Metformin Use Is Associated With Reduced Mortality in a Diverse Population With COVID-19 and Diabetes
et al., Frontiers in Endocrinology, doi:10.3389/fendo.2020.600439, Jan 2021
Metformin for COVID-19
3rd treatment shown to reduce risk in
July 2020, now with p < 0.00000000001 from 111 studies.
Lower risk for mortality, ventilation, ICU, hospitalization, progression, recovery, and viral clearance.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 219 COVID-19+ diabetes patients in the USA, showing lower mortality with existing metformin treatment.
Standard of Care (SOC) for COVID-19 in the study country,
the USA, is very poor with very low average efficacy for approved treatments1.
Only expensive, high-profit treatments were approved for early treatment. Low-cost treatments were excluded, reducing the probability of early treatment due to access and cost barriers, and eliminating complementary and synergistic benefits seen with many low-cost treatments.
This may explain in part the very high mortality seen in this study.
Results may differ in countries with improved SOC.
|
risk of death, 60.8% lower, RR 0.39, p = 0.02, treatment 8 of 76 (10.5%), control 34 of 144 (23.6%), NNT 7.6, adjusted per study, odds ratio converted to relative risk, multiple logistic regression.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Crouse et al., 13 Jan 2021, retrospective, USA, peer-reviewed, 6 authors.
Metformin Use Is Associated With Reduced Mortality in a Diverse Population With COVID-19 and Diabetes
Frontiers in Endocrinology, doi:10.3389/fendo.2020.600439
Background: Coronavirus disease-2019 (COVID-19) is a growing pandemic with an increasing death toll that has been linked to various comorbidities as well as racial disparity. However, the specific characteristics of these at-risk populations are still not known and approaches to lower mortality are lacking.
Methods: We conducted a retrospective electronic health record data analysis of 25,326 subjects tested for COVID-19 between 2/25/20 and 6/22/20 at the University of Alabama at Birmingham Hospital, a tertiary health care center in the racially diverse Southern U.S. The primary outcome was mortality in COVID-19-positive subjects and the association with subject characteristics and comorbidities was analyzed using simple and multiple linear logistic regression.
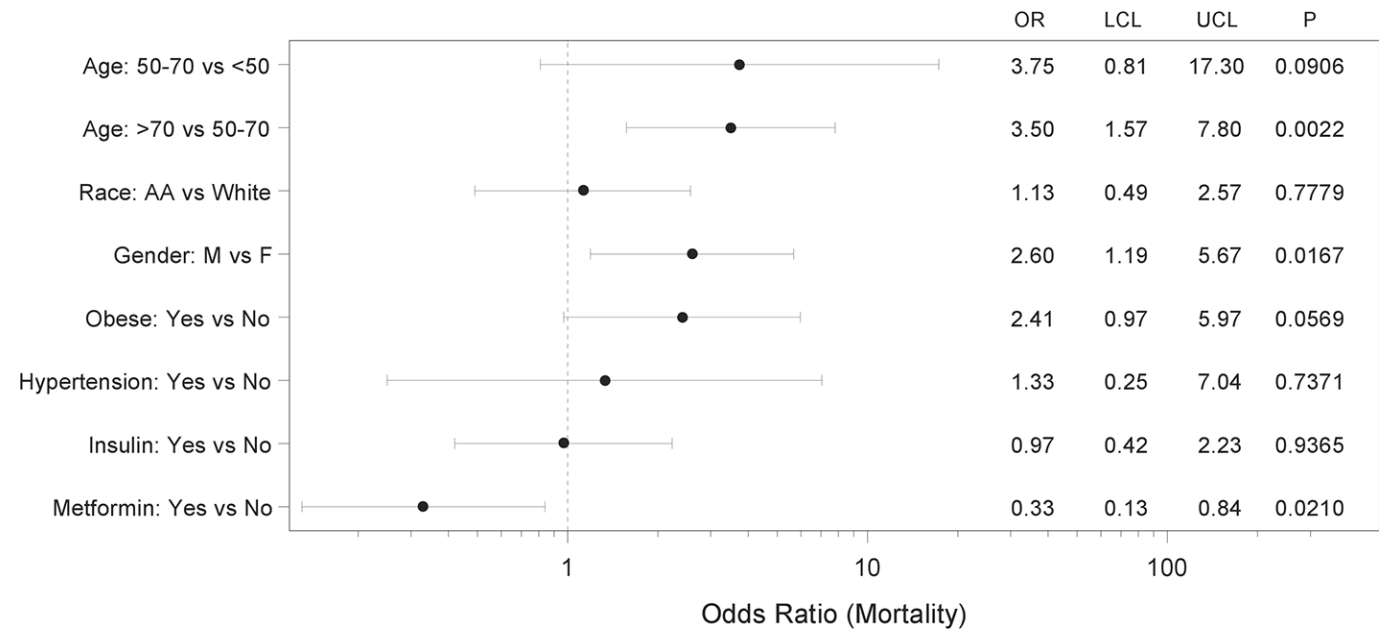
Results: The odds ratio of contracting COVID-19 was disproportionately high in Blacks/ African-Americans (OR 2.6; 95% CI 2.19-3.10; p<0.0001) and in subjects with obesity (OR 1.93; 95% CI 1.64-2.28; p<0.0001), hypertension (OR 2.46; 95% CI 2.07-2.93; p<0.0001), and diabetes (OR 2.11; 95% CI 1.78-2.48; p<0.0001). Diabetes was also associated with a dramatic increase in mortality (OR 3.62; 95% CI 2.11-6.2; p<0.0001) and emerged as an independent risk factor in this diverse population even after correcting for age, race, sex, obesity, and hypertension. Interestingly, we found that metformin treatment prior to diagnosis of COVID-19 was independently associated with a significant reduction in mortality in subjects with diabetes and COVID-19 (OR 0.33; 95% CI 0.13-0.84; p=0.0210).
Conclusion: Thus, these results suggest that while diabetes is an independent risk factor for COVID-19-related mortality, this risk is dramatically reduced in subjects taking metformin prior to diagnosis of COVID-19, raising the possibility that metformin may provide a protective approach in this high risk population.
ETHICS STATEMENT The studies involving human participants were reviewed and approved by UAB Institutional Review Board. Written informed consent for participation was not required for this study in accordance with the national legislation and the institutional requirements.
AUTHOR CONTRIBUTIONS AC and TG were responsible for data acquisition and analysis. PL performed all the statistical analyses. MM and FO helped with the approach and interpretation. AS conceived the study and wrote the manuscript. All authors contributed to the article and approved the submitted version.
Conflict of Interest: The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
Apicella, Campopiano, Mantuano, Mazoni, Coppelli et al., COVID-19 in people with diabetes: understanding the reasons for worse outcomes, Lancet Diabetes Endocrinol, doi:10.1016/S2213-8587(20)30238-2
Bramante, Ingraham, Murray, Marmor, Hoversten et al., Observational Study of Metformin and Risk of Mortality in Patients Hospitalized with Covid-19, MedRxiv Prepr Server Health Sci, doi:10.1101/2020.06.19.20135095
Burton, Fort, Seoane, Hospitalization and Mortality among Black Patients and White Patients with Covid-19, New Engl J Med, doi:10.1056/NEJMsa2011686
Cai, Chen, Wang, Luo, Liu et al., Obesity and COVID-19 Severity in a Designated Hospital in Shenzhen, China, Diabetes Care, doi:10.2337/dc20-0576
Cameron, Morrison, Levin, Mohan, Forteath et al., Anti-Inflammatory Effects of Metformin Irrespective of Diabetes Status, Circ Res, doi:10.1161/CIRCRESAHA.116.308445
Cariou, Hadjadj, Wargny, Pichelin, Al-Salameh et al., Phenotypic characteristics and prognosis of inpatients with COVID-19 and diabetes: the CORONADO study, Diabetologia, doi:10.1007/s00125-020-05180-x
Chen, Zheng, Zhang, Zhang, Wu et al., Clinical characteristics of 145 patients with corona virus disease 2019 (COVID-19) in Taizhou, Infection, doi:10.1007/s15010-020-01432-5
Christiansen, Johansen, Christensen, 'brien, Tonnesen et al., Preadmission metformin use and mortality among intensive care patients with diabetes: a cohort study, Crit Care, doi:10.1186/cc12886
Connors, Levy, COVID-19 and its implications for thrombosis and anticoagulation, Blood, doi:10.1182/blood.2020006000
Crouse, Grimes, Li, Might, Ovalle et al., Metformin Use Is Associated with Reduced Mortality in a Diverse Population with Covid-19 and Diabetes, MedRxiv Prepr Server Health Sci, doi:10.1101/2020.07.29.20164020
Golden, Yajnik, Phatak, Hanson, Knowler, Racial/ethnic differences in the burden of type 2 diabetes over the life course: a focus on the USA and India, Diabetologia, doi:10.1007/s00125-019-4968-0
Grant, The effects of metformin on the fibrinolytic system in diabetic and non-diabetic subjects, Diabete Metabol
Hariyanto, Kurniawan, Metformin use is associated with reduced mortality rate from coronavirus disease 2019 (COVID-19) infection, Obes Med, doi:10.1016/j.obmed.2020.100290
Holmes L Jr, Enwere, Williams, Ogundele, Chavan et al., Black-White Risk Differentials in COVID-19 (SARS-COV2) Transmission, Mortality and Case Fatality in the United States: Translational Epidemiologic Perspective and Challenges, Int J Environ Res Public Health, doi:10.3390/ijerph17124322
Khan, Savarimuthu, Leung, Harky, The need to manage the risk of thromboembolism in COVID-19 patients, J Vasc Surg, doi:10.1016/j.jvs.2020.05.015
Klein, Flanagan, Sex differences in immune responses, Nat Rev Immunol, doi:10.1038/nri.2016.90
Li, Wang, Chen, Zuo, Zhang et al., COVID-19 infection may cause ketosis and ketoacidosis, Diabetes Obes Metab, doi:10.1111/dom.14057
Luo, Qiu, Liu, Liu, Zheng et al., Metformin Treatment Was Associated with Decreased Mortality in COVID-19 Patients with Diabetes in a Retrospective Analysis, Am J Trop Med Hygiene, doi:10.4269/ajtmh.20-0375
Mauvais-Jarvis, Aging, Male Sex, Obesity, and Metabolic Inflammation Create the Perfect Storm for COVID-19, Diabetes, doi:10.2337/dbi19-0023
Mcfadyen, Stevens, Peter, The Emerging Threat of (Micro) Thrombosis in COVID-19 and Its Therapeutic Implications, Circ Res, doi:10.1161/CIRCRESAHA.120.317447
Mugabo, Li, Renier, The connection between C-reactive protein (CRP) and diabetic vasculopathy. Focus on preclinical findings, Curr Diabetes Rev, doi:10.2174/157339910790442628
Nogami, Muraki, Imano, Iso, Risk of disseminated intravascular coagulation in patients with type 2 diabetes mellitus: retrospective cohort study, BMJ Open, doi:10.1136/bmjopen-2016-013894
Palaiodimos, Kokkinidis, Li, Karamanis, Ognibene et al., Severe obesity, increasing age and male sex are independently associated with worse in-hospital outcomes, and higher in-hospital mortality, in a cohort of patients with COVID-19 in the Bronx, New York, Metabol: Clin Experiment, doi:10.1016/j.metabol.2020.154262
Richardson, Hirsch, Narasimhan, Crawford, Mcginn et al., Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area, Jama, doi:10.1001/jama.2020.6775
Scheen, Marre, Thivolet, Prognostic factors in patients with diabetes hospitalized for COVID-19: Findings from the CORONADO study and other recent reports, Diabetes Metab, doi:10.1016/j.diabet.2020.05.008
Tai, Shah, Doubeni, Sia, Wieland, The Disproportionate Impact of COVID-19 on Racial and Ethnic Minorities in the United States, Clin Infect Dis Off Publ Infect Dis Soc A, doi:10.1093/cid/ciaa815
Tan, Alquraini, Mizokami-Stout, Maceachern, Metformin: From Research to Clinical Practice, Endocrinol Metab Clinics North A, doi:10.1016/j.ecl.2016.06.008
Tsoyi, Jang, Nizamutdinova, Kim, Lee et al., Metformin inhibits HMGB1 release in LPS-treated RAW 264.7 cells and increases survival rate of endotoxaemic mice, Br J Pharmacol, doi:10.1111/j.1476-5381.2010.01126.x
Wang, Hu, Hu, Zhu, Liu et al., Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China, Jama, doi:10.1001/jama.2020.1585
Xin, Wei, Ji, Zheng, Gu et al., Metformin Uniquely Prevents Thrombosis by Inhibiting Platelet Activation and mtDNA Release, Sci Rep, doi:10.1038/srep36222
Yang, Han, Nilsson-Payant, Gupta, Wang et al., A Human Pluripotent Stem Cell-based Platform to Study SARS-CoV-2 Tropism and Model Virus Infection in Human Cells and Organoids, Cell Stem Cell, doi:10.1016/j.stem.2020.06.015
Zhu, She, Cheng, Qin, Zhang et al., Association of Blood Glucose Control and Outcomes in Patients with COVID-19 and Pre-existing Type 2 Diabetes, Cell Metab, doi:10.1016/j.cmet.2020.04.021
DOI record:
{
"DOI": "10.3389/fendo.2020.600439",
"ISSN": [
"1664-2392"
],
"URL": "http://dx.doi.org/10.3389/fendo.2020.600439",
"abstract": "<jats:sec><jats:title>Background</jats:title><jats:p>Coronavirus disease-2019 (COVID-19) is a growing pandemic with an increasing death toll that has been linked to various comorbidities as well as racial disparity. However, the specific characteristics of these at-risk populations are still not known and approaches to lower mortality are lacking.</jats:p></jats:sec><jats:sec><jats:title>Methods</jats:title><jats:p>We conducted a retrospective electronic health record data analysis of 25,326 subjects tested for COVID-19 between 2/25/20 and 6/22/20 at the University of Alabama at Birmingham Hospital, a tertiary health care center in the racially diverse Southern U.S. The primary outcome was mortality in COVID-19-positive subjects and the association with subject characteristics and comorbidities was analyzed using simple and multiple linear logistic regression.</jats:p></jats:sec><jats:sec><jats:title>Results</jats:title><jats:p>The odds ratio of contracting COVID-19 was disproportionately high in Blacks/African-Americans (OR 2.6; 95% CI 2.19–3.10; p&lt;0.0001) and in subjects with obesity (OR 1.93; 95% CI 1.64–2.28; p&lt;0.0001), hypertension (OR 2.46; 95% CI 2.07–2.93; p&lt;0.0001), and diabetes (OR 2.11; 95% CI 1.78–2.48; p&lt;0.0001). Diabetes was also associated with a dramatic increase in mortality (OR 3.62; 95% CI 2.11–6.2; p&lt;0.0001) and emerged as an independent risk factor in this diverse population even after correcting for age, race, sex, obesity, and hypertension. Interestingly, we found that metformin treatment prior to diagnosis of COVID-19 was independently associated with a significant reduction in mortality in subjects with diabetes and COVID-19 (OR 0.33; 95% CI 0.13–0.84; p=0.0210).</jats:p></jats:sec><jats:sec><jats:title>Conclusion</jats:title><jats:p>Thus, these results suggest that while diabetes is an independent risk factor for COVID-19-related mortality, this risk is dramatically reduced in subjects taking metformin prior to diagnosis of COVID-19, raising the possibility that metformin may provide a protective approach in this high risk population.</jats:p></jats:sec>",
"alternative-id": [
"10.3389/fendo.2020.600439"
],
"author": [
{
"affiliation": [],
"family": "Crouse",
"given": "Andrew B.",
"sequence": "first"
},
{
"affiliation": [],
"family": "Grimes",
"given": "Tiffany",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Li",
"given": "Peng",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Might",
"given": "Matthew",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ovalle",
"given": "Fernando",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Shalev",
"given": "Anath",
"sequence": "additional"
}
],
"container-title": "Frontiers in Endocrinology",
"container-title-short": "Front. Endocrinol.",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"frontiersin.org"
]
},
"created": {
"date-parts": [
[
2021,
1,
14
]
],
"date-time": "2021-01-14T07:40:50Z",
"timestamp": 1610610050000
},
"deposited": {
"date-parts": [
[
2022,
12,
11
]
],
"date-time": "2022-12-11T14:40:11Z",
"timestamp": 1670769611000
},
"funder": [
{
"DOI": "10.13039/100000002",
"award": [
"R01DK078752, U01DK120379, UL1TR001417"
],
"doi-asserted-by": "publisher",
"name": "National Institutes of Health"
}
],
"indexed": {
"date-parts": [
[
2024,
4,
8
]
],
"date-time": "2024-04-08T17:21:07Z",
"timestamp": 1712596867437
},
"is-referenced-by-count": 93,
"issued": {
"date-parts": [
[
2021,
1,
13
]
]
},
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
1,
13
]
],
"date-time": "2021-01-13T00:00:00Z",
"timestamp": 1610496000000
}
}
],
"link": [
{
"URL": "https://www.frontiersin.org/articles/10.3389/fendo.2020.600439/full",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1965",
"original-title": [],
"prefix": "10.3389",
"published": {
"date-parts": [
[
2021,
1,
13
]
]
},
"published-online": {
"date-parts": [
[
2021,
1,
13
]
]
},
"publisher": "Frontiers Media SA",
"reference": [
{
"DOI": "10.1001/jama.2020.6775",
"article-title": "Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area",
"author": "Richardson",
"doi-asserted-by": "publisher",
"journal-title": "Jama",
"key": "B1",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1016/j.metabol.2020.154262",
"article-title": "Severe obesity, increasing age and male sex are independently associated with worse in-hospital outcomes, and higher in-hospital mortality, in a cohort of patients with COVID-19 in the Bronx, New York",
"author": "Palaiodimos",
"doi-asserted-by": "publisher",
"journal-title": "Metabol: Clin Experiment",
"key": "B2",
"volume": "108",
"year": "2020"
},
{
"DOI": "10.2337/dc20-0576",
"article-title": "Obesity and COVID-19 Severity in a Designated Hospital in Shenzhen, China",
"author": "Cai",
"doi-asserted-by": "publisher",
"journal-title": "Diabetes Care",
"key": "B3",
"volume": "43",
"year": "2020"
},
{
"DOI": "10.1007/s15010-020-01432-5",
"article-title": "Clinical characteristics of 145 patients with corona virus disease 2019 (COVID-19) in Taizhou, Zhejiang, China",
"author": "Chen",
"doi-asserted-by": "publisher",
"journal-title": "Infection",
"key": "B4",
"volume": "48",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.1585",
"article-title": "Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China",
"author": "Wang",
"doi-asserted-by": "publisher",
"journal-title": "Jama",
"key": "B5",
"volume": "323",
"year": "2020"
},
{
"DOI": "10.1007/s00125-020-05180-x",
"article-title": "Phenotypic characteristics and prognosis of inpatients with COVID-19 and diabetes: the CORONADO study",
"author": "Cariou",
"doi-asserted-by": "publisher",
"journal-title": "Diabetologia",
"key": "B6",
"volume": "63",
"year": "2020"
},
{
"DOI": "10.1016/j.diabet.2020.05.008",
"article-title": "Prognostic factors in patients with diabetes hospitalized for COVID-19: Findings from the CORONADO study and other recent reports",
"author": "Scheen",
"doi-asserted-by": "publisher",
"journal-title": "Diabetes Metab",
"key": "B7",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.1056/NEJMsa2011686",
"article-title": "Hospitalization and Mortality among Black Patients and White Patients with Covid-19",
"author": "Price-Haywood",
"doi-asserted-by": "publisher",
"journal-title": "New Engl J Med",
"key": "B8",
"volume": "382",
"year": "2020"
},
{
"DOI": "10.1093/cid/ciaa815",
"article-title": "The Disproportionate Impact of COVID-19 on Racial and Ethnic Minorities in the United States",
"author": "Tai",
"doi-asserted-by": "crossref",
"key": "B9",
"volume-title": "Clin Infect Dis Off Publ Infect Dis Soc A",
"year": "2020"
},
{
"DOI": "10.3390/ijerph17124322",
"article-title": "Black-White Risk Differentials in COVID-19 (SARS-COV2) Transmission, Mortality and Case Fatality in the United States: Translational Epidemiologic Perspective and Challenges",
"author": "Holmes",
"doi-asserted-by": "publisher",
"first-page": "4322",
"journal-title": "Int J Environ Res Public Health",
"key": "B10",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1007/s00125-019-4968-0",
"article-title": "Racial/ethnic differences in the burden of type 2 diabetes over the life course: a focus on the USA and India",
"author": "Golden",
"doi-asserted-by": "publisher",
"journal-title": "Diabetologia",
"key": "B11",
"volume": "62",
"year": "2019"
},
{
"DOI": "10.1101/2020.06.19.20135095",
"article-title": "Observational Study of Metformin and Risk of Mortality in Patients Hospitalized with Covid-19",
"author": "Bramante",
"doi-asserted-by": "crossref",
"key": "B12",
"volume-title": "MedRxiv Prepr Server Health Sci",
"year": "2020"
},
{
"DOI": "10.1016/j.ecl.2016.06.008",
"article-title": "Metformin: From Research to Clinical Practice",
"author": "Tan",
"doi-asserted-by": "publisher",
"journal-title": "Endocrinol Metab Clinics North A",
"key": "B13",
"volume": "45",
"year": "2016"
},
{
"DOI": "10.4269/ajtmh.20-0375",
"article-title": "Metformin Treatment Was Associated with Decreased Mortality in COVID-19 Patients with Diabetes in a Retrospective Analysis",
"author": "Luo",
"doi-asserted-by": "publisher",
"first-page": "69",
"journal-title": "Am J Trop Med Hygiene",
"key": "B14",
"volume": "103",
"year": "2020"
},
{
"DOI": "10.1016/j.obmed.2020.100290",
"article-title": "Metformin use is associated with reduced mortality rate from coronavirus disease 2019 (COVID-19) infection",
"author": "Hariyanto",
"doi-asserted-by": "publisher",
"journal-title": "Obes Med",
"key": "B15",
"volume": "19",
"year": "2020"
},
{
"DOI": "10.1161/CIRCRESAHA.116.308445",
"article-title": "Anti-Inflammatory Effects of Metformin Irrespective of Diabetes Status",
"author": "Cameron",
"doi-asserted-by": "publisher",
"journal-title": "Circ Res",
"key": "B16",
"volume": "119",
"year": "2016"
},
{
"DOI": "10.1111/j.1476-5381.2010.01126.x",
"article-title": "Metformin inhibits HMGB1 release in LPS-treated RAW 264.7 cells and increases survival rate of endotoxaemic mice",
"author": "Tsoyi",
"doi-asserted-by": "publisher",
"journal-title": "Br J Pharmacol",
"key": "B17",
"volume": "162",
"year": "2011"
},
{
"article-title": "The effects of metformin on the fibrinolytic system in diabetic and non-diabetic subjects",
"author": "Grant",
"journal-title": "Diabete Metabol",
"key": "B18",
"volume": "17",
"year": "1991"
},
{
"DOI": "10.1038/srep36222",
"article-title": "Metformin Uniquely Prevents Thrombosis by Inhibiting Platelet Activation and mtDNA Release",
"author": "Xin",
"doi-asserted-by": "publisher",
"journal-title": "Sci Rep",
"key": "B19",
"volume": "6",
"year": "2016"
},
{
"DOI": "10.1161/CIRCRESAHA.120.317447",
"article-title": "The Emerging Threat of (Micro)Thrombosis in COVID-19 and Its Therapeutic Implications",
"author": "McFadyen",
"doi-asserted-by": "publisher",
"journal-title": "Circ Res",
"key": "B20",
"volume": "127",
"year": "2020"
},
{
"DOI": "10.1182/blood.2020006000",
"article-title": "COVID-19 and its implications for thrombosis and anticoagulation",
"author": "Connors",
"doi-asserted-by": "publisher",
"journal-title": "Blood",
"key": "B21",
"volume": "135",
"year": "2020"
},
{
"DOI": "10.1016/j.jvs.2020.05.015",
"article-title": "The need to manage the risk of thromboembolism in COVID-19 patients",
"author": "Khan",
"doi-asserted-by": "publisher",
"first-page": "799",
"journal-title": "J Vasc Surg",
"key": "B22",
"volume": "72",
"year": "2020"
},
{
"DOI": "10.1186/cc12886",
"article-title": "Preadmission metformin use and mortality among intensive care patients with diabetes: a cohort study",
"author": "Christiansen",
"doi-asserted-by": "publisher",
"first-page": "R192",
"journal-title": "Crit Care",
"key": "B23",
"volume": "17",
"year": "2013"
},
{
"DOI": "10.1016/j.cmet.2020.04.021",
"article-title": "Association of Blood Glucose Control and Outcomes in Patients with COVID-19 and Pre-existing Type 2 Diabetes",
"author": "Zhu",
"doi-asserted-by": "publisher",
"first-page": "1068",
"journal-title": "Cell Metab",
"key": "B24",
"volume": "31",
"year": "2020"
},
{
"DOI": "10.2174/157339910790442628",
"article-title": "The connection between C-reactive protein (CRP) and diabetic vasculopathy. Focus on preclinical findings",
"author": "Mugabo",
"doi-asserted-by": "publisher",
"first-page": "27",
"journal-title": "Curr Diabetes Rev",
"key": "B25",
"volume": "6",
"year": "2010"
},
{
"DOI": "10.1136/bmjopen-2016-013894",
"article-title": "Risk of disseminated intravascular coagulation in patients with type 2 diabetes mellitus: retrospective cohort study",
"author": "Nogami",
"doi-asserted-by": "publisher",
"journal-title": "BMJ Open",
"key": "B26",
"volume": "7",
"year": "2017"
},
{
"DOI": "10.1016/j.stem.2020.06.015",
"article-title": "A Human Pluripotent Stem Cell-based Platform to Study SARS-CoV-2 Tropism and Model Virus Infection in Human Cells and Organoids",
"author": "Yang",
"doi-asserted-by": "publisher",
"first-page": "125",
"journal-title": "Cell Stem Cell",
"key": "B27",
"volume": "27",
"year": "2020"
},
{
"DOI": "10.1016/S2213-8587(20)30238-2",
"article-title": "COVID-19 in people with diabetes: understanding the reasons for worse outcomes",
"author": "Apicella",
"doi-asserted-by": "publisher",
"journal-title": "Lancet Diabetes Endocrinol",
"key": "B28",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1111/dom.14057",
"article-title": "COVID-19 infection may cause ketosis and ketoacidosis",
"author": "Li",
"doi-asserted-by": "publisher",
"journal-title": "Diabetes Obes Metab",
"key": "B29",
"volume": "22",
"year": "2020"
},
{
"DOI": "10.2337/dbi19-0023",
"article-title": "Aging, Male Sex, Obesity, and Metabolic Inflammation Create the Perfect Storm for COVID-19",
"author": "Mauvais-Jarvis",
"doi-asserted-by": "publisher",
"journal-title": "Diabetes",
"key": "B30",
"volume": "69",
"year": "2020"
},
{
"DOI": "10.1038/nri.2016.90",
"article-title": "Sex differences in immune responses",
"author": "Klein",
"doi-asserted-by": "publisher",
"journal-title": "Nat Rev Immunol",
"key": "B31",
"volume": "16",
"year": "2016"
},
{
"DOI": "10.1101/2020.07.29.20164020",
"article-title": "Metformin Use Is Associated with Reduced Mortality in a Diverse Population with Covid-19 and Diabetes",
"author": "Crouse",
"doi-asserted-by": "crossref",
"key": "B32",
"volume-title": "MedRxiv Prepr Server Health Sci",
"year": "2020"
}
],
"reference-count": 32,
"references-count": 32,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.frontiersin.org/articles/10.3389/fendo.2020.600439/full"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Endocrinology, Diabetes and Metabolism"
],
"subtitle": [],
"title": "Metformin Use Is Associated With Reduced Mortality in a Diverse Population With COVID-19 and Diabetes",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.3389/crossmark-policy",
"volume": "11"
}
