Circulating Vitamin D levels status and clinical prognostic indices in COVID-19 patients
et al., Respiratory Research, doi:10.1186/s12931-021-01666-3, Mar 2021
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 52 hospitalized COVID-19 patients showing that vitamin D deficiency is associated with compromised inflammatory responses and higher pulmonary involvement. Vitamin D deficient patients also showed higher mortality, although not quite reaching statistical significance with the small sample size.
This is the 51st of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
|
risk of death, 87.6% lower, RR 0.12, p = 0.07, high D levels 0 of 30 (0.0%), low D levels 3 of 22 (13.6%), NNT 7.3, relative risk is not 0 because of continuity correction due to zero events (with reciprocal of the contrasting arm), >10 ng/mL.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Ricci et al., 3 Mar 2021, retrospective, Italy, peer-reviewed, 15 authors.
Circulating Vitamin D levels status and clinical prognostic indices in COVID-19 patients
Respiratory Research, doi:10.1186/s12931-021-01666-3
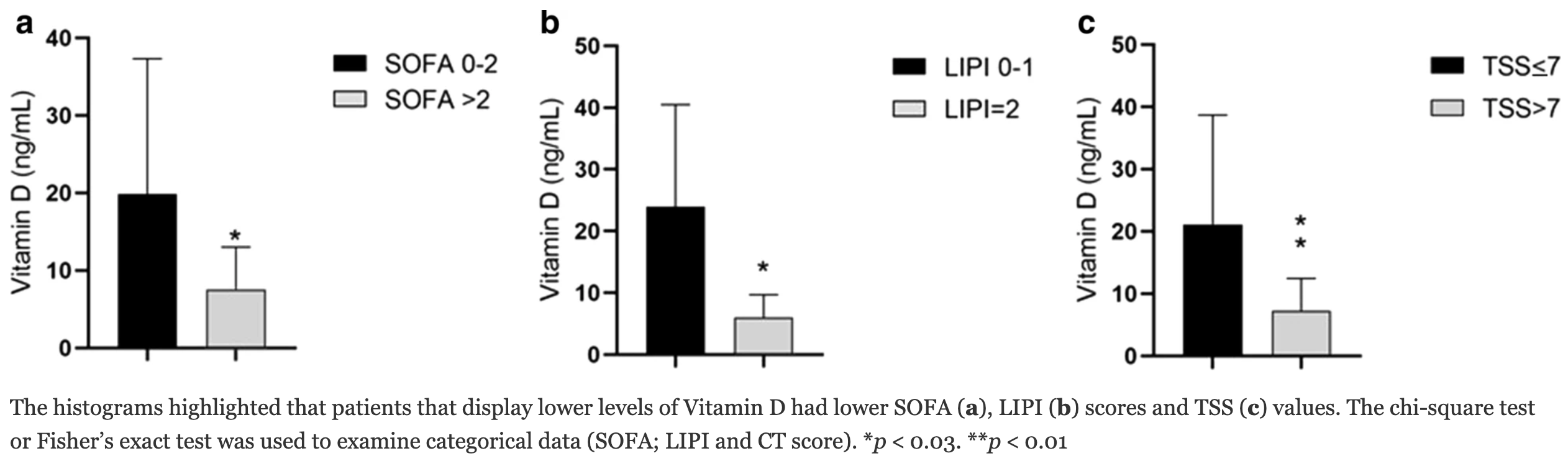
Background: Several immune mechanisms activate in COVID-19 pathogenesis. Usually, coronavirus infection is characterized by dysregulated host immune responses, interleukine-6 increase, hyper-activation of cytotoxic CD8 T lymphocytes. Interestingly, Vitamin D deficiency has been often associated with altered immune responses and infections. In the present study, we evaluated Vitamin D plasma levels in patients affected with different lung involvement during COVID-19 infection. Methods: Lymphocyte phenotypes were assessed by flow cytometry. Thoracic CT scan involvement was obtained by an image analysis program. Results: Vitamin D levels were deficient in (80%) of patients, insufficient in (6.5%) and normal in (13.5%). Patients with very low Vitamin D plasma levels had more elevated D-Dimer values, a more elevated B lymphocyte cell count, a reduction of CD8 + T lymphocytes with a low CD4/CD8 ratio, more compromised clinical findings (measured by LIPI and SOFA scores) and thoracic CT scan involvement.
Conclusions: Vitamin D deficiency is associated with compromised inflammatory responses and higher pulmonary involvement in COVID-19 affected patients. Vitamin D assessment, during COVID-19 infection, could be a useful analysis for possible therapeutic interventions.
Abbreviations VitD: Vitamin D; CT: Computed tomography; PII: Pulmonary inflammation index; SOFA: Sequential Organ Failure Assessment; LIPI: Lung Immune Prognosis Index; PBMC: Peripheral blood lymphocyte; NLR: Neutrophils and Lymphocytes ratio; dNLR: Derived Neutrophils/ Leucocytes-Neutrophils ratio; TSS: Total severity score.
Authors' contributions The authors have made the following declaration about their contributions. Conceived and designed: AR, AP, MD, BS, SG. Development and methodology: CDV, RM, VS, PA, AM, Acquisition of data: MI, CDD, AL, EM. FF. Analysis and interpretation of the results: AR, AP, MD, MI. Writing, review and revision of the manuscript: AR, AP, MD, SS Study supervision: AR, MD. All authors read and approved the final manuscript.
Ethics approval and consent to participate The study was approved by our Institutional Ethical Committee (Sapienza University of Rome, Italy) (Prot.# 52SA_2020, RIF. CE 5773_2020), on the basis that it complied with the declaration of Helsinki and that the protocol followed existing good clinical practice guidelines. A written informed consent to participate in the study was obtained from every participant. In case of adults with cognitive decline the consent to participate to the study was given by the legal guardian. An administrative permission to access the clinical/personal patient data used in our research was given by the Health Director of our Hospital, who is also a co-author of the manuscript.
Consent for..
References
Aslam, John, Bhatti, Jahangir, Kamboh, Vitamin D as a principal factor in mediating rheumatoid arthritis-derived immune response, Biomed Res Int, doi:10.1155/2019/3494937
Baeke, Takiishi, Korf, Gysemans, Mathieu, Vitamin D: modulator of the immune system, Curr Opin Pharmacol, doi:10.1016/j.coph.2010.04.001
Baeke, Van Etten, Gysemans, Overbergh, Mathieu, Vitamin D signaling in immune-mediated disorders: evolving insights and therapeutic opportunities, Mol Aspects Med, doi:10.1016/j.mam.2008.05.004
Basu, Fenton, Toll-like receptors: function and roles in lung disease, Am J Physiol Lung Cell Mol Physiol, doi:10.1152/ajplung.00323.2003
Baune, Rothermundt, Ladwig, Meisinger, Berger, Systemic inflammation (Interleukin 6) predicts all-cause mortality in men: results from a 9-year follow-up of the MEMO Study, Age (Dordr, doi:10.1007/s11357-010-9165-5
Chirumbolo, Bjørklund, Sboarina, Vella, The role of Vitamin D in the immune system as a pro-survival molecule, Clin Ther, doi:10.1016/j.clinthera.2017.03.021
Gargari, Behmanesh, Farsani, Kakhki, Azimi, Vitamin D supplementation up-regulates IL-6 and IL-17A gene expression in multiple sclerosis patients, Int Immunopharmacol, doi:10.1016/j.intimp.2015.06.033
Goncalves-Mendes, Talvas, Dualé, Guttmann, Corbin et al., Impact of Vitamin D supplementation on influenza vaccine response and immune functions in deficient elderly persons: a randomized placebo-controlled trial, Front Immunol, doi:10.3389/fimmu.2019.00065
Hansdottir, Monick, Vitamin D effects on lung immunity and respiratory diseases, Vitam Horm, doi:10.1016/B978-0-12-386960-9.00009-5
Hejazi, Modarresi-Ghazani, Entezari-Maleki, A review of Vitamin D effects on common respiratory diseases: Asthma, chronic obstructive pulmonary disease, and tuberculosis, J Res Pharm Pract, doi:10.4103/2279-042X.176542
Hensel, Mcandrews, Mcgrail, Dowlatshahi, Lebleu et al., Protection against SARS-CoV-2 by BCG vaccination is not supported by epidemiological analyses, Sci Rep, doi:10.1038/s41598-020-75491-x
Holick, Binkley, Bischoff-Ferrari, Gordon, Hanley et al., Evaluation, treatment, and prevention of vitamin D deficiency: an endocrine society clinical practice guideline, J Clin Endocrinol Metab, doi:10.1210/jc.2011-0385
Holick, Vitamin d Deficiency, N Engl J Med, doi:10.1056/NEJMra070553
Hughes, Norton, Vitamin D and respiratory health, Clin Exp Immunol, doi:10.1111/j.1365-2249.2009.04001.x
Iwasaki, Medzhitov, Regulation of adaptive immunity by the innate immune system, Science, doi:10.1126/science.1183021
Jones, Trzeciak, Kline, The Sequential Organ Failure Assessment score for predicting outcome in patients with severe sepsis and evidence of hypoperfusion at the time of emergency department presentation, Crit Care Med, doi:10.1097/CCM.0b013e31819def97
Kazandjian, Gong, Keegan, Pazdur, Blumenthal, Prognostic value of the lung immune prognostic index for patients treated for metastatic non-small cell lung cancer, JAMA Oncol, doi:10.1001/jamaoncol.2019.1747
Laaksi, Ruohola, Tuohimaa, Auvinen, Haataja et al., An association of serum vitamin D concentrations < 40 nmol/L with acute respiratory tract infection in young Finnish men, Am J Clin Nutr, doi:10.1093/ajcn/86.3.714
Liao, Liu, Yuan, Wen, Xu et al., The landscape of lung bronchoalveolar immune cells in COVID-19 revealed by single-cell RNA sequencing, MedRxiv, doi:10.1101/2020.02.23.20026690
Lips, Cashman, Lamberg-Allardt, Bischoff-Ferrari, Obermayer-Pietsch et al., Current vitamin D status in European and Middle East countries and strategies to prevent vitamin D deficiency: a position statement of the European Calcified Tissue Society, Eur J Endocrinol, doi:10.1530/EJE-18-0736
Martineau, Jolliffe, Hooper, Greenberg, Aloia et al., Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data, BMJ, doi:10.1136/bmj.i6583
Mehta, Mcauley, Brown, Sanchez, Tattersall et al., HLH across speciality collaboration, UK, COVID-19: consider cytokine storm syndromes and immunosuppression, Lancet, doi:10.1016/S0140-6736(20)30628-0
Meltzer, Best, Zhang, Vokes, Arora et al., Association of Vitamin D status and other clinical characteristics with COVID-19 test results, JAMA Netw Open, doi:10.1001/jamanetworkopen.2020.19722
Moorlag, Arts, Van Crevel, Netea, Non-specific effects of BCG vaccine on viral infections, Clin Microbiol Infect, doi:10.1016/j.cmi.2019.04.020
Navarro-Barriuso, Mansilla, Naranjo-Gómez, Sánchez-Pla, Quirant-Sánchez et al., Comparative transcriptomic profile of tolerogenic dendritic cells differentiated with vitamin D3, dexamethasone and rapamycin, Sci Rep, doi:10.1038/s41598-018-33248-7
Prietl, Treiber, Pieber, Amrein, Vitamin D and immune function, Nutrients, doi:10.3390/nu5072502
Ritchie, Singanayagam, Immunosuppression for hyperinflammation in COVID-19: a double-edged sword?, Lancet, doi:10.1016/S0140-6736(20)30691-7
Rosa, Malaguarnera, Gregorio, Palumbo, Nunnari et al., Immuno-modulatory effects of vitamin D3 in human monocyte and macrophages, Cell Immunol, doi:10.1016/j.cellimm.2012.10.009
Ross, Manson, Abrams, Aloia, Brannon et al., Report on dietary reference intakes for calcium and vitamin D from the institute of medicine: what clinicians need to know, J Clin Endocrinol Metab, doi:10.1210/jc.2010-2704
Sacn Vitamin, Report, None, GOV.UK
Teymoori-Rad, Shokri, Salimi, Marashi, The interplay between vitamin D and viral infections, Rev Med Virol, doi:10.1002/rmv.2032
Varga, Flammer, Steiger, Haberecker, Andermatt et al., Endothelial cell infection and endotheliitis in COVID-19, Lancet, doi:10.1016/S0140-6736(20)30937-5
Wang, Zhang, Richards, Kestenbaum, Van Meurs et al., Common genetic determinants of vitamin D insufficiency: a genomewide association study, Lancet, doi:10.1016/S0140-6736(10)60588-0
Xiong, Liu, Cao, Wang, Guo et al., Transcriptomic characteristics of bronchoalveolar lavage fluid and peripheral blood mononuclear cells in COVID-19 patients, Emerg Microbes Infect, doi:10.1080/22221751.2020.1747363
Zhang, Leung, Richers, Liu, Remigio et al., Vitamin D inhibits monocyte/macrophage proinflammatory cytokine production by targeting MAPK phosphatase-1, J Immunol, doi:10.4049/jimmunol.1102412
DOI record:
{
"DOI": "10.1186/s12931-021-01666-3",
"ISSN": [
"1465-993X"
],
"URL": "http://dx.doi.org/10.1186/s12931-021-01666-3",
"abstract": "<jats:title>Abstract</jats:title><jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>Several immune mechanisms activate in COVID-19 pathogenesis. Usually, coronavirus infection is characterized by dysregulated host immune responses, interleukine-6 increase, hyper-activation of cytotoxic CD8 T lymphocytes. Interestingly, Vitamin D deficiency has been often associated with altered immune responses and infections. In the present study, we evaluated Vitamin D plasma levels in patients affected with different lung involvement during COVID-19 infection.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Methods</jats:title>\n <jats:p>Lymphocyte phenotypes were assessed by flow cytometry. Thoracic CT scan involvement was obtained by an image analysis program.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>Vitamin D levels were deficient in (80%) of patients, insufficient in (6.5%) and normal in (13.5%). Patients with very low Vitamin D plasma levels had more elevated D-Dimer values, a more elevated B lymphocyte cell count, a reduction of CD8 + T lymphocytes with a low CD4/CD8 ratio, more compromised clinical findings (measured by LIPI and SOFA scores) and thoracic CT scan involvement.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Conclusions</jats:title>\n <jats:p>Vitamin D deficiency is associated with compromised inflammatory responses and higher pulmonary involvement in COVID-19 affected patients. Vitamin D assessment, during COVID-19 infection, could be a useful analysis for possible therapeutic interventions.</jats:p>\n <jats:p><jats:italic>Trial registration:</jats:italic> 'retrospectively registered'.</jats:p>\n </jats:sec>",
"alternative-id": [
"1666"
],
"article-number": "76",
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "27 July 2020"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "17 February 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "3 March 2021"
},
{
"group": {
"label": "Ethics approval and consent to participate",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1,
"value": "The study was approved by our Institutional Ethical Committee (Sapienza University of Rome, Italy) (Prot.# 52SA_2020, RIF. CE 5773_2020), on the basis that it complied with the declaration of Helsinki and that the protocol followed existing good clinical practice guidelines. A written informed consent to participate in the study was obtained from every participant. In case of adults with cognitive decline the consent to participate to the study was given by the legal guardian. An administrative permission to access the clinical/personal patient data used in our research was given by the Health Director of our Hospital, who is also a co-author of the manuscript."
},
{
"group": {
"label": "Consent for publication",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "Not applicable."
},
{
"group": {
"label": "Competing interests",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "The authors declare they have no conflict of interest."
}
],
"author": [
{
"affiliation": [],
"family": "Ricci",
"given": "Alberto",
"sequence": "first"
},
{
"affiliation": [],
"family": "Pagliuca",
"given": "Alessandra",
"sequence": "additional"
},
{
"affiliation": [],
"family": "D’Ascanio",
"given": "Michela",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Innammorato",
"given": "Marta",
"sequence": "additional"
},
{
"affiliation": [],
"family": "De Vitis",
"given": "Claudia",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mancini",
"given": "Rita",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Giovagnoli",
"given": "Simonetta",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Facchiano",
"given": "Francesco",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sposato",
"given": "Bruno",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Anibaldi",
"given": "Paolo",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Marcolongo",
"given": "Adriano",
"sequence": "additional"
},
{
"affiliation": [],
"family": "De Dominicis",
"given": "Chiara",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Laghi",
"given": "Andrea",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Muscogiuri",
"given": "Emanuele",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sciacchitano",
"given": "Salvatore",
"sequence": "additional"
}
],
"container-title": "Respiratory Research",
"container-title-short": "Respir Res",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2021,
3,
3
]
],
"date-time": "2021-03-03T18:20:11Z",
"timestamp": 1614795611000
},
"deposited": {
"date-parts": [
[
2021,
3,
3
]
],
"date-time": "2021-03-03T18:24:13Z",
"timestamp": 1614795853000
},
"indexed": {
"date-parts": [
[
2024,
1,
26
]
],
"date-time": "2024-01-26T17:46:24Z",
"timestamp": 1706291184437
},
"is-referenced-by-count": 27,
"issue": "1",
"issued": {
"date-parts": [
[
2021,
3,
3
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2021,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "http://creativecommons.org/licenses/by/4.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
3,
3
]
],
"date-time": "2021-03-03T00:00:00Z",
"timestamp": 1614729600000
}
},
{
"URL": "http://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
3,
3
]
],
"date-time": "2021-03-03T00:00:00Z",
"timestamp": 1614729600000
}
}
],
"link": [
{
"URL": "http://link.springer.com/content/pdf/10.1186/s12931-021-01666-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://link.springer.com/article/10.1186/s12931-021-01666-3/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "http://link.springer.com/content/pdf/10.1186/s12931-021-01666-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1186",
"published": {
"date-parts": [
[
2021,
3,
3
]
]
},
"published-online": {
"date-parts": [
[
2021,
3,
3
]
]
},
"published-print": {
"date-parts": [
[
2021,
12
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.1016/S0140-6736(20)30937-5",
"author": "Z Varga",
"doi-asserted-by": "publisher",
"first-page": "1417",
"journal-title": "Lancet",
"key": "1666_CR1",
"unstructured": "Varga Z, Flammer AJ, Steiger P, Haberecker M, Andermatt R, Zinkernagel AS, Mehra MR, Schuepbach RA, Ruschitzka F, Moch H. Endothelial cell infection and endotheliitis in COVID-19. Lancet. 2020;395:1417–8. https://doi.org/10.1016/S0140-6736(20)30937-5.",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30691-7",
"author": "AI Ritchie",
"doi-asserted-by": "publisher",
"first-page": "1111",
"journal-title": "Lancet",
"key": "1666_CR2",
"unstructured": "Ritchie AI, Singanayagam A. Immunosuppression for hyperinflammation in COVID-19: a double-edged sword? Lancet. 2020;395:1111. https://doi.org/10.1016/S0140-6736(20)30691-7.",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30628-0",
"author": "P Mehta",
"doi-asserted-by": "publisher",
"first-page": "1033",
"journal-title": "Lancet",
"key": "1666_CR3",
"unstructured": "Mehta P, McAuley DF, Brown M, Sanchez E, Tattersall RS, Manson JJ. HLH across speciality collaboration, UK, COVID-19: consider cytokine storm syndromes and immunosuppression. Lancet. 2020;395:1033–4. https://doi.org/10.1016/S0140-6736(20)30628-0.",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1007/s11357-010-9165-5",
"author": "BT Baune",
"doi-asserted-by": "publisher",
"first-page": "209",
"journal-title": "Age (Dordr)",
"key": "1666_CR4",
"unstructured": "Baune BT, Rothermundt M, Ladwig KH, Meisinger C, Berger K. Systemic inflammation (Interleukin 6) predicts all-cause mortality in men: results from a 9-year follow-up of the MEMO Study. Age (Dordr). 2011;33:209–17. https://doi.org/10.1007/s11357-010-9165-5.",
"volume": "33",
"year": "2011"
},
{
"DOI": "10.4103/2279-042X.176542",
"author": "ME Hejazi",
"doi-asserted-by": "publisher",
"first-page": "7",
"journal-title": "J Res Pharm Pract",
"key": "1666_CR5",
"unstructured": "Hejazi ME, Modarresi-Ghazani F, Entezari-Maleki T. A review of Vitamin D effects on common respiratory diseases: Asthma, chronic obstructive pulmonary disease, and tuberculosis. J Res Pharm Pract. 2016;5:7–15. https://doi.org/10.4103/2279-042X.176542.",
"volume": "5",
"year": "2016"
},
{
"DOI": "10.1111/j.1365-2249.2009.04001.x",
"author": "DA Hughes",
"doi-asserted-by": "publisher",
"first-page": "20",
"journal-title": "Clin Exp Immunol",
"key": "1666_CR6",
"unstructured": "Hughes DA, Norton R. Vitamin D and respiratory health. Clin Exp Immunol. 2009;158:20–5. https://doi.org/10.1111/j.1365-2249.2009.04001.x.",
"volume": "158",
"year": "2009"
},
{
"DOI": "10.1002/rmv.2032",
"author": "M Teymoori-Rad",
"doi-asserted-by": "publisher",
"first-page": "e2032",
"journal-title": "Rev Med Virol",
"key": "1666_CR7",
"unstructured": "Teymoori-Rad M, Shokri F, Salimi V, Marashi SM. The interplay between vitamin D and viral infections. Rev Med Virol. 2019;29:e2032. https://doi.org/10.1002/rmv.2032.",
"volume": "29",
"year": "2019"
},
{
"DOI": "10.1056/NEJMra070553",
"author": "MF Holick",
"doi-asserted-by": "publisher",
"first-page": "266",
"journal-title": "N Engl J Med",
"key": "1666_CR8",
"unstructured": "Holick MF. Vitamin d Deficiency. N Engl J Med. 2007;357:266–81. https://doi.org/10.1056/NEJMra070553.",
"volume": "357",
"year": "2007"
},
{
"DOI": "10.1016/S0140-6736(10)60588-0",
"author": "TJ Wang",
"doi-asserted-by": "publisher",
"first-page": "180",
"journal-title": "Lancet",
"key": "1666_CR9",
"unstructured": "Wang TJ, Zhang F, Richards JB, Kestenbaum B, van Meurs JB, Berry D, Kiel DP, Streeten EA, Ohlsson C, Koller DL, Peltonen L, Cooper JD, O’Reilly PF, Houston DK, Glazer NL, Vandenput L, Peacock M, Shi J, Rivadeneira F, McCarthy MI, Anneli P, de Boer IH, Mangino M, Kato B, Smyth DJ, Booth SL, Jacques PF, Burke GL, Goodarzi M, Cheung C-L, Wolf M, Rice K, Goltzman D, Hidiroglou N, Ladouceur M, Wareham NJ, Hocking LJ, Hart D, Arden NK, Cooper C, Malik S, Fraser WD, Hartikainen A-L, Zhai G, Macdonald HM, Forouhi NG, Loos RJ, Reid DM, Hakim A, Dennison E, Liu Y, Power C, Stevens HE, Jaana L, Vasan RS, Soranzo N, Bojunga J, Psaty BM, Lorentzon M, Foroud T, Harris TB, Hofman A, Jansson J-O, Cauley JA, Uitterlinden AG, Gibson Q, Järvelin M-R, Karasik D, Siscovick DS, Econs MJ, Kritchevsky SB, Florez JC, Todd JA, Dupuis J, Hyppönen E, Spector TD. Common genetic determinants of vitamin D insufficiency: a genome-wide association study. Lancet. 2010;376:180–8. https://doi.org/10.1016/S0140-6736(10)60588-0.",
"volume": "376",
"year": "2010"
},
{
"DOI": "10.3390/nu5072502",
"author": "B Prietl",
"doi-asserted-by": "publisher",
"first-page": "2502",
"journal-title": "Nutrients",
"key": "1666_CR10",
"unstructured": "Prietl B, Treiber G, Pieber TR, Amrein K. Vitamin D and immune function. Nutrients. 2013;5:2502–21. https://doi.org/10.3390/nu5072502.",
"volume": "5",
"year": "2013"
},
{
"DOI": "10.1016/j.coph.2010.04.001",
"author": "F Baeke",
"doi-asserted-by": "publisher",
"first-page": "482",
"journal-title": "Curr Opin Pharmacol",
"key": "1666_CR11",
"unstructured": "Baeke F, Takiishi T, Korf H, Gysemans C, Mathieu C. Vitamin D: modulator of the immune system. Curr Opin Pharmacol. 2010;10:482–96. https://doi.org/10.1016/j.coph.2010.04.001.",
"volume": "10",
"year": "2010"
},
{
"DOI": "10.1155/2019/3494937",
"author": "MM Aslam",
"doi-asserted-by": "publisher",
"journal-title": "Biomed Res Int.",
"key": "1666_CR12",
"unstructured": "Aslam MM, John P, Bhatti A, Jahangir S, Kamboh MI. Vitamin D as a principal factor in mediating rheumatoid arthritis-derived immune response. Biomed Res Int. 2019. https://doi.org/10.1155/2019/3494937.",
"year": "2019"
},
{
"DOI": "10.4049/jimmunol.1102412",
"author": "Y Zhang",
"doi-asserted-by": "publisher",
"first-page": "2127",
"journal-title": "J Immunol",
"key": "1666_CR13",
"unstructured": "Zhang Y, Leung DYM, Richers BN, Liu Y, Remigio LK, Riches DW, Goleva E. Vitamin D inhibits monocyte/macrophage proinflammatory cytokine production by targeting MAPK phosphatase-1. J Immunol. 2012;188:2127–35. https://doi.org/10.4049/jimmunol.1102412.",
"volume": "188",
"year": "2012"
},
{
"DOI": "10.1016/j.cellimm.2012.10.009",
"author": "M Di Rosa",
"doi-asserted-by": "publisher",
"first-page": "36",
"journal-title": "Cell Immunol",
"key": "1666_CR14",
"unstructured": "Di Rosa M, Malaguarnera G, De Gregorio C, Palumbo M, Nunnari G, Malaguarnera L. Immuno-modulatory effects of vitamin D3 in human monocyte and macrophages. Cell Immunol. 2012;280:36–43. https://doi.org/10.1016/j.cellimm.2012.10.009.",
"volume": "280",
"year": "2012"
},
{
"DOI": "10.1038/s41598-018-33248-7",
"author": "J Navarro-Barriuso",
"doi-asserted-by": "publisher",
"first-page": "14985",
"journal-title": "Sci Rep",
"key": "1666_CR15",
"unstructured": "Navarro-Barriuso J, Mansilla MJ, Naranjo-Gómez M, Sánchez-Pla A, Quirant-Sánchez B, Teniente-Serra A, Ramo-Tello C, Martínez-Cáceres EM. Comparative transcriptomic profile of tolerogenic dendritic cells differentiated with vitamin D3, dexamethasone and rapamycin. Sci Rep. 2018;8:14985. https://doi.org/10.1038/s41598-018-33248-7.",
"volume": "8",
"year": "2018"
},
{
"DOI": "10.1136/bmj.i6583",
"author": "AR Martineau",
"doi-asserted-by": "publisher",
"journal-title": "BMJ",
"key": "1666_CR16",
"unstructured": "Martineau AR, Jolliffe DA, Hooper RL, Greenberg L, Aloia JF, Bergman P, Dubnov-Raz G, Esposito S, Ganmaa D, Ginde AA, Goodall EC, Grant CC, Griffiths CJ, Janssens W, Laaksi I, Manaseki-Holland S, Mauger D, Murdoch DR, Neale R, Rees JR, Simpson S, Stelmach I, Kumar GT, Urashima M, Camargo CA. Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data. BMJ. 2017. https://doi.org/10.1136/bmj.i6583.",
"year": "2017"
},
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"author": "DO Meltzer",
"doi-asserted-by": "publisher",
"first-page": "e2019722",
"journal-title": "JAMA Netw Open",
"key": "1666_CR17",
"unstructured": "Meltzer DO, Best TJ, Zhang H, Vokes T, Arora V, Solway J. Association of Vitamin D status and other clinical characteristics with COVID-19 test results. JAMA Netw Open. 2020;3:e2019722. https://doi.org/10.1001/jamanetworkopen.2020.19722.",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1097/CCM.0b013e31819def97",
"author": "AE Jones",
"doi-asserted-by": "publisher",
"first-page": "1649",
"journal-title": "Crit Care Med",
"key": "1666_CR18",
"unstructured": "Jones AE, Trzeciak S, Kline JA. The Sequential Organ Failure Assessment score for predicting outcome in patients with severe sepsis and evidence of hypoperfusion at the time of emergency department presentation. Crit Care Med. 2009;37:1649–54. https://doi.org/10.1097/CCM.0b013e31819def97.",
"volume": "37",
"year": "2009"
},
{
"DOI": "10.1001/jamaoncol.2019.1747",
"author": "D Kazandjian",
"doi-asserted-by": "publisher",
"journal-title": "JAMA Oncol",
"key": "1666_CR19",
"unstructured": "Kazandjian D, Gong Y, Keegan P, Pazdur R, Blumenthal GM. Prognostic value of the lung immune prognostic index for patients treated for metastatic non-small cell lung cancer. JAMA Oncol. 2019. https://doi.org/10.1001/jamaoncol.2019.1747.",
"year": "2019"
},
{
"DOI": "10.1210/jc.2010-2704",
"author": "AC Ross",
"doi-asserted-by": "publisher",
"first-page": "53",
"issue": "2011",
"journal-title": "J Clin Endocrinol Metab",
"key": "1666_CR20",
"unstructured": "Ross AC, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, Durazo-Arvizu RA, Gallagher JC, Gallo RL, Jones G, Kovacs CS, Mayne ST, Rosen CJ, Shapses SA, The, . Report on dietary reference intakes for calcium and vitamin D from the institute of medicine: what clinicians need to know. J Clin Endocrinol Metab. 2011;96(2011):53–8. https://doi.org/10.1210/jc.2010-2704.",
"volume": "96",
"year": "2011"
},
{
"DOI": "10.1016/j.mam.2008.05.004",
"author": "F Baeke",
"doi-asserted-by": "publisher",
"first-page": "376",
"journal-title": "Mol Aspects Med",
"key": "1666_CR21",
"unstructured": "Baeke F, van Etten E, Gysemans C, Overbergh L, Mathieu C. Vitamin D signaling in immune-mediated disorders: evolving insights and therapeutic opportunities. Mol Aspects Med. 2008;29:376–87. https://doi.org/10.1016/j.mam.2008.05.004.",
"volume": "29",
"year": "2008"
},
{
"DOI": "10.1093/ajcn/86.3.714",
"author": "I Laaksi",
"doi-asserted-by": "publisher",
"first-page": "714",
"journal-title": "Am J Clin Nutr",
"key": "1666_CR22",
"unstructured": "Laaksi I, Ruohola J-P, Tuohimaa P, Auvinen A, Haataja R, Pihlajamäki H, Ylikomi T. An association of serum vitamin D concentrations < 40 nmol/L with acute respiratory tract infection in young Finnish men. Am J Clin Nutr. 2007;86:714–7. https://doi.org/10.1093/ajcn/86.3.714.",
"volume": "86",
"year": "2007"
},
{
"DOI": "10.1210/jc.2011-0385",
"author": "MF Holick",
"doi-asserted-by": "publisher",
"first-page": "1911",
"journal-title": "J Clin Endocrinol Metab",
"key": "1666_CR23",
"unstructured": "Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, Murad MH, Weaver CM. Evaluation, treatment, and prevention of vitamin D deficiency: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2011;96:1911–30. https://doi.org/10.1210/jc.2011-0385.",
"volume": "96",
"year": "2011"
},
{
"DOI": "10.1530/EJE-18-0736",
"author": "P Lips",
"doi-asserted-by": "publisher",
"journal-title": "Eur J Endocrinol.",
"key": "1666_CR24",
"unstructured": "Lips P, Cashman KD, Lamberg-Allardt C, Bischoff-Ferrari HA, Obermayer-Pietsch B, Bianchi ML, Stepan J, El-Hajj Fuleihan G, Bouillon R. Current vitamin D status in European and Middle East countries and strategies to prevent vitamin D deficiency: a position statement of the European Calcified Tissue Society. Eur J Endocrinol. 2019. https://doi.org/10.1530/EJE-18-0736.",
"year": "2019"
},
{
"key": "1666_CR25",
"unstructured": "SACN vitamin D and health report, GOV.UK. (n.d.). https://www.gov.uk/government/publications/sacn-vitamin-d-and-health-report. Accessed 6 Jul 2020."
},
{
"DOI": "10.1016/j.clinthera.2017.03.021",
"author": "S Chirumbolo",
"doi-asserted-by": "publisher",
"first-page": "894",
"journal-title": "Clin Ther",
"key": "1666_CR26",
"unstructured": "Chirumbolo S, Bjørklund G, Sboarina A, Vella A. The role of Vitamin D in the immune system as a pro-survival molecule. Clin Ther. 2017;39:894–916. https://doi.org/10.1016/j.clinthera.2017.03.021.",
"volume": "39",
"year": "2017"
},
{
"DOI": "10.1016/B978-0-12-386960-9.00009-5",
"author": "S Hansdottir",
"doi-asserted-by": "publisher",
"first-page": "217",
"journal-title": "Vitam Horm",
"key": "1666_CR27",
"unstructured": "Hansdottir S, Monick MM. Vitamin D effects on lung immunity and respiratory diseases. Vitam Horm. 2011;86:217–37. https://doi.org/10.1016/B978-0-12-386960-9.00009-5.",
"volume": "86",
"year": "2011"
},
{
"DOI": "10.1152/ajplung.00323.2003",
"author": "S Basu",
"doi-asserted-by": "publisher",
"first-page": "L887",
"journal-title": "Am J Physiol Lung Cell Mol Physiol",
"key": "1666_CR28",
"unstructured": "Basu S, Fenton MJ. Toll-like receptors: function and roles in lung disease. Am J Physiol Lung Cell Mol Physiol. 2004;286:L887-892. https://doi.org/10.1152/ajplung.00323.2003.",
"volume": "286",
"year": "2004"
},
{
"DOI": "10.1126/science.1183021",
"author": "A Iwasaki",
"doi-asserted-by": "publisher",
"first-page": "291",
"journal-title": "Science",
"key": "1666_CR29",
"unstructured": "Iwasaki A, Medzhitov R. Regulation of adaptive immunity by the innate immune system. Science. 2010;327:291–5. https://doi.org/10.1126/science.1183021.",
"volume": "327",
"year": "2010"
},
{
"DOI": "10.1016/j.intimp.2015.06.033",
"author": "B Naghavi Gargari",
"doi-asserted-by": "publisher",
"journal-title": "Int Immunopharmacol.",
"key": "1666_CR30",
"unstructured": "Naghavi Gargari B, Behmanesh M, Shirvani Farsani Z, Pahlevan Kakhki M, Azimi AR. Vitamin D supplementation up-regulates IL-6 and IL-17A gene expression in multiple sclerosis patients. Int Immunopharmacol. 2015. https://doi.org/10.1016/j.intimp.2015.06.033.",
"year": "2015"
},
{
"DOI": "10.3389/fimmu.2019.00065",
"author": "N Goncalves-Mendes",
"doi-asserted-by": "publisher",
"first-page": "65",
"journal-title": "Front Immunol",
"key": "1666_CR31",
"unstructured": "Goncalves-Mendes N, Talvas J, Dualé C, Guttmann A, Corbin V, Marceau G, Sapin V, Brachet P, Evrard B, Laurichesse H, Vasson M-P. Impact of Vitamin D supplementation on influenza vaccine response and immune functions in deficient elderly persons: a randomized placebo-controlled trial. Front Immunol. 2019;10:65. https://doi.org/10.3389/fimmu.2019.00065.",
"volume": "10",
"year": "2019"
},
{
"DOI": "10.1080/22221751.2020.1747363",
"author": "Y Xiong",
"doi-asserted-by": "publisher",
"first-page": "761",
"journal-title": "Emerg Microbes Infect",
"key": "1666_CR32",
"unstructured": "Xiong Y, Liu Y, Cao L, Wang D, Guo M, Jiang A, Guo D, Hu W, Yang J, Tang Z, Wu H, Lin Y, Zhang M, Zhang Q, Shi M, Liu Y, Zhou Y, Lan K, Chen Y. Transcriptomic characteristics of bronchoalveolar lavage fluid and peripheral blood mononuclear cells in COVID-19 patients. Emerg Microbes Infect. 2020;9:761–70. https://doi.org/10.1080/22221751.2020.1747363.",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1101/2020.02.23.20026690",
"author": "M Liao",
"doi-asserted-by": "publisher",
"journal-title": "MedRxiv.",
"key": "1666_CR33",
"unstructured": "Liao M, Liu Y, Yuan J, Wen Y, Xu G, Zhao J, Chen L, Li J, Wang X, Wang F, Liu L, Zhang S, Zhang Z. The landscape of lung bronchoalveolar immune cells in COVID-19 revealed by single-cell RNA sequencing. MedRxiv. 2020. https://doi.org/10.1101/2020.02.23.20026690.",
"year": "2020"
},
{
"DOI": "10.1016/j.cmi.2019.04.020",
"author": "SJCFM Moorlag",
"doi-asserted-by": "publisher",
"journal-title": "Clin Microbiol Infect.",
"key": "1666_CR34",
"unstructured": "Moorlag SJCFM, Arts RJW, van Crevel R, Netea MG. Non-specific effects of BCG vaccine on viral infections. Clin Microbiol Infect. 2019. https://doi.org/10.1016/j.cmi.2019.04.020.",
"year": "2019"
},
{
"key": "1666_CR35",
"unstructured": "Connecting BCG Vaccination and COVID-19: Additional Data | medRxiv, (n.d.). https://www.medrxiv.org/content/10.1101/2020.04.07.20053272v2. Accessed 16 Jan 2021."
},
{
"DOI": "10.1038/s41598-020-75491-x",
"author": "J Hensel",
"doi-asserted-by": "publisher",
"first-page": "18377",
"journal-title": "Sci Rep",
"key": "1666_CR36",
"unstructured": "Hensel J, McAndrews KM, McGrail DJ, Dowlatshahi DP, LeBleu VS, Kalluri R. Protection against SARS-CoV-2 by BCG vaccination is not supported by epidemiological analyses. Sci Rep. 2020;10:18377. https://doi.org/10.1038/s41598-020-75491-x.",
"volume": "10",
"year": "2020"
}
],
"reference-count": 36,
"references-count": 36,
"relation": {},
"resource": {
"primary": {
"URL": "https://respiratory-research.biomedcentral.com/articles/10.1186/s12931-021-01666-3"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subtitle": [],
"title": "Circulating Vitamin D levels status and clinical prognostic indices in COVID-19 patients",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "22"
}
