A Study on the Impact of Sunlight, Ultraviolet Radiation, and Temperature Variability on COVID-19 Mortality: Spatiotemporal Evidence from Small Countries and U.S. States and Territories
et al., COVID, doi:10.3390/covid6040056, Mar 2026
Sunlight for COVID-19
35th treatment shown to reduce risk in
December 2021, now with p = 0.0000011 from 6 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
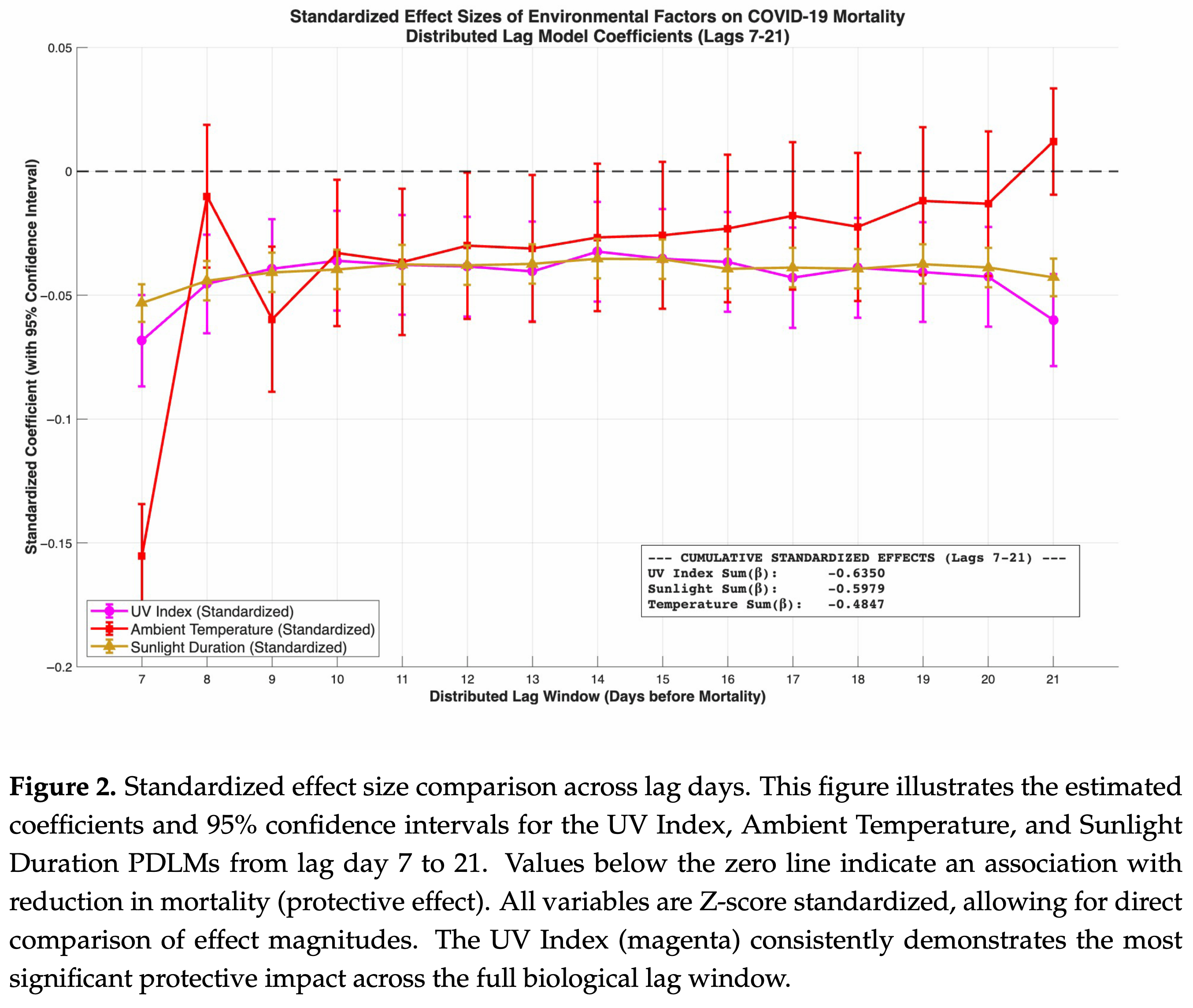
Ecological study of 129 geographical regions worldwide showing lower COVID-19 mortality with higher ambient Ultraviolet (UV) Index, sunlight duration, and temperature. Authors analyzed daily data from January 2020 to January 2023 utilizing panel Poisson Distributed Lag Models with 7-to-21-day exposure windows. Results demonstrated that a one-standard-deviation increase in the UV Index had the strongest negative association with mortality, followed by sunlight duration and ambient temperature. The study controlled for dynamic confounders like PM2.5 and relative humidity, which were found to be statistically insignificant, suggesting mortality reductions are driven by solar radiative intensity rather than simply clear or dry weather. However, the study relies on aggregate ecological data and deliberately excludes explicit seasonal controls to avoid over-adjustment bias, therefore the results cannot establish causality and may be confounded by human behavioral shifts, such as increased indoor crowding during colder months.
We calculate RR per standard deviation by exponentiating the sum of the 15 daily lag coefficients from the Poisson log-link model. For the confidence interval, we estimate the variance of the cumulative coefficient as Var(Σβₖ) = Σ SE²ₖ + 2·Σᵢ<ⱼ ρ·SEᵢ·SEⱼ, where ρ is the assumed pairwise correlation between lag estimates. The full variance-covariance matrix is not provided in the supplementary materials, so ρ must be assumed. Given the reported VIF of ~12 for UV lags, we use ρ ≈ 0.9 for a conservative confidence interval.
Several lines of evidence suggest the meteorological signal is not purely an artifact of behavioral confounding. First, PM2.5 and humidity - alternative proxies for winter conditions - were statistically insignificant when modeled alongside UV. Second, non-pharmaceutical interventions tightened during winter months and would have suppressed mortality during low-UV periods, biasing against the UV finding. Third, independent Bayesian estimates of COVID-19 seasonality that controlled for NPIs and mobility found a comparable seasonal effect magnitude1. Fourth, research indicates that seasonal differences in time spent indoors are small (~10%) and that summer mass-gathering events do not trigger respiratory illness surges, suggesting behavioral crowding is not the primary seasonal driver2. Additionally, Gavenčiak et al. found their seasonality estimate was robust to adjusting for country-level mobility data, further indicating the seasonal signal is not primarily behavioral.
|
risk of death, 45.0% lower, RR 0.55, p < 0.001, sunlight.
|
|
risk of death, 47.0% lower, RR 0.53, p < 0.001, UV Index.
|
|
risk of death, 38.0% lower, RR 0.62, p = 0.02, temperature.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Razi et al., 26 Mar 2026, retrospective, multiple countries, peer-reviewed, 2 authors, study period 21 January, 2020 - 10 January, 2023, per one std. dev. increase.
Abstract: Article
A Study on the Impact of Sunlight, Ultraviolet Radiation, and
Temperature Variability on COVID-19 Mortality: Spatiotemporal
Evidence from Small Countries and U.S. States and Territories
Murat Razi
and Manuel Graña *
Computational Intelligence Group, University of the Basque Country UPV/EHU, 20018 San Sebastian, Spain;
mrazi001@ikasle.ehu.eus
* Correspondence: manuel.grana@ehu.eus
Abstract
Academic Editor: Bruno Mégarbané
Received: 3 February 2026
Revised: 10 March 2026
Accepted: 22 March 2026
Published: 26 March 2026
Copyright: © 2026 by the authors.
Objectives: While the previous literature has established that meteorological conditions are
associated with COVID-19 mortality fluctuations, the relative effect of each of these highly
correlated factors remains unclear. This study aims to conduct a comparative analysis to determine which of three main meteorological variables—Ambient Temperature, Ultraviolet
(UV) Index, and Sunlight Duration—have the strongest negative association with COVID19 mortality. The objective is to quantify and rank their impact over a 7-to-21-day biological
exposure window. Methods: We conducted retrospective spatiotemporal analyses in the
form of panel Poisson Distributed Lag Models (PDLMs) regression using daily data from
21 January 2020 to 10 January 2023, spanning 129 distinct geographical regions worldwide.
To ensure a direct and fair comparison of effect sizes, all meteorological and environmental
variables were Z-score standardized. We estimated three independent PDLMs—each focusing separately on UV Index, Ambient Temperature, and Sunlight Duration—with lags
ranging from 7 to 21 days. These models controlled for overarching time trends and utilized
a categorical variable to account for Region Fixed Effects modeling time-invariant regional
health and socioeconomic determinants (e.g., obesity, age demographics, healthcare capacity). Furthermore, distributed lags of daily PM2.5 (air pollution) and relative humidity
were explicitly included in each model as dynamic confounders. Results: The comparison
of PDLM results reveals that the UV Index has the strongest negative association with
COVID-19 mortality. A one standard deviation increase in the UV Index corresponds
to a massive, highly significant cumulative reduction in deaths observed 1 to 3 weeks
later (p < 0.001). Sunlight Duration is the second-strongest protective meteorological factor,
whereas Ambient Temperature has the weakest effect. The distributed lags of particulate
matter (PM2.5) and relative humidity were found to be statistically insignificant when modeled alongside the meteorological variables. Conclusions: After standardizing variables
and controlling for dynamic environmental confounders like air pollution and humidity,
the study findings provide robust empirical evidence that meteorological conditions have a
strong significant association with COVID-19 mortality fluctuation with a temporal delay,
overcoming the confounding effects of merely dry or clear-air conditions.
Keywords: COVID-19 mortality; Distributed Lag Model; Poisson regression; UV index;
temperature; sunlight; environmental epidemiology
Licensee MDPI, Basel, Switzerland.
This article is an open access article
distributed under the terms and
conditions of the Creative Commons
Attribution (CC BY) license.
COVID 2026, 6, 56
https://doi.org/10.3390/covid6040056
COVID 2026, 6, 56
2 of 14
DOI record:
{
"DOI": "10.3390/covid6040056",
"ISSN": [
"2673-8112"
],
"URL": "http://dx.doi.org/10.3390/covid6040056",
"abstract": "<jats:p>Objectives: While the previous literature has established that meteorological conditions are associated with COVID-19 mortality fluctuations, the relative effect of each of these highly correlated factors remains unclear. This study aims to conduct a comparative analysis to determine which of three main meteorological variables—Ambient Temperature, Ultraviolet (UV) Index, and Sunlight Duration—have the strongest negative association with COVID-19 mortality. The objective is to quantify and rank their impact over a 7-to-21-day biological exposure window. Methods: We conducted retrospective spatiotemporal analyses in the form of panel Poisson Distributed Lag Models (PDLMs) regression using daily data from 21 January 2020 to 10 January 2023, spanning 129 distinct geographical regions worldwide. To ensure a direct and fair comparison of effect sizes, all meteorological and environmental variables were Z-score standardized. We estimated three independent PDLMs—each focusing separately on UV Index, Ambient Temperature, and Sunlight Duration—with lags ranging from 7 to 21 days. These models controlled for overarching time trends and utilized a categorical variable to account for Region Fixed Effects modeling time-invariant regional health and socioeconomic determinants (e.g., obesity, age demographics, healthcare capacity). Furthermore, distributed lags of daily PM2.5 (air pollution) and relative humidity were explicitly included in each model as dynamic confounders. Results: The comparison of PDLM results reveals that the UV Index has the strongest negative association with COVID-19 mortality. A one standard deviation increase in the UV Index corresponds to a massive, highly significant cumulative reduction in deaths observed 1 to 3 weeks later (p < 0.001). Sunlight Duration is the second-strongest protective meteorological factor, whereas Ambient Temperature has the weakest effect. The distributed lags of particulate matter (PM2.5) and relative humidity were found to be statistically insignificant when modeled alongside the meteorological variables. Conclusions: After standardizing variables and controlling for dynamic environmental confounders like air pollution and humidity, the study findings provide robust empirical evidence that meteorological conditions have a strong significant association with COVID-19 mortality fluctuation with a temporal delay, overcoming the confounding effects of merely dry or clear-air conditions.</jats:p>",
"alternative-id": [
"covid6040056"
],
"author": [
{
"ORCID": "https://orcid.org/0009-0008-2603-6825",
"affiliation": [
{
"name": "Computational Intelligence Group, University of the Basque Country UPV/EHU, 20018 San Sebastian, Spain"
}
],
"authenticated-orcid": false,
"family": "Razi",
"given": "Murat",
"sequence": "first"
},
{
"ORCID": "https://orcid.org/0000-0001-7373-4097",
"affiliation": [
{
"name": "Computational Intelligence Group, University of the Basque Country UPV/EHU, 20018 San Sebastian, Spain"
}
],
"authenticated-orcid": false,
"family": "Graña",
"given": "Manuel",
"sequence": "additional"
}
],
"container-title": "COVID",
"container-title-short": "COVID",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2026,
3,
26
]
],
"date-time": "2026-03-26T13:50:15Z",
"timestamp": 1774533015000
},
"deposited": {
"date-parts": [
[
2026,
3,
26
]
],
"date-time": "2026-03-26T14:20:11Z",
"timestamp": 1774534811000
},
"indexed": {
"date-parts": [
[
2026,
3,
26
]
],
"date-time": "2026-03-26T15:16:28Z",
"timestamp": 1774538188554,
"version": "3.50.1"
},
"is-referenced-by-count": 0,
"issue": "4",
"issued": {
"date-parts": [
[
2026,
3,
26
]
]
},
"journal-issue": {
"issue": "4",
"published-online": {
"date-parts": [
[
2026,
4
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2026,
3,
26
]
],
"date-time": "2026-03-26T00:00:00Z",
"timestamp": 1774483200000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/2673-8112/6/4/56/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "56",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2026,
3,
26
]
]
},
"published-online": {
"date-parts": [
[
2026,
3,
26
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"DOI": "10.4159/DLCL.hippocrates_cos-airs_waters_places.1923",
"doi-asserted-by": "crossref",
"key": "ref_1",
"unstructured": "Hippocrates, V. (1923). Ancient Medicine: Airs, Waters, Places; Epidemics 1 and 3; The Oath, Harvard University Press. Precepts; Nutriment. W. H. S. Jones. Loeb Classical Library 147, Trans."
},
{
"DOI": "10.1128/mbio.01426-23",
"article-title": "Seasonality of endemic COVID-19",
"author": "Townsend",
"doi-asserted-by": "crossref",
"first-page": "e01426-23",
"journal-title": "MBio",
"key": "ref_2",
"volume": "14",
"year": "2023"
},
{
"DOI": "10.1016/j.envres.2021.110874",
"article-title": "The role of seasonality in the spread of COVID-19 pandemic",
"author": "Liu",
"doi-asserted-by": "crossref",
"first-page": "110874",
"journal-title": "Environ. Res.",
"key": "ref_3",
"volume": "195",
"year": "2021"
},
{
"DOI": "10.1086/605435",
"article-title": "Are meteorological parameters associated with acute respiratory tract infections?",
"author": "Puppe",
"doi-asserted-by": "crossref",
"first-page": "861",
"journal-title": "Clin. Infect. Dis.",
"key": "ref_4",
"volume": "49",
"year": "2009"
},
{
"DOI": "10.1146/annurev-virology-012420-022445",
"article-title": "Seasonality of respiratory viral infections",
"author": "Moriyama",
"doi-asserted-by": "crossref",
"first-page": "83",
"journal-title": "Annu. Rev. Virol.",
"key": "ref_5",
"volume": "7",
"year": "2020"
},
{
"DOI": "10.1016/j.envres.2022.112711",
"article-title": "COVID-19 pandemic over 2020 (with lockdowns) and 2021 (with vaccinations): Similar effects for seasonality and environmental factors",
"author": "Coccia",
"doi-asserted-by": "crossref",
"first-page": "112711",
"journal-title": "Environ. Res.",
"key": "ref_6",
"volume": "208",
"year": "2022"
},
{
"DOI": "10.1177/0748730420987322",
"article-title": "Drivers of infectious disease seasonality: Potential implications for COVID-19",
"author": "Stevenson",
"doi-asserted-by": "crossref",
"first-page": "35",
"journal-title": "J. Biol. Rhythm.",
"key": "ref_7",
"volume": "36",
"year": "2021"
},
{
"DOI": "10.1016/j.envres.2021.112614",
"article-title": "COVID-19 seasonality in temperate countries",
"author": "Marmiere",
"doi-asserted-by": "crossref",
"first-page": "112614",
"journal-title": "Environ. Res.",
"key": "ref_8",
"volume": "206",
"year": "2022"
},
{
"DOI": "10.3389/fpubh.2020.567184",
"article-title": "Seasonality of respiratory viral infections: Will COVID-19 follow suit?",
"author": "Audi",
"doi-asserted-by": "crossref",
"first-page": "567184",
"journal-title": "Front. Public Health",
"key": "ref_9",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1155/2011/734690",
"article-title": "The effects of temperature and relative humidity on the viability of the SARS coronavirus",
"author": "Chan",
"doi-asserted-by": "crossref",
"first-page": "734690",
"journal-title": "Adv. Virol.",
"key": "ref_10",
"volume": "2011",
"year": "2011"
},
{
"DOI": "10.1146/annurev.publhealth.28.021406.144128",
"article-title": "Seasonality of infectious diseases",
"author": "Fisman",
"doi-asserted-by": "crossref",
"first-page": "127",
"journal-title": "Annu. Rev. Public Health",
"key": "ref_11",
"volume": "28",
"year": "2007"
},
{
"article-title": "Coronavirus infections in working adults: Eight-year study with 229 E and OC 43",
"author": "Hendley",
"first-page": "805",
"journal-title": "Am. Rev. Respir. Dis.",
"key": "ref_12",
"volume": "105",
"year": "1972"
},
{
"DOI": "10.1029/2021GH000413",
"article-title": "On the environmental determinants of COVID-19 seasonality",
"author": "Choi",
"doi-asserted-by": "crossref",
"first-page": "e2021GH000413",
"journal-title": "Geohealth",
"key": "ref_13",
"volume": "5",
"year": "2021"
},
{
"article-title": "Seasonality and its impact on COVID-19",
"author": "Edmunds",
"first-page": "1",
"journal-title": "Sage",
"key": "ref_14",
"volume": "63",
"year": "2020"
},
{
"DOI": "10.1016/j.psep.2021.06.043",
"article-title": "Exploring the linkage between seasonality of environmental factors and COVID-19 waves in Madrid, Spain",
"author": "Zoran",
"doi-asserted-by": "crossref",
"first-page": "583",
"journal-title": "Process Saf. Environ. Prot.",
"key": "ref_15",
"volume": "152",
"year": "2021"
},
{
"DOI": "10.1016/j.medcli.2021.10.010",
"article-title": "Influence of weather factors on the incidence of COVID-19 in Spain",
"author": "Valero",
"doi-asserted-by": "crossref",
"first-page": "255",
"journal-title": "Med. Clínica (Engl. Ed.)",
"key": "ref_16",
"volume": "159",
"year": "2022"
},
{
"DOI": "10.3390/jcm13020334",
"doi-asserted-by": "crossref",
"key": "ref_17",
"unstructured": "Quinn, G.A., Connolly, M., Fenton, N.E., Hatfill, S.J., Hynds, P., ÓhAiseadha, C., Sikora, K., Soon, W., and Connolly, R. (2024). Influence of seasonality and public-health interventions on the COVID-19 pandemic in northern Europe. J. Clin. Med., 13."
},
{
"DOI": "10.1093/ofid/ofaa443",
"article-title": "Global seasonality of human coronaviruses: A systematic review",
"author": "Park",
"doi-asserted-by": "crossref",
"first-page": "ofaa443",
"journal-title": "Proceedings of the Open Forum Infectious Diseases",
"key": "ref_18",
"volume": "Volume 7",
"year": "2020"
},
{
"article-title": "Factors influencing the seasonal patterns of infectious diseases",
"author": "Fares",
"first-page": "128",
"journal-title": "Int. J. Prev. Med.",
"key": "ref_19",
"volume": "4",
"year": "2013"
},
{
"DOI": "10.3201/eid0703.017301",
"article-title": "Seasonal variation in host susceptibility and cycles of certain infectious diseases",
"author": "Dowell",
"doi-asserted-by": "crossref",
"first-page": "369",
"journal-title": "Emerg. Infect. Dis.",
"key": "ref_20",
"volume": "7",
"year": "2001"
},
{
"DOI": "10.1128/JVI.01680-06",
"article-title": "Influenza seasonality: Underlying causes and modeling theories",
"author": "Lofgren",
"doi-asserted-by": "crossref",
"first-page": "5429",
"journal-title": "J. Virol.",
"key": "ref_21",
"volume": "81",
"year": "2007"
},
{
"DOI": "10.1111/j.1469-0691.2012.03968.x",
"article-title": "Seasonality of viral infections: Mechanisms and unknowns",
"author": "Fisman",
"doi-asserted-by": "crossref",
"first-page": "946",
"journal-title": "Clin. Microbiol. Infect.",
"key": "ref_22",
"volume": "18",
"year": "2012"
},
{
"DOI": "10.1371/journal.pone.0342510",
"doi-asserted-by": "crossref",
"key": "ref_23",
"unstructured": "Stamper, A., and Baker, R.E. (2026). Spatial patterns and environmental influences of COVID-19 outbreaks, post-Omicron. PLoS ONE, 21."
},
{
"DOI": "10.1073/pnas.2008590117",
"article-title": "Seasonality and uncertainty in global COVID-19 growth rates",
"author": "Merow",
"doi-asserted-by": "crossref",
"first-page": "27456",
"journal-title": "Proc. Natl. Acad. Sci. USA",
"key": "ref_24",
"volume": "117",
"year": "2020"
},
{
"DOI": "10.1016/j.scitotenv.2020.139016",
"article-title": "Sunlight exposure increased Covid-19 recovery rates: A study in the central pandemic area of Indonesia",
"author": "Asyary",
"doi-asserted-by": "crossref",
"first-page": "139016",
"journal-title": "Sci. Total Environ.",
"key": "ref_25",
"volume": "729",
"year": "2020"
},
{
"DOI": "10.1073/pnas.2012370118",
"article-title": "Global evidence for ultraviolet radiation decreasing COVID-19 growth rates",
"author": "Carleton",
"doi-asserted-by": "crossref",
"first-page": "e2012370118",
"journal-title": "Proc. Natl. Acad. Sci. USA",
"key": "ref_26",
"volume": "118",
"year": "2021"
},
{
"DOI": "10.1371/journal.ppat.1007327",
"doi-asserted-by": "crossref",
"key": "ref_27",
"unstructured": "Martinez, M.E. (2018). The calendar of epidemics: Seasonal cycles of infectious diseases. PLoS Pathog., 14."
},
{
"article-title": "Generalized linear models",
"author": "Nelder",
"first-page": "370",
"journal-title": "J. R. Stat. Soc. Ser. A Stat. Soc.",
"key": "ref_28",
"volume": "135",
"year": "1972"
},
{
"DOI": "10.1017/CBO9781139013567",
"doi-asserted-by": "crossref",
"key": "ref_29",
"unstructured": "Cameron, A.C., and Trivedi, P.K. (2013). Regression Analysis of Count Data, Cambridge University Press. Number 53."
},
{
"key": "ref_30",
"unstructured": "Wooldridge, J.M. (2010). Econometric Analysis of Cross Section and Panel Data, MIT Press."
},
{
"key": "ref_31",
"unstructured": "Shumway, R.H., and Stoffer, D.S. (2006). Time Series Analysis and Its Applications: With R Examples, Springer."
},
{
"DOI": "10.1093/ije/dyt092",
"article-title": "Time series regression studies in environmental epidemiology",
"author": "Bhaskaran",
"doi-asserted-by": "crossref",
"first-page": "1187",
"journal-title": "Int. J. Epidemiol.",
"key": "ref_32",
"volume": "42",
"year": "2013"
},
{
"DOI": "10.32614/CRAN.package.arm",
"doi-asserted-by": "crossref",
"key": "ref_33",
"unstructured": "Gelman, A., and Hill, J. (2007). Data Analysis Using Regression and Multilevel/Hierarchical Models, Cambridge University Press."
},
{
"key": "ref_34",
"unstructured": "Baltagi, B.H. (2008). Econometric Analysis of Panel Data, Springer."
},
{
"DOI": "10.1007/s11135-006-9018-6",
"article-title": "A caution regarding rules of thumb for variance inflation factors",
"doi-asserted-by": "crossref",
"first-page": "673",
"journal-title": "Qual. Quant.",
"key": "ref_35",
"volume": "41",
"year": "2007"
},
{
"DOI": "10.1093/infdis/jiaa274",
"article-title": "Simulated sunlight rapidly inactivates SARS-CoV-2 on surfaces",
"author": "Williams",
"doi-asserted-by": "crossref",
"first-page": "214",
"journal-title": "J. Infect. Dis.",
"key": "ref_36",
"volume": "222",
"year": "2020"
},
{
"DOI": "10.1093/infdis/jiaa334",
"article-title": "Airborne SARS-CoV-2 is rapidly inactivated by simulated sunlight",
"author": "Schuit",
"doi-asserted-by": "crossref",
"first-page": "564",
"journal-title": "J. Infect. Dis.",
"key": "ref_37",
"volume": "222",
"year": "2020"
},
{
"DOI": "10.20944/preprints202003.0235.v2",
"doi-asserted-by": "crossref",
"key": "ref_38",
"unstructured": "Grant, W.B., Lahore, H., McDonnell, S.L., Baggerly, C.A., French, C.B., Aliano, J.L., and Bhattoa, H.P. (2020). Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths. Nutrients, 12."
},
{
"DOI": "10.1038/s41598-022-19898-8",
"article-title": "Investigating the effects of absolute humidity and movement on COVID-19 seasonality in the United States",
"author": "Lin",
"doi-asserted-by": "crossref",
"first-page": "16729",
"journal-title": "Sci. Rep.",
"key": "ref_39",
"volume": "12",
"year": "2022"
},
{
"DOI": "10.1056/NEJMc2004973",
"article-title": "Aerosol and surface stability of SARS-CoV-2 as compared with SARS-CoV-1",
"author": "Bushmaker",
"doi-asserted-by": "crossref",
"first-page": "1564",
"journal-title": "N. Engl. J. Med.",
"key": "ref_40",
"volume": "382",
"year": "2020"
}
],
"reference-count": 40,
"references-count": 40,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/2673-8112/6/4/56"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [],
"subtitle": [],
"title": "A Study on the Impact of Sunlight, Ultraviolet Radiation, and Temperature Variability on COVID-19 Mortality: Spatiotemporal Evidence from Small Countries and U.S. States and Territories",
"type": "journal-article",
"update-policy": "https://doi.org/10.3390/mdpi_crossmark_policy",
"volume": "6"
}
