Impact of ultra-processed food intake on the risk of COVID-19: a prospective cohort study
et al., European Journal of Nutrition, doi:10.1007/s00394-022-02982-0, Aug 2022
Diet for COVID-19
26th treatment shown to reduce risk in
June 2021, now with p < 0.00000000001 from 30 studies, recognized in 4 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 41,012 UK Biobank participants, showing higher risk of COVID-19 cases with ultra-processed food consumption.
Standard of Care (SOC) for COVID-19 in the study country,
the United Kingdom, is very poor with very low average efficacy for approved treatments1.
The United Kingdom focused on expensive high-profit treatments, approving only one low-cost early treatment, which required a prescription and had limited adoption. The high-cost prescription treatment strategy reduces the probability of early treatment due to access and cost barriers, and eliminates complementary and synergistic benefits seen with many low-cost treatments.
|
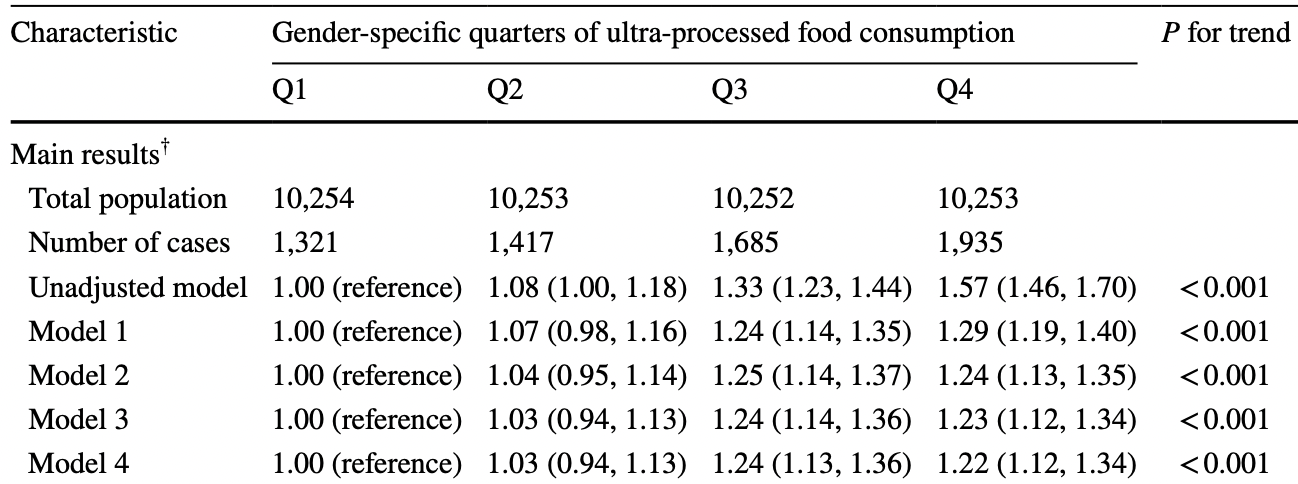
risk of case, 15.7% lower, RR 0.84, p < 0.001, higher quality diet 1,321 of 10,254 (12.9%), lower quality diet 1,935 of 10,253 (18.9%), inverted to make RR<1 favor higher quality diet, odds ratio converted to relative risk, Q4 vs. Q1, model 3 (before healthy diet score adjustment).
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Zhou et al., 16 Aug 2022, prospective, United Kingdom, peer-reviewed, 6 authors.
Contact: yaogangwang@tmu.edu.cn.
Impact of ultra-processed food intake on the risk of COVID-19: a prospective cohort study
European Journal of Nutrition, doi:10.1007/s00394-022-02982-0
Purpose Nutrition plays a key role in supporting the human immune system and reducing the risk of infections. However, there is limited evidence exploring the relationship between diet and the risk of COVID-19. This study aimed to assess the associations between consumption of ultra-processed foods (UPF) and COVID-19 risk. Methods In total, 41,012 participants from the UK Biobank study with at least 2 of up to 5 times 24-h dietary assessments were included in this study. Dietary intakes were collected using an online 24-h dietary recall questionnaire and food items were categorized according to their degree of processing by the NOVA classification. COVID-19 infection was defined as individuals tested COVID-19 positive or dead of COVID-19. Association between average UPF consumption (% daily gram intake) and COVID-19 infection was assessed by multivariable logistic regression adjusted for potential confounders. Results Compared to participants in the lowest quartile of UPF proportion (% daily gram intake) in the diet, participants in the 2nd, 3rd, and highest quartiles were associated with a higher risk of COVID-19 with the odds ratio (OR) value of 1.03 (95% CI: 0.94-1.13), 1.24 (95% CI: 1.13-1.36), and 1.22 (95% CI: 1.12-1.34), respectively (P for trend < 0.001), after adjusting for potential confounders. The results were robust in a series of sensitivity analyses. No interaction effect was identified between the UPF proportions and age groups, education level, body mass index, and comorbidity status. BMI mediated 13.2% of this association. Conclusion Higher consumption of UPF was associated with an increased risk of COVID-19 infection. Further studies are needed to better understand the underlying mechanisms in such association.
Supplementary Information The online version contains supplementary material available at https:// doi. org/ 10. 1007/ s00394-022-02982-0. Author contributions LZ and HL designed the study and drafted the statistical analysis plan. LZ compiled the data, did the statistical analysis, interpreted the data, and drafted the manuscript. HL and SZ interpreted the data, and critically revised the manuscript. HY critically revised the manuscript. YM compiled the data. YW conceived the study, critically revised the manuscript, and acquired the data and funding. All authors gave final approval and agree to be accountable for all aspects of the work ensuring integrity and accuracy. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted. Funding This study was funded by the National Natural Science Foundation of China (No. 71910107004, 91746205). The funding sources had no role in the design, execution, analyses, and interpretation of the data or decision to submit the results of this study.
Declarations Conflict of interest The authors declare that there is no conflicts of interest.
Ethical approval The ethical approvals of UK Biobank were obtained from the North West Multi-Centre Research Ethics Committee, as a Research Tissue Bank (RTB) approval. This study was approved under the UK Biobank application number 45676. Consent to participate Informed consent was obtained from all individual..
References
Armstrong, Rudkin, Allen, Dynamic linkage of COVID-19 test results between public health England's second generation surveillance system and UK Biobank, Microbial genomics, doi:10.1099/mgen.0.000397
Bandt, Monin, Obesity, nutrients and the immune system in the era of COVID-19, Nutrients, doi:10.3390/nu13020610
Belanger, Hill, Angelidi, Dalamaga, Sowers et al., Covid-19 and disparities in nutrition and obesity, N Engl J Med, doi:10.1056/NEJMp2021264
Beslay, Srour, Mejean, Ultra-processed food intake in association with BMI change and risk of overweight and obesity: a prospective analysis of the French NutriNet-Sante cohort, Plos Med, doi:10.1371/journal.pmed.1003256
Briguglio, Pregliasco, Lombardi, Perazzo, Banfi, The malnutritional status of the host as a virulence factor for new coronavirus SARS-CoV-2, Front Med, doi:10.3389/fmed.2020.00146
Buckley, Kim, Wong, Rebholz, Ultra-processed food consumption and exposure to phthalates and bisphenols in the US National health and nutrition examination survey, 2013-2014, Environ Int, doi:10.1016/j.envint.2019.105057
Bycroft, Freeman, Petkova, Ultraprocessed food intake and all-cause and cause-specific mortality in individuals with cardiovascular disease: the Moli-sani Study, Eur Heart J, doi:10.1093/eurheartj/ehab783
Calder, Nutrition, immunity and COVID-19, BMJ Nutr Prev Health, doi:10.1136/bmjnph-2020-000085
Christ, Lauterbach, Latz, Western diet and the immune system: an inflammatory connection, Immunity, doi:10.1016/j.immuni.2019.09.020
Deschasaux-Tanguy, Srour, Bourhis, Nutritional risk factors for SARS-CoV-2 infection: a prospective study within the NutriNet-Santé cohort, BMC Med, doi:10.1186/s12916-021-02168-1
Dong, Du, Gardner, An interactive web-based dashboard to track COVID-19 in real time, Lancet Infect Dis, doi:10.1016/S1473-3099(20)30120-1
Fardet, Minimally processed foods are more satiating and less hyperglycemic than ultra-processed foods: a preliminary study with 98 ready-to-eat foods, Food Funct, doi:10.1039/c6fo00107f
Fardet, Rock, Chronic diseases are first associated with the degradation and artificialization of food matrices rather than with food composition: calorie quality matters more than calorie quantity, Eur J Nutr, doi:10.1007/s00394-021-02786-8
Fiolet, Srour, Sellem, Consumption of ultraprocessed foods and cancer risk: results from NutriNet-Sante prospective cohort, BMJ (Clinical research ed, doi:10.1136/bmj.k322
Frasca, Diaz, Romero, Blomberg, Ageing and obesity similarly impair antibody responses, Clin Exp Immunol, doi:10.1111/cei.12824
Galante, Adamska, Young, The acceptability of repeat Internet-based hybrid diet assessment of previous 24-h dietary intake: administration of the Oxford WebQ in UK Biobank, Br J Nutr, doi:10.1017/S0007114515004821
Gibney, Forde, Mullally, Gibney, Ultra-processed foods in human health: a critical appraisal, Am J Clin Nutr, doi:10.3945/ajcn.117.160440
Ha, Jung, Kim, Association between environmental factors and asthma using mendelian randomization: increased effect of body mass index on adult-onset moderate-tosevere asthma subtypes, Front Genet, doi:10.3389/fgene.2021.639905
Hall, Ayuketah, Brychta, Ultra-processed diets cause excess calorie intake and weight gain: an inpatient randomized controlled trial of ad libitum food intake, Cell Metab, doi:10.1016/j.cmet.2019.05.008
Honce, Schultz-Cherry, Impact of Obesity on Influenza A virus pathogenesis, immune response, and evolution, Front Immunol, doi:10.3389/fimmu.2019.01071
Huang, Wang, Li, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China Lancet, doi:10.1016/S0140-6736(20)30183-5
Isfahani, Emam-Djomeh, Rao, Rezaei, Nutrition and immunity in COVID-19, Adv Exp Med Biol, doi:10.1007/978-3-030-63761-3_28
Lancet Diabetes, Metabolic health: a priority for the post-pandemic era, Lancet Diabetes Endocrinol, doi:10.1016/S2213-8587(21)00058-9
Lawrence, Baker, Ultra-processed food and adverse health outcomes, BMJ, doi:10.1136/bmj.l2289
Leong, Cole, Brenner, Meigs, Florez et al., Cardiometabolic risk factors for COVID-19 susceptibility and severity: a Mendelian randomization analysis, Plos Med, doi:10.1371/journal.pmed.1003553
López-Gil, García-Hermoso, Tárraga-López, Brazo-Sayavera, Dietary patterns, adherence to the food-based dietary guidelines, and ultra-processed consumption during the COVID-19 lockdown in a sample of Spanish young population, Front Pediatr, doi:10.3389/fped.2021.702731
Merino, Joshi, Nguyen, Diet quality and risk and severity of COVID-19: a prospective cohort study, Gut, doi:10.1136/gutjnl-2021-325353
Monteiro, Cannon, Levy, Ultra-processed foods: what they are and how to identify them, Public Health Nutr, doi:10.1017/S1368980018003762
Monteiro, Cannon, Moubarac, Levy, Louzada et al., The UN Decade of nutrition, the NOVA food classification and the trouble with ultra-processing, Public Health Nutr, doi:10.1017/S1368980017000234
Moser, Galindo-Fraga, Ortiz-Hernandez, Underweight, overweight, and obesity as independent risk factors for hospitalization in adults and children from influenza and other respiratory viruses, Influenza Other Respir Viruses, doi:10.1111/irv.12618
Moubarac, Parra, Cannon, Monteiro, Food classification systems based on food processing: significance and implications for policies and actions: a systematic literature review and assessment, Curr Obes Rep, doi:10.1007/s13679-014-0092-0
Mozaffarian, Dietary and policy priorities for cardiovascular disease, diabetes, and obesity: a comprehensive review, Circulation, doi:10.1161/CIRCULATIONAHA.115.018585
Myles, Fast food fever: reviewing the impacts of the western diet on immunity, Nutr J, doi:10.1186/1475-2891-13-61
Narula, Wong, Dehghan, Association of ultra-processed food intake with risk of inflammatory bowel disease: prospective cohort study, BMJ (Clinical research ed, doi:10.1136/bmj.n1554
Pazoki, Dehghan, Evangelou, Genetic predisposition to high blood pressure and lifestyle factors: associations with midlife blood pressure levels and cardiovascular events, Circulation, doi:10.1161/circulationaha.117.030898
Perez-Cornago, Pollard, Young, Description of the updated nutrition calculation of the Oxford WebQ questionnaire and comparison with the previous version among 207,144 participants in UK Biobank, Eur J Nutr, doi:10.1007/s00394-021-02558-4
Petrakis, Margina, Tsarouhas, Obesity a risk factor for increased COVID19 prevalence, severity and lethality (Review), Mol Med Rep, doi:10.3892/mmr.2020.11127
Poti, Braga, Qin, Ultra-processed food intake and obesity: what really matters for health-processing or nutrient content?, Curr Obes Rep, doi:10.1007/s13679-017-0285-4
Rico-Campa, Martinez-Gonzalez, Alvarez-Alvarez, Association between consumption of ultra-processed foods and all cause mortality: SUN prospective cohort study, BMJ, doi:10.1136/bmj.l1949
Shi, Wang, Shao, COVID-19 infection: the perspectives on immune responses, Cell Death Differ, doi:10.1038/s41418-020-0530-3
Sideleva, Suratt, Black, Obesity and asthma: an inflammatory disease of adipose tissue not the airway, Am J Respir Crit Care Med, doi:10.1164/rccm.201203-0573OC
Singh, Khan, Clinical characteristics and outcomes of coronavirus disease 2019 among patients with preexisting liver disease in the United States: a multicenter research network study, Gastroenterology, doi:10.1053/j.gastro.2020.04.064
Srour, Fezeu, Kesse-Guyot, Ultra-processed food intake and risk of cardiovascular disease: prospective cohort study (NutriNet-Sante), BMJ, doi:10.1136/bmj.l1451
Statovci, Aguilera, Macsharry, Melgar, The impact of western diet and nutrients on the microbiota and immune response at mucosal interfaces, Front Immunol, doi:10.3389/fimmu.2017.00838
Storm, Den Hertog, Van Oers, Schuit, How to improve collaboration between the public health sector and other policy sectors to reduce health inequalities? -a study in sixteen municipalities in the Netherlands, Int J Equity Health, doi:10.1186/s12939-016-0384-y
Vu, Rydland, Achenbach, Van Horn, Cornelis, Dietary behaviors and incident COVID-19 in the UK Biobank, Nutrients, doi:10.3390/nu13062114
Wang, Zhou, Li, Baseline vitamin D status, sleep patterns, and the risk of incident Type 2 diabetes in data from the UK Biobank study, Diabetes Care, doi:10.2337/dc20-1109
Wood, Harrison, Judd, Bellis, Hughes et al., The impact of behavioural risk factors on communicable diseases: a systematic review of reviews, BMC Public Health, doi:10.1186/s12889-021-12148-y
DOI record:
{
"DOI": "10.1007/s00394-022-02982-0",
"ISSN": [
"1436-6207",
"1436-6215"
],
"URL": "http://dx.doi.org/10.1007/s00394-022-02982-0",
"alternative-id": [
"2982"
],
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "27 April 2022"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "29 July 2022"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "16 August 2022"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Conflict of interest",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "The authors declare that there is no conflicts of interest."
},
{
"group": {
"label": "Ethical approval",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "The ethical approvals of UK Biobank were obtained from the North West Multi-Centre Research Ethics Committee, as a Research Tissue Bank (RTB) approval. This study was approved under the UK Biobank application number 45676."
},
{
"group": {
"label": "Consent to participate",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 4,
"value": "Informed consent was obtained from all individual participants included in the study."
},
{
"group": {
"label": "Consent for publication",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 5,
"value": "The manuscript is approved by all authors for publication."
},
{
"label": "Free to read",
"name": "free",
"value": "This content has been made available to all."
}
],
"author": [
{
"affiliation": [],
"family": "Zhou",
"given": "Lihui",
"sequence": "first"
},
{
"affiliation": [],
"family": "Li",
"given": "Huiping",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Zhang",
"given": "Shunming",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Yang",
"given": "Hongxi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ma",
"given": "Yue",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Wang",
"given": "Yaogang",
"sequence": "additional"
}
],
"container-title": "European Journal of Nutrition",
"container-title-short": "Eur J Nutr",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2022,
8,
16
]
],
"date-time": "2022-08-16T10:02:42Z",
"timestamp": 1660644162000
},
"deposited": {
"date-parts": [
[
2022,
8,
16
]
],
"date-time": "2022-08-16T13:06:02Z",
"timestamp": 1660655162000
},
"funder": [
{
"DOI": "10.13039/501100001809",
"award": [
"71910107004",
"91746205"
],
"doi-asserted-by": "publisher",
"name": "National Natural Science Foundation of China"
}
],
"indexed": {
"date-parts": [
[
2022,
8,
16
]
],
"date-time": "2022-08-16T13:42:08Z",
"timestamp": 1660657328946
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2022,
8,
16
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.springer.com/tdm",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
8,
16
]
],
"date-time": "2022-08-16T00:00:00Z",
"timestamp": 1660608000000
}
},
{
"URL": "https://www.springer.com/tdm",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
8,
16
]
],
"date-time": "2022-08-16T00:00:00Z",
"timestamp": 1660608000000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1007/s00394-022-02982-0.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1007/s00394-022-02982-0/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1007/s00394-022-02982-0.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1007",
"published": {
"date-parts": [
[
2022,
8,
16
]
]
},
"published-online": {
"date-parts": [
[
2022,
8,
16
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"author": "C Huang",
"doi-asserted-by": "publisher",
"first-page": "497",
"issue": "10223",
"journal-title": "China Lancet",
"key": "2982_CR1",
"unstructured": "Huang C, Wang Y, Li X et al (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan. China Lancet 395(10223):497–506. https://doi.org/10.1016/S0140-6736(20)30183-5",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/S1473-3099(20)30120-1",
"author": "E Dong",
"doi-asserted-by": "publisher",
"first-page": "533",
"issue": "5",
"journal-title": "Lancet Infect Dis",
"key": "2982_CR2",
"unstructured": "Dong E, Du H, Gardner L (2020) An interactive web-based dashboard to track COVID-19 in real time. Lancet Infect Dis 20(5):533–534. https://doi.org/10.1016/S1473-3099(20)30120-1",
"volume": "20",
"year": "2020"
},
{
"key": "2982_CR3",
"unstructured": "World Health Organization (2022) A clinical case definition of post COVID-19 condition by a Delphi consensus. https://www.who.int/publications/i/item/WHO-2019-nCoV-Post_COVID-19_condition-Clinical_case_definition-2021.1. Accessed 18 February 2022"
},
{
"DOI": "10.1371/journal.pmed.1003553",
"author": "A Leong",
"doi-asserted-by": "publisher",
"journal-title": "Plos Med",
"key": "2982_CR4",
"unstructured": "Leong A, Cole JB, Brenner LN, Meigs JB, Florez JC, Mercader JM (2021) Cardiometabolic risk factors for COVID-19 susceptibility and severity: a Mendelian randomization analysis. Plos Med. https://doi.org/10.1371/journal.pmed.1003553",
"year": "2021"
},
{
"DOI": "10.1016/S2213-8587(21)00058-9",
"author": "E The Lancet Diabetes",
"doi-asserted-by": "publisher",
"first-page": "189",
"issue": "4",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "2982_CR5",
"unstructured": "The Lancet Diabetes E (2021) Metabolic health: a priority for the post-pandemic era. Lancet Diabetes Endocrinol 9(4):189. https://doi.org/10.1016/S2213-8587(21)00058-9",
"volume": "9",
"year": "2021"
},
{
"DOI": "10.1053/j.gastro.2020.04.064",
"author": "S Singh",
"doi-asserted-by": "publisher",
"first-page": "768",
"issue": "2",
"journal-title": "Gastroenterology",
"key": "2982_CR6",
"unstructured": "Singh S, Khan A (2020) Clinical characteristics and outcomes of coronavirus disease 2019 among patients with preexisting liver disease in the United States: a multicenter research network study. Gastroenterology 159(2):768-771.e3. https://doi.org/10.1053/j.gastro.2020.04.064",
"volume": "159",
"year": "2020"
},
{
"DOI": "10.1186/s12889-021-12148-y",
"author": "S Wood",
"doi-asserted-by": "publisher",
"first-page": "2110",
"issue": "1",
"journal-title": "BMC Public Health",
"key": "2982_CR7",
"unstructured": "Wood S, Harrison SE, Judd N, Bellis MA, Hughes K, Jones A (2021) The impact of behavioural risk factors on communicable diseases: a systematic review of reviews. BMC Public Health 21(1):2110. https://doi.org/10.1186/s12889-021-12148-y",
"volume": "21",
"year": "2021"
},
{
"DOI": "10.1161/CIRCULATIONAHA.115.018585",
"author": "D Mozaffarian",
"doi-asserted-by": "publisher",
"first-page": "187",
"issue": "2",
"journal-title": "Circulation",
"key": "2982_CR8",
"unstructured": "Mozaffarian D (2016) Dietary and policy priorities for cardiovascular disease, diabetes, and obesity: a comprehensive review. Circulation 133(2):187–225. https://doi.org/10.1161/CIRCULATIONAHA.115.018585",
"volume": "133",
"year": "2016"
},
{
"DOI": "10.1136/bmjnph-2020-000085",
"author": "PC Calder",
"doi-asserted-by": "publisher",
"first-page": "74",
"issue": "1",
"journal-title": "BMJ Nutr Prev Health",
"key": "2982_CR9",
"unstructured": "Calder PC (2020) Nutrition, immunity and COVID-19. BMJ Nutr Prev Health 3(1):74–92. https://doi.org/10.1136/bmjnph-2020-000085",
"volume": "3",
"year": "2020"
},
{
"DOI": "10.1056/NEJMp2021264",
"author": "MJ Belanger",
"doi-asserted-by": "publisher",
"issue": "11",
"journal-title": "N Engl J Med",
"key": "2982_CR10",
"unstructured": "Belanger MJ, Hill MA, Angelidi AM, Dalamaga M, Sowers JR, Mantzoros CS (2020) Covid-19 and disparities in nutrition and obesity. N Engl J Med 383(11):e69. https://doi.org/10.1056/NEJMp2021264",
"volume": "383",
"year": "2020"
},
{
"DOI": "10.1007/978-3-030-63761-3_28",
"author": "M Moallemian Isfahani",
"doi-asserted-by": "publisher",
"first-page": "485",
"journal-title": "Adv Exp Med Biol",
"key": "2982_CR11",
"unstructured": "Moallemian Isfahani M, Emam-Djomeh Z, Rao IM, Rezaei N (2021) Nutrition and immunity in COVID-19. Adv Exp Med Biol 1318:485–497. https://doi.org/10.1007/978-3-030-63761-3_28",
"volume": "1318",
"year": "2021"
},
{
"DOI": "10.1186/s12939-016-0384-y",
"author": "I Storm",
"doi-asserted-by": "publisher",
"first-page": "97",
"journal-title": "Int J Equity Health",
"key": "2982_CR12",
"unstructured": "Storm I, den Hertog F, van Oers H, Schuit AJ (2016) How to improve collaboration between the public health sector and other policy sectors to reduce health inequalities? - a study in sixteen municipalities in the Netherlands. Int J Equity Health 15:97. https://doi.org/10.1186/s12939-016-0384-y",
"volume": "15",
"year": "2016"
},
{
"DOI": "10.1136/gutjnl-2021-325353",
"author": "J Merino",
"doi-asserted-by": "publisher",
"first-page": "2096",
"issue": "11",
"journal-title": "Gut",
"key": "2982_CR13",
"unstructured": "Merino J, Joshi AD, Nguyen LH et al (2021) Diet quality and risk and severity of COVID-19: a prospective cohort study. Gut 70(11):2096–2104. https://doi.org/10.1136/gutjnl-2021-325353",
"volume": "70",
"year": "2021"
},
{
"DOI": "10.1186/s12916-021-02168-1",
"author": "M Deschasaux-Tanguy",
"doi-asserted-by": "publisher",
"first-page": "290",
"issue": "1",
"journal-title": "BMC Med",
"key": "2982_CR14",
"unstructured": "Deschasaux-Tanguy M, Srour B, Bourhis L et al (2021) Nutritional risk factors for SARS-CoV-2 infection: a prospective study within the NutriNet-Santé cohort. BMC Med 19(1):290. https://doi.org/10.1186/s12916-021-02168-1",
"volume": "19",
"year": "2021"
},
{
"DOI": "10.1017/S1368980018003762",
"author": "CA Monteiro",
"doi-asserted-by": "publisher",
"first-page": "936",
"issue": "5",
"journal-title": "Public Health Nutr",
"key": "2982_CR15",
"unstructured": "Monteiro CA, Cannon G, Levy RB et al (2019) Ultra-processed foods: what they are and how to identify them. Public Health Nutr 22(5):936–941. https://doi.org/10.1017/S1368980018003762",
"volume": "22",
"year": "2019"
},
{
"DOI": "10.1007/s00394-021-02786-8",
"author": "A Fardet",
"doi-asserted-by": "publisher",
"journal-title": "Eur J Nutr",
"key": "2982_CR16",
"unstructured": "Fardet A, Rock E (2022) Chronic diseases are first associated with the degradation and artificialization of food matrices rather than with food composition: calorie quality matters more than calorie quantity. Eur J Nutr. https://doi.org/10.1007/s00394-021-02786-8",
"year": "2022"
},
{
"DOI": "10.3389/fmed.2020.00146",
"author": "M Briguglio",
"doi-asserted-by": "publisher",
"first-page": "146",
"journal-title": "Front Med",
"key": "2982_CR17",
"unstructured": "Briguglio M, Pregliasco FE, Lombardi G, Perazzo P, Banfi G (2020) The malnutritional status of the host as a virulence factor for new coronavirus SARS-CoV-2. Front Med 7:146. https://doi.org/10.3389/fmed.2020.00146",
"volume": "7",
"year": "2020"
},
{
"DOI": "10.3945/ajcn.117.160440",
"author": "MJ Gibney",
"doi-asserted-by": "publisher",
"first-page": "717",
"issue": "3",
"journal-title": "Am J Clin Nutr",
"key": "2982_CR18",
"unstructured": "Gibney MJ, Forde CG, Mullally D, Gibney ER (2017) Ultra-processed foods in human health: a critical appraisal. Am J Clin Nutr 106(3):717–724. https://doi.org/10.3945/ajcn.117.160440",
"volume": "106",
"year": "2017"
},
{
"DOI": "10.1186/1475-2891-13-61",
"author": "IA Myles",
"doi-asserted-by": "publisher",
"first-page": "61",
"journal-title": "Nutr J",
"key": "2982_CR19",
"unstructured": "Myles IA (2014) Fast food fever: reviewing the impacts of the western diet on immunity. Nutr J 13:61. https://doi.org/10.1186/1475-2891-13-61",
"volume": "13",
"year": "2014"
},
{
"DOI": "10.1164/rccm.201203-0573OC",
"author": "O Sideleva",
"doi-asserted-by": "publisher",
"first-page": "598",
"issue": "7",
"journal-title": "Am J Respir Crit Care Med",
"key": "2982_CR20",
"unstructured": "Sideleva O, Suratt BT, Black KE et al (2012) Obesity and asthma: an inflammatory disease of adipose tissue not the airway. Am J Respir Crit Care Med 186(7):598–605. https://doi.org/10.1164/rccm.201203-0573OC",
"volume": "186",
"year": "2012"
},
{
"DOI": "10.1136/bmj.k322",
"author": "T Fiolet",
"doi-asserted-by": "publisher",
"journal-title": "BMJ (Clinical research ed)",
"key": "2982_CR21",
"unstructured": "Fiolet T, Srour B, Sellem L et al (2018) Consumption of ultra-processed foods and cancer risk: results from NutriNet-Sante prospective cohort. BMJ (Clinical research ed) 360:k322. https://doi.org/10.1136/bmj.k322",
"volume": "360",
"year": "2018"
},
{
"DOI": "10.1136/bmj.n1554",
"author": "N Narula",
"doi-asserted-by": "publisher",
"journal-title": "BMJ (Clinical research ed)",
"key": "2982_CR22",
"unstructured": "Narula N, Wong ECL, Dehghan M et al (2021) Association of ultra-processed food intake with risk of inflammatory bowel disease: prospective cohort study. BMJ (Clinical research ed) 374:n1554. https://doi.org/10.1136/bmj.n1554",
"volume": "374",
"year": "2021"
},
{
"DOI": "10.1136/bmj.l1949",
"author": "A Rico-Campa",
"doi-asserted-by": "publisher",
"journal-title": "BMJ",
"key": "2982_CR23",
"unstructured": "Rico-Campa A, Martinez-Gonzalez MA, Alvarez-Alvarez I et al (2019) Association between consumption of ultra-processed foods and all cause mortality: SUN prospective cohort study. BMJ 365:l1949. https://doi.org/10.1136/bmj.l1949",
"volume": "365",
"year": "2019"
},
{
"DOI": "10.1136/bmj.l1451",
"author": "B Srour",
"doi-asserted-by": "publisher",
"journal-title": "BMJ",
"key": "2982_CR24",
"unstructured": "Srour B, Fezeu LK, Kesse-Guyot E et al (2019) Ultra-processed food intake and risk of cardiovascular disease: prospective cohort study (NutriNet-Sante). BMJ 365:l1451. https://doi.org/10.1136/bmj.l1451",
"volume": "365",
"year": "2019"
},
{
"DOI": "10.1038/s41586-018-0579-z",
"author": "C Bycroft",
"doi-asserted-by": "publisher",
"first-page": "203",
"issue": "7726",
"journal-title": "Nature",
"key": "2982_CR25",
"unstructured": "Bycroft C, Freeman C, Petkova D et al (2018) The UK Biobank resource with deep phenotyping and genomic data. Nature 562(7726):203–209. https://doi.org/10.1038/s41586-018-0579-z",
"volume": "562",
"year": "2018"
},
{
"DOI": "10.1093/eurheartj/ehab783",
"author": "M Bonaccio",
"doi-asserted-by": "publisher",
"first-page": "213",
"issue": "3",
"journal-title": "Eur Heart J",
"key": "2982_CR26",
"unstructured": "Bonaccio M, Costanzo S, Di Castelnuovo A et al (2022) Ultra-processed food intake and all-cause and cause-specific mortality in individuals with cardiovascular disease: the Moli-sani Study. Eur Heart J 43(3):213–224. https://doi.org/10.1093/eurheartj/ehab783",
"volume": "43",
"year": "2022"
},
{
"DOI": "10.1017/S0007114515004821",
"author": "J Galante",
"doi-asserted-by": "publisher",
"first-page": "681",
"issue": "4",
"journal-title": "Br J Nutr",
"key": "2982_CR27",
"unstructured": "Galante J, Adamska L, Young A et al (2016) The acceptability of repeat Internet-based hybrid diet assessment of previous 24-h dietary intake: administration of the Oxford WebQ in UK Biobank. Br J Nutr 115(4):681–686. https://doi.org/10.1017/S0007114515004821",
"volume": "115",
"year": "2016"
},
{
"DOI": "10.1007/s00394-021-02558-4",
"author": "A Perez-Cornago",
"doi-asserted-by": "publisher",
"first-page": "4019",
"issue": "7",
"journal-title": "Eur J Nutr",
"key": "2982_CR28",
"unstructured": "Perez-Cornago A, Pollard Z, Young H et al (2021) Description of the updated nutrition calculation of the Oxford WebQ questionnaire and comparison with the previous version among 207,144 participants in UK Biobank. Eur J Nutr 60(7):4019–4030. https://doi.org/10.1007/s00394-021-02558-4",
"volume": "60",
"year": "2021"
},
{
"DOI": "10.1017/S1368980017000234",
"author": "CA Monteiro",
"doi-asserted-by": "publisher",
"first-page": "5",
"issue": "1",
"journal-title": "Public Health Nutr",
"key": "2982_CR29",
"unstructured": "Monteiro CA, Cannon G, Moubarac JC, Levy RB, Louzada MLC, Jaime PC (2018) The UN Decade of nutrition, the NOVA food classification and the trouble with ultra-processing. Public Health Nutr 21(1):5–17. https://doi.org/10.1017/S1368980017000234",
"volume": "21",
"year": "2018"
},
{
"DOI": "10.1007/s13679-014-0092-0",
"author": "JC Moubarac",
"doi-asserted-by": "publisher",
"first-page": "256",
"issue": "2",
"journal-title": "Curr Obes Rep",
"key": "2982_CR30",
"unstructured": "Moubarac JC, Parra DC, Cannon G, Monteiro CA (2014) Food classification systems based on food processing: significance and implications for policies and actions: a systematic literature review and assessment. Curr Obes Rep 3(2):256–272. https://doi.org/10.1007/s13679-014-0092-0",
"volume": "3",
"year": "2014"
},
{
"DOI": "10.1099/mgen.0.000397",
"author": "J Armstrong",
"doi-asserted-by": "publisher",
"journal-title": "Microbial genomics",
"key": "2982_CR31",
"unstructured": "Armstrong J, Rudkin JK, Allen N et al (2020) Dynamic linkage of COVID-19 test results between public health England’s second generation surveillance system and UK Biobank. Microbial genomics. https://doi.org/10.1099/mgen.0.000397",
"year": "2020"
},
{
"DOI": "10.1161/circulationaha.117.030898",
"author": "R Pazoki",
"doi-asserted-by": "publisher",
"first-page": "653",
"issue": "7",
"journal-title": "Circulation",
"key": "2982_CR32",
"unstructured": "Pazoki R, Dehghan A, Evangelou E et al (2018) Genetic predisposition to high blood pressure and lifestyle factors: associations with midlife blood pressure levels and cardiovascular events. Circulation 137(7):653–661. https://doi.org/10.1161/circulationaha.117.030898",
"volume": "137",
"year": "2018"
},
{
"DOI": "10.2337/dc20-1109",
"author": "M Wang",
"doi-asserted-by": "publisher",
"first-page": "2776",
"issue": "11",
"journal-title": "Diabetes Care",
"key": "2982_CR33",
"unstructured": "Wang M, Zhou T, Li X et al (2020) Baseline vitamin D status, sleep patterns, and the risk of incident Type 2 diabetes in data from the UK Biobank study. Diabetes Care 43(11):2776–2784. https://doi.org/10.2337/dc20-1109",
"volume": "43",
"year": "2020"
},
{
"key": "2982_CR34",
"unstructured": "H. Pinchen, N. Powell, S. Church, P. Finglas P.H. England (Ed.) (2021) McCance and Widdowson’s The Composition of Foods Integrated Dataset 2021, User Guide. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/971021/McCance_and_Widdowsons_Composition_of_Foods_integrated_dataset_2021.pdf. Accessed 8 June 2022"
},
{
"DOI": "10.1016/j.immuni.2019.09.020",
"author": "A Christ",
"doi-asserted-by": "publisher",
"first-page": "794",
"issue": "5",
"journal-title": "Immunity",
"key": "2982_CR35",
"unstructured": "Christ A, Lauterbach M, Latz E (2019) Western diet and the immune system: an inflammatory connection. Immunity 51(5):794–811. https://doi.org/10.1016/j.immuni.2019.09.020",
"volume": "51",
"year": "2019"
},
{
"DOI": "10.3390/nu13020610",
"author": "JP De Bandt",
"doi-asserted-by": "publisher",
"journal-title": "Nutrients",
"key": "2982_CR36",
"unstructured": "De Bandt JP, Monin C (2021) Obesity, nutrients and the immune system in the era of COVID-19. Nutrients. https://doi.org/10.3390/nu13020610",
"year": "2021"
},
{
"DOI": "10.3389/fimmu.2017.00838",
"author": "D Statovci",
"doi-asserted-by": "publisher",
"first-page": "838",
"journal-title": "Front Immunol",
"key": "2982_CR37",
"unstructured": "Statovci D, Aguilera M, MacSharry J, Melgar S (2017) The impact of western diet and nutrients on the microbiota and immune response at mucosal interfaces. Front Immunol 8:838. https://doi.org/10.3389/fimmu.2017.00838",
"volume": "8",
"year": "2017"
},
{
"DOI": "10.1038/s41418-020-0530-3",
"author": "Y Shi",
"doi-asserted-by": "publisher",
"first-page": "1451",
"issue": "5",
"journal-title": "Cell Death Differ",
"key": "2982_CR38",
"unstructured": "Shi Y, Wang Y, Shao C et al (2020) COVID-19 infection: the perspectives on immune responses. Cell Death Differ 27(5):1451–1454. https://doi.org/10.1038/s41418-020-0530-3",
"volume": "27",
"year": "2020"
},
{
"DOI": "10.1016/j.envint.2019.105057",
"author": "JP Buckley",
"doi-asserted-by": "publisher",
"journal-title": "Environ Int",
"key": "2982_CR39",
"unstructured": "Buckley JP, Kim H, Wong E, Rebholz CM (2019) Ultra-processed food consumption and exposure to phthalates and bisphenols in the US National health and nutrition examination survey, 2013–2014. Environ Int 131:105057. https://doi.org/10.1016/j.envint.2019.105057",
"volume": "131",
"year": "2019"
},
{
"DOI": "10.1136/bmj.l2289",
"author": "MA Lawrence",
"doi-asserted-by": "publisher",
"journal-title": "BMJ",
"key": "2982_CR40",
"unstructured": "Lawrence MA, Baker PI (2019) Ultra-processed food and adverse health outcomes. BMJ 365:l2289. https://doi.org/10.1136/bmj.l2289",
"volume": "365",
"year": "2019"
},
{
"DOI": "10.3389/fgene.2021.639905",
"author": "TW Ha",
"doi-asserted-by": "publisher",
"journal-title": "Front Genet",
"key": "2982_CR41",
"unstructured": "Ha TW, Jung HU, Kim DJ et al (2021) Association between environmental factors and asthma using mendelian randomization: increased effect of body mass index on adult-onset moderate-to-severe asthma subtypes. Front Genet 12:639905. https://doi.org/10.3389/fgene.2021.639905",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.3390/nu13062114",
"author": "TT Vu",
"doi-asserted-by": "publisher",
"first-page": "2114",
"issue": "6",
"journal-title": "Nutrients",
"key": "2982_CR42",
"unstructured": "Vu TT, Rydland KJ, Achenbach CJ, Van Horn L, Cornelis MC (2021) Dietary behaviors and incident COVID-19 in the UK Biobank. Nutrients 13(6):2114. https://doi.org/10.3390/nu13062114",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1039/c6fo00107f",
"author": "A Fardet",
"doi-asserted-by": "publisher",
"first-page": "2338",
"issue": "5",
"journal-title": "Food Funct",
"key": "2982_CR43",
"unstructured": "Fardet A (2016) Minimally processed foods are more satiating and less hyperglycemic than ultra-processed foods: a preliminary study with 98 ready-to-eat foods. Food Funct 7(5):2338–2346. https://doi.org/10.1039/c6fo00107f",
"volume": "7",
"year": "2016"
},
{
"DOI": "10.1111/irv.12618",
"author": "JS Moser",
"doi-asserted-by": "publisher",
"first-page": "3",
"issue": "1",
"journal-title": "Influenza Other Respir Viruses",
"key": "2982_CR44",
"unstructured": "Moser JS, Galindo-Fraga A, Ortiz-Hernandez AA et al (2019) Underweight, overweight, and obesity as independent risk factors for hospitalization in adults and children from influenza and other respiratory viruses. Influenza Other Respir Viruses 13(1):3–9. https://doi.org/10.1111/irv.12618",
"volume": "13",
"year": "2019"
},
{
"DOI": "10.3892/mmr.2020.11127",
"author": "D Petrakis",
"doi-asserted-by": "publisher",
"first-page": "9",
"issue": "1",
"journal-title": "Mol Med Rep",
"key": "2982_CR45",
"unstructured": "Petrakis D, Margina D, Tsarouhas K et al (2020) Obesity a risk factor for increased COVID19 prevalence, severity and lethality (Review). Mol Med Rep 22(1):9–19. https://doi.org/10.3892/mmr.2020.11127",
"volume": "22",
"year": "2020"
},
{
"DOI": "10.3389/fimmu.2019.01071",
"author": "R Honce",
"doi-asserted-by": "publisher",
"first-page": "1071",
"journal-title": "Front Immunol",
"key": "2982_CR46",
"unstructured": "Honce R, Schultz-Cherry S (2019) Impact of Obesity on Influenza A virus pathogenesis, immune response, and evolution. Front Immunol 10:1071. https://doi.org/10.3389/fimmu.2019.01071",
"volume": "10",
"year": "2019"
},
{
"DOI": "10.1111/cei.12824",
"author": "D Frasca",
"doi-asserted-by": "publisher",
"first-page": "64",
"issue": "1",
"journal-title": "Clin Exp Immunol",
"key": "2982_CR47",
"unstructured": "Frasca D, Diaz A, Romero M, Blomberg BB (2017) Ageing and obesity similarly impair antibody responses. Clin Exp Immunol 187(1):64–70. https://doi.org/10.1111/cei.12824",
"volume": "187",
"year": "2017"
},
{
"DOI": "10.1016/j.cmet.2019.05.008",
"author": "KD Hall",
"doi-asserted-by": "publisher",
"first-page": "67",
"issue": "1",
"journal-title": "Cell Metab",
"key": "2982_CR48",
"unstructured": "Hall KD, Ayuketah A, Brychta R et al (2019) Ultra-processed diets cause excess calorie intake and weight gain: an inpatient randomized controlled trial of ad libitum food intake. Cell Metab 30(1):67-77.e3. https://doi.org/10.1016/j.cmet.2019.05.008",
"volume": "30",
"year": "2019"
},
{
"DOI": "10.1007/s13679-017-0285-4",
"author": "JM Poti",
"doi-asserted-by": "publisher",
"first-page": "420",
"issue": "4",
"journal-title": "Curr Obes Rep",
"key": "2982_CR49",
"unstructured": "Poti JM, Braga B, Qin B (2017) Ultra-processed food intake and obesity: what really matters for health-processing or nutrient content? Curr Obes Rep 6(4):420–431. https://doi.org/10.1007/s13679-017-0285-4",
"volume": "6",
"year": "2017"
},
{
"DOI": "10.1371/journal.pmed.1003256",
"author": "M Beslay",
"doi-asserted-by": "publisher",
"issue": "8",
"journal-title": "Plos Med",
"key": "2982_CR50",
"unstructured": "Beslay M, Srour B, Mejean C et al (2020) Ultra-processed food intake in association with BMI change and risk of overweight and obesity: a prospective analysis of the French NutriNet-Sante cohort. Plos Med 17(8):e1003256. https://doi.org/10.1371/journal.pmed.1003256",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.3389/fped.2021.702731",
"author": "JF López-Gil",
"doi-asserted-by": "publisher",
"journal-title": "Front Pediatr",
"key": "2982_CR51",
"unstructured": "López-Gil JF, García-Hermoso A, Tárraga-López PJ, Brazo-Sayavera J (2021) Dietary patterns, adherence to the food-based dietary guidelines, and ultra-processed consumption during the COVID-19 lockdown in a sample of Spanish young population. Front Pediatr 9:702731. https://doi.org/10.3389/fped.2021.702731",
"volume": "9",
"year": "2021"
}
],
"reference-count": 51,
"references-count": 51,
"relation": {},
"resource": {
"primary": {
"URL": "https://link.springer.com/10.1007/s00394-022-02982-0"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Nutrition and Dietetics",
"Medicine (miscellaneous)"
],
"subtitle": [],
"title": "Impact of ultra-processed food intake on the risk of COVID-19: a prospective cohort study",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy"
}
