Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients
et al., Int. Immunopharmacol., doi:10.1016/j.intimp.2020.107088, Oct 2020
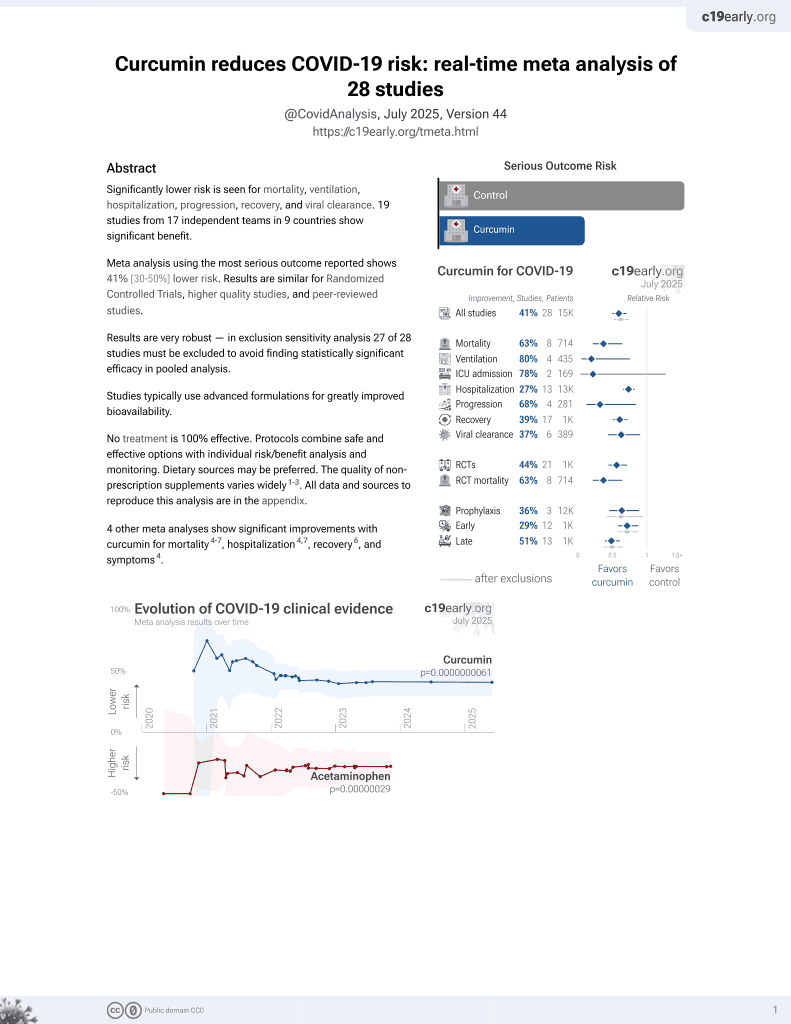
Curcumin for COVID-19
16th treatment shown to reduce risk in
February 2021, now with p = 0.0000000061 from 28 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
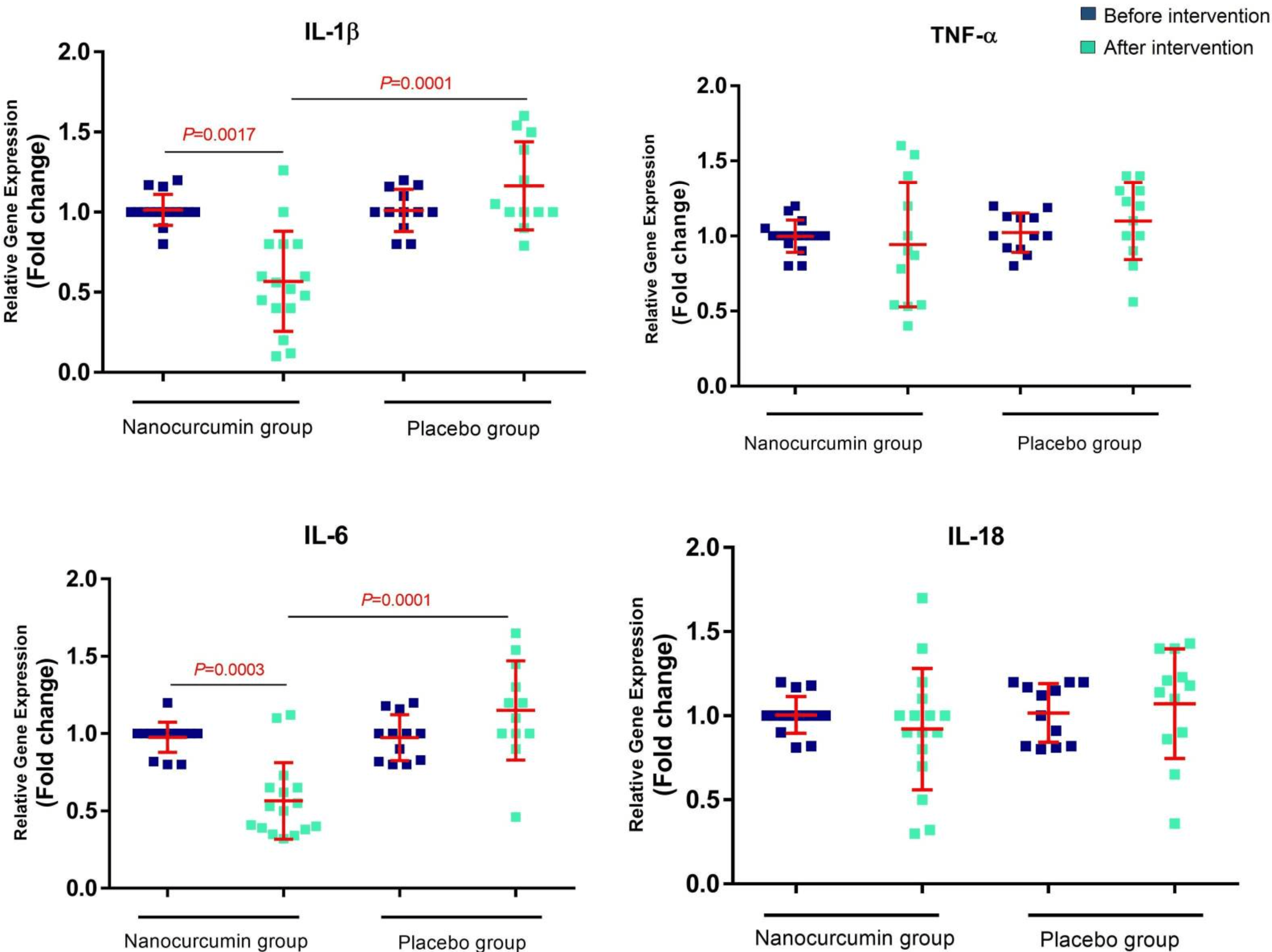
Small RCT with 40 nano-curcumin patients and 40 control patients showing lower mortality with treatment. Authors conclude that nano-curcumin may be able to modulate the increased rate of inflammatory cytokines especially IL-1β and IL-6 mRNA expression and cytokine secretion in COVID-19 patients, which may improve clinical outcomes.
This is the 1st of 21 COVID-19 RCTs for curcumin, which collectively show efficacy with p=0.0000022.
This is the 1st of 28 COVID-19 controlled studies for curcumin, which collectively show efficacy with p=0.0000000061.
|
risk of death, 50.0% lower, RR 0.50, p = 0.30, treatment 4 of 20 (20.0%), control 8 of 20 (40.0%), NNT 5.0.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Valizadeh et al., 20 Oct 2020, Double Blind Randomized Controlled Trial, Iran, peer-reviewed, 12 authors.
Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients
International Immunopharmacology, doi:10.1016/j.intimp.2020.107088
Since January 2020 Elsevier has created a COVID-19 resource centre with free information in English and Mandarin on the novel coronavirus COVID-19. The COVID-19 resource centre is hosted on Elsevier Connect, the company's public news and information website. Elsevier hereby grants permission to make all its COVID-19-related research that is available on the COVID-19 resource centre -including this research content -immediately available in PubMed Central and other publicly funded repositories, such as the WHO COVID database with rights for unrestricted research re-use and analyses in any form or by any means with acknowledgement of the original source. These permissions are granted for free by Elsevier for as long as the COVID-19 resource centre remains active.
Declaration of Competing Interest The authors declared that there is no conflict of interest.
Appendix A. Supplementary material Supplementary data to this article can be found online at https:// doi.org/10.1016/j.intimp.2020.107088.
References
Afolayan, Erinwusi, Oyeyemi, Immunomodulatory activity of curcuminentrapped poly d, l-lactic-co-glycolic acid nanoparticles in mice, Integrative Medicine Res
Aggarwal, Kumar, Bharti, Anticancer potential of curcumin: preclinical and clinical studies, Anticancer Res
Ay, Bakır, Bozkurt, Kayis, Hakki, Positive effect of curcumin on experimental peridontitis via suppression of IL-1-beta and IL-6 expression level, International Journal for Vitamin and Nutrition Research
Bose, Panda, Mukherjee, Sa, Curcumin and tumor immune-editing: resurrecting the immune system, Cell division
Cascella, Rajnik, Cuomo, Dulebohn, Napoli, Features, evaluation and treatment coronavirus (COVID-19)
Catanzaro, Corsini, Rosini, Racchi, Lanni, Immunomodulators inspired by nature: a review on curcumin and echinacea, Molecules
Conti, Ronconi, Caraffa, Gallenga, Ross et al., Induction of pro-inflammatory cytokines (IL-1 and IL-6) and lung inflammation by Coronavirus-19 (COVI-19 or SARS-CoV-2): anti-inflammatory strategies, J. Biol. Regul. Homeost. Agents
Corkum, Ings, Burgess, Karwowska, Kroll et al., Immune cell subsets and their gene expression profiles from human PBMC isolated by Vacutainer Cell Preparation Tube (CPT™) and standard density gradient, BMC immunology
Dei Cas, Ghidoni, Dietary curcumin: correlation between bioavailability and health potential, Nutrients
Derosa, Maffioli, Simental-Mendia, Bo, Sahebkar, Effect of curcumin on circulating interleukin-6 concentrations: a systematic review and meta-analysis of randomized controlled trials, Pharmacol. Res
Dolati, Ahmadi, Aghebti-Maleki, Nikmaram, Marofi et al., Nanocurcumin is a potential novel therapy for multiple sclerosis by influencing inflammatory mediators, Pharmacol. Rep
Dolati, Ahmadi, Rikhtegar, Babaloo, Ayromlou et al., Changes in Th17 cells function after nanocurcumin use to treat multiple sclerosis, Int. Immunopharmacol
Feldmann, Maini, Woody, Holgate, Winter et al., Trials of anti-tumour necrosis factor therapy for COVID-19 are urgently needed, The Lancet
Gera, Sharma, Ghosh, Huynh, Lee et al., Nanoformulations of curcumin: an emerging paradigm for improved remedial application, Oncotarget
Ghaebi, Osali, Valizadeh, Roshangar, Ahmadi, Vaccine development and therapeutic design for 2019-nCoV/SARS-CoV-2: Challenges and chances, Journal of cellular physiology
Gupta, Patchva, Aggarwal, Therapeutic roles of curcumin: lessons learned from clinical trials, AAPS J
Han, Ma, Li, Liu, Zhao et al., Profiling serum cytokines in COVID-19 patients reveals IL-6 and IL-10 are disease severity predictors, Emerging Microbes Infect
Hatamipour, Sahebkar, Alavizadeh, Dorri, Jaafari, Novel nanomicelle formulation to enhance bioavailability and stability of curcuminoids, Iranian J. Basic Medical Sci
Henry, De Oliveira, Benoit, Plebani, Lippi, Hematologic, biochemical and immune biomarker abnormalities associated with severe illness and mortality in coronavirus disease 2019 (COVID-19): a meta-analysis, Clinical Chem. Laboratory Medicine (CCLM)
Hewlings, Kalman, Curcumin: a review of its' effects on human health, Foods
Huang, Wang, Li, Ren, Zhao et al., Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, The lancet
Li, Fan, Lai, Han, Li et al., Coronavirus infections and immune responses, J. Med. Virol
Li, Ma, Acute respiratory failure in COVID-19: is it "typical" ARDS?, Crit. Care
Marchetti, Swartzwelter, Koenders, Azam, Tengesdal et al., NLRP3 inflammasome inhibitor OLT1177 suppresses joint inflammation in murine models of acute arthritis, Arthritis Res. Therapy
Mouzaoui, Rahim, Djerdjouri, Aminoguanidine and curcumin attenuated tumor necrosis factor (TNF)-α-induced oxidative stress, colitis and hepatotoxicity in mice, Int. Immunopharmacol
Okabayashi, Kariwa, Yokota, Iki, Indoh et al., Cytokine regulation in SARS coronavirus infection compared to other respiratory virus infections, Journal of medical virology
Ruan, Yang, Wang, Jiang, Song, Clinical predictors of mortality due to COVID-19 based on an analysis of data of 150 patients from Wuhan, China, Intensive care medicine
Sahebkar, Cicero, Simental-Mendía, Aggarwal, Gupta, Curcumin downregulates human tumor necrosis factor-α levels: A systematic review and meta-analysis ofrandomized controlled trials, Pharmacol. Res
Schneider, Hossain, Vandermolen, Nicol, Comparison of remicade to curcumin for the treatment of Crohn's disease: A systematic review, Complementary Therapies Medicine
Taghizadieh, Mikaeili, Ahmadi, Valizadeh, Acute kidney injury in pregnant women following SARS-CoV-2 infection: A case report from Iran
Tay, Poh, Rénia, Macary, Ng, The trinity of COVID-19: immunity, inflammation and intervention, Nat. Rev. Immunol
Trivedi, Mondal, Gangwar, Jana, Immunomodulatory potential of nanocurcumin-based formulation, Inflammopharmacology
Ulhaq, Soraya, Interleukin-6 as a potential biomarker of COVID-19 progression
Wang, Yang, Li, Wen, Zhang, Clinical features of 69 cases with coronavirus disease 2019
Weiss, Leibowitz, Coronavirus pathogenesis, advances in virus research
Weiss, Navas-Martin, Coronavirus pathogenesis and the emerging pathogen severe acute respiratory syndrome coronavirus, Microbiol. Mol. Biol. Rev
Yavarpour-Bali, Ghasemi-Kasman, Pirzadeh, Curcumin-loaded nanoparticles: A novel therapeutic strategy in treatment of central nervous system disorders, Int. J. Nanomed
Zhao, Liu, Yi, Wang, Qiao et al., Curcumin inhibiting Th17 cell differentiation by regulating the metabotropic glutamate receptor-4 expression on dendritic cells, Int. Immunopharmacol
DOI record:
{
"DOI": "10.1016/j.intimp.2020.107088",
"ISSN": [
"1567-5769"
],
"URL": "http://dx.doi.org/10.1016/j.intimp.2020.107088",
"alternative-id": [
"S1567576920321895"
],
"article-number": "107088",
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "International Immunopharmacology"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.intimp.2020.107088"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "Published by Elsevier B.V."
}
],
"author": [
{
"affiliation": [],
"family": "Valizadeh",
"given": "Hamed",
"sequence": "first"
},
{
"affiliation": [],
"family": "Abdolmohammadi-vahid",
"given": "Samaneh",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Danshina",
"given": "Svetlana",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ziya Gencer",
"given": "Mehmet",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ammari",
"given": "Ali",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sadeghi",
"given": "Armin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Roshangar",
"given": "Leila",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Aslani",
"given": "Saeed",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Esmaeilzadeh",
"given": "Abdolreza",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ghaebi",
"given": "Mahnaz",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Valizadeh",
"given": "Sepehr",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ahmadi",
"given": "Majid",
"sequence": "additional"
}
],
"container-title": "International Immunopharmacology",
"container-title-short": "International Immunopharmacology",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2020,
10,
20
]
],
"date-time": "2020-10-20T16:35:26Z",
"timestamp": 1603211726000
},
"deposited": {
"date-parts": [
[
2020,
12,
17
]
],
"date-time": "2020-12-17T19:01:11Z",
"timestamp": 1608231671000
},
"indexed": {
"date-parts": [
[
2024,
4,
4
]
],
"date-time": "2024-04-04T04:35:15Z",
"timestamp": 1712205315412
},
"is-referenced-by-count": 176,
"issued": {
"date-parts": [
[
2020,
12
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2020,
12,
1
]
],
"date-time": "2020-12-01T00:00:00Z",
"timestamp": 1606780800000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S1567576920321895?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S1567576920321895?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "107088",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2020,
12
]
]
},
"published-print": {
"date-parts": [
[
2020,
12
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"article-title": "Coronavirus pathogenesis, advances in virus research",
"author": "Weiss",
"first-page": "85",
"journal-title": "Elsevier",
"key": "10.1016/j.intimp.2020.107088_b0005",
"year": "2011"
},
{
"article-title": "The trinity of COVID-19: immunity, inflammation and intervention",
"author": "Tay",
"first-page": "1",
"journal-title": "Nat. Rev. Immunol.",
"key": "10.1016/j.intimp.2020.107088_b0010",
"year": "2020"
},
{
"DOI": "10.1128/MMBR.69.4.635-664.2005",
"article-title": "Coronavirus pathogenesis and the emerging pathogen severe acute respiratory syndrome coronavirus",
"author": "Weiss",
"doi-asserted-by": "crossref",
"first-page": "635",
"issue": "4",
"journal-title": "Microbiol. Mol. Biol. Rev.",
"key": "10.1016/j.intimp.2020.107088_b0015",
"volume": "69",
"year": "2005"
},
{
"article-title": "Features, evaluation and treatment coronavirus (COVID-19), Statpearls [internet]",
"author": "Cascella",
"journal-title": "StatPearls Publishing",
"key": "10.1016/j.intimp.2020.107088_b0020",
"year": "2020"
},
{
"DOI": "10.1002/jmv.25685",
"article-title": "Coronavirus infections and immune responses",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "424",
"issue": "4",
"journal-title": "J. Med. Virol.",
"key": "10.1016/j.intimp.2020.107088_b0025",
"volume": "92",
"year": "2020"
},
{
"DOI": "10.1186/s13054-020-02911-9",
"article-title": "Acute respiratory failure in COVID-19: is it “typical” ARDS?",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Crit. Care",
"key": "10.1016/j.intimp.2020.107088_b0030",
"volume": "24",
"year": "2020"
},
{
"DOI": "10.1016/j.rmcr.2020.101090",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2020.107088_b0035",
"unstructured": "A. Taghizadieh, H. Mikaeili, M. Ahmadi, H. Valizadeh, Acute kidney injury in pregnant women following SARS-CoV-2 infection: A case report from Iran, Respiratory medicine case reports (2020) 101090."
},
{
"DOI": "10.1002/jcp.29771",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2020.107088_b0040",
"unstructured": "M. Ghaebi, A. Osali, H. Valizadeh, L. Roshangar, M. Ahmadi, Vaccine development and therapeutic design for 2019‐nCoV/SARS‐CoV‐2: Challenges and chances, Journal of cellular physiology (2020)."
},
{
"article-title": "Induction of pro-inflammatory cytokines (IL-1 and IL-6) and lung inflammation by Coronavirus-19 (COVI-19 or SARS-CoV-2): anti-inflammatory strategies",
"author": "Conti",
"first-page": "1",
"issue": "2",
"journal-title": "J. Biol. Regul. Homeost. Agents",
"key": "10.1016/j.intimp.2020.107088_b0045",
"volume": "34",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"article-title": "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "497",
"issue": "10223",
"journal-title": "The lancet",
"key": "10.1016/j.intimp.2020.107088_b0050",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1186/s13075-018-1664-2",
"article-title": "NLRP3 inflammasome inhibitor OLT1177 suppresses joint inflammation in murine models of acute arthritis",
"author": "Marchetti",
"doi-asserted-by": "crossref",
"first-page": "169",
"issue": "1",
"journal-title": "Arthritis Res. Therapy",
"key": "10.1016/j.intimp.2020.107088_b0055",
"volume": "20",
"year": "2018"
},
{
"DOI": "10.2139/ssrn.3562887",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2020.107088_b0060",
"unstructured": "Z.S. Ulhaq, G.V. Soraya, Interleukin-6 as a potential biomarker of COVID-19 progression, Médecine et Maladies Infectieuses (2020)."
},
{
"DOI": "10.1080/22221751.2020.1770129",
"article-title": "Profiling serum cytokines in COVID-19 patients reveals IL-6 and IL-10 are disease severity predictors",
"author": "Han",
"doi-asserted-by": "crossref",
"first-page": "1123",
"issue": "1",
"journal-title": "Emerging Microbes Infect.",
"key": "10.1016/j.intimp.2020.107088_b0065",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30858-8",
"article-title": "Trials of anti-tumour necrosis factor therapy for COVID-19 are urgently needed",
"author": "Feldmann",
"doi-asserted-by": "crossref",
"first-page": "1407",
"issue": "10234",
"journal-title": "The Lancet",
"key": "10.1016/j.intimp.2020.107088_b0070",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/j.pharep.2018.05.008",
"article-title": "Nanocurcumin is a potential novel therapy for multiple sclerosis by influencing inflammatory mediators",
"author": "Dolati",
"doi-asserted-by": "crossref",
"first-page": "1158",
"issue": "6",
"journal-title": "Pharmacol. Rep.",
"key": "10.1016/j.intimp.2020.107088_b0075",
"volume": "70",
"year": "2018"
},
{
"DOI": "10.2147/IJN.S208332",
"article-title": "Curcumin-loaded nanoparticles: A novel therapeutic strategy in treatment of central nervous system disorders",
"author": "Yavarpour-Bali",
"doi-asserted-by": "crossref",
"first-page": "4449",
"journal-title": "Int. J. Nanomed.",
"key": "10.1016/j.intimp.2020.107088_b0080",
"volume": "14",
"year": "2019"
},
{
"DOI": "10.1208/s12248-012-9432-8",
"article-title": "Therapeutic roles of curcumin: lessons learned from clinical trials",
"author": "Gupta",
"doi-asserted-by": "crossref",
"first-page": "195",
"issue": "1",
"journal-title": "AAPS J.",
"key": "10.1016/j.intimp.2020.107088_b0085",
"volume": "15",
"year": "2013"
},
{
"article-title": "Anticancer potential of curcumin: preclinical and clinical studies",
"author": "Aggarwal",
"first-page": "363",
"issue": "1/A",
"journal-title": "Anticancer Res.",
"key": "10.1016/j.intimp.2020.107088_b0090",
"volume": "23",
"year": "2003"
},
{
"DOI": "10.3390/foods6100092",
"article-title": "Curcumin: a review of its’ effects on human health",
"author": "Hewlings",
"doi-asserted-by": "crossref",
"first-page": "92",
"issue": "10",
"journal-title": "Foods",
"key": "10.1016/j.intimp.2020.107088_b0095",
"volume": "6",
"year": "2017"
},
{
"DOI": "10.1016/j.intimp.2018.05.018",
"article-title": "Changes in Th17 cells function after nanocurcumin use to treat multiple sclerosis",
"author": "Dolati",
"doi-asserted-by": "crossref",
"first-page": "74",
"journal-title": "Int. Immunopharmacol.",
"key": "10.1016/j.intimp.2020.107088_b0100",
"volume": "61",
"year": "2018"
},
{
"DOI": "10.1186/s13008-015-0012-z",
"article-title": "Curcumin and tumor immune-editing: resurrecting the immune system",
"author": "Bose",
"doi-asserted-by": "crossref",
"first-page": "6",
"issue": "1",
"journal-title": "Cell division",
"key": "10.1016/j.intimp.2020.107088_b0105",
"volume": "10",
"year": "2015"
},
{
"DOI": "10.1016/j.imr.2018.02.004",
"article-title": "Immunomodulatory activity of curcumin-entrapped poly d, l-lactic-co-glycolic acid nanoparticles in mice",
"author": "Afolayan",
"doi-asserted-by": "crossref",
"first-page": "168",
"issue": "2",
"journal-title": "Integrative Medicine Res.",
"key": "10.1016/j.intimp.2020.107088_b0110",
"volume": "7",
"year": "2018"
},
{
"DOI": "10.1007/s10787-017-0395-3",
"article-title": "Immunomodulatory potential of nanocurcumin-based formulation",
"author": "Trivedi",
"doi-asserted-by": "crossref",
"first-page": "609",
"issue": "6",
"journal-title": "Inflammopharmacology",
"key": "10.1016/j.intimp.2020.107088_b0115",
"volume": "25",
"year": "2017"
},
{
"article-title": "Novel nanomicelle formulation to enhance bioavailability and stability of curcuminoids",
"author": "Hatamipour",
"first-page": "282",
"issue": "3",
"journal-title": "Iranian J. Basic Medical Sci.",
"key": "10.1016/j.intimp.2020.107088_b0120",
"volume": "22",
"year": "2019"
},
{
"DOI": "10.1186/s12865-015-0113-0",
"article-title": "Immune cell subsets and their gene expression profiles from human PBMC isolated by Vacutainer Cell Preparation Tube (CPT™) and standard density gradient",
"author": "Corkum",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "BMC immunology",
"key": "10.1016/j.intimp.2020.107088_b0125",
"volume": "16",
"year": "2015"
},
{
"DOI": "10.1002/jmv.20556",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2020.107088_b0130",
"unstructured": "T. Okabayashi, H. Kariwa, S.i. Yokota, S. Iki, T. Indoh, N. Yokosawa, I. Takashima, H. Tsutsumi, N. Fujii, Cytokine regulation in SARS coronavirus infection compared to other respiratory virus infections, Journal of medical virology 78(4) (2006) 417-424."
},
{
"DOI": "10.1007/s00134-020-05991-x",
"article-title": "Clinical predictors of mortality due to COVID-19 based on an analysis of data of 150 patients from Wuhan, China",
"author": "Ruan",
"doi-asserted-by": "crossref",
"first-page": "846",
"issue": "5",
"journal-title": "Intensive care medicine",
"key": "10.1016/j.intimp.2020.107088_b0135",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.1093/cid/ciaa272",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2020.107088_b0140",
"unstructured": "Z. Wang, B. Yang, Q. Li, L. Wen, R. Zhang, Clinical features of 69 cases with coronavirus disease 2019 in Wuhan, China, Clinical infectious diseases (2020)."
},
{
"DOI": "10.1515/cclm-2020-0369",
"article-title": "Hematologic, biochemical and immune biomarker abnormalities associated with severe illness and mortality in coronavirus disease 2019 (COVID-19): a meta-analysis",
"author": "Henry",
"doi-asserted-by": "crossref",
"first-page": "1021",
"issue": "7",
"journal-title": "Clinical Chem. Laboratory Medicine (CCLM)",
"key": "10.1016/j.intimp.2020.107088_b0145",
"volume": "58",
"year": "2020"
},
{
"DOI": "10.1016/j.intimp.2017.02.017",
"article-title": "Curcumin inhibiting Th17 cell differentiation by regulating the metabotropic glutamate receptor-4 expression on dendritic cells",
"author": "Zhao",
"doi-asserted-by": "crossref",
"first-page": "80",
"journal-title": "Int. Immunopharmacol.",
"key": "10.1016/j.intimp.2020.107088_b0150",
"volume": "46",
"year": "2017"
},
{
"DOI": "10.3390/molecules23112778",
"article-title": "Immunomodulators inspired by nature: a review on curcumin and echinacea",
"author": "Catanzaro",
"doi-asserted-by": "crossref",
"first-page": "2778",
"issue": "11",
"journal-title": "Molecules",
"key": "10.1016/j.intimp.2020.107088_b0155",
"volume": "23",
"year": "2018"
},
{
"DOI": "10.3390/nu11092147",
"article-title": "Dietary curcumin: correlation between bioavailability and health potential",
"author": "Dei Cas",
"doi-asserted-by": "crossref",
"first-page": "2147",
"issue": "9",
"journal-title": "Nutrients",
"key": "10.1016/j.intimp.2020.107088_b0160",
"volume": "11",
"year": "2019"
},
{
"DOI": "10.18632/oncotarget.19164",
"article-title": "Nanoformulations of curcumin: an emerging paradigm for improved remedial application",
"author": "Gera",
"doi-asserted-by": "crossref",
"first-page": "66680",
"issue": "39",
"journal-title": "Oncotarget",
"key": "10.1016/j.intimp.2020.107088_b0165",
"volume": "8",
"year": "2017"
},
{
"DOI": "10.1024/0300-9831/a000672",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2020.107088_b0170",
"unstructured": "Z.Y. Ay, B. Bakır, Ş.B. Bozkurt, S.A. Kayis, S.S. Hakki, Positive effect of curcumin on experimental peridontitis via suppression of IL-1-beta and IL-6 expression level, International Journal for Vitamin and Nutrition Research (2020)."
},
{
"DOI": "10.1016/j.ctim.2017.06.002",
"article-title": "Comparison of remicade to curcumin for the treatment of Crohn’s disease: A systematic review",
"author": "Schneider",
"doi-asserted-by": "crossref",
"first-page": "32",
"journal-title": "Complementary Therapies Medicine",
"key": "10.1016/j.intimp.2020.107088_b0175",
"volume": "33",
"year": "2017"
},
{
"DOI": "10.1016/j.intimp.2011.10.010",
"article-title": "Aminoguanidine and curcumin attenuated tumor necrosis factor (TNF)-α-induced oxidative stress, colitis and hepatotoxicity in mice",
"author": "Mouzaoui",
"doi-asserted-by": "crossref",
"first-page": "302",
"issue": "1",
"journal-title": "Int. Immunopharmacol.",
"key": "10.1016/j.intimp.2020.107088_b0180",
"volume": "12",
"year": "2012"
},
{
"DOI": "10.1016/j.phrs.2016.07.004",
"article-title": "Effect of curcumin on circulating interleukin-6 concentrations: a systematic review and meta-analysis of randomized controlled trials",
"author": "Derosa",
"doi-asserted-by": "crossref",
"first-page": "394",
"journal-title": "Pharmacol. Res.",
"key": "10.1016/j.intimp.2020.107088_b0185",
"volume": "111",
"year": "2016"
},
{
"DOI": "10.1016/j.phrs.2016.03.026",
"article-title": "Curcumin downregulates human tumor necrosis factor-α levels: A systematic review and meta-analysis ofrandomized controlled trials",
"author": "Sahebkar",
"doi-asserted-by": "crossref",
"first-page": "234",
"journal-title": "Pharmacol. Res.",
"key": "10.1016/j.intimp.2020.107088_b0190",
"volume": "107",
"year": "2016"
}
],
"reference-count": 38,
"references-count": 38,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S1567576920321895"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Pharmacology",
"Immunology",
"Immunology and Allergy"
],
"subtitle": [],
"title": "Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "89"
}
