Paracetamol Is Associated with a Lower Risk of COVID-19 Infection and Decreased ACE2 Protein Expression: A Retrospective Analysis
et al., COVID, doi:10.3390/covid1010018, Aug 2021
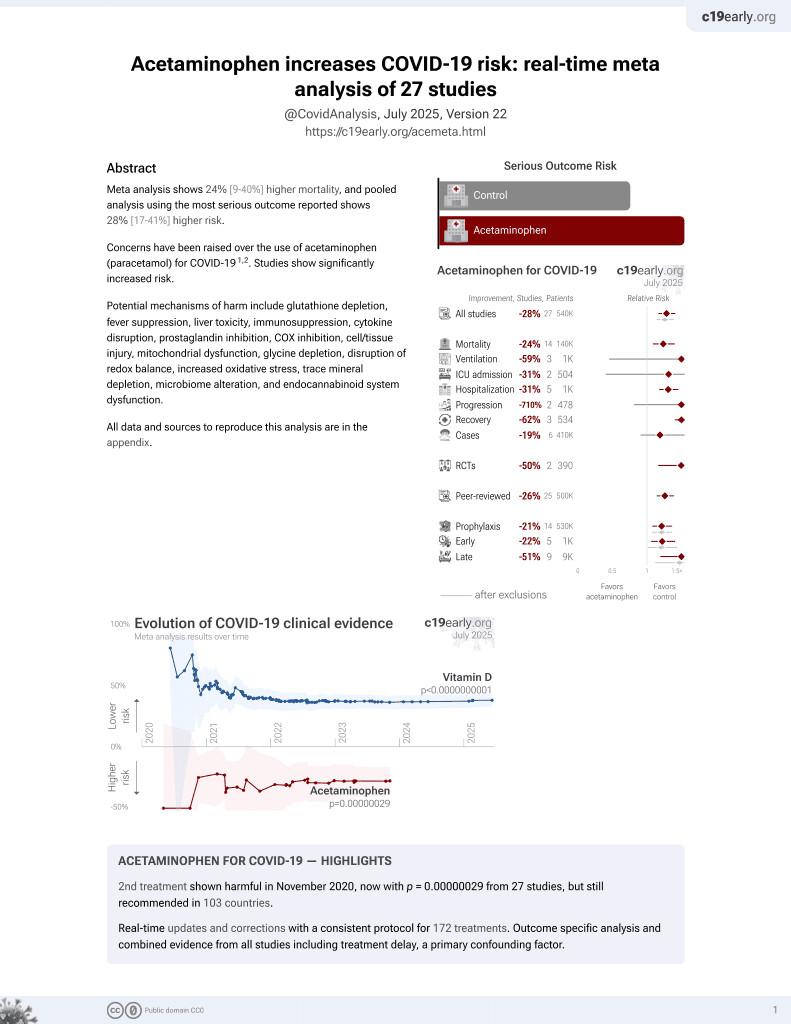
2nd treatment shown to increase risk in
November 2020, now with p = 0.00000029 from 27 studies, but still recommended in 103 countries.
6,600+ studies for
220+ treatments. c19early.org
|
UK Biobank retrospective showing lower cases with acetaminophen use.
Acetaminophen is also known as paracetamol, Tylenol, Panadol, Calpol, Tempra, Calprofen, Doliprane, Efferalgan, Grippostad C, Dolo, Acamol, Fevadol, Crocin, and Perfalgan.
Standard of Care (SOC) for COVID-19 in the study country,
the United Kingdom, is very poor with very low average efficacy for approved treatments1.
The United Kingdom focused on expensive high-profit treatments, approving only one low-cost early treatment, which required a prescription and had limited adoption. The high-cost prescription treatment strategy reduces the probability of early treatment due to access and cost barriers, and eliminates complementary and synergistic benefits seen with many low-cost treatments.
Study covers ibuprofen and acetaminophen.
|
risk of case, 7.0% lower, OR 0.93, p = 0.004, RR approximated with OR.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Leal et al., 16 Aug 2021, retrospective, United Kingdom, peer-reviewed, 5 authors, study period 16 March, 2020 - 1 February, 2021.
Contact: martins.lmiguel@gmail.com (corresponding author), njs76@mrc-tox.cam.ac.uk, yzy21@cam.ac.uk, yc487@cam.ac.uk, gf334@mrc-tox.cam.ac.uk.
Paracetamol Is Associated with a Lower Risk of COVID-19 Infection and Decreased ACE2 Protein Expression: A Retrospective Analysis
COVID, doi:10.3390/covid1010018
Ibuprofen is a common over-the-counter drug taken for pain relief. However, recent studies have raised concerns about its potential toxic effect with coronavirus disease 2019 (COVID-19), which is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). It has been proposed that ibuprofen may increase levels of angiotensin-converting enzyme 2 (ACE2), the human receptor for SARS-CoV-2 infection. Therefore, paracetamol is suggested as an alternative to ibuprofen for treating COVID-19 symptoms. Nevertheless, the relationship between intake of paracetamol or ibuprofen and either susceptibility to infection by SARS-CoV-2 or modulation of cellular ACE2 levels remains unclear. In this study, we combined data from human medical records and cells in culture to explore the role of the intake of these drugs in COVID-19. Although ibuprofen did not influence COVID-19 infectivity or ACE2 levels, paracetamol intake was associated with a lower occurrence of COVID-19 in our cohort. We also found that paracetamol led to decreased ACE2 protein levels in cultured cells. Our work identifies a putative protective effect of paracetamol against SARS-CoV-2 infection. Future work should explore the molecular mechanisms underlying the relationship between paracetamol and COVID-19.
Conflicts of Interest: The authors declare no competing interests nor conflict of interest.
Abbreviations
References
Armstrong, Rudkin, Allen, Crook, Wilson et al., Dynamic Linkage of COVID-19 Test Results between Public Health England's Second Generation Surveillance System and UK Biobank, Microb. Genom, doi:10.1099/mgen.0.000397
Behrends, Giskeødegård, Bravo-Santano, Letek, Keun, Acetaminophen Cytotoxicity in HepG2 Cells Is Associated with a Decoupling of Glycolysis from the TCA Cycle, Loss of NADPH Production, and Suppression of Anabolism, Arch. Toxicol, doi:10.1007/s00204-018-2371-0
Bombardo, Malagola, Chen, Rudnicka, Graf et al., Ibuprofen and Diclofenac Treatments Reduce Proliferation of Pancreatic Acinar Cells upon Inflammatory Injury and Mitogenic Stimulation, Br. J. Pharmacol, doi:10.1111/bph.13867
Bourgonje, Abdulle, Timens, Hillebrands, Navis et al., Angiotensin-Converting Enzyme 2 (ACE2), SARS-CoV-2 and the Pathophysiology of Coronavirus Disease 2019 (COVID-19), J. Pathol, doi:10.1002/path.5471
Bushra, Aslam, An Overview of Clinical Pharmacology of Ibuprofen, Oman Med. J, doi:10.5001/omj.2010.49
Bycroft, Freeman, Petkova, Band, Elliott et al., The UK Biobank Resource with Deep Phenotyping and Genomic Data, Nature, doi:10.1038/s41586-018-0579-z
Clarke, Belyaev, Lambert, Turner, Epigenetic Regulation of Angiotensin-Converting Enzyme 2 (ACE2) by SIRT1 under Conditions of Cell Energy Stress, Clin. Sci, doi:10.1042/CS20130291
Fang, Karakiulakis, Roth, Are Patients with Hypertension and Diabetes Mellitus at Increased Risk for COVID-19 Infection?, Lancet Respir. Med, doi:10.1016/S2213-2600(20)30116-8
François, Desrumaux, Cans, Pin, Pavese et al., Prevalence and Risk Factors of Suppurative Complications in Children with Pneumonia, Acta Paediatr, doi:10.1111/j.1651-2227.2010.01734.x
Gervin, Nordeng, Ystrom, Reichborn-Kjennerud, Lyle, Long-Term Prenatal Exposure to Paracetamol Is Associated with DNA Methylation Differences in Children Diagnosed with ADHD, Clin. Epigenetics, doi:10.1186/s13148-017-0376-9
Grippo, Navarra, Orsi, Manno, Grande et al., The Role of COVID-19 in the Death of SARS-CoV-2-Positive Patients: A Study Based on Death Certificates, J. Clin. Med, doi:10.3390/jcm9113459
Hao, Wang, Sun, Ding, Wu et al., Unidirectional Inversion of Ibuprofen in Caco-2 Cells: Developing a Suitable Model for Presystemic Chiral Inversion Study, Biol. Pharm. Bull, doi:10.1248/bpb.28.682
Harrison, Lin, Wang, Mechanisms of SARS-CoV-2 Transmission and Pathogenesis, Trends Immunol
Heikkinen, Mönkkönen, Korjamo, Kinetics of Cellular Retention during Caco-2 Permeation Experiments: Role of Lysosomal Sequestration and Impact on Permeability Estimates, J. Pharmacol. Exp. Ther, doi:10.1124/jpet.108.145797
Herichová, Šoltésová, Szántóová, Mravec, Neupauerová et al., Effect of Angiotensin II on Rhythmic Per2 Expression in the Suprachiasmatic Nucleus and Heart and Daily Rhythm of Activity in Wistar Rats, Regul. Pept, doi:10.1016/j.regpep.2013.06.016
Hoffmann, Kleine-Weber, Schroeder, Krüger, Herrler et al., SARS-CoV-2 Cell Entry Depends on ACE2 and TMPRSS2 and Is Blocked by a Clinically Proven Protease Inhibitor, Cell, doi:10.1016/j.cell.2020.02.052
Jóźwiak-Bebenista, Nowak, Paracetamol: Mechanism of Action, Applications and Safety Concern, Acta Pol. Pharm
Karcioglu, Bas, Hosseinzadeh, Kolahforoush, Simsik et al., Commission of Human Medicines More Advice on the Use of Ibuprofen for COVID-19, Drug Ther. Bull, doi:10.1136/dtb.2020.000032
Kluyver, Ragan-Kelley, Pérez, Granger, Bussonnier et al., Jupyter Notebooks-A Publishing Format for Reproducible Computational Workflows
Krenke, Krawiec, Kraj, Peradzynska, Krauze et al., Risk Factors for Local Complications in Children with Community-Acquired Pneumonia, Clin. Respir. J, doi:10.1111/crj.12524
Leidgens, Seliger, Jachnik, Welz, Leukel et al., Ibuprofen and Diclofenac Restrict Migration and Proliferation of Human Glioma Cells by Distinct Molecular Mechanisms, PLoS ONE, doi:10.1371/journal.pone.0140613
Liao, Lin, Yu, Hsu, Pang et al., Ibuprofen Inhibited Migration of Skeletal Muscle Cells in Association with Downregulation of P130cas and CrkII Expressions, Skelet. Muscle, doi:10.1186/s13395-019-0208-z
Lumley, Diehr, Emerson, Chen, The Importance of the Normality Assumption in Large Public Health Data Sets, Annu. Rev. Public Health, doi:10.1146/annurev.publhealth.23.100901.140546
Lund, Kristensen, Reilev, Christensen, Thomsen et al., Adverse Outcomes and Mortality in Users of Non-Steroidal Anti-Inflammatory Drugs Who Tested Positive for SARS-CoV-2: A Danish Nationwide Cohort Study, PLoS Med, doi:10.1371/journal.pmed.1003308
Martins-Filho, Do Nascimento-Júnior, Santos, No Current Evidence Supporting Risk of Using Ibuprofen in Patients with COVID-19, Int. J. Clin. Pract, doi:10.1111/ijcp.13576
Moore, Carleton, Blin, Bosco-Levy, Droz, Does Ibuprofen Worsen COVID-19?, Drug Saf, doi:10.1007/s40264-020-00953-0
Pierce, Franklin, Campbell, Tonge, Chen et al., Cell Culture Model for Acetaminophen-Induced Hepatocyte Death in Vivo, Biochem. Pharmacol, doi:10.1016/S0006-2952(02)01180-2
Powis, Message for All Clinical Staff: Anti-Inflammatory Medications
Prieto, Hoffmann, Tirelli, Tancredi, González et al., An Exploratory Study of Two Caco-2 Cell Models for Oral Absorption: A Report on Their within-Laboratory and between-Laboratory Variability, and Their Predictive Capacity, Altern. Lab. Anim. ATLA, doi:10.1177/026119291003800510
Qiao, Wang, Chen, Zhang, Liu et al., Ibuprofen Attenuates Cardiac Fibrosis in Streptozotocin-Induced Diabetic Rats, Cardiology, doi:10.1159/000375362
Rinott, Kozer, Shapira, Bar-Haim, Youngster, Ibuprofen Use and Clinical Outcomes in COVID-19 Patients, Clin. Microbiol. Infect. Publ. Eur. Soc. Clin. Microbiol. Infect. Dis, doi:10.1016/j.cmi.2020.06.003
Sanchis-Gomar, Lavie, Perez-Quilis, Henry, Lippi, Angiotensin-Converting Enzyme 2 and Antihypertensives (Angiotensin Receptor Blockers and Angiotensin-Converting Enzyme Inhibitors) in Coronavirus Disease 2019, Mayo Clin. Proc, doi:10.1016/j.mayocp.2020.03.026
Schmittgen, Livak, Analyzing Real-Time PCR Data by the Comparative C(T) Method, Nat. Protoc, doi:10.1038/nprot.2008.73
Siissalo, Laine, Tolonen, Kaukonen, Finel et al., Caco-2 Cell Monolayers as a Tool to Study Simultaneous Phase II Metabolism and Metabolite Efflux of Indomethacin, Paracetamol and 1-Naphthol, Int. J. Pharm
Smith, Sausville, Girish, Yuan, Vasudevan et al., Cigarette Smoke Exposure and Inflammatory Signaling Increase the Expression of the SARS-CoV-2 Receptor ACE2 in the Respiratory Tract, Dev. Cell, doi:10.1016/j.devcel.2020.05.012
Sudlow, Gallacher, Allen, Beral, Burton et al., UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age, PLoS Med, doi:10.1371/journal.pmed.1001779
Team, Development Core A Language and Environment for Statistical Computing, R Found. Stat. Comput
Travaglio, Yu, Popovic, Selley, Leal et al., Links between Air Pollution and COVID-19 in England, Environ. Pollut, doi:10.1016/j.envpol.2020.115859
Vad, Yount, Moore, Weidanz, Moridani, Biochemical Mechanism of Acetaminophen (APAP) Induced Toxicity in Melanoma Cell Lines, J. Pharm. Sci, doi:10.1002/jps.21505
Wilcox, Cryer, Triadafilopoulos, Patterns of Use and Public Perception of Over-the-Counter Pain Relievers: Focus on Nonsteroidal Antiinflammatory Drugs, J. Rheumatol
Williamson, Walker, Bhaskaran, Bacon, Bates et al., Factors Associated with COVID-19-Related Death Using OpenSAFELY, Nature, doi:10.1038/s41586-020-2521-4
Wojnarová, Kutinová Canová, Farghali, Kučera, Sirtuin 1 Modulation in Rat Model of Acetaminophen-Induced Hepatotoxicity, Physiol. Res, doi:10.33549/physiolres.933205
Yu, Travaglio, Popovic, Leal, Martins, Alzheimer's and Parkinson's Diseases Predict Different COVID-19 Outcomes: A UK Biobank Study, Geriatrics, doi:10.3390/geriatrics6010010
DOI record:
{
"DOI": "10.3390/covid1010018",
"ISSN": [
"2673-8112"
],
"URL": "http://dx.doi.org/10.3390/covid1010018",
"abstract": "<jats:p>Ibuprofen is a common over-the-counter drug taken for pain relief. However, recent studies have raised concerns about its potential toxic effect with coronavirus disease 2019 (COVID-19), which is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). It has been proposed that ibuprofen may increase levels of angiotensin-converting enzyme 2 (ACE2), the human receptor for SARS-CoV-2 infection. Therefore, paracetamol is suggested as an alternative to ibuprofen for treating COVID-19 symptoms. Nevertheless, the relationship between intake of paracetamol or ibuprofen and either susceptibility to infection by SARS-CoV-2 or modulation of cellular ACE2 levels remains unclear. In this study, we combined data from human medical records and cells in culture to explore the role of the intake of these drugs in COVID-19. Although ibuprofen did not influence COVID-19 infectivity or ACE2 levels, paracetamol intake was associated with a lower occurrence of COVID-19 in our cohort. We also found that paracetamol led to decreased ACE2 protein levels in cultured cells. Our work identifies a putative protective effect of paracetamol against SARS-CoV-2 infection. Future work should explore the molecular mechanisms underlying the relationship between paracetamol and COVID-19.</jats:p>",
"alternative-id": [
"covid1010018"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-9868-816X",
"affiliation": [],
"authenticated-orcid": false,
"family": "Leal",
"given": "Nuno Santos",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-4800-9392",
"affiliation": [],
"authenticated-orcid": false,
"family": "Yu",
"given": "Yizhou",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-6025-6097",
"affiliation": [],
"authenticated-orcid": false,
"family": "Chen",
"given": "Yuwen",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Fedele",
"given": "Giorgio",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Martins",
"given": "Luís Miguel",
"sequence": "additional"
}
],
"container-title": "COVID",
"container-title-short": "COVID",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2021,
8,
17
]
],
"date-time": "2021-08-17T01:28:04Z",
"timestamp": 1629163684000
},
"deposited": {
"date-parts": [
[
2021,
8,
17
]
],
"date-time": "2021-08-17T02:07:45Z",
"timestamp": 1629166065000
},
"indexed": {
"date-parts": [
[
2022,
8,
18
]
],
"date-time": "2022-08-18T22:29:33Z",
"timestamp": 1660861773301
},
"is-referenced-by-count": 3,
"issue": "1",
"issued": {
"date-parts": [
[
2021,
8,
16
]
]
},
"journal-issue": {
"issue": "1",
"published-online": {
"date-parts": [
[
2021,
9
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
8,
16
]
],
"date-time": "2021-08-16T00:00:00Z",
"timestamp": 1629072000000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/2673-8112/1/1/18/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "218-229",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2021,
8,
16
]
]
},
"published-online": {
"date-parts": [
[
2021,
8,
16
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"article-title": "Patterns of Use and Public Perception of Over-the-Counter Pain Relievers: Focus on Nonsteroidal Antiinflammatory Drugs",
"author": "Wilcox",
"first-page": "2218",
"journal-title": "J. Rheumatol.",
"key": "ref1",
"volume": "32",
"year": "2005"
},
{
"DOI": "10.5001/omj.2010.49",
"doi-asserted-by": "publisher",
"key": "ref2"
},
{
"article-title": "Paracetamol: Mechanism of Action, Applications and Safety Concern",
"author": "Jóźwiak-Bebenista",
"first-page": "11",
"journal-title": "Acta Pol. Pharm.",
"key": "ref3",
"volume": "71",
"year": "2014"
},
{
"DOI": "10.1016/j.it.2020.10.004",
"doi-asserted-by": "publisher",
"key": "ref4"
},
{
"DOI": "10.1016/j.cell.2020.02.052",
"doi-asserted-by": "publisher",
"key": "ref5"
},
{
"DOI": "10.1002/path.5471",
"doi-asserted-by": "publisher",
"key": "ref6"
},
{
"DOI": "10.1016/j.mayocp.2020.03.026",
"doi-asserted-by": "publisher",
"key": "ref7"
},
{
"DOI": "10.1136/dtb.2020.000032",
"doi-asserted-by": "publisher",
"key": "ref8"
},
{
"DOI": "10.1007/s40264-020-00953-0",
"doi-asserted-by": "publisher",
"key": "ref9"
},
{
"key": "ref10"
},
{
"DOI": "10.1016/S2213-2600(20)30116-8",
"doi-asserted-by": "publisher",
"key": "ref11"
},
{
"DOI": "10.1159/000375362",
"doi-asserted-by": "publisher",
"key": "ref12"
},
{
"DOI": "10.1016/j.cmi.2020.06.003",
"doi-asserted-by": "publisher",
"key": "ref13"
},
{
"DOI": "10.1371/journal.pmed.1001779",
"doi-asserted-by": "publisher",
"key": "ref14"
},
{
"DOI": "10.1099/mgen.0.000397",
"doi-asserted-by": "publisher",
"key": "ref15"
},
{
"DOI": "10.1007/s00204-018-2371-0",
"doi-asserted-by": "publisher",
"key": "ref16"
},
{
"DOI": "10.1016/S0006-2952(02)01180-2",
"doi-asserted-by": "publisher",
"key": "ref17"
},
{
"DOI": "10.1177/026119291003800510",
"doi-asserted-by": "publisher",
"key": "ref18"
},
{
"DOI": "10.1016/j.ijpharm.2009.08.044",
"doi-asserted-by": "publisher",
"key": "ref19"
},
{
"DOI": "10.1002/jps.21505",
"doi-asserted-by": "publisher",
"key": "ref20"
},
{
"DOI": "10.1111/bph.13867",
"doi-asserted-by": "publisher",
"key": "ref21"
},
{
"DOI": "10.1248/bpb.28.682",
"doi-asserted-by": "publisher",
"key": "ref22"
},
{
"DOI": "10.1124/jpet.108.145797",
"doi-asserted-by": "publisher",
"key": "ref23"
},
{
"DOI": "10.1371/journal.pone.0140613",
"doi-asserted-by": "publisher",
"key": "ref24"
},
{
"DOI": "10.1186/s13395-019-0208-z",
"doi-asserted-by": "publisher",
"key": "ref25"
},
{
"DOI": "10.1038/nprot.2008.73",
"doi-asserted-by": "publisher",
"key": "ref26"
},
{
"DOI": "10.1016/j.devcel.2020.05.012",
"doi-asserted-by": "publisher",
"key": "ref27"
},
{
"DOI": "10.1016/j.envpol.2020.115859",
"doi-asserted-by": "publisher",
"key": "ref28"
},
{
"DOI": "10.3390/geriatrics6010010",
"doi-asserted-by": "publisher",
"key": "ref29"
},
{
"DOI": "10.1038/s41586-020-2521-4",
"doi-asserted-by": "publisher",
"key": "ref30"
},
{
"DOI": "10.1146/annurev.publhealth.23.100901.140546",
"doi-asserted-by": "publisher",
"key": "ref31"
},
{
"article-title": "Development Core A Language and Environment for Statistical Computing",
"journal-title": "R Found. Stat. Comput.",
"key": "ref32",
"volume": "2",
"year": "2018"
},
{
"article-title": "Jupyter Notebooks—A Publishing Format for Reproducible Computational Workflows",
"author": "Kluyver",
"first-page": "87",
"key": "ref33",
"series-title": "Proceedings of the Positioning and Power in Academic Publishing: Players, Agents and Agendas—Proceedings of the 20th International Conference on Electronic Publishing",
"year": "2016"
},
{
"DOI": "10.1038/s41586-018-0579-z",
"doi-asserted-by": "publisher",
"key": "ref34"
},
{
"DOI": "10.1111/j.1651-2227.2010.01734.x",
"doi-asserted-by": "publisher",
"key": "ref35"
},
{
"DOI": "10.1111/crj.12524",
"doi-asserted-by": "publisher",
"key": "ref36"
},
{
"DOI": "10.1111/ijcp.13576",
"doi-asserted-by": "publisher",
"key": "ref37"
},
{
"DOI": "10.1016/j.regpep.2013.06.016",
"doi-asserted-by": "publisher",
"key": "ref38"
},
{
"DOI": "10.1371/journal.pmed.1003308",
"doi-asserted-by": "publisher",
"key": "ref39"
},
{
"DOI": "10.1186/s13148-017-0376-9",
"doi-asserted-by": "publisher",
"key": "ref40"
},
{
"DOI": "10.33549/physiolres.933205",
"doi-asserted-by": "publisher",
"key": "ref41"
},
{
"DOI": "10.1042/CS20130291",
"doi-asserted-by": "publisher",
"key": "ref42"
},
{
"DOI": "10.3390/jcm9113459",
"doi-asserted-by": "publisher",
"key": "ref43"
}
],
"reference-count": 43,
"references-count": 43,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/2673-8112/1/1/18"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Paracetamol Is Associated with a Lower Risk of COVID-19 Infection and Decreased ACE2 Protein Expression: A Retrospective Analysis",
"type": "journal-article",
"volume": "1"
}