Anti-androgens may protect against severe COVID-19 outcomes: results from a prospective cohort study of 77 hospitalized men
et al., Journal of the European Academy of Dermatology and Venereology, doi:10.1111/jdv.16953, NCT04368897, Sep 2020
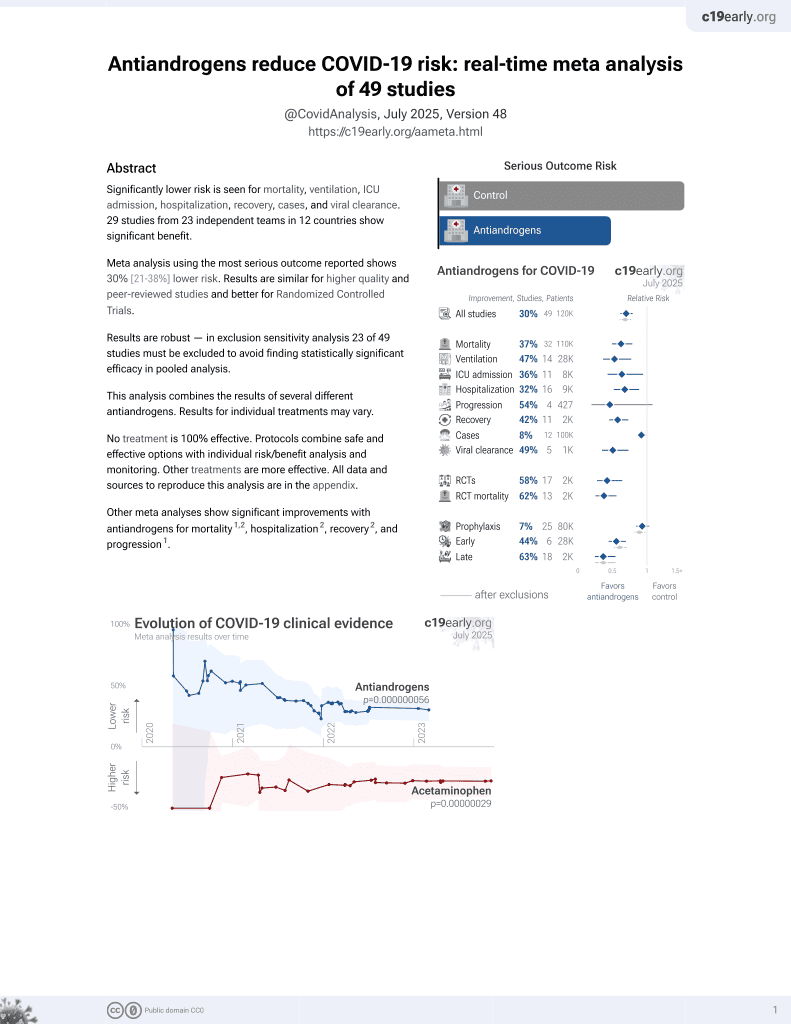
7th treatment shown to reduce risk in
September 2020, now with p = 0.000000056 from 49 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
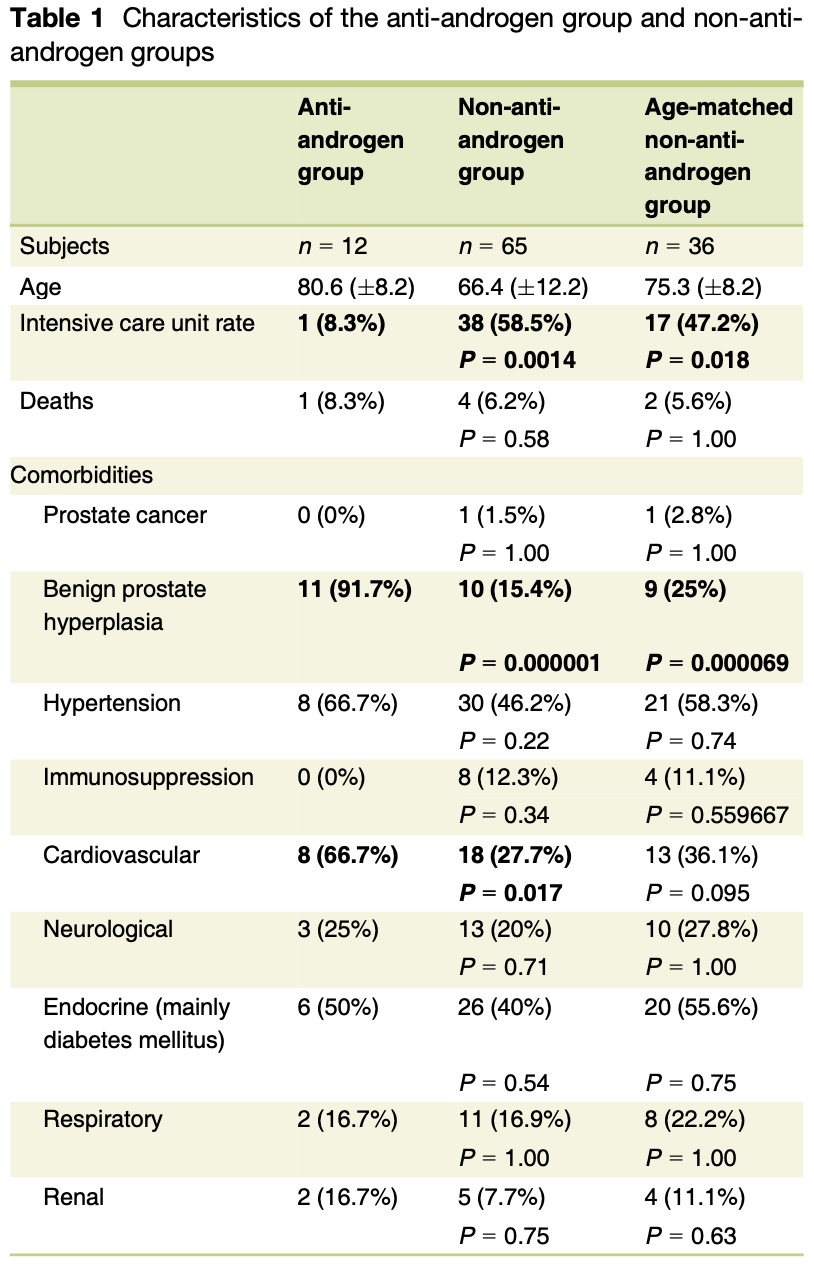
Prospective study of 77 men hospitalized with COVID-19, 12 taking antiandrogens (9 dutasteride, 2 finasteride, 1 spironolactone), showing lower ICU admission with treatment (statistically significant with age-matched controls only when excluding the spironolactone patient). NCT04368897 (history).
|
risk of ICU admission, 81.0% lower, RR 0.19, p = 0.08, treatment 1 of 12 (8.3%), control 17 of 36 (47.2%), NNT 2.6, adjusted per study, age-matched controls.
|
|
risk of ICU admission, 86.0% lower, RR 0.14, p = 0.04, treatment 1 of 12 (8.3%), control 38 of 65 (58.5%), NNT 2.0, adjusted per study, all controls.
|
|
risk of death, 50.0% higher, RR 1.50, p = 1.00, treatment 1 of 12 (8.3%), control 2 of 36 (5.6%), age-matched controls.
|
|
risk of death, 35.4% higher, RR 1.35, p = 0.58, treatment 1 of 12 (8.3%), control 4 of 65 (6.2%), all controls.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Goren et al., 25 Sep 2020, prospective, Brazil, peer-reviewed, 15 authors, trial NCT04368897 (history).
Are SARS‐CoV‐2 IgA antibodies in paediatric patients with chilblain‐like lesions indicative of COVID‐19 asymptomatic or paucisymptomatic infection?
Journal of the European Academy of Dermatology and Venereology, doi:10.1111/jdv.16934
was positive in eight cases, borderline in two, and negative in three, including the COVID-19 patient. Overall, serology for S1-specific IgA and IgG in the 30 patients shows that 16 (53.3%) were positive for IgA, whereas IgG was detectable in five (16.6%; Fig. 1f ). We have recently reported that high levels of IgG and IgA can be detected in adult patients with severe COVID-19, while IgA, and to a lower extent IgG, is increased in asymptomatic individuals. 6 As IgA is the most abundant antibody at mucosal sites, a strong local protection may prevent viral spread and damage to the respiratory tract, explaining the lack of symptoms. The ELISA used for the detection of anti-S1 IgG and IgA has been demonstrated to be specific and sensitive. 7, 8 Of note, antibodies against S1 are often neutralizing 9 and may prevent severe disease and further immune responses. 6 Our findings indicate that, similar to asymptomatic adults, paediatric patients would respond to SARS-CoV-2 producing more IgA than IgG. On the other hand, a single patient had detectable IgG against SARS-CoV-2 nucleoprotein. Anti-nucleoprotein IgG is present in the great majority of hospitalized adult patients, but only in one-third of paucisymptomatic individuals, suggesting that disease severity influences the specificity of the antibodies produced. 10 In conclusion, the detection of S1-specific IgA in paediatric patients with chilblain-like lesions strongly points to a previous, mostly asymptomatic SARS-CoV-2 infection with inflammatory sequelae.
Conflicts of interest None to be reported for all authors. A. Diociaiuti, 1,*, † S. Giancristoforo, 1, † S. Terreri, 2 M. Corbeddu, 1 C. Concato, 3 M. Ciofi Degli Atti, 4 G. Zambruno, 5 R. Carsetti, 6, † M. El Hachem 1, †
Conflicts of interest None declared.
References
Andina, Noguera-Morel, Bascuas-Arribas, Chilblains in children in the setting of COVID-19 pandemic, Pediatr Dermatol
Beavis, Matushek, Abeleda, Evaluation of the EUROIM-MUN Anti-SARS-CoV-2 ELISA assay for detection of IgA and IgG antibodies, J Clin Virol
Carsetti, Zaffina, Mortari, Spectrum of innate and adaptive immune response to SARS CoV 2 infection across asymptomatic, mild and severe cases; a longitudinal cohort study, medRxiv, doi:10.1101/2020.06.22.20137141
Caturegli, Materi, Howard, Caturegli, Clinical validity of serum antibodies to SARS-CoV-2: a case-control study, Ann Intern Med
Cleach, Dousset, Assier, Most chilblains observed during the COVID-19 outbreak occur in patients who are negative for COVID-19 on PCR and serology testing, Br J Dermatol
El Hachem, Diociaiuti, Concato, A clinical, histopathological and laboratory study of 19 consecutive Italian paediatric patients with chilblain-like lesions: lights and shadows on the relationship with COVID-19 infection, J Eur Acad Dermatol Venereol
Freeman, Mcmahon, Lipoff, Pernio-like skin lesions associated with COVID-19: a case series of 318 patients from 8 countries, J Am Acad Dermatol
Gebhard, Regitz-Zagrosek, Neuhauser, Morgan, Klein, Impact of sex and gender on COVID-19 outcomes in Europe, Biol Sex Differ
Ghazizadeh, Majd, Richter, Androgen regulates SARS-CoV-2 receptor levels and is associated with severe COVID-19 symptoms in men, bioRxiv, doi:10.1101/2020.05.12.091082
Grzelak, Temmam, Planchais, SARS-CoV-2 serological analysis of COVID-19 hospitalized patients, pauci-symptomatic individuals and blood donors, medRxiv, doi:10.1101/2020.04.21.20068858
Montopoli, Zumerle, Vettor, Androgen-deprivation therapies for prostate cancer and risk of infection by SARS-CoV-2: a populationbased study (N = 4532), Ann Oncol
Salgado, Handler, Schwartz, Shedding light on onychomadesis, Cutis
Seydoux, Homad, Maccamy, Analysis of a SARS-CoV-2-infected individual reveals development of potent neutralizing antibodies with limited somatic mutation, Immunity
Wadman, Sex hormones signal why virus hits men harder, Science
Wambier, Goren, Vaño-Galv An, Androgen sensitivity gateway to COVID-19 disease severity, Drug Dev Res
Wambier, Vaño-Galv An, Mccoy, Androgenetic alopecia present in the majority of hospitalized COVID-19 patients -the "Gabrin sign, J Am Acad Dermatol
DOI record:
{
"DOI": "10.1111/jdv.16953",
"ISSN": [
"0926-9959",
"1468-3083"
],
"URL": "http://dx.doi.org/10.1111/jdv.16953",
"alternative-id": [
"10.1111/jdv.16953"
],
"assertion": [
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Received",
"name": "received",
"order": 0,
"value": "2020-08-08"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Accepted",
"name": "accepted",
"order": 1,
"value": "2020-09-08"
},
{
"group": {
"label": "Publication History",
"name": "publication_history"
},
"label": "Published",
"name": "published",
"order": 2,
"value": "2020-10-21"
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-8190-2289",
"affiliation": [
{
"name": "Applied Biology, Inc. Irvine CA USA"
}
],
"authenticated-orcid": false,
"family": "Goren",
"given": "A.",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-4636-4489",
"affiliation": [
{
"name": "Department of Dermatology Alpert Medical School of Brown University Providence RI USA"
}
],
"authenticated-orcid": false,
"family": "Wambier",
"given": "C.G.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Infectious Diseases Unit Ramón y Cajal Hospital Madrid Spain"
}
],
"family": "Herrera",
"given": "S.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-1577-9910",
"affiliation": [
{
"name": "Applied Biology, Inc. Irvine CA USA"
}
],
"authenticated-orcid": false,
"family": "McCoy",
"given": "J.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0003-2773-7494",
"affiliation": [
{
"name": "Dermatology Department Ramón y Cajal Hospital Madrid Spain"
}
],
"authenticated-orcid": false,
"family": "Vaño‐Galván",
"given": "S.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Infectious Diseases Unit Ramón y Cajal Hospital Madrid Spain"
}
],
"family": "Gioia",
"given": "F.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Infectious Diseases Unit Ramón y Cajal Hospital Madrid Spain"
}
],
"family": "Comeche",
"given": "B.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Infectious Diseases Unit Ramón y Cajal Hospital Madrid Spain"
}
],
"family": "Ron",
"given": "R.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Infectious Diseases Unit Ramón y Cajal Hospital Madrid Spain"
}
],
"family": "Serrano‐Villar",
"given": "S.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-1561-414X",
"affiliation": [
{
"name": "Department of Dermatology São Paulo State University Botucatu Brazil"
}
],
"authenticated-orcid": false,
"family": "Ramos",
"given": "P.M.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Clinical Endocrinology Federal University of São Paulo Medical School Sao Paulo Brazil"
}
],
"family": "Cadegiani",
"given": "F.A.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Dermatology and Venereology Hospital Sestre Milosrdnice Zagreb Croatia"
}
],
"family": "Kovacevic",
"given": "M.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Dermatology and Cutaneous Surgery Miller School of Medicine University of Miami Miami FL USA"
}
],
"family": "Tosti",
"given": "A.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Ronald O. Perelman Department of Dermatology at the New York University School of Medicine New York NY USA"
}
],
"family": "Shapiro",
"given": "J.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Sinclair Dermatology Melbourne VIC Australia"
}
],
"family": "Sinclair",
"given": "R.",
"sequence": "additional"
}
],
"container-title": "Journal of the European Academy of Dermatology and Venereology",
"container-title-short": "Acad Dermatol Venereol",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"onlinelibrary.wiley.com"
]
},
"created": {
"date-parts": [
[
2020,
9,
26
]
],
"date-time": "2020-09-26T00:00:25Z",
"timestamp": 1601078425000
},
"deposited": {
"date-parts": [
[
2023,
9,
3
]
],
"date-time": "2023-09-03T18:20:00Z",
"timestamp": 1693765200000
},
"indexed": {
"date-parts": [
[
2024,
4,
3
]
],
"date-time": "2024-04-03T14:41:29Z",
"timestamp": 1712155289658
},
"is-referenced-by-count": 43,
"issue": "1",
"issued": {
"date-parts": [
[
2020,
10,
21
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2021,
1
]
]
}
},
"language": "en",
"license": [
{
"URL": "http://onlinelibrary.wiley.com/termsAndConditions#vor",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2020,
10,
21
]
],
"date-time": "2020-10-21T00:00:00Z",
"timestamp": 1603238400000
}
}
],
"link": [
{
"URL": "https://onlinelibrary.wiley.com/doi/pdf/10.1111/jdv.16953",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://onlinelibrary.wiley.com/doi/full-xml/10.1111/jdv.16953",
"content-type": "application/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://onlinelibrary.wiley.com/doi/pdf/10.1111/jdv.16953",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "311",
"original-title": [],
"prefix": "10.1111",
"published": {
"date-parts": [
[
2020,
10,
21
]
]
},
"published-online": {
"date-parts": [
[
2020,
10,
21
]
]
},
"published-print": {
"date-parts": [
[
2021,
1
]
]
},
"publisher": "Wiley",
"reference": [
{
"DOI": "10.1126/science.368.6495.1038",
"doi-asserted-by": "publisher",
"key": "e_1_2_4_2_1"
},
{
"DOI": "10.1186/s13293-020-00304-9",
"doi-asserted-by": "publisher",
"key": "e_1_2_4_3_1"
},
{
"DOI": "10.1002/ddr.21688",
"doi-asserted-by": "publisher",
"key": "e_1_2_4_4_1"
},
{
"DOI": "10.1016/j.jaad.2020.05.079",
"doi-asserted-by": "publisher",
"key": "e_1_2_4_5_1"
},
{
"DOI": "10.1016/j.annonc.2020.04.479",
"doi-asserted-by": "publisher",
"key": "e_1_2_4_6_1"
},
{
"article-title": "Androgen regulates SARS‐CoV‐2 receptor levels and is associated with severe COVID‐19 symptoms in men",
"author": "Ghazizadeh Z",
"journal-title": "bioRxiv",
"key": "e_1_2_4_7_1",
"year": "2020"
}
],
"reference-count": 6,
"references-count": 6,
"relation": {
"has-review": [
{
"asserted-by": "object",
"id": "10.3410/f.738737953.793579347",
"id-type": "doi"
}
]
},
"resource": {
"primary": {
"URL": "https://onlinelibrary.wiley.com/doi/10.1111/jdv.16953"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Infectious Diseases",
"Dermatology"
],
"subtitle": [],
"title": "Anti‐androgens may protect against severe COVID‐19 outcomes: results from a prospective cohort study of 77 hospitalized men",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1002/crossmark_policy",
"volume": "35"
}
