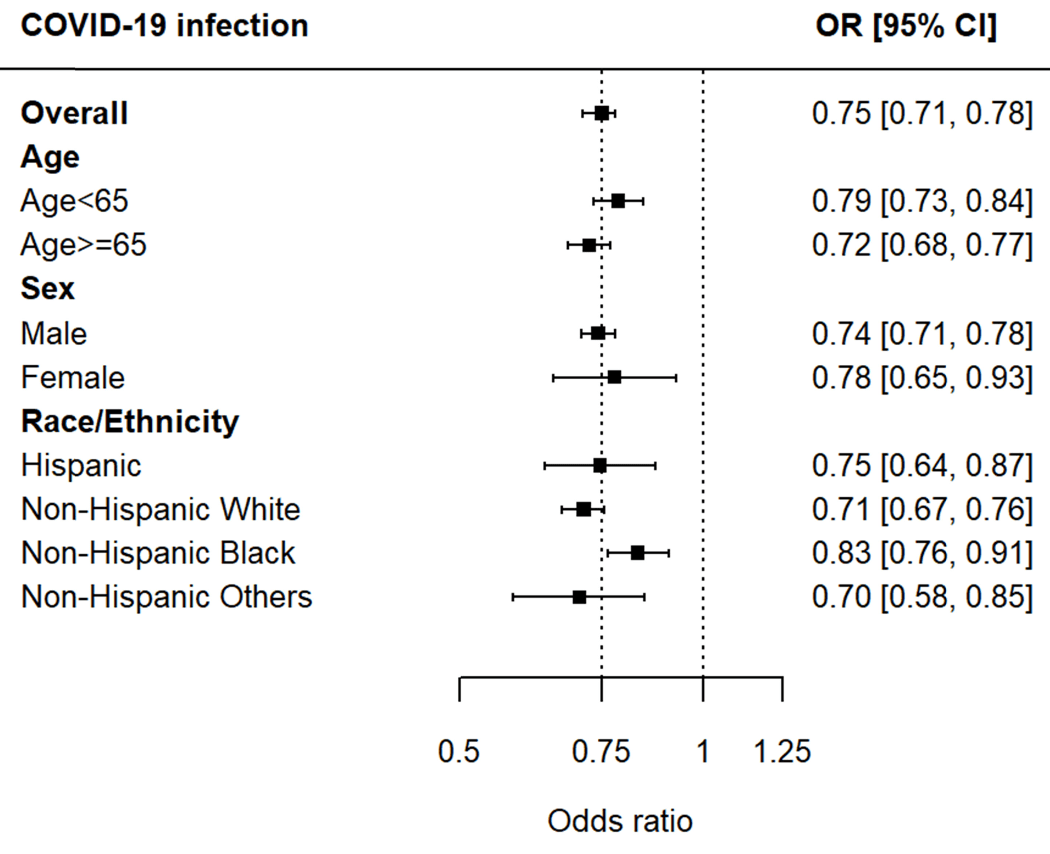
Iodine contrast exposure and incident COVID-19 infection
et al., Frontiers in Medicine, doi:10.3389/fmed.2022.1033601, Dec 2022
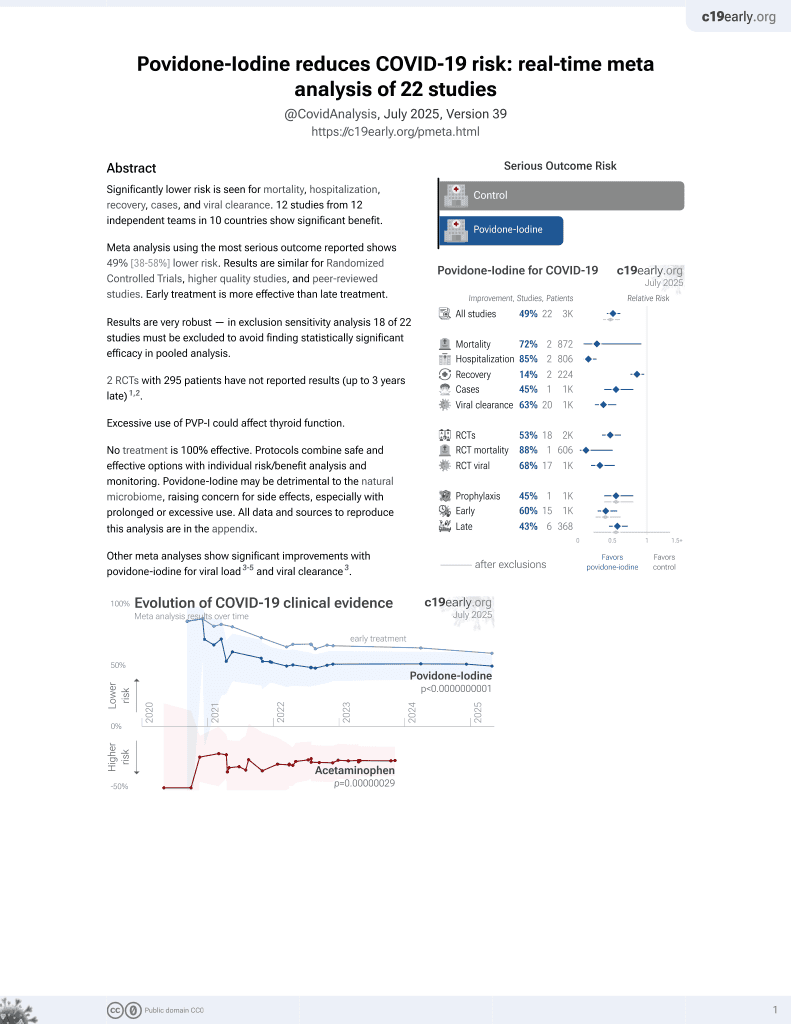
PVP-I for COVID-19
14th treatment shown to reduce risk in
February 2021, now with p = 0.0000000037 from 21 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 530,942 COVID-19 tests in the USA, showing lower incidence of cases with exposure to iodine contrast for imaging within the last 60 days.
Standard of Care (SOC) for COVID-19 in the study country,
the USA, is very poor with very low average efficacy for approved treatments1.
Only expensive, high-profit treatments were approved for early treatment. Low-cost treatments were excluded, reducing the probability of early treatment due to access and cost barriers, and eliminating complementary and synergistic benefits seen with many low-cost treatments.
|
risk of case, 23.7% lower, RR 0.76, p < 0.001, NNT 48, adjusted per study, odds ratio converted to relative risk, multivariable.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Tsai et al., 1 Dec 2022, retrospective, USA, peer-reviewed, 11 authors, study period 1 March, 2020 - 31 December, 2020.
Contact: angela.leung@va.gov.
Iodine contrast exposure and incident COVID-19 infection
Frontiers in Medicine, doi:10.3389/fmed.2022.1033601
Background: Iodine and particularly its oxidated forms have long been recognized for its effective antiseptic properties. Limited in vitro and in vivo data suggest that iodine exposure may rapidly inactivate, reduce transmission, and reduce infectivity of SARS-CoV-2. We hypothesized that iodine exposure may be associated with decreased incident COVID-19 infection.
Methods: A retrospective population-level cohort analysis was performed of the U.S. Veterans Health Administration between 1 March 2020 and 31 December 2020, before the widespread availability of vaccines against SARS-CoV-2. Multivariable logistic regression models estimated the adjusted odds ratios (OR) and 95% confidence intervals (CI) of the associations between iodinated contrast exposure and incident COVID-19 infection, adjusting for age, sex, race/ethnicity, place of residence, socioeconomic status, and insurance status. Results: 530,942 COVID-19 tests from 333,841 Veterans (mean ± SD age, 62.7 ± 15.2 years; 90.2% men; 61.9% non-Hispanic Whites) were analyzed, of whom 9% had received iodinated contrast ≤60 days of a COVID-19 test. Iodine exposure was associated with decreased incident COVID-19 test positivity (OR, 0.75 95% CI, 0.71-0.78). In stratified analyses, the associations between iodinated contrast use and decreased COVID-19 infection risk did not differ by age, sex, and race/ethnicity.
Ethics statement The studies involving human participants were reviewed and approved by the VA Greater Los Angeles Healthcare System Institutional Review Board. Written informed consent for participation was not required for this study in accordance with the national legislation and the institutional requirements.
Author contributions AL: concept and design. MM and AL: acquisition, analysis, or interpretation of data. KT, KI, and AL: drafting of the manuscript. KT, KI, MM, JK, YA, ML, NN, JC, RE, MB, and AL: critical review of the manuscript. MM, KI, and AL: statistical analysis. All authors contributed to the article and approved the submitted version.
Conflict of interest The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher's note All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Author disclaimer The contents do not represent the views of the U.S. Department of Veterans Affairs or the United States Government.
Supplementary material The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/..
References
Backer, Hollowell, Use of iodine for water disinfection: iodine toxicity and maximum recommended dose, Environ Health Perspect, doi:10.1289/ehp.00108679
Banfi, Fischer, Zabner, Durairaj, Lorentzen et al., Halides in the Treatment of Pathogenic Infection
Bigliardi, Alsagoff, El-Kafrawi, Pyon, Wa et al., Povidone iodine in wound healing: a review of current concepts and practices, Int J Surg, doi:10.1016/j.ijsu.2017.06.073
Darouiche, Wall, Jr, Itani, Otterson et al., Chlorhexidine-alcohol versus povidone-iodine for surgical-site antisepsis, N Engl J Med, doi:10.1056/NEJMoa0810988
Derscheid, Van Geelen, Berkebile, Gallup, Hostetter et al., Increased concentration of iodide in airway secretions is associated with reduced respiratory syncytial virus disease severity, Am J Respir Cell Mol Biol, doi:10.1165/rcmb.2012-0529OC
Frank, Capriotti, Brown, Tessema, Povidone-iodine use in sinonasal and oral cavities: a review of safety in the COVID-19 era, Ear Nose Throat J, doi:10.1177/0145561320932318
Geiszt, Witta, Baffi, Lekstrom, Leto, Dual oxidases represent novel hydrogen peroxide sources supporting mucosal surface host defense, FASEB J, doi:10.1096/fj.02-1104fje
Guenezan, Garcia, Strasters, Jousselin, Lévêque et al., Povidone iodine mouthwash, gargle, and nasal spray to reduce nasopharyngeal viral load in patients with COVID-19: a randomized clinical trial, doi:10.1001/jamaoto.2020.5490
Hollowell, Staehling, Hannon, Flanders, Gunter et al., Iodine nutrition in the United States. Trends and public health implications: iodine excretion data from national health and nutrition examination surveys I and III (1971-1974 and 1988-1994), J Clin Endocrinol Metab, doi:10.1210/jcem.83.10.5168
Kariwa, Fujii, Takashima, Inactivation of SARS coronavirus by means of povidone-iodine, physical conditions and chemical reagents, Dermatology, doi:10.1159/000089211
Katagiri, Asakura, Sasaki, Hirota, Notsu et al., Estimation of habitual iodine intake in Japanese adults using 16 d diet records over four seasons with a newly developed food composition database for iodine, Br J Nutr, doi:10.1017/S0007114515002019
Lee, Chang, He, Pearce, Braverman et al., Urinary iodine excretion and serum thyroid function in adults after iodinated contrast administration, Thyroid, doi:10.1089/thy.2015.0024
Lee, Rhee, Leung, Braverman, Brent et al., A review: radiographic iodinated contrast media-induced thyroid dysfunction, J Clin Endocrinol Metab, doi:10.1210/jc.2014-3292
Leung, Avram, Brenner, Duntas, Ehrenkranz et al., Potential risks of excess iodine ingestion and exposure: statement by the American thyroid association public health committee, Thyroid, doi:10.1089/thy.2014.0331
Leung, Braverman, Smith ; Bindman, Kwan, Marlow et al., Trends in use of medical imaging in US health care systems and in Ontario, Nat Rev Endocrinol, doi:10.1001/jama.2019.11456
Mathieu, Ritchie, Rodés-Guirao, Appel, Giattino et al., Coronavirus Pandemic (COVID-19
Mcdonnell, Burke, Disinfection: is it time to reconsider spaulding?, J Hosp Infect
Nicola, Carrasco, Masini-Repiso, Dietary I(-) absorption: expression and regulation of the Na(+)/I(-) symporter in the intestine, Vitam Horm, doi:10.1016/bs.vh.2014.12.002
Otten, Hellwig, Meyers, DRI: Dietary Reference Intakes: The Essential Guide to Nutrient Requirements
Paleiron, Mayet, Marbac, Perisse, Barazzutti et al., Impact of tobacco smoking on the risk of COVID-19: a large scale retrospective cohort study, doi:10.1093/ntr/ntab004
Patel, Gingerich, Widman, Sarr, Tripp et al., Susceptibility of influenza viruses to hypothiocyanite and hypoiodite produced by lactoperoxidase in a cell-free system, BMC Oral Health, doi:10.1186/s12903-022-02082-9
Sarr, Tóth, Gingerich, Rada, Antimicrobial actions of dual oxidases and lactoperoxidase, J Microbiol, doi:10.1007/s12275-018-7545-1
Schöckel, Jost, Seidensticker, Lengsfeld, Palkowitsch et al., Developments in X-ray contrast media and the potential impact on computed tomography, Invest Radiol, doi:10.1097/RLI.0000000000000696
Seikai, Takada, Hasebe, Kajihara, Okuya et al., Gargling with povidone iodine has a short-term inhibitory effect on SARS-CoV-2 in patients with COVID-19, J Hosp Infect, doi:10.1016/j.jhin.2022.01.001
Shoemake, Ley, Newcomer, Heller, Gerson et al., Efficacy of oral administration of sodium iodide to prevent bovine respiratory disease complex, Am J Respir Cell Mol Biol, doi:10.1165/ajrcmb.22.6.3980
DOI record:
{
"DOI": "10.3389/fmed.2022.1033601",
"ISSN": [
"2296-858X"
],
"URL": "http://dx.doi.org/10.3389/fmed.2022.1033601",
"abstract": "<jats:sec><jats:title>Background</jats:title><jats:p>Iodine and particularly its oxidated forms have long been recognized for its effective antiseptic properties. Limited <jats:italic>in vitro</jats:italic> and <jats:italic>in vivo</jats:italic> data suggest that iodine exposure may rapidly inactivate, reduce transmission, and reduce infectivity of SARS-CoV-2. We hypothesized that iodine exposure may be associated with decreased incident COVID-19 infection.</jats:p></jats:sec><jats:sec><jats:title>Methods</jats:title><jats:p>A retrospective population-level cohort analysis was performed of the U.S. Veterans Health Administration between 1 March 2020 and 31 December 2020, before the widespread availability of vaccines against SARS-CoV-2. Multivariable logistic regression models estimated the adjusted odds ratios (OR) and 95% confidence intervals (CI) of the associations between iodinated contrast exposure and incident COVID-19 infection, adjusting for age, sex, race/ethnicity, place of residence, socioeconomic status, and insurance status.</jats:p></jats:sec><jats:sec><jats:title>Results</jats:title><jats:p>530,942 COVID-19 tests from 333,841 Veterans (mean ± SD age, 62.7 ± 15.2 years; 90.2% men; 61.9% non-Hispanic Whites) were analyzed, of whom 9% had received iodinated contrast ≤60 days of a COVID-19 test. Iodine exposure was associated with decreased incident COVID-19 test positivity (OR, 0.75 95% CI, 0.71–0.78). In stratified analyses, the associations between iodinated contrast use and decreased COVID-19 infection risk did not differ by age, sex, and race/ethnicity.</jats:p></jats:sec><jats:sec><jats:title>Conclusion</jats:title><jats:p>Iodine exposure may be protective against incident COVID-19 infection. Weighed against the risks of supraphysiologic iodine intake, dietary, and supplemental iodine nutrition not to exceed its Tolerable Upper Limit may confer an antimicrobial benefit against SARS-CoV-2. A safe but antimicrobial level of iodine supplementation may be considered in susceptible individuals, particularly in geographic regions where effective COVID-19 vaccines are not yet readily available.</jats:p></jats:sec>",
"alternative-id": [
"10.3389/fmed.2022.1033601"
],
"author": [
{
"affiliation": [],
"family": "Tsai",
"given": "Karen",
"sequence": "first"
},
{
"affiliation": [],
"family": "Inoue",
"given": "Kosuke",
"sequence": "additional"
},
{
"affiliation": [],
"family": "McClean",
"given": "Michael",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kaunitz",
"given": "Jonathan D.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Akiba",
"given": "Yasutada",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lee",
"given": "Martin L.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Neverova",
"given": "Natalia V.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Currier",
"given": "Jesse W.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ebrahimi",
"given": "Ramin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Bashir",
"given": "Muhammad T.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Leung",
"given": "Angela M.",
"sequence": "additional"
}
],
"container-title": "Frontiers in Medicine",
"container-title-short": "Front. Med.",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"frontiersin.org"
]
},
"created": {
"date-parts": [
[
2022,
12,
1
]
],
"date-time": "2022-12-01T05:54:57Z",
"timestamp": 1669874097000
},
"deposited": {
"date-parts": [
[
2022,
12,
1
]
],
"date-time": "2022-12-01T05:55:02Z",
"timestamp": 1669874102000
},
"funder": [
{
"DOI": "10.13039/100000738",
"award": [
"5|01CX0011845, I01BX001245"
],
"doi-asserted-by": "publisher",
"name": "U.S. Department of Veterans Affairs"
}
],
"indexed": {
"date-parts": [
[
2022,
12,
2
]
],
"date-time": "2022-12-02T05:55:11Z",
"timestamp": 1669960511897
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2022,
12,
1
]
]
},
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
12,
1
]
],
"date-time": "2022-12-01T00:00:00Z",
"timestamp": 1669852800000
}
}
],
"link": [
{
"URL": "https://www.frontiersin.org/articles/10.3389/fmed.2022.1033601/full",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1965",
"original-title": [],
"prefix": "10.3389",
"published": {
"date-parts": [
[
2022,
12,
1
]
]
},
"published-online": {
"date-parts": [
[
2022,
12,
1
]
]
},
"publisher": "Frontiers Media SA",
"reference": [
{
"journal-title": "COVID-19 Mortality Analyses. Johns Hopkins Coronavirus Resource Centre.",
"key": "B1",
"year": "2022"
},
{
"DOI": "10.1016/j.ijsu.2017.06.073",
"article-title": "Povidone iodine in wound healing: a review of current concepts and practices.",
"author": "Bigliardi",
"doi-asserted-by": "publisher",
"first-page": "260",
"journal-title": "Int J Surg.",
"key": "B2",
"volume": "44",
"year": "2017"
},
{
"DOI": "10.1056/NEJMoa0810988",
"article-title": "Chlorhexidine-alcohol versus povidone-iodine for surgical-site antisepsis.",
"author": "Darouiche",
"doi-asserted-by": "publisher",
"first-page": "18",
"journal-title": "N Engl J Med.",
"key": "B3",
"volume": "362",
"year": "2010"
},
{
"DOI": "10.1289/ehp.00108679",
"article-title": "Use of iodine for water disinfection: iodine toxicity and maximum recommended dose.",
"author": "Backer",
"doi-asserted-by": "publisher",
"first-page": "679",
"journal-title": "Environ Health Perspect.",
"key": "B4",
"volume": "108",
"year": "2000"
},
{
"author": "Otten",
"first-page": "p. 320",
"journal-title": "DRI: Dietary Reference Intakes: The Essential Guide to Nutrient Requirements.",
"key": "B5",
"year": "2006"
},
{
"DOI": "10.1038/nrendo.2013.251",
"article-title": "Consequences of excess iodine.",
"author": "Leung",
"doi-asserted-by": "publisher",
"first-page": "136",
"journal-title": "Nat Rev Endocrinol.",
"key": "B6",
"volume": "10",
"year": "2014"
},
{
"DOI": "10.1001/jama.2019.11456",
"article-title": "Trends in use of medical imaging in US health care systems and in Ontario, Canada, 2000-2016.",
"author": "Smith-Bindman",
"doi-asserted-by": "publisher",
"first-page": "843",
"journal-title": "JAMA.",
"key": "B7",
"volume": "322",
"year": "2019"
},
{
"DOI": "10.1097/RLI.0000000000000696",
"article-title": "Developments in X-ray contrast media and the potential impact on computed tomography.",
"author": "Schöckel",
"doi-asserted-by": "publisher",
"first-page": "592",
"journal-title": "Invest Radiol.",
"key": "B8",
"volume": "55",
"year": "2020"
},
{
"DOI": "10.1210/jc.2014-3292",
"article-title": "A review: radiographic iodinated contrast media-induced thyroid dysfunction.",
"author": "Lee",
"doi-asserted-by": "publisher",
"first-page": "376",
"journal-title": "J Clin Endocrinol Metab.",
"key": "B9",
"volume": "100",
"year": "2015"
},
{
"DOI": "10.1089/thy.2015.0024",
"article-title": "Urinary iodine excretion and serum thyroid function in adults after iodinated contrast administration.",
"author": "Lee",
"doi-asserted-by": "publisher",
"first-page": "471",
"journal-title": "Thyroid.",
"key": "B10",
"volume": "25",
"year": "2015"
},
{
"DOI": "10.1016/bs.vh.2014.12.002",
"article-title": "Dietary I(-) absorption: expression and regulation of the Na(+)/I(-) symporter in the intestine.",
"author": "Nicola",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Vitam Horm.",
"key": "B11",
"volume": "98",
"year": "2015"
},
{
"DOI": "10.1007/s12275-018-7545-1",
"article-title": "Antimicrobial actions of dual oxidases and lactoperoxidase.",
"author": "Sarr",
"doi-asserted-by": "publisher",
"first-page": "373",
"journal-title": "J Microbiol.",
"key": "B12",
"volume": "56",
"year": "2018"
},
{
"DOI": "10.1165/rcmb.2012-0529OC",
"article-title": "Increased concentration of iodide in airway secretions is associated with reduced respiratory syncytial virus disease severity.",
"author": "Derscheid",
"doi-asserted-by": "publisher",
"first-page": "389",
"journal-title": "Am J Respir Cell Mol Biol.",
"key": "B13",
"volume": "50",
"year": "2014"
},
{
"DOI": "10.1016/j.jhin.2011.05.002",
"article-title": "Disinfection: is it time to reconsider spaulding?",
"author": "McDonnell",
"doi-asserted-by": "publisher",
"first-page": "163",
"journal-title": "J Hosp Infect.",
"key": "B14",
"volume": "78",
"year": "2011"
},
{
"DOI": "10.1177/0145561320932318",
"article-title": "Povidone-iodine use in sinonasal and oral cavities: a review of safety in the COVID-19 era.",
"author": "Frank",
"doi-asserted-by": "publisher",
"first-page": "586",
"journal-title": "Ear Nose Throat J.",
"key": "B15",
"volume": "99",
"year": "2020"
},
{
"DOI": "10.1159/000089211",
"article-title": "Inactivation of SARS coronavirus by means of povidone-iodine, physical conditions and chemical reagents.",
"author": "Kariwa",
"doi-asserted-by": "publisher",
"first-page": "119",
"journal-title": "Dermatology.",
"key": "B16",
"volume": "212",
"year": "2006"
},
{
"DOI": "10.1096/fj.02-1104fje",
"article-title": "Dual oxidases represent novel hydrogen peroxide sources supporting mucosal surface host defense.",
"author": "Geiszt",
"doi-asserted-by": "publisher",
"first-page": "1502",
"journal-title": "FASEB J.",
"key": "B17",
"volume": "17",
"year": "2003"
},
{
"DOI": "10.1371/journal.pone.0199167",
"article-title": "Susceptibility of influenza viruses to hypothiocyanite and hypoiodite produced by lactoperoxidase in a cell-free system.",
"author": "Patel",
"doi-asserted-by": "publisher",
"first-page": "e0199167",
"journal-title": "PLoS One.",
"key": "B18",
"volume": "13",
"year": "2018"
},
{
"DOI": "10.1186/s12903-022-02082-9",
"article-title": "In vitro inactivation of SARS-CoV-2 using a povidone-iodine oral rinse.",
"author": "Shet",
"doi-asserted-by": "publisher",
"first-page": "47",
"journal-title": "BMC Oral Health.",
"key": "B19",
"volume": "22",
"year": "2022"
},
{
"DOI": "10.1016/j.jhin.2022.01.001",
"article-title": "Gargling with povidone iodine has a short-term inhibitory effect on SARS-CoV-2 in patients with COVID-19.",
"author": "Seikai",
"doi-asserted-by": "publisher",
"first-page": "179",
"journal-title": "J Hosp Infect.",
"key": "B20",
"volume": "123",
"year": "2022"
},
{
"DOI": "10.1001/jamaoto.2020.5490",
"article-title": "Povidone iodine mouthwash, gargle, and nasal spray to reduce nasopharyngeal viral load in patients with COVID-19: a randomized clinical trial.",
"author": "Guenezan",
"doi-asserted-by": "publisher",
"first-page": "400",
"journal-title": "JAMA Otolaryngol Head Neck Surg.",
"key": "B21",
"volume": "147",
"year": "2021"
},
{
"author": "Tsai",
"journal-title": "COVID-19 Tests. Mendeley Data 2022.",
"key": "B22",
"year": "2022"
},
{
"DOI": "10.1089/thy.2014.0331",
"article-title": "Potential risks of excess iodine ingestion and exposure: statement by the American thyroid association public health committee.",
"author": "Leung",
"doi-asserted-by": "publisher",
"first-page": "145",
"journal-title": "Thyroid.",
"key": "B23",
"volume": "25",
"year": "2015"
},
{
"author": "Banfi",
"journal-title": "Halides in the Treatment of Pathogenic Infection. United States Patent Application.",
"key": "B24",
"year": "2009"
},
{
"DOI": "10.1111/jvim.14903",
"article-title": "Efficacy of oral administration of sodium iodide to prevent bovine respiratory disease complex.",
"author": "Shoemake",
"doi-asserted-by": "publisher",
"first-page": "516",
"journal-title": "J Vet Intern Med.",
"key": "B25",
"volume": "32",
"year": "2018"
},
{
"DOI": "10.1165/ajrcmb.22.6.3980",
"article-title": "The lactoperoxidase system functions in bacterial clearance of airways.",
"author": "Gerson",
"doi-asserted-by": "publisher",
"first-page": "665",
"journal-title": "Am J Respir Cell Mol Biol.",
"key": "B26",
"volume": "22",
"year": "2000"
},
{
"DOI": "10.1093/ntr/ntab004",
"article-title": "Impact of tobacco smoking on the risk of COVID-19: a large scale retrospective cohort study.",
"author": "Paleiron",
"doi-asserted-by": "publisher",
"first-page": "1398",
"journal-title": "Nicotine Tob Res.",
"key": "B27",
"volume": "23",
"year": "2021"
},
{
"DOI": "10.20935/AL1211",
"article-title": "Ingestion of cyanogens from cassava generates disinfectant hypothiocyanite that may decrease the transmissibility of SARS-CoV-2.",
"author": "Kaunitz",
"doi-asserted-by": "publisher",
"first-page": "1211",
"journal-title": "Acad Lett",
"key": "B28",
"year": "2021"
},
{
"author": "Mathieu",
"journal-title": "Coronavirus Pandemic (COVID-19).",
"key": "B29",
"year": "2020"
},
{
"DOI": "10.1017/S0007114515002019",
"article-title": "Estimation of habitual iodine intake in Japanese adults using 16 d diet records over four seasons with a newly developed food composition database for iodine.",
"author": "Katagiri",
"doi-asserted-by": "publisher",
"first-page": "624",
"journal-title": "Br J Nutr.",
"key": "B30",
"volume": "114",
"year": "2015"
},
{
"DOI": "10.1210/jcem.83.10.5168",
"article-title": "Iodine nutrition in the United States. Trends and public health implications: iodine excretion data from national health and nutrition examination surveys I and III (1971-1974 and 1988-1994).",
"author": "Hollowell",
"doi-asserted-by": "publisher",
"first-page": "3401",
"journal-title": "J Clin Endocrinol Metab.",
"key": "B31",
"volume": "83",
"year": "1998"
}
],
"reference-count": 31,
"references-count": 31,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.frontiersin.org/articles/10.3389/fmed.2022.1033601/full"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Iodine contrast exposure and incident COVID-19 infection",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.3389/crossmark-policy",
"volume": "9"
}
