The role of probiotics in coronavirus disease-19 infection in Wuhan: A retrospective study of 311 severe patients
et al., International Immunopharmacology, doi:10.1016/j.intimp.2021.107531, Mar 2021
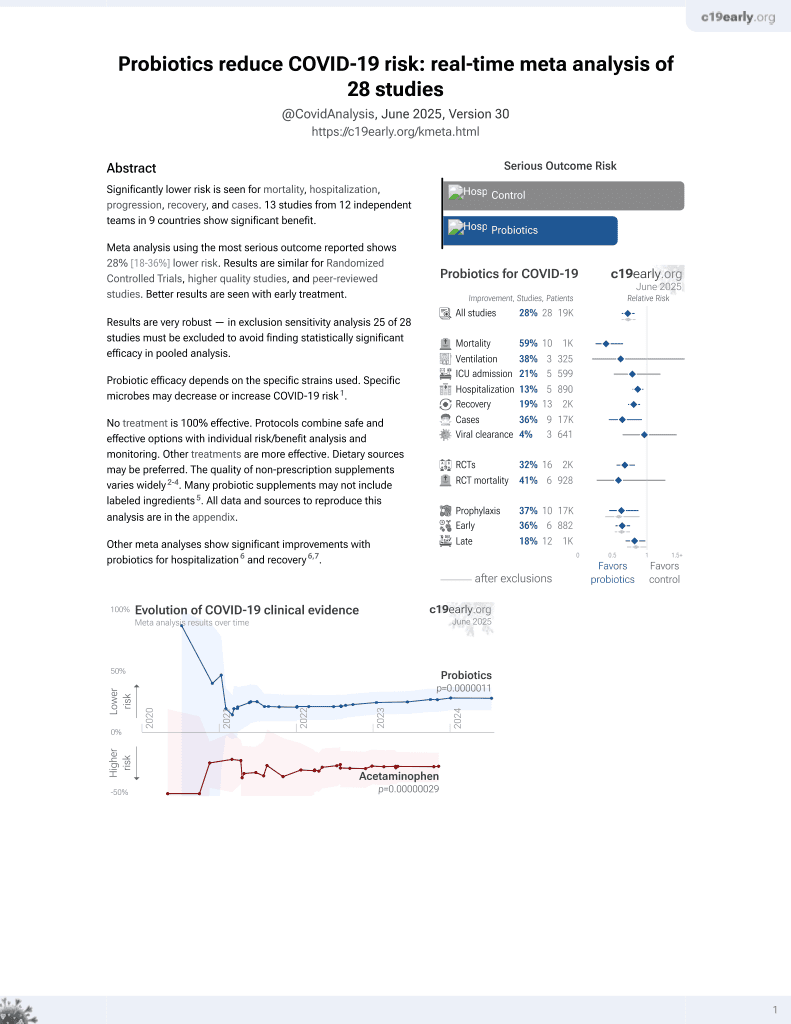
Probiotics for COVID-19
19th treatment shown to reduce risk in
March 2021, now with p = 0.00000044 from 29 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
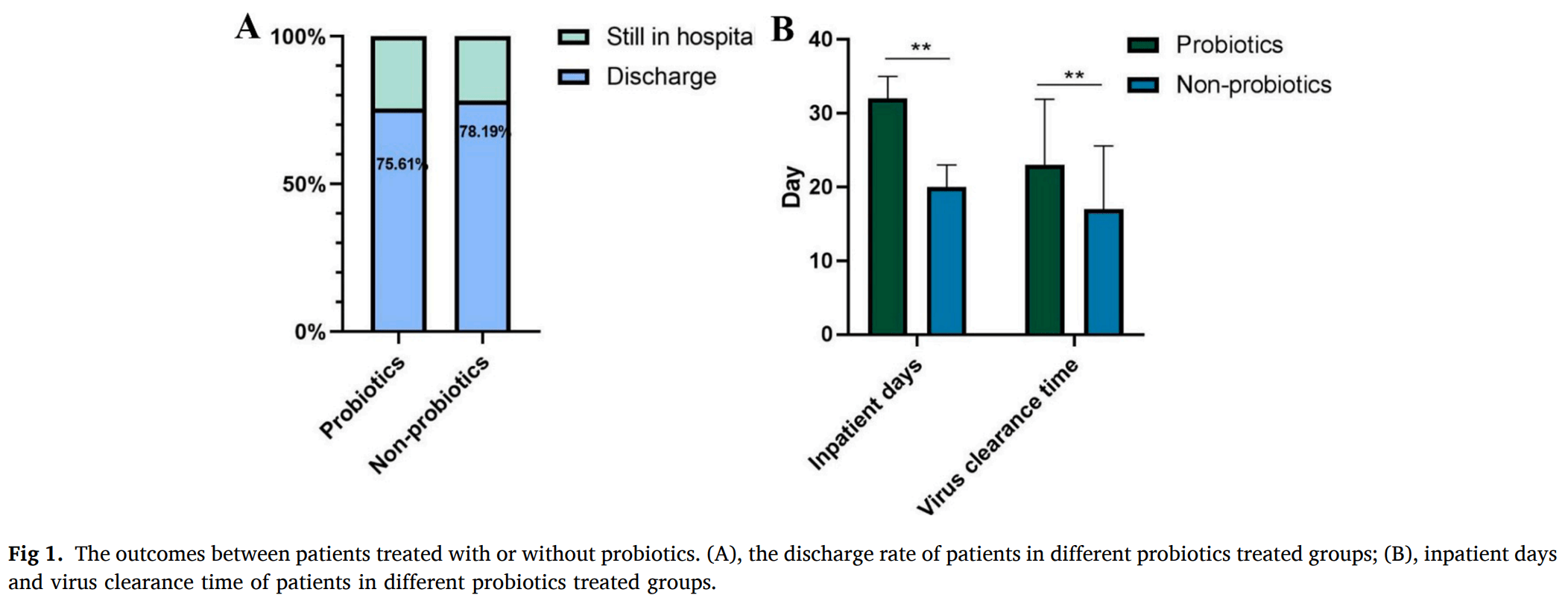
Retrospective 311 severe condition hospitalized patients in China, 123 treated with probiotics, showing slower viral clearance and recovery with treatment. Authors note that probiotics were able to moderate immunity and decrease the incidence of secondary infections.
Probiotic efficacy depends on the specific strains used. Specific microbes may decrease or increase COVID-19 risk1.
Viral load measured by PCR may not accurately reflect infectious virus measured by viral culture. Porter et al. show that viral load early in infection was correlated with infectious virus, but viral load late in infection could be high even with low or undetectable infectious virus. Assessing viral load later in infection may underestimate reductions in infectious virus with treatment.
Standard of Care (SOC) for COVID-19 in the study country,
China, is poor with low average efficacy for approved treatments3.
|
risk of no hospital discharge, 11.8% higher, RR 1.12, p = 0.68, treatment 30 of 123 (24.4%), control 41 of 188 (21.8%).
|
|
time to discharge, 60.0% higher, relative time 1.60, p < 0.001, treatment 123, control 188.
|
|
time to viral-, 35.3% higher, relative time 1.35, p < 0.001, treatment 123, control 188.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
1.
Li et al., Large-scale genetic correlation studies explore the causal relationship and potential mechanism between gut microbiota and COVID-19-associated risks, BMC Microbiology, doi:10.1186/s12866-024-03423-0.
Li et al., 5 Mar 2021, retrospective, China, peer-reviewed, 7 authors, average treatment delay 13.0 days.
The role of probiotics in coronavirus disease-19 infection in Wuhan: A retrospective study of 311 severe patients
International Immunopharmacology, doi:10.1016/j.intimp.2021.107531
Since January 2020 Elsevier has created a COVID-19 resource centre with free information in English and Mandarin on the novel coronavirus COVID-19. The COVID-19 resource centre is hosted on Elsevier Connect, the company's public news and information website. Elsevier hereby grants permission to make all its COVID-19-related research that is available on the COVID-19 resource centre -including this research content -immediately available in PubMed Central and other publicly funded repositories, such as the WHO COVID database with rights for unrestricted research re-use and analyses in any form or by any means with acknowledgement of the original source. These permissions are granted for free by Elsevier for as long as the COVID-19 resource centre remains active.
References
Aziz, Fatima, Assaly, Elevated Interleukin-6 and Severe COVID-19: A Meta-Analysis, J. Med. Virol
Bao, Li, Zhang, Kang, Chen et al., Comparative analysis of laboratory indexes of severe and non-severe patients infected with COVID-19, Clin. Chim. Acta
Baud, Dimopoulou Agri, Gibson, Reid, Giannoni, Using Probiotics to Flatten the Curve of Coronavirus Disease COVID-2019 Pandemic, Front. Public Health
Bozkurt, Quigley, The probiotic Bifidobacterium in the management of Coronavirus: A theoretical basis, Int.. J. Immunopathol. Pharmacol
Cao, Wang, Wen, Liu, Wang et al., A Trial of Lopinavir-Ritonavir in Adults Hospitalized with Severe Covid-19, New Engl. J. Med
Chan, Wong, Tang, COVID-19: An Update on the Epidemiological, Clinical, Preventive and Therapeutic Evidence and Guidelines of Integrative Chinese-Western Medicine for the Management of 2019 Novel Coronavirus Disease, Am. J. Chin. Med
Cole-Jeffrey, Liu, Katovich, Raizada, Shenoy, ACE2 and Microbiota: Emerging Targets for Cardiopulmonary Disease Therapy, J. Cardiovasc. Pharmacol
Coomes, Haghbayan, Interleukin-6 in Covid-19: A systematic review andmeta-analysis, Rev. Med. Virol
Cox, Pyne, Saunders, Fricker, Oral administration of the probiotic Lactobacillus fermentum VRI-003 and mucosal immunity in endurance athletes, Br. J. Sports Med
Cui, Jiang, Hao, Qu, Hu, New advances in exopolysaccharides production of Streptococcus thermophilus, Arch. Microbiol
Di Renzo, Gualtieri, Pivari, Soldati, Attinà et al., COVID-19: Is there a role for immunonutrition in obese patient?, J. Transl. Med
Diao, Wang, Tan, Chen, Liu et al., Reduction and Functional Exhaustion of T Cells in Patients with Coronavirus Disease, COVID
Din, Mazhar, Waseem, Ahmad, Bibi et al., SARS-CoV-2 microbiome dysbiosis linked disorders and possible probiotics role, Biomed. Pharmacother
Ettinger, Macdonald, Reid, Burton, The influence of the human microbiome and probiotics on cardiovascular health, Gut Microbes
Gao, Howden, Stinear, Evolution of virulence in Enterococcus faecium, a hospital-adapted opportunistic pathogen, Curr. Opin. Microbiol
Gombart, Pierre, Maggini, A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection, Nutrients
Gorbalenya, Baker, Baric, De Groot, Drosten et al., Coronaviridae Study Group of the International Committee on Taxonomy of, The species Severe acute respiratory syndrome-related coronavirus: classifying 2019-nCoV and naming it SARS-CoV-2, Nature Microbiol
Hu, Zhang, Lin, Tang, Chan et al., Review article: Probiotics, prebiotics and dietary approaches during COVID-19 pandemic, Trends Food Sci. Technol
Huang, Wang, Li, Ren, Zhao et al., Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet
Hur, Lee, Gut Microbiota and Metabolic Disorders, Diabetes Metab. J
Imai, Kuba, Ohto-Nakanishi, Penninger, Angiotensin-converting enzyme 2 (ACE2) in disease pathogenesis, Circ. J.: Official J. Jpn. Circ. Soc
Isolauri, Sütas, Kankaanpää, Arvilommi, Salminen, Probiotics: effects on immunity, The American journal of clinical nutrition
Kanauchi, Andoh, Abubakar, Yamamoto, Probiotics and Paraprobiotics in Viral Infection: Clinical Application and Effects on the Innate and Acquired Immune Systems, Curr. Pharm. Des
Kawahara, Takahashi, Oishi, Tanaka, Masuda et al., Consecutive oral administration of Bifidobacterium longum MM-2 improves the defense system against influenza virus infection by enhancing natural killer cell activity in a murine model, Microbiol. Immunol
Ling, C-reactive protein levels in the early stage of COVID-19, Med. Maladies Infectieuses
Liu, Hu, Xu, Ding, Zhu, Characterization of Bacillus cereus in Dairy Products in China, Toxins
Liu, Zhang, Yang, Zhang, Yi, The Potential Role of IL-6 in Monitoring Coronavirus Disease
Losick, Bacillus subtilis: a bacterium for all seasons, Curr. Biol.: CB
Lu, Drug treatment options for the 2019-new coronavirus (2019-nCoV), BioSci. Trends
Lu, Hu, Fan, Liu, Yin et al., for patients with confirmed or suspected severe acute respiratory syndrome coronavirus 2 disease (COVID-19) during the early stage of outbreak in Wuhan
Lu, Zhao, Li, Niu, Yang et al., Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding, Lancet
Luo, Zhou, Yan, Guo, Wang et al., Prognostic value of C-reactive protein in patients with COVID-19
Mahooti, Miri, Abdolalipour, Ghaemi, The immunomodulatory effects of probiotics on respiratory viral infections: A hint for COVID-19 treatment?, Microb. Pathog
Mohtashami, Mohamadi, Azimi-Nezhad, Saeidi, Nia et al., Lactobacillus bulgaricus and Lactobacillus plantarum improve diabetic wound healing through modulating inflammatory factors, Biotechnol. Appl. Biochem. n/a
Oliva, Di Nardo, Ferrari, Mallardo, Rossi et al., Randomised clinical trial: the effectiveness of Lactobacillus reuteri ATCC 55730 rectal enema in children with active distal ulcerative colitis, Aliment. Pharmacol. Ther
Panel On Dietetic, Products, Allergies, Guidance on the scientific requirements for health claims related to the immune system, the gastrointestinal tract and defence against pathogenic microorganisms
Phelan, Katz, Gostin, The Novel Coronavirus Originating in Wuhan, China Challenges for Global Health Governance, JAMA-J. Am. Med. Assoc
Rozga, Cheng, Handu, Effects of Probiotics in Conditions or Infections Similar to COVID-19 on Health Outcomes: An Evidence Analysis Center Scoping Review, J. Acad. Nutr. Diet
Sheng, He, Sun, Zhang, Kong et al., Synbiotic supplementation containing Bifidobacterium infantis and xylooligosaccharides alleviates dextran sulfate sodium-induced ulcerative colitis, Food Funct
Sundararaman, Ray, Ravindra, Halami, Role of probiotics to combat viral infections with emphasis on COVID-19, Appl. Microbiol. Biotechnol
Taghizadeh Moghaddam, Javadi, Matin, Reduction of bisphenol A by Lactobacillus acidophilus and Lactobacillus plantarum in yoghurt, Int. J. Dairy Technol
Wan, Forsythe, El-Nezami, Probiotics interaction with foodborne pathogens: a potential alternative to antibiotics and future challenges, Crit. Rev. Food Sci. Nutr
Wu, Lewis, Pae, Meydani, Nutritional Modulation of Immune Function: Analysis of Evidence, Mechanisms, and Clinical Relevance, Front. Immunol
Wu, Xiao, Zhang, Gu, Lee et al., SARS-CoV-2 titers in wastewater are higher than expected from clinically confirmed cases
Zeng, Wang, Zhang, Qi, Wang et al., Effect of probiotics on the incidence of ventilator-associated pneumonia in critically ill patients: a randomized controlled multicenter trial, Intensive Care Med
Zhang, Yu, Zhao, Zhang, Zhai et al., Colonization and probiotic function of Bifidobacterium longum, J. Funct. Foods
Zhou, Li, Qian, Lin, Nan et al., Predicting the Risk of Clinical Deterioration in Patients with Severe COVID-19 Infection Using Machine Learning, SSRN Electron. J
Zolnikova, Komkova, Potskherashvili, Trukhmanov, Ivashkin, Application of probiotics for acute respiratory tract infections, Italian J. Med
DOI record:
{
"DOI": "10.1016/j.intimp.2021.107531",
"ISSN": [
"1567-5769"
],
"URL": "http://dx.doi.org/10.1016/j.intimp.2021.107531",
"alternative-id": [
"S1567576921001673"
],
"article-number": "107531",
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "The role of probiotics in coronavirus disease-19 infection in Wuhan: A retrospective study of 311 severe patients"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "International Immunopharmacology"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.intimp.2021.107531"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2021 Elsevier B.V. All rights reserved."
}
],
"author": [
{
"affiliation": [],
"family": "Li",
"given": "Qiang",
"sequence": "first"
},
{
"affiliation": [],
"family": "Cheng",
"given": "Fang",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Xu",
"given": "Qiling",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Su",
"given": "Yuyong",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Cai",
"given": "Xuefeng",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Zeng",
"given": "Fang",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Zhang",
"given": "Yu",
"sequence": "additional"
}
],
"container-title": "International Immunopharmacology",
"container-title-short": "International Immunopharmacology",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2021,
3,
7
]
],
"date-time": "2021-03-07T14:30:45Z",
"timestamp": 1615127445000
},
"deposited": {
"date-parts": [
[
2023,
4,
15
]
],
"date-time": "2023-04-15T09:10:11Z",
"timestamp": 1681549811000
},
"funder": [
{
"DOI": "10.13039/501100012166",
"award": [
"2017YFC0909900"
],
"doi-asserted-by": "publisher",
"name": "National Key Research and Development Program of China"
}
],
"indexed": {
"date-parts": [
[
2024,
4,
1
]
],
"date-time": "2024-04-01T15:20:16Z",
"timestamp": 1711984816699
},
"is-referenced-by-count": 34,
"issued": {
"date-parts": [
[
2021,
6
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
1
]
],
"date-time": "2021-06-01T00:00:00Z",
"timestamp": 1622505600000
}
},
{
"URL": "https://doi.org/10.15223/policy-017",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
1
]
],
"date-time": "2021-06-01T00:00:00Z",
"timestamp": 1622505600000
}
},
{
"URL": "https://doi.org/10.15223/policy-037",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
1
]
],
"date-time": "2021-06-01T00:00:00Z",
"timestamp": 1622505600000
}
},
{
"URL": "https://doi.org/10.15223/policy-012",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
1
]
],
"date-time": "2021-06-01T00:00:00Z",
"timestamp": 1622505600000
}
},
{
"URL": "https://doi.org/10.15223/policy-029",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
1
]
],
"date-time": "2021-06-01T00:00:00Z",
"timestamp": 1622505600000
}
},
{
"URL": "https://doi.org/10.15223/policy-004",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
6,
1
]
],
"date-time": "2021-06-01T00:00:00Z",
"timestamp": 1622505600000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S1567576921001673?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S1567576921001673?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "107531",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
6
]
]
},
"published-print": {
"date-parts": [
[
2021,
6
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1001/jama.2020.1097",
"article-title": "The Novel Coronavirus Originating in Wuhan, China Challenges for Global Health Governance",
"author": "Phelan",
"doi-asserted-by": "crossref",
"first-page": "709",
"issue": "8",
"journal-title": "JAMA-J. Am. Med. Assoc.",
"key": "10.1016/j.intimp.2021.107531_b0005",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1038/s41564-020-0695-z",
"article-title": "The species Severe acute respiratory syndrome-related coronavirus: classifying 2019-nCoV and naming it SARS-CoV-2",
"author": "Gorbalenya",
"doi-asserted-by": "crossref",
"first-page": "536",
"issue": "4",
"journal-title": "Nature Microbiol.",
"key": "10.1016/j.intimp.2021.107531_b0010",
"volume": "5",
"year": "2020"
},
{
"article-title": "COVID-19: An Update on the Epidemiological, Clinical, Preventive and Therapeutic Evidence and Guidelines of Integrative Chinese-Western Medicine for the Management of 2019 Novel Coronavirus Disease",
"author": "Chan",
"first-page": "1",
"journal-title": "Am. J. Chin. Med.",
"key": "10.1016/j.intimp.2021.107531_b0015",
"year": "2020"
},
{
"key": "10.1016/j.intimp.2021.107531_b0020",
"unstructured": "New coronavirus pneumonial prevention and control program (version 7.0) (in Chinese), 2020. http://www.nhc.gov.cn/xcs/zhengcwj/202003/46c9294a7dfe4cef80dc7f5912eb1989.shtml."
},
{
"DOI": "10.1016/j.biopha.2020.110947",
"article-title": "SARS-CoV-2 microbiome dysbiosis linked disorders and possible probiotics role",
"author": "Din",
"doi-asserted-by": "crossref",
"journal-title": "Biomed. Pharmacother.",
"key": "10.1016/j.intimp.2021.107531_b0025",
"volume": "133",
"year": "2021"
},
{
"DOI": "10.4093/dmj.2015.39.3.198",
"article-title": "Gut Microbiota and Metabolic Disorders",
"author": "Hur",
"doi-asserted-by": "crossref",
"first-page": "198",
"issue": "3",
"journal-title": "Diabetes Metab. J.",
"key": "10.1016/j.intimp.2021.107531_b0030",
"volume": "39",
"year": "2015"
},
{
"DOI": "10.1101/2020.04.05.20051540",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2021.107531_b0035",
"unstructured": "F. Wu, A. Xiao, J. Zhang, X. Gu, W.L. Lee, K. Kauffman, W. Hanage, M. Matus, N. Ghaeli, N. Endo, C. Duvallet, K. Moniz, T. Erickson, P. Chai, J. Thompson, E. Alm, SARS-CoV-2 titers in wastewater are higher than expected from clinically confirmed cases, 2020, 2020.04.05.20051540."
},
{
"DOI": "10.4081/itjm.2018.931",
"article-title": "Application of probiotics for acute respiratory tract infections",
"author": "Zolnikova",
"doi-asserted-by": "crossref",
"first-page": "32",
"issue": "1",
"journal-title": "Italian J. Med.",
"key": "10.1016/j.intimp.2021.107531_b0040",
"volume": "12",
"year": "2018"
},
{
"DOI": "10.1111/1348-0421.12210",
"article-title": "Consecutive oral administration of Bifidobacterium longum MM-2 improves the defense system against influenza virus infection by enhancing natural killer cell activity in a murine model",
"author": "Kawahara",
"doi-asserted-by": "crossref",
"first-page": "1",
"issue": "1",
"journal-title": "Microbiol. Immunol.",
"key": "10.1016/j.intimp.2021.107531_b0045",
"volume": "59",
"year": "2015"
},
{
"DOI": "10.1016/S0140-6736(20)30251-8",
"article-title": "Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding",
"author": "Lu",
"doi-asserted-by": "crossref",
"first-page": "565",
"issue": "10224",
"journal-title": "Lancet",
"key": "10.1016/j.intimp.2021.107531_b0050",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1253/circj.CJ-10-0045",
"article-title": "Angiotensin-converting enzyme 2 (ACE2) in disease pathogenesis",
"author": "Imai",
"doi-asserted-by": "crossref",
"first-page": "405",
"issue": "3",
"journal-title": "Circ. J.: Official J. Jpn. Circ. Soc.",
"key": "10.1016/j.intimp.2021.107531_b0055",
"volume": "74",
"year": "2010"
},
{
"DOI": "10.1097/FJC.0000000000000307",
"article-title": "ACE2 and Microbiota: Emerging Targets for Cardiopulmonary Disease Therapy",
"author": "Cole-Jeffrey",
"doi-asserted-by": "crossref",
"first-page": "540",
"issue": "6",
"journal-title": "J. Cardiovasc. Pharmacol.",
"key": "10.1016/j.intimp.2021.107531_b0060",
"volume": "66",
"year": "2015"
},
{
"DOI": "10.4161/19490976.2014.983775",
"article-title": "The influence of the human microbiome and probiotics on cardiovascular health",
"author": "Ettinger",
"doi-asserted-by": "crossref",
"first-page": "719",
"issue": "6",
"journal-title": "Gut Microbes",
"key": "10.1016/j.intimp.2021.107531_b0065",
"volume": "5",
"year": "2014"
},
{
"DOI": "10.3389/fimmu.2018.03160",
"article-title": "Nutritional Modulation of Immune Function: Analysis of Evidence, Mechanisms, and Clinical Relevance",
"author": "Wu",
"doi-asserted-by": "crossref",
"first-page": "3160",
"journal-title": "Front. Immunol.",
"key": "10.1016/j.intimp.2021.107531_b0070",
"volume": "9",
"year": "2018"
},
{
"DOI": "10.1093/ajcn/73.2.444s",
"article-title": "Probiotics: effects on immunity",
"author": "Isolauri",
"doi-asserted-by": "crossref",
"first-page": "444s",
"issue": "2 Suppl",
"journal-title": "The American journal of clinical nutrition",
"key": "10.1016/j.intimp.2021.107531_b0075",
"volume": "73",
"year": "2001"
},
{
"DOI": "10.1002/jmv.25948",
"article-title": "Elevated Interleukin-6 and Severe COVID-19: A Meta-Analysis",
"author": "Aziz",
"doi-asserted-by": "crossref",
"journal-title": "J. Med. Virol.",
"key": "10.1016/j.intimp.2021.107531_b0080",
"year": "2020"
},
{
"DOI": "10.2174/1381612824666180116163411",
"article-title": "Probiotics and Paraprobiotics in Viral Infection: Clinical Application and Effects on the Innate and Acquired Immune Systems",
"author": "Kanauchi",
"doi-asserted-by": "crossref",
"first-page": "710",
"issue": "6",
"journal-title": "Curr. Pharm. Des.",
"key": "10.1016/j.intimp.2021.107531_b0085",
"volume": "24",
"year": "2018"
},
{
"DOI": "10.3389/fpubh.2020.00186",
"article-title": "Using Probiotics to Flatten the Curve of Coronavirus Disease COVID-2019 Pandemic",
"author": "Baud",
"doi-asserted-by": "crossref",
"first-page": "186",
"journal-title": "Front. Public Health",
"key": "10.1016/j.intimp.2021.107531_b0090",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1111/j.1365-2036.2011.04939.x",
"article-title": "Randomised clinical trial: the effectiveness of Lactobacillus reuteri ATCC 55730 rectal enema in children with active distal ulcerative colitis",
"author": "Oliva",
"doi-asserted-by": "crossref",
"first-page": "327",
"issue": "3",
"journal-title": "Aliment. Pharmacol. Ther.",
"key": "10.1016/j.intimp.2021.107531_b0095",
"volume": "35",
"year": "2012"
},
{
"DOI": "10.1016/j.tifs.2020.12.009",
"article-title": "Review article: Probiotics, prebiotics and dietary approaches during COVID-19 pandemic",
"author": "Hu",
"doi-asserted-by": "crossref",
"first-page": "187",
"journal-title": "Trends Food Sci. Technol.",
"key": "10.1016/j.intimp.2021.107531_b0100",
"volume": "108",
"year": "2021"
},
{
"DOI": "10.1177/2058738420961304",
"article-title": "The probiotic Bifidobacterium in the management of Coronavirus: A theoretical basis",
"author": "Bozkurt",
"doi-asserted-by": "crossref",
"journal-title": "Int.. J. Immunopathol. Pharmacol.",
"key": "10.1016/j.intimp.2021.107531_b0105",
"volume": "34",
"year": "2020"
},
{
"DOI": "10.1007/s00134-016-4303-x",
"article-title": "Effect of probiotics on the incidence of ventilator-associated pneumonia in critically ill patients: a randomized controlled multicenter trial",
"author": "Zeng",
"doi-asserted-by": "crossref",
"first-page": "1018",
"issue": "6",
"journal-title": "Intensive Care Med.",
"key": "10.1016/j.intimp.2021.107531_b0110",
"volume": "42",
"year": "2016"
},
{
"DOI": "10.1186/s12967-020-02594-4",
"article-title": "COVID-19: Is there a role for immunonutrition in obese patient?",
"author": "Di Renzo",
"doi-asserted-by": "crossref",
"first-page": "415",
"issue": "1",
"journal-title": "J. Transl. Med.",
"key": "10.1016/j.intimp.2021.107531_b0115",
"volume": "18",
"year": "2020"
},
{
"DOI": "10.2903/j.efsa.2016.4369",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2021.107531_b0120",
"unstructured": "N. EFSA Panel on Dietetic Products, Allergies, Guidance on the scientific requirements for health claims related to the immune system, the gastrointestinal tract and defence against pathogenic microorganisms, 14(1) (2016) 4369."
},
{
"DOI": "10.3390/nu12010236",
"article-title": "A Review of Micronutrients and the Immune System-Working in Harmony to Reduce the Risk of Infection",
"author": "Gombart",
"doi-asserted-by": "crossref",
"issue": "1",
"journal-title": "Nutrients",
"key": "10.1016/j.intimp.2021.107531_b0125",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1039/D0FO00518E",
"article-title": "Synbiotic supplementation containing Bifidobacterium infantis and xylooligosaccharides alleviates dextran sulfate sodium-induced ulcerative colitis",
"author": "Sheng",
"doi-asserted-by": "crossref",
"first-page": "3964",
"issue": "5",
"journal-title": "Food Funct.",
"key": "10.1016/j.intimp.2021.107531_b0130",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1111/1471-0307.12706",
"article-title": "Reduction of bisphenol A by Lactobacillus acidophilus and Lactobacillus plantarum in yoghurt",
"author": "Taghizadeh Moghaddam",
"doi-asserted-by": "crossref",
"first-page": "737",
"issue": "4",
"journal-title": "Int. J. Dairy Technol.",
"key": "10.1016/j.intimp.2021.107531_b0135",
"volume": "73",
"year": "2020"
},
{
"DOI": "10.3390/toxins12070454",
"article-title": "Characterization of Bacillus cereus in Dairy Products in China",
"author": "Liu",
"doi-asserted-by": "crossref",
"issue": "7",
"journal-title": "Toxins",
"key": "10.1016/j.intimp.2021.107531_b0140",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/j.jff.2018.12.022",
"article-title": "Colonization and probiotic function of Bifidobacterium longum",
"author": "Zhang",
"doi-asserted-by": "crossref",
"first-page": "157",
"journal-title": "J. Funct. Foods",
"key": "10.1016/j.intimp.2021.107531_b0145",
"volume": "53",
"year": "2019"
},
{
"key": "10.1016/j.intimp.2021.107531_b0150",
"unstructured": "M. Mohtashami, M. Mohamadi, M. Azimi-Nezhad, J. Saeidi, F.F. Nia, A. Ghasemi, Lactobacillus bulgaricus and Lactobacillus plantarum improve diabetic wound healing through modulating inflammatory factors, Biotechnol. Appl. Biochem. n/a(n/a)."
},
{
"DOI": "10.1007/s00203-017-1366-1",
"article-title": "New advances in exopolysaccharides production of Streptococcus thermophilus",
"author": "Cui",
"doi-asserted-by": "crossref",
"first-page": "799",
"issue": "6",
"journal-title": "Arch. Microbiol.",
"key": "10.1016/j.intimp.2021.107531_b0155",
"volume": "199",
"year": "2017"
},
{
"DOI": "10.1016/j.mib.2017.11.030",
"article-title": "Evolution of virulence in Enterococcus faecium, a hospital-adapted opportunistic pathogen",
"author": "Gao",
"doi-asserted-by": "crossref",
"first-page": "76",
"journal-title": "Curr. Opin. Microbiol.",
"key": "10.1016/j.intimp.2021.107531_b0160",
"volume": "41",
"year": "2018"
},
{
"DOI": "10.1016/j.cub.2020.06.083",
"article-title": "Bacillus subtilis: a bacterium for all seasons",
"author": "Losick",
"doi-asserted-by": "crossref",
"first-page": "R1146",
"issue": "19",
"journal-title": "Curr. Biol.: CB",
"key": "10.1016/j.intimp.2021.107531_b0165",
"volume": "30",
"year": "2020"
},
{
"DOI": "10.5582/bst.2020.01020",
"article-title": "Drug treatment options for the 2019-new coronavirus (2019-nCoV)",
"author": "Lu",
"doi-asserted-by": "crossref",
"first-page": "69",
"issue": "1",
"journal-title": "BioSci. Trends",
"key": "10.1016/j.intimp.2021.107531_b0170",
"volume": "14",
"year": "2020"
},
{
"article-title": "Effects of Probiotics in Conditions or Infections Similar to COVID-19 on Health Outcomes: An Evidence Analysis Center Scoping Review",
"author": "Rozga",
"journal-title": "J. Acad. Nutr. Diet.",
"key": "10.1016/j.intimp.2021.107531_b0175",
"year": "2020"
},
{
"DOI": "10.1016/j.micpath.2020.104452",
"article-title": "The immunomodulatory effects of probiotics on respiratory viral infections: A hint for COVID-19 treatment?",
"author": "Mahooti",
"doi-asserted-by": "crossref",
"journal-title": "Microb. Pathog.",
"key": "10.1016/j.intimp.2021.107531_b0180",
"volume": "148",
"year": "2020"
},
{
"key": "10.1016/j.intimp.2021.107531_b0185",
"unstructured": "A. Sundararaman, M. Ray, P.V. Ravindra, P.M. Halami, Role of probiotics to combat viral infections with emphasis on COVID-19, Appl. Microbiol. Biotechnol. 16."
},
{
"key": "10.1016/j.intimp.2021.107531_b0190",
"unstructured": "E.A. Coomes, H. Haghbayan, Interleukin-6 in Covid-19: A systematic review andmeta-analysis, Rev. Med. Virol. 9."
},
{
"DOI": "10.2139/ssrn.3548761",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2021.107531_b0195",
"unstructured": "T. Liu, J. Zhang, Y. Yang, L. Zhang, J.J.S.E.J. Yi, The Potential Role of IL-6 in Monitoring Coronavirus Disease 2019, (2020)."
},
{
"DOI": "10.1056/NEJMoa2001282",
"article-title": "A Trial of Lopinavir-Ritonavir in Adults Hospitalized with Severe Covid-19",
"author": "Cao",
"doi-asserted-by": "crossref",
"first-page": "1787",
"issue": "19",
"journal-title": "New Engl. J. Med.",
"key": "10.1016/j.intimp.2021.107531_b0200",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"article-title": "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "497",
"issue": "10223",
"journal-title": "Lancet",
"key": "10.1016/j.intimp.2021.107531_b0205",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/j.cca.2020.06.009",
"article-title": "Comparative analysis of laboratory indexes of severe and non-severe patients infected with COVID-19",
"author": "Bao",
"doi-asserted-by": "crossref",
"first-page": "180",
"journal-title": "Clin. Chim. Acta",
"key": "10.1016/j.intimp.2021.107531_b0210",
"volume": "509",
"year": "2020"
},
{
"DOI": "10.1101/2020.02.18.20024364",
"doi-asserted-by": "crossref",
"key": "10.1016/j.intimp.2021.107531_b0215",
"unstructured": "B. Diao, C. Wang, Y. Tan, X. Chen, Y. Liu, L. Ning, L. Chen, M. Li, Y.-P. Liu, G. Wang, Z. Yuan, Z. Feng, Y. Wu, Y. Chen, Reduction and Functional Exhaustion of T Cells in Patients with Coronavirus Disease 2019 (COVID-19), 2020."
},
{
"DOI": "10.1136/bjsm.2007.044628",
"article-title": "Oral administration of the probiotic Lactobacillus fermentum VRI-003 and mucosal immunity in endurance athletes",
"author": "Cox",
"doi-asserted-by": "crossref",
"first-page": "222",
"issue": "4",
"journal-title": "Br. J. Sports Med.",
"key": "10.1016/j.intimp.2021.107531_b0220",
"volume": "44",
"year": "2010"
},
{
"DOI": "10.1080/10408398.2018.1490885",
"article-title": "Probiotics interaction with foodborne pathogens: a potential alternative to antibiotics and future challenges",
"author": "Wan",
"doi-asserted-by": "crossref",
"first-page": "3320",
"issue": "20",
"journal-title": "Crit. Rev. Food Sci. Nutr.",
"key": "10.1016/j.intimp.2021.107531_b0225",
"volume": "59",
"year": "2019"
},
{
"article-title": "C-reactive protein levels in the early stage of COVID-19",
"author": "Ling",
"journal-title": "Med. Maladies Infectieuses",
"key": "10.1016/j.intimp.2021.107531_b0230",
"year": "2020"
},
{
"article-title": "Prognostic value of C-reactive protein in patients with COVID-19",
"author": "Luo",
"journal-title": "Clin. Infect. Diseas.: An Official Publication of the Infectious Diseases Society of America",
"key": "10.1016/j.intimp.2021.107531_b0235",
"year": "2020"
},
{
"article-title": "Predicting the Risk of Clinical Deterioration in Patients with Severe COVID-19 Infection Using Machine Learning",
"author": "Zhou",
"journal-title": "SSRN Electron. J.",
"key": "10.1016/j.intimp.2021.107531_b0240",
"year": "2020"
},
{
"article-title": "ACP risk grade: a simple mortality index for patients with confirmed or suspected severe acute respiratory syndrome coronavirus 2 disease (COVID-19) during the early stage of outbreak in Wuhan, China",
"author": "Lu",
"journal-title": "medRxiv",
"key": "10.1016/j.intimp.2021.107531_b0245",
"year": "2020"
}
],
"reference-count": 49,
"references-count": 49,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S1567576921001673"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Pharmacology",
"Immunology",
"Immunology and Allergy"
],
"subtitle": [],
"title": "The role of probiotics in coronavirus disease-19 infection in Wuhan: A retrospective study of 311 severe patients",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "95"
}
