COVID-19 effects on diet, sleep, and physical activity among mid- to late-adolescents residing in the deep south in the United States
et al., Journal of Pediatric Nursing, doi:10.1016/j.pedn.2023.06.003, Jun 2023
Diet for COVID-19
26th treatment shown to reduce risk in
June 2021, now with p < 0.00000000001 from 30 studies, recognized in 4 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
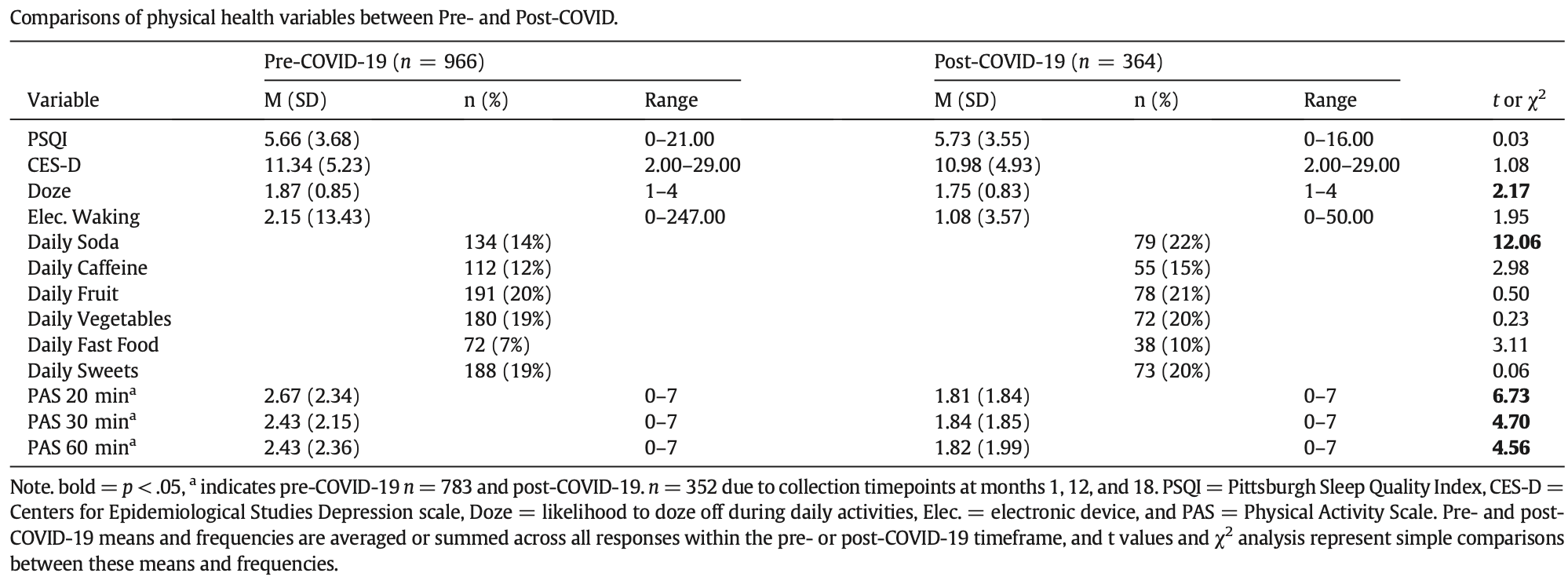
Prospective study tracking sleep, diet, and physical activity for adolescents in the USA before and during the COVID-19 pandemic, showing negative health effects of the pandemic / restrictions.
Stavrinos et al., 7 Jun 2023, retrospective, USA, peer-reviewed, 6 authors, study period 13 March, 2020 - 1 June, 2020.
Contact: dstavrin@uab.edu, bmcmanus@uab.edu, mcgwin@uab.edu, moonpie@uab.edu, rachaelg@uab.edu, kaidend7@uab.edu.
COVID-19 effects on diet, sleep, and physical activity among mid- to late-adolescents residing in the deep south in the United States
Journal of Pediatric Nursing, doi:10.1016/j.pedn.2023.06.003
This study investigated the differential impact of COVID-19 on United States (US) adolescents' physical health as a function of sociodemographic factors over 18 months. It was hypothesized that the impact of COVID-19 and its mitigation efforts on physical health factors would vary by sociodemographic factors. Design and methods: Data were drawn from a longitudinal study in which participants (ages 16 or 18) selfreported sleep, diet, and physical activity over 18months. Participants were enrolled between 2018 and 2022. Participants (n = 190, 73% Black/African American, 53% female) provided 1330 reports over 194 weeks (93 weeks before and 101 weeks after COVID-19 restrictions implementation). Results: Physical health outcomes moderated by demographic factors were measured and assessed over 18 months. Multilevel models and general estimated equations estimated the impact of COVID-19 restrictions on participants' health outcomes. Sleep and physical activity worsened after COVID-19 regardless of moderating factors, but some specific outcomes varied across subgroups. Conclusions: This study diversifies the literature on the impact of COVID-19 and its mitigation measures on adolescents' social health. Further, it is based in the US's Deep South, largely populated by those identifying as Black/ African American or of low socioeconomic status. Both subgroups are underrepresented in US-based health outcomes research. COVID-19 directly and indirectly impacted adolescents' physical health. Practice implications: Understanding if and how COVID-19 impacted adolescents' health will inform nursing practice to adapt to and overcome adverse sequelae to promote positive patient health outcomes.
References
Ammar, Brach, Trabelsi, Chtourou, Boukhris et al., Effects of COVID-19 home confinement on eating behaviour and physical activity: Results of the ECLB-COVID19 international online survey, Nutrients, doi:10.3390/nu12061583
Becker, Gregory, Editorial perspective: Perils and promise for child and adolescent sleep and associated psychopathology during the COVID-19 pandemic, The Journal of Child Psychology and Psychiatry, doi:10.1111/jcpp.13278
Bjorgvinsson, Kertz, Bigda-Peyton, Mccoy, Aderka, Psychometric properties of the CES-D-10 in a psychiatric sample, Assessment, doi:10.1177/1073191113481998
Butt, Weinberg, Breckon, Claytor, Adolescent physical activity participation and motivational determinants across gender, age, and race, Journal of Physical Activity and Health, doi:10.1123/jpah.8.8.1074
Buysse, Reynolds, Iii, Monk, Berman et al., The Pittsburgh sleep quality index: A new instrument for psychiatric practice and research, Psychiatry Research
Carriedo, Cecchini, Fernández-Río, Méndez-Giménez, Resilience and physical activity in people under home isolation due to COVID-19: A preliminary evaluation
Chaput, Willumsen, Bull, Chou, Ekelund et al., 2020 WHO guidelines on physical activity and sedentary behaviour for children and adolescents aged 5-17 years: Summary of the evidence, International Journal of Behavioral Nutrition and Physical Activity, doi:10.1186/s12966-020-01037-z
Cheval, Sivaramakrishnan, Maltagliati, Fessler, Forestier et al., Relationships between changes in self-reported physical activity, sedentary behaviour and health during the coronavirus (COVID-19) pandemic in France and Switzerland, Journal of Sports Sciences, doi:10.1080/02640414.2020.1841396
Crowley, Wolfson, Tarokh, Carskadon, An update on adolescent sleep: New evidence informing the perfect storm model, Journal of Adolescence, doi:10.1016/j.adolescence.2018.06.001
Di Renzo, Gualtieri, Pivari, Soldati, Attinà et al., Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey, Journal of Translational Medicine, doi:10.1186/s12967-020-02399-5
Dooley, Rhodes, Bandealy, Pandemic recovery for children-Beyond reopening schools, JAMA Pediatrics, doi:10.1001/jamapediatrics.2021.3227
Hayes, Krippendorff, Answering the call for a standard reliability measure for coding data, Communication and Measures, doi:10.1080/19312450709336664
Jia, Liu, Xie, Yuan, Chen et al., Changes in dietary patterns among youths in China during COVID-19 epidemic: The COVID-19 impact on lifestyle change survey (COINLICS), Appetite, doi:10.1016/j.appet.2020.105015
Kołota, Głąbska, Analysis of food habits during pandemic in a polish population-based sample of primary school adolescents: Diet and activity of youth during COVID-19 (DAY-19) study, Nutrients, doi:10.3390/nu13113711
Kumar, Akbarialiabad, Kouhanjani, Kiburi, Shidhaye et al., Association of Major Disease Outbreaks with Adolescent and Youth Mental Health in low-and middle-income countries: A systematic scoping review, JAMA Psychiatry, doi:10.1001/jamapsychiatry.2022.3109
Li, Zhang, Wang, Ozaki, Wang et al., Association of Home Quarantine and Mental Health among Teenagers in Wuhan, China, during the COVID-19 pandemic, JAMA Pediatrics, doi:10.1001/jamapediatrics.2020.5499
Liu, Wang, Villberg, Torsheim, Tynjaelae et al., Reliability and validity of family affluence scale (FAS II) among adolescents in Beijing, Child Indicators Research, doi:10.1007/s12187-011-9131-5
López-Bueno, López-Sánchez, Casajús, Calatayud, Gil-Salmerón et al., Health-related behaviors among school-aged children and adolescents during the Spanish Covid-19 confinement, Frontiers in Pediatrics
Madigan, Eirich, Pador, Mcarthur, Neville, Assessment of changes in child and adolescent screen time during the COVID-19 pandemic: A systematic review and Meta-analysis, JAMA Pediatrics, doi:10.1001/jamapediatrics.2022.4116
Marczyk Organek, Taylor, Petrie, Martin, Greenleaf et al., Adolescent sleep disparities: Sex and racial/ethnic differences, Sleep Health, doi:10.1016/j.sleh.2014.12.003
Maslowsky, Ozer, Developmental trends in sleep duration in adolescence and young adulthood: Evidence from a national United States sample, Journal of Adolescent Health, doi:10.1016/j.jadohealth.2013.10.201
Mata, Onofre, Martins, Adolescents' perceived barriers to physical activity during the COVID-19 pandemic, Children (Basel), doi:10.3390/children9111726
Mccarthy, Potts, Fisher, Physical activity behavior before, during, and after COVID-19 restrictions: Longitudinal smartphone-tracking study of adults in the United Kingdom, Journal of Medical Internet Research, doi:10.2196/23701
Mcguine, Biese, Petrovska, Hetzel, Reardon et al., Mental health, physical activity, and quality of life of US adolescent athletes during COVID-19-related school closures and sport cancellations: A study of 13000 athletes, Journal of Athletic Training, doi:10.4085/1062-6050-0478.20
Michel, Bernier, Thompson, Physical activity in children, JAMA Pediatrics, doi:10.1001/jamapediatrics.2022.0477
Ming, Radhakrishnan, Kang, Pecor, Gender, headaches, and sleep health in high school students, Journal of Women's Health, doi:10.1089/jwh.2015.5681
Morin, Carrier, Bastien, Godbout, Sleep and circadian rhythm in response to the COVID-19 pandemic, Canadian Journal of Public Health, doi:10.17269/s41997-020-00382-7
Nathan, George, Ng, Wenden, Bai et al., Impact of COVID-19 restrictions on Western Australian Children's physical activity and screen time, International Journal of Environmental Research and Public Health, doi:10.3390/ijerph18052583
Perrault, Bayer, Peuvrier, Afyouni, Ghisletta et al., Reducing the use of screen electronic devices in the evening is associated with improved sleep and daytime vigilance in adolescents, Sleep
Pietrobelli, Fearnbach, Ferruzzi, Vrech, Heo et al., Effects of COVID-19 lockdown on lifestyle behaviors in children with obesity: Longitudinal study update, Obesity Science and Practice, doi:10.1002/osp4.581
Pontes, Williams, Pontes, Interactions between race/ethnicity and gender on physical activity among US high school students: Youth risk behavior survey 2011-2017, Journal of Pediatric Nursing, doi:10.1016/j.pedn.2021.02.013
Radloff, The CES-D scale: A self-report depression scale for research in the general population, Applied Psychological Measurement
Raniti, Waloszek, Schwartz, Allen, Trinder, Factor structure and psychometric properties of the Pittsburgh sleep quality index in communitybased adolescents, Sleep, doi:10.1093/sleep/zsy066
Revell, Eastman, How to trick mother nature into letting you fly around or stay up all night, Journal of Biological Rhythms, doi:10.1177/0748730405277233
Rossi, Behme, Breuer, Physical activity of children and adolescents during the COVID-19 pandemic-a scoping review, International Journal of Environmental Research and Public Health, doi:10.3390/ijerph182111440
Schmidt, Anedda, Burchartz, Eichsteller, Kolb et al., Physical activity and screen time of children and adolescents before and during the COVID-19 lockdown in Germany: A natural experiment, Scientific Reports, doi:10.1038/s41598-020-78438-4
Shaw, Bertrand, Deprez, Ko, Zello et al., The impact of the COVID-19 pandemic on diet, fitness, and sedentary behaviour of elite Paraathletes, doi:10.1016/j.dhjo.2021.101091
Skeldon, Derks, Dijk, Modelling changes in sleep timing and duration across the lifespan: Changes in circadian rhythmicity or sleep homeostasis?, Sleep Medicine Reviews, doi:10.1016/j.smrv.2015.05.011
Stern, Wagner, Thompson, Current and COVID-19 challenges with childhood and adolescent sleep, JAMA Pediatrics, doi:10.1001/jamapediatrics.2020.2784
Tan, Tan, Tan, Trajectories of food choice motives and weight status of Malaysian youths during the COVID-19 pandemic, Nutrients, doi:10.3390/nu13113752
Ten Velde, Lubrecht, Arayess, Van Loo, Hesselink et al., Physical activity behaviour and screen time in Dutch children during the COVID-19 pandemic: Pre-, during-and post-school closures, Pediatric Obesity, doi:10.1111/ijpo.12779
Viner, Russell, Saulle, Croker, Stansfield et al., School closures during social lockdown and mental health, health behaviors, and well-being among children and adolescents during the first COVID-19 wave: A systematic review, JAMA Pediatrics, doi:10.1001/jamapediatrics.2021.5840
DOI record:
{
"DOI": "10.1016/j.pedn.2023.06.003",
"ISSN": [
"0882-5963"
],
"URL": "http://dx.doi.org/10.1016/j.pedn.2023.06.003",
"alternative-id": [
"S0882596323001276"
],
"assertion": [
{
"label": "This article is maintained by",
"name": "publisher",
"value": "Elsevier"
},
{
"label": "Article Title",
"name": "articletitle",
"value": "COVID-19 effects on diet, sleep, and physical activity among mid- to late-adolescents residing in the deep south in the United States"
},
{
"label": "Journal Title",
"name": "journaltitle",
"value": "Journal of Pediatric Nursing"
},
{
"label": "CrossRef DOI link to publisher maintained version",
"name": "articlelink",
"value": "https://doi.org/10.1016/j.pedn.2023.06.003"
},
{
"label": "Content Type",
"name": "content_type",
"value": "article"
},
{
"label": "Copyright",
"name": "copyright",
"value": "© 2023 Published by Elsevier Inc."
}
],
"author": [
{
"affiliation": [],
"family": "Stavrinos",
"given": "Despina",
"sequence": "first"
},
{
"affiliation": [],
"family": "McManus",
"given": "Benjamin",
"sequence": "additional"
},
{
"affiliation": [],
"family": "McGwin",
"given": "Gerald",
"sequence": "additional",
"suffix": "Jr"
},
{
"affiliation": [],
"family": "Underhill",
"given": "Andrea T.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "George",
"given": "Rachael",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Kennedy",
"given": "Kaiden",
"sequence": "additional"
}
],
"container-title": "Journal of Pediatric Nursing",
"container-title-short": "Journal of Pediatric Nursing",
"content-domain": {
"crossmark-restriction": true,
"domain": [
"clinicalkey.com.au",
"pediatricnursing.org",
"clinicalkey.com",
"elsevier.com",
"sciencedirect.com"
]
},
"created": {
"date-parts": [
[
2023,
6,
7
]
],
"date-time": "2023-06-07T23:41:13Z",
"timestamp": 1686181273000
},
"deposited": {
"date-parts": [
[
2023,
6,
16
]
],
"date-time": "2023-06-16T06:02:25Z",
"timestamp": 1686895345000
},
"indexed": {
"date-parts": [
[
2023,
6,
17
]
],
"date-time": "2023-06-17T04:20:30Z",
"timestamp": 1686975630179
},
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2023,
6
]
]
},
"language": "en",
"license": [
{
"URL": "https://www.elsevier.com/tdm/userlicense/1.0/",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
6,
1
]
],
"date-time": "2023-06-01T00:00:00Z",
"timestamp": 1685577600000
}
},
{
"URL": "https://doi.org/10.15223/policy-017",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
6,
1
]
],
"date-time": "2023-06-01T00:00:00Z",
"timestamp": 1685577600000
}
},
{
"URL": "https://doi.org/10.15223/policy-037",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
6,
1
]
],
"date-time": "2023-06-01T00:00:00Z",
"timestamp": 1685577600000
}
},
{
"URL": "https://doi.org/10.15223/policy-012",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
6,
1
]
],
"date-time": "2023-06-01T00:00:00Z",
"timestamp": 1685577600000
}
},
{
"URL": "https://doi.org/10.15223/policy-029",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
6,
1
]
],
"date-time": "2023-06-01T00:00:00Z",
"timestamp": 1685577600000
}
},
{
"URL": "https://doi.org/10.15223/policy-004",
"content-version": "stm-asf",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
6,
1
]
],
"date-time": "2023-06-01T00:00:00Z",
"timestamp": 1685577600000
}
}
],
"link": [
{
"URL": "https://api.elsevier.com/content/article/PII:S0882596323001276?httpAccept=text/xml",
"content-type": "text/xml",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://api.elsevier.com/content/article/PII:S0882596323001276?httpAccept=text/plain",
"content-type": "text/plain",
"content-version": "vor",
"intended-application": "text-mining"
}
],
"member": "78",
"original-title": [],
"prefix": "10.1016",
"published": {
"date-parts": [
[
2023,
6
]
]
},
"published-print": {
"date-parts": [
[
2023,
6
]
]
},
"publisher": "Elsevier BV",
"reference": [
{
"DOI": "10.3390/nu12061583",
"article-title": "Effects of COVID-19 home confinement on eating behaviour and physical activity: Results of the ECLB-COVID19 international online survey",
"author": "Ammar",
"doi-asserted-by": "crossref",
"issue": "6",
"journal-title": "Nutrients",
"key": "10.1016/j.pedn.2023.06.003_bb0005",
"volume": "12",
"year": "2020"
},
{
"DOI": "10.1111/jcpp.13278",
"article-title": "Editorial perspective: Perils and promise for child and adolescent sleep and associated psychopathology during the COVID-19 pandemic [advance online publication]",
"author": "Becker",
"doi-asserted-by": "crossref",
"first-page": "757",
"issue": "7",
"journal-title": "The Journal of Child Psychology and Psychiatry",
"key": "10.1016/j.pedn.2023.06.003_bb0010",
"volume": "61",
"year": "2020"
},
{
"DOI": "10.1177/1073191113481998",
"article-title": "Psychometric properties of the CES-D-10 in a psychiatric sample",
"author": "Bjorgvinsson",
"doi-asserted-by": "crossref",
"first-page": "429",
"issue": "4",
"journal-title": "Assessment",
"key": "10.1016/j.pedn.2023.06.003_bb0015",
"volume": "20",
"year": "2013"
},
{
"DOI": "10.1123/jpah.8.8.1074",
"article-title": "Adolescent physical activity participation and motivational determinants across gender, age, and race",
"author": "Butt",
"doi-asserted-by": "crossref",
"first-page": "1074",
"issue": "8",
"journal-title": "Journal of Physical Activity and Health",
"key": "10.1016/j.pedn.2023.06.003_bb0020",
"volume": "8",
"year": "2011"
},
{
"DOI": "10.1016/0165-1781(89)90047-4",
"article-title": "The Pittsburgh sleep quality index: A new instrument for psychiatric practice and research",
"author": "Buysse",
"doi-asserted-by": "crossref",
"first-page": "193",
"issue": "2",
"journal-title": "Psychiatry Research",
"key": "10.1016/j.pedn.2023.06.003_bb0025",
"volume": "28",
"year": "1989"
},
{
"DOI": "10.1016/j.mhpa.2020.100361",
"article-title": "Resilience and physical activity in people under home isolation due to COVID-19: A preliminary evaluation",
"author": "Carriedo",
"doi-asserted-by": "crossref",
"journal-title": "Mental Health and Physical Activity",
"key": "10.1016/j.pedn.2023.06.003_bb0030",
"volume": "19",
"year": "2020"
},
{
"author": "Center for Disease Control and Prevention [CDC]",
"key": "10.1016/j.pedn.2023.06.003_bb0035",
"series-title": "COVID Data Tracker",
"year": "2022"
},
{
"DOI": "10.1186/s12966-020-01037-z",
"article-title": "2020 WHO guidelines on physical activity and sedentary behaviour for children and adolescents aged 5-17 years: Summary of the evidence",
"author": "Chaput",
"doi-asserted-by": "crossref",
"first-page": "141",
"issue": "1",
"journal-title": "International Journal of Behavioral Nutrition and Physical Activity",
"key": "10.1016/j.pedn.2023.06.003_bb0040",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1080/02640414.2020.1841396",
"article-title": "Relationships between changes in self-reported physical activity, sedentary behaviour and health during the coronavirus (COVID-19) pandemic in France and Switzerland",
"author": "Cheval",
"doi-asserted-by": "crossref",
"first-page": "699",
"issue": "6",
"journal-title": "Journal of Sports Sciences",
"key": "10.1016/j.pedn.2023.06.003_bb0045",
"volume": "39",
"year": "2021"
},
{
"DOI": "10.1016/j.adolescence.2018.06.001",
"article-title": "An update on adolescent sleep: New evidence informing the perfect storm model",
"author": "Crowley",
"doi-asserted-by": "crossref",
"first-page": "55",
"journal-title": "Journal of Adolescence",
"key": "10.1016/j.pedn.2023.06.003_bb0050",
"volume": "67",
"year": "2018"
},
{
"DOI": "10.1186/s12967-020-02399-5",
"article-title": "Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey",
"author": "Di Renzo",
"doi-asserted-by": "crossref",
"first-page": "229",
"issue": "1",
"journal-title": "Journal of Translational Medicine",
"key": "10.1016/j.pedn.2023.06.003_bb0055",
"volume": "18",
"year": "2020"
},
{
"DOI": "10.1001/jamapediatrics.2021.3227",
"article-title": "Pandemic recovery for children—Beyond reopening schools",
"author": "Dooley",
"doi-asserted-by": "crossref",
"first-page": "347",
"issue": "4",
"journal-title": "JAMA Pediatrics",
"key": "10.1016/j.pedn.2023.06.003_bb0060",
"volume": "176",
"year": "2022"
},
{
"DOI": "10.1080/19312450709336664",
"article-title": "Answering the call for a standard reliability measure for coding data",
"author": "Hayes",
"doi-asserted-by": "crossref",
"first-page": "77",
"issue": "1",
"journal-title": "Communication and Measures",
"key": "10.1016/j.pedn.2023.06.003_bb0065",
"volume": "1",
"year": "2007"
},
{
"DOI": "10.1016/j.appet.2020.105015",
"article-title": "Changes in dietary patterns among youths in China during COVID-19 epidemic: The COVID-19 impact on lifestyle change survey (COINLICS)",
"author": "Jia",
"doi-asserted-by": "crossref",
"journal-title": "Appetite",
"key": "10.1016/j.pedn.2023.06.003_bb0070",
"volume": "158",
"year": "2021"
},
{
"DOI": "10.3390/nu13113711",
"article-title": "Analysis of food habits during pandemic in a polish population-based sample of primary school adolescents: Diet and activity of youth during COVID-19 (DAY-19) study",
"author": "Kołota",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "Nutrients",
"key": "10.1016/j.pedn.2023.06.003_bb0075",
"volume": "13",
"year": "2021"
},
{
"DOI": "10.1001/jamapsychiatry.2022.3109",
"article-title": "Association of Major Disease Outbreaks with Adolescent and Youth Mental Health in low- and middle-income countries: A systematic scoping review",
"author": "Kumar",
"doi-asserted-by": "crossref",
"first-page": "1232",
"issue": "12",
"journal-title": "JAMA Psychiatry",
"key": "10.1016/j.pedn.2023.06.003_bb0080",
"volume": "79",
"year": "2022"
},
{
"DOI": "10.1001/jamapediatrics.2020.5499",
"article-title": "Association of Home Quarantine and Mental Health among Teenagers in Wuhan, China, during the COVID-19 pandemic",
"author": "Li",
"doi-asserted-by": "crossref",
"first-page": "313",
"issue": "3",
"journal-title": "JAMA Pediatrics",
"key": "10.1016/j.pedn.2023.06.003_bb0085",
"volume": "175",
"year": "2021"
},
{
"DOI": "10.1007/s12187-011-9131-5",
"article-title": "Reliability and validity of family affluence scale (FAS II) among adolescents in Beijing, China",
"author": "Liu",
"doi-asserted-by": "crossref",
"first-page": "235",
"journal-title": "Child Indicators Research",
"key": "10.1016/j.pedn.2023.06.003_bb0090",
"volume": "5",
"year": "2012"
},
{
"DOI": "10.3389/fped.2020.00573",
"article-title": "Health-related behaviors among school-aged children and adolescents during the Spanish Covid-19 confinement",
"author": "López-Bueno",
"doi-asserted-by": "crossref",
"first-page": "573",
"journal-title": "Frontiers in Pediatrics",
"key": "10.1016/j.pedn.2023.06.003_bb0095",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1001/jamapediatrics.2022.4116",
"article-title": "Assessment of changes in child and adolescent screen time during the COVID-19 pandemic: A systematic review and Meta-analysis",
"author": "Madigan",
"doi-asserted-by": "crossref",
"first-page": "1188",
"issue": "12",
"journal-title": "JAMA Pediatrics",
"key": "10.1016/j.pedn.2023.06.003_bb0100",
"volume": "176",
"year": "2022"
},
{
"DOI": "10.1016/j.sleh.2014.12.003",
"article-title": "Adolescent sleep disparities: Sex and racial/ethnic differences",
"author": "Marczyk Organek",
"doi-asserted-by": "crossref",
"first-page": "36",
"issue": "1",
"journal-title": "Sleep Health",
"key": "10.1016/j.pedn.2023.06.003_bb0105",
"volume": "1",
"year": "2015"
},
{
"DOI": "10.1016/j.jadohealth.2013.10.201",
"article-title": "Developmental trends in sleep duration in adolescence and young adulthood: Evidence from a national United States sample",
"author": "Maslowsky",
"doi-asserted-by": "crossref",
"first-page": "691",
"issue": "6",
"journal-title": "Journal of Adolescent Health",
"key": "10.1016/j.pedn.2023.06.003_bb0110",
"volume": "54",
"year": "2014"
},
{
"article-title": "Adolescents’ perceived barriers to physical activity during the COVID-19 pandemic",
"author": "Mata",
"issue": "11",
"journal-title": "Children (Basel)",
"key": "10.1016/j.pedn.2023.06.003_bb0115",
"volume": "9",
"year": "2022"
},
{
"DOI": "10.2196/23701",
"article-title": "Physical activity behavior before, during, and after COVID-19 restrictions: Longitudinal smartphone-tracking study of adults in the United Kingdom",
"author": "McCarthy",
"doi-asserted-by": "crossref",
"issue": "2",
"journal-title": "Journal of Medical Internet Research",
"key": "10.1016/j.pedn.2023.06.003_bb0120",
"volume": "23",
"year": "2021"
},
{
"DOI": "10.4085/1062-6050-0478.20",
"article-title": "Mental health, physical activity, and quality of life of US adolescent athletes during COVID-19-related school closures and sport cancellations: A study of 13000 athletes",
"author": "McGuine",
"doi-asserted-by": "crossref",
"first-page": "11",
"issue": "1",
"journal-title": "Journal of Athletic Training",
"key": "10.1016/j.pedn.2023.06.003_bb0125",
"volume": "56",
"year": "2021"
},
{
"DOI": "10.1001/jamapediatrics.2022.0477",
"article-title": "Physical activity in children",
"author": "Michel",
"doi-asserted-by": "crossref",
"first-page": "622",
"issue": "6",
"journal-title": "JAMA Pediatrics",
"key": "10.1016/j.pedn.2023.06.003_bb0130",
"volume": "176",
"year": "2022"
},
{
"DOI": "10.1089/jwh.2015.5681",
"article-title": "Gender, headaches, and sleep health in high school students",
"author": "Ming",
"doi-asserted-by": "crossref",
"first-page": "930",
"issue": "9",
"journal-title": "Journal of Women’s Health",
"key": "10.1016/j.pedn.2023.06.003_bb0135",
"volume": "25",
"year": "2016"
},
{
"DOI": "10.17269/s41997-020-00382-7",
"article-title": "Sleep and circadian rhythm in response to the COVID-19 pandemic",
"author": "Morin",
"doi-asserted-by": "crossref",
"first-page": "654",
"issue": "5",
"journal-title": "Canadian Journal of Public Health",
"key": "10.1016/j.pedn.2023.06.003_bb0140",
"volume": "111",
"year": "2020"
},
{
"DOI": "10.3390/ijerph18052583",
"article-title": "Impact of COVID-19 restrictions on Western Australian Children’s physical activity and screen time",
"author": "Nathan",
"doi-asserted-by": "crossref",
"issue": "5",
"journal-title": "International Journal of Environmental Research and Public Health",
"key": "10.1016/j.pedn.2023.06.003_bb0145",
"volume": "18",
"year": "2021"
},
{
"article-title": "Reducing the use of screen electronic devices in the evening is associated with improved sleep and daytime vigilance in adolescents",
"author": "Perrault",
"first-page": "1",
"journal-title": "Sleep",
"key": "10.1016/j.pedn.2023.06.003_bb0150",
"volume": "42(9)",
"year": "2019"
},
{
"DOI": "10.1002/osp4.581",
"article-title": "Effects of COVID-19 lockdown on lifestyle behaviors in children with obesity: Longitudinal study update",
"author": "Pietrobelli",
"doi-asserted-by": "crossref",
"first-page": "525",
"issue": "4",
"journal-title": "Obesity Science and Practice",
"key": "10.1016/j.pedn.2023.06.003_bb0155",
"volume": "8",
"year": "2022"
},
{
"DOI": "10.1016/j.pedn.2021.02.013",
"article-title": "Interactions between race/ethnicity and gender on physical activity among US high school students: Youth risk behavior survey 2011-2017",
"author": "Pontes",
"doi-asserted-by": "crossref",
"first-page": "100",
"journal-title": "Journal of Pediatric Nursing",
"key": "10.1016/j.pedn.2023.06.003_bb0160",
"volume": "60",
"year": "2021"
},
{
"DOI": "10.1177/014662167700100306",
"article-title": "The CES-D scale: A self-report depression scale for research in the general population",
"author": "Radloff",
"doi-asserted-by": "crossref",
"first-page": "385",
"issue": "3",
"journal-title": "Applied Psychological Measurement",
"key": "10.1016/j.pedn.2023.06.003_bb0165",
"volume": "1",
"year": "1977"
},
{
"DOI": "10.1093/sleep/zsy066",
"article-title": "Factor structure and psychometric properties of the Pittsburgh sleep quality index in community-based adolescents",
"author": "Raniti",
"doi-asserted-by": "crossref",
"issue": "6",
"journal-title": "Sleep",
"key": "10.1016/j.pedn.2023.06.003_bb0170",
"volume": "41",
"year": "2018"
},
{
"DOI": "10.1177/0748730405277233",
"article-title": "How to trick mother nature into letting you fly around or stay up all night",
"author": "Revell",
"doi-asserted-by": "crossref",
"first-page": "353",
"issue": "4",
"journal-title": "Journal of Biological Rhythms",
"key": "10.1016/j.pedn.2023.06.003_bb0175",
"volume": "20",
"year": "2005"
},
{
"DOI": "10.3390/ijerph182111440",
"article-title": "Physical activity of children and adolescents during the COVID-19 pandemic-a scoping review",
"author": "Rossi",
"doi-asserted-by": "crossref",
"issue": "21",
"journal-title": "International Journal of Environmental Research and Public Health",
"key": "10.1016/j.pedn.2023.06.003_bb0180",
"volume": "18",
"year": "2021"
},
{
"DOI": "10.1038/s41598-020-78438-4",
"article-title": "Physical activity and screen time of children and adolescents before and during the COVID-19 lockdown in Germany: A natural experiment",
"author": "Schmidt",
"doi-asserted-by": "crossref",
"first-page": "21780",
"issue": "1",
"journal-title": "Scientific Reports",
"key": "10.1016/j.pedn.2023.06.003_bb0185",
"volume": "10",
"year": "2020"
},
{
"DOI": "10.1016/j.dhjo.2021.101091",
"article-title": "The impact of the COVID-19 pandemic on diet, fitness, and sedentary behaviour of elite Para-athletes",
"author": "Shaw",
"doi-asserted-by": "crossref",
"issue": "3",
"journal-title": "Disability and Health Journal",
"key": "10.1016/j.pedn.2023.06.003_bb0190",
"volume": "14",
"year": "2021"
},
{
"DOI": "10.1016/j.smrv.2015.05.011",
"article-title": "Modelling changes in sleep timing and duration across the lifespan: Changes in circadian rhythmicity or sleep homeostasis?",
"author": "Skeldon",
"doi-asserted-by": "crossref",
"first-page": "96",
"journal-title": "Sleep Medicine Reviews",
"key": "10.1016/j.pedn.2023.06.003_bb0195",
"volume": "28",
"year": "2016"
},
{
"DOI": "10.1001/jamapediatrics.2020.2784",
"article-title": "Current and COVID-19 challenges with childhood and adolescent sleep",
"author": "Stern",
"doi-asserted-by": "crossref",
"first-page": "1124",
"issue": "11",
"journal-title": "JAMA Pediatrics",
"key": "10.1016/j.pedn.2023.06.003_bb0200",
"volume": "174",
"year": "2020"
},
{
"DOI": "10.3390/nu13113752",
"article-title": "Trajectories of food choice motives and weight status of Malaysian youths during the COVID-19 pandemic",
"author": "Tan",
"doi-asserted-by": "crossref",
"issue": "11",
"journal-title": "Nutrients",
"key": "10.1016/j.pedn.2023.06.003_bb0205",
"volume": "13",
"year": "2021"
},
{
"article-title": "Physical activity behaviour and screen time in Dutch children during the COVID-19 pandemic: Pre-, during- and post-school closures",
"author": "ten Velde",
"issue": "9",
"journal-title": "Pediatric Obesity",
"key": "10.1016/j.pedn.2023.06.003_bb0210",
"volume": "16",
"year": "2021"
},
{
"DOI": "10.1001/jamapediatrics.2021.5840",
"article-title": "School closures during social lockdown and mental health, health behaviors, and well-being among children and adolescents during the first COVID-19 wave: A systematic review",
"author": "Viner",
"doi-asserted-by": "crossref",
"first-page": "400",
"issue": "4",
"journal-title": "JAMA Pediatrics",
"key": "10.1016/j.pedn.2023.06.003_bb0215",
"volume": "176",
"year": "2022"
}
],
"reference-count": 43,
"references-count": 43,
"relation": {},
"resource": {
"primary": {
"URL": "https://linkinghub.elsevier.com/retrieve/pii/S0882596323001276"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"Pediatrics"
],
"subtitle": [],
"title": "COVID-19 effects on diet, sleep, and physical activity among mid- to late-adolescents residing in the deep south in the United States",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1016/elsevier_cm_policy"
}
stavrinos
