Clinical course of COVID-19 patients treated with ECMO: A multicenter study in Daegu, South Korea
et al., Heart & Lung, doi:10.1016/j.hrtlng.2020.10.010, Dec 2020
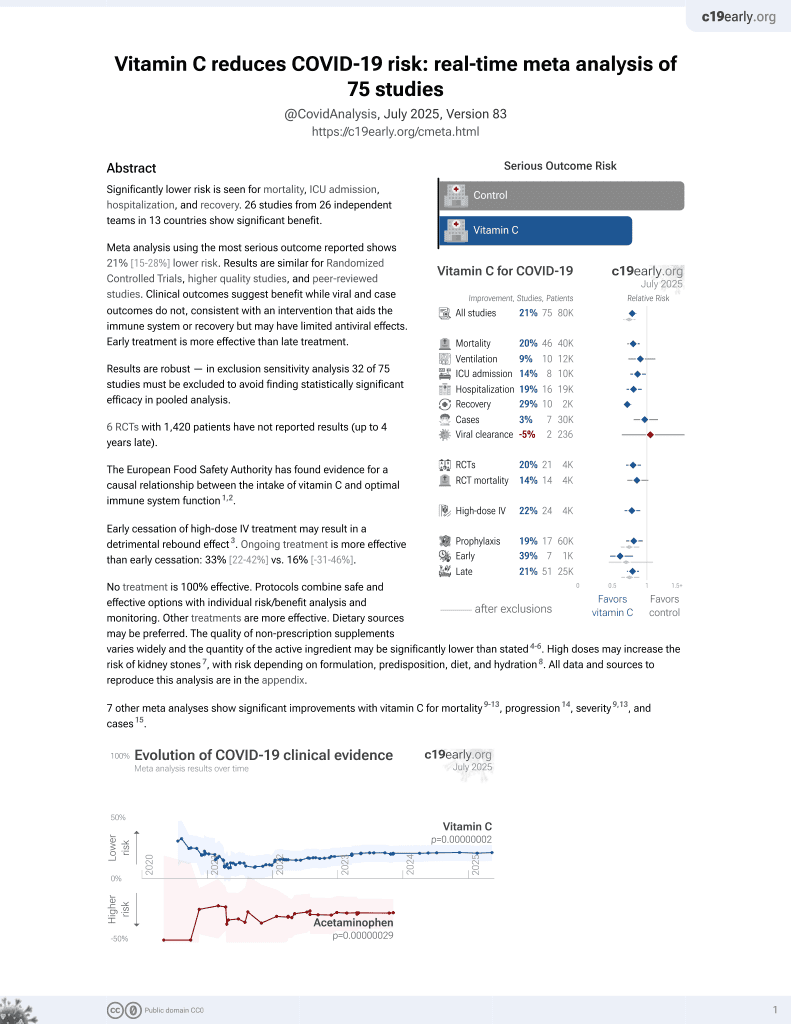
Vitamin C for COVID-19
6th treatment shown to reduce risk in
September 2020, now with p = 0.000000069 from 72 studies, recognized in 22 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
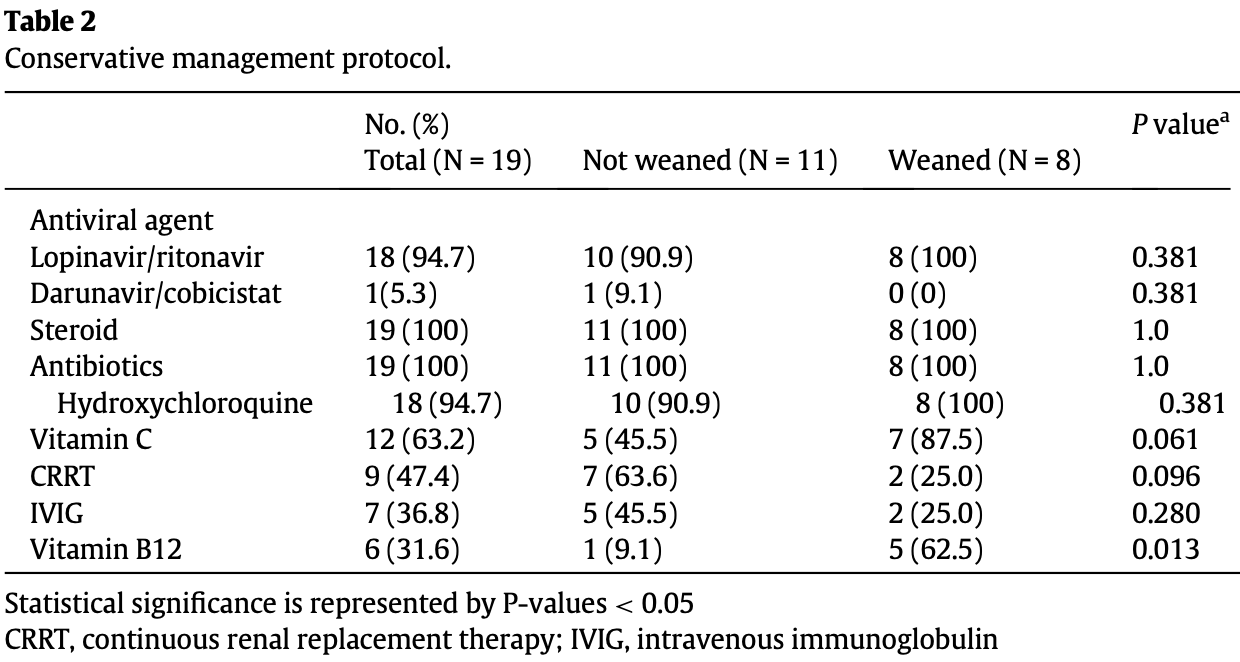
Retrospective 19 COVID-19 ECMO patients in South Korea, showing a higher rate of weaning from ECMO with vitamin C treatment, without statistical significance. Authors perform multivariate analysis but do not provide full results, only reporting p > 0.05.
This is the 8th of 72 COVID-19 controlled studies for vitamin C, which collectively show efficacy with p=0.000000069.
20 studies are RCTs, which show efficacy with p=0.0016.
This study is excluded in the after exclusion results of meta-analysis:
very late stage, ECMO patients.
Study covers vitamin B12 and vitamin C.
|
risk of no recovery, 51.4% lower, RR 0.49, p = 0.15, treatment 5 of 12 (41.7%), control 6 of 7 (85.7%), NNT 2.3, weaning from ECMO.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Jang et al., 16 Dec 2020, retrospective, South Korea, peer-reviewed, median age 63.0, 10 authors, study period February 2020 - April 2020, dosage not specified.
Contact: whiteuri09@gmail.com.
Clinical course of COVID-19 patients treated with ECMO: A multicenter study in Daegu, South Korea
Heart & Lung, doi:10.1016/j.hrtlng.2020.10.010
Background: The COVID-19 pandemic has caused an epidemic of critical patients, some of whom have been treated with extracorporeal membrane oxygenation (ECMO). This purpose of study is to describe the clinical course of COVID-19 patients treated with ECMO. Methods: A multicentered study of critical patients with COVID-19 treated at six hospitals in Daegu was conducted between January and April 2020. Results: Among the 80 patients receiving mechanical ventilation support, 19 (24%) were treated with ECMO included (median age 63.0 years). Eight of the 19 patients (42%) were weaned off ECMO (9.8 days, IQR 7.0-13.7). Among them, four patients were also weaned off mechanical ventilation (33.4 days, IQR 29.3 -35.7), three were still receiving mechanical ventilation (50.9 days), and one expired after ECMO weaning. According to the univariate analysis, the factor that was associated with successful ECMO weaning was vitamin B12 treatment (p = 0.028). Conclusions: During the COVID-19 epidemic, ECMO weaning and mortality rates were 42% and 58%, respectively.
Ethical approval All studies were approved by the national ethics committee.
Declaration of Competing Interests The authors have no conflicts of interest to declare.
References
Alpha, Lawrence, Rajiv, Orlando, Ramesh, Intravenous vitamin C as adjunctive therapy for enterovirus/rhinovirus induced acute respiratory distress syndrome, World J Crit Care Med
Alshahrani, Sindi, Alshamsi, Al-Omari, El Tahan et al., Extracorporeal membrane oxygenation for severe Middle East respiratory syndrome coronavirus, Ann Intensive Care
Arabi, Al-Omari, Mandourah, Al-Hameed, Sindi et al., Critically Ill patients with the middle east respiratory syndrome: A multicenter retrospective cohort study, Crit Care Med
Australia, Jones, Bailey, Beca, Extracorporeal membrane oxygenation for 2009 influenza A(H1N1) acute respiratory distress syndrome, JAMA
Berger, Oudemans-Van Straaten, Vitamin C supplementation in the critically ill patient, Curr Opin Clin Nutr Metab Care
Chen, Zhou, Dong, Qu, Gong et al., Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study, Lancet
Fisher, Kraskauskas, Martin, Farkas, Wegelin et al., Mechanisms of attenuation of abdominal sepsis induced acute lung injury by ascorbic acid, Am J Physiol Lung Cell Mol Physiol
Fisher, Seropian, Kraskauskas, Thakkae, Voelkel et al., Ascorbic acid attenuates lipopolysaccharide induced acute lung injury, Crit Care Med
Fisher, Seropian, Kraskauskas, Thakkar, Voelkel et al., Ascorbic acid attenuates lipopolysaccharide-induced acute lung injury, Crit Care Med
Force, Ranieri, Rubenfeld, Thompson, Ferguson, Acute respiratory distress syndrome: the Berlin Definition, JAMA
Fowler, Aa, Syed, Knowlson, Sculthorpe et al., Medical respiratory intensive care unit nursing. Phase I safety trial of intravenous ascorbic acid in patients with severe sepsis, J Transl Med
Frank, Gutierrez, Jones, Allen, Dobbs, Matthay MA Low tidal volume reduces epithelial and endothelial injury in acid-injured rat lungs, Am J Respir Crit Care Med
Gaies, Gurney, Yen, Napoli, Gajarski et al., Vasoactiveinotropic score as a predictor of morbidity and mortality in infants after cardiopulmonary bypass, Pediatr Crit Care Med
Gattinoni, Tonetti, Cressoni, Cadringher, Herrmann et al., Ventilator-related causes of lung injury: the mechanical power, Intensive Care Med
Goligher, Tomlinson, Hajage, Wijeysundera, Fan et al., Extracorporeal membrane oxygenation for severe acute respiratory distress syndrome and posterior probability of mortality benefit in a post hoc bayesian analysis of a randomized clinical trial, JAMA
Grasso, Stripoli, Mazzone, Pezzuto, Lacitignola et al., Low respiratory rate plus minimally invasive extracorporeal Co2 removal decreases systemic and pulmonary inflammatory mediators in experimental Acute Respiratory Distress Syndrome, Crit Care Med
Huang, Wang, Li, Ren, Zhao et al., Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet
Jacobs, Stammers, Louis, Hayanga, Firstenberg et al., Extracorporeal membrane oxygenation in the treatment of severe pulmonary and cardiac compromise in coronavirus disease 2019: Experience with 32 patients, ASAIO
Li, Guan, Wu, Wang, Zhou et al., Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia, N Engl J Med
Luyt, Brechot, Demondion, Jovanovic, Hekimian et al., Brain injury during venovenous extracorporeal membrane oxygenation, Intensive Care Med
Noah, Peek, Finney, Griffiths, Harrison et al., Referral to an extracorporeal membrane oxygenation center and mortality among patients with severe 2009 influenza A(H1N1), JAMA
Osho, Moonsamy, Hibbert, Shelton, Trahanas et al., Venovenous extracorporeal membrane oxygenation for respiratory failure in COVID-19 patients: Early experience from a major academic medical center in North America, Ann Surg
Phelan, Katz, Lo, The novel coronavirus originating in Wuhan, China: Challenges for global health governance, JAMA
Rhodes, Evans, Alhazzani, Levy, Antonelli et al., Surviving sepsis campaign: international guidelines for management of sepsis and septic shock: 2016, Intensive Care Med
Schmidt, Hajage, Lebreton, Monsel, Voiriot et al., Extracorporeal membrane oxygenation for severe acute respiratory distress syndrome associated with COVID-19: A retrospective cohort study, Lancet Respir Med
Schwartz, Munoz, Schneider, Mak, Kaskel et al., New equations to estimate GFR in children with CKD, J Am Soc Nephrol
Wang, Hu, Hu, Zhu, Liu et al., Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China, JAMA
Wu, Mcgoogan, Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: Summary of a report of 72314 cases from the Chinese center for disease control and prevention, JAMA
Yang, Yu, Xu, Shu, Xia et al., Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study, Lancet Respir Med
Zhang, Hu, Luo, Fang, Li, Clinical features and short-term outcomes of 221 patients with COVID-19 in Wuhan, China, J Clin Virol
Zhou, Yu, Du, Fan, Liu et al., Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study, Lancet
DOI record:
{
"DOI": "10.1016/j.hrtlng.2020.10.010",
"ISSN": [
"0147-9563"
],
"URL": "http://dx.doi.org/10.1016/j.hrtlng.2020.10.010",
"alternative-id": [
"S0147956320304027"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Clinical course of COVID-19 patients treated with ECMO: A multicenter study in Daegu, South Korea"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Heart & Lung"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.hrtlng.2020.10.010"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2020 Elsevier Inc. All rights reserved."
}
],
"author": [
{
"affiliation": [],
"family": "Jang",
"given": "Woo Sung",
"sequence": "first"
},
{
"affiliation": [],
"family": "Kim",
"given": "JaeBum",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Baek",
"given": "Jonghyun",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jung",
"given": "Hanna",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jang",
"given": "Jae Seok",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Park",
"given": "Jae Seok",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Oh",
"given": "Tak-Hyuk",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jang",
"given": "Se Yong",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kim",
"given": "Yun Seok",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kwon",
"given": "Yong Shik",
"sequence": "additional"
}
],
"container-title": "Heart & Lung",
"container-title-short": "Heart & Lung",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"clinicalkey.jp",
"heartandlung.org",
"clinicalkey.com",
"clinicalkey.es",
"clinicalkey.com.au",
"clinicalkey.fr",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2020,
10,
19
]
],
"date-time": "2020-10-19T22:04:05Z",
"timestamp": 1603145045000
},
"deposited": {
"date-parts": [
[
2021,
12,
20
]
],
"date-time": "2021-12-20T05:47:30Z",
"timestamp": 1639979250000
},
"indexed": {
"date-parts": [
[
2022,
5,
23
]
],
"date-time": "2022-05-23T07:33:54Z",
"timestamp": 1653291234549
},
"is-referenced-by-count": 5,
"issue": "1",
"issued": {
"date-parts": [
[
2021,
1
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2021,
1
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
1,
1
]
],
"date-time": "2021-01-01T00:00:00Z",
"timestamp": 1609459200000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S0147956320304027?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S0147956320304027?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "21-27",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2021,
1
]
]
},
"published-print": {
"date-parts": [
[
2021,
1
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.1001/jama.2020.2648",
"article-title": "Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: Summary of a report of 72314 cases from the Chinese center for disease control and prevention",
"author": "Wu",
"doi-asserted-by": "crossref",
"first-page": "1239",
"journal-title": "JAMA",
"key": "10.1016/j.hrtlng.2020.10.010_bib0001",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30566-3",
"article-title": "et al: Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study",
"author": "Zhou",
"doi-asserted-by": "crossref",
"first-page": "1054",
"journal-title": "Lancet",
"key": "10.1016/j.hrtlng.2020.10.010_bib0002",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.1585",
"article-title": "et al: Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China",
"author": "Wang",
"doi-asserted-by": "crossref",
"first-page": "1061",
"journal-title": "JAMA",
"key": "10.1016/j.hrtlng.2020.10.010_bib0003",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1001/jama.2018.14276",
"article-title": "Extracorporeal membrane oxygenation for severe acute respiratory distress syndrome and posterior probability of mortality benefit in a post hoc bayesian analysis of a randomized clinical trial",
"author": "Goligher",
"doi-asserted-by": "crossref",
"first-page": "2251",
"journal-title": "JAMA",
"key": "10.1016/j.hrtlng.2020.10.010_bib0004",
"volume": "320",
"year": "2018"
},
{
"DOI": "10.1186/s13613-017-0350-x",
"article-title": "et al: Extracorporeal membrane oxygenation for severe Middle East respiratory syndrome coronavirus",
"author": "Alshahrani",
"doi-asserted-by": "crossref",
"first-page": "3",
"journal-title": "Ann Intensive Care",
"key": "10.1016/j.hrtlng.2020.10.010_bib0005",
"volume": "8",
"year": "2018"
},
{
"DOI": "10.1001/jama.2009.1535",
"article-title": "Extracorporeal membrane oxygenation for 2009 influenza A(H1N1) acute respiratory distress syndrome",
"author": "Davies",
"doi-asserted-by": "crossref",
"first-page": "1888",
"journal-title": "JAMA",
"key": "10.1016/j.hrtlng.2020.10.010_bib0006",
"volume": "302",
"year": "2009"
},
{
"DOI": "10.1001/jama.2011.1471",
"article-title": "Referral to an extracorporeal membrane oxygenation center and mortality among patients with severe 2009 influenza A(H1N1)",
"author": "Noah",
"doi-asserted-by": "crossref",
"first-page": "1659",
"journal-title": "JAMA",
"key": "10.1016/j.hrtlng.2020.10.010_bib0007",
"volume": "306",
"year": "2011"
},
{
"key": "10.1016/j.hrtlng.2020.10.010_bib0008",
"unstructured": "(2020) WHO: Clinical management of severe acute respiratory infection when COVID-19 is suspected: interim guidance, 28 January 2020"
},
{
"DOI": "10.1016/S2213-2600(20)30079-5",
"article-title": "et al: Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study",
"author": "Yang",
"doi-asserted-by": "crossref",
"first-page": "478",
"journal-title": "Lancet Respir Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0009",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1016/j.jcv.2020.104364",
"article-title": "et al: Clinical features and short-term outcomes of 221 patients with COVID-19 in Wuhan, China",
"author": "Zhang",
"doi-asserted-by": "crossref",
"journal-title": "J Clin Virol",
"key": "10.1016/j.hrtlng.2020.10.010_bib0010",
"volume": "127",
"year": "2020"
},
{
"article-title": "et al: Acute respiratory distress syndrome: the Berlin Definition",
"author": "Force",
"first-page": "2526",
"journal-title": "JAMA",
"key": "10.1016/j.hrtlng.2020.10.010_bib0011",
"volume": "307",
"year": "2012"
},
{
"DOI": "10.1007/s00134-017-4683-6",
"article-title": "Surviving sepsis campaign: international guidelines for management of sepsis and septic shock: 2016",
"author": "Rhodes",
"doi-asserted-by": "crossref",
"first-page": "304",
"journal-title": "Intensive Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0012",
"volume": "43",
"year": "2017"
},
{
"DOI": "10.1097/PCC.0b013e3181b806fc",
"article-title": "Vasoactive-inotropic score as a predictor of morbidity and mortality in infants after cardiopulmonary bypass",
"author": "Gaies",
"doi-asserted-by": "crossref",
"first-page": "234",
"journal-title": "Pediatr Crit Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0013",
"volume": "11",
"year": "2010"
},
{
"DOI": "10.1681/ASN.2008030287",
"article-title": "New equations to estimate GFR in children with CKD",
"author": "Schwartz",
"doi-asserted-by": "crossref",
"first-page": "629",
"journal-title": "J Am Soc Nephrol",
"key": "10.1016/j.hrtlng.2020.10.010_bib0014",
"volume": "20",
"year": "2009"
},
{
"DOI": "10.1097/CCM.0000000000002621",
"article-title": "Critically Ill patients with the middle east respiratory syndrome: A multicenter retrospective cohort study",
"author": "Arabi",
"doi-asserted-by": "crossref",
"first-page": "1683",
"journal-title": "Crit Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0015",
"volume": "45",
"year": "2017"
},
{
"DOI": "10.1016/S0140-6736(20)30211-7",
"article-title": "et al: Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study",
"author": "Chen",
"doi-asserted-by": "crossref",
"first-page": "507",
"journal-title": "Lancet",
"key": "10.1016/j.hrtlng.2020.10.010_bib0016",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"article-title": "et al: Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "497",
"journal-title": "Lancet",
"key": "10.1016/j.hrtlng.2020.10.010_bib0017",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1056/NEJMoa2001316",
"article-title": "Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "1199",
"journal-title": "N Engl J Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0018",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.1097",
"article-title": "The novel coronavirus originating in Wuhan, China: Challenges for global health governance",
"author": "Phelan",
"doi-asserted-by": "crossref",
"first-page": "709",
"journal-title": "JAMA",
"key": "10.1016/j.hrtlng.2020.10.010_bib0019",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1097/MAT.0000000000001185",
"article-title": "Extracorporeal membrane oxygenation in the treatment of severe pulmonary and cardiac compromise in coronavirus disease 2019: Experience with 32 patients",
"author": "Jacobs",
"doi-asserted-by": "crossref",
"first-page": "722",
"journal-title": "ASAIO",
"key": "10.1016/j.hrtlng.2020.10.010_bib0020",
"volume": "66",
"year": "2020"
},
{
"DOI": "10.1016/S2213-2600(20)30328-3",
"article-title": "Extracorporeal membrane oxygenation for severe acute respiratory distress syndrome associated with COVID-19: A retrospective cohort study",
"author": "Schmidt",
"doi-asserted-by": "crossref",
"journal-title": "Lancet Respir Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0021",
"year": "2020"
},
{
"DOI": "10.1097/SLA.0000000000004084",
"article-title": "Veno-venous extracorporeal membrane oxygenation for respiratory failure in COVID-19 patients: Early experience from a major academic medical center in North America",
"author": "Osho",
"doi-asserted-by": "crossref",
"first-page": "e75",
"journal-title": "Ann Surg",
"key": "10.1016/j.hrtlng.2020.10.010_bib0022",
"volume": "272",
"year": "2020"
},
{
"DOI": "10.1007/s00134-016-4318-3",
"article-title": "Brain injury during venovenous extracorporeal membrane oxygenation",
"author": "Luyt",
"doi-asserted-by": "crossref",
"first-page": "897",
"journal-title": "Intensive Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0023",
"volume": "42",
"year": "2016"
},
{
"DOI": "10.5492/wjccm.v6.i1.85",
"article-title": "Intravenous vitamin C as adjunctive therapy for enterovirus/rhinovirus induced acute respiratory distress syndrome",
"author": "Alpha",
"doi-asserted-by": "crossref",
"first-page": "85",
"journal-title": "World J Crit Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0024",
"volume": "6",
"year": "2017"
},
{
"DOI": "10.1097/CCM.0b013e3182120cb8",
"article-title": "Ascorbic acid attenuates lipopolysaccharide-induced acute lung injury",
"author": "25. Fisher",
"doi-asserted-by": "crossref",
"first-page": "1454",
"journal-title": "Crit Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0025",
"volume": "39",
"year": "2011"
},
{
"DOI": "10.1097/MCO.0000000000000148",
"article-title": "Vitamin C supplementation in the critically ill patient",
"author": "Berger",
"doi-asserted-by": "crossref",
"first-page": "193",
"journal-title": "Curr Opin Clin Nutr Metab Care",
"key": "10.1016/j.hrtlng.2020.10.010_bib0026",
"volume": "18",
"year": "2015"
},
{
"DOI": "10.1164/ajrccm.165.2.2108087",
"article-title": "Matthay MA Low tidal volume reduces epithelial and endothelial injury in acid-injured rat lungs",
"author": "Frank",
"doi-asserted-by": "crossref",
"first-page": "242",
"journal-title": "Am J Respir Crit Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0027",
"volume": "165",
"year": "2002"
},
{
"DOI": "10.1007/s00134-016-4505-2",
"article-title": "Ventilator-related causes of lung injury: the mechanical power",
"author": "Gattinoni",
"doi-asserted-by": "crossref",
"first-page": "1567",
"journal-title": "Intensive Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0028",
"volume": "42",
"year": "2016"
},
{
"DOI": "10.1097/CCM.0000000000000312",
"article-title": "Low respiratory rate plus minimally invasive extracorporeal Co2 removal decreases systemic and pulmonary inflammatory mediators in experimental Acute Respiratory Distress Syndrome",
"author": "Grasso",
"doi-asserted-by": "crossref",
"first-page": "e451",
"journal-title": "Crit Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0029",
"volume": "42",
"year": "2014"
},
{
"DOI": "10.1152/ajplung.00300.2011",
"article-title": "Mechanisms of attenuation of abdominal sepsis induced acute lung injury by ascorbic acid",
"author": "Fisher",
"doi-asserted-by": "crossref",
"first-page": "L20",
"journal-title": "Am J Physiol Lung Cell Mol Physiol",
"key": "10.1016/j.hrtlng.2020.10.010_bib0030",
"volume": "303",
"year": "2012"
},
{
"DOI": "10.1097/CCM.0b013e3182120cb8",
"article-title": "Ascorbic acid attenuates lipopolysaccharide induced acute lung injury",
"author": "Fisher",
"doi-asserted-by": "crossref",
"first-page": "1454",
"issue": "6",
"journal-title": "Crit Care Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0031",
"volume": "39",
"year": "2011"
},
{
"DOI": "10.1186/1479-5876-12-32",
"article-title": "Medical respiratory intensive care unit nursing. Phase I safety trial of intravenous ascorbic acid in patients with severe sepsis",
"author": "Fowler",
"doi-asserted-by": "crossref",
"first-page": "32",
"journal-title": "J Transl Med",
"key": "10.1016/j.hrtlng.2020.10.010_bib0032",
"volume": "12",
"year": "2014"
}
],
"reference-count": 32,
"references-count": 32,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S0147956320304027"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Cardiology and Cardiovascular Medicine",
"Critical Care and Intensive Care Medicine",
"Pulmonary and Respiratory Medicine"
],
"subtitle": [],
"title": "Clinical course of COVID-19 patients treated with ECMO: A multicenter study in Daegu, South Korea",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy",
"volume": "50"
}