Vitamin D Supplementation and Prior Oral Poliovirus Vaccination Decrease Odds of COVID-19 Outcomes among Adults Recently Inoculated with Inactivated Poliovirus Vaccine
et al., Vaccines, doi:10.3390/vaccines12020121, NCT04639375, Jan 2024
Vitamin D for COVID-19
8th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 137 studies, recognized in 18 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Retrospective 282 adults recently vaccinated against poliovirus showing vitamin D supplementation associated with lower COVID-19 PCR+ cases, lower symptomatic cases, and shorter duration of symptoms.
This is the 126th of 137 COVID-19 controlled studies for vitamin D, which collectively show efficacy with p<0.0000000001.
41 studies are RCTs, which show efficacy with p=0.00000049.
Standard of Care (SOC) for COVID-19 in the study country,
the USA, is very poor with very low average efficacy for approved treatments1.
Only expensive, high-profit treatments were approved for early treatment. Low-cost treatments were excluded, reducing the probability of early treatment due to access and cost barriers, and eliminating complementary and synergistic benefits seen with many low-cost treatments.
|
risk of symptomatic case, 91.0% lower, OR 0.09, p < 0.001, treatment 100, control 182, adjusted per study, multivariable, RR approximated with OR.
|
|
risk of case, 88.0% lower, OR 0.12, p = 0.001, treatment 100, control 182, adjusted per study, multivariable, RR approximated with OR.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Comunale et al., 24 Jan 2024, retrospective, USA, peer-reviewed, 6 authors, study period November 2020 - May 2021, dosage not specified, trial NCT04639375 (history).
Contact: bcomuna1@alumni.jh.edu (corresponding author).
Vitamin D Supplementation and Prior Oral Poliovirus Vaccination Decrease Odds of COVID-19 Outcomes among Adults Recently Inoculated with Inactivated Poliovirus Vaccine
Vaccines, doi:10.3390/vaccines12020121
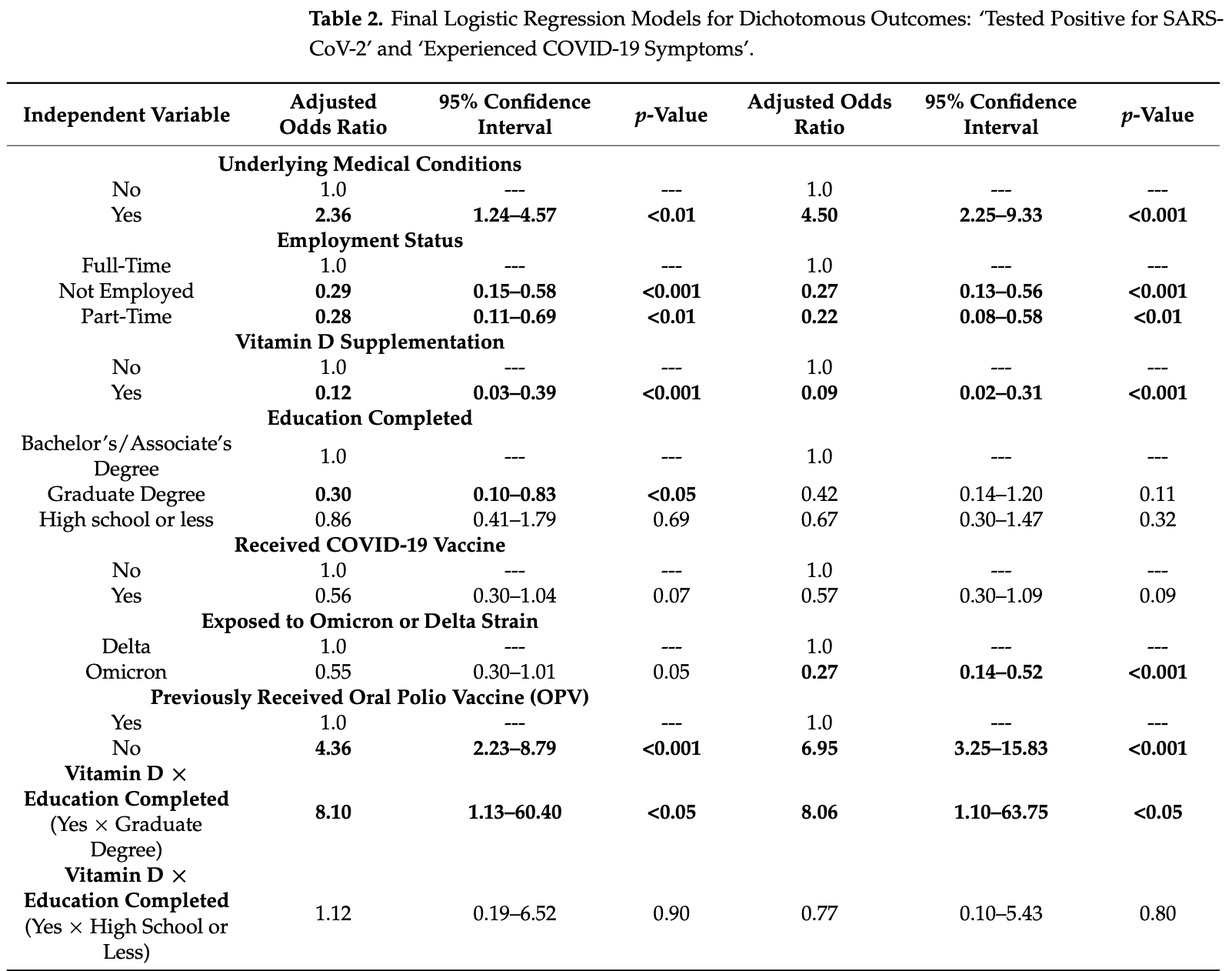
Background: Structural and functional commonalities between poliovirus and severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) suggest that poliovirus inoculation may induce antibodies that mitigate the coronavirus disease (COVID-19). No known studies have evaluated COVID-19 risk factors in adults recently vaccinated against poliovirus. Study Objective: Among adults with no history of COVID-19 infection or vaccination, who recently received an inactivated poliovirus vaccine (IPV), we sought to determine which biological factors and social determinants of health (SDOH) may be associated with (1) testing positive for SARS-CoV-2, (2) experiencing COVID-19 symptoms, and (3) a longer duration of COVID-19 symptoms. Methods: The influence of biological factors and SDOH on SARS-CoV-2 infection and COVID-19 symptoms were evaluated among 282 adults recently inoculated with IPV. Participant-reported surveys were analyzed over 12 months post-enrollment. Bivariate and multivariate linear and logistic regression models identified associations between variables and COVID-19 outcomes. Results: Adjusting for COVID-19 vaccinations, variants, and other SDOH, secondary analyses revealed that underlying conditions, employment, vitamin D, education, and the oral poliovirus vaccination (OPV) were associated with COVID-19 outcomes. The odds of testing positive for SARS-CoV-2 and experiencing symptoms were significantly reduced among participants who took vitamin D (OR 0.12 and OR 0.09, respectively). Unemployed or part-time working participants were 72% less likely to test positive compared with full-time workers. No prior dose of OPV was one of the strongest predictors of SARS-CoV-2 infection (OR 4.36) and COVID-19 symptoms (OR 6.95). Conclusions: Findings suggest that prophylactic measures and mucosal immunity may mitigate the risk and severity of COVID-19 outcomes. Larger-scale studies may inform future policies.
Supplementary Materials: The following supporting information can be downloaded at: https:// www.mdpi.com/article/10.3390/vaccines12020121/s1, Table S1 . Participant Demographics and Characteristics. Table S2 . Main Effects of Predictor Variables.
Funding: The secondary data analysis presented here received no external funding.
Institutional Review Board Statement: The Johns Hopkins School of Public Health Institutional Review Board reviewed this secondary analysis study and deemed it exempt. The original study from which data were derived was conducted in accordance with the Declaration of Helsinki, and approved by the Institutional Review Board of Advarra (Protocol # Pro00046994, October 2020). Informed Consent Statement: Informed consent was obtained from all subjects involved in the study.
Conflicts of Interest: The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
Abedi, Olulana, Avula, Chaudhary, Khan et al., Racial, Economic, and Health Inequality and COVID-19 Infection in the United States, J. Racial Ethn. Health Disparit, doi:10.1007/s40615-020-00833-4
Acosta, Garg, Pham, Whitaker, Anglin et al., Racial and Ethnic Disparities in Rates of COVID-19-Associated Hospitalization, Intensive Care Unit Admission, and in-Hospital Death in the United States from March 2020 to February 2021, JAMA Netw. Open, doi:10.1001/jamanetworkopen.2021.30479
Angelucci, Angrisani, Bennett, Kapteyn, Schaner, Remote Work and the Heterogeneous Impact of COVID-19 on Employment and Health
Apelberg, Buckley, White, Socioeconomic and racial disparities in cancer risk from air toxics in Maryland, Environ. Health Perspect, doi:10.1289/ehp.7609
Avdiu, Nayyar, When face-to-face interactions become an occupational hazard: Jobs in the time of COVID-19, Econ. Lett, doi:10.1016/j.econlet.2020.109648
Aygun, Vitamin D may protect against multiple organ damage caused by COVID-19, Bratisl Lek Listy, doi:10.4149/BLL_2020_143
Azar, Shen, Romanelli, Lockhart, Smits et al., Disparities in Outcomes among COVID-19 Patients in a Large Health Care System in California, Health Aff, doi:10.1377/hlthaff.2020.00598
Barr, Health Disparities in the United States: Social Class, Race, Ethnicity, and Social Determinants Of Health
Bhuiyan, Khan, Jony, Robinson, Nguyen et al., The Disproportionate Impact of COVID-19 among Undocumented Immigrants and Racial Minorities in the US, Int. J. Environ. Res. Public Health, doi:10.3390/ijerph182312708
Bialek, Boundy, Bowen, Chow, Cohn et al., Severe Outcomes among Patients with Coronavirus Disease 2019 (COVID-19)-United States, MMWR Morb. Mortal. Wkly. Rep, doi:10.15585/mmwr.mm6912e2
Carlsten, Gulati, Hines, Rose, Scott et al., COVID-19 as an occupational disease, Am. J. Ind. Med, doi:10.1002/ajim.23222
Castañeda, Holmes, Madrigal, Young, Beyeler et al., Immigration as a social determinant of health, Annu. Rev. Public Health, doi:10.1146/annurev-publhealth-032013-182419
Chae, Lee, Rifai, Ridker, Blood Pressure and Inflammation in Apparently Healthy Men, Hypertension, doi:10.1161/01.HYP.38.3.399
Comunale, Engineer, Jiang, Andrews, Liu et al., Poliovirus Vaccination Induces a Humoral Immune Response That Cross Reacts with SARS-CoV-2, Front. Med, doi:10.3389/fmed.2021.710010
Comunale, Jackson-Ward, Jiang, Ward, Liu et al., Inactivated Poliovirus Vaccine Induces Antibodies that Inhibit RNA Synthesis of SARS-CoV-2: An open-label, pre-post vaccine clinical trial, medRxiv, doi:10.1101/2021.10.05.21264598
Comunale, Larson, Hsu, Jackson-Ward, Azodoh et al., Prior Oral Poliovirus Vaccination Decreases Odds of COVID-19 Outcomes
Daneshkhah, Agrawal, Eshein, Subramanian, Roy et al., Evidence for possible association of vitamin D status with cytokine storm and unregulated inflammation in COVID-19 patients, Aging Clin. Exp. Res, doi:10.1007/s40520-020-01677-y
Di Filippo, Frara, Terenzi, Nannipieri, Locatelli et al., Lack of vitamin D predicts impaired long-term immune response to COVID-19 vaccination, Endocrine, doi:10.1007/s12020-023-03481-w
Dingel, Neiman, How many jobs can be done at home?, J. Public Econ, doi:10.1016/j.jpubeco.2020.104235
Dütsch, COVID-19 and the labour market: What are the working conditions in critical jobs?, J. Labour Mark. Res, doi:10.1186/s12651-022-00315-6
Figueroa, Wadhera, Lee, Yeh, Sommers, Community-Level Factors Associated with Racial And Ethnic Disparities In COVID-19 Rates In Massachusetts, Health Aff, doi:10.1377/hlthaff.2020.01040
Foote, Murphy, Wilkens, Hankin, Henderson et al., Factors associated with dietary supplement use among healthy adults of five ethnicities: The Multiethnic Cohort Study, Am. J. Epidemiol
Franceschi, Bonafe, Valensin, Olivieri, De Luca et al., Inflamm-aging: An evolutionary perspective on immunosenescence, Ann. N. Y. Acad. Sci, doi:10.1111/j.1749-6632.2000.tb06651.x
Gangopadhyaya, Karpman, Aarons, As the COVID-19 Recession Extended into the Summer of 2020
Ghosh, Venkatraman, Soroka, Reshetnyak, Rajan et al., Association between overcrowded households, multigenerational households, and COVID-19: A cohort study, Public Health, doi:10.1016/j.puhe.2021.07.039
Gould, Shierholz, Not Everybody Can Work from Home: Black and Hispanic Workers are Much Less Likely to be Able to Telework
Grant, Lahore, Mcdonnell, Baggerly, French et al., Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths, Nutrients, doi:10.3390/nu12040988
Griffith, Innes, The relationship of socio-economic factors to the use of vitamin supplements in the city of windsor, Nutr. Res, doi:10.1016/S0271-5317(83)80006-2
Hawkins, Differential occupational risk for COVID-19 and other infection exposure according to race and ethnicity, Am. J. Ind. Med, doi:10.1002/ajim.23145
Hawkins, Disparities in Access to Paid Sick Leave During the First Year of the COVID-19 Pandemic, J. Occup. Environ. Med, doi:10.1097/JOM.0000000000002784
Hayawi, Shahriar, Serhani, Alashwal, Masud, Vaccine versus Variants (3Vs): Are the COVID-19 Vaccines Effective against the Variants? A Systematic Review, Vaccines, doi:10.3390/vaccines9111305
Henein, Vancheri, Longo, Vancheri, The Role of Inflammation in Cardiovascular Disease, Int. J. Mol. Sci, doi:10.3390/ijms232112906
Herremans, Reimerink, Buisman, Kimman, Koopmans, Induction of mucosal immunity by inactivated poliovirus vaccine is dependent on previous mucosal contact with live virus, J. Immunol, doi:10.4049/jimmunol.162.8.5011
Herrick, Storandt, Afful, Pfeiffer, Schleicher et al., Vitamin D status in the United States, 2011-2014, Am. J. Clin. Nutr, doi:10.1093/ajcn/nqz037
Höpping, Mcelhaney, Fonville, Powers, Beyer et al., The confounded effects of age and exposure history in response to influenza vaccination, Vaccine, doi:10.1016/j.vaccine.2015.11.058
Ilie, Stefanescu, Smith, The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality, Aging Clin. Exp. Res, doi:10.1007/s40520-020-01570-8
Javanmardi, Keshavarzi, Akbari, Emami, Pirbonyeh, Prevalence of underlying diseases in died cases of COVID-19: A systematic review and meta-analysis, PLoS ONE, doi:10.1371/journal.pone.0241265
Jin, Bai, He, Wu, Liu et al., Gender Differences in Patients with COVID-19: Focus on Severity and Mortality, Front. Public Health, doi:10.3389/fpubh.2020.00152
John, Giri, Karthikeyan, Iturriza-Gomara, Muliyil et al., Effect of a single inactivated poliovirus vaccine dose on intestinal immunity against poliovirus in children previously given oral vaccine: An open-label, randomised controlled trial, Lancet, doi:10.1016/S0140-6736(14)60934-X
Kim, Kim, Son, Heo, Nam et al., Vaccine Effect on Household Transmission of Omicron and Delta SARS-CoV-2 Variants, J. Korean Med. Sci, doi:10.3346/jkms.2023.38.e9
Klein, Flanagan, Sex differences in immune responses, Nat. Rev. Immunol, doi:10.1038/nri.2016.90
Klein, Jedlicka, Pekosz, The Xs and Y of immune responses to viral vaccines, Lancet Infect. Dis, doi:10.1016/S1473-3099(10)70049-9
Lewnard, Hong, Patel, Kahn, Lipsitch et al., Clinical outcomes associated with SARS-CoV-2 Omicron (B.1.1.529) variant and BA.1/BA.1.1 or BA.2 subvariant infection in Southern California, Nat. Med, doi:10.1038/s41591-022-01887-z
Li, Xiang, Liang, Deng, Wang et al., Characterization of SARS-CoV-2-Specific Humoral and Cellular Immune Responses Induced by Inactivated COVID-19 Vaccines in a Real-World Setting, Front. Immunol, doi:10.3389/fimmu.2021.802858
Lin, Xu, Gu, Zeng, Wheeler et al., Effectiveness of Bivalent Boosters against Severe Omicron Infection, N. Engl. J. Med, doi:10.1056/NEJMc2215471
Lips, De Jongh, Van Schoor, Trends in Vitamin D Status Around the World, JBMR Plus, doi:10.1002/jbm4.10585
Lipsitch, Swerdlow, Finelli, Defining the Epidemiology of COVID-19-Studies Needed, N. Engl. J. Med, doi:10.1056/NEJMp2002125
Lopez Bernal, Andrews, Gower, Gallagher, Simmons et al., Effectiveness of COVID-19 Vaccines against the B.1.617.2 (Delta) Variant, N. Engl. J. Med, doi:10.1056/NEJMoa2108891
Lyngse, Mortensen, Denwood, Christiansen, Møller et al., Household transmission of the SARS-CoV-2 Omicron variant in Denmark, Nat. Commun, doi:10.1038/s41467-022-33328-3
Mackenbach, Kulhánová, Bopp, Deboosere, Eikemo et al., Variations in the relation between education and cause-specific mortality in 19 European populations: A test of the "fundamental causes" theory of social inequalities in health, Soc. Sci. Med, doi:10.1016/j.socscimed.2014.05.021
Mcmaughan, Oloruntoba, Smith, Socioeconomic Status and Access to Healthcare: Interrelated Drivers for Healthy Aging, Front. Public Health, doi:10.3389/fpubh.2020.00231
Mehraeen, Karimi, Barzegary, Vahedi, Afsahi et al., Predictors of mortality in patients with COVID-19-a systematic review, Eur. J. Integr. Med, doi:10.1016/j.eujim.2020.101226
Meltzer, Best, Zhang, Vokes, Arora et al., Association of Vitamin D Status and Other Clinical Characteristics with COVID-19 Test Results, JAMA Netw. Open, doi:10.1001/jamanetworkopen.2020.19722
Miller, Dyslipidemia and cardiovascular risk: The importance of early prevention, QJM, doi:10.1093/qjmed/hcp065
Mohamed, Moulin, Schiöth, Sex differences in COVID-19: The role of androgens in disease severity and progression, Endocrine, doi:10.1007/s12020-020-02536-6
Morante-García, Zapata-Boluda, García-González, Campuzano-Cuadrado, Calvillo et al., Influence of Social Determinants of Health on COVID-19 Infection in Socially Vulnerable Groups, Int. J. Environ. Res. Public Health, doi:10.3390/ijerph19031294
Morgan, Klein, The intersection of sex and gender in the treatment of influenza, Curr. Opin. Virol, doi:10.1016/j.coviro.2019.02.009
Mueller, Mcnamara, Sinclair, Why does COVID-19 disproportionately affect older people?, Aging, doi:10.18632/aging.103344
Márquez, Chung, Marches, Rossi, Nehar-Belaid et al., Sexual-dimorphism in human immune system aging, Nat. Commun, doi:10.1038/s41467-020-14396-9
Nakaya, Hagan, Duraisingham, Lee, Kwissa et al., Systems Analysis of Immunity to Influenza Vaccination across Multiple Years and in Diverse Populations Reveals Shared Molecular Signatures, Immunity, doi:10.1016/j.immuni.2015.11.012
Nardone, Casey, Morello-Frosch, Mujahid, Balmes et al., Associations between historical residential redlining and current age-adjusted rates of emergency department visits due to asthma across eight cities in California: An ecological study, Lancet Planet. Health, doi:10.1016/S2542-5196(19)30241-4
Palacio, Tamariz, Social Determinants of Health Mediate COVID-19 Disparities in South Florida, J. Gen. Intern. Med, doi:10.1007/s11606-020-06341-9
Paul, Arif, Pokhrel, Ghosh, The Association of Social Determinants of Health with COVID-19 Mortality in Rural and Urban Counties, J. Rural Health, doi:10.1111/jrh.12557
Pennell, Galligan, Fish, Sex affects immunity, J. Autoimmun, doi:10.1016/j.jaut.2011.11.013
Pol, Held, Westerbergh, Lindbäck, Alexander et al., Dyslipidemia and Risk of Cardiovascular Events in Patients with Atrial Fibrillation Treated with Oral Anticoagulation Therapy: Insights from the ARISTOTLE (Apixaban for Reduction in Stroke and Other Thromboembolic Events in Atrial Fibrillation) Trial, J. Am. Heart Assoc, doi:10.1161/JAHA.117.007444
Rezende, Thome, Schveitzer, De Souza-Júnior, Szwarcwald, Adults at high-risk of severe coronavirus disease-2019 (COVID-19) in Brazil, Rev. Saude Publica, doi:10.11606/s1518-8787.2020054002596
Roth, Abrams, Aloia, Bergeron, Bourassa et al., Global prevalence and disease burden of vitamin D deficiency: A roadmap for action in low-and middle-income countries, Ann. N. Y. Acad. Sci, doi:10.1111/nyas.13968
Roth, Martz, Yeo, Prosser, Bell et al., Are national vitamin D guidelines sufficient to maintain adequate blood levels in children? Can, J. Public Health, doi:10.1007/BF03405185
Rucker, Allan, Fick, Hanley, Vitamin D insufficiency in a population of healthy western Canadians, CMAJ
Saydah, Imperatore, Beckles, Socioeconomic status and mortality: Contribution of health care access and psychological distress among U.S. adults with diagnosed diabetes, Diabetes Care, doi:10.2337/dc11-1864
Sekulic, Stajic, Skevin, Kocovic, Zaric et al., Lifestyle, Physical Activity, Eating and Hygiene Habits: A Comparative Analysis Before and During the COVID-19 Pandemic in Student Population, Front. Public Health, doi:10.3389/fpubh.2022.862816
Shakoor, Feehan, Al Dhaheri, Ali, Platat et al., Immune-boosting role of vitamins D, C, E, zinc, selenium and omega-3 fatty acids: Could they help against COVID-19?, Maturitas, doi:10.1016/j.maturitas.2020.08.003
Singu, Acharya, Challagundla, Byrareddy, Impact of Social Determinants of Health on the Emerging COVID-19 Pandemic in the United States, Front. Public Health, doi:10.3389/fpubh.2020.00406
Sterlin, Mathian, Miyara, Mohr, Anna et al., IgA dominates the early neutralizing antibody response to SARS-CoV-2, Sci. Transl. Med, doi:10.1126/scitranslmed.abd2223
Tai, Shah, Doubeni, Sia, Wieland, The Disproportionate Impact of COVID-19 on Racial and Ethnic Minorities in the United States, Clin. Infect. Dis, doi:10.1093/cid/ciaa815
Thiab, Nassar, Thiab, Basheti, Medications and natural products used in Jordan for prevention or treatment of COVID-19 infection during the second wave of the pandemic: A cross-sectional online survey, Saudi Pharm. J, doi:10.1016/j.jsps.2022.03.006
Tsalamandris, Antonopoulos, Oikonomou, Papamikroulis, Vogiatzi et al., The Role of Inflammation in Diabetes: Current Concepts and Future Perspectives, Eur. Cardiol. Rev, doi:10.15420/ecr.2018.33.1
Wang, Li, Gao, Xue, Pang et al., Analysis of Dietary Supplement Use and Influencing Factors in the Mongolian Population, BioMed Res. Int, doi:10.1155/2022/4064588
Ward, Whitaker, Flower, Tang, Atchison et al., Population antibody responses following COVID-19 vaccination in 212,102 individuals, Nat. Commun, doi:10.1038/s41467-022-28527-x
Wu, Nethery, Sabath, Braun, Dominici, Air pollution and COVID-19 mortality in the United States: Strengths and limitations of an ecological regression analysis, Sci. Adv, doi:10.1126/sciadv.abd4049
Ye, Zhang, Wei, Cao, Yuan et al., Equitable access to COVID-19 vaccines makes a life-saving difference to all countries, Nat. Hum. Behav, doi:10.1038/s41562-022-01289-8
Zepp, Principles of vaccine design-Lessons from nature, Vaccine, doi:10.1016/j.vaccine.2010.07.020
DOI record:
{
"DOI": "10.3390/vaccines12020121",
"ISSN": [
"2076-393X"
],
"URL": "http://dx.doi.org/10.3390/vaccines12020121",
"abstract": "<jats:p>Background: Structural and functional commonalities between poliovirus and severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) suggest that poliovirus inoculation may induce antibodies that mitigate the coronavirus disease (COVID-19). No known studies have evaluated COVID-19 risk factors in adults recently vaccinated against poliovirus. Study Objective: Among adults with no history of COVID-19 infection or vaccination, who recently received an inactivated poliovirus vaccine (IPV), we sought to determine which biological factors and social determinants of health (SDOH) may be associated with (1) testing positive for SARS-CoV-2, (2) experiencing COVID-19 symptoms, and (3) a longer duration of COVID-19 symptoms. Methods: The influence of biological factors and SDOH on SARS-CoV-2 infection and COVID-19 symptoms were evaluated among 282 adults recently inoculated with IPV. Participant-reported surveys were analyzed over 12 months post-enrollment. Bivariate and multivariate linear and logistic regression models identified associations between variables and COVID-19 outcomes. Results: Adjusting for COVID-19 vaccinations, variants, and other SDOH, secondary analyses revealed that underlying conditions, employment, vitamin D, education, and the oral poliovirus vaccination (OPV) were associated with COVID-19 outcomes. The odds of testing positive for SARS-CoV-2 and experiencing symptoms were significantly reduced among participants who took vitamin D (OR 0.12 and OR 0.09, respectively). Unemployed or part-time working participants were 72% less likely to test positive compared with full-time workers. No prior dose of OPV was one of the strongest predictors of SARS-CoV-2 infection (OR 4.36) and COVID-19 symptoms (OR 6.95). Conclusions: Findings suggest that prophylactic measures and mucosal immunity may mitigate the risk and severity of COVID-19 outcomes. Larger-scale studies may inform future policies.</jats:p>",
"alternative-id": [
"vaccines12020121"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0003-2242-5475",
"affiliation": [
{
"name": "Department of Health Policy and Management, Johns Hopkins Bloomberg School of Public Health, Johns Hopkins University, Baltimore, MD 21205, USA"
}
],
"authenticated-orcid": false,
"family": "Comunale",
"given": "Brittany A.",
"sequence": "first"
},
{
"affiliation": [
{
"name": "Department of Health Policy and Management, Johns Hopkins Bloomberg School of Public Health, Johns Hopkins University, Baltimore, MD 21205, USA"
}
],
"family": "Hsu",
"given": "Yea-Jen",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Dartmouth-Hitchcock Medical Center, Geisel School of Medicine at Dartmouth, Hanover, NH 03755, USA"
},
{
"name": "Department of Palliative Medicine, Dartmouth-Hitchcock Medical Center, Lebanon, NH 03756, USA"
}
],
"family": "Larson",
"given": "Robin J.",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Biological Sciences, University of California, San Diego, La Jolla, CA 92161, USA"
}
],
"family": "Singh",
"given": "Aditi",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0001-7434-308X",
"affiliation": [
{
"name": "Department of Health Policy and Management, Johns Hopkins Bloomberg School of Public Health, Johns Hopkins University, Baltimore, MD 21205, USA"
},
{
"name": "Cedars-Sinai Medical Center, Los Angeles, CA 90048, USA"
}
],
"authenticated-orcid": false,
"family": "Jackson-Ward",
"given": "Erin",
"sequence": "additional"
},
{
"affiliation": [
{
"name": "Department of Health Policy and Management, Johns Hopkins Bloomberg School of Public Health, Johns Hopkins University, Baltimore, MD 21205, USA"
},
{
"name": "Department of Anesthesiology and Critical Care Medicine, Johns Hopkins School of Medicine, Baltimore, MD 21205, USA"
}
],
"family": "Engineer",
"given": "Lilly D.",
"sequence": "additional"
}
],
"container-title": "Vaccines",
"container-title-short": "Vaccines",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2024,
1,
24
]
],
"date-time": "2024-01-24T12:42:16Z",
"timestamp": 1706100136000
},
"deposited": {
"date-parts": [
[
2024,
1,
24
]
],
"date-time": "2024-01-24T13:59:58Z",
"timestamp": 1706104798000
},
"indexed": {
"date-parts": [
[
2024,
1,
25
]
],
"date-time": "2024-01-25T00:29:42Z",
"timestamp": 1706142582515
},
"is-referenced-by-count": 0,
"issue": "2",
"issued": {
"date-parts": [
[
2024,
1,
24
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2024,
2
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2024,
1,
24
]
],
"date-time": "2024-01-24T00:00:00Z",
"timestamp": 1706054400000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/2076-393X/12/2/121/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "121",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2024,
1,
24
]
]
},
"published-online": {
"date-parts": [
[
2024,
1,
24
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"DOI": "10.1056/NEJMp2002125",
"article-title": "Defining the Epidemiology of COVID-19—Studies Needed",
"author": "Lipsitch",
"doi-asserted-by": "crossref",
"first-page": "1194",
"journal-title": "N. Engl. J. Med.",
"key": "ref_1",
"volume": "382",
"year": "2020"
},
{
"key": "ref_2",
"unstructured": "World Health Organization (2023, December 12). Coronavirus Disease 2019 Situtation Report—72. Available online: https://apps.who.int/iris/bitstream/handle/10665/331685/nCoVsitrep01Apr2020-eng.pdf."
},
{
"DOI": "10.15585/mmwr.mm6912e2",
"doi-asserted-by": "crossref",
"key": "ref_3",
"unstructured": "CDC COVID-19 Response Team, Bialek, S., Boundy, E., Bowen, V., Chow, N., Cohn, A., Dowling, N., Ellington, S., Gierke, R., and Hall, A. (2020). Severe Outcomes among Patients with Coronavirus Disease 2019 (COVID-19)-United States, February 12–March 16, 2020. MMWR Morb. Mortal. Wkly. Rep., 69, 343–346."
},
{
"DOI": "10.18632/aging.103344",
"article-title": "Why does COVID-19 disproportionately affect older people?",
"author": "Mueller",
"doi-asserted-by": "crossref",
"first-page": "9959",
"journal-title": "Aging",
"key": "ref_4",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1111/j.1749-6632.2000.tb06651.x",
"article-title": "Inflamm-aging: An evolutionary perspective on immunosenescence",
"author": "Franceschi",
"doi-asserted-by": "crossref",
"first-page": "244",
"journal-title": "Ann. N. Y. Acad. Sci.",
"key": "ref_5",
"volume": "908",
"year": "2000"
},
{
"DOI": "10.3390/ijms232112906",
"doi-asserted-by": "crossref",
"key": "ref_6",
"unstructured": "Henein, M.Y., Vancheri, S., Longo, G., and Vancheri, F. (2022). The Role of Inflammation in Cardiovascular Disease. Int. J. Mol. Sci., 23."
},
{
"DOI": "10.15420/ecr.2018.33.1",
"article-title": "The Role of Inflammation in Diabetes: Current Concepts and Future Perspectives",
"author": "Tsalamandris",
"doi-asserted-by": "crossref",
"first-page": "50",
"journal-title": "Eur. Cardiol. Rev.",
"key": "ref_7",
"volume": "14",
"year": "2019"
},
{
"DOI": "10.1161/01.HYP.38.3.399",
"article-title": "Blood Pressure and Inflammation in Apparently Healthy Men",
"author": "Chae",
"doi-asserted-by": "crossref",
"first-page": "399",
"journal-title": "Hypertension",
"key": "ref_8",
"volume": "38",
"year": "2001"
},
{
"DOI": "10.1371/journal.pone.0241265",
"doi-asserted-by": "crossref",
"key": "ref_9",
"unstructured": "Javanmardi, F., Keshavarzi, A., Akbari, A., Emami, A., and Pirbonyeh, N. (2020). Prevalence of underlying diseases in died cases of COVID-19: A systematic review and meta-analysis. PLoS ONE, 15."
},
{
"DOI": "10.1016/j.eujim.2020.101226",
"article-title": "Predictors of mortality in patients with COVID-19–a systematic review",
"author": "Mehraeen",
"doi-asserted-by": "crossref",
"first-page": "101226",
"journal-title": "Eur. J. Integr. Med.",
"key": "ref_10",
"volume": "40",
"year": "2020"
},
{
"DOI": "10.11606/s1518-8787.2020054002596",
"article-title": "Adults at high-risk of severe coronavirus disease-2019 (COVID-19) in Brazil",
"author": "Rezende",
"doi-asserted-by": "crossref",
"first-page": "50",
"journal-title": "Rev. Saude Publica",
"key": "ref_11",
"volume": "54",
"year": "2020"
},
{
"DOI": "10.1111/jrh.12557",
"article-title": "The Association of Social Determinants of Health with COVID-19 Mortality in Rural and Urban Counties",
"author": "Paul",
"doi-asserted-by": "crossref",
"first-page": "278",
"journal-title": "J. Rural Health",
"key": "ref_12",
"volume": "37",
"year": "2021"
},
{
"key": "ref_13",
"unstructured": "Centers for Disease Control and Prevention (2023, December 12). Underlying Medical Conditions. Updated 25 June 2020, Available online: https://covid.cdc.gov/covid-data-tracker/#underlying-med-conditions."
},
{
"DOI": "10.20944/preprints202003.0235.v2",
"doi-asserted-by": "crossref",
"key": "ref_14",
"unstructured": "Grant, W.B., Lahore, H., McDonnell, S.L., Baggerly, C.A., French, C.B., Aliano, J.L., and Bhattoa, H.P. (2020). Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths. Nutrients, 12."
},
{
"DOI": "10.1001/jamanetworkopen.2020.19722",
"article-title": "Association of Vitamin D Status and Other Clinical Characteristics with COVID-19 Test Results",
"author": "Meltzer",
"doi-asserted-by": "crossref",
"first-page": "e2019722",
"journal-title": "JAMA Netw. Open",
"key": "ref_15",
"volume": "3",
"year": "2020"
},
{
"article-title": "Vitamin D may protect against multiple organ damage caused by COVID-19",
"author": "Aygun",
"first-page": "870",
"journal-title": "Bratisl Lek Listy.",
"key": "ref_16",
"volume": "121",
"year": "2020"
},
{
"DOI": "10.1007/s40520-020-01677-y",
"article-title": "Evidence for possible association of vitamin D status with cytokine storm and unregulated inflammation in COVID-19 patients",
"author": "Daneshkhah",
"doi-asserted-by": "crossref",
"first-page": "2141",
"journal-title": "Aging Clin. Exp. Res.",
"key": "ref_17",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1016/j.maturitas.2020.08.003",
"article-title": "Immune-boosting role of vitamins D, C, E, zinc, selenium and omega-3 fatty acids: Could they help against COVID-19?",
"author": "Shakoor",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Maturitas",
"key": "ref_18",
"volume": "143",
"year": "2021"
},
{
"DOI": "10.1016/j.jaut.2011.11.013",
"article-title": "Sex affects immunity",
"author": "Pennell",
"doi-asserted-by": "crossref",
"first-page": "J282",
"journal-title": "J. Autoimmun.",
"key": "ref_19",
"volume": "38",
"year": "2012"
},
{
"DOI": "10.1038/nri.2016.90",
"article-title": "Sex differences in immune responses",
"author": "Klein",
"doi-asserted-by": "crossref",
"first-page": "626",
"journal-title": "Nat. Rev. Immunol.",
"key": "ref_20",
"volume": "16",
"year": "2016"
},
{
"DOI": "10.1038/s41467-022-28527-x",
"article-title": "Population antibody responses following COVID-19 vaccination in 212,102 individuals",
"author": "Ward",
"doi-asserted-by": "crossref",
"first-page": "907",
"journal-title": "Nat. Commun.",
"key": "ref_21",
"volume": "13",
"year": "2022"
},
{
"DOI": "10.3389/fimmu.2021.802858",
"article-title": "Characterization of SARS-CoV-2-Specific Humoral and Cellular Immune Responses Induced by Inactivated COVID-19 Vaccines in a Real-World Setting",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "802858",
"journal-title": "Front. Immunol.",
"key": "ref_22",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1007/s12020-020-02536-6",
"article-title": "Sex differences in COVID-19: The role of androgens in disease severity and progression",
"author": "Mohamed",
"doi-asserted-by": "crossref",
"first-page": "3",
"journal-title": "Endocrine",
"key": "ref_23",
"volume": "71",
"year": "2021"
},
{
"DOI": "10.3389/fpubh.2020.00152",
"article-title": "Gender Differences in Patients with COVID-19: Focus on Severity and Mortality",
"author": "Jin",
"doi-asserted-by": "crossref",
"first-page": "152",
"journal-title": "Front. Public Health",
"key": "ref_24",
"volume": "8",
"year": "2020"
},
{
"key": "ref_25",
"unstructured": "Pan American Health Organization (2023, December 12). Social Determinants of Health. Updated 2021. Available online: https://www.paho.org/en/topics/social-determinants-health."
},
{
"DOI": "10.3390/ijerph19031294",
"doi-asserted-by": "crossref",
"key": "ref_26",
"unstructured": "Morante-García, W., Zapata-Boluda, R.M., García-González, J., Campuzano-Cuadrado, P., Calvillo, C., and Alarcón-Rodríguez, R. (2022). Influence of Social Determinants of Health on COVID-19 Infection in Socially Vulnerable Groups. Int. J. Environ. Res. Public Health, 19."
},
{
"key": "ref_27",
"unstructured": "Barr, D.A. (2019). Health Disparities in the United States: Social Class, Race, Ethnicity, and Social Determinants Of Health, Johns Hopkins University Press. [3rd ed.]."
},
{
"DOI": "10.1016/j.socscimed.2014.05.021",
"article-title": "Variations in the relation between education and cause-specific mortality in 19 European populations: A test of the “fundamental causes” theory of social inequalities in health",
"author": "Mackenbach",
"doi-asserted-by": "crossref",
"first-page": "51",
"journal-title": "Soc. Sci. Med.",
"key": "ref_28",
"volume": "127",
"year": "2015"
},
{
"DOI": "10.2337/dc11-1864",
"article-title": "Socioeconomic status and mortality: Contribution of health care access and psychological distress among U.S. adults with diagnosed diabetes",
"author": "Saydah",
"doi-asserted-by": "crossref",
"first-page": "49",
"journal-title": "Diabetes Care",
"key": "ref_29",
"volume": "36",
"year": "2013"
},
{
"DOI": "10.3389/fpubh.2020.00406",
"article-title": "Impact of Social Determinants of Health on the Emerging COVID-19 Pandemic in the United States",
"author": "Singu",
"doi-asserted-by": "crossref",
"first-page": "406",
"journal-title": "Front. Public Health",
"key": "ref_30",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.3389/fpubh.2020.00231",
"article-title": "Socioeconomic Status and Access to Healthcare: Interrelated Drivers for Healthy Aging",
"author": "McMaughan",
"doi-asserted-by": "crossref",
"first-page": "231",
"journal-title": "Front. Public Health",
"key": "ref_31",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1097/JOM.0000000000002784",
"article-title": "Disparities in Access to Paid Sick Leave During the First Year of the COVID-19 Pandemic",
"author": "Hawkins",
"doi-asserted-by": "crossref",
"first-page": "370",
"journal-title": "J. Occup. Environ. Med.",
"key": "ref_32",
"volume": "65",
"year": "2023"
},
{
"DOI": "10.1007/s11606-020-06341-9",
"article-title": "Social Determinants of Health Mediate COVID-19 Disparities in South Florida",
"author": "Palacio",
"doi-asserted-by": "crossref",
"first-page": "472",
"journal-title": "J. Gen. Intern. Med.",
"key": "ref_33",
"volume": "36",
"year": "2021"
},
{
"DOI": "10.1016/j.econlet.2020.109648",
"article-title": "When face-to-face interactions become an occupational hazard: Jobs in the time of COVID-19",
"author": "Avdiu",
"doi-asserted-by": "crossref",
"first-page": "109648",
"journal-title": "Econ. Lett.",
"key": "ref_34",
"volume": "197",
"year": "2020"
},
{
"DOI": "10.1186/s12651-022-00315-6",
"article-title": "COVID-19 and the labour market: What are the working conditions in critical jobs?",
"doi-asserted-by": "crossref",
"first-page": "10",
"journal-title": "J. Labour Mark. Res.",
"key": "ref_35",
"volume": "56",
"year": "2022"
},
{
"key": "ref_36",
"unstructured": "Gould, E., and Shierholz, H. (2023, December 12). Not Everybody Can Work from Home: Black and Hispanic Workers are Much Less Likely to be Able to Telework. Economic Policy Institute. Updated 19 March 2020. Available online: https://www.epi.org/blog/black-and-hispanic-workers-are-much-less-likely-to-be-able-to-work-from-home/."
},
{
"DOI": "10.1016/j.jpubeco.2020.104235",
"article-title": "How many jobs can be done at home?",
"author": "Dingel",
"doi-asserted-by": "crossref",
"first-page": "104235",
"journal-title": "J. Public Econ.",
"key": "ref_37",
"volume": "189",
"year": "2020"
},
{
"key": "ref_38",
"unstructured": "Angelucci, M., Angrisani, M., Bennett, D., Kapteyn, A., and Schaner, S. (2024, January 18). Remote Work and the Heterogeneous Impact of COVID-19 on Employment and Health. Available online: http://www.nber.org/papers/w27749."
},
{
"DOI": "10.1002/ajim.23145",
"article-title": "Differential occupational risk for COVID-19 and other infection exposure according to race and ethnicity",
"author": "Hawkins",
"doi-asserted-by": "crossref",
"first-page": "817",
"journal-title": "Am. J. Ind. Med.",
"key": "ref_39",
"volume": "63",
"year": "2020"
},
{
"DOI": "10.1002/ajim.23222",
"article-title": "COVID-19 as an occupational disease",
"author": "Carlsten",
"doi-asserted-by": "crossref",
"first-page": "227",
"journal-title": "Am. J. Ind. Med.",
"key": "ref_40",
"volume": "64",
"year": "2021"
},
{
"DOI": "10.1289/ehp.7609",
"article-title": "Socioeconomic and racial disparities in cancer risk from air toxics in Maryland",
"author": "Apelberg",
"doi-asserted-by": "crossref",
"first-page": "693",
"journal-title": "Environ. Health Perspect.",
"key": "ref_41",
"volume": "113",
"year": "2005"
},
{
"DOI": "10.1016/S2542-5196(19)30241-4",
"article-title": "Associations between historical residential redlining and current age-adjusted rates of emergency department visits due to asthma across eight cities in California: An ecological study",
"author": "Nardone",
"doi-asserted-by": "crossref",
"first-page": "e24",
"journal-title": "Lancet Planet. Health",
"key": "ref_42",
"volume": "4",
"year": "2020"
},
{
"key": "ref_43",
"unstructured": "American Lung Association (2023, December 12). Disparities in the Impact of Air Pollution. Updated 17 November 2022. Available online: https://www.lung.org/clean-air/outdoors/who-is-at-risk/disparities."
},
{
"DOI": "10.1126/sciadv.abd4049",
"article-title": "Air pollution and COVID-19 mortality in the United States: Strengths and limitations of an ecological regression analysis",
"author": "Wu",
"doi-asserted-by": "crossref",
"first-page": "eabd4049",
"journal-title": "Sci. Adv.",
"key": "ref_44",
"volume": "6",
"year": "2020"
},
{
"DOI": "10.1007/s40615-020-00833-4",
"article-title": "Racial, Economic, and Health Inequality and COVID-19 Infection in the United States",
"author": "Abedi",
"doi-asserted-by": "crossref",
"first-page": "732",
"journal-title": "J. Racial Ethn. Health Disparit.",
"key": "ref_45",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.1377/hlthaff.2020.01040",
"article-title": "Community-Level Factors Associated with Racial And Ethnic Disparities In COVID-19 Rates In Massachusetts",
"author": "Figueroa",
"doi-asserted-by": "crossref",
"first-page": "1984",
"journal-title": "Health Aff.",
"key": "ref_46",
"volume": "39",
"year": "2020"
},
{
"DOI": "10.1377/hlthaff.2020.00598",
"article-title": "Disparities in Outcomes among COVID-19 Patients in a Large Health Care System in California",
"author": "Azar",
"doi-asserted-by": "crossref",
"first-page": "1253",
"journal-title": "Health Aff.",
"key": "ref_47",
"volume": "39",
"year": "2020"
},
{
"DOI": "10.1001/jamanetworkopen.2021.30479",
"article-title": "Racial and Ethnic Disparities in Rates of COVID-19–Associated Hospitalization, Intensive Care Unit Admission, and in-Hospital Death in the United States from March 2020 to February 2021",
"author": "Acosta",
"doi-asserted-by": "crossref",
"first-page": "e2130479",
"journal-title": "JAMA Netw. Open",
"key": "ref_48",
"volume": "4",
"year": "2021"
},
{
"DOI": "10.1093/cid/ciaa815",
"article-title": "The Disproportionate Impact of COVID-19 on Racial and Ethnic Minorities in the United States",
"author": "Tai",
"doi-asserted-by": "crossref",
"first-page": "703",
"journal-title": "Clin. Infect. Dis.",
"key": "ref_49",
"volume": "72",
"year": "2021"
},
{
"key": "ref_50",
"unstructured": "Gangopadhyaya, A., Karpman, M., and Aarons, J. (2024, January 18). As the COVID-19 Recession Extended into the Summer of 2020, More Than 3 Million Adults Lost Employer-Sponsored Health Insurance Coverage and 2 Million Became Uninsured. Available online: https://www.rwjf.org/content/dam/farm/reports/issue_briefs/2020/rwjf462707."
},
{
"DOI": "10.1146/annurev-publhealth-032013-182419",
"article-title": "Immigration as a social determinant of health",
"author": "Holmes",
"doi-asserted-by": "crossref",
"first-page": "375",
"journal-title": "Annu. Rev. Public Health",
"key": "ref_51",
"volume": "36",
"year": "2015"
},
{
"DOI": "10.2139/ssrn.3909781",
"doi-asserted-by": "crossref",
"key": "ref_52",
"unstructured": "Bhuiyan, M.T.H., Khan, I.M., Jony, S.S.R., Robinson, R., Nguyen, U.-S.D.T., Keellings, D., Rahman, M.S., and Haque, U. (2021). The Disproportionate Impact of COVID-19 among Undocumented Immigrants and Racial Minorities in the US. Int. J. Environ. Res. Public Health, 18."
},
{
"DOI": "10.1038/s41562-022-01289-8",
"article-title": "Equitable access to COVID-19 vaccines makes a life-saving difference to all countries",
"author": "Ye",
"doi-asserted-by": "crossref",
"first-page": "207",
"journal-title": "Nat. Hum. Behav.",
"key": "ref_53",
"volume": "6",
"year": "2022"
},
{
"DOI": "10.3390/vaccines9111305",
"doi-asserted-by": "crossref",
"key": "ref_54",
"unstructured": "Hayawi, K., Shahriar, S., Serhani, M.A., Alashwal, H., and Masud, M.M. (2021). Vaccine versus Variants (3Vs): Are the COVID-19 Vaccines Effective against the Variants? A Systematic Review. Vaccines, 9."
},
{
"article-title": "Effectiveness of COVID-19 Vaccines against the B.1.617.2 (Delta) Variant",
"author": "Andrews",
"first-page": "585",
"journal-title": "N. Engl. J. Med.",
"key": "ref_55",
"volume": "385",
"year": "2023"
},
{
"DOI": "10.1056/NEJMc2215471",
"article-title": "Effectiveness of Bivalent Boosters against Severe Omicron Infection",
"author": "Lin",
"doi-asserted-by": "crossref",
"first-page": "764",
"journal-title": "N. Engl. J. Med.",
"key": "ref_56",
"volume": "388",
"year": "2023"
},
{
"key": "ref_57",
"unstructured": "COVID-19 Vaccine Tracker (2024, January 18). Approved Vaccines. Available online: https://covid19.trackvaccines.org/vaccines/approved/."
},
{
"DOI": "10.3389/fmed.2021.710010",
"article-title": "Poliovirus Vaccination Induces a Humoral Immune Response That Cross Reacts with SARS-CoV-2",
"author": "Comunale",
"doi-asserted-by": "crossref",
"first-page": "1285",
"journal-title": "Front. Med.",
"key": "ref_58",
"volume": "8",
"year": "2021"
},
{
"DOI": "10.1016/j.vaccine.2010.07.020",
"article-title": "Principles of vaccine design—Lessons from nature",
"author": "Zepp",
"doi-asserted-by": "crossref",
"first-page": "C14",
"journal-title": "Vaccine",
"key": "ref_59",
"volume": "28",
"year": "2010"
},
{
"DOI": "10.1101/2021.10.05.21264598",
"doi-asserted-by": "crossref",
"key": "ref_60",
"unstructured": "Comunale, B.A., Jackson-Ward, E., Jiang, Y., Ward, L.P., Liu, Q., Ji, L., Lai, M., Engineer, L., Comunale, R.A., and Xie, Q. (2021). Inactivated Poliovirus Vaccine Induces Antibodies that Inhibit RNA Synthesis of SARS-CoV-2: An open-label, pre-post vaccine clinical trial. medRxiv, medRxiv:2021.10.05.21264598."
},
{
"key": "ref_61",
"unstructured": "Comunale, B.A., Larson, R.J., Hsu, Y.-J., Jackson-Ward, E., Azodoh, C., Singh, A., and Engineer, L. (2023). Prior Oral Poliovirus Vaccination Decreases Odds of COVID-19 Outcomes. [Ph.D. Dissertation, Johns Hopkins Bloomberg School of Public Health]."
},
{
"DOI": "10.1093/qjmed/hcp065",
"article-title": "Dyslipidemia and cardiovascular risk: The importance of early prevention",
"author": "Miller",
"doi-asserted-by": "crossref",
"first-page": "657",
"journal-title": "QJM",
"key": "ref_62",
"volume": "102",
"year": "2009"
},
{
"DOI": "10.1161/JAHA.117.007444",
"article-title": "Dyslipidemia and Risk of Cardiovascular Events in Patients with Atrial Fibrillation Treated with Oral Anticoagulation Therapy: Insights from the ARISTOTLE (Apixaban for Reduction in Stroke and Other Thromboembolic Events in Atrial Fibrillation) Trial",
"author": "Pol",
"doi-asserted-by": "crossref",
"first-page": "e007444",
"journal-title": "J. Am. Heart Assoc.",
"key": "ref_63",
"volume": "7",
"year": "2018"
},
{
"DOI": "10.1038/s41591-022-01887-z",
"article-title": "Clinical outcomes associated with SARS-CoV-2 Omicron (B.1.1.529) variant and BA.1/BA.1.1 or BA.2 subvariant infection in Southern California",
"author": "Lewnard",
"doi-asserted-by": "crossref",
"first-page": "1933",
"journal-title": "Nat. Med.",
"key": "ref_64",
"volume": "28",
"year": "2022"
},
{
"DOI": "10.1038/s41467-022-33328-3",
"article-title": "Household transmission of the SARS-CoV-2 Omicron variant in Denmark",
"author": "Lyngse",
"doi-asserted-by": "crossref",
"first-page": "5573",
"journal-title": "Nat. Commun.",
"key": "ref_65",
"volume": "13",
"year": "2022"
},
{
"DOI": "10.3346/jkms.2023.38.e9",
"article-title": "Vaccine Effect on Household Transmission of Omicron and Delta SARS-CoV-2 Variants",
"author": "Kim",
"doi-asserted-by": "crossref",
"first-page": "e9",
"journal-title": "J. Korean Med. Sci.",
"key": "ref_66",
"volume": "38",
"year": "2023"
},
{
"key": "ref_67",
"unstructured": "California Department of Public Health (2023, December 12). Variants in California. Updated 7 July 2023, Available online: https://covid19.ca.gov/variants/#in-california."
},
{
"DOI": "10.1038/s41467-020-14396-9",
"article-title": "Sexual-dimorphism in human immune system aging",
"author": "Chung",
"doi-asserted-by": "crossref",
"first-page": "751",
"journal-title": "Nat. Commun.",
"key": "ref_68",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1016/S1473-3099(10)70049-9",
"article-title": "The Xs and Y of immune responses to viral vaccines",
"author": "Klein",
"doi-asserted-by": "crossref",
"first-page": "338",
"journal-title": "Lancet Infect. Dis.",
"key": "ref_69",
"volume": "10",
"year": "2010"
},
{
"DOI": "10.1016/j.coviro.2019.02.009",
"article-title": "The intersection of sex and gender in the treatment of influenza",
"author": "Morgan",
"doi-asserted-by": "crossref",
"first-page": "35",
"journal-title": "Curr. Opin. Virol.",
"key": "ref_70",
"volume": "35",
"year": "2019"
},
{
"DOI": "10.1016/j.immuni.2015.11.012",
"article-title": "Systems Analysis of Immunity to Influenza Vaccination across Multiple Years and in Diverse Populations Reveals Shared Molecular Signatures",
"author": "Nakaya",
"doi-asserted-by": "crossref",
"first-page": "1186",
"journal-title": "Immunity",
"key": "ref_71",
"volume": "43",
"year": "2015"
},
{
"DOI": "10.1016/j.vaccine.2015.11.058",
"article-title": "The confounded effects of age and exposure history in response to influenza vaccination",
"author": "McElhaney",
"doi-asserted-by": "crossref",
"first-page": "540",
"journal-title": "Vaccine",
"key": "ref_72",
"volume": "34",
"year": "2016"
},
{
"DOI": "10.1016/j.puhe.2021.07.039",
"article-title": "Association between overcrowded households, multigenerational households, and COVID-19: A cohort study",
"author": "Ghosh",
"doi-asserted-by": "crossref",
"first-page": "273",
"journal-title": "Public Health",
"key": "ref_73",
"volume": "198",
"year": "2021"
},
{
"DOI": "10.1093/ajcn/nqz037",
"article-title": "Vitamin D status in the United States, 2011–2014",
"author": "Herrick",
"doi-asserted-by": "crossref",
"first-page": "150",
"journal-title": "Am. J. Clin. Nutr.",
"key": "ref_74",
"volume": "110",
"year": "2019"
},
{
"DOI": "10.1002/jbm4.10585",
"article-title": "Trends in Vitamin D Status Around the World",
"author": "Lips",
"doi-asserted-by": "crossref",
"first-page": "e10585",
"journal-title": "JBMR Plus",
"key": "ref_75",
"volume": "5",
"year": "2021"
},
{
"article-title": "Vitamin D insufficiency in a population of healthy western Canadians",
"author": "Rucker",
"first-page": "1517",
"journal-title": "CMAJ",
"key": "ref_76",
"volume": "166",
"year": "2002"
},
{
"DOI": "10.1007/BF03405185",
"article-title": "Are national vitamin D guidelines sufficient to maintain adequate blood levels in children?",
"author": "Roth",
"doi-asserted-by": "crossref",
"first-page": "443",
"journal-title": "Can. J. Public Health",
"key": "ref_77",
"volume": "96",
"year": "2005"
},
{
"DOI": "10.1007/s40520-020-01570-8",
"article-title": "The role of vitamin D in the prevention of coronavirus disease 2019 infection and mortality",
"author": "Ilie",
"doi-asserted-by": "crossref",
"first-page": "1195",
"journal-title": "Aging Clin. Exp. Res.",
"key": "ref_78",
"volume": "32",
"year": "2020"
},
{
"DOI": "10.1007/s12020-023-03481-w",
"article-title": "Lack of vitamin D predicts impaired long-term immune response to COVID-19 vaccination",
"author": "Frara",
"doi-asserted-by": "crossref",
"first-page": "536",
"journal-title": "Endocrine",
"key": "ref_79",
"volume": "82",
"year": "2023"
},
{
"DOI": "10.1016/S0271-5317(83)80006-2",
"article-title": "The relationship of socio-economic factors to the use of vitamin supplements in the city of windsor",
"author": "Griffith",
"doi-asserted-by": "crossref",
"first-page": "445",
"journal-title": "Nutr. Res.",
"key": "ref_80",
"volume": "3",
"year": "1983"
},
{
"DOI": "10.1111/nyas.13968",
"article-title": "Global prevalence and disease burden of vitamin D deficiency: A roadmap for action in low- and middle-income countries",
"author": "Roth",
"doi-asserted-by": "crossref",
"first-page": "44",
"journal-title": "Ann. N. Y. Acad. Sci.",
"key": "ref_81",
"volume": "1430",
"year": "2018"
},
{
"DOI": "10.4049/jimmunol.162.8.5011",
"article-title": "Induction of mucosal immunity by inactivated poliovirus vaccine is dependent on previous mucosal contact with live virus",
"author": "Herremans",
"doi-asserted-by": "crossref",
"first-page": "5011",
"journal-title": "J. Immunol.",
"key": "ref_82",
"volume": "162",
"year": "1999"
},
{
"DOI": "10.1126/scitranslmed.abd2223",
"article-title": "IgA dominates the early neutralizing antibody response to SARS-CoV-2",
"author": "Sterlin",
"doi-asserted-by": "crossref",
"first-page": "eabd2223",
"journal-title": "Sci. Transl. Med.",
"key": "ref_83",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1016/S0140-6736(14)60934-X",
"article-title": "Effect of a single inactivated poliovirus vaccine dose on intestinal immunity against poliovirus in children previously given oral vaccine: An open-label, randomised controlled trial",
"author": "John",
"doi-asserted-by": "crossref",
"first-page": "1505",
"journal-title": "Lancet",
"key": "ref_84",
"volume": "384",
"year": "2014"
},
{
"DOI": "10.3389/fpubh.2022.862816",
"article-title": "Lifestyle, Physical Activity, Eating and Hygiene Habits: A Comparative Analysis Before and During the COVID-19 Pandemic in Student Population",
"author": "Sekulic",
"doi-asserted-by": "crossref",
"first-page": "862816",
"journal-title": "Front. Public Health",
"key": "ref_85",
"volume": "10",
"year": "2022"
},
{
"DOI": "10.1016/j.jsps.2022.03.006",
"article-title": "Medications and natural products used in Jordan for prevention or treatment of COVID-19 infection during the second wave of the pandemic: A cross-sectional online survey",
"author": "Thiab",
"doi-asserted-by": "crossref",
"first-page": "856",
"journal-title": "Saudi Pharm. J.",
"key": "ref_86",
"volume": "30",
"year": "2022"
},
{
"DOI": "10.1155/2022/4064588",
"doi-asserted-by": "crossref",
"key": "ref_87",
"unstructured": "Wang, Z., Li, W.T., Gao, Y., Xue, X., Pang, H., Hao, W., Xia, Y., Wang, S., Su, X., and Zhao, L. (2022). Analysis of Dietary Supplement Use and Influencing Factors in the Mongolian Population. BioMed Res. Int., 2022."
},
{
"DOI": "10.1093/aje/kwg072",
"article-title": "Factors associated with dietary supplement use among healthy adults of five ethnicities: The Multiethnic Cohort Study",
"author": "Foote",
"doi-asserted-by": "crossref",
"first-page": "888",
"journal-title": "Am. J. Epidemiol.",
"key": "ref_88",
"volume": "157",
"year": "2003"
}
],
"reference-count": 88,
"references-count": 88,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/2076-393X/12/2/121"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Pharmacology (medical)",
"Infectious Diseases",
"Drug Discovery",
"Pharmacology",
"Immunology"
],
"subtitle": [],
"title": "Vitamin D Supplementation and Prior Oral Poliovirus Vaccination Decrease Odds of COVID-19 Outcomes among Adults Recently Inoculated with Inactivated Poliovirus Vaccine",
"type": "journal-article",
"volume": "12"
}
