Adherence to the Mediterranean Diet Association with Serum Inflammatory Factors Stress Oxidative and Appetite in COVID-19 Patients
et al., Medicina, doi:10.3390/medicina59020227, Jan 2023
Diet for COVID-19
26th treatment shown to reduce risk in
June 2021, now with p < 0.00000000001 from 30 studies, recognized in 4 countries.
No treatment is 100% effective. Protocols
combine treatments.
6,600+ studies for
220+ treatments. c19early.org
|
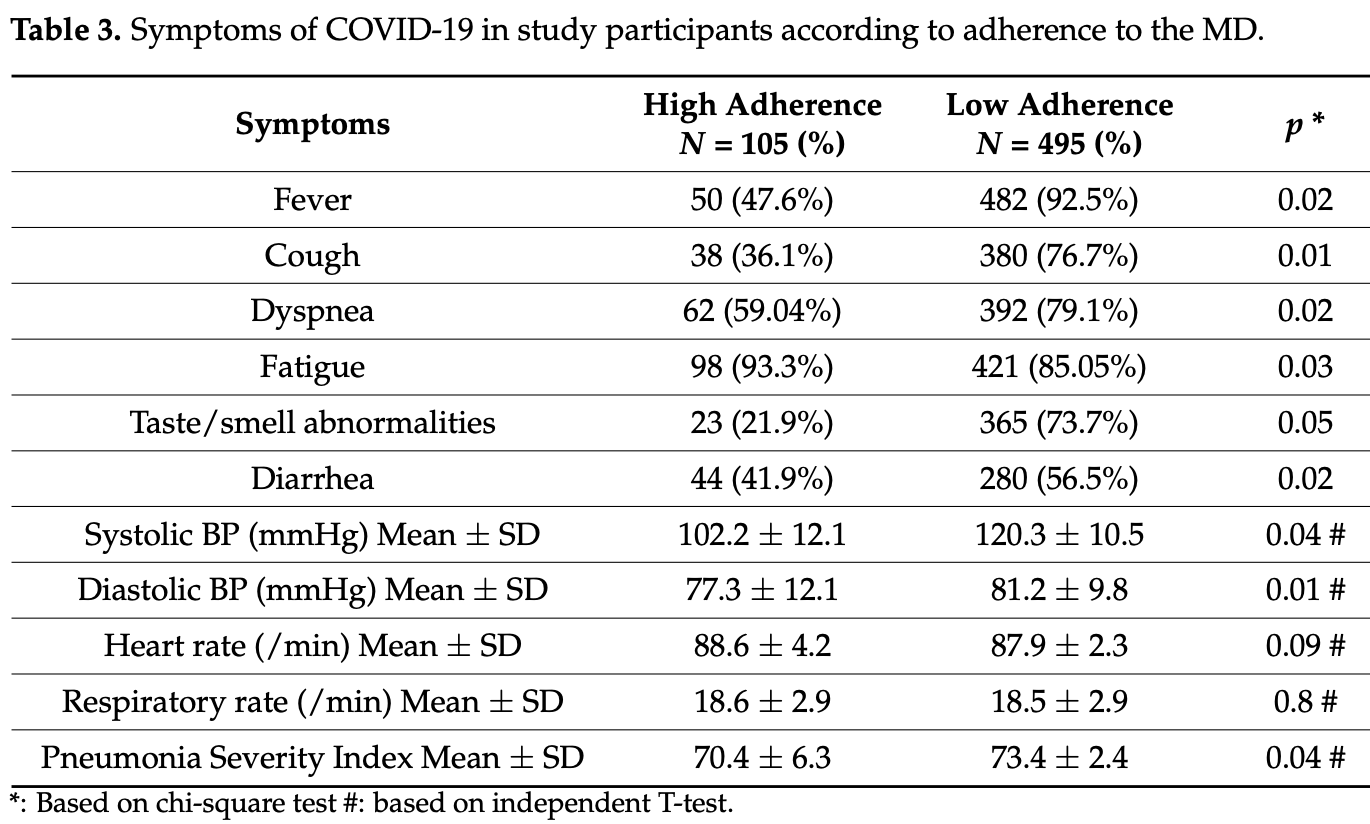
Retrospective 600 COVID-19 patients in Iran with moderate/severe CT scans, showing lower prevalence of dyspnea, fever, taste/smell abnormalities, and cough with high adherence to the Mediterranean diet in unadjusted results.
This study is excluded in the after exclusion results of meta-analysis:
unadjusted results with no group details.
|
risk of progression, 25.4% lower, RR 0.75, p < 0.001, higher quality diet 62 of 105 (59.0%), lower quality diet 392 of 495 (79.2%), NNT 5.0, dyspnea.
|
|
risk of progression, 51.1% lower, RR 0.49, p < 0.001, higher quality diet 50 of 105 (47.6%), lower quality diet 482 of 495 (97.4%), NNT 2.0, fever.
|
|
risk of progression, 70.3% lower, RR 0.30, p < 0.001, higher quality diet 23 of 105 (21.9%), lower quality diet 365 of 495 (73.7%), NNT 1.9, taste/smell.
|
|
risk of progression, 9.7% higher, RR 1.10, p = 0.03, higher quality diet 98 of 105 (93.3%), lower quality diet 421 of 495 (85.1%), fatigue.
|
|
risk of progression, 52.9% lower, RR 0.47, p < 0.001, higher quality diet 38 of 105 (36.2%), lower quality diet 380 of 495 (76.8%), NNT 2.5, cough.
|
|
risk of progression, 25.9% lower, RR 0.74, p = 0.007, higher quality diet 44 of 105 (41.9%), lower quality diet 280 of 495 (56.6%), NNT 6.8, diarrhea.
|
| Effect extraction follows pre-specified rules prioritizing more serious outcomes. Submit updates |
Mohajeri et al., 26 Jan 2023, retrospective, Iran, peer-reviewed, survey, 3 authors.
Contact: mahsa.mohajeri.93@gmail.com (corresponding author), arrigo.cicero@unibo.it.
Adherence to the Mediterranean Diet Association with Serum Inflammatory Factors Stress Oxidative and Appetite in COVID-19 Patients
Medicina, doi:10.3390/medicina59020227
Background and Objectives: The Mediterranean diet's bioactive components are suggested to strengthen the immune system and to exert anti-inflammatory actions. This study investigated the association between adherence to the Mediterranean diet with serum inflammatory factors, total antioxidant capacity, appetite, and symptoms of COVID-19 patients. Materials and Methods: This crosssectional study was conducted among 600 Iranian COVID-19 patients selected by a simple random method. The ten-item Mediterranean diet adherence questionnaire was used to assess diet adherence. At the beginning of the study, 5 cc of blood was taken from all patients for measurement of serum interleukin 1β) IL-1β), tumor necrosis factor (TNF-α), malondialdehyde (MDA), high sensitivity Creactive protein (hs-CRP) and total antioxidant capacity (TAC). A human ELISA kit with serial number 950.090.096 produced by the Diaclone Company was used to test this cytokine using the sandwich ELISA method. Results: One hundred and five patients presented a high adherence and 495 patients presented a low adherence to the Mediterranean diet. The incidence of fever, cough, diarrhea, taste changes, and pneumonia severity index were significantly lower in patients who adhered to the Mediterranean diet more than other patients. Serum levels of tumor necrosis factor (5.7 ± 2.1 vs. 6.9 ± 2.8 p = 0.02), interleukin 1 beta (3.2 ± 0.02 vs. 4.9 ± 0.01 p = 0.02), high-sensitivity C-reactive protein (17.08 ± 4.2 vs. 19.8 ± 2.5 p = 0.03), and malondialdehyde (5.7 ± 0.2 vs. 6.2 ± 0.3 p = 0.02) were significantly lower in patients who adhered more to the Mediterranean diet than other patients.
Conclusion: The Mediterranean diet can improve the symptoms and elevated serum inflammatory factors in COVID-19 patients, so clinical trial studies are suggested to confirm this effect.
Informed Consent Statement: Informed consent was obtained from all subjects involved in the study. Written informed consent has been obtained from the patients to publish this paper.
Data Availability Statement: Data is unavailable due to privacy or ethical restrictions.
Conflicts of Interest: The authors declare no conflict of interest.
References
Akbari, Tabrizi, Lankarani, Aria, Vakili et al., The role of cytokine profile and lymphocyte subsets in the severity of coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis, Life Sci, doi:10.1016/j.lfs.2020.118167
Anania, Perla, Olivero, Pacifico, Chiesa, Mediterranean diet and nonalcoholic fatty liver disease, World J. Gastroenterol, doi:10.3748/wjg.v24.i19.2083
Angelidi, Kokkinos, Katechaki, Ros, Mantzoros, Mediterranean diet as a nutritional approach for COVID-19, Metab. Clin. Exp
Angelis, Chrysohoou, Tzorovili, Laina, Xydis et al., The Mediterranean diet benefit on cardiovascular hemodynamics and erectile function in chronic heart failure male patients by decoding central and peripheral vessel rheology, Nutrients, doi:10.3390/nu13010108
Baratta, Cammisotto, Tozzi, Coronati, Bartimoccia et al., High Compliance to Mediterranean Diet Associates with Lower Platelet Activation and Liver Collagen Deposition in Patients with Nonalcoholic Fatty Liver Disease, Nutrients, doi:10.3390/nu14061209
Barrea, Vetrani, Caprio, Cataldi, Ghoch et al., From the Ketogenic Diet to the Mediterranean Diet: The Potential Dietary Therapy in Patients with Obesity after CoVID-19 Infection (Post CoVID Syndrome), Curr. Obes. Rep, doi:10.1007/s13679-022-00475-z
Bouayad, Innate immune evasion by SARS-CoV-2: Comparison with SARS-CoV, Rev. Med. Virol, doi:10.1002/rmv.2135
Calder, Carr, Gombart, Eggersdorfer, Optimal nutritional status for a well-functioning immune system is an important factor to protect against viral infections, Nutrients, doi:10.3390/nu12041181
Chrysohoou, Panagiotakos, Pitsavos, Das, Stefanadis, Adherence to the Mediterranean diet attenuates inflammation and coagulation process in healthy adults: The ATTICA Study, J. Am. Coll. Cardiol, doi:10.1016/j.jacc.2004.03.039
Ciotti, Ciccozzi, Terrinoni, Jiang, Wang et al., The COVID-19 pandemic, Crit. Rev. Clin. Lab. Sci, doi:10.1080/10408363.2020.1783198
Davis, Bryan, Hodgson, Murphy, Definition of the Mediterranean diet: A literature review, Nutrients
Fedullo, Schiattarella, Morlando, Raguzzini, Toti et al., Mediterranean Diet for the Prevention of Gestational Diabetes in the Covid-19 Era: Implications of Il-6 In Diabesity, Int. J. Mol. Sci, doi:10.3390/ijms22031213
Finicelli, Di Salle, Galderisi, Peluso, The Mediterranean Diet: An Update of the Clinical Trials, Nutrients, doi:10.3390/nu14142956
Finicelli, Squillaro, Di Cristo, Di Salle, Melone et al., Metabolic syndrome, Mediterranean diet, and polyphenols: Evidence and perspectives, J. Cell. Physiol, doi:10.1002/jcp.27506
Gantenbein, Kanaka-Gantenbein, Mediterranean diet as an antioxidant: The impact on metabolic health and overall wellbeing, Nutrients, doi:10.3390/nu13061951
García-Montero, Fraile-Martínez, Gómez-Lahoz, Pekarek, Castellanos et al., Nutritional components in Western diet versus Mediterranean diet at the gut microbiota-immune system interplay. Implications for health and disease, Nutrients, doi:10.3390/nu13020699
Greene, Roberts, Frugé, Negative association between Mediterranean diet adherence and COVID-19 cases and related deaths in Spain and 23 OECD countries: An ecological study, Front. Nutr, doi:10.3389/fnut.2021.591964
Guilleminault, Williams, Scott, Berthon, Jensen et al., Diet and asthma: Is it time to adapt our message?, Nutrients, doi:10.3390/nu9111227
Jafarzadeh, Chauhan, Saha, Jafarzadeh, Nemati, Contribution of monocytes and macrophages to the local tissue inflammation and cytokine storm in COVID-19: Lessons from SARS and MERS, and potential therapeutic interventions, Life Sci, doi:10.1016/j.lfs.2020.118102
Koebnick, Black, Wu, Shu, Mackay et al., A diet high in sugar-sweetened beverage and low in fruits and vegetables is associated with adiposity and a pro-inflammatory adipokine profile, Br. J. Nutr, doi:10.1017/S0007114518002726
Koloverou, Panagiotakos, Pitsavos, Chrysohoou, Georgousopoulou et al., Adherence to Mediterranean diet and 10-year incidence (2002-2012) of diabetes: Correlations with inflammatory and oxidative stress biomarkers in the ATTICA cohort study, Diabetes Metab. Res. Rev, doi:10.1002/dmrr.2672
Koopen, Almeida, Attaye, Witjes, Rampanelli et al., Effect of fecal microbiota transplantation combined with Mediterranean diet on insulin sensitivity in subjects with metabolic syndrome, Front. Microbiol, doi:10.3389/fmicb.2021.662159
Lampropoulos, Konsta, Dradaki, Roumpou, Dri et al., Effects of Mediterranean diet on hospital length of stay, medical expenses, and mortality in elderly, hospitalized patients: A 2-year observational study, Nutrition, doi:10.1016/j.nut.2020.110868
Maiorino, Bellastella, Longo, Caruso, Esposito, Mediterranean diet and COVID-19: Hypothesizing potential benefits in people with diabetes, Front. Endocrinol, doi:10.3389/fendo.2020.574315
Martín-Peláez, Fito, Castaner, Mediterranean diet effects on type 2 diabetes prevention, disease progression, and related mechanisms. A review, Nutrients, doi:10.3390/nu12082236
Martínez-Colón, Ratnasiri, Chen, Jiang, Zanley et al., SARS-CoV-2 infection drives an inflammatory response in human adipose tissue through infection of adipocytes and macrophages, Sci. Transl. Med, doi:10.1126/scitranslmed.abm9151
Martínez-González, Salas-Salvadó, Estruch, Corella, Fitó et al., Benefits of the Mediterranean diet: Insights from the PREDIMED study, Prog. Cardiovasc. Dis, doi:10.1016/j.pcad.2015.04.003
Mazzocchi, Leone, Agostoni, Pali-Schöll, The secrets of the Mediterranean diet. Does [only] olive oil matter?, Nutrients, doi:10.3390/nu11122941
Mcelvaney, Mcevoy, Mcelvaney, Carroll, Murphy et al., Characterization of the inflammatory response to severe COVID-19 illness, Am. J. Respir. Crit. Care Med, doi:10.1164/rccm.202005-1583OC
Mentella, Scaldaferri, Ricci, Gasbarrini, Miggiano, Cancer and Mediterranean diet: A review, Nutrients, doi:10.3390/nu11092059
Merad, Subramanian, Wang, An aberrant inflammatory response in severe COVID-19, Cell Host Microbe, doi:10.1016/j.chom.2021.06.018
Morvaridi, Jafarirad, Seyedian, Alavinejad, Cheraghian, The effects of extra virgin olive oil and canola oil on inflammatory markers and gastrointestinal symptoms in patients with ulcerative colitis, Eur. J. Clin. Nutr, doi:10.1038/s41430-019-0549-z
Naureen, Dhuli, Donato, Aquilanti, Velluti et al., Foods of the Mediterranean diet: Tomato, olives, chili pepper, wheat flour and wheat germ, J. Prev. Med. Hyg
Noce, Marrone, Urciuoli, Di Daniele, Di Lauro et al., Usefulness of extra virgin olive oil minor polar compounds in the management of chronic kidney disease patients, Nutrients, doi:10.3390/nu13020581
Nomikos, Fragopoulou, Antonopoulou, Panagiotakos, Mediterranean diet and platelet-activating factor; a systematic review, Clin. Biochem, doi:10.1016/j.clinbiochem.2018.08.004
Perez-Araluce, Martinez-Gonzalez, Fernández-Lázaro, Bes-Rastrollo, Gea et al., Mediterranean diet and the risk of COVID-19 in the 'Seguimiento Universidad de Navarra' cohort, Clin. Nutr, doi:10.1016/j.clnu.2021.04.001
Pieri, Ciotti, Nuccetelli, Perrone, Caliò et al., Serum Amyloid A Protein as a useful biomarker to predict COVID-19 patients severity and prognosis, Int. Immunopharmaco, doi:10.1016/j.intimp.2021.107512
Polverino, Goeminne, Mcdonnell, Aliberti, Marshall et al., European Respiratory Society guidelines for the management of adult bronchiectasis, Eur. Respir. J, doi:10.1183/13993003.00629-2017
Saura-Calixto, Goni, Definition of the Mediterranean diet based on bioactive compounds, Crit. Rev. Food Sci. Nutr, doi:10.1080/10408390701764732
Schröder, Fitó, Estruch, Martínez-González, Corella et al., A short screener is valid for assessing Mediterranean diet adherence among older Spanish men and women, J. Nutr, doi:10.3945/jn.110.135566
Serra-Majem, Roman-Vinas, Sanchez-Villegas, Guasch-Ferre, Corella et al., Benefits of the Mediterranean diet: Epidemiological and molecular aspects, Mol. Asp. Med, doi:10.1016/j.mam.2019.06.001
Song, Li, Xie, Hou, You, Cytokine storm induced by SARS-CoV-2, Clin. Chim. Acta, doi:10.1016/j.cca.2020.06.017
Sorić Hosman, Kos, Lamot, Serum amyloid A in inflammatory rheumatic diseases: A compendious review of a renowned biomarker, Front. Immunol, doi:10.3389/fimmu.2020.631299
Strasser, Wolters, Weyh, Krüger, Ticinesi, The effects of lifestyle and diet on gut microbiota composition, inflammation and muscle performance in our aging society, Nutrients, doi:10.3390/nu13062045
Sureda, Bibiloni, Julibert, Bouzas, Argelich et al., Adherence to the Mediterranean Diet and Inflammatory Markers, Nutrients, doi:10.3390/nu10010062
Tanacan, Yazihan, Erol, Anuk, Yetiskin et al., The impact of COVID-19 infection on the cytokine profile of pregnant women: A prospective case-control study, Cytokine, doi:10.1016/j.cyto.2021.155431
Trichopoulou, Martínez-González, Tong, Forouhi, Khandelwal et al., Definitions and potential health benefits of the Mediterranean diet: Views from experts around the world, BMC Med, doi:10.1186/1741-7015-12-112
Ullah, Khan, Basharat, Huo, Ud Din et al., Evaluation of Cardiac Biomarkers and Expression Analysis of IL-1, IL-6, IL-10, IL-17, and IL-25 among COVID-19 Patients from Pakistan, Viruses, doi:10.3390/v14102149
Valle, Kim-Schulze, Huang, Beckmann, Nirenberg et al., An inflammatory cytokine signature predicts COVID-19 severity and survival, Nat. Med, doi:10.1038/s41591-020-1051-9
Veček, Mucalo, Dragun, Miličević, Pribisalić et al., The association between salt taste perception, mediterranean diet and metabolic syndrome: A cross-sectional study, Nutrients
Yaghoubi, Youssefi, Jabbari Azad, Farzad, Yavari et al., Total antioxidant capacity as a marker of severity of COVID-19 infection: Possible prognostic and therapeutic clinical application, J. Med. Virol
DOI record:
{
"DOI": "10.3390/medicina59020227",
"ISSN": [
"1648-9144"
],
"URL": "http://dx.doi.org/10.3390/medicina59020227",
"abstract": "<jats:p>Background and Objectives: The Mediterranean diet’s bioactive components are suggested to strengthen the immune system and to exert anti-inflammatory actions. This study investigated the association between adherence to the Mediterranean diet with serum inflammatory factors, total antioxidant capacity, appetite, and symptoms of COVID-19 patients. Materials and Methods: This cross-sectional study was conducted among 600 Iranian COVID-19 patients selected by a simple random method. The ten-item Mediterranean diet adherence questionnaire was used to assess diet adherence. At the beginning of the study, 5 cc of blood was taken from all patients for measurement of serum interleukin 1β) IL-1β), tumor necrosis factor (TNF-α), malondialdehyde (MDA), high sensitivity C-reactive protein (hs-CRP) and total antioxidant capacity (TAC). A human ELISA kit with serial number 950.090.096 produced by the Diaclone Company was used to test this cytokine using the sandwich ELISA method. Results: One hundred and five patients presented a high adherence and 495 patients presented a low adherence to the Mediterranean diet. The incidence of fever, cough, diarrhea, taste changes, and pneumonia severity index were significantly lower in patients who adhered to the Mediterranean diet more than other patients. Serum levels of tumor necrosis factor (5.7 ± 2.1 vs. 6.9 ± 2.8 p = 0.02), interleukin 1 beta (3.2 ± 0.02 vs. 4.9 ± 0.01 p = 0.02), high-sensitivity C-reactive protein (17.08 ± 4.2 vs. 19.8 ± 2.5 p = 0.03), and malondialdehyde (5.7 ± 0.2 vs. 6.2 ± 0.3 p = 0.02) were significantly lower in patients who adhered more to the Mediterranean diet than other patients. Conclusion: The Mediterranean diet can improve the symptoms and elevated serum inflammatory factors in COVID-19 patients, so clinical trial studies are suggested to confirm this effect.</jats:p>",
"alternative-id": [
"medicina59020227"
],
"author": [
{
"affiliation": [
{
"name": "Digestive Disease Research Center, Ardabil University of Medical Sciences, Ardabil 56189-85991, Iran"
}
],
"family": "Mohajeri",
"given": "Mahsa",
"sequence": "first"
},
{
"ORCID": "http://orcid.org/0000-0002-3348-3796",
"affiliation": [
{
"name": "Energy Management Research Center, University of Mohaghegh Ardabili, Ardabil 56199-11367, Iran"
}
],
"authenticated-orcid": false,
"family": "Mohajery",
"given": "Reza",
"sequence": "additional"
},
{
"ORCID": "http://orcid.org/0000-0002-4367-3884",
"affiliation": [
{
"name": "Medicine and Surgery Sciences Department, Alma Mater Studiorum University of Bologna, 40126 Bologna, Italy"
},
{
"name": "IRCCS AOU S. Orsola-Malpighi University Hospital, 40138 Bologna, Italy"
}
],
"authenticated-orcid": false,
"family": "Cicero",
"given": "Arrigo F. G.",
"sequence": "additional"
}
],
"container-title": "Medicina",
"container-title-short": "Medicina",
"content-domain": {
"crossmark-restriction": false,
"domain": []
},
"created": {
"date-parts": [
[
2023,
1,
26
]
],
"date-time": "2023-01-26T06:30:30Z",
"timestamp": 1674714630000
},
"deposited": {
"date-parts": [
[
2023,
1,
26
]
],
"date-time": "2023-01-26T07:17:39Z",
"timestamp": 1674717459000
},
"indexed": {
"date-parts": [
[
2023,
1,
27
]
],
"date-time": "2023-01-27T06:00:31Z",
"timestamp": 1674799231359
},
"is-referenced-by-count": 0,
"issue": "2",
"issued": {
"date-parts": [
[
2023,
1,
26
]
]
},
"journal-issue": {
"issue": "2",
"published-online": {
"date-parts": [
[
2023,
2
]
]
}
},
"language": "en",
"license": [
{
"URL": "https://creativecommons.org/licenses/by/4.0/",
"content-version": "vor",
"delay-in-days": 0,
"start": {
"date-parts": [
[
2023,
1,
26
]
],
"date-time": "2023-01-26T00:00:00Z",
"timestamp": 1674691200000
}
}
],
"link": [
{
"URL": "https://www.mdpi.com/1648-9144/59/2/227/pdf",
"content-type": "unspecified",
"content-version": "vor",
"intended-application": "similarity-checking"
}
],
"member": "1968",
"original-title": [],
"page": "227",
"prefix": "10.3390",
"published": {
"date-parts": [
[
2023,
1,
26
]
]
},
"published-online": {
"date-parts": [
[
2023,
1,
26
]
]
},
"publisher": "MDPI AG",
"reference": [
{
"DOI": "10.1080/10408363.2020.1783198",
"article-title": "The COVID-19 pandemic",
"author": "Ciotti",
"doi-asserted-by": "crossref",
"first-page": "365",
"journal-title": "Crit. Rev. Clin. Lab. Sci.",
"key": "ref_1",
"volume": "57",
"year": "2020"
},
{
"DOI": "10.3390/nu12041181",
"doi-asserted-by": "crossref",
"key": "ref_2",
"unstructured": "Calder, P.C., Carr, A.C., Gombart, A.F., and Eggersdorfer, M. (2020). Optimal nutritional status for a well-functioning immune system is an important factor to protect against viral infections. Nutrients, 12."
},
{
"DOI": "10.1183/13993003.00629-2017",
"article-title": "European Respiratory Society guidelines for the management of adult bronchiectasis",
"author": "Polverino",
"doi-asserted-by": "crossref",
"first-page": "1700629",
"journal-title": "Eur. Respir. J.",
"key": "ref_3",
"volume": "50",
"year": "2017"
},
{
"DOI": "10.1164/rccm.202005-1583OC",
"article-title": "Characterization of the inflammatory response to severe COVID-19 illness",
"author": "McElvaney",
"doi-asserted-by": "crossref",
"first-page": "812",
"journal-title": "Am. J. Respir. Crit. Care Med.",
"key": "ref_4",
"volume": "202",
"year": "2020"
},
{
"DOI": "10.1016/j.chom.2021.06.018",
"article-title": "An aberrant inflammatory response in severe COVID-19",
"author": "Merad",
"doi-asserted-by": "crossref",
"first-page": "1043",
"journal-title": "Cell Host Microbe",
"key": "ref_5",
"volume": "29",
"year": "2021"
},
{
"DOI": "10.1016/j.lfs.2020.118102",
"article-title": "Contribution of monocytes and macrophages to the local tissue inflammation and cytokine storm in COVID-19: Lessons from SARS and MERS, and potential therapeutic interventions",
"author": "Jafarzadeh",
"doi-asserted-by": "crossref",
"first-page": "118102",
"journal-title": "Life Sci.",
"key": "ref_6",
"volume": "257",
"year": "2020"
},
{
"DOI": "10.1002/rmv.2135",
"article-title": "Innate immune evasion by SARS-CoV-2: Comparison with SARS-CoV",
"author": "Bouayad",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Rev. Med. Virol.",
"key": "ref_7",
"volume": "30",
"year": "2020"
},
{
"DOI": "10.1016/j.cca.2020.06.017",
"article-title": "Cytokine storm induced by SARS-CoV-2. Clin",
"author": "Song",
"doi-asserted-by": "crossref",
"first-page": "280",
"journal-title": "Chim. Acta.",
"key": "ref_8",
"volume": "509",
"year": "2020"
},
{
"DOI": "10.1126/scitranslmed.abm9151",
"article-title": "SARS-CoV-2 infection drives an inflammatory response in human adipose tissue through infection of adipocytes and macrophages",
"author": "Ratnasiri",
"doi-asserted-by": "crossref",
"first-page": "eabm9151",
"journal-title": "Sci. Transl. Med.",
"key": "ref_9",
"volume": "14",
"year": "2022"
},
{
"DOI": "10.1016/j.lfs.2020.118167",
"article-title": "The role of cytokine profile and lymphocyte subsets in the severity of coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis",
"author": "Akbari",
"doi-asserted-by": "crossref",
"first-page": "118167",
"journal-title": "Life Sci.",
"key": "ref_10",
"volume": "258",
"year": "2020"
},
{
"DOI": "10.1016/j.intimp.2021.107512",
"article-title": "Serum Amyloid A Protein as a useful biomarker to predict COVID-19 patients severity and prognosis",
"author": "Pieri",
"doi-asserted-by": "crossref",
"first-page": "107512",
"journal-title": "Int. Immunopharmaco.",
"key": "ref_11",
"volume": "95",
"year": "2021"
},
{
"DOI": "10.3389/fimmu.2020.631299",
"article-title": "Serum amyloid A in inflammatory rheumatic diseases: A compendious review of a renowned biomarker",
"author": "Kos",
"doi-asserted-by": "crossref",
"first-page": "631299",
"journal-title": "Front. Immunol.",
"key": "ref_12",
"volume": "11",
"year": "2021"
},
{
"DOI": "10.1016/j.cyto.2021.155431",
"article-title": "The impact of COVID-19 infection on the cytokine profile of pregnant women: A prospective case-control study",
"author": "Tanacan",
"doi-asserted-by": "crossref",
"first-page": "155431",
"journal-title": "Cytokine",
"key": "ref_13",
"volume": "140",
"year": "2021"
},
{
"DOI": "10.3390/v14102149",
"doi-asserted-by": "crossref",
"key": "ref_14",
"unstructured": "Ullah, R., Khan, J., Basharat, N., Huo, D., Ud Din, A., and Wang, G. (2022). Evaluation of Cardiac Biomarkers and Expression Analysis of IL-1, IL-6, IL-10, IL-17, and IL-25 among COVID-19 Patients from Pakistan. Viruses, 14."
},
{
"DOI": "10.3748/wjg.v24.i19.2083",
"article-title": "Mediterranean diet and nonalcoholic fatty liver disease",
"author": "Anania",
"doi-asserted-by": "crossref",
"first-page": "2083",
"journal-title": "World J. Gastroenterol.",
"key": "ref_15",
"volume": "24",
"year": "2018"
},
{
"DOI": "10.1080/10408390701764732",
"article-title": "Definition of the Mediterranean diet based on bioactive compounds",
"author": "Goni",
"doi-asserted-by": "crossref",
"first-page": "145",
"journal-title": "Crit. Rev. Food Sci. Nutr.",
"key": "ref_16",
"volume": "49",
"year": "2009"
},
{
"DOI": "10.1186/1741-7015-12-112",
"doi-asserted-by": "crossref",
"key": "ref_17",
"unstructured": "Trichopoulou, A., Martínez-González, M.A., Tong, T.Y., Forouhi, N.G., Khandelwal, S., Prabhakaran, D., Mozaffarian, D., and de Lorgeril, M. (2014). Definitions and potential health benefits of the Mediterranean diet: Views from experts around the world. BMC Med., 12."
},
{
"DOI": "10.3390/nu12082236",
"doi-asserted-by": "crossref",
"key": "ref_18",
"unstructured": "Martín-Peláez, S., Fito, M., and Castaner, O. (2020). Mediterranean diet effects on type 2 diabetes prevention, disease progression, and related mechanisms. A review. Nutrients, 12."
},
{
"DOI": "10.1002/jcp.27506",
"article-title": "Metabolic syndrome, Mediterranean diet, and polyphenols: Evidence and perspectives",
"author": "Finicelli",
"doi-asserted-by": "crossref",
"first-page": "5807",
"journal-title": "J. Cell. Physiol.",
"key": "ref_19",
"volume": "234",
"year": "2019"
},
{
"DOI": "10.3390/nu12041164",
"doi-asserted-by": "crossref",
"key": "ref_20",
"unstructured": "Veček, N.N., Mucalo, L., Dragun, R., Miličević, T., Pribisalić, A., Patarčić, I., Hayward, C., Polašek, O., and Kolčić, I. (2020). The association between salt taste perception, mediterranean diet and metabolic syndrome: A cross-sectional study. Nutrients, 12."
},
{
"DOI": "10.3389/fmicb.2021.662159",
"article-title": "Effect of fecal microbiota transplantation combined with Mediterranean diet on insulin sensitivity in subjects with metabolic syndrome",
"author": "Koopen",
"doi-asserted-by": "crossref",
"first-page": "662159",
"journal-title": "Front. Microbiol.",
"key": "ref_21",
"volume": "12",
"year": "2021"
},
{
"DOI": "10.3390/nu14142956",
"doi-asserted-by": "crossref",
"key": "ref_22",
"unstructured": "Finicelli, M., Di Salle, A., Galderisi, U., and Peluso, G. (2022). The Mediterranean Diet: An Update of the Clinical Trials. Nutrients, 14."
},
{
"DOI": "10.3390/nu11092059",
"doi-asserted-by": "crossref",
"key": "ref_23",
"unstructured": "Mentella, M.C., Scaldaferri, F., Ricci, C., Gasbarrini, A., and Miggiano, G.A.D. (2019). Cancer and Mediterranean diet: A review. Nutrients, 11."
},
{
"DOI": "10.3390/nu11122941",
"doi-asserted-by": "crossref",
"key": "ref_24",
"unstructured": "Mazzocchi, A., Leone, L., Agostoni, C., and Pali-Schöll, I. (2019). The secrets of the Mediterranean diet. Does [only] olive oil matter?. Nutrients, 11."
},
{
"DOI": "10.3945/jn.110.135566",
"article-title": "A short screener is valid for assessing Mediterranean diet adherence among older Spanish men and women",
"author": "Estruch",
"doi-asserted-by": "crossref",
"first-page": "1140",
"journal-title": "J. Nutr.",
"key": "ref_25",
"volume": "141",
"year": "2011"
},
{
"DOI": "10.1007/s13679-022-00475-z",
"article-title": "From the Ketogenic Diet to the Mediterranean Diet: The Potential Dietary Therapy in Patients with Obesity after CoVID-19 Infection (Post CoVID Syndrome)",
"author": "Barrea",
"doi-asserted-by": "crossref",
"first-page": "144",
"journal-title": "Curr. Obes. Rep.",
"key": "ref_26",
"volume": "11",
"year": "2022"
},
{
"DOI": "10.3389/fnut.2021.591964",
"article-title": "Negative association between Mediterranean diet adherence and COVID-19 cases and related deaths in Spain and 23 OECD countries: An ecological study",
"author": "Greene",
"doi-asserted-by": "crossref",
"first-page": "591964",
"journal-title": "Front. Nutr.",
"key": "ref_27",
"volume": "8",
"year": "2021"
},
{
"article-title": "Mediterranean diet and the risk of COVID-19 in the ‘Seguimiento Universidad de Navarra’ cohort",
"author": "Gea",
"first-page": "3061",
"journal-title": "Clin. Nutr.",
"key": "ref_28",
"volume": "41",
"year": "2021"
},
{
"DOI": "10.3390/ijms22031213",
"doi-asserted-by": "crossref",
"key": "ref_29",
"unstructured": "Fedullo, A.L., Schiattarella, A., Morlando, M., Raguzzini, A., Toti, E., De Franciscis, P., and Peluso, I. (2021). Mediterranean Diet for the Prevention of Gestational Diabetes in the Covid-19 Era: Implications of Il-6 In Diabesity. Int. J. Mol. Sci., 22."
},
{
"DOI": "10.3390/nu9111227",
"doi-asserted-by": "crossref",
"key": "ref_30",
"unstructured": "Guilleminault, L., Williams, E.J., Scott, H.A., Berthon, B.S., Jensen, M., and Wood, L.G. (2017). Diet and asthma: Is it time to adapt our message?. Nutrients, 9."
},
{
"DOI": "10.1002/dmrr.2672",
"article-title": "Adherence to Mediterranean diet and 10-year incidence (2002–2012) of diabetes: Correlations with inflammatory and oxidative stress biomarkers in the ATTICA cohort study",
"author": "Koloverou",
"doi-asserted-by": "crossref",
"first-page": "73",
"journal-title": "Diabetes Metab. Res. Rev.",
"key": "ref_31",
"volume": "32",
"year": "2016"
},
{
"DOI": "10.3389/fendo.2020.574315",
"article-title": "Mediterranean diet and COVID-19: Hypothesizing potential benefits in people with diabetes",
"author": "Maiorino",
"doi-asserted-by": "crossref",
"first-page": "574315",
"journal-title": "Front. Endocrinol.",
"key": "ref_32",
"volume": "11",
"year": "2020"
},
{
"DOI": "10.1016/j.nut.2020.110868",
"article-title": "Effects of Mediterranean diet on hospital length of stay, medical expenses, and mortality in elderly, hospitalized patients: A 2-year observational study",
"author": "Lampropoulos",
"doi-asserted-by": "crossref",
"first-page": "110868",
"journal-title": "Nutrition",
"key": "ref_33",
"volume": "79",
"year": "2020"
},
{
"DOI": "10.1038/s41591-020-1051-9",
"article-title": "An inflammatory cytokine signature predicts COVID-19 severity and survival",
"author": "Huang",
"doi-asserted-by": "crossref",
"first-page": "1636",
"journal-title": "Nat. Med.",
"key": "ref_34",
"volume": "26",
"year": "2020"
},
{
"DOI": "10.1002/jmv.27500",
"article-title": "Total antioxidant capacity as a marker of severity of COVID-19 infection: Possible prognostic and therapeutic clinical application",
"author": "Yaghoubi",
"doi-asserted-by": "crossref",
"first-page": "1558",
"journal-title": "J. Med. Virol.",
"key": "ref_35",
"volume": "94",
"year": "2022"
},
{
"DOI": "10.3390/nu10010062",
"doi-asserted-by": "crossref",
"key": "ref_36",
"unstructured": "Sureda, A., Bibiloni, M.D., Julibert, A., Bouzas, C., Argelich, E., Llompart, I., Pons, A., and Tur, J.A. (2018). Adherence to the Mediterranean Diet and Inflammatory Markers. Nutrients, 10."
},
{
"DOI": "10.1016/j.jacc.2004.03.039",
"article-title": "Adherence to the Mediterranean diet attenuates inflammation and coagulation process in healthy adults: The ATTICA Study",
"author": "Chrysohoou",
"doi-asserted-by": "crossref",
"first-page": "152",
"journal-title": "J. Am. Coll. Cardiol.",
"key": "ref_37",
"volume": "44",
"year": "2004"
},
{
"DOI": "10.1016/j.pcad.2015.04.003",
"article-title": "Benefits of the Mediterranean diet: Insights from the PREDIMED study",
"author": "Estruch",
"doi-asserted-by": "crossref",
"first-page": "50",
"journal-title": "Prog. Cardiovasc. Dis.",
"key": "ref_38",
"volume": "58",
"year": "2015"
},
{
"DOI": "10.3390/nu7115459",
"article-title": "Definition of the Mediterranean diet: A literature review",
"author": "Davis",
"doi-asserted-by": "crossref",
"first-page": "9139",
"journal-title": "Nutrients",
"key": "ref_39",
"volume": "7",
"year": "2015"
},
{
"article-title": "Foods of the Mediterranean diet: Tomato, olives, chili pepper, wheat flour and wheat germ",
"author": "Naureen",
"first-page": "E4",
"journal-title": "J. Prev. Med. Hyg.",
"key": "ref_40",
"volume": "63",
"year": "2022"
},
{
"DOI": "10.3390/nu13061951",
"doi-asserted-by": "crossref",
"key": "ref_41",
"unstructured": "Gantenbein, K.V., and Kanaka-Gantenbein, C. (2021). Mediterranean diet as an antioxidant: The impact on metabolic health and overall wellbeing. Nutrients, 13."
},
{
"DOI": "10.1017/S0007114518002726",
"article-title": "A diet high in sugar-sweetened beverage and low in fruits and vegetables is associated with adiposity and a pro-inflammatory adipokine profile",
"author": "Koebnick",
"doi-asserted-by": "crossref",
"first-page": "1230",
"journal-title": "Br. J. Nutr.",
"key": "ref_42",
"volume": "120",
"year": "2018"
},
{
"DOI": "10.1038/s41430-019-0549-z",
"article-title": "The effects of extra virgin olive oil and canola oil on inflammatory markers and gastrointestinal symptoms in patients with ulcerative colitis",
"author": "Morvaridi",
"doi-asserted-by": "crossref",
"first-page": "891",
"journal-title": "Eur. J. Clin. Nutr.",
"key": "ref_43",
"volume": "74",
"year": "2020"
},
{
"DOI": "10.3390/nu13020581",
"doi-asserted-by": "crossref",
"key": "ref_44",
"unstructured": "Noce, A., Marrone, G., Urciuoli, S., Di Daniele, F., Di Lauro, M., Zaitseva, A.P., Di Daniele, N., and Romani, A. (2021). Usefulness of extra virgin olive oil minor polar compounds in the management of chronic kidney disease patients. Nutrients, 13."
},
{
"article-title": "Mediterranean diet as a nutritional approach for COVID-19. Metab",
"author": "Angelidi",
"first-page": "154407",
"journal-title": "Clin. Exp.",
"key": "ref_45",
"volume": "114",
"year": "2021"
},
{
"DOI": "10.3390/nu13010108",
"doi-asserted-by": "crossref",
"key": "ref_46",
"unstructured": "Angelis, A., Chrysohoou, C., Tzorovili, E., Laina, A., Xydis, P., Terzis, I., Ioakeimidis, N., Aznaouridis, K., Vlachopoulos, C., and Tsioufis, K. (2020). The Mediterranean diet benefit on cardiovascular hemodynamics and erectile function in chronic heart failure male patients by decoding central and peripheral vessel rheology. Nutrients, 13."
},
{
"DOI": "10.1016/j.mam.2019.06.001",
"article-title": "Benefits of the Mediterranean diet: Epidemiological and molecular aspects",
"author": "Corella",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Mol. Asp. Med.",
"key": "ref_47",
"volume": "67",
"year": "2019"
},
{
"DOI": "10.3390/nu13062045",
"doi-asserted-by": "crossref",
"key": "ref_48",
"unstructured": "Strasser, B., Wolters, M., Weyh, C., Krüger, K., and Ticinesi, A. (2021). The effects of lifestyle and diet on gut microbiota composition, inflammation and muscle performance in our aging society. Nutrients, 13."
},
{
"DOI": "10.3390/nu14061209",
"doi-asserted-by": "crossref",
"key": "ref_49",
"unstructured": "Baratta, F., Cammisotto, V., Tozzi, G., Coronati, M., Bartimoccia, S., Castellani, V., Nocella, C., D’Amico, A., Angelico, F., and Carnevale, R. (2022). High Compliance to Mediterranean Diet Associates with Lower Platelet Activation and Liver Collagen Deposition in Patients with Nonalcoholic Fatty Liver Disease. Nutrients, 14."
},
{
"DOI": "10.1016/j.clinbiochem.2018.08.004",
"article-title": "Mediterranean diet and platelet-activating factor; a systematic review",
"author": "Nomikos",
"doi-asserted-by": "crossref",
"first-page": "1",
"journal-title": "Clin. Biochem.",
"key": "ref_50",
"volume": "60",
"year": "2018"
},
{
"DOI": "10.3390/nu13020699",
"doi-asserted-by": "crossref",
"key": "ref_51",
"unstructured": "García-Montero, C., Fraile-Martínez, O., Gómez-Lahoz, A., Pekarek, L., Castellanos, A., Noguerales-Fraguas, F., Coca, S., Guijarro, L., García-Honduvilla, N., and Asúnsolo, A. (2021). Nutritional components in Western diet versus Mediterranean diet at the gut microbiota–immune system interplay. Implications for health and disease. Nutrients, 13."
}
],
"reference-count": 51,
"references-count": 51,
"relation": {},
"resource": {
"primary": {
"URL": "https://www.mdpi.com/1648-9144/59/2/227"
}
},
"score": 1,
"short-title": [],
"source": "Crossref",
"subject": [
"General Medicine"
],
"subtitle": [],
"title": "Adherence to the Mediterranean Diet Association with Serum Inflammatory Factors Stress Oxidative and Appetite in COVID-19 Patients",
"type": "journal-article",
"volume": "59"
}
