Associations of pre-pandemic levels of physical function and physical activity with COVID-19-like symptoms during the outbreak
et al., Aging Clinical and Experimental Research, doi:10.1007/s40520-021-02006-7, Oct 2021
Exercise for COVID-19
9th treatment shown to reduce risk in
October 2020, now with p < 0.00000000001 from 68 studies.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
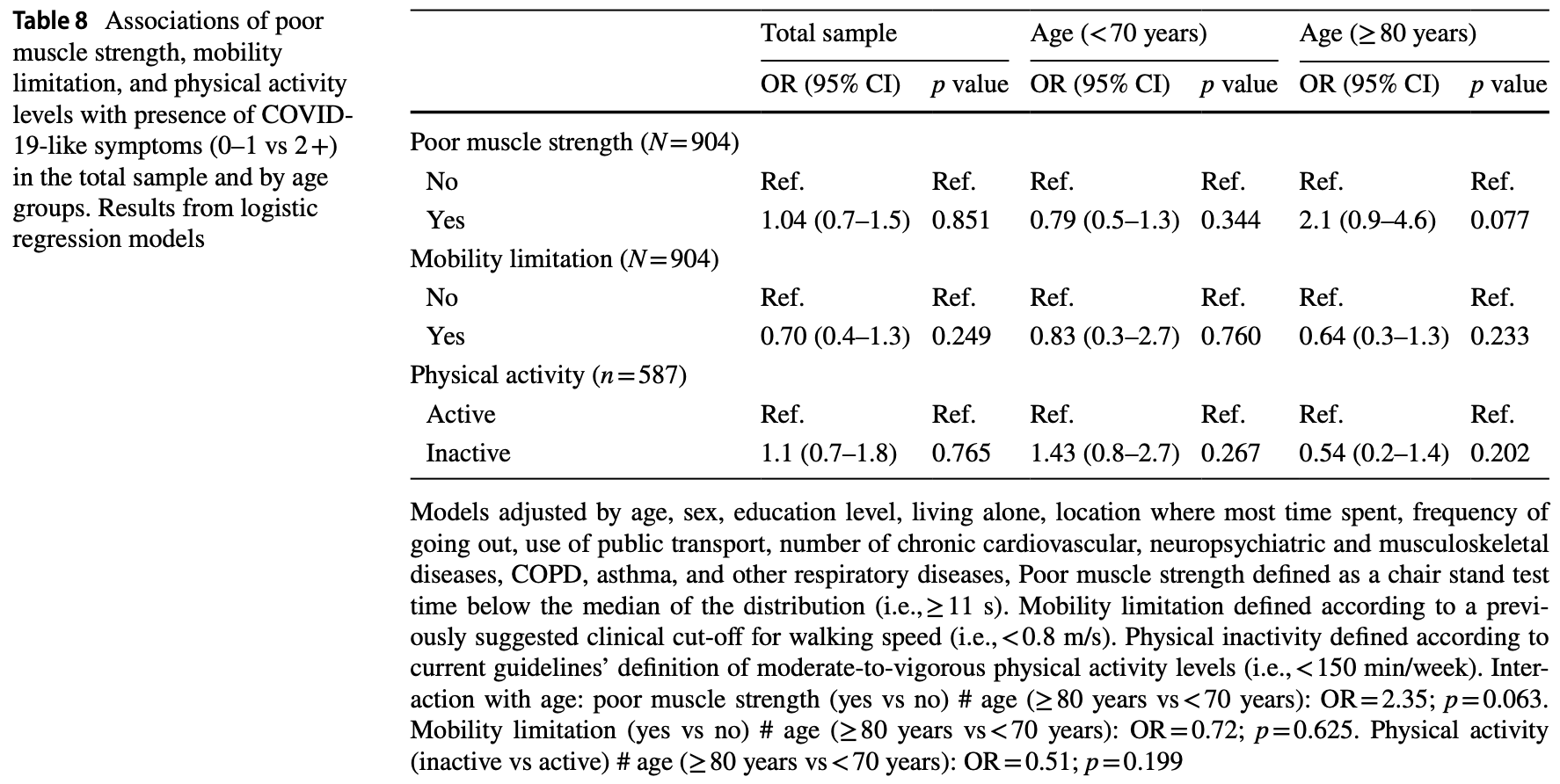
Retrospective 904 patients in Sweden, showing higher risk of COVID-19-like symptoms with poor muscle strength. Risk was slightly higher for physical inactivity, without statistical significance.
|
risk of symptomatic case, 9.1% lower, OR 0.91, p = 0.71, high activity levels 362, low activity levels 225, adjusted per study, inverted to make OR<1 favor high activity levels, 2+ symptoms, Table 8, physically active vs. inactive, multivariable, RR approximated with OR.
|
|
risk of symptomatic case, 3.8% lower, OR 0.96, p = 0.85, high activity levels 362, low activity levels 225, adjusted per study, inverted to make OR<1 favor high activity levels, 1+ symptoms, Table 2, model 2, physically active vs. inactive, multivariable, RR approximated with OR.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Saadeh et al., 30 Oct 2021, retrospective, Sweden, peer-reviewed, 6 authors, study period March 2020 - June 2020.
Associations of pre-pandemic levels of physical function and physical activity with COVID-19-like symptoms during the outbreak
Aging Clinical and Experimental Research, doi:10.1007/s40520-021-02006-7
Background One's physical function and physical activity levels can predispose or protect from the development of respiratory infections. We aimed to explore the associations between pre-pandemic levels of physical function and physical activity and the development of COVID-19-like symptoms in Swedish older adults. Methods We analyzed data from 904 individuals aged ≥ 68 years from the population-based Swedish National study on Aging and Care in Kungsholmen. COVID-19-like symptoms were assessed by phone interview (March-June 2020) and included fever, cough, sore throat and/or a cold, headache, pain in muscles, legs and joints, loss of taste and/or odor, breathing difficulties, chest pain, gastrointestinal symptoms, and eye inflammation. Muscle strength, mobility, and physical activity were examined in 2016-2018 by objective testing. Data were analyzed using logistic regression models in the total sample and stratifying by age. Results During the first outbreak of the pandemic, 325 (36%) individuals from our sample developed COVID-19-like symptoms. Those with slower performance in the chair stand test had an odds ratio (OR) of 1.5 (95% confidence interval [CI] 1.1-2.1) for presenting with COVID-19-like symptoms compared to better performers, after adjusting for potential confounders. The association was even higher among people aged ≥ 80 years (OR 2.6; 95% CI 1.5-4.7). No significant associations were found between walking speed or engagement in moderate-to-vigorous physical activity and the likelihood to develop COVID-19-like symptoms. Conclusion Poor muscle strength, a possible indicator of frailty, may predispose older adults to higher odds of developing COVID-19-like symptoms, especially among the oldest-old.
Author contributions M Saadeh and A-K Welmer developed the study concept and design. M Saadeh performed the data analysis and drafted the manuscript. M Saadeh, A-K Welmer, A Calderón-Larrañaga, D L. Vetrano, P von Rosen, and L Fratiglioni interpreted the data. All authors provided critical revisions and approved the final version of the manuscript for submission. Funding Open access funding provided by Karolinska Institute. This work was supported by the funders of The Swedish National study on Aging and Care (SNAC): the Ministry of Health and Social Affairs, Sweden; the participating county councils and municipalities; and the Swedish Research Council. Specific grants were obtained from the Swedish Research Council (2017-06088); the Swedish Research Council for Health, Working Life and Welfare (2016-07175); Karolinska Institutet's Strategic Young Scholar Grants in Epidemiology or Biostatistics (SFO-EPI); and the Swedish National Graduate School on Ageing and Health (SWEAH). A specific grant was obtained for this study from the Swedish Research Council (2020-05931). The financial sponsors played no role in the design, execution, analysis and interpretation of data, or writing of the study.
Declarations Conflict of interest The authors declare that they have no competing interests.
Statement of human and animal rights
Informed consent The principles of autonomy and integrity, the rule of consent and the demand for research.
Consent for publication Not applicable. Open..
References
Adorni, Prinelli, Bianchi, Self-reported symptoms of SARS-CoV-2 infection in a nonhospitalized population in Italy: cross-sectional study of the EPICOVID19 Web-Based Survey, JMIR Public Health Surveill
Akınoğlu, Kocahan, Özkan, The relationship between peripheral muscle strength and respiratory function and respiratory muscle strength in athletes, J Exerc Rehabil
Bonanad, García-Blas, Tarazona-Santabalbina, The effect of age on mortality in patients with COVID-19: a metaanalysis with 611,583 subjects, J Am Med Dir Assoc
Calderón-Larrañaga, Vetrano, Onder, Assessing and measuring chronic multimorbidity in the older population: a proposal for its operationalization, J Gerontol Ser A
Campbell, Turner, Debunking the myth of exerciseinduced immune suppression: redefining the impact of exercise on immunological health across the lifespan, Front Immunol
Carfì, Bernabei, Landi, Persistent symptoms in patients after acute COVID-19, JAMA
Cheval, Sieber, Maltagliati, Muscle strength is associated with COVID-19 hospitalization in adults 50 years of age and older, medRxiv
Clegg, Barber, Young, The Home-based Older People's Exercise (HOPE) trial: a pilot randomised controlled trial of a home-based exercise intervention for older people with frailty, Age Ageing
Cucinotta, Vanelli, WHO declares COVID-19 a pandemic, Acta Biomed
Dinh, Njemini, Onyema, Strength endurance training but not intensive strength training reduces senescence-prone T cells in peripheral blood in community-dwelling elderly women, J Gerontol Ser A
Dohrn, Gardiner, Winkler, Device-measured sedentary behavior and physical activity in older adults differ by demographic and health-related factors, Eur Rev Aging Phys Act
Edwardson, Winkler, Bodicoat, Considerations when using the activPAL monitor in field-based research with adult populations, J Sport Heal Sci
Ekram, Woods, Britt, The association between frailty and all-cause mortality in communitydwelling older individuals: an umbrella review, J Frailty Aging
Folkhälsomyndigheten, Groups at risk of serious illness
Fried, Tangen, Walston, Frailty in older adults: evidence for a phenotype, J Gerontol Ser A
Fritz, Lusardi, White paper: "walking speed: the sixth vital sign, J Geriatr Phys Ther
Hewitt, Carter, Vilches-Moraga, The effect of frailty on survival in patients with COVID-19 (COPE): a multicentre, European, observational cohort study, Lancet Public Heal
Huang, Lu, Huang, Obesity in patients with COVID-19: a systematic review and meta-analysis, Metabolism
Kapasi, Ouslander, Schnelle, Effects of an exercise intervention on immunologic parameters in frail elderly nursing home residents, J Gerontol Ser A
Kehler, Theou, The impact of physical activity and sedentary behaviors on frailty levels, Mech Ageing Dev
Kirwan, Mccullough, Butler, Sarcopenia during COVID-19 lockdown restrictions: long-term health effects of short-term muscle loss, GeroScience
Kumar, Arora, Sharma, Is diabetes mellitus associated with mortality and severity of COVID-19? A metaanalysis, Diabetes Metab Syndr
Lavie, Ozemek, Carbone, Sedentary behavior, exercise, and cardiovascular health, Circ Res
Maltese, Corsonello, Rosa, Frailty and COVID-19: a systematic scoping review, J Clin Med
Marengoni, Zucchelli, Vetrano, Beyond chronological age: frailty and multimorbidity predict, J Gerontol A Biol Sci Med Sci
Nelke, Dziewas, Minnerup, Skeletal muscle as potential central link between sarcopenia and immune senescence, EBioMedicine
Nieman, Henson, Austin, Upper respiratory tract infection is reduced in physically fit and active adults, Br J Sports Med
Nieman, Wentz, The compelling link between physical activity and the body's defense system, J Sport Heal Sci
Pranata, Henrina, Lim, Clinical frailty scale and mortality in COVID-19: a systematic review and doseresponse meta-analysis: clinical frailty scale in COVID-19, Arch Gerontol Geriatr
Saadeh, Welmer, Dekhtyar, The role of psychological and social well-being on physical function trajectories in older adults, J Gerontol Ser A, doi:10.1093/gerona/glaa114
Simpson, Lowder, Spielmann, Exercise and the aging immune system, Ageing Res Rev
Studenski, Gait speed and survival in older adults, JAMA
Tudor-Locke, Han, Aguiar, How fast is fast enough? Walking cadence (steps/min) as a practical estimate of intensity in adults: a narrative review, Br J Sports Med
Unim, Palmieri, Noce, Prevalence of COVID-19-related symptoms by age group, Aging Clin Exp Res
Woods, Ceddia, Wolters, Effects of 6 months of moderate aerobic exercise training on immune function in the elderly, Mech Ageing Dev
Yates, Razieh, Zaccardi, Obesity, walking pace and risk of severe COVID-19: analysis of UK Biobank, medRxiv
DOI record:
{
"DOI": "10.1007/s40520-021-02006-7",
"ISSN": [
"1720-8319"
],
"URL": "http://dx.doi.org/10.1007/s40520-021-02006-7",
"abstract": "<jats:title>Abstract</jats:title><jats:sec>\n <jats:title>Background</jats:title>\n <jats:p>One’s physical function and physical activity levels can predispose or protect from the development of respiratory infections. We aimed to explore the associations between pre-pandemic levels of physical function and physical activity and the development of COVID-19-like symptoms in Swedish older adults.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Methods</jats:title>\n <jats:p>We analyzed data from 904 individuals aged ≥ 68 years from the population-based Swedish National study on Aging and Care in Kungsholmen. COVID-19-like symptoms were assessed by phone interview (March–June 2020) and included fever, cough, sore throat and/or a cold, headache, pain in muscles, legs and joints, loss of taste and/or odor, breathing difficulties, chest pain, gastrointestinal symptoms, and eye inflammation. Muscle strength, mobility, and physical activity were examined in 2016–2018 by objective testing. Data were analyzed using logistic regression models in the total sample and stratifying by age.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Results</jats:title>\n <jats:p>During the first outbreak of the pandemic, 325 (36%) individuals from our sample developed COVID-19-like symptoms. Those with slower performance in the chair stand test had an odds ratio (OR) of 1.5 (95% confidence interval [CI] 1.1–2.1) for presenting with COVID-19-like symptoms compared to better performers, after adjusting for potential confounders. The association was even higher among people aged ≥ 80 years (OR 2.6; 95% CI 1.5–4.7). No significant associations were found between walking speed or engagement in moderate-to-vigorous physical activity and the likelihood to develop COVID-19-like symptoms.</jats:p>\n </jats:sec><jats:sec>\n <jats:title>Conclusion</jats:title>\n <jats:p>Poor muscle strength, a possible indicator of frailty, may predispose older adults to higher odds of developing COVID-19-like symptoms, especially among the oldest-old.</jats:p>\n </jats:sec>",
"alternative-id": [
"2006"
],
"assertion": [
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Received",
"name": "received",
"order": 1,
"value": "26 August 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "Accepted",
"name": "accepted",
"order": 2,
"value": "15 October 2021"
},
{
"group": {
"label": "Article History",
"name": "ArticleHistory"
},
"label": "First Online",
"name": "first_online",
"order": 3,
"value": "30 October 2021"
},
{
"group": {
"label": "Declarations",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 1
},
{
"group": {
"label": "Conflict of interest",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 2,
"value": "The authors declare that they have no competing interests."
},
{
"group": {
"label": "Statement of human and animal rights",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 3,
"value": "SNAC-K was approved by the Regional Ethical Review Board in Stockholm (Dnrs: 2001-114, 2004-929/3, 2007/279-31, 2010/2:4, 2013/3:6, 2016/730-31/1), and written informed consent was obtained from participants or their next of kin."
},
{
"group": {
"label": "Informed consent",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 4,
"value": "The principles of autonomy and integrity, the rule of consent and the demand for research."
},
{
"group": {
"label": "Consent for publication",
"name": "EthicsHeading"
},
"name": "Ethics",
"order": 5,
"value": "Not applicable."
}
],
"author": [
{
"ORCID": "http://orcid.org/0000-0002-2689-5784",
"affiliation": [],
"authenticated-orcid": false,
"family": "Saadeh",
"given": "Marguerita",
"sequence": "first"
},
{
"affiliation": [],
"family": "Calderón-Larrañaga",
"given": "Amaia",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Vetrano",
"given": "Davide Liborio",
"sequence": "additional"
},
{
"affiliation": [],
"family": "von Rosen",
"given": "Philip",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Fratiglioni",
"given": "Laura",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Welmer",
"given": "Anna-Karin",
"sequence": "additional"
}
],
"container-title": [
"Aging Clinical and Experimental Research"
],
"content-domain": {
"crossmark-restriction": false,
"domain": [
"link.springer.com"
]
},
"created": {
"date-parts": [
[
2021,
10,
30
]
],
"date-time": "2021-10-30T06:17:31Z",
"timestamp": 1635574651000
},
"deposited": {
"date-parts": [
[
2022,
1,
27
]
],
"date-time": "2022-01-27T10:27:37Z",
"timestamp": 1643279257000
},
"funder": [
{
"DOI": "10.13039/501100004359",
"award": [
"(2020-05931)",
"(2017-06088)"
],
"doi-asserted-by": "crossref",
"name": "Vetenskapsrådet"
},
{
"DOI": "10.13039/501100006636",
"award": [
"(2016-07175)"
],
"doi-asserted-by": "publisher",
"name": "Forskningsrådet om Hälsa, Arbetsliv och Välfärd"
},
{
"DOI": "10.13039/501100001861",
"award": [
"(2016-07175)"
],
"doi-asserted-by": "publisher",
"name": "Forskningsrådet för Arbetsliv och Socialvetenskap"
},
{
"DOI": "10.13039/501100004047",
"doi-asserted-by": "crossref",
"name": "Karolinska Institute"
}
],
"indexed": {
"date-parts": [
[
2022,
4,
3
]
],
"date-time": "2022-04-03T16:44:26Z",
"timestamp": 1649004266676
},
"is-referenced-by-count": 0,
"issn-type": [
{
"type": "electronic",
"value": "1720-8319"
}
],
"issue": "1",
"issued": {
"date-parts": [
[
2021,
10,
30
]
]
},
"journal-issue": {
"issue": "1",
"published-print": {
"date-parts": [
[
2022,
1
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "tdm",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
10,
30
]
],
"date-time": "2021-10-30T00:00:00Z",
"timestamp": 1635552000000
}
},
{
"URL": "https://creativecommons.org/licenses/by/4.0",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2021,
10,
30
]
],
"date-time": "2021-10-30T00:00:00Z",
"timestamp": 1635552000000
}
}
],
"link": [
{
"URL": "https://link.springer.com/content/pdf/10.1007/s40520-021-02006-7.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/article/10.1007/s40520-021-02006-7/fulltext.html",
"content-type": "text/html",
"content-version": "vor",
"intended-application": "text-mining"
},
{
"URL": "https://link.springer.com/content/pdf/10.1007/s40520-021-02006-7.pdf",
"content-type": "application/pdf",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "297",
"original-title": [],
"page": "235-247",
"prefix": "10.1007",
"published": {
"date-parts": [
[
2021,
10,
30
]
]
},
"published-online": {
"date-parts": [
[
2021,
10,
30
]
]
},
"published-print": {
"date-parts": [
[
2022,
1
]
]
},
"publisher": "Springer Science and Business Media LLC",
"reference": [
{
"key": "2006_CR1",
"unstructured": "World Health Organization (2021) Coronavirus [Internet]. Available from: https://www.who.int/health-topics/coronavirus#tab=tab_3"
},
{
"key": "2006_CR2",
"unstructured": "Folkhälsomyndigheten (2021) Groups at risk of serious illness [Internet]. Available from: https://www.folkhalsomyndigheten.se/the-public-health-agency-of-sweden/communicable-disease-control/covid-19/covid-19-and-at-risk-groups/"
},
{
"DOI": "10.2196/21866",
"author": "F Adorni",
"doi-asserted-by": "publisher",
"first-page": "e21866",
"journal-title": "JMIR Public Health Surveill",
"key": "2006_CR3",
"unstructured": "Adorni F, Prinelli F, Bianchi F et al (2020) Self-reported symptoms of SARS-CoV-2 infection in a nonhospitalized population in Italy: cross-sectional study of the EPICOVID19 Web-Based Survey. JMIR Public Health Surveill 6:e21866",
"volume": "6",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.12603",
"author": "A Carfì",
"doi-asserted-by": "publisher",
"first-page": "603",
"journal-title": "JAMA",
"key": "2006_CR4",
"unstructured": "Carfì A, Bernabei R, Landi F (2020) Persistent symptoms in patients after acute COVID-19. JAMA 324:603",
"volume": "324",
"year": "2020"
},
{
"DOI": "10.21203/rs.3.rs-84994/v1",
"doi-asserted-by": "crossref",
"key": "2006_CR5",
"unstructured": "Ekram ARMS, Woods RL, Britt C et al (2021) The association between frailty and all-cause mortality in community-dwelling older individuals: an umbrella review. J Frailty Aging 10:320–326"
},
{
"DOI": "10.12965/jer.1836518.259",
"author": "B Akınoğlu",
"doi-asserted-by": "publisher",
"first-page": "44",
"journal-title": "J Exerc Rehabil",
"key": "2006_CR6",
"unstructured": "Akınoğlu B, Kocahan T, Özkan T (2019) The relationship between peripheral muscle strength and respiratory function and respiratory muscle strength in athletes. J Exerc Rehabil 15:44–49",
"volume": "15",
"year": "2019"
},
{
"DOI": "10.1016/j.ebiom.2019.10.034",
"author": "C Nelke",
"doi-asserted-by": "publisher",
"first-page": "381",
"journal-title": "EBioMedicine",
"key": "2006_CR7",
"unstructured": "Nelke C, Dziewas R, Minnerup J et al (2019) Skeletal muscle as potential central link between sarcopenia and immune senescence. EBioMedicine 49:381–388",
"volume": "49",
"year": "2019"
},
{
"DOI": "10.1519/00139143-200932020-00002",
"author": "S Fritz",
"doi-asserted-by": "publisher",
"first-page": "46",
"journal-title": "J Geriatr Phys Ther",
"key": "2006_CR8",
"unstructured": "Fritz S, Lusardi M (2009) White paper: “walking speed: the sixth vital sign.” J Geriatr Phys Ther 32:46–49",
"volume": "32",
"year": "2009"
},
{
"DOI": "10.1016/j.mad.2019.03.004",
"author": "DS Kehler",
"doi-asserted-by": "publisher",
"first-page": "29",
"journal-title": "Mech Ageing Dev",
"key": "2006_CR9",
"unstructured": "Kehler DS, Theou O (2019) The impact of physical activity and sedentary behaviors on frailty levels. Mech Ageing Dev 180:29–41",
"volume": "180",
"year": "2019"
},
{
"DOI": "10.1161/CIRCRESAHA.118.312669",
"author": "CJ Lavie",
"doi-asserted-by": "publisher",
"first-page": "799",
"journal-title": "Circ Res",
"key": "2006_CR10",
"unstructured": "Lavie CJ, Ozemek C, Carbone S et al (2019) Sedentary behavior, exercise, and cardiovascular health. Circ Res 124:799–815",
"volume": "124",
"year": "2019"
},
{
"DOI": "10.1136/bjsm.2010.077875",
"author": "DC Nieman",
"doi-asserted-by": "publisher",
"first-page": "987",
"journal-title": "Br J Sports Med",
"key": "2006_CR11",
"unstructured": "Nieman DC, Henson DA, Austin MD et al (2011) Upper respiratory tract infection is reduced in physically fit and active adults. Br J Sports Med 45:987–992",
"volume": "45",
"year": "2011"
},
{
"author": "D Cucinotta",
"first-page": "157",
"journal-title": "Acta Biomed",
"key": "2006_CR12",
"unstructured": "Cucinotta D, Vanelli M (2020) WHO declares COVID-19 a pandemic. Acta Biomed 91:157–160",
"volume": "91",
"year": "2020"
},
{
"DOI": "10.1186/s11556-020-00241-x",
"author": "IM Dohrn",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Eur Rev Aging Phys Act",
"key": "2006_CR13",
"unstructured": "Dohrn IM, Gardiner PA, Winkler E et al (2020) Device-measured sedentary behavior and physical activity in older adults differ by demographic and health-related factors. Eur Rev Aging Phys Act 17:1–11",
"volume": "17",
"year": "2020"
},
{
"DOI": "10.1093/gerona/glaa114",
"author": "M Saadeh",
"doi-asserted-by": "publisher",
"journal-title": "J Gerontol Ser A",
"key": "2006_CR14",
"unstructured": "Saadeh M, Welmer A-K, Dekhtyar S et al (2020) The role of psychological and social well-being on physical function trajectories in older adults. J Gerontol Ser A. https://doi.org/10.1093/gerona/glaa114",
"year": "2020"
},
{
"DOI": "10.1001/jama.2010.1923",
"author": "S Studenski",
"doi-asserted-by": "publisher",
"first-page": "50",
"journal-title": "JAMA",
"key": "2006_CR15",
"unstructured": "Studenski S (2011) Gait speed and survival in older adults. JAMA 305:50",
"volume": "305",
"year": "2011"
},
{
"DOI": "10.1016/j.jshs.2016.02.002",
"author": "CL Edwardson",
"doi-asserted-by": "publisher",
"first-page": "162",
"journal-title": "J Sport Heal Sci",
"key": "2006_CR16",
"unstructured": "Edwardson CL, Winkler EAH, Bodicoat DH et al (2017) Considerations when using the activPAL monitor in field-based research with adult populations. J Sport Heal Sci 6:162–178",
"volume": "6",
"year": "2017"
},
{
"key": "2006_CR17",
"unstructured": "World Health Organization (2020 Public consultation on the draft WHO Guidelines on physical activity and sedentary behaviour for children and adolescents, adults and older adults 2020 [Internet]. Available from: https://www.who.int/news-room/articles-detail/public-consultation-on-the-draft-who-guidelines-on-physical-activity-and-sedentary-behaviour-for-children-and-adolescents-adults-and-older-adults-2020"
},
{
"DOI": "10.1136/bjsports-2017-097628",
"author": "C Tudor-Locke",
"doi-asserted-by": "publisher",
"first-page": "776",
"journal-title": "Br J Sports Med",
"key": "2006_CR18",
"unstructured": "Tudor-Locke C, Han H, Aguiar EJ et al (2018) How fast is fast enough? Walking cadence (steps/min) as a practical estimate of intensity in adults: a narrative review. Br J Sports Med 52:776–788",
"volume": "52",
"year": "2018"
},
{
"author": "A Calderón-Larrañaga",
"first-page": "1417",
"journal-title": "J Gerontol Ser A",
"key": "2006_CR19",
"unstructured": "Calderón-Larrañaga A, Vetrano DL, Onder G et al (2017) Assessing and measuring chronic multimorbidity in the older population: a proposal for its operationalization. J Gerontol Ser A 72:1417–1423",
"volume": "72",
"year": "2017"
},
{
"DOI": "10.1016/j.dsx.2020.04.044",
"author": "A Kumar",
"doi-asserted-by": "publisher",
"first-page": "535",
"journal-title": "Diabetes Metab Syndr",
"key": "2006_CR20",
"unstructured": "Kumar A, Arora A, Sharma P et al (2020) Is diabetes mellitus associated with mortality and severity of COVID-19? A meta-analysis. Diabetes Metab Syndr 14:535–545",
"volume": "14",
"year": "2020"
},
{
"DOI": "10.1016/j.metabol.2020.154378",
"author": "Y Huang",
"doi-asserted-by": "publisher",
"first-page": "154378",
"journal-title": "Metabolism",
"key": "2006_CR21",
"unstructured": "Huang Y, Lu Y, Huang Y-M et al (2020) Obesity in patients with COVID-19: a systematic review and meta-analysis. Metabolism 113:154378",
"volume": "113",
"year": "2020"
},
{
"DOI": "10.1093/gerona/glaa291",
"doi-asserted-by": "crossref",
"key": "2006_CR22",
"unstructured": "Marengoni A, Zucchelli A, Vetrano DL et al (2021) Beyond chronological age: frailty and multimorbidity predict. J Gerontol A Biol Sci Med Sci 76: 38–45"
},
{
"DOI": "10.1007/s40520-021-01809-y",
"author": "B Unim",
"doi-asserted-by": "publisher",
"first-page": "1145",
"journal-title": "Aging Clin Exp Res",
"key": "2006_CR23",
"unstructured": "Unim B, Palmieri L, Lo Noce C et al (2021) Prevalence of COVID-19-related symptoms by age group. Aging Clin Exp Res 33:1145–1147",
"volume": "33",
"year": "2021"
},
{
"DOI": "10.1093/gerona/56.3.M146",
"author": "LP Fried",
"doi-asserted-by": "publisher",
"first-page": "M146",
"journal-title": "J Gerontol Ser A",
"key": "2006_CR24",
"unstructured": "Fried LP, Tangen CM, Walston J et al (2001) Frailty in older adults: evidence for a phenotype. J Gerontol Ser A 56:M146–M157",
"volume": "56",
"year": "2001"
},
{
"DOI": "10.1016/j.archger.2020.104324",
"author": "R Pranata",
"doi-asserted-by": "publisher",
"first-page": "104324",
"journal-title": "Arch Gerontol Geriatr",
"key": "2006_CR25",
"unstructured": "Pranata R, Henrina J, Lim MA et al (2021) Clinical frailty scale and mortality in COVID-19: a systematic review and dose-response meta-analysis: clinical frailty scale in COVID-19. Arch Gerontol Geriatr 93:104324",
"volume": "93",
"year": "2021"
},
{
"DOI": "10.3390/jcm9072106",
"author": "G Maltese",
"doi-asserted-by": "publisher",
"first-page": "2106",
"journal-title": "J Clin Med",
"key": "2006_CR26",
"unstructured": "Maltese G, Corsonello A, Di Rosa M et al (2020) Frailty and COVID-19: a systematic scoping review. J Clin Med 9:2106",
"volume": "9",
"year": "2020"
},
{
"DOI": "10.1016/S2468-2667(20)30146-8",
"author": "J Hewitt",
"doi-asserted-by": "publisher",
"first-page": "e444",
"journal-title": "Lancet Public Heal",
"key": "2006_CR27",
"unstructured": "Hewitt J, Carter B, Vilches-Moraga A et al (2020) The effect of frailty on survival in patients with COVID-19 (COPE): a multicentre, European, observational cohort study. Lancet Public Heal 5:e444–e451",
"volume": "5",
"year": "2020"
},
{
"author": "B Cheval",
"first-page": "1529",
"journal-title": "medRxiv",
"key": "2006_CR28",
"unstructured": "Cheval B, Sieber S, Maltagliati S et al (2021) Muscle strength is associated with COVID-19 hospitalization in adults 50 years of age and older. medRxiv 65:1529",
"volume": "65",
"year": "2021"
},
{
"author": "T Yates",
"first-page": "1",
"journal-title": "medRxiv",
"key": "2006_CR29",
"unstructured": "Yates T, Razieh C, Zaccardi F et al (2020) Obesity, walking pace and risk of severe COVID-19: analysis of UK Biobank. medRxiv 200:1–11",
"volume": "200",
"year": "2020"
},
{
"DOI": "10.3389/fimmu.2018.00001",
"author": "JP Campbell",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Front Immunol",
"key": "2006_CR30",
"unstructured": "Campbell JP, Turner JE (2018) Debunking the myth of exercise-induced immune suppression: redefining the impact of exercise on immunological health across the lifespan. Front Immunol 9:1–21",
"volume": "9",
"year": "2018"
},
{
"DOI": "10.1093/ageing/afu033",
"author": "A Clegg",
"doi-asserted-by": "publisher",
"first-page": "687",
"journal-title": "Age Ageing",
"key": "2006_CR31",
"unstructured": "Clegg A, Barber S, Young J et al (2014) The Home-based Older People’s Exercise (HOPE) trial: a pilot randomised controlled trial of a home-based exercise intervention for older people with frailty. Age Ageing 43:687–695",
"volume": "43",
"year": "2014"
},
{
"DOI": "10.1016/j.jshs.2018.09.009",
"author": "DC Nieman",
"doi-asserted-by": "publisher",
"first-page": "201",
"journal-title": "J Sport Heal Sci",
"key": "2006_CR32",
"unstructured": "Nieman DC, Wentz LM (2019) The compelling link between physical activity and the body’s defense system. J Sport Heal Sci 8:201–217",
"volume": "8",
"year": "2019"
},
{
"DOI": "10.1093/gerona/58.7.M636",
"author": "ZF Kapasi",
"doi-asserted-by": "publisher",
"first-page": "M636",
"journal-title": "J Gerontol Ser A",
"key": "2006_CR33",
"unstructured": "Kapasi ZF, Ouslander JG, Schnelle JF et al (2003) Effects of an exercise intervention on immunologic parameters in frail elderly nursing home residents. J Gerontol Ser A 58:M636–M643",
"volume": "58",
"year": "2003"
},
{
"DOI": "10.1016/S0047-6374(99)00014-7",
"author": "JA Woods",
"doi-asserted-by": "publisher",
"first-page": "1",
"journal-title": "Mech Ageing Dev",
"key": "2006_CR34",
"unstructured": "Woods JA, Ceddia MA, Wolters BW et al (1999) Effects of 6 months of moderate aerobic exercise training on immune function in the elderly. Mech Ageing Dev 109:1–19",
"volume": "109",
"year": "1999"
},
{
"DOI": "10.1007/s11357-020-00272-3",
"author": "R Kirwan",
"doi-asserted-by": "publisher",
"first-page": "1547",
"journal-title": "GeroScience",
"key": "2006_CR35",
"unstructured": "Kirwan R, McCullough D, Butler T et al (2020) Sarcopenia during COVID-19 lockdown restrictions: long-term health effects of short-term muscle loss. GeroScience 42:1547–1578",
"volume": "42",
"year": "2020"
},
{
"DOI": "10.1016/j.jamda.2020.05.045",
"author": "C Bonanad",
"doi-asserted-by": "publisher",
"first-page": "915",
"journal-title": "J Am Med Dir Assoc",
"key": "2006_CR36",
"unstructured": "Bonanad C, García-Blas S, Tarazona-Santabalbina F et al (2020) The effect of age on mortality in patients with COVID-19: a meta-analysis with 611,583 subjects. J Am Med Dir Assoc 21:915–918",
"volume": "21",
"year": "2020"
},
{
"DOI": "10.1016/j.arr.2012.03.003",
"author": "RJ Simpson",
"doi-asserted-by": "publisher",
"first-page": "404",
"journal-title": "Ageing Res Rev",
"key": "2006_CR37",
"unstructured": "Simpson RJ, Lowder TW, Spielmann G et al (2012) Exercise and the aging immune system. Ageing Res Rev 11:404–420",
"volume": "11",
"year": "2012"
},
{
"DOI": "10.1093/gerona/gly229",
"author": "H Cao Dinh",
"doi-asserted-by": "publisher",
"first-page": "1870",
"journal-title": "J Gerontol Ser A",
"key": "2006_CR38",
"unstructured": "Cao Dinh H, Njemini R, Onyema OO et al (2019) Strength endurance training but not intensive strength training reduces senescence-prone T cells in peripheral blood in community-dwelling elderly women. J Gerontol Ser A 74:1870–1878",
"volume": "74",
"year": "2019"
}
],
"reference-count": 38,
"references-count": 38,
"relation": {},
"resource": {
"primary": {
"URL": "https://link.springer.com/10.1007/s40520-021-02006-7"
}
},
"score": 1,
"short-container-title": [
"Aging Clin Exp Res"
],
"short-title": [],
"source": "Crossref",
"subject": [
"Geriatrics and Gerontology",
"Aging"
],
"subtitle": [],
"title": [
"Associations of pre-pandemic levels of physical function and physical activity with COVID-19-like symptoms during the outbreak"
],
"type": "journal-article",
"update-policy": "http://dx.doi.org/10.1007/springer_crossmark_policy",
"volume": "34"
}
