Association of Serum Zinc and Inflammatory Markers with the Severity of COVID-19 Infection in Adult Patients
et al., Nutrients, doi:10.3390/nu15020340, Jan 2023
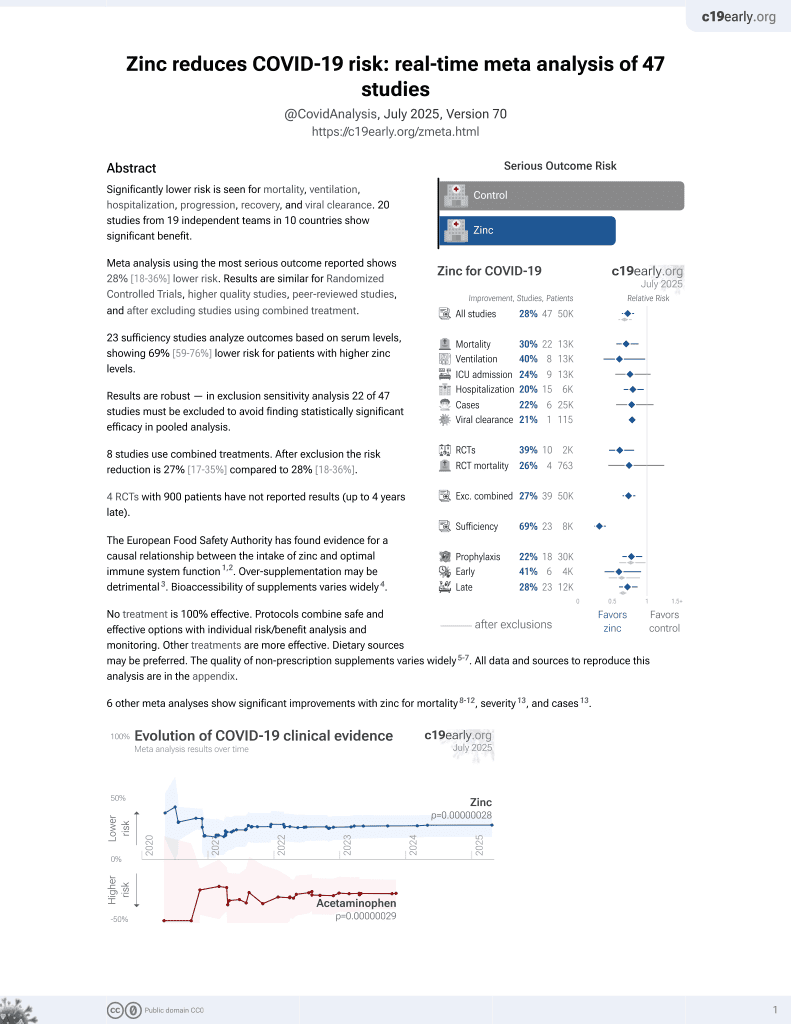
Zinc for COVID-19
2nd treatment shown to reduce risk in
July 2020, now with p = 0.00000012 from 41 studies, recognized in 23 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
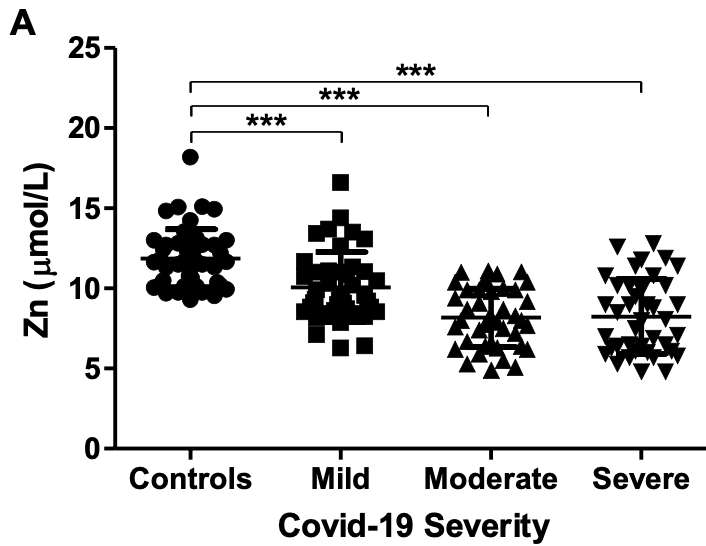
Prospective study of 123 COVID+ patients and 48 controls, showing significantly lower zinc levels in COVID-19 patients, and a negative correlation between zinc levels and COVID-19 severity. Moderate and severe cases were significantly older, however the negative correlation remained significant after adjusting for age.
Almasaud et al., 10 Jan 2023, prospective, Saudi Arabia, peer-reviewed, 8 authors, study period 25 June, 2020 - 3 March, 2022.
Contact: iqbalja@ngha.med.sa (corresponding author).
Association of Serum Zinc and Inflammatory Markers with the Severity of COVID-19 Infection in Adult Patients
Nutrients, doi:10.3390/nu15020340
COVID-19 infection can spread in the host body without any adequate immune response. Zinc is an essential trace element with strong immunoregulatory and antiviral properties and its deficiency might lead to inflammation and oxidative stress. The aim of the current study was to determine the association of serum zinc and inflammatory markers with the severity of COVID-19 infection. This was a prospective observational study in which 123 COVID-19-positive adult patients and 48 controls were recruited. The initial comparative analysis was conducted between COVID-19 patients and controls. COVID-19-positive patients were further divided into three different groups (mild, moderate, and severe) based on the severity of COVID-19 infection. COVID-19 patients showed significantly lower serum zinc levels (8.8 ± 2.3 µmol/L) compared to healthy controls (11.9 ± 1.8 µmol/L). There was a negative correlation between serum zinc levels and the severity of COVID-19 infection (r = −0.584, p < 0.0001) and this effect was independent of age (r = −0.361, p < 0.0001). Furthermore, inflammatory markers showed a positive correlation with the severity of COVID-19 infection and a negative correlation with the levels of serum zinc. The study demonstrated an association between COVID-19 infection with low serum zinc levels and elevated inflammatory markers. Further studies to assess the significance of this observation are needed, which may justify zinc supplementation to mitigate the severity of COVID-19 infection.
Author Contributions: A.S.A. and J.I. contributed to the conception and design of the study. J.C., A.A.A., A.A.Q., A.A. and Z.N. helped in the recruitment and collection of demographic data from the patients. S.A. conducted the biochemical and hematological assessment of the samples. A.S.A. and J.I. performed data analysis and interpretation. J.I. drafted the first manuscript. A.S.A., J.C., A.A.A.
Conflicts of Interest: The authors declare no conflict of interest.
References
Asghar, Haider Kazmi, Khan, Akram, Hassan et al., Poor Prognostic Biochemical Markers Predicting Fatalities Caused by COVID-19: A Retrospective Observational Study From a Developing Country, Cureus, doi:10.7759/cureus.9575
Berg, Bolt, Andersen, Owen, Zinc potentiates the antiviral action of human IFN-alpha tenfold, J. Interferon Cytokine Res, doi:10.1089/10799900152434330
Besecker, Bao, Bohacova, Papp, Sadee et al., The human zinc transporter SLC39A8 (Zip8) is critical in zinc-mediated cytoprotection in lung epithelia, Am. J. Physiol. Lung Cell. Mol. Physiol, doi:10.1152/ajplung.00057.2008
Broman, Bernardson, Bursell, Wernerman, Flaring et al., Serum selenium in critically ill patients: Profile and supplementation in a depleted region, Acta Anaesthesiol. Scand, doi:10.1111/aas.13573
Cakman, Kirchner, Rink, Zinc supplementation reconstitutes the production of interferon-alpha by leukocytes from elderly persons, J. Interferon Cytokine Res, doi:10.1089/jir.1997.17.469
Cecchini, Cecchini, SARS-CoV-2 infection pathogenesis is related to oxidative stress as a response to aggression, Med. Hypotheses, doi:10.1016/j.mehy.2020.110102
Choi, Ryter, Levine, Autophagy in human health and disease, N. Engl. J. Med, doi:10.1056/NEJMra1205406
Conti, Ronconi, Caraffa, Gallenga, Ross et al., Induction of pro-inflammatory cytokines (IL-1 and IL-6) and lung inflammation by Coronavirus-19 (COVID-19 or SARS-CoV-2): Anti-inflammatory strategies, J. Biol. Regul. Homeost. Agents, doi:10.23812/CONTI-E
Devaux, Rolain, Raoult, ACE2 receptor polymorphism: Susceptibility to SARS-CoV-2, hypertension, multi-organ failure, and COVID-19 disease outcome, J. Microbiol. Immunol. Infect, doi:10.1016/j.jmii.2020.04.015
Gordon, Hardigan, A Case-Control Study for the Effectiveness of Oral Zinc in the Prevention and Mitigation of COVID-19, Front. Med, doi:10.3389/fmed.2021.756707
Hasan, Rink, Haase, Chelation of Free Zn 2+ Impairs Chemotaxis, Phagocytosis, Oxidative Burst, Degranulation, and Cytokine Production by Neutrophil Granulocytes, Biol. Trace Elem. Res, doi:10.1007/s12011-015-0515-0
Huang, Wang, Li, Ren, Zhao et al., Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China, Lancet, doi:10.1016/S0140-6736(20)30183-5
Ibs, Rink, Zinc-altered immune function, J. Nutr, doi:10.1093/jn/133.5.1452S
Jackson, Farzan, Chen, Choe, Mechanisms of SARS-CoV-2 entry into cells, Nat. Rev. Mol. Cell Biol
Jahromi, Moradi Tabriz, Togha, Ariyanfar, Ghorbani et al., The correlation between serum selenium, zinc, and COVID-19 severity: An observational study, BMC Infect. Dis, doi:10.1186/s12879-021-06617-3
Jiang, Mizushima, Autophagy and human diseases, Cell Res, doi:10.1038/cr.2013.161
Jothimani, Kailasam, Danielraj, Nallathambi, Ramachandran et al., COVID-19: Poor outcomes in patients with zinc deficiency, Int. J. Infect. Dis
Kaushal, Kaur, Sarma, Bhattacharyya, Sharma et al., Serum ferritin as a predictive biomarker in COVID-19. A systematic review, meta-analysis and meta-regression analysis, J. Crit. Care, doi:10.1016/j.jcrc.2021.09.023
Korant, Kauer, Butterworth, Zinc ions inhibit replication of rhinoviruses, Nature, doi:10.1038/248588a0
Krenn, Gaudernak, Holzer, Lanke, Van Kuppeveld et al., Antiviral activity of the zinc ionophores pyrithione and hinokitiol against picornavirus infections, J. Virol, doi:10.1128/JVI.01543-08
Lanke, Krenn, Melchers, Seipelt, Van Kuppeveld, PDTC inhibits picornavirus polyprotein processing and RNA replication by transporting zinc ions into cells, J. Gen. Virol, doi:10.1099/vir.0.82634-0
Laur, Kinscherf, Pomytkin, Kaiser, Knes et al., ICP-MS trace element analysis in serum and whole blood, PLoS ONE, doi:10.1371/journal.pone.0233357
Li, Li, Zhang, Wang, Expression of the SARS-CoV-2 cell receptor gene ACE2 in a wide variety of human tissues, Infect. Dis. Poverty, doi:10.1186/s40249-020-00662-x
Liuzzi, Yoo, Role of zinc in the regulation of autophagy during ethanol exposure in human hepatoma cells, Biol. Trace Elem. Res, doi:10.1007/s12011-013-9816-3
Matute-Bello, Liles, Steinberg, Kiener, Mongovin et al., Soluble Fas ligand induces epithelial cell apoptosis in humans with acute lung injury (ARDS), J. Immunol
Meijer, Codogno, Autophagy: Regulation and role in disease, Crit. Rev. Clin. Lab. Sci, doi:10.1080/10408360903044068
Overbeck, Rink, Haase, Modulating the immune response by oral zinc supplementation: A single approach for multiple diseases, Arch. Immunol. Ther. Exp, doi:10.1007/s00005-008-0003-8
Pal, Squitti, Picozza, Pawar, Rongioletti et al., Zinc and COVID-19: Basis of Current Clinical Trials, Biol. Trace Elem. Res, doi:10.1007/s12011-020-02437-9
Prasad, Zinc in human health: Effect of zinc on immune cells, Mol. Med, doi:10.2119/2008-00033.Prasad
Shankar, Prasad, Zinc and immune function: The biological basis of altered resistance to infection, Am. J. Clin. Nutr, doi:10.1093/ajcn/68.2.447S
Velthuis, Van Den Worm, Sims, Baric, Snijder et al., Zn 2+ inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture, PLoS Pathog, doi:10.1371/journal.ppat.1001176
Wessels, Rolles, Rink, The Potential Impact of Zinc Supplementation on COVID-19 Pathogenesis, Front. Immunol, doi:10.3389/fimmu.2020.01712
Xu, Gong, Sun, Cai, Liu et al., Impact of Selenium Deficiency on Inflammation, Oxidative Stress, and Phagocytosis in Mouse Macrophages, Biol. Trace Elem. Res, doi:10.1007/s12011-019-01775-7
Zhang, Liu, Potential interventions for novel coronavirus in China: A systematic review, J. Med. Virol
DOI record:
{
"DOI": "10.3390/nu15020340",
"ISSN": [
"2072-6643"
],
"URL": "http://dx.doi.org/10.3390/nu15020340",
"abstract": "<jats:p>COVID-19 infection can spread in the host body without any adequate immune response. Zinc is an essential trace element with strong immunoregulatory and antiviral properties and its deficiency might lead to inflammation and oxidative stress. The aim of the current study was to determine the association of serum zinc and inflammatory markers with the severity of COVID-19 infection. This was a prospective observational study in which 123 COVID-19-positive adult patients and 48 controls were recruited. The initial comparative analysis was conducted between COVID-19 patients and controls. COVID-19-positive patients were further divided into three different groups (mild, moderate, and severe) based on the severity of COVID-19 infection. COVID-19 patients showed significantly lower serum zinc levels (8.8 ± 2.3 µmol/L) compared to healthy controls (11.9 ± 1.8 µmol/L). There was a negative correlation between serum zinc levels and the severity of COVID-19 infection (r = −0.584, p < 0.0001) and this effect was independent of age (r = −0.361, p < 0.0001). Furthermore, inflammatory markers showed a positive correlation with the severity of COVID-19 infection and a negative correlation with the levels of serum zinc. The study demonstrated an association between COVID-19 infection with low serum zinc levels and elevated inflammatory markers. Further studies to assess the significance of this observation are needed, which may justify zinc supplementation to mitigate the severity of COVID-19 infection.</jats:p>",
"alternative-id": [
"nu15020340"
],
"author": [
{
"affiliation": [],
"family": "Almasaud",
"given": "Abdulaziz Saad",
"sequence": "first"
},
{
"affiliation": [],
"family": "Chalabi",
"given": "Jamal",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Arfaj",
"given": "Abdulmajid Al",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-2413-6637",
"affiliation": [],
"authenticated-orcid": false,
"family": "Qarni",
"given": "Ali Al",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Alkroud",
"given": "Ammar",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Nagoor",
"given": "Zuheb",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Akhtar",
"given": "Sana",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-9021-2271",
"affiliation": [],
"authenticated-orcid": false,
"family": "Iqbal",
"given": "Jahangir",
"sequence": "additional"
}
],
"container-title": "Nutrients",
"container-title-short": "Nutrients",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
1,
11
]
],
"date-time": "2023-01-11T07:59:54Z",
"timestamp": 1673423994000
},
"deposited": {
"date-parts": [
[
2023,
1,
11
]
],
"date-time": "2023-01-11T08:35:07Z",
"timestamp": 1673426107000
},
"funder": [
{
"DOI": "10.13039/501100013302",
"award": [
"RA20/027/A"
],
"doi-asserted-by": "publisher",
"name": "KAIMRC"
}
],
"indexed": {
"date-parts": [
[
2023,
1,
12
]
],
"date-time": "2023-01-12T07:04:39Z",
"timestamp": 1673507079437
},
"is-referenced-by-count": 0,
"issue": "2",
"issued": {
"date-parts": [
[
2023,
1,
10
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2023,
1
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
1,
10
]
],
"date-time": "2023-01-10T00:00:00Z",
"timestamp": 1673308800000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/2072-6643/15/2/340/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "340",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2023,
1,
10
]
]
},
"published-online": {
"date-parts": [
[
2023,
1,
10
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"article-title": "Induction of pro-inflammatory cytokines (IL-1 and IL-6) and lung inflammation by Coronavirus-19 (COVID-19 or SARS-CoV-2): Anti-inflammatory strategies",
"author": "Conti",
"first-page": "327",
"journal-title": "J. Biol. Regul. Homeost. Agents",
"key": "ref_1",
"volume": "34",
"year": "2020"
},
{
"DOI": "10.1016/j.mehy.2020.110102",
"article-title": "SARS-CoV-2 infection pathogenesis is related to oxidative stress as a response to aggression",
"author": "Cecchini",
"doi-asserted-by": "crossref",
"first-page": "110102",
"journal-title": "Med. Hypotheses",
"key": "ref_2",
"volume": "143",
"year": "2020"
},
{
"DOI": "10.1007/s00005-008-0003-8",
"article-title": "Modulating the immune response by oral zinc supplementation: A single approach for multiple diseases",
"author": "Overbeck",
"doi-asserted-by": "crossref",
"first-page": "15",
"journal-title": "Arch. Immunol. Ther. Exp.",
"key": "ref_3",
"volume": "56",
"year": "2008"
},
{
"DOI": "10.1007/s12011-015-0515-0",
"article-title": "Chelation of Free Zn2+ Impairs Chemotaxis, Phagocytosis, Oxidative Burst, Degranulation, and Cytokine Production by Neutrophil Granulocytes",
"author": "Hasan",
"doi-asserted-by": "crossref",
"first-page": "79",
"journal-title": "Biol. Trace Elem. Res.",
"key": "ref_4",
"volume": "171",
"year": "2016"
},
{
"DOI": "10.1093/jn/133.5.1452S",
"article-title": "Zinc-altered immune function",
"author": "Ibs",
"doi-asserted-by": "crossref",
"first-page": "1452S",
"journal-title": "J. Nutr.",
"key": "ref_5",
"volume": "133",
"year": "2003"
},
{
"DOI": "10.1038/cr.2013.161",
"article-title": "Autophagy and human diseases",
"author": "Jiang",
"doi-asserted-by": "crossref",
"first-page": "69",
"journal-title": "Cell Res.",
"key": "ref_6",
"volume": "24",
"year": "2014"
},
{
"DOI": "10.1056/NEJMra1205406",
"article-title": "Autophagy in human health and disease",
"author": "Choi",
"doi-asserted-by": "crossref",
"first-page": "651",
"journal-title": "N. Engl. J. Med.",
"key": "ref_7",
"volume": "368",
"year": "2013"
},
{
"DOI": "10.1080/10408360903044068",
"article-title": "Autophagy: Regulation and role in disease",
"author": "Meijer",
"doi-asserted-by": "crossref",
"first-page": "210",
"journal-title": "Crit. Rev. Clin. Lab. Sci.",
"key": "ref_8",
"volume": "46",
"year": "2009"
},
{
"DOI": "10.1007/s12011-013-9816-3",
"article-title": "Role of zinc in the regulation of autophagy during ethanol exposure in human hepatoma cells",
"author": "Liuzzi",
"doi-asserted-by": "crossref",
"first-page": "350",
"journal-title": "Biol. Trace Elem. Res.",
"key": "ref_9",
"volume": "156",
"year": "2013"
},
{
"DOI": "10.1038/248588a0",
"article-title": "Zinc ions inhibit replication of rhinoviruses",
"author": "Korant",
"doi-asserted-by": "crossref",
"first-page": "588",
"journal-title": "Nature",
"key": "ref_10",
"volume": "248",
"year": "1974"
},
{
"DOI": "10.1099/vir.0.82634-0",
"article-title": "PDTC inhibits picornavirus polyprotein processing and RNA replication by transporting zinc ions into cells",
"author": "Lanke",
"doi-asserted-by": "crossref",
"first-page": "1206",
"journal-title": "J. Gen. Virol.",
"key": "ref_11",
"volume": "88",
"year": "2007"
},
{
"DOI": "10.1128/JVI.01543-08",
"article-title": "Antiviral activity of the zinc ionophores pyrithione and hinokitiol against picornavirus infections",
"author": "Krenn",
"doi-asserted-by": "crossref",
"first-page": "58",
"journal-title": "J. Virol.",
"key": "ref_12",
"volume": "83",
"year": "2009"
},
{
"DOI": "10.1371/journal.ppat.1001176",
"doi-asserted-by": "crossref",
"key": "ref_13",
"unstructured": "Te Velthuis, A.J., van den Worm, S.H., Sims, A.C., Baric, R.S., Snijder, E.J., and van Hemert, M.J. (2010). Zn2+ inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture. PLoS Pathog., 6."
},
{
"DOI": "10.1089/jir.1997.17.469",
"article-title": "Zinc supplementation reconstitutes the production of interferon-alpha by leukocytes from elderly persons",
"author": "Cakman",
"doi-asserted-by": "crossref",
"first-page": "469",
"journal-title": "J. Interferon Cytokine Res.",
"key": "ref_14",
"volume": "17",
"year": "1997"
},
{
"DOI": "10.1089/10799900152434330",
"article-title": "Zinc potentiates the antiviral action of human IFN-alpha tenfold",
"author": "Berg",
"doi-asserted-by": "crossref",
"first-page": "471",
"journal-title": "J. Interferon Cytokine Res.",
"key": "ref_15",
"volume": "21",
"year": "2001"
},
{
"DOI": "10.1002/jmv.25707",
"article-title": "Potential interventions for novel coronavirus in China: A systematic review",
"author": "Zhang",
"doi-asserted-by": "crossref",
"first-page": "479",
"journal-title": "J. Med. Virol.",
"key": "ref_16",
"volume": "92",
"year": "2020"
},
{
"DOI": "10.1186/s12879-021-06617-3",
"doi-asserted-by": "crossref",
"key": "ref_17",
"unstructured": "Razeghi Jahromi, S., Moradi Tabriz, H., Togha, M., Ariyanfar, S., Ghorbani, Z., Naeeni, S., Haghighi, S., Jazayeri, A., Montazeri, M., and Talebpour, M. (2021). The correlation between serum selenium, zinc, and COVID-19 severity: An observational study. BMC Infect. Dis., 21."
},
{
"DOI": "10.1093/ajcn/68.2.447S",
"article-title": "Zinc and immune function: The biological basis of altered resistance to infection",
"author": "Shankar",
"doi-asserted-by": "crossref",
"first-page": "447S",
"journal-title": "Am. J. Clin. Nutr.",
"key": "ref_18",
"volume": "68",
"year": "1998"
},
{
"DOI": "10.2119/2008-00033.Prasad",
"article-title": "Zinc in human health: Effect of zinc on immune cells",
"author": "Prasad",
"doi-asserted-by": "crossref",
"first-page": "353",
"journal-title": "Mol. Med.",
"key": "ref_19",
"volume": "14",
"year": "2008"
},
{
"DOI": "10.1038/s41580-021-00418-x",
"article-title": "Mechanisms of SARS-CoV-2 entry into cells",
"author": "Jackson",
"doi-asserted-by": "crossref",
"first-page": "3",
"journal-title": "Nat. Rev. Mol. Cell Biol.",
"key": "ref_20",
"volume": "23",
"year": "2022"
},
{
"DOI": "10.1016/S0140-6736(20)30183-5",
"article-title": "Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "497",
"journal-title": "Lancet",
"key": "ref_21",
"volume": "395",
"year": "2020"
},
{
"DOI": "10.1371/journal.pone.0233357",
"doi-asserted-by": "crossref",
"key": "ref_22",
"unstructured": "Laur, N., Kinscherf, R., Pomytkin, K., Kaiser, L., Knes, O., and Deigner, H.P. (2020). ICP-MS trace element analysis in serum and whole blood. PLoS ONE, 15."
},
{
"DOI": "10.1007/s12011-019-01775-7",
"article-title": "Impact of Selenium Deficiency on Inflammation, Oxidative Stress, and Phagocytosis in Mouse Macrophages",
"author": "Xu",
"doi-asserted-by": "crossref",
"first-page": "237",
"journal-title": "Biol. Trace Elem. Res.",
"key": "ref_23",
"volume": "194",
"year": "2020"
},
{
"article-title": "Poor Prognostic Biochemical Markers Predicting Fatalities Caused by COVID-19: A Retrospective Observational Study From a Developing Country",
"author": "Asghar",
"first-page": "e9575",
"journal-title": "Cureus",
"key": "ref_24",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1016/j.jcrc.2021.09.023",
"article-title": "Serum ferritin as a predictive biomarker in COVID-19. A systematic review, meta-analysis and meta-regression analysis",
"author": "Kaushal",
"doi-asserted-by": "crossref",
"first-page": "172",
"journal-title": "J. Crit. Care",
"key": "ref_25",
"volume": "67",
"year": "2022"
},
{
"DOI": "10.1016/j.ijid.2020.09.014",
"article-title": "COVID-19: Poor outcomes in patients with zinc deficiency",
"author": "Jothimani",
"doi-asserted-by": "crossref",
"first-page": "343",
"journal-title": "Int. J. Infect. Dis.",
"key": "ref_26",
"volume": "100",
"year": "2020"
},
{
"DOI": "10.3389/fimmu.2020.01712",
"article-title": "The Potential Impact of Zinc Supplementation on COVID-19 Pathogenesis",
"author": "Wessels",
"doi-asserted-by": "crossref",
"first-page": "1712",
"journal-title": "Front. Immunol.",
"key": "ref_27",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1111/aas.13573",
"article-title": "Serum selenium in critically ill patients: Profile and supplementation in a depleted region",
"author": "Broman",
"doi-asserted-by": "crossref",
"first-page": "803",
"journal-title": "Acta Anaesthesiol. Scand.",
"key": "ref_28",
"volume": "64",
"year": "2020"
},
{
"DOI": "10.1007/s12011-020-02437-9",
"article-title": "Zinc and COVID-19: Basis of Current Clinical Trials",
"author": "Pal",
"doi-asserted-by": "crossref",
"first-page": "2882",
"journal-title": "Biol. Trace Elem. Res.",
"key": "ref_29",
"volume": "199",
"year": "2021"
},
{
"DOI": "10.1152/ajplung.00057.2008",
"article-title": "The human zinc transporter SLC39A8 (Zip8) is critical in zinc-mediated cytoprotection in lung epithelia",
"author": "Besecker",
"doi-asserted-by": "crossref",
"first-page": "L1127",
"journal-title": "Am. J. Physiol. Lung Cell. Mol. Physiol.",
"key": "ref_30",
"volume": "294",
"year": "2008"
},
{
"DOI": "10.4049/jimmunol.163.4.2217",
"article-title": "Soluble Fas ligand induces epithelial cell apoptosis in humans with acute lung injury (ARDS)",
"author": "Liles",
"doi-asserted-by": "crossref",
"first-page": "2217",
"journal-title": "J. Immunol.",
"key": "ref_31",
"volume": "163",
"year": "1999"
},
{
"DOI": "10.1016/j.jmii.2020.04.015",
"article-title": "ACE2 receptor polymorphism: Susceptibility to SARS-CoV-2, hypertension, multi-organ failure, and COVID-19 disease outcome",
"author": "Devaux",
"doi-asserted-by": "crossref",
"first-page": "425",
"journal-title": "J. Microbiol. Immunol. Infect.",
"key": "ref_32",
"volume": "53",
"year": "2020"
},
{
"DOI": "10.1186/s40249-020-00662-x",
"article-title": "Expression of the SARS-CoV-2 cell receptor gene ACE2 in a wide variety of human tissues",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "45",
"journal-title": "Infect. Dis. Poverty",
"key": "ref_33",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.3389/fmed.2021.756707",
"article-title": "A Case-Control Study for the Effectiveness of Oral Zinc in the Prevention and Mitigation of COVID-19",
"author": "Gordon",
"doi-asserted-by": "crossref",
"first-page": "756707",
"journal-title": "Front. Med.",
"key": "ref_34",
"volume": "8",
"year": "2021"
}
],
"reference-count": 34,
"references-count": 34,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/2072-6643/15/2/340"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Food Science",
"Nutrition and Dietetics"
],
"subtitle": [],
"title": "Association of Serum Zinc and Inflammatory Markers with the Severity of COVID-19 Infection in Adult Patients",
"type": "journal-article",
"volume": "15"
}
