Immunomodulatory role of Nanocurcumin in COVID-19 patients with dropped natural killer cells frequency and function
et al., European Journal of Pharmacology, doi:10.1016/j.ejphar.2022.175267, IRCT20200324046851N1, Sep 2022
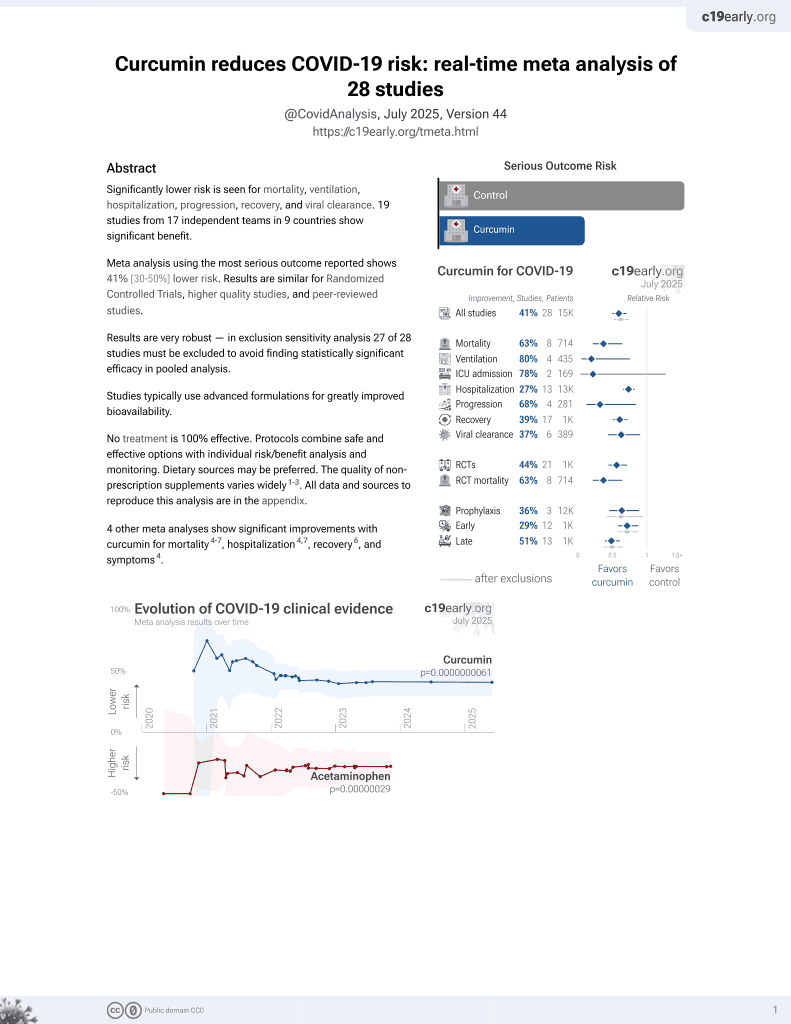
Curcumin for COVID-19
16th treatment shown to reduce risk in
February 2021, now with p = 0.0000000061 from 28 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
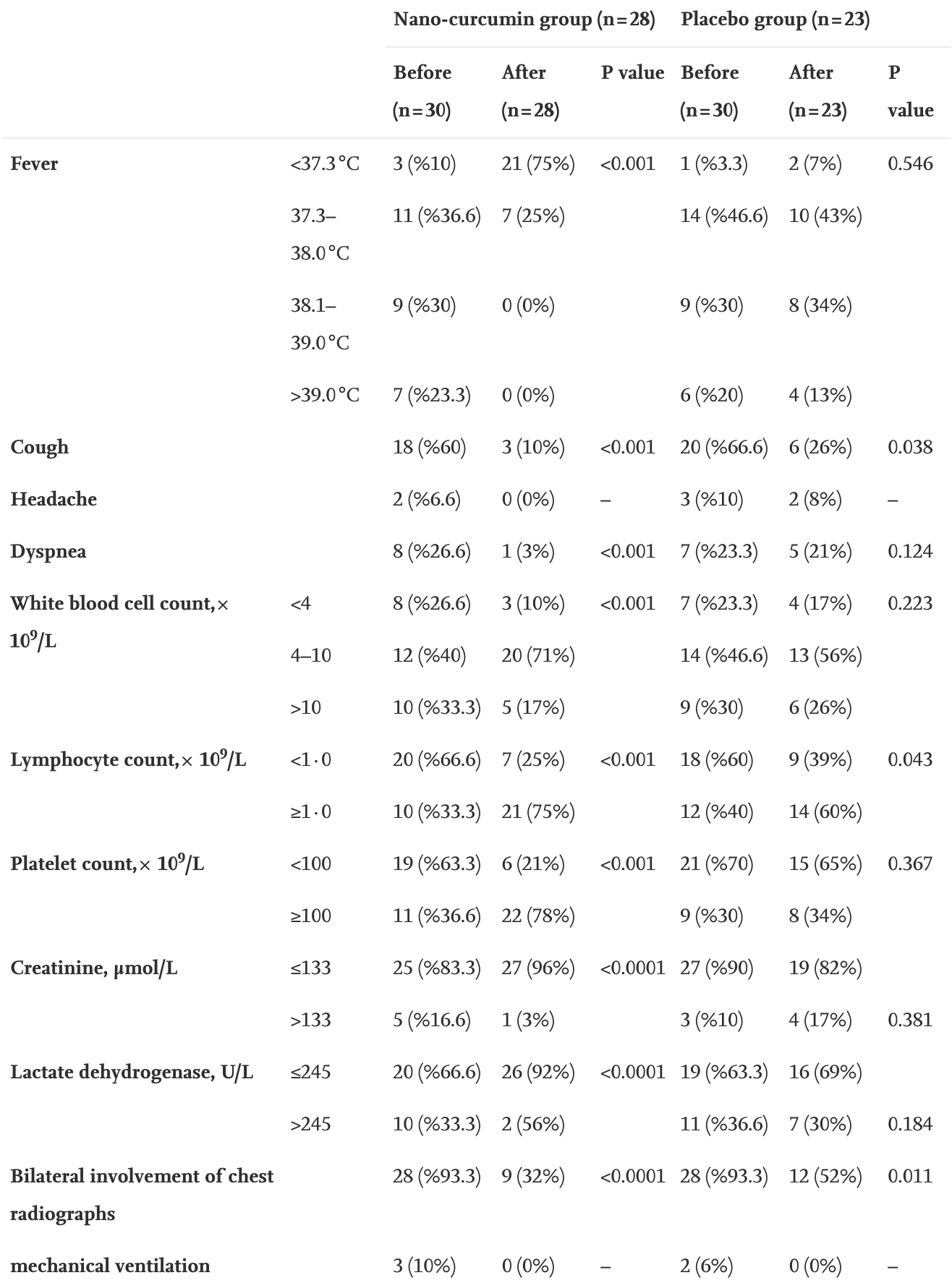
RCT with 30 nanocurcumin and 30 control patients in Iran, showing lower mortality and improved recovery, without statistical significance, and improved NK cell function. 160mg nanocurcumin for 21 days.
This is the 15th of 21 COVID-19 RCTs for curcumin, which collectively show efficacy with p=0.0000022.
This is the 21st of 28 COVID-19 controlled studies for curcumin, which collectively show efficacy with p=0.0000000061.
|
risk of death, 71.4% lower, RR 0.29, p = 0.15, treatment 2 of 30 (6.7%), control 7 of 30 (23.3%), NNT 6.0.
|
|
risk of no recovery, 86.3% lower, RR 0.14, p = 0.04, treatment 1 of 28 (3.6%), control 6 of 23 (26.1%), NNT 4.4, dyspnea.
|
|
risk of no recovery, 89.9% lower, RR 0.10, p = 0.04, treatment 0 of 28 (0.0%), control 4 of 23 (17.4%), NNT 5.8, relative risk is not 0 because of continuity correction due to zero events (with reciprocal of the contrasting arm), fever >39.0.
|
|
risk of no recovery, 38.4% lower, RR 0.62, p = 0.17, treatment 9 of 28 (32.1%), control 12 of 23 (52.2%), NNT 5.0, bilateral chest radiograph involvement.
|
|
risk of no recovery, 58.9% lower, RR 0.41, p = 0.27, treatment 3 of 28 (10.7%), control 6 of 23 (26.1%), NNT 6.5, cough.
|
|
risk of no recovery, 81.6% lower, RR 0.18, p = 0.20, treatment 0 of 28 (0.0%), control 2 of 23 (8.7%), NNT 12, relative risk is not 0 because of continuity correction due to zero events (with reciprocal of the contrasting arm), headache.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Abbaspour-Aghdam et al., 17 Sep 2022, Randomized Controlled Trial, placebo-controlled, Iran, peer-reviewed, 16 authors, trial IRCT20200324046851N1.
Contact: ahmadi.m@tbzmed.ac.ir.
Immunomodulatory role of Nanocurcumin in COVID-19 patients with dropped natural killer cells frequency and function
European Journal of Pharmacology, doi:10.1016/j.ejphar.2022.175267
This is a PDF file of an article that has undergone enhancements after acceptance, such as the addition of a cover page and metadata, and formatting for readability, but it is not yet the definitive version of record. This version will undergo additional copyediting, typesetting and review before it is published in its final form, but we are providing this version to give early visibility of the article. Please note that, during the production process, errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
helpful choice in modulating immune system dysregulated responses like increased NK cells in COVID-19 patients.
Abbreviations Severe acute respiratory coronavirus (SARS-CoV); 2019 novel coronavirus (2019-nCoV) ; Chronic mild stress (CMS); Phytohaemagglutinin (PHA); Peripheral blood mononuclear cells (PBMCs); Nuclear factor kappa-light-chain-enhancer of activated B cells (NF-κB); Natural killer (NK); Tumour necrosis factor α (TNFα); Regulatory cells (Tregs) .
Conflict of Interests Statement The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be considered as a potential conflict of interest.
References
Aggarwal, Kumar, Bharti, Anticancer potential of curcumin: preclinical and clinical studies, Anticancer research
Ahmadi, Abdolmohamadi-Vahid, Ghaebi, Dolati, Abbaspour-Aghdam et al., Sirolimus as a new drug to treat RIF patients with elevated Th17/Treg ratio: A double-blind, phase II randomized clinical trial, International immunopharmacology
Ahmadi, Hajialilo, Dolati, Eghbal-Fard, Heydarlou et al., The effects of nanocurcumin on Treg cell responses and treatment of ankylosing spondylitis patients: A randomized, double-blind, placebocontrolled clinical trial, Journal of cellular biochemistry
Ahmadi, Yousefi, Disturbed Th17/Treg balance, cytokines, and miRNAs in peripheral blood of patients with Behcet's disease
Björkström, Ljunggren, Michaëlsson, Emerging insights into natural killer cells in human peripheral tissues, Nature reviews. Immunology
Björkström, Ponzetta, Natural killer cells and unconventional T cells in COVID-19, Current opinion in virology
Bosmann, Ward, Role of C3, C5 and anaphylatoxin receptors in acute lung injury and in sepsis, Advances in experimental medicine and biology
Carvelli, Demaria, Vély, Batista, Chouaki Benmansour et al., Association of COVID-19 inflammation with activation of the C5a-C5aR1 axis
Coperchini, Chiovato, Croce, Magri, Rotondi, The cytokine storm in COVID-19: An overview of the involvement of the chemokine/chemokine-receptor system, Cytokine & Growth Factor Reviews
Dolati, Aghebati-Maleki, Ahmadi, Marofi, Babaloo et al., Nanocurcumin restores aberrant miRNA expression profile in multiple sclerosis, randomized, double-blind, placebo-controlled trial, Journal of cellular physiology
Dolati, Ahmadi, Aghebti-Maleki, Nikmaram, Marofi et al., Nanocurcumin is a potential novel therapy for multiple sclerosis by influencing inflammatory mediators, Pharmacological Reports
Eeden, Khan, Osman, Cohen Tervaert, Natural killer cell dysfunction and its role in COVID-19, International Journal of Molecular Sciences
Eghbal-Fard, Yousefi, The imbalance of Th17/Treg axis involved in the pathogenesis of preeclampsia
Esmaeilzadeh, Jafari, Tahmasebi, Elahi, Khosh, Immune-Based Therapy for COVID-19, Advances in experimental medicine and biology
Esmaeilzadeh, Rostami, Yeganeh, Tahmasebi, Recent advances in antibody-based immunotherapy strategies for COVID-19
Fathi, Rezaei, Lymphopenia in COVID-19: Therapeutic opportunities, Cell biology international
Fiala, Halder, Almasi, Sagong, Leung et al., Curcuminoids and ω-3 fatty acids with anti-oxidants potentiate cytotoxicity of natural killer cells against pancreatic ductal adenocarcinoma cells and inhibit interferon γ production, Frontiers in physiology
Flora, Gupta, Tiwari, Nanocurcumin: a promising therapeutic advancement over native curcumin, Critical reviews in therapeutic drug carrier systems
Fusakio, Mohammed, Laumonnier, Hoebe, Köhl et al., C5a regulates NKT and NK cell functions in sepsis, Journal of immunology
Gao, Hu, Zhang, Li, Zhu et al., Highly pathogenic coronavirus N protein aggravates lung injury by MASP-2-mediated complement overactivation, MedRxiv
Ghaebi, Tahmasebi, Jozghorbani, Sadeghi, Thangavelu et al., Risk factors for adverse outcomes of COVID-19 patients: Possible basis for diverse responses to the novel coronavirus SARS-CoV-2, Life sciences
Ghosh, Banerjee, Sil, The beneficial role of curcumin on inflammation, diabetes and neurodegenerative disease: A recent update, Food and Chemical Toxicology
Giamarellos-Bourboulis, Netea, Rovina, Akinosoglou, Antoniadou et al., The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak-an update on the status, Military Medical Research
Gupta, Patchva, Aggarwal, Therapeutic roles of curcumin: lessons learned from clinical trials, The AAPS journal
Hajialilo, Dolati, Abdolmohammadi-Vahid, Ahmadi, Kamrani et al., Nanocurcumin: A novel strategy in treating ankylosing spondylitis by modulating Th17 cells frequency and function, Journal of cellular biochemistry
Hatamipour, Sahebkar, Alavizadeh, Dorri, Jaafari, Novel nanomicelle formulation to enhance bioavailability and stability of curcuminoids, Iranian journal of basic medical sciences
Izadi, Tahmasebi, Pustokhina, Yumashev, Lakzaei et al., Changes in Th17 cells frequency and function after ozone therapy used to treat multiple sclerosis patients, Frontiers in pharmacology
Khan, Ahmad, Chattopadhyay, Komal, Chaudhary et al., The therapeutic and preventive efficacy of curcumin and its derivatives in esophageal cancer, Asian Pacific Journal of Cancer Prevention: APJCP
Koutsakos, Rowntree, Hensen, Chua, Van De Sandt et al., Integrated immune dynamics define correlates of COVID-19 severity and antibody responses, Cell reports. Medicine
Lee, Cho, Improved anti-cancer effect of curcumin on breast cancer cells by increasing the activity of natural killer cells, Journal of microbiology and biotechnology
Lestari, Indrayanto, Curcumin. Profiles of drug substances, excipients and related methodology
Li, Huang, Wang, Ingbar, Wang, Acute lung injury in patients with COVID-19 infection, Clinical and Translational Medicine
Li, Huang, Wang, Ingbar, Wang, Acute lung injury in patients with COVID-19 infection, Clinical and translational medicine
Lin, Gonzalez, Cunningham-Rundles, Dorante, Marshall et al., CD56+ dim and CD56+ bright cell activation and apoptosis in hepatitis C virus infection, Clinical & Experimental Immunology
Ma, Shayeganpour, Brocks, Lavasanifar, Samuel, High-performance liquid chromatography analysis of curcumin in rat plasma: application to pharmacokinetics of polymeric micellar formulation of curcumin, Biomedical chromatography : BMC
Market, Angka, Martel, Bastin, Olanubi et al., Flattening the COVID-19 curve with natural killer cell based immunotherapies, Frontiers in immunology
Marofi, Azizi, Motavalli, Vahedi, Nasimi et al., COVID-19: Our Current Knowledge of Epidemiology, Pathology, Therapeutic Approaches, and Diagnostic Methods, Anti-cancer agents in medicinal chemistry
Mastellos, Pires Da Silva, Fonseca, Fonseca, Auxiliadora-Martins et al., Complement C3 vs C5 inhibition in severe COVID-19: Early clinical findings reveal differential biological efficacy, Clinical immunology
Mohanty, Das, Sahoo, Sustained wound healing activity of curcumin loaded oleic acid based polymeric bandage in a rat model, Molecular pharmaceutics
Muller, Keck, Challenges and solutions for the delivery of biotech drugs--a review of drug nanocrystal technology and lipid nanoparticles, Journal of biotechnology
Mythri, Jagatha, Pradhan, Andersen, Bharath, Mitochondrial complex I inhibition in Parkinson's disease: how can curcumin protect mitochondria?, Antioxidants & redox signaling
Osman, Faridi, Sligl, Shabani-Rad, Dharmani-Khan et al., Impaired natural killer cell counts and cytolytic activity in patients with severe COVID-19, Blood advances
Pasrija, Naime, The deregulated immune reaction and cytokines release storm (CRS) in COVID-19 disease, International immunopharmacology
Rahimi, Mohammadpour, Dastani, Jaafari, Abnous et al., The effect of nano-curcumin on HbA1c, fasting blood glucose, and lipid profile in diabetic subjects: a randomized clinical trial
Sadeghi, Tahmasebi, Mahmood, Kuznetsova, Valizadeh et al., Th17 and Treg cells function in SARS-CoV2 patients compared with healthy controls, Journal of cellular physiology
Taghiloo, Aliyali, Abedi, Mehravaran, Sharifpour et al., Apoptosis and immunophenotyping of peripheral blood lymphocytes in Iranian COVID-19 patients: clinical and laboratory characteristics, Journal of medical virology
Tahmasebi, El-Esawi, Mahmoud, Timoshin, Valizadeh et al., Immunomodulatory effects of Nanocurcumin on Th17 cell responses in mild and severe COVID-19 patients, Journal of cellular physiology
Tahmasebi, Khosh, Esmaeilzadeh, The outlook for diagnostic purposes of the 2019-novel coronavirus disease, Journal of Cellular Physiology
Tahmasebi, Qasim, Krivenkova, Zekiy, Thangavelu et al., The effects of Oxygen-Ozone therapy on regulatory Tcell responses in multiple sclerosis patients
Trivedi, Mondal, Gangwar, Jana, Immunomodulatory potential of nanocurcuminbased formulation, Inflammopharmacology
Valizadeh, Abdolmohammadi-Vahid, Danshina, Gencer, Ammari et al., Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients, International immunopharmacology
Valizadeh, Abdolmohammadi-Vahid, Danshina, Ziya Gencer, Ammari et al., Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients, International immunopharmacology
Vietzen, Zoufaly, Traugott, Aberle, Aberle et al., Deletion of the NKG2C receptor encoding KLRC2 gene and HLA-E variants are risk factors for severe COVID-19, International journal of antimicrobial agents
Wilk, Rustagi, A single-cell atlas of the peripheral immune response in patients with severe COVID-19
Wu, Wu, Liu, Yang, The SARS-CoV-2 outbreak: what we know, International Journal of Infectious Diseases
Yadav, Mishra, Singh, Mehrotra, Singh, Immunomodulatory effects of curcumin, Immunopharmacology and immunotoxicology
Yan, Gao, New insights for C5a and C5a receptors in sepsis, Frontiers in immunology
Yan, Shin, Pang, Meng, Lai, The First 75 Days of Novel Coronavirus (SARS-CoV-2) Outbreak: Recent Advances
Zheng, Gao, Wang, Song, Liu et al., Functional exhaustion of antiviral lymphocytes in COVID-19 patients, Cellular & molecular immunology
Zheng, Gao, Wang, Song, Liu et al., J o u r n a l P r e -p r o o f Highlights -In Coronavirus disease 2019 (COVID-19), Hyper inflammatory state is derived from overactivation of the inflammatory cells and factors. -Nanocurcumin is an herbal-based agent with anti-inflammatory, antiviral and immunomodulatory properties. -Nanocurcumin could significantly increase the frequency and cytotoxicity of NK cell in COVID-19 patients. -Nanocurcumin could remarkably enhance the expression levels of activating receptors of NK cells in COVID-19 patients. -Nanocurcumin could notably reduce the expression levels of inhibitory receptors of NK cells in COVID-19 patients. -Nanocurcumin could meaningfully decline the serum levels of IL-1, IL-6, TNF-, and C5a in COVID-19 patients, Cell Mol Immunol
Zheng, SARS-CoV-2: an Emerging Coronavirus that Causes a Global Threat, International journal of biological sciences
Ćurković, Košec, Ćurković, Math and aftermath of COVID-19 pandemic and its interrelationship from the resilience perspective, The Journal of Infection
DOI record:
{
"DOI": "10.1016/j.ejphar.2022.175267",
"ISSN": [
"0014-2999"
],
"URL": "http://dx.doi.org/10.1016/j.ejphar.2022.175267",
"alternative-id": [
"S0014299922005283"
],
"article-number": "175267",
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "Immunomodulatory role of Nanocurcumin in COVID-19 patients with dropped natural killer cells frequency and function"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "European Journal of Pharmacology"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.ejphar.2022.175267"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2022 Published by Elsevier B.V."
}
],
"author": [
{
"affiliation": [],
"family": "Abbaspour-Aghdam",
"given": "Sanaz",
"sequence": "first"
},
{
"affiliation": [],
"family": "Hazrati",
"given": "Ali",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Abdolmohammadi-Vahid",
"given": "Samaneh",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Tahmasebi",
"given": "Safa",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mohseni",
"given": "Jafar",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Valizadeh",
"given": "Hamed",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Nadiri",
"given": "Mehdi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Mikaeili",
"given": "Haleh",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sadeghi",
"given": "Armin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Yousefi",
"given": "Mehdi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Roshangar",
"given": "Leila",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Nikzad",
"given": "Behzad",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jadidi-Niaragh",
"given": "Farhad",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kafil",
"given": "Hossein Samadi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Malekpour",
"given": "Kosar",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ahmadi",
"given": "Majid",
"sequence": "additional"
}
],
"container-title": "European Journal of Pharmacology",
"container-title-short": "European Journal of Pharmacology",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2022,
9,
17
]
],
"date-time": "2022-09-17T12:30:13Z",
"timestamp": 1663417813000
},
"deposited": {
"date-parts": [
[
2022,
9,
17
]
],
"date-time": "2022-09-17T12:31:00Z",
"timestamp": 1663417860000
},
"indexed": {
"date-parts": [
[
2022,
9,
18
]
],
"date-time": "2022-09-18T05:22:38Z",
"timestamp": 1663478558909
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2022,
9
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
9,
1
]
],
"date-time": "2022-09-01T00:00:00Z",
"timestamp": 1661990400000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S0014299922005283?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S0014299922005283?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"page": "175267",
"prefix": "10.1016",
"published": {
"date-parts": [
[
2022,
9
]
]
},
"published-print": {
"date-parts": [
[
2022,
9
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"article-title": "Anticancer potential of curcumin: preclinical and clinical studies",
"author": "Aggarwal",
"first-page": "363",
"journal-title": "Anticancer Res.",
"key": "10.1016/j.ejphar.2022.175267_bib1",
"volume": "23",
"year": "2003"
},
{
"DOI": "10.1016/j.intimp.2019.105730",
"article-title": "Sirolimus as a new drug to treat RIF patients with elevated Th17/Treg ratio: a double-blind, phase II randomized clinical trial",
"author": "Ahmadi",
"doi-asserted-by": "crossref",
"journal-title": "Int. Immunopharm.",
"key": "10.1016/j.ejphar.2022.175267_bib2",
"volume": "74",
"year": "2019"
},
{
"DOI": "10.1002/jcb.28901",
"article-title": "The effects of nanocurcumin on Treg cell responses and treatment of ankylosing spondylitis patients: a randomized, double‐blind, placebo‐controlled clinical trial",
"author": "Ahmadi",
"doi-asserted-by": "crossref",
"first-page": "103",
"journal-title": "J. Cell. Biochem.",
"key": "10.1016/j.ejphar.2022.175267_bib3",
"volume": "121",
"year": "2020"
},
{
"DOI": "10.1002/jcp.27207",
"article-title": "Disturbed Th17/Treg balance, cytokines, and miRNAs in peripheral blood of patients with Behcet's disease",
"author": "Ahmadi",
"doi-asserted-by": "crossref",
"first-page": "3985",
"journal-title": "J. Cell. Physiol.",
"key": "10.1016/j.ejphar.2022.175267_bib4",
"volume": "234",
"year": "2019"
},
{
"DOI": "10.1038/nri.2016.34",
"article-title": "Emerging insights into natural killer cells in human peripheral tissues",
"author": "Björkström",
"doi-asserted-by": "crossref",
"first-page": "310",
"journal-title": "Nat. Rev. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib5",
"volume": "16",
"year": "2016"
},
{
"DOI": "10.1016/j.coviro.2021.06.005",
"article-title": "Natural killer cells and unconventional T cells in COVID-19",
"author": "Björkström",
"doi-asserted-by": "crossref",
"first-page": "176",
"journal-title": "Curr. Opin. Virol.",
"key": "10.1016/j.ejphar.2022.175267_bib6",
"volume": "49",
"year": "2021"
},
{
"DOI": "10.1007/978-1-4614-0106-3_9",
"article-title": "Role of C3, C5 and anaphylatoxin receptors in acute lung injury and in sepsis",
"author": "Bosmann",
"doi-asserted-by": "crossref",
"first-page": "147",
"journal-title": "Adv. Exp. Med. Biol.",
"key": "10.1016/j.ejphar.2022.175267_bib7",
"volume": "946",
"year": "2012"
},
{
"article-title": "Association of COVID-19 inflammation with activation of the C5a-C5aR1 axis",
"author": "Carvelli",
"first-page": "146",
"journal-title": "Regular and young investigator award abstracts",
"key": "10.1016/j.ejphar.2022.175267_bib8",
"volume": "588",
"year": "2020"
},
{
"DOI": "10.1016/j.cytogfr.2020.05.003",
"article-title": "The cytokine storm in COVID-19: an overview of the involvement of the chemokine/chemokine-receptor system",
"author": "Coperchini",
"doi-asserted-by": "crossref",
"first-page": "25",
"journal-title": "Cytokine Growth Factor Rev.",
"key": "10.1016/j.ejphar.2022.175267_bib9",
"volume": "53",
"year": "2020"
},
{
"DOI": "10.1016/j.jinf.2020.06.020",
"article-title": "Math and aftermath of COVID-19 pandemic and its interrelationship from the resilience perspective",
"author": "Ćurković",
"doi-asserted-by": "crossref",
"journal-title": "J. Infect.",
"key": "10.1016/j.ejphar.2022.175267_bib10",
"year": "2020"
},
{
"DOI": "10.1002/jcp.26301",
"article-title": "Nanocurcumin restores aberrant miRNA expression profile in multiple sclerosis, randomized, double‐blind, placebo‐controlled trial",
"author": "Dolati",
"doi-asserted-by": "crossref",
"first-page": "5222",
"journal-title": "J. Cell. Physiol.",
"key": "10.1016/j.ejphar.2022.175267_bib11",
"volume": "233",
"year": "2018"
},
{
"DOI": "10.1016/j.pharep.2018.05.008",
"article-title": "Nanocurcumin is a potential novel therapy for multiple sclerosis by influencing inflammatory mediators",
"author": "Dolati",
"doi-asserted-by": "crossref",
"first-page": "1158",
"journal-title": "Pharmacol. Rep.",
"key": "10.1016/j.ejphar.2022.175267_bib12",
"volume": "70",
"year": "2018"
},
{
"DOI": "10.1002/jcp.27315",
"article-title": "The imbalance of Th17/Treg axis involved in the pathogenesis of preeclampsia",
"author": "Eghbal-Fard",
"doi-asserted-by": "crossref",
"first-page": "5106",
"journal-title": "J. Cell. Physiol.",
"key": "10.1016/j.ejphar.2022.175267_bib13",
"volume": "234",
"year": "2019"
},
{
"DOI": "10.1007/978-3-030-63761-3_26",
"article-title": "Immune-based therapy for COVID-19",
"author": "Esmaeilzadeh",
"doi-asserted-by": "crossref",
"first-page": "449",
"journal-title": "Adv. Exp. Med. Biol.",
"key": "10.1016/j.ejphar.2022.175267_bib14",
"volume": "1318",
"year": "2021"
},
{
"DOI": "10.1002/jcb.30017",
"article-title": "Recent advances in antibody-based immunotherapy strategies for COVID-19",
"author": "Esmaeilzadeh",
"doi-asserted-by": "crossref",
"journal-title": "J. Cell. Biochem.",
"key": "10.1016/j.ejphar.2022.175267_bib15",
"year": "2021"
},
{
"DOI": "10.1002/cbin.11403",
"article-title": "Lymphopenia in COVID‐19: therapeutic opportunities",
"author": "Fathi",
"doi-asserted-by": "crossref",
"first-page": "1792",
"journal-title": "Cell Biol. Int.",
"key": "10.1016/j.ejphar.2022.175267_bib16",
"volume": "44",
"year": "2020"
},
{
"article-title": "Curcuminoids and ω-3 fatty acids with anti-oxidants potentiate cytotoxicity of natural killer cells against pancreatic ductal adenocarcinoma cells and inhibit interferon γ production",
"author": "Fiala",
"first-page": "129",
"journal-title": "Front. Physiol.",
"key": "10.1016/j.ejphar.2022.175267_bib17",
"volume": "6",
"year": "2015"
},
{
"DOI": "10.1615/CritRevTherDrugCarrierSyst.2013007236",
"article-title": "Nanocurcumin: a promising therapeutic advancement over native curcumin",
"author": "Flora",
"doi-asserted-by": "crossref",
"first-page": "331",
"journal-title": "Crit. Rev. Ther. Drug Carrier Syst.",
"key": "10.1016/j.ejphar.2022.175267_bib18",
"volume": "30",
"year": "2013"
},
{
"DOI": "10.4049/jimmunol.1100338",
"article-title": "C5a regulates NKT and NK cell functions in sepsis",
"author": "Fusakio",
"doi-asserted-by": "crossref",
"first-page": "5805",
"journal-title": "J. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib19",
"volume": "187",
"year": "2011"
},
{
"article-title": "Highly pathogenic coronavirus N protein aggravates lung injury by MASP-2-mediated complement over-activation",
"author": "Gao",
"journal-title": "medRxiv",
"key": "10.1016/j.ejphar.2022.175267_bib20",
"year": "2020"
},
{
"DOI": "10.1016/j.lfs.2021.119503",
"article-title": "Risk factors for adverse outcomes of COVID-19 patients: possible basis for diverse responses to the novel coronavirus SARS-CoV-2",
"author": "Ghaebi",
"doi-asserted-by": "crossref",
"journal-title": "Life Sci.",
"key": "10.1016/j.ejphar.2022.175267_bib21",
"volume": "277",
"year": "2021"
},
{
"DOI": "10.1016/j.fct.2015.05.022",
"article-title": "The beneficial role of curcumin on inflammation, diabetes and neurodegenerative disease: a recent update",
"author": "Ghosh",
"doi-asserted-by": "crossref",
"first-page": "111",
"journal-title": "Food Chem. Toxicol.",
"key": "10.1016/j.ejphar.2022.175267_bib22",
"volume": "83",
"year": "2015"
},
{
"DOI": "10.1016/j.chom.2020.04.009",
"article-title": "Complex immune dysregulation in COVID-19 patients with severe respiratory failure",
"author": "Giamarellos-Bourboulis",
"doi-asserted-by": "crossref",
"first-page": "992",
"journal-title": "Cell Host Microbe",
"key": "10.1016/j.ejphar.2022.175267_bib23",
"volume": "27",
"year": "2020"
},
{
"article-title": "The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak–an update on the status",
"author": "Guo",
"first-page": "1",
"journal-title": "Mil. Med. Res.",
"key": "10.1016/j.ejphar.2022.175267_bib24",
"volume": "7",
"year": "2020"
},
{
"DOI": "10.1208/s12248-012-9432-8",
"article-title": "Therapeutic roles of curcumin: lessons learned from clinical trials",
"author": "Gupta",
"doi-asserted-by": "crossref",
"first-page": "195",
"journal-title": "AAPS J.",
"key": "10.1016/j.ejphar.2022.175267_bib25",
"volume": "15",
"year": "2013"
},
{
"DOI": "10.1002/jcb.28488",
"article-title": "Nanocurcumin: a novel strategy in treating ankylosing spondylitis by modulating Th17 cells frequency and function",
"author": "Hajialilo",
"doi-asserted-by": "crossref",
"first-page": "12027",
"journal-title": "J. Cell. Biochem.",
"key": "10.1016/j.ejphar.2022.175267_bib26",
"volume": "120",
"year": "2019"
},
{
"article-title": "Novel nanomicelle formulation to enhance bioavailability and stability of curcuminoids",
"author": "Hatamipour",
"first-page": "282",
"journal-title": "Iran. J. Basic Med. Sci.",
"key": "10.1016/j.ejphar.2022.175267_bib27",
"volume": "22",
"year": "2019"
},
{
"DOI": "10.1016/j.msard.2020.102466",
"article-title": "Changes in Th17 cells frequency and function after ozone therapy used to treat multiple sclerosis patients",
"author": "Izadi",
"doi-asserted-by": "crossref",
"journal-title": "Mult. Scler. Relat. Disord.",
"key": "10.1016/j.ejphar.2022.175267_bib28",
"volume": "46",
"year": "2020"
},
{
"DOI": "10.3389/fphar.2020.00487",
"article-title": "Nanocurcumin: a promising candidate for therapeutic applications",
"author": "Karthikeyan",
"doi-asserted-by": "crossref",
"first-page": "487",
"journal-title": "Front. Pharmacol.",
"key": "10.1016/j.ejphar.2022.175267_bib29",
"volume": "11",
"year": "2020"
},
{
"author": "Khan",
"key": "10.1016/j.ejphar.2022.175267_bib30",
"series-title": "New Look to Phytomedicine: Advancements in Herbal Products as Novel Drug Leads",
"year": "2018"
},
{
"DOI": "10.31557/APJCP.2019.20.5.1329",
"article-title": "The therapeutic and preventive efficacy of curcumin and its derivatives in esophageal cancer",
"author": "Komal",
"doi-asserted-by": "crossref",
"first-page": "1329",
"journal-title": "Asian Pac. J. Cancer Prev. APJCP",
"key": "10.1016/j.ejphar.2022.175267_bib31",
"volume": "20",
"year": "2019"
},
{
"article-title": "Integrated immune dynamics define correlates of COVID-19 severity and antibody responses. Cell reports",
"author": "Koutsakos",
"journal-title": "Medicine",
"key": "10.1016/j.ejphar.2022.175267_bib32",
"volume": "2",
"year": "2021"
},
{
"DOI": "10.4014/jmb.1801.01074",
"article-title": "Improved anti-cancer effect of curcumin on breast cancer cells by increasing the activity of natural killer cells",
"author": "Lee",
"doi-asserted-by": "crossref",
"first-page": "874",
"journal-title": "J. Microbiol. Biotechnol.",
"key": "10.1016/j.ejphar.2022.175267_bib33",
"volume": "28",
"year": "2018"
},
{
"DOI": "10.1016/B978-0-12-800173-8.00003-9",
"article-title": "Curcumin",
"author": "Lestari",
"doi-asserted-by": "crossref",
"first-page": "113",
"journal-title": "Profiles Drug Subst. Excipients Relat. Methodol.",
"key": "10.1016/j.ejphar.2022.175267_bib34",
"volume": "39",
"year": "2014"
},
{
"DOI": "10.1002/ctm2.16",
"article-title": "Acute lung injury in patients with COVID-19 infection",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "20",
"journal-title": "Clin. Transl. Med.",
"key": "10.1016/j.ejphar.2022.175267_bib35",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1002/ctm2.16",
"article-title": "Acute lung injury in patients with COVID‐19 infection",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "20",
"journal-title": "Clin. Transl. Med.",
"key": "10.1016/j.ejphar.2022.175267_bib36",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1111/j.1365-2249.2004.02523.x",
"article-title": "CD56+ dim and CD56+ bright cell activation and apoptosis in hepatitis C virus infection",
"author": "Lin",
"doi-asserted-by": "crossref",
"first-page": "408",
"journal-title": "Clin. Exp. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib37",
"volume": "137",
"year": "2004"
},
{
"DOI": "10.1002/bmc.795",
"article-title": "High-performance liquid chromatography analysis of curcumin in rat plasma: application to pharmacokinetics of polymeric micellar formulation of curcumin",
"author": "Ma",
"doi-asserted-by": "crossref",
"first-page": "546",
"journal-title": "Biomed. Chromatogr. : BMC (Biomed. Chromatogr.)",
"key": "10.1016/j.ejphar.2022.175267_bib38",
"volume": "21",
"year": "2007"
},
{
"DOI": "10.3389/fimmu.2020.01512",
"article-title": "Flattening the COVID-19 curve with natural killer cell based immunotherapies",
"author": "Market",
"doi-asserted-by": "crossref",
"journal-title": "Front. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib39",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.2174/1871520621666210201101245",
"article-title": "COVID-19: our current knowledge of epidemiology, pathology, therapeutic approaches, and diagnostic methods",
"author": "Marofi",
"doi-asserted-by": "crossref",
"journal-title": "Anti Cancer Agents Med. Chem.",
"key": "10.1016/j.ejphar.2022.175267_bib40",
"year": "2021"
},
{
"DOI": "10.1016/j.clim.2020.108598",
"article-title": "Complement C3 vs C5 inhibition in severe COVID-19: early clinical findings reveal differential biological efficacy",
"author": "Mastellos",
"doi-asserted-by": "crossref",
"journal-title": "Clin. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib41",
"volume": "220",
"year": "2020"
},
{
"author": "Maucourant",
"key": "10.1016/j.ejphar.2022.175267_bib42",
"volume": "vol. 5",
"year": "2020"
},
{
"DOI": "10.1021/mp300075u",
"article-title": "Sustained wound healing activity of curcumin loaded oleic acid based polymeric bandage in a rat model",
"author": "Mohanty",
"doi-asserted-by": "crossref",
"first-page": "2801",
"journal-title": "Mol. Pharm.",
"key": "10.1016/j.ejphar.2022.175267_bib43",
"volume": "9",
"year": "2012"
},
{
"DOI": "10.1016/j.jbiotec.2004.06.007",
"article-title": "Challenges and solutions for the delivery of biotech drugs--a review of drug nanocrystal technology and lipid nanoparticles",
"author": "Muller",
"doi-asserted-by": "crossref",
"first-page": "151",
"journal-title": "J. Biotechnol.",
"key": "10.1016/j.ejphar.2022.175267_bib44",
"volume": "113",
"year": "2004"
},
{
"DOI": "10.1089/ars.2006.1479",
"article-title": "Mitochondrial complex I inhibition in Parkinson's disease: how can curcumin protect mitochondria?",
"author": "Mythri",
"doi-asserted-by": "crossref",
"first-page": "399",
"journal-title": "Antioxidants Redox Signal.",
"key": "10.1016/j.ejphar.2022.175267_bib45",
"volume": "9",
"year": "2007"
},
{
"DOI": "10.1182/bloodadvances.2020002650",
"article-title": "Impaired natural killer cell counts and cytolytic activity in patients with severe COVID-19",
"author": "Osman",
"doi-asserted-by": "crossref",
"first-page": "5035",
"journal-title": "Blood Adv.",
"key": "10.1016/j.ejphar.2022.175267_bib46",
"volume": "4",
"year": "2020"
},
{
"DOI": "10.1016/j.intimp.2020.107225",
"article-title": "The deregulated immune reaction and cytokines release storm (CRS) in COVID-19 disease",
"author": "Pasrija",
"doi-asserted-by": "crossref",
"journal-title": "Int. Immunopharm.",
"key": "10.1016/j.ejphar.2022.175267_bib47",
"volume": "90",
"year": "2021"
},
{
"article-title": "The effect of nano-curcumin on HbA1c, fasting blood glucose, and lipid profile in diabetic subjects: a randomized clinical trial",
"author": "Rahimi",
"first-page": "567",
"journal-title": "Avicenna J. Phytomed.",
"key": "10.1016/j.ejphar.2022.175267_bib48",
"volume": "6",
"year": "2016"
},
{
"DOI": "10.1038/s41577-020-0320-7",
"article-title": "Complement as a target in COVID-19?",
"author": "Risitano",
"doi-asserted-by": "crossref",
"first-page": "343",
"journal-title": "Nat. Rev. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib49",
"volume": "20",
"year": "2020"
},
{
"DOI": "10.1002/jcp.30047",
"article-title": "Th17 and Treg cells function in SARS‐CoV2 patients compared with healthy controls",
"author": "Sadeghi",
"doi-asserted-by": "crossref",
"first-page": "2829",
"journal-title": "J. Cell. Physiol.",
"key": "10.1016/j.ejphar.2022.175267_bib50",
"volume": "236",
"year": "2021"
},
{
"DOI": "10.1002/jmv.26505",
"article-title": "Apoptosis and immunophenotyping of peripheral blood lymphocytes in Iranian COVID‐19 patients: clinical and laboratory characteristics",
"author": "Taghiloo",
"doi-asserted-by": "crossref",
"first-page": "1589",
"journal-title": "J. Med. Virol.",
"key": "10.1016/j.ejphar.2022.175267_bib51",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.1002/jcp.30233",
"article-title": "Immunomodulatory effects of Nanocurcumin on Th17 cell responses in mild and severe COVID‐19 patients",
"author": "Tahmasebi",
"doi-asserted-by": "crossref",
"first-page": "5325",
"issue": "7",
"journal-title": "J. Cell. Physiol.",
"key": "10.1016/j.ejphar.2022.175267_bib52",
"volume": "236",
"year": "2021"
},
{
"DOI": "10.1002/jcp.29804",
"article-title": "The outlook for diagnostic purposes of the 2019-novel coronavirus disease",
"author": "Tahmasebi",
"doi-asserted-by": "crossref",
"first-page": "9211",
"journal-title": "J. Cell. Physiol.",
"key": "10.1016/j.ejphar.2022.175267_bib53",
"volume": "235",
"year": "2020"
},
{
"DOI": "10.1002/cbin.11589",
"article-title": "The effects of Oxygen‐Ozone therapy on regulatory T‐cell responses in multiple sclerosis patients",
"author": "Tahmasebi",
"doi-asserted-by": "crossref",
"journal-title": "Cell Biol. Int.",
"key": "10.1016/j.ejphar.2022.175267_bib54",
"year": "2021"
},
{
"author": "Tahmasebi",
"key": "10.1016/j.ejphar.2022.175267_bib55",
"series-title": "Nanocurcumin Improves Treg Cell Responses in Patients with Mild and Severe SARS-CoV2",
"year": "2021"
},
{
"DOI": "10.1007/s10787-017-0395-3",
"article-title": "Immunomodulatory potential of nanocurcumin-based formulation",
"author": "Trivedi",
"doi-asserted-by": "crossref",
"first-page": "609",
"journal-title": "Inflammopharmacology",
"key": "10.1016/j.ejphar.2022.175267_bib56",
"volume": "25",
"year": "2017"
},
{
"DOI": "10.1016/j.intimp.2020.107088",
"article-title": "Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients",
"author": "Valizadeh",
"doi-asserted-by": "crossref",
"journal-title": "Int. Immunopharm.",
"key": "10.1016/j.ejphar.2022.175267_bib57",
"volume": "89",
"year": "2020"
},
{
"DOI": "10.1016/j.intimp.2020.107088",
"article-title": "Nano-curcumin therapy, a promising method in modulating inflammatory cytokines in COVID-19 patients",
"author": "Valizadeh",
"doi-asserted-by": "crossref",
"journal-title": "Int. Immunopharm.",
"key": "10.1016/j.ejphar.2022.175267_bib58",
"volume": "89",
"year": "2020"
},
{
"DOI": "10.3390/ijms21176351",
"article-title": "Natural killer cell dysfunction and its role in COVID-19",
"author": "van Eeden",
"doi-asserted-by": "crossref",
"first-page": "6351",
"journal-title": "Int. J. Mol. Sci.",
"key": "10.1016/j.ejphar.2022.175267_bib59",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1038/s41436-020-01077-7",
"article-title": "Deletion of the NKG2C receptor encoding KLRC2 gene and HLA-E variants are risk factors for severe COVID-19",
"author": "Vietzen",
"doi-asserted-by": "crossref",
"first-page": "963",
"journal-title": "Genet. Med.",
"key": "10.1016/j.ejphar.2022.175267_bib60",
"volume": "23",
"year": "2021"
},
{
"DOI": "10.1016/j.ijantimicag.2020.105948",
"article-title": "Review of the 2019 novel coronavirus (SARS-CoV-2) based on current evidence",
"author": "Wang",
"doi-asserted-by": "crossref",
"journal-title": "Int. J. Antimicrob. Agents",
"key": "10.1016/j.ejphar.2022.175267_bib61",
"volume": "55",
"year": "2020"
},
{
"author": "Wilk",
"first-page": "1070",
"journal-title": "A single-cell atlas of the peripheral immune response in patients with severe COVID-19",
"key": "10.1016/j.ejphar.2022.175267_bib62",
"volume": "26",
"year": "2020"
},
{
"DOI": "10.1016/j.ijid.2020.03.004",
"article-title": "The SARS-CoV-2 outbreak: what we know",
"author": "Wu",
"doi-asserted-by": "crossref",
"first-page": "44",
"journal-title": "Int. J. Infect. Dis.",
"key": "10.1016/j.ejphar.2022.175267_bib63",
"volume": "94",
"year": "2020"
},
{
"DOI": "10.1080/08923970500242244",
"article-title": "Immunomodulatory effects of curcumin",
"author": "Yadav",
"doi-asserted-by": "crossref",
"first-page": "485",
"journal-title": "Immunopharmacol. Immunotoxicol.",
"key": "10.1016/j.ejphar.2022.175267_bib64",
"volume": "27",
"year": "2005"
},
{
"DOI": "10.3389/fimmu.2012.00368",
"article-title": "New insights for C5a and C5a receptors in sepsis",
"author": "Yan",
"doi-asserted-by": "crossref",
"first-page": "368",
"journal-title": "Front. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib65",
"volume": "3",
"year": "2012"
},
{
"DOI": "10.3390/ijerph17072323",
"article-title": "The first 75 Days of novel coronavirus (SARS-CoV-2) outbreak: recent advances, prevention, and treatment",
"author": "Yan",
"doi-asserted-by": "crossref",
"journal-title": "Int. J. Environ. Res. Publ. Health",
"key": "10.1016/j.ejphar.2022.175267_bib66",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.7150/ijbs.45053",
"article-title": "SARS-CoV-2: an emerging coronavirus that causes a global threat",
"author": "Zheng",
"doi-asserted-by": "crossref",
"first-page": "1678",
"journal-title": "Int. J. Biol. Sci.",
"key": "10.1016/j.ejphar.2022.175267_bib67",
"volume": "16",
"year": "2020"
},
{
"DOI": "10.1038/s41423-020-0402-2",
"article-title": "Functional exhaustion of antiviral lymphocytes in COVID-19 patients",
"author": "Zheng",
"doi-asserted-by": "crossref",
"first-page": "533",
"journal-title": "Cell. Mol. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib68",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1038/s41423-020-0402-2",
"article-title": "Functional exhaustion of antiviral lymphocytes in COVID-19 patients",
"author": "Zheng",
"doi-asserted-by": "crossref",
"first-page": "533",
"journal-title": "Cell. Mol. Immunol.",
"key": "10.1016/j.ejphar.2022.175267_bib69",
"volume": "17",
"year": "2020"
}
],
"reference-count": 69,
"references-count": 69,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S0014299922005283"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Pharmacology"
],
"subtitle": [],
"title": "Immunomodulatory role of Nanocurcumin in COVID-19 patients with dropped natural killer cells frequency and function",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy"
}
