Cannabis consumption is associated with lower COVID-19 severity among hospitalized patients: a retrospective cohort analysis
et al., Journal of Cannabis Research, doi:10.1186/s42238-022-00152-x, Aug 2022
Retrospective 1,831 hospitalized COVID-19 patients in the USA, showing lower mechanical ventilation and ICU admission, but no significant difference in mortality.
Standard of Care (SOC) for COVID-19 in the study country,
the USA, is very poor with very low average efficacy for approved treatments1.
Only expensive, high-profit treatments were approved for early treatment. Low-cost treatments were excluded, reducing the probability of early treatment due to access and cost barriers, and eliminating complementary and synergistic benefits seen with many low-cost treatments.
|
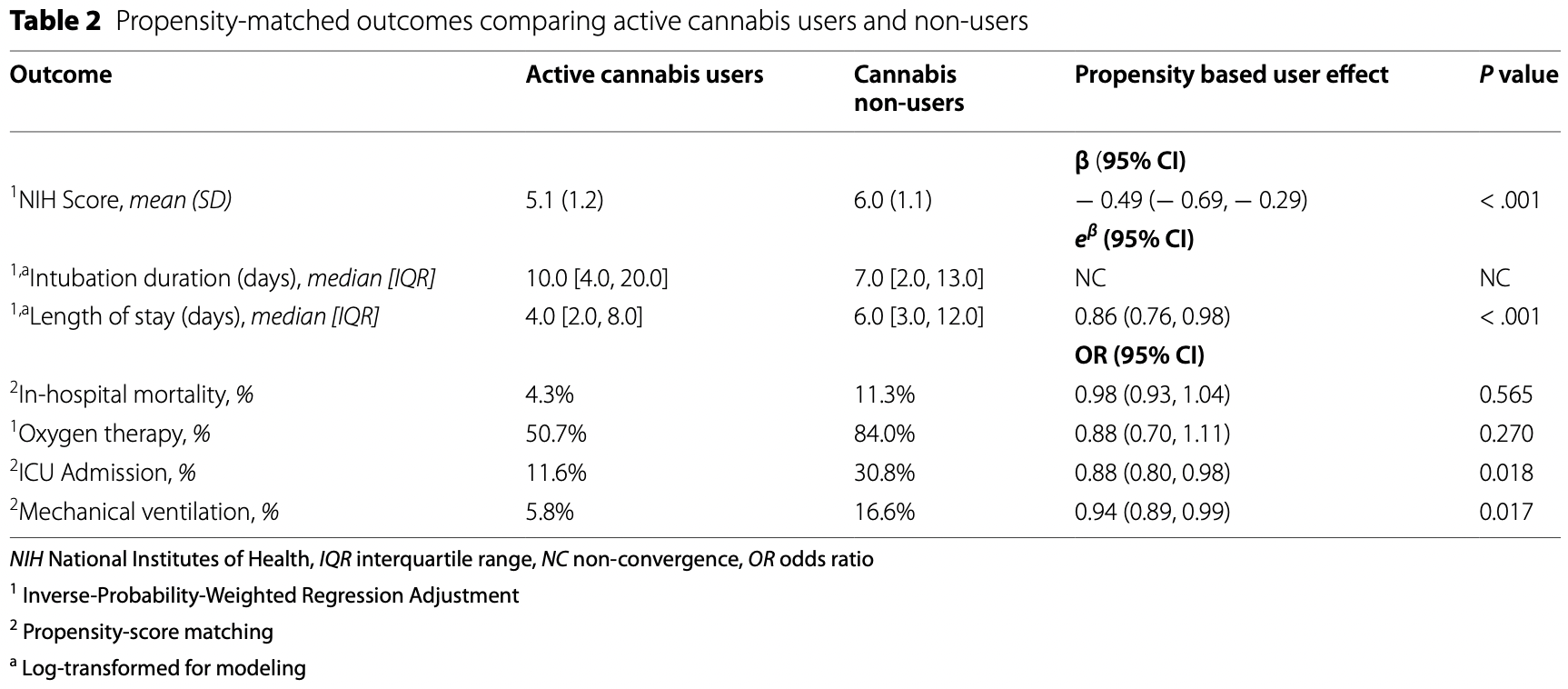
risk of death, 1.8% lower, RR 0.98, p = 0.56, treatment 3 of 69 (4.3%), control 199 of 1,762 (11.3%), odds ratio converted to relative risk, propensity score matching.
|
|
risk of mechanical ventilation, 5.1% lower, RR 0.95, p = 0.02, treatment 3 of 69 (4.3%), control 292 of 1,762 (16.6%), NNT 8.2, odds ratio converted to relative risk, propensity score matching.
|
|
risk of ICU admission, 8.6% lower, RR 0.91, p = 0.02, treatment 8 of 69 (11.6%), control 543 of 1,762 (30.8%), NNT 5.2, odds ratio converted to relative risk, propensity score matching.
|
|
risk of oxygen therapy, 2.6% lower, RR 0.97, p = 0.27, treatment 35 of 69 (50.7%), control 1,417 of 1,762 (80.4%), NNT 3.4, odds ratio converted to relative risk, propensity score weighting.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Shover et al., 5 Aug 2022, retrospective, USA, peer-reviewed, 7 authors, study period 12 February, 2020 - 27 February, 2021.
Contact: ibarjaktarevic@mednet.ucla.edu (corresponding author).
Cannabis consumption is associated with lower COVID-19 severity among hospitalized patients: a retrospective cohort analysis
Journal of Cannabis Research, doi:10.1186/s42238-022-00152-x
Background: While cannabis is known to have immunomodulatory properties, the clinical consequences of its use on outcomes in COVID-19 have not been extensively evaluated. We aimed to assess whether cannabis users hospitalized for COVID-19 had improved outcomes compared to non-users.
Methods: We conducted a retrospective analysis of 1831 patients admitted to two medical centers in Southern California with a diagnosis of COVID-19. We evaluated outcomes including NIH COVID-19 Severity Score, need for supplemental oxygen, ICU (intensive care unit) admission, mechanical ventilation, length of hospitalization, and in-hospital death for cannabis users and non-users. Cannabis use was reported in the patient's social history. Propensity matching was used to account for differences in age, body-mass index, sex, race, tobacco smoking history, and comorbidities known to be risk factors for COVID-19 mortality between cannabis users and non-users.
Results: Of 1831 patients admitted with COVID-19, 69 patients reported active cannabis use (4% of the cohort). Active users were younger (44 years vs. 62 years, p < 0.001), less often diabetic (23.2% vs 37.2%, p < 0.021), and more frequently active tobacco smokers (20.3% vs. 4.1%, p < 0.001) compared to non-users. Notably, active users had lower levels of inflammatory markers upon admission than non-users-CRP (C-reactive protein) (3.7 mg/L vs 7.6 mg/L, p < 0.001), ferritin (282 μg/L vs 622 μg/L, p < 0.001), D-dimer (468 ng/mL vs 1140 ng/mL, p = 0.017), and procalcitonin (0.10 ng/mL vs 0.15 ng/mL, p = 0.001). Based on univariate analysis, cannabis users had significantly better outcomes compared to non-users as reflected in lower NIH scores (5.1 vs 6.0, p < 0.001), shorter hospitalization (4 days vs 6 days, p < 0.001), lower ICU admission rates (12% vs 31%, p < 0.001), and less need for mechanical ventilation (6% vs 17%, p = 0.027). Using propensity matching, differences in overall survival were not statistically significant between cannabis users and non-users, nevertheless ICU admission was 12 percentage points lower (p = 0.018) and intubation rates were 6 percentage points lower (p = 0.017) in cannabis users. Conclusions: This retrospective cohort study suggests that active cannabis users hospitalized with COVID-19 had better clinical outcomes compared with non-users, including decreased need for ICU admission or mechanical
Abbreviations
Supplementary Information The online version contains supplementary material available at https:// doi. org/ 10. 1186/ s42238-022-00152-x. Additional file 1: Supplemental Table 1 . NIH Severity Score and Definitions (Beigel et al. 2020) . Supplemental Table 2 . Covariate balance after propensity weighting or matching.
Authors' contributions JAF designed the database and obtained regulatory approvals. CMS and PY reviewed the data. CMS, NJJ, and RGB developed the analytic plan. NJJ analyzed the data. CMS, PY, RGB, DPT, and IB drafted and/or critically edited the manuscript. All authors reviewed and approved the final version of the manuscript for submission.
Declarations Ethics approval and consent to participate This study was reviewed and approved by the UCLA Institutional Review Board (20-000473).
Competing interests RGB received personal consulting fees from Viatris/Theravance Biopharma, unrelated to this work. IZB reports consulting for Astra Zeneca, GSK, Viatris/ Theravance, Aerogen, Verona Pharma and Grifols. Dr. Buhr is employed by the Veterans Health Administration. The views and findings of this manuscript do not necessarily reflect the opinions of the United States Government. • fast, convenient online submission • thorough peer review by experienced researchers in your field • rapid publication on acceptance • support for research data, including large and complex data types • gold Open Access which fosters wider collaboration and increased..
References
Beigel, :677 Remdesivir for the Treatment of Covid-19 -Final Report, N Engl J Med
Biotechs, Stero Biotechs supports an Exploratory Study of CBD-based treatment for COVID-19 severe patients
Borgonhi, Volpatto, Ornell, Rabelo-Da-Ponte, Kessler, Multiple clinical risks for cannabis users during the COVID-19 pandemic, Addict Sci Clin Pract
Chadi, Minato, Stanwick, Cannabis vaping: Understanding the health risks of a rapidly emerging trend, Paediatr Child Health
Colmenero, Epidemiological pattern, incidence, and outcomes of COVID-19 in liver transplant patients, J Hepatol
Dai, Richter, A National Survey of Marijuana Use Among US Adults With Medical Conditions, 2016-2017, JAMA Netw Open
Gold, COVID-19 Case Surveillance: Trends in Person-Level Case Data Completeness, United States, Public Health Rep
Guillon, Hiemstra, Si-Tahar, Pulmonary immune responses against SARS-CoV-2 infection: harmful or not?, Intensive Care Med, doi:10.1007/s00134-020-06170-8
Han, Mallampalli, The acute respiratory distress syndrome: from mechanism to translation, J Immunol
Harris, Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support, J Biomed Inform
Harris, The REDCap Consortium: Building an International Community of Software Platform Partners, J Biomed Inform
Ioannidis, Global perspective of COVID-19 epidemiology for a full-cycle pandemic, Eur J Clin Invest
Lancet, Medicine. The EVALI outbreak and vaping in the COVID-19 era, Lancet Respir Med
Maresz, Direct suppression of CNS autoimmune inflammation via the cannabinoid receptor CB1 on neurons and CB2 on autoreactive T cells, Nat Med
Mcgilveray, Pharmacokinetics of cannabinoids, Pain Res Manag
Mohammed, Δ9-Tetrahydrocannabinol Prevents Mortality from Acute Respiratory Distress Syndrome through the Induction of Apoptosis in Immune Cells, Leading to Cytokine Storm Suppression, Int J Mol Sci
Moore, Augustson, Moser, Budney, Respiratory Effects of Marijuana and Tobacco Use in a U.S. Sample, J Gen Intern Med
Onaivi, Sharma, Cannabis for COVID-19: can cannabinoids quell the cytokine storm?, Fut Sci OA
Paland, The Immunopathology of COVID-19 and the Cannabis Paradigm, Front Immunol
Patanavanich, Glantz, Smoking Is Associated With COVID-19 Progression: A Meta-analysis, Nicotine Tob Res
Pink, C-reactive protein and procalcitonin for antimicrobial stewardship in COVID-19, Infection, doi:10.1007/s15010-021-01615-8
Russell, Rueda, Room, Tyndall, Fischer, Routes of administration for cannabis use -basic prevalence and related health outcomes: A scoping review and synthesis, Int J Drug Policy
Saadatian-Elahi, Tobacco smoking and severity of COVID-19: Experience from a hospital-based prospective cohort study in Lyon, France, J Med Virol, doi:10.1002/jmv.27233
Tashkin, Roth, Pulmonary effects of inhaled cannabis smoke, Am J Drug Alcohol Abuse
Van Breemen, Cannabinoids Block Cellular Entry of SARS-CoV-2 and the Emerging Variants, J Nat Prod, doi:10.1021/acs.jnatprod.1c00946
Wang, Kaelber, Xu, Volkow, COVID-19 risk and outcomes in patients with substance use disorders: analyses from electronic health records in the United States, Mol Psychiatry
Wang, Wang, Davis, Volkow, Xu, Increased risk for COVID-19 breakthrough infection in fully vaccinated patients with substance use disorders in the United States between December 2020 and, World Psychiatry, doi:10.1002/wps.20921
DOI record:
{
"DOI": "10.1186/s42238-022-00152-x",
"ISSN": [
"2522-5782"
],
"URL": "http://dx.doi.org/10.1186/s42238-022-00152-x",
"abstract": "<jats:title>Abstract</jats:title><jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>While cannabis is known to have immunomodulatory properties, the clinical consequences of its use on outcomes in COVID-19 have not been extensively evaluated. We aimed to assess whether cannabis users hospitalized for COVID-19 had improved outcomes compared to non-users.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Methods</jats:title>\n <jats:p>We conducted a retrospective analysis of 1831 patients admitted to two medical centers in Southern California with a diagnosis of COVID-19. We evaluated outcomes including NIH COVID-19 Severity Score, need for supplemental oxygen, ICU (intensive care unit) admission, mechanical ventilation, length of hospitalization, and in-hospital death for cannabis users and non-users. Cannabis use was reported in the patient’s social history. Propensity matching was used to account for differences in age, body-mass index, sex, race, tobacco smoking history, and comorbidities known to be risk factors for COVID-19 mortality between cannabis users and non-users.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>Of 1831 patients admitted with COVID-19, 69 patients reported active cannabis use (4% of the cohort). Active users were younger (44 years vs. 62 years, <jats:italic>p</jats:italic> < 0.001), less often diabetic (23.2% vs 37.2%, <jats:italic>p</jats:italic> < 0.021), and more frequently active tobacco smokers (20.3% vs. 4.1%, <jats:italic>p</jats:italic> < 0.001) compared to non-users. Notably, active users had lower levels of inflammatory markers upon admission than non-users—CRP (C-reactive protein) (3.7 mg/L vs 7.6 mg/L, <jats:italic>p</jats:italic> < 0.001), ferritin (282 μg/L vs 622 μg/L, <jats:italic>p</jats:italic> < 0.001), D-dimer (468 ng/mL vs 1140 ng/mL, <jats:italic>p</jats:italic> = 0.017), and procalcitonin (0.10 ng/mL vs 0.15 ng/mL, <jats:italic>p</jats:italic> = 0.001). Based on univariate analysis, cannabis users had significantly better outcomes compared to non-users as reflected in lower NIH scores (5.1 vs 6.0, <jats:italic>p</jats:italic> < 0.001), shorter hospitalization (4 days vs 6 days, <jats:italic>p</jats:italic> < 0.001), lower ICU admission rates (12% vs 31%, <jats:italic>p</jats:italic> < 0.001), and less need for mechanical ventilation (6% vs 17%, <jats:italic>p</jats:italic> = 0.027). Using propensity matching, differences in overall survival were not statistically significant between cannabis users and non-users, nevertheless ICU admission was 12 percentage points lower (<jats:italic>p</jats:italic> = 0.018) and intubation rates were 6 percentage points lower (<jats:italic>p</jats:italic> = 0.017) in cannabis users.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Conclusions</jats:title>\n <jats:p>This retrospective cohort study suggests that active cannabis users hospitalized with COVID-19 had better clinical outcomes compared with non-users, including decreased need for ICU admission or mechanical ventilation. However, our results need to be interpreted with caution given the limitations of a retrospective analysis. Prospective and observational studies will better elucidate the effects cannabis use in COVID-19 patients.</jats:p>\n </jats:sec>",
"alternative-id": [
"152"
],
"article-number": "46",
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "18 January 2022"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "3 July 2022"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "5 August 2022"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Ethics approval and consent to participate",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "This study was reviewed and approved by the UCLA Institutional Review Board (20-000473)."
},
{
"group": {
"label": "Competing interests",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "RGB received personal consulting fees from Viatris/Theravance Biopharma, unrelated to this work. IZB reports consulting for Astra Zeneca, GSK, Viatris/Theravance, Aerogen, Verona Pharma and Grifols. Dr. Buhr is employed by the Veterans Health Administration. The views and findings of this manuscript do not necessarily reflect the opinions of the United States Government."
}
],
"author": [
{
"affiliation": [],
"family": "Shover",
"given": "Carolyn M.",
"sequence": "first"
},
{
"affiliation": [],
"family": "Yan",
"given": "Peter",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Jackson",
"given": "Nicholas J.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Buhr",
"given": "Russell G.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Fulcher",
"given": "Jennifer A.",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Tashkin",
"given": "Donald P.",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-8096-0858",
"affiliation": [],
"authenticated-orcid": false,
"family": "Barjaktarevic",
"given": "Igor",
"sequence": "additional"
}
],
"container-title": "Journal of Cannabis Research",
"container-title-short": "J Cannabis Res",
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2022,
8,
5
]
],
"date-time": "2022-08-05T12:19:54Z",
"timestamp": 1659701994000
},
"deposited": {
"date-parts": [
[
2022,
8,
5
]
],
"date-time": "2022-08-05T12:20:46Z",
"timestamp": 1659702046000
},
"funder": [
{
"DOI": "10.13039/100016206",
"award": [
"UL1TR001881"
],
"doi-asserted-by": "crossref",
"name": "UCLA Clinical and Translational Science Institute"
},
{
"award": [
"KL2TR001882"
],
"name": "NIH/NCATS"
}
],
"indexed": {
"date-parts": [
[
2022,
8,
5
]
],
"date-time": "2022-08-05T12:42:01Z",
"timestamp": 1659703321448
},
"is-referenced-by-count": 0,
"issue": "1",
"issued": {
"date-parts": [
[
2022,
8,
5
]
]
},
"journal-issue": {
"issue": "1",
"published-online": {
"date-parts": [
[
2022,
12
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
8,
5
]
],
"date-time": "2022-08-05T00:00:00Z",
"timestamp": 1659657600000
}
},
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2022,
8,
5
]
],
"date-time": "2022-08-05T00:00:00Z",
"timestamp": 1659657600000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1186/s42238-022-00152-x.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1186/s42238-022-00152-x/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1186/s42238-022-00152-x.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"prefix": "10.1186",
"published": {
"date-parts": [
[
2022,
8,
5
]
]
},
"published-online": {
"date-parts": [
[
2022,
8,
5
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"key": "152_CR1",
"unstructured": "2020 National Survey of Drug Use and Health (NSDUH) Releases | CBHSQ Data. https://www.samhsa.gov/data/release/2020-national-survey-drug-use-and-health-nsduh-releases. Accessed 1 Oct 2021."
},
{
"DOI": "10.1186/s13054-020-03406-3",
"author": "J Beigel",
"doi-asserted-by": "publisher",
"first-page": "677",
"journal-title": "Crit Care",
"key": "152_CR2",
"unstructured": "Beigel J, et al. Remedesivir for the Treatment of COVID-19 - Final Report. Crit Care. 2020;24:677 Remdesivir for the Treatment of Covid-19 - Final Report. N Engl J Med. 2020 Nov 5;383(19):1813-1826 (2020).",
"volume": "24",
"year": "2020"
},
{
"key": "152_CR3",
"unstructured": "Biotechs, S. Stero Biotechs supports an Exploratory Study of CBD-based treatment for COVID-19 severe patients. https://www.prnewswire.com/il/news-releases/stero-biotechs-supports-an-exploratory-study-of-cbd-based-treatment-for-covid-19-severe-patients-301200798.html. Accessed 1 Oct 2021."
},
{
"DOI": "10.1186/s13722-021-00214-0",
"author": "EM Borgonhi",
"doi-asserted-by": "publisher",
"first-page": "5",
"journal-title": "Addict Sci Clin Pract",
"key": "152_CR4",
"unstructured": "Borgonhi EM, Volpatto VL, Ornell F, Rabelo-da-Ponte FD, Kessler FHP. Multiple clinical risks for cannabis users during the COVID-19 pandemic. Addict Sci Clin Pract. 2021;16:5.",
"volume": "16",
"year": "2021"
},
{
"DOI": "10.1093/pch/pxaa016",
"doi-asserted-by": "crossref",
"key": "152_CR5",
"unstructured": "Chadi N, Minato C, Stanwick R. Cannabis vaping: Understanding the health risks of a rapidly emerging trend. Paediatr Child Health. 2020;25(Suppl 1):S16–S20."
},
{
"DOI": "10.1016/j.jhep.2020.07.040",
"author": "J Colmenero",
"doi-asserted-by": "publisher",
"first-page": "148",
"journal-title": "J Hepatol",
"key": "152_CR6",
"unstructured": "Colmenero J, et al. Epidemiological pattern, incidence, and outcomes of COVID-19 in liver transplant patients. J Hepatol. 2021;74:148–55.",
"volume": "74",
"year": "2021"
},
{
"key": "152_CR7",
"unstructured": "Coronavirus Disease (COVID-19) Situation Reports. https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports. Aaccessed 1 Oct 2021."
},
{
"DOI": "10.1001/jamanetworkopen.2019.11936",
"author": "H Dai",
"doi-asserted-by": "publisher",
"journal-title": "JAMA Netw Open",
"key": "152_CR8",
"unstructured": "Dai H, Richter KP. A National Survey of Marijuana Use Among US Adults With Medical Conditions, 2016-2017. JAMA Netw Open. 2019;2:e1911936.",
"volume": "2",
"year": "2019"
},
{
"DOI": "10.1177/00333549211006973",
"author": "JAW Gold",
"doi-asserted-by": "publisher",
"first-page": "466",
"journal-title": "Public Health Rep",
"key": "152_CR9",
"unstructured": "Gold JAW, et al. COVID-19 Case Surveillance: Trends in Person-Level Case Data Completeness, United States, April 5-September 30, 2020. Public Health Rep. 2021;136:466–74.",
"volume": "136",
"year": "2021"
},
{
"DOI": "10.1007/s00134-020-06170-8",
"doi-asserted-by": "publisher",
"key": "152_CR10",
"unstructured": "Guillon A, Hiemstra PS, Si-Tahar M. Pulmonary immune responses against SARS-CoV-2 infection: harmful or not? Intensive Care Med. 2020;1–4. https://doi.org/10.1007/s00134-020-06170-8."
},
{
"DOI": "10.4049/jimmunol.1402513",
"author": "S Han",
"doi-asserted-by": "publisher",
"first-page": "855",
"journal-title": "J Immunol",
"key": "152_CR11",
"unstructured": "Han S, Mallampalli RK. The acute respiratory distress syndrome: from mechanism to translation. J Immunol. 2015;194:855–60.",
"volume": "194",
"year": "2015"
},
{
"DOI": "10.1016/j.jbi.2008.08.010",
"author": "PA Harris",
"doi-asserted-by": "publisher",
"first-page": "377",
"journal-title": "J Biomed Inform",
"key": "152_CR12",
"unstructured": "Harris PA, et al. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42:377–81.",
"volume": "42",
"year": "2009"
},
{
"DOI": "10.1016/j.jbi.2019.103208",
"author": "PA Harris",
"doi-asserted-by": "publisher",
"journal-title": "J Biomed Inform",
"key": "152_CR13",
"unstructured": "Harris PA, et al. The REDCap Consortium: Building an International Community of Software Platform Partners. J Biomed Inform. 2019;95:103208.",
"volume": "95",
"year": "2019"
},
{
"key": "152_CR14",
"unstructured": "Hospitalized Adults: Therapeutic Management. COVID-19 Treatment Guidelines https://www.covid19treatmentguidelines.nih.gov/management/clinical-management/hospitalized-adults%2D%2Dtherapeutic-management/. Accessed 1 Oct 2021."
},
{
"author": "JPA Ioannidis",
"journal-title": "Eur J Clin Invest",
"key": "152_CR15",
"unstructured": "Ioannidis JPA. Global perspective of COVID-19 epidemiology for a full-cycle pandemic. Eur J Clin Invest. 2020;50:e13423.",
"volume": "50",
"year": "2020"
},
{
"DOI": "10.1038/nm1561",
"author": "K Maresz",
"doi-asserted-by": "publisher",
"first-page": "492",
"journal-title": "Nat Med",
"key": "152_CR16",
"unstructured": "Maresz K, et al. Direct suppression of CNS autoimmune inflammation via the cannabinoid receptor CB1 on neurons and CB2 on autoreactive T cells. Nat Med. 2007;13:492–7.",
"volume": "13",
"year": "2007"
},
{
"DOI": "10.1155/2005/242516",
"author": "IJ McGilveray",
"doi-asserted-by": "publisher",
"first-page": "15A",
"issue": "Suppl A",
"journal-title": "Pain Res Manag",
"key": "152_CR17",
"unstructured": "McGilveray IJ. Pharmacokinetics of cannabinoids. Pain Res Manag. 2005;10(Suppl A):15A–22A.",
"volume": "10",
"year": "2005"
},
{
"DOI": "10.3390/ijms21176244",
"doi-asserted-by": "crossref",
"key": "152_CR18",
"unstructured": "Mohammed A, et al. Δ9-Tetrahydrocannabinol Prevents Mortality from Acute Respiratory Distress Syndrome through the Induction of Apoptosis in Immune Cells, Leading to Cytokine Storm Suppression. Int J Mol Sci. 21(17):6244."
},
{
"DOI": "10.1111/j.1525-1497.2004.40081.x",
"author": "BA Moore",
"doi-asserted-by": "publisher",
"first-page": "33",
"journal-title": "J Gen Intern Med",
"key": "152_CR19",
"unstructured": "Moore BA, Augustson EM, Moser RP, Budney AJ. Respiratory Effects of Marijuana and Tobacco Use in a U.S. Sample. J Gen Intern Med. 2005;20:33–7.",
"volume": "20",
"year": "2005"
},
{
"DOI": "10.2144/fsoa-2020-0124",
"doi-asserted-by": "crossref",
"key": "152_CR20",
"unstructured": "Onaivi ES, Sharma V. Cannabis for COVID-19: can cannabinoids quell the cytokine storm? Fut Sci OA. 2020;6:FSO625."
},
{
"DOI": "10.3389/fimmu.2021.631233",
"author": "N Paland",
"doi-asserted-by": "publisher",
"journal-title": "Front Immunol",
"key": "152_CR21",
"unstructured": "Paland N, et al. The Immunopathology of COVID-19 and the Cannabis Paradigm. Front Immunol. 2021;12:631233.",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.1093/ntr/ntaa082",
"author": "R Patanavanich",
"doi-asserted-by": "publisher",
"first-page": "1653",
"journal-title": "Nicotine Tob Res",
"key": "152_CR22",
"unstructured": "Patanavanich R, Glantz SA. Smoking Is Associated With COVID-19 Progression: A Meta-analysis. Nicotine Tob Res. 2020;22:1653–6.",
"volume": "22",
"year": "2020"
},
{
"DOI": "10.1007/s15010-021-01615-8",
"doi-asserted-by": "publisher",
"key": "152_CR23",
"unstructured": "Pink I, et al. C-reactive protein and procalcitonin for antimicrobial stewardship in COVID-19. Infection. 2021. https://doi.org/10.1007/s15010-021-01615-8."
},
{
"key": "152_CR24",
"unstructured": "Recent Trends in Marijuana Use In Los Angeles County. (2018)."
},
{
"DOI": "10.1016/j.drugpo.2017.11.008",
"author": "C Russell",
"doi-asserted-by": "publisher",
"first-page": "87",
"journal-title": "Int J Drug Policy",
"key": "152_CR25",
"unstructured": "Russell C, Rueda S, Room R, Tyndall M, Fischer B. Routes of administration for cannabis use - basic prevalence and related health outcomes: A scoping review and synthesis. Int J Drug Policy. 2018;52:87–96.",
"volume": "52",
"year": "2018"
},
{
"DOI": "10.1002/jmv.27233",
"doi-asserted-by": "publisher",
"key": "152_CR26",
"unstructured": "Saadatian-Elahi M, et al. Tobacco smoking and severity of COVID-19: Experience from a hospital-based prospective cohort study in Lyon, France. J Med Virol. 2021:10.1002/jmv.27233. https://doi.org/10.1002/jmv.27233."
},
{
"DOI": "10.1080/00952990.2019.1627366",
"author": "DP Tashkin",
"doi-asserted-by": "publisher",
"first-page": "596",
"journal-title": "Am J Drug Alcohol Abuse",
"key": "152_CR27",
"unstructured": "Tashkin DP, Roth MD. Pulmonary effects of inhaled cannabis smoke. Am J Drug Alcohol Abuse. 2019;45:596–609.",
"volume": "45",
"year": "2019"
},
{
"DOI": "10.1016/S2213-2600(20)30360-X",
"author": "The Lancet Respiratory Medicine",
"doi-asserted-by": "publisher",
"first-page": "831",
"journal-title": "Lancet Respir Med",
"key": "152_CR28",
"unstructured": "The Lancet Respiratory Medicine. The EVALI outbreak and vaping in the COVID-19 era. Lancet Respir Med. 2020;8:831.",
"volume": "8",
"year": "2020"
},
{
"DOI": "10.1021/acs.jnatprod.1c00946",
"doi-asserted-by": "publisher",
"key": "152_CR29",
"unstructured": "van Breemen RB, et al. Cannabinoids Block Cellular Entry of SARS-CoV-2 and the Emerging Variants. J Nat Prod. 2022. https://doi.org/10.1021/acs.jnatprod.1c00946."
},
{
"DOI": "10.1002/wps.20921",
"doi-asserted-by": "publisher",
"key": "152_CR30",
"unstructured": "Wang L, Wang Q, Davis PB, Volkow ND, Xu R. Increased risk for COVID-19 breakthrough infection in fully vaccinated patients with substance use disorders in the United States between December 2020 and August 2021. World Psychiatry. 2021a:10.1002/wps.20921. https://doi.org/10.1002/wps.20921."
},
{
"DOI": "10.1038/s41380-020-00880-7",
"author": "QQ Wang",
"doi-asserted-by": "publisher",
"first-page": "30",
"journal-title": "Mol Psychiatry",
"key": "152_CR31",
"unstructured": "Wang QQ, Kaelber DC, Xu R, Volkow ND. COVID-19 risk and outcomes in patients with substance use disorders: analyses from electronic health records in the United States. Mol Psychiatry. 2021b;26:30–9.",
"volume": "26",
"year": "2021"
}
],
"reference-count": 31,
"references-count": 31,
"relation": {},
"resource": {
"primary": {
"URL": "https://jcannabisresearch.biomedcentral.com/articles/10.1186/s42238-022-00152-x"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Cannabis consumption is associated with lower COVID-19 severity among hospitalized patients: a retrospective cohort analysis",
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "4"
}