Retrospective Assessment of Treatments of Hospitalized Covid-19 Patients
et al., medRxiv, doi:10.1101/2021.04.20.21255792, May 2021
Metformin for COVID-19
3rd treatment shown to reduce risk in
July 2020, now with p < 0.00000000001 from 112 studies.
Lower risk for mortality, ventilation, ICU, hospitalization, progression, recovery, and viral clearance.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
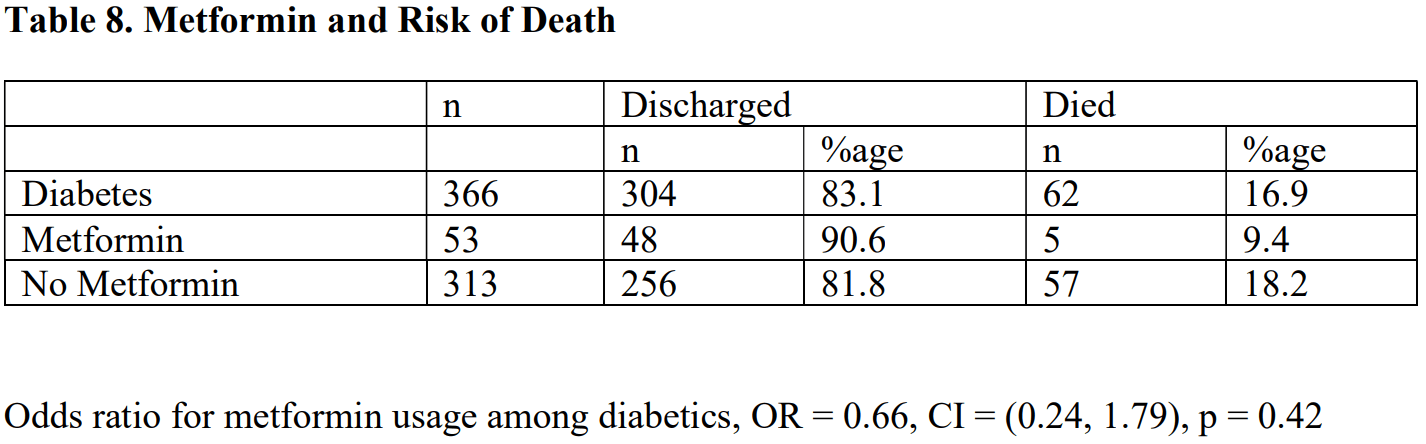
Retrospective 1,035 hospitalized patients in India. Of 366 diabetic patients, there was lower mortality for the 53 that were on metformin.
Although the 30% lower mortality is not statistically significant, it is consistent with the significant 36% lower mortality [32‑40%] from meta-analysis of the 74 mortality results to date.
This study is excluded in the after exclusion results of meta-analysis:
minimal details provided.
|
risk of death, 29.6% lower, RR 0.70, p = 0.42, treatment 5 of 53 (9.4%), control 57 of 313 (18.2%), adjusted per study, odds ratio converted to relative risk.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Ravindra et al., 5 May 2021, retrospective, India, peer-reviewed, 14 authors.
Retrospective Assessment of Treatments of Hospitalized Covid-19 Patients
doi:10.1101/2021.04.20.21255792
Infection with SARS-Cov-2 virus, is associated with significant morbidity and mortality, in addition to the economic burden it has put on the country. While waiting for a vaccine that gives adequate protection, it is necessary to understand the course of the infection and identify drugs that could reduce its impact. The results of this multicenter study involving 1035 hospitalized patients in Pune, identified diabetes, hypertension and low lymphocyte counts as predictors of mortality. There is also an indication that multiple comorbidities add to risk of severe disease and mortality. Data from metformin treated diabetics raises the possibility of considering repurposing of this drug in a larger study. It is also noted that Hydroxychloroquine, dexamethasone, azithromycin and remdesivir were associated with lower overall mortality. Diabetes and hypertension put Covid infected patients at greater risk of death, coexistence of both diseases further augment the risk, and must be aggressively treated.
References
Agarwal, Mukherjee, Kumar, Chatterjee, Bhatnagar et al., Convalescent plasma in the management of moderate covid-19 in adults in India: open label phase II multicentre randomised controlled trial (PLACID Trial), BMJ, doi:10.1136/bmj.m3939
Bello-Chavolla, Bahena-López, Antonio-Villa, Predicting Mortality Due to SARS-CoV-2: A Mechanistic Score Relating Obesity and Diabetes to COVID-19 Outcomes in Mexico, J Clin Endocrinol Metab, doi:10.1210/clinem/dgaa346
Bhadade, Harde, Desouza, Appraisal of Critically Ill COVID-19 Patients at a Dedicated COVID Hospital, J Assoc Physicians India
Bhadra, Mukherjee, Sarkar, Impact of population density on Covid-19 infected and mortality rate in India, Model Earth Syst Environ
Chakrabarti, Kaur, Singh, Chakrabarti, Krishnatreya et al., Of Cross-immunity, Herd Immunity and Country-specific Plans: Experiences from COVID-19 in India, Aging Dis
Debnath, Banerjee, Berk, Genetic gateways to COVID-19 infection: Implications for risk, severity, and outcomes, FASEB J
Erener, Diabetes, infection risk and COVID-19, Mol Metab, doi:10.1016/j.molmet.2020.101044
Fidel Pl, Noverr, Could an unrelated live attenuated vaccine serve as a preventive measure to dampen septic inflammation associated with COVID-19 infection?, mBio, doi:10.1128/mBio.00907-20
Jain, Yuan, Predictive symptoms and comorbidities for severe COVID-19 and intensive care unit admission: a systematic review and meta-analysis, Int J Public Health
Karadag, Increase in COVID-19 cases and case-fatality and case-recovery rates in Europe: A cross-temporal meta-analysis, J Med Virol
Khan, Adil, Alkhathlan, Tahir, Saif et al., COVID-19: A Global Challenge with Old History, Epidemiology and Progress So Far, Molecules, doi:10.3390/molecules26010039
Lally, Tsoukas, Halladay, Metformin is Associated with Decreased 30-Day Mortality Among Nursing Home Residents Infected with SARS-CoV2, J Am Med Dir Assoc
Madan, Pahuja, Mohan, Pandey, Madan et al., TB infection and BCG vaccination: are we protected from COVID-19?, Public Health
Mahajan, Kaushal, Epidemic Trend of COVID-19 Transmission in India During Lockdown-1 Phase, J Community Health
Mukherjee, COVID-19 and lockdown: Insights from Mumbai, Indian J Public Health
Pandey, Pathak, Pandey, Ivermectin in COVID-19: What do we know?, Diabetes Metab Syndr
Rawat, Kumari, Saha, COVID-19 vaccine: A recent update in pipeline vaccines, their design and development strategies, Eur J Pharmacol, doi:10.1016/j.ejphar.2020.173751
Richardson, Hirsch, Narasimhan, Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area, JAMA
Rod, Oviedo-Trespalacios, Cortes-Ramirez, A brief-review of the risk factors for covid-19 severity, Rev Saude Publica, doi:10.11606/s1518-8787.2020054002481
Singh, Singh, Modeling tempo of COVID-19 pandemic in India and significance of lockdown, J Public Aff, doi:10.1002/pa.2257
Stasi, Fallani, Voller, Silvestri, Treatment for COVID-19: An overview, Eur J Pharmacol, doi:10.1016/j.ejphar.2020.173644
Tadic, Cuspidi, Sala, COVID-19 and diabetes: Is there enough evidence?, J Clin Hypertens
Terpos, Ntanasis-Stathopoulos, Elalamy, Hematological findings and complications of COVID-19, Am J Hematol
Wiesner, Busch, David, Treatment of severe COVID-19 courses in intensive care medicine, Internist (Berl)
Wynants, Van Calster, Prediction models for diagnosis and prognosis of covid-19 infection: systematic review and critical appraisal, BMJ, doi:10.1136/bmj.m1328
Yang, Zheng, Gou, Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis, Int J Infect Dis
Ye, Fu, Ren, Wang, Wang et al., Treatment with convalescent plasma for COVID-19 patients in Wuhan, China, J Med Virol
DOI record:
{
"DOI": "10.1101/2021.04.20.21255792",
"URL": "http://dx.doi.org/10.1101/2021.04.20.21255792",
"abstract": "<jats:title>Abstract</jats:title><jats:p>Infection with SARS-Cov-2 virus, is associated with significant morbidity and mortality, in addition to the economic burden it has put on the country. While waiting for a vaccine that gives adequate protection, it is necessary to understand the course of the infection and identify drugs that could reduce its impact. The results of this multicenter study involving 1035 hospitalized patients in Pune, identified diabetes, hypertension and low lymphocyte counts as predictors of mortality. There is also an indication that multiple comorbidities add to risk of severe disease and mortality. Data from metformin treated diabetics raises the possibility of considering repurposing of this drug in a larger study. It is also noted that Hydroxychloroquine, dexamethasone, azithromycin and remdesivir were associated with lower overall mortality. Diabetes and hypertension put Covid infected patients at greater risk of death, coexistence of both diseases further augment the risk, and must be aggressively treated.</jats:p>",
"accepted": {
"date-parts": [
[
2021,
5,
5
]
]
},
"author": [
{
"affiliation": [],
"family": "Ravindra",
"given": "Ghooi",
"sequence": "first"
},
{
"affiliation": [],
"family": "Chitra",
"given": "Lele",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Madhur",
"given": "Motwani",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Santosh",
"given": "Dixit",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Venugopalan",
"given": "Premnath",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Sundeep",
"given": "Salvi",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Shreepad",
"given": "Bhat",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Piyush",
"given": "Chaudhari",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Pradeep",
"given": "D’Costa",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Ashwini",
"given": "Jahagirdar",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Abhay",
"given": "Mane",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Vikram",
"given": "Padbidri",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Chetan",
"given": "Pande",
"sequence": "additional"
},
{
"affiliation": [],
"family": "Urvi",
"given": "Shukla",
"sequence": "additional"
}
],
"container-title": [],
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2021,
4,
24
]
],
"date-time": "2021-04-24T04:50:36Z",
"timestamp": 1619239836000
},
"deposited": {
"date-parts": [
[
2021,
5,
6
]
],
"date-time": "2021-05-06T15:17:14Z",
"timestamp": 1620314234000
},
"group-title": "Epidemiology",
"indexed": {
"date-parts": [
[
2022,
4,
5
]
],
"date-time": "2022-04-05T16:48:37Z",
"timestamp": 1649177317178
},
"institution": [
{
"name": "medRxiv"
}
],
"is-referenced-by-count": 0,
"issued": {
"date-parts": [
[
2021,
4,
23
]
]
},
"link": [
{
"URL": "https://syndication.highwire.org/content/doi/10.1101/2021.04.20.21255792",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "246",
"original-title": [],
"posted": {
"date-parts": [
[
2021,
4,
23
]
]
},
"prefix": "10.1101",
"published": {
"date-parts": [
[
2021,
4,
23
]
]
},
"publisher": "Cold Spring Harbor Laboratory",
"reference": [
{
"DOI": "10.1016/j.ejphar.2020.173644",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.1"
},
{
"article-title": "Treatment of severe COVID-19 courses in intensive care medicine",
"first-page": "804",
"issue": "8",
"journal-title": "Internist (Berl)",
"key": "2021050608150588000_2021.04.20.21255792v2.2",
"volume": "61",
"year": "2020"
},
{
"DOI": "10.1002/jmv.25882",
"article-title": "Treatment with convalescent plasma for COVID-19 patients in Wuhan, China",
"doi-asserted-by": "crossref",
"first-page": "1890",
"issue": "10",
"journal-title": "J Med Virol",
"key": "2021050608150588000_2021.04.20.21255792v2.3",
"volume": "92",
"year": "2020"
},
{
"DOI": "10.1136/bmj.m3939",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.4"
},
{
"DOI": "10.1016/j.ejphar.2020.173751",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.5"
},
{
"DOI": "10.1002/jmv.26035",
"article-title": "Increase in COVID-19 cases and case-fatality and case-recovery rates in Europe: A cross-temporal meta-analysis",
"doi-asserted-by": "crossref",
"first-page": "1511",
"issue": "9",
"journal-title": "J Med Virol",
"key": "2021050608150588000_2021.04.20.21255792v2.6",
"volume": "92",
"year": "2020"
},
{
"DOI": "10.1007/s10900-020-00863-3",
"article-title": "Epidemic Trend of COVID-19 Transmission in India During Lockdown-1 Phase",
"doi-asserted-by": "crossref",
"first-page": "1291",
"issue": "6",
"journal-title": "J Community Health",
"key": "2021050608150588000_2021.04.20.21255792v2.7",
"volume": "45",
"year": "2020"
},
{
"DOI": "10.1007/s40808-020-00984-7",
"doi-asserted-by": "crossref",
"key": "2021050608150588000_2021.04.20.21255792v2.8",
"unstructured": "Bhadra A , Mukherjee A , Sarkar K. Impact of population density on Covid-19 infected and mortality rate in India. Model Earth Syst Environ. 2020:1–7."
},
{
"DOI": "10.3390/molecules26010039",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.9"
},
{
"DOI": "10.1016/j.puhe.2020.05.042",
"article-title": "TB infection and BCG vaccination: are we protected from COVID-19?",
"doi-asserted-by": "crossref",
"first-page": "91",
"journal-title": "Public Health",
"key": "2021050608150588000_2021.04.20.21255792v2.10",
"volume": "185",
"year": "2020"
},
{
"DOI": "10.1128/mBio.00907-20",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.11"
},
{
"DOI": "10.14336/AD.2020.1104",
"article-title": "Of Cross-immunity, Herd Immunity and Country-specific Plans: Experiences from COVID-19 in India",
"doi-asserted-by": "crossref",
"first-page": "1339",
"issue": "6",
"journal-title": "Aging Dis",
"key": "2021050608150588000_2021.04.20.21255792v2.12",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1096/fj.202001115R",
"article-title": "Genetic gateways to COVID-19 infection: Implications for risk, severity, and outcomes",
"doi-asserted-by": "crossref",
"first-page": "8787",
"issue": "7",
"journal-title": "FASEB J",
"key": "2021050608150588000_2021.04.20.21255792v2.13",
"volume": "34",
"year": "2020"
},
{
"DOI": "10.1007/s00038-020-01390-7",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.14"
},
{
"DOI": "10.1002/pa.2257",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.15"
},
{
"DOI": "10.4103/ijph.IJPH_508_20",
"article-title": "COVID-19 and lockdown: Insights from Mumbai",
"doi-asserted-by": "crossref",
"first-page": "S168",
"journal-title": "Indian J Public Health",
"key": "2021050608150588000_2021.04.20.21255792v2.16",
"volume": "64",
"year": "2020"
},
{
"DOI": "10.1001/jama.2020.6775",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.17"
},
{
"DOI": "10.1210/clinem/dgaa346",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.18"
},
{
"article-title": "COVID-19 and diabetes: Is there enough evidence?",
"first-page": "943",
"journal-title": "J Clin Hypertens (Greenwich)",
"key": "2021050608150588000_2021.04.20.21255792v2.19",
"volume": "6",
"year": "2020"
},
{
"DOI": "10.1016/j.molmet.2020.101044",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.20"
},
{
"DOI": "10.11606/s1518-8787.2020054002481",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.21"
},
{
"DOI": "10.1016/j.ijid.2020.03.017",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.22"
},
{
"DOI": "10.1016/j.jamda.2020.10.031",
"article-title": "Metformin is Associated with Decreased 30-Day Mortality Among Nursing Home Residents Infected with SARS-CoV2",
"doi-asserted-by": "crossref",
"first-page": "193",
"issue": "1",
"journal-title": "J Am Med Dir Assoc",
"key": "2021050608150588000_2021.04.20.21255792v2.23",
"volume": "22",
"year": "2021"
},
{
"DOI": "10.1136/bmj.m1328",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.24"
},
{
"DOI": "10.1002/ajh.25829",
"doi-asserted-by": "publisher",
"key": "2021050608150588000_2021.04.20.21255792v2.25"
},
{
"article-title": "Appraisal of Critically Ill COVID-19 Patients at a Dedicated COVID Hospital",
"first-page": "14",
"issue": "9",
"journal-title": "J Assoc Physicians India",
"key": "2021050608150588000_2021.04.20.21255792v2.26",
"volume": "68",
"year": "2020"
},
{
"DOI": "10.1016/j.dsx.2020.09.027",
"article-title": "Ivermectin in COVID-19: What do we know?",
"doi-asserted-by": "crossref",
"first-page": "1921",
"issue": "6",
"journal-title": "Diabetes Metab Syndr",
"key": "2021050608150588000_2021.04.20.21255792v2.27",
"volume": "14",
"year": "2020"
}
],
"reference-count": 27,
"references-count": 27,
"relation": {},
"resource": {
"primary": {
"URL": "http://medrxiv.org/lookup/doi/10.1101/2021.04.20.21255792"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subtitle": [],
"subtype": "preprint",
"title": "Retrospective Assessment of Treatments of Hospitalized Covid-19 Patients",
"type": "posted-content"
}
