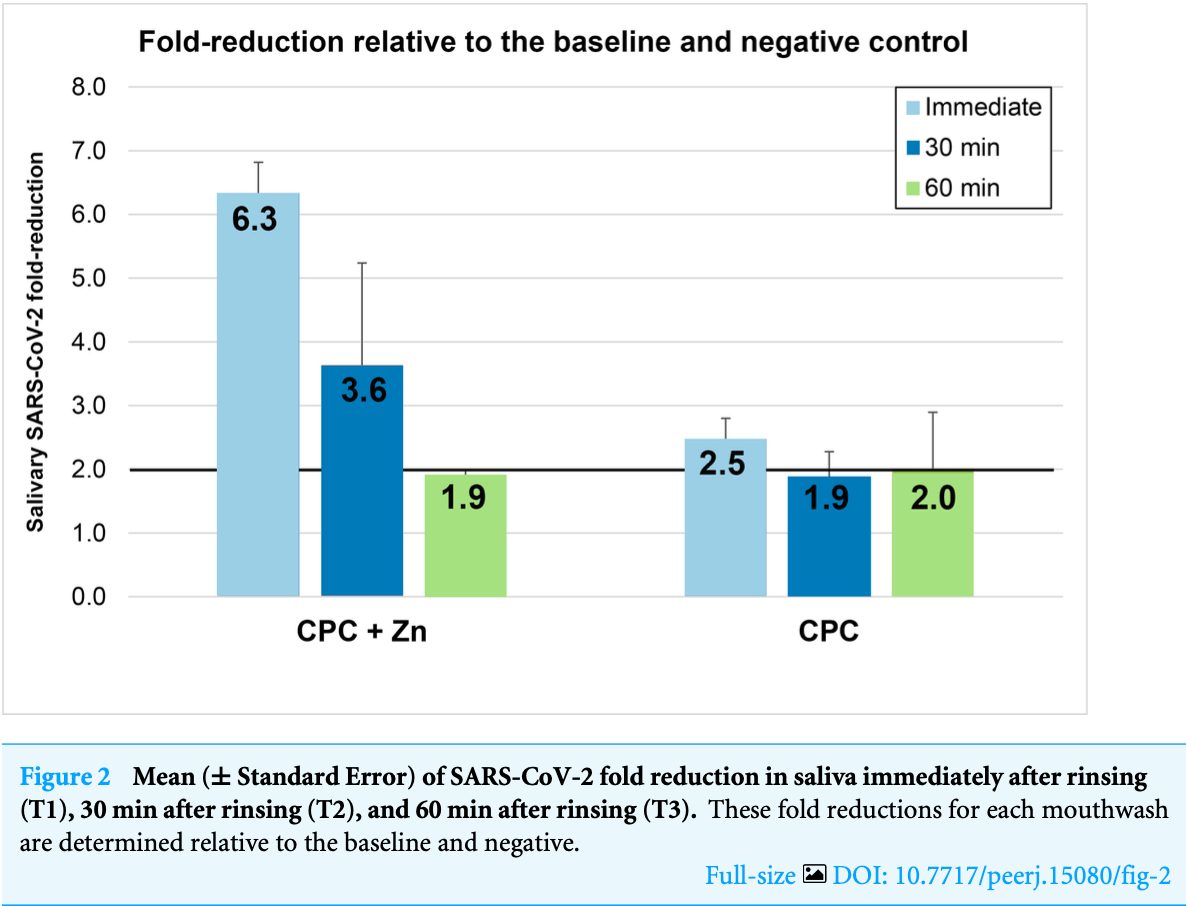
RCT 95 hospitalized COVID-19 patients showing reduced salivary SARS-CoV-2 viral load after rinsing with cetylpyridinium chloride (CPC) or CPC plus zinc mouthwashes. CPC plus zinc mouthwash reduced viral load by 6.3-fold at 5 minutes, 3.6-fold at 30 minutes, and 1.9-fold at 60 minutes compared to baseline. CPC alone reduced viral load by 2.5-fold at 5 minutes, 1.9-fold at 30 minutes, and 2.0-fold at 60 minutes. Results are only provided for short-term viral load via PCR.
The paper claims inclusion of up to 7 days symptoms, but the clinical data shows many patients with longer delays, up to 11 days.
Analysis of short-term changes in viral load using PCR may not detect
effective treatments because PCR is unable to differentiate between intact
infectious virus and non-infectious or destroyed virus particles. For example
Tarragó-Gil, Alemany perform RCTs with cetylpyridinium chloride
(CPC) mouthwash that show no difference in PCR viral load, however there was
significantly increased detection of SARS-CoV-2 nucleocapsid protein,
indicating viral lysis. CPC inactivates SARS-CoV-2 by degrading its membrane,
exposing the nucleocapsid of the virus. To better estimate changes in viral
load and infectivity, methods like viral culture that can
differentiate intact vs. degraded virus are preferred.
This study is excluded in meta-analysis:
study only provides short-term viral load results.
|
fold change relative to baseline and control, 50.0% lower, RR 0.50, p = 0.005, treatment 31, control 32, inverted to make RR<1 favor treatment, 60 min.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Bezinelli et al., 18 Dec 2023, Double Blind Randomized Controlled Trial, Brazil, peer-reviewed, 10 authors, trial NCT04902976 (history).
Reduction of SARS-CoV-2 viral load in saliva after rinsing with mouthwashes containing cetylpyridinium chloride: a randomized clinical study
PeerJ, doi:10.7717/peerj.15080
Background. Symptomatic patients with COVID-19 typically have a high SARS-CoV-2 viral load in their saliva. Procedures to reduce the viral load in their oral cavity are important for mitigating the viral transmission. Methods. This randomized clinical trial investigated the impact of two mouthwashes (0.075% cetylpyridinium chloride plus 0.28% zinc lactate (CPC+Zn) (n = 32), and 0.075% cetylpyridinium chloride (CPC) (n = 31)) on the viral load of SARS-CoV-2 in saliva when compared to the distilled water negative control (n = 32). Saliva was collected before (T0) and after (5 min, T1; 30 min, T2; and 60 min, T3) the intervention. Viral load in saliva was measured by qRT-PCR assays. The data in both groups was normalized for T0 and Negative Control, resulting in fold change values. Results. CPC+Zn oral solution reduced the viral load in saliva by 6.34-fold at T1, 3.6fold at T2 and 1.9-fold at T3. Rinsing with the CPC mouthwash reduced the viral load in saliva by 2.5-fold at T1, 1.9-fold at T2 and 2.0-fold at T3. Conclusion. CPC+Zn mouthwash or with the CPC mouthwash reduced the viral load in saliva of COVID-19 patients immediately after rinsing. These reductions extended up to 60 min.
ADDITIONAL INFORMATION AND DECLARATIONS Funding The study was funded by the Colgate-Palmolive Company and the Latin American Oral Health Association. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Grant Disclosures The following grant information was disclosed by the authors: Colgate-Palmolive Company and Latin American Oral Health Association.
Competing Interests The authors declare there are no competing interests.
Author Contributions • Leticia M. Bezinelli conceived and designed the experiments, analyzed the data, authored or reviewed drafts of the article, and approved the final draft. • Luciana Corrêa conceived and designed the experiments, analyzed the data, prepared figures and/or tables, authored or reviewed drafts of the article, and approved the final draft. • Stephany Beyerstedt performed the experiments, authored or reviewed drafts of the article, and approved the final draft. • Marcella L. Franco performed the experiments, authored or reviewed drafts of the article, and approved the final draft. • Érika B. Rangel analyzed the data, authored or reviewed drafts of the article, and approved the final draft. • Carlos Guillermo Benítez performed the experiments, analyzed the data, prepared figures and/or tables, authored or reviewed drafts of the article, and approved the final draft. • Nelson Hamerschlak conceived and designed the experiments, authored or reviewed drafts of the..
References
Alemany, Perez-Zsolt, Raïch-Regué, Basagoiti, Ouchi et al., Cetylpyridinium chloride mouthwash to reduce shedding of infectious SARS-CoV-2: a double-blind randomized clinical trial, Journal of Dental Research, doi:10.1177/00220345221102310
Alzahrani, Bamashmous, Alkharobi, Alghamdi, Alharbi et al., Mouth rinses efficacy on salivary SARS-CoV-2 viral load: a randomized clinical trial, Journal of Medical Virology, doi:10.1002/jmv.28412
Anderson, Patterson, Richards, Pitol, Edwards et al., CPC-containing oral rinses inactivate SARS-CoV-2 variants and are active in the presence of human saliva, Journal of Medical Microbiology, doi:10.1099/jmm.0.001508
Ausina-Márquez, Ferrer, Oral antiseptics against coronavirus: in-vitro and clinical evidence, Journal of Hospital Infection, doi:10.1016/j.jhin.2021.04.004
Barrueco, Moreno, Martínez-Beneyto, García-Vázquez, González et al., Effect of oral antiseptics in reducing SARS-CoV-2 infectivity: evidence from a randomized double-blind clinical trial, Emerging Microbes & Infections, doi:10.1080/22221751.2022.2098059
Basagoiti, Perez-Zsolt, León, Blanc, Raïch-Regué et al., Mouthwashes with CPC reduce the infectivity of SARS-CoV-2 variants in vitro, Journal of Dental Research, doi:10.1177/00220345211029269
Bañó-Polo, Martínez-Gil, Del Pino, Massoli, Mingarro et al., Cetylpyridinium chloride promotes disaggregation of SARS-CoV-2 virus-like particles, Journal of Oral Microbiology, doi:10.1080/20002297.2022.2030094
Bezinelli, Corrêa, Beyerstedt, Rangel, Benitez et al., Antimicrobial oral lavage reduces the SARS-CoV-2 load in intubated patients: randomized clinical trial, Journal of Oral Microbiology, doi:10.1080/20002297.2022.2152179
Bezinelli, None, PeerJ
Carrouel, Gonçalves, Conte, Campus, Fisher et al., Antiviral activity of reagents in mouth rinses against SARS-CoV-2, Journal of Dental Research, doi:10.1177/0022034520967933
Dalman, Deeter, Nimishakavi, Duan, Fold change and p-value cutoffs significantly alter microarray interpretations, BMC Bioinformatics, doi:10.1186/1471-2105-13-S2-S11
Do Amaral, Hassan, Sloniak, Pannuti, Romito et al., Effects of antimicrobial mouthwashes on the human oral microbiome: systematic review of controlled clinical trials, International Journal of Dental Hygiene, doi:10.1111/idh.12617
Eby, Zinc ion availability-the determinant of efficacy in zinc lozenge treatment of common colds, Journal of Antimicrobial Chemotherapy, doi:10.1093/oxfordjournals.jac.a020864
Eduardo, Corrêa, Heller, Daep, Benitez et al., Salivary SARS-CoV-2 load reduction with mouthwash use: a randomized pilot clinical trial, Heliyon, doi:10.1016/j.heliyon.2021.e07346
Feres, Figueiredo, Faveri, Stewart, De Vizio, The effectiveness of a preprocedural mouthrinse containing cetylpyridinium chloride in reducing bacteria in the dental office, The Journal of the American Dental Association, doi:10.14219/jada.archive.2010.0193
Fernandes, Pacheco, Borges, Athwal, De et al., Saliva in the diagnosis of COVID-19: a review and new research directions, Journal of Dental Research, doi:10.1177/0022034520960070
Ferrer, Barrueco, Martinez-Beneyto, Moreno, Ausina-Márquez et al., Clinical evaluation of antiseptic mouth rinses to reduce salivary load of SARS-CoV-2, Scientific Reports, doi:10.1038/s41598-021-03461-y
Hartig, Stephens, Foster, Fontes, Kinzel et al., Stopping the COVID-19 pandemic in dental offices: a review of SARS-CoV-2 transmission and cross-infection prevention, Experimental Biology and Medicine, doi:10.1177/15353702211034164
He, Wei, Fan, Hu, Sreenivasan, A clinical study to assess the 12-hour antimicrobial effects of cetylpyridinium chloride mouthwashes on supragingival plaque bacteria, Journal of Clinical Dentistry
Hu, Li, Sreenivasan, Vizio, A randomized, double-blind clinical study to assess the antimicrobial effects of a cetylpyridinium chloride mouth rinse on dental plaque bacteria, Clinical Therapeutics, doi:10.1016/j.clinthera.2009.11.004
Huang, Pérez, Kato, Mikami, Okuda et al., Autopsy Consortium, HCA Oral and Craniofacial Biological Network, Nature Medicine, doi:10.1038/s41591-021-01296-8
Iebba, Zanotta, Campisciano, Zerbato, Bella et al., Profiling of oral microbiota and cytokines in COVID-19 patients, Frontiers in Microbiology, doi:10.3389/fmicb.2021.671813
Izzetti, Nisi, Gabriele, Graziani, COVID-19 transmission in dental practice: brief review of preventive measures in Italy, Journal of Dental Research, doi:10.1177/0022034520920580
Koch-Heier, Hoffmann, Schindler, Lussi, Planz, Inactivation of SARS-CoV-2 through Treatment with the Mouth Rinsing Solutions ViruProX ® and BacterX ® Pro, Microorganisms, doi:10.3390/microorganisms9030521
Komine, Yamaguchi, Okamoto, Yamamoto, Virucidal activity of oral care products against SARS-CoV-2 in vitro, Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology, doi:10.1016/j.ajoms.2021.02.002
Mendoza, Ubillús, Bolívar, Palacios, Lopez et al., Antiviral effect of mouthwashes against SARS-COV-2: a systematic review, The Saudi Dental Journal, doi:10.1016/j.sdentj.2022.01.006
Miller, Annavajhala, Chong, Park, Nobel et al., Oral microbiome alterations and SARS-CoV-2 saliva viral load in patients with COVID-19, Microbiology Spectrum, doi:10.1128/Spectrum.00055-21
Okamoto, Saito, Okabayashi, Komine, Virucidal activity and mechanism of action of cetylpyridinium chloride against SARS-CoV-2, Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology, doi:10.1016/j.ajoms.2022.04.001
Read, Obeid, Ahlenstiel, Ahlenstiel, The role of zinc in antiviral immunity, Advances in Nutrition, doi:10.1093/advances/nmz013
Ren, Wang, Cui, Lu, Wang et al., Alterations in the human oral and gut microbiomes and lipidomics in COVID-19, Gut, doi:10.1136/gutjnl-2020-323826
Retamal-Valdes, Soares, Stewart, Figueiredo, Faveri et al., Effectiveness of a pre-procedural mouthwash in reducing bacteria in dental aerosols: randomized clinical trial, Brazilian Oral Research, doi:10.1590/1807-3107BOR-2017.vol31.0021
Saadh, Almaaytah, Alaraj, Dababneh, Sa'adeh et al., Punicalagin and zinc (II) ions inhibit the activity of SARS-CoV-2 3CL-protease in vitro, European Review for Medical and Pharmacological Sciences, doi:10.26355/eurrev_202105_25958
Sarma, Gumber, Kilpatrick, Effect of CPC mouthrinses on spike protein binding to ACE2 receptor, Journal of Dental Research
Seneviratne, Balan, Ko, Udawatte, Lai et al., Efficacy of commercial mouth-rinses on SARS-CoV-2 viral load in saliva: randomized control trial in Singapore, Infection, doi:10.1007/s15010-020-01563-9
Takeda, Sawa, Sasaki, Orba, Maishi et al., Antiviral effect of cetylpyridinium chloride in mouthwash on SARS-CoV-2, Scientific Reports, doi:10.1038/s41598-022-18367-6
Velthuis, Van Den Worm, Sims, Baric, Snijder et al., Zn(2+) inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture, PLOS Pathogens, doi:10.1371/journal.ppat.1001176
Viloria Winnett, Porter, Romano, Savela, Akana et al., Morning SARS-CoV-2 testing yields better detection of infection due to higher viral loads in saliva and nasal swabs upon waking, Microbiology Spectrum, doi:10.1128/spectrum.03873-22
Wyllie, Fournier, Casanovas-Massana, Campbell, Tokuyama et al., Saliva or Nasopharyngeal Swab Specimens for Detection of SARS-CoV-2, New England Journal of Medicine, doi:10.1056/NEJMc2016359
Yoon, Yoon, Song, Yoon, Lim et al., Clinical significance of a high SARS-CoV-2 viral load in the saliva, Journal of Korean Medical Science, doi:10.3346/jkms.2020.35.e195
Zhao, Erwin, Xue, How many differentially expressed genes: a perspective from the comparison of genotypic and phenotypic distances, Genomics, doi:10.1016/j.ygeno.2017.08.007
Zhu, Guo, Xu, Chen, Viral dynamics of SARS-CoV-2 in saliva from infected patients, Journal of Infection, doi:10.1016/j.jinf.2020.06.059
DOI record:
{
"DOI": "10.7717/peerj.15080",
"ISSN": [
"2167-8359"
],
"URL": "http://dx.doi.org/10.7717/peerj.15080",
"abstract": "<jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>Symptomatic patients with COVID-19 typically have a high SARS-CoV-2 viral load in their saliva. Procedures to reduce the viral load in their oral cavity are important for mitigating the viral transmission.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>Methods</jats:title>\n <jats:p>This randomized clinical trial investigated the impact of two mouthwashes (0.075% cetylpyridinium chloride plus 0.28% zinc lactate (CPC+Zn) (<jats:italic>n</jats:italic> = 32), and 0.075% cetylpyridinium chloride (CPC) (<jats:italic>n</jats:italic> = 31)) on the viral load of SARS-CoV-2 in saliva when compared to the distilled water negative control (<jats:italic>n</jats:italic> = 32). Saliva was collected before (T0) and after (5 min, T1; 30 min, T2; and 60 min, T3) the intervention. Viral load in saliva was measured by qRT-PCR assays. The data in both groups was normalized for T0 and Negative Control, resulting in fold change values.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>CPC+Zn oral solution reduced the viral load in saliva by 6.34-fold at T1, 3.6-fold at T2 and 1.9-fold at T3. Rinsing with the CPC mouthwash reduced the viral load in saliva by 2.5-fold at T1, 1.9-fold at T2 and 2.0-fold at T3.</jats:p>\n </jats:sec>\n <jats:sec>\n <jats:title>Conclusion</jats:title>\n <jats:p>CPC+Zn mouthwash or with the CPC mouthwash reduced the viral load in saliva of COVID-19 patients immediately after rinsing. These reductions extended up to 60 min.</jats:p>\n </jats:sec>",
"alternative-id": [
"10.7717/peerj.15080"
],
"article-number": "e15080",
"author": [
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
}
],
"family": "Bezinelli",
"given": "Leticia M.",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Universidade de São Paulo, Sao Paulo, Brazil"
}
],
"family": "Corrêa",
"given": "Luciana",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
}
],
"family": "Beyerstedt",
"given": "Stephany",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
}
],
"family": "Franco",
"given": "Marcella L.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
}
],
"family": "Rangel",
"given": "Érika B.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Latin American Oral Health Association, Sao Paulo, Brazil"
}
],
"family": "Benítez",
"given": "Carlos Guillermo",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
}
],
"family": "Hamerschlak",
"given": "Nelson",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
}
],
"family": "Pinho",
"given": "João R.R.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
},
{
"name": "Universidade Cruzeiro do Sul, Sao Paulo, Brazil"
},
{
"name": "University of Texas at San Antonio, San Antonio, TX, United States of America"
}
],
"family": "Heller",
"given": "Debora",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Hospital Israelita Albert Einstein, Sao Paulo, Brazil"
}
],
"family": "Eduardo",
"given": "Fernanda P.",
"sequence": "additional"
}
],
"container-title": "PeerJ",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
12,
18
]
],
"date-time": "2023-12-18T08:11:20Z",
"timestamp": 1702887080000
},
"deposited": {
"date-parts": [
[
2023,
12,
18
]
],
"date-time": "2023-12-18T08:11:33Z",
"timestamp": 1702887093000
},
"funder": [
{
"name": "Colgate-Palmolive Company and Latin American Oral Health Association"
}
],
"indexed": {
"date-parts": [
[
2023,
12,
19
]
],
"date-time": "2023-12-19T00:38:41Z",
"timestamp": 1702946321443
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2023,
12,
18
]
]
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "unspecified",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
12,
18
]
],
"date-time": "2023-12-18T00:00:00Z",
"timestamp": 1702857600000
}
}
],
"link": [
{
"URL": "https://peerj.com/articles/15080.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://peerj.com/articles/15080.xml",
"content-type": "application/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://peerj.com/articles/15080.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://peerj.com/articles/15080.pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "4443",
"original-title": [],
"page": "e15080",
"prefix": "10.7717",
"published": {
"date-parts": [
[
2023,
12,
18
]
]
},
"published-online": {
"date-parts": [
[
2023,
12,
18
]
]
},
"publisher": "PeerJ",
"reference": [
{
"DOI": "10.1177/00220345221102310",
"article-title": "Cetylpyridinium chloride mouthwash to reduce shedding of infectious SARS-CoV-2: a double-blind randomized clinical trial",
"author": "Alemany",
"doi-asserted-by": "publisher",
"first-page": "220345221102310",
"journal-title": "Journal of Dental Research",
"key": "10.7717/peerj.15080/ref-1",
"volume": "21",
"year": "2022"
},
{
"DOI": "10.1002/jmv.28412",
"article-title": "Mouth rinses efficacy on salivary SARS-CoV-2 viral load: a randomized clinical trial",
"author": "Alzahrani",
"doi-asserted-by": "publisher",
"first-page": "e28412",
"issue": "1",
"journal-title": "Journal of Medical Virology",
"key": "10.7717/peerj.15080/ref-2",
"volume": "95",
"year": "2023"
},
{
"DOI": "10.1099/jmm.0.001508",
"article-title": "CPC-containing oral rinses inactivate SARS-CoV-2 variants and are active in the presence of human saliva",
"author": "Anderson",
"doi-asserted-by": "publisher",
"first-page": "001508",
"issue": "2",
"journal-title": "Journal of Medical Microbiology",
"key": "10.7717/peerj.15080/ref-3",
"volume": "71",
"year": "2022"
},
{
"DOI": "10.1080/20002297.2022.2030094",
"article-title": "Cetylpyridinium chloride promotes disaggregation of SARS-CoV-2 virus-like particles",
"author": "Bañó-Polo",
"doi-asserted-by": "publisher",
"first-page": "2030094",
"issue": "1",
"journal-title": "Journal of Oral Microbiology",
"key": "10.7717/peerj.15080/ref-4",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1177/00220345211029269",
"article-title": "Mouthwashes with CPC reduce the infectivity of SARS-CoV-2 variants in vitro",
"author": "Muñoz Basagoiti",
"doi-asserted-by": "publisher",
"first-page": "1265",
"issue": "11",
"journal-title": "Journal of Dental Research",
"key": "10.7717/peerj.15080/ref-5",
"volume": "100",
"year": "2021"
},
{
"DOI": "10.1080/20002297.2022.2152179",
"article-title": "Antimicrobial oral lavage reduces the SARS-CoV-2 load in intubated patients: randomized clinical trial",
"author": "Bezinelli",
"doi-asserted-by": "publisher",
"first-page": "2152179",
"issue": "1",
"journal-title": "Journal of Oral Microbiology",
"key": "10.7717/peerj.15080/ref-6",
"volume": "15",
"year": "2023"
},
{
"DOI": "10.1177/0022034520967933",
"article-title": "Antiviral activity of reagents in mouth rinses against SARS-CoV-2",
"author": "Carrouel",
"doi-asserted-by": "publisher",
"first-page": "124",
"issue": "2",
"journal-title": "Journal of Dental Research",
"key": "10.7717/peerj.15080/ref-7",
"volume": "100",
"year": "2021"
},
{
"DOI": "10.1186/1471-2105-13-S2-S11",
"article-title": "Fold change and p-value cutoffs significantly alter microarray interpretations",
"author": "Dalman",
"doi-asserted-by": "publisher",
"first-page": "S11",
"issue": "Suppl 2",
"journal-title": "BMC Bioinformatics",
"key": "10.7717/peerj.15080/ref-8",
"volume": "13",
"year": "2012"
},
{
"DOI": "10.1111/idh.12617",
"article-title": "Effects of antimicrobial mouthwashes on the human oral microbiome: systematic review of controlled clinical trials",
"author": "do Amaral",
"doi-asserted-by": "publisher",
"first-page": "128",
"issue": "1",
"journal-title": "International Journal of Dental Hygiene",
"key": "10.7717/peerj.15080/ref-9",
"volume": "21",
"year": "2023"
},
{
"DOI": "10.1093/oxfordjournals.jac.a020864",
"article-title": "Zinc ion availability–the determinant of efficacy in zinc lozenge treatment of common colds",
"author": "Eby",
"doi-asserted-by": "publisher",
"first-page": "483",
"issue": "4",
"journal-title": "Journal of Antimicrobial Chemotherapy",
"key": "10.7717/peerj.15080/ref-10",
"volume": "40",
"year": "1997"
},
{
"DOI": "10.1016/j.heliyon.2021.e07346",
"article-title": "Salivary SARS-CoV-2 load reduction with mouthwash use: a randomized pilot clinical trial",
"author": "Eduardo",
"doi-asserted-by": "publisher",
"first-page": "e07346",
"issue": "6",
"journal-title": "Heliyon",
"key": "10.7717/peerj.15080/ref-11",
"volume": "7",
"year": "2021"
},
{
"DOI": "10.14219/jada.archive.2010.0193",
"article-title": "The effectiveness of a preprocedural mouthrinse containing cetylpyridinium chloride in reducing bacteria in the dental office",
"author": "Feres",
"doi-asserted-by": "publisher",
"first-page": "415",
"issue": "4",
"journal-title": "The Journal of the American Dental Association",
"key": "10.7717/peerj.15080/ref-12",
"volume": "141",
"year": "2010"
},
{
"DOI": "10.1177/0022034520960070",
"article-title": "Saliva in the diagnosis of COVID-19: a review and new research directions",
"author": "Fernandes",
"doi-asserted-by": "publisher",
"first-page": "1435",
"issue": "13",
"journal-title": "Journal of Dental Research",
"key": "10.7717/peerj.15080/ref-13",
"volume": "99",
"year": "2020"
},
{
"DOI": "10.1038/s41598-021-03461-y",
"article-title": "Clinical evaluation of antiseptic mouth rinses to reduce salivary load of SARS-CoV-2",
"author": "Ferrer",
"doi-asserted-by": "publisher",
"first-page": "24392",
"issue": "1",
"journal-title": "Scientific Reports 22;",
"key": "10.7717/peerj.15080/ref-14",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1177/15353702211034164",
"article-title": "Stopping the COVID-19 pandemic in dental offices: a review of SARS-CoV-2 transmission and cross-infection prevention",
"author": "Hartig",
"doi-asserted-by": "publisher",
"first-page": "15353702211034164",
"journal-title": "Experimental Biology and Medicine",
"key": "10.7717/peerj.15080/ref-15",
"volume": "3",
"year": "2021"
},
{
"article-title": "A clinical study to assess the 12-hour antimicrobial effects of cetylpyridinium chloride mouthwashes on supragingival plaque bacteria",
"author": "He",
"first-page": "195",
"issue": "6",
"journal-title": "Journal of Clinical Dentistry",
"key": "10.7717/peerj.15080/ref-16",
"volume": "22",
"year": "2011"
},
{
"DOI": "10.1016/j.clinthera.2009.11.004",
"article-title": "A randomized, double-blind clinical study to assess the antimicrobial effects of a cetylpyridinium chloride mouth rinse on dental plaque bacteria",
"author": "Hu",
"doi-asserted-by": "publisher",
"first-page": "2540",
"issue": "11",
"journal-title": "Clinical Therapeutics",
"key": "10.7717/peerj.15080/ref-17",
"volume": "31",
"year": "2009"
},
{
"DOI": "10.1038/s41591-021-01296-8",
"article-title": "SARS-CoV-2 infection of the oral cavity and saliva",
"author": "Huang",
"doi-asserted-by": "publisher",
"first-page": "892",
"issue": "5",
"journal-title": "Nature Medicine",
"key": "10.7717/peerj.15080/ref-18",
"volume": "27",
"year": "2021"
},
{
"DOI": "10.3389/fmicb.2021.671813",
"article-title": "Profiling of oral microbiota and cytokines in COVID-19 patients",
"author": "Iebba",
"doi-asserted-by": "publisher",
"first-page": "671813",
"journal-title": "Frontiers in Microbiology",
"key": "10.7717/peerj.15080/ref-19",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1177/0022034520920580",
"article-title": "COVID-19 transmission in dental practice: brief review of preventive measures in Italy",
"author": "Izzetti",
"doi-asserted-by": "publisher",
"first-page": "1030",
"issue": "9",
"journal-title": "Journal of Dental Research",
"key": "10.7717/peerj.15080/ref-20",
"volume": "99",
"year": "2020"
},
{
"DOI": "10.3390/microorganisms9030521",
"article-title": "Inactivation of SARS-CoV-2 through Treatment with the Mouth Rinsing Solutions ViruProX® and BacterX® Pro",
"author": "Koch-Heier",
"doi-asserted-by": "publisher",
"first-page": "521",
"issue": "3",
"journal-title": "Microorganisms",
"key": "10.7717/peerj.15080/ref-21",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1016/j.ajoms.2021.02.002",
"article-title": "Virucidal activity of oral care products against SARS-CoV-2 in vitro",
"author": "Komine",
"doi-asserted-by": "publisher",
"first-page": "475",
"issue": "4",
"journal-title": "Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology",
"key": "10.7717/peerj.15080/ref-22",
"volume": "33",
"year": "2021"
},
{
"DOI": "10.1016/j.jhin.2021.04.004",
"article-title": "Oral antiseptics against coronavirus: in-vitro and clinical evidence",
"author": "Mateos-Moreno",
"doi-asserted-by": "publisher",
"first-page": "30",
"journal-title": "Journal of Hospital Infection",
"key": "10.7717/peerj.15080/ref-23",
"volume": "113",
"year": "2021"
},
{
"DOI": "10.1016/j.sdentj.2022.01.006",
"article-title": "Antiviral effect of mouthwashes against SARS-COV-2: a systematic review",
"author": "Mezarina Mendoza",
"doi-asserted-by": "publisher",
"first-page": "167",
"issue": "3",
"journal-title": "The Saudi Dental Journal",
"key": "10.7717/peerj.15080/ref-24",
"volume": "34",
"year": "2022"
},
{
"DOI": "10.1128/Spectrum.00055-21",
"article-title": "Oral microbiome alterations and SARS-CoV-2 saliva viral load in patients with COVID-19",
"author": "Miller",
"doi-asserted-by": "publisher",
"first-page": "e0005521",
"issue": "2",
"journal-title": "Microbiology Spectrum",
"key": "10.7717/peerj.15080/ref-25",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1016/j.ajoms.2022.04.001",
"article-title": "Virucidal activity and mechanism of action of cetylpyridinium chloride against SARS-CoV-2",
"author": "Okamoto",
"doi-asserted-by": "publisher",
"first-page": "800",
"issue": "6",
"journal-title": "Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology",
"key": "10.7717/peerj.15080/ref-26",
"volume": "34",
"year": "2022"
},
{
"DOI": "10.1093/advances/nmz013",
"article-title": "The role of zinc in antiviral immunity",
"author": "Read",
"doi-asserted-by": "publisher",
"first-page": "696",
"issue": "4",
"journal-title": "Advances in Nutrition",
"key": "10.7717/peerj.15080/ref-27",
"volume": "10",
"year": "2019"
},
{
"DOI": "10.1136/gutjnl-2020-323826",
"article-title": "Alterations in the human oral and gut microbiomes and lipidomics in COVID-19",
"author": "Ren",
"doi-asserted-by": "publisher",
"first-page": "1253",
"issue": "7",
"journal-title": "Gut",
"key": "10.7717/peerj.15080/ref-28",
"volume": "70",
"year": "2021"
},
{
"DOI": "10.1590/1807-3107BOR-2017.vol31.0021",
"article-title": "Effectiveness of a pre-procedural mouthwash in reducing bacteria in dental aerosols: randomized clinical trial",
"author": "Retamal-Valdes",
"doi-asserted-by": "publisher",
"first-page": "e21",
"journal-title": "Brazilian Oral Research",
"key": "10.7717/peerj.15080/ref-29",
"volume": "31",
"year": "2017"
},
{
"DOI": "10.26355/eurrev_202105_25958",
"article-title": "Punicalagin and zinc (II) ions inhibit the activity of SARS-CoV-2 3CL-protease in vitro",
"author": "Saadh",
"doi-asserted-by": "publisher",
"first-page": "3908",
"issue": "10",
"journal-title": "European Review for Medical and Pharmacological Sciences",
"key": "10.7717/peerj.15080/ref-30",
"volume": "25",
"year": "2021"
},
{
"DOI": "10.1080/22221751.2022.2098059",
"article-title": "Effect of oral antiseptics in reducing SARS-CoV-2 infectivity: evidence from a randomized double-blind clinical trial",
"author": "Sánchez Barrueco",
"doi-asserted-by": "publisher",
"first-page": "1833",
"issue": "1",
"journal-title": "Emerging Microbes & Infections",
"key": "10.7717/peerj.15080/ref-31",
"volume": "11",
"year": "2022"
},
{
"article-title": "Effect of CPC mouthrinses on spike protein binding to ACE2 receptor",
"author": "Sarma",
"issue": "Spec Iss A",
"journal-title": "Journal of Dental Research",
"key": "10.7717/peerj.15080/ref-32",
"volume": "100",
"year": "2020"
},
{
"DOI": "10.1007/s15010-020-01563-9",
"article-title": "Efficacy of commercial mouth-rinses on SARS-CoV-2 viral load in saliva: randomized control trial in Singapore",
"author": "Seneviratne",
"doi-asserted-by": "publisher",
"first-page": "305",
"issue": "2",
"journal-title": "Infection",
"key": "10.7717/peerj.15080/ref-33",
"volume": "49",
"year": "2021"
},
{
"DOI": "10.1038/s41598-022-18367-6",
"article-title": "Antiviral effect of cetylpyridinium chloride in mouthwash on SARS-CoV-2",
"author": "Takeda",
"doi-asserted-by": "publisher",
"first-page": "14050",
"issue": "1",
"journal-title": "Scientific Reports",
"key": "10.7717/peerj.15080/ref-34",
"volume": "12",
"year": "2022"
},
{
"DOI": "10.1371/journal.ppat.1001176",
"article-title": "Zn(2+) inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture",
"author": "te Velthuis",
"doi-asserted-by": "publisher",
"first-page": "e1001176",
"issue": "11",
"journal-title": "PLOS Pathogens",
"key": "10.7717/peerj.15080/ref-35",
"volume": "6",
"year": "2010"
},
{
"DOI": "10.1128/spectrum.03873-22",
"article-title": "Morning SARS-CoV-2 testing yields better detection of infection due to higher viral loads in saliva and nasal swabs upon waking",
"author": "Viloria Winnett",
"doi-asserted-by": "publisher",
"first-page": "e0387322",
"issue": "6",
"journal-title": "Microbiology Spectrum",
"key": "10.7717/peerj.15080/ref-36",
"volume": "10",
"year": "2022"
},
{
"DOI": "10.1056/NEJMc2016359",
"article-title": "Saliva or Nasopharyngeal Swab Specimens for Detection of SARS-CoV-2",
"author": "Wyllie",
"doi-asserted-by": "publisher",
"first-page": "1283",
"issue": "13",
"journal-title": "New England Journal of Medicine",
"key": "10.7717/peerj.15080/ref-37",
"volume": "383",
"year": "2020"
},
{
"DOI": "10.3346/jkms.2020.35.e195",
"article-title": "Clinical significance of a high SARS-CoV-2 viral load in the saliva",
"author": "Yoon",
"doi-asserted-by": "publisher",
"first-page": "e195",
"issue": "20",
"journal-title": "Journal of Korean Medical Science",
"key": "10.7717/peerj.15080/ref-38",
"volume": "35",
"year": "2020"
},
{
"DOI": "10.1016/j.ygeno.2017.08.007",
"article-title": "How many differentially expressed genes: a perspective from the comparison of genotypic and phenotypic distances",
"author": "Zhao",
"doi-asserted-by": "publisher",
"first-page": "67",
"issue": "1",
"journal-title": "Genomics",
"key": "10.7717/peerj.15080/ref-39",
"volume": "110",
"year": "2018"
},
{
"DOI": "10.1016/j.jinf.2020.06.059",
"article-title": "Viral dynamics of SARS-CoV-2 in saliva from infected patients",
"author": "Zhu",
"doi-asserted-by": "publisher",
"first-page": "e48",
"issue": "3",
"journal-title": "Journal of Infection",
"key": "10.7717/peerj.15080/ref-40",
"volume": "81",
"year": "2020"
}
],
"reference-count": 40,
"references-count": 40,
"relation": {},
"resource": {
"primary": {
"URL": "https://peerj.com/articles/15080"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Agricultural and Biological Sciences",
"General Biochemistry, Genetics and Molecular Biology",
"General Medicine",
"General Neuroscience"
],
"subtitle": [],
"title": "Reduction of SARS-CoV-2 viral load in saliva after rinsing with mouthwashes containing cetylpyridinium chloride: a randomized clinical study",
"type": "journal-article",
"volume": "11"
}
