Clinical Characteristics and Comorbidities associated with SARS-CoV-2 breakthrough infection in the University of California Healthcare Systems
et al., The American Journal of the Medical Sciences, doi:10.1016/j.amjms.2023.04.019, May 2023
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
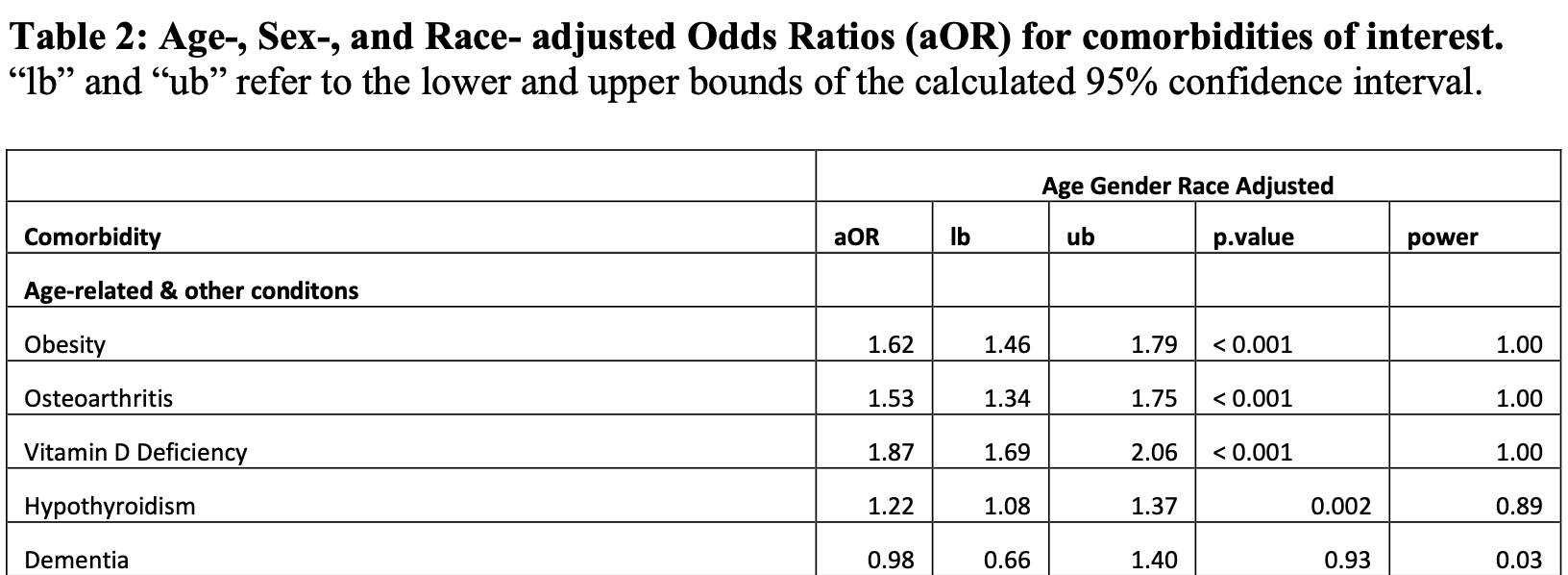
Retrospective 110,380 patients in the USA, showing higher risk of COVID-19 breakthrough cases with vitamin D deficiency.
Authors note that "lockdown measures pose an increased risk for individuals to develop vitamin D deficiency".
This paper was delayed by peer review >10 months.
This is the 179th of 232 COVID-19 sufficiency studies for vitamin D, which collectively show higher levels reduce risk with p<0.0000000001.
Standard of Care (SOC) for COVID-19 in the study country,
the USA, is very poor with very low average efficacy for approved treatments1.
Only expensive, high-profit treatments were approved for early treatment. Low-cost treatments were excluded, reducing the probability of early treatment due to access and cost barriers, and eliminating complementary and synergistic benefits seen with many low-cost treatments.
|
risk of case, 46.5% lower, OR 0.53, p < 0.001, high D levels (≥20ng/mL) 96,894, low D levels (<20ng/mL) 13,486, adjusted per study, inverted to make OR<1 favor high D levels (≥20ng/mL), breakthrough case, multivariable, RR approximated with OR.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Hogarth et al., 3 May 2023, retrospective, USA, peer-reviewed, median age 56.0, 9 authors, study period 1 January, 2021 - 8 November, 2021.
Contact: rongkeko@health.ucsd.edu (corresponding author).
Clinical characteristics and comorbidities associated with SARS-CoV-2 breakthrough infection in the University of California Healthcare Systems
The American Journal of the Medical Sciences, doi:10.1016/j.amjms.2023.04.019
This is a PDF file of an article that has undergone enhancements after acceptance, such as the addition of a cover page and metadata, and formatting for readability, but it is not yet the definitive version of record. This version will undergo additional copyediting, typesetting and review before it is published in its final form, but we are providing this version to give early visibility of the article. Please note that, during the production process, errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Conflicts of Interest The authors declare no conflict of interest.
Role of Funder/Sponsor The funding sources had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Additional Contributions: The authors thank the Center for Data-driven Insights and Innovation at UC Health (CDI2; https://www.ucop.edu/uc-health/functions/center-for-data-driveninsights-and-innovations-cdi2.html), for its analytical and technical support related to use of the UC Health Data Warehouse and related data assets, including the UC COVID Research Data Set (CORDS). Figure Legend
References
Antos, Kwong, Balmorez, Villanueva, Murakami, Unusually High Risks of COVID-19 Mortality with Age-Related Comorbidities: An Adjusted Meta-Analysis Method to Improve the Risk Assessment of Mortality Using the Comorbid Mortality Data, Infect Dis Rep, doi:10.3390/idr13030065
Bajaj, Gadi, Spihlman, Wu, Choi et al., Aging, Immunity, and COVID-19: How Age Influences the Host Immune Response to Coronavirus Infections?, Front Physiol, doi:10.3389/fphys.2020.571416
Bernal, Andrews, Gower, Effectiveness of Covid-19 Vaccines against the B.1.617.2 (Delta) Variant, N Engl J Med, doi:10.1056/NEJMoa2108891
Castillo, Costa, Barrios, Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study, J Steroid Biochem Mol Biol. Oct, doi:10.1016/j.jsbmb.2020.105751
Cfd, Risk for COVID-19 infection, hospitalization, and death by age group, Centers for Disease Control and Prevention
Chemaitelly, Tang, Hasan, Waning of BNT162b2 Vaccine Protection against SARS-CoV-2 Infection in Qatar, N Engl J Med, doi:10.1056/NEJMoa2114114
Cowling, Ng, Ip, Community psychological and behavioral responses through the first wave of the 2009 influenza A(H1N1) pandemic in Hong Kong, J Infect Dis. Sep, doi:10.1086/655811
Dupont, Power calculations for matched case-control studies, Biometrics. Dec
Flythe, Assimon, Tugman, Characteristics and Outcomes of Individuals With Pre-existing Kidney Disease and COVID-19 Admitted to Intensive Care Units in the United States, Am J Kidney Dis, doi:10.1053/j.ajkd.2020.09.003
Gallagher, Vitamin D and aging, Endocrinol Metab Clin North Am, doi:10.1016/j.ecl.2013.02.004
Goicoechea, Cámara, Macías, COVID-19: clinical course and outcomes of 36 hemodialysis patients in Spain, Kidney Int, doi:10.1016/j.kint.2020.04.031
Goldberg, Mandel, Bar-On, Waning immunity after the BNT162b2 vaccine in Israel
Hossein-Nezhad, Holick, Vitamin D for health: a global perspective, Mayo Clin Proc. Jul, doi:10.1016/j.mayocp.2013.05.011
Jonathan, Thomas, Gregory, Bojana, The regulation of ACE-2 in the heart and lungs. The Southwest Respiratory and Critical Care, doi:10.12746/swrccc.v9i40.895
Khan, Khan, Mustagir, Rana, Islam et al., Effects of underlying morbidities on the occurrence of deaths in COVID-19 patients: A systematic review and metaanalysis, J Glob Health. Dec, doi:10.7189/jogh.10.020503
Kim, Crimmins, How does age affect personal and social reactions to COVID-19: Results from the national Understanding America Study, PLoS One, doi:10.1371/journal.pone.0241950
Kompaniyets, Agathis, Nelson, Underlying Medical Conditions Associated With Severe COVID-19 Illness Among Children, JAMA Netw Open, doi:10.1001/jamanetworkopen.2021.11182
Lab, Self-reported compliance and attitudes about social distancing during the COVID-19 outbreak
Lerner, Klein, Hardesty, Panagiotou, Misquith et al., Comparison of COVID-19 outcomes in organ transplant recipients (OTr) and non-transplant patients: a study protocol for rapid review. Syst Rev, doi:10.1186/s13643-021-01854-8
Lin, Savoia, Agboola, Viswanath, What have we learned about communication inequalities during the H1N1 pandemic: a systematic review of the literature, doi:10.1186/1471-2458-14-484
Lips, Vitamin D deficiency and secondary hyperparathyroidism in the elderly: consequences for bone loss and fractures and therapeutic implications, Endocr Rev. Aug, doi:10.1210/edrv.22.4.0437
Maghbooli, Sahraian, Ebrahimi, Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection, PLoS One, doi:10.1371/journal.pone.0239799
Meehan, Penckofer, The Role of Vitamin D in the Aging Adult, J Aging Gerontol. Dec, doi:10.12974/2309-6128.2014.02.02.1
Moline, Whitaker, Deng, Effectiveness of COVID-19 Vaccines in Preventing Hospitalization Among Adults Aged ≥65 Years -COVID-NET, 13 States, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm7032e3
Naaber, Tserel, Kangro, Dynamics of antibody response to BNT162b2 vaccine after six months: a longitudinal prospective study, Lancet Reg Health Eur. Nov, doi:10.1016/j.lanepe.2021.100208
Ni, Yang, Yang, Role of angiotensin-converting enzyme 2 (ACE2) in COVID-19, Crit Care, doi:10.1186/s13054-020-03120-0
Pilishvili, Gierke, Ke, Effectiveness of mRNA Covid-19 Vaccine among U.S. Health Care Personnel, N Engl J Med, doi:10.1056/NEJMoa2106599
Polack, Thomas, Kitchin, Safety and Efficacy of the BNT162b2 mRNA Covid-19 Vaccine, N Engl J Med, doi:10.1056/NEJMoa2034577
Puranik, Lenehan, Silvert, Comparison of two highly-effective mRNA vaccines for COVID-19 during periods of Alpha and Delta variant prevalence. medRxiv, doi:10.1101/2021.08.06.21261707
Rentsch, Kidwai-Khan, Tate, Covid-19 by Race and Ethnicity: A National Cohort Study of 6 Million United States Veterans. medRxiv
Rosenberg, Dorabawila, Easton, COVID-19 vaccine effectiveness in New York state
Saraff, Sunshine, Arch Dis Child, doi:10.1136/archdischild-2014-307214<216
Schmidt, Labaki, Hsu, COVID-19 vaccination and breakthrough infections in patients with cancer, Ann Oncol, doi:10.1016/j.annonc.2021.12.006
Self, Tenforde, Rhoads, Comparative Effectiveness of Moderna, Pfizer-BioNTech, and Janssen (Johnson & Johnson) Vaccines in Preventing COVID-19 Hospitalizations Among Adults Without Immunocompromising Conditions -United States, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm7038e1
Sharma, Oda, Holodniy, COVID-19 Vaccine Breakthrough Infections in Veterans Health Administration, doi:10.1101/2021.09.23.21263864
Sheikh, Robertson, Taylor, BNT162b2 and ChAdOx1 nCoV-19 Vaccine Effectiveness against Death from the Delta Variant, N Engl J Med, doi:10.1056/NEJMc2113864
Stahl, Brown, None, Cell Therapy Strategies to Combat Immunosenescence
Sun, Zheng, Madhira, Association Between Immune Dysfunction and COVID-19 Breakthrough Infection After SARS-CoV-2 Vaccination in the US, JAMA Intern Med, doi:10.1001/jamainternmed.2021.7024
Tartof, Slezak, Fischer, Effectiveness of mRNA BNT162b2 COVID-19 vaccine up to 6 months in a large integrated health system in the USA: a retrospective cohort study, Lancet, doi:10.1016/s0140-6736(21)02183-8
Tenforde, Self, Adams, Association Between mRNA Vaccination and COVID-19 Hospitalization and Disease Severity, Jama, doi:10.1001/jama.2021.19499
Von Elm, Altman, Egger, Pocock, Gøtzsche et al., The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies, J Clin Epidemiol. Apr, doi:10.1016/j.jclinepi.2007.11.008
Wang, Berger, Xu, Risks of SARS-CoV-2 Breakthrough Infection and Hospitalization in Fully Vaccinated Patients With Multiple Myeloma, JAMA Netw Open, doi:10.1001/jamanetworkopen.2021.37575
Williamson, Walker, Bhaskaran, Factors associated with COVID-19-related death using OpenSAFELY, Nature. Aug, doi:10.1038/s41586-020-2521-
Wilson, Sharma, Schluechtermann, Factors influencing risk for COVID-19 exposure among young adults aged 18-23 years, Morbidity and Mortality Weekly Report
Woodward, Epidemiology: study design and data analysis, Centers for Disease Control and Prevention. COVID Data Tracker
Wu, Chen, Cai, Risk Factors Associated With Acute Respiratory Distress Syndrome and Death in Patients With Coronavirus Disease, JAMA Intern Med, doi:10.1001/jamainternmed.2020.0994
Yilmazkuday, COVID-19 and Unequal Social Distancing across Demographic Groups, doi:10.1111/rsp3.12329
DOI record:
{
"DOI": "10.1016/j.amjms.2023.04.019",
"ISSN": [
"0002-9629"
],
"URL": "http://dx.doi.org/10.1016/j.amjms.2023.04.019",
"alternative-id": [
"S0002962923011667"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Clinical Characteristics and Comorbidities associated with SARS-CoV-2 breakthrough infection in the University of California Healthcare Systems"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "The American Journal of the Medical Sciences"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.amjms.2023.04.019"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2023 Published by Elsevier Inc. on behalf of Southern Society for Clinical Investigation."
}
],
"author": [
{
"affiliation": [],
"family": "Hogarth",
"given": "Michael",
"sequence": "first"
},
{
"affiliation": [],
"family": "John",
"given": "Daniel",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Li",
"given": "Yuxiang",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wang-Rodriguez",
"given": "Jessica",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Chakladar",
"given": "Jaideep",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Li",
"given": "Wei Tse",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mehta",
"given": "Sanjay R.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jain",
"given": "Sharad",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ongkeko",
"given": "Weg M.",
"sequence": "additional"
}
],
"container-title": "The American Journal of the Medical Sciences",
"container-title-short": "The American Journal of the Medical Sciences",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"clinicalkey.fr",
"clinicalkey.jp",
"clinicalkey.com.au",
"clinicalkey.es",
"amjmedsci.org",
"clinicalkey.com",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2023,
5,
3
]
],
"date-time": "2023-05-03T17:13:36Z",
"timestamp": 1683134016000
},
"deposited": {
"date-parts": [
[
2023,
5,
6
]
],
"date-time": "2023-05-06T06:15:36Z",
"timestamp": 1683353736000
},
"indexed": {
"date-parts": [
[
2023,
5,
7
]
],
"date-time": "2023-05-07T04:23:24Z",
"timestamp": 1683433404913
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2023,
5
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
5,
1
]
],
"date-time": "2023-05-01T00:00:00Z",
"timestamp": 1682899200000
}
},
{
"URL": "http://creativecommons.org/licenses/by-nc-nd/4.0/",
"content-version": "vor",
"delay-in-days": 4,
"start": {
"date-parts": [
[
2023,
5,
5
]
],
"date-time": "2023-05-05T00:00:00Z",
"timestamp": 1683244800000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S0002962923011667?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S0002962923011667?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"prefix": "10.1016",
"published": {
"date-parts": [
[
2023,
5
]
]
},
"published-print": {
"date-parts": [
[
2023,
5
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1056/NEJMoa2034577",
"article-title": "Safety and Efficacy of the BNT162b2 mRNA Covid-19 Vaccine",
"author": "Polack",
"doi-asserted-by": "crossref",
"first-page": "2603",
"issue": "27",
"journal-title": "N Engl J Med",
"key": "10.1016/j.amjms.2023.04.019_bib0001",
"volume": "383",
"year": "2020"
},
{
"DOI": "10.1056/NEJMoa2106599",
"article-title": "Effectiveness of mRNA Covid-19 Vaccine among U.S. Health Care Personnel",
"author": "Pilishvili",
"doi-asserted-by": "crossref",
"first-page": "e90",
"issue": "25",
"journal-title": "N Engl J Med",
"key": "10.1016/j.amjms.2023.04.019_bib0002",
"volume": "385",
"year": "2021"
},
{
"DOI": "10.15585/mmwr.mm7038e1",
"article-title": "Comparative Effectiveness of Moderna, Pfizer-BioNTech, and Janssen (Johnson & Johnson) Vaccines in Preventing COVID-19 Hospitalizations Among Adults Without Immunocompromising Conditions - United States, March-August 2021",
"author": "Self",
"doi-asserted-by": "crossref",
"first-page": "1337",
"issue": "38",
"journal-title": "MMWR Morb Mortal Wkly Rep.",
"key": "10.1016/j.amjms.2023.04.019_bib0003",
"volume": "70",
"year": "2021"
},
{
"DOI": "10.15585/mmwr.mm7032e3",
"article-title": "Effectiveness of COVID-19 Vaccines in Preventing Hospitalization Among Adults Aged ≥65 Years - COVID-NET, 13 States, February-April 2021",
"author": "Moline",
"doi-asserted-by": "crossref",
"first-page": "1088",
"issue": "32",
"journal-title": "MMWR Morb Mortal Wkly Rep.",
"key": "10.1016/j.amjms.2023.04.019_bib0004",
"volume": "70",
"year": "2021"
},
{
"DOI": "10.1056/NEJMc2113864",
"article-title": "BNT162b2 and ChAdOx1 nCoV-19 Vaccine Effectiveness against Death from the Delta Variant",
"author": "Sheikh",
"doi-asserted-by": "crossref",
"first-page": "2195",
"issue": "23",
"journal-title": "N Engl J Med",
"key": "10.1016/j.amjms.2023.04.019_bib0005",
"volume": "385",
"year": "2021"
},
{
"DOI": "10.1001/jama.2021.19499",
"article-title": "Association Between mRNA Vaccination and COVID-19 Hospitalization and Disease Severity",
"author": "Tenforde",
"doi-asserted-by": "crossref",
"first-page": "2043",
"issue": "20",
"journal-title": "Jama",
"key": "10.1016/j.amjms.2023.04.019_bib0006",
"volume": "326",
"year": "2021"
},
{
"DOI": "10.1056/NEJMoa2114114",
"article-title": "Waning of BNT162b2 Vaccine Protection against SARS-CoV-2 Infection in Qatar",
"author": "Chemaitelly",
"doi-asserted-by": "crossref",
"first-page": "e83",
"issue": "24",
"journal-title": "N Engl J Med",
"key": "10.1016/j.amjms.2023.04.019_bib0007",
"volume": "385",
"year": "2021"
},
{
"article-title": "Comparison of two highly-effective mRNA vaccines for COVID-19 during periods of Alpha and Delta variant prevalence",
"author": "Puranik",
"journal-title": "medRxiv",
"key": "10.1016/j.amjms.2023.04.019_bib0008",
"year": "2021"
},
{
"DOI": "10.1056/NEJMoa2116063",
"article-title": "COVID-19 vaccine effectiveness in New York state",
"author": "Rosenberg",
"doi-asserted-by": "crossref",
"first-page": "116",
"issue": "2",
"journal-title": "New England Journal of Medicine",
"key": "10.1016/j.amjms.2023.04.019_bib0009",
"volume": "386",
"year": "2022"
},
{
"DOI": "10.1016/S0140-6736(21)02183-8",
"article-title": "Effectiveness of mRNA BNT162b2 COVID-19 vaccine up to 6 months in a large integrated health system in the USA: a retrospective cohort study",
"author": "Tartof",
"doi-asserted-by": "crossref",
"first-page": "1407",
"issue": "10309",
"journal-title": "Lancet",
"key": "10.1016/j.amjms.2023.04.019_bib0010",
"volume": "398",
"year": "2021"
},
{
"article-title": "Dynamics of antibody response to BNT162b2 vaccine after six months: a longitudinal prospective study",
"author": "Naaber",
"journal-title": "Lancet Reg Health Eur.",
"key": "10.1016/j.amjms.2023.04.019_bib0011",
"volume": "10",
"year": "2021"
},
{
"DOI": "10.3390/idr13030065",
"article-title": "Unusually High Risks of COVID-19 Mortality with Age-Related Comorbidities: An Adjusted Meta-Analysis Method to Improve the Risk Assessment of Mortality Using the Comorbid Mortality Data",
"author": "Antos",
"doi-asserted-by": "crossref",
"first-page": "700",
"issue": "3",
"journal-title": "Infect Dis Rep",
"key": "10.1016/j.amjms.2023.04.019_bib0012",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1001/jamanetworkopen.2021.11182",
"article-title": "Underlying Medical Conditions Associated With Severe COVID-19 Illness Among Children",
"author": "Kompaniyets",
"doi-asserted-by": "crossref",
"issue": "6",
"journal-title": "JAMA Netw Open",
"key": "10.1016/j.amjms.2023.04.019_bib0013",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.1056/NEJMoa2108891",
"article-title": "Effectiveness of Covid-19 Vaccines against the B.1.617.2 (Delta) Variant",
"author": "Lopez Bernal",
"doi-asserted-by": "crossref",
"first-page": "585",
"issue": "7",
"journal-title": "N Engl J Med",
"key": "10.1016/j.amjms.2023.04.019_bib0014",
"volume": "385",
"year": "2021"
},
{
"DOI": "10.1056/NEJMoa2114228",
"article-title": "Waning immunity after the BNT162b2 vaccine in Israel",
"author": "Goldberg",
"doi-asserted-by": "crossref",
"first-page": "e85",
"issue": "24",
"journal-title": "New England Journal of Medicine",
"key": "10.1016/j.amjms.2023.04.019_bib0015",
"volume": "385",
"year": "2021"
},
{
"article-title": "COVID-19 Vaccine Breakthrough Infections in Veterans Health Administration",
"author": "Sharma",
"journal-title": "medRxiv",
"key": "10.1016/j.amjms.2023.04.019_bib0016",
"year": "2021"
},
{
"key": "10.1016/j.amjms.2023.04.019_bib0017",
"unstructured": "Rentsch CT, Kidwai-Khan F, Tate JP, et al. Covid-19 by Race and Ethnicity: A National Cohort Study of 6 Million United States Veterans. medRxiv. May 18"
},
{
"DOI": "10.1001/jamainternmed.2021.7024",
"article-title": "Association Between Immune Dysfunction and COVID-19 Breakthrough Infection After SARS-CoV-2 Vaccination in the US",
"author": "Sun",
"doi-asserted-by": "crossref",
"first-page": "153",
"issue": "2",
"journal-title": "JAMA Intern Med",
"key": "10.1016/j.amjms.2023.04.019_bib0018",
"volume": "182",
"year": "2022"
},
{
"DOI": "10.1016/j.annonc.2021.12.006",
"article-title": "COVID-19 vaccination and breakthrough infections in patients with cancer",
"author": "Schmidt",
"doi-asserted-by": "crossref",
"first-page": "340",
"issue": "3",
"journal-title": "Ann Oncol",
"key": "10.1016/j.amjms.2023.04.019_bib0019",
"volume": "33",
"year": "2022"
},
{
"DOI": "10.1001/jamanetworkopen.2021.37575",
"article-title": "Risks of SARS-CoV-2 Breakthrough Infection and Hospitalization in Fully Vaccinated Patients With Multiple Myeloma",
"author": "Wang",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "JAMA Netw Open",
"key": "10.1016/j.amjms.2023.04.019_bib0020",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.1016/j.jclinepi.2007.11.008",
"article-title": "The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies",
"author": "von Elm",
"doi-asserted-by": "crossref",
"first-page": "344",
"issue": "4",
"journal-title": "J Clin Epidemiol",
"key": "10.1016/j.amjms.2023.04.019_bib0021",
"volume": "61",
"year": "2008"
},
{
"DOI": "10.2307/2531743",
"article-title": "Power calculations for matched case-control studies",
"author": "Dupont",
"doi-asserted-by": "crossref",
"first-page": "1157",
"issue": "4",
"journal-title": "Biometrics",
"key": "10.1016/j.amjms.2023.04.019_bib0022",
"volume": "44",
"year": "1988"
},
{
"author": "Woodward",
"first-page": "24",
"key": "10.1016/j.amjms.2023.04.019_bib0023",
"series-title": "Epidemiology: study design and data analysis",
"year": "2013"
},
{
"key": "10.1016/j.amjms.2023.04.019_bib0024",
"unstructured": "Centers for Disease Control and Prevention. COVID Data Tracker. Atlanta, GA: US Department of Health and Human Services, CDC; 2022, December 20. https://covid.cdc.gov/covid-data-tracker"
},
{
"DOI": "10.7189/jogh.10.020503",
"article-title": "Effects of underlying morbidities on the occurrence of deaths in COVID-19 patients: A systematic review and meta-analysis",
"author": "Khan",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "J Glob Health",
"key": "10.1016/j.amjms.2023.04.019_bib0025",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1038/s41586-020-2521-4",
"article-title": "Factors associated with COVID-19-related death using OpenSAFELY",
"author": "Williamson",
"doi-asserted-by": "crossref",
"first-page": "430",
"issue": "7821",
"journal-title": "Nature",
"key": "10.1016/j.amjms.2023.04.019_bib0026",
"volume": "584",
"year": "2020"
},
{
"DOI": "10.1001/jamainternmed.2020.0994",
"article-title": "Risk Factors Associated With Acute Respiratory Distress Syndrome and Death in Patients With Coronavirus Disease 2019 Pneumonia in Wuhan, China",
"author": "Wu",
"doi-asserted-by": "crossref",
"first-page": "934",
"issue": "7",
"journal-title": "JAMA Intern Med",
"key": "10.1016/j.amjms.2023.04.019_bib0027",
"volume": "180",
"year": "2020"
},
{
"DOI": "10.1016/j.kint.2020.04.031",
"article-title": "COVID-19: clinical course and outcomes of 36 hemodialysis patients in Spain",
"author": "Goicoechea",
"doi-asserted-by": "crossref",
"first-page": "27",
"issue": "1",
"journal-title": "Kidney Int",
"key": "10.1016/j.amjms.2023.04.019_bib0028",
"volume": "98",
"year": "2020"
},
{
"DOI": "10.1053/j.ajkd.2020.09.003",
"article-title": "Characteristics and Outcomes of Individuals With Pre-existing Kidney Disease and COVID-19 Admitted to Intensive Care Units in the United States",
"author": "Flythe",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "Am J Kidney Dis",
"key": "10.1016/j.amjms.2023.04.019_bib0029",
"volume": "77",
"year": "2021"
},
{
"DOI": "10.1186/s13643-021-01854-8",
"article-title": "Comparison of COVID-19 outcomes in organ transplant recipients (OTr) and non-transplant patients: a study protocol for rapid review",
"author": "Lerner",
"doi-asserted-by": "crossref",
"first-page": "299",
"issue": "1",
"journal-title": "Syst Rev.",
"key": "10.1016/j.amjms.2023.04.019_bib0030",
"volume": "10",
"year": "2021"
},
{
"DOI": "10.1186/s13054-020-03120-0",
"article-title": "Role of angiotensin-converting enzyme 2 (ACE2) in COVID-19",
"author": "Ni",
"doi-asserted-by": "crossref",
"first-page": "422",
"issue": "1",
"journal-title": "Crit Care.",
"key": "10.1016/j.amjms.2023.04.019_bib0031",
"volume": "24",
"year": "2020"
},
{
"article-title": "The regulation of ACE-2 in the heart and lungs",
"author": "Jonathan",
"key": "10.1016/j.amjms.2023.04.019_bib0032",
"volume": "9",
"year": "2021"
},
{
"article-title": "Prevention",
"key": "10.1016/j.amjms.2023.04.019_bib0033",
"series-title": "Risk for COVID-19 infection, hospitalization, and death by age group",
"year": "2021"
},
{
"key": "10.1016/j.amjms.2023.04.019_bib0034",
"unstructured": "Provisional COVID-19 Deaths by Sex and Age. https://data.cdc.gov/NCHS/Provisional-COVID-19-Deaths-by-Sex-and-Age/9bhg-hcku"
},
{
"article-title": "Aging, Immunity, and COVID-19: How Age Influences the Host Immune Response to Coronavirus Infections?",
"author": "Bajaj",
"journal-title": "Front Physiol",
"key": "10.1016/j.amjms.2023.04.019_bib0035",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1080/15476278.2015.1120046",
"article-title": "Cell Therapy Strategies to Combat Immunosenescence",
"author": "Stahl",
"doi-asserted-by": "crossref",
"first-page": "159",
"issue": "4",
"journal-title": "Organogenesis",
"key": "10.1016/j.amjms.2023.04.019_bib0036",
"volume": "11",
"year": "2015"
},
{
"DOI": "10.1371/journal.pone.0241950",
"article-title": "How does age affect personal and social reactions to COVID-19: Results from the national Understanding America Study",
"author": "Kim",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "PLoS One",
"key": "10.1016/j.amjms.2023.04.019_bib0037",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.15585/mmwr.mm6941e2",
"article-title": "Factors influencing risk for COVID-19 exposure among young adults aged 18–23 years—Winnebago County, Wisconsin, March–July 2020",
"author": "Wilson",
"doi-asserted-by": "crossref",
"first-page": "1497",
"issue": "41",
"journal-title": "Morbidity and Mortality Weekly Report",
"key": "10.1016/j.amjms.2023.04.019_bib0038",
"volume": "69",
"year": "2020"
},
{
"DOI": "10.1086/655811",
"article-title": "Community psychological and behavioral responses through the first wave of the 2009 influenza A(H1N1) pandemic in Hong Kong",
"author": "Cowling",
"doi-asserted-by": "crossref",
"first-page": "867",
"issue": "6",
"journal-title": "J Infect Dis",
"key": "10.1016/j.amjms.2023.04.019_bib0039",
"volume": "202",
"year": "2010"
},
{
"DOI": "10.1186/1471-2458-14-484",
"article-title": "What have we learned about communication inequalities during the H1N1 pandemic: a systematic review of the literature",
"author": "Lin",
"doi-asserted-by": "crossref",
"first-page": "484",
"journal-title": "BMC Public Health",
"key": "10.1016/j.amjms.2023.04.019_bib0040",
"volume": "14",
"year": "2014"
},
{
"DOI": "10.31219/osf.io/bv28d",
"doi-asserted-by": "crossref",
"key": "10.1016/j.amjms.2023.04.019_bib0041",
"unstructured": "Lab B.Self-reported compliance and attitudes about social distancing during the COVID-19 outbreak. 2020."
},
{
"DOI": "10.2139/ssrn.3580302",
"doi-asserted-by": "crossref",
"key": "10.1016/j.amjms.2023.04.019_bib0042",
"unstructured": "Yilmazkuday H. COVID-19 and Unequal Social Distancing across Demographic Groups. Aug 18 2020;doi:10.1111/rsp3.12329"
},
{
"DOI": "10.1016/j.mayocp.2013.05.011",
"article-title": "Vitamin D for health: a global perspective",
"author": "Hossein-nezhad",
"doi-asserted-by": "crossref",
"first-page": "720",
"issue": "7",
"journal-title": "Mayo Clin Proc",
"key": "10.1016/j.amjms.2023.04.019_bib0043",
"volume": "88",
"year": "2013"
},
{
"DOI": "10.1016/j.ecl.2013.02.004",
"article-title": "Vitamin D and aging",
"author": "Gallagher",
"doi-asserted-by": "crossref",
"first-page": "319",
"issue": "2",
"journal-title": "Endocrinol Metab Clin North Am",
"key": "10.1016/j.amjms.2023.04.019_bib0044",
"volume": "42",
"year": "2013"
},
{
"DOI": "10.1210/edrv.22.4.0437",
"article-title": "Vitamin D deficiency and secondary hyperparathyroidism in the elderly: consequences for bone loss and fractures and therapeutic implications",
"author": "Lips",
"doi-asserted-by": "crossref",
"first-page": "477",
"issue": "4",
"journal-title": "Endocr Rev.",
"key": "10.1016/j.amjms.2023.04.019_bib0045",
"volume": "22",
"year": "2001"
},
{
"DOI": "10.12974/2309-6128.2014.02.02.1",
"article-title": "The Role of Vitamin D in the Aging Adult",
"author": "Meehan",
"doi-asserted-by": "crossref",
"first-page": "60",
"issue": "2",
"journal-title": "J Aging Gerontol",
"key": "10.1016/j.amjms.2023.04.019_bib0046",
"volume": "2",
"year": "2014"
},
{
"DOI": "10.1016/j.jsbmb.2020.105751",
"article-title": "Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study",
"author": "Entrenas Castillo",
"doi-asserted-by": "crossref",
"journal-title": "J Steroid Biochem Mol Biol",
"key": "10.1016/j.amjms.2023.04.019_bib0047",
"volume": "203",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0239799",
"article-title": "Vitamin D sufficiency, a serum 25-hydroxyvitamin D at least 30 ng/mL reduced risk for adverse clinical outcomes in patients with COVID-19 infection",
"author": "Maghbooli",
"doi-asserted-by": "crossref",
"issue": "9",
"journal-title": "PLoS One",
"key": "10.1016/j.amjms.2023.04.019_bib0048",
"volume": "15",
"year": "2020"
},
{
"DOI": "10.1136/archdischild-2014-307214",
"article-title": "Sunshine and vitamin D",
"author": "Saraff",
"doi-asserted-by": "crossref",
"first-page": "190",
"issue": "2",
"journal-title": "Arch Dis Child.",
"key": "10.1016/j.amjms.2023.04.019_bib0049",
"volume": "101",
"year": "2016"
}
],
"reference-count": 49,
"references-count": 49,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S0002962923011667"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Clinical Characteristics and Comorbidities associated with SARS-CoV-2 breakthrough infection in the University of California Healthcare Systems",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy"
}
