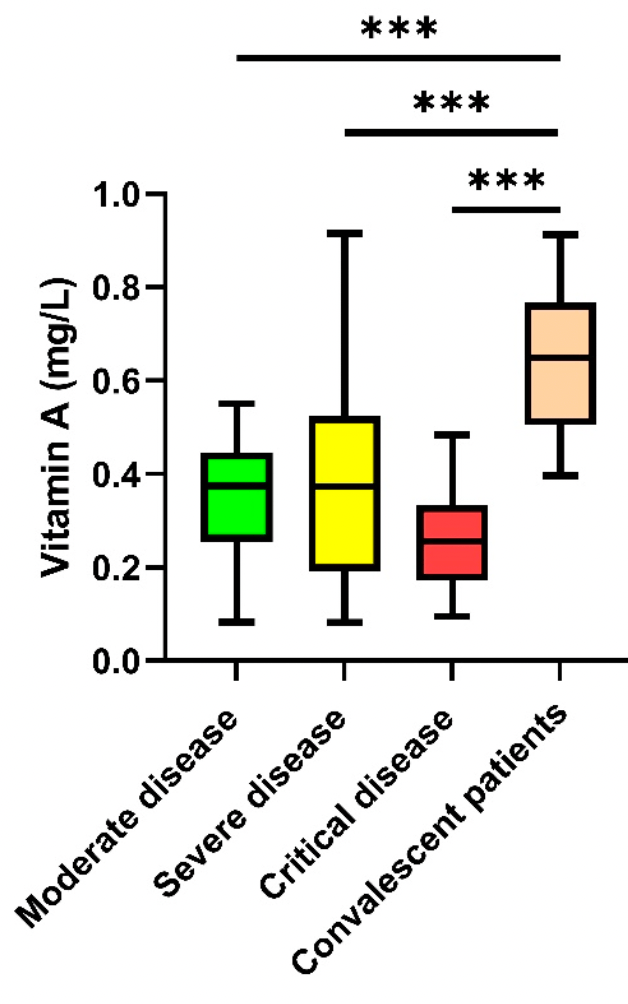
Significantly Reduced Retinol Binding Protein 4 (RBP4) Levels in Critically Ill COVID-19 Patients
et al., Nutrients, doi:10.3390/nu14102007, May 2022
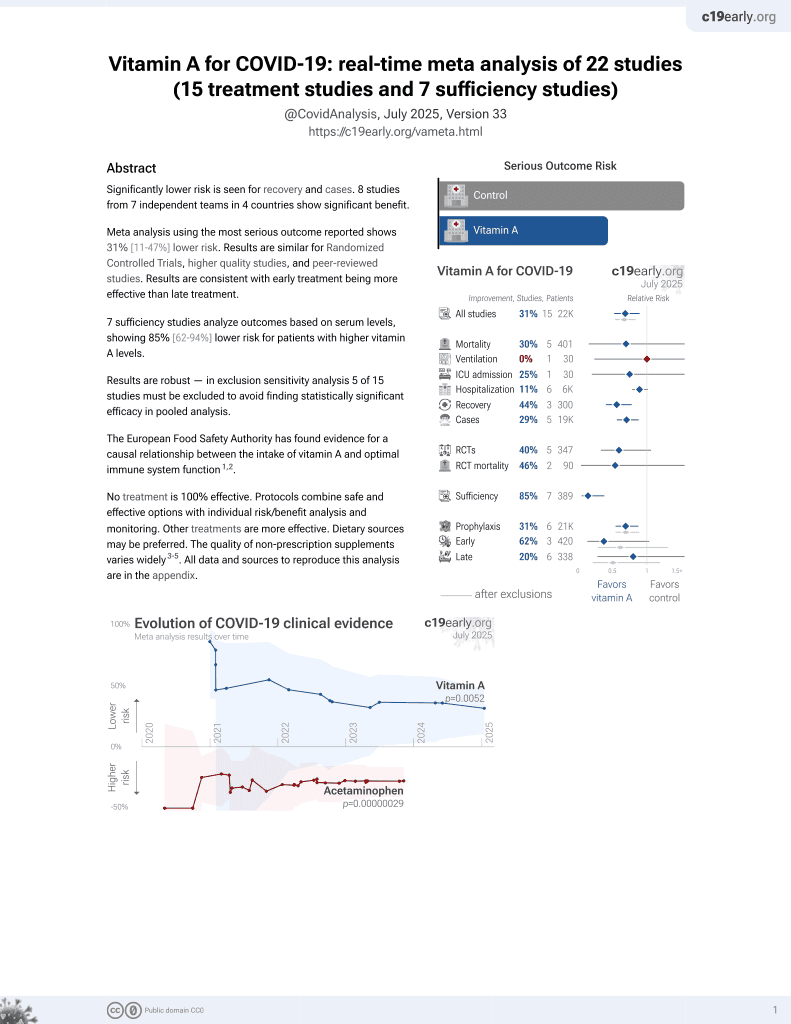
Vitamin A for COVID-19
49th treatment shown to reduce risk in
May 2023, now with p = 0.004 from 14 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
Prospective study of 59 hospitalized COVID-19 patients and 20 matched convalescent control patients in Germany, showing significantly lower vitamin A levels in COVID-19 patients.
Vollenberg et al., 10 May 2022, prospective, Germany, peer-reviewed, 4 authors.
Contact: richard.vollenberg@ukmuenster.de (corresponding author), phil-robin.tepasse@ukmuenster.de, anna.huesing-kabar@ukmuenster.de, manfred.fobker@ukmuenster.de.
Significantly Reduced Retinol Binding Protein 4 (RBP4) Levels in Critically Ill COVID-19 Patients
Nutrients, doi:10.3390/nu14102007
The SARS-CoV-2 virus is the causative agent of the COVID-19 pandemic. The disease causes respiratory failure in some individuals accompanied by marked hyperinflammation. Vitamin A (syn. retinol) can exist in the body in the storage form as retinyl ester, or in the transcriptionally active form as retinoic acid. The main function of retinol binding protein 4 (RBP4), synthesized in the liver, is to transport hydrophobic vitamin A to various tissues. Vitamin A has an important role in the innate and acquired immune system. In particular, it is involved in the repair of lung tissue after infections. In viral respiratory diseases such as influenza pneumonia, vitamin A supplementation has been shown to reduce mortality in animal models. In critically ill COVID-19 patients, a significant decrease in plasma vitamin A levels and an association with increased mortality have been observed. However, there is no evidence on RBP4 in relation to COVID-19. This prospective, multicenter, observational, crosssectional study examined RBP4 (enzyme-linked immunosorbent assay) and vitamin A plasma levels (high-performance liquid chromatography) in COVID-19 patients, including 59 hospitalized patients. Of these, 19 developed critical illness (ARDS/ECMO), 20 developed severe illness (oxygenation disorder), and 20 developed moderate illness (no oxygenation disorder). Twenty age-matched convalescent patients following SARS-CoV-2 infection, were used as a control group. Reduced RBP4 plasma levels significantly correlated with impaired liver function and elevated inflammatory markers (CRP, lymphocytopenia). RBP4 levels were decreased in hospitalized patients with critical illness compared to nonpatients (p < 0.01). In comparison, significantly lower vitamin A levels were detected in hospitalized patients regardless of disease severity. Overall, we conclude that RBP4 plasma levels are significantly reduced in critically ill COVID-19 patients during acute inflammation, and vitamin A levels are significantly reduced in patients with moderate/severe/critical illness during the acute phase of illness.
Informed Consent Statement: Informed consent was obtained from all subjects involved in the study.
Data Availability Statement: Data cannot be made public as personal patient data are included.
Conflicts of Interest: The authors declare no conflict of interest.
References
Aklamati, Mulenga, Dueker, Buchholz, Peerson et al., Accelerator mass spectrometry can be used to assess vitamin A metabolism quantitatively in boys in a community setting, J. Nutr, doi:10.3945/jn.110.125500
Aksoy, Karadag, Wollina, Angiotensin II receptors: Impact for COVID-19 severity, Dermatol. Ther
Bajzová, Kováčiková, Vítková, Klimčáková, Polák et al., Retinol-binding protein 4 expression in visceral and subcutaneous fat in human obesity, Physiol. Res, doi:10.33549/physiolres.931379
Blaner, Brun, Calderon, Golczak, Retinol-binding protein 2 (RBP2): Biology and pathobiology, Crit. Rev. Biochem. Mol. Biol, doi:10.1080/10409238.2020.1768207
Blaner, Li, Brun, Yuen, Lee et al., Vitamin A Absorption, Storage and Mobilization, Subcell. Biochem, doi:10.1007/978-94-024-0945-1_4
Blaner, Vitamin A signaling and homeostasis in obesity, diabetes, and metabolic disorders, Pharmacol. Ther, doi:10.1016/j.pharmthera.2019.01.006
Broch, Vendrell, Ricart, Richart, Fernández-Real, Circulating retinol-binding protein-4, insulin sensitivity, insulin secretion, and insulin disposition index in obese and nonobese subjects, Diabetes Care, doi:10.2337/dc06-2034
Chen, Xiao, Hu, Ge, Tian et al., SARS-CoV-2 Nucleocapsid Protein Interacts with RIG-I and Represses RIG-Mediated IFN-β Production, Viruses, doi:10.3390/v13010047
Cho, Youn, Lee, Lee, Min et al., Plasma retinol-binding protein-4 concentrations are elevated in human subjects with impaired glucose tolerance and type 2 diabetes, Diabetes Care, doi:10.2337/dc06-0360
Cooper, Hepatic clearance of plasma chylomicron remnants, Semin. Liver Dis, doi:10.1055/s-2008-1040408
Cummings, Baldwin, Abrams, Jacobson, Meyer et al., Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: A prospective cohort study, Lancet, doi:10.1016/S0140-6736(20)31189-2
Den Hollander, Mcgee, Ziviello, Banfi, Dryja et al., A homozygous missense mutation in the IRBP gene (RBP3) associated with autosomal recessive retinitis pigmentosa, Investig. Ophthalmol. Vis. Sci, doi:10.1167/iovs.08-2497
Du, Yang, Liu, Liu, COVID-19 and liver dysfunction: Epidemiology, association and potential mechanisms, Clin. Res. Hepatol. Gastroenterol, doi:10.1016/j.clinre.2021.101793
Erikstrup, Mortensen, Nielsen, Fischer, Plomgaard et al., RBP-to-retinol ratio, but not total RBP, is elevated in patients with type 2 diabetes, Diabetes Obes. Metab, doi:10.1111/j.1463-1326.2008.00901.x
Fang, Karakiulakis, Roth, Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection?, Lancet Respir. Med, doi:10.1016/S2213-2600(20)30116-8
Flach, Basten, Schreiner, Dietmann, Greco et al., Retinol binding protein 1 affects Xenopus anterior neural development via all-trans retinoic acid signaling, Dev. Dyn
Frey, Nagl, Henze, Raila, Schlosser et al., Isoforms of retinol binding protein 4 (RBP4) are increased in chronic diseases of the kidney but not of the liver, Lipids Health Dis
Frieman, Yount, Heise, Kopecky-Bromberg, Palese et al., Severe acute respiratory syndrome coronavirus ORF6 antagonizes STAT1 function by sequestering nuclear import factors on the rough endoplasmic reticulum/Golgi membrane, J. Virol, doi:10.1128/JVI.01012-07
Fu, Gaelings, Jalovaara, Kakkola, Kinnunen et al., Protein profiling of nasopharyngeal aspirates of hospitalized and outpatients revealed cytokines associated with severe influenza A(H1N1)pdm09 virus infections: A pilot study, Cytokine, doi:10.1016/j.cyto.2016.07.003
Gagliardi, Tieri, Ortona, Ruggieri, ACE2 expression and sex disparity in COVID-19, Cell Death Discov, doi:10.1038/s41420-020-0276-1
Gieng, Green, Green, Rosales, Model-based compartmental analysis indicates a reduced mobilization of hepatic vitamin A during inflammation in rats, J. Lipid Res, doi:10.1194/jlr.M600528-JLR200
Gudas, Emerging roles for retinoids in regeneration and differentiation in normal and disease states, Biochim. Biophys. Acta, doi:10.1016/j.bbalip.2011.08.002
Hamming, Cooper, Haagmans, Hooper, Korstanje et al., The emerging role of ACE2 in physiology and disease, J. Pathol, doi:10.1002/path.2162
Hoffmann, Begon, Lafon, Duprey, Influence of glenohumeral joint muscle insertion on moment arms using a finite element model, Comput. Methods Biomech. Biomed. Eng, doi:10.1080/10255842.2020.1789606
Janke, Engeli, Boschmann, Adams, Böhnke et al., Retinol-binding protein 4 in human obesity, Diabetes, doi:10.2337/db06-0616
Jones, Oshansky, Bajracharya, Tang, Sun et al., Retinol binding protein and vitamin D associations with serum antibody isotypes, serum influenza virus-specific neutralizing activities and airway cytokine profiles, Clin. Exp. Immunol, doi:10.1111/cei.12718
Kessel, Vollenberg, Masjosthusmann, Hinze, Wittkowski et al., Discrimination of COVID-19 From Inflammation-Induced Cytokine Storm Syndromes Using Disease-Related Blood Biomarkers, Arthritis Rheumatol, doi:10.1002/art.41763
Kotnik, Fischer-Posovszky, Wabitsch, RBP4: A controversial adipokine, Eur. J. Endocrinol, doi:10.1530/EJE-11-0431
Krasinski, Cohn, Russell, Schaefer, Postprandial plasma vitamin A metabolism in humans: A reassessment of the use of plasma retinyl esters as markers for intestinally derived chylomicrons and their remnants, Metabolism
Kuba, Imai, Rao, Gao, Guo et al., A crucial role of angiotensin converting enzyme 2 (ACE2) in SARS coronavirus-induced lung injury, Nat. Med, doi:10.1038/nm1267
Kumar, Kumar, Bedi, Gupta, Kumar et al., Role of vitamins and minerals as immunity boosters in COVID-19, Inflammopharmacology, doi:10.1007/s10787-021-00826-7
Lamers, Haagmans, SARS-CoV-2 pathogenesis, Nat. Rev. Microbiol, doi:10.1038/s41579-022-00713-0
Muenzner, Tuvia, Deutschmann, Witte, Tolkachov et al., Retinol-binding protein 4 and its membrane receptor STRA6 control adipogenesis by regulating cellular retinoid homeostasis and retinoic acid receptor α activity, Mol. Cell. Biol, doi:10.1128/MCB.00221-13
Méry, Epaulard, Borel, Toussaint, Le Gouellec, COVID-19: Underlying Adipokine Storm and Angiotensin 1-7 Umbrella, Front. Immunol, doi:10.3389/fimmu.2020.01714
Nardo, Schneeweiss-Gleixner, Bakail, Dixon, Lax et al., Pathophysiological mechanisms of liver injury in COVID-19, Liver Int, doi:10.1111/liv.14730
Nawijn, Timens, Can ACE2 expression explain SARS-CoV-2 infection of the respiratory epithelia in COVID-19?, Mol. Syst. Biol, doi:10.15252/msb.20209841
O'byrne, Blaner, Retinol and retinyl esters: Biochemistry and physiology, J. Lipid Res, doi:10.1194/jlr.R037648
Olsen, Blomhoff, Retinol, Retinoic Acid, and Retinol-Binding Protein 4 are Differentially Associated with Cardiovascular Disease, Type 2 Diabetes, and Obesity: An Overview of Human Studies, Adv. Nutr, doi:10.1093/advances/nmz131
Porzionato, Emmi, Barbon, Boscolo-Berto, Stecco et al., Sympathetic activation: A potential link between comorbidities and COVID-19, FEBS J, doi:10.1111/febs.15481
Ranieri, Rubenfeld, Thompson, Ferguson, Caldwell et al., Acute respiratory distress syndrome: The Berlin Definition, JAMA, doi:10.1001/jama.2012.5669
Raverdeau, Mills, Modulation of T cell and innate immune responses by retinoic Acid, J. Immunol, doi:10.4049/jimmunol.1303245
Roma, Krini, Hantzi, Sakka, Panayiotou et al., Retinol Binding Protein 4 in children with Inflammatory Bowel Disease: A negative correlation with the disease activity, Hippokratia
Sarohan, Kızıl, ˙inkaya, Mahmud, Akram et al., A novel hypothesis for COVID-19 pathogenesis: Retinol depletion and retinoid signaling disorder, Cell. Signal, doi:10.1016/j.cellsig.2021.110121
Shoemark, Colenso, Toelzer, Gupta, Sessions et al., Molecular Simulations suggest Vitamins, Retinoids and Steroids as Ligands of the Free Fatty Acid Pocket of the SARS-CoV-2 Spike Protein**, Angew. Chem. Int. Ed. Engl, doi:10.1002/anie.202015639
Spiegel, Pichlmair, Martínez-Sobrido, Cros, García-Sastre et al., Inhibition of Beta interferon induction by severe acute respiratory syndrome coronavirus suggests a two-step model for activation of interferon regulatory factor 3, J. Virol, doi:10.1128/JVI.79.4.2079-2086.2005
Steinhoff, Lass, Schupp, Biological Functions of RBP4 and Its Relevance for Human Diseases, Front. Physiol, doi:10.3389/fphys.2021.659977
Stephensen, Lietz, Vitamin A in resistance to and recovery from infection: Relevance to SARS-CoV2, Br. J. Nutr, doi:10.1017/S0007114521000246
Stephensen, Vitamin A, infection, and immune function, Annu. Rev. Nutr, doi:10.1146/annurev.nutr.21.1.167
Tepasse, Hafezi, Lutz, Kühn, Wilms et al., Persisting SARS-CoV-2 viraemia after rituximab therapy: Two cases with fatal outcome and a review of the literature, Br. J. Haematol, doi:10.1111/bjh.16896
Tepasse, Vollenberg, Fobker, Kabar, Schmidt et al., Vitamin A Plasma Levels in COVID-19 Patients: A Prospective Multicenter Study and Hypothesis, Nutrients, doi:10.3390/nu13072173
Timoneda, Rodríguez-Fernández, Zaragozá, Marín, Cabezuelo et al., Vitamin A Deficiency and the Lung, Nutrients, doi:10.3390/nu10091132
Tsutsumi, Okuno, Tannous, Piantedosi, Allan et al., Retinoids and retinoid-binding protein expression in rat adipocytes, J. Biol. Chem
Ulgen, Herder, Kühn, Willenberg, Schott et al., Association of serum levels of retinol-binding protein 4 with male sex but not with insulin resistance in obese patients, Arch. Physiol. Biochem
Vollenberg, Matern, Nowacki, Fuhrmann, Padberg et al., Prone Position in Mechanically Ventilated COVID-19 Patients: A Multicenter Study, J. Clin. Med
Yang, Ye, Zhu, Wang, Deng et al., Middle East respiratory syndrome coronavirus ORF4b protein inhibits type I interferon production through both cytoplasmic and nuclear targets, Sci. Rep, doi:10.1038/srep17554
Yao-Borengasser, Varma, Bodles, Rasouli, Phanavanh et al., Retinol binding protein 4 expression in humans: Relationship to insulin resistance, inflammation, and response to pioglitazone, J. Clin. Endocrinol. Metab, doi:10.1210/jc.2006-0816
Zabetian-Targhi, Mahmoudi, Rezaei, Mahmoudi, Retinol binding protein 4 in relation to diet, inflammation, immunity, and cardiovascular diseases, Adv. Nutr, doi:10.3945/an.115.008292
Zhao, Meng, Kumar, Wu, Huang et al., Lymphopenia is associated with severe coronavirus disease 2019 (COVID-19) infections: A systemic review and meta-analysis, Int. J. Infect. Dis, doi:10.1016/j.ijid.2020.04.086
Zhong, Huang, Yang, Li, Liu et al., Upregulation of angiotensin-converting enzyme 2 by all-trans retinoic acid in spontaneously hypertensive rats, Hypertension, doi:10.1161/01.HYP.0000146400.57221.74
Zhou, Wu, Qin, Yin, Association of all-trans retinoic acid treatment with the renin-angiotensin aldosterone system expression in glomerulosclerosis rats, J. Renin Angiotensin Aldosterone Syst, doi:10.1177/1470320312465220
DOI record:
{
"DOI": "10.3390/nu14102007",
"ISSN": [
"2072-6643"
],
"URL": "http://dx.doi.org/10.3390/nu14102007",
"abstract": "<jats:p>The SARS-CoV-2 virus is the causative agent of the COVID-19 pandemic. The disease causes respiratory failure in some individuals accompanied by marked hyperinflammation. Vitamin A (syn. retinol) can exist in the body in the storage form as retinyl ester, or in the transcriptionally active form as retinoic acid. The main function of retinol binding protein 4 (RBP4), synthesized in the liver, is to transport hydrophobic vitamin A to various tissues. Vitamin A has an important role in the innate and acquired immune system. In particular, it is involved in the repair of lung tissue after infections. In viral respiratory diseases such as influenza pneumonia, vitamin A supplementation has been shown to reduce mortality in animal models. In critically ill COVID-19 patients, a significant decrease in plasma vitamin A levels and an association with increased mortality have been observed. However, there is no evidence on RBP4 in relation to COVID-19. This prospective, multicenter, observational, cross-sectional study examined RBP4 (enzyme-linked immunosorbent assay) and vitamin A plasma levels (high-performance liquid chromatography) in COVID-19 patients, including 59 hospitalized patients. Of these, 19 developed critical illness (ARDS/ECMO), 20 developed severe illness (oxygenation disorder), and 20 developed moderate illness (no oxygenation disorder). Twenty age-matched convalescent patients following SARS-CoV-2 infection, were used as a control group. Reduced RBP4 plasma levels significantly correlated with impaired liver function and elevated inflammatory markers (CRP, lymphocytopenia). RBP4 levels were decreased in hospitalized patients with critical illness compared to nonpatients (p < 0.01). In comparison, significantly lower vitamin A levels were detected in hospitalized patients regardless of disease severity. Overall, we conclude that RBP4 plasma levels are significantly reduced in critically ill COVID-19 patients during acute inflammation, and vitamin A levels are significantly reduced in patients with moderate/severe/critical illness during the acute phase of illness.</jats:p>",
"alternative-id": [
"nu14102007"
],
"author": [
{
"ORCID": "http://orcid.org/0000-0003-3208-7924",
"affiliation": [],
"authenticated-orcid": false,
"family": "Vollenberg",
"given": "Richard",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-2757-4755",
"affiliation": [],
"authenticated-orcid": false,
"family": "Tepasse",
"given": "Phil-Robin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Fobker",
"given": "Manfred",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Hüsing-Kabar",
"given": "Anna",
"sequence": "additional"
}
],
"container-title": "Nutrients",
"container-title-short": "Nutrients",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2022,
5,
11
]
],
"date-time": "2022-05-11T01:52:11Z",
"timestamp": 1652233931000
},
"deposited": {
"date-parts": [
[
2022,
5,
11
]
],
"date-time": "2022-05-11T02:21:10Z",
"timestamp": 1652235670000
},
"indexed": {
"date-parts": [
[
2022,
5,
11
]
],
"date-time": "2022-05-11T19:41:41Z",
"timestamp": 1652298101593
},
"is-referenced-by-count": 0,
"issue": "10",
"issued": {
"date-parts": [
[
2022,
5,
10
]
]
},
"journal-issue": {
"issue": "10",
"published-online": {
"date-parts": [
[
2022,
5
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
5,
10
]
],
"date-time": "2022-05-10T00:00:00Z",
"timestamp": 1652140800000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/2072-6643/14/10/2007/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "2007",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2022,
5,
10
]
]
},
"published-online": {
"date-parts": [
[
2022,
5,
10
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"DOI": "10.1038/s41564-020-0695-z",
"doi-asserted-by": "publisher",
"key": "ref1"
},
{
"DOI": "10.3390/jcm10051046",
"doi-asserted-by": "publisher",
"key": "ref2"
},
{
"DOI": "10.1016/S0140-6736(20)31189-2",
"doi-asserted-by": "publisher",
"key": "ref3"
},
{
"DOI": "10.1111/bjh.16896",
"doi-asserted-by": "publisher",
"key": "ref4"
},
{
"DOI": "10.1038/s41579-022-00713-0",
"doi-asserted-by": "publisher",
"key": "ref5"
},
{
"DOI": "10.1002/art.41763",
"doi-asserted-by": "publisher",
"key": "ref6"
},
{
"DOI": "10.3389/fphys.2021.659977",
"doi-asserted-by": "publisher",
"key": "ref7"
},
{
"DOI": "10.1016/j.bbalip.2011.08.002",
"doi-asserted-by": "publisher",
"key": "ref8"
},
{
"DOI": "10.4049/jimmunol.1303245",
"doi-asserted-by": "publisher",
"key": "ref9"
},
{
"DOI": "10.3390/nu10091132",
"doi-asserted-by": "publisher",
"key": "ref10"
},
{
"DOI": "10.3390/nu13072173",
"doi-asserted-by": "publisher",
"key": "ref11"
},
{
"DOI": "10.1146/annurev.nutr.21.1.167",
"doi-asserted-by": "publisher",
"key": "ref12"
},
{
"DOI": "10.1038/nm1267",
"doi-asserted-by": "publisher",
"key": "ref13"
},
{
"DOI": "10.1017/S0007114521000246",
"doi-asserted-by": "publisher",
"key": "ref14"
},
{
"DOI": "10.1080/10255842.2020.1789606",
"doi-asserted-by": "publisher",
"key": "ref15"
},
{
"DOI": "10.15252/msb.20209841",
"doi-asserted-by": "publisher",
"key": "ref16"
},
{
"DOI": "10.1002/path.2162",
"doi-asserted-by": "publisher",
"key": "ref17"
},
{
"DOI": "10.1038/s41420-020-0276-1",
"doi-asserted-by": "publisher",
"key": "ref18"
},
{
"DOI": "10.1161/01.HYP.0000146400.57221.74",
"doi-asserted-by": "publisher",
"key": "ref19"
},
{
"DOI": "10.1177/1470320312465220",
"doi-asserted-by": "publisher",
"key": "ref20"
},
{
"DOI": "10.1016/S2213-2600(20)30116-8",
"doi-asserted-by": "publisher",
"key": "ref21"
},
{
"DOI": "10.1111/dth.13989",
"doi-asserted-by": "publisher",
"key": "ref22"
},
{
"DOI": "10.3389/fimmu.2020.01714",
"doi-asserted-by": "publisher",
"key": "ref23"
},
{
"DOI": "10.1111/febs.15481",
"doi-asserted-by": "publisher",
"key": "ref24"
},
{
"DOI": "10.1194/jlr.R037648",
"doi-asserted-by": "publisher",
"key": "ref25"
},
{
"DOI": "10.1016/0026-0495(90)90249-c",
"doi-asserted-by": "publisher",
"key": "ref26"
},
{
"DOI": "10.1128/MCB.00221-13",
"doi-asserted-by": "publisher",
"key": "ref27"
},
{
"DOI": "10.1007/978-94-024-0945-1_4",
"doi-asserted-by": "publisher",
"key": "ref28"
},
{
"DOI": "10.1002/dvdy.313",
"doi-asserted-by": "publisher",
"key": "ref29"
},
{
"DOI": "10.1080/10409238.2020.1768207",
"doi-asserted-by": "publisher",
"key": "ref30"
},
{
"DOI": "10.1167/iovs.08-2497",
"doi-asserted-by": "publisher",
"key": "ref31"
},
{
"DOI": "10.1093/advances/nmz131",
"doi-asserted-by": "publisher",
"key": "ref32"
},
{
"DOI": "10.3945/an.115.008292",
"doi-asserted-by": "publisher",
"key": "ref33"
},
{
"DOI": "10.1001/jama.2012.5669",
"doi-asserted-by": "publisher",
"key": "ref34"
},
{
"DOI": "10.1111/liv.14730",
"doi-asserted-by": "publisher",
"key": "ref35"
},
{
"DOI": "10.1186/1476-511X-7-29",
"doi-asserted-by": "publisher",
"key": "ref36"
},
{
"DOI": "10.1016/S0021-9258(18)46017-6",
"article-title": "Retinoids and retinoid-binding protein expression in rat adipocytes",
"author": "Tsutsumi",
"doi-asserted-by": "crossref",
"first-page": "1805",
"journal-title": "J. Biol. Chem.",
"key": "ref37",
"volume": "267",
"year": "1992"
},
{
"DOI": "10.1016/j.clinre.2021.101793",
"doi-asserted-by": "publisher",
"key": "ref38"
},
{
"DOI": "10.1111/j.1463-1326.2008.00901.x",
"doi-asserted-by": "publisher",
"key": "ref39"
},
{
"DOI": "10.1016/j.cyto.2016.07.003",
"doi-asserted-by": "publisher",
"key": "ref40"
},
{
"article-title": "Retinol Binding Protein 4 in children with Inflammatory Bowel Disease: A negative correlation with the disease activity",
"author": "Roma",
"first-page": "360",
"journal-title": "Hippokratia",
"key": "ref41",
"volume": "16",
"year": "2012"
},
{
"DOI": "10.1194/jlr.M600528-JLR200",
"doi-asserted-by": "publisher",
"key": "ref42"
},
{
"DOI": "10.3945/jn.110.125500",
"doi-asserted-by": "publisher",
"key": "ref43"
},
{
"DOI": "10.1016/j.ijid.2020.04.086",
"doi-asserted-by": "publisher",
"key": "ref44"
},
{
"DOI": "10.1016/j.cellsig.2021.110121",
"doi-asserted-by": "publisher",
"key": "ref45"
},
{
"DOI": "10.1002/anie.202015639",
"doi-asserted-by": "publisher",
"key": "ref46"
},
{
"DOI": "10.1007/s10787-021-00826-7",
"doi-asserted-by": "publisher",
"key": "ref47"
},
{
"DOI": "10.1111/cei.12718",
"doi-asserted-by": "publisher",
"key": "ref48"
},
{
"DOI": "10.1128/JVI.79.4.2079-2086.2005",
"doi-asserted-by": "publisher",
"key": "ref49"
},
{
"DOI": "10.1128/JVI.01012-07",
"doi-asserted-by": "publisher",
"key": "ref50"
},
{
"DOI": "10.1038/srep17554",
"doi-asserted-by": "publisher",
"key": "ref51"
},
{
"DOI": "10.3390/v13010047",
"doi-asserted-by": "publisher",
"key": "ref52"
},
{
"DOI": "10.1055/s-2008-1040408",
"doi-asserted-by": "publisher",
"key": "ref53"
},
{
"DOI": "10.1016/j.pharmthera.2019.01.006",
"doi-asserted-by": "publisher",
"key": "ref54"
},
{
"DOI": "10.33549/physiolres.931379",
"doi-asserted-by": "publisher",
"key": "ref55"
},
{
"DOI": "10.2337/db06-0616",
"doi-asserted-by": "publisher",
"key": "ref56"
},
{
"DOI": "10.1210/jc.2006-0816",
"doi-asserted-by": "publisher",
"key": "ref57"
},
{
"DOI": "10.2337/dc06-2034",
"doi-asserted-by": "publisher",
"key": "ref58"
},
{
"DOI": "10.2337/dc06-0360",
"doi-asserted-by": "publisher",
"key": "ref59"
},
{
"DOI": "10.3109/13813451003631421",
"doi-asserted-by": "publisher",
"key": "ref60"
},
{
"DOI": "10.1530/EJE-11-0431",
"doi-asserted-by": "publisher",
"key": "ref61"
}
],
"reference-count": 61,
"references-count": 61,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/2072-6643/14/10/2007"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Food Science",
"Nutrition and Dietetics"
],
"subtitle": [],
"title": "Significantly Reduced Retinol Binding Protein 4 (RBP4) Levels in Critically Ill COVID-19 Patients",
"type": "journal-article",
"volume": "14"
}
