Chronic diseases, chest computed tomography, and laboratory tests as predictors of severe respiratory failure and death in elderly Brazilian patients hospitalized with COVID-19: a prospective cohort study
et al., BMC Geriatrics, doi:10.1186/s12877-022-02776-3, Feb 2022
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 201 COVID+ hospitalized adults in Brazil, mean age 73, showing a lower risk of mortality and respiratory failure with vitamin D supplementation in unadjusted results, without statistical significance, and a higher risk of progression to mechanical ventilation with vitamin D levels <40ng/dl.
This is the 71st of 137 COVID-19 controlled studies for vitamin D, which collectively show efficacy with p<0.0000000001.
41 studies are RCTs, which show efficacy with p=0.00000049.
|
risk of death, 22.1% lower, RR 0.78, p = 0.61, treatment 8 of 113 (7.1%), control 8 of 88 (9.1%), NNT 50, excluded in exclusion analyses:
unadjusted results with no group details.
|
|
risk of progression, 30.8% lower, RR 0.69, p = 0.26, treatment 16 of 113 (14.2%), control 18 of 88 (20.5%), NNT 16, respiratory failure, excluded in exclusion analyses:
unadjusted results with no group details.
|
|
risk of mechanical ventilation, 84.4% lower, OR 0.16, p = 0.03, cutoff 40ng/dl, inverted to make OR<1 favor high D levels (≥40ng/dl), risk of mechanical ventilation for vitamin D levels >40ng/ml, RR approximated with OR, outcome based on serum levels.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Junior et al., 17 Feb 2022, prospective, Brazil, peer-reviewed, 6 authors, dosage not specified.
Chronic diseases, chest computed tomography, and laboratory tests as predictors of severe respiratory failure and death in elderly Brazilian patients hospitalized with COVID-19: a prospective cohort study
BMC Geriatrics, doi:10.1186/s12877-022-02776-3
Background: The primary risk factors for severe respiratory failure and death in the elderly hospitalized with COVID-19 remain unclear. Objective: To determine the association of chronic diseases, chest computed tomography (CT), and laboratory tests with severe respiratory failure and mortality in older adults hospitalized with COVID-19. Method: This was a prospective cohort with 201 hospitalized older adults with COVID-19. Chronic diseases, chest CT, laboratory tests, and other data were collected within the first 48 h of hospitalization. Outcomes were progression to severe respiratory failure with the need of mechanical ventilation (SRF/MV) and death.
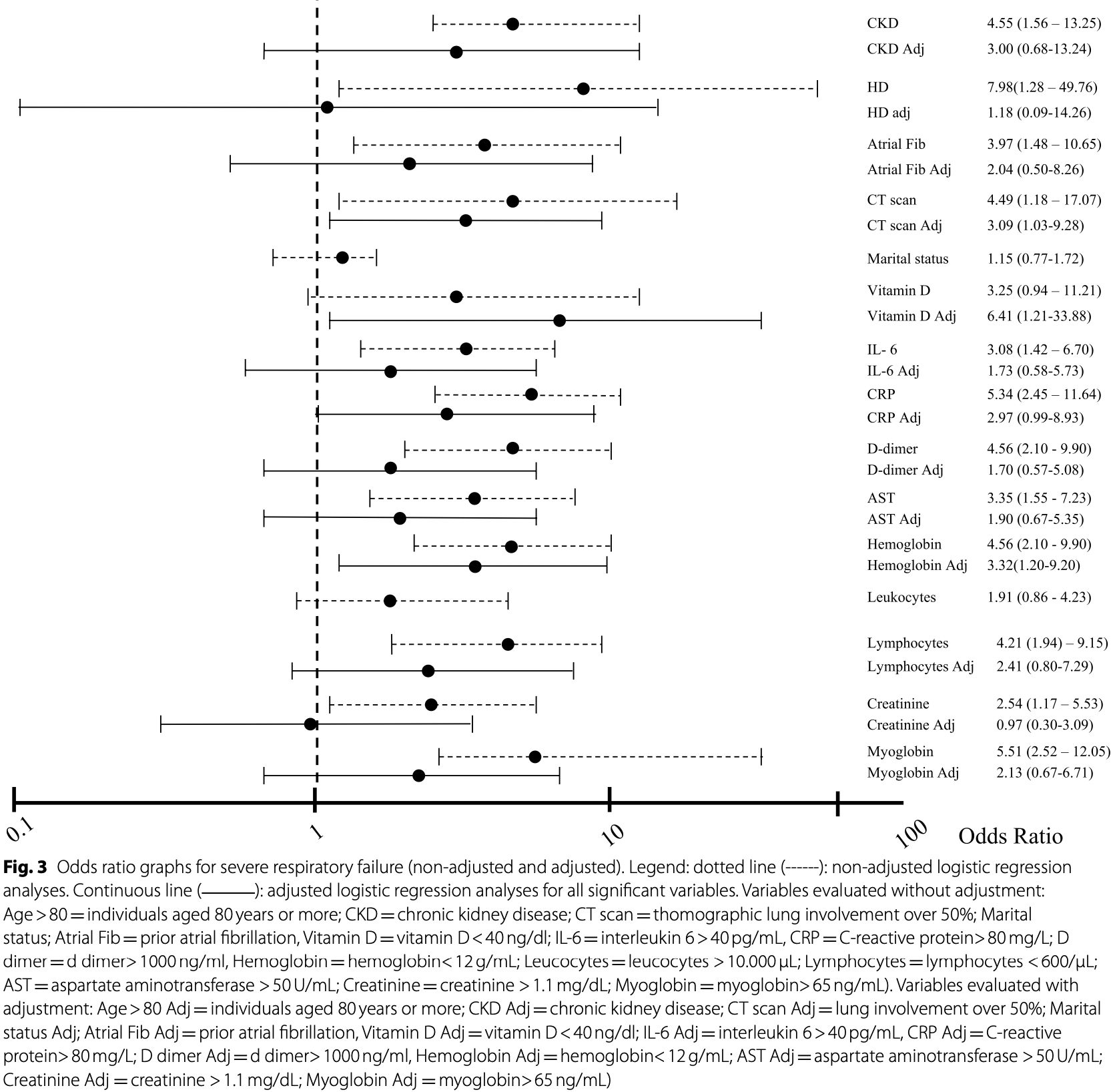
Results: The mean age was 72.7 ± 9.2 years, and 63.2% were men. SRF/MV occurred in 16.9% (p < 0.001), and death occurred in 8%. In the adjusted regression analyses, lung involvement over 50% [odds ratio (OR): 3.09 (1.03-9.28; 0.043)], C-reactive protein (CRP) > 80 ng/mL [OR: 2.97 (0.99-8.93; 0.052)], Vitamin D < 40 ng/mL [OR: 6.41 (1.21-33.88; 0.029)], and hemoglobin < 12 g/mL ; 0.020)] were independent predictors for SFR/MV, while chronic atrial fibrillation ; 0.001)], cancer history 0.026)] and IL-6 > 40 pg/ mL [OR:10.01 (1.66-60.13; 0.012)] were independent predictors of death.
Conclusion: In hospitalized older adults with COVID-19, tomographic pulmonary involvement > 50%, anemia, vitamin D below 40 ng/mL, and CRP above 80 mg/L were independent risk factors for progression to SRF/MV. The presence of chronic atrial fibrillation, previous cancer, IL-6 > 40 pg/mL, and anemia were independent predictors of death.
Abbreviations 25(OH)D: 25-hydroxyvitamin-D; ALT: alanine transaminase; AST: aspartate aminotransferase; CKD: chronic kidney disease (non-hemodialysis); Creat: creatinine; CRP: C-reactive protein; CT: computed tomography; ESRD: end-stage renal disease (on HD); HD: hemodialysis; Hb: hemoglobin; ICU: intensive care units; IL: interleukin; LDH: lactate dehydrogenase; Myo: myoglobin; SRF/MV: severe respiratory failure with the need of mechanical ventilation; TLeuc: total leucocytes; TLymp: total lymphocytes; TNF: tumor necrosis factor.
Authors' contributions Accordance statement and authors' specific areas of contributions: Statements; All authors confirm authorship and participation in the preparation of the manuscript. This material has not been previously published, is not presently under consideration for publication elsewhere, nor will it be submitted elsewhere while it is under reviewed by your Journal. No other submissions or publications include material that is largely duplicative of that presented in the manuscript or derived from the same subjects. If accepted, the paper will not be published elsewhere in the same form, in English or in any other language, including electronically, without the written consent of the copyright holder. No references were blacked-out. The authors declare that they agree with all the statements presented in this manuscript. This manuscript had been read and approved by all authors. Authors' specific areas of contributions; AFJ, EA, SJMI,..
References
Baktash, Hosack, Patel, Shah, Kandiah et al., Vitamin D status and outcomes for hospitalised older patients with COVID-19, Postgrad Med J, doi:10.1136/postgradmedj-2020-138712
Bellmann-Weiler, Lanser, Barket, Rangger, Schapfl et al., Prevalence and Predictive Value of Anemia and Dysregulated Iron Homeostasis in Patients with COVID-19 Infection, J Clin Med
Bergamaschi, Borrelli De Andreis, Aronico, Lenti, Barteselli et al., Anemia in patients with Covid-19: pathogenesis and clinical significance, Clin Exp Med, doi:10.1007/s10238-020-00679-4
Biesalski, Vitamin D deficiency and co-morbidities in COVID-19 patients -A fatal relationship? NFS J
Blanco-Melo, Nilsson-Payant, Liu, Uhl, Hoagland et al., Imbalanced Host Response to SARS-CoV-2 Drives Development of COVID-19, Cell
Bonanad, García-Blas, Tarazona-Santabalbina, Sanchis, Bertomeu-González et al., The effect of age on mortality in patients with COVID-19: a Meta-analysis with 611,583 subjects, J Am Med Dir Assoc
Bôas, Ibge, População sem instrução cai e tempo médio de estudo atinge 9,4 anos. Valor Econômico
Carpagnano, Lecce, Quaranta, Zito, Buonamico et al., Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19, J Endocrinol Invest, doi:10.1007/s40618-020-01370-x
Castillo, Costa, Barrios, Díaz, Miranda et al., Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study, J Steroid Biochem Mol Biol
Cdc Covid-, Severe Outcomes Among Patients with Coronavirus Disease 2019 (COVID-19) -United States, MMWR Morb Mortal Wkly Rep, doi:10.15585/mmwr.mm6912e2
Cereda, Bogliolo, Lobascio, Barichella, Zecchinelli et al., Vitamin D supplementation and outcomes in coronavirus disease 2019 (COVID-19) patients from the outbreak area of Lombardy, Italy, Nutrition
Cereser, Da Re, Zuiani, Girometti, Chest high-resolution computed tomography is associated to short-time progression to severe disease in patients with COVID-19 pneumonia, Clin Imaging
Chen, Wu, Guo, Cao, Huang et al., Clinical and immunological features of severe and moderate coronavirus disease 2019, J Clin Invest
Cho, Stout-Delgado, Aging and Lung Disease, Annu Rev Physiol, doi:10.1146/annurev-physiol-021119-034610
Colombi, Bodini, Petrini, Maffi, Morelli et al., Well-aerated lung on admitting chest CT to predict adverse outcome in COVID-19 pneumonia, Radiology, doi:10.1148/radiol.2020201433
Easty, Farr, Hennessy, New Roles for Vitamin D Superagonists: From COVID to Cancer, Front Endocrinol, doi:10.3389/fendo.2021.644298/full
Franceschi, Capri, Monti, Giunta, Olivieri et al., Inflammaging and anti-inflammaging: a systemic perspective on aging and longevity emerged from studies in humans, Mech Ageing Dev
Fried, Tangen, Walston, Newman, Hirsch et al., Frailty in older adults: Evidence for a phenotype, Journals Gerontol -Ser A Biol Sci Med Sci
Ganz, Anemia of Inflammation. Longo DL, N Engl J Med, doi:10.1056/NEJMra1804281
Guan, Ni, Hu, Liang, Ou et al., Clinical characteristics of coronavirus disease 2019 in China, N Engl J Med, doi:10.1056/NEJMoa2002032
Hamming, Timens, Bulthuis, Lely, Navis et al., Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis, J Pathol, doi:10.1002/path.1570
Henry, De Oliveira, Benoit, Plebani, Lippi, Hematologic, biochemical and immune biomarker abnormalities associated with severe illness and mortality in coronavirus disease 2019 (COVID-19): a meta-analysis, Clin Chem Lab Med, doi:10.1515/cclm-2020-0369/html
Huang, Wang, Li, Ren, Zhao et al., Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet
Kuba, Imai, Penninger, Angiotensin-converting enzyme 2 in lung diseases, Curr Opin Pharmacol
Laguna-Goya, Utrero-Rico, Talayero, Lasa-Lazaro, Ramirez-Fernandez et al., IL-6-based mortality risk model for hospitalized patients with COVID-19, J Allergy Clin Immunol, doi:10.1016/j.jaci.2020.07.009
Li, Kong, Wei, Chen, Liu et al., 1,25-Dihydroxyvitamin D3 is a negative endocrine regulator of the renin-angiotensin system, J Clin Invest
Li, Liu, Zhang, Xu, Dai et al., SARS-CoV-2 and viral sepsis: observations and hypotheses, Lancet
Loganathan, Kuppusamy, Wankhar, Gurugubelli, Mahadevappa et al., Angiotensin-converting enzyme 2 (ACE2): COVID 19 gate way to multiple organ failure syndromes, Respir Physiol Neurobiol
Lotfi, Hamblin, Rezaei, COVID-19: transmission, prevention, and potential therapeutic opportunities, Clin Chim Acta
Meftahi, Jangravi, Sahraei, Bahari, The possible pathophysiology mechanism of cytokine storm in elderly adults with COVID-19 infection: the contribution of "inflame-aging, Inflamm Res, doi:10.1007/s00011-020-01372-8
Morley, Malmstrom, Miller, A simple frailty questionnaire (FRAIL) predicts outcomes in middle aged African Americans, J Nutr Health Aging, doi:10.1007/s12603-012-0084-2
Murai, Fernandes, Sales, Pinto, Goessler et al., Effect of a Single High Dose of Vitamin D 3 on Hospital Length of Stay in Patients With Moderate to Severe COVID-19, JAMA
Park, Macrophages: a Trojan horse in COVID-19?, Nat Rev Immunol
Prietl, Treiber, Pieber, Amrein, Vitamin D and immune function, Nutrients
Radujkovic, Hippchen, Tiwari-Heckler, Dreher, Boxberger, Vitamin D Deficiency and Outcome of COVID-19 Patients, Nutrients
Rizzo, Vieceli, Sega, Fortini, Marracino et al., COVID-19 in the heart and the lungs: could we "Notch" the inflammatory storm?, Basic Res Cardiol, doi:10.1007/s00395-020-0791-5
Rockwood, A global clinical measure of fitness and frailty in elderly people, Can Med Assoc J, doi:10.1503/cmaj.050051
Smet, Smet, Herroelen, Gryspeerdt, Martens, Serum 25(OH)D level on hospital admission associated with COVID-19 stage and mortality, Am J Clin Pathol
Subedi, Tchen, Gaire, Hu, Hu, Adjunctive Nutraceutical Therapies for COVID-19, Int J Mol Sci
Tali, Leblanc, Sadiq, Oyewunmi, Camargo et al., Tools and Techniques for Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2)/COVID-19 Detection, Clin Microbiol Rev, doi:10.1128/CMR.00228-20
Taneri, Gómez-Ochoa, Llanaj, Raguindin, Rojas et al., Anemia and iron metabolism in COVID-19: a systematic review and meta-analysis, Eur J Epidemiol, doi:10.1007/s10654-020-00678-5
Tao, Xu, Yang, Xu, Liu, Anemia is associated with severe illness in COVID-19: a retrospective cohort study, J Med Virol, doi:10.1002/jmv.26444
Turcato, Panebianco, Zaboli, Scheurer, Ausserhofer et al., Correlation between arterial blood gas and CT volumetry in patients with SARS-CoV-2 in the emergency department, Int J Infect Dis
Turrubiates-Hernández, Sánchez-Zuno, González-Estevez, Hernández-Bello, Macedo-Ojeda et al., Potential immunomodulatory effects of vitamin D in the prevention of severe coronavirus disease 2019: An ally for Latin America (Review), Int J Mol Med, doi:10.3892/ijmm.2021.4865
Vita, Lauretani, Bauer, Bautmans, Shardell et al., Relationship between vitamin D and inflammatory markers in older individuals, Age, doi:10.1007/s11357-014-9694-4
Wang, Deng, Gou, Fu, Zhang et al., Preliminary study to identify severe from moderate cases of COVID-19 using combined hematology parameters, Ann Transl Med
Weiss, Goodnough, Anemia of chronic disease, N Engl J Med, doi:10.1056/NEJMra041809
Xu, Wu, Jiang, Xu, Ying et al., Clinical findings in a group of patients infected with the 2019 novel coronavirus (SARS-Cov-2) outside of Wuhan, China: retrospective case series, BMJ, doi:10.1136/bmj.m792
Xudong, Junzhu, Xingxiang, Furong, Yanrong, Age-and gender-related difference of ACE2 expression in rat lung, Life Sci
Ye, Wang, Mao, The pathogenesis and treatment of the `cytokine storm' in COVID-19, J Infect
Yuan, Pan, Kong, Zheng, Szeto et al., 1,25-Dihydroxyvitamin D3 suppresses renin gene transcription by blocking the activity of the cyclic AMP response element in the renin gene promoter, J Biol Chem
Zhang, Xu, Zhou, Chen, Li et al., Clinical characteristics and chest CT imaging features of critically ill COVID-19 patients, Eur Radiol, doi:10.1007/s00330-020-06955-x
Zheng, Gao, Wang, Song, Liu et al., Functional exhaustion of antiviral lymphocytes in COVID-19 patients, Cell Mol Immunol
DOI record:
{
"DOI": "10.1186/s12877-022-02776-3",
"ISSN": [
"1471-2318"
],
"URL": "http://dx.doi.org/10.1186/s12877-022-02776-3",
"abstract": "<jats:title>Abstract</jats:title><jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>The primary risk factors for severe respiratory failure and death in the elderly hospitalized with COVID-19 remain unclear.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Objective</jats:title>\n <jats:p>To determine the association of chronic diseases, chest computed tomography (CT), and laboratory tests with severe respiratory failure and mortality in older adults hospitalized with COVID-19.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Method</jats:title>\n <jats:p>This was a prospective cohort with 201 hospitalized older adults with COVID-19. Chronic diseases, chest CT, laboratory tests, and other data were collected within the first 48 h of hospitalization. Outcomes were progression to severe respiratory failure with the need of mechanical ventilation (SRF/MV) and death.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>The mean age was 72.7 ± 9.2 years, and 63.2% were men. SRF/MV occurred in 16.9% (<jats:italic>p</jats:italic> < 0.001), and death occurred in 8%. In the adjusted regression analyses, lung involvement over 50% [odds ratio (OR): 3.09 (1.03–9.28; 0.043)], C-reactive protein (CRP) > 80 ng/mL [OR: 2.97 (0.99–8.93; 0.052)], Vitamin D < 40 ng/mL [OR: 6.41 (1.21–33.88; 0.029)], and hemoglobin < 12 g/mL [OR: 3.32 (1.20–9.20; 0.020)] were independent predictors for SFR/MV, while chronic atrial fibrillation [OR: 26.72 (3.87–184.11; 0.001)], cancer history [OR:8.32 (1.28–53.91; 0.026)] and IL-6 > 40 pg/mL [OR:10.01 (1.66–60.13; 0.012)] were independent predictors of death.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Conclusion</jats:title>\n <jats:p>In hospitalized older adults with COVID-19, tomographic pulmonary involvement > 50%, anemia, vitamin D below 40 ng/mL, and CRP above 80 mg/L were independent risk factors for progression to SRF/MV. The presence of chronic atrial fibrillation, previous cancer, IL-6 > 40 pg/mL, and anemia were independent predictors of death.</jats:p>\n </jats:sec>",
"alternative-id": [
"2776"
],
"article-number": "132",
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "27 September 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "18 January 2022"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "17 February 2022"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Ethics approval and consent to participate",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "The authors confirm that all the methodology used in this study was carried out in accordance with the relevant ethical guidelines and regulations described in the Declaration of Helsinky. All participants or caregivers / family members signed the Informed Consent Form (ICF). The signing was performed in person by a member of the study team or through an electronic document sent to the participant, after a phone call in which the ICF was read and explained by a member of the study team. The project and Informed Consent Form (ICF) were approved by the Ethics Committee of the Hospital Israelita Albert Einstein and of Plataforma Brasil under the numbers: 4.082.096 e 4.186.636 ."
},
{
"group": {
"label": "Consent for publication",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "Not applicable."
},
{
"group": {
"label": "Competing interests",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 4,
"value": "The authors declare that they have no competing interests."
}
],
"author": [
{
"affiliation": [],
"family": "Junior",
"given": "Alberto Frisoli",
"sequence": "first"
},
{
"affiliation": [],
"family": "Azevedo",
"given": "Elaine",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Paes",
"given": "Angela Tavares",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Lima",
"given": "Eliene",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Campos Guerra",
"given": "João Carlos",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ingham",
"given": "Sheila Jean Mc Neill",
"sequence": "additional"
}
],
"container-title": [
"BMC Geriatrics"
],
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2022,
2,
17
]
],
"date-time": "2022-02-17T04:25:44Z",
"timestamp": 1645071944000
},
"deposited": {
"date-parts": [
[
2022,
2,
17
]
],
"date-time": "2022-02-17T04:26:24Z",
"timestamp": 1645071984000
},
"indexed": {
"date-parts": [
[
2022,
2,
17
]
],
"date-time": "2022-02-17T04:41:27Z",
"timestamp": 1645072887194
},
"is-referenced-by-count": 0,
"issn-type": [
{
"type": "electronic",
"value": "1471-2318"
}
],
"issue": "1",
"issued": {
"date-parts": [
[
2022,
2,
17
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2022,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
2,
17
]
],
"date-time": "2022-02-17T00:00:00Z",
"timestamp": 1645056000000
}
},
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
2,
17
]
],
"date-time": "2022-02-17T00:00:00Z",
"timestamp": 1645056000000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1186/s12877-022-02776-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1186/s12877-022-02776-3/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1186/s12877-022-02776-3.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1186",
"published": {
"date-parts": [
[
2022,
2,
17
]
]
},
"published-online": {
"date-parts": [
[
2022,
2,
17
]
]
},
"published-print": {
"date-parts": [
[
2022,
12
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"DOI": "10.15585/mmwr.mm6912e2",
"doi-asserted-by": "publisher",
"key": "2776_CR1",
"unstructured": "CDC COVID-19 Response Team. Severe Outcomes Among Patients with Coronavirus Disease 2019 (COVID-19) — United States, February 12–March 16, 2020. MMWR Morb Mortal Wkly Rep. 2020;69:343–346. DOI: https://doi.org/10.15585/mmwr.mm6912e2."
},
{
"DOI": "10.1056/NEJMoa2002032",
"author": "W Guan",
"doi-asserted-by": "publisher",
"first-page": "1708",
"issue": "18",
"journal-title": "N Engl J Med.",
"key": "2776_CR2",
"unstructured": "Guan W, Ni Z, Hu Y, Liang W, Ou C, He J, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020;382(18):1708–20 Available from: http://www.nejm.org/doi/10.1056/NEJMoa2002032.",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1136/bmj.m792",
"doi-asserted-by": "publisher",
"key": "2776_CR3",
"unstructured": "Xu X-W, Wu X-X, Jiang X-G, Xu K-J, Ying L-J, Ma C-L, et al. Clinical findings in a group of patients infected with the 2019 novel coronavirus (SARS-Cov-2) outside of Wuhan, China: retrospective case series. BMJ. 2020;27;368:m792. https://doi.org/10.1136/bmj.m792."
},
{
"DOI": "10.1016/j.mad.2006.11.016",
"author": "C Franceschi",
"doi-asserted-by": "publisher",
"first-page": "92",
"issue": "1",
"journal-title": "Mech Ageing Dev",
"key": "2776_CR4",
"unstructured": "Franceschi C, Capri M, Monti D, Giunta S, Olivieri F, Sevini F, et al. Inflammaging and anti-inflammaging: a systemic perspective on aging and longevity emerged from studies in humans. Mech Ageing Dev. 2007;128(1):92–105 Available from: https://linkinghub.elsevier.com/retrieve/pii/S0047637406002491.",
"volume": "128",
"year": "2007"
},
{
"DOI": "10.1016/j.jinf.2020.03.037",
"author": "Q Ye",
"doi-asserted-by": "publisher",
"first-page": "607",
"issue": "6",
"journal-title": "J Infect",
"key": "2776_CR5",
"unstructured": "Ye Q, Wang B, Mao J. The pathogenesis and treatment of the `cytokine storm’ in COVID-19. J Infect. 2020;80(6):607–13 Available from: https://linkinghub.elsevier.com/retrieve/pii/S0163445320301651.",
"volume": "80",
"year": "2020"
},
{
"DOI": "10.1007/s00395-020-0791-5",
"doi-asserted-by": "crossref",
"key": "2776_CR6",
"unstructured": "Rizzo P, Vieceli Dalla Sega F, Fortini F, Marracino L, Rapezzi C, Ferrari R. COVID-19 in the heart and the lungs: could we “Notch” the inflammatory storm? Basic Res Cardiol. 2020;115(3):31. Available from: http://link.springer.com/10.1007/s00395-020-0791-5"
},
{
"DOI": "10.1016/j.jaci.2020.07.009",
"doi-asserted-by": "publisher",
"key": "2776_CR7",
"unstructured": "Laguna-Goya R, Utrero-Rico A, Talayero P, Lasa-Lazaro M, Ramirez-Fernandez A, Naranjo L, et al. IL-6–based mortality risk model for hospitalized patients with COVID-19. J Allergy Clin Immunol. 2020;146(4):799-807.e9. https://doi.org/10.1016/j.jaci.2020.07.009."
},
{
"DOI": "10.1016/j.cell.2020.04.026",
"doi-asserted-by": "crossref",
"key": "2776_CR8",
"unstructured": "Blanco-Melo D, Nilsson-Payant BE, Liu W-C, Uhl S, Hoagland D, Møller R, et al. Imbalanced Host Response to SARS-CoV-2 Drives Development of COVID-19. Cell. 2020;181(5)."
},
{
"DOI": "10.1172/JCI137244",
"author": "G Chen",
"doi-asserted-by": "publisher",
"first-page": "2620",
"issue": "5",
"journal-title": "J Clin Invest.",
"key": "2776_CR9",
"unstructured": "Chen G, Wu D, Guo W, Cao Y, Huang D, Wang H, et al. Clinical and immunological features of severe and moderate coronavirus disease 2019. J Clin Invest. 2020;130(5):2620–9 Available from: https://www.jci.org/articles/view/137244.",
"volume": "130",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"doi-asserted-by": "crossref",
"key": "2776_CR10",
"unstructured": "Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395(10223)."
},
{
"DOI": "10.3390/nu5072502",
"author": "B Prietl",
"doi-asserted-by": "publisher",
"first-page": "2502",
"issue": "7",
"journal-title": "Nutrients",
"key": "2776_CR11",
"unstructured": "Prietl B, Treiber G, Pieber T, Amrein K. Vitamin D and immune function. Nutrients. 2013;5(7):2502–21 Available from: http://www.mdpi.com/2072-6643/5/7/2502.",
"volume": "5",
"year": "2013"
},
{
"DOI": "10.1016/j.nfs.2020.06.001",
"doi-asserted-by": "crossref",
"key": "2776_CR12",
"unstructured": "Biesalski HK. Vitamin D deficiency and co-morbidities in COVID-19 patients – A fatal relationship? NFS J. 2020;20:10–21. Available from: https://linkinghub.elsevier.com/retrieve/pii/S2352364620300067"
},
{
"DOI": "10.1007/s12603-012-0084-2",
"author": "JE Morley",
"doi-asserted-by": "publisher",
"first-page": "601",
"issue": "7",
"journal-title": "J Nutr Health Aging",
"key": "2776_CR13",
"unstructured": "Morley JE, Malmstrom TK, Miller DK. A simple frailty questionnaire (FRAIL) predicts outcomes in middle aged African Americans. J Nutr Health Aging. 2012;16(7):601–8 Available from: http://link.springer.com/10.1007/s12603-012-0084-2.",
"volume": "16",
"year": "2012"
},
{
"DOI": "10.1007/s40618-020-01370-x",
"author": "GE Carpagnano",
"doi-asserted-by": "publisher",
"first-page": "765",
"issue": "4",
"journal-title": "J Endocrinol Invest",
"key": "2776_CR14",
"unstructured": "Carpagnano GE, Di Lecce V, Quaranta VN, Zito A, Buonamico E, Capozza E, et al. Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19. J Endocrinol Invest. 2021;44(4):765–71 Available from: http://link.springer.com/10.1007/s40618-020-01370-x.",
"volume": "44",
"year": "2021"
},
{
"DOI": "10.1093/ajcp/aqaa252",
"author": "D De Smet",
"doi-asserted-by": "publisher",
"first-page": "381",
"issue": "3",
"journal-title": "Am J Clin Pathol",
"key": "2776_CR15",
"unstructured": "De Smet D, De Smet K, Herroelen P, Gryspeerdt S, Martens GA. Serum 25(OH)D level on hospital admission associated with COVID-19 stage and mortality. Am J Clin Pathol. 2021;155(3):381–8 Available from: https://academic.oup.com/ajcp/article/155/3/381/6000689.",
"volume": "155",
"year": "2021"
},
{
"DOI": "10.1136/postgradmedj-2020-138712",
"doi-asserted-by": "crossref",
"key": "2776_CR16",
"unstructured": "Baktash V, Hosack T, Patel N, Shah S, Kandiah P, Van den Abbeele K, et al. Vitamin D status and outcomes for hospitalised older patients with COVID-19. Postgrad Med J. 2020;postgradmedj-2020-138712. Available from: https://pmj.bmj.com/lookup/doi/10.1136/postgradmedj-2020-138712"
},
{
"DOI": "10.3390/nu12092757",
"doi-asserted-by": "crossref",
"key": "2776_CR17",
"unstructured": "Radujkovic A, Hippchen T, Tiwari-Heckler S, Dreher S, Boxberger M, Merle U. Vitamin D Deficiency and Outcome of COVID-19 Patients. Nutrients. 2020;12(9):2757. Available from: https://www.mdpi.com/2072-6643/12/9/2757"
},
{
"key": "2776_CR18",
"unstructured": "Villas Bôas B. IBGE: População sem instrução cai e tempo médio de estudo atinge 9,4 anos. Valor Econômico. 2020 [cited 2021 May 8]. Available from: https://valor.globo.com/brasil/noticia/2020/07/15/ibge-populacao-sem-instrucao-cai-e-tempo-medio-de-estudo-atinge-94-anos.ghtml"
},
{
"DOI": "10.1515/cclm-2020-0369",
"author": "BM Henry",
"doi-asserted-by": "publisher",
"first-page": "1021",
"issue": "7",
"journal-title": "Clin Chem Lab Med",
"key": "2776_CR19",
"unstructured": "Henry BM, de Oliveira MHS, Benoit S, Plebani M, Lippi G. Hematologic, biochemical and immune biomarker abnormalities associated with severe illness and mortality in coronavirus disease 2019 (COVID-19): a meta-analysis. Clin Chem Lab Med. 2020;58(7):1021–8 Available from: https://www.degruyter.com/document/doi/10.1515/cclm-2020-0369/html.",
"volume": "58",
"year": "2020"
},
{
"DOI": "10.1002/jmv.26444",
"author": "Z Tao",
"doi-asserted-by": "publisher",
"first-page": "1478",
"issue": "3",
"journal-title": "J Med Virol",
"key": "2776_CR20",
"unstructured": "Tao Z, Xu J, Chen W, Yang Z, Xu X, Liu L, et al. Anemia is associated with severe illness in COVID-19: a retrospective cohort study. J Med Virol. 2021;93(3):1478–88 Available from: https://onlinelibrary.wiley.com/doi/10.1002/jmv.26444.",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.21037/atm-20-3391",
"author": "C Wang",
"doi-asserted-by": "publisher",
"first-page": "593",
"issue": "9",
"journal-title": "Ann Transl Med",
"key": "2776_CR21",
"unstructured": "Wang C, Deng R, Gou L, Fu Z, Zhang X, Shao F, et al. Preliminary study to identify severe from moderate cases of COVID-19 using combined hematology parameters. Ann Transl Med. 2020;8(9):593 Available from: http://atm.amegroups.com/article/view/42413/html.",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1007/s10654-020-00678-5",
"author": "PE Taneri",
"doi-asserted-by": "publisher",
"first-page": "763",
"issue": "8",
"journal-title": "Eur J Epidemiol",
"key": "2776_CR22",
"unstructured": "Taneri PE, Gómez-Ochoa SA, Llanaj E, Raguindin PF, Rojas LZ, Roa-Díaz ZM, et al. Anemia and iron metabolism in COVID-19: a systematic review and meta-analysis. Eur J Epidemiol. 2020;35(8):763–73 Available from: https://link.springer.com/10.1007/s10654-020-00678-5.",
"volume": "35",
"year": "2020"
},
{
"DOI": "10.3390/jcm9082429",
"doi-asserted-by": "crossref",
"key": "2776_CR23",
"unstructured": "Bellmann-Weiler R, Lanser L, Barket R, Rangger L, Schapfl A, Schaber M, et al. Prevalence and Predictive Value of Anemia and Dysregulated Iron Homeostasis in Patients with COVID-19 Infection. J Clin Med. 2020;9(8):2429. Available from: https://www.mdpi.com/2077-0383/9/8/2429"
},
{
"DOI": "10.1056/NEJMra041809",
"author": "G Weiss",
"doi-asserted-by": "publisher",
"first-page": "1011",
"issue": "10",
"journal-title": "N Engl J Med",
"key": "2776_CR24",
"unstructured": "Weiss G, Goodnough LT. Anemia of chronic disease. N Engl J Med. 2005;352(10):1011–23 Available from: http://www.nejm.org/doi/abs/10.1056/NEJMra041809.",
"volume": "352",
"year": "2005"
},
{
"DOI": "10.1056/NEJMra1804281",
"doi-asserted-by": "crossref",
"key": "2776_CR25",
"unstructured": "Ganz T. Anemia of Inflammation. Longo DL, editor. N Engl J Med. 2019;381(12):1148–57. Available from: http://www.nejm.org/doi/10.1056/NEJMra1804281"
},
{
"DOI": "10.1007/s10238-021-00699-8",
"doi-asserted-by": "crossref",
"key": "2776_CR26",
"unstructured": "Bergamaschi G, Borrelli de Andreis F, Aronico N, Lenti MV, Barteselli C, Merli S, et al. Anemia in patients with Covid-19: pathogenesis and clinical significance. Clin Exp Med. 2021;21(2):239–46. Available from: https://link.springer.com/10.1007/s10238-020-00679-4"
},
{
"DOI": "10.1128/CMR.00228-20",
"doi-asserted-by": "crossref",
"key": "2776_CR27",
"unstructured": "Safiabadi Tali SH, LeBlanc JJ, Sadiq Z, Oyewunmi OD, Camargo C, Nikpour B, et al. Tools and Techniques for Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2)/COVID-19 Detection. Clin Microbiol Rev. 2021;34(3). Available from: https://journals.asm.org/doi/10.1128/CMR.00228-20"
},
{
"DOI": "10.1148/radiol.2020201433",
"author": "D Colombi",
"doi-asserted-by": "publisher",
"first-page": "E86",
"issue": "2",
"journal-title": "Radiology",
"key": "2776_CR28",
"unstructured": "Colombi D, Bodini FC, Petrini M, Maffi G, Morelli N, Milanese G, et al. Well-aerated lung on admitting chest CT to predict adverse outcome in COVID-19 pneumonia. Radiology. 2020;296(2):E86–96 Available from: http://pubs.rsna.org/doi/10.1148/radiol.2020201433.",
"volume": "296",
"year": "2020"
},
{
"DOI": "10.1016/j.clinimag.2020.10.037",
"doi-asserted-by": "crossref",
"key": "2776_CR29",
"unstructured": "Cereser L, Da Re J, Zuiani C, Girometti R. Chest high-resolution computed tomography is associated to short-time progression to severe disease in patients with COVID-19 pneumonia. Clin Imaging. 2021;70:61–6. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0899707120304010"
},
{
"DOI": "10.1016/j.ijid.2020.06.033",
"author": "G Turcato",
"doi-asserted-by": "publisher",
"first-page": "233",
"journal-title": "Int J Infect Dis",
"key": "2776_CR30",
"unstructured": "Turcato G, Panebianco L, Zaboli A, Scheurer C, Ausserhofer D, Wieser A, et al. Correlation between arterial blood gas and CT volumetry in patients with SARS-CoV-2 in the emergency department. Int J Infect Dis. 2020;97:233–5 Available from: https://linkinghub.elsevier.com/retrieve/pii/S1201971220304689.",
"volume": "97",
"year": "2020"
},
{
"DOI": "10.1007/s00330-020-06955-x",
"author": "N Zhang",
"doi-asserted-by": "publisher",
"first-page": "6151",
"issue": "11",
"journal-title": "Eur Radiol",
"key": "2776_CR31",
"unstructured": "Zhang N, Xu X, Zhou L-Y, Chen G, Li Y, Yin H, et al. Clinical characteristics and chest CT imaging features of critically ill COVID-19 patients. Eur Radiol. 2020;30(11):6151–60 Available from: https://link.springer.com/10.1007/s00330-020-06955-x.",
"volume": "30",
"year": "2020"
},
{
"DOI": "10.1146/annurev-physiol-021119-034610",
"author": "SJ Cho",
"doi-asserted-by": "publisher",
"first-page": "433",
"issue": "1",
"journal-title": "Annu Rev Physiol",
"key": "2776_CR32",
"unstructured": "Cho SJ, Stout-Delgado HW. Aging and Lung Disease. Annu Rev Physiol. 2020;82(1):433–59 Available from: https://www.annualreviews.org/doi/10.1146/annurev-physiol-021119-034610.",
"volume": "82",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30920-X",
"author": "H Li",
"doi-asserted-by": "publisher",
"first-page": "1517",
"issue": "10235",
"journal-title": "Lancet",
"key": "2776_CR33",
"unstructured": "Li H, Liu L, Zhang D, Xu J, Dai H, Tang N, et al. SARS-CoV-2 and viral sepsis: observations and hypotheses. Lancet. 2020;395(10235):1517–20 Available from: https://linkinghub.elsevier.com/retrieve/pii/S014067362030920X.",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1007/s00011-020-01372-8",
"doi-asserted-by": "crossref",
"key": "2776_CR34",
"unstructured": "Meftahi GH, Jangravi Z, Sahraei H, Bahari Z. The possible pathophysiology mechanism of cytokine storm in elderly adults with COVID-19 infection: the contribution of “inflame-aging.” Inflamm Res 2020;69(9):825–839. Available from: http://link.springer.com/10.1007/s00011-020-01372-8"
},
{
"DOI": "10.1038/s41577-020-0317-2",
"author": "MD Park",
"doi-asserted-by": "publisher",
"first-page": "351",
"issue": "6",
"journal-title": "Nat Rev Immunol",
"key": "2776_CR35",
"unstructured": "Park MD. Macrophages: a Trojan horse in COVID-19? Nat Rev Immunol. 2020;20(6):351 Available from: http://www.nature.com/articles/s41577-020-0317-2.",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1038/s41423-020-0402-2",
"author": "M Zheng",
"doi-asserted-by": "publisher",
"first-page": "533",
"issue": "5",
"journal-title": "Cell Mol Immunol",
"key": "2776_CR36",
"unstructured": "Zheng M, Gao Y, Wang G, Song G, Liu S, Sun D, et al. Functional exhaustion of antiviral lymphocytes in COVID-19 patients. Cell Mol Immunol. 2020;17(5):533–5 Available from: http://www.nature.com/articles/s41423-020-0402-2.",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1007/s11357-014-9694-4",
"doi-asserted-by": "crossref",
"key": "2776_CR37",
"unstructured": "De Vita F, Lauretani F, Bauer J, Bautmans I, Shardell M, Cherubini A, et al. Relationship between vitamin D and inflammatory markers in older individuals. Age (Omaha). 2014;36(4):9694. Available from: http://link.springer.com/10.1007/s11357-014-9694-4"
},
{
"DOI": "10.1016/j.resp.2020.103548",
"doi-asserted-by": "crossref",
"key": "2776_CR38",
"unstructured": "loganathan S, Kuppusamy M, Wankhar W, Gurugubelli KR, Mahadevappa VH, Lepcha L, et al. Angiotensin-converting enzyme 2 (ACE2): COVID 19 gate way to multiple organ failure syndromes. Respir Physiol Neurobiol. 2021;283:103548. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1569904820302068"
},
{
"DOI": "10.1016/j.lfs.2005.09.038",
"author": "X Xudong",
"doi-asserted-by": "publisher",
"first-page": "2166",
"issue": "19",
"journal-title": "Life Sci",
"key": "2776_CR39",
"unstructured": "Xudong X, Junzhu C, Xingxiang W, Furong Z, Yanrong L. Age- and gender-related difference of ACE2 expression in rat lung. Life Sci. 2006;78(19):2166–71 Available from: https://linkinghub.elsevier.com/retrieve/pii/S0024320505010386.",
"volume": "78",
"year": "2006"
},
{
"DOI": "10.1016/j.coph.2006.03.001",
"author": "K Kuba",
"doi-asserted-by": "publisher",
"first-page": "271",
"issue": "3",
"journal-title": "Curr Opin Pharmacol",
"key": "2776_CR40",
"unstructured": "Kuba K, Imai Y, Penninger J. Angiotensin-converting enzyme 2 in lung diseases. Curr Opin Pharmacol. 2006;6(3):271–6 Available from: https://linkinghub.elsevier.com/retrieve/pii/S1471489206000579.",
"volume": "6",
"year": "2006"
},
{
"DOI": "10.3389/fendo.2021.644298",
"doi-asserted-by": "crossref",
"key": "2776_CR41",
"unstructured": "Easty DJ, Farr CJ, Hennessy BT. New Roles for Vitamin D Superagonists: From COVID to Cancer. Front Endocrinol (Lausanne). 2021;12. Available from: https://www.frontiersin.org/articles/10.3389/fendo.2021.644298/full"
},
{
"DOI": "10.1002/path.1570",
"doi-asserted-by": "crossref",
"key": "2776_CR42",
"unstructured": "Hamming I, Timens W, Bulthuis M, Lely A, Navis G, van Goor H. Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J Pathol. 2004;203(2):631–7. Available from: http://doi.wiley.com/10.1002/path.1570"
},
{
"DOI": "10.1172/JCI0215219",
"author": "YC Li",
"doi-asserted-by": "publisher",
"first-page": "229",
"issue": "2",
"journal-title": "J Clin Invest",
"key": "2776_CR43",
"unstructured": "Li YC, Kong J, Wei M, Chen Z-F, Liu SQ, Cao L-P. 1,25-Dihydroxyvitamin D3 is a negative endocrine regulator of the renin-angiotensin system. J Clin Invest. 2002;110(2):229–38 Available from: http://www.jci.org/articles/view/15219.",
"volume": "110",
"year": "2002"
},
{
"DOI": "10.1074/jbc.M705495200",
"author": "W Yuan",
"doi-asserted-by": "publisher",
"first-page": "29821",
"issue": "41",
"journal-title": "J Biol Chem",
"key": "2776_CR44",
"unstructured": "Yuan W, Pan W, Kong J, Zheng W, Szeto FL, Wong KE, et al. 1,25-Dihydroxyvitamin D3 suppresses renin gene transcription by blocking the activity of the cyclic AMP response element in the renin gene promoter. J Biol Chem. 2007;282(41):29821–30 Available from: https://linkinghub.elsevier.com/retrieve/pii/S0021925820717400.",
"volume": "282",
"year": "2007"
},
{
"DOI": "10.3892/ijmm.2021.4865",
"doi-asserted-by": "crossref",
"key": "2776_CR45",
"unstructured": "Turrubiates-Hernández F, Sánchez-Zuno G, González-Estevez G, Hernández-Bello J, Macedo-Ojeda G, Muñoz-Valle J. Potential immunomodulatory effects of vitamin D in the prevention of severe coronavirus disease 2019: An ally for Latin America (Review). Int J Mol Med. 2021;47(4):32. Available from: http://www.spandidos-publications.com/10.3892/ijmm.2021.4865"
},
{
"DOI": "10.3390/ijms22041963",
"doi-asserted-by": "crossref",
"key": "2776_CR46",
"unstructured": "Subedi L, Tchen S, Gaire BP, Hu B, Hu K. Adjunctive Nutraceutical Therapies for COVID-19. Int J Mol Sci. 2021;22(4):1963. Available from: https://www.mdpi.com/1422-0067/22/4/1963"
},
{
"DOI": "10.1016/j.cca.2020.05.044",
"doi-asserted-by": "crossref",
"key": "2776_CR47",
"unstructured": "Lotfi M, Hamblin MR, Rezaei N. COVID-19: transmission, prevention, and potential therapeutic opportunities. Clin Chim Acta. 2020;508:254–66. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0009898120302503."
},
{
"DOI": "10.1001/jama.2020.26848",
"doi-asserted-by": "crossref",
"key": "2776_CR48",
"unstructured": "Murai IH, Fernandes AL, Sales LP, Pinto AJ, Goessler KF, Duran CSC, et al. Effect of a Single High Dose of Vitamin D 3 on Hospital Length of Stay in Patients With Moderate to Severe COVID-19. JAMA. 2021 ;325(11):1053. Available from: https://jamanetwork.com/journals/jama/fullarticle/2776738"
},
{
"DOI": "10.1016/j.nut.2020.111055",
"doi-asserted-by": "crossref",
"key": "2776_CR49",
"unstructured": "Cereda E, Bogliolo L, Lobascio F, Barichella M, Zecchinelli AL, Pezzoli G, et al. Vitamin D supplementation and outcomes in coronavirus disease 2019 (COVID-19) patients from the outbreak area of Lombardy, Italy. Nutrition 2021;82:111055. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0899900720303385"
},
{
"DOI": "10.1016/j.jsbmb.2020.105751",
"doi-asserted-by": "crossref",
"key": "2776_CR50",
"unstructured": "Entrenas Castillo M, Entrenas Costa LM, Vaquero Barrios JM, Alcalá Díaz JF, López Miranda J, Bouillon R, et al. “Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study.” J Steroid Biochem Mol Biol. 2020;203:105751. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0960076020302764"
},
{
"DOI": "10.1016/j.jamda.2020.05.045",
"author": "C Bonanad",
"doi-asserted-by": "publisher",
"first-page": "915",
"issue": "7",
"journal-title": "J Am Med Dir Assoc",
"key": "2776_CR51",
"unstructured": "Bonanad C, García-Blas S, Tarazona-Santabalbina F, Sanchis J, Bertomeu-González V, Fácila L, et al. The effect of age on mortality in patients with COVID-19: a Meta-analysis with 611,583 subjects. J Am Med Dir Assoc. 2020;21(7):915–8 Available from: https://linkinghub.elsevier.com/retrieve/pii/S1525861020304412.",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1503/cmaj.050051",
"author": "K Rockwood",
"doi-asserted-by": "publisher",
"first-page": "489",
"issue": "5",
"journal-title": "Can Med Assoc J",
"key": "2776_CR52",
"unstructured": "Rockwood K. A global clinical measure of fitness and frailty in elderly people. Can Med Assoc J. 2005;173(5):489–95 Available from: http://www.cmaj.ca/cgi/doi/10.1503/cmaj.050051.",
"volume": "173",
"year": "2005"
},
{
"DOI": "10.1093/gerona/56.3.M146",
"doi-asserted-by": "crossref",
"key": "2776_CR53",
"unstructured": "Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: Evidence for a phenotype. Journals Gerontol - Ser A Biol Sci Med Sci. 2001;56(3):M146--56. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=11253156"
}
],
"reference-count": 53,
"references-count": 53,
"relation": {},
"score": 1,
"short-container-title": [
"BMC Geriatr"
],
"short-title": [],
"source": "Crossref",
"subject": [
"Geriatrics and Gerontology"
],
"subtitle": [],
"title": [
"Chronic diseases, chest computed tomography, and laboratory tests as predictors of severe respiratory failure and death in elderly Brazilian patients hospitalized with COVID-19: a prospective cohort study"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "22"
}
