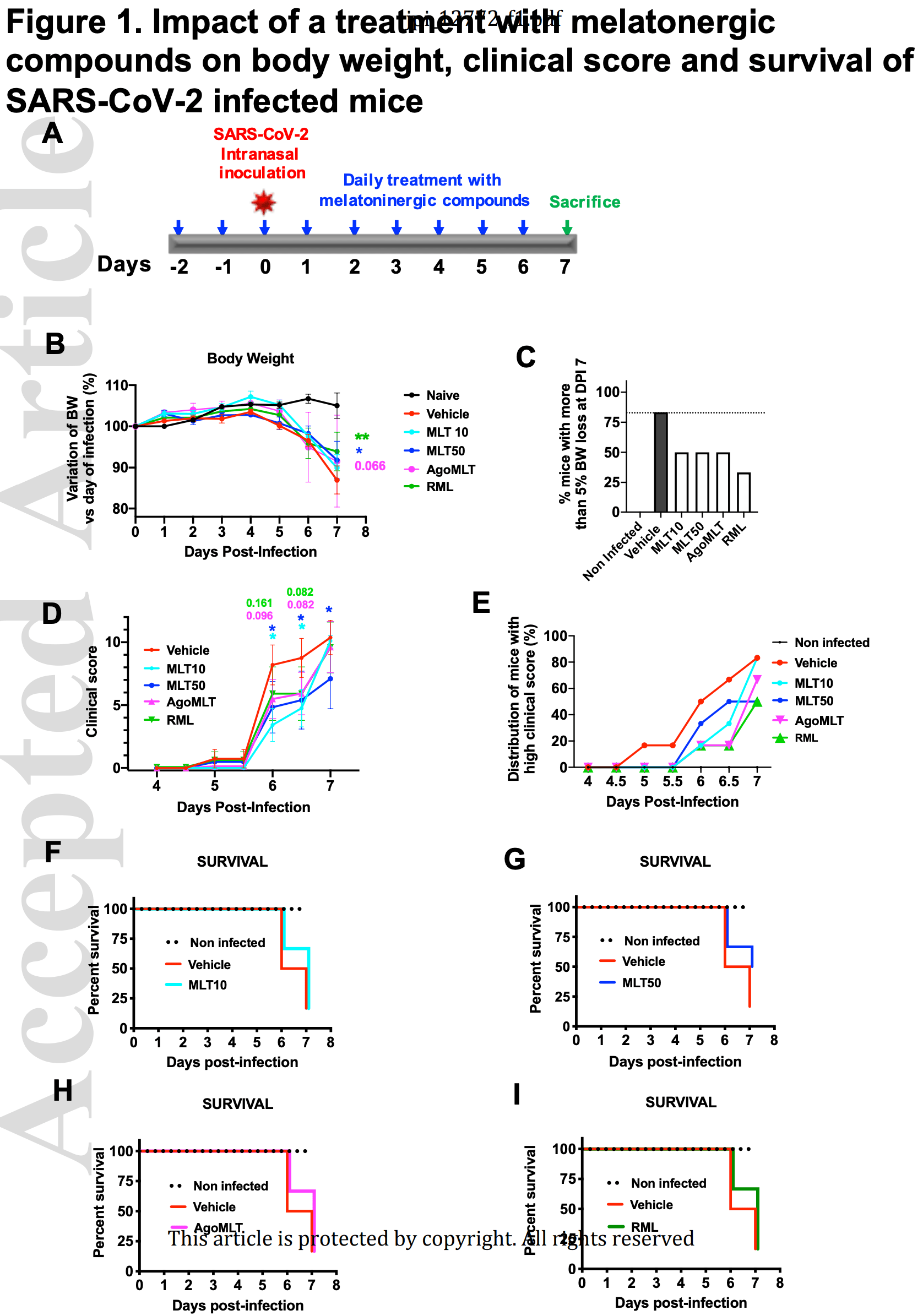
Therapeutic potential of melatonin and melatonergic drugs on K18-hACE2 mice infected with SARS-CoV-2
et al., Journal of Pineal Research, doi:10.1111/jpi.12772, Sep 2021
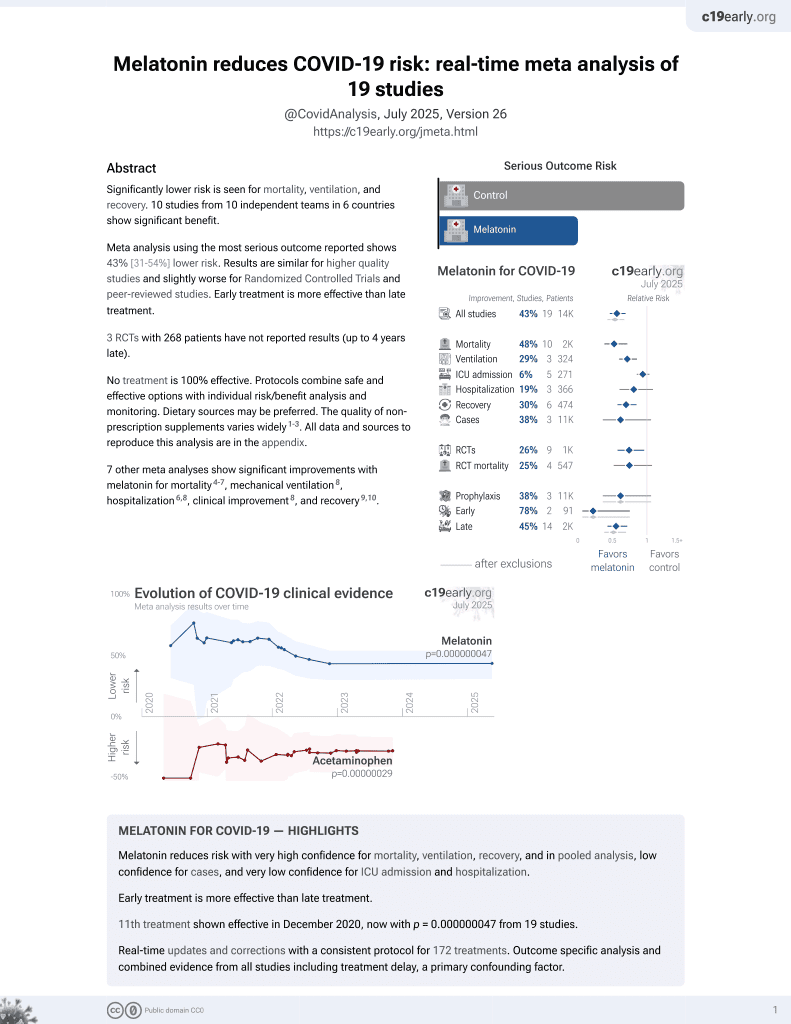
Melatonin for COVID-19
25th treatment shown to reduce risk in
May 2021, now with p = 0.000000015 from 18 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Study of melatonin and melatonergic compounds with mice expressing the human ACE2 receptor (K18-hACE2). Daily administration of melatonin, agomelatine or ramelteon delayed the occurrence of severe clinical outcome with improvement of survival, especially with high melatonin dose.
7 preclinical studies support the efficacy of melatonin for COVID-19:
Melatonin may restore altered redox homeostasis in COVID-197, modulates type III interferon responses and reduces inflammatory cytokine production in TLR3 receptor agonist stimulated viral inflammation while preserving tissue integrity4, and negatively regulates genes critical for viral entry in lung tissue, including reduced expression of FURIN and components of the CD147 complex, while potentially disrupting TMPRSS2/ACE2-mediated entry mechanisms3.
Melatonin reduces oxidative stress, inhibits NET formation, and protects tissues through anti-inflammatory and antioxidant actions8.
1.
Acharya et al., Potential therapeutic intervention of melatonin against COVID-19: A comparative pharmacokinetic study, Melatonin Research, doi:10.32794/mr112500181.
2.
Kumar Yadalam et al., Assessing the therapeutic potential of angomelatine, ramelteon, and melatonin against SARS-Cov-2, Saudi Journal of Biological Sciences, doi:10.1016/j.sjbs.2022.01.049.
3.
Fernandes et al., Melatonin-Index as a biomarker for predicting the distribution of presymptomatic and asymptomatic SARS-CoV-2 carriers, Melatonin Research, doi:10.32794/mr11250090.
4.
Šeškutė et al., Antiviral Effect of Melatonin on Caco-2 Cell Organoid Culture: Trick or Treat?, International Journal of Molecular Sciences, doi:10.3390/ijms252211872.
5.
Cecon et al., Melatonin drugs inhibit SARS-CoV-2 entry into the brain and virus-induced damage of cerebral small vessels, bioRxiv, doi:10.1101/2021.12.30.474561.
6.
Cecon (B) et al., Therapeutic potential of melatonin and melatonergic drugs on K18-hACE2 mice infected with SARS-CoV-2, Journal of Pineal Research, doi:10.1111/jpi.12772.
Cecon et al., 29 Sep 2021, peer-reviewed, 11 authors.
Therapeutic potential of melatonin and melatonergic drugs on K18‐ hACE2 mice infected with SARS‐CoV‐2
Journal of Pineal Research, doi:10.1111/jpi.12772
Word count: 181 As the COVID-19 pandemic grows, several therapeutic candidates are being tested or undergoing clinical trials. Although prophylactic vaccination against SARS-CoV-2 infection has been shown to be effective, no definitive treatment exists to date in the event of infection. The rapid spread of infection by SARS-CoV-2 and its variants fully warrants the continued evaluation of drug treatments for COVID-19, especially in the context of repurposing of already available and safe drugs. Here we explored the therapeutic potential of melatonin and melatonergic compounds in attenuating COVID-19 pathogenesis in mice expressing human ACE2 receptor (K18-hACE2), strongly susceptible to SARS-CoV-2 infection. Daily administration of melatonin, agomelatine or ramelteon delays the occurrence of severe clinical outcome with improvement of survival, especially with high melatonin dose. Although no changes in most lung inflammatory cytokines are observed, treatment with melatonergic compounds limits the exacerbated local lung production of type I and type III interferons, which is likely associated with the observed improved symptoms in treated mice. The promising results from this preclinical study should encourage studies examining the benefits of repurposing melatonergic drugs to treat COVID-19 and related diseases in humans.
AUTHOR CONTRIBUTIONS Conceptualization, E.C., J.D., and R.
COMPETING INTERESTS The authors declare no competing interest.
References
Acharya, Liu, Gack, Dysregulation of type I interferon responses in COVID-19, Nat Rev Immunol
Acuna-Castroviejo, Escames, Figueira, De La Oliva, Borobia et al., Clinical trial to test the efficacy of melatonin in COVID-19, J Pineal Res
Arce, Costoya, SARS-CoV-2 infection in K18-ACE2 transgenic mice replicates human pulmonary disease in COVID-19, Cell Mol Immunol
Bao, Deng, Huang, The pathogenicity of SARS-CoV-2 in hACE2 transgenic mice, Nature
Bastard, Rosen, Zhang, Autoantibodies against type I IFNs in patients with life-threatening COVID-19, Science
Boutin, Jockers, Melatonin controversies, an update, J Pineal Res
Bravo, Dangerfield, Taylor, Johnson, Remdesivir is a delayed translocation inhibitor of SARS-CoV-2 replication, Mol Cell
Broggi, Ghosh, Sposito, Type III interferons disrupt the lung epithelial barrier upon viral recognition, Science
Cajochen, Krauchi, Mori, Graw, Wirz-Justice, Melatonin and S-20098 increase REM sleep and wakeup propensity without modifying NREM sleep homeostasis, Am J Physiol
Cardinali, Srinivasan, Brzezinski, Brown, Melatonin and its analogs in insomnia and depression, J Pineal Res
Carrillo-Vico, Lardone, Naji, Beneficial pleiotropic actions of melatonin in an experimental model of septic shock in mice: regulation of pro-/anti-inflammatory cytokine network, protection against oxidative damage and anti-apoptotic effects, J Pineal Res
Chen, Chen, Yang, Melatonin pretreatment enhances the therapeutic effects of exogenous mitochondria against hepatic ischemia-reperfusion injury in rats through suppression of mitochondrial permeability transition, J Pineal Res
Cho, Bhutani, Kim, Irwin, Anti-inflammatory effects of melatonin: A systematic review and metaanalysis of clinical trials, Brain Behav Immun
Crespo, Fernandez-Palanca, San-Miguel, Alvarez, Gonzalez-Gallego et al., Melatonin modulates mitophagy, innate immunity and circadian clocks in a model of viral-induced fulminant hepatic failure, J Cell Mol Med
Crespo, San-Miguel, Sanchez, Melatonin inhibits the sphingosine kinase 1/sphingosine-1-phosphate signaling pathway in rabbits with fulminant hepatitis of viral origin, J Pineal Res
De Bodinat, Guardiola-Lemaitre, Mocaer, Renard, Munoz et al., Agomelatine, the first melatonergic antidepressant: discovery, characterization and development, Nat Rev Drug Discov
Dubocovich, Delagrange, Krause, Sugden, Cardinali et al., International Union of Basic and Clinical Pharmacology. LXXV. Nomenclature, classification, and pharmacology of G protein-coupled melatonin receptors, Pharmacol Rev
Dubocovich, Melatonin receptors: role on sleep and circadian rhythm regulation, Sleep Med
Garcia, Volt, Venegas, Disruption of the NF-kappaB/NLRP3 connection by melatonin requires retinoid-related orphan receptor-alpha and blocks the septic response in mice, FASEB J
Gerbier, Ndiaye-Lobry, De Morentin, Pharmacological evidence for transactivation within melatonin MT2 and serotonin 5-HT2C receptor heteromers in mouse brain, FASEB J
Golden, Cline, Zeng, Human angiotensin-converting enzyme 2 transgenic mice infected with SARS-CoV-2 develop severe and fatal respiratory disease, JCI Insight
Group, Horby, Lim, Dexamethasone in Hospitalized Patients with Covid-19, N Engl J Med
Hadjadj, Yatim, Barnabei, Impaired type I interferon activity and inflammatory responses in severe COVID-19 patients, Science
Hardeland, Aging, Melatonin, and the Pro-and Anti-Inflammatory Networks, Int J Mol Sci
Hassan, Case, Winkler, A SARS-CoV-2 Infection Model in Mice Demonstrates Protection by Neutralizing Antibodies, Cell
Huang, Cao, Liu, Shi, Wei, Inhibitory effect of melatonin on lung oxidative stress induced by respiratory syncytial virus infection in mice, J Pineal Res
Huang, Wang, Li, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet
Israelow, Song, Mao, Mouse model of SARS-CoV-2 reveals inflammatory role of type I interferon signaling, J Exp Med
Jiang, Liu, Chen, Pathogenesis of SARS-CoV-2 in Transgenic Mice Expressing Human Angiotensin-Converting Enzyme 2, Cell
Jockers, Delagrange, Dubocovich, Update on melatonin receptors: IUPHAR Review 20, Br J Pharmacol
Johnson, Suess, Griffiths, Ramelteon: a novel hypnotic lacking abuse liability and sedative adverse effects, Arch Gen Psychiatry
Karim, Tolbert, Cao, Disposition kinetics and tolerance of escalating single doses of ramelteon, a highaffinity MT1 and MT2 melatonin receptor agonist indicated for treatment of insomnia, J Clin Pharmacol
King, Sprent, Dual Nature of Type I Interferons in SARS-CoV-2-Induced Inflammation, Trends Immunol
Laing, Lorenc, Molino, Barrio, A dynamic COVID-19 immune signature includes associations with poor prognosis, Nat Med
Lee, Lowen, Animal models for SARS-CoV-2, Curr Opin Virol
Lee, Park, Jeong, Immunophenotyping of COVID-19 and influenza highlights the role of type I interferons in development of severe COVID-19, Sci Immunol
Letko, Marzi, Munster, Functional assessment of cell entry and receptor usage for SARS-CoV-2 and other lineage B betacoronaviruses, Nat Microbiol
Liu, Clough, Hutchinson, Adamah-Biassi, Popovska-Gorevski et al., MT1 and MT2 Melatonin Receptors: A Therapeutic Perspective, Annu Rev Pharmacol Toxicol
Liu, Jockers, Structure-Based Virtual Screening Accelerates GPCR Drug Discovery, Trends Pharmacol Sci
Liu, Labani, Cecon, Jockers, Melatonin Target Proteins: Too Many or Not Enough?, Front Endocrinol
Loo, Dalery, Macher, Payen, Pilot study comparing in blind the therapeutic effect of two doses of agomelatine, melatonin-agonist and selective 5HT2c receptors antagonist, in the treatment of major depressive disorders
Lucas, Wong, Klein, Longitudinal analyses reveal immunological misfiring in severe COVID-19, Nature
Major, Crotta, Llorian, Type I and III interferons disrupt lung epithelial repair during recovery from viral infection, Science
Mccray, Pewe, Wohlford-Lenane, Lethal infection of K18-hACE2 mice infected with severe acute respiratory syndrome coronavirus, J Virol
Mcelroy, Winstanley, Martens, A randomized, placebo-controlled study of adjunctive ramelteon in ambulatory bipolar I disorder with manic symptoms and sleep disturbance, Int Clin Psychopharmacol
Mehta, Mcauley, Brown, COVID-19: consider cytokine storm syndromes and immunosuppression, Lancet
Menachery, Yount, Sims, SARS-like WIV1-CoV poised for human emergence, Proc Natl Acad Sci U S A
Millan, Marin, Kamal, The melatonergic agonist and clinically active antidepressant, agomelatine, is a neutral antagonist at 5-HT(2C) receptors, Int J Neuropsychopharmacol
Moreau, Burgess, Sturek, Donlan, Petri et al., Evaluation of K18-hACE2 Mice as a Model of SARS-CoV-2 Infection, Am J Trop Med Hyg
Munoz ; Fontela, Dowling, Funnell, Animal models for COVID-19, Nature
Nair, Jacob, A simple practice guide for dose conversion between animals and human, J Basic Clin Pharm
Nordlund, Lerner, The effects of oral melatonin on skin color and on the release of pituitary hormones, J Clin Endocrinol Metab
Oladunni, Park, Pino, Lethality of SARS-CoV-2 infection in K18 human angiotensin-converting enzyme 2 transgenic mice, Nat Commun
Papavasiliou, Cotzias, Duby, Steck, Bell et al., Melatonin and parkinsonism, JAMA
Rathnasinghe, Strohmeier, Amanat, Comparison of transgenic and adenovirus hACE2 mouse models for SARS-CoV-2 infection, Emerg Microbes Infect
Salvador, Brown-Clay, Fornace, Gadd45 in stress signaling, cell cycle control, and apoptosis, Adv Exp Med Biol
Snell, Mcgaha, Brooks, Type I Interferon in Chronic Virus Infection and Cancer, Trends Immunol
Sposito, Broggi, Pandolfi, Severity of SARS-CoV-2 infection as a function of the interferon landscape across the respiratory tract of COVID-19 patients
Sun, Chen, Gu, A Mouse Model of SARS-CoV-2 Infection and Pathogenesis, Cell Host Microbe
Sun, Lee, Kao, Systemic combined melatonin-mitochondria treatment improves acute respiratory distress syndrome in the rat, J Pineal Res
Tay, Poh, Renia, Macary, Ng, The trinity of COVID-19: immunity, inflammation and intervention, Nat Rev Immunol
Waldhauser, Waldhauser, Lieberman, Deng, Lynch et al., Bioavailability of oral melatonin in humans, Neuroendocrinology
Wang, Wei, Shen, Protective effect of melatonin against liver injury in mice induced by Bacillus Calmette-Guerin plus lipopolysaccharide, World J Gastroenterol
Weinreich, Sivapalasingam, Norton, REGN-COV2, a Neutralizing Antibody Cocktail, in Outpatients with Covid-19, N Engl J Med
Winkler, Bailey, Kafai, SARS-CoV-2 infection of human ACE2-transgenic mice causes severe lung inflammation and impaired function, Nat Immunol
Wu, Peng, Liao, Pao, Huang et al., Melatonin receptor agonist protects against acute lung injury induced by ventilator through up-regulation of IL-10 production, Respir Res
Xu, Wang, Ning, Zhao, Chen, Maternally administered melatonin differentially regulates lipopolysaccharide-induced proinflammatory and anti-inflammatory cytokines in maternal serum, amniotic fluid, fetal liver, and fetal brain, J Pineal Res
Yinda, Port, Bushmaker, K18-hACE2 mice develop respiratory disease resembling severe COVID-19, PLoS Pathog
Zhai, Wang, Jiao, Melatonin and other indoles show antiviral activities against swine coronaviruses in vitro at pharmacological concentrations, J Pineal Res
Zhang, Bastard, Liu, Inborn errors of type I IFN immunity in patients with life-threatening COVID-19, Science
Zhang, Li, Grailer, Melatonin alleviates acute lung injury through inhibiting the NLRP3 inflammasome, J Pineal Res
Zhou, Hou, Shen, A network medicine approach to investigation and population-based validation of disease manifestations and drug repurposing for COVID-19, PLoS Biol
Zhou, Hou, Shen, Huang, Martin et al., Network-based drug repurposing for novel coronavirus 2019-nCoV/SARS-CoV-2, Cell Discov
Zhou, Ren, Zhang, Heightened Innate Immune Responses in the Respiratory Tract of COVID-19 Patients, Cell Host Microbe
Zhou, Zhao, An, Zhang, Jiang et al., Melatonin prevents lung injury induced by hepatic ischemiareperfusion through anti-inflammatory and anti-apoptosis effects, Int Immunopharmacol
Zisapel, New perspectives on the role of melatonin in human sleep, circadian rhythms and their regulation, Br J Pharmacol
DOI record:
{
"DOI": "10.1111/jpi.12772",
"ISSN": [
"0742-3098",
"1600-079X"
],
"URL": "http://dx.doi.org/10.1111/jpi.12772",
"abstract": "<jats:title>Abstract</jats:title><jats:p>As the COVID‐19 pandemic grows, several therapeutic candidates are being tested or undergoing clinical trials. Although prophylactic vaccination against SARS‐CoV‐2 infection has been shown to be effective, no definitive treatment exists to date in the event of infection. The rapid spread of infection by SARS‐CoV‐2 and its variants fully warrants the continued evaluation of drug treatments for COVID‐19, especially in the context of repurposing of already available and safe drugs. Here, we explored the therapeutic potential of melatonin and melatonergic compounds in attenuating COVID‐19 pathogenesis in mice expressing human ACE2 receptor (K18‐<jats:italic>hACE2</jats:italic>), strongly susceptible to SARS‐CoV‐2 infection. Daily administration of melatonin, agomelatine, or ramelteon delays the occurrence of severe clinical outcome with improvement of survival, especially with high melatonin dose. Although no changes in most lung inflammatory cytokines are observed, treatment with melatonergic compounds limits the exacerbated local lung production of type I and type III interferons, which is likely associated with the observed improved symptoms in treated mice. The promising results from this preclinical study should encourage studies examining the benefits of repurposing melatonergic drugs to treat COVID‐19 and related diseases in humans.</jats:p>",
"alternative-id": [
"10.1111/jpi.12772"
],
"assertion": [
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Received",
"name": "received",
"order": 0,
"value": "2021-07-02"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Accepted",
"name": "accepted",
"order": 1,
"value": "2021-09-28"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Published",
"name": "published",
"order": 2,
"value": "2021-10-15"
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0003-2387-9313",
"affiliation": [
{
"name": "Institut Cochin INSERM CNRS Université de Paris Paris France"
}
],
"authenticated-orcid": false,
"family": "Cecon",
"given": "Erika",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Institut Cochin INSERM CNRS Université de Paris Paris France"
}
],
"family": "Izabelle",
"given": "Charlotte",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-8642-8187",
"affiliation": [
{
"name": "UMR Virologie INRAE ANSES École Nationale Vétérinaire d'Alfort Maisons‐Alfort France"
}
],
"authenticated-orcid": false,
"family": "Poder",
"given": "Sophie Le",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-5060-4334",
"affiliation": [
{
"name": "Institut Cochin INSERM CNRS Université de Paris Paris France"
}
],
"authenticated-orcid": false,
"family": "Real",
"given": "Fernando",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Institut Cochin INSERM CNRS Université de Paris Paris France"
}
],
"family": "Zhu",
"given": "Aiwei",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-2336-5099",
"affiliation": [
{
"name": "School of Medicine Le Kremlin‐Bicêtre Hôpital Marie Lannelongue, INSERM UMRS 999 Université Paris‐Saclay Le Plessis‐Robinson France"
}
],
"authenticated-orcid": false,
"family": "Tu",
"given": "Ly",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-5996-665X",
"affiliation": [
{
"name": "School of Medicine Le Kremlin‐Bicêtre Hôpital Marie Lannelongue, INSERM UMRS 999 Université Paris‐Saclay Le Plessis‐Robinson France"
}
],
"authenticated-orcid": false,
"family": "Ghigna",
"given": "Maria Rosa",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-3372-0656",
"affiliation": [
{
"name": "UMR Virologie INRAE ANSES École Nationale Vétérinaire d'Alfort Maisons‐Alfort France"
}
],
"authenticated-orcid": false,
"family": "Klonjkowski",
"given": "Bernard",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-9577-7474",
"affiliation": [
{
"name": "Institut Cochin INSERM CNRS Université de Paris Paris France"
}
],
"authenticated-orcid": false,
"family": "Bomsel",
"given": "Morgane",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-4354-1750",
"affiliation": [
{
"name": "Institut Cochin INSERM CNRS Université de Paris Paris France"
}
],
"authenticated-orcid": false,
"family": "Jockers",
"given": "Ralf",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-6871-2678",
"affiliation": [
{
"name": "Institut Cochin INSERM CNRS Université de Paris Paris France"
}
],
"authenticated-orcid": false,
"family": "Dam",
"given": "Julie",
"sequence": "additional"
}
],
"container-title": "Journal of Pineal Research",
"container-title-short": "Journal of Pineal Research",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"onlinelibrary.wiley.com"
]
},
"created": {
"date-parts": [
[
2021,
9,
29
]
],
"date-time": "2021-09-29T19:09:41Z",
"timestamp": 1632942581000
},
"deposited": {
"date-parts": [
[
2023,
8,
28
]
],
"date-time": "2023-08-28T02:32:27Z",
"timestamp": 1693189947000
},
"funder": [
{
"DOI": "10.13039/501100007175",
"doi-asserted-by": "publisher",
"name": "Conseil National de la Recherche Scientifique"
},
{
"DOI": "10.13039/501100001677",
"doi-asserted-by": "publisher",
"name": "Institut National de la Santé et de la Recherche Médicale"
},
{
"DOI": "10.13039/501100001665",
"doi-asserted-by": "publisher",
"name": "Agence Nationale de la Recherche"
},
{
"DOI": "10.13039/501100004431",
"doi-asserted-by": "publisher",
"name": "Fondation de France"
}
],
"indexed": {
"date-parts": [
[
2024,
4,
30
]
],
"date-time": "2024-04-30T16:29:43Z",
"timestamp": 1714494583398
},
"is-referenced-by-count": 21,
"issue": "1",
"issued": {
"date-parts": [
[
2021,
10,
15
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2022,
1
]
]
}
},
"language": "en",
"license": [
{
"URL": "http://onlinelibrary.wiley.com/termsAndConditions#vor",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
10,
15
]
],
"date-time": "2021-10-15T00:00:00Z",
"timestamp": 1634256000000
}
}
],
"link": [
{
"URL": "https://onlinelibrary.wiley.com/doi/pdf/10.1111/jpi.12772",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://onlinelibrary.wiley.com/doi/full-xml/10.1111/jpi.12772",
"content-type": "application/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://onlinelibrary.wiley.com/doi/pdf/10.1111/jpi.12772",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "311",
"original-title": [],
"prefix": "10.1111",
"published": {
"date-parts": [
[
2021,
10,
15
]
]
},
"published-online": {
"date-parts": [
[
2021,
10,
15
]
]
},
"published-print": {
"date-parts": [
[
2022,
1
]
]
},
"publisher": "Wiley",
"reference": [
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_2_1"
},
{
"DOI": "10.1038/s41577-020-0311-8",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_3_1"
},
{
"DOI": "10.1056/NEJMoa2035002",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_4_1"
},
{
"DOI": "10.1016/j.molcel.2021.01.035",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_5_1"
},
{
"DOI": "10.1056/NEJMoa2021436",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_6_1"
},
{
"DOI": "10.1016/j.sleep.2007.10.007",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_7_1"
},
{
"DOI": "10.1111/bph.13536",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_8_1"
},
{
"DOI": "10.3389/fendo.2019.00791",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_9_1"
},
{
"DOI": "10.3390/ijms20051223",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_10_1"
},
{
"DOI": "10.1111/jpi.12199",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_11_1"
},
{
"DOI": "10.1111/jpi.12322",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_12_1"
},
{
"DOI": "10.1146/annurev-pharmtox-010814-124742",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_13_1"
},
{
"DOI": "10.1038/s41564-020-0688-y",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_14_1"
},
{
"DOI": "10.1038/nrd3140",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_15_1"
},
{
"DOI": "10.1097/YIC.0b013e3283400d35",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_16_1"
},
{
"DOI": "10.1038/s41421-020-0153-3",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_17_1"
},
{
"DOI": "10.1371/journal.pbio.3000970",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_18_1"
},
{
"DOI": "10.1111/jpi.12754",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_19_1"
},
{
"DOI": "10.4269/ajtmh.20-0762",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_20_1"
},
{
"article-title": "Human angiotensin‐converting enzyme 2 transgenic mice infected with SARS‐CoV‐2 develop severe and fatal respiratory disease. JCI",
"author": "Golden JW",
"first-page": "e142032",
"issue": "19",
"journal-title": "Insight",
"key": "e_1_2_8_21_1",
"volume": "5",
"year": "2020"
},
{
"DOI": "10.1371/journal.ppat.1009195",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_22_1"
},
{
"DOI": "10.1038/s41467-020-19891-7",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_23_1"
},
{
"DOI": "10.1038/s41590-020-0778-2",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_24_1"
},
{
"DOI": "10.1038/s41423-020-00616-1",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_25_1"
},
{
"DOI": "10.1038/s41586-020-2787-6",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_26_1"
},
{
"DOI": "10.1016/j.coviro.2021.03.009",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_27_1"
},
{
"DOI": "10.1016/S0140-6736(20)30628-0",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_28_1"
},
{
"DOI": "10.1038/s41586-020-2588-y",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_29_1"
},
{
"DOI": "10.1126/sciimmunol.abd1554",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_30_1"
},
{
"DOI": "10.1126/science.abc3545",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_31_1"
},
{
"DOI": "10.1126/science.abc2061",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_32_1"
},
{
"DOI": "10.1016/j.cell.2021.08.016",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_33_1"
},
{
"DOI": "10.1080/22221751.2020.1838955",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_34_1"
},
{
"DOI": "10.1016/j.cell.2020.06.011",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_35_1"
},
{
"DOI": "10.1084/jem.20201241",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_36_1"
},
{
"DOI": "10.1038/s41586-020-2312-y",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_37_1"
},
{
"DOI": "10.1016/j.chom.2020.05.020",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_38_1"
},
{
"DOI": "10.1128/JVI.02012-06",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_39_1"
},
{
"DOI": "10.1073/pnas.1517719113",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_40_1"
},
{
"DOI": "10.1016/j.cell.2020.05.027",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_41_1"
},
{
"DOI": "10.1186/s12931-020-1325-2",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_42_1"
},
{
"DOI": "10.1017/S1461145710001045",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_43_1"
},
{
"DOI": "10.1096/fj.202000305R",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_44_1"
},
{
"DOI": "10.1159/000123997",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_45_1"
},
{
"DOI": "10.1124/pr.110.002832",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_46_1"
},
{
"DOI": "10.1111/bph.14116",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_47_1"
},
{
"DOI": "10.1111/j.1600-079X.2011.00962.x",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_48_1"
},
{
"DOI": "10.1016/j.tips.2020.04.001",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_49_1"
},
{
"DOI": "10.1111/jpi.12683",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_50_1"
},
{
"DOI": "10.1096/fj.15-273656",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_51_1"
},
{
"DOI": "10.1111/jpi.12326",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_52_1"
},
{
"DOI": "10.4103/0976-0105.177703",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_53_1"
},
{
"DOI": "10.1177/0091270005283461",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_54_1"
},
{
"DOI": "10.1001/archpsyc.63.10.1149",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_55_1"
},
{
"article-title": "Melatonin and S‐20098 increase REM sleep and wake‐up propensity without modifying NREM sleep homeostasis",
"author": "Cajochen C",
"first-page": "R1189",
"issue": "4",
"journal-title": "Am J Physiol",
"key": "e_1_2_8_56_1",
"volume": "272",
"year": "1997"
},
{
"article-title": "Pilot study comparing in blind the therapeutic effect of two doses of agomelatine, melatonin‐ agonist and selective 5HT2c receptors antagonist, in the treatment of major depressive disorders",
"author": "Loo H",
"first-page": "165",
"issue": "2",
"journal-title": "Encephale",
"key": "e_1_2_8_57_1",
"volume": "29",
"year": "2003"
},
{
"DOI": "10.1210/jcem-45-4-768",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_58_1"
},
{
"DOI": "10.1001/jama.1972.03200140072031",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_59_1"
},
{
"DOI": "10.1111/jpi.12702",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_60_1"
},
{
"DOI": "10.1016/j.it.2021.02.003",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_61_1"
},
{
"DOI": "10.1038/s41591-020-1038-6",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_62_1"
},
{
"DOI": "10.1126/science.abd4585",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_63_1"
},
{
"DOI": "10.1126/science.abd4570",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_64_1"
},
{
"DOI": "10.1016/j.chom.2020.04.017",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_65_1"
},
{
"DOI": "10.1016/j.it.2017.05.005",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_66_1"
},
{
"DOI": "10.1038/s41577-020-0346-x",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_67_1"
},
{
"DOI": "10.1126/science.abc6027",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_68_1"
},
{
"DOI": "10.1007/978-1-4614-8289-5_1",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_69_1"
},
{
"DOI": "10.3748/wjg.v10.i18.2690",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_70_1"
},
{
"DOI": "10.1111/j.1600-079X.2005.00265.x",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_71_1"
},
{
"DOI": "10.1111/j.1600-079X.2007.00445.x",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_72_1"
},
{
"DOI": "10.1016/j.intimp.2015.10.012",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_73_1"
},
{
"DOI": "10.1111/j.1600-079X.2009.00733.x",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_74_1"
},
{
"DOI": "10.1111/jpi.12335",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_75_1"
},
{
"DOI": "10.1016/j.jff.2019.04.062",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_76_1"
},
{
"DOI": "10.1111/jcmm.15398",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_77_1"
},
{
"DOI": "10.1016/j.bbi.2021.01.034",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_78_1"
},
{
"DOI": "10.1016/j.ejphar.2021.174193",
"doi-asserted-by": "publisher",
"key": "e_1_2_8_79_1"
}
],
"reference-count": 78,
"references-count": 78,
"relation": {},
"resource": {
"primary": {
"URL": "https://onlinelibrary.wiley.com/doi/10.1111/jpi.12772"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "Therapeutic potential of melatonin and melatonergic drugs on K18‐<i>hACE2</i> mice infected with SARS‐CoV‐2",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1002/crossmark_policy",
"volume": "72"
}
